Lymphatic and respiratory system
1/69
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
Lymph
Lymph is derived from plasma but has fewer dissolved
proteins
The purpose of lymph
washes over tissues to deliver nutrients and
remove wastes, cell debris, bacteria, viruses, and loose
(possible cancerous) cells.
why does lymph leave the blood vessel
due to blood pressure
how is lymph returned to blood stream
by open-ended
lymph vessels through the skeletal muscle action
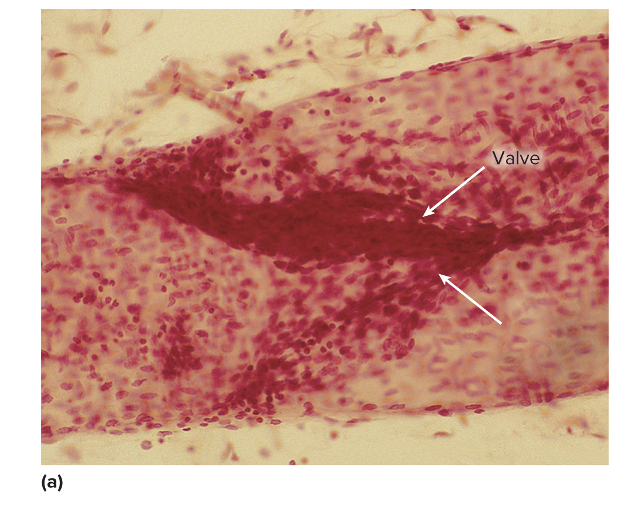
this is an image of
valves in lymphatic vessels
Lymphatic collecting ducts return lymph to the
bloodstream where
at the subclavian veins.
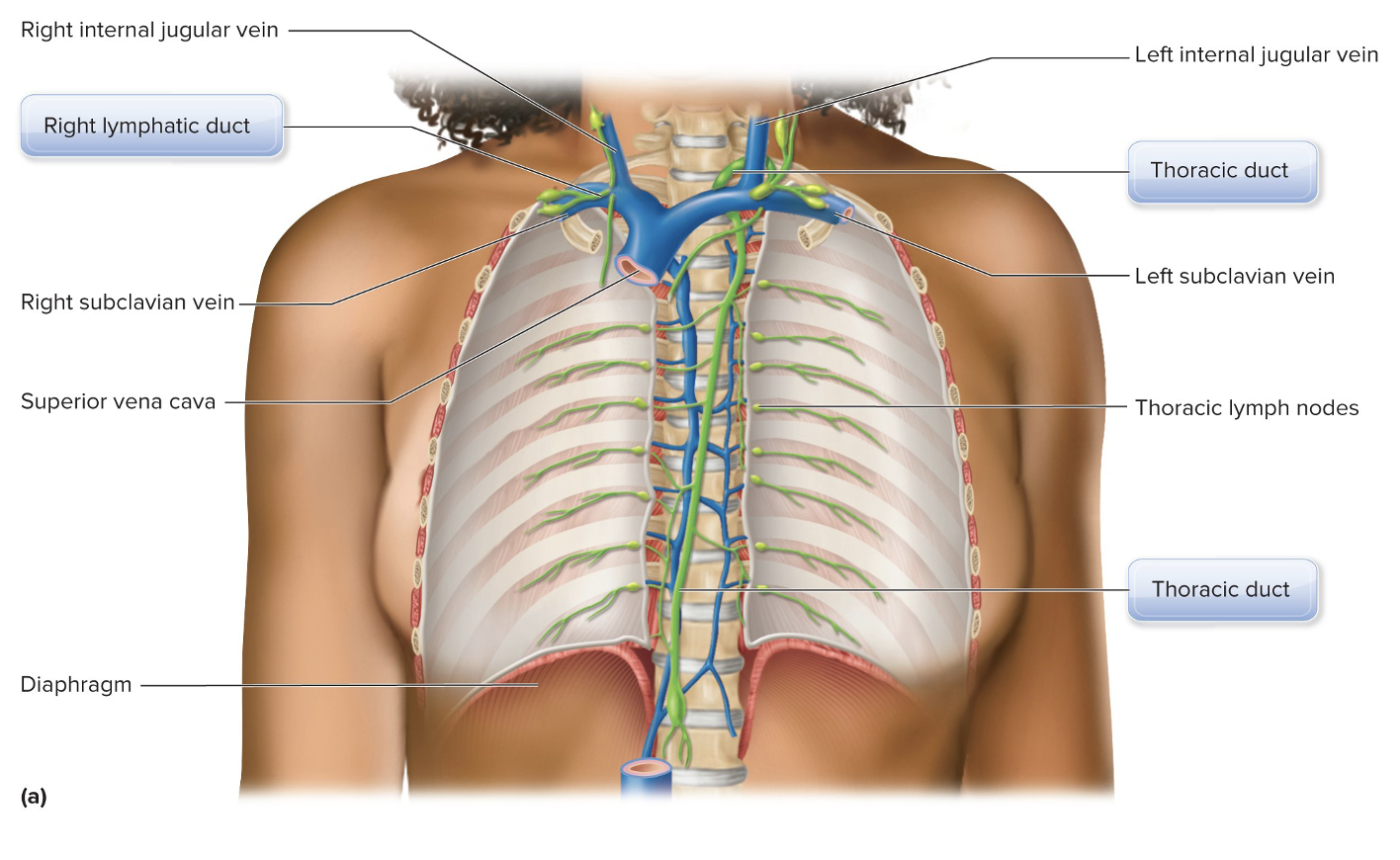
what does this picture show
Anatomy of the Lymphatic System
Natural Killer (NK) cells
Cells of the Lymphatic System
Lymphocytes that destroy bacteria, fight against transplanted
tissues, attack virally infected cells, and destroy cancer cells
T cells are lymphocytes that are important because
they in help nonspecific
defense and specific immunity.
T-helper cells
