4.1 SEXUAL HUMANS
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
Scrotum and function
External sac of skin hold testes out body
Keep testes 2°C cooler than body temp
Essential for spermatogenesis (make sperm)
Testes
Male reproductive organs produce sperm and hormones
Produce sperm in seminiferous tubules
Produce testosterone
Testes histology
Seminiferous tubules → site of sperm production
Sertoli cells → support developing sperm
Leydig → Secrete testosterone
Epididymis
Long coiled tube back each testis
Store sperm
Sperm mature gain motility
Vas deferens
Muscular tube transport sperm
Carries sperm from epididymis → urethra during ejaculation
Seminal vesicle
Gland produce seminal fluid
Secret fluid reach fructose( sperm energy)
Make most semen volume
Prostate gland
Gland below bladder
Produce alkaline fluid neutralise acidic conditions in vagina → protect sperm
Urethra
Tube run through penis
Carries semen and urine (not same time)
Penis
External male organ for reproduction
Deliver semen into vagina
Erectile tissue fill with blood → erection
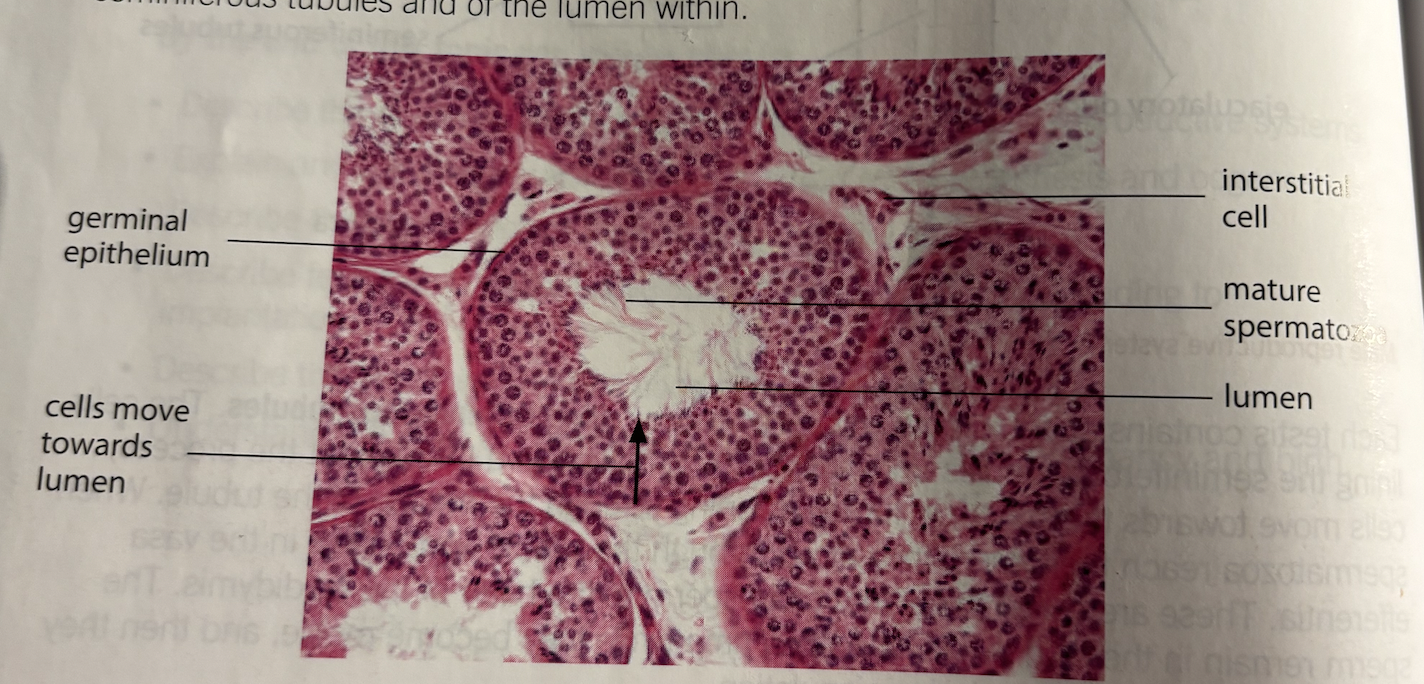
Testis histological examination step
Seminiferous tubules circular
Central lumen
Cells in layers (stages of spermatogenesis)
Sperm near lumen
Leydig between tubules
Sertoli cells large support
Germinal epithelium cells outer (primary spermatocytes)
Spermatozoa tails seen lumen
Circ
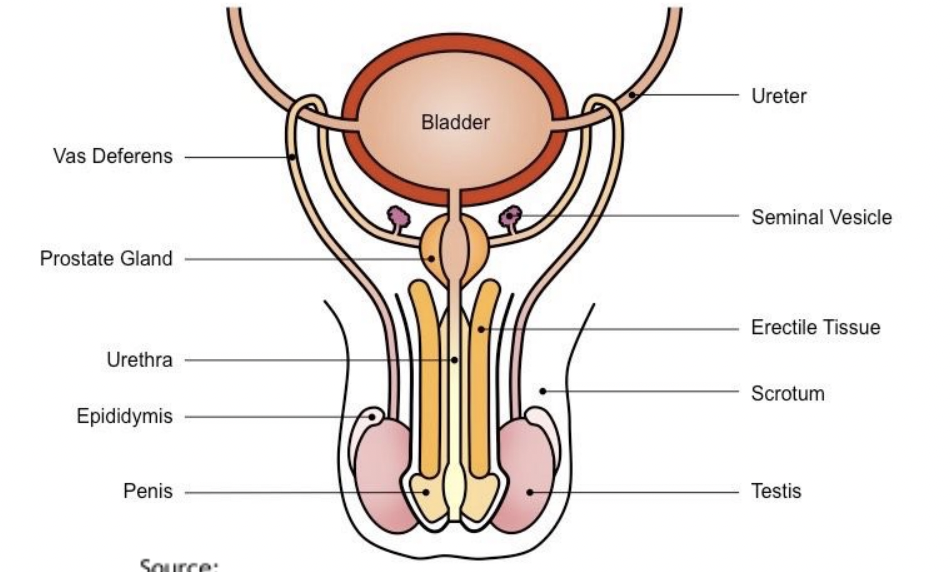
Male reproductive system
Seminal vesicle
Prostate gland
Ejaculatory duct
Vas deferens
Epididymis
Seminiferous tubules
Testis
Urethra
Adaptions of testes
Lots of seminiferous → Large surface area
Cells different development stages
Sertoli cells support sperm
Leydig produce testosterone
Lumen allow sperm release
Ovary
Female reproductive organ produce eggs and hormones
Produce eggs for fertilisation
Secrete oestrogen and progesterone control menstrual cycle
Oviducts
Tube connect ovaries to uterus
Site of fertilisation
Move egg to uterus via cilia and muscular contractions
Uterus
Muscular organ where foetus develop
Site of implantation (not fertilisation)
Provide nutrients and protection for developing embryo
Endometrium
Inner lining of uterus
Thickens each cycle to prepare implantation
Shed during menstruation (if no implantation)
Cervix
Narrow neck connect uterus and vagina
