Rheumatology
1/127
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
128 Terms
inflammatory joint disorders
RA, SLE, GOUT
monoarticular joint disorders
gout, trauma, septic arthritis, lyme, osteoarthritis
oligoarticular (2-4) joint disorders
reactive arthritis, psoriatic arthritis, IBD
polyarticular (≥5) joint disorders
RA, SLE
DIP involvement joint disorders
osteoarthriits, psoriatic arthritis
MCP involvement joint disorders
RA, SLE, pseudogout
first metatarsal phalangeal involvement joint disorders
gout, osteoarthritis
a degenerative arthritis and wearing down of the joints
osteorthritis
what are the sxs/s of osteoarthritis?
joint pain, crepitus, decreased mobility, pain with use and weight bearing, Heberden + Bouchard nodes
what is the diagnostic for osteoarthritis (and what would you expect to see?)
XR: sclerosis, osteophytes, decreased joint space
what is the treatment for osteoarthritis?
- moderate exercise, PT, assistive devices
- topicals (capsaicin cream, diclofenac gel)
- oral tylenol or NSAIDS (tylenol 1st line since it is safer)
- joint injections (steroid, hyaluronate, PRP)
- surgery (replacements)
gout
sxs/s?
diagnostics?
treatment? (acute attack and between attacks)
swelling, tenderness, redness, warmth, pain (great toe MTP is most common location), +- tophi
