Urinary System Anatomy, Functions, and Regulation in Human Physiology
1/99
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
100 Terms
What are the primary functions of the urinary system?
Eliminate organic wastes, regulate plasma ion levels, regulate blood volume and blood pressure, adjust water loss, release cardiovascular hormones, stabilize blood pH, and conserve nutrients.
What are the main components of the urinary system?
Kidneys, ureters, urinary bladder, and urethra.
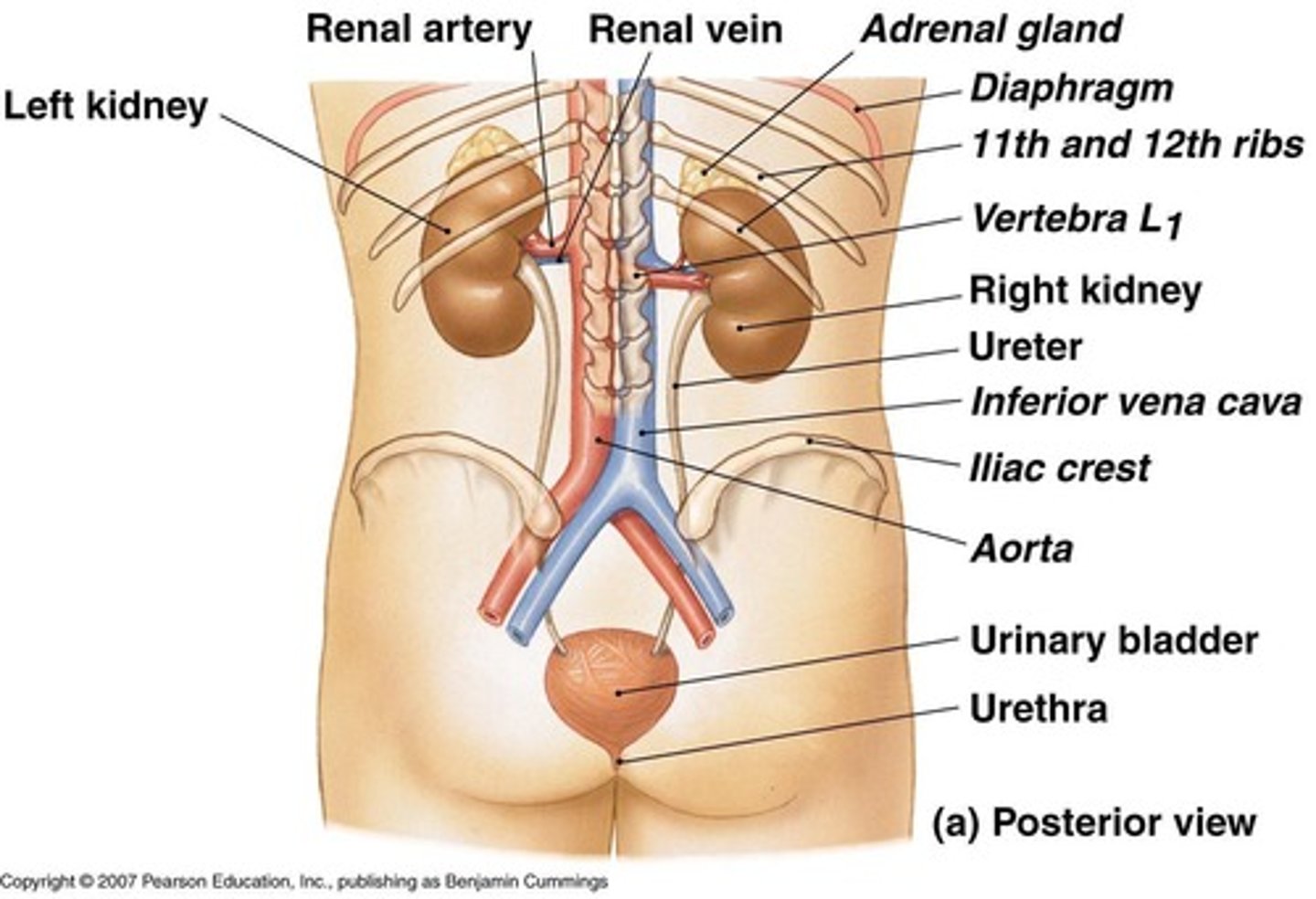
What is the role of the kidneys in the urinary system?
Produce urine, a fluid made of water, ions, and soluble compounds.
What surrounds the kidneys?
A fibrous capsule.
Where do the renal artery and renal nerve enter the kidney?
At the hilum.
What is the renal pelvis?
The area where urine collects from calyces before leaving to the ureter.
