chap. 22 - peripheral vascular system
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
arteries
carry oxygenated, nutrient-rich blood from the heart to the capillaries
arterial walls → thick + strong to withstand high pressure, contain elastic fibers to stretch with each heartbeat
each heartbeat — creates a surge of blood = arterial pulse
pulse amplitude (0-4+ scale)
0 = absent
1+ = weak, diminished (easy to obliterate)
2+ = normal (obliterates with moderate pressure)
3+ = strong (requires firm pressure to obliterate)
4+ = bounding (cannot obliterate)
allen test
evaluates patency of radial + ulnar arteries
normal/patent artery → palm color returns in 3-5 secs
abnormal/occluded artery → persistent pallor = arterial insufficiency
steps:
patients rest hand with palm up + make a fist
occlude both radial + ulnar arteries with thumbs
patient opens hand → palm appears pale
release pressure on 1 artery
veins
carry deoxygenated, waste-laden blood from tissue back to the heart
upper body → superior vena cava → right atrium
lower body → inferior vena cava → right atrium
hold 70% body blood volume (low-pressure system)
vein walls → thinner + less muscular than arteries, larger in diameter + can expand to accommodate increased volume (reduces workload on heart)
how veins work
veins operate in a low-pressure system (no strong pump pushes blood forward)
blood from legs must travel upward to the heart against gravity
venous return: 1. one-way valves
found in deep, superficial, and perforator veins
prevent backflow + keep blood moving toward the heart
venous return: 2. skeletal muscle contraction
walking + movement “milk” blood up the legs
muscle squeezes veins → pushes blood through valves
venous return: 3. pressure gradient from breathing
inspiration → decreases intra-thoracic pressure + increases abdominal pressure
creates a gradient that helps pull blood upward
valve opening
valves open when leg muscles squeeze on the vein and this lets blood movie in an upward direction
valve closing
valves close when the leg muscles relax and this prevents blood from leaking downward
capillaries
connect arterioles to venules + regulate fluid balance
maintain equilibrium between vascular + interstitial spaces
capillaries key processes
hydrostatic pressure pushes oxy, water, nutrients out of capillaries into tissues
tissues pick up nutrients + release waste products (CO2, metabolites)
osmotic pressure pulls fluid back into capillaries
remaining excess fluid is collected by lymphatic capillaries
MATTERS bc it is essential for perfusion, fluid balance, and preventing edema
lymphatic system
works alongside vascular system to drain excess fluid + maintain balance
removes extra fluid and proteins from interstitial spaces and returns to venous circulation
interstitial space
fluid filled spaces located between cells + tissue
acts as a reservoir for fluid → can lead to edema if not drained properly
peripheral artery disease (PAD)
narrowing/blockage of arteries from plaque buildup (atherosclerosis)
leads to reduced or stopped blood flow → tissue damage
complications → heart attack, stroke/TIA, renal artery stenosis, amputation
PAD s/s
intermittent claudication (leg pain with activity relieved by rest)
atypical leg pain (non-classic presentations)
ischemic rest pain (constant forefoot pain; worse with elevation, improved with dependency)
leg numbness or weakness
coldness in the lower leg or foot, sores on toes, feet, legs that wont heal
change in color of legs
hair loss or slower hair growth
PAD prevention/education
quit smoking
control diabetes + keep A1C in target range
exercise regularly
maintain healthy BP, cholesterol, weight
eat a heart-healthy diet low in saturated fat
venous insufficiency
occurs when leg veins struggle to send blood back to the heart, causing blood to pool (stasis)
damage to vein walls impairs blood flow
primarily caused by damaged vein valves or prior blood clots (DVT)
managed w/ compression stockings, elevation, exercise
venous insufficiency risk factors
long periods or standing, sitting, immobility
lack of muscle activity → blood pools in legs
varicose veins (dilated, tortuous) increase venous pressure
venous insufficiency s/s
pain → aching, cramping
pulses → present but may be difficult to palpate through edema
skin → PIGMENTATION in gaiter area
thickened + tough
REDDISH-BLUE color
associated w/ dermatitis
venous insufficiency grading scale
stage 0-1 → no visible signs or spider veins/mild reticular veins
stage 2 → visible varicose veins
stage 3 → edema (swelling) without skin changes
stage 4 → skin changes (discoloration, eczema, lipodermatosclerosis)
stage 5-6 → healed ulcer (5) or active, open skin ulcers (6)
venous insufficiency ulcer characteristics
location = medial MALLEOLUS or anterior TIBIAL area
pain = superficial: minimal pain, but may be very painful
depth = SUPERFICIAL
shape = IRREGULAR border
base = granulation tissue → beefy RED to YELLOW fibrinous in chronic ulcer
leg edema = moderate to severe
SWOLLEN, DISCOLORATION in leg
ELEVATION HELPS
arterial insufficiency ulcer characteristics
location = tips of TOES, toes webs, heel, other pressure areas
pain = VERY painful
depth = DEEP (often involves joint space)
shape = CIRCULAR
base = PALE BLACK to dry + gangrene
leg edema = minimal unless extremity kept in dependent position constantly to relieve pain
HAIR LOSS + SHINY/THIN SKIN in legs
ELEVATION DOES NOT HELP
raynaud disorder
vasoconstriction/vasospasm of fingers or toes
rapid color changes = pallor → cyanosis → redness
darker skin = dusky, dark blue/purple tones
episodes usually bilateral + last mins to hrs
common in → female at birth + under age 30
raynaud disorder s/s
swelling, pain, numbness, tingling, burning, throbbing, coldness
thrombophlebitis (superficial)
results from thrombus formation in superficial veins
often seen w/ unilateral localized pain, achiness, edema, redness, warm to touch
due to intravenous (IV) lines or injury to vein
lymphedema
results from damaged or blocked lymphatic circulation
caused by → cancer treatments (breast surgery)
usually affects 1 extremity
prominent venous patterning w/ edema may indicate venous obstruction
lymphedema stage 1
asymptomatic
no visible swelling
early functional changes only
lymphedema stage 2
reversible/early swelling
noticeable swelling (may decrease w/ elevation)
skin soft + pits slightly
lymphedema stage 3
irreversible/moderate lymphedema
persistent swelling w/ no elevation improvement
skin changes begin (fibrosis, thickening, firmness)
limb becomes harder/heavier
lymphedema stage 4
lyphostatic: elephantiasis
extensive swelling + severe enlargement of limb
marked skin thickening + scarring
tissue fibrosis + deformity present
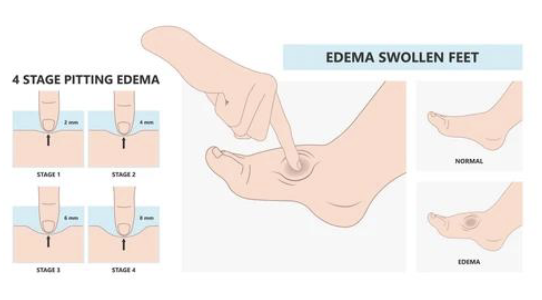
pitting edema
temporary swelling caused by water retention
often heart or venous issues (associated w/ systemic problems: heart failure, hepatic cirrhosis)
leaves dimple when pressed
usually responds to elevation + meds (diuretics)
older adult considerations
w/ arterial disease → coldness, color change, numbness, abnormal sensations
w/ aging → lymphatic tissue is lost, resulting in smaller + fewer lymph nodes
hair loss on lower extremities (not absolute sign of arterial insufficiency)
varicosities = common