+ needle-shaped crystals in the synovial fluid (via arthrocentesis)
acute: rest, ice, NSAID + colchicine x 5-7 days (corticosteroid if can't have NSAID)
btw: allopurinol or febuxostat (1st line)
(can add probenecid if uric acid is >6)
when is ULT indicated for treatment of gout?
≥2 attacks/year, CKD, tophi, urolithiasis, chronic
gout in the big toe
podagra
gout prevention
low purine diet, avoid organ meats, avoid EtOh, high fluid intake, avoid thiazides and loops
Rhomboid-shaped, positively birefringent calcium pyrophosphate dihydrate (CPPD) crystals on joint fluid aspirate.
pseudogout
gout or pseudo gout
joint cartilage calcifications
psuedogout
gout or pseudo gout
spindle shaped crystals
gout
gout or pseudo gout
no birefringence under polarized light
gout
gout or pseudo gout
no bony changes
pseudogout
chronic systemic disease characterized by autoimmune inflammatory changes of multiple joints
rheumatoid arthritis (RA)
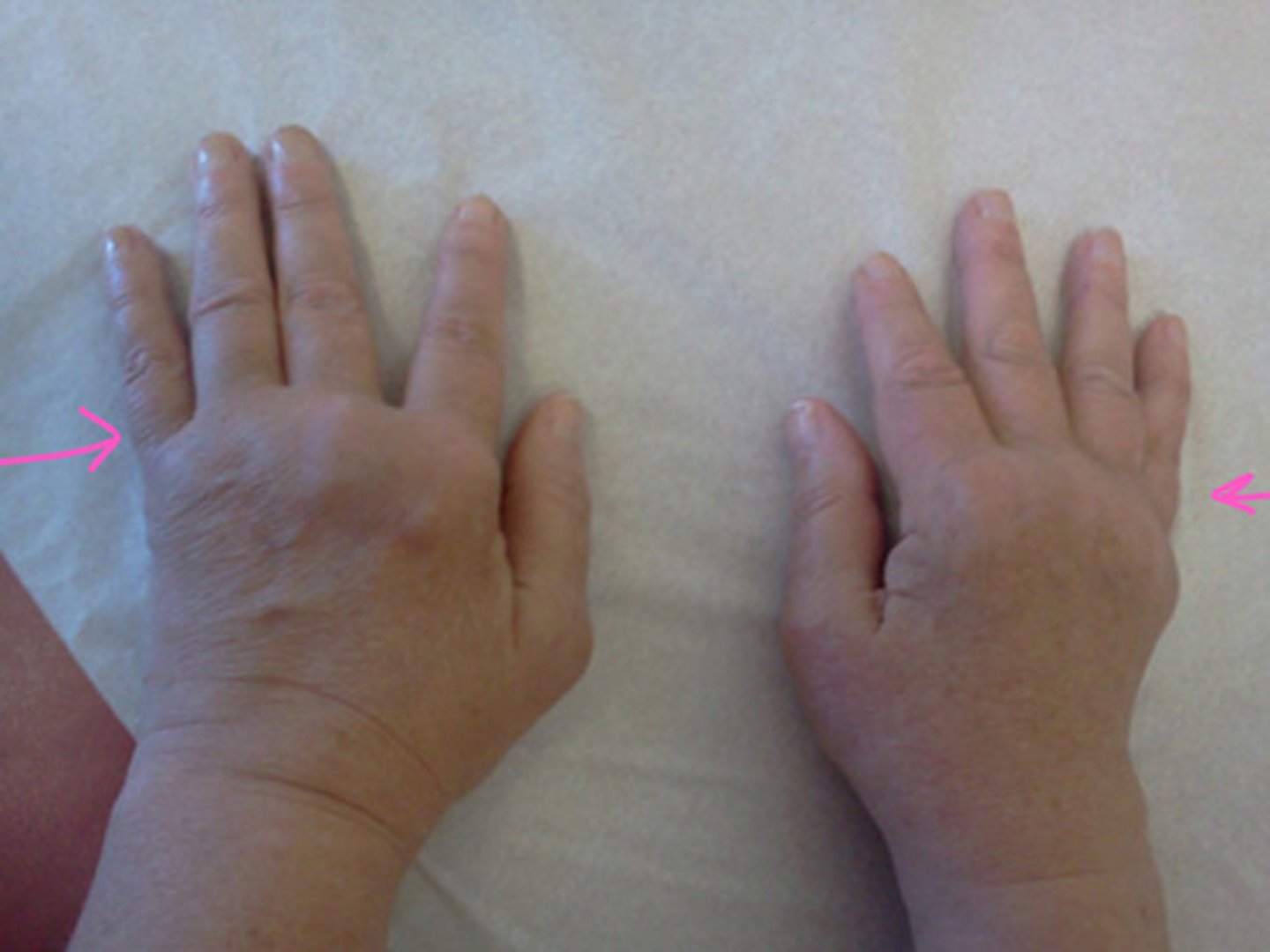
what are the sxs/s of rheumatoid arthritis?
symmetric swelling of multiple joints, tenderness, pain, morning stiffness, deformity
(PIP, MCP, wrists, knees, ankles, MTPs)
MC joint involved in RA
MTP
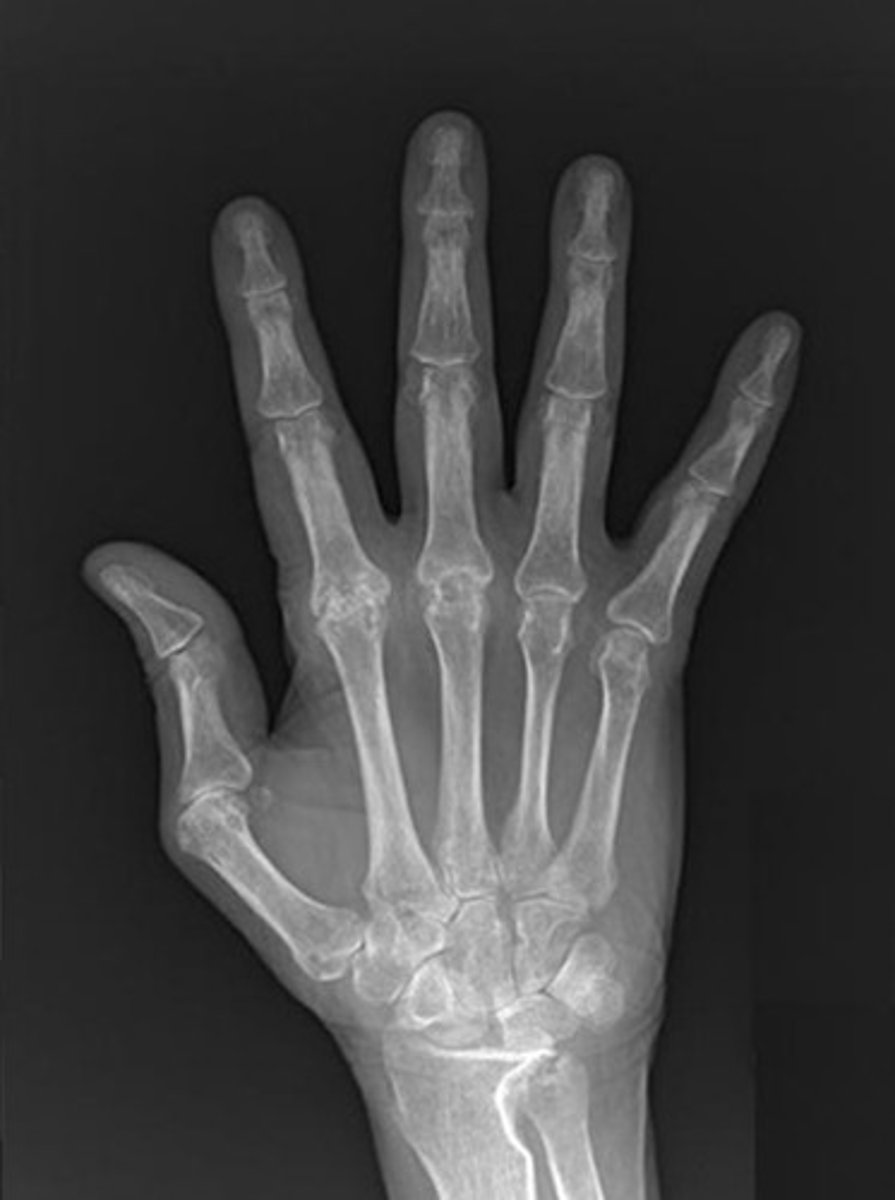
what labs/tests are diagnostic for rheumatoid arthritis?
