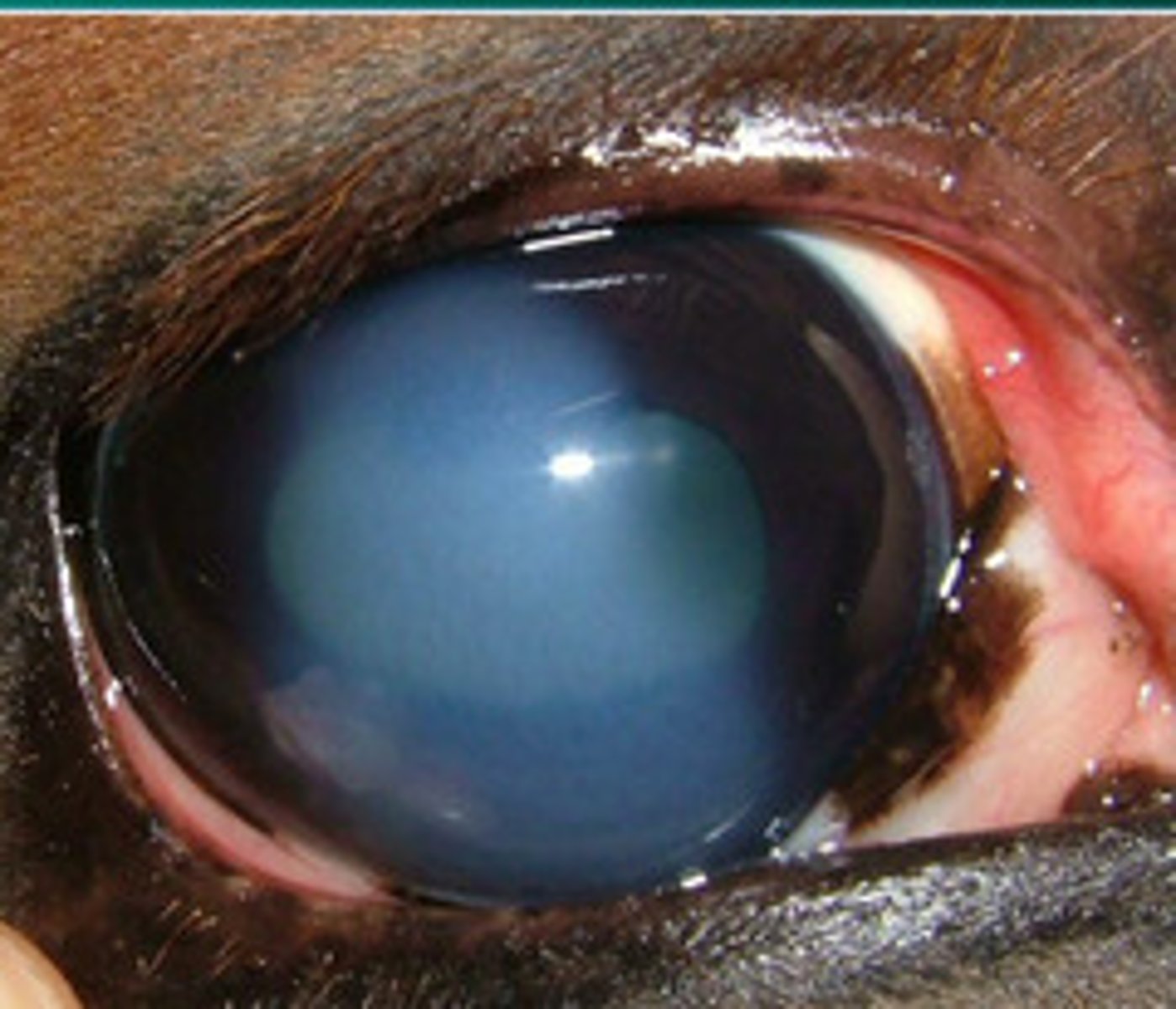
27 Corneal Ulcers and Corneal Healing in the Horse
1/63
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
64 Terms
VERTICALLY: 23-36 mm
HORIZONTALLY: 28-32 mm
What is the size of the equine cornea vertically and horizontally in health?
CENTRALLY: 1.0-1.5 mm
PERIPHERALLY: 1.0 mm
What is the thickness of the equine cornea centrally and peripherally in health?
Collagen
The cornea is a highly organized stroma made of WHAT?
It takes about 7 minutes = matters because it means medication will be there for 7 minutes before it is wiped away, so it needs to be permeable
What is the tear replacement rate for equine tears? Why does this matter?
Superficial ulcer
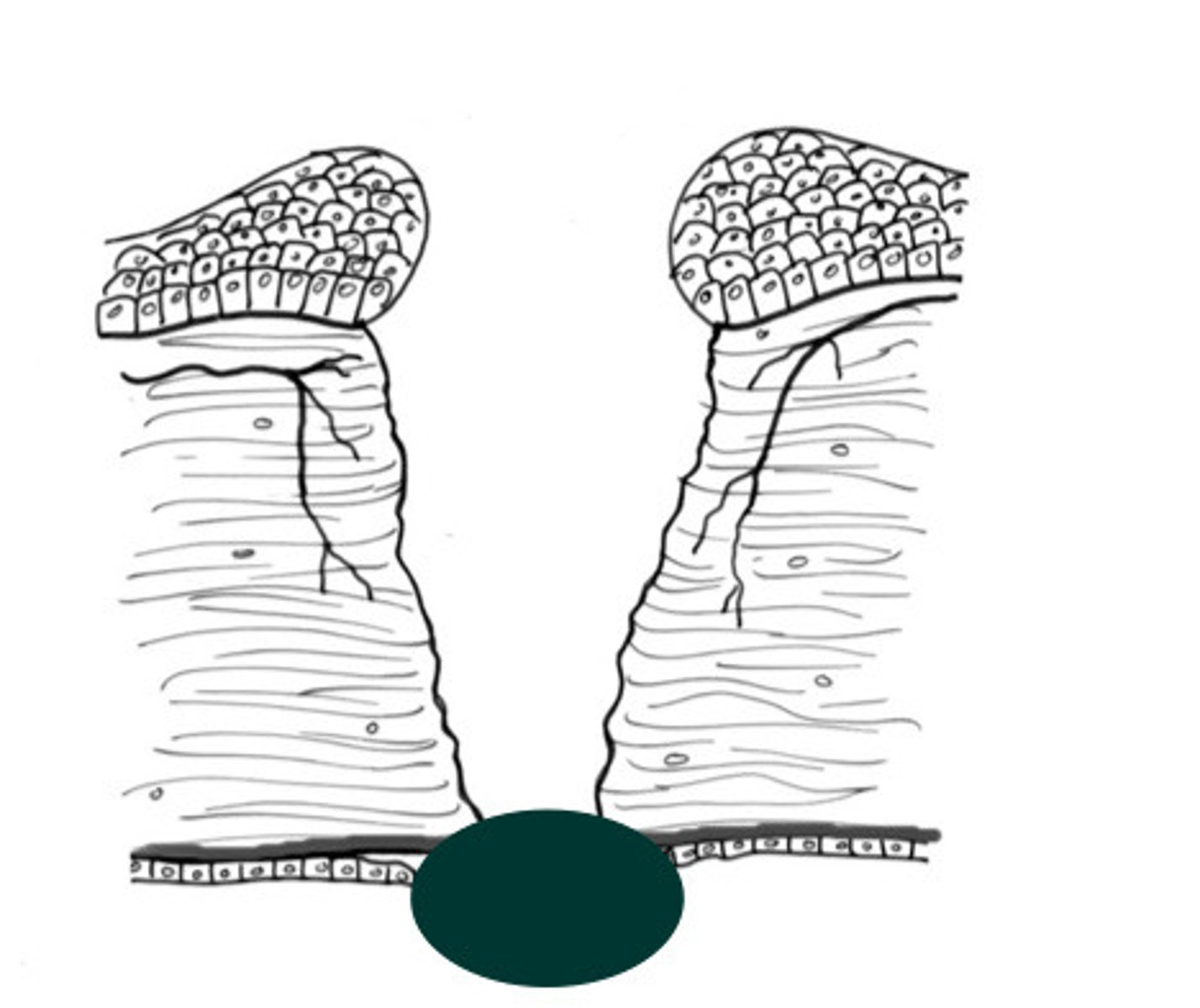
Describe what type of cornea ulcer is happening here, where the epithelium is gone?
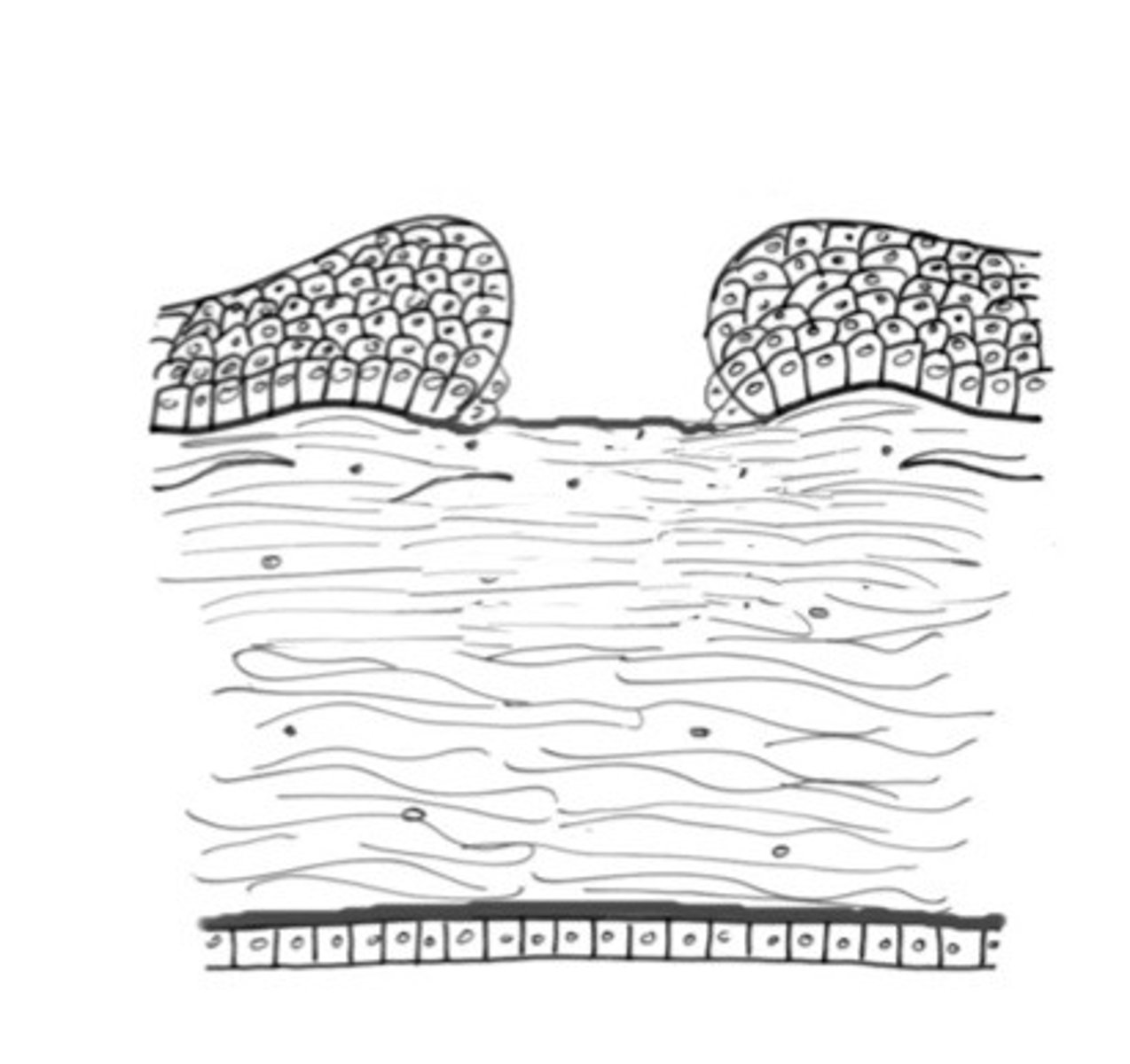
Desmetocoele
Describe what type of cornea ulcer is happening here, where the deepest layer is exposed?
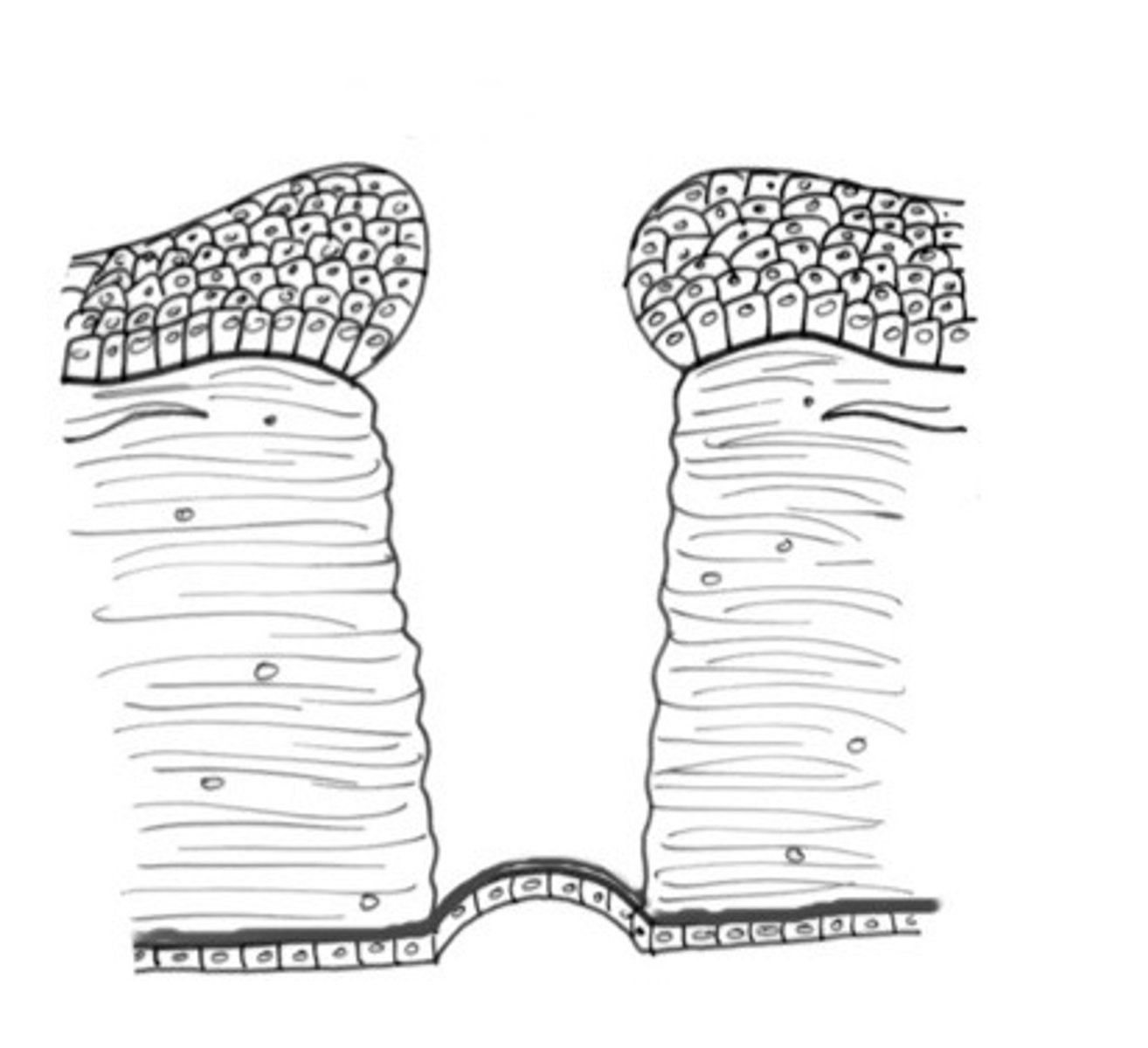
Deep ulcer
Describe what type of cornea ulcer is happening here, where collagen is lost?
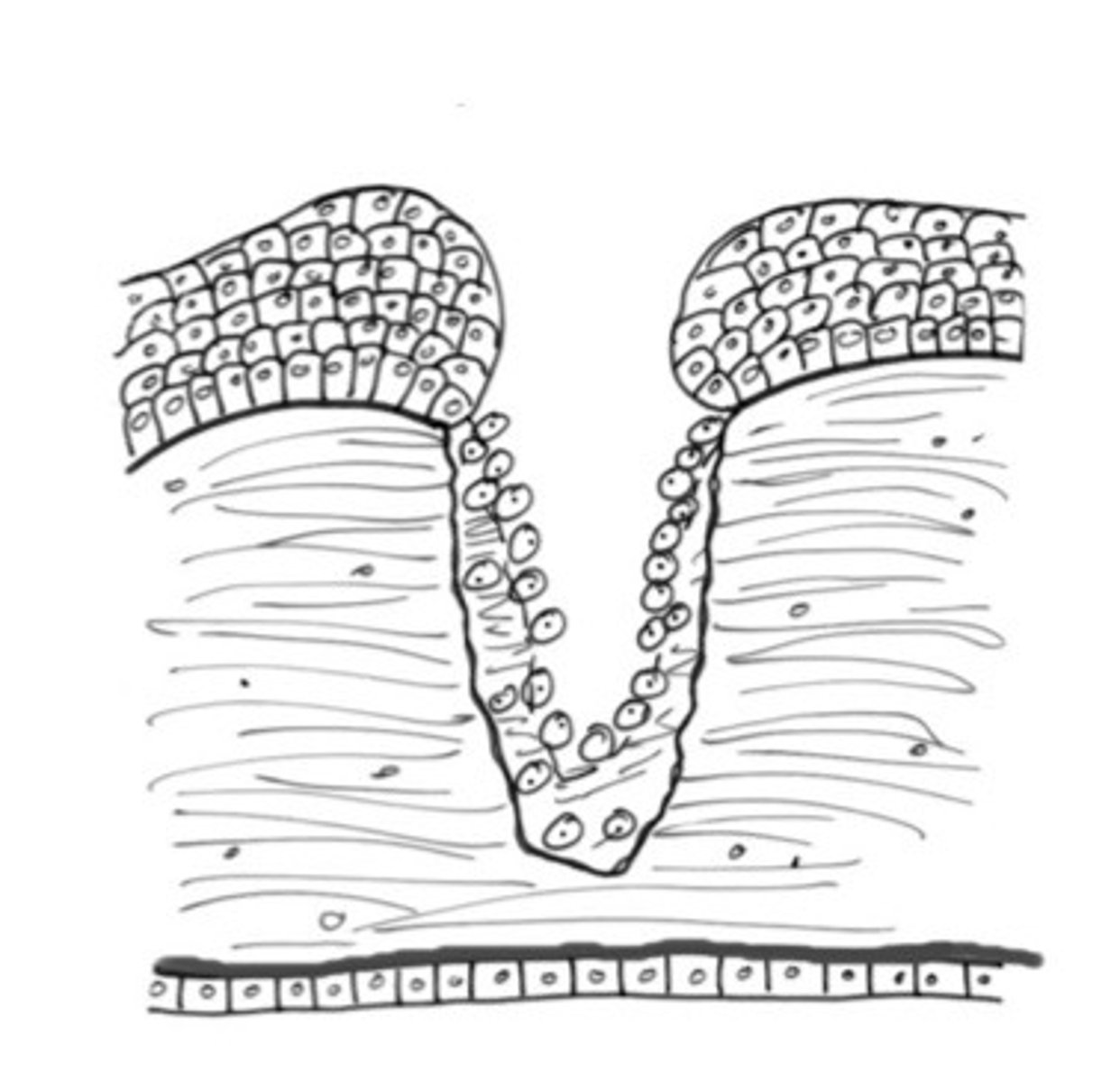
Iris prolapse
Describe what type of cornea ulcer is happening here, where the eye plugs the hole in case of rupture?
