Exam 1: Validity Testing, Mesenteric Doppler, Liver Doppler, Liver Pathologies, Liver Transplant, Renal Doppler, Renal Transplant
1/186
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
187 Terms
Gold Standard
Well-established, reliable diagnostic method used as a reference
Gold Standard for Vascular Imaging
Angiography
Validity
Ability of a test to distinguish between who has the disease and who does not
True Positive (TP)
Those who have disease and a positive test
Ultrasound shows disease, gold standard shows disease
True Negative (TN)
Those who do not have disease and a negative test
Ultrasound shows no disease, gold standard shows no disease
False Positive (FP)
Those who do not have disease and a positive test
Ultrasound shows disease, gold standard shows no disease
False Negative (FN)
Those who have disease and a negative test
Ultrasound shows no disease, gold standard shows disease
Sensitivity
Ability of test to correctly detect patients with disease compared to the gold standard - positive sonogram with positive gold standard
Sensitivity Formula
Number of true positive tests
Number of all positive tests by gold standard
Specificity
Ability of test to correctly detect patients without disease compared to the gold standard - negative sonogram with negative gold standard
Specificity Formula
Number of true negative tests
Number of all negative tests by gold standard
Positive Predictive Value (PPV)
Probability that a positive test result reflects the actual presence of disease
Portion of patients with a positive test that have disease
Positive Predictive Value (PPV) Formula
Number of true positive tests
Number of all positive noninvasive tests
Negative Predictive Value (NPV)
Probability that a negative test result reflects the actual absence of disease
Portion of patients with a negative test that do not have disease
Negative Predictive Value (NPV) Formula
Number of true negative tests
Number of all negative noninvasive tests
Accuracy
Degree of closeness of a test result to the actual value
Percentage of overall correct results
Must lie between sensitivity & specificity and PPV & NPV
Accuracy Formula
Total number of correct tests
Total number of all tests
Reliability
Consistency of obtaining similar results under similar conditions - reflects accuracy over time
Increasing Cut-Off Values
Improves specificity
More true negatives
Decreasing Cut-Off Values
Improves sensitivity
More true positives
Why is Validity Testing Important?
Required part of accreditation for labs
Ensures reason, quality, & completeness of exams
Ensures lab follows protocol & quality standards