+ RF (rheumatoid factor) and + anti-CCP antibodies
elevated ESR and CRP
XR: uniform joint space narrowing, erosions
osteoarthritis or RA?
multijoint involvement, symmetric
RA
osteoarthritis or RA?
bouchard and herbens nodes
osteoarthritis
osteoarthritis or RA?
PIP joint involvement
both
osteoarthritis or RA?
morning stiffness
RA
osteoarthritis or RA?
DIP joint involvement
osteoarthritis
osteoarthritis or RA?
monoarticular joint pain worse with activity, better with rest
osteoarthritis
osteoarthritis or RA?
hip or knee pain
osteoarthritis
osteoarthritis or RA?
wrist and MCP pain
RA
what is the first-line treatment for rheumatoid arthritis?
other treatment options?
methotrexate (MTX)
- other disease modifying antirheumatic drugs (sulfasalazine, hydroxychloroquine, janus kinase inhibitors, biologics)
- NSAIDs (can be added for pain relief)
- prednisone daily - bridge only
- steroid injections
(medications can be combined; but you cannot combine biologics)
the following are characteristic of what disease?
in young women
rash over sun-exposed areas
joint sxs
anemia, leukopenia, thrombocytopenia
ANAs, anti-double stranded DNA antibodies
SLE
inflammatory autoimmune disorder of autoantiboides to nuclear antigens that effects multiple organ systems
systemic lupus erythematosus (SLE)
what serology tests (antibodies) are diagnostic for SLE?
ANA (antinuclear antibody), anti-dsDNA, and anti-smith ab
diminished serum complement levels (esp during flare)
what physical exam findings can be found with SLE?
malar rash, discoid skin lesions, oral ulcers, arthritis
11 criteria for classification of SLE
malar rash
discoid rash
photosensitivity
oral ulcers
arthritis
serositis
kidney disease
neurologic disease (seizures)
hematologic disorders
immunologic abnormalities (antibodies)
positive ANA
*need 4/11 for positive diagnosis
what is the treatment for SLE?
- pt education and emotional support
- avoid sun
- NSAIDs (minor joint involvement)
- topical steroids (for rashes)
- hydroxycholoroquine (DOC for rashes and joints)
- corticosteroids (for other organ involvement)
- immunosuppressants (long-term control)
- cyclophosphamide (refractory dz)
which SLE antibody is most sensitive for SLE?
ANA
which SLE antibody is most specific for SLE?
