PPA 524 ER Pharm
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
48 Terms
What are the 7 causes of DKA?
1.infection
2.physical or emotional trauma, starvation from anorexia
3.medication noncompliance
4.heart attack or stroke
5.pancreatitis
6.pregnancy
7.alcohol or drug abuse, particularly cocaine
For diabetic ketoacidosis , how will the following labs present?
K
pH
pCO2
HCO3
You’ll have to check these every what?
1.potassium FIRST
1.hydrogen ion displaces K+ from intracellular space
2.usually high (normal is 3.5-5.2)
3.can drop precipitously as acidosis is corrected
2.pH
low (less than 7.35)
3.pCO2
1.usually low
2.rapid, shallow breathing
4.HCO3-
usually low
EVERY HOUR

For DKA how does blood sugar present and what are 3 other labs you want to get?
ublood sugar
usually over 250mg/dL
can have euglycemic DKA
starvation, chronic liver disease, pregnancy, infection, alcohol use, SGLT2 inhibitors
ubeta-hydroxybutyrate (BHB) – ketone body
upositive
umagnesium, phosphate
uanion gap
([Na] + [K]) – ([HCO3] + [Cl]), normal 14-18
[Na] – ([HCO3] + [Cl]), normal 10-14
4 step tx for DKA?
BUCKETS of intravenous fluids bc they are dehydrated from osmotic diuresis of hyperglycemia
•NaCl 0.9% (normal saline solution)
–
insulin – regular insulin STAT
•bolus
•continuous IV infusion
•
potassium
other
at BS of 250mg/dL, D5%NS or D5% 0.45%NS
lower BS 50-150mg/dL/hr
Tx in general for hypoglycemia?
Sx?
Tx medication 1 with forms?
Med 2 with MOA and AE and protip?
uinsulin, most oral medications for diabetes
usymptoms of hypoglycemia:
Shakiness or trembling
Sweating
Hunger
Dizziness or lightheadedness
Anxiety or irritability, confusion, blurred vision
Fast heartbeat
utx: dextrose 50% IV; glucagon IM, IV, intranasal (IN)
utx: octreotide (Sandostatin) SQ or IV
MOA: antagonizes pancreatic insulin release
AE: diarrhea, abdominal discomfort
pro tip: type 1 DM pts will not respond to it bc they don’t produce insulin
5 immediate considerations for status epilecpticus
1.electrolyte disturbances
2.hypoglycemia
3.drug withdrawal (benzodiazepine, baclofen)
4.AED withdrawal
5.organic neurologic disease
cerebrovascular accident
tumors
head trauma
what is first line for immediate control of status epilepticus?
(3) other types?
MOA
AE
benzodiazepines
MOA: GABA agonist
AE: respiratory depression, sedation, amnesia
lorazepam (Ativan)
diazepam (Valium)
midazolam (Versed)
(3) meds for secondary control, immediately following benzodiazepine for status epilepticus? WHICH IS FIRST LINE and dose for adult?
plus
phenobarbital IV
ketamine IV
MOA
AE
for both
fosphenytoin (Cerebyx) IV/IM or phenytoin IV
valproic acid IV (Depacon)
levetiracetam IV (Keppra) (FIRST LINE), give 1 GRAM and likely more later
phenobarbital IV
MOA: GABA potentiation
AE: sedation
ketamine IV
MOA: glutamate and NMDA antagonist
AE: dissociative reaction, hypotension, anxiety
Status Asthmaticus
2 immediate considerations
5 meds
immediate considerations
oxygen saturation
acid/base status
medications
for sure IV fluids
for sure albuterol 2.5mg neb q20min x3, then hourly
methylprednisolone (Solu-Medrol) 125mg IV x1
ipratropium (Atrovent) 0.5mg SAMA neb (NOT PO)
magnesium 2gm IVPB over 20min x2
Alcohol withdrawal timing of events:
occurs in first few ___ after stopping, lasts ___; these 5 sx appear ____
________ and _____; most withdrawal episodes, even untreated, stop here
seizures (what type seizures?) in 10-15%
______; rare; mortality is 20%
first few hours after stopping, lasts 3-5 days; tremor, tachycardia, diaphoresis, anxiety, N/V
auditory and visual disturbances; most withdrawal episodes, even untreated, stop here
seizures (generalized tonic-clonic) in 10-15%
delirium tremens; rare; mortality is 20%
Clinical Institute Withdrawal Assessment for Alcohol (CIWA-Ar) Score
(10) sx CIWA measures
range:
what to what is mild?
nausea/vomiting, tremor, sweat, anxiety, activity, tactile disturbance, auditory disturbance, visual disturbance, headache, orientation
range: 0-67
8-10 = mild
Acute tx of alcohol withdrawal
general class with 3 ex. and protip?
