Final review 203 combined flash
1/1108
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
1109 Terms
ITLS
globally recognized program designed to train prehospital providers in the rapid assessment and treatment of trauma patients. Emphasizes a structured, systematic approach to trauma care to improve survival and outcomes. One of the only EMS-specific courses
ITLS key concepts
Systematic approach:•Using the primary and secondary survey to identify life-threatening injuries quickly.⚬Uses ABCDE (Airway, Breathing, Circulation, Disability, Exposure/Environment) as a core framework.
High-Performance Teamwork
•Coordinating effectively with other responders on scene.
Evidence-Based Interventions
Following best-practice guidelines for airway management, shock treatment, and spinal immobilization
Scene Safety & Triage
•Assessing hazards, prioritizing care, and determining transport urgency.
GOALS OF ITLS
1.Provide rapid and accurate patient assessment in the prehospital setting.
2.Deliver immediate life-saving interventions for trauma patients.
3.Enhance decision-making and critical thinking under stress.
4.Promote team coordination and patient safety during emergency responses.
PRIMARY SURVEY
•Perform scene size-up
•Conduct initial assessment
•Perform rapid trauma survey or focused exam
•Make critical interventions
•Prepare for transport
•Contact OLMC if needed
SECONDARY SURVERY
•Repeat initial assessment
•Repeat vital signs and consider monitors
•Perform neurological exam
•Conduct detailed head-to-toe assessment
REASSESSMENT
•Repeat initial assessment
•Repeat vital signs and monitor
Reassess abdomen, check for injuries and interventions
BLUNT TRAUMA
•Motor Vehicle Collisions (MVC)
•Falls
•Struck by object / impact injuries
PENETRATING TRAUMA
•Stab wounds/knife injuries
•Gunshot wounds/ballistics
•Impaled objects causing injury
•Penetrating objects that breach the skin
OTHER TRAUMA
•Blast injuries / explosions
Understanding MOI
helps predict injury patterns and severity for rapid assessment and intervention.
PRIMARY GOALS
•Minimize injury and reduce preventable death
Prevent secondary insults (e.g., hypoxia, hypotension, hypothermia
ASSESSMENT & INTERVENTION: X-ABC
•X – eXtanguishing injuries (severe bleeding control)
•A – Airway
•B – Breathing
•C – Circulation