anti-smith
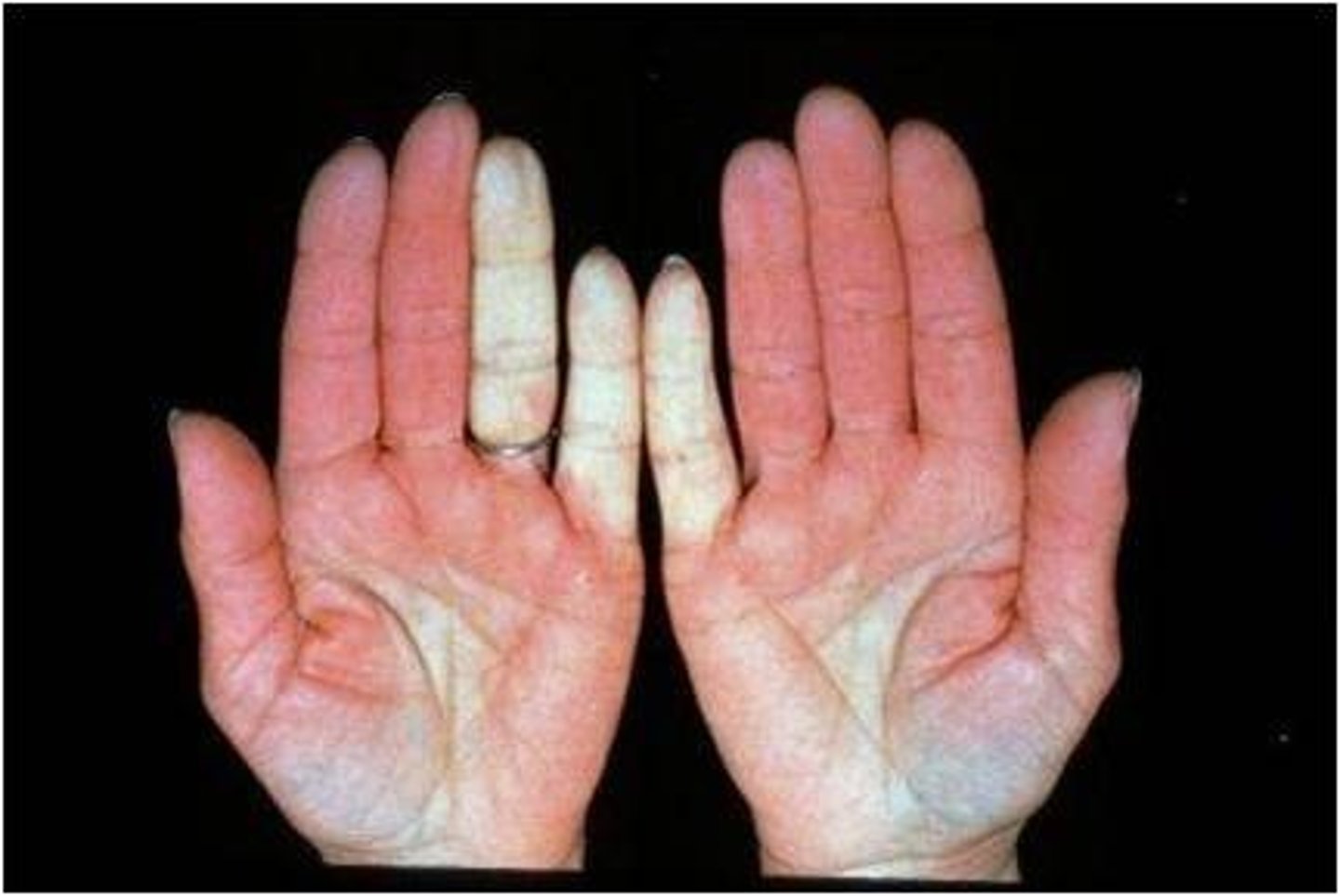
paroxysmal digital ischemia, most commonly caused by an exaggerated response of digital arterioles to cold or emotional stress
Raynaud's phenomenon
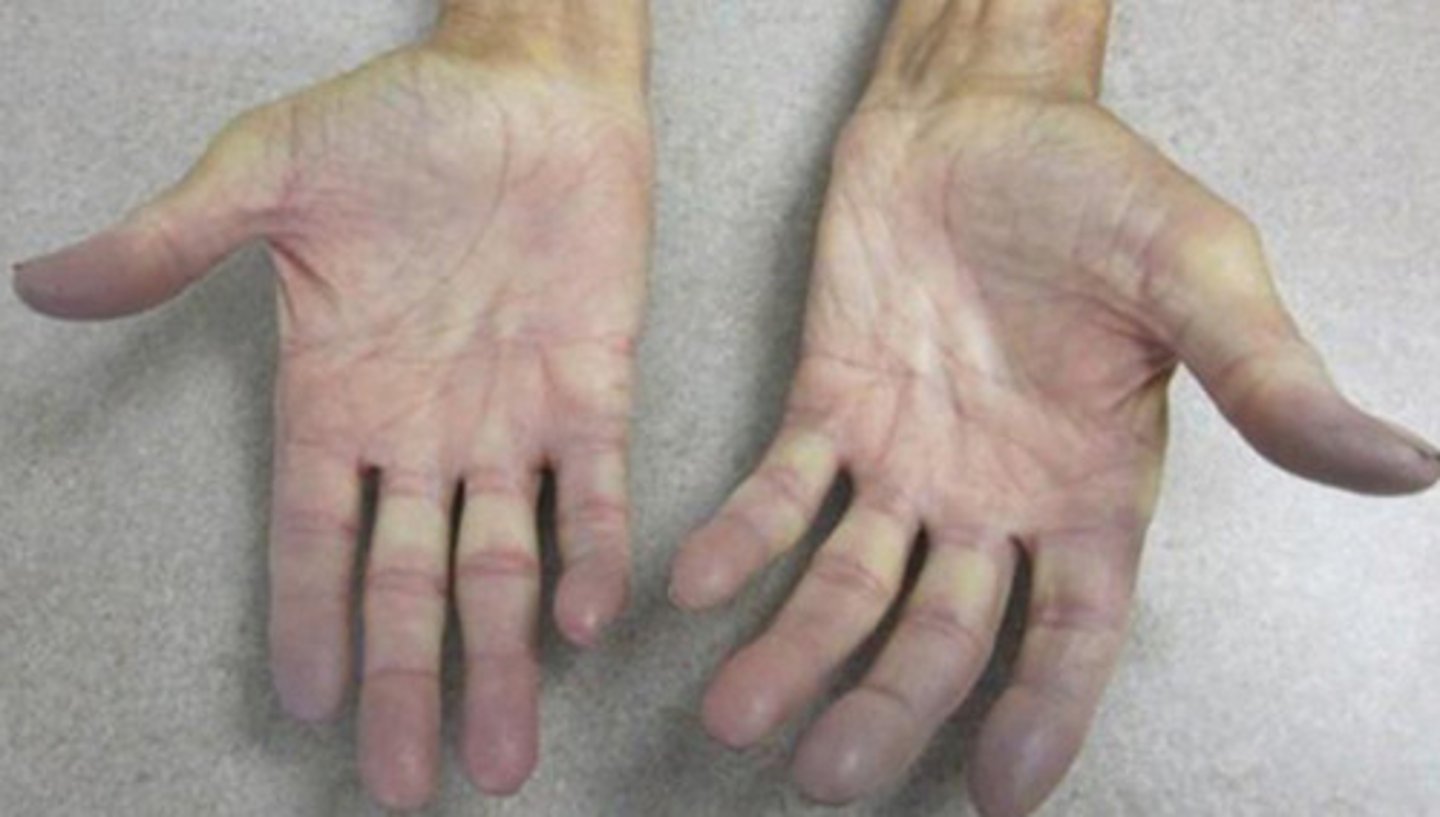
what are the sxs/s of Raynaud's phenomenon?
treatment?
pallor, bluish discoloration of fingers, toes (pulses intact), pain, bilateral
CCB (1st-line)
avoid cold exposure
a rare chronic disorder characterized by diffuse fibrosis of the skin and internal organs
systemic sclerosis (scleroderma)
skin thickening confined to the face, neck, and distal extremities (a type of systemic sclerosis)
limited disease (CREST syndrome)
widespread thickening of skin with area of increased pigmentation and depigmentation (a type of systemic sclerosis)
diffuse disease
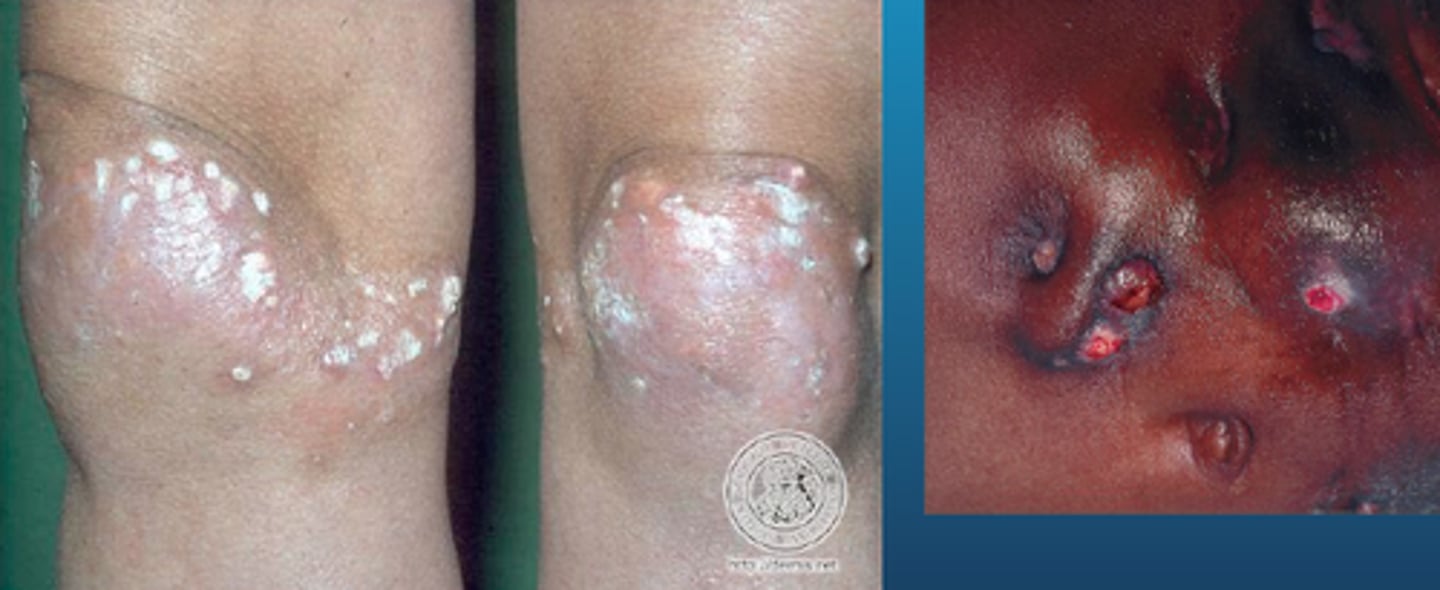
what are the sxs/s of limited systemic sclerosis?
diffuse?
Raynaud's initially, then 1 or more CREST features (calcinosis, raynauds, esophogeal dysmotility, sclerodactyly, telangiectasias)
