TB - MedPath
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
What does this refer to
Infection caused by Mycobacterium tuberculosis, an acid-fast bacillus
Leading cause of death from a curable infectious disease throughout the world
Tuberculosis
What does this refer to
Acid-fast bacillus with mycolic acid cell wall
Slow-growing, intracellular pathogen
Resistant to desiccation and common disinfectants
Mycobacterium tuberculosis
What does this refer to
High prevalence in Africa, Asia
Risk groups: immunosuppressed, homeless, healthcare workers
Rising multi-drug resistant (MDR) and extensively drug-resistant (XDR) TB strains
Epidemiology of TB
What does this refer to
Inhalation of droplet nuclei
Requires prolonged close contact
Bacilli reach alveoli and are phagocytosed
TB Transmission
What does this refer to
Tranmitted by inhalation of respiratory droplets
Requires prolonged close contact
Bacilli reach alveoli and are phagocytosed
Tubercle formation: Granulomatous lesion
Isolation of bacilli by enclosing them in tubercles and surrounding the tubercles with scar tissue
Caseous necrosis: Cheeselike material
May remain dormant for life or cause active disease
Tuberculosis Transmission and Infection
What does this refer to
Cell-mediated immunity essential
Activation of macrophages by IFN-gamma
Granuloma formation contains infection
Immune Response to TB
What does this refer to
Central necrosis surrounded by epithelioid cells, lymphocytes
Caseating necrosis hallmark of TB
May calcify or cavitate
Granuloma Formation
What does this refer to
Cheese-like necrosis due to hypoxia and immune attack
Diagnostic of TB in histology
Associated with cavitary lesions
Caseating Necrosis
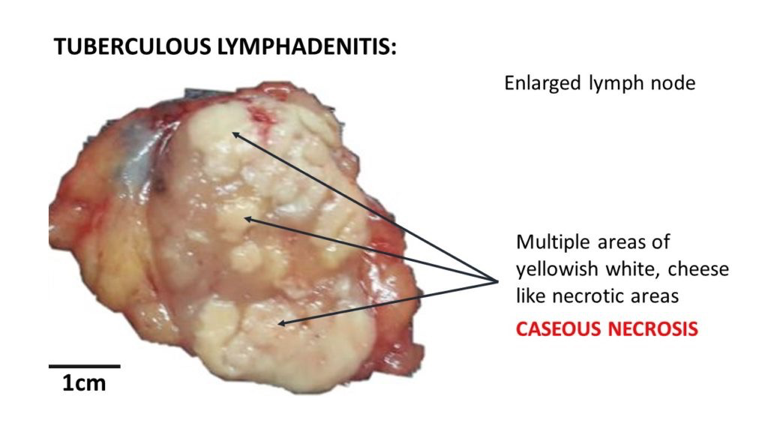
What does this refer to
Formation of Ghon focus and Ghon complex
Most cases resolve or become latent
Initial immune containment by macrophages and T cells
Primary TB Infection
What does this refer to
_______: positive test, no symptoms, non-contagious
Latent TB
What does this refer to
________: symptomatic, contagious, radiologic abnormalities
Active TB
What does this refer to
Latent tuberculosis infection: Asymptomatic
Fatigue, weight loss, lethargy, anorexia (loss of appetite), a low-grade fever that usually occurs in the afternoon, and night sweats; purulent cough
Clinical Manifestations of TB
What does this refer to
Positive tuberculin skin test (TST) a purified protein derivative (PPD): Does not differentiate past, latent, or active disease
Sputum culture, immunoassays, indirect drug susceptibility testing
Chest radiographs
Diagnosis of TB
What does this refer to
TB lymphadenitis (scrofula), CNS TB (meningitis), miliary spread
Bone (Pott’s disease), GI, genitourinary TB
More common in immunocompromised
Extrapulmonary TB
What does this refer to
Occurs when immunity wanes (HIV, steroids)
Apical lung involvement due to higher oxygen tension
Constitutional symptoms and productive cough
Reactivation TB
What does this refer to
Failure of immune containment
Seen in young children and immunosuppressed
Dissemination to hilar nodes and bloodstream
Progressive Primary TB
What does this refer to
Hematogenous dissemination of bacilli
Tiny nodules throughout lung fields
High mortality if untreated
Miliary TB Pathophysiology
What does this refer to
Often lacks typical granulomas
More extrapulmonary involvement
May require biopsy and PCR for diagnosis
TB in Immunocompromised
What does this refer to
Rapid progression and atypical presentation
Overlapping toxicity of treatments
Higher risk of MDR-TB
TB-HIV Coinfection
What does this refer to
CXR: upper lobe cavitation, lymphadenopathy
Histology: granulomas with caseation
Ziehl-Neelsen stain shows acid-fast bacilli
Radiographic and Histologic Findings
What does this refer to
Three early morning samples recommended
AFB smear: rapid but low sensitivity
Culture: gold standard, takes weeks
Sputum Testing
What does this refer to
GeneXpert MTB/RIF: rapid TB and rifampin resistance
PCR-based assays detect DNA
