Public Health and Health Behavior
1/153
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
154 Terms
Three domains of public health?
1. Health improvement - Efforts to aimed at preventing disease, promoting health and reducing inequalities
2. Health protection - Measures to control ID (immunisations), safeguard against emergencies, and environmental hazards
3. Health care - Focus on clinical effectiveness, efficiency, audit, and clinical governance // organisation and delivery of safe, high quality services
What is Health Psychology? Domains?
Study of health behavior, illness behavior, and sick role behavior -
1. Health behaviour - Actions aimed at preventing disease, such as maintaining a healthy diet
2. Illness behaviour - Actions aimed at seeking remedy, such as visiting a doctor
3. Sick role behaviour - Actions aimed at getting well, such as taking medication and resting
What is health behavior
Actions aimed at preventing disease, such as maintaining a healthy diet
What is illness behavior
Actions aimed at seeking remedy, such as visiting a doctor
What is sick role behavior
Actions aimed at getting well, such as taking medication and resting
WHO estimation of medication adherence?
In developed countries, the average is 50%
Health psychology - Interventions at the population level vs individual level?
Health promotion - process of enabling people to exert control over their health
Patient-centred approach - care responsive to individual needs
What is health promotion?
Process of enabling people to control their health, includes:
- Awareness campaigns e.g. 5 a day and every mind matters
- Screening and immunisations
What is patient-centered approach?
Care responsive to individual needs
What is unrealistic optimism?
Continuing health-damaging behaviors due to inaccurate risk and susceptibility perceptions
4 factors influencing perception of risk?
- lack of personal experience
- belief in preventability (by personal action),
- believing that the problem is infrequent
- that if it hasn't happened by now, its not likely to
Transition points named by NICE - aka points in life at which interventions are thought to be more effective? (6)
- leaving school
- entering the workforce
- becoming a parent
- unemployment
- retirement
- bereavement
Name a few models and theories of behaviour change?
- Health belief model
- Theory of planned behaviour
- Trans-theoretical model
- Social norms theory
- Motivational interviewing
- Social marketing
- Nudging (choice of architecture) e.g. fruits and veg near till
- Financial incentives
What is the health belief model?
(Becker, 1974) Perceived barriers have been demonstrated to be the most important factor in addressing behaviour change in patients. Individuals will change if they believe:
1. they are susceptible to the condition
2. that the behaviour has serious consequences
3. that taking action reduces susceptibility
4. that the benefits of acting outweigh costs
Critique the health belief model?
- Does not consider outcome expectancy or self-efficacy
- Does not consider influence of emotions on behaviour
- Does not differentiate between first time and repeat behaviour
What is the theory of planned behavior?
Proposes the best predictor of behaviour change is INTENTION, which is determined by:
1. Personal attitude to the behaviour
2. Social pressure to change behaviour (social norm)
3. Person's perceived behaviour control
Critique the theory of planned behaviour? (4)
- Lacks temporal element or lack of direction and causality
- Doesn't take into account emotions
- Doesn't explain the 3 factors interact to determine intention
- Doesn't take into account habits and routines
Stages of change in the trans-theoretical model
PC-PAM
pre-contemplation, contemplation, preparation, action, maintenance
Critique the trans-theoretical model / advantages of it?
Advantages - accounts for relapse and temporal element
Critique -
- not everyone move through every stage linearly
- change might operate on a continuum rather than discrete stages
- doesn't take into account habits, culture, social and economics
Social norms theory?
Behavior influenced by perceived norms within a social group
Motivational interviewing?
Communication technique to elicit behavior change
Social marketing?
Applying marketing principles to promote behavior change
Nudging?
Choice architecture to encourage desired behaviors, e.g., placing fruits and vegetables near the till
Financial incentives?
Offering rewards to motivate behavior change
Central elements to developing food behaviour (4)?
- maternal diet
- breastfeeding
- parenting practices
- age of food introduction and types of food given
What is Non-organic feeding disorders (NOFED)?
High prevalence in under 6s, includes feeding aversion, food refusal, and negative mealtime interactions
What are the determinants of health?
P - place of residence
R - race
O - occupation
G - gender
R - religion
E - education
S - socio-economic
S - social capital
What is equity? Subtypes of equity?
Differentiate against equality?
Equity = giving people what they need to achieve equal
outcomes
- Subtypes = horizontal and vertical equity
Equality = everyone having an equal share
What is horizontal equity?