polyarthralgia, weight loss, malaise, skin changes of trunk + proximal ext, non-pitting edema
what positive serology can you see with diffuse systemic sclerosis?
limited?
ANA, anti-SCL-70
ANA, anti-SCL-70, anti-centromere
T or F:
there is no effective treatment for the underlying disease process of systemic sclerosis
T
(treatment focuses on the organ systems involved)
what is the treatment for systemic sclerosis?
(skin, renal, GI, lung, pulmonary HTN, refractory diffuse systemic)
MTX or mycophenolate
ACEI
PPI
mycophenolate or cyclophosphamide
CCB or PDE5 inhibitors
myeloablation then stem cells OR immunosuppression w/ cyclophosphamide
(refer all to rheumatology)
systemic autoimmune disorder due to the immunedysfunction of the lacrimal and salivary glands
Sjogren syndrome
what are the sxs/s of Sjogren syndrome?
dry eyes and mouth
systemic: dysphagia, vasculitis, pleuritis, ILD, neuropathies, pancreatitis, kidney dysfunction
what positive serology tests can you see with Sjogren syndrome?
what other diagnostics can be done?
ANA, RF, anti-SS-A, anti-SS-B
Schirmer test, biopsy
what is the treatment of Sjogren syndrome?
artificial tears, lacrimal plugs, cyclosporine drops, pilocarpine PO
keep mouth moist (sip water, gum/candy)
syndrome of pain and stiffness involving the proximal muscles mainly, neck, shoulders, and hips
polymyalgia rheumatica (PMR)
what are the sxs/s of polymyalgia rheumatica (PMR)?
symmetrical muscle pain/stiffness in shoulder and hips with abrupt onset
nocturnal pain, AM stiffness
fever
what is the diagnostic test for polymyalgia rheumatica (PMR)?
elevated ESR and CRP
what is the treatment for polymyalgia rheumatica (PMR)?
prednisone 10-20 mg x 2-4 weeks, then taper
*patient should improve remarkably in 3 days
(sarilumab if refractory)
systemic panarteritis affecting medium and large sized vessels; often coexists with PMR
giant cell arteritis
what are the sxs/s of giant cell arteritis?
HA, scalp tenderness, visual (amaurosis fugax or diplopia), jaw claudication
what diagnostics can help in the diagnosis of giant cell arteritis?
elevated ESR and CRP, definitive: temporal artery biopsy, imaging
what is the treatment for giant cell arteritis?