(4) vitamins w/ form and duration
protip for the most important vitamin?
(3) other generalish things you need to give?
benzodiazepines
lorazepam (Ativan) IV or PO
diazepam (Valium) IV or PO
chlordiazepoxide (Librium) PO only
pro tip: could be scheduled with a taper or used PRN based on symptoms
vitamins
multivitamin in IV fluids (1 bag of IV fluids per day, the rest are plain) OR oral multivitamin if tolerated
thiamin BEFORE GIVE GLUCOSE: 100mg IM or IV or PO daily for 3 days, then 50-100mg orally every day as follow-up
WILL GET WERNICKE’S encephalopathy if don’t give thiamin 1st before glucose
alcohol abusers should take PO thiamin in general
folic acid: 1mg IM or IV or PO daily
vitamin K: if prothrombin time/INR elevated and liver is functioning
fluid replacement/electrolytes
NS
LR
D5LR or D5NS (ONLY after thiamin)
magnesium
potassium
what med do you give to stop acute seizures?
NO anti-epileptics unless what?
lorazepam (Ativan) to stop acute seizures
NO anti-epileptic drug (AED) therapy is warranted unless status epilepticus develops
(5) meds for long term tx of alcohol withdrawal and how each works
disulfiram (Antabuse) – inhibits aldehyde dehydrogenase; with alcohol, increases serum levels of acetaldehyde
this induces vomiting and is same process that occurs when you drink too much
it’s a deterrent so that they can get turned off from drinking
naltrexone (ReVia) – narcotic antagonist, decreases cravings
clonidine (Catapres) - alpha 2 agonist lowers BP via vasodilation to lower HR
