4 - Implant-Assisted Removable Dentures - Combined Lectures (Dr. Muftu)
1/164
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
165 Terms
Edentulism
What has the following characteristics?
- Is an international problem, particularly in the older age groups
- Remains as an incurable, functionally and psychologically disruptive illness
True
T/F: Fixed or removable complete dentures utilizing dental implants may help in rehabilitation of lost function, esthetics, phonetics, and improve patient satisfaction
Moderate to severe bone loss
Reduced chewing function
Poor fitting dentures/sore spots
Digestive and nutritional problems
What are 4 clinical consequences of edentulism?
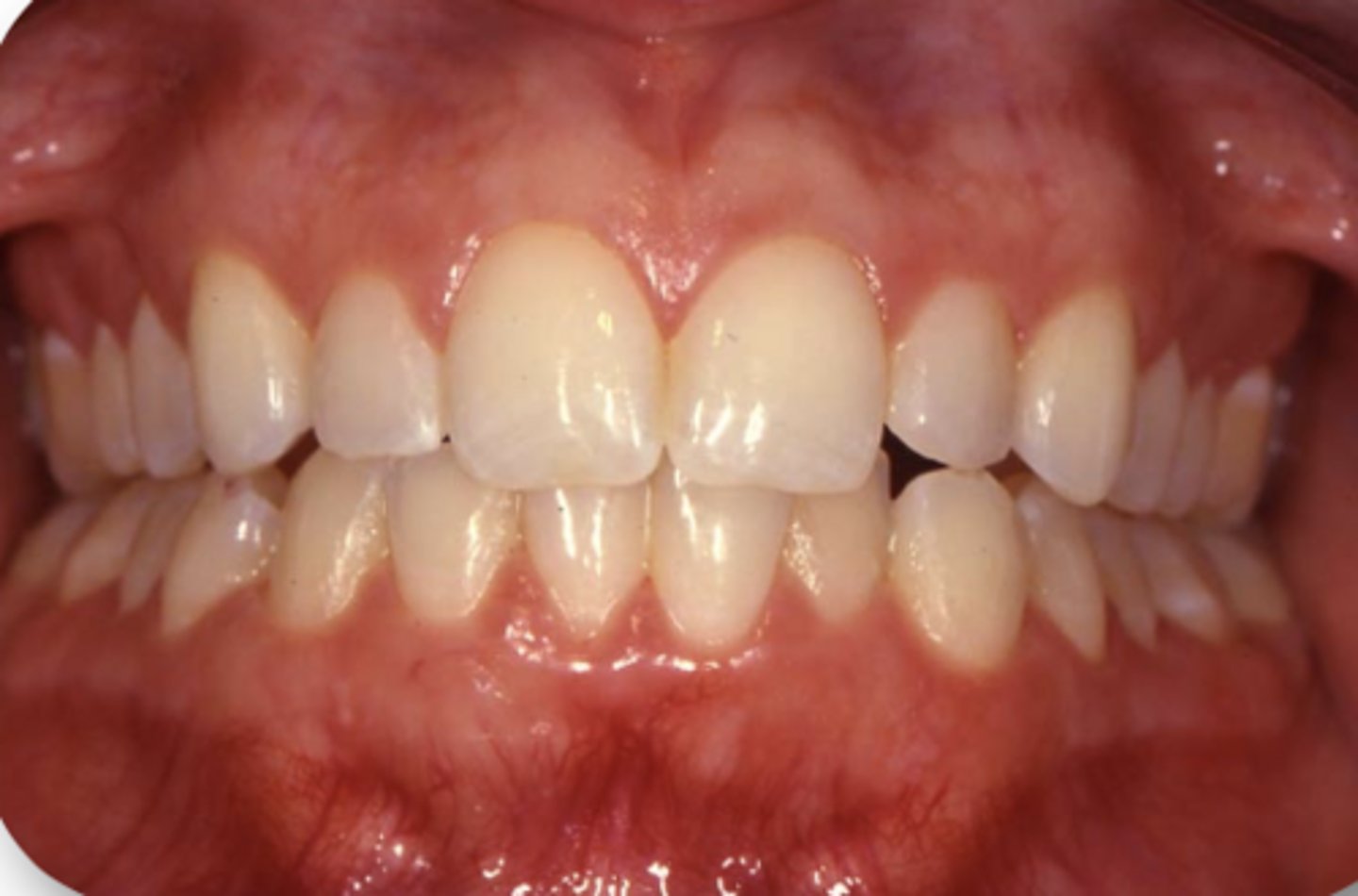
~45 cm^2
In a full, healthy dentition, there is about ___square centimeters of pericemental/periodontal support per arch
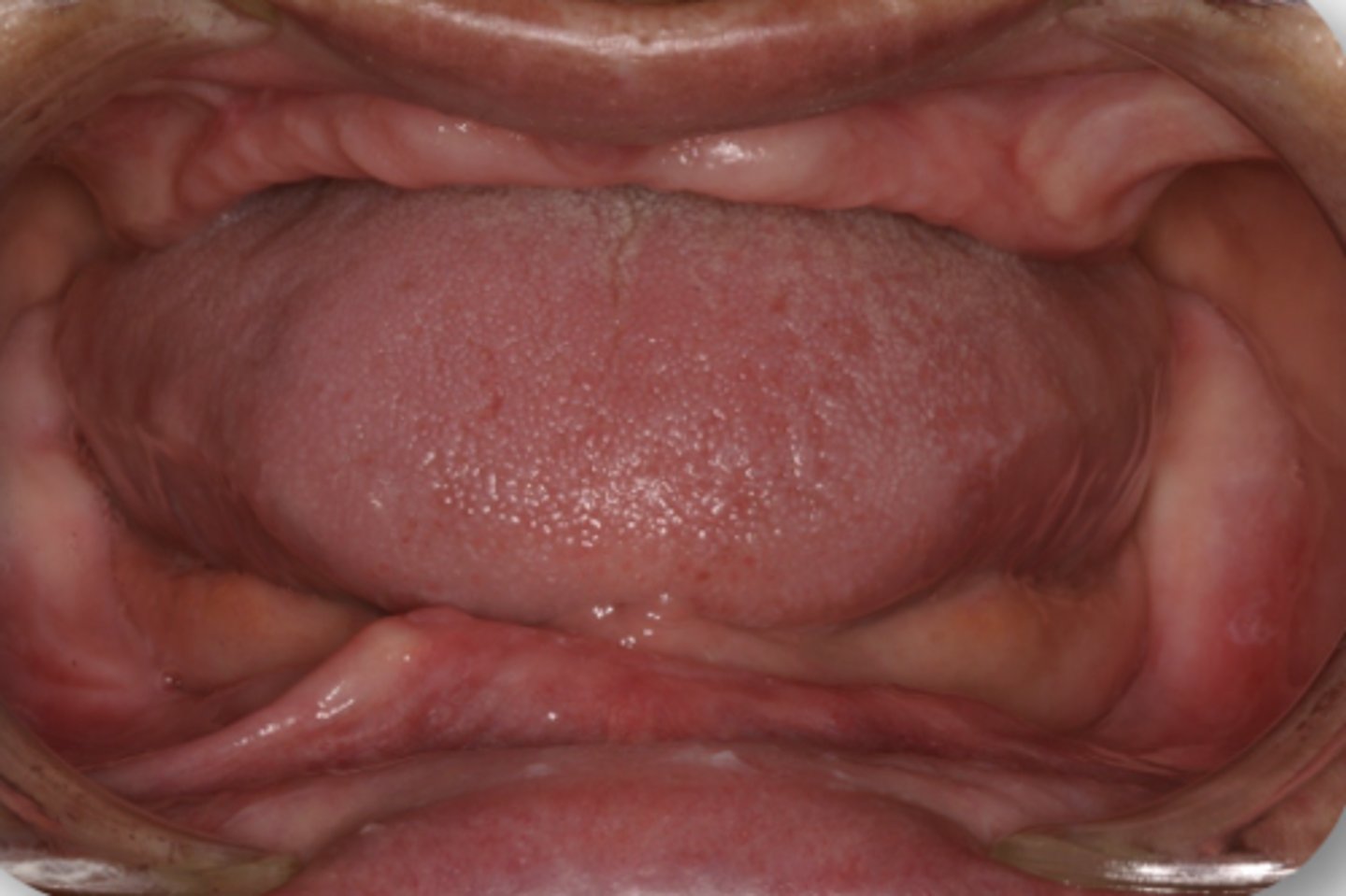
~ 22.96 cm^2
In a denture bearing area, there is about ___square centimeters of support in the maxilla
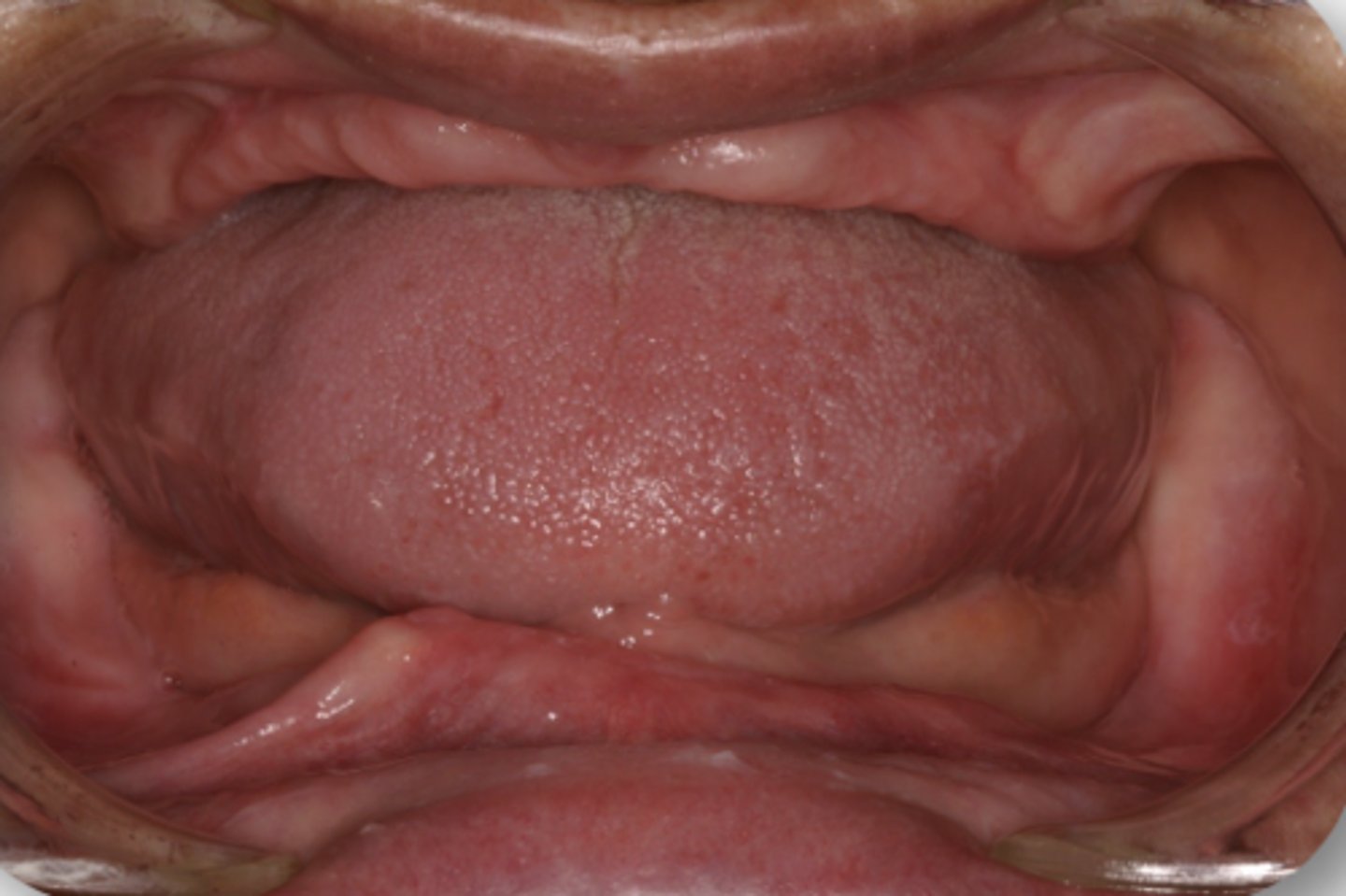
~ 12.25 cm^2
In a denture bearing area, there is about ___square centimeters of support in the mandible
No!
- There are clear indications and little doubt that the removable denture plays an important causative role in the bone resorption process
- This is supported by studies showing significant differences in residual alveolar bone between edentulous subjects wearing or not wearing removable dentures. Subjects not wearing dentures had more remaining bone.
Do dentures prevent bone loss?
2 to 3
*removable dentures play an important causative role in bone resorption process
Removable full or partial dentures accelerate bone resorption by a factor of ___ to ___
Sleeping