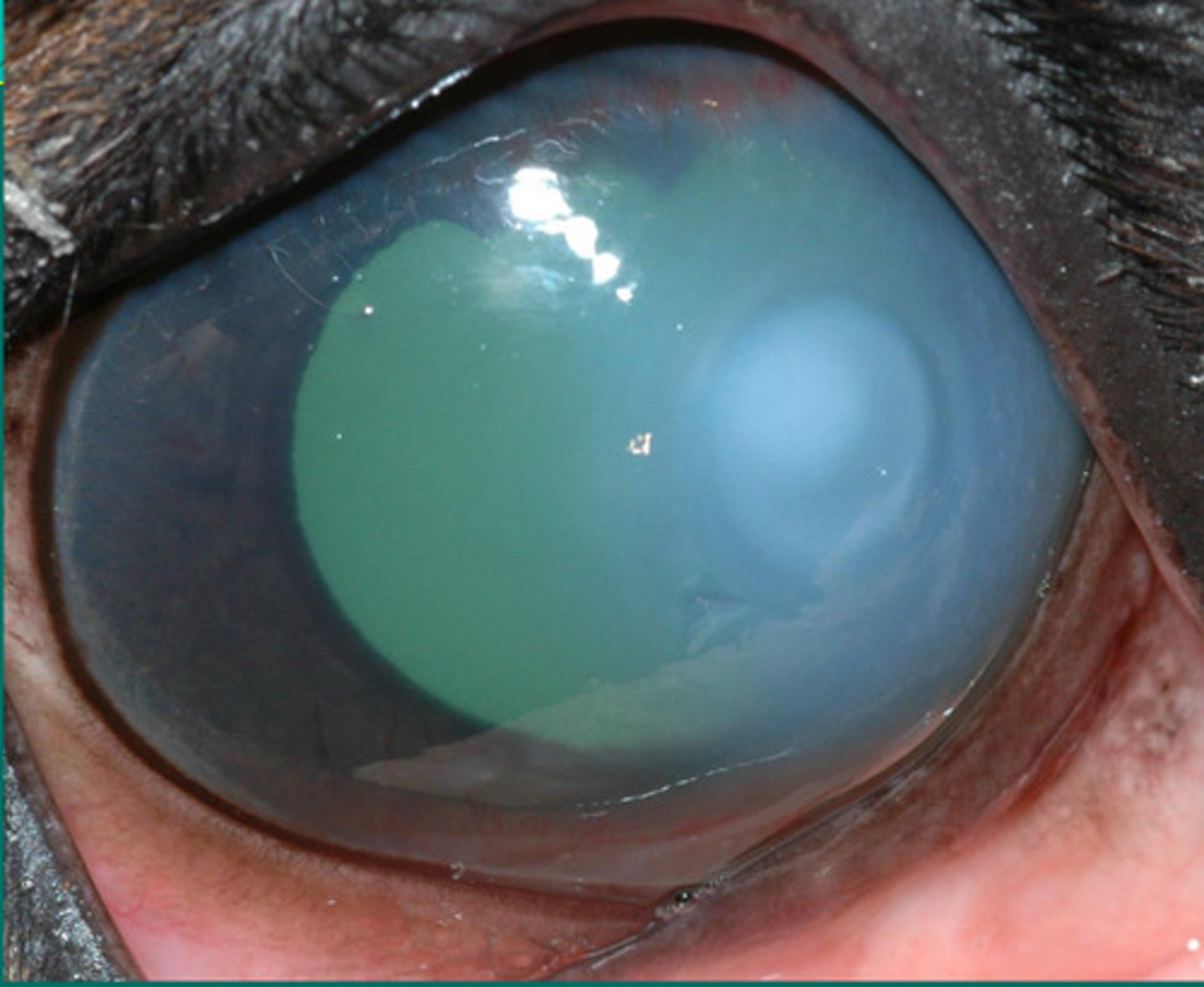
Cornea ulcer = superficial with cellular infiltrate but the dark ring around it shows that part is thinner
Describe what you are seeing?
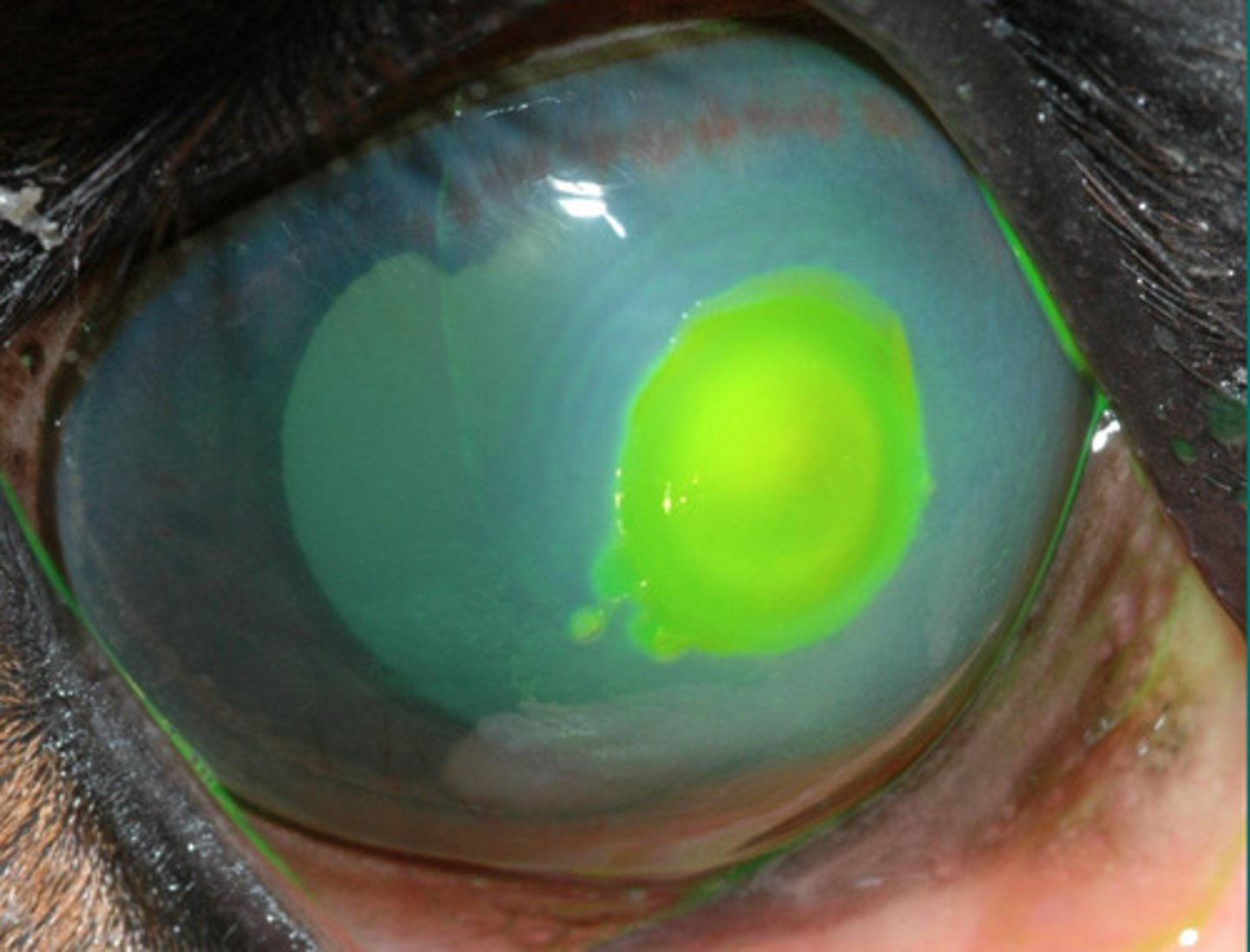
Stained corneal ulcer
Describe what you are seeing?
Cornea abrasion (faint uptake)
Describe what you are seeing?
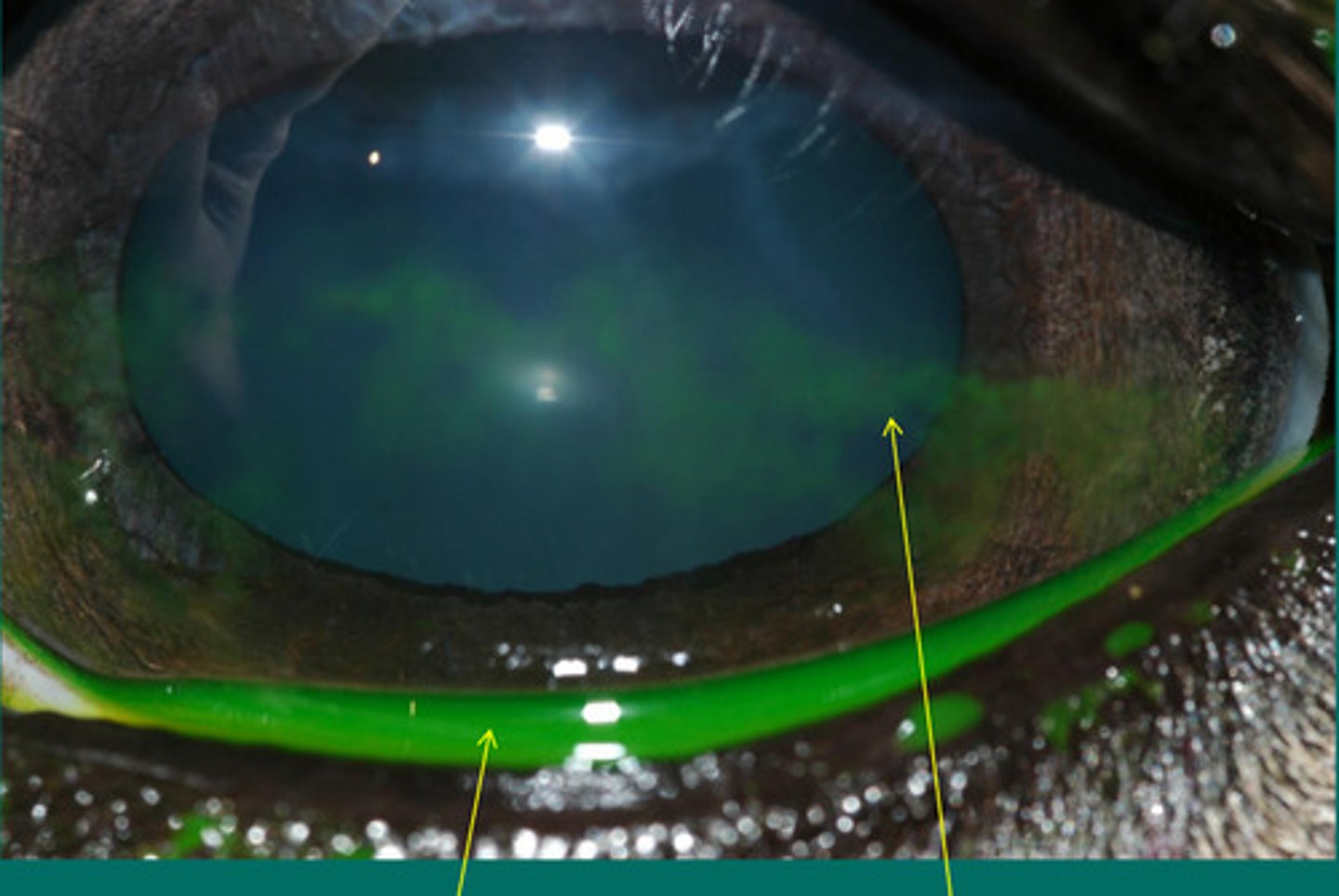
Superficial abrasion
Describe what type of cornea insult is happening here?

Sequestrum from fungal plaque
Describe what you are seeing?
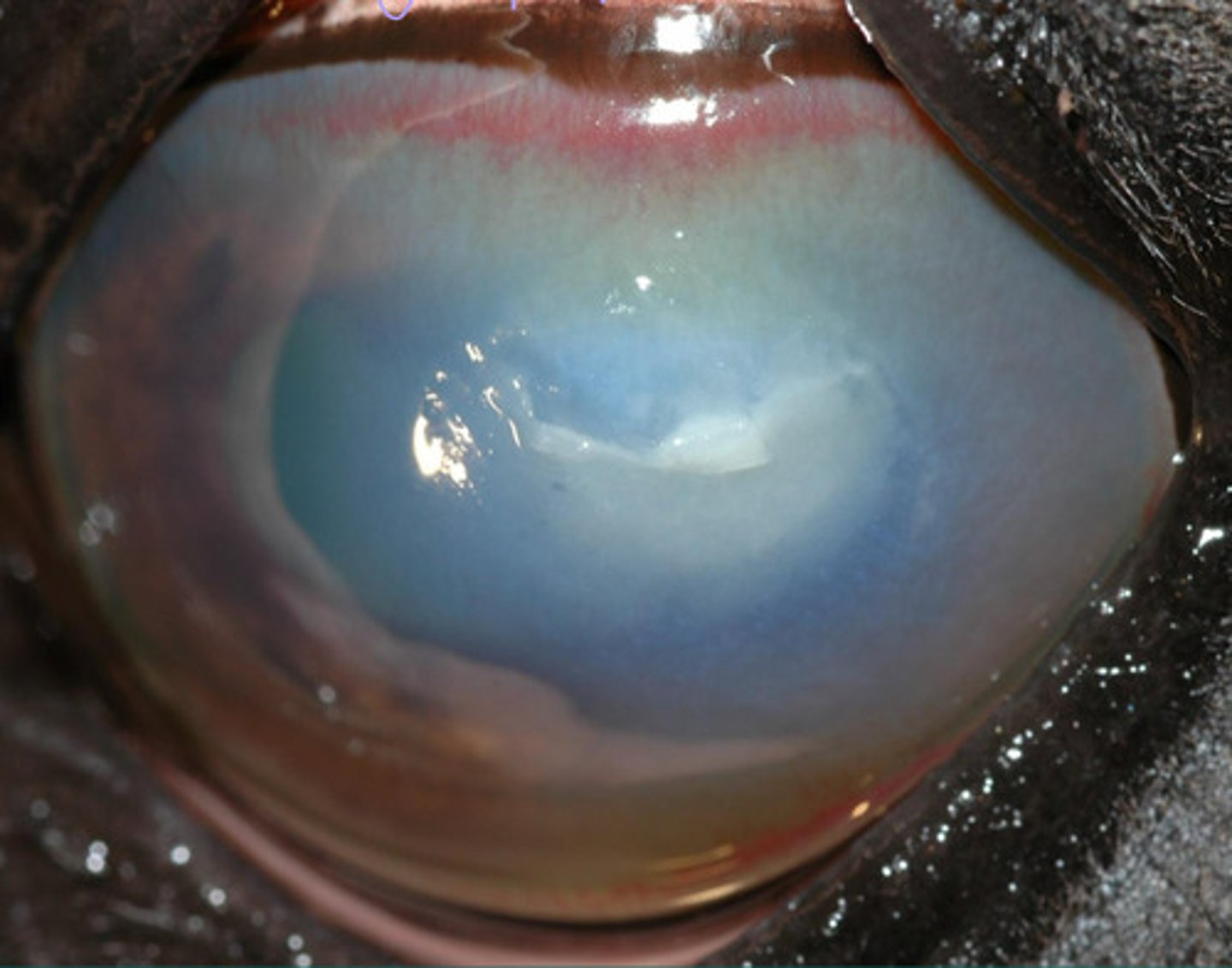
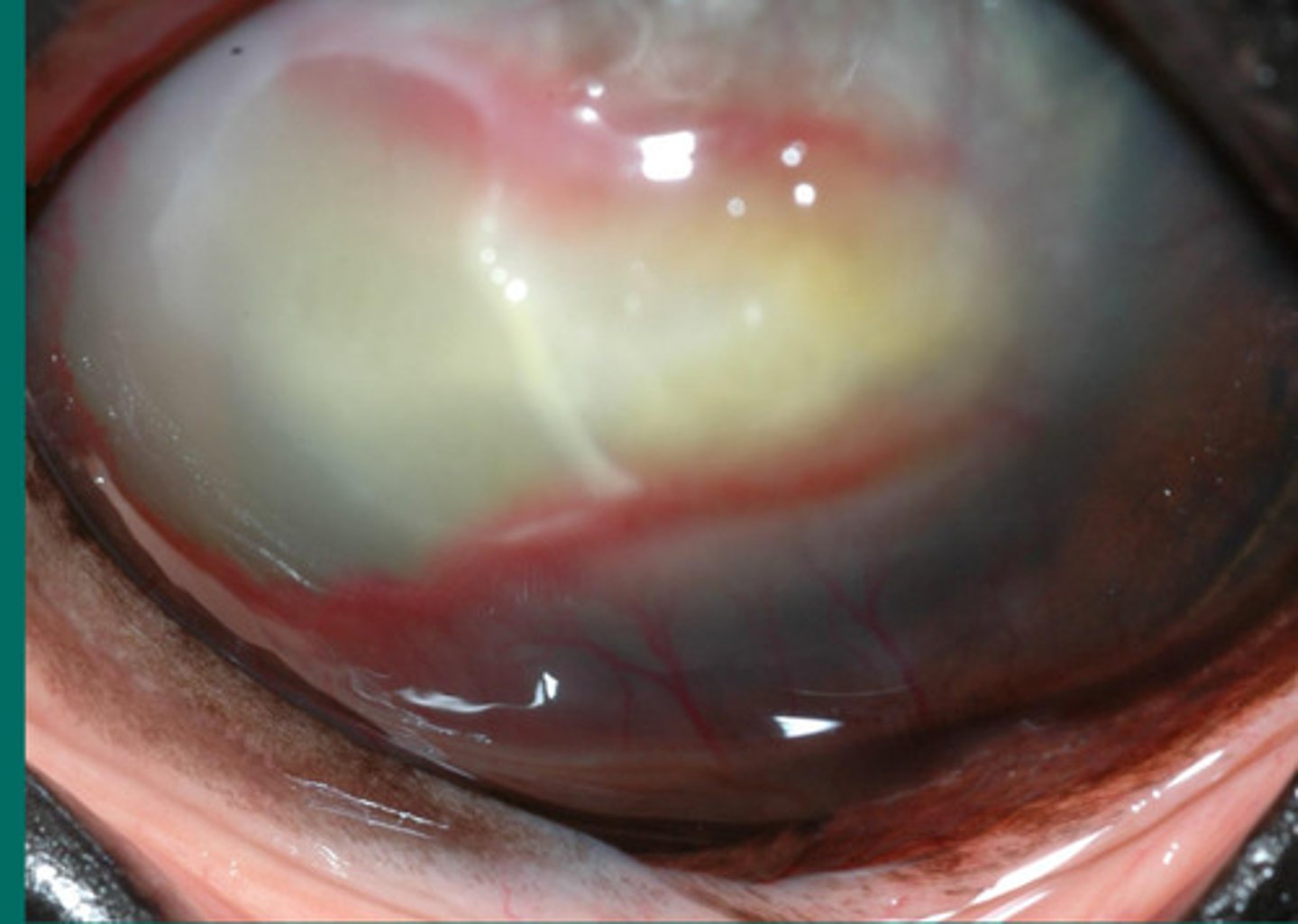
White shows that there is an abscess in this eye, indicating neutrophils
Describe what you are seeing?