Important for nonspecific defense and specific immunity
Recognize foreign pathogens and activate the cells to fight them
T-cytotoxic cells
Directly kill cells infected by viruses and cancer cells in specific
immunity
T-memory cells
Specific immunity
Allow repeat exposure to be fought more swiftly
B cells are lymphocytes that serve
as antigen-presenting
cells (APCs) and are important in humoral immunity
because they produce antibodies
B-plasma cells
Important in specific immunity
• Produce antibodies
• Dissolved proteins in plasma that seek out specific foreign antigens
for their destruction
B-memory cells
Pathogens that have been introduced to the body so that repeat
exposure can be fought more swiftly
Macrophages
Monocytes that have migrated to the tissues, where they
phagocytize bacteria, debris, and dead neutrophils
Dendritic cells
Located in the epidermis and serve as APCs
Lymph nodes
Filter lymph on its way back to the bloodstream
• Located throughout the body, but mainly in trunk:
• Cervical
• Axillary
• Thoracic
• Abdominal
• Pelvic
• Intestinal and mesenteric
• Popliteal
• Inguinal
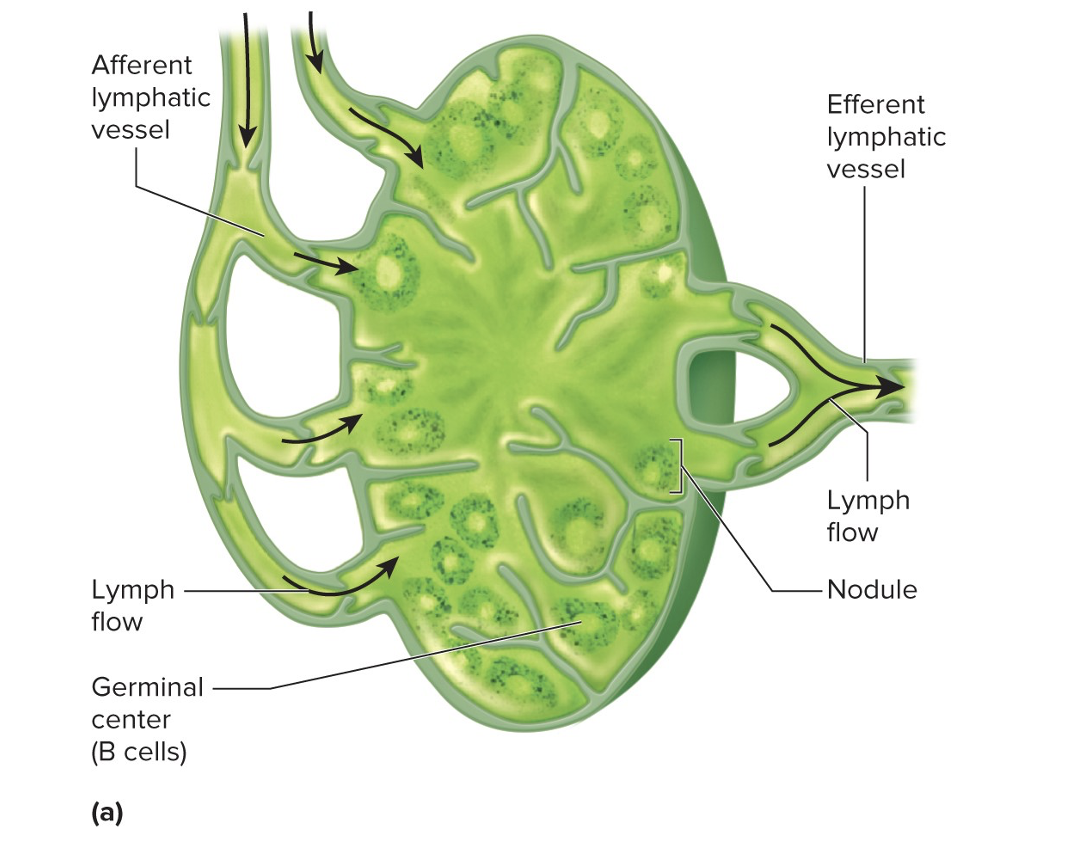
this image shows
lymph node
Thymus gland
The thymus gland matures T cells that recognize foreign antigens,
and it destroys T cells that react to self-antigens.
• Largest in children
• Atrophies in adults
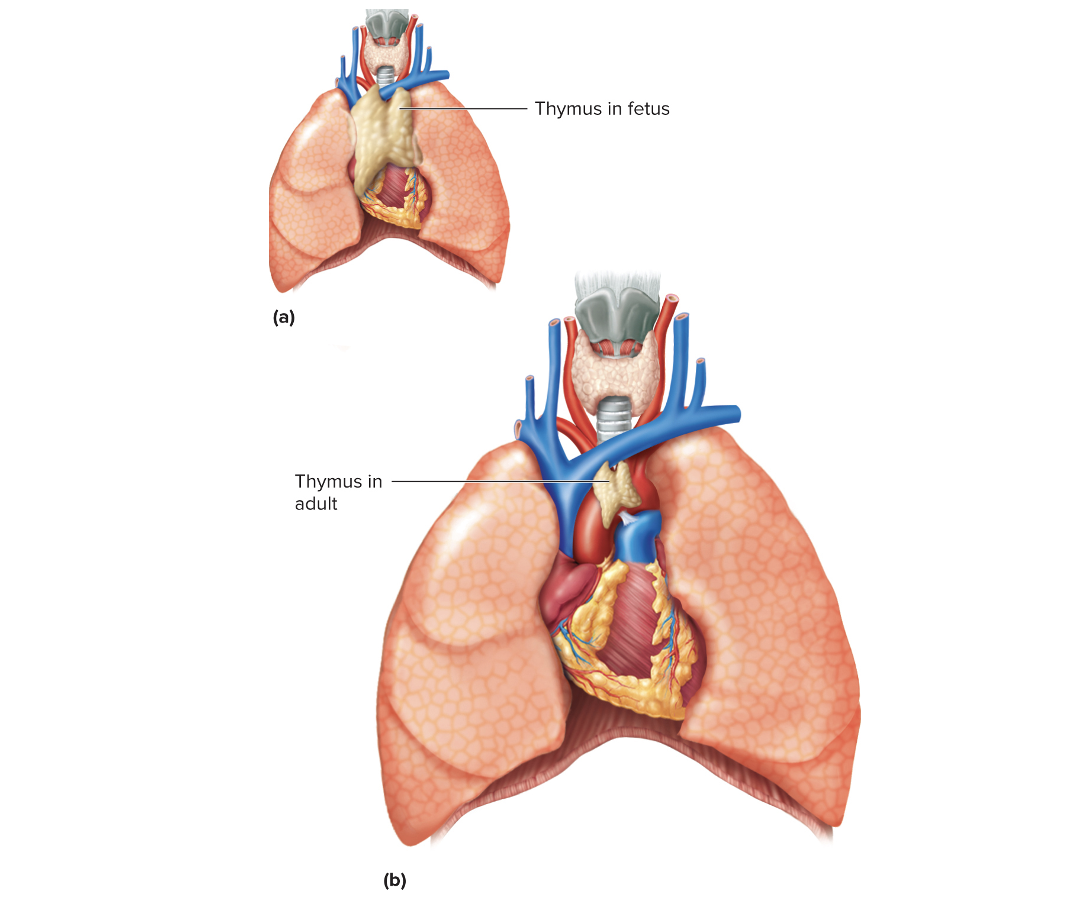
This image shows the BLANK in adults and children
Thymus gland
Spleen
Red pulp to store red blood cells
• Regulates the amount of fluid in the blood by transferring excess fluid to
the lymphatic system as lymph
• White pulp to store lymphocytes and macrophages
• Battle site for lymphocytes to attack pathogens
Three Lines of Defense
The three lines of defense against pathogens are:
1. External barriers
2. Inflammation, antimicrobial proteins, fever, and other active
attacks
3. Specific immunity
The first two lines are nonspecific defenses, while the third is BLANK
specific immunity
Nonspecific defenses
are widespread and function the
same way every time.
Specific immunity
requires a prior exposure to a
pathogen so that it can recognize, react, and remember
the pathogen.
This immunity reacts faster and stronger to repeated exposures
to a pathogen.
(Nonspecific Defenses)
External barriers include
the skin and mucous
membranes.
(Nonspecific Defenses)
Skin
Keratin is a tough protein that bacteria cannot easily break through.
• Skin is dry, with few nutrients for bacteria and other pathogens.
• The skin has an acid mantle, which makes it inhospitable for bacteria
and other pathogens.
(Nonspecific Defenses)
Mucous membranes
Mucus traps microbes.
• Mucus, tears, and saliva contain lysozymes to destroy pathogens.
• Deep to the mucous membranes is loose areolar connective tissue with
fibers to hamper the progress of pathogens.
(Nonspecific Defenses)
Inflammation functions to ….
limit the spread of pathogens, to
remove debris and damaged tissue, and to initiate tissue
repair
(Nonspecific Defenses)
Inflammation involves the release of…
vasodilators from damaged tissue and basophils and the margination, diapedesis, and chemotaxis of leukocytes that phagocytize pathogens along the way.
