Mobility PPT
1/78
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
79 Terms
At the completion of this module, the learner will be able to:
1.Describe the effects of aging on musculoskeletal function.
2.List the benefits of activity.
3.Describe the adjustments that may need to be made in exercise programs in late life.
4.Discuss the challenges older adults may face in maintaining an active state.
5.List actions that could benefit an older adult who has impaired mobility.
6.Discuss the role of nutrition in musculoskeletal health.
7.Describe factors contributing to, symptoms of, and related nursing care for fractures, osteoarthritis, rheumatoid arthritis, osteoporosis, gout, and podiatric conditions.
8.Discuss pain management measures for musculoskeletal problems.
9.Identify ways to reduce risks of injury associated with musculoskeletal problems.
10.Describe measures to facilitate independence in persons with musculoskeletal problems.
OBJECTIVES
OBJECTIVES
what’re the effects of aging on musculoskeletal fxn?
•Decline in size and number of muscle fibers and reduction in muscle mass
•Connective tissue changes reducing flexibility
•Sarcopenia
•Psychosocial factors impacting activity
define sarcopenia
•Decline in walking speed or grip strength
•Can lead to disability
what’re some of the psychosocial factors that impact activity?
•Loss of spouse and/or friends; retirement; financial limitations; poor health; relocation to smaller home or facility
break down what sarcopenia is SPECIFICALLY for men and women?
<30kg for men and less than 20kg for women (generally)
what are the following exemplifying:
•Difficulty engaging in activity and exercise 2/2 shortness of breath
•Decreased peripheral tissue perfusion
•Increased fatigue, decreased stamina, and/or reduced muscle strength
•Decreased ROM
•Difficulty seeing, hearing, and feeling due to sensory-related changes with aging
•Chronic conditions/pain
•Financial situation
Potential Barriers to Maintaining an Active State
what are some ways we can promote musculoskeletal health in the OA?
•Promote physical exercise in all age groups
•Tailor exercise to the older adult
•The mind–body connection
•Prevent inactivity
Nutrition
•Educate and encourage regular exercise
Exercise programs
what should exercise programs address for promoting physical exercise in all age groups?
•Cardiovascular endurance
•Flexibility
Strength training
what should exercise programs address for cardiovascular endurance?
•aerobic, reach at least 55% of maximum heart rate, moderate intensity at least 30 minutes 5 days a week; adjustments per conditions
what should exercise programs address for flexibility?
•gentle stretching 5–10 minutes before and after other exercises; major muscle groups stretched at least twice weekly
what should exercise programs address for strength training?
resistance and progression, set of 8 to 12 repetitions at least twice weekly
how do we calculate the maximum heart rate (when exercising)?
220 − age
how do we calculate the target heart rate (when exercising)?
•maximum heart rate × 75%
how do we calculate the target heart rate RANGE (when exercising)?
65% to 80% of maximum heart rate
what can heart rate monitors provide with regards to target heart rates and exercising?
they can provide feedback on heart rate during exercise without the inconvenience of having to stop to palpate the pulse.
what are the benefits for exercise programs that’re tailored to OAs?
•Delay or prevent some age-related effects
•Cardiovascular: improve oxygen intake, lower resting blood pressure
•Musculoskeletal: increase muscle strength, flexibility, slow rate of bone loss
•Improve body tone, circulation, appetite, digestion, elimination, respiration, immunity, sleep, self-concept
•Provide opportunities for socialization, recreation, motivational support
what shoul dyou do if you have an OA who is unable to participate in formal exercise programs?