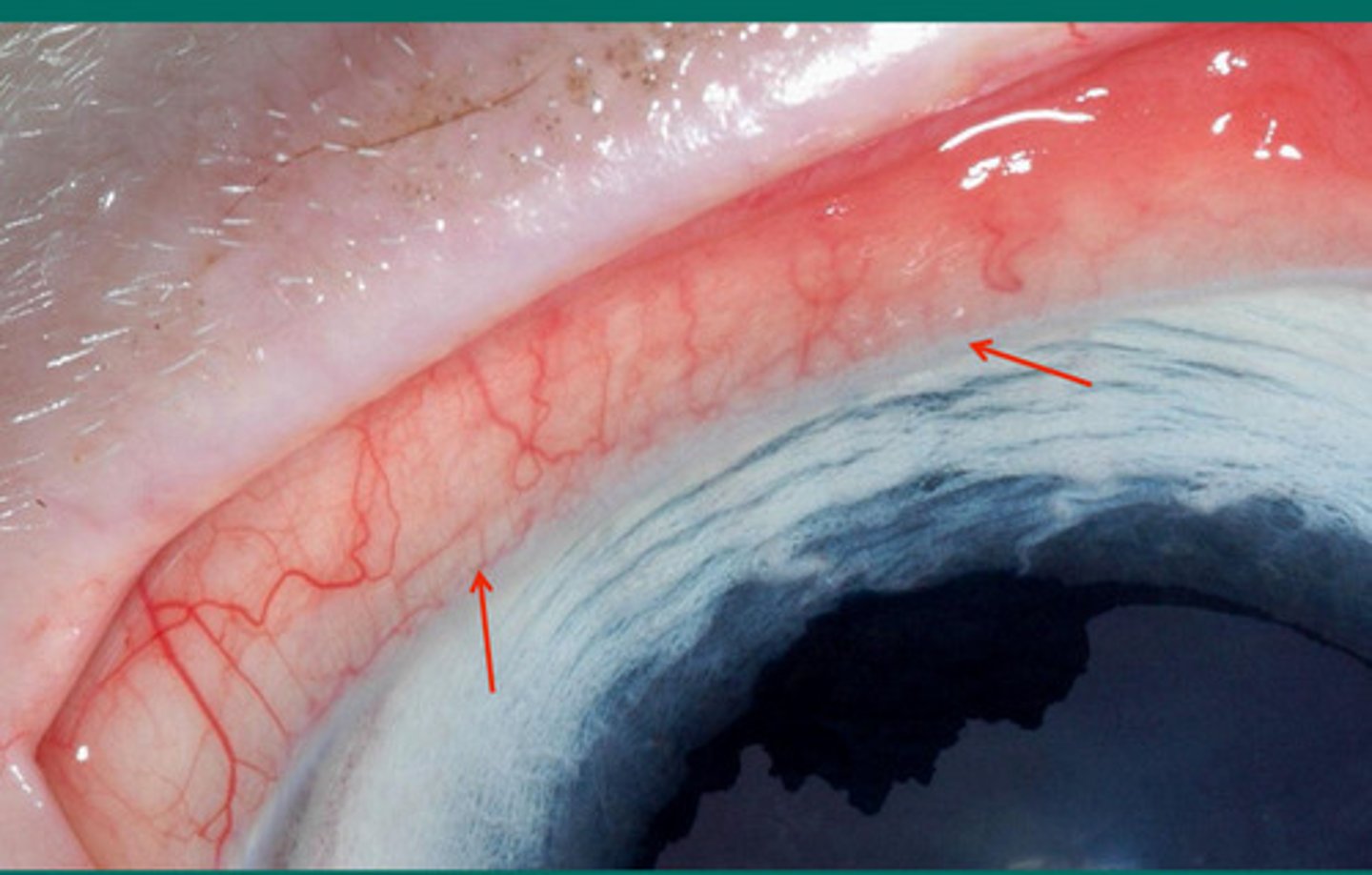
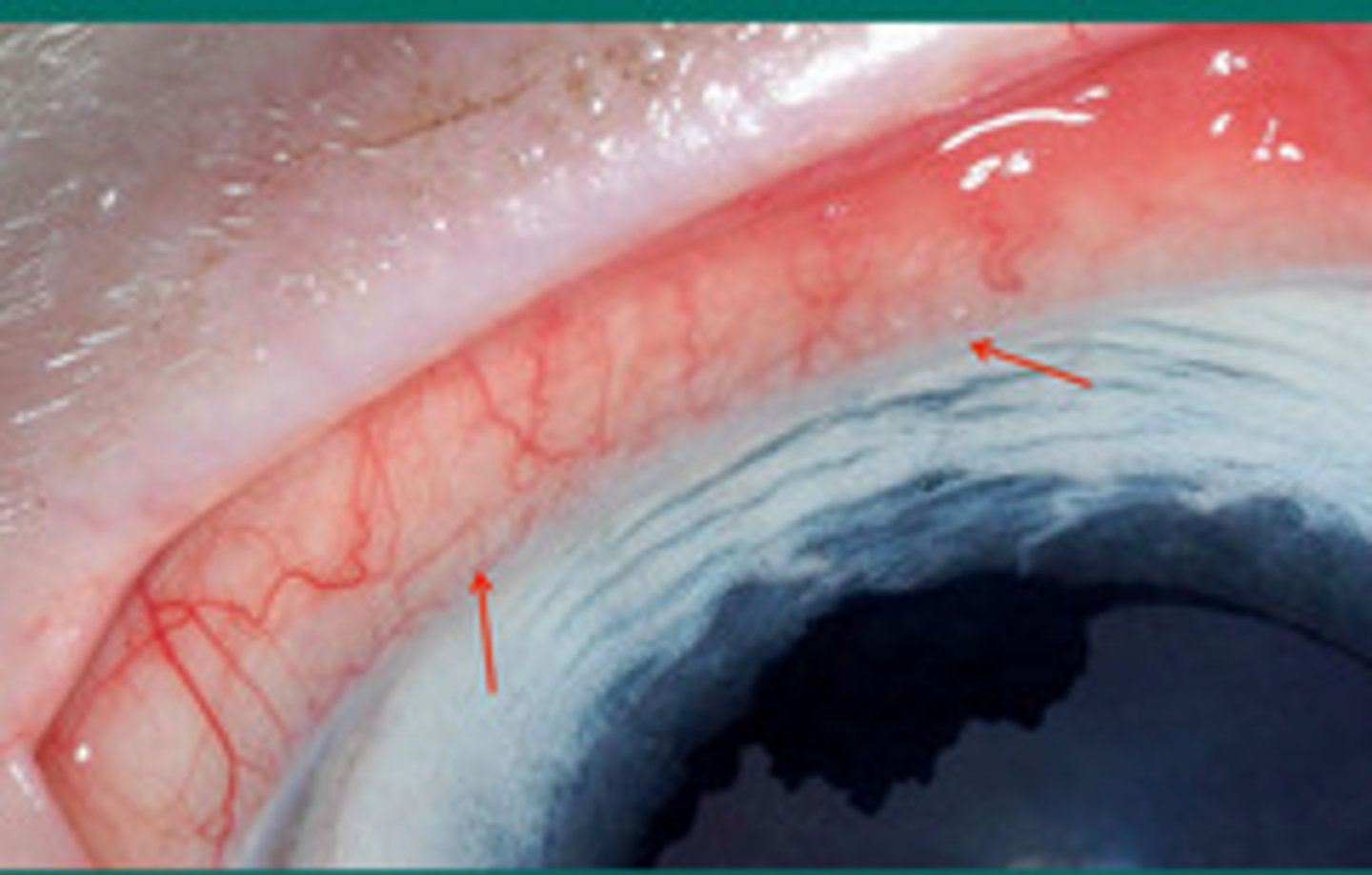
Limbal stem cells
What is the term for where the arrows are pointing?
Where the ulcer healing begins
What is the purpose of limbal stem cells?
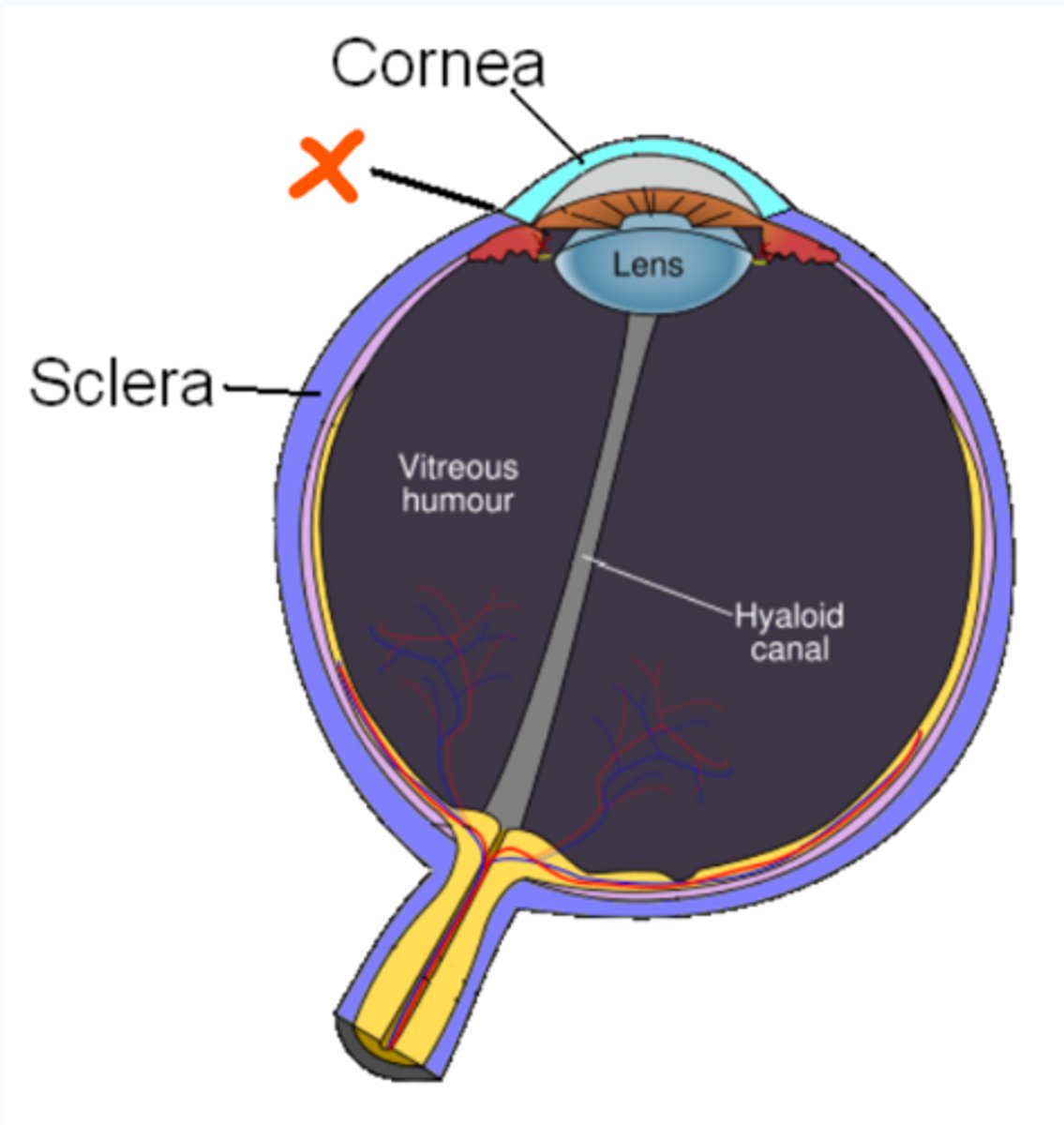
Limbus
What is the name of the line that divides the cornea and the sclera, at the X?
Corneal epithelium moves about 1 mm per day
5 mm = 5 days
The epithelium at the ulcer edge and the limbus moving across the ulcer to heal it is called corneal epithelial migration. How fast does this process move, and if there is a 5 mm diameter ulcer, this takes about how long to heal if it is a more superficial injury?
Both move at 1 mm per day
How fast does the epithelium move to facilitate corneal healing in horses? How about the vessels?
6 weeks
How long does it take for the epithelium of the cornea to attach the epithelial cell basement membrane to the stroma when healing corneal ulcers?
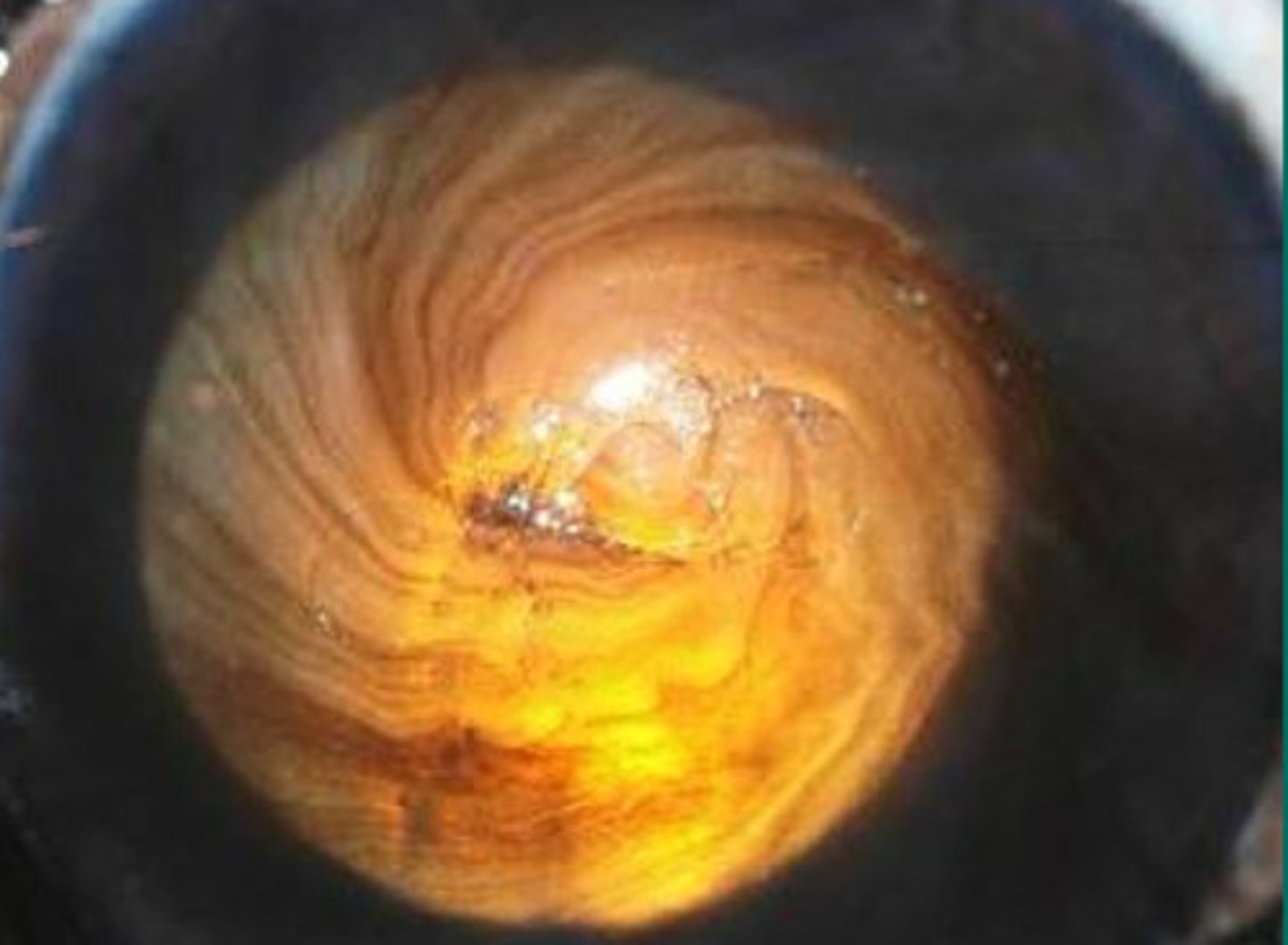
This "whorl" is the healing pattern of epithelial limbal cell movement
What does this pattern mean?