acamprosate (Campral) – may increase activity of GABA system and decreases activity of glutamate
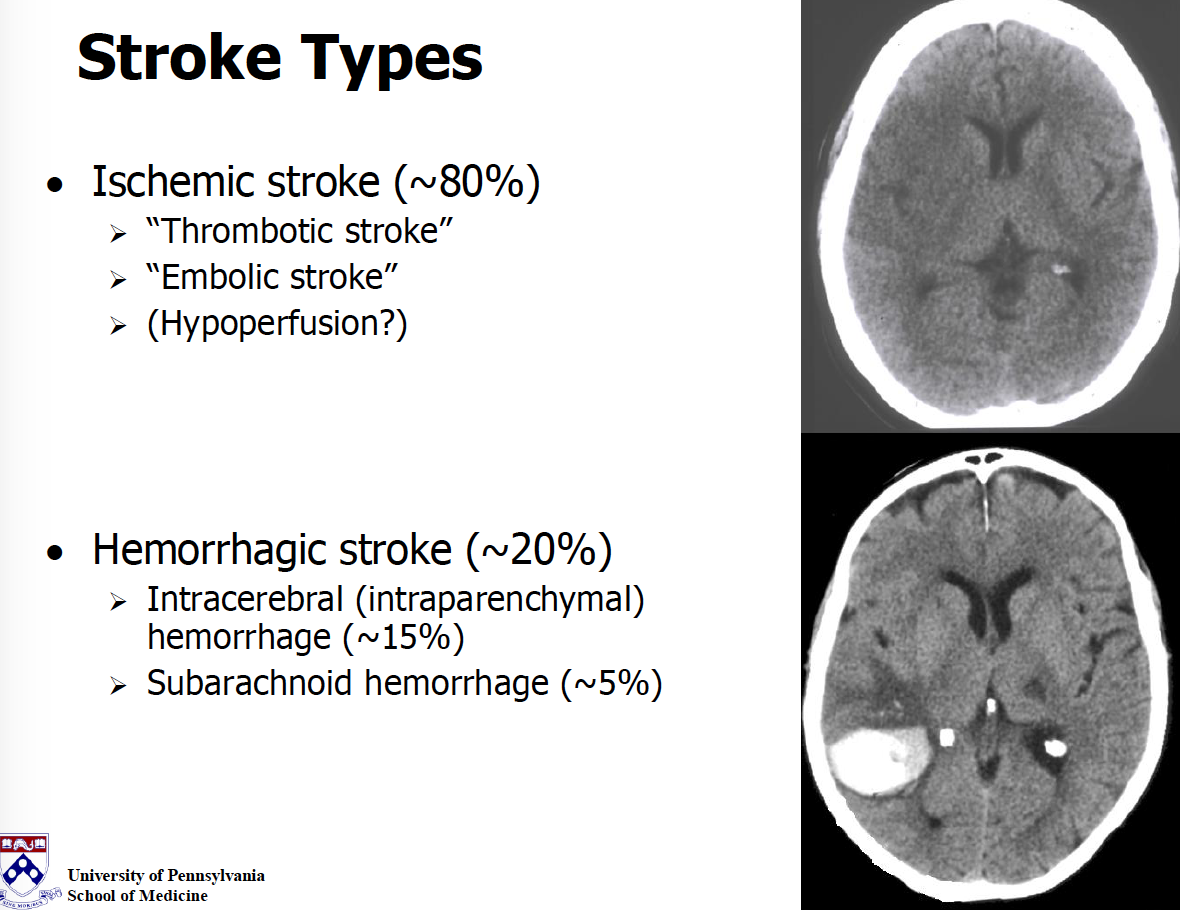
med for CVA?
MOA
AE
-hour (up to ___ hour) window from time of ____ to _____
____ tests
_____ criteria
_____ stabilization
dose: ______
______ – single _____
tissue plasminogen activator (tPA, Activase)
MOA: activates clot dissolution cascade
AE: bruising, bleeding, hemorrhagic conversion
3-hour (up to 4.5 hour) window from time of symptom onset to be able to still give the drug uuyfv
diagnostic tests
inclusion/exclusion criteria
vital sign stabilization
dose: 0.9mg/kg (maximum 90mg), 10% IV bolus over 1 minute then 90% as infusion over 1 hour
tnk-tPA – single IV bolus
Pulmonary embolism tx?
(3) different options
Then what IF massive PE
DOAC (rivaroxaban, apixaban, dabigatran)
or
IV heparin infusion
or
SQ enoxaparin or dalteparin or fondaparinux
or
IF massive PE + hemodynamic instability: alteplase (tPA) 100mg IV infusion over 2 hours followed by parenteral anticoagulation
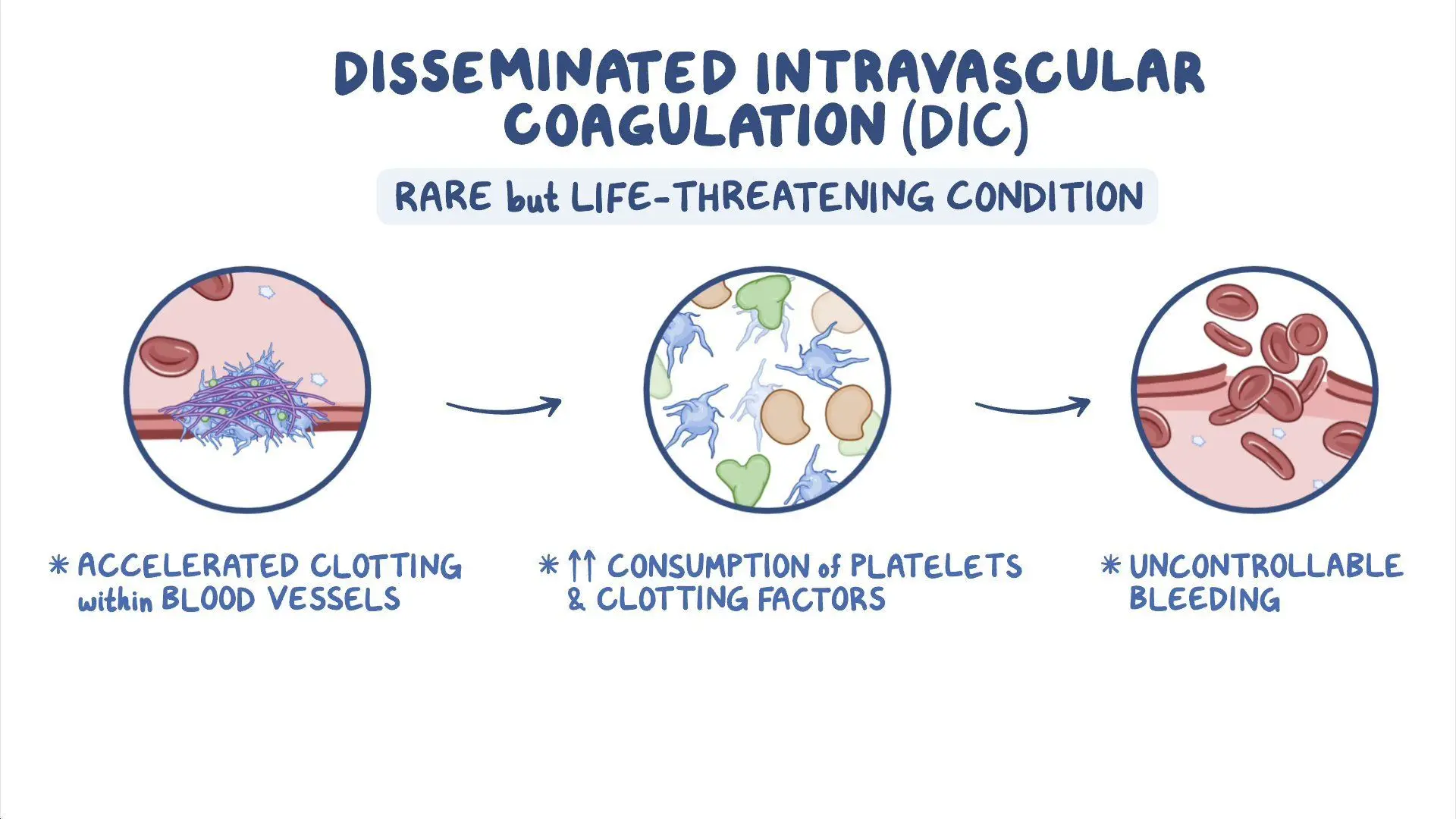
Disseminated intravascular coagulopathy (5) part tx?
What is DIC?
heparin – prevents consumption of clotting factors
activated protein C
intravenous fluids
fresh frozen plasma
packed red cells if anemic
(3) part tx for anaphylaxis?
2 ex. for each except first?
epinephrine
Epi-Pen
antihistamine
diphenhydramine (Benadryl) - H1antagonist
cimetidine (Tagamet) PO -H1/2 antagonist
corticosteroids
prednisone