•Build less aggressive exercises into daily activities and promote maximum activity during routine care activities
•Provide partial/complete assistance for ROM exercises and use of assistive devices prn
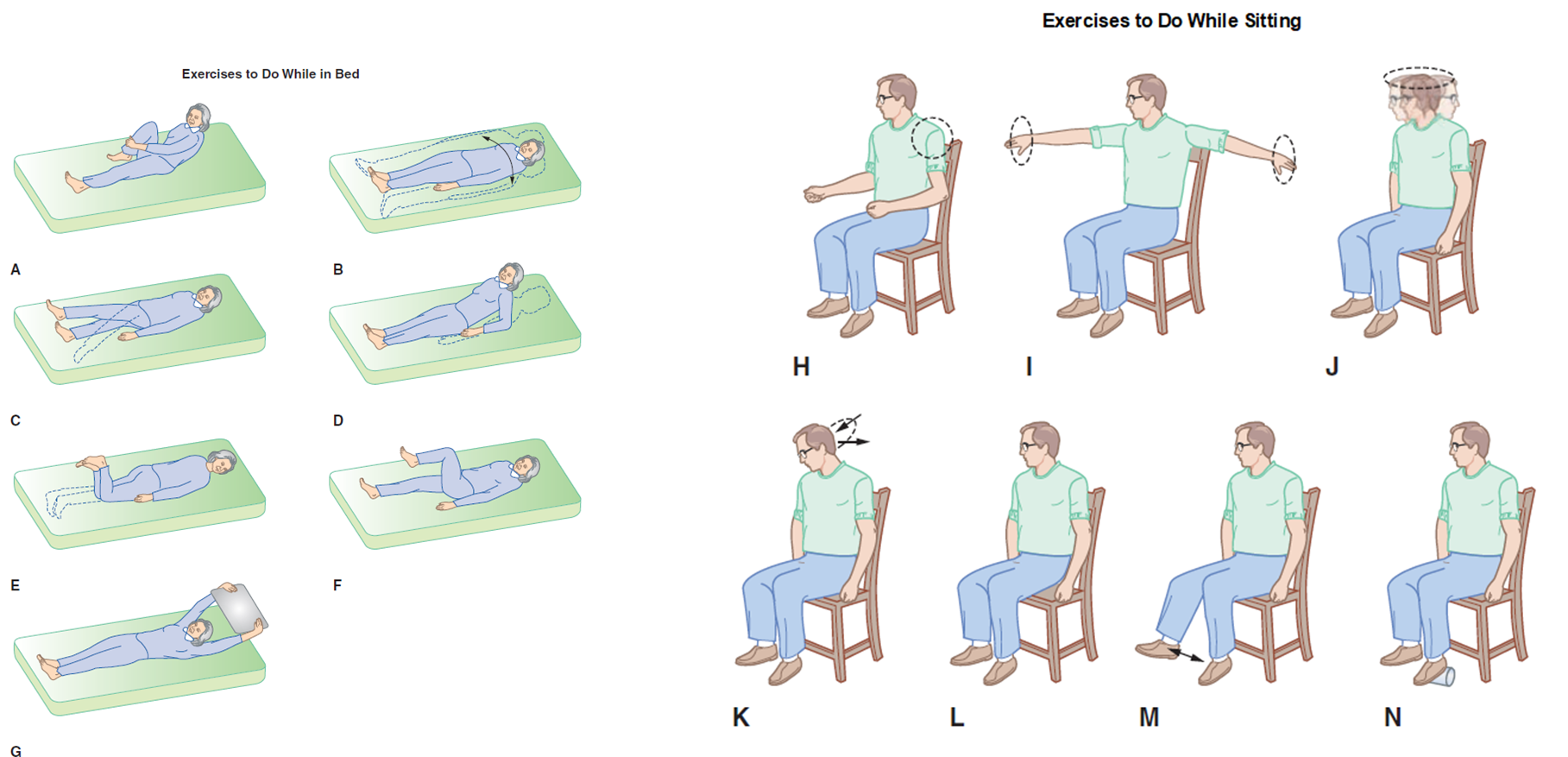
exercises for OAs
exercises for OAs
what is the “mind-body connection” for OA and exercise/overall health?
•Cognitive and emotional states can influence physical activity
•Physical activity can have positive effects on mood and cognition
what are some things to keep in mind when promoting the mind-body connection for yhe OA?
Individualized activities based on unique interests:
•Current hobbies or activities OR new interests
•Pets, family
•Consider the 4 M’s Framework
what is “therapeutic recreation” for the mind-body connection in the OA?
•Structured leisure with specific goal in mind
what should nurses always keep in mind when promoting the mind-body connection in the OA?