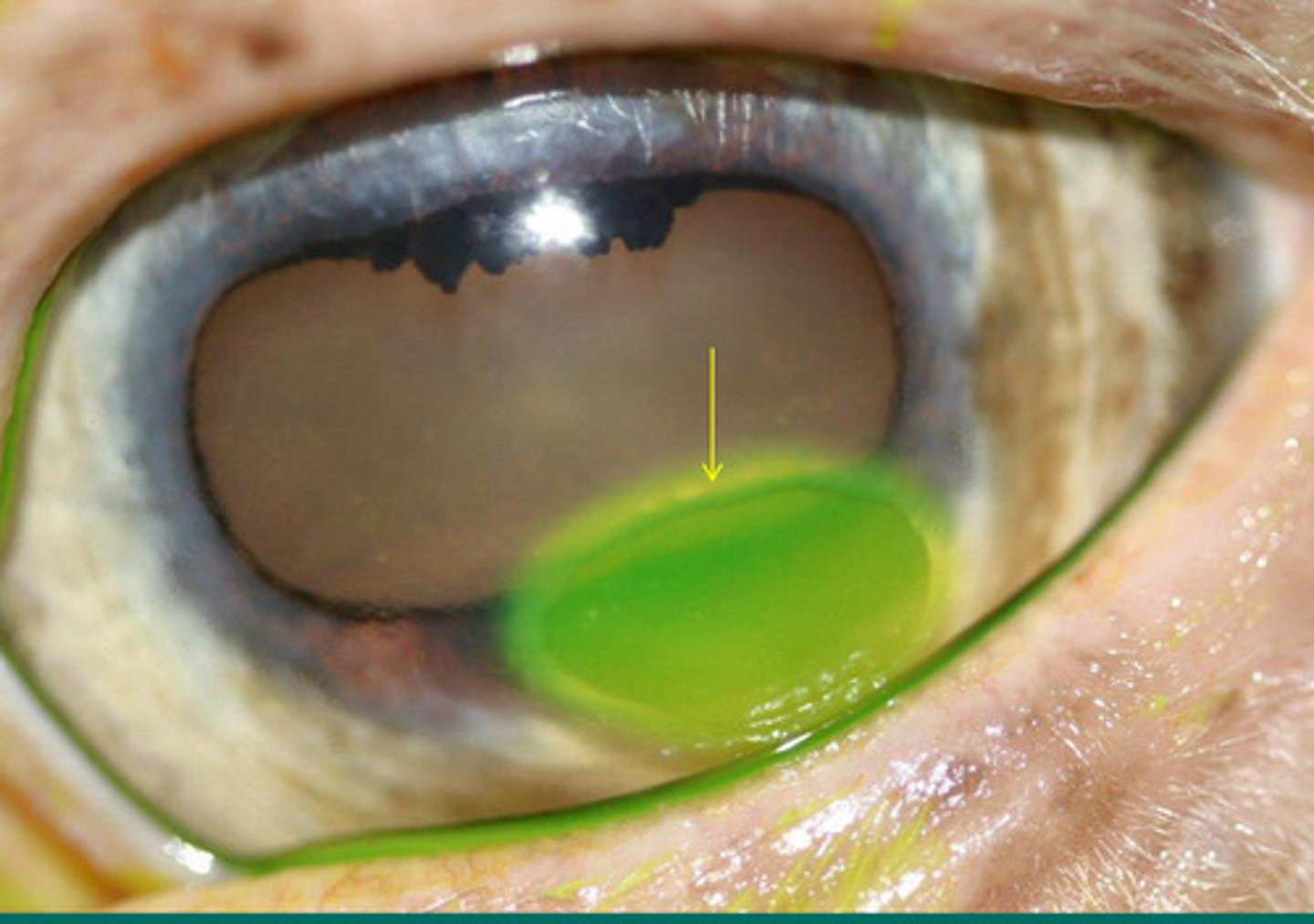
Since the tongue has not dissolved, it means there is little migration of epithelial limbal cell movement for healing
What does this appearance tell you about ulcer healing?
Top image = tongues = convex edge = very little migration of epithelial limbal cells for healing
Bottom image = rounded = concave edge = appropriate migration of epithelial limbal cells for healing
What do these two appearances tell you about ulcer healing?

Fibonacci sequence
What is the name of the pattern in which cells heal and grow in nature?
d. proteases increase in both eyes
note: these will decrease as the ulcer resolves
In which eye will proteases be elevated if the horse only has an ulcer in ONE eye?
a. proteases elevated in affected eye only
b. proteases elevated in unaffected eye only
c. proteases do not change
d. proteases increase in both eyes
The collagen in the stroma is starting to melt = corneal melting ulcer
Describe what you are seeing?
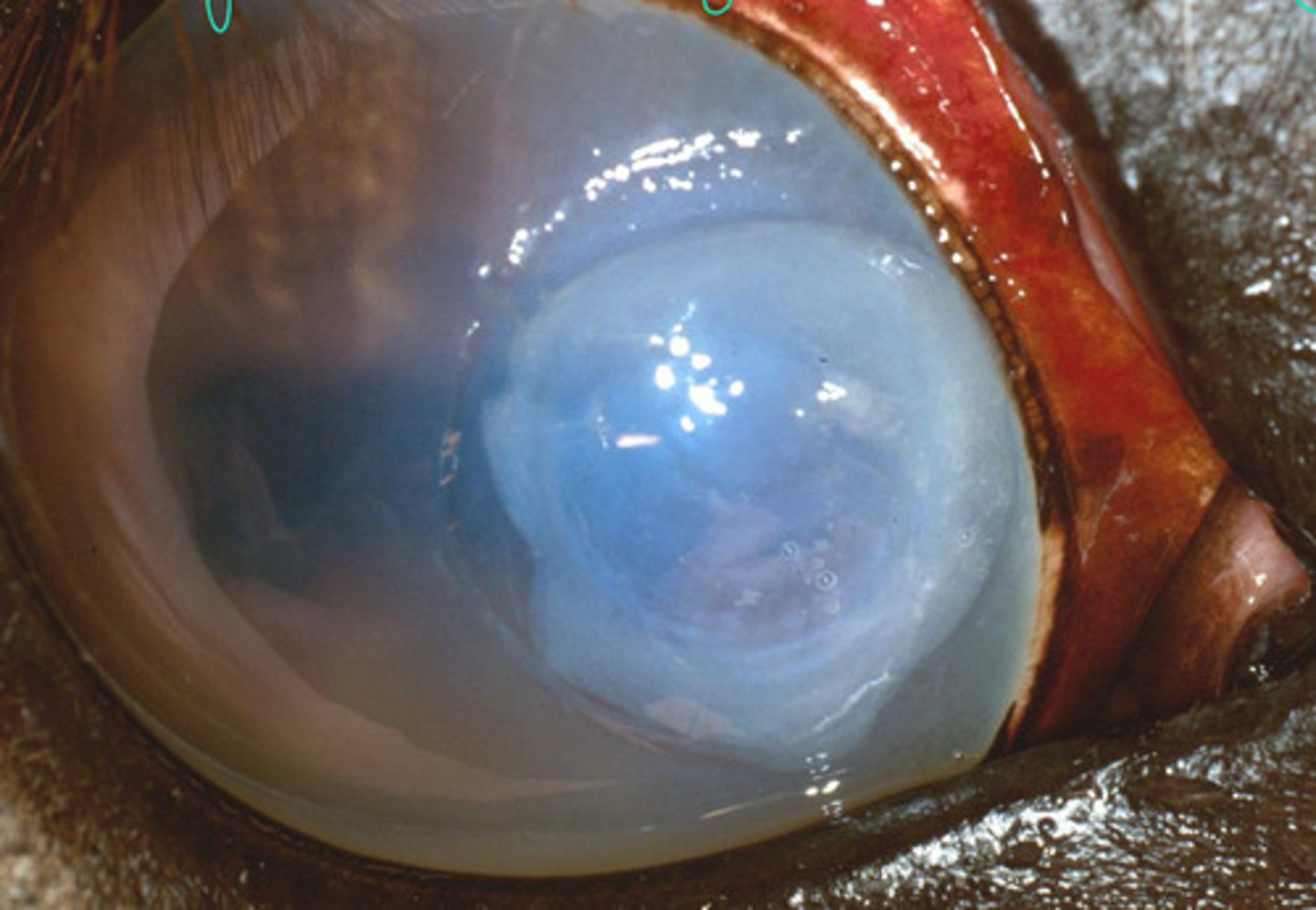
The collagen in the stroma (cornea) is melting as a result of proteases
What part of the stroma is sloughing off when corneal ulcers are "melting"?
The thickest layer of the cornea
What is the stroma of the cornea?
Anterior uveitis
EVERY horse with a corneal ulcer has WHAT?
inflammation of the iris and ciliary body
note: meaning that the inflammation is not just on the surface (the cornea) but has affected the internal vascular structures of the eye (iris and ciliary body)
What is anterior uveitis?
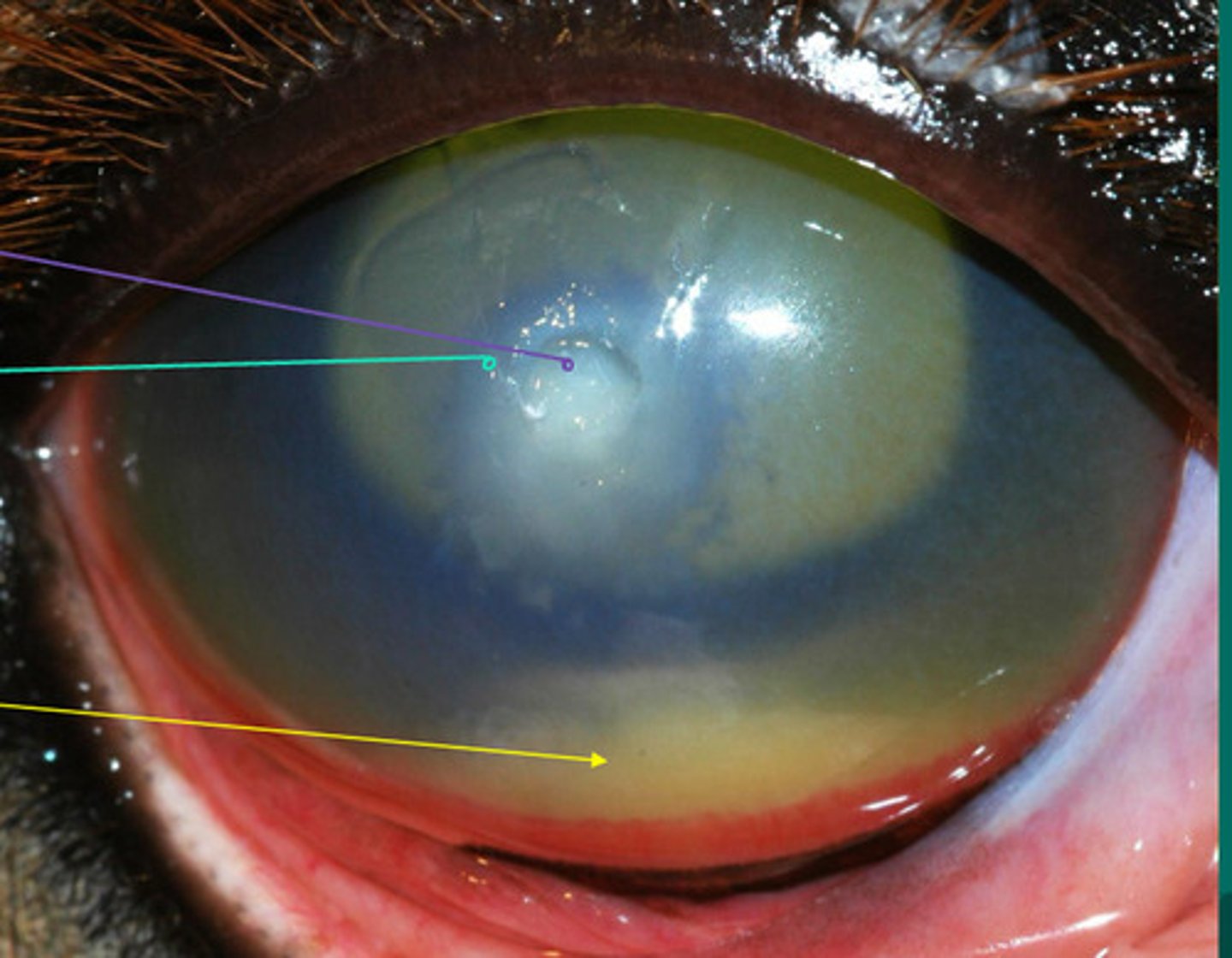
Purple: white in eye = a more superficial defect
Green: grey in eye = a deeper defect in the cornea
Yellow: hypopyon inside the anterior chamber
What are the different arrows pointing to?
1. sterilize the ulcer surface (get rid of infection)
2. inhibit tear film protease activity
3. reduce corneal edema
4. minimize uveitis
5. control corneal fibrosis
6. replace missing collagen
Name the 6 things you do to manage corneal ulcers in horses?
Conjunctival ulcer --> same as a corneal ulcer
What is happening here? How do you treat?
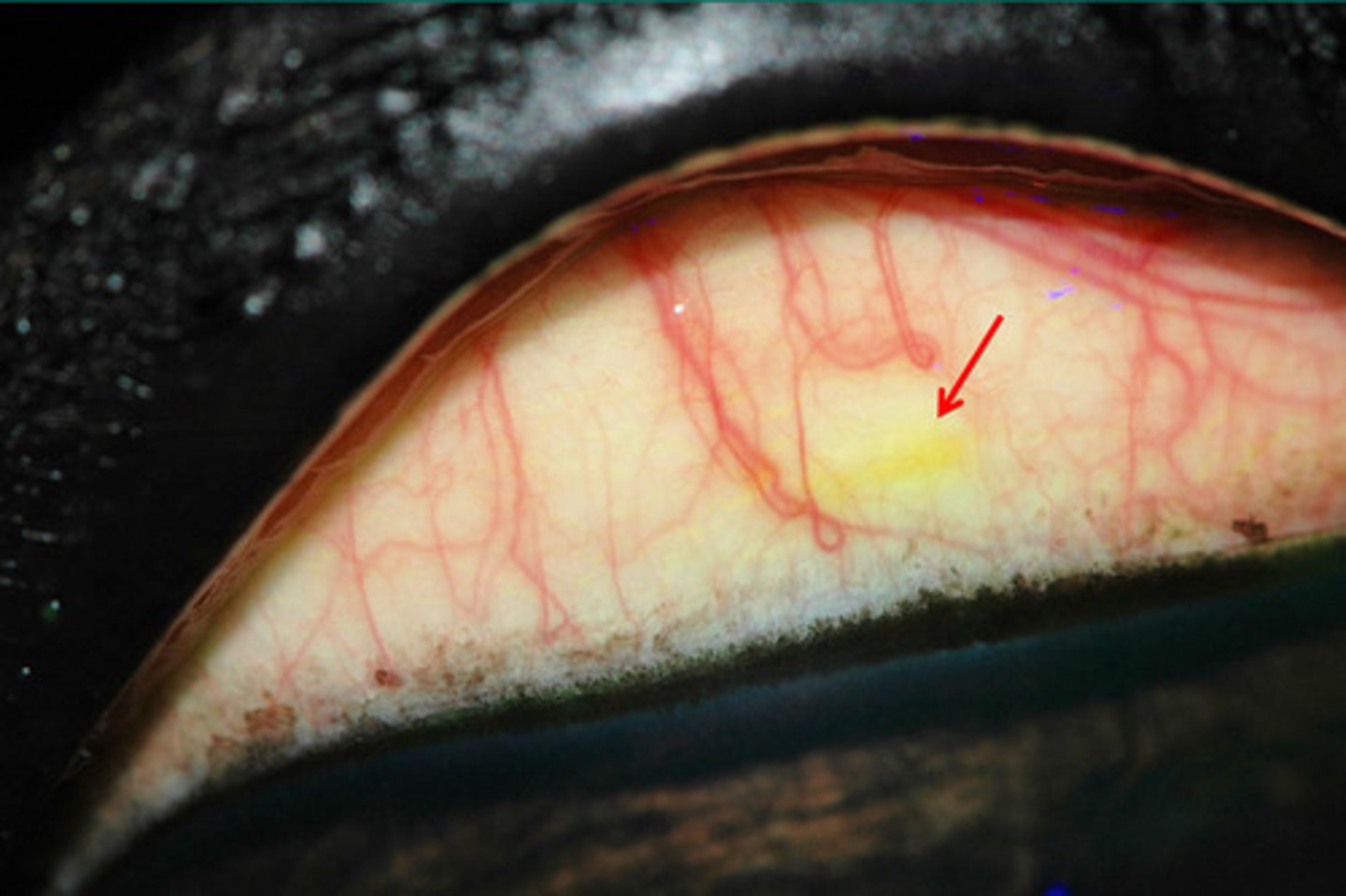
Edges are smooth = healing well = as long as it continues to heal, no need to debride
Describe the edges of this lesion and what this means for debridement
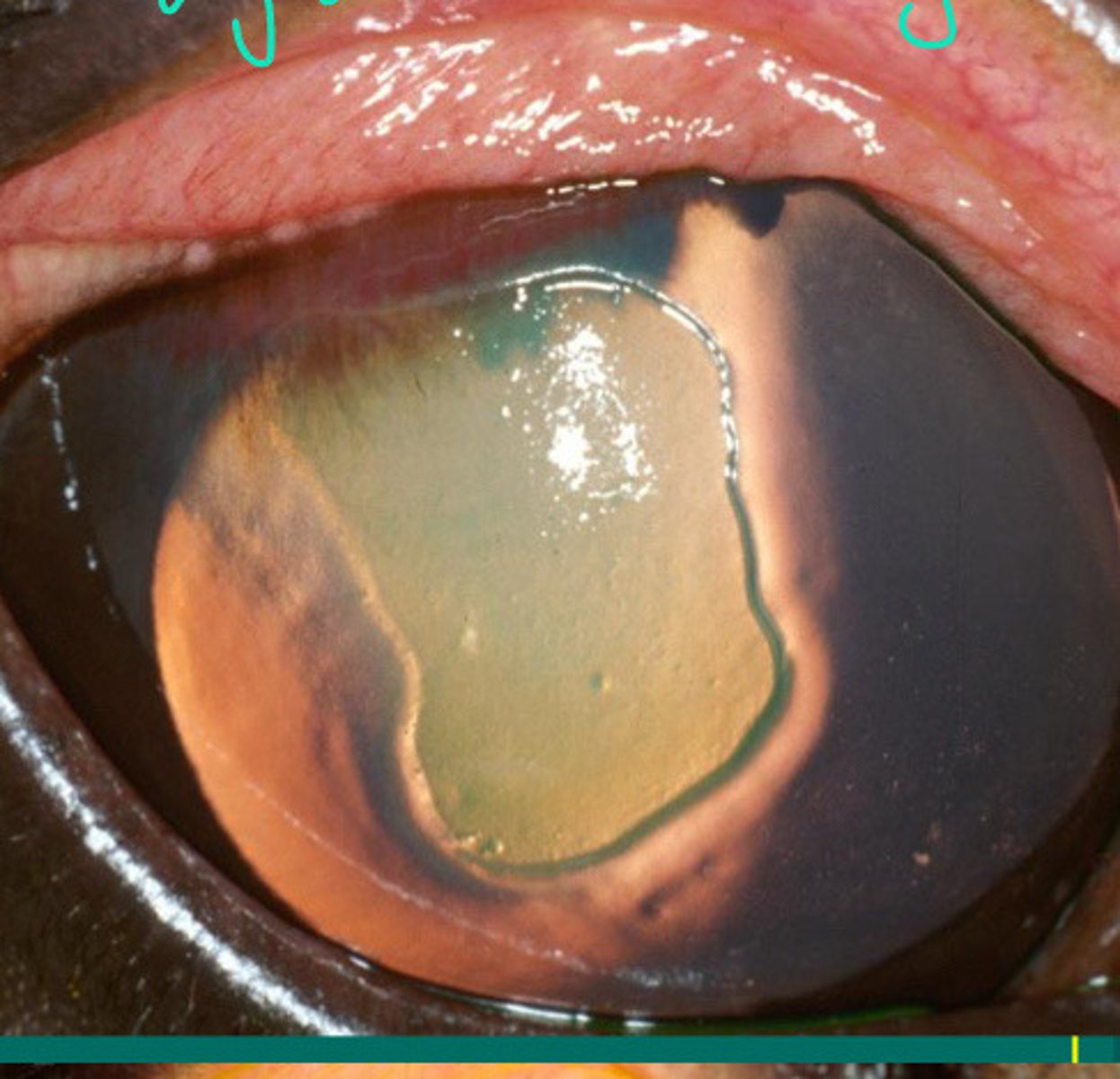
Edges are rough. If this has not moved in 6 weeks --> debridement
Describe the edges of this lesion and what this means for debridement
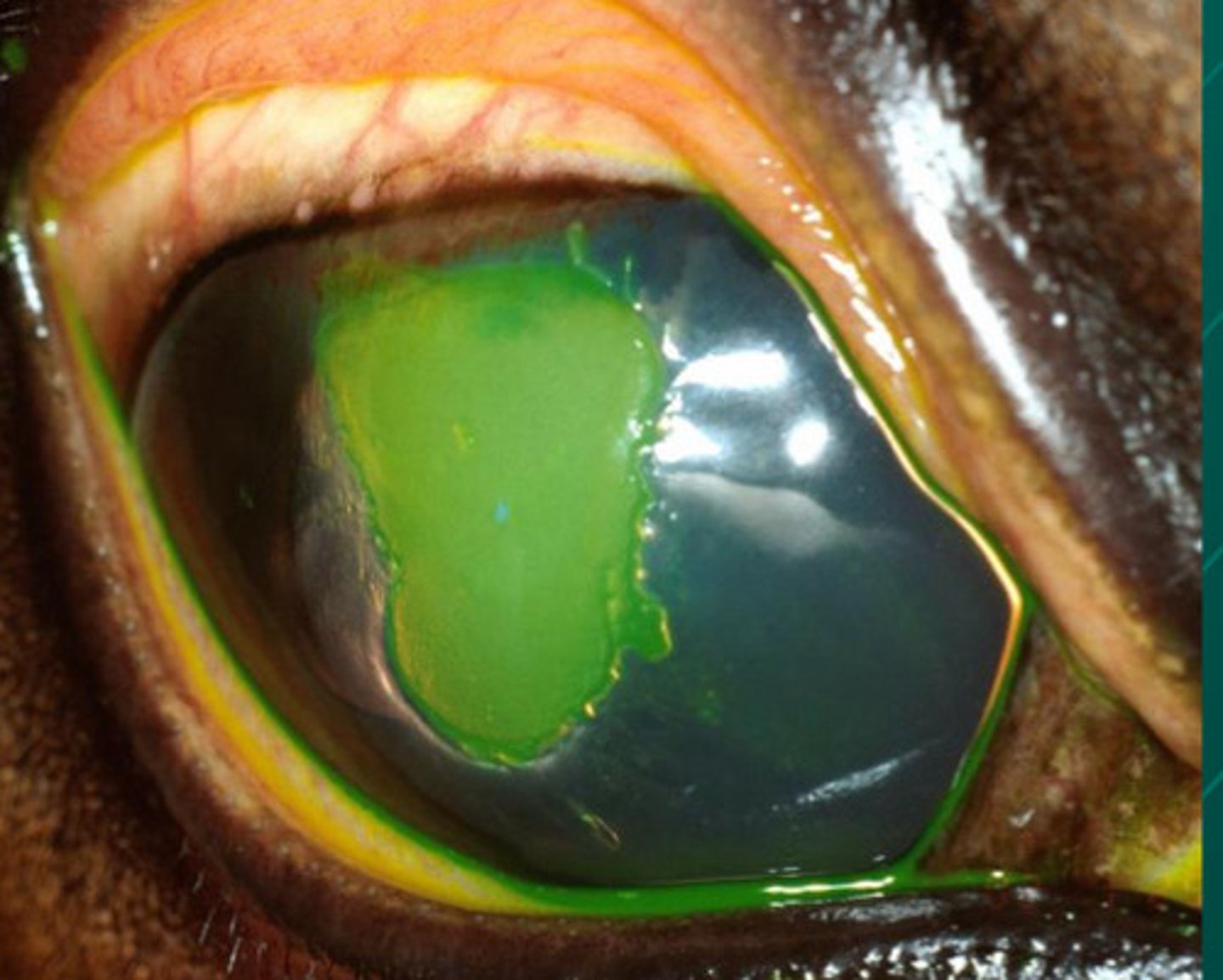
6 weeks
At what point in time should you consider a corneal ulcer "nonhealing", so you likely do debridement?