methylprednisolone (Solu-Medrol, Depo-Medrol)
(4) part tx for Gastrointestinal Hemmorrhage?
with an example
nothing by mouth = NPO (nil per os) bc need to locate specific bleeding source
H2RA - histamine H2-receptor antagonists or H2-blockers. It works by decreasing the amount of acid produced by the stomach.
famotidine IV (Pepcid)
PPI
pantoprazole IV (Protonix)
IV fluids
code blue (ACLS)
give these to tx what?
epinephrine
___
atropine
___
amiodarone (Cordarone)
___
magnesium
___
epinephrine - alpha-1 vasoconstrictor, b-1 increases HR,
vfib, asystole, bradycardia
atropine
bradycardia
amiodarone (Cordarone)
vfib, vtach
magnesium
vfib, vtach, torsades
what are the 5 steps for PRE-op care?
which 2 examples for each one except straightforward ones
NPO
stopping anti-platelet medications
aspirin = 5-7 days
clopidogrel, prasugrel = 5-7 days
ticagrelor = 3-5 days
stopping immunosuppressive medications
stopping anticoagulant medications
warfarin = 5 days
apixaban, rivaroxaban, dabigatran = 2-3 days
prophylactic antibiotic
most: cefazolin (or clindamycin or vancomycin)
GI: cefazolin + metronidazole (or FQ + metronidazole)
Infectious Diseases – Antimicrobial Prophylaxis
choice of agent and dose depends on what 5 things?
surgery being performed
patient allergies
patient weight
timing of antibiotic prophylaxis
30-60 minutes prior to cut
single dose to 48 hours post-op
what is PONV risk assessment used for?
what are the MOA for the 5 meds?
what are 2 other things you need to give/do?