Patient Prep for Mesenteric Study
NPO ≥ 6 hours - schedule early to avoid bowel gas
No smoking or gum chewing
Medications with water only
Patient supine
Low frequency curved transducer
Protocol for Mesenteric Study
RUQ first - eliminate GB as pain source
Pre and post-prandial images - 2D, color, spectral
Aorta at level of celiac axis and SMA
Origin of celiac axis
Origin of SMA
Origin of IMA
Celiac Artery Doppler Waveform
Low resistant
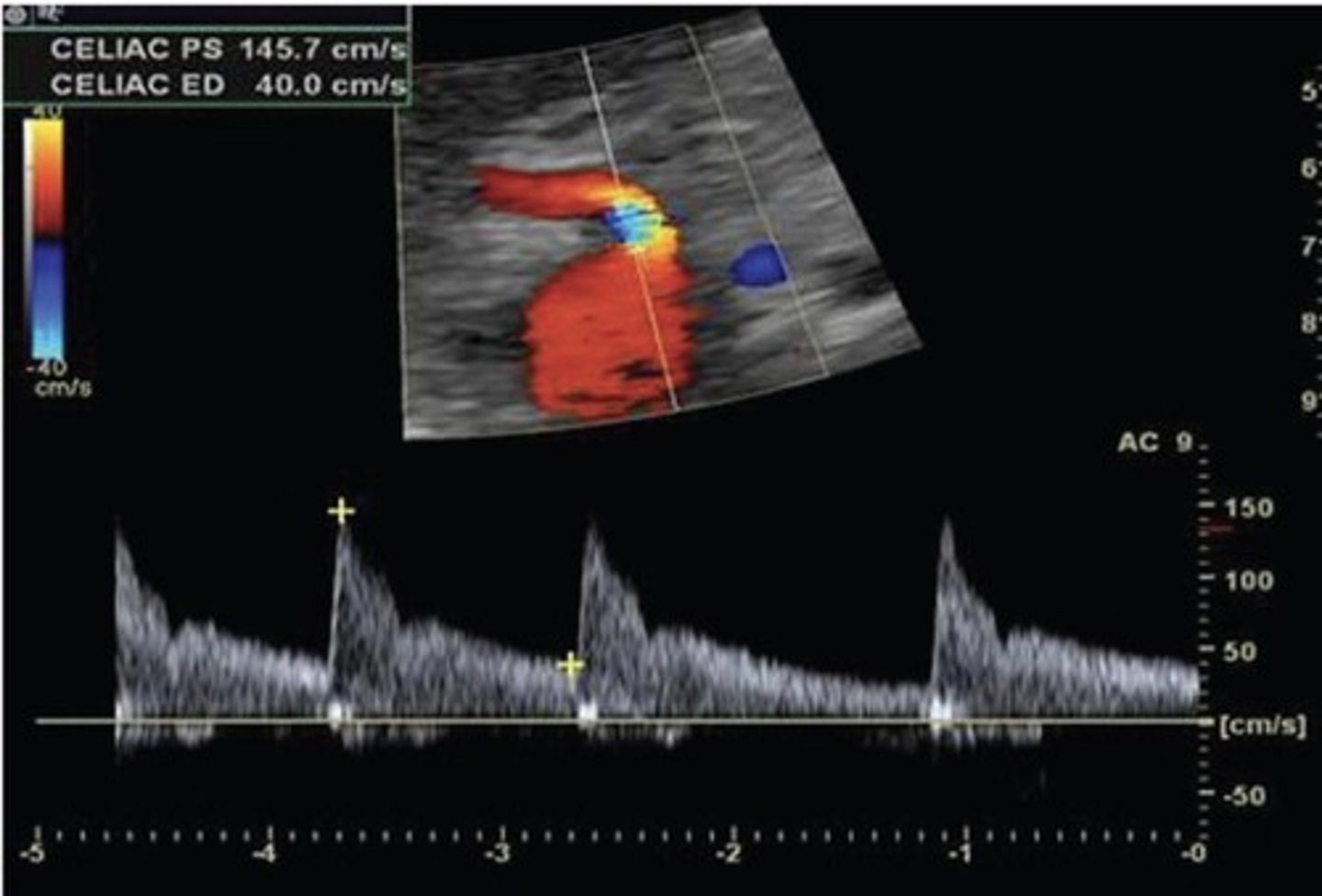
Celiac Artery PSV
101 cm/sec
Celiac Artery RI
0
70% Celiac Artery Stenosis PSV
≥ 200 cm/sec
Celiac Artery Occlusion
Results in SMA collaterals diverting blood through gastroduodenal artery toward the liver and spleen
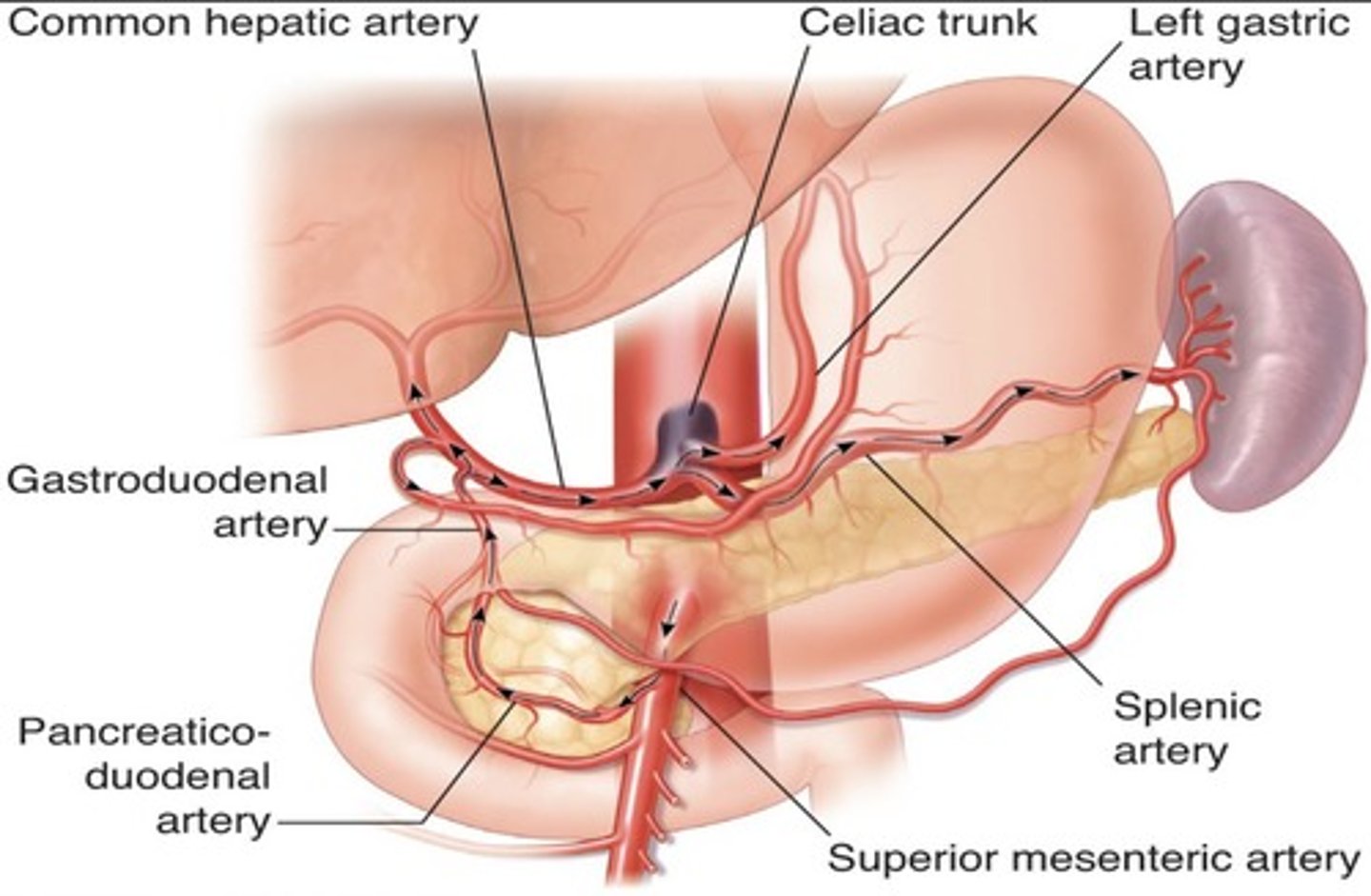
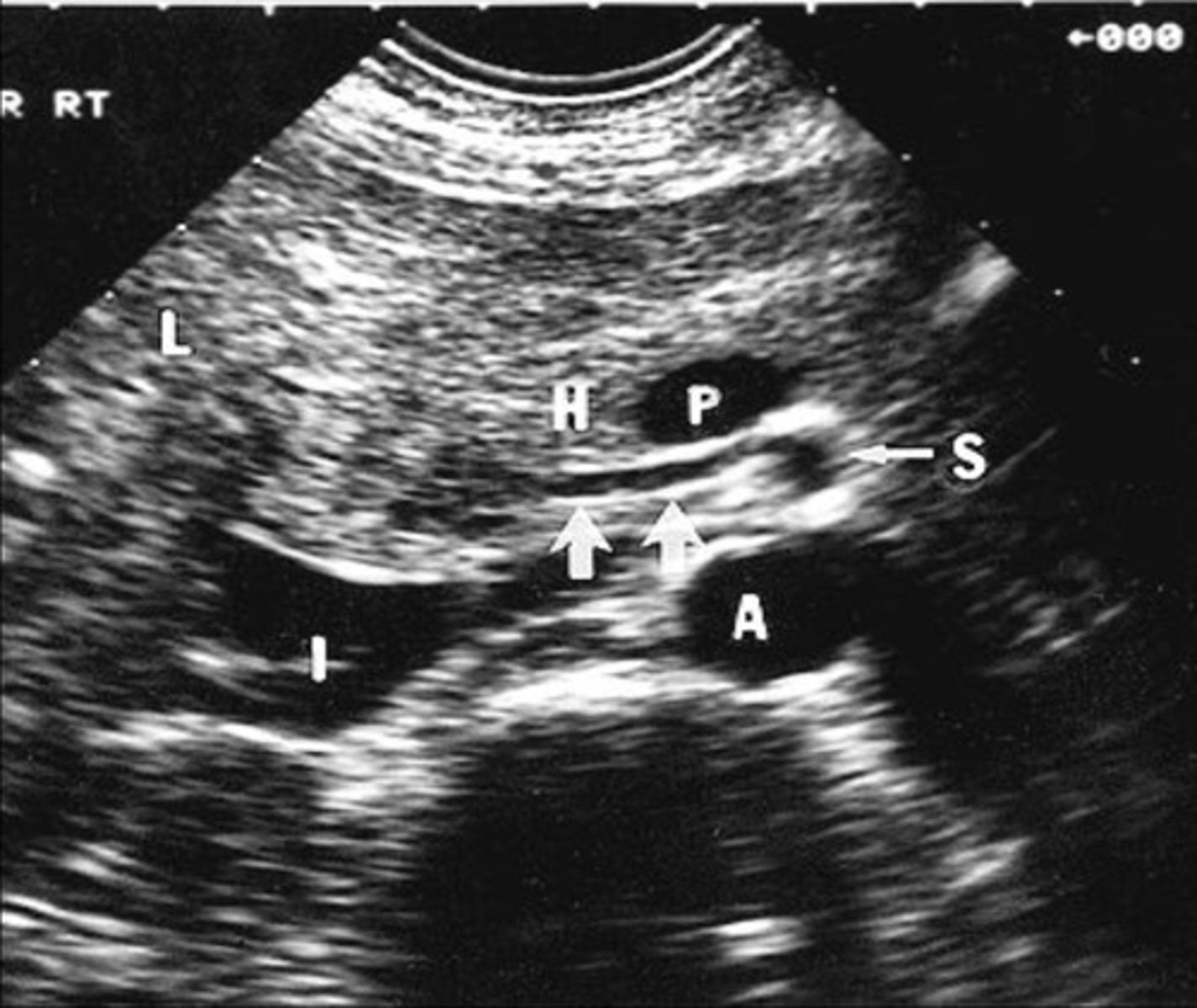
Replaced Right Hepatic Artery
Right hepatic artery branches off something else besides celiac artery - usually SMA
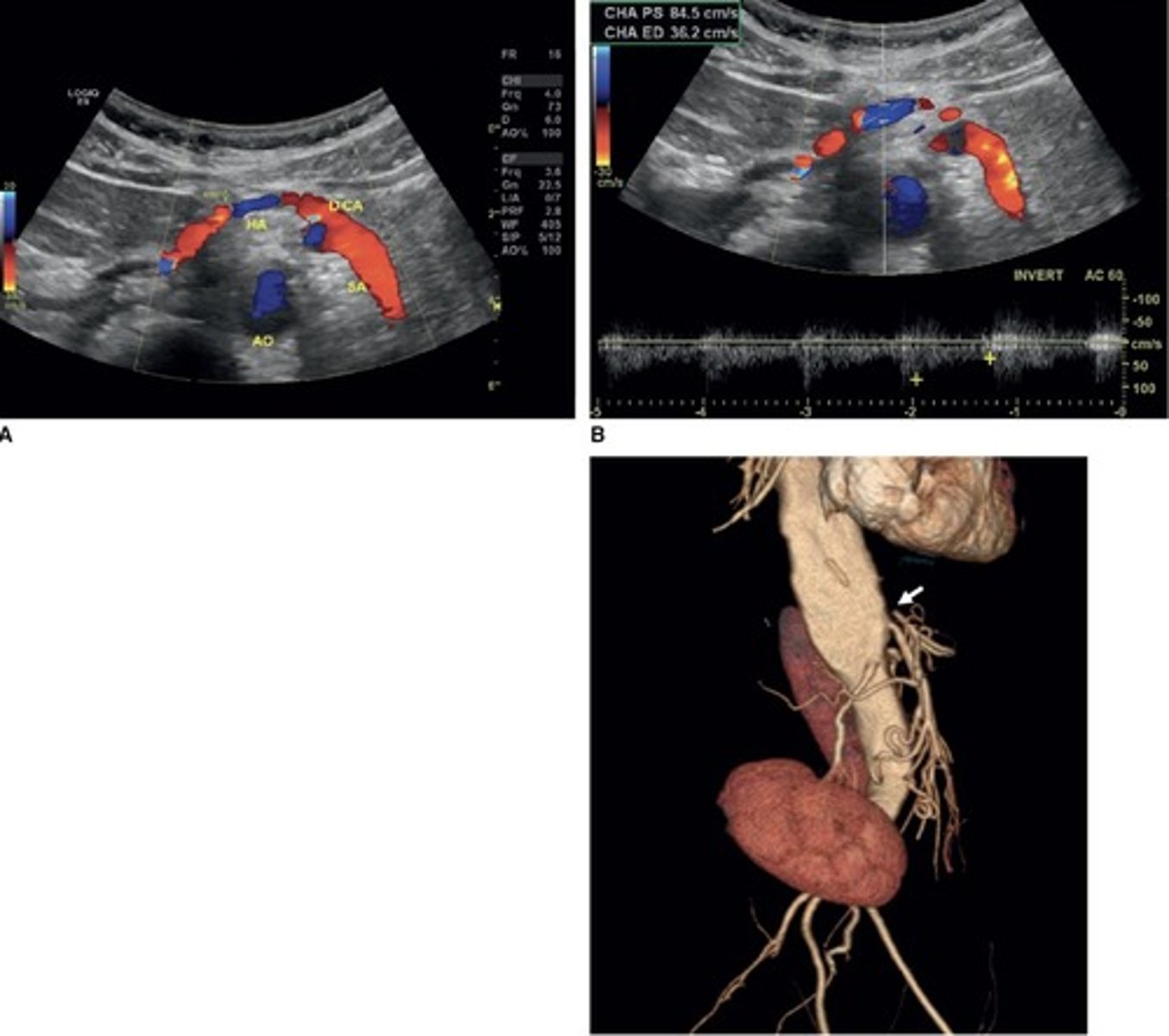
Hepatic Artery Retrograde Flow
Due to celiac artery occlusion
Blood flows towards splenic artery - RABT color pattern
Pre-Prandial SMA Doppler
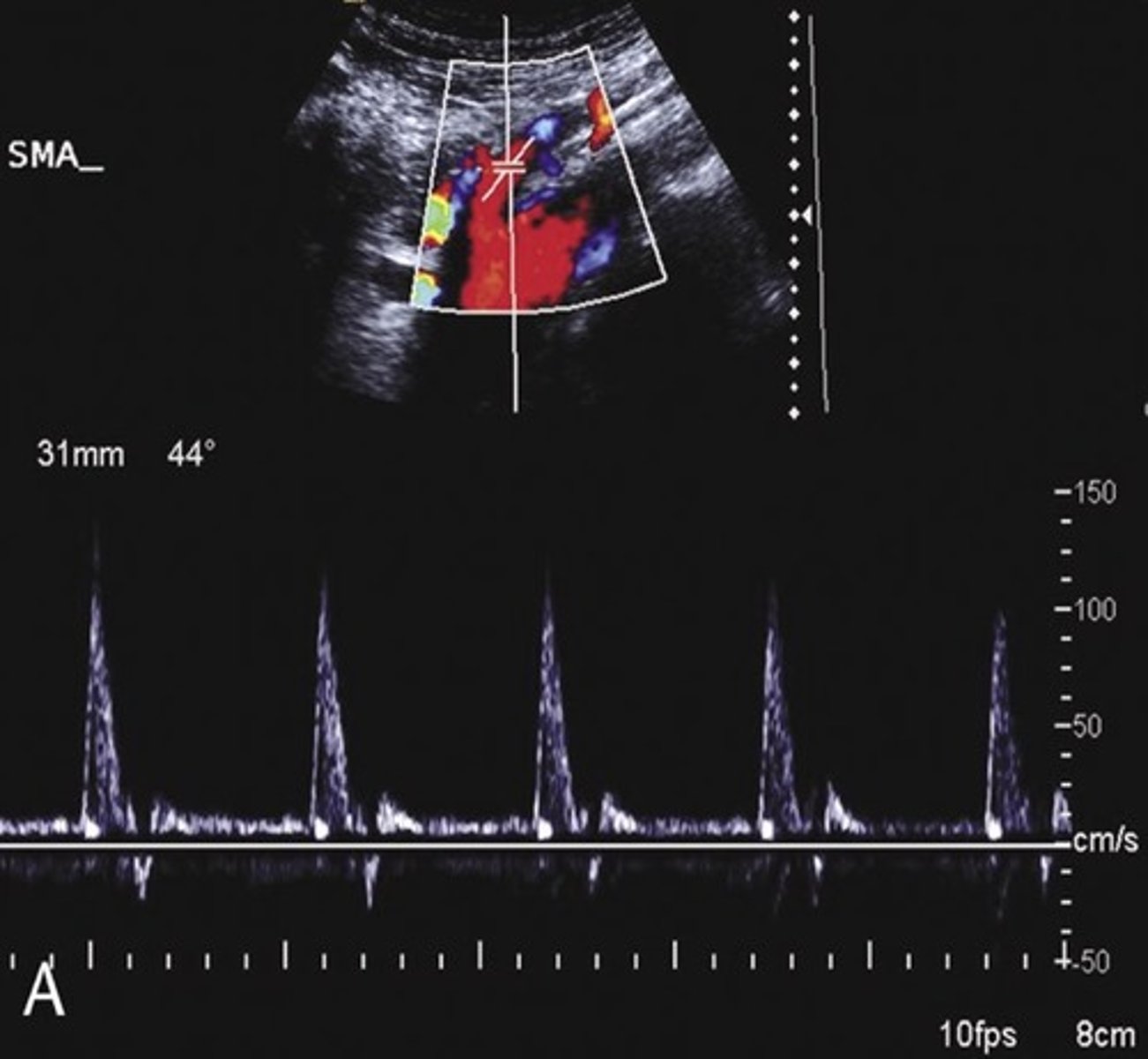
Post-Prandial SMA Doppler
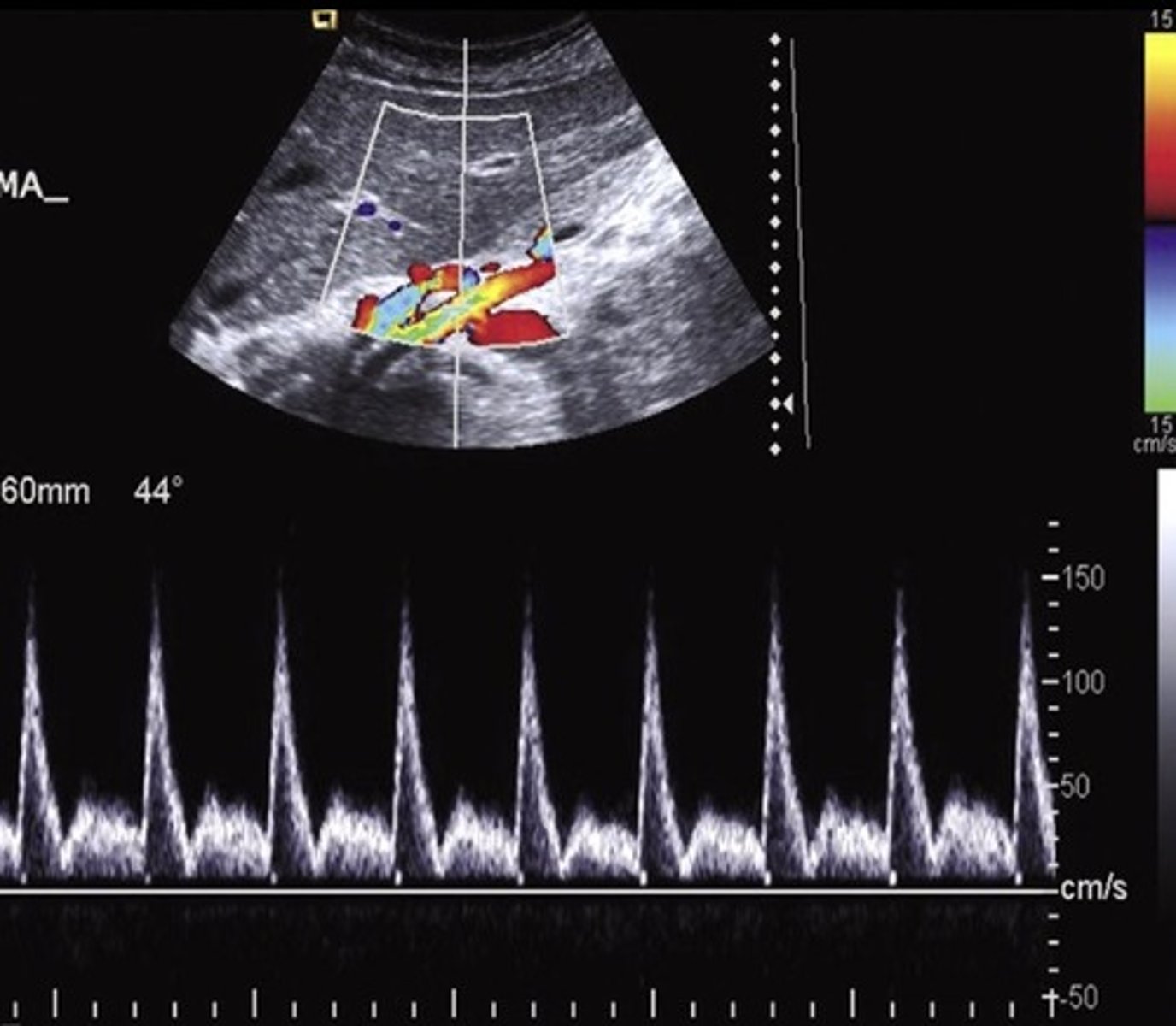
SMA PSV
113 cm/sec
SMA Stenosis
High velocity jet
Distal tardus parvus flow
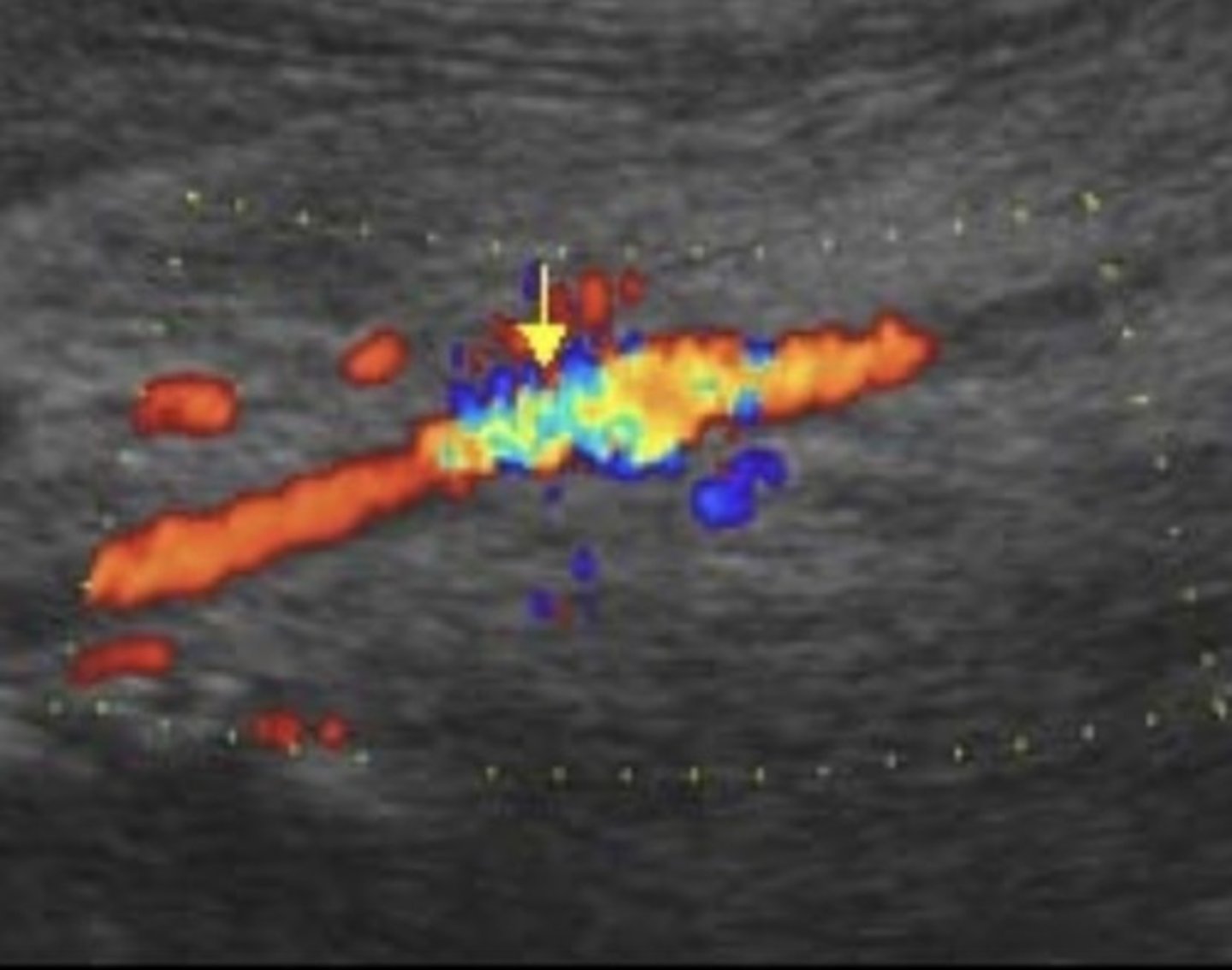