Denture use during ___________ hours is especially destructive, particularly if the patient presents with chronic bruxing and grinding habits.
Periodontal disease
(Rather than waiting until the bone is resorbed or the patient complains of problems with the prostheses, the dental professional should educate the patient about the bone loss process after tooth loss. The patient should be made aware the bone loss process can be arrested by a dental implant.)
The dental implant profession should treat bone loss after tooth extraction in a similar fashion as bone loss from what?
Psychological
These are all ________ effects of edentulism:
- Premature aging
- Less enjoyment of foods
- Lowered self confidence
- Socially inhibited
- Seldom laugh
- Change in personal relationships
- Poor self image
- Secrecy of situation
- Worry
With loose fitting dentures
What are the psychological effects of edentulism magnified by?
- Psychosocial benefits (pt satisfaction, quality of life)
- Functional benefits (biting force, improvement in masticatory performance, nutrition, sensation/tactile sensation)
- Anatomical benefits (residual ridge maintenance, prevention of muscle atrophy)
What patient centered outcomes are we focused on when it comes to restoring dentition with implants? (3)
False (need of complete dentures is increasing)
T/F: There is an overall decrease in the need for complete dentures due to a decline in edentulism, despite the population of older patients is living longer
True
T/F: A study from 2002 showed that the adult population in need of 1 or 2 complete dentures will increase from 33.6 million adults in 1991 to 37.9 million adults in 2020
True
T/F: A study from 2002 showed that the 10% decline in edentulism experienced each decade will be more than offset by the 79% increase in the adult population older than 55 years.
