Pregnancy
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
Retaining the embryo, or product of fertilization, inside the mother’s body for a period of time
What is embryo retention?
Advantages- Predator avoidance, precociality, partitioning of niches
Disadvantages- Risk of predation, energetic cost, death if mom dies, possible matings decrease
Can you name one advantage and one disadvantages/trade off w/fecundity?
Cilia move the fertilized egg to the uterus
An experiment in which a portion of the oviduct was removed and reinserted in reverse prevented implantation (cilia were beating in reverse)
How does the fertilized egg move to the uterus? What data support this?
The conceptus breaking away from the ZP
The conceptus cannot implant while inside the ZP
What is zona hatching, and why does it occur?
Protection from the mom’s immune system, keeps conceptus cells together, protection from merging with another conceptus
What protection is lost during zona hatching?
Yes
Does zona hatching need to occur prior to implantation?
Invasive
Can you name the type of implantation humans have?
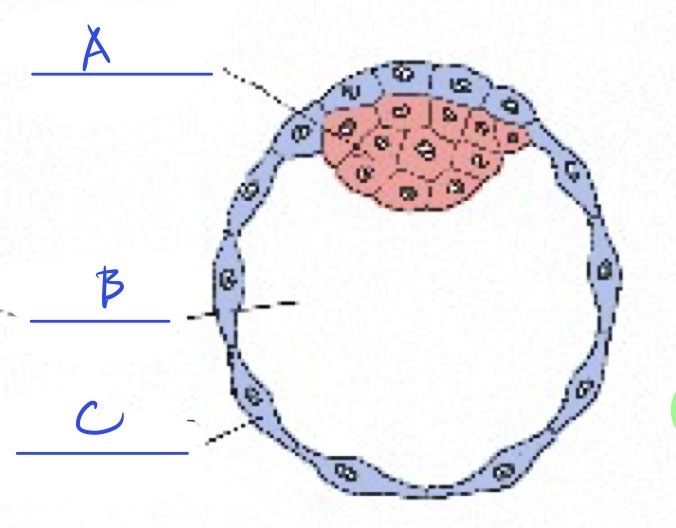
A. Inner cell mass
B. Blastoceole
C. Trophoblast
Can you ID the parts of a blastocyst mentioned in class?
The hatched blastocyst attaches to the stratum functionalis (unstable to stable) and invades it 7-10 days after fertilization
How does implantation occur (general)?
The blastocyst in the posterior fundus
What implants during implantation, where?
Remove mucin glycoproteins
Remove long microvilli
Form pinopodes
What are the changes in the endometrium during the “transition to receptivity” in the uterus and what mediates these changes on an endocrine and molecular level?
It must face the SF
What direction must the ICM face during implantation?
The blastocyst “rolls” so that the inner cell mass faces the stratum functionalis
The trophoblast of the blastocyst secretes cytokines (IL-1)
The SF secretes LIF from endometrial glands in response to IL-1, signaling receptivity to LIF receptors on the blastocyst
What happens during the first process of attachment to the endometrium- what short range signals are secreted by the trophoblast and by the SF (showing SF is receptive!)?
Decidualization
What is the name of the process that happens to the cells of the SF to prime the endometrium?
The endometrium is not primed for invasion (the 3 changes cannot occur)
What happens if decidualization does not occur?
Attachment of the trophoblast is is made more stable with cell adhesion molecules
Both trophoblast and SF secrete prostaglandins
Local increases of vascular permeability causes serum proteins to leak into the site of implantation
Fibroblasts release MMPs
Trophoblast of blastocyst release MMPs and TIMPs, lysing the epithelial cells of the SF
The materials of the lysed cells are used by the blastocyst
Blastocyst “buries” itself into the SF
SF heals over blastocyst
What happens during the process of invasion?
Give the fetus oxygen, glucose, and other nutrients, and removes toxins and wastes
What are the functions of the placenta?
The mom’s blood enters the placenta on the mom’s side and exchanges nutrients and oxygen to the fetus’s side
How are nutrients and oxygen brought to the fetus?
No
Do mom and baby blood mix?
Induces relaxation of the GI tract which slows digestion
What does high progesterone do to the GI tract during pregnancy?
More nutrients can get pulled out for the fetus
Why is slowed digestion in the mom good for the fetus?
12 months
How long is it recommended to breastfeed an infant (as possible)?
Yes, decreases the chances that the mom will eat something bad that will harm the fetus
Is NVP (morning sickness) beneficial to the fetus?
hCG
What hormone is detected for the pregnancy test?
This indicates the presence of a conceptus secreting hCG (from syncytiotrophoblast)
Why is hCG used for pregnancy tests (and what secretes it)?
The corpus luteum is rescued, progesterone production continues (the uterine lining is kept and the myometrium stays quiet)
What is the result of hCG being present in the woman’s body?
hCG from the syncytiotrophoblast
What is the long range signal secreted by the embryo to the mom?
The CL is not rescused, progesterone drops, the SF is shed, and the conceptus is lost
What happens if the hCG signal does not occur?
Cortisol from the fetal adrenal glands travels through the placenta, increasing placental estrogen production and decreasing progesterone production/reduces progesterone receptors
Increase in estrogen causes the myometrium to begin contractions
What triggers parturition at the endocrine level?
Decrease in progesterone causes myometrium to begin contracting
Stretch receptors in the cervix signal release of oxytocin from the neurohypophysis
Oxytocin causes more contractions
Even more pressure signals even more oxytocin to be released until birth
How do increases in oxytocin and decreases in progesterone/PR (humans!) contribute to progression of labor?
Relaxin and prostaglandins upregulate MMPs from fibroblasts, which then decrease collagen and help rearrange collagen fibers in the cervix. Hyaluronic acid draws water around collagen fibers. All of these events result in a thinned, softened cervix
How do relaxin, prostaglandins, hyaluronic acid, and MMPs contribute to cervical changes?
Dilation
What is the name of what happens to the cervix during labor onset?
Muscle fibers of the myometrium contract and but do not relax all the way, getting shorter and shorter with each contraction
What is brachystasis?