May form pus
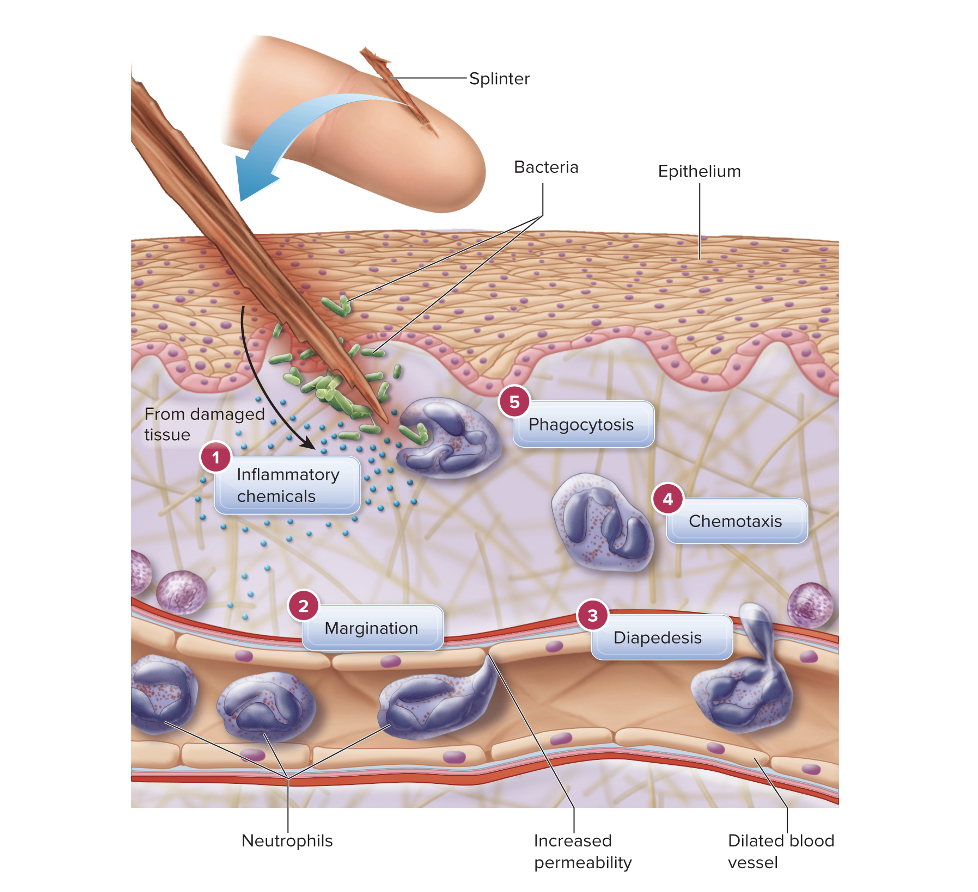
In this image it shows
The Inflammatory Response
Fever
Nonspecific Defenses
Defense initiated by pyrogens from macrophages that cause the
hypothalamus to reset the body’s temperature.
Other attacks from leukocytes complete the list of
nonspecific defenses.
Neutrophils fight bacteria.
Basophils release histamine to promote inflammation.
Eosinophils attack worm parasites.
Monocytes become macrophages to phagocytize bacteria.
Humoral (antibody-mediated) immunity
Involves B cells producing antibodies
• T helper cells activate B cells by releasing interleukin-2.
• Stimulated B cells differentiate into plasma cells and
memory B cells.
Humoral (antibody-mediated) immunity
Primary immune response
• The first time you are exposed to the pathogen
• The response is slow; 3 to 6 days for activation and 10 more days
for peak antibody production.
Secondary immune response
Subsequent times exposed to the same pathogen
• Fast response; 2 to 5 days for peak response
• Due to the quick response, you usually don’t get “sick."
Cellular (Cell Mediated) immunity
T cytotoxic cells directly kill cells with foreign antigens
• Very effective against virally infected cells
• Both types of specific immunity require T helper cells to
recognize what is foreign.
involves the release of interleukin-1
Forms of Acquired Immunity
Passive
• Immunity acquired through someone or something else
Active
• Body actively creating its own immunity
Natural
• Immunity accomplished through naturally occurring means
Artificial
• Immunity not acquired naturally
Artificial active immunity
Artificial active immunity is achieved through vaccination, where the
body's immune system is exposed to a weakened or inactivated
form of a pathogen to produce antibodies and memory cells,
providing protection against future infection. This contrasts with
natural active immunity, which occurs when the body encounters a
live pathogen and fights it off.
Artificial passive immunity
Artificial passive immunity is conferred when a person is given pre-
made antibodies (immunoglobulin) from another person or animal,
rather than their own body producing them.
types of vaccines
Live attenuated vaccines:
-These vaccines contain a weakened or modified form
of the virus or bacteria that causes the disease. They
stimulate a strong immune response, often leading to long-
lasting immunity.
