Txt Planning Exam 1 | Quizlet
1/190
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
191 Terms
what are the four W's of dialogue history ?
when
where
what
why
what are the main things evaluated under the cardiovascular system ?
cardiovascular disease
coronary artery disease / angina
heart murmurs
hypertension
palpitations
what are the main things evaluated under neuological history ?
stroke
seizure
syncope/dizziness
what are main things evaluated in respitory system ?
asthma
COPD
what are the main things evaluated in hematologic and endocrine assesment ?
anemia
kidney function
liver conditions
diabetes
what are the four parts of information gathering ?
1-patient history
2-radoigraphic examination
3-clinical examination
4-diagnostic aids
what are signs ?
findings discovered by a dentist during an examination
what are symptoms ?
findings verbally revealed by the patients themself ususually because they are causing problems
if a specific symptom is the motivating factor for a patient seeking txt it is refered to as ?
cheif complaint
precise terms that identify a particular disease or problem from signs and symptoms
diagnosis
what are the components of a patient history ?
demographic data
chief concern / complaint history
general health history
medication history
personal history
what is included in a patients demographic history ?
patients name
adress
phone number
physican name/number
insurance info.
national id.
what is the cut-off BP that if its highter than this you need to wait 10 min and retake it ?
160/100
what is included in protected health information (PHI) ?
medical findings
dianoses
txt notes
demographic data that could identify pt.
when can you use PHI according to HIPPA ?
txt. purposes
obtaining payment for services
quality assurance activities
assisting legal authorities
what information do we collect when we obtain vital signs ?
temperature
pulse
respiration
blood pressure
what factors affect vital signs ?
emotional factors --> stress , fear
physical factors --> ilness , drinking , eating , exercise
what is the normal temperature for an adult ?
98.6 F
an adult fever is present with a temperature greater than _______
100.4 F
core temp. _______ as you get older
decreases
--> so old peoples fever could start at a lower temp.
pulse is ?
number of heartbeats per minute
pulse is measure in ?
beats per minute
whats the normal pulse for adults ?
60-100 BPM
tachycardia is ?
heart rate of more than 100 BPM
bradycardia is ?
herat rate less than 60 BPM
when taking a patients pulse we are looking at ________ , _________ , and _____
rate , rythym , strength
where is most common area to measure pulse in dental office ?
radial pulse
what is the typical amount of time we take pulse for ?
30 sec (then mult. by 2)
respirations are measured in ?
breaths per minute
when watching respirations you are observing ________ , _________ , and _____
rate , depth , rythm
rate of repirations is ?
breaths per minute
depth of respirations is ?
labored or unlabored
rythm of respirations is ?
regular or irregular
what is the typical amount of time we take respirations for ?
30 sec ( then mult. by 2)
what do you use to measure blood pressure ?
sphygmomanometer or electronic / digital device
what is blood pressure measured in ?
millimeters of mercury (mm Hg)
high BP can cause damage to vessels increasing chance of ?
stroke
heart attack
kidney disease
sounds heard during BP are known as ?
korotkoff sounds
the first sound heard during taking BP is ?
systolic
the last sound heard during taking BP is ?
diastolic
an undersized BP artificially ______BP
raises
an oversized BP artificially ______BP
lowers
when a cuff fits properly the inflatable bladder should cover _____ circumpherence of the pts arm
80%
(want to fit 2 fingers under cuff)
systolic pressure is ?
the amount of pressure your blood exerts against the artery walls when heart beats
diastolic pressure is ?
the amount of pressure your blood exerts against your artery walls when your heart relaxes between beats
you take BP on the _______ artery
brachial
what type of patients are more likley to have an ausculatory gap?
pt.'s with hypertension or atheroscleosis
an ausculatory gap may lead to ?
underestimation of systolic or overestimation of diastolic
how to we avoid errors in in measuring BP in pt.'s with an ausculatory gap ?
measure pulse obliteration pressure prior to using ausculatory method when getting BP
how do you measure pulse obliteration pressure ?