•Consult specialists in various fields
•Adequate time and patience necessary
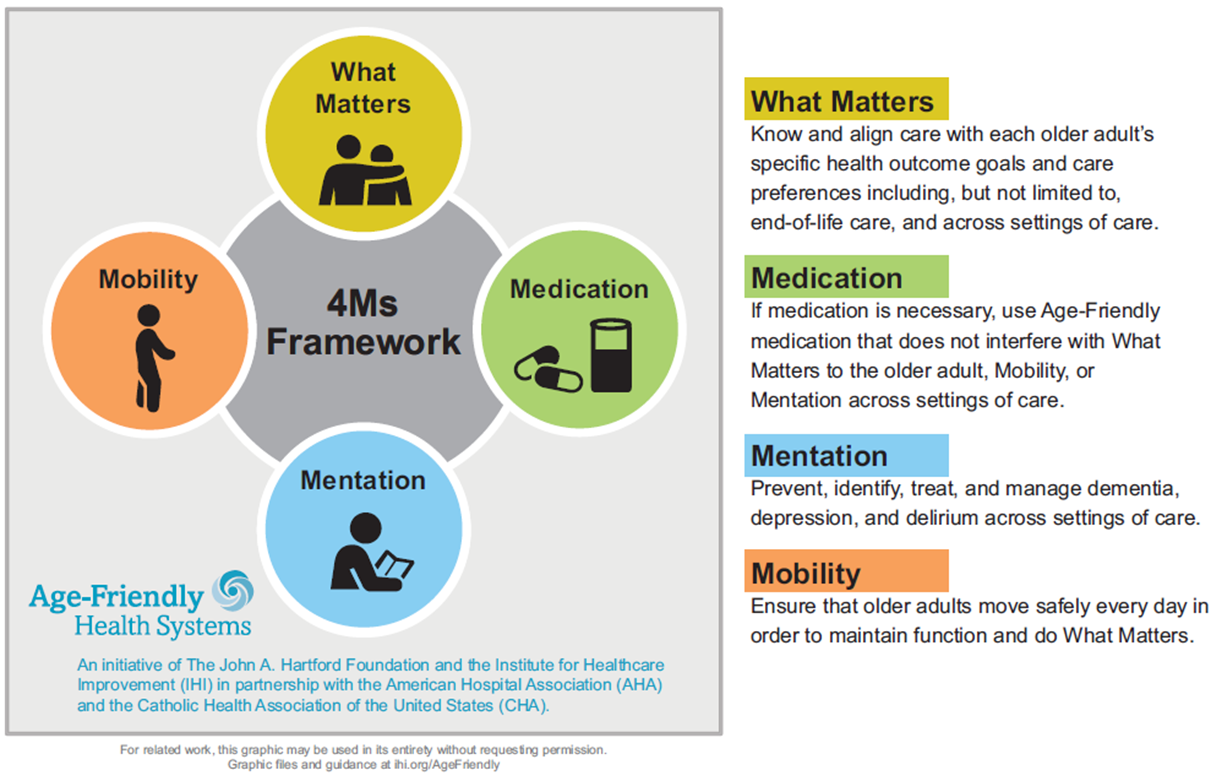
mind-body connection visual
mind-body connection visual
what does inactivity result in?
deconditioning and increased risk of complications
what happens to activity and thus preventing inactivity w age?
there is a need to compensate for age-related changes (sarcopenia, decreased endurance, etc.)
what should you as the nurse keep in mind when preventing inactivity in the OA?
•Suggest pastimes that can stimulate movement/create purpose
•Demonstrate sincere interest in their individual interests, preferences, and abilities
•Inform about local resources including transportation
•Avoid stereotyping (assuming they like an activity (ex: dominoes) just because of their age)
what do you need to recognize w regards to nutrition for the OA?
•Recognize the importance of good nutrition.
what type of diet is needed for the OA to maintain the structure of bones and muscles?
Well-balanced diet rich in protein and minerals
Calcium: minimum of 1,500 mg daily
•=Both quality and quantity are important.
what does obesity do to the OA?
•Obesity places strain on the joints.
•encourage Weight reduction
what are the following:
•Difficulty performing ADLs and/or IADLs
•Risk of injury
•Powerlessness, isolation, difficulty interacting
•Pain (acute, chronic)
•Anxiety, Fear, difficulty sleeping
•Difficulty engaging in activities, exercise, and mobility
potential nursing problems related to the msk system
what are the biggest causes of fractures for the OA?
•trauma, cancer metastasis to bone, osteoporosis, etc.