TRAUMA TRIAGE DECISIONS
•When in doubt, transport to a trauma center, if it will take a long time to reach a definitive care facility. •Assess need for air transport
PREVENTION & PUBLIC EDUCATION
•Promote injury prevention programs
•Increase public awareness of trauma risks
ITLS patient assessment
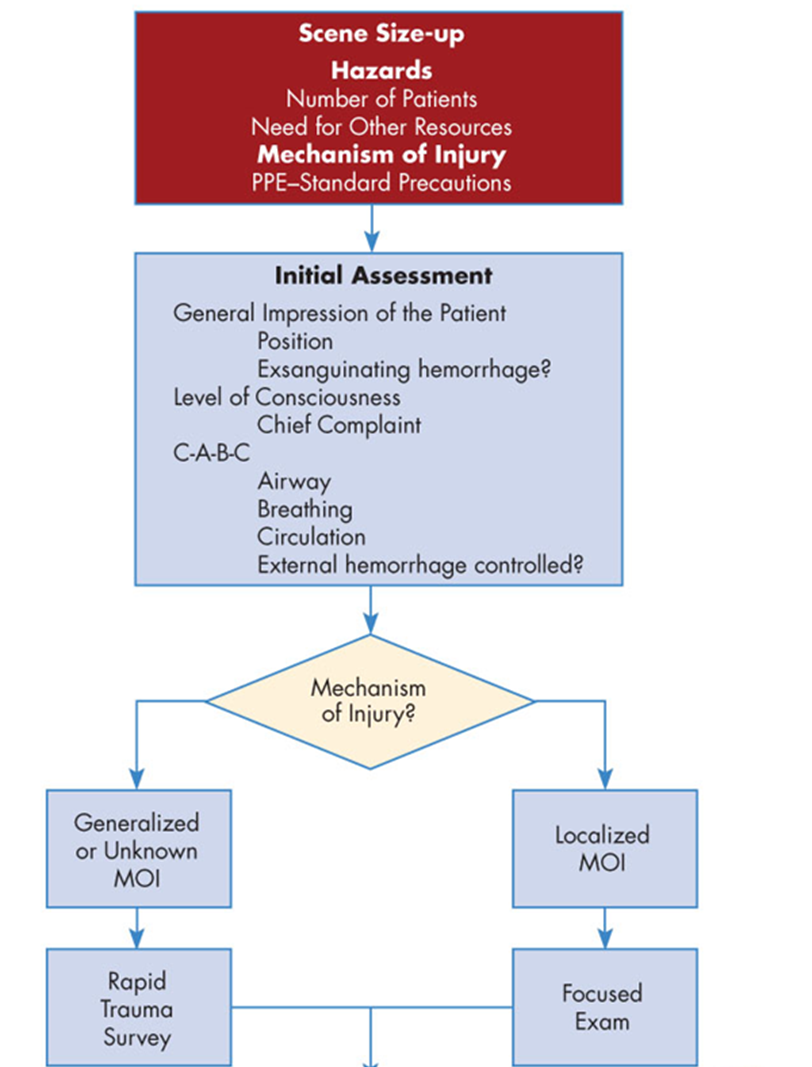
Scene Size-Up
•Establish medical command / incident command
•Perform PPE and control hazards
•Request additional resources as needed
•Begin triage in multi-patient events
Initial Assessment & Interventions
•Reposition patient if necessary
•Control bleeding: direct pressure, hemostatic gauze, tourniquet
•Airway management: open airway, assist ventilations, provide oxygen
•Begin CPR if indicated
•Perform rapid extrication if patient safety or access requires
Survey Selection
Deciding Which Survey to Perform
•Base primary survey choice on:
⚬Mechanism of Injury (MOI)
⚬Initial patient assessment
Rapid Trauma Survey (Load & Go Patients)
•Indications: life-threatening injuries
•Critical Actions:
⚬Decompress tension pneumothorax (ALS)
⚬Seal open chest wounds
⚬Apply spinal motion restriction (SMR) if indicated after assessment
Transport & En route
Load & Go (Rapid Transport)
•Rapid transport to trauma center (ground or air)
•Early notification to receiving facility
•Establish IV en route, administer TXA if indicated (ALS)
•Continuous monitoring and reassessment
Not Load & Go (Stable Patient)
•Complete secondary survey
•Establish IV access en route
•Monitor and reassess vital signs
•Perform splinting and wound care as needed
Critical actions critical thinking
Always prioritize life-threatening conditions first, but adapt interventions based on patient stability and transport urgency.
ITLS PATIENT ASSESSMENT Key responsibilities
•Delegate interventions to team members during the primary survey
•Do not interrupt the completion of the primary survey except for:
⚬Scene danger or hazards
⚬Exsanguinating hemorrhage
⚬Airway obstruction
⚬Cardiac arrest
Key Point:
•The team leader ensures efficient workflow, patient safety, and situational awareness while allowing the team to complete the primary survey rapidly and effectively.
Portage trauma assessment
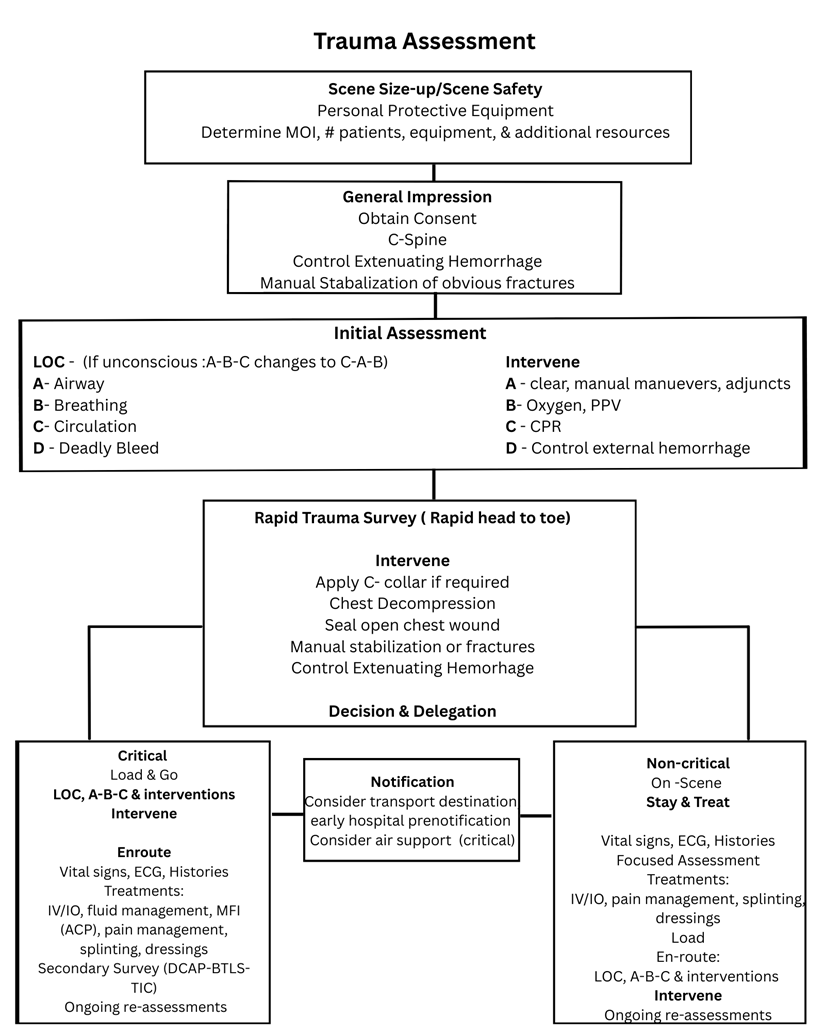
SCENE SIZE UP/SCENE SAFETY
Are there any hazards?
