Neurocognitive Disorders
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
38 Terms
types of neurocognitive disorders
Delirium
Dementia (Alzheimer's and other NCD's)
Frontotemporal lobe disease
Lewy bodies
Vascular dementia
Traumatic brain injury
delirium vs dementia
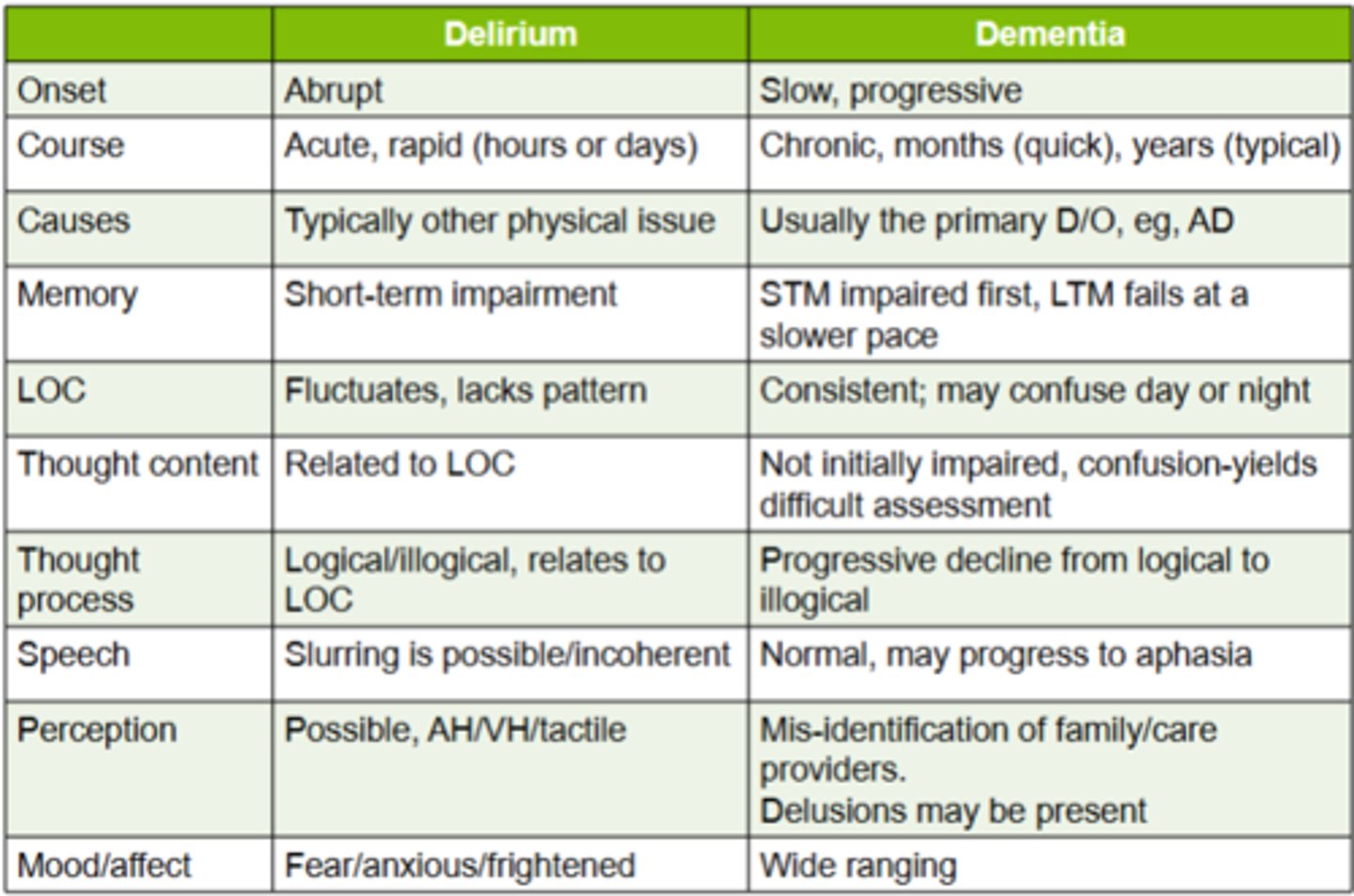
type of delirium
hyperactive: agitation, restlessness
hypoactive: apathy, quiet
mixed: combination
unclassified: manifestations dont fit in either category
delirium causes

nursing interventions for delirium
Prevent physical harm due to confusion, aggression, or fluid and electrolyte imbalance.
