Infertility
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
Infertility is defined as the inability to conceive within ______ months
12
For patients over the age of 35, infertility is defined as the inability to conceive within ________ months
6
Infertility can be categorized into:
Primary infertility
Secondary infertility
What’s the difference between these?
Primary: unable to conceive first child
Secondary: has a child but struggling to conceive second
Male infertility can be a result of:
Inadequate number of sperm (or none)
Decreased sperm motility
Obstruction of spermatic ducts or vas deferens
Scrotal varicocele
When the veins wrapping around the spermatic cord are dilated. Appears as vascular black looking bubbles on ultrasound. What infertility problem is this referring to:
Scrotal varicocele
Hormonal imbalances
Mullerian/structural abnormalities
Endometriosis
Ovaries (such as PCOS)
Fallopian tube complications (PIS, adhesions, etc.
The following are all contributors to:
infertility in women
Impaired functional activity of the gonads (ovaries/testicles) with resulting hormonal imbalances is termed:
Hypogandism
If the hypothalamic pituitary gonadal axis is interupted at any level for any reason it is broadly defined as ________________
Hypogandism
True or false: Only males can be affected by hypogonadism
False; women can be affected too
Hypergonadotropic hypogonadism is associated with primary or secondary hypogonadism
Primary
Primary hypogonadism can be congenital or acquired. Why is it referred to as hypergonadotropic hypogonadism?
Production of the hormones estrogen/testosterone are greatly depleted sooooo the hypothalamus and pituitary are working overtime (hyperactive) to stimulate the hormone levels
Hypergonadotropic hypogonadism is associated with
________ FSH & LH
_________ estrogen/testosterone (sex steroids)
High; low
___________________ occurs due to problems with either the hypothalamus or pituitary gland
Secondary: hypogonadotropic hypogonadism
Hypogonadotropic hypogonadism is associated with
________ FSH & LH
_________ estrogen/testosterone (sex steroids)
Low FSH & LH: follicles will not be stimulated
Low: ovulation will not occur
a condition in which the pituitary gland produces too much prolactin is associated with ______________ hypogonadism and is termed _________________
Hypogonadotropic; hyperprolactinemia
If there is a not enough progesterone produced in the luteal phase, the endometrial lining may appear _________ than expected on ultrasound
thinner
Associaited with infertility and very early pregnancy loss
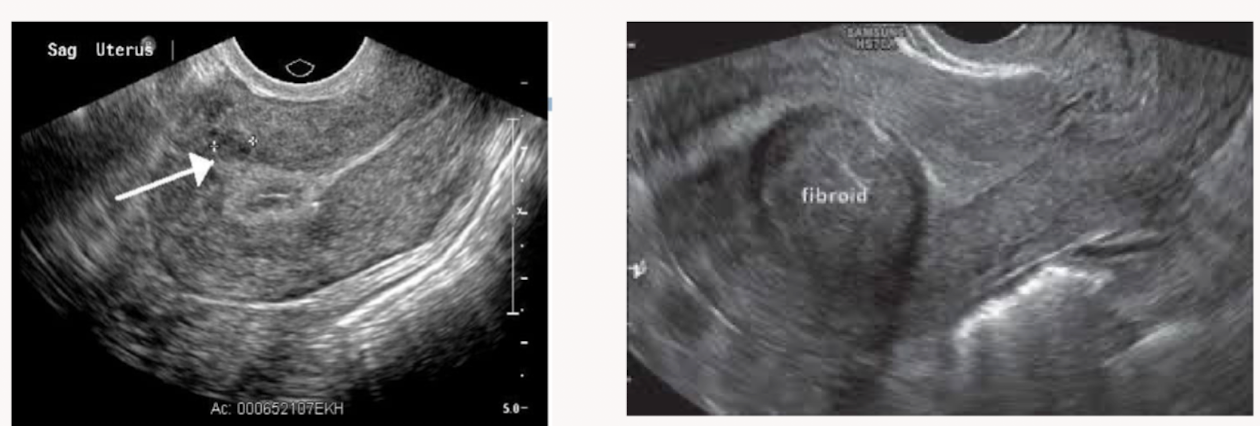
Which patient is likely to have fertility problems?