•People, odors, pets, live wires, crowds, egress path, fire
How many patients need assistance?
What is the MOI?
Do you need additional resources?
•Law enforcement, additional EMS units (ALS, BLS), air support, fire, hazmat, and an electrical company
What is the environment?
•Weather, safety concerns
Do you have appropriate PPE – Personal Protective Equipment on before approaching the patient?
Are bystanders on scene for additional information?
Is the scene information the same as the information dispatch gave you?
GENERAL IMPRESSION
As you approach the patient, observe:
What is the patient’s age, sex, weight, and height?
What is the patient's position?
•Relaxed
•Sitting, standing, ambulatory
•Supine, recumbent
•Tripod
•Pacing
Observe the Level of activity and/or distress the patient is displaying.
•Work of breathing
•Anxiousness
•Fatigue
•Not moving (unresponsive)
•Patient tracking, you or not aware of your presence
Note the skin color and condition.
Introduce yourself and obtain Consent
C-SPINE/SMR ITLS RECOMENDATIONS
Consider SMR when any of the following are present:
Patient Complaints / Clinical Findings
•Spinal deformity or visible injury
•Pain or tenderness along the spine
Trauma Mechanism / Patient Condition
•Blunt trauma with altered level of consciousness (LOC)
•High-energy mechanism of injury (e.g., MVC, falls > 3m)
•Drug or alcohol impairment affecting mental status
Neurological Considerations
•Focal neurological complaints
•Unable to adequately assess for spinal injury clinically due to altered LOC or distracting injuries
Key Point:
•When in doubt, apply SMR to protect the spine until full assessment can be performed.
INITIAL PATIENT ASSESSMENT
PEARLS – C-A-B-D-E
C – Control Life-Threatening Bleeding
•Direct pressure, hemostatic gauze, tourniquet
A – Airway
•Open airway, assist ventilations, suction if needed
B – Breathing
•Assess respiratory effort, provide oxygen, manage chest injuries
C – Circulation
•Check pulses, control bleeding, monitor perfusion
D – Disability (Neurologic Status)
•Assess level of consciousness, pupils, GCS
E – Exposure & Environment
•Fully expose patient to identify injuries
•Prevent hypothermia, maintain scene safety
idea
Vectors
The average direction and strength of ventricular depolarization.
Axis Deviation
The direction in which the main vector of depolarization points in the frontal plane.
R-Wave Progression
The change in height of the R wave across the precordial leads from V1 to V6.
Ventricular Hypertrophy
Structural thickening of the ventricular myocardium due to chronic pressure or volume overload.
Bundle Branch Block
A blockage of the electrical conduction pathways in the ventricles.
Fascicular Block
A block in one of the divisions of the bundle branches.
Ischemic Mimics
Conditions that can present similarly to ischemia on an ECG.
Diagnostic Pitfalls
Common errors or misunderstandings that may lead to incorrect diagnoses.
ST Elevation
A change in the ECG that indicates that the heart is not receiving enough blood.
J-Point
The point on the ECG where the QRS complex transitions into the ST segment.
Inferior STEMI
Myocardial infarction affecting the inferior wall of the heart.
Anterior STEMI
Myocardial infarction affecting the anterior wall of the heart.
LBBB
Left Bundle Branch Block; a blockage affecting the left side of the heart's conduction system.