Used for pre-op care
prochlorperazine (Compazine)
MOA: dopamine antagonist
metoclopramide (Reglan)
MOA: dopamine antagonist
ondansetron (Zofran)
MOA: serotonin antagonist
scopolamine (TransdermSCOP)
MOA: anticholinergic patch
AE: dry mouth, confusion
midazolam (Versed)
MOA: GABA agonist
AE: sedation, amnesia
analgesic
blood sugar management
MOA of anesthesia – Local Anesthetics
primary differences are what 3 things?
3 uses?
MOA: inhibits initiation and conduction of nerve impulses by blocking sodium channels
primary differences are onset, duration, and chemical class
uses
diagnose
treat (pain management)
facilitate surgery
3 common local ESTER anesthetics with onset and duration?
Epi typically what?
esters
tetracaine (Pontocaine)
onset: <15min
duration: 2-3hr
procaine (Novocaine)
onset: 2-5min
duration: 15-60min
NOTE: epinephrine generally increases duration of action and decreases bleeding)
3 common local AMIDE anesthetics with onset and duration?
what should you do with these 2?
Epi typically what?
amides
lidocaine (Xylocaine)
onset: <2min
duration: 30-60min
bupivacaine (Marcaine)
onset: 5min
duration: 2-4hr
COMBINE THESE 2 for longer duration and efficacy
(NOTE: epinephrine generally increases duration of action and decreases bleeding)
what 5 things do you need to do for INTRA-op care?
MOA + AE of the agent?
Paralyzing agent (paralyzing agents are needed for surgery bc be fr you want them knocked out for duration)
MOA: inhibits ACh at skeletal muscle receptor
AE: respiratory failure, hypotension
analgesics
sedative
amnesia-inducing agent
blood sugar management
6 step NAAARB management of POST-op care?
nausea and vomiting (PONV – a complication of general anesthesia & analgesia)
analgesic(s)
antibiotic
anticoagulation for DVT prophylaxis
blood sugar management (over 80 under 150)
restarting most medications held pre-operatively
etomidate (Amidate)
what is it/for?
MOA
AE
if you give this be ready to what?
used for anesthesia
MOA: GABA agonist
AE: adrenal suppression, apnea, myoclonus
be ready to INTUBATE
propofol (Diprivan)
what is it/for?
MOA
AE
if you give this be ready to what?
used for anesthesia
MOA: GABA agonist
AE: hypotension, apnea, hypertriglyceridemia (lipid emulsion), injection site reactions, infusion syndrome
be ready to INTUBATE
ketamine (Ketalar)
what is it/for?
MOA
AE
used for anesthesia
MOA: NMDA antagonist (amnesia, analgesia, anesthetic)
AE: ***dissociative reaction-yemporary***, tachycardia, hypertension or hypotension
2 nondepolarizing paralytic anesthetics with onset and duration?
what does nondepolarizing mean?
need to give what and when with paralytic agents?
remember to what with paralytics?
atracurium (Tracrium)
onset: 2-3min
duration: 35-45min
rocuronium (Zemuron)
onset: 1 minute
duration: 45-60 minutes
nondepolarzing means they won’t twitch before going into sedation
NEED TO GIVE AMNESIA MED (PROPOFOL) BEFORE paralytic agent
INTUBATE pts STAT AFTER GIVE PARALYTIC bc they paralyze diaphragm too
1 depolarizing paralytic anesthetic with onset, duration, and protip?
depolarzing paralytics cause what?
MOA
succinylcholine (Anectine)
onset: 1min
duration: 5-10min
pro tip: avoid in patients with hyperkalemia, skeletal muscle injury
Depolarization can cause a release of K+ from muscle cells, potentially leading to dangerously high K+ levels, especially in patients with certain condition
DEPOLARIZING PARALYTICS CAUSE TWITCHING before paralysis sets in
Depolarizing muscle relaxants, such as succinylcholine, act as agonists at the nicotinic acetylcholine receptors (nAChRs) at the neuromuscular junction.