Inactivated vaccines:
-These vaccines use killed or inactivated versions of
the virus or bacteria. They are generally safe for people
with weakened immune systems, but may require booster
shots for continued protection
Functions of the Lymphatic System
The lymphatic system helps maintain the fluid balance in
the blood.
The lymphatic system distributes lymph to wash over
tissues to deliver nutrients and remove wastes.
The lymphatic system carries absorbed products of lipid
digestion.
Effects of Aging on the Lymphatic System
The thymus gland shrinks with age.
The number of new T cells decreases with age.
The immune response may slow with age.
Lymphatic System Disorders
Splenomegaly
Enlargement of the spleen that can be caused by any
number of pathological conditions, including anemia,
cancers, and certain infections.
Lymphatic System Disorders
Autoimmune disorders are the result of the immune system attacking self-antigens.
Rheumatoid arthritis (RA)
is a chronic autoimmune
disease where the body's
immune system
mistakenly attacks the
joints, leading to
inflammation, pain, and
potential damage.
Respiratory anatomy in the head
and neck
Nasal cavity > nose >
nasopharynx, oropharynx, and
laryngopharynx > larynx
Respiratory anatomy in the thoracic
cavity
> Trachea > main bronchi >
bronchial tree > bronchioles >
alveoli
Nasal Cavity
The mucous membranes of the nasal cavity warm and
moisturize the air and remove debris
Nasal conchae
provide extra surface area.
Vestibule
is the anterior part of the nasal cavity lined by