The population is older patients is growing and they are living longer
Although there is an overall decrease in edentulism in the US population, why is the need for complete dentures predicted to still increase?
- Medical risk factors
- Functional impairment
- Possible onset of dependency and frailty
What are three concerns with increasingly older patients?
Class I
ID the classification of prosthodontic diagnostic index:
Ideal or minimally compromised
May be treated and experience satisfactory results with conventional, complete dentures
How can you treat patients with a class I prosthodontic diagnostic index?
Should be treated by clinicians with extensive prosthodontic, implant, and surgical experience
How can you treat patients with a class IV prosthodontic diagnostic index?
Class II
ID the classification of prosthodontic diagnostic index:
Moderately compromised
Class III
ID the classification of prosthodontic diagnostic index:
Substantially compromised
Class IV
ID the classification of prosthodontic diagnostic index:
Severely compromised
Reduced bone height
PDI screening identifies many edentulous patients as high-complexity (Class IV), largely due to anatomical limitations like ________
Overdenture
Define the following:
- Any removable dental prosthesis that covers and rests on one or more remaining natural teeth, the roots of natural teeth, and/or dental implants
- A dental prosthesis that covers and is partially supported by natural teeth, natural tooth roots, and/or dental implants
Types of overdentures
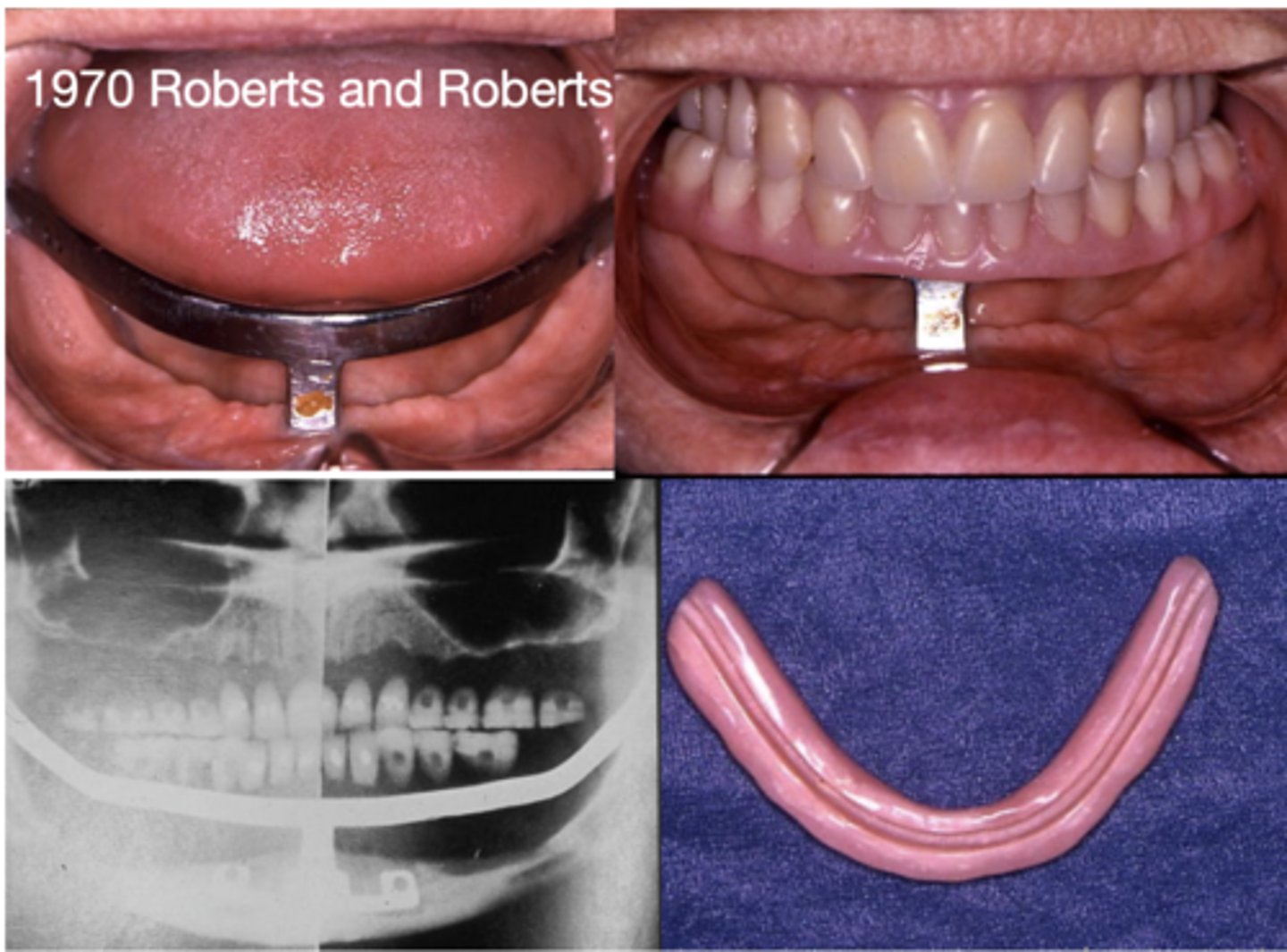
What do the following show?
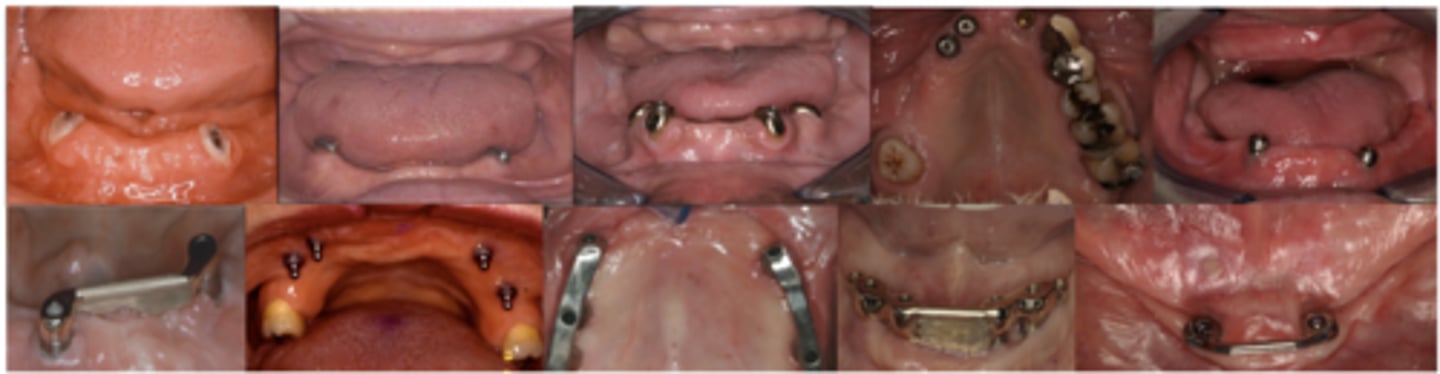
mucosal insert
Define the following:
Any metal form attached to the tissue surface of a removable denture prosthesis that mechanically engages in a surgically prepared site
Mucosal inserts
What are these images showing?