Perform comprehensive nursing assessment to aid in identifying cause.
Assist with proper health management to eradicate underlying cause.
Use supportive measures to relieve distress.
#1 Nursing Priority is SAFETY and getting the underlying cause of the delirium treated!
Ex: Terry's story of delirium after his heart surgery - YouTube
dementia characteristics
Insidious onset
Slow, progressive development
Usually a primary disorder, but might be related to other illnesses
Impaired short-term memory
Long-term memory slowly failing
Level of consciousness unchanged
Thought content normal initially, later confusion
Eventual loss of ability to abstract
Misidentification, delusions
Affect alterations 12
dementias, neurocognitive disorders
Alzheimer’s (AD or DAT)
Vascular: if the question mentions cardiac history
Diffuse Lewy Body Disease
AIDS Dementia Complex
Frontotemporal Lobe Dementia (Pick’s Disease)
Parkinson’s Disease: neurological
Creutzfeldt-Jakob Disease: mad cow disease
Huntington’s Disease: chorea, hereditary genetic
Wernicke-Korsakoff: wet brain, thiamine deficiency in alcoholics
Traumatic Brain Injury
alzheimers disease
Alzheimer’s disease (AD) is the most common form of dementia in the elderly affecting more than 5 million Americans.
Cognitive deficits appear and progress gradually/slowly
Loss of short-term memory is an essential feature of AD and is usually its first manifestation.
Loss of memory for _recent events__ is an essential feature of AD and is usually its first manifestation.
Diagnosis is made after all other disorders have been ruled out.
Age is the most significant risk factor; rarely diagnosed before age 60
Hx of head injury, cardiovascular disease, lower levelsof education, and being female are also risk factors.
etiology of alzheimers
Cholinergic Deficit: What neurotransmitter? ach: neurotransmitter used in the PNS and CNS (cognition, memory, concentration)
Neuronal Loss: cerebral cortex, hippocampus, amygdala, forebrain
Neurofibrillary Tangles: cellular nutrition transport
Beta Amyloid Plaques: oxidative stress, free radicals
Genetics
diagnosis of AD
Diagnosis is based primarily on clinical features.
Autopsy of brains of individuals with AD reveals extracellular deposition of amyloid-beta protein, neurofibrillay tangles, senile (neuritic) plaques, and loss of neurons.
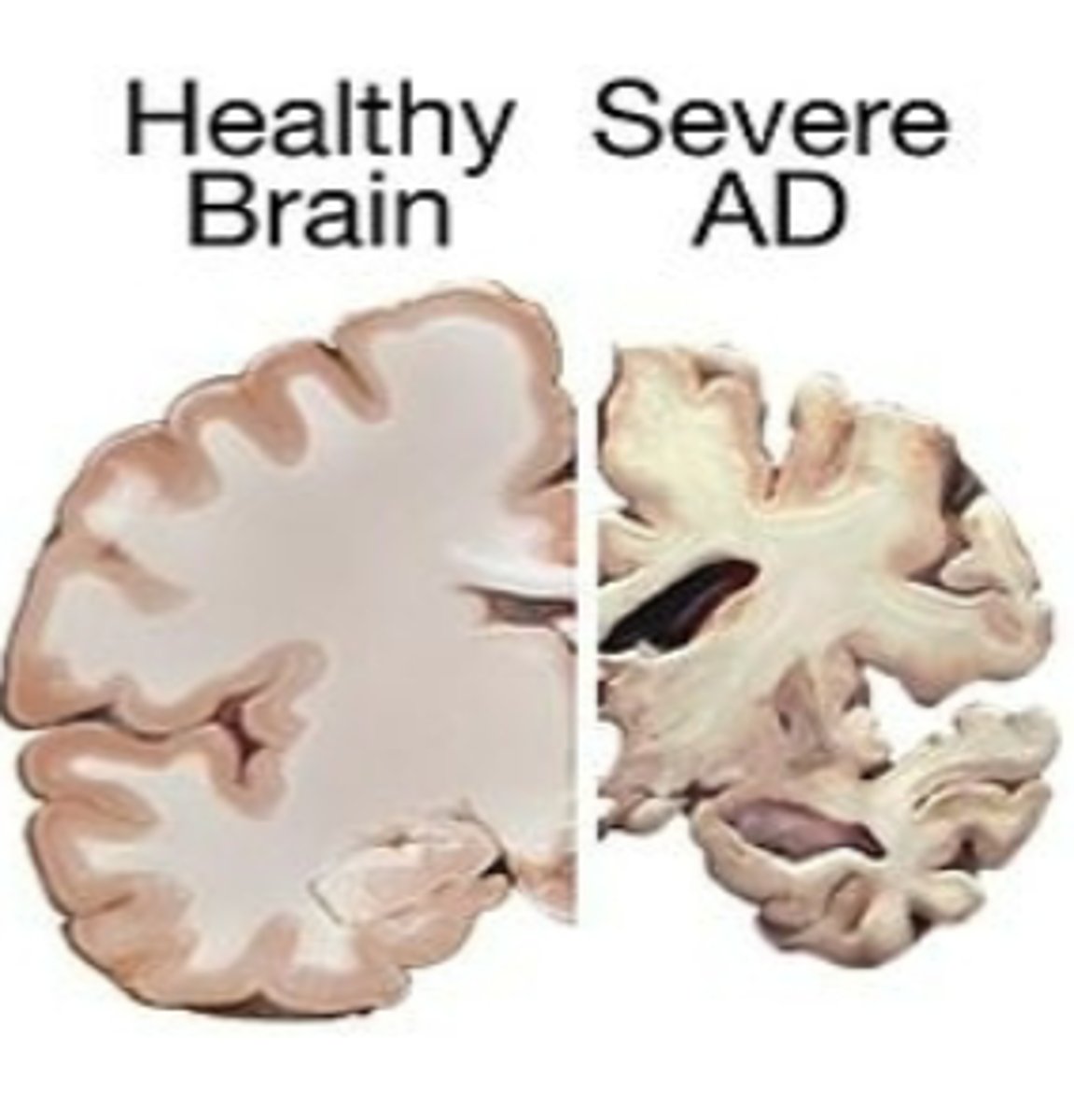