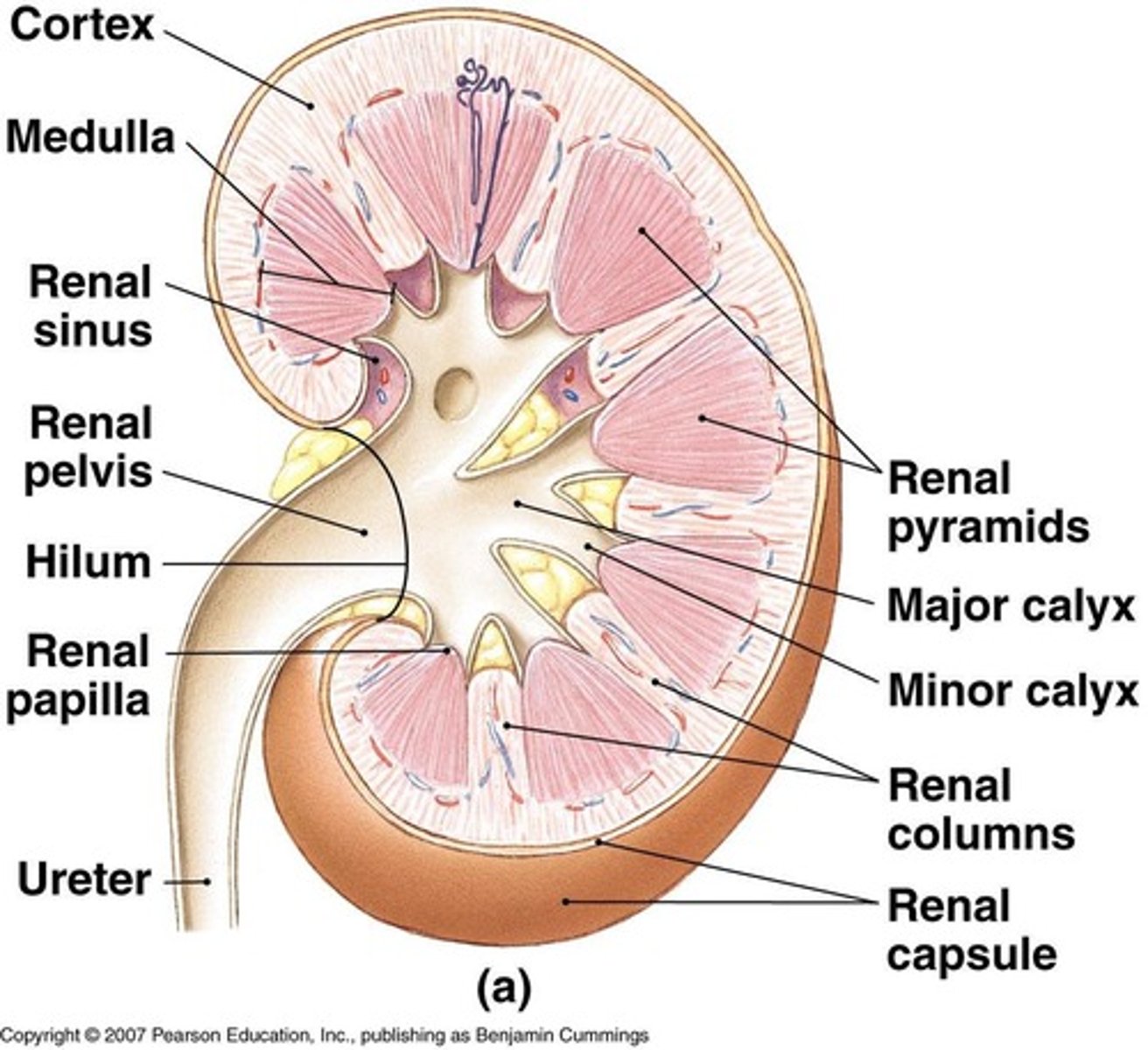
How many nephrons are typically found in each kidney?
About one million nephrons.
What is the basic functional unit of the kidney?
The nephron.
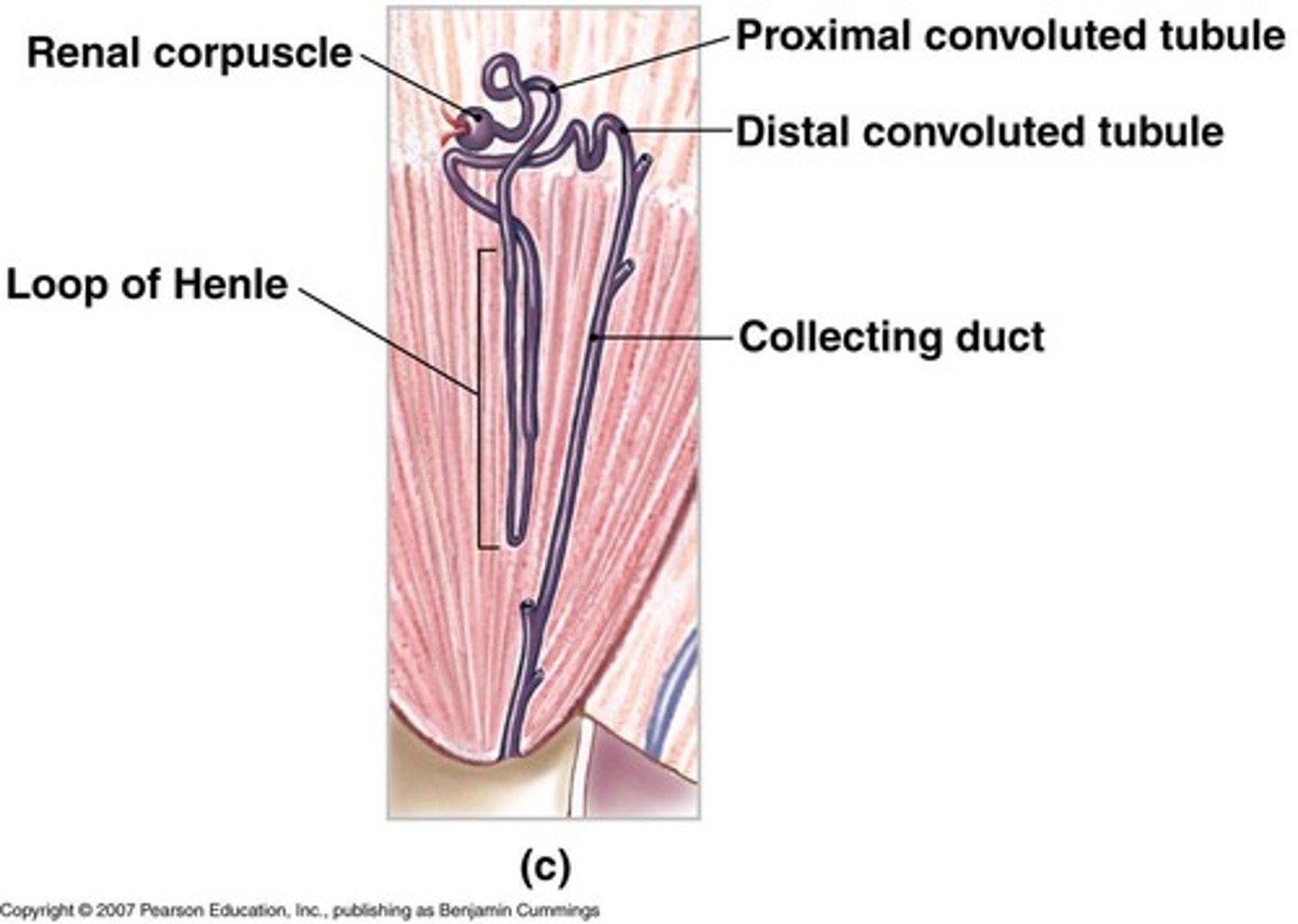
What are the two main parts of the nephron?
Renal corpuscle and renal tubule.
What is the pathway of urine through the nephron?