70% SMA Stenosis PSV
≥ 275 cm/sec
SMA Dissection
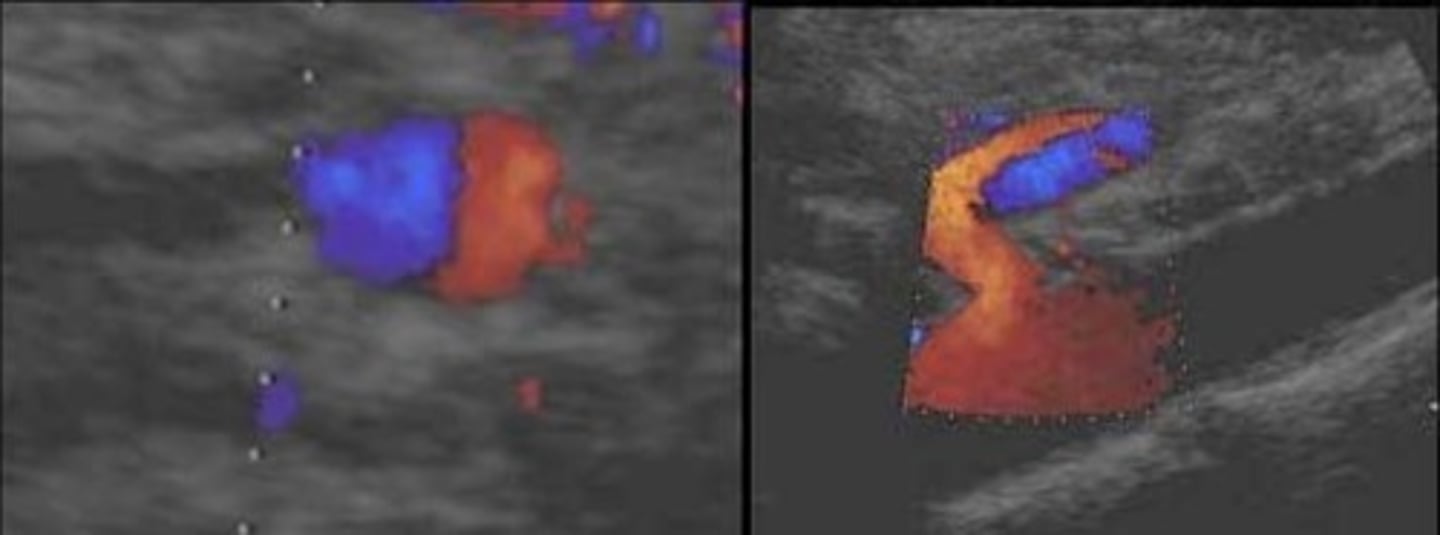
Common Trunk Variant
Celiac and SMA come off common trunk
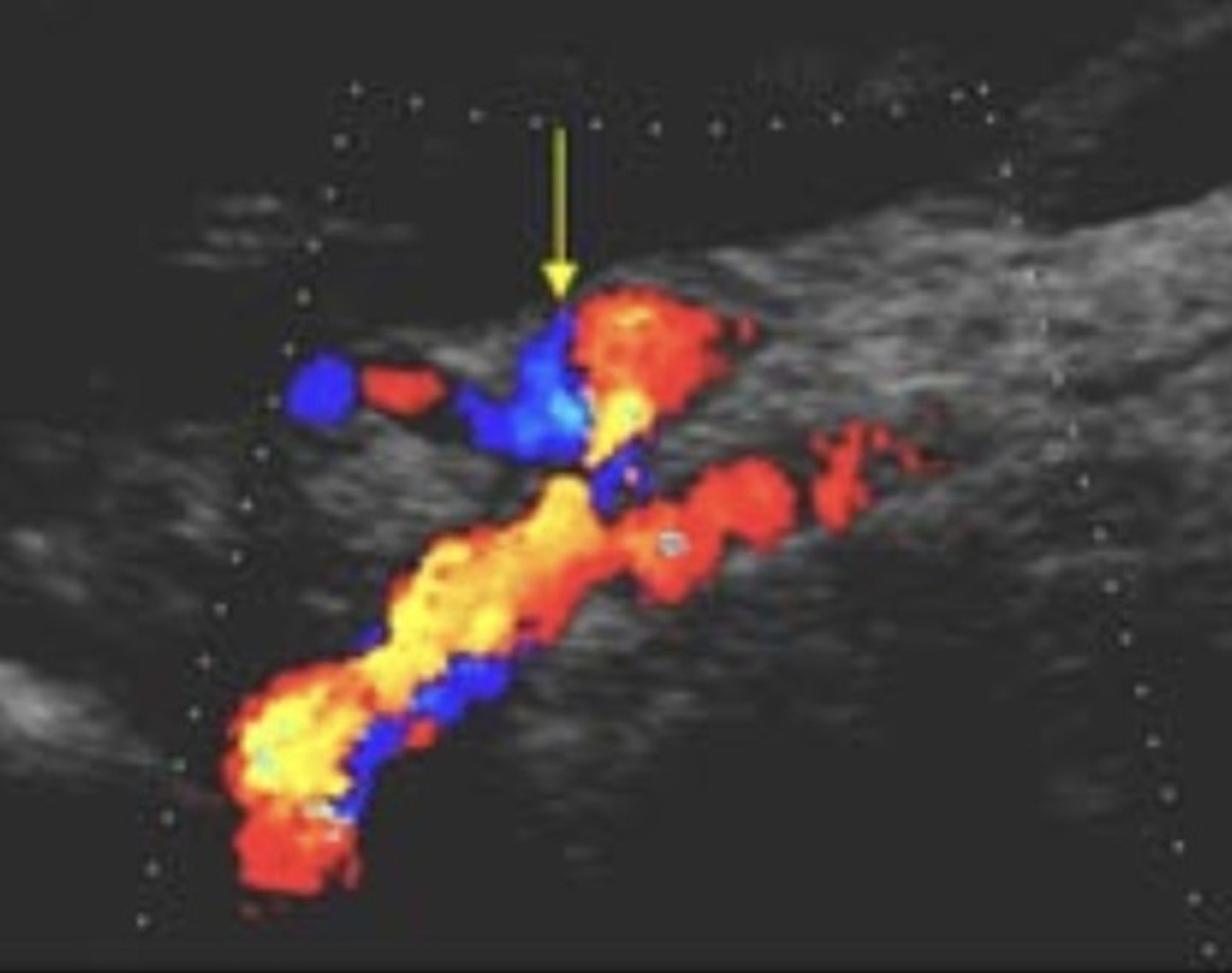
IMA
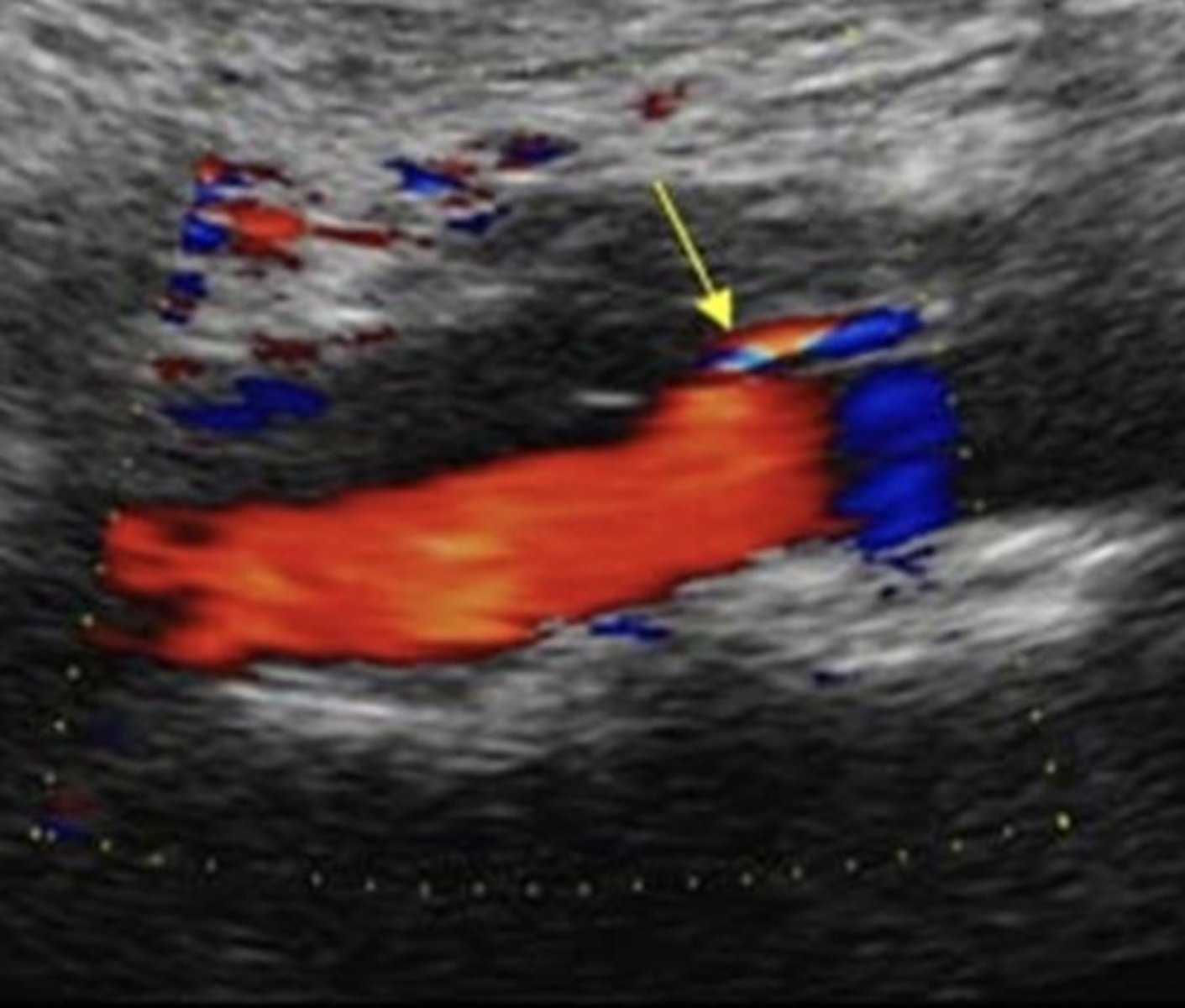
IMA PSV
141 cm/sec
IMA Stenosis PSV
> 200 cm/sec
Prominent IMA
Due to SMA occlusion
Acute Mesenteric Ischemia
Thrombosis of one or more mesenteric vessels
Life threatening - requires immediate intervention
Severe cramping/pain - disproportional pain
Chronic Mesenteric Ischemia
Low resistant pre-prandial doppler signals
70% occlusion of 2/3 splanchnic arteries required for diagnosis (celiac, SMA, IMA)
Epigastric pain after eating - fear of food, weight loss, decreased nutrition
Compensatory Flow
Elevated velocities in normal collateral vessels
No stenotic profile seen
Aneurysm
Most common in splenic artery
Life threatening if ruptured
Dissection
Separation of channels - flap line
To and fro flow
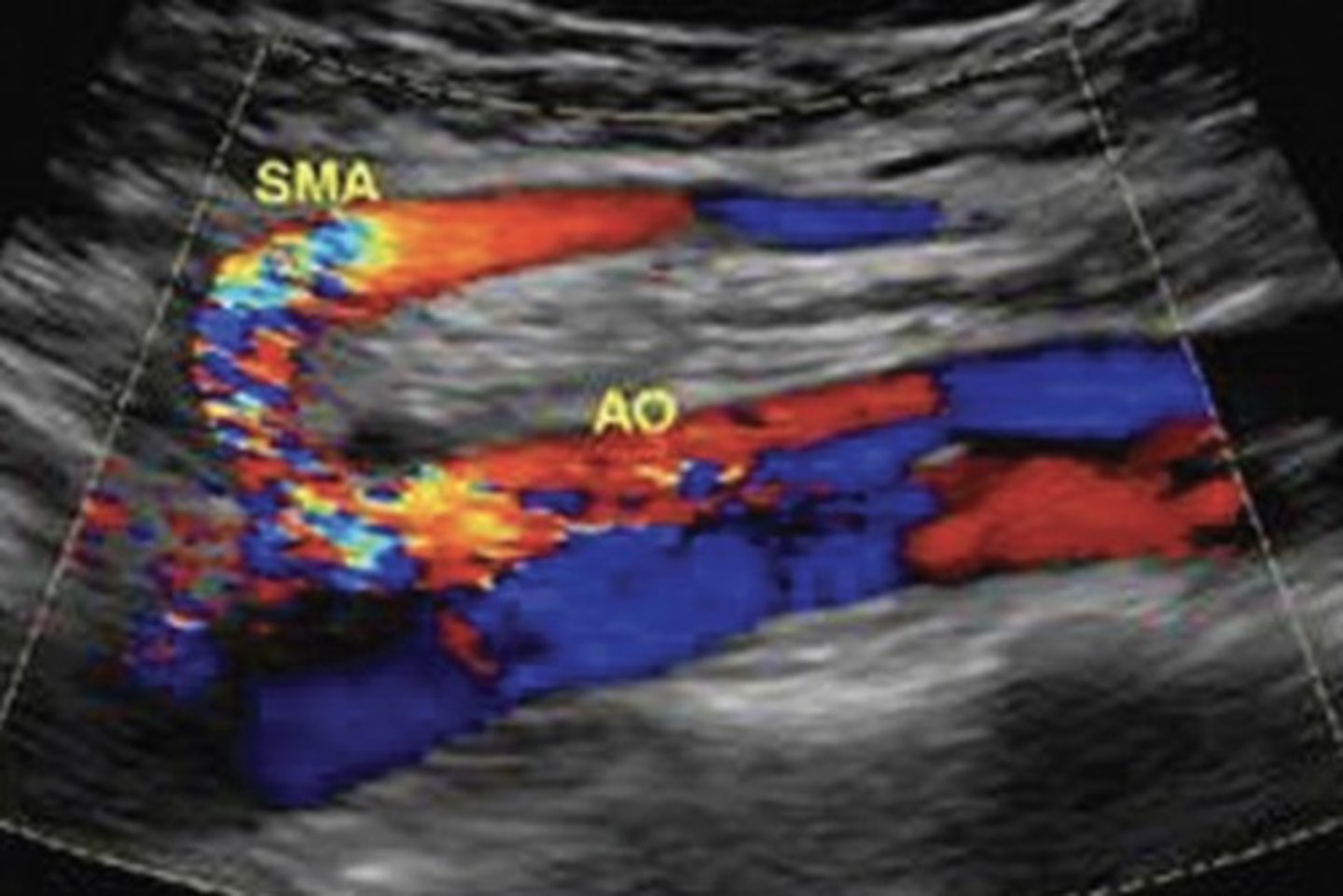
Bypass Graft Protocol
Inflow artery
Proximal anastomosis
Length of graft
Distal anastomosis
Outflow artery
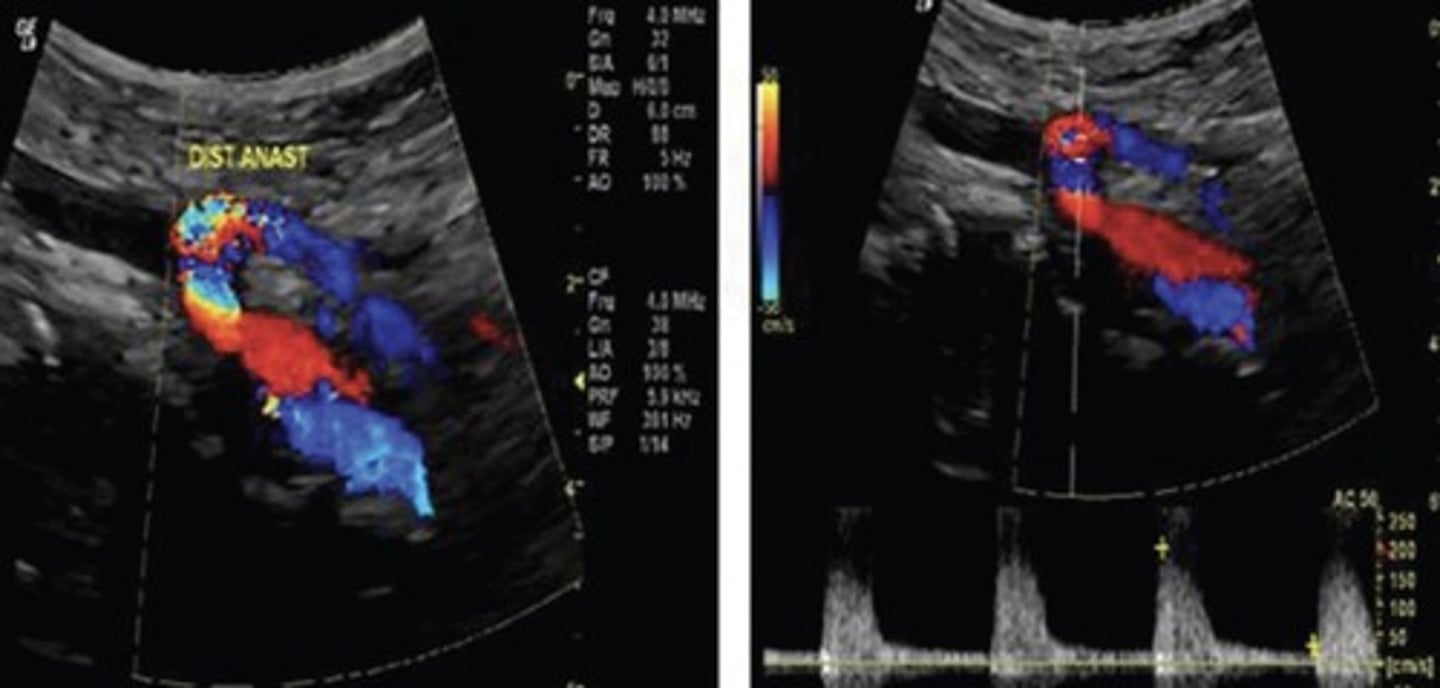
Median Arcuate Ligament Syndrome (MALS)
Compression of celiac axis during exhalation by median arcuate ligament
Pain relieved by inhalation