ASAP high dose prednisone (40-60 mg) x 1 month then taper
necrotizing arteritis of medium vessels with predilection fro skin, peripheral nerves, renal arteries, heart, and brain (NOT the lungs)
polyarteritis nodosa (PAN)
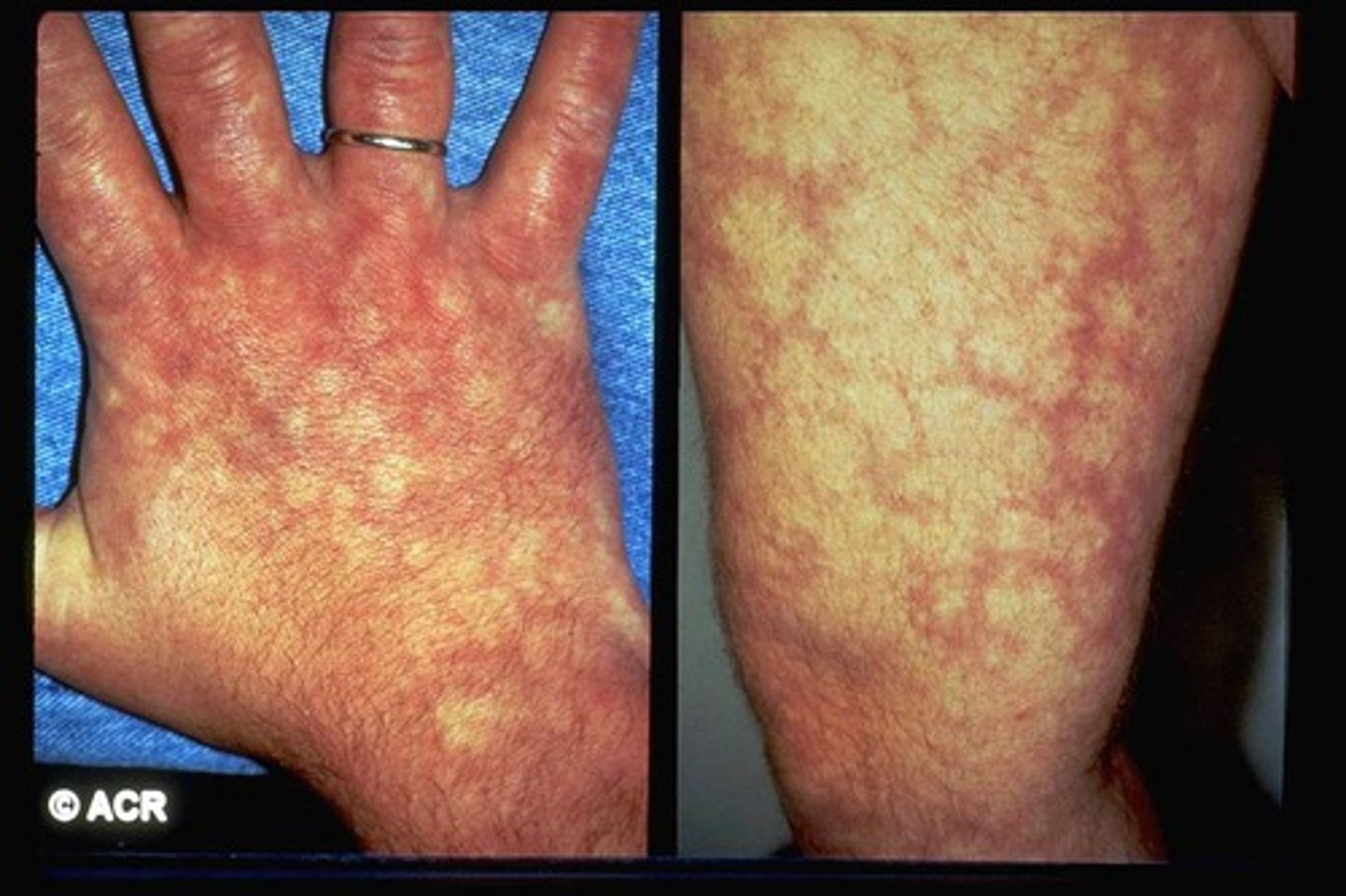
what are the sxs/s of polyarteritis nodosa (PAN)?
fever, malaise, weight loss, pain in extremities (joints, muscles), skin findings (livedo reticularis, subQ nodules, ulcers), digital gangrene, HTN
what tests can help in the diagnosis of polyarteritis nodosa (PAN)?
labs: anemia, leukocytosis, elevated ESR and CRP
diagnose via biopsy or vascular imaging
what is the treatment for polyarteritis nodosa (PAN)?