•Common sites: femur, distal radius, vertebrae
what are the features of brittle bones in the OA and fractures?
they fracture more easily and heal at a slower rate
•Potential for complications associated with immobility
what are some interventions for fractures that’re aimed at prevention?
•Caution against unsafe and/or risky activities
•Postural hypotension
•Proper shoes and assistive devices

fall prevention visual
fall prevention visual
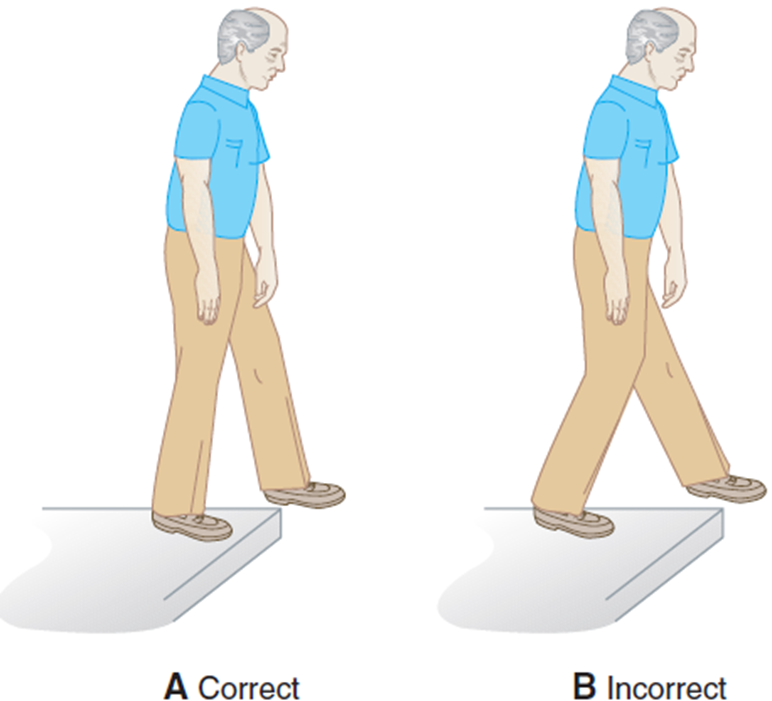
correct method for stepping to/fro a curb (place both feet near the edge of the curb before stepping)
when would be the biggest thing that happened in an OA that would make you suspect a fx?
a fall
your OA pt presents w the following s/sx:
pain, change in shape or length of limb, abnormal or restricted motion, edema, spasm of surrounding tissue, discoloration of tissues, open fracture
what are you thinking?
they likely have a fx
does absence of s/sx rule out there being a fx in an OA?
NO — overt signs or symptoms may appear later
what should you as the nurse do when a possible fx occured?
•Immobilize injured site during transport for evaluation
•Nursing observation essential
define osteoarthritis
•Progressive deterioration of joint cartilage with the formation of new bone at the joint surface
your pt presents w the following:
no systemic symptoms; distal joints may develop bony nodules (Heberden’s nodes); uncomfortable during damp weather and periods of extended use
what’s going on?
osteoarthritis
what’s the tx/management for osteoarthritis?
•Pain: analgesics (acetaminophen)
•Rest, heat or ice, t’ai chi, aquatherapy, gentle massage, acupuncture, splints, braces, canes
•Maintain proper body alignment; use good body mechanics
•Weight reduction
•Household assistance or assistive devices
•PT/OT
•Arthroplasty
what’re the nursing interventions for osteoarthritis?
•Ensure patient and caregivers understand instructions and adhere to plan of care
define rheumatoid arthritis
•Chronic autoimmune systemic disease
•Peak incidence 40-50 years of age
•Thought to be genetic
•70-80% have an antibody called Rheumatoid Factor (RF)
your pt presents w the following:
•joint pain, swelling, redness, warmth, deformity, loss of function, and joint stiffness
•Usually bilateral and symmetrical
•Nodules in hands and feet in later stages
what’s going on?
rheumatoid arthritis
is rheumatoid arthritis a normal part of aging?
NOT a normal part of aging; AND has a Greater incidence in females
what are the nursing interventions for rheumatoid arthritis tx?
•Green tea and ginger may improve symptoms
•Educate on disease, administration of medications and potential s/e, exercise regimens, use of assistive devices, methods to avoid and reduce pain
•Advise consulting with provider before investing in quick cure or relief
what meds are great for rheumatoid arthritis?