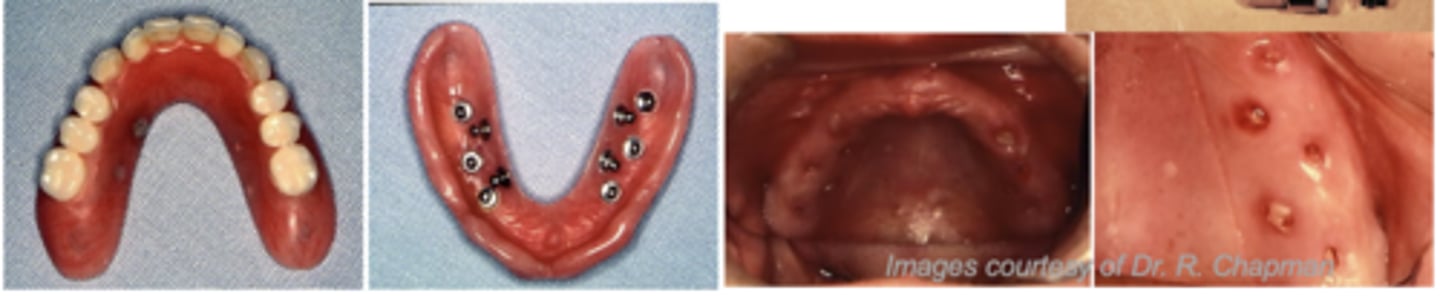
Subperiosteal implant
What type of implant?
Subperiosteal implant
What type of implant?
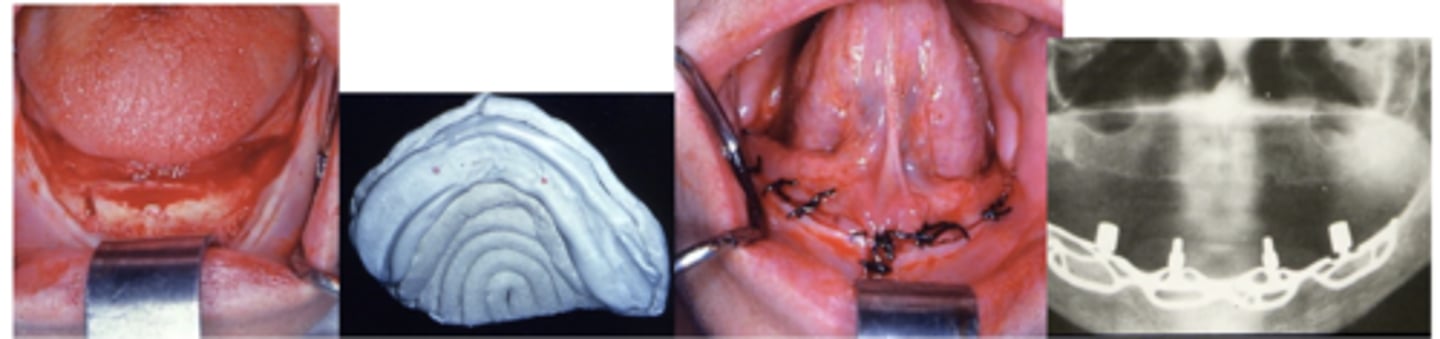
Transmandibular implant
What type of implant?
Ramus frame implant
What type of implant?
- Conventional CD
- Tooth-retained OD
What are two treatment options for soon to be edentulous patients?
- Conventional CD
- Implant-assisted removable complete denture
- Implant-supported removable complete denture
- Implant-supported fixed complete denture
What are four treatment options for completely edentulous patients?
True
T/F: The following treatment options are within the scope of predoctoral prosthodontics, including immediate/ interim complete dentures.
- Conventional CD
- Implant-assisted removable complete denture
Overdentures on natural teeth
All of the following are advantages of what?
- Maintenance of more residual ridge integrity
- Improved denture stability and retention
- Psychological aspect
- Motivation
- Patient perception of a 'retained natural feeling'
- Better occlusal awareness, biting force, neuromuscular control
Overdentures on natural teeth
All of the following are disadvantages of what?
- Lack of oral hygiene motivation (Caries, Periodontal disease)
- Additional expenses
- Endodontics
- Copings, attachments
- Weaker denture base (if not reinforced with metal)
- Caries on abutment
- Periodontal status of abutment
A 5-year retrospective Analysis of Survival and Prosthodontic Complications showed that the main two problems with abutment teeth for over dentures were what?
Secondary caries on retained roots, under overdentures
What is this showing?