Equal treatment for people with equal healthcare needs, regardless of individual characteristics -
e.g. all individuals with pneumonia should be treated equally
What is vertical equity?
Unequal treatment for unequal need, based on individual characteristics - e.g. patients with cold and pneumonia should be treated differently
Define Equality?
Everyone having an equal share
What is the inverse care law?
The availability of good medical care tends to vary inversely with the need for it in the population served
Levels of interventions in public health? Examples?
- Individual - e.g. immunisation
- Community - on a local level e.g. community and playgrounds
- Ecological (population) e.g. clean air act, legislation to ban smoking in public places
What is a health needs assessment?
= resource allocation
Systematic method for reviewing health issues facing a population, setting priorities and allocating resources to improve health and reduce inequalities
NICE definition of need?
- 2017 SAQ (1 mark)
ability to benefit from an intervention
NICE definition of demand? & supply?
what individuals ask for / what is provided (i.e. the services that are available)
Four types of social needs as deemed by Bradshaw (1972)?
Normative need
Felt need
Expressed need (demanded need)
Comparative Need
Define normative need & give an example?
Need that is defined by experts. Normative needs are not absolute and there may be different standards laid down by different experts.
Vaccinations // a decision by a surgeon that a patient needs an operation
Define felt need & give an example?
Need perceived by an individual. Felt needs are limited by individual perceptions and knowledge of services.
Having a headache, feeling knee pain
Define expressed / demanded need & give an example?
Felt needs turned into action. Help seeking.
Going to the dentist for a toothache
Define comparative need & give an example?
Needs identified by comparing the services received by one group of individuals with those received by another comparable group.
A rural village may identify a need for a well or a school if the neighbouring village has one
What is an example of a health related intervention that is supplied, but not needed or demanded? Why?
- 2017 3a SAQ (1 mark) (1 mark)
Routine Caesarean sections on women with a history of a previous Caesarean section
What is an example of a health related intervention that is supplied, needed but not demanded? Why?
- 2017 SAQ (1 mark) (1 mark)
Health promotion; screening procedures; psychiatric treatment; vaccinations
What is an example of a health related intervention that is supplied and demanded, but not needed?
- prescription of antibiotics for uncomplicated viral URTI / mild infection
- vitamins
- over the counter antibiotics
What is an example of a health related intervention that is demanded and needed but not supplied?
Elective procedures being delayed by large waiting lists
Approaches to health needs assessment
Epidemiological, corporate, and comparative approaches
How might an epidemiological approach to health needs look like?
- 2017 SAQ (2 marks)
Considers the
- epidemiology of the condition (inci + prev + morb + mort)
- current service provision
- effectiveness and cost-effectiveness of interventions and services
- Data is from: disease registry, hospital admissions, GP databases, mortality data, primary data collection
Critique the epidemiological approach to health needs?
ADV
- uses existing data
- provides data on disease incidence / mortality / morbidity
DISADV
- quality of data variable
- data collected may not be data required
- does not consider felt needs / opinions of patients
How might a corporate approach to health needs look like?
- 2017 SAQ (1 mark)
Asking the local population what their health needs are
- Use of focus groups, interviews and public meetings
- Wide variety of stakeholder e.g. teachers, healthcare professionals, social workers, charity works, local businesses, council workers and politicians
Critique the corporate approach to health needs?
ADV
- based on felt and expressed needs to population
- Recognise detailed knowledge and experiences of those working with population
- takes into account wider range of views
DISADV
- can be difficult to distinguish need from demand
- groups may have vested interests
- may have political agendas
How might a comparative approach to health needs look like?
- 2017 SAQ (1 mark)
- Compare the needs/provision of healthcare in one population with another
- Can be spatial (e.g. different towns) or social (e.g. two age groups in the same town)
Critique the comparative approach to health needs?