•NSAIDs, systemic steroids, disease-modifying antirheumatic drugs (DMARDs): Methotrexate, Hydroxychloroquine (plaquenil)
what are some broad tx for rheumatoid arthirits?
•Rest, limb support, ROM exercises, assistive devices, heat, gentle massage
•Surgery
what’s the most prevalent metabolic disease of the bone?
osteoporosis
where is osteoporosis seen in life?
primarily adults in middle to later life
what can “cause” osteoporosis?
•Any health problem associated with inadequate calcium intake, excessive calcium loss, poor calcium absorption can cause osteoporosis
what’re the risk factors for osteoporosis?
•Advanced age (women over 65, men over 80)
•Ethnicity
•Calcium deficiency
Vitamin D deficiency
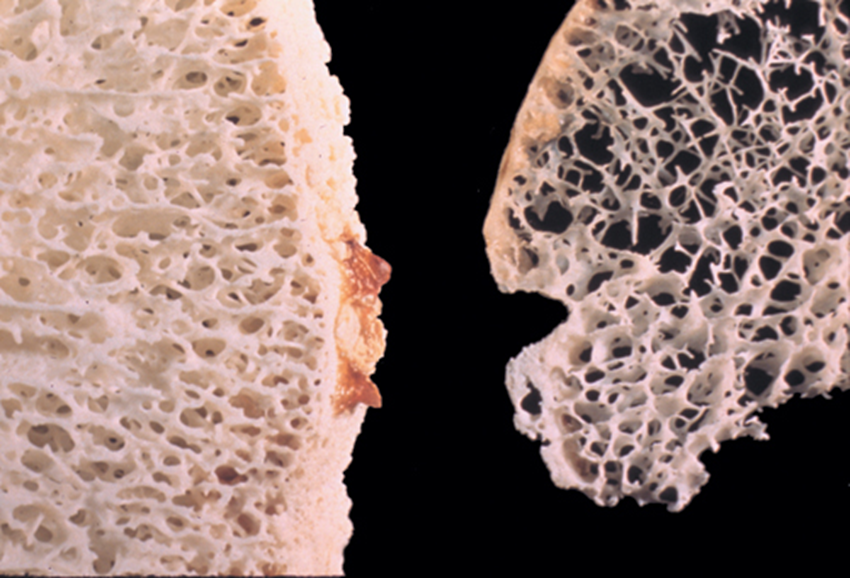
Image: Femoral head of an 82-year-old woman with osteoporosis and femoral neck fracture (right), compared with a normal control bone cut to the same thickness (left).
Image: Femoral head of an 82-year-old woman with osteoporosis and femoral neck fracture (right), compared with a normal control bone cut to the same thickness (left).
why is osteoporosis commonly seen in older women?
because Estrogen plays important role in bone remodeling and regulates osteoblasts. In post-menopausal women there is a lack of estrogen which inhibits bone growth.
what can osteoporosis cause?
•May cause kyphosis, spinal pain, and fractures
how is osteoporosis dx?
•(often asymptomatic)
•Bone density via DEXA scan
what does the treatment for osteoporosis depend on?
on underlying cause
what’re some meds, diet, and exercise recommendations when treating osteoporosis?
•Medications: calcium supplements, vitamin D supplements, selective estrogen receptor modulators, synthetic calcitonin, bisphosphonates
•Diet: rich in protein and calcium
Exercise, weight bearing activities
what’re the nursing considerations for the pt w osteoporosis?
•Advise against heavy lifting, jumping, and similar activities
•Individuals providing care must be gentle to avoid fractures
•ROM exercises and ambulation important
what is going on w gout?
•Metabolic disorder in which excess uric acid accumulates in the blood, uric acid crystals deposited in and around joints
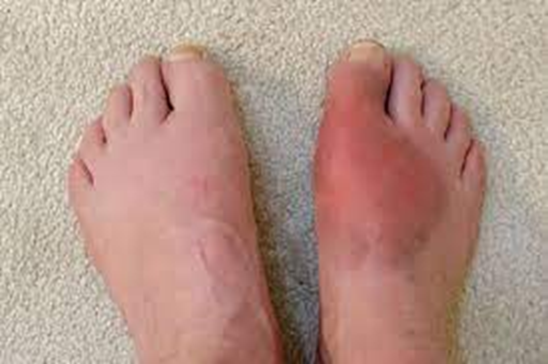
gout visual
gout visual
your pt presents w the followinf:
•Severe pain/tenderness of joint; warmth, redness, swelling of surrounding tissue; during acute attack, pain can be quite severe and impact mobility; may wax and wane
what’s going on?
gout
what’s the tx for gout?