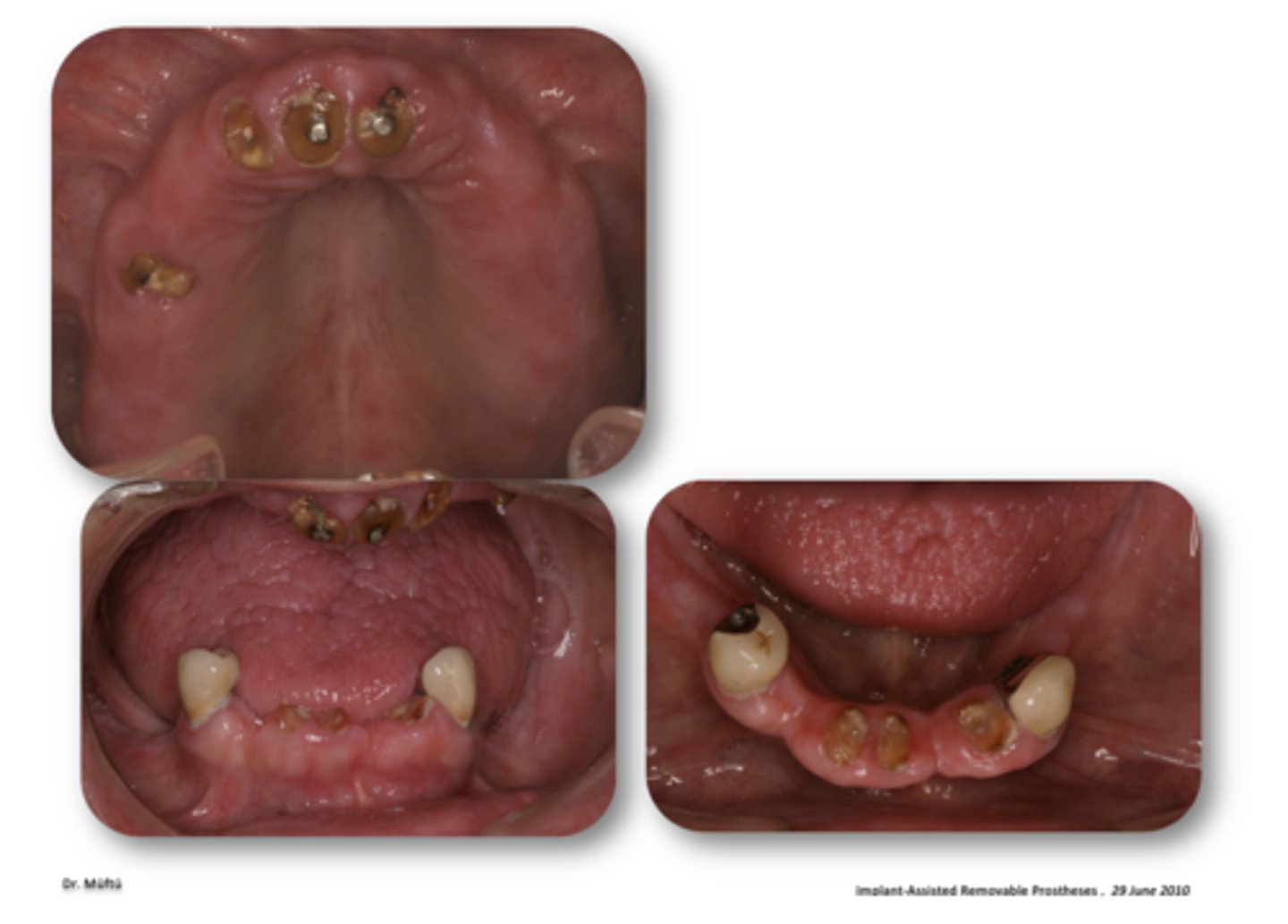
False - may still be a viable option
T/F: Overdenture are not a viable option for patients who can not have dental implants due to systemic conditions, medications, fear of surgery, etc
A - Should be REDUCING salivary flow rates to increase the risk of caries, stomatitis, gingivitis and fungal infections
Many of the drugs used to treat chronic medical conditions can adversely impact oral health, including all of the following EXCEPT:
A) Increasing salivary flow rates to increase the risk of caries, stomatitis, gingivitis and fungal infections
B) Periodontal disease kept in balance through maintenance of oral hygiene can rapidly progress when conditions change
C) Exposed root surfaces are highly susceptible to root caries
E) Wishes, expectations and demand of the patient (this is a non-clinical parameter)
All of the following are clinical decision parameters for overdentures, EXCEPT:
A) Strategic importance of the tooth
B) Load it will be expected to withstand
C) Patient’s oral hygiene
D) Extent of treatment necessary to save the tooth
E) Wishes, expectations and demand of the patient
Denture retention
What has the following characteristics?
- The resistance in the movement of a denture away from its tissue foundation especially in a vertical direction
- A quality of a denture that holds it to the tissue foundation and/or abutment teeth
Denture stability
What has the following characteristics?
- The resistance of a denture to movement on its tissue foundation, especially to lateral (horizontal) forces as opposed to vertical displacement
