PHYS C3
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
Ionisation mechanisms
physical process of energy transfer
Direct ionisation
Particle’s positive charge attracts electrons from surrounding atoms, creating ions by pulling them out of shell
Particles’s negative charge exerts repulsive force on atom’s electrons, ejecting it from shell
Indirect ionisation
Electrically neutral particles/rays transfer energy to surrounding atomic electrons inducing photoelectric effect or Compton scattering, creating ions
Compton scattering
X-ray photon collides with an electron, transferring a fraction of its energy. Causes photon to change direction and electron to be ejected
Linear Energy Transfer (LET)
Rate of energy absorption in the medium, keV/μm
High LET
densely ionising
deposits large amount of energy over very small area
produces essentially all direct action in DNA
e.g alpha particles
Medium LET
moderately ionising
energy deposit depends on speed of neutron (fast moving = little energy deposit)
produces predominantly direct action in DNA
e.g protons and neutrons
Low LET
does not give up energy quickly
deposits energy over a large distance
produces predominantly indirect action in DNA
e.g x-ray and γ-ray photons - produce fast moving electrons that deposit their energy sparsely
Radiation Injury
Ionisation energy may be transferred through a chain of chemical reactions and free radicals formation, causing irreversible damage to important cellular molecules
Radiosensitive cell site
DNA molecule within the nucleus
DNA
DNA’s large size makes it a ready radiation target
DNA damage is the main reason for biological and health effects
Secondary charged particles
Produced when a neutral particle/ray interacts with an atom, transferring kinetic energy and causing the emission of a charged particle
Free radical
Uncharged molecule that contains a single unpaired electron in the outer shell
Direct Action
Occurs when absorbed ionisng energy or secondary charged particles deposit energy in the target atom causing direct ionization or excitation and thus breaking chemical bonds in DNA
Indirect Action
Body absorbs radiation (usually low LET) which ionises cellular water, producing ion pairs and free radicals (like hydroxyl radicals, OH*). The free radicals cause potentially repairable ionizing damage to DNA but in the presence of O2, they react to form DNA peroxyl radicals which creates chemically stable lesions, permanently damaging DNA (oxygen fixation hypothesis)
Exposure
flow of photons per unit time (photon flux) through a point of interest in air at a given distance from a radiation source
Unit: C/kg
KERMA
Kinetic energy released per unit mass
The amount of kinetic energy transferred to the electrons released in photon-matter interactions
Unit: Gy (1 J/kg)
relates energy released in matter to energy absorbed in matter to determine extent of biological effect
Absorbed Dose
Amount of radiation energy absorbed by medium
This can be from scattered radiation in the room as well as directly from source’s beam
Unit: Gy (1 J/kg)
Equivalent Dose (HT)
Sum of absorbed dose of all radiation types multiplied by radiation weighting factor (wr) which accounts for differences in biological effectiveness between radiation types
when wr=1, equivalent dose = absorbed dose
Unit: Sv (also 1J/kg but only used for HT)
Most important for radiation therapists
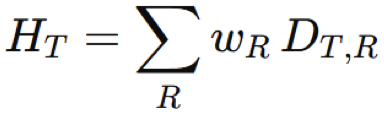
Radiation weighting factor (wr)
Photons, electrons, myons = 1
protons, charged pions = 2
Alpha particles, heavy ions, fission fragments = 20
Effective Dose (E)
the sum over tissues and organs of the equivalent dose HT multiplied by the tissue weighting factor wT (organs sensitivity to radiation)
If more than one organ is exposed sum the effective doses to all exposed organs
If only part of organ is exposed, dose is averaged over whole organ not just exposed area
Accounts for stochastic cancer risk and heritable effects allowing estimation of whole body risk
Most important for radiographer
Unit: Sv
Functional Sub-Units (FSU)
compartment of an organ that performs part of the organ's function