1-put BP cuff over brachial artery
2-palpate radial pulse
3-inflate to 80 mmhg
4-inflate cuff 10 mmhg every 2-3 seconds stopping when pulse dissapears
5-once pulse dissapears deflate cuff at rate of 2 mmhg/sec
6-the reading that the pulse reappers at is pulse obliteration pressure
when taking BP what portion of stehtescope do you place over skin ?
bell
when taking BP with somone with ausculatory gap what do you inflate cuff to ?
20-30 mm hg above pulse obliteration pressure
how do you take BP normally ?
deflate cuff at a rate of 2 mm hg while listening to sounds
--> first sound is systolic
--> dissapearence of sounds is equal to diastolic
slowly defalfe for additional 10 mmhg beyond last kortkoff sound to ensure get diatolic
whats is the BP where no dental txt will be done without med. consult ?
180-209 / 110-119
what is type 1 diabetes ?
defficiency in insulin production due to autoimmune destruction of beta cells in pancreas
what are the classic symptoms of type 1 diabetes ?
polyuria
polydypsia
polyphagia
what are the classic symptoms of type 2 diabetes ?
metabolic disorders chracterized insulin resistance
what is gestational diabetes ?
hyperglycemia during preganacy in a women w/o diabetes prior (diabetes resistance)
** most common in last trimester
someone with diabtes with HbA1c <7% is grade __
B
someone with diabtes with HbA1c >/= 7% is grade __
C
what does the finger-stick measure ?
random blood glucose test
measures glycemic control at this moment in time only
what does hemoglobin A1c test ?
measures the glycated hemoglobin giving a more accurate measure of glycemic control over a 3 month period
whats a normal A1c ?
below 5.7 %
whats pre-diabetes A1c ?
5.7-6.4%
whats diabetes A1c ?
6.5% and above
when should u test a patient with finger stick ?
-known diabeteic before procedure
-any pt. who feels lightheaded or not well during procedure
-during med. emergency if pt. looses conciosness
what vital signs should u take when a pt. passes out ?
finger stick (glucose)
BP
pulse
when should u do a Hemoglobin A1c test ?
-known diabetic who is non-compliant w/ PCP
-unlown status but oral signs of delayed wound healing
-screening for high risk during COE / Tx planning
a score of ___ on the prediabetes risk test means you are at an increased risk for having prediabetes
5 or higher
what is fingerstick measurment unit of measurement ?
mg/dL
fingerstick measurment 54 mg/dL is ?
severe low
fingerstick measurment 70 mg/dL is ?
low
fingerstick measurment 70-125 mg/dL is ?
normal
fingerstick measurment 126-180 mg/dL is ?
high
fingerstick measurment above 180 mg/dL is ?
severe high
where do you find the physcial exam form ?
EHR --> FORMS ---> PHYSICAL EXAM FORM
when do you complete the physical exam form ?
during COE , update as needed at POE
what are the 3 tabs in the physical exam form ?
physical exam :extraoral
physical exam : intraoral
summary assesment
what are the main parts of the intraoral exam ?
periodontal survey
musculoskeletal screening
history
muscles of mastication
joint screening
occlusal survey
bony exocytosis / tissue undercuts
what are the main parts of the extraoral exam ?
vital signs
extraoral survey
extraoral survey diagram
what are the components of the musculoskeletal history screening ?
signs / symtptoms
history of pain or dysfunction in TMJ/muscle
history of trauma
history of orofacialpain and no diagnosis
where do you palpate the medial pterygoid ?
intraoral
where do you palpate the lateral pterygoid ?
intraoral
what do you do prior to the first COE appt. ?
1-review radiographs and interp.