Triple antibiotic, antifungal, EDTA (antiprotease), systemic flunixin, atropine, debride if not healing more than 6 weeks
Name some medications you can use for superficial ulcer treatment with minimal corneal tissue loss?
If you suspect fungal infection is causing the issue, especially common with melting ulcers
Why do you typically tend to use antifungals if there are ulcers in the horse eye?
Antifungals
Miconazole, amphotericin, natamycin, and voriconzole are all examples of WHAT type of medication used in horses with ulcers?
Debride
This ulcer has been healing for 8 weeks and there is loose epithelium. What should you do?
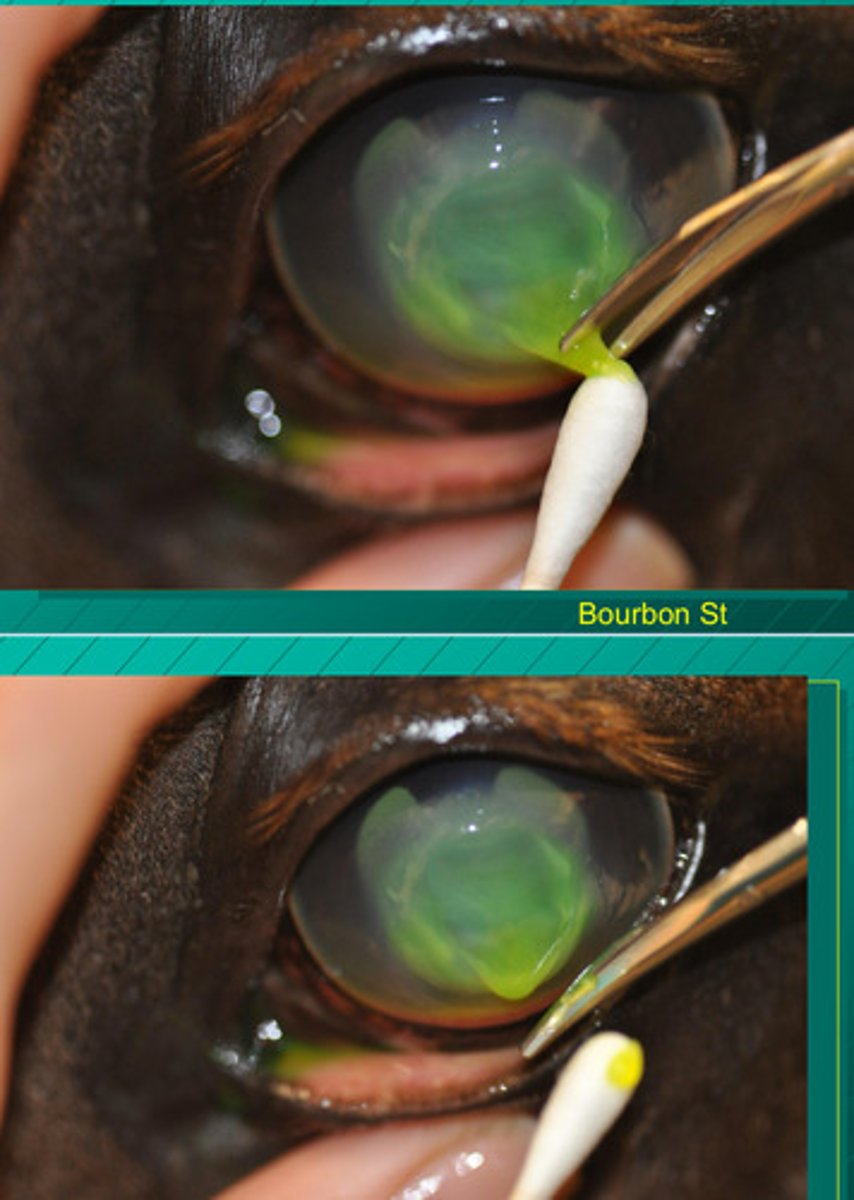
Cotton swab, algerbrush II burr with 3.5 mm burr
What tools can you use for debridement in horses of nonhealing ulcers?
Melting ulcer --> need keratectomy
Describe this ulcer and talk about what you can do to fix it?
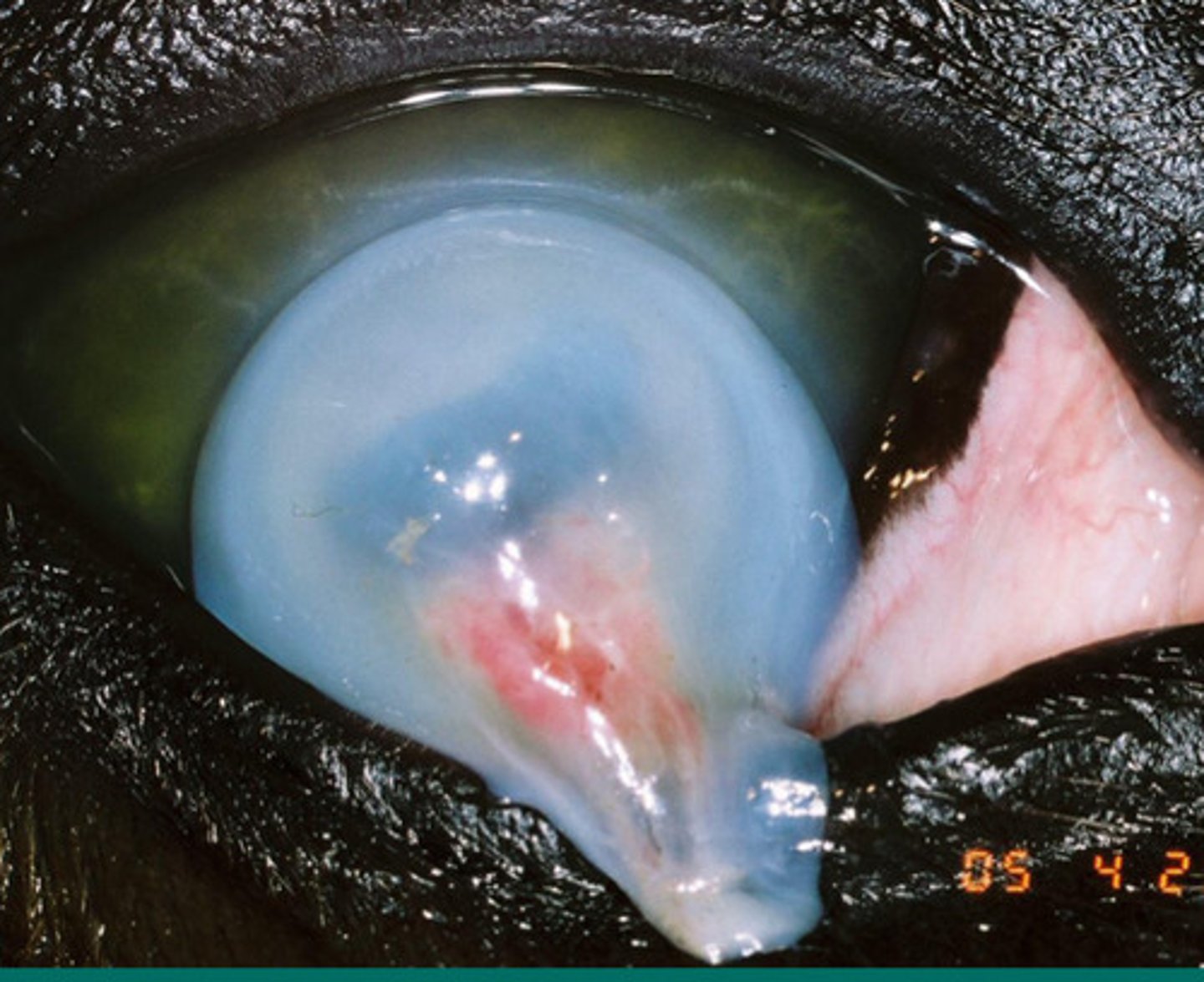
Keratectomy to fix melting ulcers
What is the term for this procedure?
Desmetocele --> eye is near rupture
Describe this eye issue and what it implies is going to happen next to this eye if untreated?

"Grooves" in the ulcer
What is the term for this ulcer appearance where there is thinning at the periphery and progressive, often a precursor to desmetocele?
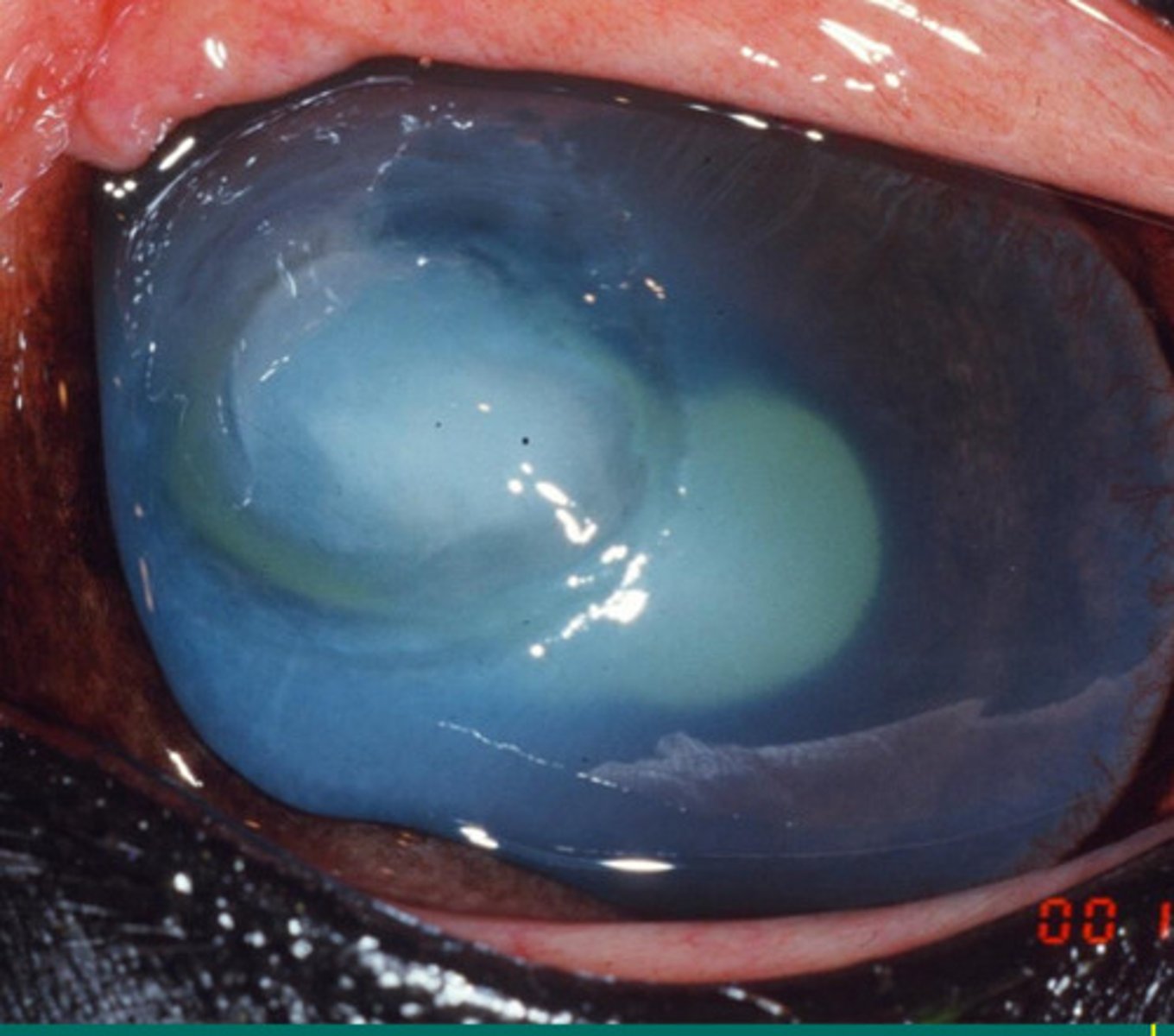
Desmetocele
What is happening here?
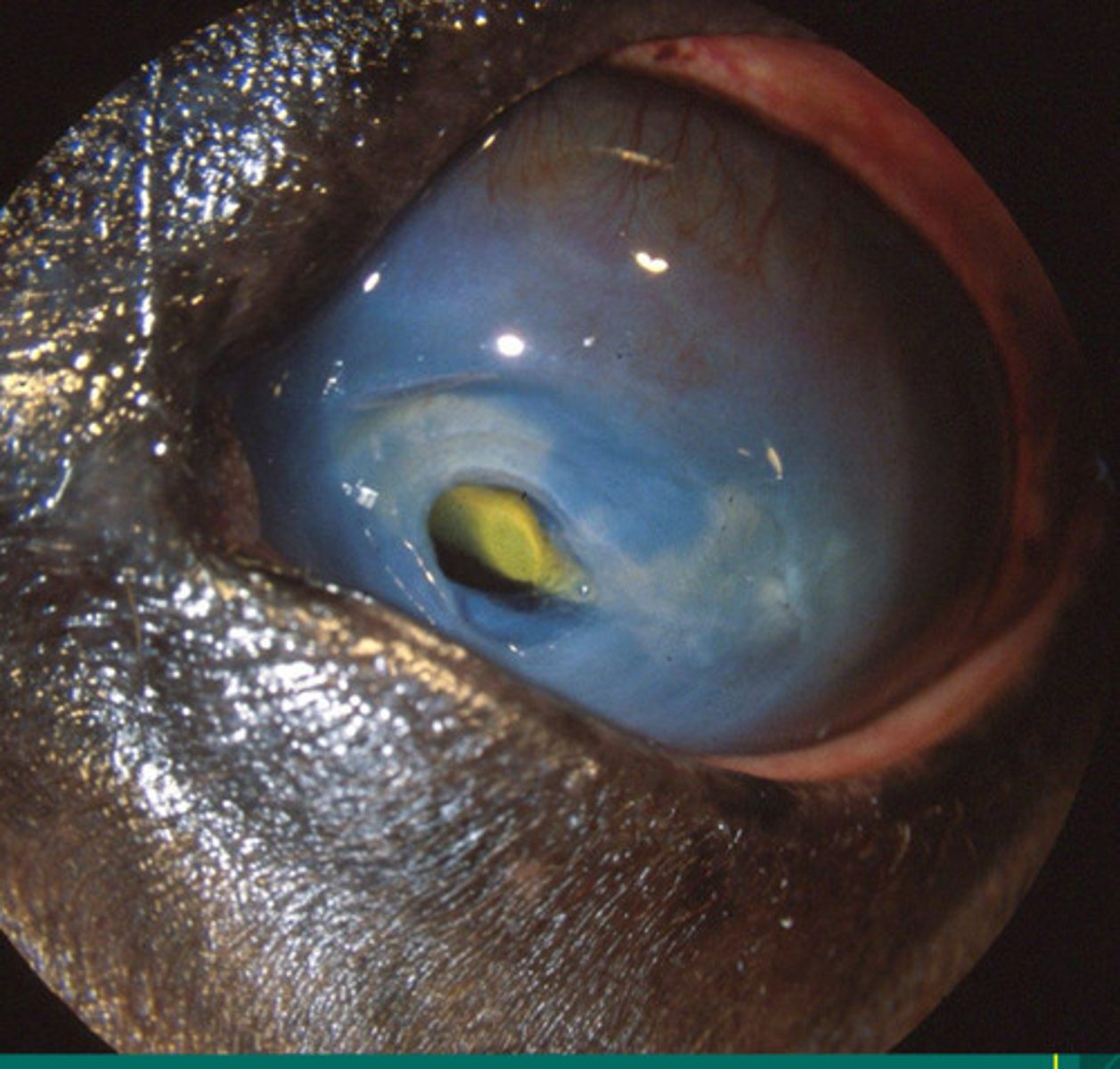
Deep ulcers, desmetoceles and perforated ulcers
The following surgeries are all indicated for treatment of WHAT TYPE of eye issue?