Patient on the right because the fibroid is larger and more centrally located (pushing into the endometrium)
Why are congenital uterine anomalies, which result from defects in Müllerian duct development, often associated with renal anomalies?
Because the reproductive and urinary systems develop at the same time during development
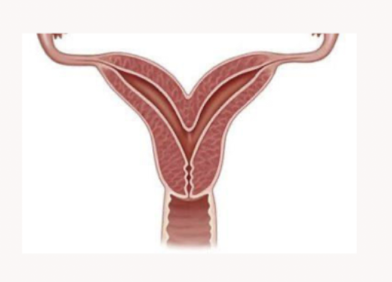
Name the uterine anomaly
Bicornuate uterus: caused by partial failure of fusioon
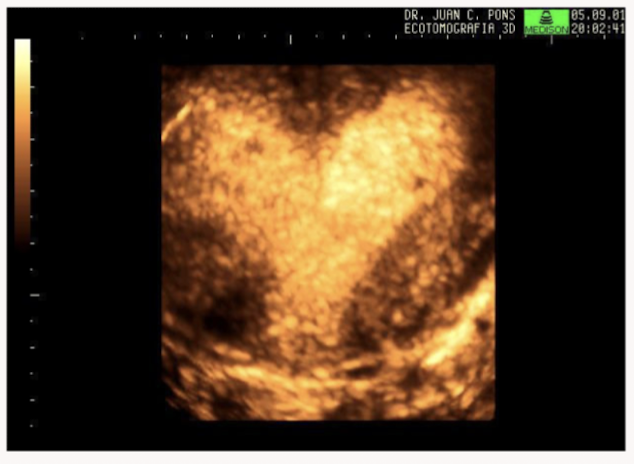
Name the uterine anomaly
Bicornuate uterus: caused by partial failure of fusioon
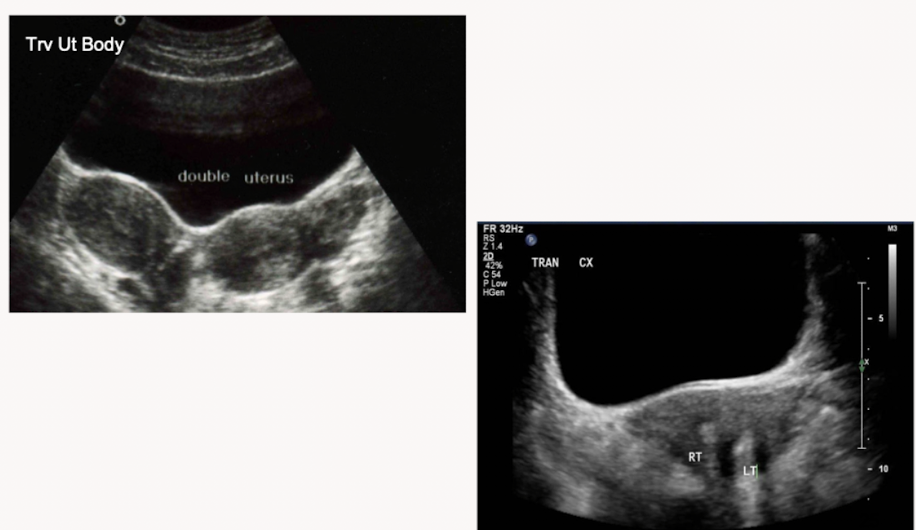
Name the uterine anomaly
Uterus didellphys: failure of fusion resulting in 2 uteri, 2 cervices and 2 vaginal canals
Best proved in transverse
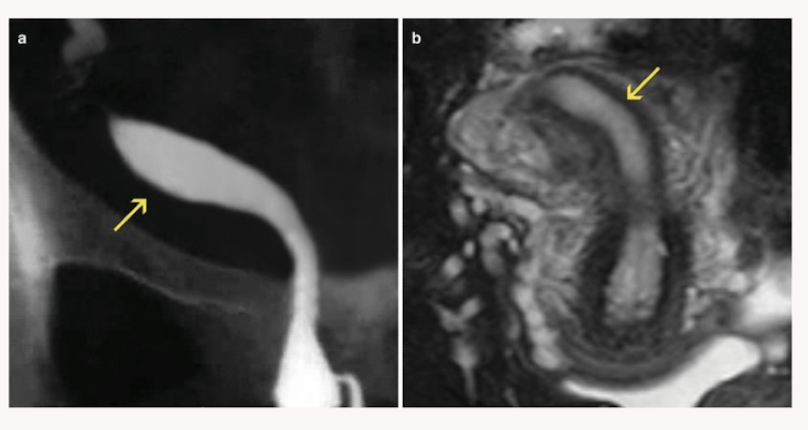
Name the uterine anomaly
Unicornute uterus: usually only has one functioning fallopian tube. May have a rudimentary horn