They bind to these receptors, mimicking the action of acetylcholine, a neurotransmitter that normally stimulates muscle contraction.
However, unlike acetylcholine, which is rapidly broken down, depolarizing agents remain bound to the receptors for a longer period, causing a sustained depolarization of the muscle membrane.
This prolonged depolarization prevents the muscle from responding to further nerve signals, leading to paralysis
sugammadex (Bridion)
MOA
AE
Protip
MOA: complexes with rocuronium and vecuronium; reversal agent
AE: bradycardia, hypotension, afib, AV block, nausea, cardiac arrest, hypersensitivity, Vfib
pro tips: may need repeat doses; given in PACU
what paralytic do you give for for malignant hyperthermia?
what is malignant hyperthermia?
dantroline
(a rare but serious complication of general anesthetics & succinylcholine)
what is the 2 step Rapid sequence induction of anesthesia (in the field, E.D., or O.R.)?
midazolam (Versed) or propofol or etomidate or ketamine
succinylcholine or atracurium (Tracrium) or rocuronium (Zemuron) or another NMB
what is PONV?
6 meds for it?
prochlorperazine (Compazine)
MOA: dopamine antagonist
metoclopramide (Reglan)
MOA: dopamine antagonist
ondansetron (Zofran)
MOA: serotonin antagonist
scopolamine (TransdermSCOP)
MOA: anticholinergic
dexamethasone (Decadron)
MOA: corticosteroid
aprepitant PO, fosaprepitant IV (Emend)
MOA: neurokinin antagonist
AE: headache, hypersensitivity,
post-operative nausea and vomiting (a complication of general anesthesia & analgesia)
4 meds for ICU sedation?
dexmedetomidine (Precedex) MOA + AE
benzodiazepine (lorazepam, diazepam, midazolam) – frequent administration or continuous infusion to keep patient calm and/or reduce fighting the ventilator
propofol (Diprivan) – alternative to benzo. continuous infusion for short-term (up to 3 days), the drug is suspended in oil so it increases their triglycerides, chronic use = HLD
dexmedetomidine (Precedex)
MOA: centrally-acting alpha-2 agonist, reducing NE secretion and producing analgesia
AE: hypotension, bradycardia, hyperthermia (w/ precedex infusions in OR)
delirium/agitation – haloperidol (Haldol)
what should you do in ICU care regarding:
narcotics
NM blockade
environment
narcotic (fentanyl, hydromorphone, morphine)
frequent administration or continuous infusion to minimize pain and/or reduce fighting the ventilator
neuromuscular blockade
paralyze patient to prevent fighting the ventilator, must be given with sedation +/- analgesia to prevent panic
environmental conditions
bright lights, loud noise, overnight interruptions contribute to delirium and agitation
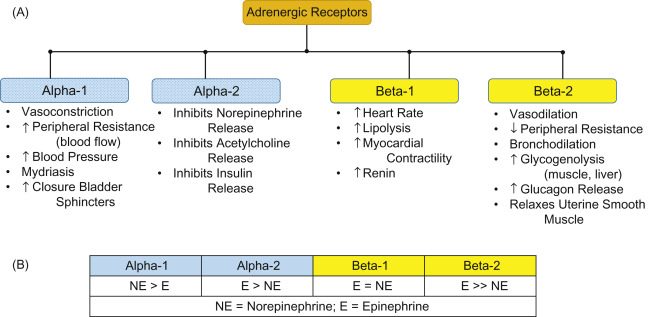
4 vasopressors for ICU care?
receptors for all?
what do they each do?
