image intensification fluoroscopy
1/55
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
56 Terms
what are the three types of fluoroscopy
direct/conventional fluoroscopy
image intensification tube
digital systems
what is the fluoroscopic imaging capability that provides single-capture still images similar to radiography
static (spot film)
what is the fluoroscopic imaging capability that provides continous real-time imaging in motion
dynamic (fluoroscopy, cinefluoroscopy)
what is the actual recording of the dynamic imaging
cinematic
cine-fluoroscopy
“cine”
rods
night vision
black and white only
takes longer to adaptwh
what is the scientific name for night vision
scotopic
cones
photopic vision
detects color and fine detail
adapt quickly
are rods or cones used in fluoro
rods
what does the image intensifier do
converts X-rays into a visible light image of high intensity
how much does the image intensifier amplify image brightness
increases brightness 500-800 times
automatic brightness control (ABC) AKA
automatic exposure rate control (AERC)
this automatically adjusts exposure factors in response to variations in thickness and density of anatomy or contrast material during fluoroscopy
automatic brightness control (ABC)
the concentration of photoelectrons at the input phosphor compared to the output phosphor
minification gain
this is a type of blooming that is described as a contrast reducing haze on the image
veiling glare
what is veil glare caused by
scattering of x ray light
electrons inside the image intensifier tube
how is veil glare fixed
use a grid
use appropriate collimation
the measure of the ability of the image intensifier to increase the brightness level of the image
brightness gain
kinetic energy gained by photoelectrons as they are accelerated from the photocathode to the output phosphor
flux gain
this is a decrease in image brightness
vignetting