2-enter radiographic findngs on worksheet
3-fill out the odontgram in axium
4-call patient or use or use mail in forms and fill out history
5-familiarize yourself with pt. meds
exostoses
slow grow
fine unless denture
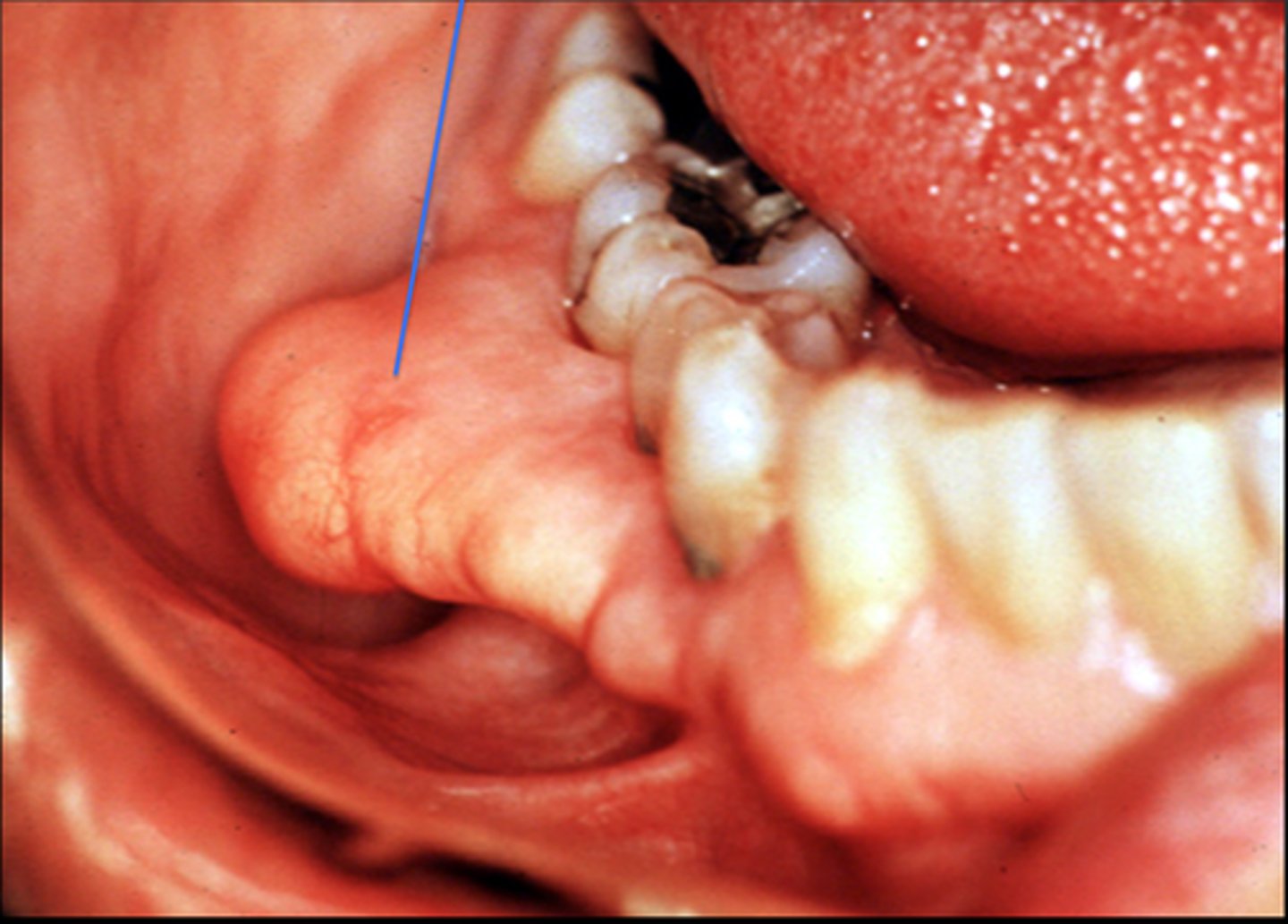
Fordyce granules
yellow
buccal
sebaceous glands
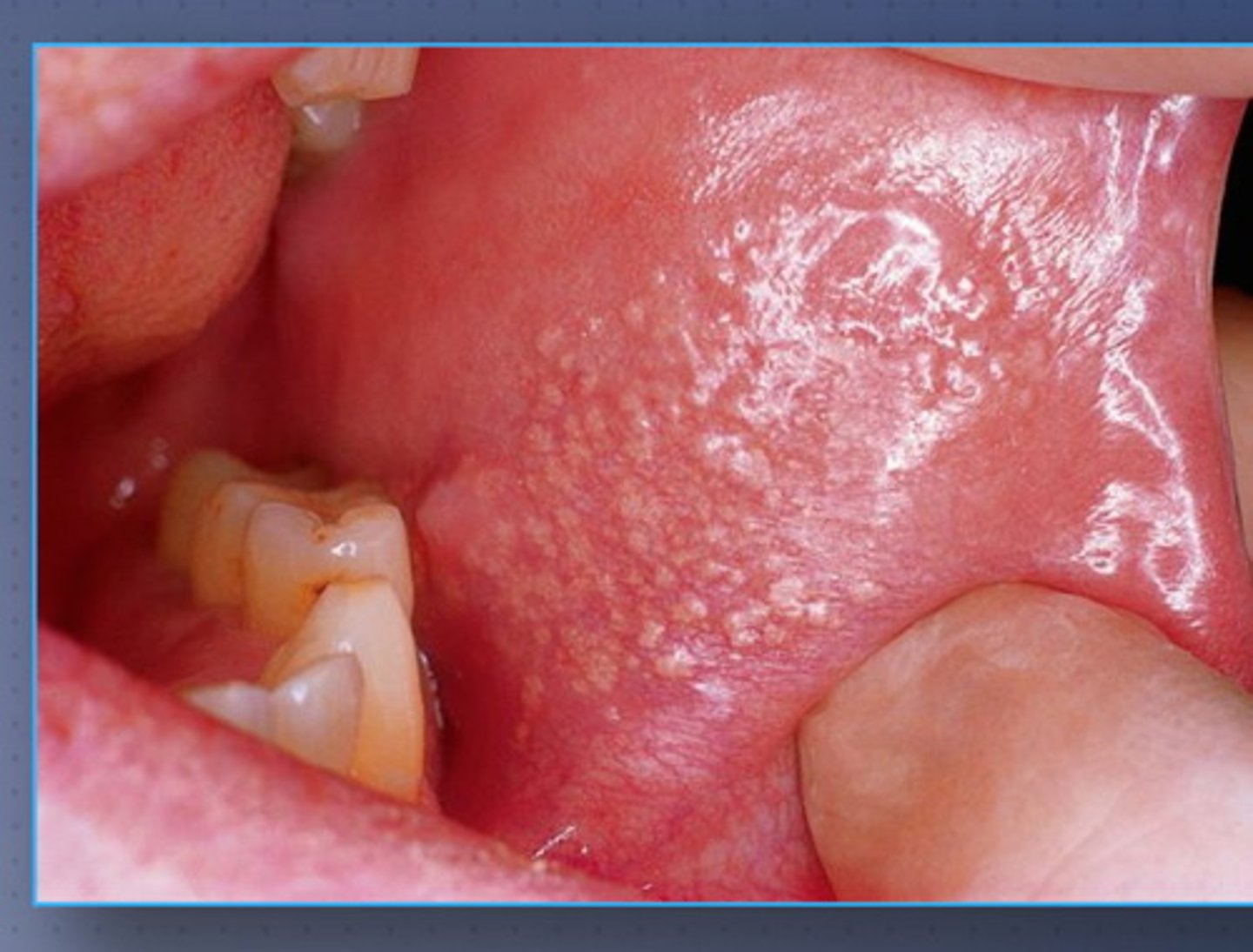