Produce mucus (change during cycle)
Keep foetus in uterus during pregnancy
Vagina
Muscular tube connect uterus to outside body
Receive penis during intercourse
Act as birth canal
Exit for mendtrual flow
Pathway of egg and hormone link
Ovary → Oviduct → Uterus → Cervix → Vagina
Oestrogen → rebuilds endometrium
Progesterone → Maintain endometrium
Histology of Ovary
Outer germinal epithelium
Primary follicles
Secondary follicle
Histology of Secondary follicle
Outer theca cells support follicle
Antrum - fluid filled cavity help. oocyte detach
Secondary oocyte
Haploid metaphase 2
Surround zona pellucida (glycoprotein layer) corona radiata
Three layers of uterus walls
Perimetrium thin outside
Myometrium muscle layer
Endometrium innermost good blood supply shed
Spermatogenesis definition
Process spermatozoa are produced from diploid germinal epithelium in seminiferous tubules of testes
Stages of seprmatogenesis
Spermatogonia (2n) Stem
Divide by mitosis
Primary spermatocytes (2n)
Meiosis I
Secondary spermatocytes (n)
Undergo meiosis II
Spermatids (n)
no tail
Maturation
Spermatozoa (n)
Full developed motile
How many sperm cells does one spermatogonium produce
4 spem cells
Sertoli cells
In seminiferous tubules
Nourish developing sperm
Support spermatogenesis
Blood testis barrier
Leydig cells
Between tubules
Secrete testosterone
Testosterone funciton
Stimulate spermatogenesis
Control male secondary sexual characteristics
Structure of mature sperm cell
Head
Haploid nucleus → genetic material
Acrosome→ enzyme to penetrate egg
Midpiece
Mitochondria packed → ATP for movement
Tail - flagellum
Enable movement
Oogenesis
Process secondary oocyte produced in ovary
Stages of oogenesis
Germinal epithelium
Outer layer of ovary produce oogonia
Oogonia(2n)
Diploid stem
Mitosis( before birth)
Primary oocyte (2n)
Start meiosis 1
Arrested in prophase until puberty
After puberty - Primary oocyte completes meiosis 1
Secondary oocyte (n)
First polar body (n)
Secondary oocyte
Start meiosis 2 stop at metaphase 2
Next stage to secondary oocyte if fertilisation occur
Meiosis 2 completed
Second polar body formed
Ovum (n)
Follicle development
Primary follicle
Primary oocyte surround by follicle cells
Secondary follicle
More granulosa cell layers
Beginning of fluid space
Graafian mature
Large antrum (fluid filled cavity)