what is vignetting caused by
curved input phosphor and object to image distance
what does vignetting effect
reduces contrast and image detail on the edges of the image
how do you correct vignetting
image processing
adjust II
reducing OID
what does the input phosphor of the II tube do
converts incoming x ray photons into visible light photons
helps in reducing image noise and improving contrast
what does the output phosphor do
converts accelerated electrons back into visible light photons
produces the final intensified image displayed on the monitor
what does the anode do
a positively charged component that attracts and accelerates electrons towards the ouput phosphor
plays a role in image brightness and contrast enhancement
what does the photocathode do
comprised of photoemissive metal: cesium and antimony
in direct contact with the input phosphor to prevent divergence of the light
photoemissive material that absorbs the light photons and emits electrons via photoemission
what do the electrostatic focusing lenses do
series of charged electrodes that focus and accelerate electrons
directs electrons towards the anode
helps in maintaining image clarity and magnification control
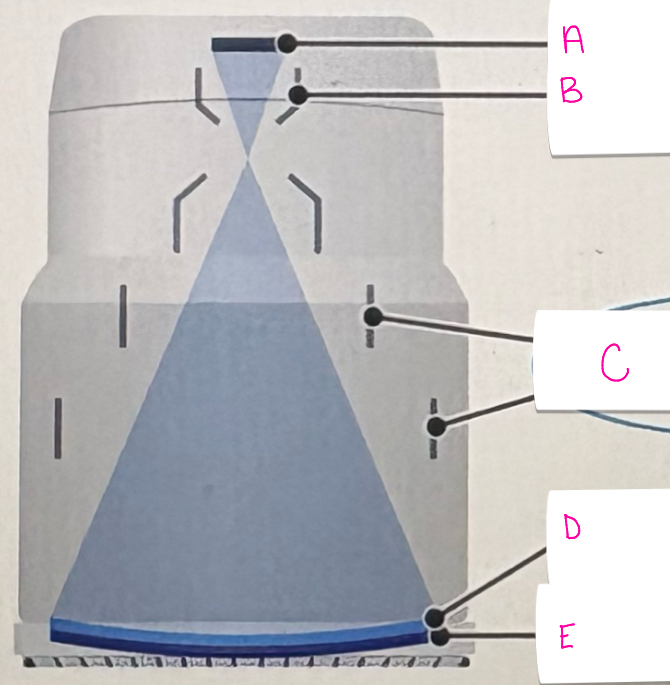
what does letter A demonstrate
output phosphor
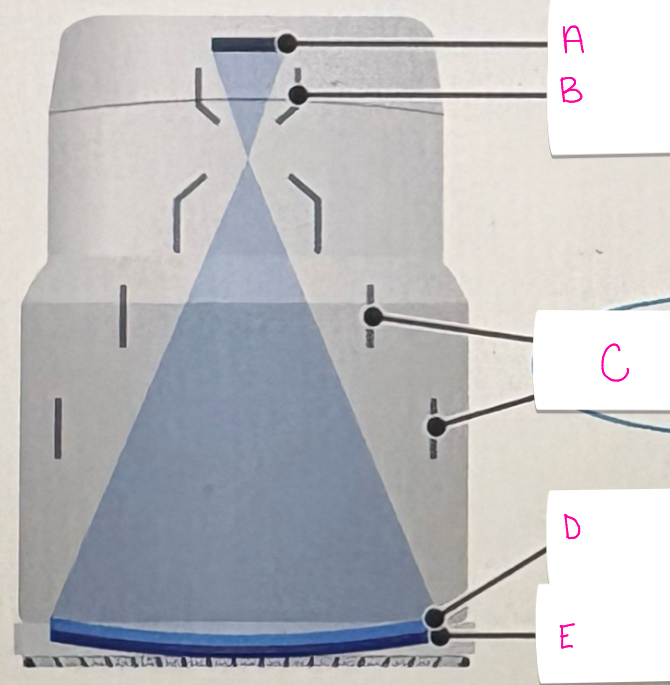
what does letter B demonstrate
anode
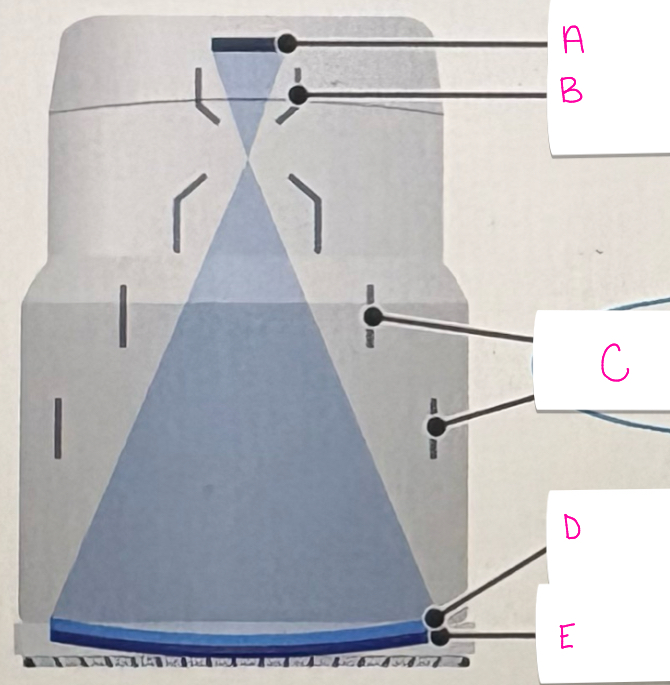
what does letter C demonstrate
electrostatic focusing lenses
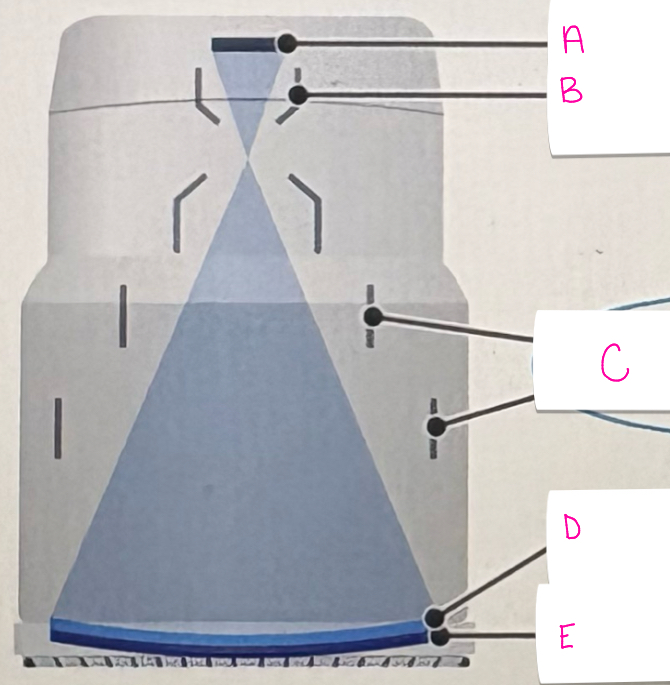
what does letter D demonstrate
photocathode
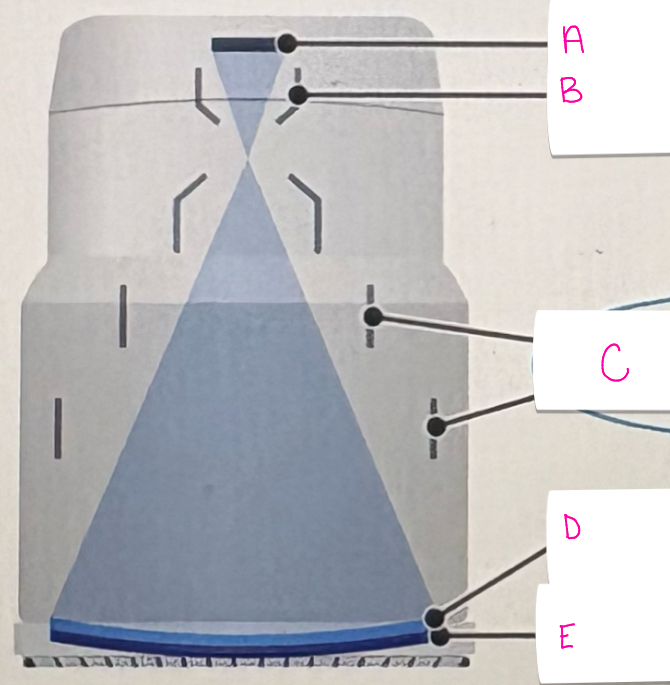
what does letter E represent
input phosphor
what is the input phosphot made of
cesium iodide
what is the output phosphor made of
zinc cadmium sulfide
what is the minimum SSD for fixed units
15” or 38 cm
what is the minimum SSD for mobile units
12” or 30 cm
what is photoemission
absorbs light photons and emits electrons