methylprednisolone 1 gm IV x 3 days
cyclophoshamide followed by MTX
treat Hep B
an inflammatory myopathy characterized by chronic inflammation of skeletal muscle
polymyositis
what are the sxs/s of polymyositis?
painless, proximal muscle weakness (shoulder and hips), gottron papules, heliotrope eyes
+- rash (shawl sign) -> dermatomyositis
fatigue, fever, weight loss
what tests (and results) can be ordered for polymyositis?
elevated muscle enzymes (CK, aldolase, LDH)
muscle/skin biopsy
what is the treatment for polymyositis?
steroids, MTX, TNF-a inhibitors
arthritis without rheumatoid factor with strong association with HLAB27
seronegative spondyloarthropathies
• Ankylosing spondylitis
• Reactive arthritis
• Psoriatic arthritis
• IBD related arthritis
joint inflammation often triggered by an infection somewhere else (GU or GI; chlamydia, salmonella, parvovirus B19)
reactive arthritis
what are the sxs/s of reactive arthritis?
conjunctivitis/uveitis, urethritis/cervicitis, arthritis (knee or ankle)
keratoderma blennarrhagica
what tests should be ordered for reactive arthritis?
NAAT, HLA-B27, joint aspiration (would be sterile)
what is the treatment for reactive arthritis?
NSAID and treat underlying infection
what are the sxs/s of psoriatic arthritis?
preceding psoriasis (silver scales, nail pitting)
asymmetric arthritis, sausage finger and toe appearance (dactylitis)
what are the XR findings for psoriatic arthritis?
osteolysis, pencil-in-cup deformity, sacroilitis, relative lack of osteoporosis
(none sensitive or specific)
what are the treatment options for psoriatic arthritis?
TNF inhibitors, IL-23 inhibitors, PDE-4 inhibitors, MTX
a chronic disease of pain processing characterized by widespread MSK pain, fatigue, and painful localized soft tissue areas
fibromyalgia
what are the sxs/s of fibromyalgia?
widespread chronic pain, severe fatigue, sleep dysfunction, cognitive impairment, depression/anxiety, HA
tense, ropy muscles
no swelling, rash, deformity, mass
fibromyalgia diagnosis
painful tender points (need 11 of 18 for diagnosis; present for >3 months)
*diagnosis of exclusion
what are the treatment options for fibromyalgia?
non-pharmalogical and pharmacological (lyrica, cymbalta, savella)
loss of bone mineralization, reducing bone integrity and strength, increasing risk of fracture
osteoporosis
what pt population most often gets osteoporosis?
white women
what are the sxs/s of osteoporosis?
asx until fracture
can have height loss
what are some possible causes of osteoporosis?
aging, small body size, alcoholism, cigarette smoking, white ethnicity, female gender, genetics, hormone deficiency (estrogen), carbonated beverages, immobilization, long-term med use (steroids, PPIs, SSRIs)
what medications can cause osteoporosis?
corticosteroids, heparin, PPIs, SSRis, SGLT2-i, GnRH
what is the best test for osteoporosis diagnosis?
DEXA scan hip and spine (T-score of less than -2.5 S.D.)
normal DEXA t score
-1 and higher
osteopenia DEXA t score
-2.5 to -1
what is the treatment for osteoporosis?
weight bearing exercise, smoking/alcohol cessation, calcium + vit D
bisphosphonate
when do you treat osteopenia (pharmacologically?
if they get a fracture / have high FRAX score
Risk assessment tool that calculates a patients 10-year risk of developing an osteoporosis related fracture
FRAX score
what is the screening recommendation for osteoporosis?
women 65 year or older
(or younger women with more than 1 risk factor)
infection and inflammation of the bone and bone marrow
(acute or chronic)
osteomyelitis
what are the 3 mechanisms of infection for osteomyelitis?
bloodstream, local infection (cellulitis goes deep), penetrating trauma (or surgery)
what are some risk factors for osteomyelitis?
DM, sickle cell, HIV/AIDS, RA, IV drug use, alcoholism, long term steroid use, recent penetrating trauma
what is the treatment for osteomyelitis?
surgical debridement and IV abx for weeks
osteomyelitis diagnosis
XR -> bony erosions
osteomyelitis symptoms
localized bone pain, swelling, redness, and warmth at the infection site, often accompanied by fever, chills, and fatigue
*usually a cellulitis that has existed for weeks