Filtered in the renal corpuscle, flows into the proximal convoluted tubule (PCT), then the loop of Henle, followed by the distal convoluted tubule (DCT), and exits to the collecting duct.
What is the glomerulus?
A knot of interconnected capillaries within the renal corpuscle.
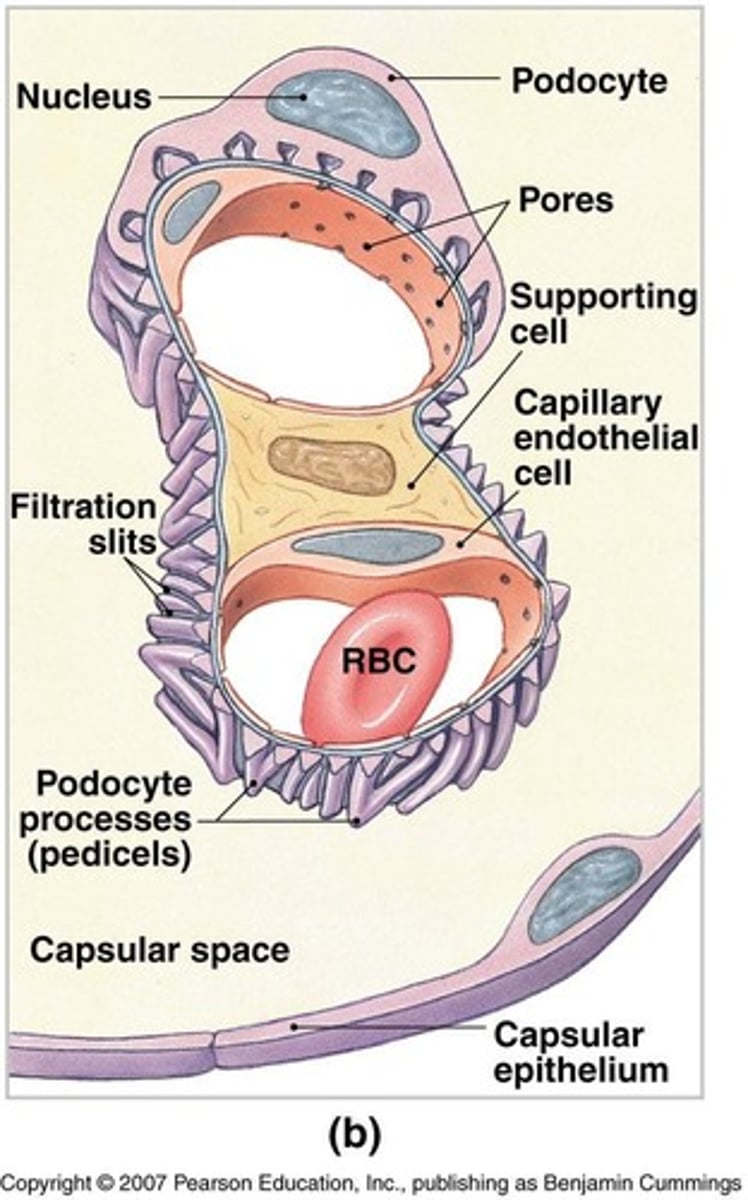
What is Bowman's capsule?
A structure that encloses the glomerulus and is made of squamous epithelium.