where does photoemission occur
in the photocathode
what is the mA range used in fluoroscopy
0.5 - 5.0mA
what happens to patient dose when frames per second increase
when frames per second increases = patient dose increases
what happens to patient dose when frames per second decreases
when frames per second decreases = patient dose decreases
what happens to patient dose when magnification mode is used
when magnification mode is used patient dose increases
where is the tube located in fluoroscopy
located under the patient
what is the image intensification tube enclosed with and what does that maintain
enclosed in a glass envelope to maintain a vaccum
what part of the II tube is concave and the largest
input phosphor
what happens to magnification when the focal point moves
magnification occurs when focal point moves closer to input and farther from output
what happens to contrast with magnification
better contrast resolution
what happens to FOV with magnification
decreased FOV
after how long of fluoro will the alarm sound
after 5 minutes of continuous fluoroscopy
what is the function of the CCD and CMOS in fluoro
the electrical device that collects light photons from the output phosphor and converts them into electrons
what is the unit of measure for luminous intensity
candelas
what is the output phosphor measured in
candelas
what is the source of technologist radiation
the patient is the primary source of technologist radiation
what are the radiation protections steps the technologist should take
if you are in the room stand behind the radiologist
tube should always be under the patient if possible
stand on the II side of the c-arm
what is backscatter
the largest amount of scatter radiation is produced where the x ray beam enters the patient
where should you stand to receive the least dose
stand on the image receptor (intensifier II side) of the c-arm