lecture 18 -- barrier defenses
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
adaptive vs innate immunity
innate — rapid, non-spec.
adaptive — slower, very specific (^ effective)
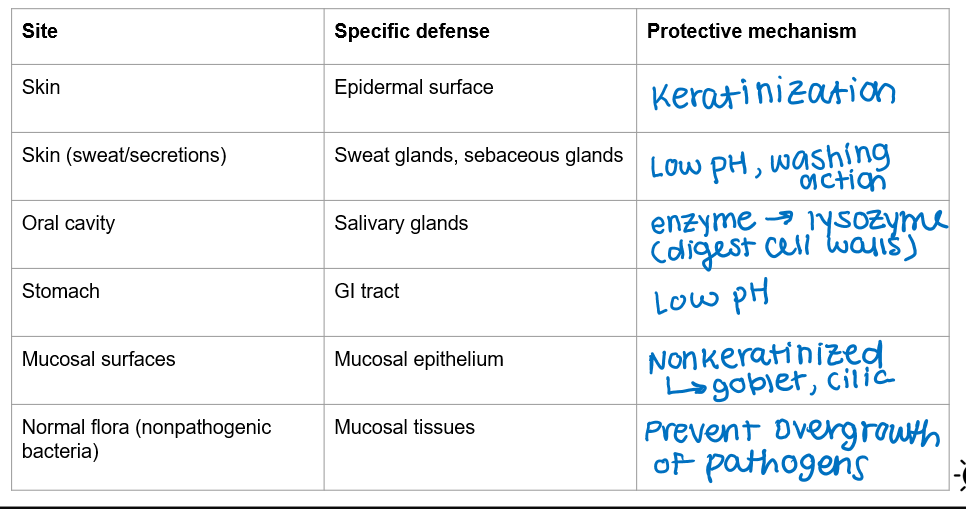
barrier defenses
site | specific defense | protective mechanism
skin — epidermal surface — keratinization
skin (sweat/secretions) — sweat glands, sebaceous glands — low pH, washing action
oral cavity — salivary glands — enzyme → lysozyme (digest cell walls)
stomach — GI tract — low pH
mucosal surfaces — mucosal epithelium — nonkeratinized → goblet, cilia
normal flora (nonpathogenic bacteria) — mucosal tissues — prevent overgrowth of pathogens
cells of innate immune response — phagocytes
fast acting
first line of defense after barriers
engulf particles/cells
main types involved in innate immunity
macrophages/monocytes, neutrophils
some pathogens are easily cleared by phagocytes, others have become resistant
cells of innate immune response — NK cells
natural killer cells
type of lymphocyte
can induce apoptosis 2 ways:
extrinsic apoptosis via fas ligand
intracellular apoptosis via perforins and granzymes
cell recognition mechanism unclear
extrinsic apoptosis via fas ligand for NK
external fas R connected to fas-associated DEATH DOMAIN (FADD)
intracellular apoptosis via perforins and granzymes
perforins = form pores on infected cell membranes
granzymes = trigger apoptosis
macrophages
type of while blood cell
irregularly shaped
agranulocyte
versatile - can be fixed or mobile; participate in various physiological processes
present in many tissues; primary location = body cavities/organs
monocytes are the precursors for macrophages
neutrophils
type of white blood cell
granulocytes
granules = vasoactive mediators
circulate in the blood, attracted to infected tissues via chemotaxis (directed migration in response to chemical signaling)
primary location = blood
pattern recognition receptors (PRRs) — what are they, what patterns do they recognize? present where?
