Approach to scale
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
Explain what scale is
Desquamated corneocytes on skin and in the hair coat
Normal skin physiology: a little scale (dandruff) is normal
What does pathological scaling result from?
Abnormal desquamation (shedding of corneocytes)
Abnormal cornification (creation of the outer cornified layer of epithelium)
Inflammation (increased keratinocyte turnover)
Bacterial and fungal enzymatic action
Can be adherent or loosely attached
Why may scale be confused with crusts?
Crusts result from the hardening of pus, serum and/or blood to form a solid material on the skin surface
Scale can become trapped in skin exudates and form part of crusts
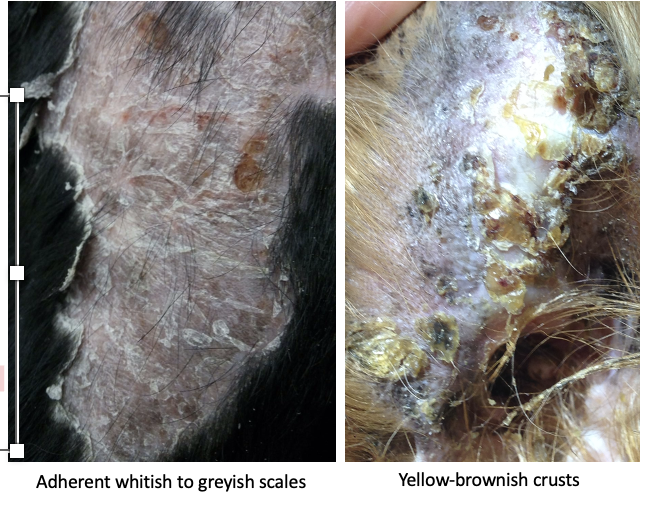
What is the difference between 1° and 2° scaling?
Primary: direct result of disease pathology
Secondary: due to skin inflammation, internal disease or external factors (including environment)
Much more common than 1°
What causes scale in bacterial infection?
Staphylococcus pseudintermedius causes folliculitis (inflammation of hair follicle) and follicular pustule
Following rupture of the pustule and central hair loss, a spreading circle of scale is seen (epidermal collarette)
Darkening of the skin (hyperpigmentation due to the previously present inflammation
Amount of scale dependent on bacterial toxins
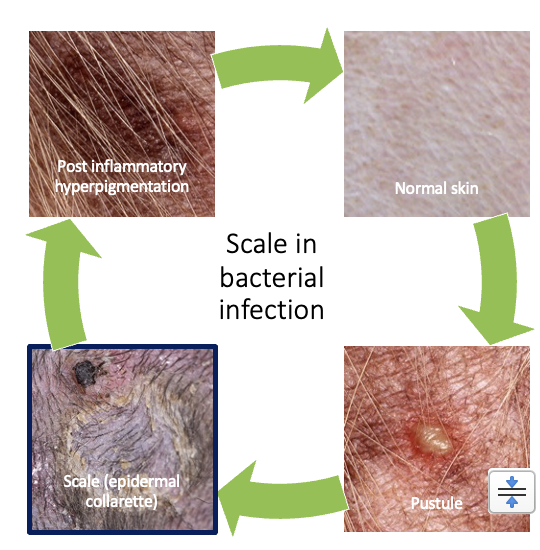
List of Ddxs for scaling
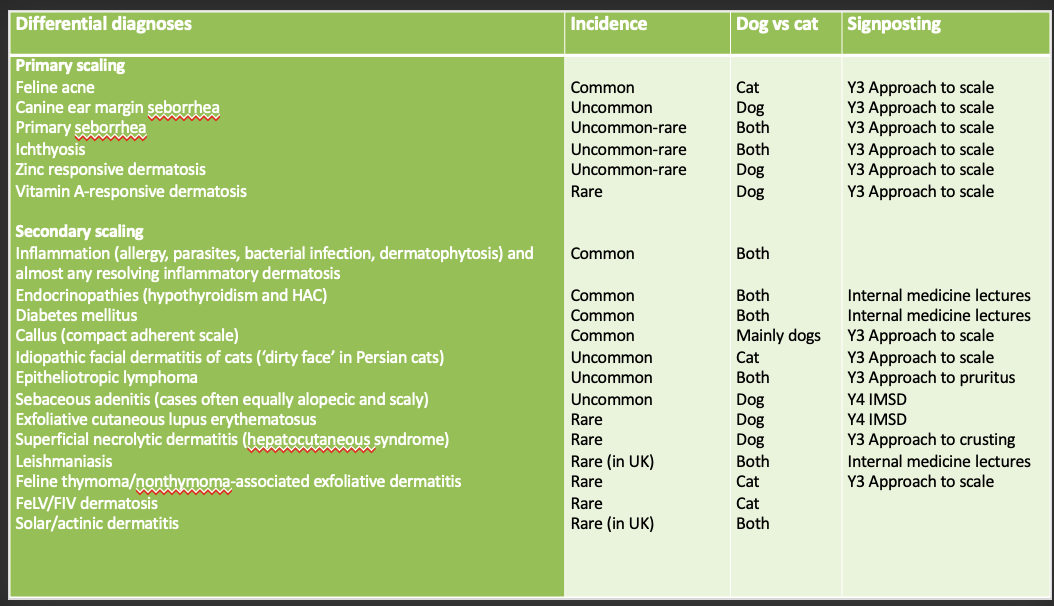
How do you approach a patient where scaling is present?