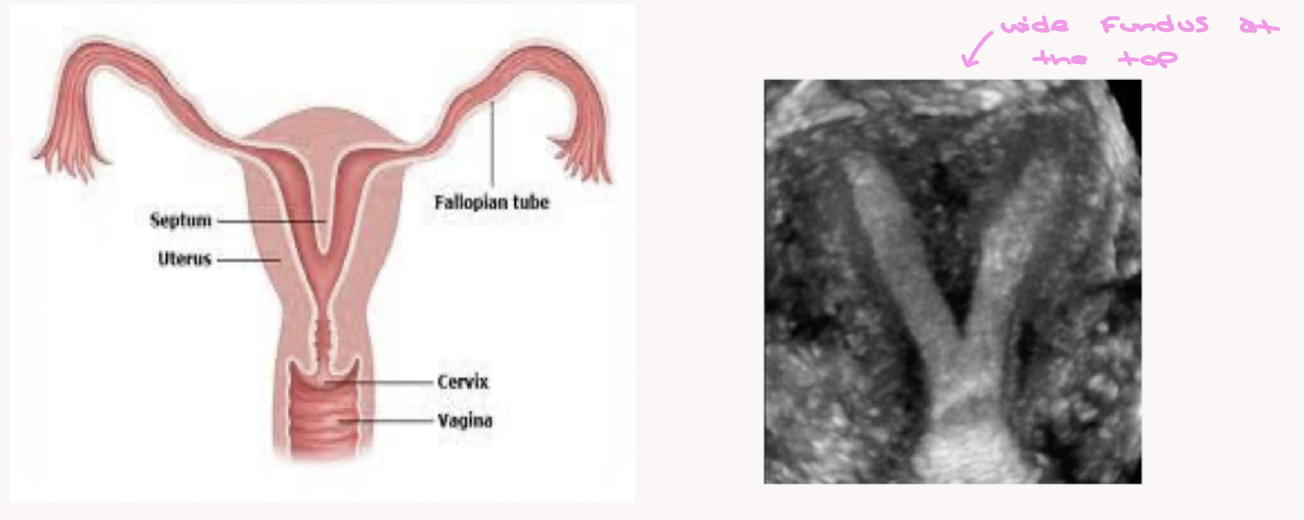
Name the uterine anomaly
Septate uterus: A single wide fundus but with two uterine cavities (septum in the middle)
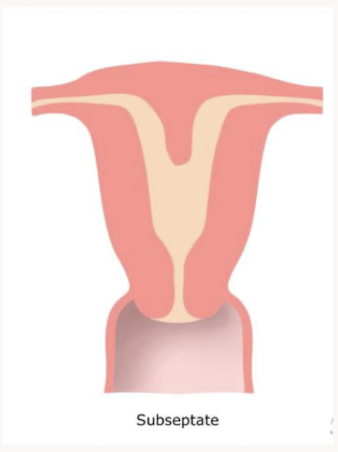
The septum is only partially dividing the uterine cavity. Name the uterine anomaly
Subseptate uterus
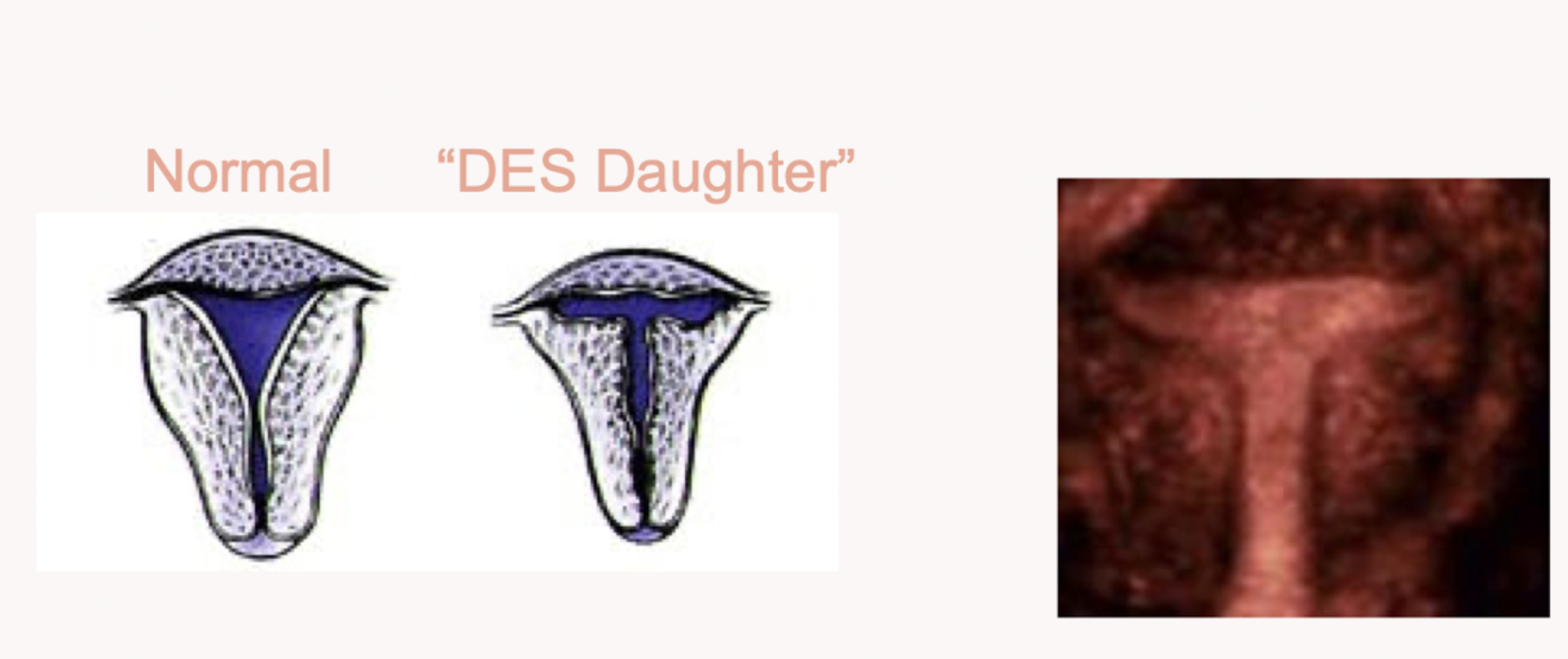
Which uterine anomaly is caused by DES (diethylstilbestrol) which is linked to vaginal cancer?