amalgam tatoo
lingual tonsils
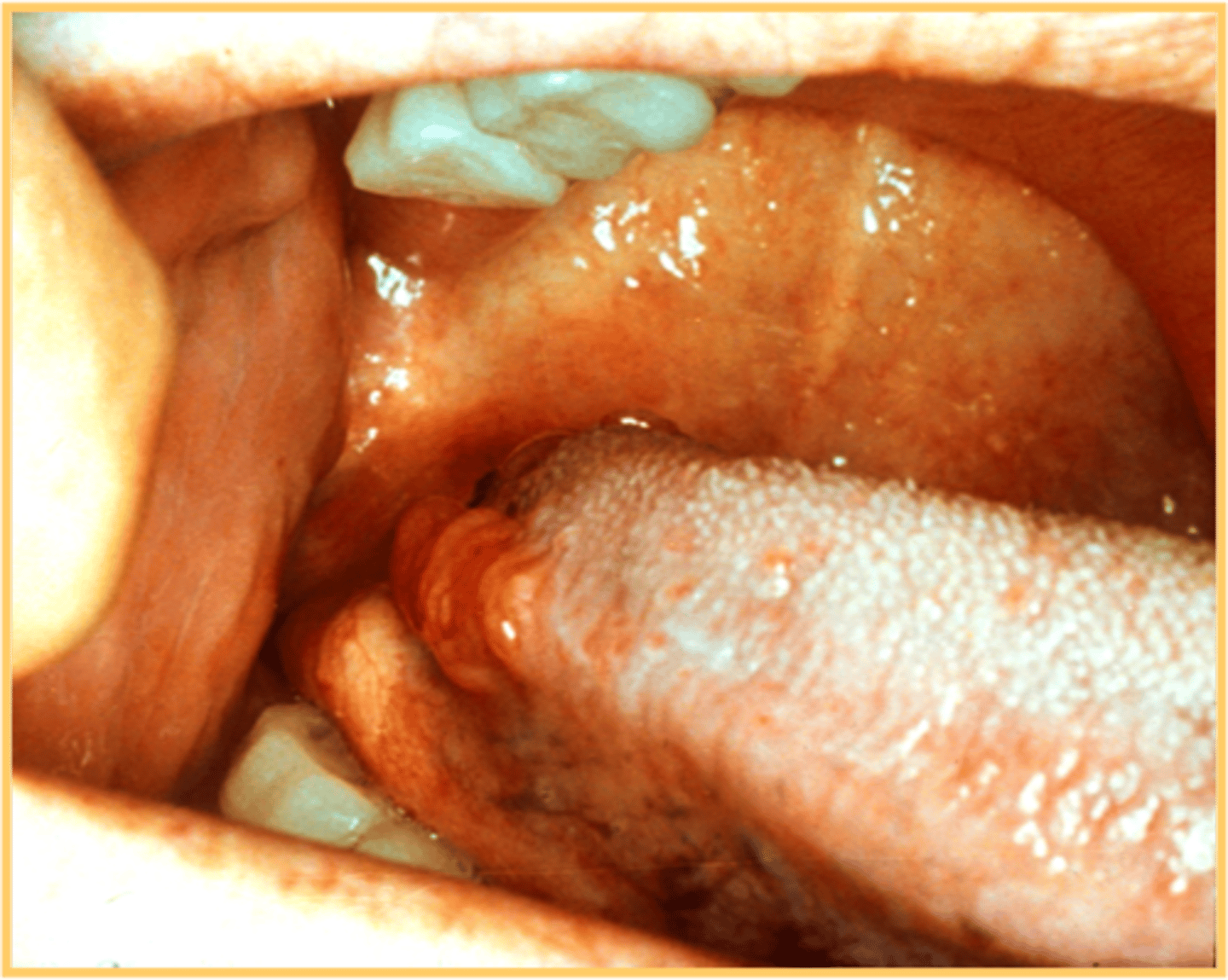
leukoedema
milky white
when stretch goes away
bilateral / symmetrical
buccal
wrinkles