If pruritis present most likely parasites, bacterial infection and/or allergic skin disease
Check for parasites
Check for secondary infections
In older dogs perform baseline testing for endocrine/metabolic diseases: urinalysis, haematology & biochemistry
Skin biopsy
Genetic testing if indicated
Ichthyosis of the Golden retriever, Great Dane and American Bulldog
Epidermolytic hyperkeratosis of the Norfolk terrier
Lethal acrodermatitis of the Bull Terrier & Miniature Bull Terrier (very rare)
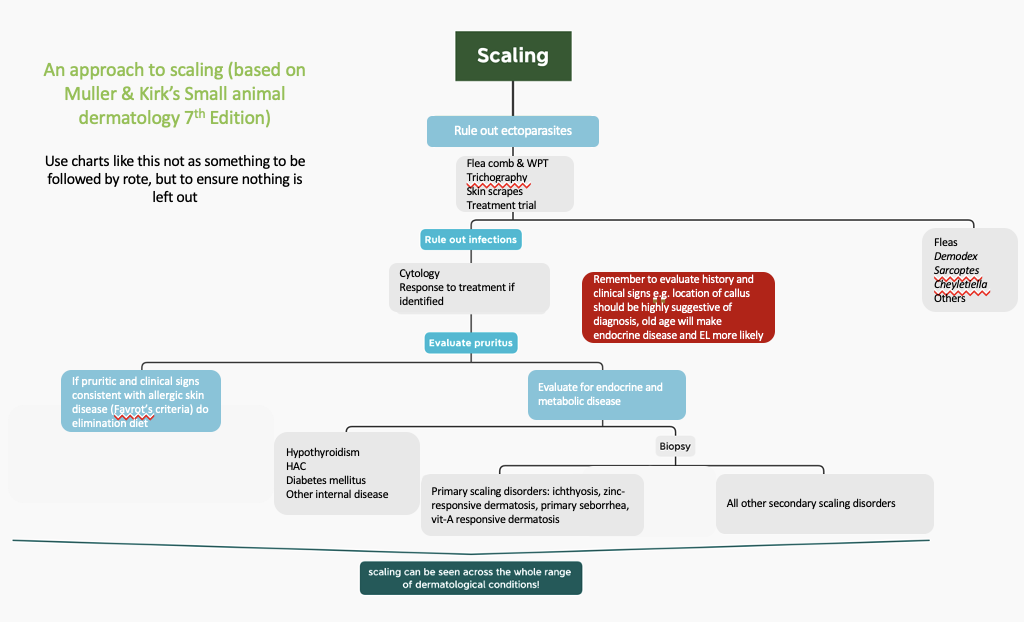
List the diseases where scale is a major presenting sign?
Zinc responsive dermatosis
Ichytyosis of the Golden Retriever
Ear margin Seborrhea
Feline thymoma/non thymoma-associated exfoliative dermatitis
Feline idiopathic facial dermatitis
Feline acne
What are the two types of zinc responsive dermatosis?
Type I: genetically-induced defective intestinal absorption of Zn
Siberian huskies, alaskan malmutes, english bull terries predisposed
Type II: rapidly growing dogs fed a Zn deficient diet (or over-supplemented with substances that interfere with Zn absorption)
Juvenile largre/ giant breed dogs
How does zinc responsive dermatosis present?
Primary: erythema, 50% cases pruritic
Secondary: scale, alopecia, suppuration & crusting +/- SBI
Periocular, perioral, chin, ears, occasionally genitals
May see hyperkeratotic footpads
Sites of trauma (Zn required for normal keratinisation)
How is zinc responsive dermatosis diagnosed?
Skin biopsy
Parakeratosis key finding
How is zinc responsive dermatosis treated?