stratified squamous epithelial tissue with stiff guard hairs
to block debris from entering the respiratory tract.

Which system is this
THE RESPIRATORY SYSTEM
Pharynx
The pharynx is composed of the nasopharynx,
oropharynx, and laryngopharynx.
The epithelial tissue varies in each part of the pharynx
based on the materials that travel through each area.
Larynx
The larynx is a cartilaginous box that contains the vocal cords.
• Thyroid cartilage
• Arytenoid cartilage
• Corniculate cartilage
Muscles in the larynx move cartilages that allow the vocal cords to
vibrate to produce sound.
Epiglottis
blocks the entrance to the trachea when swallowing
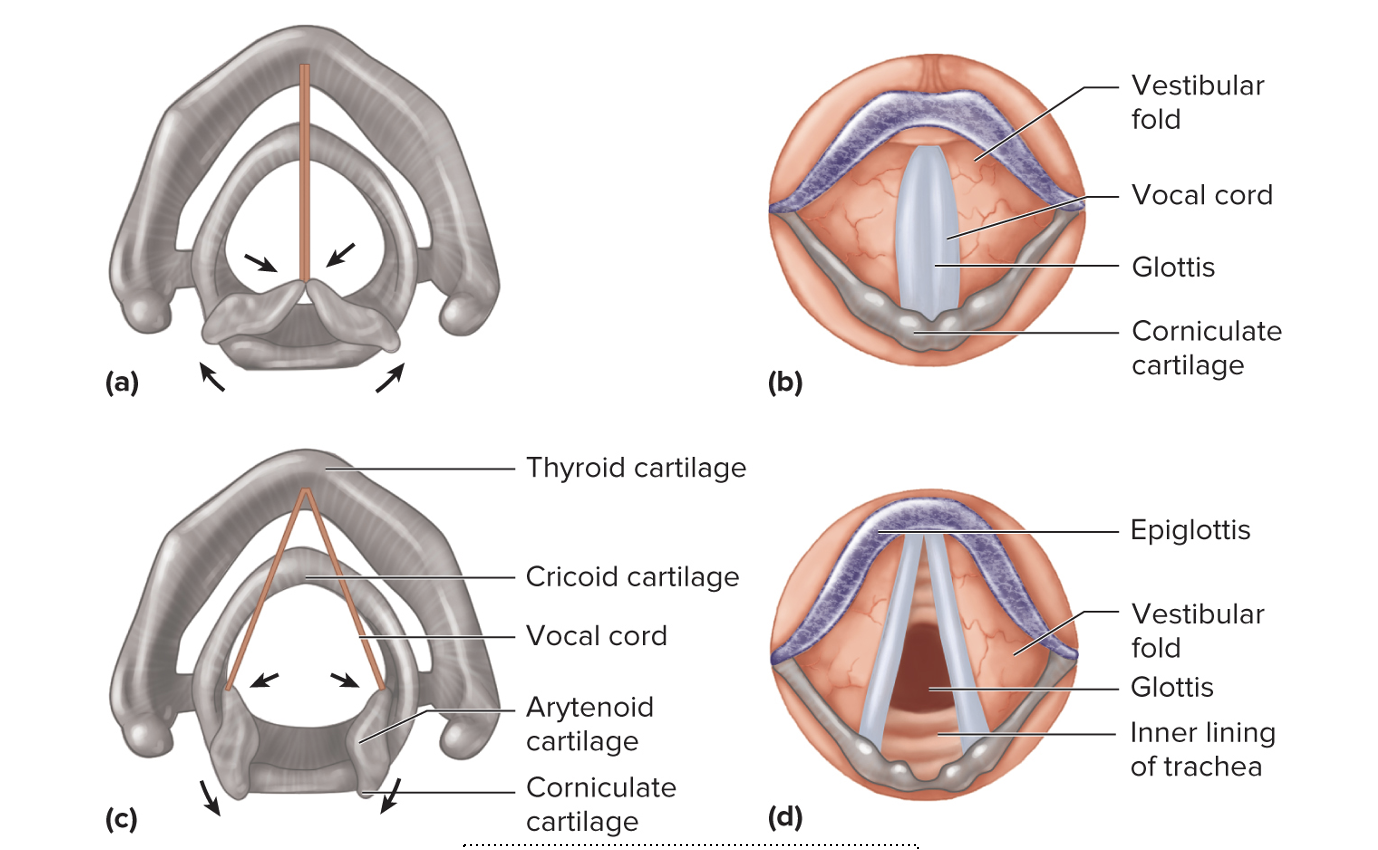
Labeling of which system
THE RESPIRATORY SYSTEM
Lungs and the Bronchial Tree
Each main bronchus enters a lung and then further divides to form the bronchial tree.
• Lobar bronchi go to each lobe of the lung
• The left lung has two lobes and the right lung has three lobes due to
the position of the heart.
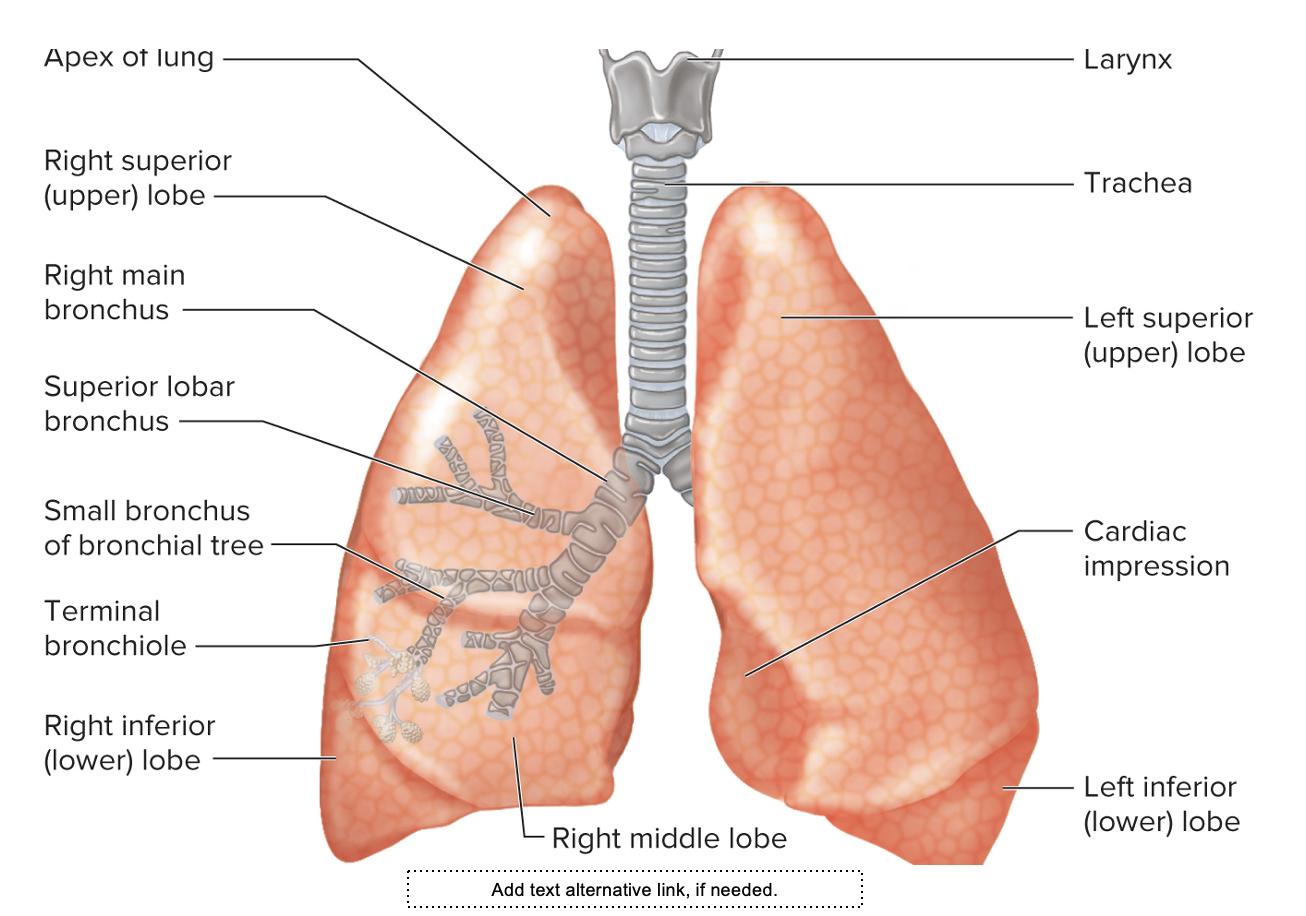
Labeling of ..
The lungs
Alveoli
Surfactant reduces the surface tension of water so that
alveoli do not collapse.
The respiratory membrane is composed of the thin layer of
water with surfactant in the alveoli, the single squamous
cell alveolar wall, and the single cell capillary wall.
Mechanics of Taking a Breath
Inspiration results from intercostal muscles and the diaphragm’s contracting to increase the volume of the thoracic cavity, thereby decreasing its pressure.
Air flows due to pressure gradients.