- 2017 SAQ (1 mark)
ADV
- quick and cheap if data available
- shows quality of service in the compared groups
DISADV
- can be difficult to find comparable population
- data may not be available / high quality
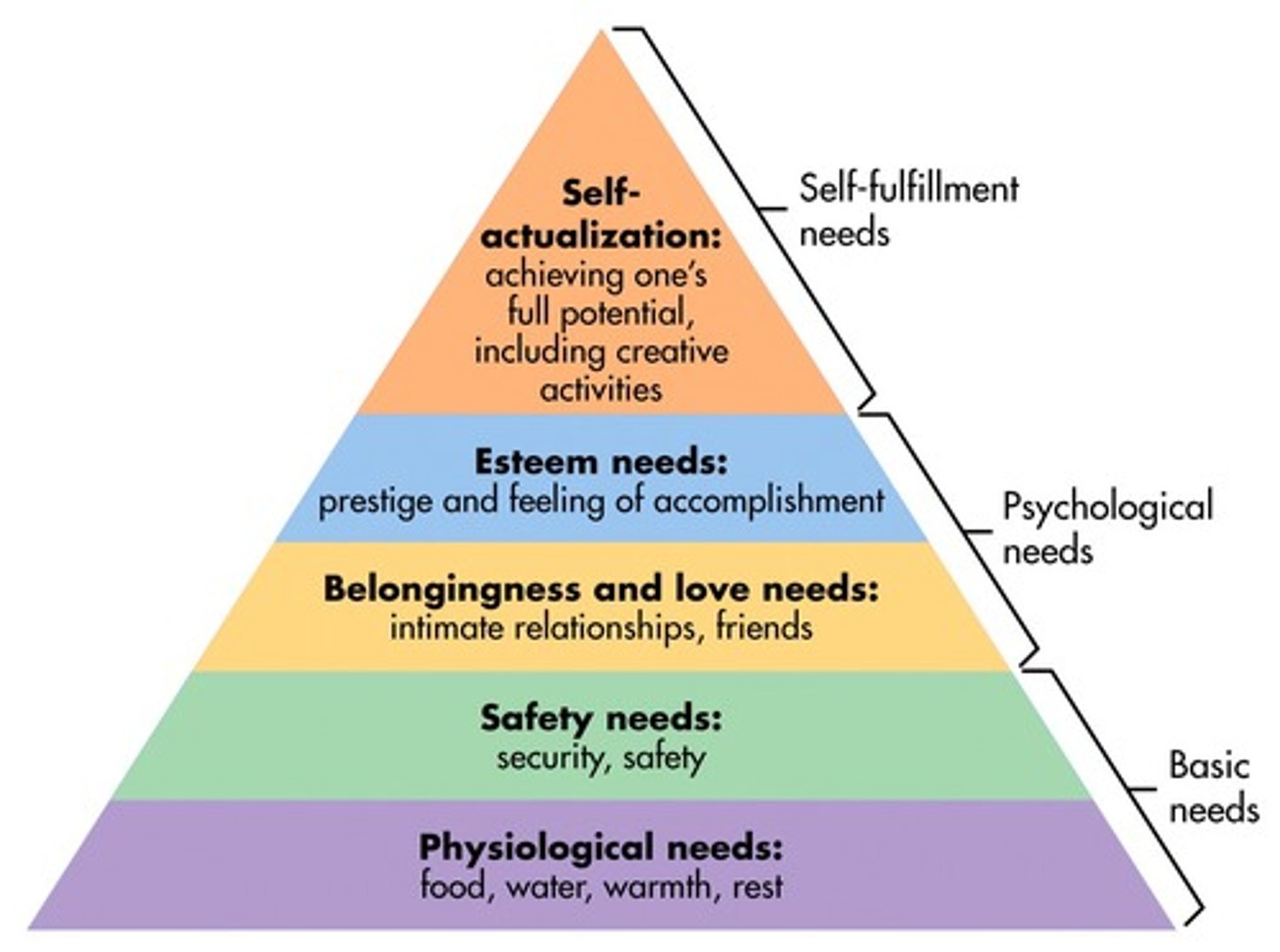
Maslow's hierarchy of needs - describe and what is self-actualization?
Self-actualization - a person's motivation to reach their full potential. Their basic needs must be met before actual self-actualization can be achieved.
- this includes morality, creativity, spontaneity, problem solving, lack of prejudice
Pyramid =
Self-actualization
Esteem
Love / belonging
Safety
Physiological
3 Resource allocation methods and what are they based on?
Egalitarian - Provide all care that is necessary and required to everyone
(equal but expensive)
Maximising - based solely on consequences
(resources allocated to those most likely to benefit, but those who don't make the cut receives nothing)
Libertarian - Each individual responsible for own health
(promotes positive engagement, but most diseases are not self inflicted)
What is utilitarianism?
