BIOL 373 Unit 6 pt. 1
1/24
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
25 Terms
Absorption
Transport nutrients, water, ions, vitamins across epithelium
Pathway of absorption
Lumen → epithelium → interstitial fluid → blood
Why do barriers need to exist in the gastrointestinal function? + problems that arise
Aim is to digest macromolecules, but not the macromolecules that make itself up. Problems that arise when barrier is not followed are peptic, and duodenal ulcers
Why is an extensive system of entry required for GI function?
GI lining largest area of contact between internal and external environment.
Protection of pathogens is mediated by (5)
Epithelial barrier, mucus, digestive enzymes, acid, and Gut-Associated Lymphoid Tissue (GALT)
What is GALT?
Gut-Associated Lymphoid Tissue (GALT) “mucosa” - gentler immune system that understands the difference between proteins that need to be digested and pathogen proteins.
What does the GI need to balance
Water input/output - balance between secretion (exocrine) and reabsorption
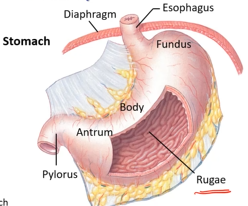
Stomach gross anatomy
stomach entry from esophagus
pylorus exit to small intestine
characteristic folds (rugae), mucosal surface!
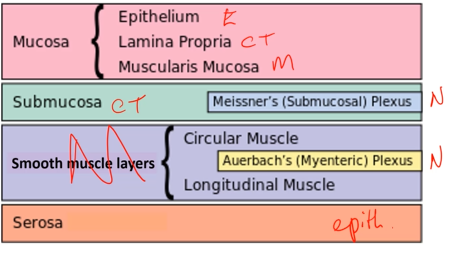
Characteristics of a mucosal surface
Mucosa - consists of epithelial lining, connective tissue (lamina propia, and muscle layer (muscularis mucosae)
Submucosa - on the outside of the muscle layer
Two more layers of smooth muscle (circular and longitudinal)
Serosa - epithelial layer, basically a bag
Neurons go through and in between layers
First neural plexus is submucosal plexus, and second is myenteric plexus (runs through circular and longitudinal muscle)
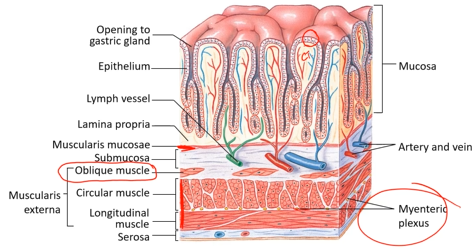
Stomach microanatomy (differences from typical mucosal surfaces)
In addition to circular and longitudinal muscle, it has diagonal muscle (oblique muscle) because the stomach is a bag rather than a tube and must contract in more dimensions.
Epithelial lined gastric glands - exocrine secretion, secreting out to a surface. Rugae are typical of bag-like organs that need to expand.
Small intestine zones
Duodenum, jejunum, ileum → in that order
Small intestine gross anatomy
Circular and longitudinal muscle, and a thin layer of muscle (mucosa and submucosa)
Has PLICA - folds, unlike rugae, these do not disappear as the intestine expands or shrinks. Intestinal villi.
Peyer’s patch - only evidence of an immune system in the small intestine, very numerous.
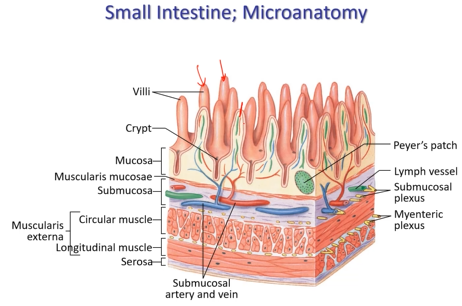
3 mechanisms to increase surface area
Intestine (pleca), villus (cross epithelial barrier and picked up by circulatory system or the lacteal), epithelium (at cellular level, microvilli)
4 functions of the Gi tract
Motility, secretion, and digestion
Patterns of gut motility
Peristalsis - moving food from mouth to anus (contract circular muscle to pinch bolus forward)
Segmental contraction - mixing
Single-unit smooth muscle
Gut muscle is single-unit smooth muscle, interconnected by gap junctions, contracts as a single unit, autonomic neuron dumps neurotransmitter and bathes smooth muscle in depolarization.
Two types of gut contraction
Tonic (minutes to hours) - smooth muscle sphincters, keeps food from moving backwards.
Phasic (few seconds):
between meals - migrating motor complexes to sweep tract, stomach to small intestine
during/after meals - peristaltic and segmental contractions
Slow wave potentials
Slow waves creep up but don’t reach threshold, no contraction. If they do, the ultimate amplitude is how long it stays to polarize. Force and duration is influenced by amplitude and frequency of action potentials.
Similar to pacemaker potentials
Process of action potential durign an above threshold slow wave
Opening of voltage-gated Ca channels → action potentials → contraction
Amplitude and duration of contraction is influenced by
neurotransmitters, hormones, and paracrine factors
Slow wave frequency is set by…
pacemaker cells called interstitial cells of Cajal, found between smooth muscle layers.
Does slow wave frequency differ between duodenum and stomach?
Yes duodenum has more frequency than stomach.
How are water and ions secreted into the lumen?
Ions transported via membrane transporters.
Water follows osmotic gradient.
Water and ions can sometimes pass between cells via paracellular routes.
Membrane transporters involved in secretion of ions
Na+/K+-ATPase, NKCC cotransporter, Cl-/HCO3- exchanger, Na+/H+ exchanger (NHE), H+/K+-ATPase
Ion channels involved in secretion of ions
ENac, K+ channels, Cl- channels (including CFTR channels)