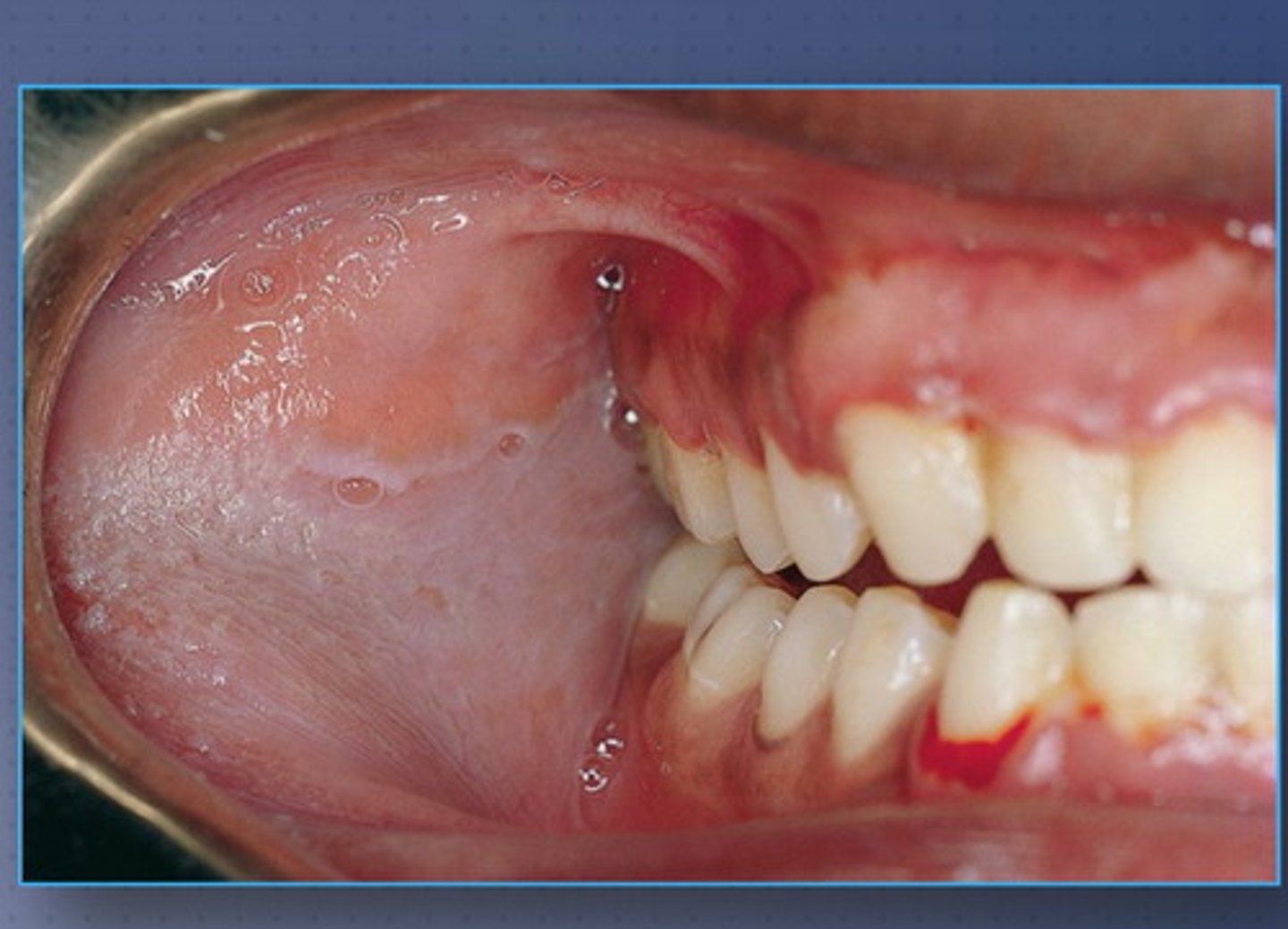
cheek chewing (morsicatio buccarum)
along occlusal
bilateral / symmetrical
shaggy
geographic tongue
associated with immune eitology
asymp.