Total damage to an organ (tissue response) depends on how many FSUs are destroyed
FSU Arrangements
Serial: each FSU in a line, if one FSU fails organ experiences harmful effects, organs susceptible to high point (hot spot) doses - where radiopharmaceutical is concentrated in one area, e.g spinal cord, oesophagus
Parallel: each FSU functions independently, loss of one FSU leads to a slight decrease in organ function, organs more sensitive to volume effects - toxicity caused by large number of FSUs being irradiated, e.g liver, kidneys
Mixed organs: combination of serial and parallel, e.g lungs, brain
Biological Response
Cells respond to DNA damage and protein and lipid oxidation within minutes by changing the activation of certain genes and modifying proteins
Types of Effects
Stochastic effects
Tissue Reactions
Stochastic effects
random
long-term
probability increases with dose
no threshold dose
severity does not depend on dose
caused by accumulated exposure
dominant concern in diagnostic imaging
e.g hereditary effects, radiation carcinogenesis
Natural Incidence
The background radiation dose (not from medical radiation procedures) at which a disease occurs spontaneously (‘normal risk’)
Tissue Reactions
immediate
whole body doses of >1Gy needed
severe
there is a threshold dose below which no effect is seen and for which repair mechanisms will prevent effects
above the threshold, effects always occur and severity increases with dose
different effects, tissues and people have different threshold doses
Dominant concern in radiation therapy and lengthy high-dose-rate fluoroscopic procedures
e.g hair loss, sterility (inability to conceive), cataracts (blurry vision)
Thresholds
No Observed Effects (<100 mSv)
Increased Cancer Risk (100 mSv+)
Radiation Sickness (0.5 Sv - 1 Sv)
Lethal Doses (>10 Sv)
Acute Radiation Syndrome
acute illness caused by irradiation of entire body by a high dose of penetrating radiation in minutes
Radiation Sickness: 4 Organ Systems
Cutaneous (C)
Haematopoietic (H)
Gastrointestinal (GI)
Neurovascular/Cerebrovascular/Central Nervous System (N/CV/CNS)
Cutaneous (C)
hair follicle damage (epilation) and skin damage
Few hours = itching and erythema (redness)
Days/weeks = increased reddening and ulceration
Possible regeneration
High doses can be permanent
Haematopoietic (H)
0.7–10 Gy
bone marrow and lymphatic organs damage
causes drop in blood cell counts
results in infection and haemorrhage
usually death within weeks
Gastrointestinal (GI)
>8 -10 Gy
destroys intestines lining
causes severe diarrhea, dehydration, electrolyte imbalance and sepsis
death within 2 weeks
Neurovascular/Cerebrovascular/Central Nervous System (N/CV/CNS)
>20 Gy
Brain and cardiovascular system damage
causes extreme nervousness, confusion, nausea, vomiting, loss of consciousness and circulatory collapse
Death within hours to a few days
Treatment Goals
manage symptoms, prevent infection and support the body's recovery from bone marrow damage
Treatment Options
Immediate decontamination via washing skin and clothing
Supportive care via fluids, antibiotics, pain relief, and blood products
Specific Medical Countermeasures like Potassium Iodide to protect thyroid from radioactive iodine, Hematopoietic Stem Cell Transplant (HSCT) for severe bone marrow damage if cytokine therapy fails, and Prussian Blue to help remove internal cesium and thallium
Embryo and Foetus Radiation Effects - Cancer
In-utero exposure of dose >10–20 mGy = increased stochastic risk of childhood cancer, particularly leukaemia (6% per Gy)
Embryo and Foetus Radiation Stages
Pre-implantation: first days of pregnancy, highest risk of death, if fetus survives they will be symptom free
Organogenesis: first weeks, highest risk of malformations
Fetus: until birth, highest risk of growth and mental retardation, lowest death risk
Why is baby’s likelihood of death highest in earliest stage of pregnancy?
Baby has:
Rapid cell division
Less capacity for DNA damage repair
Higher likelihood that a single mutation is propagated.
Relative risk
is compared to a baseline risk (natural rate), it is not a measure of the absolute chance of something occurring
e.g if RR = 1.3 it is 1.3 times the baseline risk