Useful in smear-negative, HIV-positive patients
NAAT and Molecular Tests
Which anti-TB drug is the following
________: inhibits mycolic acid synthesis
Rifampin: inhibits RNA polymerase
Pyrazinamide: effective in acidic pH
Ethambutol: inhibits cell wall synthesis
Isoniazid
Which anti-TB drug is the following
Isoniazid: inhibits mycolic acid synthesis
______: inhibits RNA polymerase
Pyrazinamide: effective in acidic pH
Ethambutol: inhibits cell wall synthesis
RIfampin
Which anti-TB drug is the following
Isoniazid: inhibits mycolic acid synthesis
Rifampin: inhibits RNA polymerase
________: effective in acidic pH
Ethambutol: inhibits cell wall synthesis
Pyrazinamide
Which anti-TB drug is the following
Isoniazid: inhibits mycolic acid synthesis
Rifampin: inhibits RNA polymerase
Pyrazinamide: effective in acidic pH
________: inhibits cell wall synthesis
Ethambutol
What is the TB treatment regimen for intensive phase (2 months)
RIPE
What is the TB treatment regimen for continuation phase (4-7 months)
INH + RIB
What does this refer to
Isoniazid, rifampin, pyrazinamide, and ethambutol
Drug-resistant bacilli: Combination of at least four drugs to which the microorganism is susceptible, administering for 18 months
Review drug effectiveness at 6 months.
Treatment of TB
What does this refer to
Resistant to at least INH and RIF
Requires second-line agents: fluoroquinolones, injectables
Longer duration and more toxic regimen
MDR-TB
What does this refer to
DOT: directly observed therapy
Contact tracing and screening
TB control programs and vaccination (BCG)
Public Health Measures
What size leads to a positive diagnosis of TB in the general population
> 15 mm
What size leads to a positive diagnosis of TB in healthcare workers
> 10 mm
What size leads to a positive diagnosis of TB in immunocompromised population
> 5 mm induration
What does this refer to
Infection of the lower respiratory tract
Responsible for more disease and death than any other infection
Pneumonia
What does this refer to
Hospital-acquired
Ventilator-associated pneumonia
Nosocomial pneumonia
What does this refer to
Streptococcus pneumoniae
Community-acquired pneumonia
What does this refer to
Aspiration
Inhalation
Endotracheal tubes and suctioning
Bacteremia in lungs
Respiratory defenses cannot destroy the microorganism
Routes of infection for pneumonia
What form of pneumonia is commonly seen in the form of influenza
Viral pneumonia
What does this refer to
Inhalation of airborne droplets or spores
Aspiration of oropharyngeal contents
Hematogenous spread from distant sites
Direct extension from contiguous structures
Pathogen Entry and Transmission
What does this refer to
Recognition by pattern recognition receptors (PRRs)
Activation of innate immunity
Recruitment of neutrophils and macrophages
Release of cytokines and chemokines
Immune Response to Inhaled Pathogens
What does this refer to
Inflammatory infiltrate disrupts alveolar architecture
Increased capillary permeability → alveolar flooding
Surfactant inactivation and atelectasis
Inflammation and Alveolar Damage
What does this refer to
Shunting and V/Q mismatch
Decreased diffusion capacity due to edema
Hypoxemia leads to increased respiratory effort
Hypoxemia and Impaired Gas Exchange
What does this refer to
Dysregulated immune response
High levels of IL-6, TNF-alpha, and others
Capillary leak syndrome, hypotension, multiorgan failure
Cytokine Storm and Systemic Effects
What does this refer to
Sudden onset, short duration, exudative phase
CAP
Acute pulmonary infections
What does this refer to
prolonged, granuloma formation, fibrosis
TB or fungal infections
Chronic pulmonary infections
What does this refer to
Preceded by an upper respiratory infection
Cough, dyspnea, and fever
Chills, malaise, and pleuritic chest pain
Clinical manifestations of pneumona
What does this refer to
Prevention of aspiration
Respiratory isolation of immunocompromised individuals
Vaccination for appropriate populations
Reduction of ventilator-associated pulmonary infections through a variety of oral hygiene and endotracheal tube interventions