•Low-purine diet (avoid pork, red meat, shrimp, wine)
•Medications:
—•Acute attacks: colchicine
—•Long-term management: colchicine, allopurinol, probenecid, indomethacin
•Avoid alcohol and thiazide diuretics
•Dietary supplements: vitamin E, folic acid, eicosapentaenoic acid, yucca, devil’s claw
what’re the nursing interventions for gout?
•monitor pain, encourage fluid intake
what are the characteristics of podiatric conditions in OAs?
•Foot problems are a common occurrence (Podogeriatrics)
•Refer to podiatry (they should NOT be cutting their own nails)
•Education related to proper foot care, footwear, orthotic inserts, importance of seeking professional care for problems
check feet daily, careful w water temps
what are the nursing interventions for podiatric conditions in the OA?
•Offer foot massages if not contraindicated
•Effectively identify and seek treatment to improve mobility and independence
what are the BRAOD podiatric risks in the OA?
•Impaired circulation and sensation
•Common deformities include bunions, hammertoe, corns
•High-Risk Nail and Skin care (•Thick, long nails or cracked dry skin create easy points for infection (i.e cellulitis))
•Foot/Ankle immobility: Arthritis and loss of connective tissue elasticity reduces stability; Plantar fascitis
•Infections
what is going on w impaired circulation and sensation for podiatric risks in the OA?
Peripheral neuropathy and PVD >> delayed wound healing and unnoticed injury
what do the common foot deformities do to the OA?
Cause pain that limits ability to wear shoes of tolerate WB
what are some infections that affect the OA in their feet? (podiatric)
•Onychomycosis: fungal infection of nail or nail bed; treatment: antifungal preparations
•Tinea pedis: athlete’s foot; fungal infection of foot; breaks in skin can lead to bacterial infections
what are some other injuries that affect an OA podiatrically?
Ingrown nails (onychocryptosis):
•As nail grows, edge cuts into tissue, leading to inflammation
•Treatment: Soaks and topical antibiotics; podiatrist removal of ingrown portion and cleaning of area
what happens if msk conditions and the pain associated isnt addressed?
•if unrelieved, QOL affected
•Joint pain, muscle cramps
•Essential in promoting optimal physical, mental, and social function
—Heat, passive stretching, back rubs, resting, supporting painful joints during transfers, using assistive devices, correct positioning, diversional activities, alternative therapies
how do we prevent injury msk in the OA?
•Safety interventions essential: activities, clothing, heat, careful handling of individual
how/why do we promote independence for msk in the OA?
•Impact on physical, emotional, and social well-being
•Interventions: assistive devices
Is the following statement true or false?
A primary goal of nursing interventions for older adults with a musculoskeletal disorder is to promote independence.
True
(Rationale: One of the goals of the nursing interventions is to help each older adult with regaining and maintaining his or her independence as much as possible.)
Which of the following diets is encouraged for those who have the diagnosis of gout?
(Rationale: Dietary treatment for gout aims to reduce sodium urate through a low-purine diet, which means avoidance of bacon, turkey, veal, liver, kidney, brain, anchovies, sardines, herring, smelt, mackerel, salmon, and legumes.)
Low purine
Which of the following bones are a common site for fractures in older adults as a result of a fall? Select all that apply.
A.Neck of the femur
B.Distal radius
C.Vertebrae
D.Rib
Ankle
(Rationale: All bones in the older adult are at risk of being fractured during a fall; however, the more common sites include the neck of the femur, the distal radius (referred to as Colles’ fracture), and the vertebrae.)
A. Neck of femur; B. Distal radius; C. Vertebrae
Is the following statement true or false?
Systemic symptoms often accompany osteoarthritis.
False
(Rationale: Systemic symptoms are not common in persons with osteoarthritis. Systemic symptoms are more common with rheumatoid arthritis and include fatigue, malaise, weakness, weight loss, wasting, fever, and anemia.)