full Lec exam 2
1/186
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
187 Terms
Pericardium
Tough membrane covering the heart
Hypertrophic Cardiomyopathy
An enlarged heart condition in non-athletes.
Pulmonary Circuits
Transport blood to & from the lungs; picksup oxygen and releases carbon dioxide.
Systemic circuit
Transports oxygenated blood to the rest of the body and returns deoxygenated blood to the heart.
Cardiac Muscles have what type of discs?
intercalated Discs
Myofibrils
smallest functional unit of your cardiac muscle
Inside muscle of heart
Endocardium
Middle muscle of heart
Myocardium
Outer cavity of heart
pericardial cavity
Outer fiber of heart
fibrous pericardial
Chordae tendineae
string-like extensions that connect heart valves to papillary muscles
Papillary muscles
extension of myocardium where chordae tendineae attach. In ventricles, strong muscle bands.
Trabeculae carnae
ridges of muscles covered by endocardium. Top layer present in ventricles
Mitral Regurgitation
A condition where the mitral valve fails to close properly, allowing blood to flow backward into the left atrium. One common cause is the rupture of the chordae tendineae, which compromises the valve’s ability to seal effectively.
Surgical repairs for mitral regurgitation
chordal transfer and chordal replacement
Mitral Valve Prolapse
valve leaflets bulge into the left atrium during systole
Repair strategies for mitral valve prolapse
artificial chordae tendineae
Myocardial contractile cells
bulk (99%) of the heart muscle responsible for contraction and pumping blood.
Myocardial conducting cells
(1% of cells) form the conduction system of the heart
Sinoatrial (SA) Node: Pacemaker
superior and posterior walls of the right atrium; generates 60-100 beats/min.
Atrioventricular (AV) Node
inferior portion of the right atrium within the atrioventricular septum.
Atrioventricular Bundle (Bundle of His)
Moves impulses from the AV Node through the interventricular septum, dividing into left and right bundle branches.
Purkinje Fibers
Spread impulses throughout the ventricles, ensuring coordinated contraction.
Calcium (Ca2+)
triggers depolarization
Sodium (Na+)
tries to keep membrane potential positive
Potassium (K+)
tries to keeps MP negative
Depolarization
1st, contract
Repolarization
End, relax
Cardiac Cycle
starting from atrium contracting (systole) to ventricle relaxing (diastole)
Systole (contraction)
Contraction of the heart where blood is pumped into circulation.
Diastole (relaxation)
Relaxation phase as chambers refill with blood.
When do potassium channels close?
after refractory period, which is when repolarization takes place
ECG or EKG
Electrocardiogram
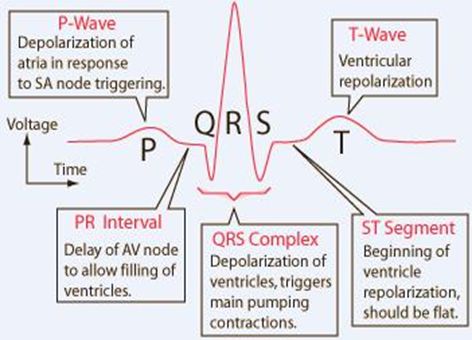
P wave
Signal from the atria. (Small peak. sinoatrial node/depolarization)
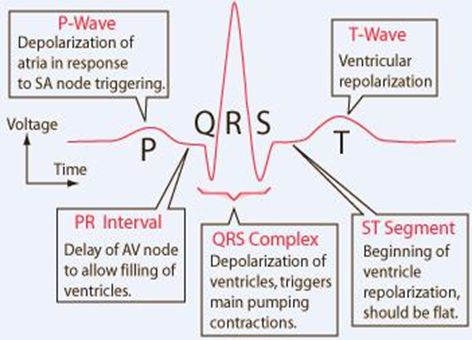
QRS Complex
Signals from the ventricles. (bundle of his. Q bottom of peak, R peak, S bottom of peak.)
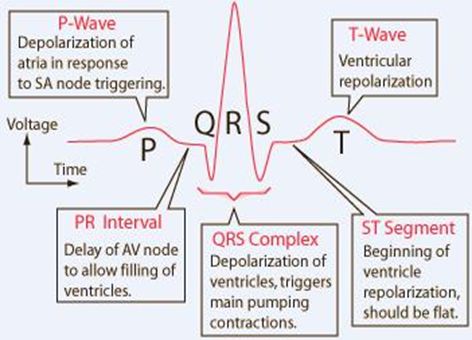
T wave
Indicates recovery phase of ventricles. (thru apex thru purkinje fibers)
Auscultation
stethoscope to chest to hear heart sounds
Inhalation
increases blood flow into the right side of the heart and may increase the amplitude of right-sided heart murmurs.
Expiration
partially restricts blood flow into the left side of the heart and may amplify left-sided heart murmurs.
Atherosclerosis
Build up of plaque in arteries
Arteries
blood vessel that carries blood away from the heart, branching into smaller vessels (arterioles)
Capillaries
A microscopic channel that supplies blood to the tissues, a process called perfusion
Tunica Intima of artery
usually appears wavy.
Tunica Media of artery
thickest layer in arteries. smooth muscle cells and elastic fibers.
Tunica externa of artery
Nervi vasorum and vasa vasorum present
Tunica intima of veins
endothelium appears smooth. no internal elastic membrane
Tunica media of vein
normally thinner than the tunica externa. smooth muscle cells and collagenous fibers predominate. nervi vasorum and vasa vasorum present. external elastic membrane absent.
tunica externa of vein
thickest layer in veins. collagenous and smooth fibers predominate. nervi vasorum and vasa vasorum present.