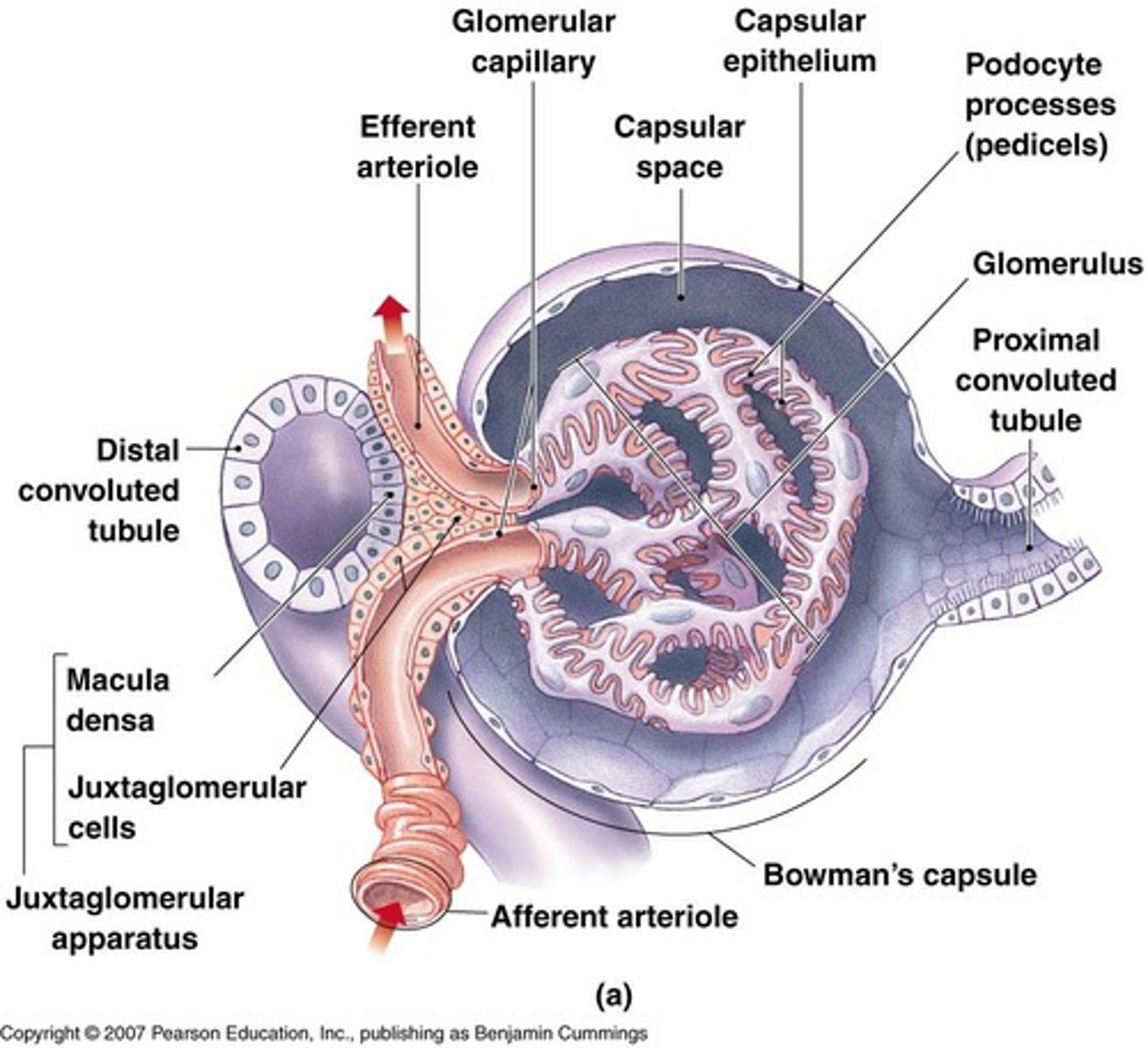
What occurs in the proximal convoluted tubule (PCT)?
Reabsorption of critical substances such as nutrients, ions, and proteins from the filtrate.
What is the function of the loop of Henle?
It consists of a descending limb that is permeable to water and an ascending limb that is impermeable to water and solutes.
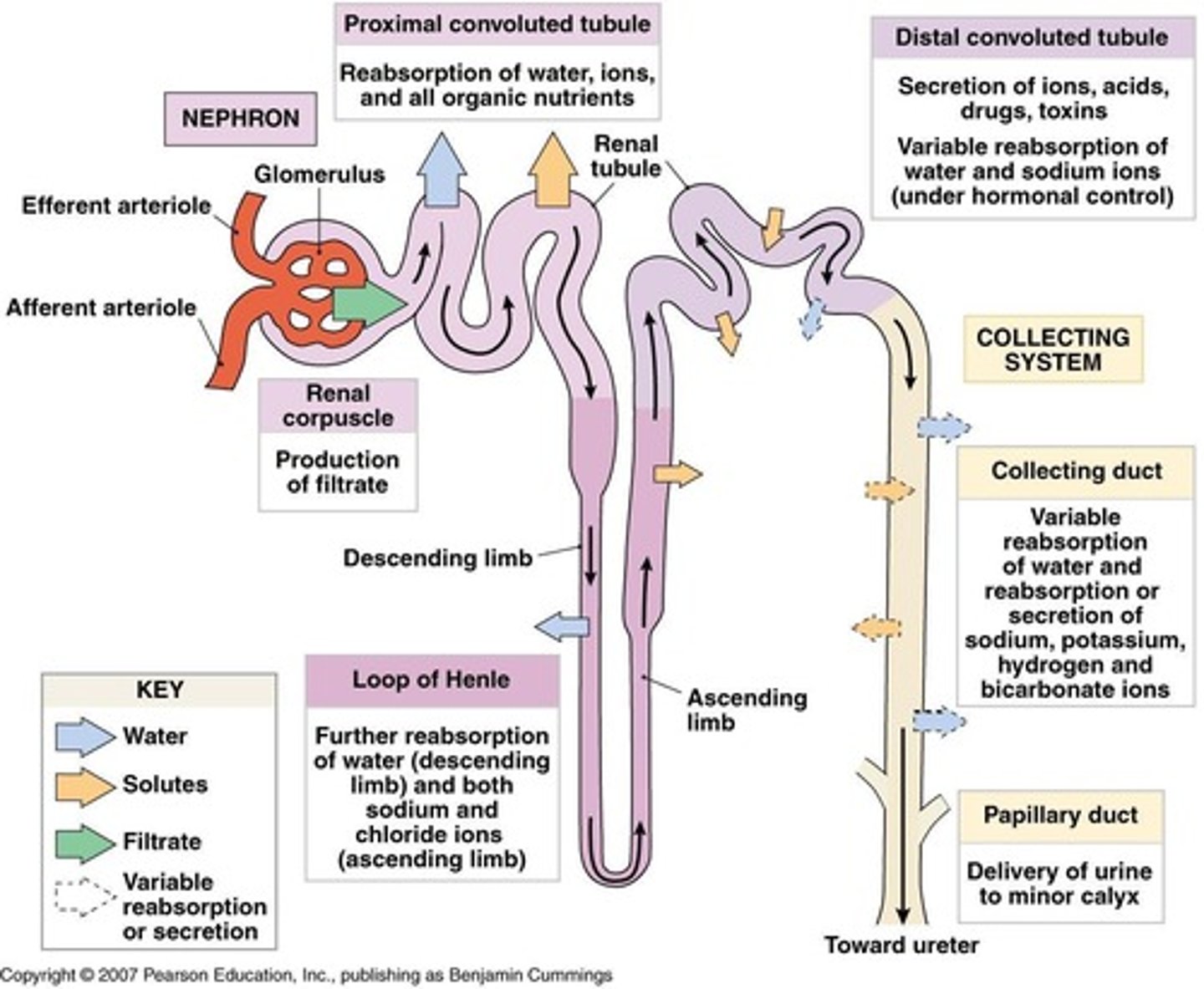
What happens in the distal convoluted tubule (DCT)?
It actively secretes substances into urine and reabsorbs sodium.
What is the role of the collecting ducts?