Secondar oocyte ready for ovulation
Corpus luteum
Form follicle after ovulation
Secrete progesterone (maintain endometrium)
Structure of secondary oocyte
Corona radiata
Follicle granulosa cells layer protect and nourish ooctye
Zona pellucida
Glycoprotein layer Fertilisation (sperm binding)
Cell membrane - Control entry of sperm
First polar body - small haploid extra chromosomes
Secondary oocyte arrested at metaphase 2
Fertilisation definition
Fusion of haploid nuclei of sperm and secondary oocyte to form diploid zygote
Occur in oviduct
Cortical reaction
Triggered by sperm entry
Cortical granules release enzymes
Zona pellucida modified →fertilisation membrane
Prevent polyspermy
Acrosome reaction
Sperm contact zona pellucida
Acrosome release hydrolase enzymes
Digest zona pellucia
Allow sperm reach oocyte
Capacitation
Increase membrane permeability of sperm
Prepare sperm for acrosome reaction
Process of fertilisation
Sperm reach oviduct
Intercourse sperm vagina→ uterus → oviduct
Capacitation (sperm membrane more permeable)
Acrosome reaction (sperm contacr zona pellucida) release hydrolysing enzymes
Fusion of membrane sperm + secodnary oocyte → Sperm nucleus enter oocyte
Cortical reaction- cortical granules elease enzymes → fertilisation membrane
Complesion of meiosis 2n
Ovum (egg)
Second polar body
Female + male nucleus → diploid zygote
Implantation
Blastocyst embeds into endometrium of uterus
Attach to endometrium
Embed to uterine lining
Endometrium must be thickened maintained by progesterone
Implantation stages
Cleavage (mitosis)
After fertilisation zygote divide repeatedly by mitosis → ball of cells
Formation of blastocyst → hollow ball of cells inner cell mass (future embryo
Blastocyst move oviduct → uterus
Implantation attach endometrium thicken
Placenta formation
Maternal tissue (endometrium)
Foetal tissue (bastocyst)
Placenta formation and fucntion
Maternal tissue (endometrium)
Foetal tissue (blastocyst)
Exchange nutrients, oxygen and waste
Primary oocyte before puberty
Begin meiosis 1
Arrested in prophase 1
Remain dormant until puberty
Difference between primary and secondary oocytes
Primary
Diploid
Arrested in prophase 1
Large
Secondary
Haploid
Arrested in metaphase 2
Small surround by polar body and corona radiata
What happens during ovulation?