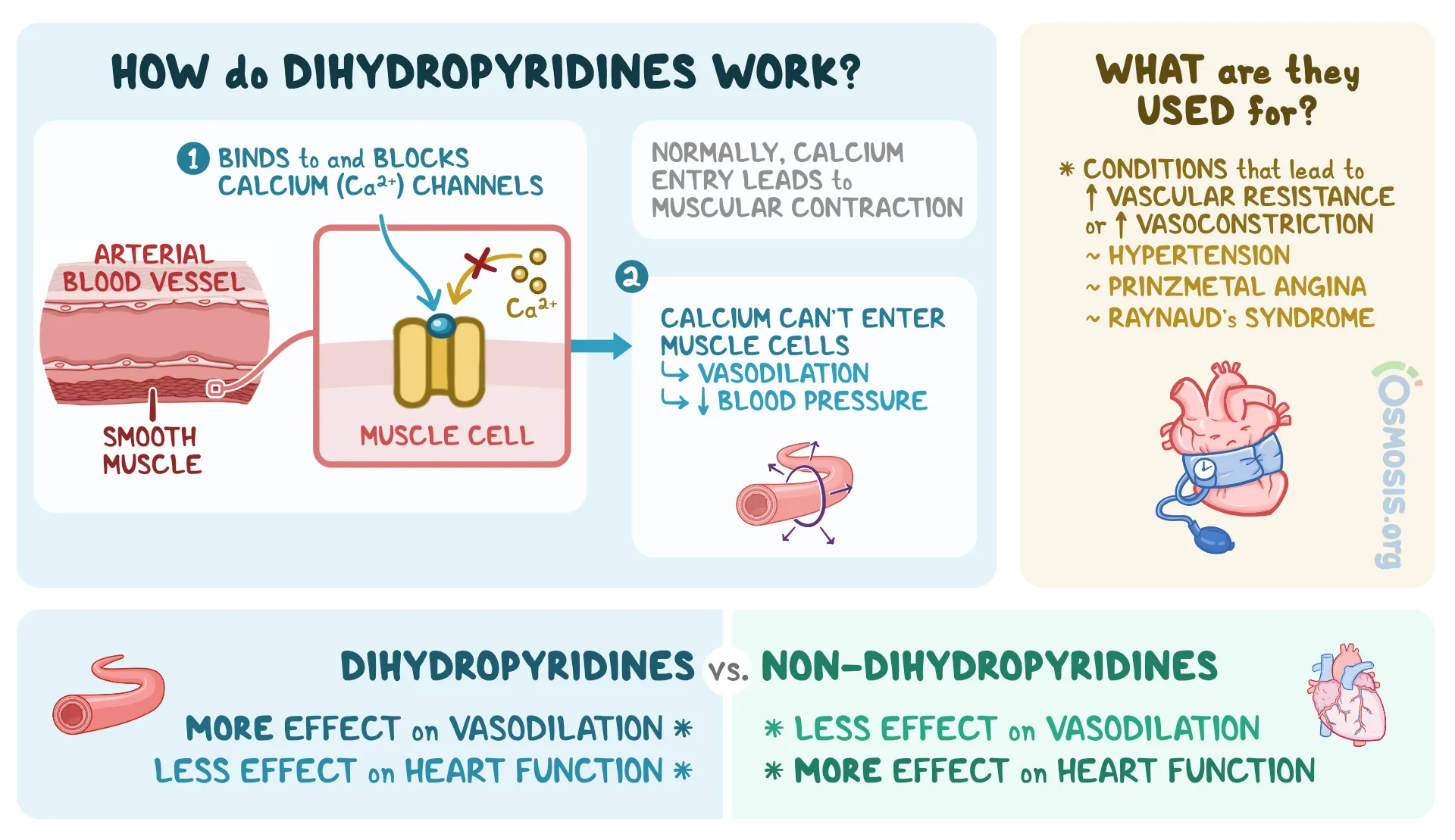
3 meds for BP?
pressors
epinephrine: a1, B1, B2
norepinephrine: B1 and a1
phenylephrine: a1 (when used alone may cause bradycardia initially)
dopamine: B1 and a1
B1 increases HR
B2 bronchodilation
A1 vasoconstriction
blood pressure reduction
nitroprusside/nitroglycerin
labetalol: injection or continuous infusion
nicardipine (Cardene): dihydropyridine CCB (dilates vessels w/o effecting HR)
4 notes about ICU care regarding:
PICC lines
Parenteral nutrition
Infection control
Abx therapy
central venous access – PICC lines or central lines
parenteral nutrition transitioning to enteral nutrition
infection control
wash hands
glove and gown
aggressive antibiotic therapy – ANY infection that originates in the ICU is considered nosocomial until proven otherwise; must address resistant bacteria (Pseudomonas, MRSA, MRSE, VRE, fungi, etc)
3 things for DVT prophylaxis?