They receive urine from nephrons and adjust the final osmotic pressure of urine.
What are the primary metabolic wastes excreted in urine?
Urea, creatinine, uric acid, and excess ions.
What are the three processes involved in urine formation?
Filtration, reabsorption, and secretion.
What drives the filtration process at the glomerulus?
Blood pressure forces fluid and dissolved substances across the endothelial wall of glomerular capillaries into the capsular space.
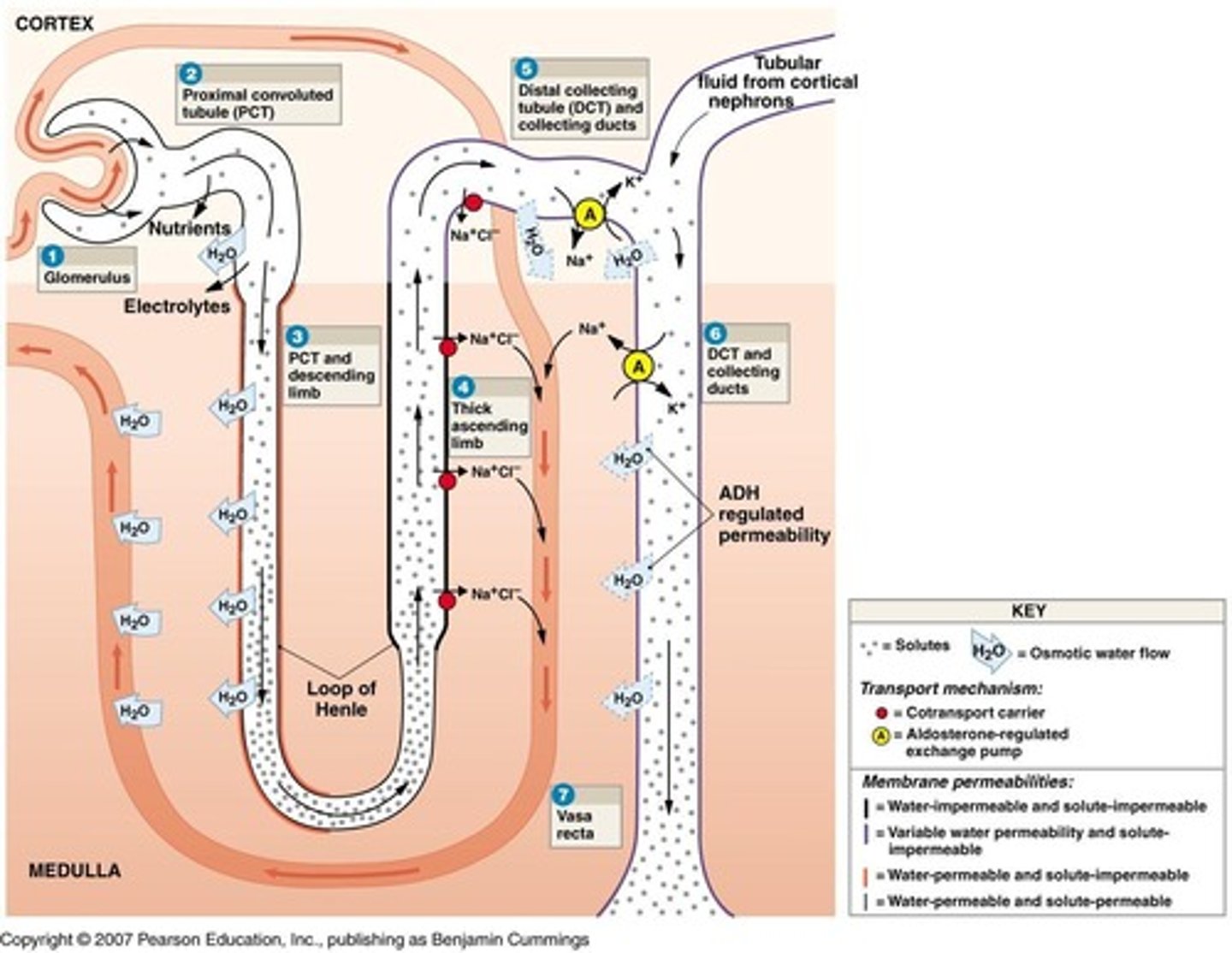
What is the glomerular filtration rate (GFR)?