Consequences of an action should be measured by effects - greatest good for the greatest number of people
What is deontology?
DUTY BASED ETHICS, right or wrong are decided based on the action,
It specifically does not look to consequences of actions to determine right or wrong. Instead it examines a situation for the existence of essential right or wrong.
What is the opposite of deontology?
Duty based ethics - right or wrong is dependent on the situation / circumstance
What is virtue ethics?
Actions are judged based on the character of the individual carrying out the action
= Based on the virtues they hold
Define evaluation? Provide examples of evaluation frameworks?
Assessment of whether a service achieves its objectives
e.g. Donabedian's framework of health service evaluation, Maxwell's dimensions of Quality of health
What is Donabedian's framework of health service evaluation? What does it include?
A framework used to evaluate health services - Donabedian's looks at the structure, process and outcome of the health service.
- Structure: actually is the service e.g. how many heart surgeons there are
- Process - how does the process work
- Outcome - 5 Ds = death, disease, disability, discomfort, dissatisfaction
Issues with the way Donabedian's framework evaluates the health service?
▪ Link between health service and health outcome can be difficult to confirm
▪ Time lag between service and outcome may be long
▪ Large sample sizes may be needed
▪ Data may not be available or have a problem with it (CART = completeness, accuracy, relevance, timeliness)
What is Maxwell's Dimensions of Quality of health care
A framework used to evaluate health services - Maxwells looks at the 3E's & 3A's:
- Effectiveness, efficiency, equity
- Acceptability, accessibility, & appropriateness
What processes are in a health needs assessment?
Needs assessment - Planning - Implementation - Evaluation
What is epidemiology?
The study of the frequency, distribution and determinants of diseases and health-related states in populations in order to prevent and control disease.
Define Incidence
- 2018 3b SAQ (1 mark)
Number of new cases in a population over a period of time
Define (point) Prevalence
- 2018 3b SAQ (1 mark)
Number of existing cases in a population at a particular point in time
Define Absolute risk
the incidence of disease in a population - with specific numbers and units
Define Relative risk
Risk in one category compared to another
= risk in exposed group A / risk in unexposed group B
Define Attributable risk
Rate of disease in the exposed population that maybe attributed to exposure
= risk of control grp - risk of exposed group = excess risk caused by exposure
Define number needed to treat?
average number of patients who need to be treated to prevent one additional bad outcome
= inverse of absolute risk (1 / AR)
Define Bias?
A systemic deviation from the true estimation of the association between exposure and outcome
= example of a systematic error
Types of bias:
- selection bias
- information bias
- allocation bias
- publication bias
- lead time bias
- length time bias
Name four information bias? Explain?
Measurement bias
- diff equip measuring differently
Observer bias
- observer expectations influence reporting
Recall bias
- past events not recalled correctly
Reporting bias
- ppl don't report the truth due to shame / judgement
Define selection bias?
unintended differences between the participants in different groups - may present during the selection or allocation process
Define Information bias?
errors in procedures for gathering relevant information
-ex: in recall, collecting data, interviews & reporting
Define publication bias?
bias that occurs when research that is published isn't representative of all completed studies - trials with negative results are less likely to be published
Define lead time bias?
Screening identifies diseases earlier and therefore gives the impression that survival is prolonged but survival time is actually unchanged.
Define length time bias?
diseases that progress rapidly from onset to symptoms are less likely to be detected by screening than disease that progresses slowly - screening identifies more tx-responsive subgroup
Define Confounding factors?
- 2018 3b SAQ
Factor associated with exposure and outcome but not on the causal pathway
e.g. smoking causes lung cancer but alcohol consumption is associated with both (dependence, lifestyle etc)
What is the Bradford Hill criteria for causality?
•In 1965 Austin Bradford-Hill detailed criteria for assessing evidence of causation:
- Strength
- Dose-response
- Consistency
- Specificity
- Temporality
- Biological plausibility
- Coherence
- Analogy
Meeting the Bradford-Hill criteria confirms:
True association
What is reverse causality?
A situation in which one variable is said to cause another variable, when in reality the reverse is true.
e.g. stress could have caused HTN rather than HTN causing stress
Types of prevention? Explain?