Evaluate in supine & upright positions and with inspiration & expiration
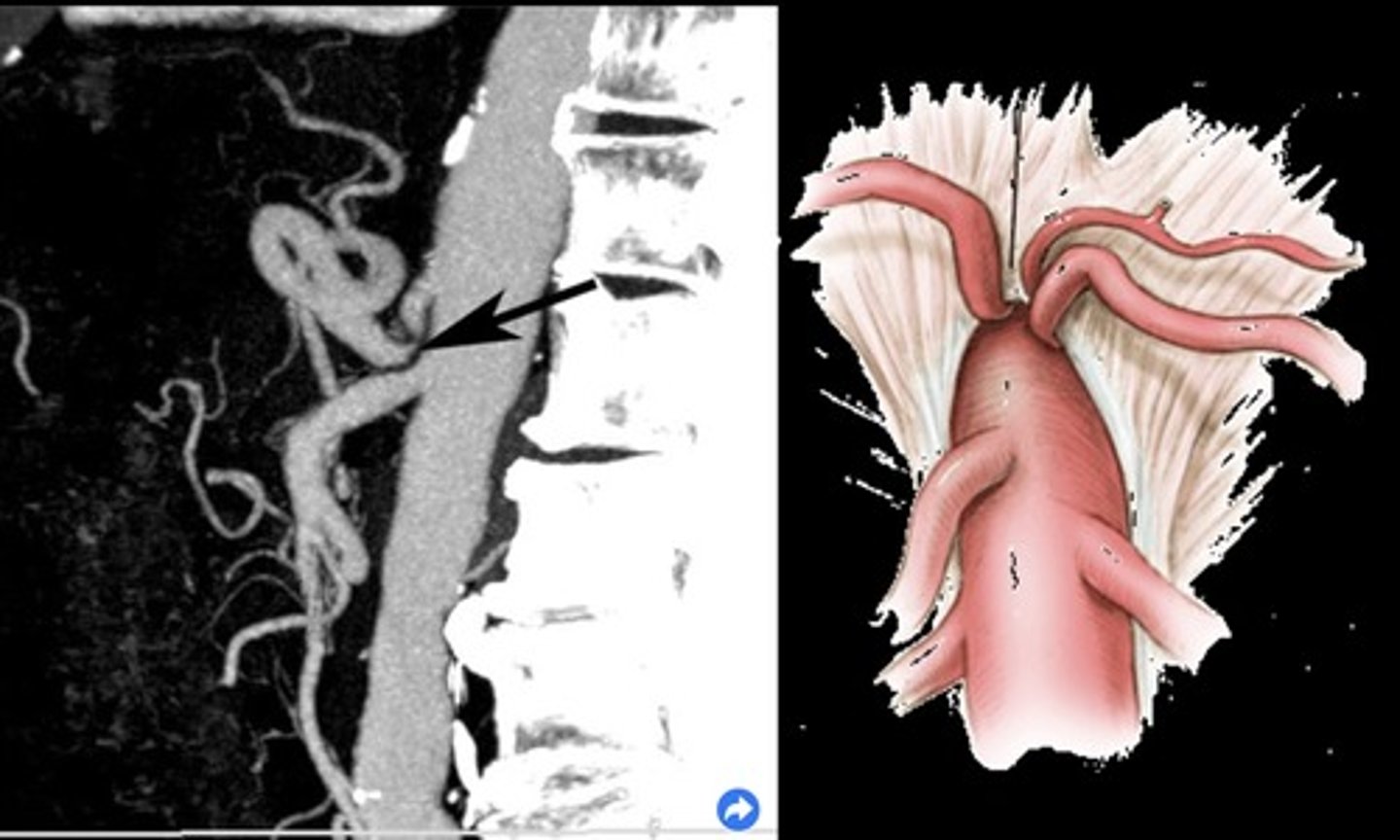
Celiac Artery PSV with MALS
> 250 cm/sec during expiration that normalizes with inspiration
Patient Prep for Liver Doppler
Fasting 8-12 hours
No smoking or chewing gum
Pre-Hepatic/Inflow Vessels
Portal Vein
Hepatic Artery
Intrahepatic/Sinusoidal Vessels
Sinusoids/capillaries
Hepatocytes
Post-Hepatic/Outflow Vessels
Central Veins
Sublobular Veins
Hepatic Veins
IVC
Left Gastric Vein (coronary vein) Diameter
> 6 mm
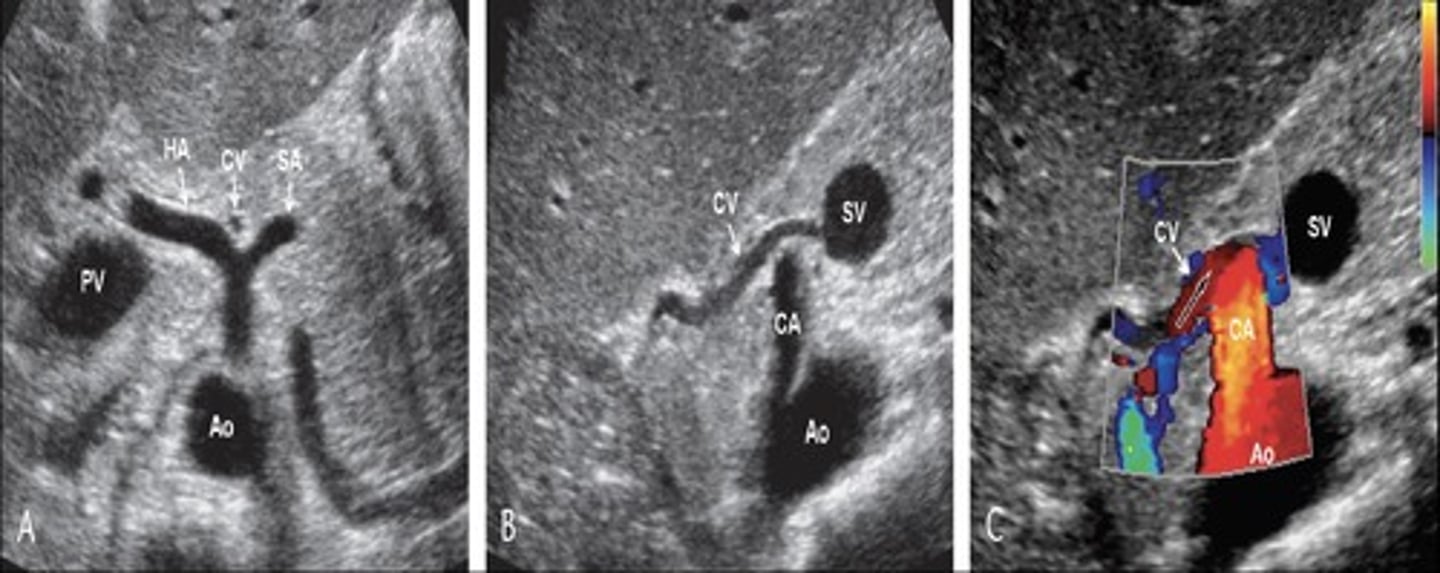
Left Gastric Vein (coronary vein) Doppler Flow
Hepatofugal
Main Portal Vein
Junction of splenic vein & SMV
Brings blood from bowel and spleen into liver
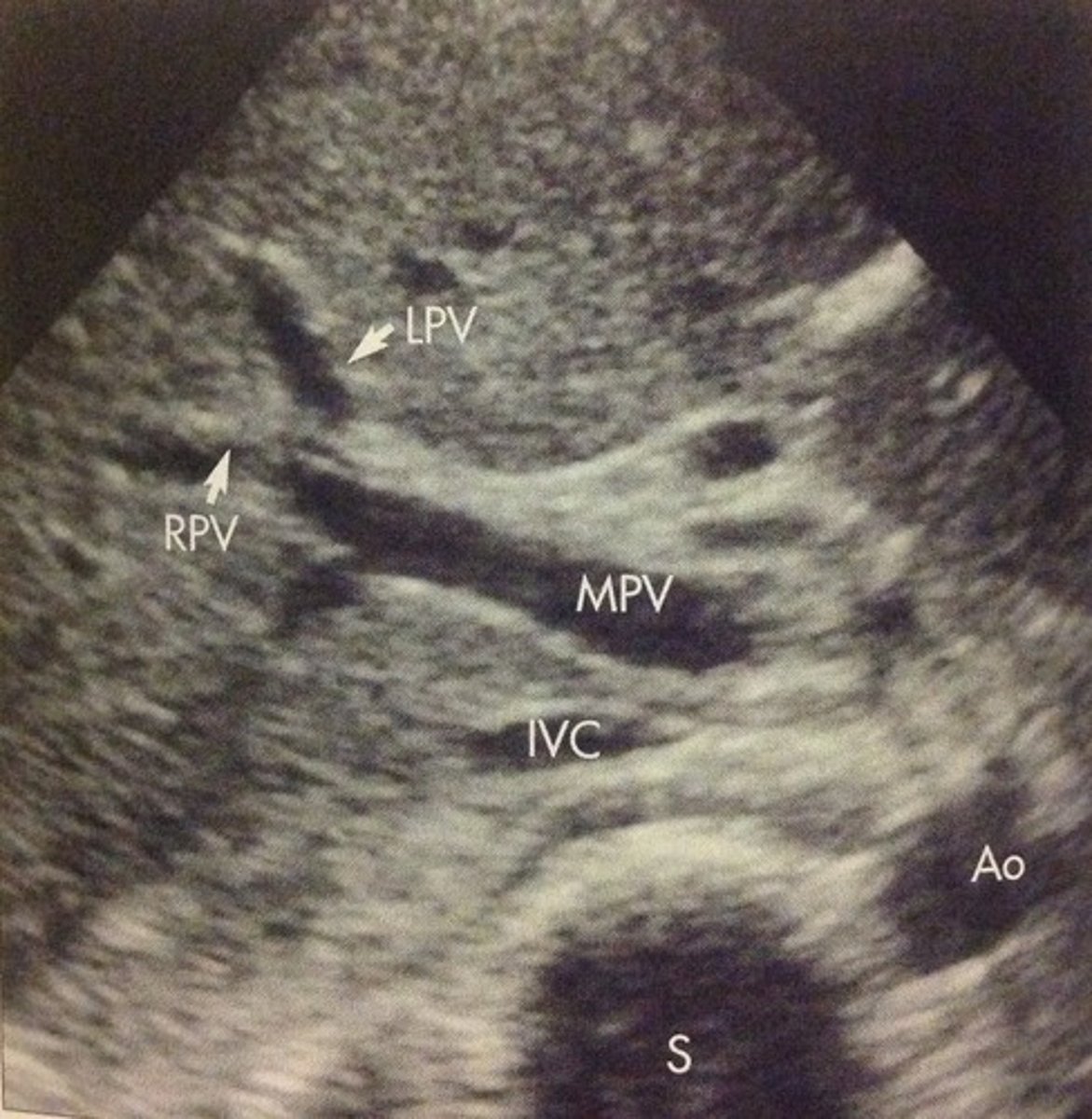
Main Portal Vein Diameter
≤ 13mm (resting)
≤ 16 mm (deep inhalation/valsalva)
Main Portal Vein Doppler Waveform
Monophasic continuous waveform
Hepatopetal flow (antegrade flow)
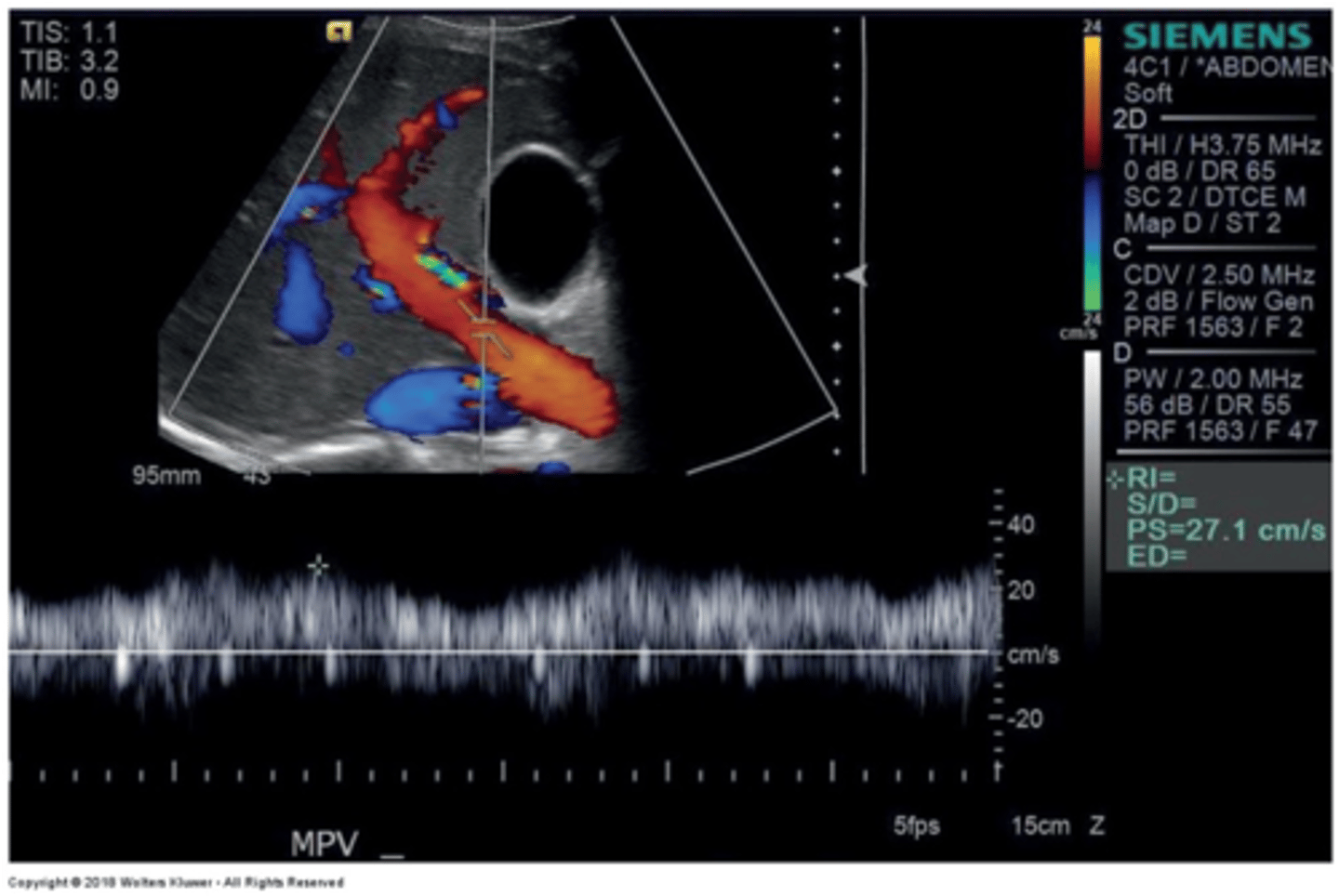
Main Portal Vein PSV
16-31 cm/sec
Slight respiratory variation
-> breath in = decreased velocity
-> breath out or eating = increased velocity
Hepatic Vein Diameter
6 mm
≤ 9 mm (when CHF is present)
Hepatic Vein Doppler Waveform
Triphasic
Antegrade & retrograde flow - cardiac pressure changes
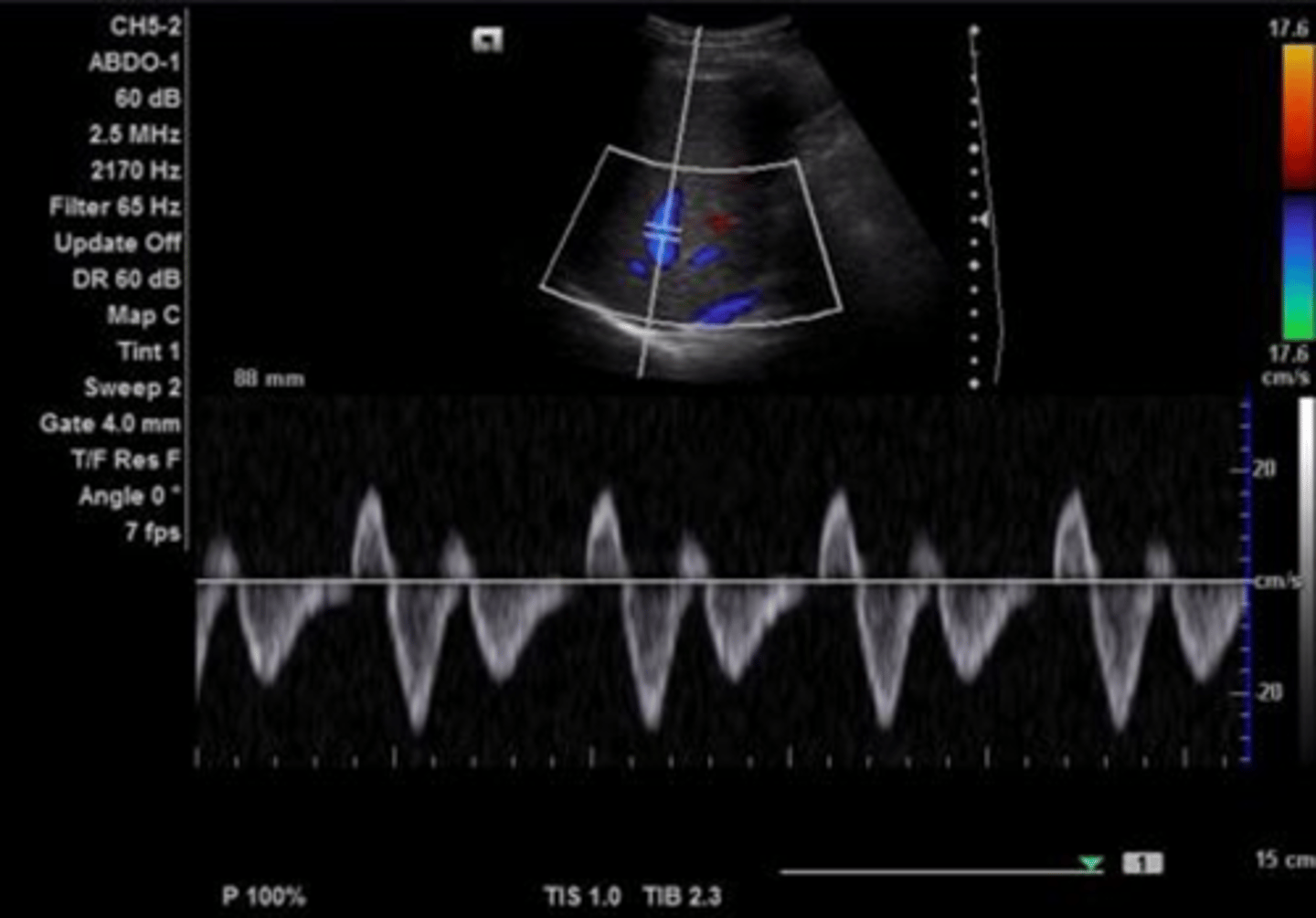