Pleural membranes cause the lung to expand with the
thoracic cavity.
Normal inspiration is caused by
contraction of the intercostal muscles and diaphragm.
• Forced inspiration involves additional muscles such as the
sternocleidomastoid and pectoralis minor.
Normal expiration is caused by
the relaxation of the intercostal muscles and diaphragm
A spirometer can be used
to measure lung volumes and lung capacities
Compliance measures
how well the lung can expand and return to shape.
• Decreased compliance in chronic obstructive pulmonary
disorders
Gas Exchange
Gas exchange happens between the alveoli and the
capillaries in the lung and between the capillaries and the
tissues of the body.
Gases diffuse across membranes because of a
concentration gradient until the concentrations on both
sides of the membrane are equal.
Factors that influence gas exchange
Concentration of the Gases
• Creates a gradient for diffusion
• Membrane area
• The greater the membrane area, the
greater the opportunity for diffusion.
• Membrane thickness
• Thicker membranes make gas
exchange more difficult.
• Solubility of the gas
• Must be soluble in water to diffuse
across the respiratory membrane
Lung perfusion (blood flow to
alveoli)
Alveolar capillaries constrict where the partial pressure of oxygen is low, so blood is diverted to where the partial pressure of oxygen is high.
Alveolar ventilation
(air flow to alveoli)
Bronchioles dilate if partial pressure of carbon dioxide
increases
Bronchioles constrict if the partial pressure of carbon dioxide
decreases