no txt.
trigggered by spicy food
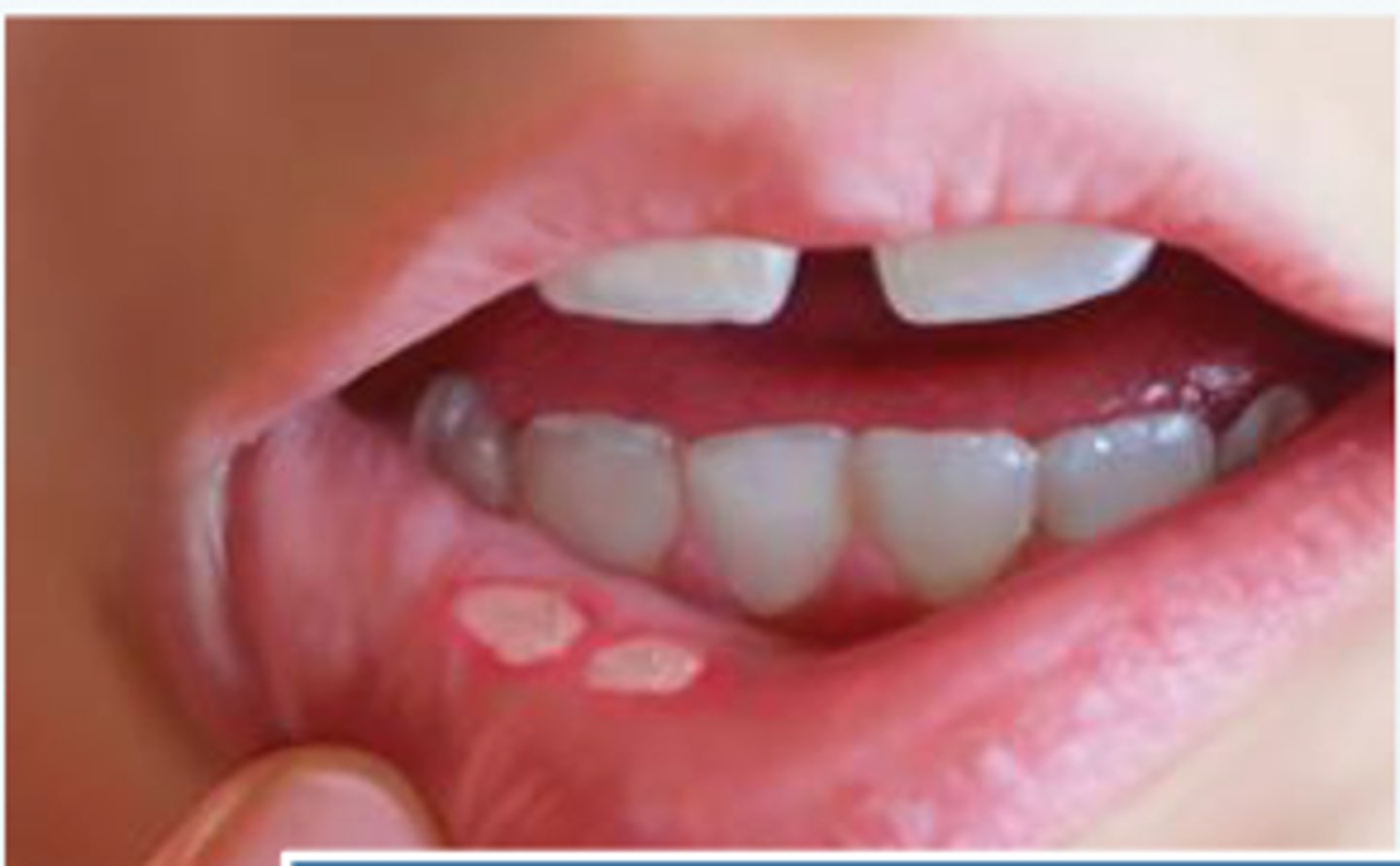