Hepatic Vein Doppler
S wave: ventricular systole
D wave: atrial filling
A wave: atrial contraction
Inspiration depresses systolic wave
Exhalation augments systolic wave
Valsalva diminishes pulsatility
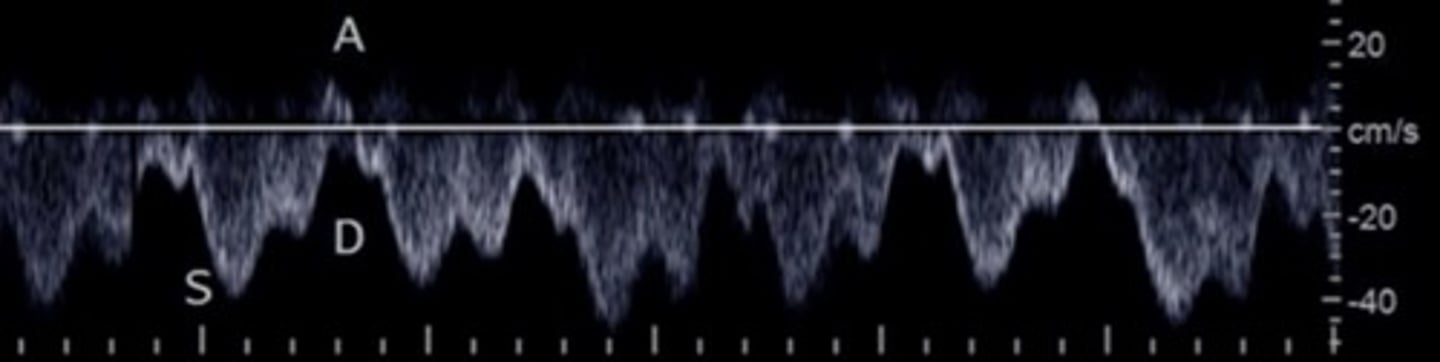
Hepatic Vein PSV
20-39 cm/sec
Hepatic Artery
Right branch of celiac trunk
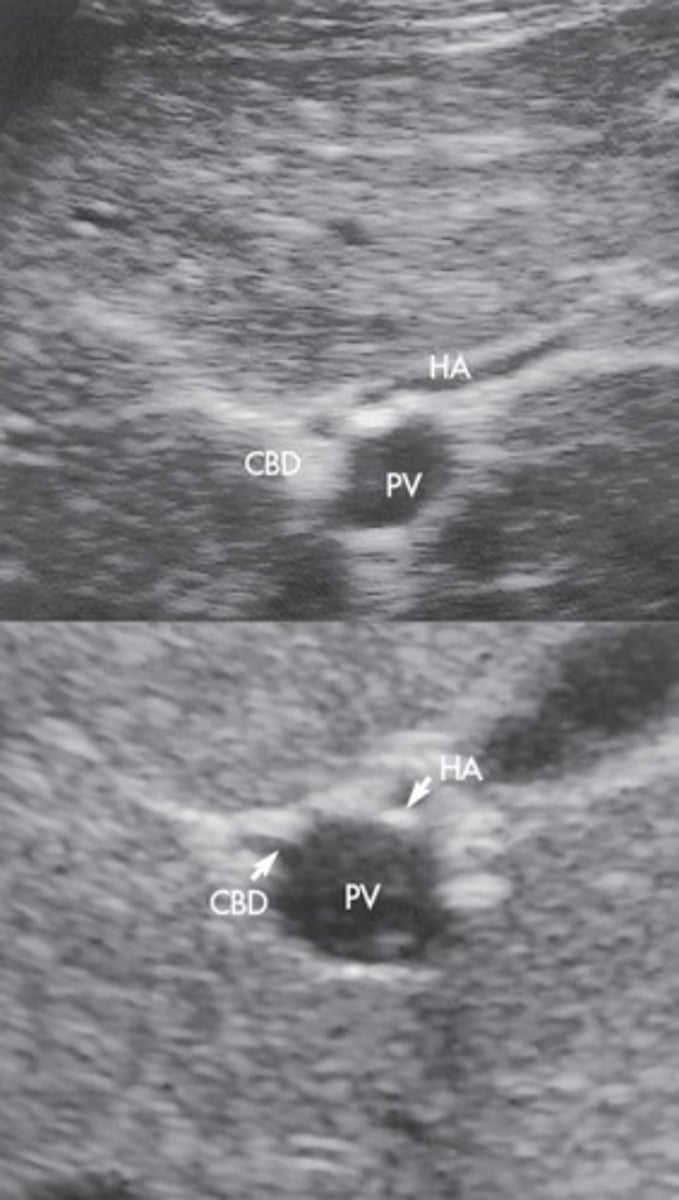
Hepatic Artery Doppler Waveform
Hepatopetal
Low resistant monophasic pan-diastolic forward flow
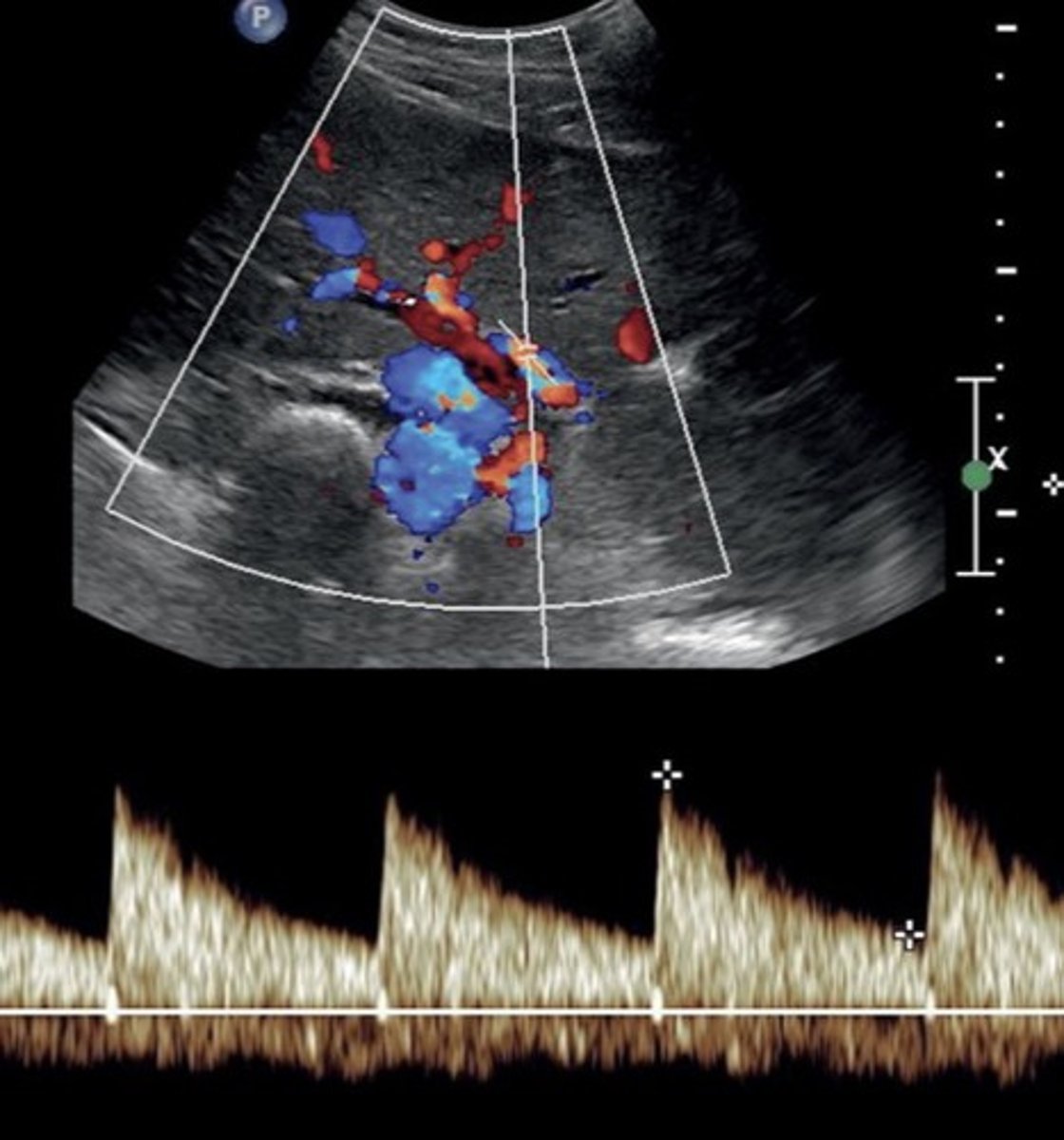
Hepatic Artery PSV
70-120 cm/sec
Hepatic Artery RI
0.5 - 0.7
Hepatic Buffer Response
When PV flow increases, HA flow decreases (post-prandial)
Splenic Vein Diameter
10 mm
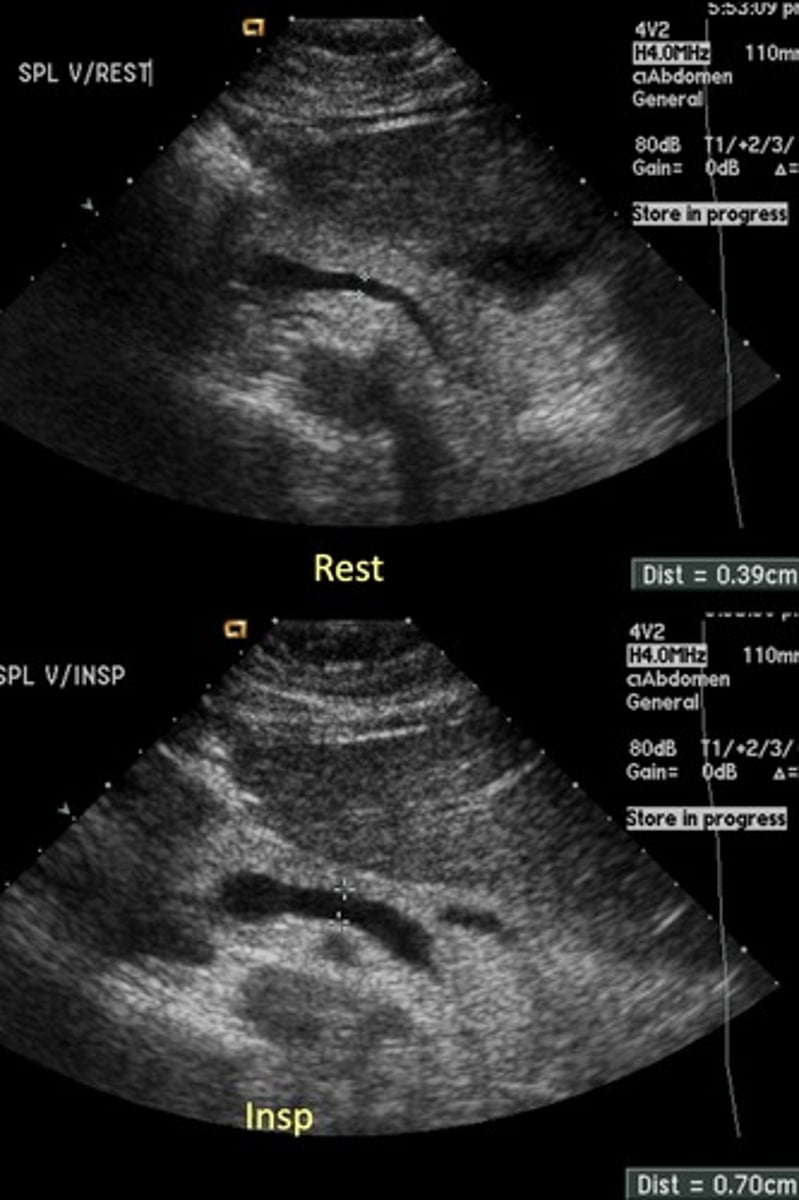
Splenic Vein Doppler Waveform
Hepatopetal flow
Continuous monophasic with slight respiratory variation
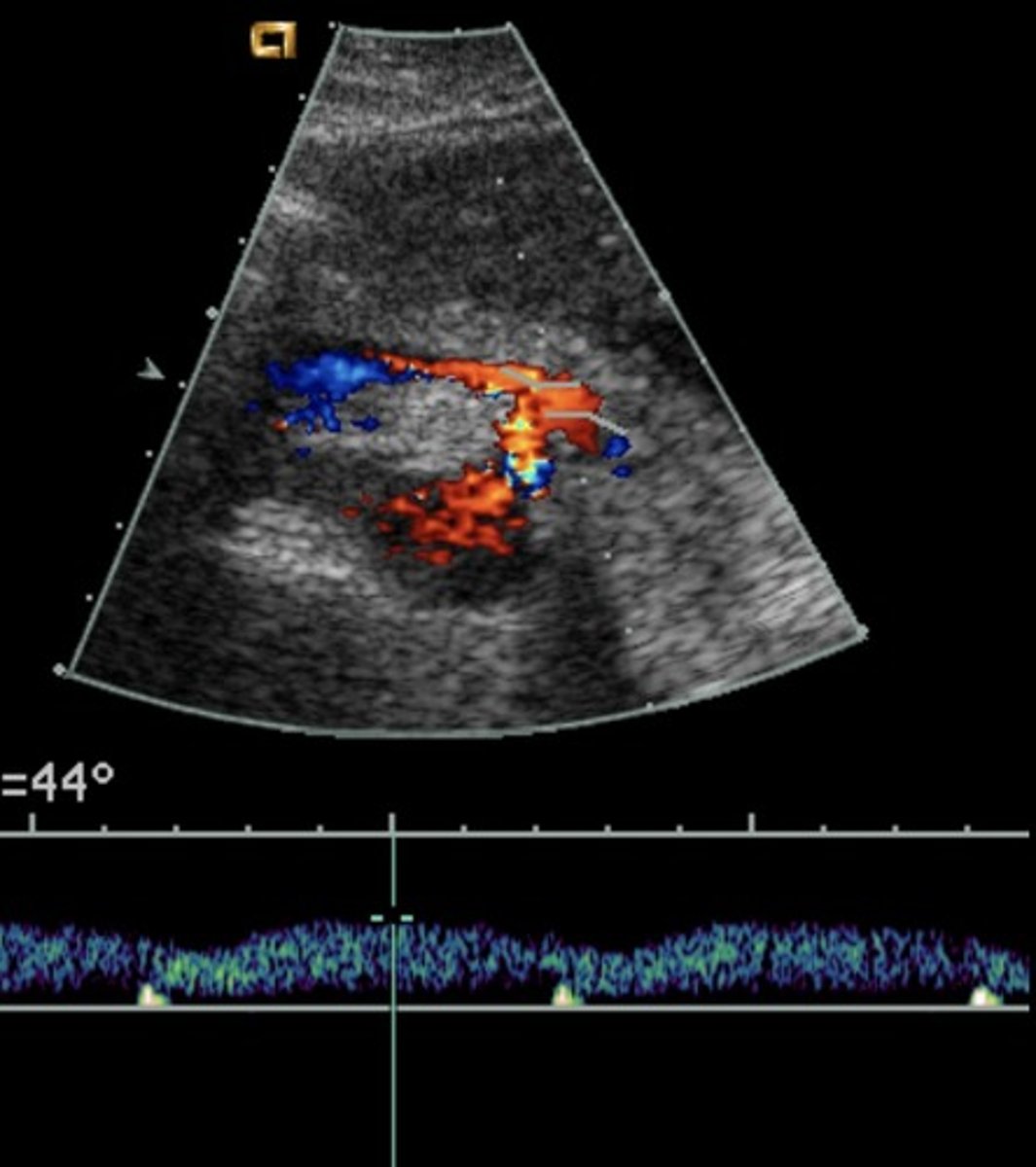
Splenic Vein PSV
9-30 cm/sec
SMV Diameter
10 mm
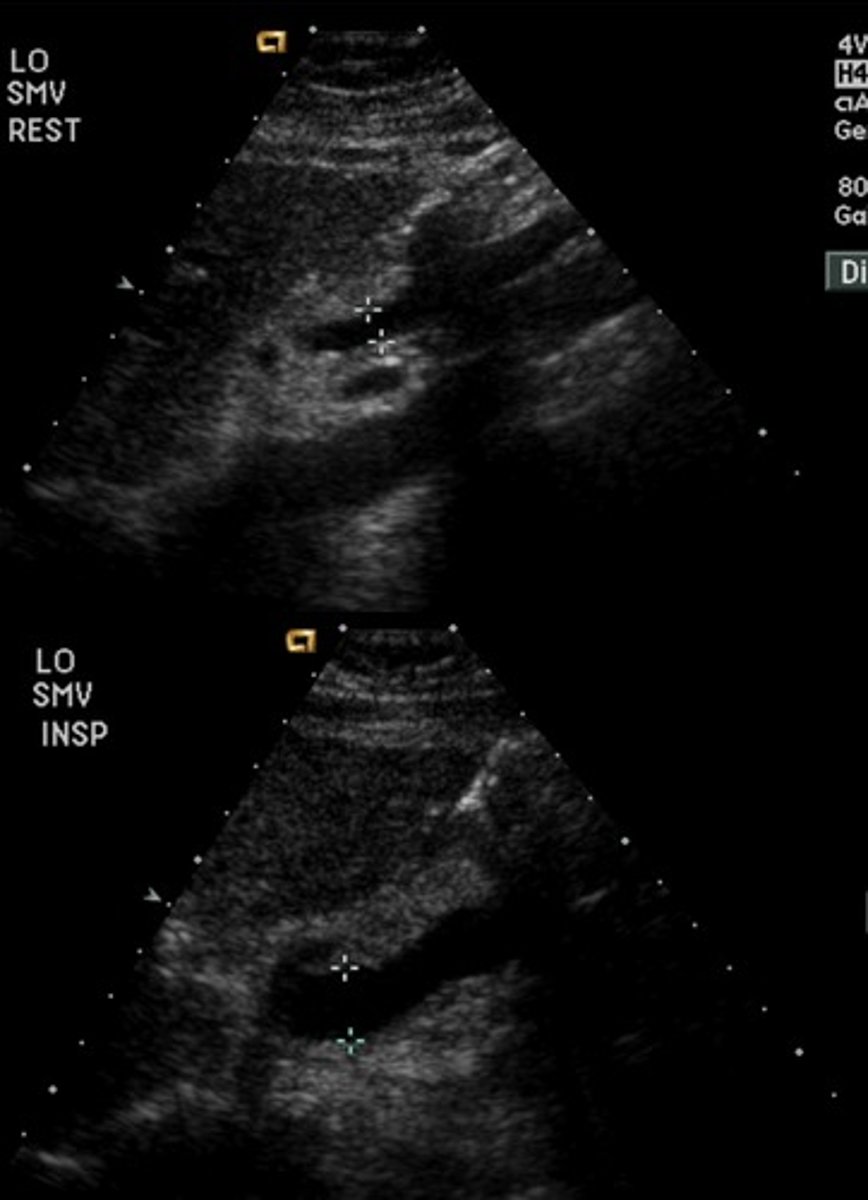
SMV Doppler Waveform
Hepatopetal flow
Continuous monophasic with slight respiratory variation
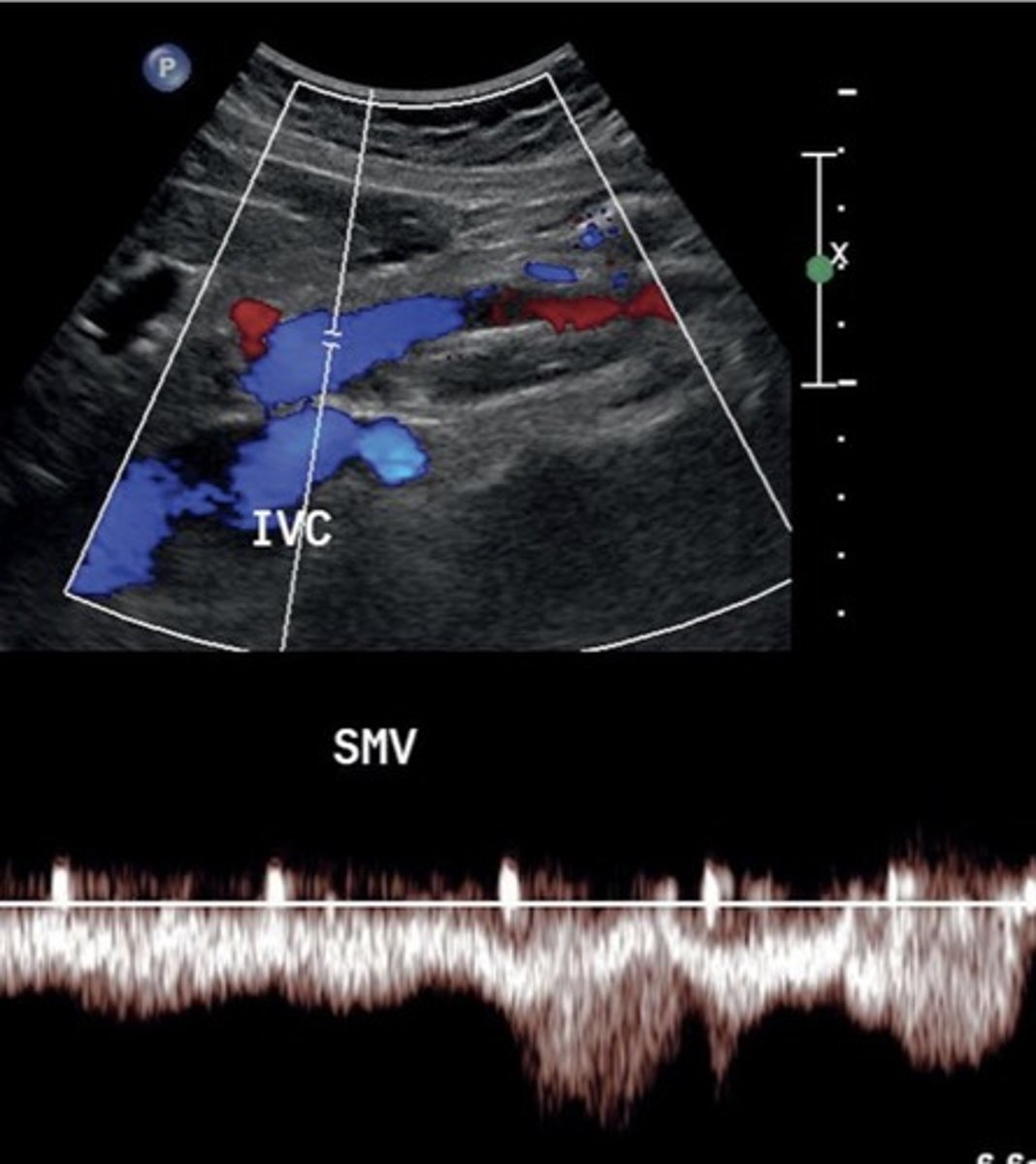
SMV PSV
8-40 cm/sec
IVC Diameter
15-25 mm
valsalva = max diameter
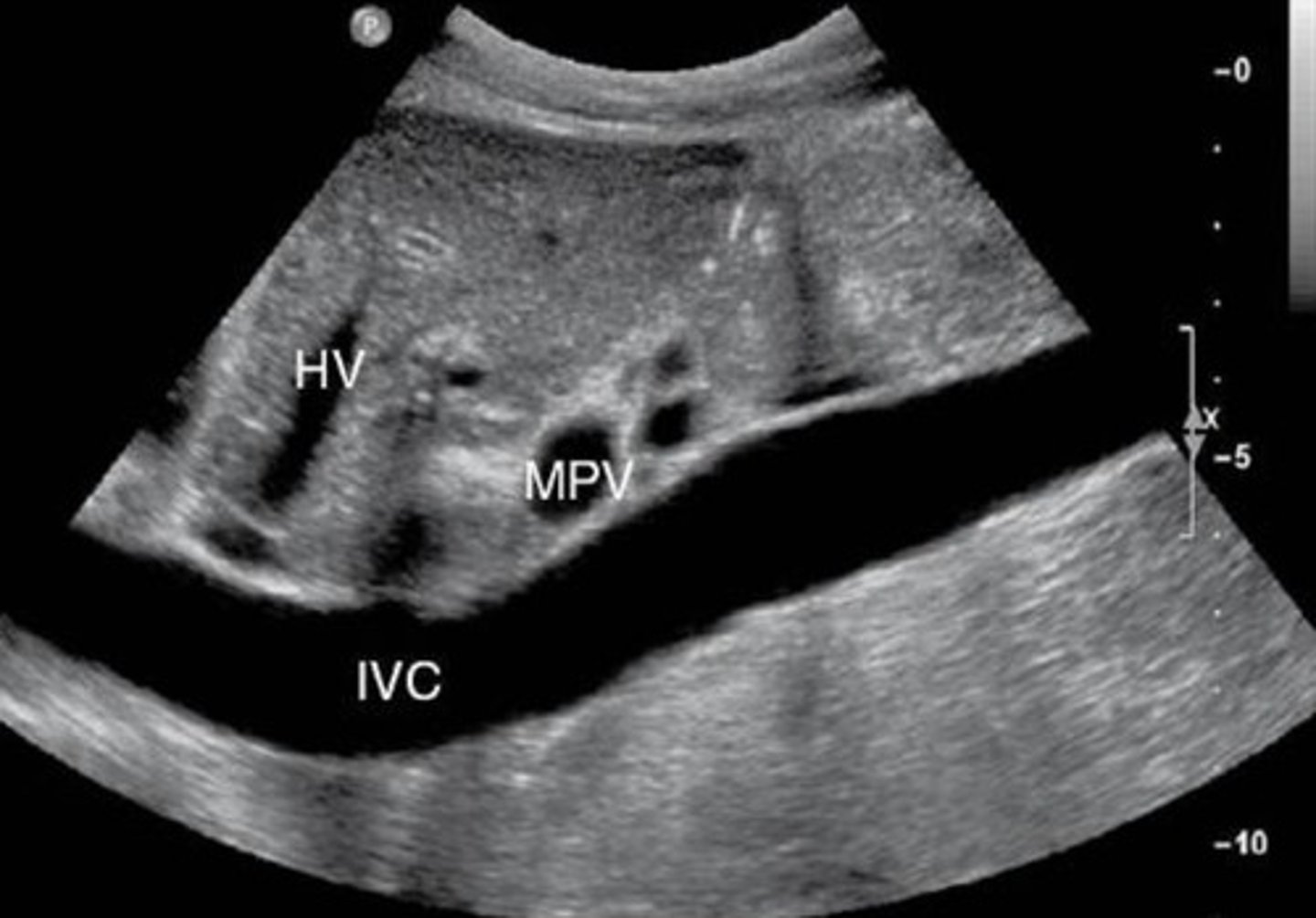
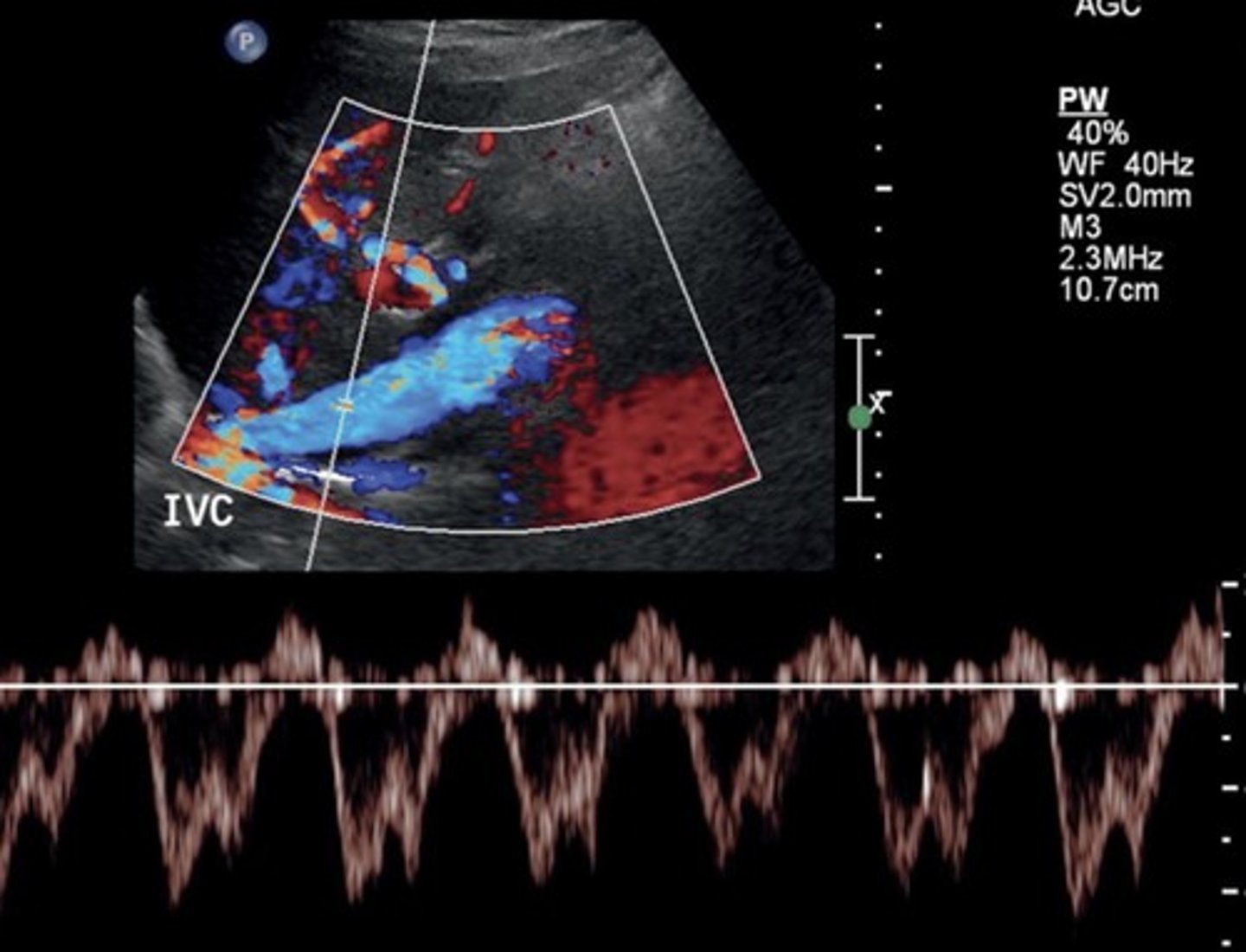
IVC PSV
44-118 cm/sec
Increases with inspiration
Sub-Xiphoid/Transverse Epigastric & Left Sagittal