The rate at which blood is filtered through the glomeruli, which depends on blood pressure.
What triggers the release of renin?
A decline in filtration pressure (blood pressure) detected by the juxtaglomerular apparatus.
What is the significance of the kidneys in relation to blood volume and pressure?
They help regulate blood volume and pressure through filtration and reabsorption processes.
How much filtrate is produced at the glomeruli each day?
Roughly 180 liters.
What is the consequence of not reabsorbing the majority of filtrate?
It could lead to fatal dehydration.
What is the function of the juxtaglomerular apparatus?
It releases renin and erythropoietin and is located at the start of the distal convoluted tubule.
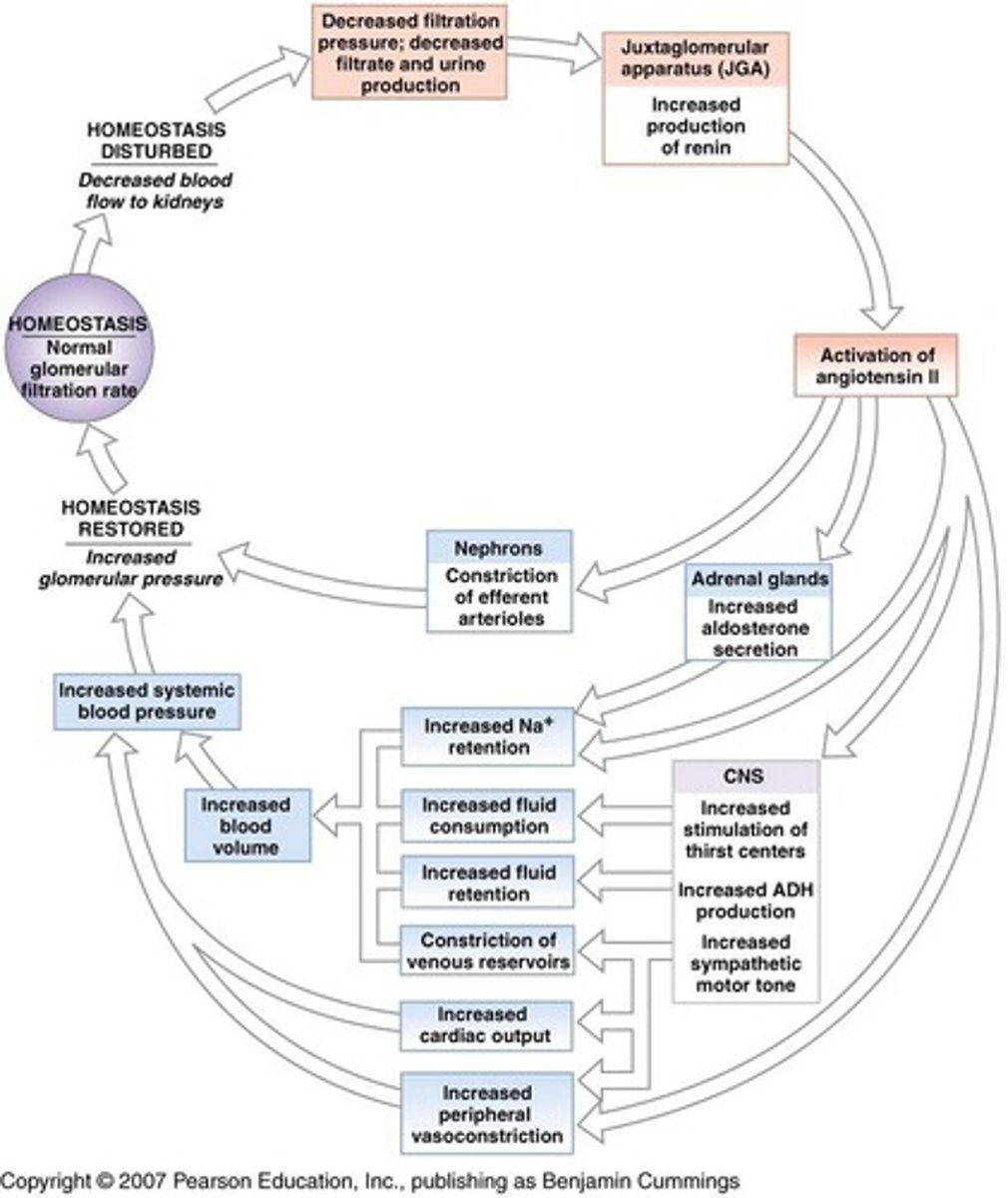
What is the role of peritubular capillaries?