Type I:
Zn supplementation
Zinc sulphate traditionally used – may cause vomiting
Consider prednisolone (increases Zn absorption) and EFAs if poor response
Type II: correct diet
What is the pathogenesis of ichthyosis of the Golden Retriever
Genetic: mutation in PNPLA1-gene
Leads to abnormal cleavage of desmosomes between corneocytes during desquamation
How does ichthyosis of the Golden Retriever present?
Seen from a few weeks old but may be older when scaling noted
Golden retrievers and goldendoodles
Non pruritic (unless SBI which is not usually present)
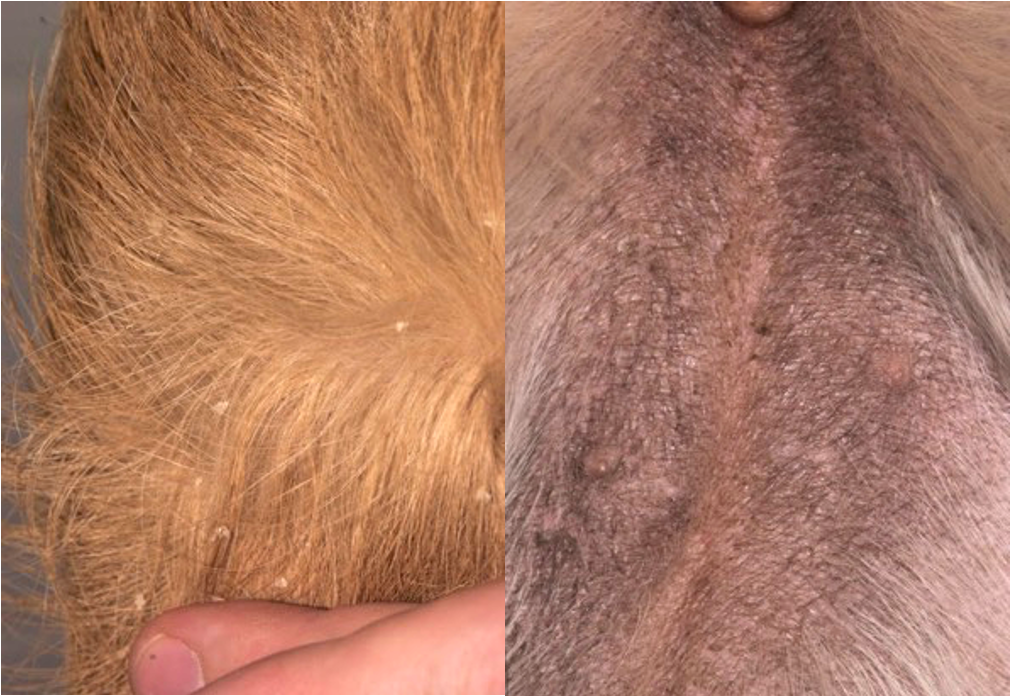
Variable amounts (can be large) of large flakes of non-adherent scale
Hyperpigmentation
Generalised but often more noticeable on ventrum (particularly hyperpigmentation)
How is ichthyosis of the Golden Retriever diagnosed?
Rule out parasites (unlikely as non-pruritic)
Skin biopsy
Genetic testing widely available (part of official UK Kennel Club DNA testing scheme) - if several puppies in litter affected consider skipping biopsy and performing genetic testing
How is ichthyosis of the Golden Retriever treated?
Skin barrier function not compromised so secondary bacterial infection uncommon, but can get microbial otitis
Scaling is cosmetic disease: symptomatic treatment only
How does ear margin seborrhea present?
