Lab Practical #2
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
Arteries: Elastic
Close to the heart
Large
Most expandable
Arteries: Muscular
medium sized
named arteries in the body
Arteries: Arterioles
smallest
“Resistance vessels”
Blood vessels: Capillaries
provide exchange of materials in tissues
narrowest vessel
one cell layer - endothelium
Blood vessels: Veins
65% of blood volume is in the veins
low pressure because of thin walls and large lumens
veins draining into the vena cavae
Draining the arm:
radial and ulnar veins - brachial vein - axillary vein
Subclavian vein recieves:
Venous blood from axillary vein
Venous blood from skin and muscles of head and neck via external jugular vein
Internal jugular vein drains the dural sinuses of brain
Left and right brachiocephalic veins recieve veniys blood from:
subclavian veins
vertebral veins
internal jugular veins
Path of blood through circulatory system
Heart - large arteries - medium arteries - arterioles - capillary beds - venules - mediium veins - large veins - heart
Pulmonary Circulation
Capillary beds exchange around alveoli permit gas exchange (CO2 for O2)
Nourishing blood supply for the lungs provided by bronchial arteries, not pulmonary circulation
Hepatic portal system
veins drain the:
digestive system
spleen
pancreas
major veins
inferior and superior mesenteric veins
splenic vein
left gastric vein
Capillary beds of digestive system absorb nutrients
liver helps maintain proper glucose, fat and protein cconcentrations
Liver filters toxins
Blood drains into hepatic veins as it leaves liver
Fetal circulation
Fetus receives exchanges of gases, nutrients, and wastes through the placenta
Umbilical cord vessels:
umbilical vein - carries blood rish in nutrients and oxygen to fetus
umbilical arteries (2) - carry carbon dioxide from fetus to placenta
Blood flow bypasses liver through the ductus venosus and enters interior vena cava
Blood flow bypasses the lungs
blood enters right atrium and is shunted to left atrium through foramen ovale
ductous arteriosus connects aorta and pulmonary trunk
Cerebral arterial circle
Circle of Willis - protects brain blood supplly if one artery is blocked or narrowed. It reroutes blood
Internal carotid arteries divide into anterior and middle cerebral arteries
supply most of cerebrum