affected areas of the brain alzheimers
Frontal lobe- impaired problem solving, poor judgment, personality changes, aggressiveness
Parietal lobe- inability remain oriented in environment
Temporal lobe- inability to recall words, inability to use words correctly (language comprehension), late stages contributes to delusions and hallucinations
Occipital lobe-unable to recognize familiar objects, impaired language interpretation
Hippocampus- impaired memory STM initially, late stages-unable to form new memories
Amygdala-impaired emotions
four A's of AD
1. Amnesia: memory (both old and new)
2. Aphasia: language
1. Expressive: broca, written or oral: know what they want to say, just cant say it
2. Receptive: wernicke, speak normal, no understanding, content doesent make sense
3. Apraxia: movement
4. Agnosia: Recognition of objects, people
classic behaviors of AS
Word-finding difficulty
Difficulty concentration
Misinterpreting the environment: visual hallucinations (late)
Delusions: dead relatives alive, pathologic jealousy
Pathological jealousy
Stealing odd things
Illusions
Somatic preoccupations
Misidentification
Sundowning- severe (Stage 6); symptoms seem to worsen in the late afternoon and evening (increased confusion and agitation)
Loss of ability to care for oneself
defense mechanisms AD
Denial - Client/Family refuse to believe that changes are taking place
Confabulation - Client makes up stories when questioned about events or activities that they do not remember, can be unconscious attempt to save self esteem
Perseveration - repeats phrases/behaviors
Avoidance of questions
stages of AD: mild
Decreased short-term memory
Word-finding difficulties
Decreased decision-making, concentration, reasoning, judgment
Difficulty performing usual activities
Denial
Getting lost/misplacing objects
Repetitive questioning
stages of AD: moderate
aphasia, Apraxia, agnosia, poor comprehension
Disorientation
Blunted affect
Misidentification
Sleep disturbance
Delusions (later in mild)
Needs help with activities of daily living, supervision with meals
Emotional lability
Wanders
Urinary incontinence
stages of AD: severe
Gait disturbance
Unable to feed self
Urinary and bowel incontinence
Bedridden/require turning q2h
Swallowing difficulty
24-hour supervision
stages of AD
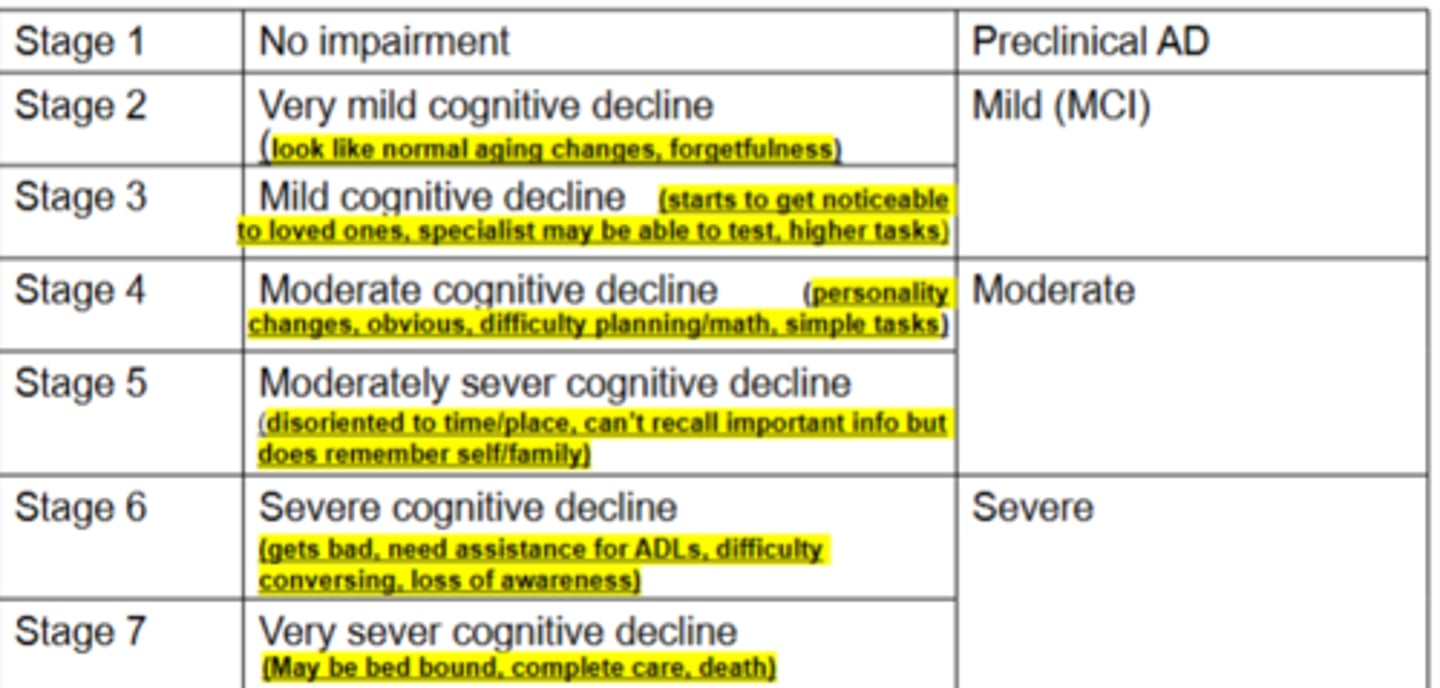