Reciprocal Changes
ECG changes that are mirrored in the leads opposite to the leads showing indicative changes.
Hyperkalemia
An elevated level of potassium in the blood, which can affect heart rhythm.
Brugada Syndrome
A genetic condition that can lead to dangerous arrhythmias.
WPW Syndrome
Wolff-Parkinson-White Syndrome; a condition where an additional electrical pathway in the heart can lead to rapid heart rates.
PE
Pulmonary Embolism; a blockage in one of the pulmonary arteries in the lungs.
LVH
Left Ventricular Hypertrophy; thickening of the heart's left ventricle.
Ventricular Paced Rhythms
ECG rhythms resulting from an artificial pacemaker.
Electrical Axis
The net direction of electrical activity during ventricular depolarization.
Hexaxial Reference System
A method to determine the electrical axis of the heart using the six frontal limb leads.
Left Axis Deviation (LAD)
A change in the direction of the heart's electrical axis towards the left.
Right Axis Deviation (RAD)
A change in the direction of the heart's electrical axis towards the right.
Extreme Axis Deviation
An axis deviation that occurs between -90° and -180° or 90° and 180°.
Classic STEMI Criteria
Defined by specific ST elevation patterns in contiguous leads on an ECG.
De Winter Pattern
Up-sloping ST depression at the J-point in V1-V6 with tall, symmetric T waves, indicating LAD occlusion.
Wellens' Syndrome
A warning pattern indicating critical proximal LAD stenosis.
Pneumonic for STEMI Locations
A memory aid to remember the anatomical regions affected by ST elevation.
Height Measurement for LVH
The criteria used to assess the voltage changes that indicate left ventricular hypertrophy.
Sokolow-Lyon Criteria
A measure used to screen for left ventricular hypertrophy by combining R and S wave measurements.
Poor R-Wave Progression
Decreased size of R waves from V1 to V6; often signifies anterior MI or LVH.
Causes of Poor R-Wave Progression
Includes conditions such as left bundle branch block, anterior MI, tension (LVH), and emphysema.
Common Questions - Cardiac Axis
Questions typically asked regarding interpretation and implications of axis deviations.
Acute Coronary Syndrome
A range of conditions associated with sudden reduced blood flow to the heart.
Dysrhythmia
An irregularity in the rhythm of the heartbeat.
Electrolyte Imbalance
An abnormal level of electrolytes in the body, which can affect heart function.
ST Segment Morphologies
The various shapes of the ST segment that can indicate different cardiac conditions.
ECG Lead Placement
The correct positioning of leads on the body to accurately record the electrical activity of the heart.
T Wave
The part of the ECG that represents ventricular repolarization.
Troponin
A protein released during heart muscle damage; often checked to diagnose myocardial infarction.
Strain Pattern
Changes on the ECG that indicate stress on the heart muscle usually seen in VT or RVH.
Rise in myocardial oxygen demand
The need for increased oxygen by the heart muscle during stress or activity.
Electrophysiological Changes
Alterations in the electrical activity of heart tissue caused by various conditions.
ECG Interpretation
The process of analyzing an electrocardiogram to assess heart function.
Reciprocal ST Depression
ST segment depression observed in leads opposite to those showing ST elevation.
Cardiac Myocyte
A muscle cell of the heart, responsible for its contraction.
Echocardiogram
An ultrasound of the heart used to visualize heart structures and function.
Cardiac Compliance
The ability of the heart to expand and fill with blood.
Atrial Fibrillation
An irregular, often rapid heart rate that can increase the risk of strokes.
Septal Infarction
An infarction that affects the septum (the wall between ventricles) of the heart.
ST Segment Depression
A downward deviation of the ST segment from the baseline, often indicating ischemia.
Critical Lesion
A blockage in a coronary artery that significantly impairs blood flow to the heart.
Pulmonary Hypertension
Increased blood pressure in the pulmonary arteries, which can lead to RVH.
Cor Pulmonale
Right heart failure due to lung disease.
Heart Failure
A condition in which the heart is unable to pump sufficiently to maintain blood flow.
Diagnosis
The identification of the nature of an illness or condition.
Cardiac Monitoring
Continuous observation of heart activity using electrocardiography.
Rescue Intervention
Emergency procedures performed to restore normal heart function.
Electrocardiographic Changes
Alterations in the ECG patterns that can indicate various cardiac conditions.
Lateral Wall Infarction
Infarction affecting the lateral wall of the heart, typically seen in V5 and V6.