- A quality of a denture that permits it to maintain a state of equilibrium in relation to its tissue foundation and/or abutment teeth
Denture support
What has the following characteristics?
- The foundation area on which a dental prosthesis rests
- With respect to dental prostheses, the resistance to displacement towards the basal tissue or underlying structures
Implant-retained/ tissue-supported
Describe the retention and support for this denture
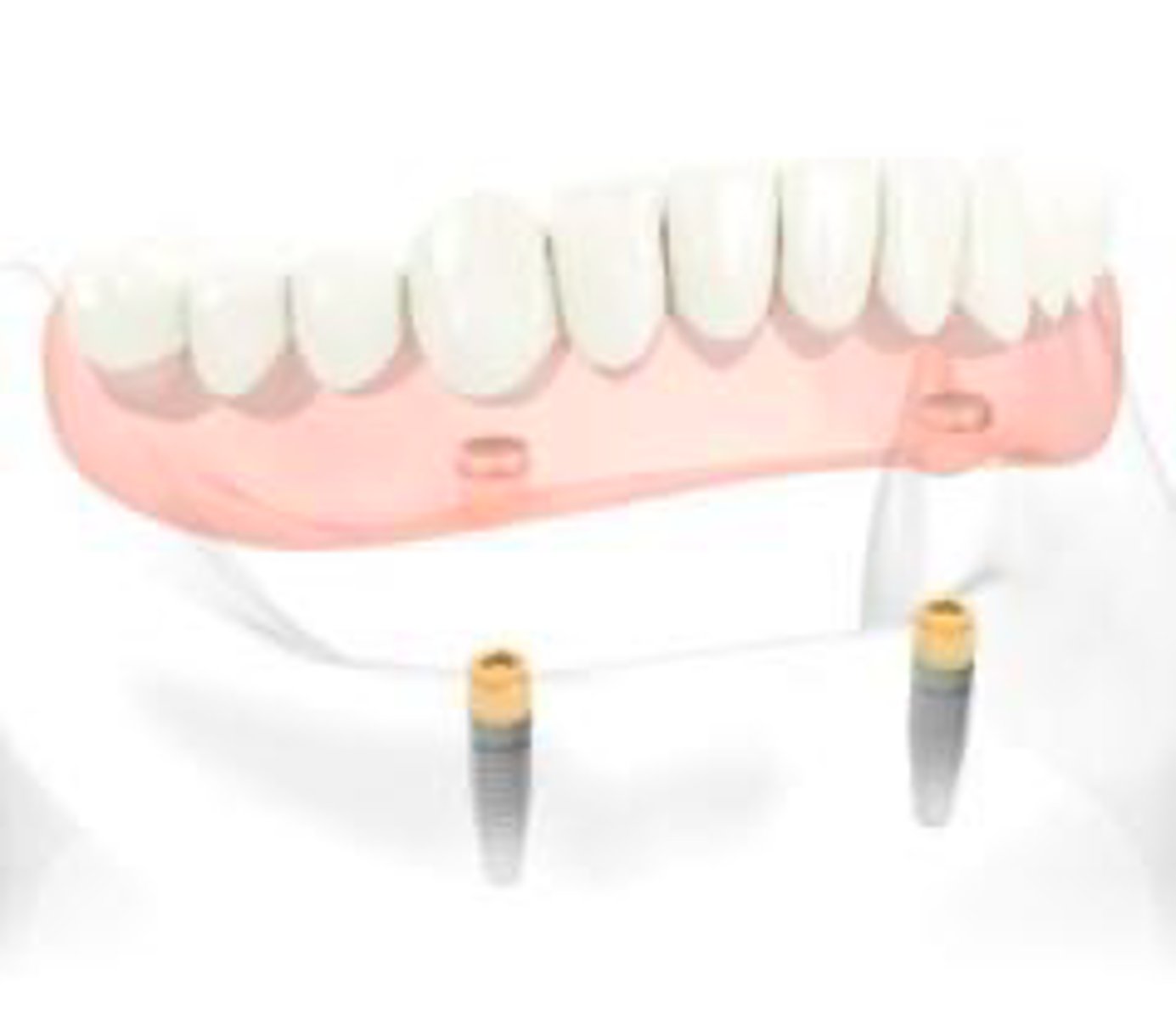
Implant-retained/ implant- supported
Describe the retention and support for this denture
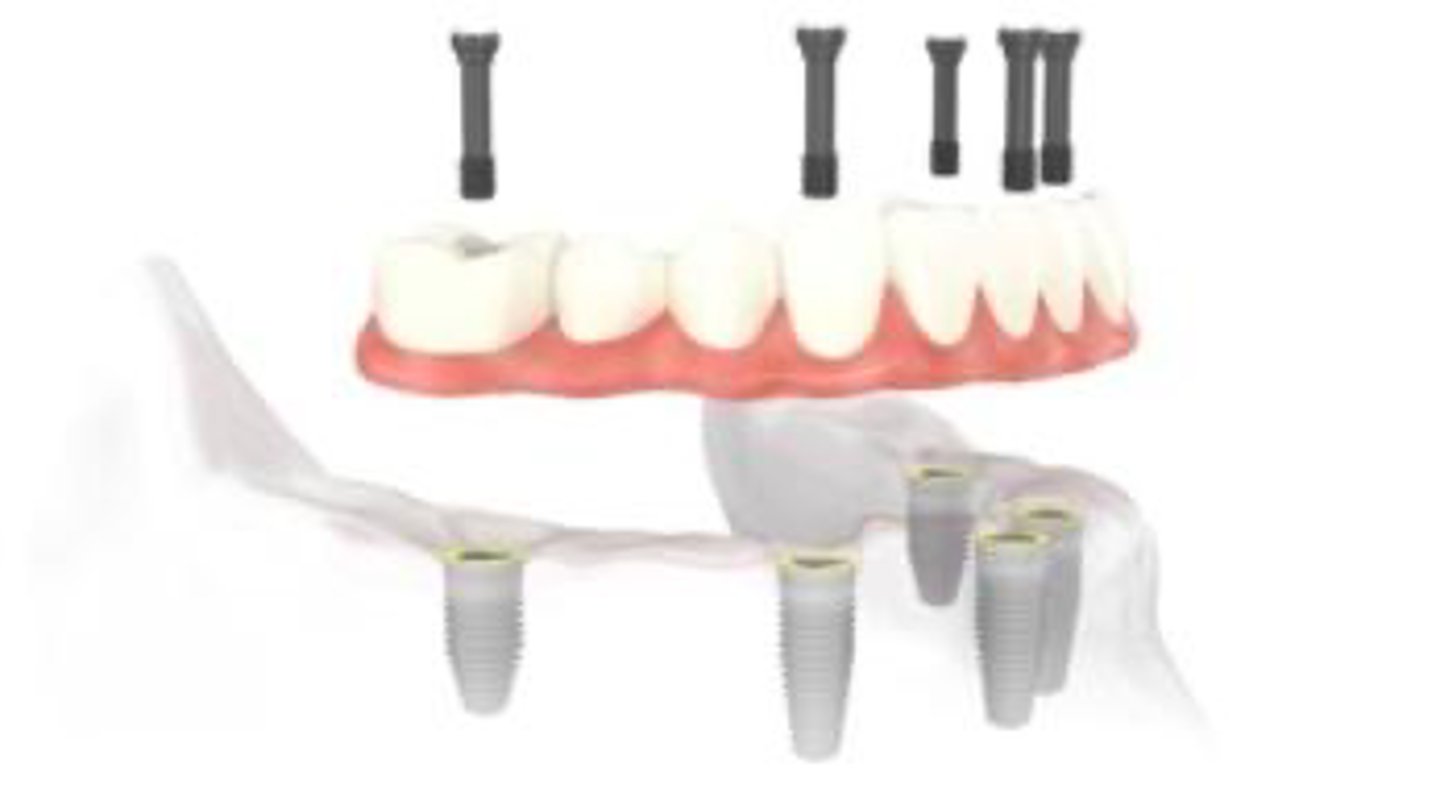
Decrease
Implant-assisted removable prostheses showed a _______ in bone resorption rate over conventional dentures
Increase
Implant-assisted removable prostheses showed a _______ in prosthetic retention and stability over conventional dentures
Increase
Implant-assisted removable prostheses showed a _______ in masticatory efficacy and chewing ability over conventional dentures
Decrease
Implant-assisted removable prostheses showed a _______ in soft-tissue trauma over conventional dentures
true
T/F: There is more satisfaction and better oral health-related quality of life with mandibular IOD compared with conventional CDs, independent of sociodemographic factors, anatomy, number of implants and type of superstructure
False, limited amount of evidence
T/F: There is a sufficient amount of evidence available on the benefits of maxillary implant assisted complete prostheses over conventional dentures
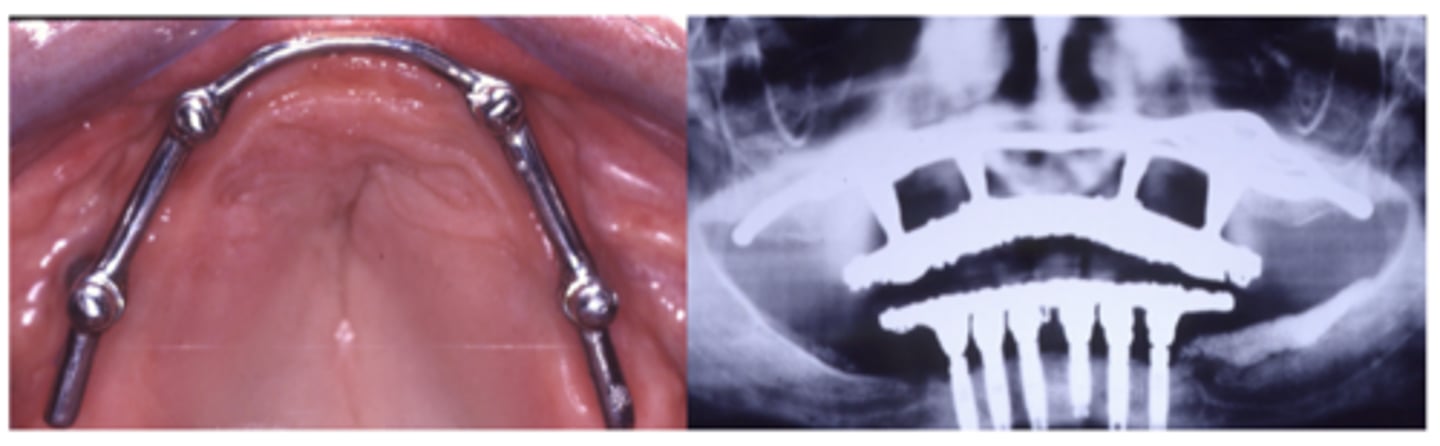
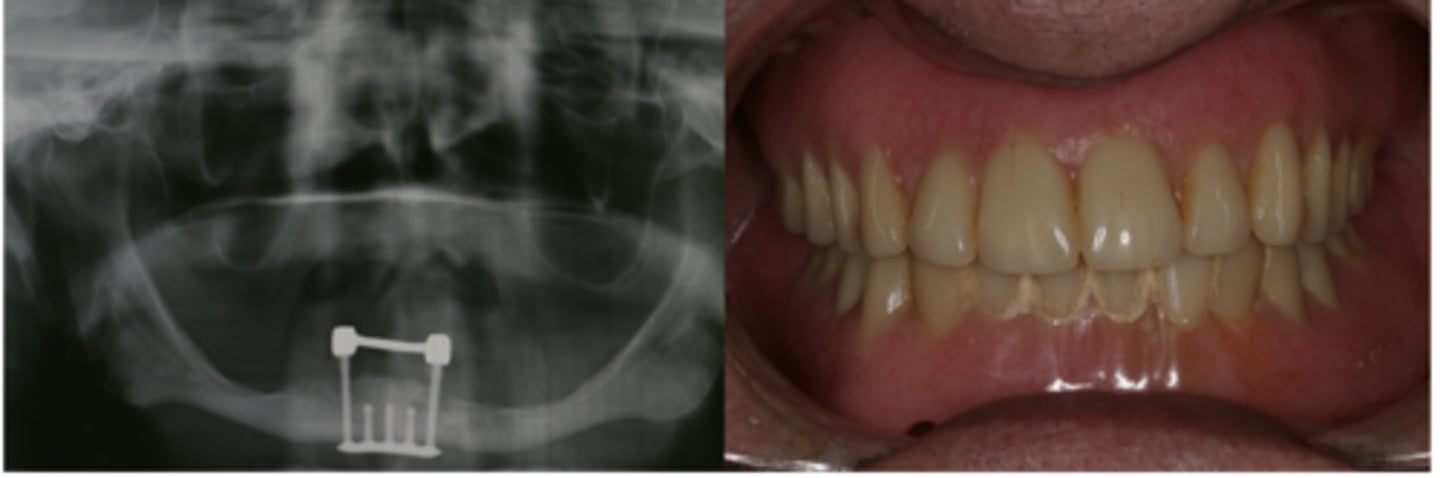
Implant-assisted removable complete denture
What are these images showing?