Conjunctival flap surgery
Amniotic membrane transplant
Penetrating keratoplasty
Lamellar keratoplasty
Antibiotics (tobramycin or cefazolin), voriconazole (antifungal), atropine to dilate pupil, serum OR EDTA (not both, antiproteases). Flunixin. Keratotomy if indicated
Name some medications used to treat deep, melting, or fungal ulcers?
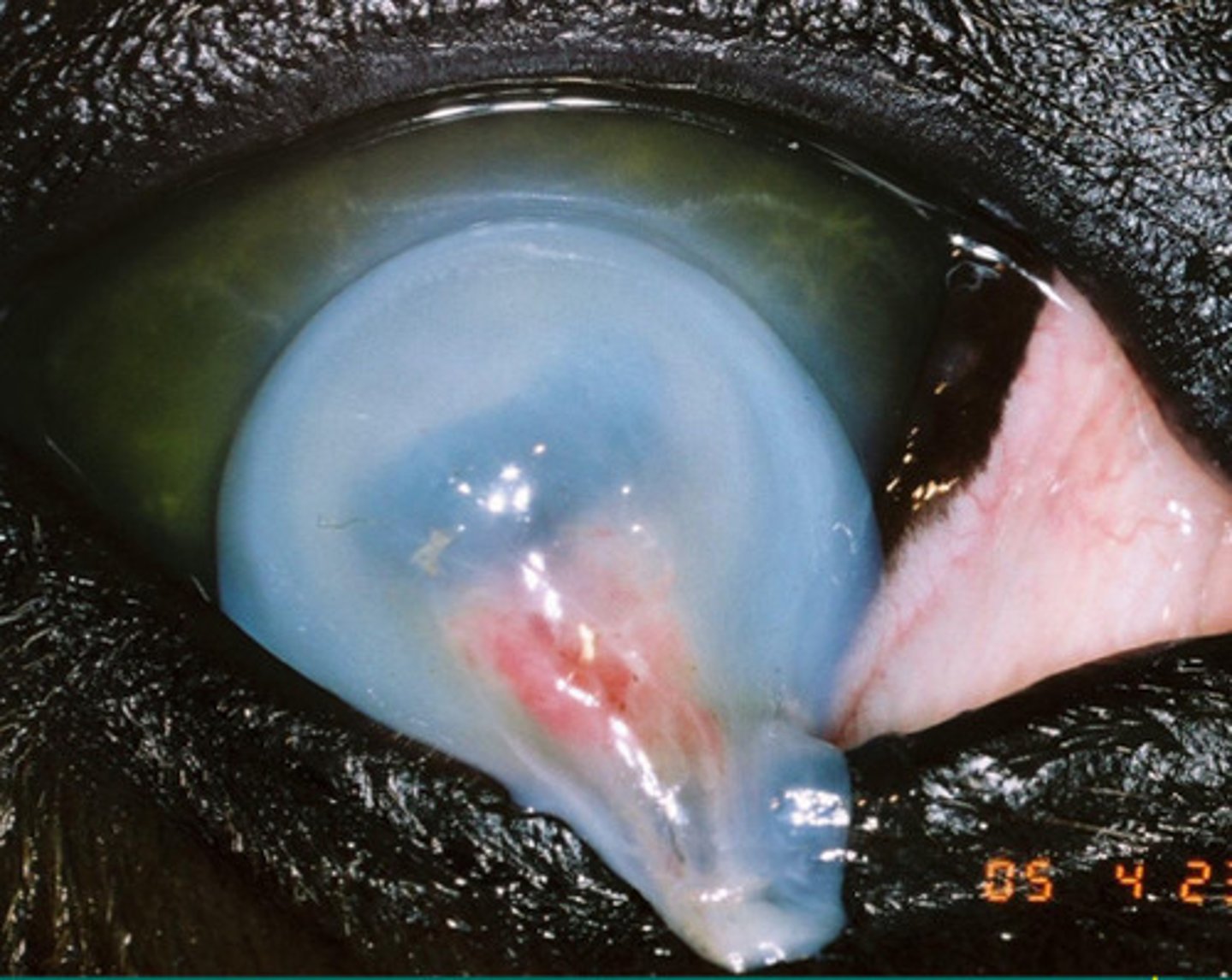
Pseudomonas (gram negative)
Tobramycin or ciprofloxacin are medications used to treat WHAT BACTERIA if it is involved in causing deep or melting ulcers?
beta Streptococcus (gram positive)
Cefazolin is medication used to treat WHAT BACTERIA if it is involved in causing deep or melting ulcers?
Iris prolapse
What is happening here after the cornea has ruptured?
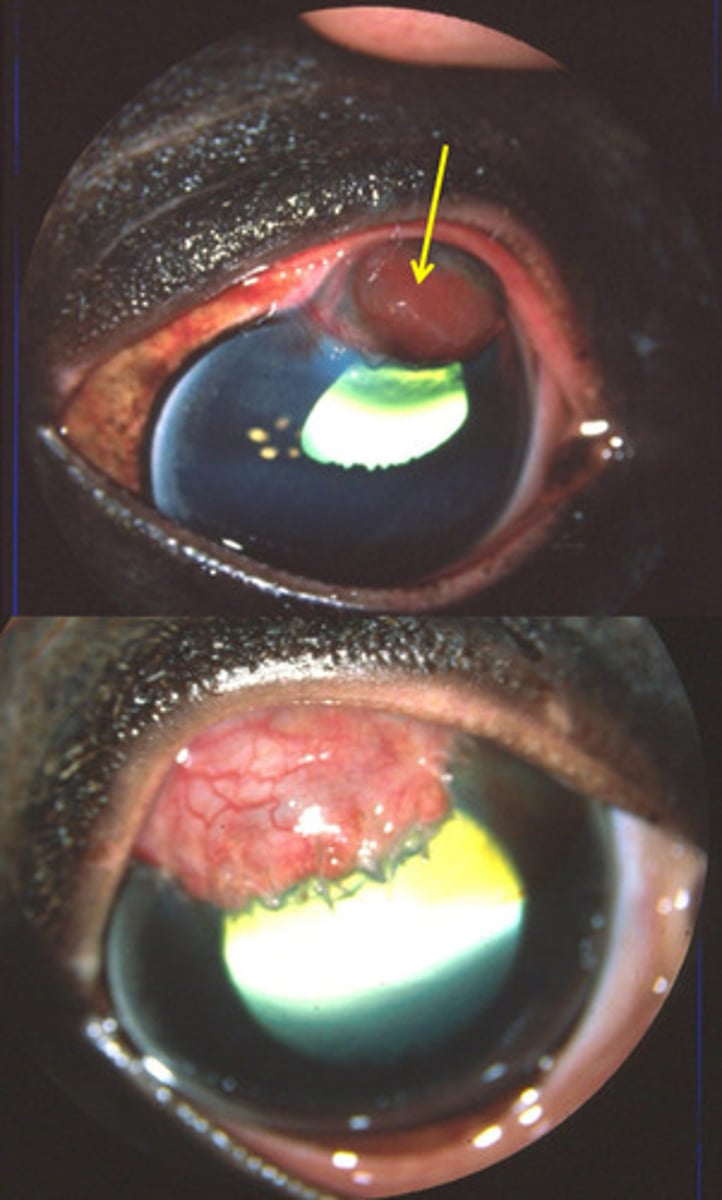
Dilate the pupil, helps with eye pain, makes capillaries in the iris stronger
What 3 things does atropine do to benefit eyes?
1. immune mediated epithelial keratitis
2. chronic superficial stromal immune mediated keratitis
3. chronic RECURRENT DEEP stromal immune mediated keratitis
4. eosinophilic keratitis
5. immune mediated endothelitis
Name the nonulcerative keratopathies that commonly affect horses (5):
a. immune mediated epithelial keratitis
What is the name of this unilateral disease, where horses have slight ocular discomfort and a rough surface of the eye resulting in faint fluorescein stain pattern but no corneal vascularization going on:
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
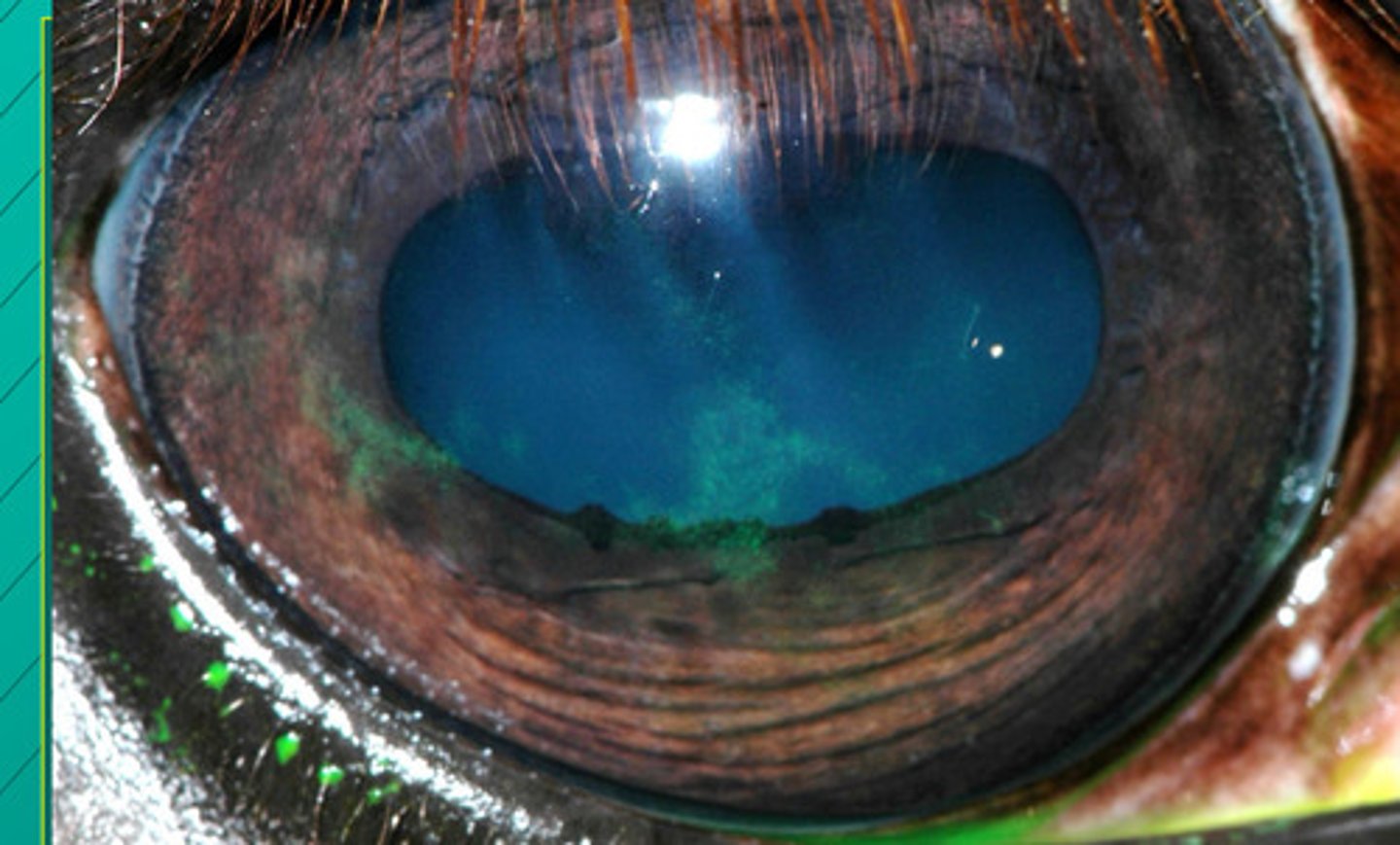
Diclofenac (NSAID) and cyclosporine (immunomodulator)
Immune mediated epithelial keratitis is cureable. Name the 2 treatments
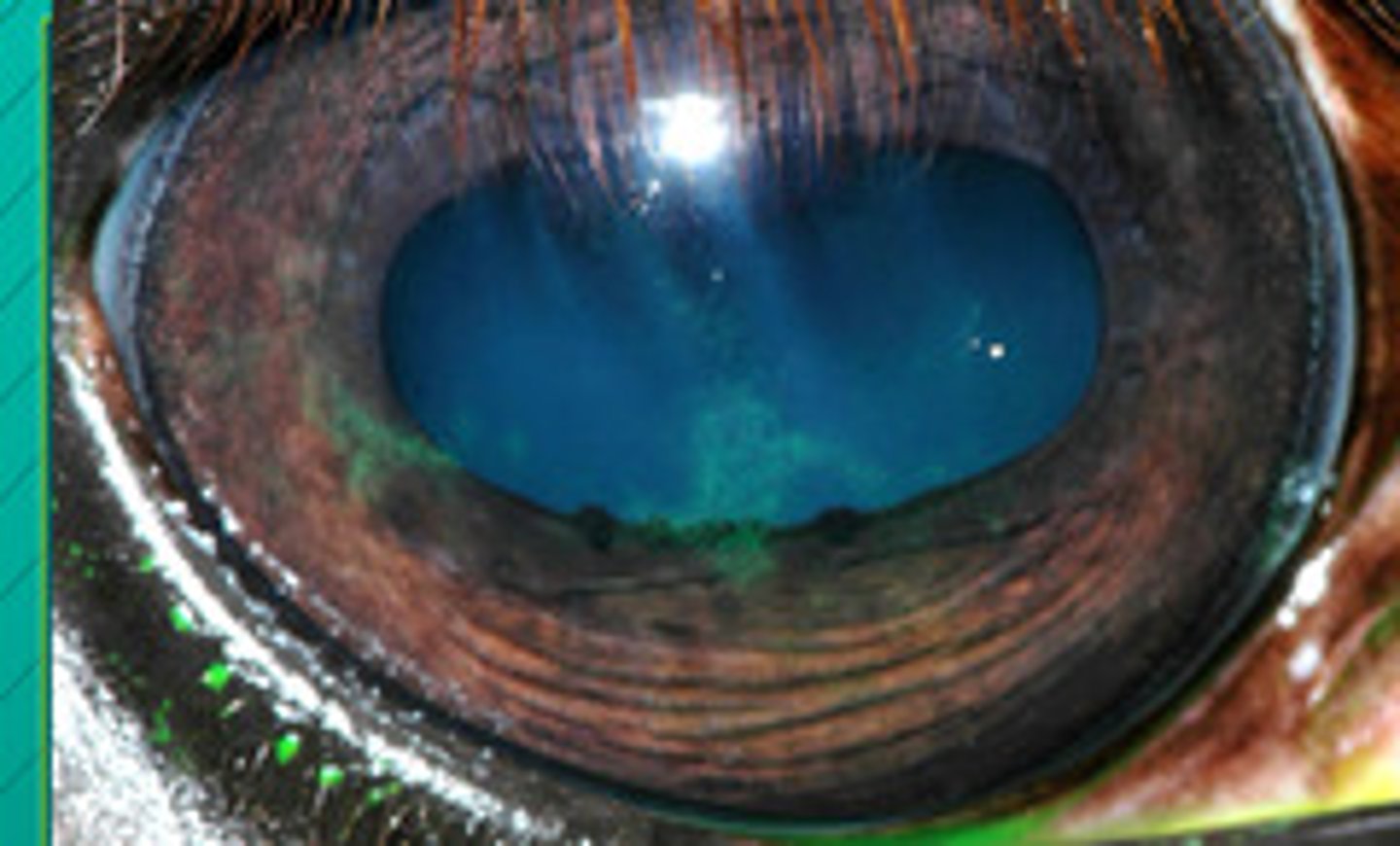
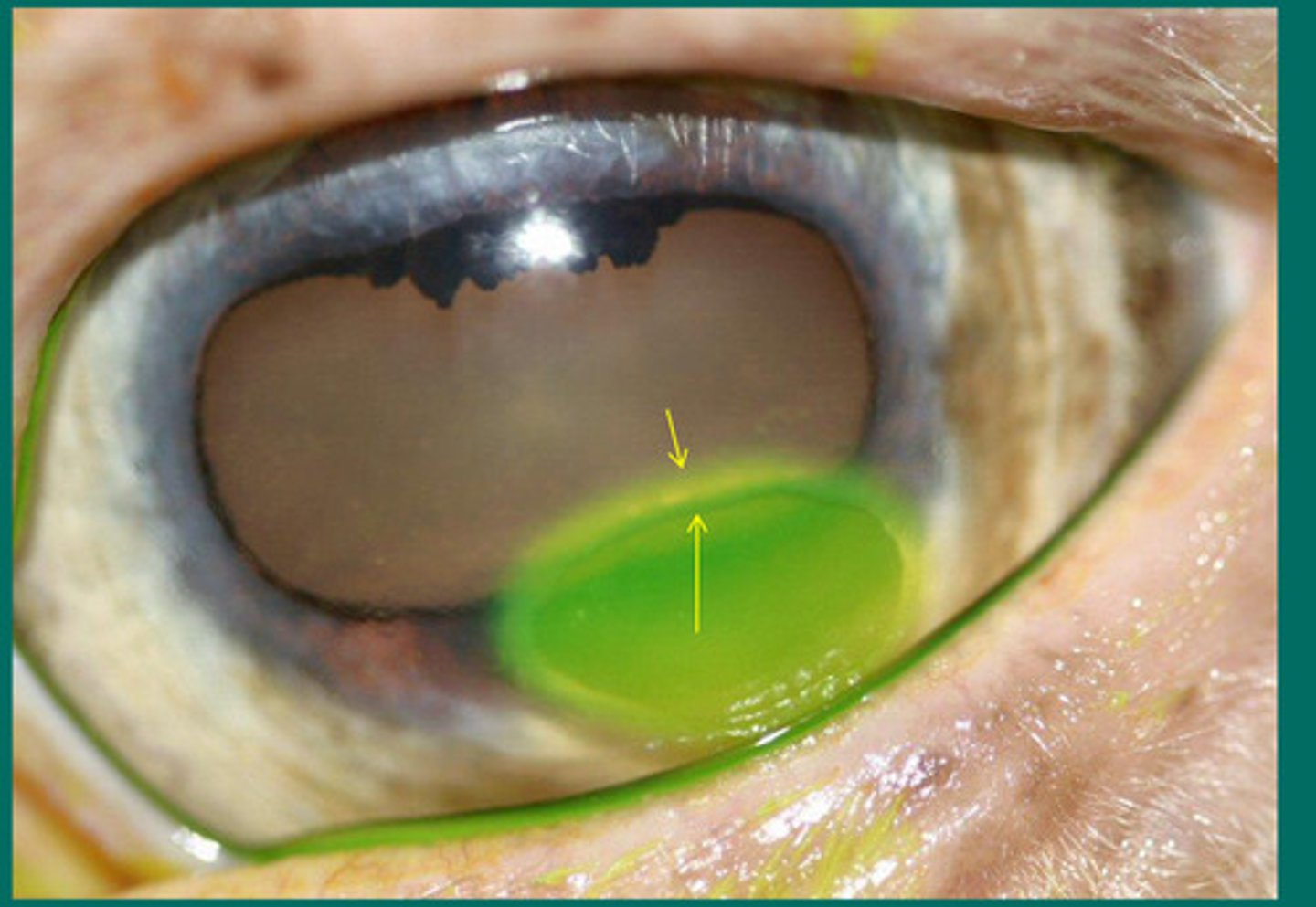
b. chronic SUPERFICAL stromal immune mediated keratitis
What is name of this prominent superficial vascularization causing epithelial edema and lesions under the upper eyelid but NOT ulcerated?