stages of AD cont
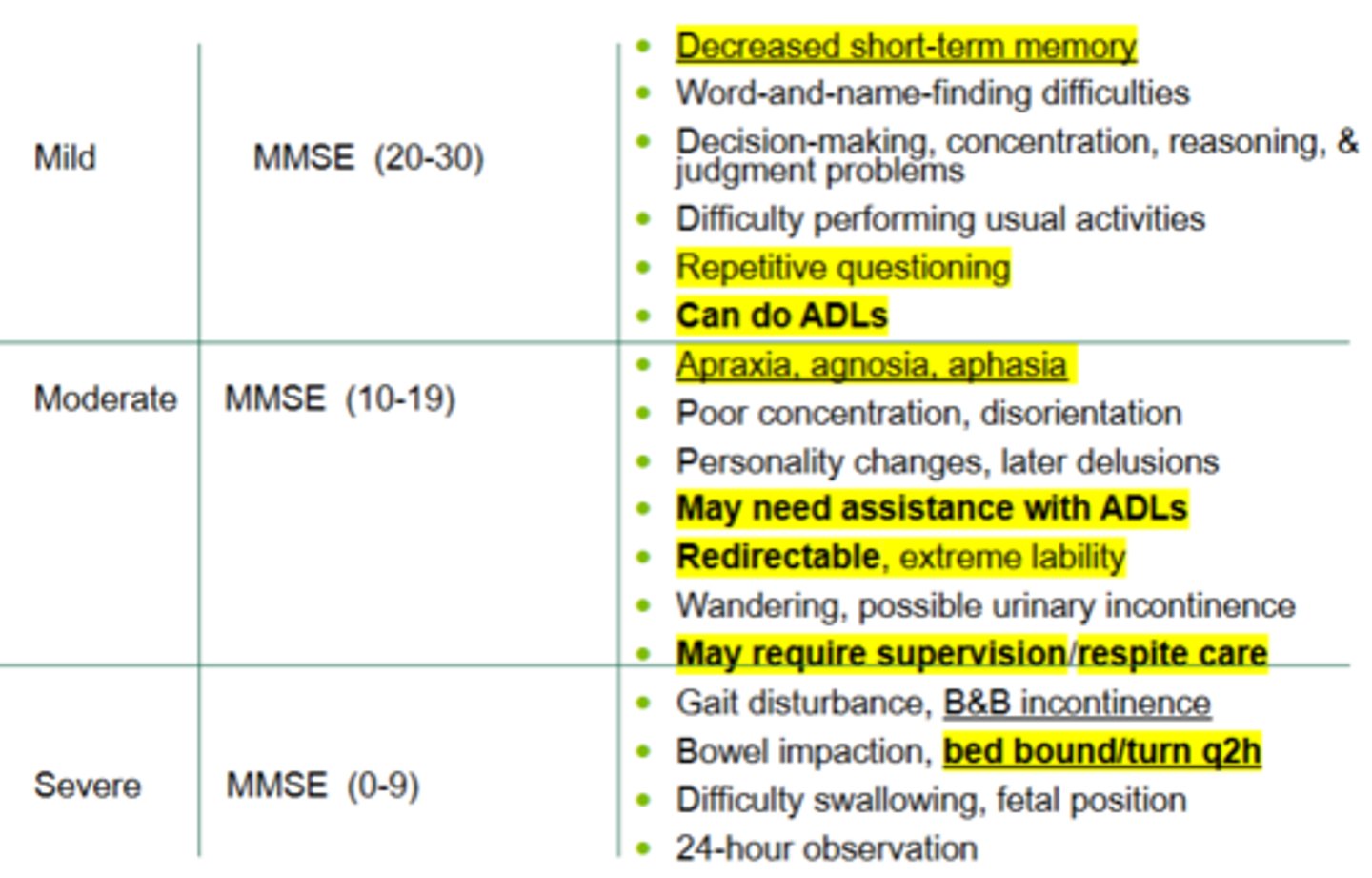
screening assessment tools
Mini-mental status examination (MMSE)
Confusion Assessment Method (CAM)
Neelon/Champagne (NEECHAM) Confusion Scale
Functional Dementia Scale
Brief Interview for Mental Status (BIMS)
Functional Assessment Screening Tool (FAST)
Global Deterioration Scale
Blessed Dementia Scale: uses a secondary sourcelike family
MMSE
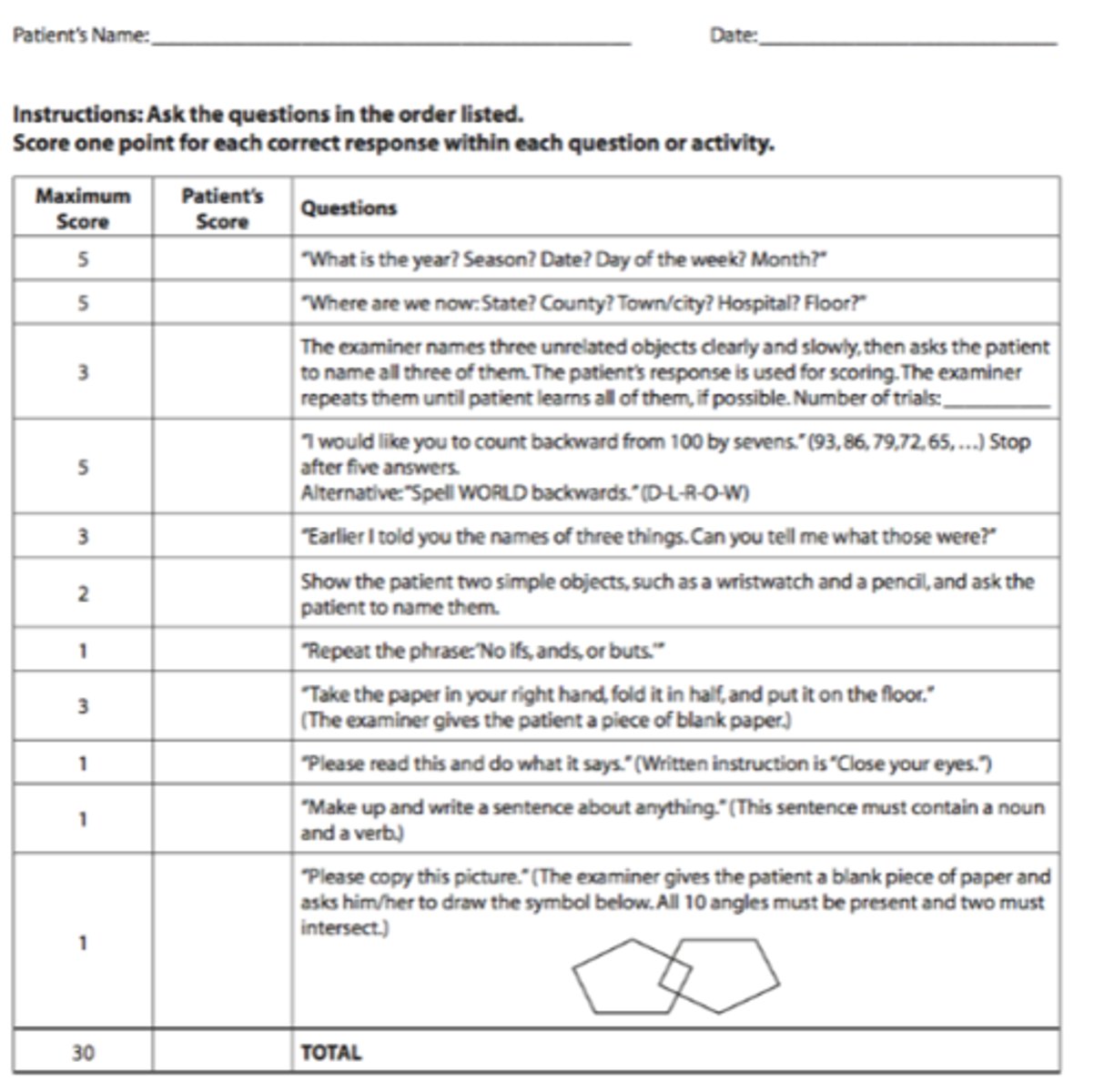
AD involves the death of
brain cells, neurodegenerative
AD risk factors
age, genetics, lifestyle
nursing interventions for AD
Articulate words clearly/provide short simple directions
A calm approach works best
Avoid arguing and go along with the concern followed by therapeutic distraction
Provide prompts and reminders for patients with short-term memory loss
Provide reality orientation for those with higher cognitive functioning
Provide a structured environment with a set schedule
Do not rush the patient
nursing interventions cont
Do not shout if the patient is hard of hearing
Observe patient during ADLs and determine the need for assistance
Set realistic goals – goals will need to be adjusted as the patient’s cognition declines.