Prevention of pneumonia
What does this refer to
Gram stain and culture
AFB smear and culture for TB
PCR and multiplex panels for rapid ID
Sputum Analysis and Microbiologic Testing
What does this refer to
Establishment of adequate ventilation and oxygenation
May require mechanical ventilation
Adequate hydration
Good pulmonary hygiene (e.g., deep breathing, coughing, chest physical therapy)
Bacterial pneumonia: Antibiotics
Viral pneumonia: Supportive therapy alone, unless secondary bacterial infection is present
Severe cases: Antiviral medications and/or antifungal, multiple drugs
Treatment for pneumonia
What does this refer to
Community-acquired vs. healthcare-associated
Common organisms: S. pneumoniae, H. influenzae, Legionella
Pathogenesis: alveolar invasion → exudate formation
Clinical: fever, productive cough, pleuritic chest pain
Bacterial Pneumonia
What does this refer to
Gram-positive diplococcus
Virulence factors: capsule, pneumolysin
Lobar consolidation on imaging
Rust-colored sputum, positive urine antigen test
Streptococcus pneumoniae
What does this refer to
__________: thick, mucoid sputum; cavitating pneumonia
Klebsiella
What does this refer to
________: common in CF, ventilator-associated infections
Pseudomonas
What does this refer to
__________: common in CF, ventilated-associated infections
Pseudomonas
What does this refer to
_____________: necrotizing pneumonia, empyema risk
MRSA
What type of atypical bacteria is the following
__________: walking pneumonia, extrapulmonary signs
Mycoplasma pneumoniae
What type of atypical bacteria is the following
__________: slow onset, pharyngitis
Chlamydia pneumoniae
What type of atypical bacteria is the following
___________: high fever, GI symptoms, hyponatremia
Legionella
What does this refer to
Influenza, RSV, adenovirus, SARS-CoV-2
Direct cytopathic effects and immune-mediated injury
Diffuse alveolar damage, ground-glass opacities
Viral Pneumonia
What does this refer to
Viral replication → epithelial cell death
Disruption of tight junctions
Induction of pro-inflammatory cytokines
Pathophysiology of Viral Lung Injury
What type of fungal pneumonia is the following
____________: inhaled spores, granulomas in immunocompetent
Histoplasmosis
What type of fungal pneumonia is the following
_____________: desert exposure, nodular infiltrates
Coccidioidomycosis
What type of fungal pneumonia is the following
________: invasive disease in neutropenic patients
Aspergillus
What does this refer to
Broad range of pathogens including PCP, CMV
Atypical presentations and rapid progression
Requires aggressive diagnostics and empiric therapy
Immunocompromised Host Infections
What does this refer to
Entry of gastric/oropharyngeal contents
Mixed flora: anaerobes, streptococci
Seen in altered mental status, stroke, intoxication
Aspiration Pneumonia
What does this refer to
Tissue necrosis and liquefaction
Complication of severe bacterial infection
Empyema: pus in pleural space, requires drainage
Necrotizing Pneumonia and Empyema
What does this refer to
ICU and ventilator-associated pneumonia
Biofilm formation, MDR organisms
Prevention: hand hygiene, VAP bundles
Nosocomial Infections
What does this refer to
Circumscribed area of suppuration and destruction of lung parenchyma
Follows consolidation of lung tissue, in which inflammation causes alveoli to fill with fluid, pus, and microorganisms.
Necrosis (death and decay) of consolidated tissue: abscess empties into the bronchus, leaving a cavity
Cavitation: Process of abscess emptying and cavity formation
Most common cause: Aspiration
Abscess formation and cavitation
What does this refer to
Fever, cough, chills, sputum production, and pleural pain
Bronchus involvement: Severe cough, copious amounts of often foul-smelling sputum, and occasionally hemoptysis
Clinical manifestation of abscess
What does this refer to
Antibiotics
Chest physical therapy, including chest percussion and postural drainage
Bronchoscopy: To drain the abscess
Treatment for Abscess