Mainly adult onset, but can occur in puppies
Marked breed predilection in Dachshunds
Non-pruritic (unless SBI)
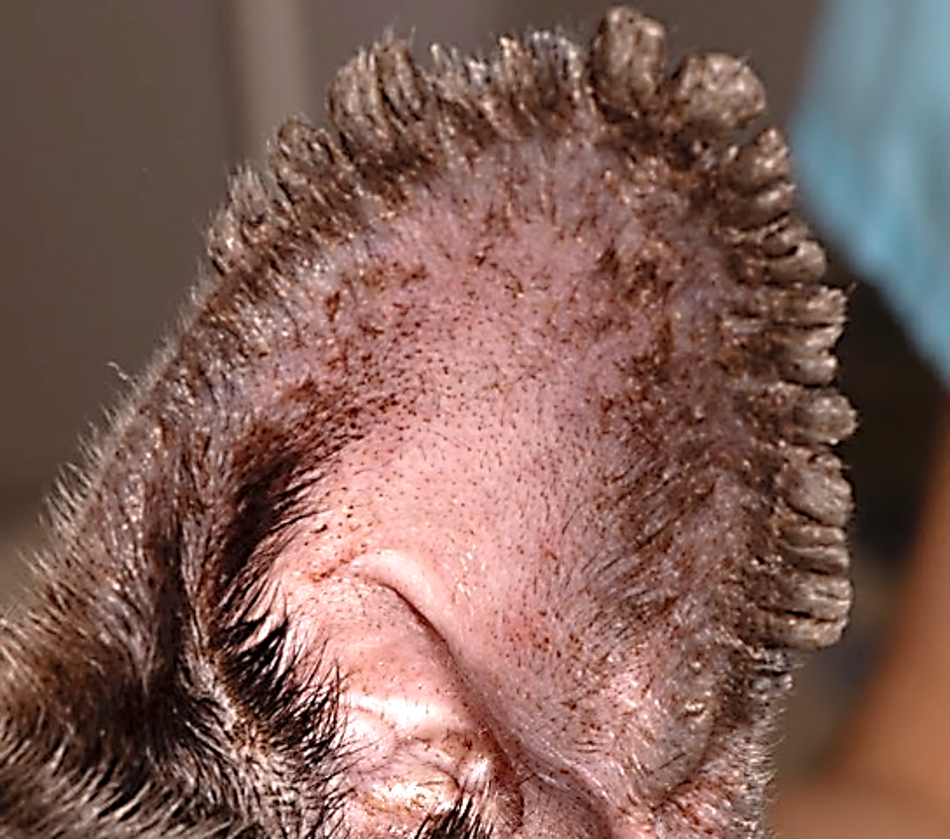
White to pigmented, adherent scale +/- follicular casts
With chronicity may see fissuring of skin and SBI
Distribution: pinnal margins (medial and lateral aspects)

How is ear margin seborrhea diagnosed?
Rule out parasites: particularly demodicosis and sarcoptic mange (unlikely as non-pruritic)
Skin biopsy (although initial clinical diagnosis and treatment trial acceptable)
How is ear margin seborrhea treated?
Emollient rinses, Vaseline, propylene glycol
Surgery to remove pinnal margin (rarely required!)
What are the general features of feline thymoma/nonthymoma-associated exfoliative dermatitis?
Rare paraneoplastic syndrome
Middle to older age cats
Non-pruritic
+/- signs of respiratory compromise (due to thymoma in thorax)
No association with thymoma in some cases
Thymoma and non-thymoma cases are indistinguishable clinically and histopathologically – advanced imaging required
How does feline thymoma/nonthymoma-associated exfoliative dermatitis present?
Diffuse erythema and scaling (large 1+ cm flakes of skin), +/- alopecia
Distribution: generalised
How is feline thymoma/ non thymoma-associated exfoliative dermatitis diagnosed?
Skin biopsy
Thoracic radiography / CT
How is feline thymoma/ non thymoma-associated exfoliative dermatitis treated?
Surgery to remove thymoma may be curative
Immunomodulatory drugs can be used- more beneficial in nonthymoma associated
Guarded prognosis
What are the general features of feline idiopathic facial dermatitis?
Disease of unknown aetiology complicated by microbial overgrowth
Young to middle aged cats
Persians and similar breeds (e.g. exotic shorthair), Himalayan cats
Variable pruritus (common with SBI or Malassezia overgrowth)
How does feline idiopathic facial dermatitis present?
Tightly adherent, greasy black scale +/- erosion, ulceration and exudation
Distribution: periocular skin, nasal folds, muzzle, chin
How is feline idiopathic facial dermatitis diagnosed?
Diagnosis of exclusion: rule out parasites, microbial infection (including dermatophytosis), consider allergic skin disease if generalised disease
Cytology: Malassezia overgrowth common
How is feline idiopathic facial dermatitis treated?
Anti-yeast therapy: ideally topical but may need to consider systemic if cat wont permit topicals or concern with proximity to eyes
Keratolytic shampoos
Immunomodulation: ciclosporin, prednisolone, topical tacrolimus
What is feline acne?
Common keratinisation disorder of cats
how does feline acne present?
Dark, waxy to dry scale adherent to hair base +/- comedones
Distribution: chin (less commonly lips)
How is feline acne diagnosed?
Largely clinical diagnosis: rule out Demodex cati
Cytology: Malassezia overgrowth, SBI
How is feline acne treated?
Topical antiseptics +/- antimicrobials
Topical keratolytic
Prednisolone if significant inflammation present
What are keratoplastic/keratolytic products?
Reduce scale production . sulphur and coal tar shampoos = keratoplastic
Or remove scale e.g. salicylic acid shampoos = keratolytic
Delicate balance between removing scale and causing excessive drying
Used before moisturizing products
What are moisturizing and emollient products?
Reduce transepidermal water loss and prevent inflammation e.g. products containing oils, propylene glycol and urea
Best used after other products have removed scale / treated secondary infections