Continous capillary
Found in almost all vascularized tissues. No indentations, no breaks. One layer of continuous membrane. glucose, water, gases and hormones can pass.
Fenestrated Capillaries
Contains pores (fenestrations) in addition to tight junctions in the endothelial lining. The holes act as a filter. small intestine and kidneys; permeable to larger molecules.
Sinusoid Capillaries
Least common type; flattened, with extensive intercellular gaps and incomplete basement membranes.
Intracellular gaps that allows substances in and out
Location: Liver, spleen, lymph nodes, and bone marrow. Passage of largest molecules like plasma proteins and cells.
Metarteriole
A vessel with structural characteristics of both an arteriole and a capillary.
Vasomotion
Irregular pulsating flow within capillaries.
Capillary Hydrostatic Pressure (CHP):
The pressure exerted by blood against capillary walls.
Blood Colloidal Osmotic Pressure (BCOP)
Pressure created by colloidal proteins in the blood.
Net Filtration Pressure (NFP)
Interaction of hydrostatic and osmotic pressures, driving fluid out of the capillary.
Blood pressure
Force of blood against artery walls. Measured in large arteries.Drives blood flow through arteries and veins. More specific; key factor in capillary exchange influencing fluid movement.
Blood Hydrostatic Pressure
Pressure exerted by blood plasma inside capillaries. Measured in capillaries. Helps push fluids out of capillaries into tissues.
Pulse pressure
Difference between systolic (top number) and diastolic (bottom number) pressure. 120/80 = 40mmHg. Greater than 40mmHh is unhealthy.
Neural mechanisms
cranial nerves, medulla
Endocrine mechanisms
renal, adrenal, brain, heart
Autoregulatory mechanisms
vasodilators, vasoconstrictors
Neurological regulation depends on cardiovascular centers in the
medulla oblongata
Vascular Baroreceptors
Found in aortic and carotid sinuses; help monitor blood pressure.
Low-pressure baroreceptors located in venae cavae and right atrium.
3 vessels in pulmonary circuit
pulmonary trunk, pulmonary arteries, pulmonary veins.
Aorta and the systemic arteries
send blood to virtually every organ of the body
Brachiocephalic artery
located only on the right side of the body with no corresponding artery on the left, branches into right subclavian artery and the right common carotid artery. All go up to your brain.
external carotid artery
Supplies blood to face, lower jaw, neck, esophagus, larynx.
internal carotid atrery
Forms carotid sinus (contains baroreceptors and chemoreceptors); supplies blood to the brain, eyes, vertebral arteries.
Transient Ischemic Attack (TIA, mini-stroke)
Loss of blood flow for a few seconds results in temporary neurological loss. often go unnoticed.
cerebrovascular accident (CVA)
Irreversible brain damage or stroke, with interruption for 3-4 minutes.
Superior vena Cava
Drains most of the body above the diaphragm.
Internal Jugular Veins
drain blood from the brain and superficial facial vein.
Inferior Vena Cava
Large systemic vein draining blood from areas beneath the diaphragm; empties into the right atrium.
Renal Vein
Largest vein entering the inferior vena cava; drains the kidneys.
Adrenal Vein
Drains adrenal gland
Hepatic Vein
Drains blood from the liver to inferior vena cava.
Cirrhosis
Damage to liver sinusoids
Umbilical vein
Carries oxygen-rich blood from mother to fetal heart via ductus venosus.
What marks the location of the former foramen ovale
Fossa Ovalis
Ductus Venosus
Bypasses fetal liver, connecting umbilical vein to fetal heart.
Lymph Nodes
Small, bean-shaped organs located throughout the lymphatic system.
Lacteals
lymphatic capillaries transport dietary lipids and lipid-soluble vitamins to the bloodstream.
Chyle
Formed when dietary triglycerides combine with other lipids and proteins as they enter lacteals, resulting in a milky fluid.
Functions of Chyle
Contains lymphocytes (white blood cells), contributing to the body's immune defenses.
Innate Immune responses
Rapid response involving specialized cells and soluble factors.
Examples of Innate immune responses
Neutrophils, lymphocytes, macrophages&monocytes, eosinophils, basophils. Never Let Monkeys Eat Bananas
Natural Killer cells
Contain cytotoxic (cell-killing) granules; detect and destroy what doesnt belong to you, using a “fas ligand”.
Monocytes & Macrophages (innate)
monocytes circulate in the blood, they grow into macrophages and engulf pathogen through phagocytosis.
Immunosenescence
is the loss of immune function with age. Shrinking of thymus gland starts after puberty. It keeps shrinking until about 35 -45 yrs after which shrinkage happens at 1% per year.
Gene Implication of immunosenescence
FOXN1 implicated in the aging process of thymic function.
Primary routes of entry
Afferent lymphatic vessels
Primary route of exit
Efferent vessels
Spleen
attached to the lateral border of the stomach via the gastrosplenic ligament
Glycoproteins are held together by
disulfide bonds
Light chain
Variable region (top) (beta chain)
Heavy chain
constant region (bottom) (alpha chain)
Class switching
change of one antibody class to another
IgM
first antibody made in primary response, antibody produced in a B cells can change.
IgG
late primary responses and the main antibody of secondary responses in the blood. only antibody that Can cross through the placenta. Moms take vaccines so immunity passes to baby.