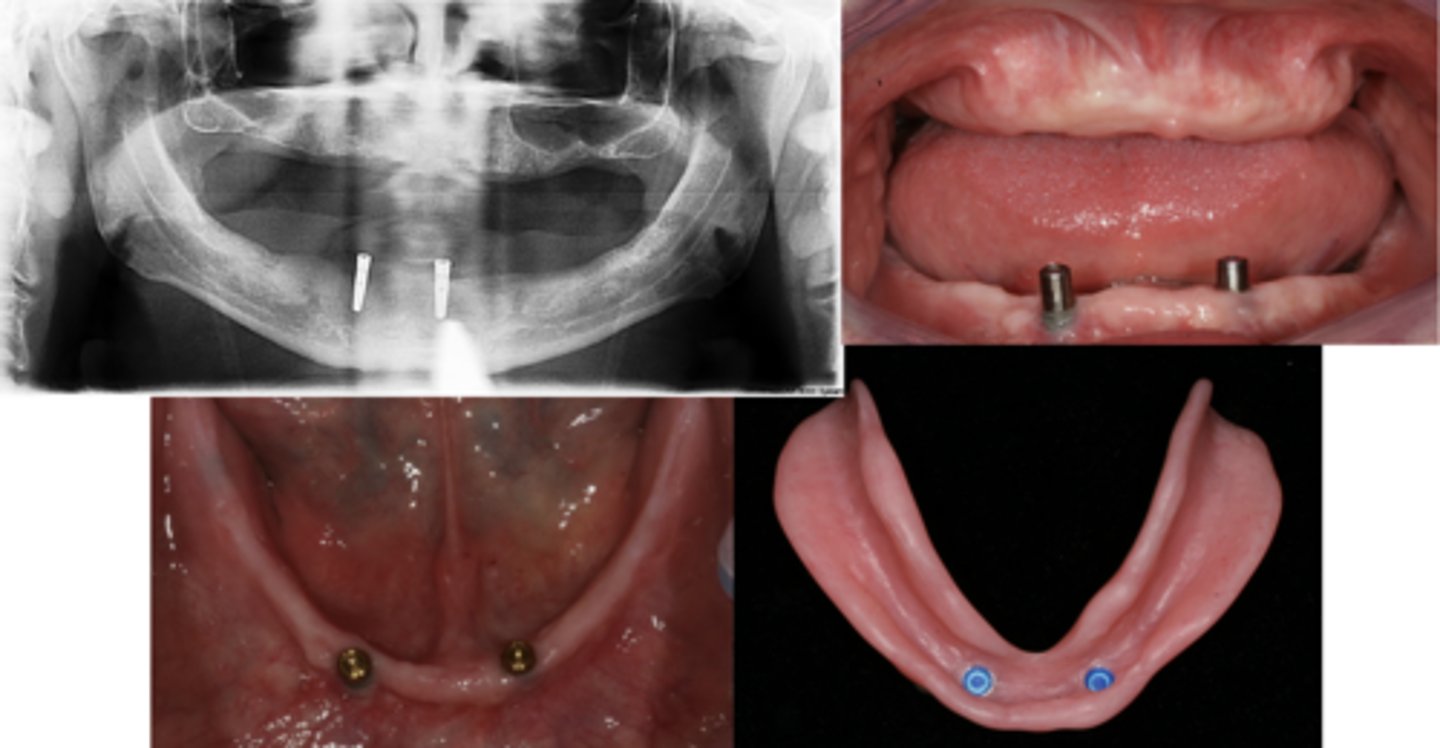
Mandibular implant ODs
The following are patients who benefit from what?
- Usually elderly (65-80yrs)
- Edentulous in maxilla and mandible
- Worn CDs for many years
- Demand stabilization of the denture
- Exhibit extremely reduced residual dentition that can not be maintained
Maxillary implant ODs
The following are patients who benefit from what?
- Younger segment of older pts (50-60)
- No experience with maxillary removable prosthesis
- Hopeless residual maxillary dentition
- Fearful of becoming edentulous
- High esthetic demands
- Natural teeth or fixed pros in mandible
- Desire fixed reconstruction
True
T/F: When it comes to a patient's ability to speak, a complete denture may be more beneficial than an implant assisted fixed appliance
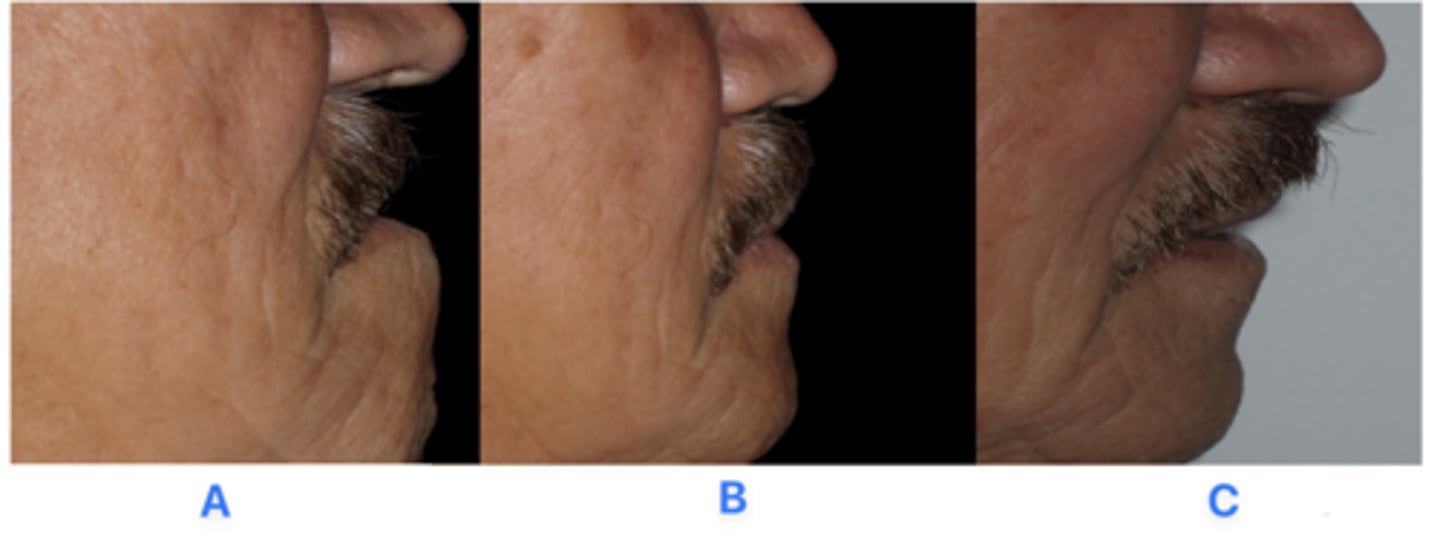
Differences of lip support:
A - Without denture
B - Fixed Implant Bridge
C - Denture with flange
What are the difference between the three images?