They facilitate the exchange of substances between the renal tubule and the bloodstream.
What is the significance of the renal artery?
It supplies blood to the kidneys.
What is the role of the renal vein?
It drains blood from the kidneys.
What are the minor calyces?
Structures that collect urine from the collecting ducts before it moves to the major calyces.
What percentage of filtrate is reabsorbed by the Proximal Convoluted Tubule (PCT)?
60-70%
What substances are reabsorbed by the PCT?
Nutrients, sodium, other ions, and water
What does the PCT do with reabsorbed substances?
Releases them into venous drainage for return to the bloodstream
What is the primary function of the Loop of Henle?
Reclaims water and ions from filtrate
What occurs in the ascending limb of the Loop of Henle?
Pumps out sodium and chloride ions
What occurs in the descending limb of the Loop of Henle?
Absorbs water
What effect does interstitial osmotic pressure have on tubular fluid?
Pulls water from tubular fluid
What happens to urea concentration as fluid is lost in the Loop of Henle?
Urea concentration rises
What is the role of the Distal Convoluted Tubule (DCT)?
Performs final adjustments by secreting or reabsorbing ions
What ions are exchanged in the DCT?
Reabsorbs sodium in exchange for secreted potassium and hydrogen ions
How does aldosterone affect sodium reabsorption?
Increases sodium reabsorption and potassium loss
What does Antidiuretic Hormone (ADH) regulate?
Water loss
How does ADH affect the DCT and collecting duct?
Makes them permeable to water, allowing water to exit to interstitial fluid
What is the result of high ADH levels on urine concentration?
Urine becomes concentrated (low in water, high in solute)
What percentage of water is typically reabsorbed from the filtrate by renal tubules?
More than 99%
What is the water content range of normal urine?
93% to 97%
What mechanisms are involved in reabsorption in the kidneys?
Diffusion, osmosis, and active transport
What principle describes the mechanism of water reabsorption?
Water follows salt
What type of process is secretion in the kidneys?
A selective, carrier-mediated process
What regulates filtration pressure in the kidneys?
Changes in diameter of afferent and efferent arterioles.
How does sympathetic activation affect kidney function?
It causes powerful vasoconstriction of afferent arterioles, decreasing GFR and redirecting blood flow to other organs.
Name a hormone involved in the hormonal control of kidney function.
Angiotensin II, Aldosterone, ADH, or Atrial natriuretic peptide (ANP).
What marks the end of urine modification?
When fluid enters the renal pelvis.
What is the primary function of the ureters?
To transport urine from the renal pelvis to the urinary bladder.
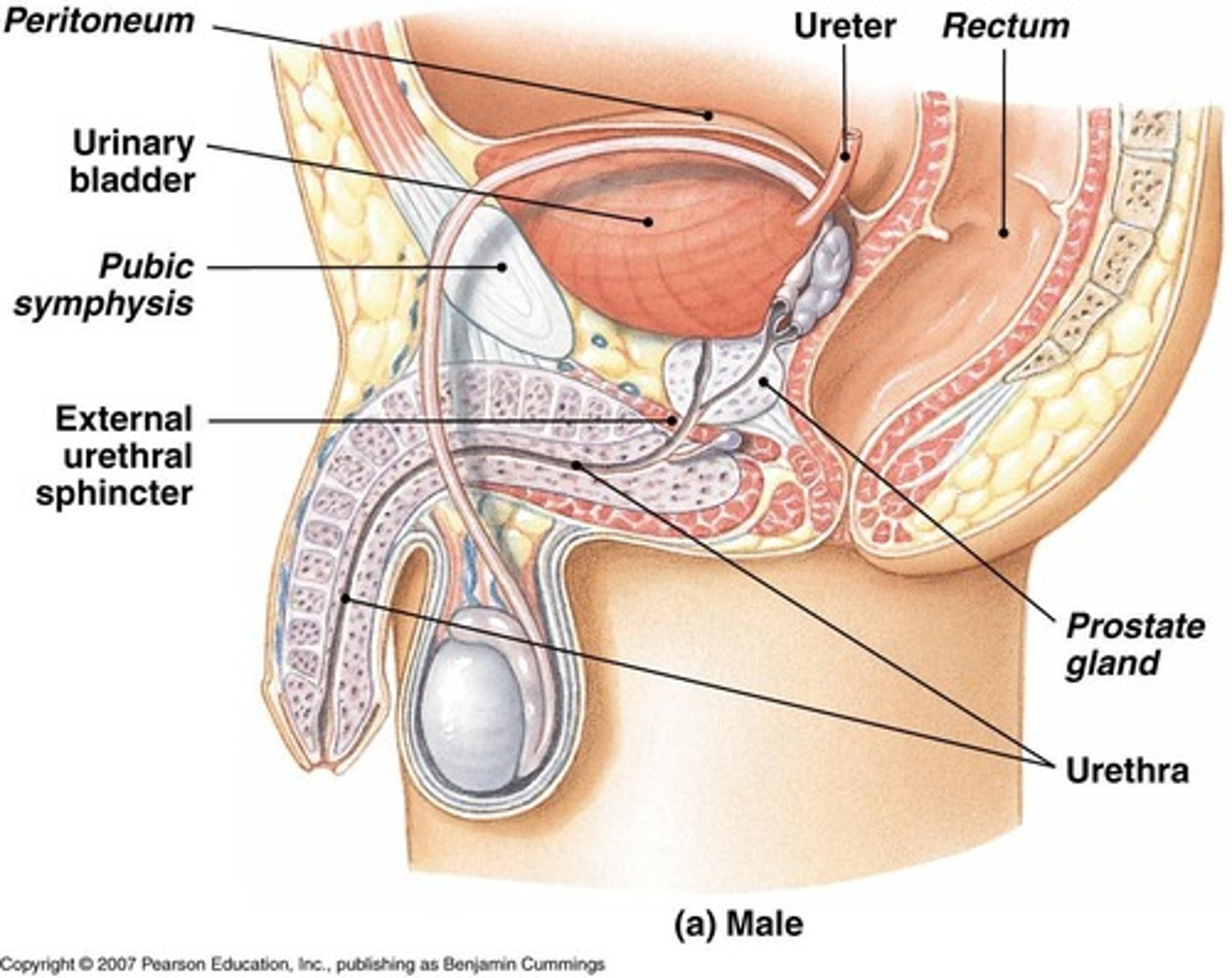
What type of muscle contracts to push urine toward the bladder?