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
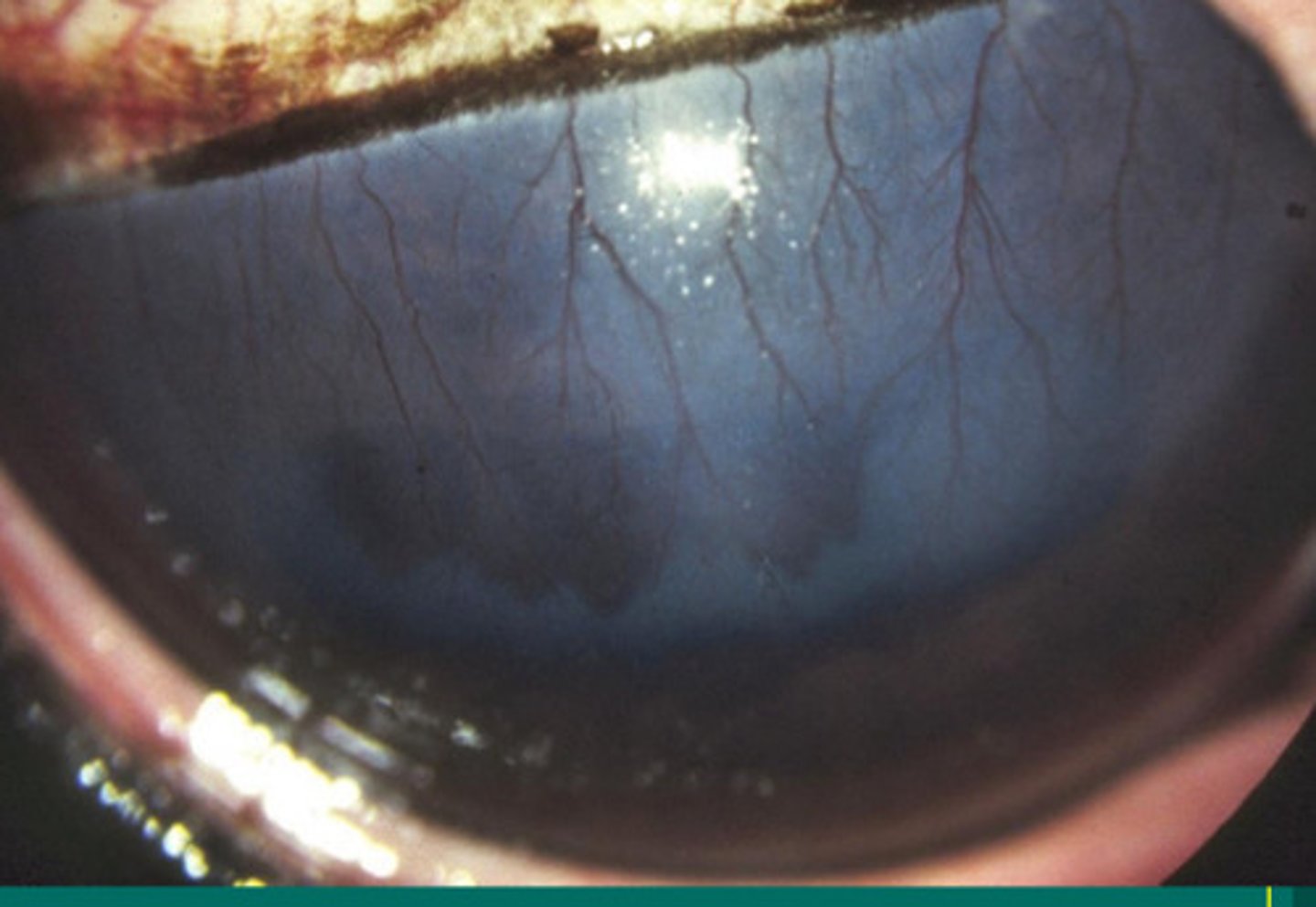
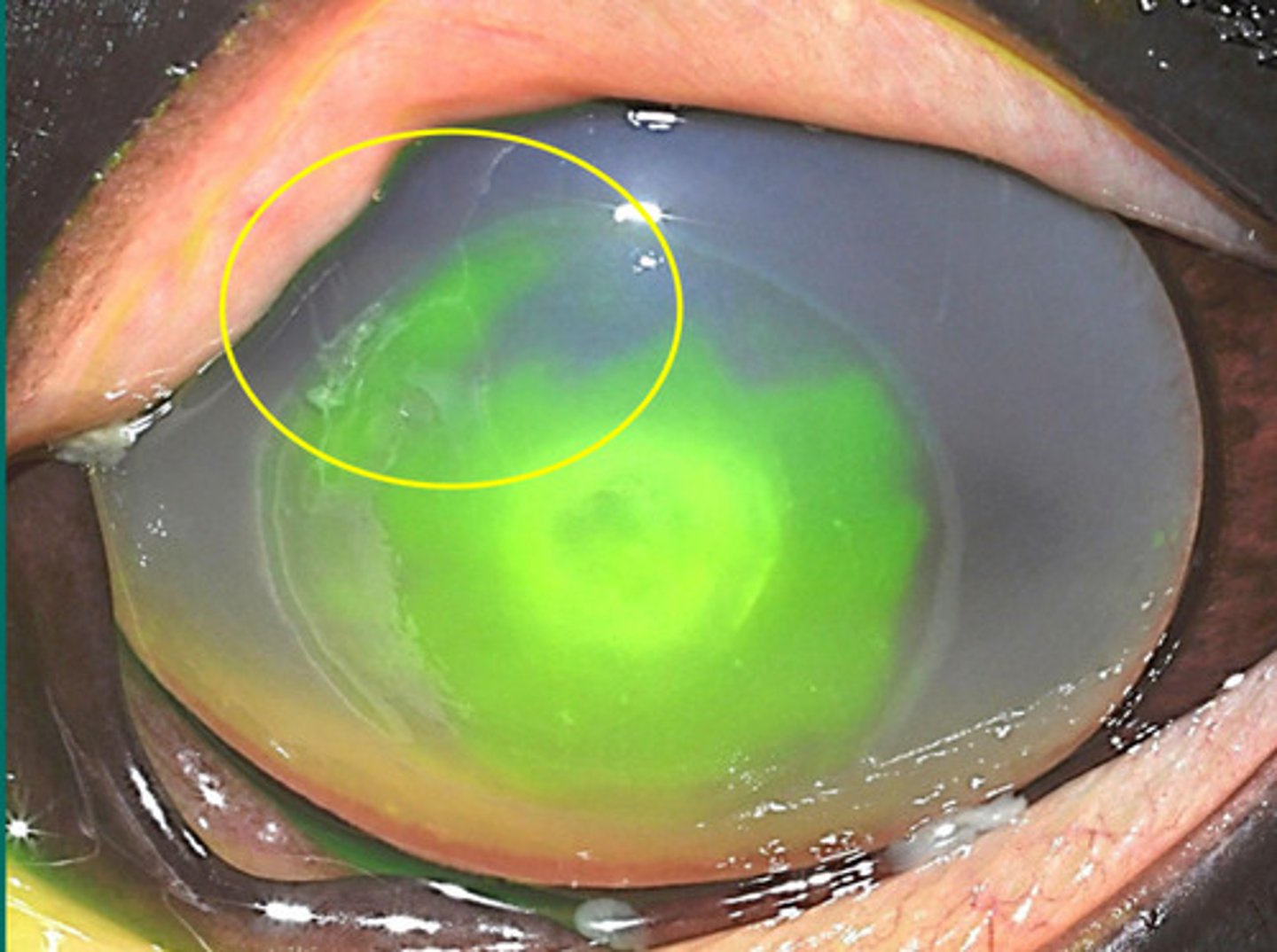
c. chronic RECURRENT DEEP stromal immune mediated keratitis
What is the name of this deep fibrovascular reactivity and edema, where depth is indicated by green fluid filling up the stroma and capillary leakage:
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
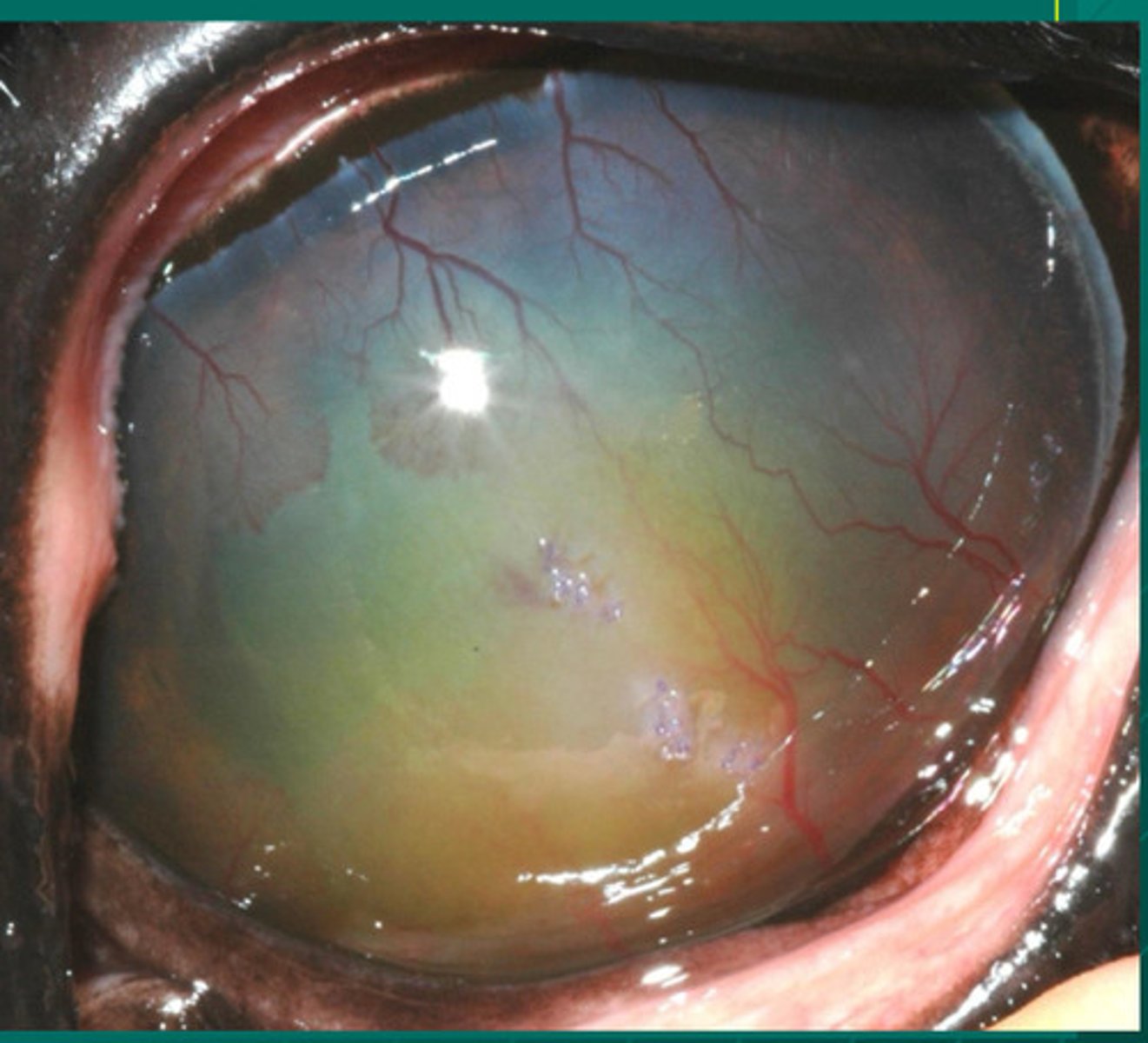
c. chronic RECURRENT DEEP stromal immune mediated keratitis
What is happening in this eye, where plasma staining is evident?
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
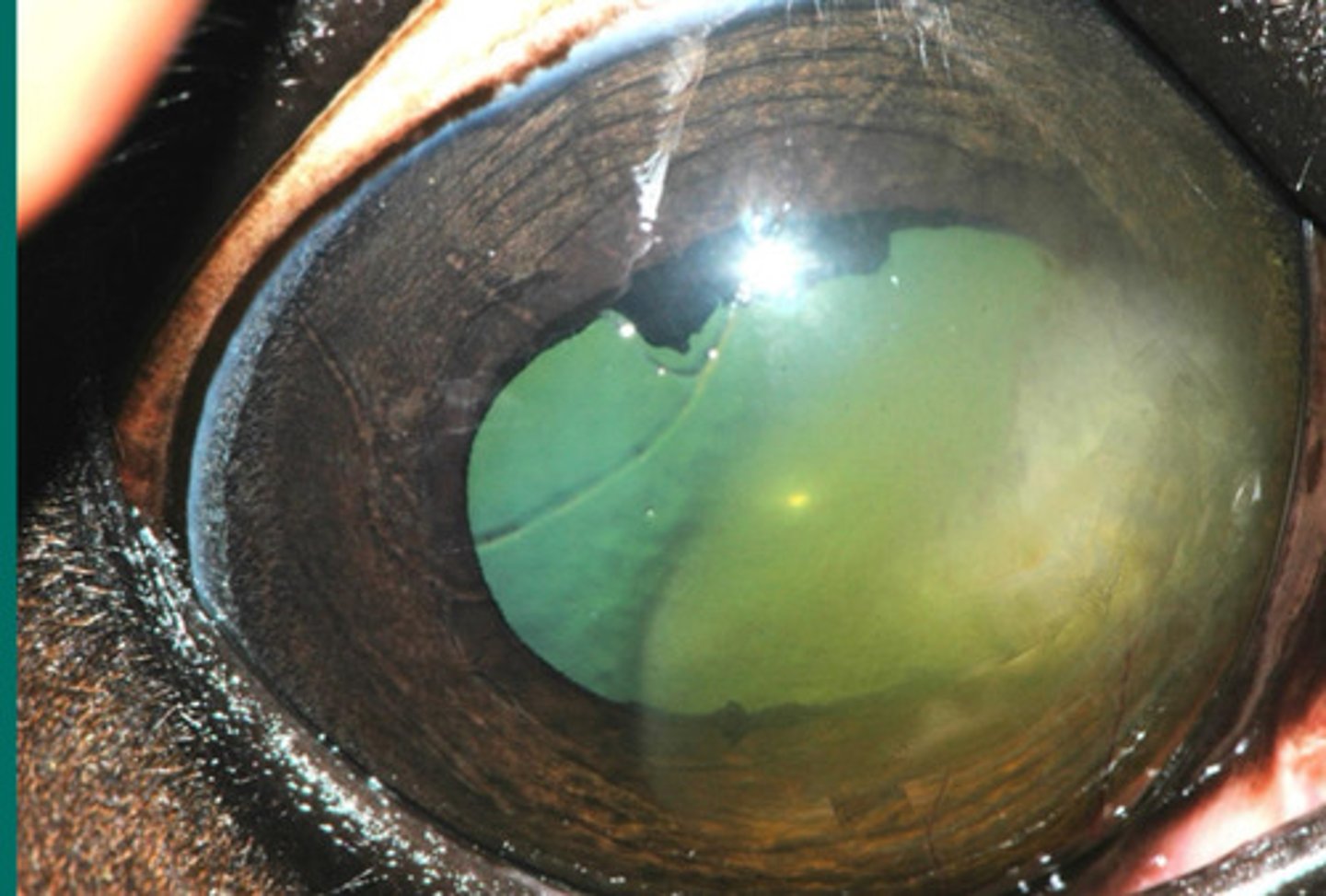
d. eosinophilic keratitis
What is happening in this eye, where there are raised limbal lesions resembling tumors which have sulfur type granules (yellow) visible?