Removable
ID if the following describes the indications/ features of a removable or fixed implant assisted prosthesis:
- 12-20mm of vertical space
- Patients lacking dexterity
- Oral/maxillofacial defects
- Severe bone loss
- Malpositioned implants
- High nocturnal parafunction
- Financially limited
Fixed
ID if the following describes the indications/features of a removable or fixed implant assisted prosthesis:
- 8-10mm of vertical space
- Younger pts
- Psychological needs
- Mild/moderate bone loss
- NO horizontal bone loss
Removable
ID if the following describes the advantages of a removable or fixed implant assisted prosthesis:
- Easier to clean
- Phonetics
- Provides lip support
- Technically easier to make
Fixed
ID if the following describes the advantages of a removable or fixed implant assisted prosthesis:
- Can be made of acrylic or porcelain
- Esthetics
- Higher bite force
- Better stability/retention
Removable
ID if the following describes the disadvantages of a removable or fixed implant assisted prosthesis:
- Causes more mucosal problems
- Wear of components
Fixed
ID if the following describes the disadvantages of a removable or fixed implant assisted prosthesis:
- Requires more implants
- Accumulation of food posteriorly
- More difficult/expensive to make, adjust and redo
True
(57% stated that their patients with IODs were equally satisfied as those treated with IFDPs)
T/F: According to the 2015 study by International College of Prosthodontics members, implant overdentures (IODs) and implant fixed dentures (IFDPs) provide similar patient satisfaction
Cost
According to the 2015 study by International College of Prosthodontics members, what was the main reason people chose Implant Overdenture over a Implant Fixed Denture (complete) Prostheses?
- Stud attachments (Bar, ERA, Locator, Locator Rtx)
- Bars (Round, Hader, Dolder, Free-Form)
What are the 2 types of attachment systems for implant overdentures?
Locator (stud type)
What is the most universal attachment system for implant overdentures?
4 implants
What is the minimum recommended number of implants used for a complete maxillary denture design without palatal coverage?
Bars
What provides more retention than solitary abutments for maxillary dentures?
Equally satisfied
(At this time, there is no consensus for treatment of edentulous maxillae)
What are patients more satisfied with: bars or solitary anchors retaining a maxillary implant OD?
True
T/F: Maxillary implant prostheses should not be considered as a general treatment of choice in patients with good bony support for maxillary conventional prostheses
True!
T/F: For a maxillary denture SAC assessment, theres is NOTHING straightforward about the procedure
Advanced
What is the SAC assessment level for maxillary ODs?
>10 mm Inter-arch distance (bar & clip retained)
Advanced
What is the SAC assessment level for maxillary ODs?
>8 mm Inter-arch distance (stud elements)
Advanced
What is the SAC assessment level for maxillary ODs?
Early Loading protocol (bar&clip)
Advanced
What is the SAC assessment level for maxillary ODs?
Conventional/early Loading protocol (Stud) elements
Advanced
What is the SAC assessment level for maxillary ODs?
Low esthetic risk
Advanced
What is the SAC assessment level for maxillary ODs?
Removable interim restorations during healing
Complex
What is the SAC assessment level for maxillary ODs?
Inter-arch distance (bar & clip retained): <10 mm = not indicated
Complex
What is the SAC assessment level for maxillary ODs?
Inter-arch distance (stud elements): <8 mm = not indicated
Complex
What is the SAC assessment level for maxillary ODs?
Immediate loading protocol (bar & clip) elements
Complex
What is the SAC assessment level for maxillary ODs?
Moderate/high esthetic risk (unrealistic expectations)
2-implant overdenture
The evidence currently available suggests that restoration of the edentulous mandible with a conventional denture is no longer the most appropriate first choice prosthodontic treatment.
There is now overwhelming evidence that a _________ should become the first-choice treatment for the edentulous mandible
Standard of care
_______ is a legal term denoting the level of a conduct a physician or healthcare provider must meet in treating a patient so as not to be guilty of negligence, usually called malpractice
- It is generally defined simply as what a reasonably prudent physician (or a specialist) would do in the same or similar circumstances
True
T/F: Whilst it is accepted that the two-implant overdenture is not the gold standard of implant therapy, it is the minimum standard that should be sufficient for most people, taking into account performance, patient satisfaction, cost and clinical time.
Straightforward
What is the SAC assessment level for mandibular ODs?
Inter-arch distance (stud elements): >8 mm
Straightforward
What is the SAC assessment level for mandibular ODs?
Number of implants: 2
Straightforward
What is the SAC assessment level for mandibular ODs?
Loading protocol: Conventional/early
Straightforward
What is the SAC assessment level for mandibular ODs?
Low esthetic risk
Straightforward
What is the SAC assessment level for mandibular ODs?
Removable interim restorations during healing
Advanced
What is the SAC assessment level for mandibular ODs?
Inter-arch distance (bar&clip retained): >10 mm
Advanced
What is the SAC assessment level for mandibular ODs?
Number of implants: 3 or more
Advanced
What is the SAC assessment level for mandibular ODs?
Moderate/high esthetic risk (unrealistic expectations)
Advanced
What is the SAC assessment level for mandibular ODs?
Occlusal parafunction: absent
Advanced
What is the SAC assessment level for mandibular ODs?
Occlusal scheme issues (fixed opposing arch): Anterior guidance
Advanced
What is the SAC assessment level for mandibular ODs?
Occlusal scheme issues (CD opposing arch): Balanced
Complex
What is the SAC assessment level for mandibular ODs?
Inter-arch distance (bar&clip retained): <10 mm = not indicated
Complex
What is the SAC assessment level for mandibular ODs?
Inter-arch distance (stud elements): <8mm = not indicated