Smooth muscle in the walls of the ureters.
What is the function of the urinary bladder?
To store urine; it is a distensible muscular sac.
What are the internal features of the urinary bladder?
Trigone, Neck, Internal urethral sphincter, and Detrussor muscle.
What triggers the micturition reflex?
Stretch receptors in the bladder wall.
How does voluntary urination occur?
By coupling the micturition reflex with relaxation of the external urinary sphincter.
What are the three types of homeostasis required for fluid balance?
Fluid balance, Electrolyte balance, and Acid-base balance.
What are the two fluid compartments in the body?
Intracellular fluid (ICF) and Extracellular fluid (ECF).
What percentage of total body water is intracellular fluid (ICF)?
About 60%.
What percentage of total body water is extracellular fluid (ECF)?
About 40%.
What maintains water balance in the body?
Water intake normally equals water loss.
How is water gained in the body?
Through eating, drinking, and aerobic metabolism.
What happens during a fluid shift?
Water moves to establish osmotic equilibrium between ECF and ICF.
What can cause cellular swelling?
Hypotonic ECF pushes water into cells.
What is the impact of sodium ion balance on water balance?
Total electrolyte concentration affects water balance; sodium gain/loss can cause problems.
What stimulates sodium reabsorption along the distal convoluted tubule (DCT)?
Aldosterone.
What happens to potassium ion excretion when sodium levels are low?
Urinary excretion of potassium increases.
What is the relationship between fluid balance and electrolyte balance?
They are interrelated; fluid shifts can mitigate the impact of water gains or losses.
What is the normal pH range of body fluids?
pH 7.35 to pH 7.45
What does a pH greater than 7.45 indicate?
Alkalosis (too alkaline)
What does a pH less than 7.35 indicate?
Acidosis (too acidic)
What is the most important factor affecting pH in the body?
Carbonic acid
How is carbonic acid formed?
CO2 reacts with H2O
What happens to pH as CO2 levels increase?
pH decreases
What happens to pH as CO2 levels decrease?
pH increases
What are metabolic acids?
Acids produced by metabolism, such as lactic acid and ketone bodies
What is the role of buffer systems in the body?
To resist changes in pH
What are the three major buffer systems in the body?
Protein buffer system, carbonic acid-bicarbonate buffer system, phosphate buffer system
What is the function of the protein buffer system?
Amino acid subunits respond to H+ changes
What does the carbonic acid-bicarbonate buffer system do?
Resists pH changes in ECF caused by metabolic acids
What is the function of the phosphate buffer system?
Resists pH changes within cells
What is respiratory compensation?
Changes in ventilation that lead to changes in pH by raising or lowering CO2 levels
What is renal compensation?
Kidney varies H+ secretion and bicarbonate reabsorption depending on pH of ECF
What are the two classes of acid-base disorders?
Respiratory acid-base disorder and metabolic acid-base disorder
What causes respiratory acid-base disorder?
Abnormal respiratory function leading to large changes in CO2 levels
What causes metabolic acid-base disorder?
Formation of organic acids or conditions disturbing bicarbonate levels
What is the most common acute acid-base disorder?
Respiratory acidosis
What age-related changes occur in the urinary system?
Loss of functional nephrons, reduced GFR, reduced response to ADH, urinary retention in men, drop in body water and mineral content
How do sweat glands assist in fluid balance?
By eliminating water and solutes, especially sodium and chloride ions
What role does the axial skeleton play in the urinary system?
Provides protection for kidneys and ureters
How does the muscular system contribute to urination?
Sphincter controls urination by closing urethral opening
What is the role of the nervous system in the urinary system?
Adjusts renal blood pressure and controls urination
What hormones adjust fluid and electrolyte reabsorption in kidneys?
Aldosterone and ADH
What does the cardiovascular system do in relation to the urinary system?
Delivers blood for filtration and accepts reabsorbed fluids and solutes
How does the lymphatic system assist the urinary system?
Provides defenses against urinary tract infections
What role does the respiratory system play in acid-base balance?
Regulates pH by eliminating carbon dioxide
How does the digestive system contribute to fluid balance?
Absorbs water and ions needed to maintain normal body fluid concentrations
What is the function of the reproductive system in relation to urinary health?
Accessory organ secretions may prevent urethral infections in males