Monitor physical needs – assess for visual acuity, hydration, nutritional needs, ability to communicate needs, ability to function safely in environment.
Allow patient to be as independent as possible, as longas possible
Intervene early when the patient begins to escalate
MORE nursing interventions
Interventions are based on the patient’s ability to participate in self-care.
Set realistic goals, dependent on the patient’s level of functioning.
Safety is a special concern, because of abnormal posture and movement.
Be patient and allow extra time for tasks.
Begin safety, fall precautions as needed.
Monitor sleep, hydration, nutrition, elimination, and physical status.
Encourage ventilation of feelings
milieu management AD
Observe patient preference for temperature and lighting
Reduce noxious sounds
TV: purposeful viewing only
Match personalities of roommates when possible
Memory aids
Calendar, notes, illustrated directions
Large-print directions, pill boxes3
community resources for AD
Transportation services
Supervision and care when the primary care giver is out of the home
Information on support groups in the community
Meals on Wheels
Information on respite and residential services
Telephone numbers for help lines
Home health services
Caregiver support
goals for dementia treatments
Restore neurotransmitter loss
Chiefly, acetylcholine (Ach)
Glutamate
Halt neuronal death
psychopharmacology: AD
Acetylcholinesterase inhibitors: for mild to moderate disease
Tacrine (Cognex)
Donepezil (Aricept)
Rivastigmine (Exelon)
Galantamine (Razadyne)
Memantine (Namenda)—for moderate to severe disease; the only approved medication for Alzheimer disease that is not an AChE inhibitor
enzymes
Produced via genetic coding
Drive energy production and material for building blocks of life
Catalyst of metabolic change
Cholinesterase (ChE) breaks down Ach
- ACh can no longer activate cholinergic receptors
- Treatment goal: prevent ACh breakdown by blockingChE37
cholinergic pathways
Selectively destroyed in Alzheimer disease (AD)
1. Inflammation drives selective dysfunction.
2. Immune cells synthesize and degrade Ach.
3. Anti inflammatory cholinergic pathway mediates immunoregulation via cortico-limbic system and nicotinic receptors.
4. Loss of ACh in (a) hippocampus and (b) amygdala causes memory loss.
psychopharmacology
Majority of Alzheimer medications work within CNS (cerebral cortex)
Acetylcholinesterase (AChE) & butyrylcholinesterase (BuChE) are enzymes that terminate the actions of acetylcholine.
Used in mild to moderate AD
Acetylcholine loss occurs in people with Alzheimer’s Disease. The goal of these meds is to increase the level of acetylcholine and therefore slow disease progression and improve cognition.
Cholinesterase inhibitors
- Aricept (donepezil) - (AChE) inhibitor
- Exelon (rivastigmine) - (AChE) & (BuChE) inhibitor
- Razadyne (galantamine) - (AChE) inhibitor
Adverse effects: _facial flushing, leg cramps, GI (n/v and diarrhea),bradycardia, syncope (take Aricept at night to sleep through theside effects of that cause fainting from the irregular heartbeat)
Contraindicated: Asthma/COPD-increase Ach can lead to bronchoconstriction
cholinesterase inhibitors
Elevate ACh levels to prolong cognitive abilities.
Temporarily mask neurodegeneration.
Improve function but do not slow disease
what are the cholinesterase inhibitors
Tacrine—Cognex
- Inhibited both AChE and BChE
- Discontinued: severe hepatotoxicity
Donepezil—Aricept
- More selective for AChE; reversible inhibitor
Rivastigmine—Exelon
- Irreversible inhibitor of ChE
Galantamine—Razadyne
- Preference for AChE over BChE
- Can stimulate presynaptic muscarinic receptors: fewerSEs42
agents that may retard neurodegeneration
NMDA receptor inhibitors
- Memantine—Namenda
- Could theoretically prevent neuronal death
Secretase inhibitors
- Serious side effects with these drugs
Dihydropyridine calcium channel blockers
- Possible new preventive tools to slow vessel changes
namenda (memantine)

possible drugs to prevent AD
Strategies being tested to modify progression include
NSAIDs
Statins
Estrogen
Antioxidants
B and E vitamins
Antiamyloid immunotherapy