immune cells recognize patterns of pathogen-specific molecules using PRRs
PRRs = membrane-bound receptors that recognize pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs)
PAMPs'/DAMPs can be on pathogens or body cells
PAMPs'/DAMPs may be soluble molecules or structural characteristics
PRRs can be present
intracellularly → endosomal or cytosolic
extracellularly → cell surface or soluble
soluble mediators of innate immune responses (cyto and chemo)
cytokines
signaling molecules for short distance communication
secreted into the receiving cells’ intracellular space; induces change
chemokines
similar function to cytokines, but long distance
facilitate chemotaxis
soluble mediators of innate immune responses? (early induced proteins)
not constitutively present; made as needed
ex: interferons
cells infected with viruses secrete interferons
the interferons induce adjacent cells to make antiviral proteins
phagocytes also have receptors for EIPs
enhances phagocytosis via opsonization
“tag” a pathogen for phagocytosis
soluble mediators of innate immune responses — the complement system
series of constitutive proteins in blood plasma
made in the liver
function in the adaptive immune responses too
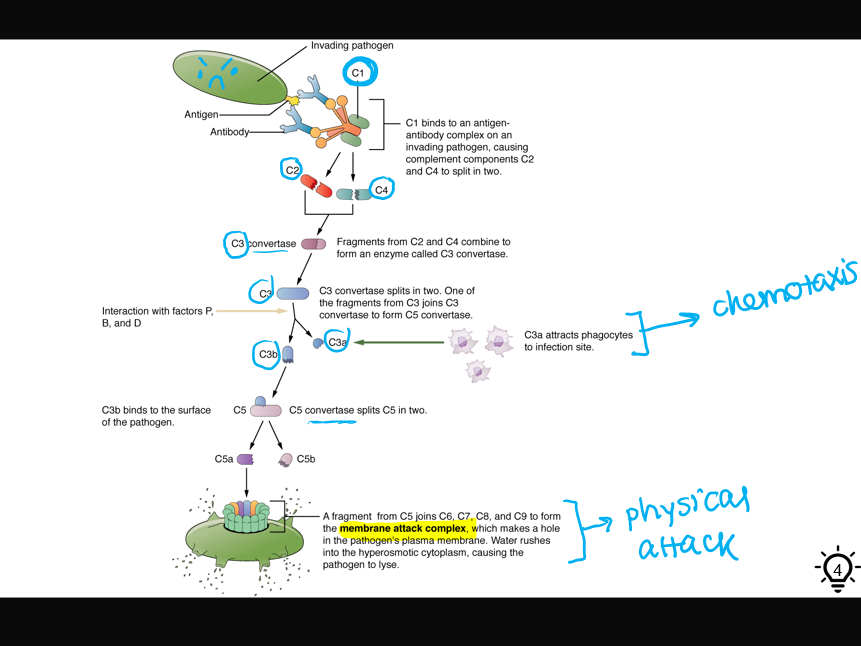
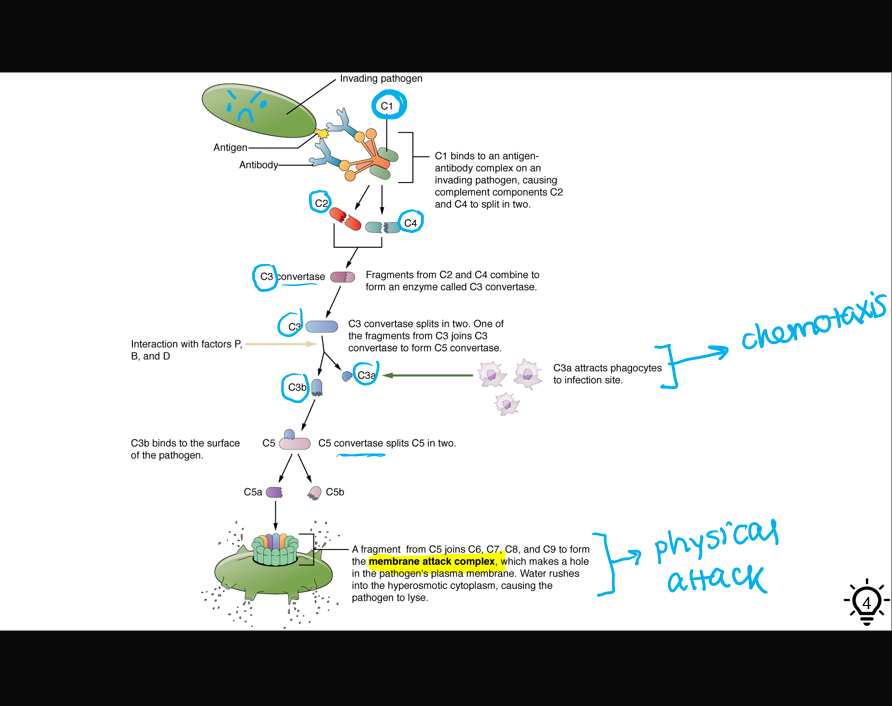
once the first protein (C1) is activated, it triggers a cascade of events that will result in 3 things:
opsonization of the pathogen
chemotaxis of phagocytes
physical destruction of the pathogen
** not part of early immune response
the inflammatory response
hallmark of the innate immune system response
4 characteristics: heat, redness, pain, swelling
does not have to be initiated by infection
recruits phagocytic cells to clear cellular debris and prep for wound repair
recruits other innate immune cells to clear potential infection
isolates the site — prevent/decrease spread of any pathogens
may be acute or chronic
4 phases of inflammatory response
tissue injury
injured cell → release contents → stimulate release mast cell granules + inflammatory mediators (IMs)
vasodilation
inflammatory mediation cause vasodilation
relaxing vascular smooth muscle
^ heat, ^ redness, ^ access
^ vascular permeability
stimulated by IMs
causes fluid to leak into interstitium → edema
phagocyte recruitment
LOTs of chemotaxis, neutrophils, macrophages
pus → accumulated cellular remains of phagocytes (purulent)