Secondary oocyte is released from Graafian follicle
Moves into fallopian tube (oviduct)
First polar body may remain outside or nearby
Follicle develops into corpus luteum
Structure associated with secondary oocyte after ovulation
Corona radiata - Granulosa cells nourish oocyte
Zona pellucida - Glycoprotein layer sperm binding prevent polyspermy
First polar body - Contain extra chromosomes meiosis 1
Cortical granules - Fuse membrane after sperm entry - modify zona pellucida
Cell membrane chromosomes - Secondary oocyte arrested metaphase 2 spindle hold chromosomes for completion of fertilisation
4 Hormones controling menstrual cycle
FSH (follicle stimulating hormone)
LSH (luteinising hormone)
Oestrogen
Progesterone
Stages of menstruation
Menstruation
Low oestrogen + progesterone
Endometrium breaks down
Follicular FSH released from anterior pituitary stimulate
Maturation follicle secrete oestrogen
Oestrogen rise
Repair endometrium
Inhibit FSH + Stimulate LH
LH surge → Ovulation
Follicle → corpus luteum
Progesterone - from corpus luteum maintain endometrium
Inhibit FSH + LH
Menstruation if no fertilisation occur
Corpus luteum breaks down
Progesterone fall
Endometrium breaks down
FSH
Anterior pituitary
Stimulates follicle development
Forms theca → oestrogen
LH
Anterior pituitary
Cause graafian follicle
Pregnancy hCG
Human chorionic Gonadtrophin
Secreted by embryo
Maintain corpus luteum
What happens due to maintaining corpus luteum
Progesterone level stay high
Endometrium maintained
No menstruation
Birth hormone
Oxytocin released by posterior pituitary
Stimulate uterine contractions
Positive feedback of oxytocin
Contractions→ More oxytocin → stronger contractions
Lactation
Prolactin
From anterior pituitary
Stimulate milk production
Oxytocin
cause milk ejection
Early pregnancy
Embryo secrete hCG
hCG maintain corpus luteum
Corpus luteum → continue secrete progesterone
Later pregnancy hormones
Placenta secretes proesterogen + oestrogen
High concentrations
Progesterone
Maintain endometrium
Inhibit uterine contractions
Inhibit FSH LH
Oestrogen
Stimulate growth of uterus
Stimulate development of mammary glands
Labour hormonal cahnges
Oestrogen increase
Progesterone decrease
allow uterus to contract
Oxytocin
Posterior pituitary → uterine contractions
Prolactin
Anterior pituitary
Stimulate milk production
Structures and adaptions of placenta
Chorionic villi
Finger like projections
Contain foetal capillaries
Increase surface area
Intervillous spaces
Fill with maternal blood
Blood vessels
Umbilical artery → foetus → placenta
Umbilical vein → placenta → foetus
Counter-current flow
Maternal and foetal blood opposite directions
Maintain steep concentration gradient
Functions of placenta
Exchange
Oxygen glucose → foetus
Carbon dioxide urea → mother
Barrier
Prevent blood mix
Protect pressure difference
Hormone production
Secrete hCG progesterone and oestrogen
Amniotic fluid
Acts as shock absorber
Protect foetus from damage0
Oestrogen to oxytocin
Oestrogen stimulates oxytocin receptors on uterus make contractions more effective