Vertebral arteries join once within the skull to form basilar artery
posterior cerebral arteries form from the division of the basilar artery
Phases of cardiac cycle
atrial diastole - blood delivered into atria via veins
80% of blood flows passively into ventricles
artrial systole
last 20%of blood left in atria delivered to ventricles by atrial systole
ventricular systole
ventricular contractions - closing the AV valves
ejection phase - blood pumped into great arteries
ventricular diastole
Pulse
Surges of pressure in arteries - heart rate
Normal range for resting: 60-100 bpm
Average resting heart rate: 70-76 bpm
60 sec / heart beat duration
Blood pressure
pressure exerted against walls of arteries
systolic blood pressure: pressure against walls of arteries during ventricular systole
diastolic blood pressure: pressure against the arterial wall during ventricular diastole
SDP/DBP mmHg
Calculating overall blood pressure
CO = SV x HR
BP = CO x TPR
CO - amount of blood pumped by the heart in one minute
SV - amount of blood pumped by left ventricle during one contraction
TPR - amount of force exerted on circulating blood by the vasculature
Pulse pressure
SBP - DBP
MAP
DBP + (pulse pressure/3)
or
(SBP + (2 x DBP)) / 3
Heart sounds
1st sound: lub - closure of AV valves
2nd sound: dub - closure of SL valves
Heart murmur
abnormal heart sound
indicated a defect in one of the valves
Upper division:
structures found in head and neck
external nose, nasal cavity, paranasal cavity and pharynx
Functions
dilters, warms and moistens incoming air
chamber for voice
smell
Upper division: pharynx
connects nasal and oral cavities to larynx and esophogus
Nasopharynx
respiration
Oropharynx
respiratory and digestive functions
Laryngopharynx
respiratory and digestive
Lower divison: larynx
prevents food/fluid from entering lungs
allows passage of air and produces sound
composed of cartiaginous and membranous structures
Cartilages of larynx
thyroid (Adams apple)
cricoid cartilage
Arytenoid carteliage - anchors vocal folds
epiglottis - closes opening of trachea during swallowing
Lower division: trachea
walls reinforced with C-rings of hyaline cartilage
lined wit pseudostratified ciliated columnar epithelium
Lower division: bronchi
branching respiratory tubes
divides into right and left plmonary bronchi
Lower division: lungs