Left Hepatic V at IVC: blue
Ascending Left Hepatic V: red
Hepatic Artery: red
Porta Hepatis: red
Portal Confluence: blue
Splenic Vein: red
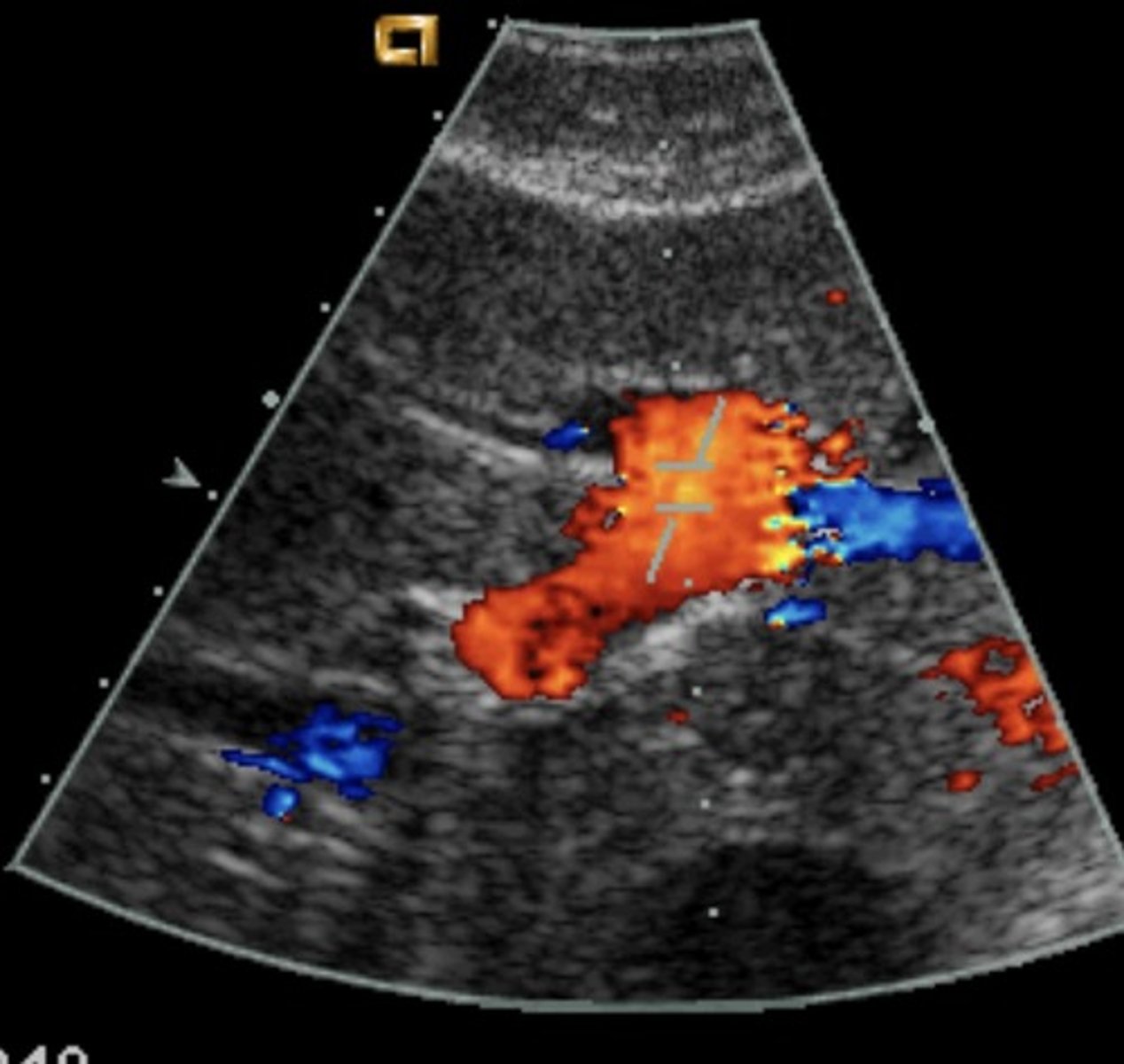
Right Subcostal Margin
Porta hepatis, MPV, anterior RPV, HA: red
Posterior RPV : blue
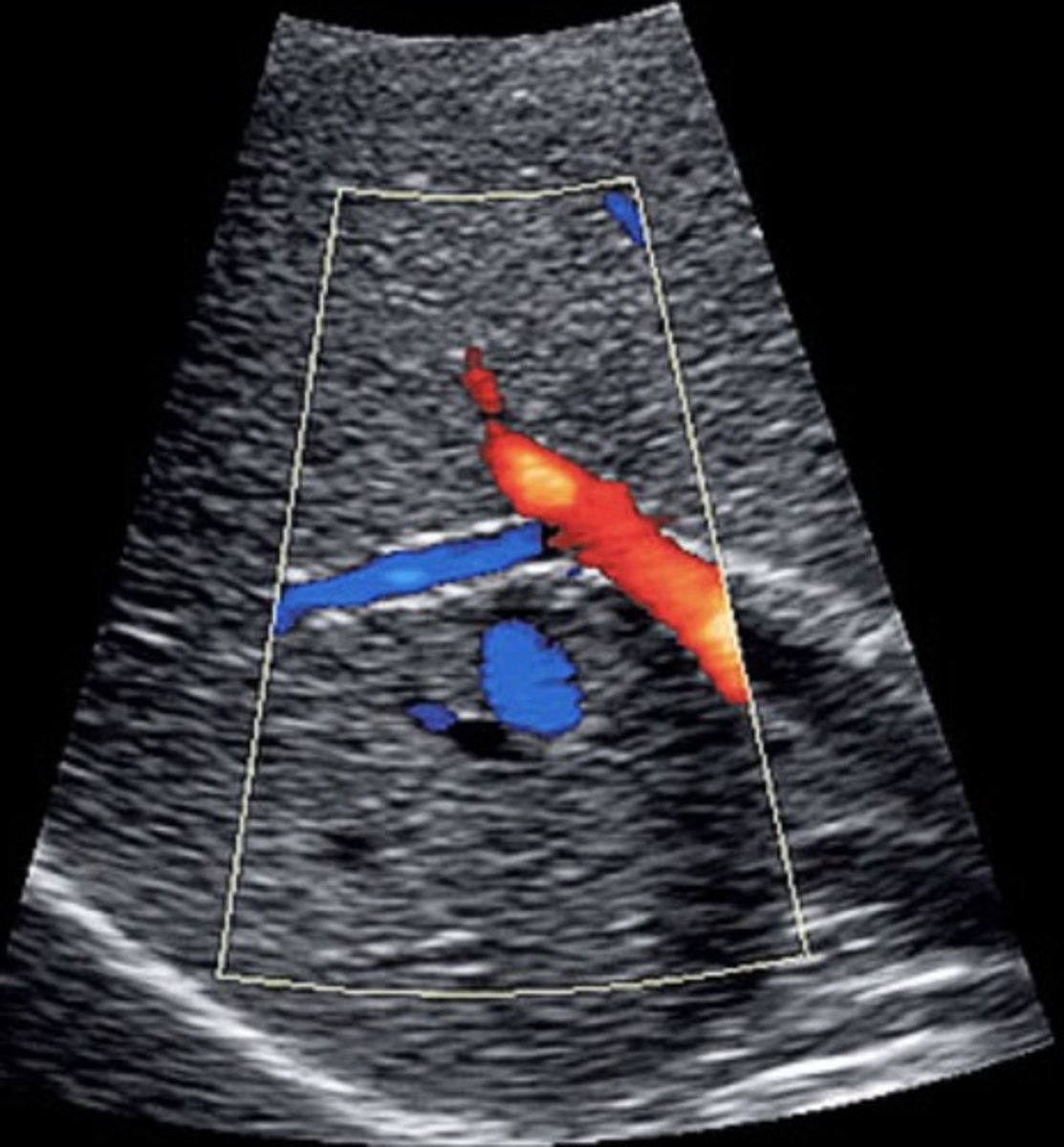
Right Intercostal
Porta hepatis: red
Portal-Splenic confluence: red
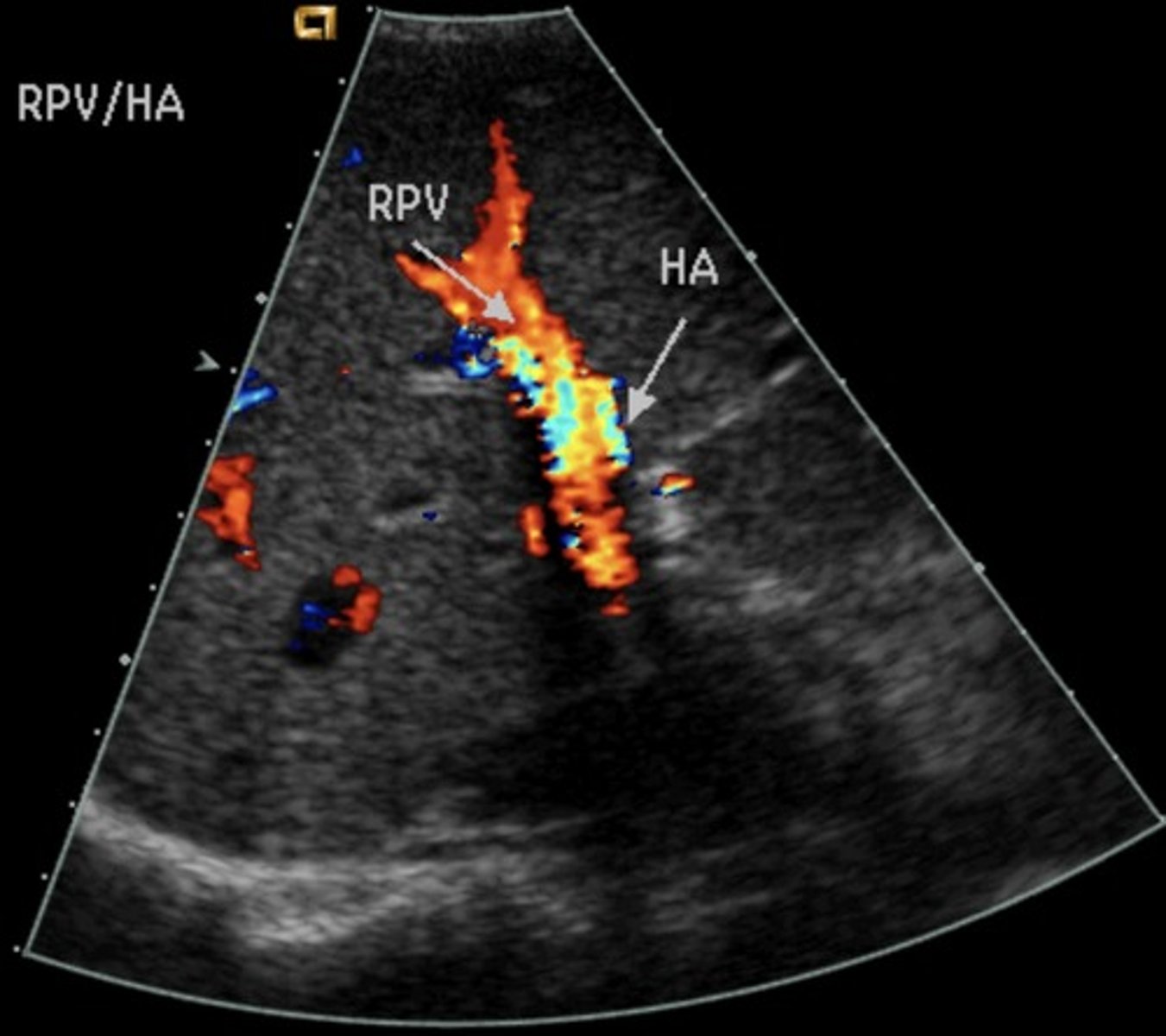
Left Coronal Oblique
Splenic vein: blue
Splenic artery: red
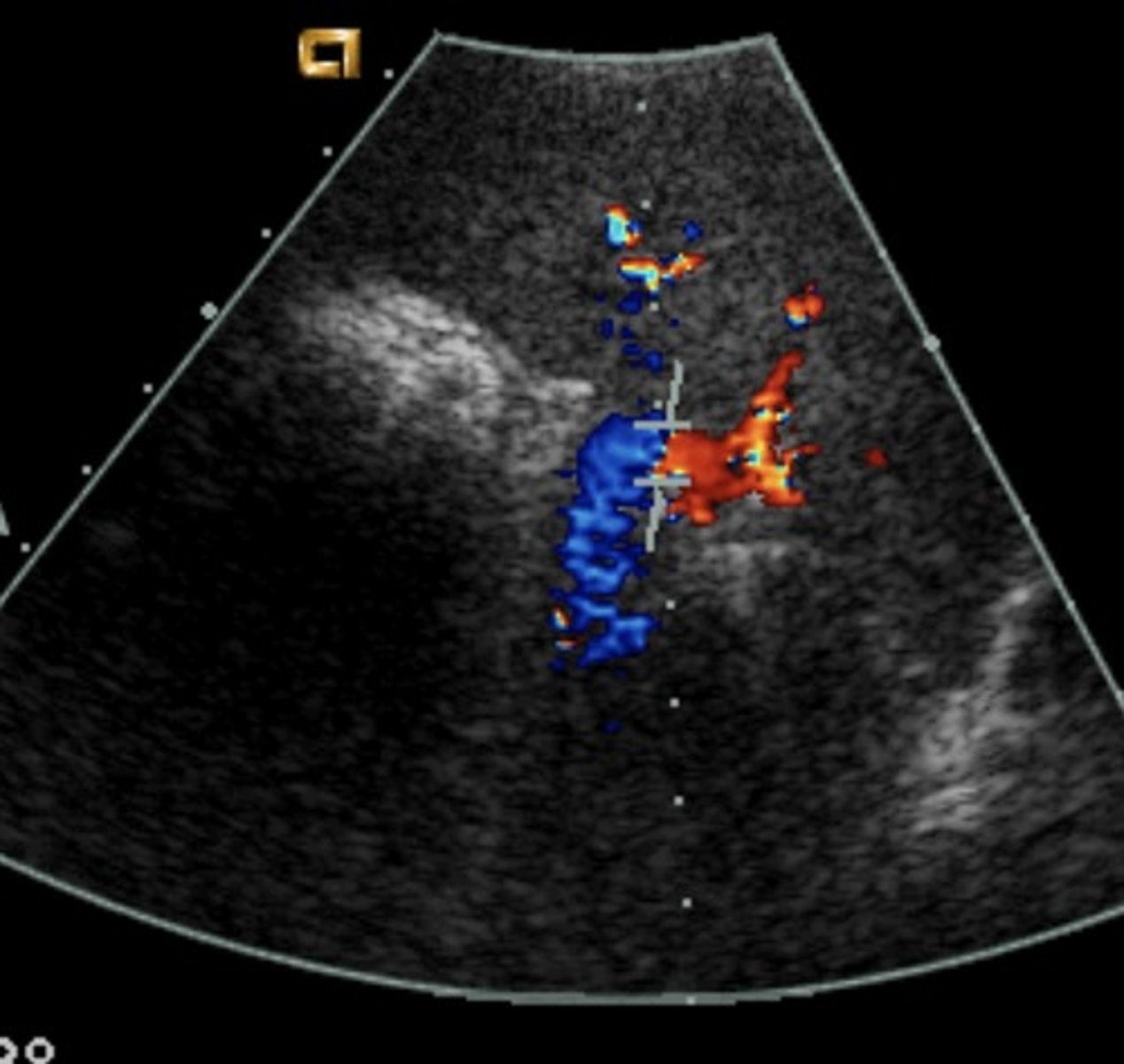
Portal Pressure Formula
IVC pressure - portal vein pressure
Portal Vein Pressure
5-10 mmHg
≥ 15 mmHg = clinically significant
Portal HTN
Increased pressure in portal venous system
Not diagnosed with spectral Doppler -> diagnosed with gray scale & color
Causes of Portal HTN
Hepatitis C
Hepatitis B
Alcoholic cirrhosis
Primary Biliary Cirrhosis
Autoimmune Hepatitis
Hereditary Hematochromatosis
Schistosomiasis
Portal HTN 2D Findings
Large pulmonary vein
Collaterals
Splenomegaly
Ascites
Enlarged hepatic artery
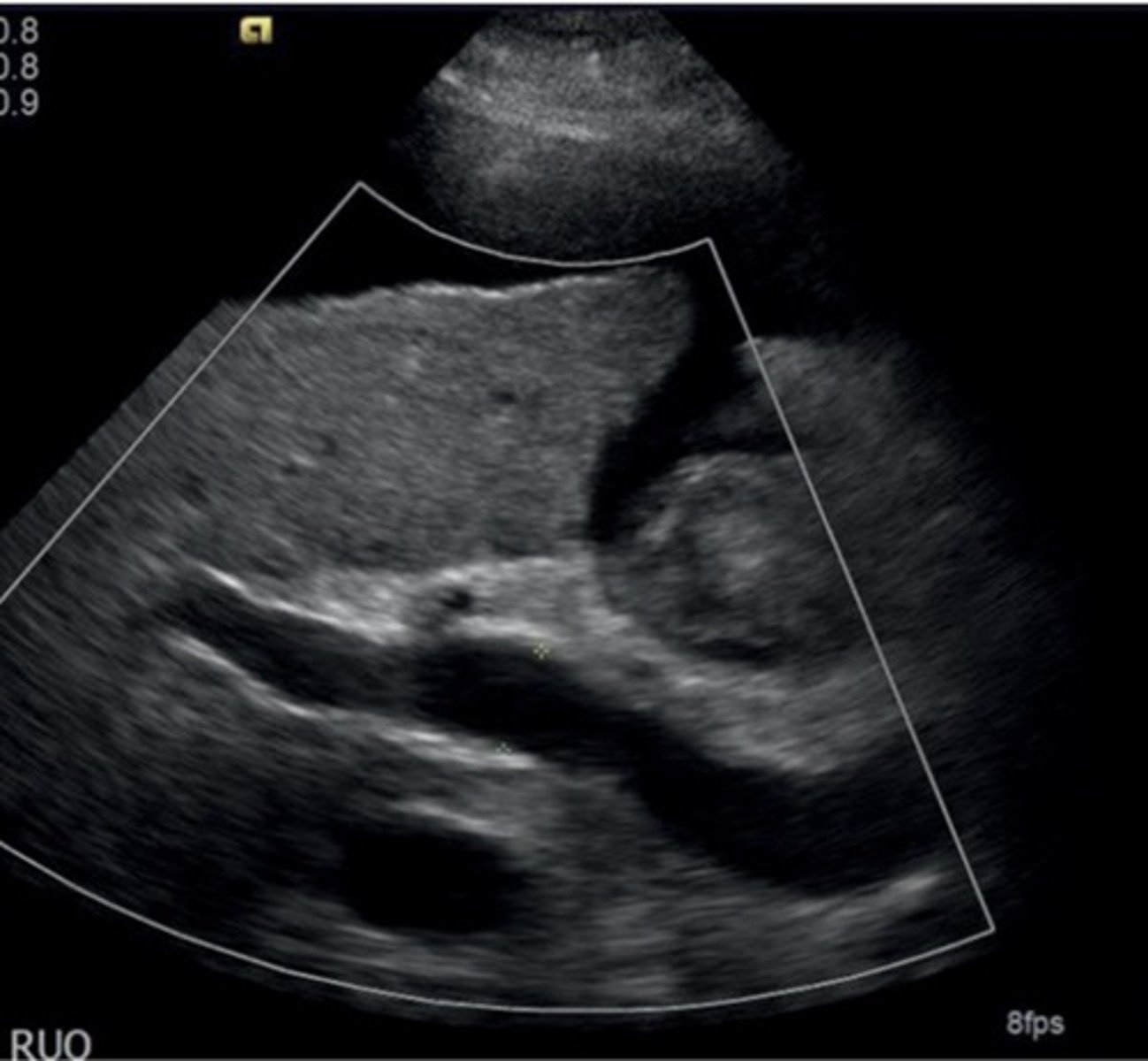
Portal HTN Doppler Findings
Slow, hepatofugal flow in portal vein
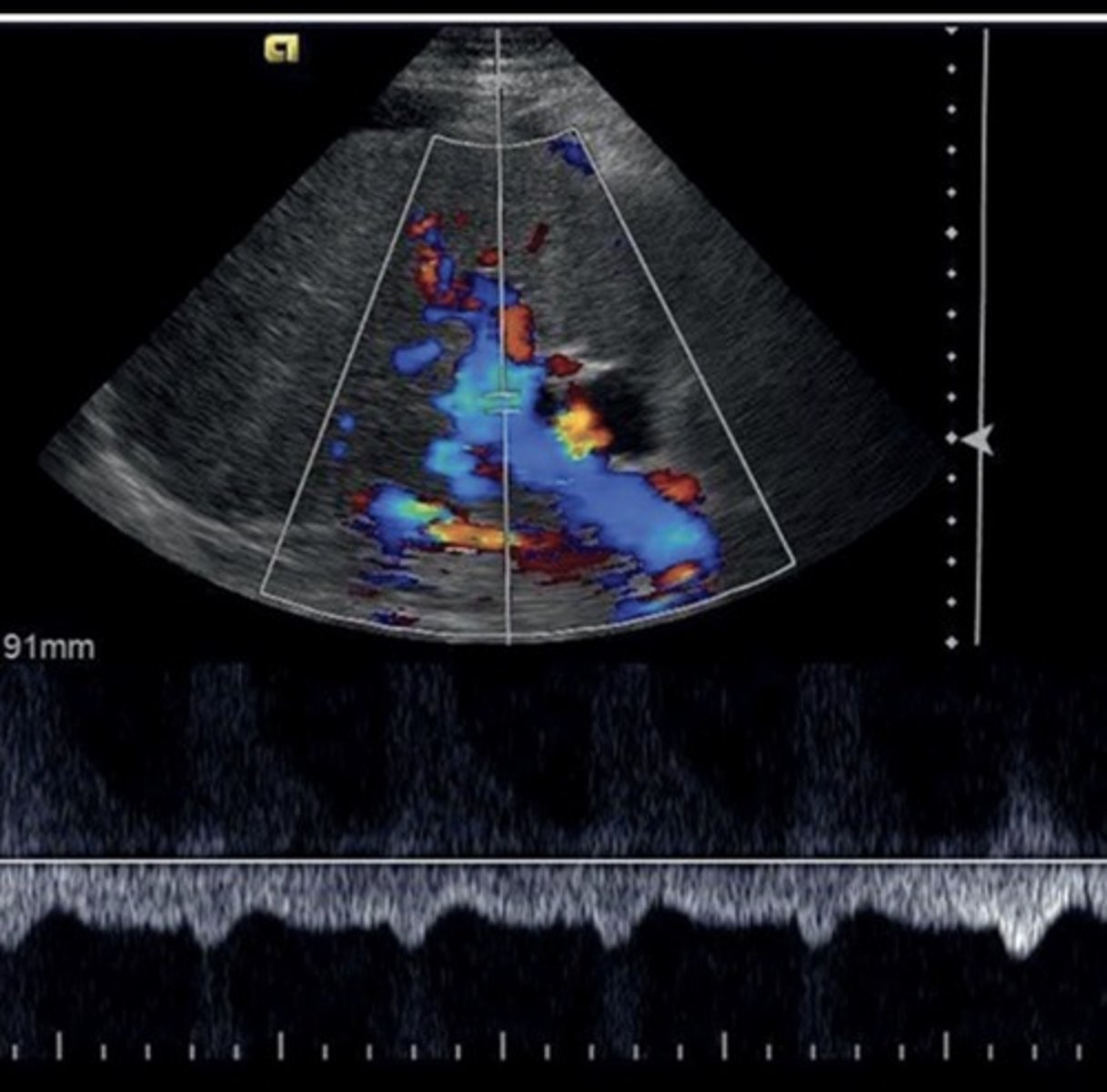
Cirrhosis
End-stage liver disease
Cirrhosis Findings
Portalization of hepatic veins
Collaterals