PRIMARY - preventing a disease before it happens
- vaccines
SECONDARY - catching a disease in the early/pre-clincical phase & prevent it from worsening
- screening
TERTIARY - preventing complications of disease
- prevent worsening renal function in CKD
(2) Approaches to prevention? Explain?
POPULATION BASED - Preventative measure delivered on a population wide basis (or to a relevant subgroup)
Seeks to shift the risk factor distribution curve
E.g. dietary salt reduction through legislation, working with the food industry reformulation, PH advice to the general public should shift the blood, pressure distribution curve to the left
HIGH RISK APPROACH - Identifies and treats individuals above a chosen cut-off
E.g. screening for people with high blood pressure and treating them
What is the prevention paradox?
A preventative measure that benefits the population but offers little to each individual
E.g. If all male British doctors wore their car seat belts on every journey throughout their working lives, then for one life saved there would be 400 who never benefit from it.
Types of disease screening (5)?
- Population-based
- opportunistic
- communicable diseases
- pre-employment
- commercially provided
What is the criteria for screening disease used by the NHS? Broadly describe the criteria?
Wilson and Junger criteria.
Condition - should be important. Hx, staging, RF & disease markers should be understood.
Screening should be ongoing and not one off. Cost effective.
Test - simple, safe, precise and validated screening. Acceptable to population. Target population, distribution of results and cut off defined and agreed. Agreed policy on further diagnosis of those with + results and choices available.
Treatment - effective intervention / tx available for those identified, and evidence exists of early tx giving better outcomes than late. Agreed policy on who to tx and facilities available.
Wilson and Jungner criteria - explain for 6 points?
In Exam Season NAP
Important disease
Effective tx available
Simple and safe
Natural hx of disease known
Acceptable (not too invasive)
Policy on who to treat agreed
Disadvantages of screening?
- exposure of well individuals to distressing or harmful diagnostic tests
- detection and treatment of sub-clinical diseases that would never cause any problems
- preventative measures may cause harm to individual or population
Young people and adult screening programmes?
AAA
Bowel cancer
Breast cancer
Cervical screening
Diabetic eye
Define sensitivity? Formula?
the ability of a test to correctly identify those who actually have the disease (true positives)
TP/(TP + FN)
Define specificity? Formula?
the ability of a test to correctly identify those who do not actually have the disease
proportion of people without disease correctly excluded by screening test
TN/(TN + FP)
What is a positive predictive value?
Probability that a pt w/ a positive test truly has the disease.
The more specific a test, the higher its PPV
Prevalence dependent: the higher the disease prevalence, the higher the PPV of the test for that disease
What is a negative predictive value?
Probability that a pt w/ a neg test truly does not have the disease.
The more sensitive a test, the higher its NPV.
Prevalence dependent: the lower the disease prevalence, the higher the NPV of the test for that disease
What is a cohort study?
preplanned following at least two subset (exposed vs unexposed) of population over a period of time
incidence of disease compared.
observational and prospective. uses relative risk.
Advantages and disadvantages of cohort studies?
ADV
- Follow up rare exposures
- Identifies risk factors
- Sequence of happenings can prove cause-effect
- Multiple exposure and outcomes can be measured
DISADV
- Expensive and time consuming.
- Large sample size required
- Impractical for rare diseases / long latent periods
- Subjects may be lost to follow-up during the course of the study.
- Exposures can be misclassified.
What are case-control studies?
Retrospective look on subjects that have the outcome of interest
Groups with and without a disease are selected and past exposures identified
Advantages and disadvantages of case control studies?
ADV
- quick
- good for rare & long latency diseases
- multiple exposures can be studied
DISADV
- selection & information bias
- impractical for rare exposures
- hard to establish sequence of events
- difficult to tell apart confounding factors
What is a cross-sectional study?
exposure and outcome are measured simultaneously at a particular point (snapshot study)
Advantages and disadvantages of cross-sectional studies?
ADV
- Can assess a large sample size
- Quick
- Provides prevalence data
- Provides trend data
- Hypothesis generating
- Can rptx = show change overtime
DISADV
- Risk of reverse causality
- Unclear timeline
- Not useful in rare diseases
- Difficult to establish an in-depth developmental assessment of the interrelationships of the phenomena
What is a randomised control trial?
a study where a group of STRICTLY SELECTED participants are then RANDOMLY ALLOCATED to either an experimental group or a control group
Allows for comparison in order to assess the effectiveness of an intervention