soft: spongy organs
Cardiac notch
concavity or left lung that provides space for the heart
left lung - 2 lobes
right lung - 3 lobes
Plurae of lungs
pariteal pleura - outer layer that attach thoracic walls and diaphragm
visceral pleura - inner layer, cover external surface of lung
process of respiration
1) pulmonary ventilation
2) external respiration - gas exchange
3) transport of respiratory gasses to tissues
internal respiration - gas exchange between blood and tissues
mechanics of respiration
inspiration - air moves to lungs
thoracic cavity increase in size
intrapulmonary volume increases
intrapulmonary volume decreases
air flows to area of low pressure (in lungs)
expiration - air moves out of lungs
thoracic cavity decreases in size
intrapulmonary volume decreases
intrapulmonary pressure increases
air flows to area of low pressure (out of lungs)
bronchial sounds
produced by air rushing through the large respiratory passageways
abornmal sounds - wheezing, rales
diseased tissue, mucus or pus
Obstructive diseases
increased resistance in airways
normal vital capcity but decrease rate of air flow due to bronchoconstriction
asthma, chronic bronchitis
Restrictive disease
lung capacity declines
Polio, tuberculosis
Carbonic acid-bicardbonate buffer systems
Arterial blood pH is maintained at 7.4 by buffer system
CO2 diffuses into blood from tissues
in red blood cells CO2 combines with H20 to form H2Co3 - carbonic acid
H2CO3 breaks down into HCO3 - biocarbonate ion and H+
H+ are neutralized by attaching onto hemoglobin
HCO3 moves into plasma
How buffer system maintains blood pH
If pH decreases - increase in H+
If pH increases - decrease in H+
Hyperventilation
fast deep breathing
decreased carbonic acid and H+
results in alkalosis - higher than normal pH
Hypoventilation
slow or shallow breathing
increased carbonic acid and H+
results in respirator acidosis - lower than normal pH
Tidal volume
amount of air inhaled or exhaled in a normal breath
ERV
expiratory reserve volume - max amount of air exhaled after normal breath
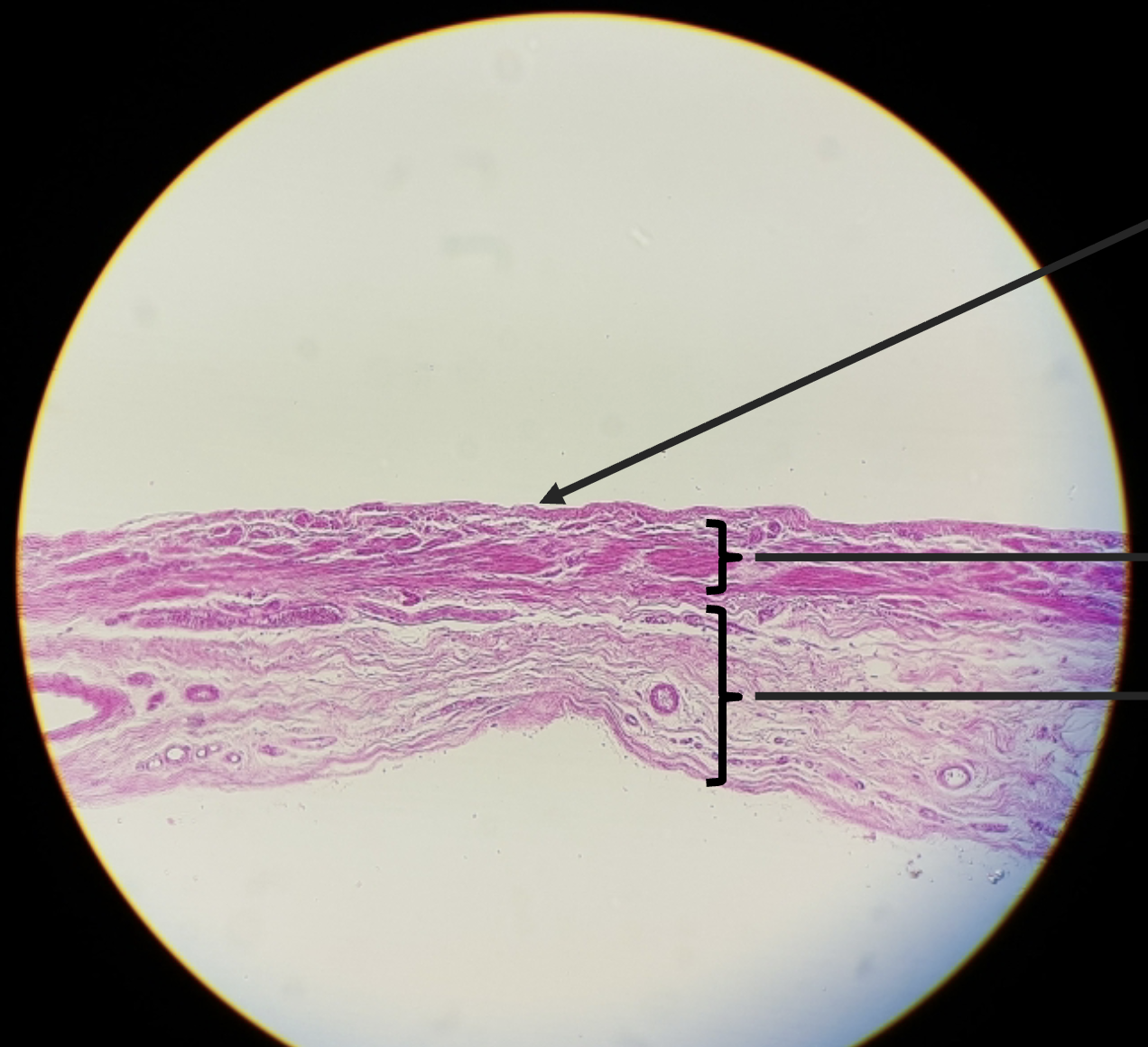
Vena cava
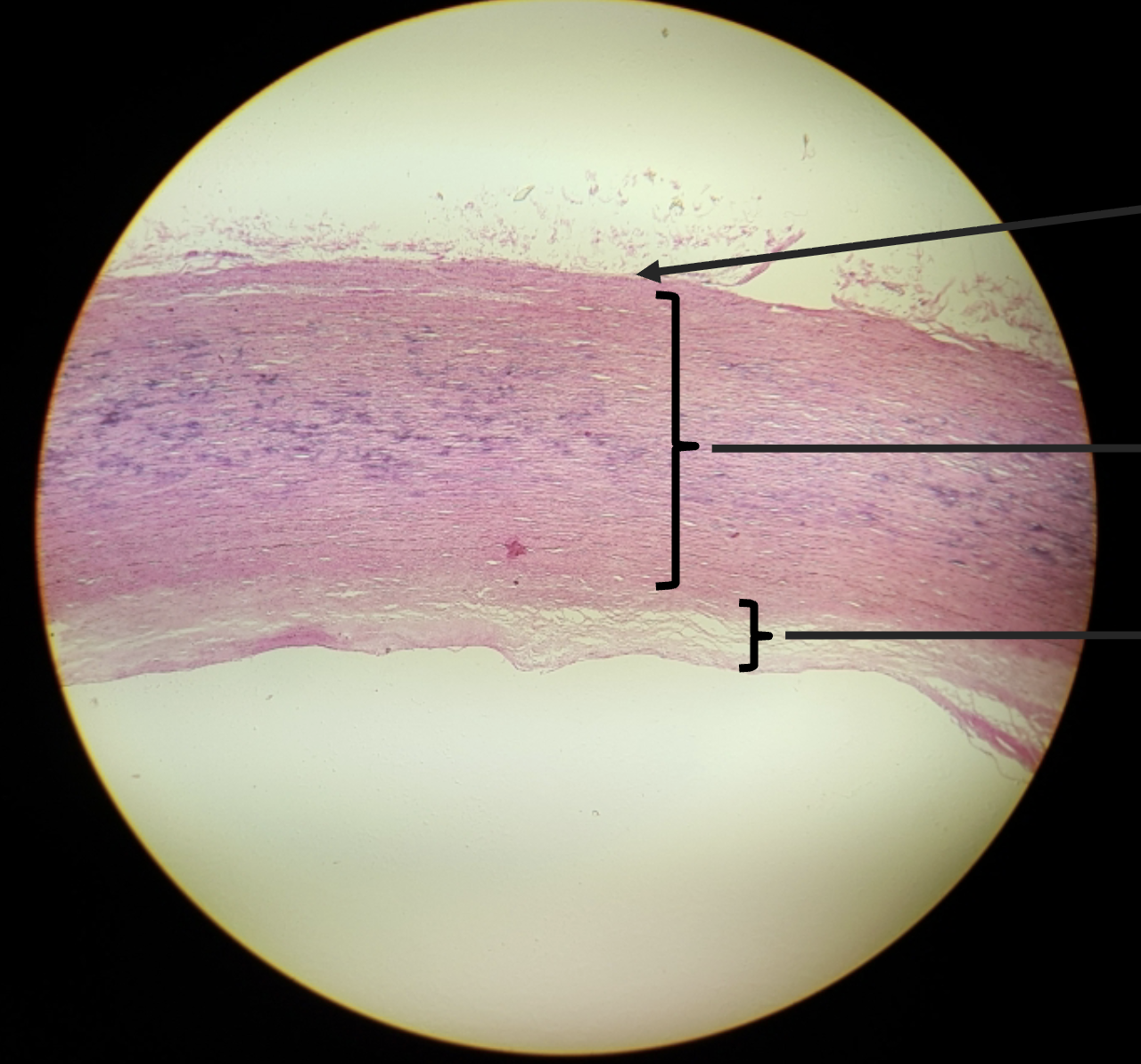
Aorta
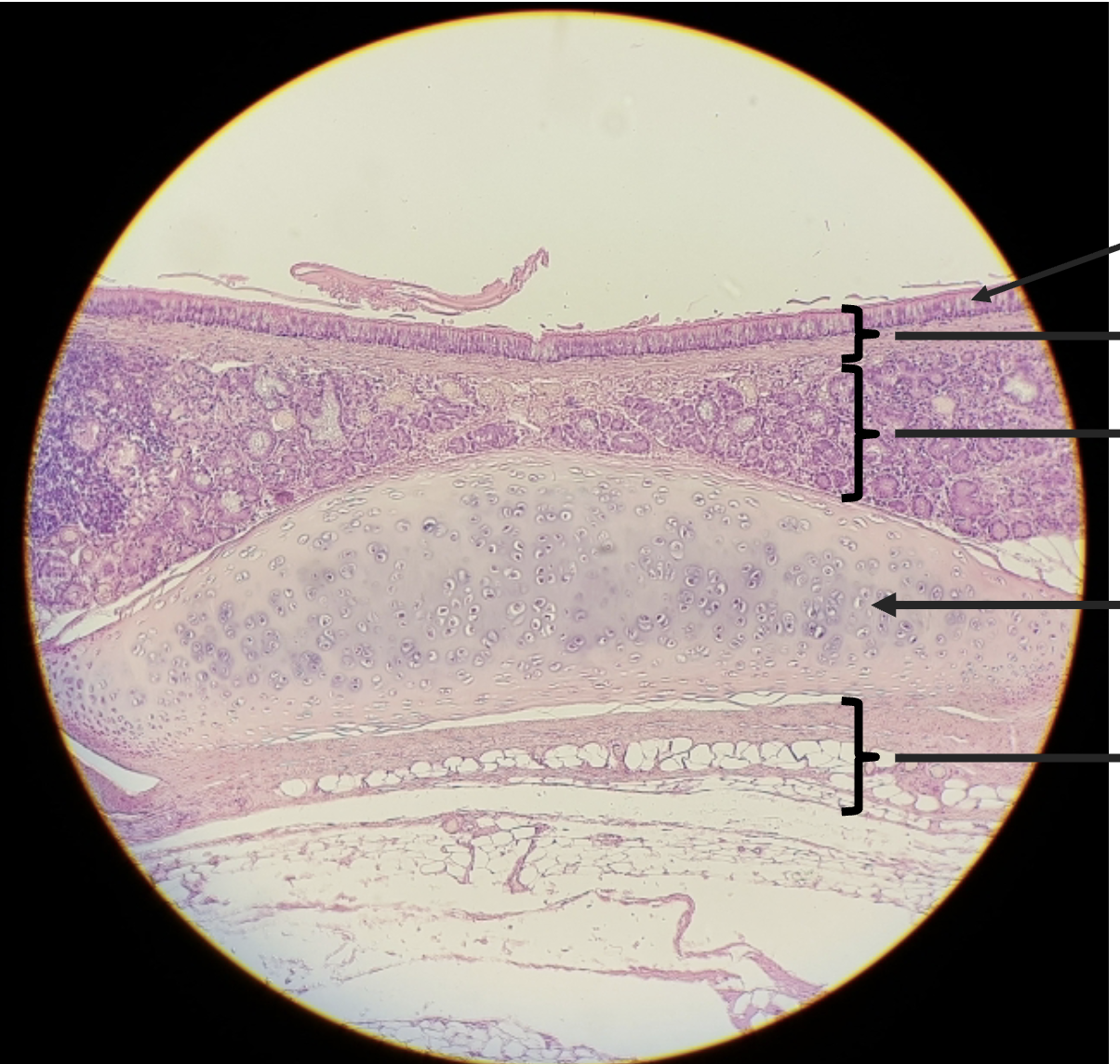
trachea
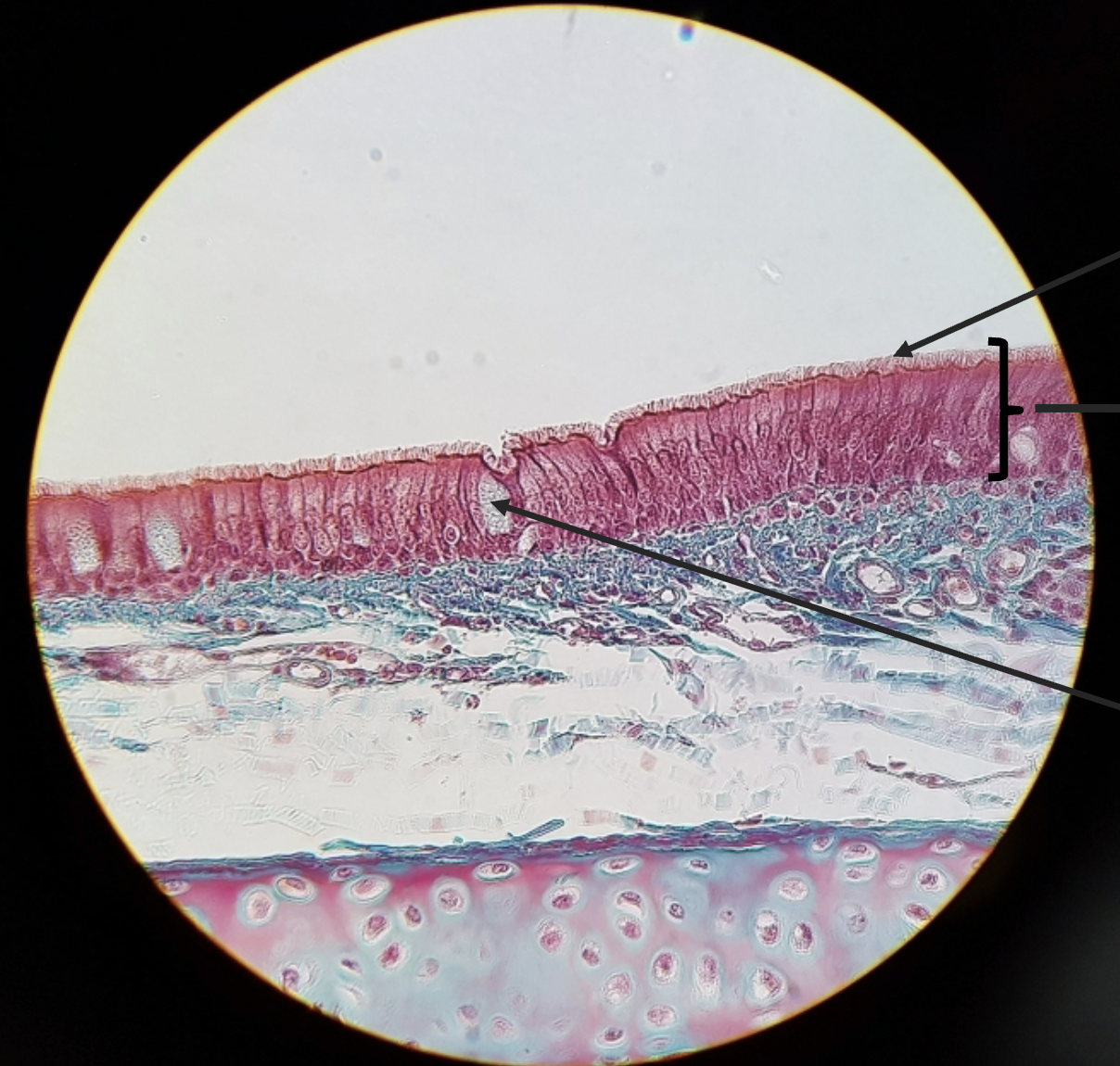
Pseudostratified ciliated epithelium
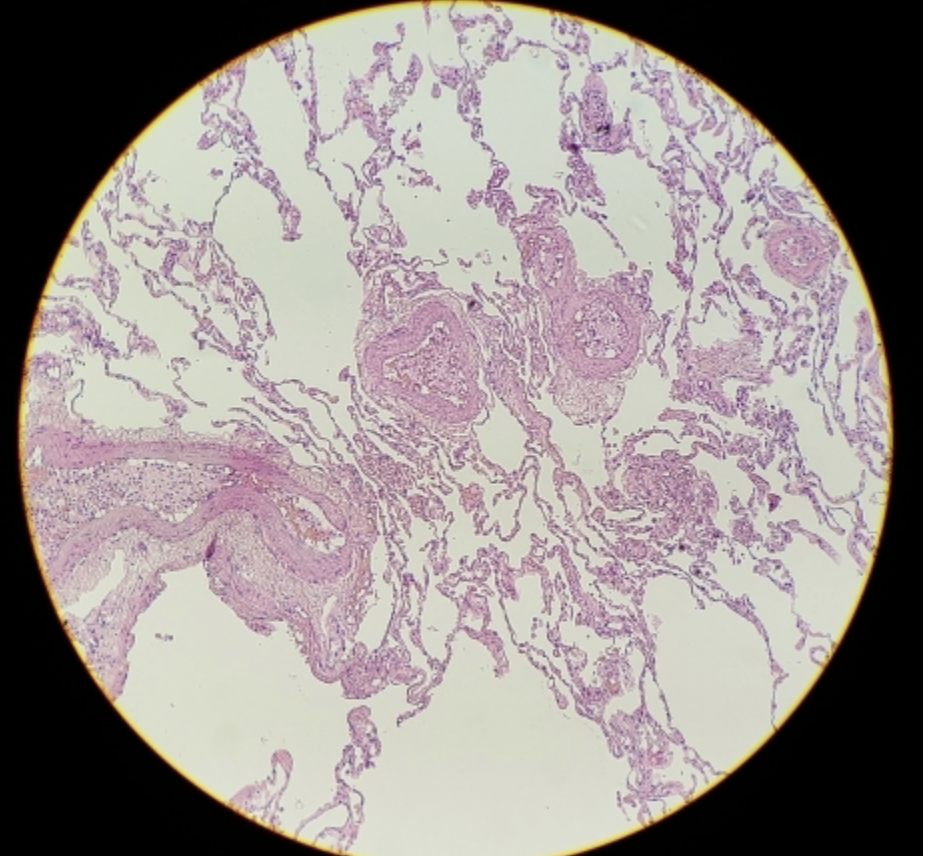
healthy lung