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
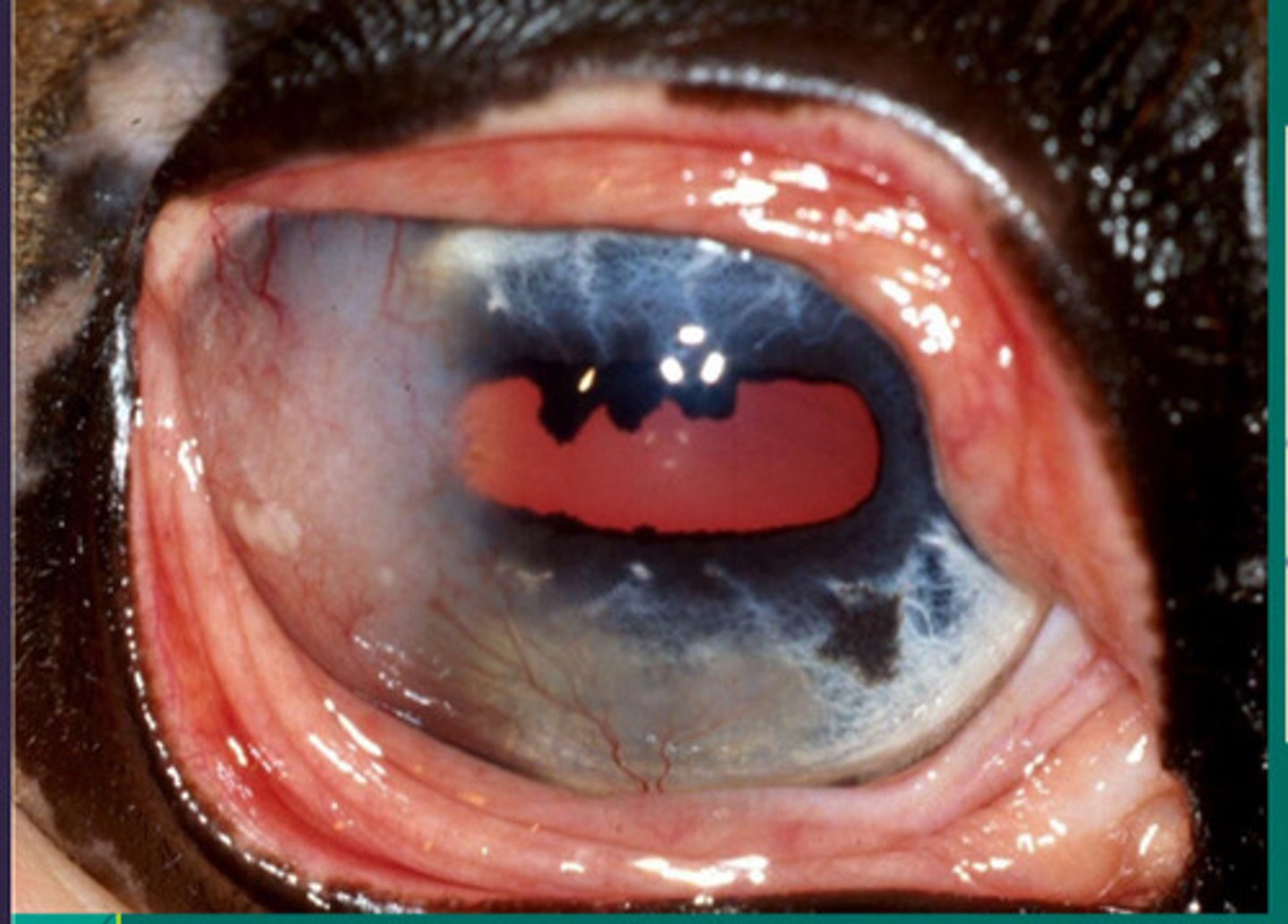
d. eosinophilic keratitis
What is happening in this eye, where there are raised limbal lesions resembling tumors which have sulfur type granules (yellow) visible?
a. immune mediated epithelial keratitis
b. chronic SUPERFICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
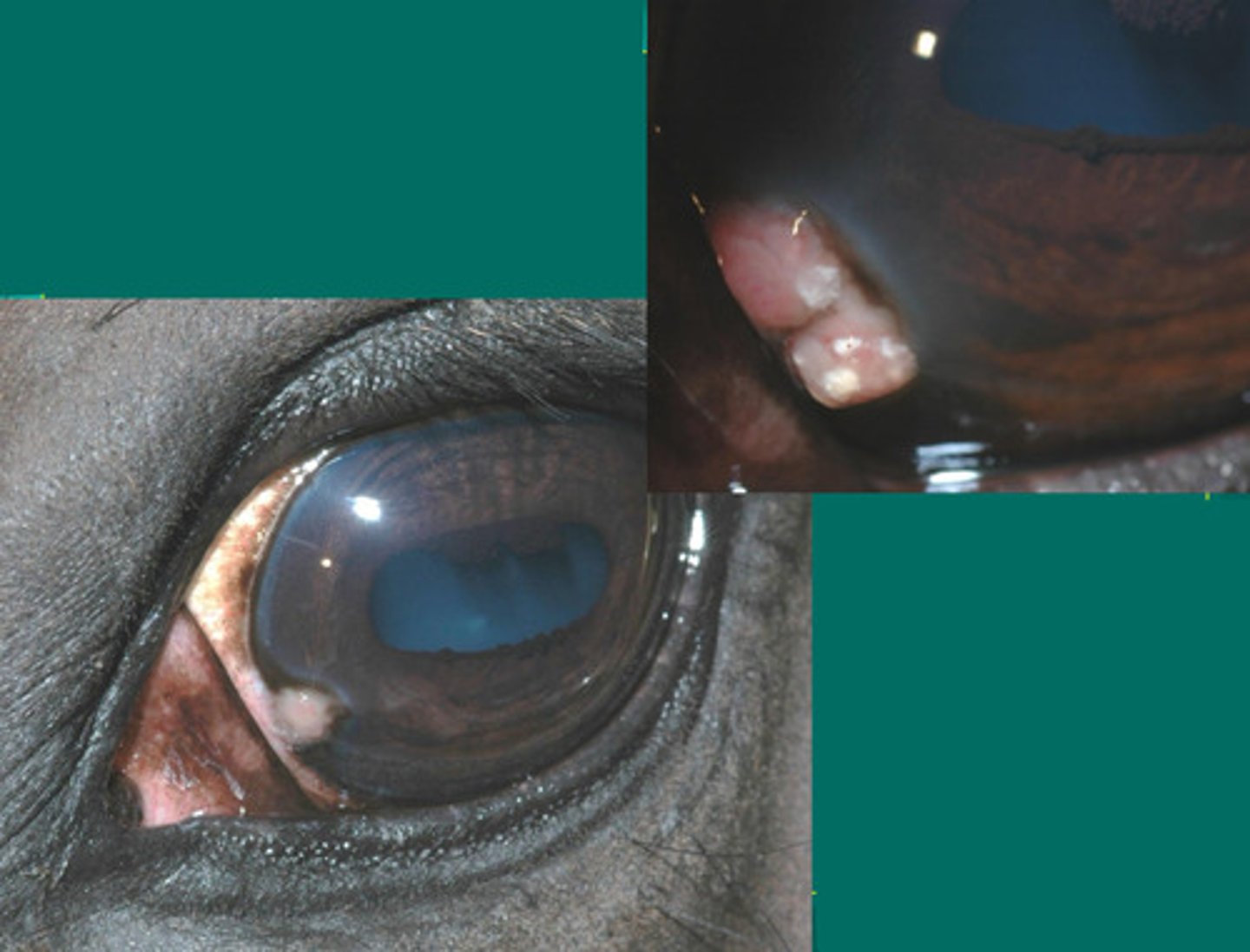
Cyclosporine. Topical steroids if NO ULCER
What is the best treatment for eosinophilic keratitis?
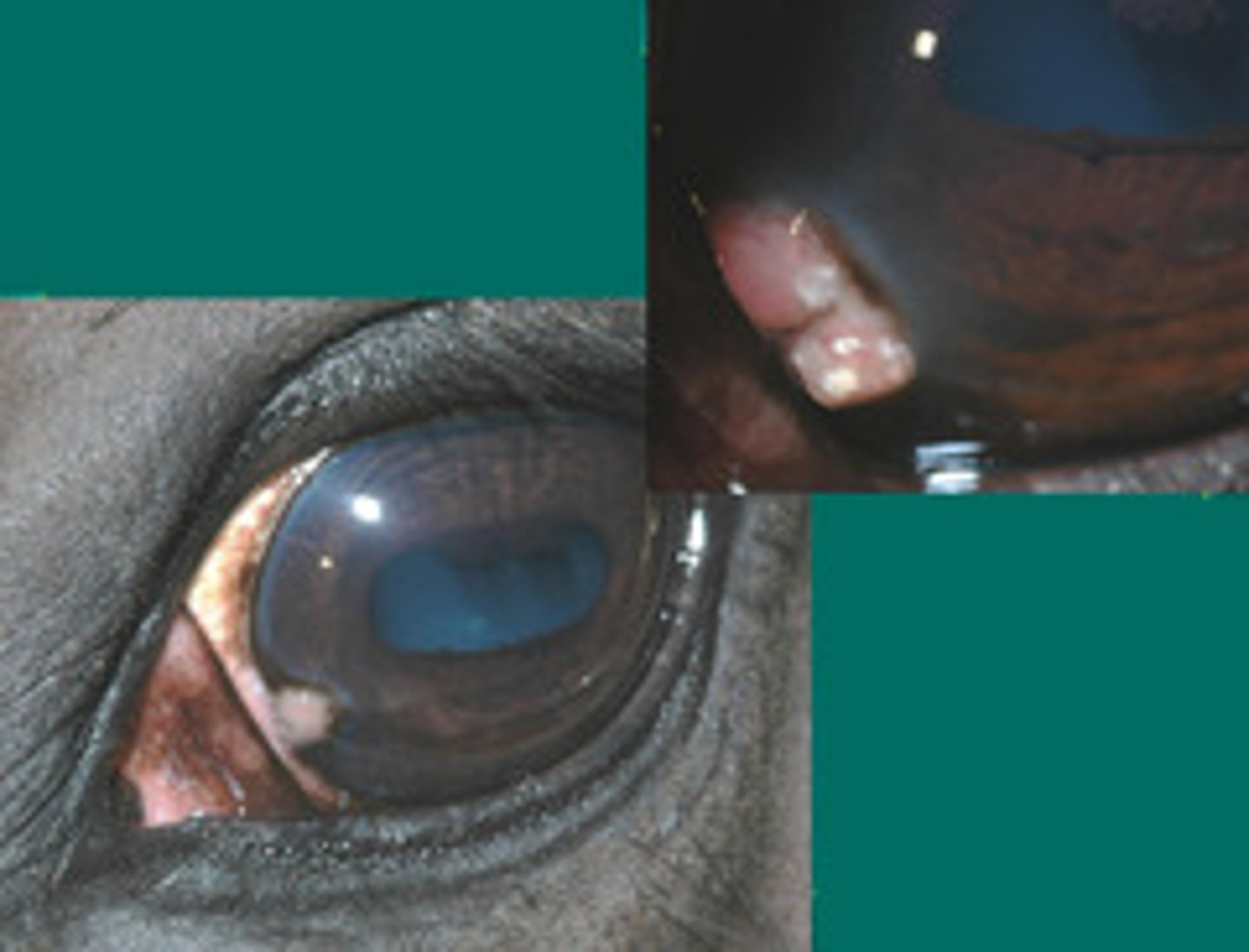
e. immune mediated endothelitis
What is happening in this eye, where deep in the cornea there is central edema which has the potential to cause "melting"?
a. immune mediated epithelial keratitis
b. chronic SUPERFIICAL stromal immune mediated keratitis
c. chronic RECURRENT DEEP stromal immune mediated keratitis
d. eosinophilic keratitis
e. immune mediated endothelitis
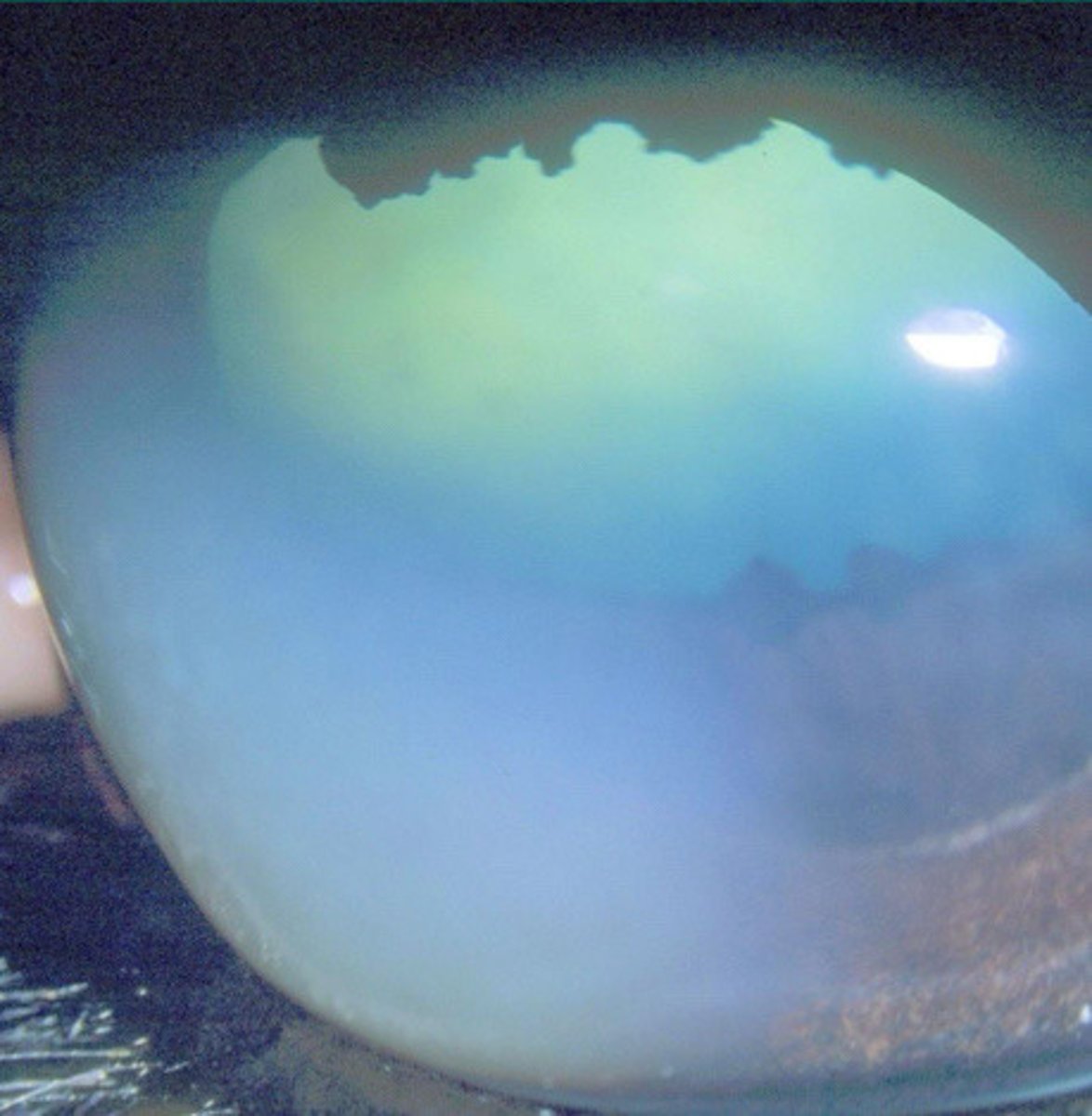
Topical dexamethasone, hypertonics, cyclosporine
What is the treatment for immune mediated endothelitis?
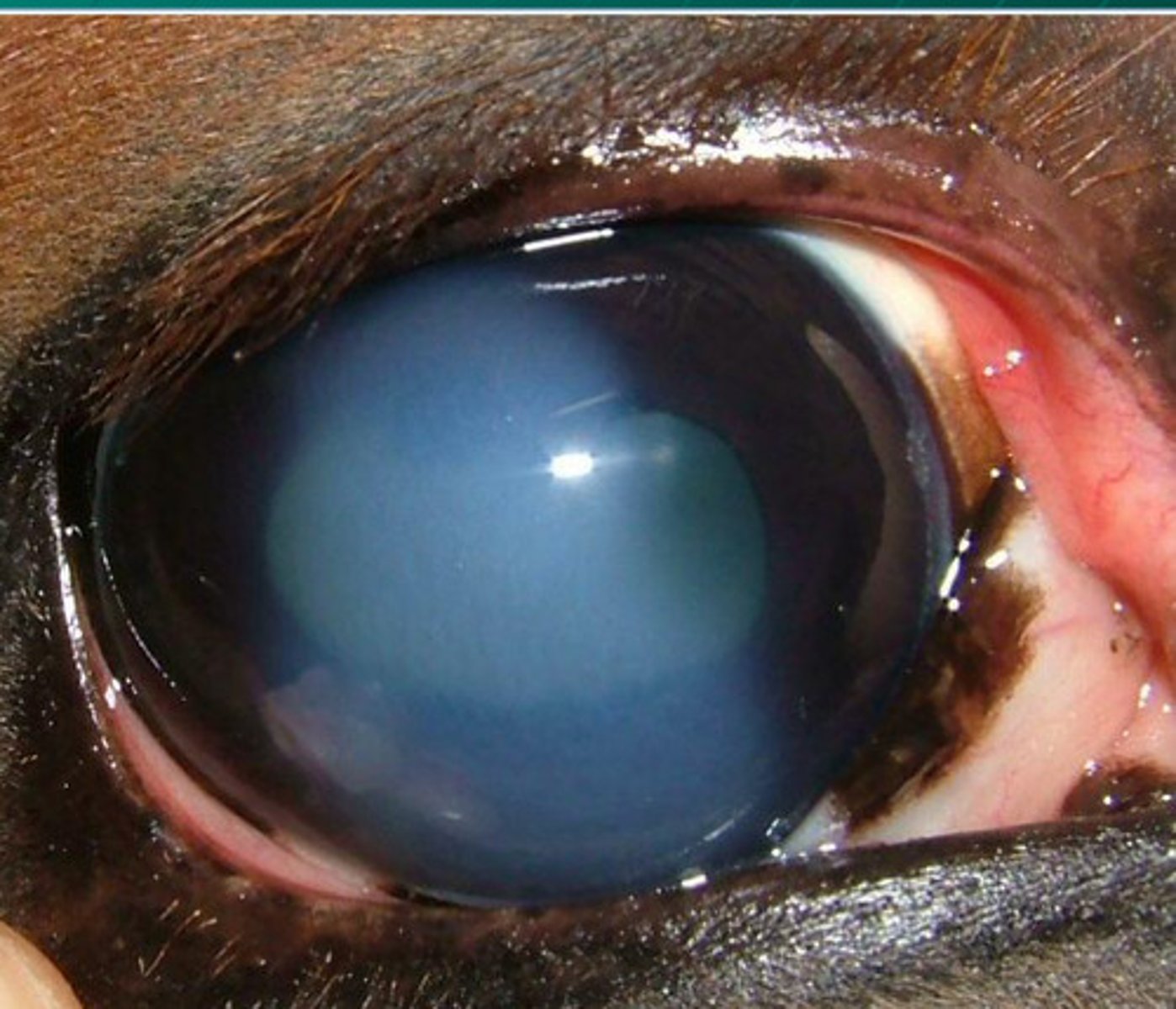
Glaucoma
What is the problem with immune mediated endothelitis? What can it progress to?