T shaped uterus
When evaluating the cervix a diameter of less than ____mm may indicate cervical stenosis
1mm
When assessing the endometrium the sonographer evaluates what three things:
1) thickness
2) echgenicity
3) contour (should be homogenous)
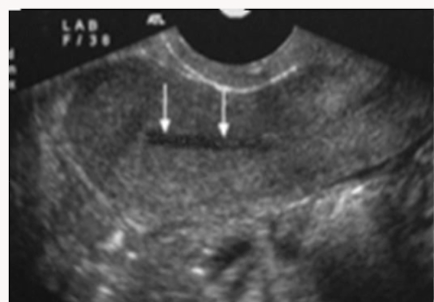
Identify the endometrial phase
During menstruation (may even see movement)
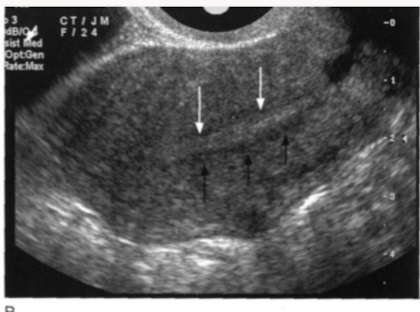
Identify the endometrial phase
early proliferative
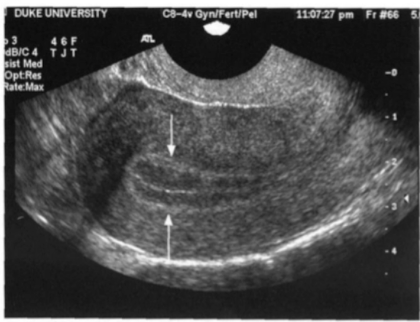
Identify the endometrial phase
Late proliferative (2 line sign)
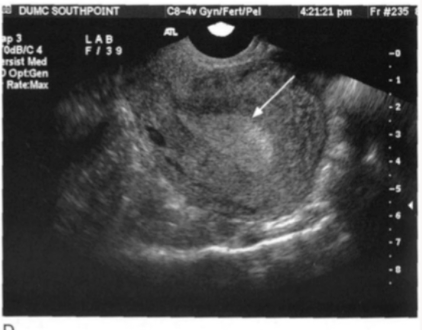
Identify the endometrial phase
Secretory phase: uniformly echogenic and thick
A surgical method used to evalute the fallopian tubes. Considered the gold standard as there will be a definitive diagnosis
Laparoscopy
Which type of procedure involves inserting a catheter through the cervix and injecting contrast/dye to evaluate the uterus and fallopian tube
HSG
A follicle in the ovary measuring greater than ______ is considered cystic
2.5
With this condition follicles grow but ovulation will not occur
PCOS
Define anovulation
an absence of ovulation
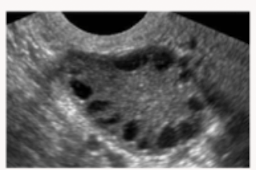
The “string of pearls sign”: a rounded ovary with multiple small immature follicles on the periphery is what condition?
PCOS
What is the difference between “in vitro” and “in vivo”
In vitro: fertilization occurs in a lab setting “in the glass”
In vivo: fertilization occurs in the mother “in the living”
common infertility treatment options: Medications are given between days 3-5 in order to cause development and enlargement of many follicles. Follicles are then imaged and measured. They should measure 15-20mm
Ovarian induction (stimulation) therapy
GIFT (Gamete intrafallopian Transfer)
“put the sperm & the egg in the correct spots within the body so they can meet for their blind date”.
The eggs and sperm are placed in the correct spots through a catheter and fertilization will take place in vivo (within the woman’s body)
ZIFT: Zygote Intrafallopian transfer
Fertilization occurs outside the body and the zygote is then implanted
Intrauterine inseination is used to treat male infertility. What is it??
A catheter containing sperm is placed into the uterine fundus
Ovarian hyperstimulation syndrome (OHSS)
a potential complication of ART in response to medication the ovaries enlarge due to the follicles being overstimulated