2 things for stress ulcer prophylaxis?
DVT prophylaxis
enoxaparin (Lovenox), dalteparin (Fragmin), fondaparinux (Arixtra), heparin
TED hose
intermittent pneumatic compression devices (IPCD)
stress ulcer prophylaxis
H2RA (famotidine IV)
PPI (pantoprazole IV)
acid/base management in ICU
pH = x
HCO3- = x
pCO2 = x
6 buffers?
compensation
fast
increased x
decreased x
slow
increased x
increased x
pH = 7.35-7.45
HCO3- = 22-28
pCO2 = 35-45
buffers
albumin & other proteins
hemoglobin
phosphate
bicarbonate
trapping of H+ by ammonia (NH3)
release of H+ by ammonium (NH4+)
compensation
fast
increased respiration rate to lower pCO2
decreased respiration rate to raise pCO2
slow
increased H+ elimination by kidneys
increased HCO3- synthesis and/or conservation by kidneys
metabolic acidosis
lab values
cuases
meds that cause (4)
Tx:
sepsis:
ketoacidosis:
hypoperfusion:
meds:
pH = less than 7.35
HCO3- = low (consumption or loss)
pCO2 = normal, then low
causes: sepsis, ketoacidosis, hypo-perfusion, diarrhea
medications
nephrotoxic medications
excess normal saline solution
propofol (Diprivan)
aspirin
Tx:
sepsis: aggressive antibiotic therapy, fluid resuscitation, blood pressure control
ketoacidosis: insulin (if DKA), fluids
hypo-perfusion: fluids, pressor medications (AFTER fluid resuscitation)
medications: discontinue offender, bicarbonate (for aspirin OD); bicarbonate for pH below 7.2
metabolic alkalosis
labs
causes
meds that cause
Tx
pH = greater than 7.45
HCO3- = elevated
pCO2 = normal, then high
causes: NG suction
medications: antacids (e.g., calcium carbonate), diuretics
treatment: H2RA or PPI, sodium chloride infusion, potassium supplementation, carbonic anhydrase inhibitor
respiratory ACIDosis
labs
causes
meds that cause
Tx
pH = less than 7.35
HCO3- = normal, then high
pCO2 = high
causes: respiratory failure
medications
opioid analgesics
propofol
treatment: ventilation, B2 agonist, steroids, naloxone (beware of pulmonary edema)
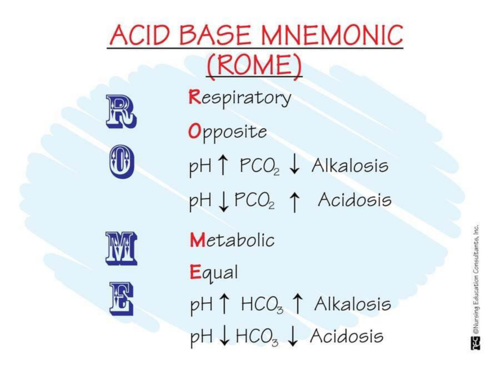
respiratory ALKAlosis
labs
causes
med causes
Tx
pH = greater than 7.45
HCO3- = normal, then low
pCO2 = low
causes: pain, anxiety, hyperventilation
medications: aspirin (due to metabolic acidosis)
treatment: analgesic, benzodiazepine
just fyi why don’t paralytics stop the heart?
The short answer is: none! The better answer is: Neuromuscular blocking drugs like atracurium, rocuronium, mivacurium etc act on the neuromuscular junction. They antagonise nicotinic acetylcholine receptors and this cause an inability to pass inputs from nerve to muscle cells (as opposed to suxamethonium which agonises the nictotinic receptors hence people twitch briefly after sux before paralysis sets in).
Cardiac tissues do utilise acetylcholine but they have muscarinic receptors and as such the neuromuscular blockers have no effect. Cardiac tissue also has an intrinsic automaticity which organises cardiac impulses/beating.
It is interesting that when you 'reverse' neuromuscular blockers with neostigmine (an acetylcholineesterase inhibitor) you get more acetylcholine available but not just at the neuromuscular junction, also in cardiac tissue. This means that neostigmine alone would cause a bradycardia (potentially significantly) and so we (almost) always give it with glycopyrrolate which causes a relative tachycardia.