Hepatofugal flow in portal vein & splenic vein
Coronary Vein Collateral
Can lead to esophageal varices
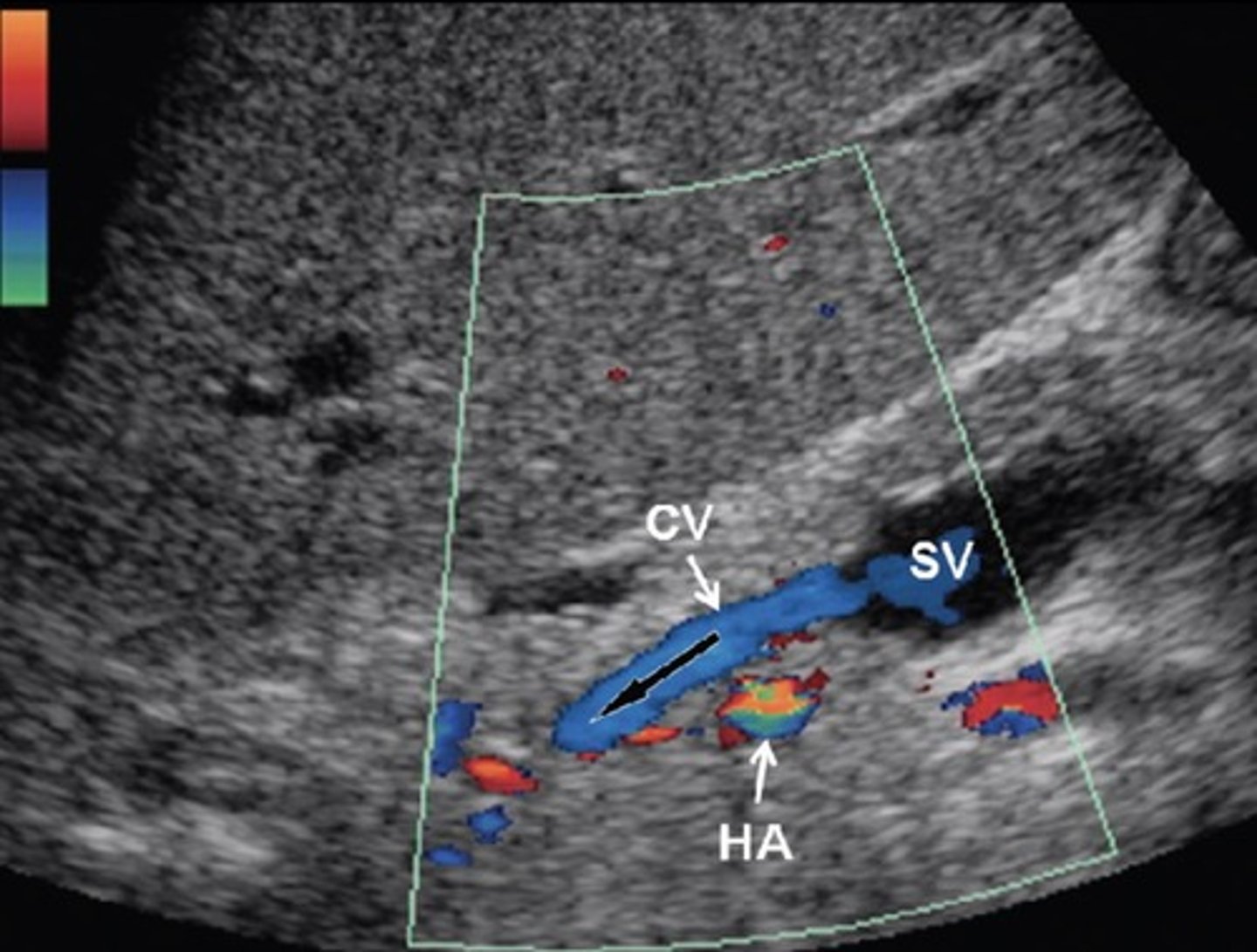
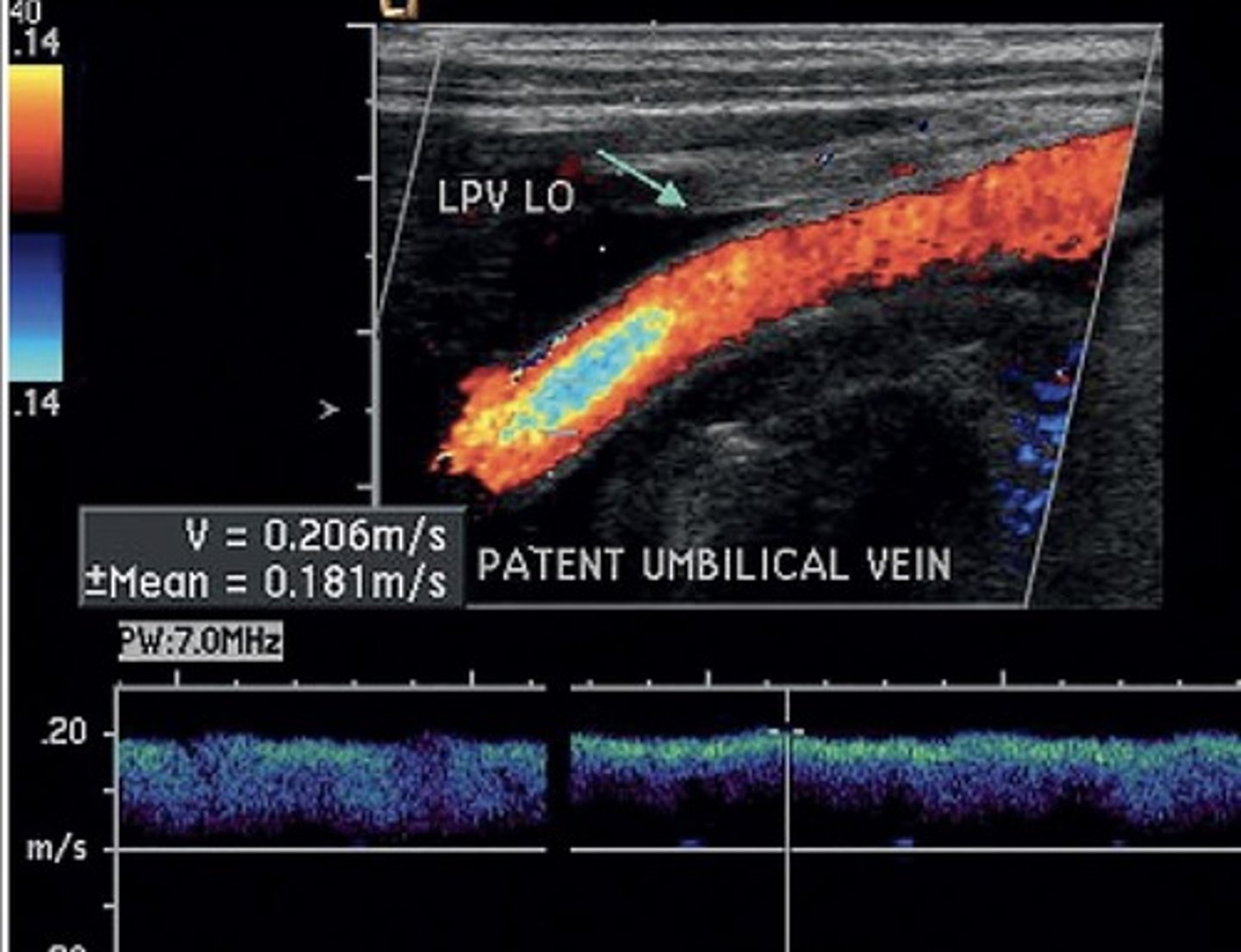
Recanalized Paraumbilical Vein
Ligamentum teres recanalizes
Courses from left portal vein to anterior abdominal wall
Hepatofugal flow

Recanalized Paraumbilical Vein Diameter
> 3 mm
Recanalized Paraumbilical Vein PSV
> 5 cm/sec
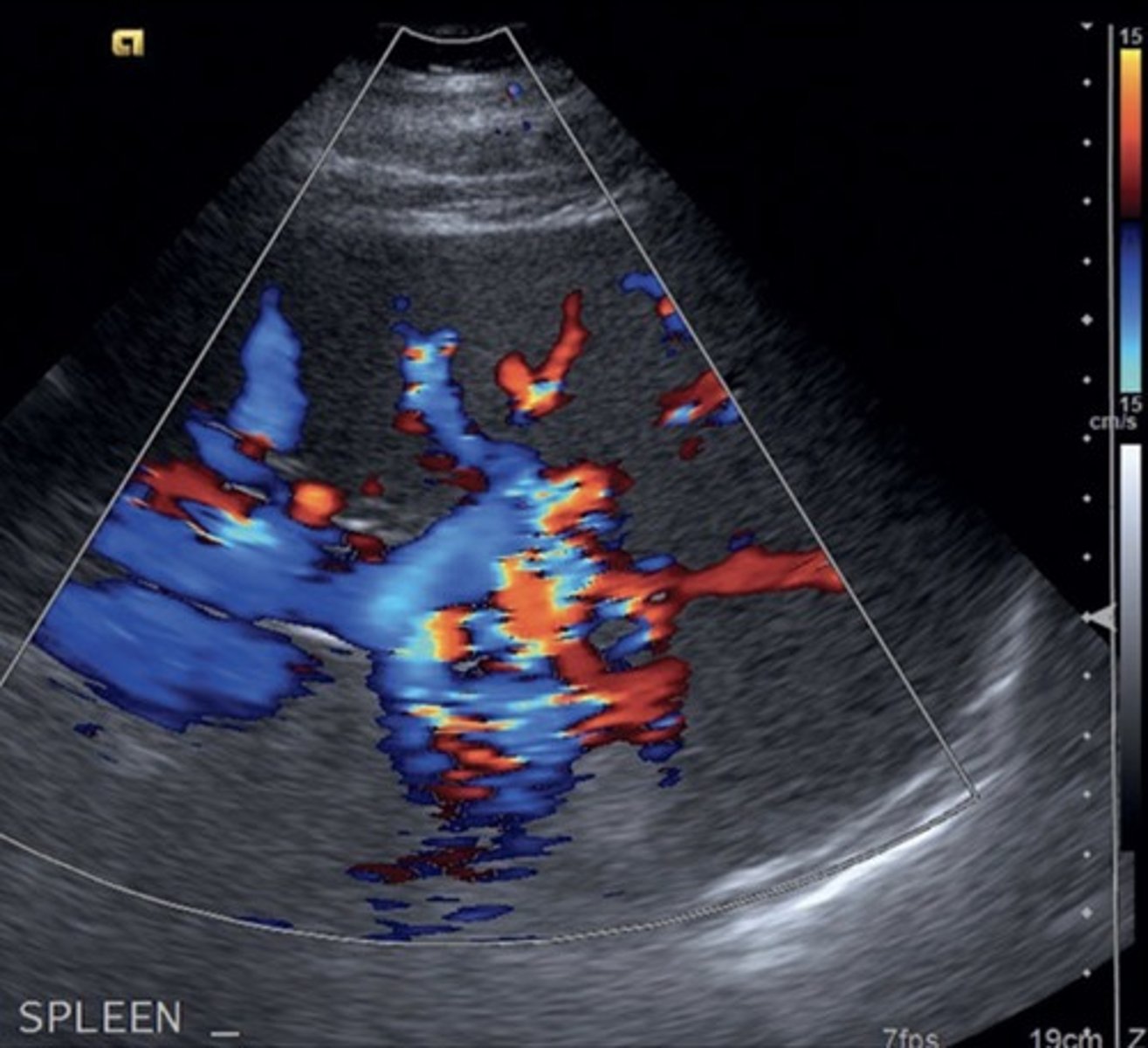
Splenorenal Shunt
Prominent veins at splenic hilum
Hepatofugal flow in splenic vein
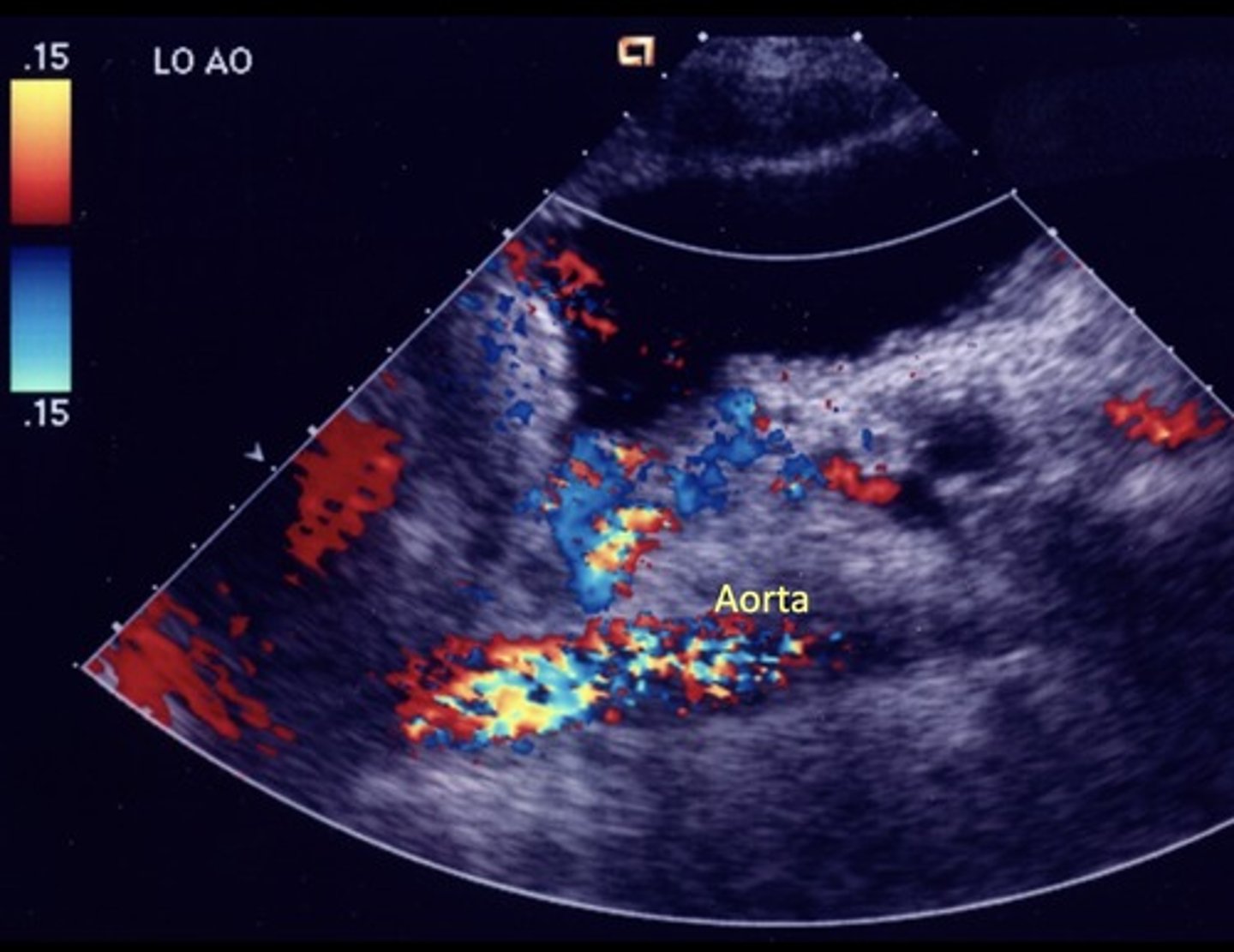
Gastroesophageal Veins/Esophageal Varices
Originate from gastroesophageal junction posterior to left liver lobe
Due to hepatofugal flow in coronary vein shunt
High risk of rupture
Gallbladder Varices
Serpentine anechoic structures along GB wall
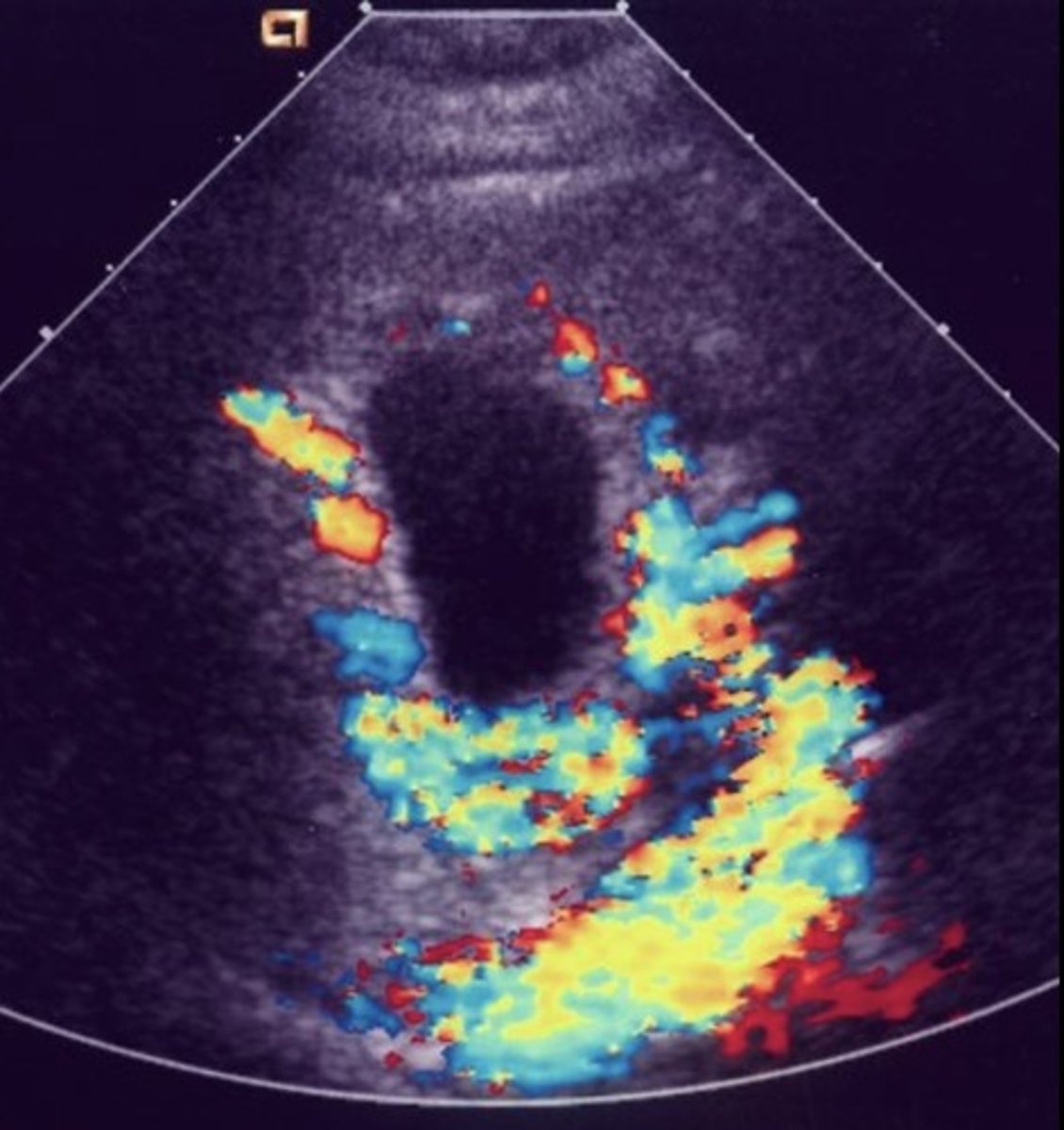
Gallbladder Varices Diameter
3-8 mm
AV Fistula
Arterialized portal vein flow - hepatic artery to portal vein shunting
Leads to portal HTN
AV Fistula Causes
Trauma
Penetrating trauma
Iatrogenic trauma- biopsies, invasive imaging procedures
AV Fistula Findings
Large anechoic spaces
Increased portal vein pulsatility & velocities
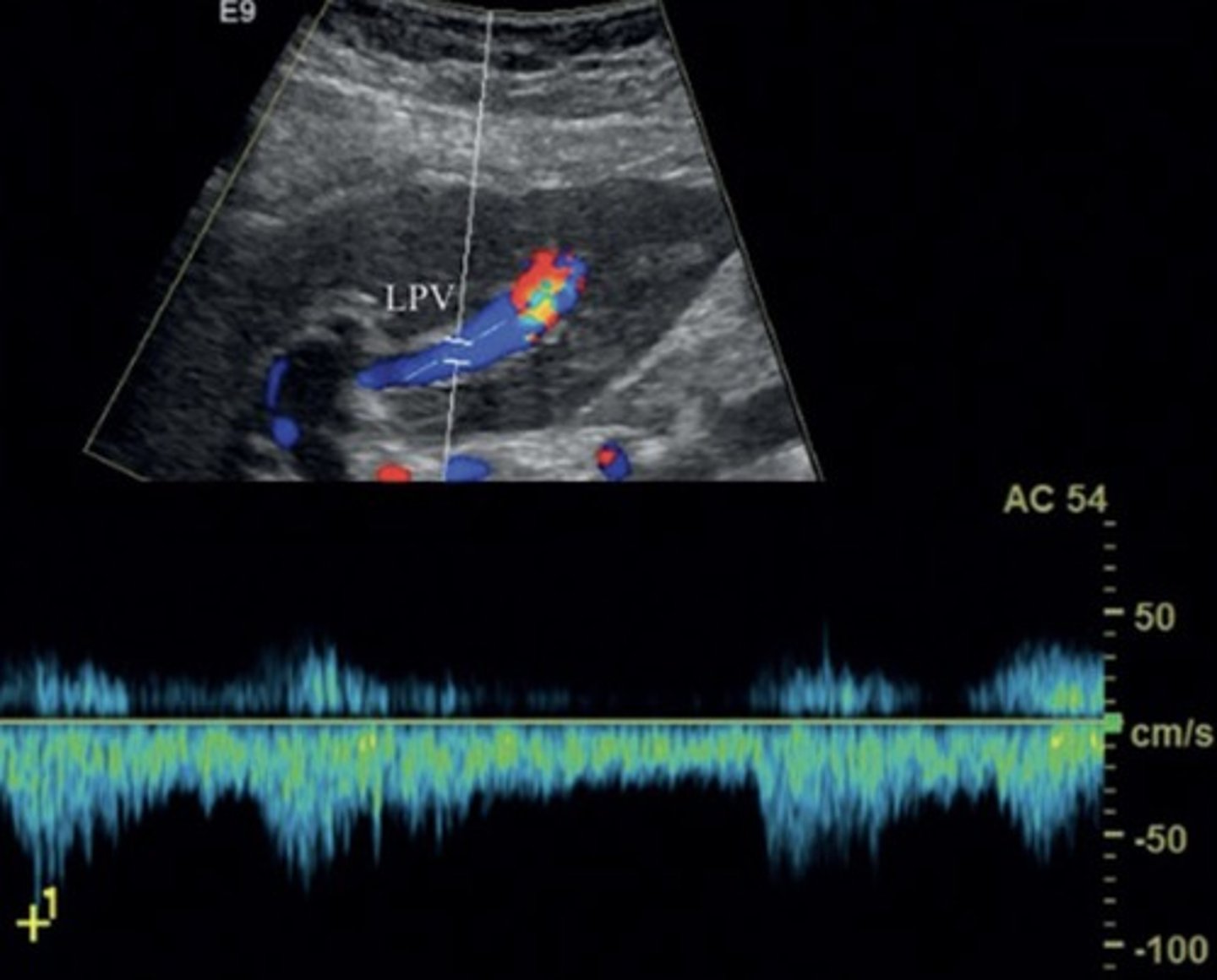
Aterialization of the Liver
Max portal vein pressure leads to increased hepatic artery flow