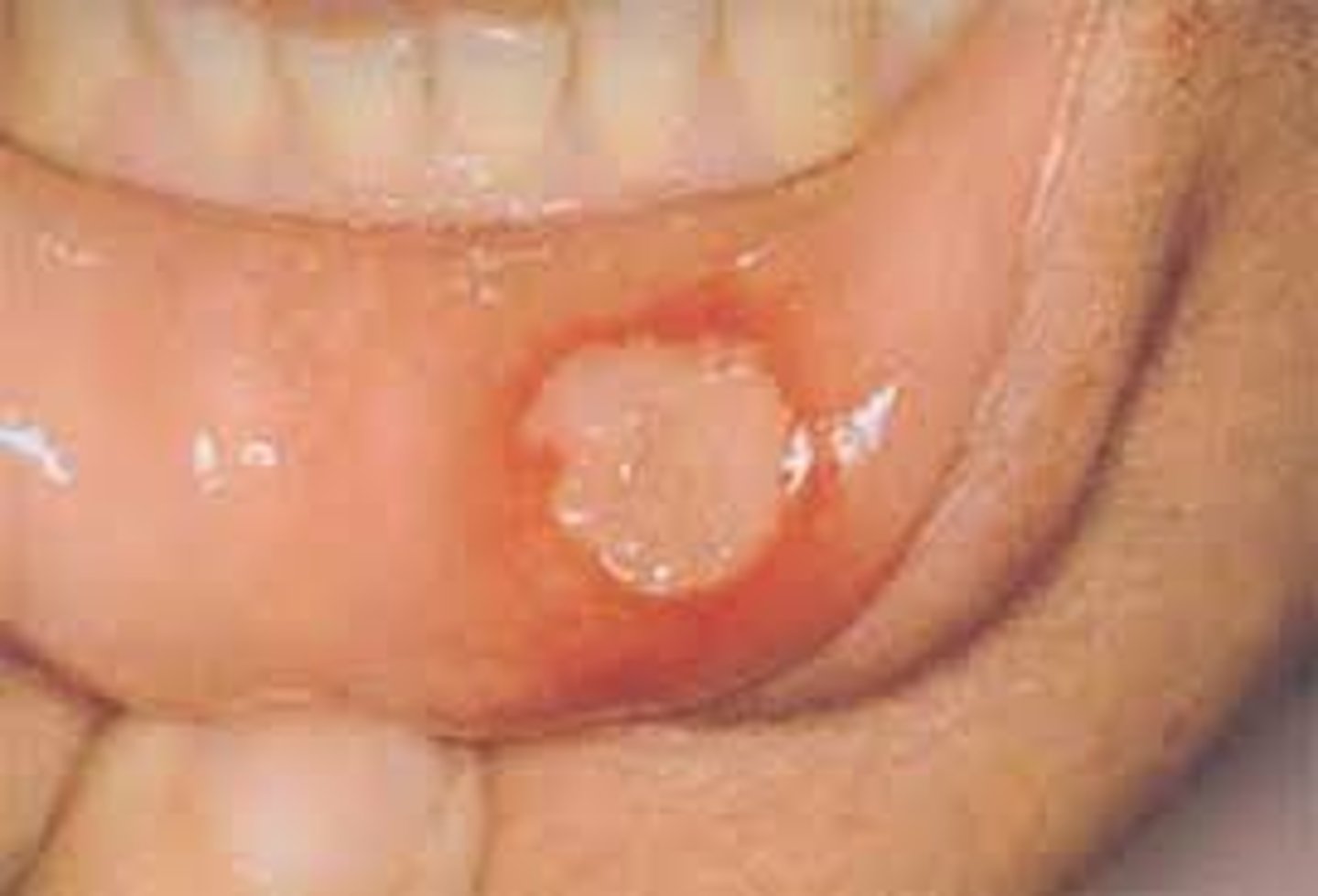
minor apathous stomatis (apthae)
heal without scarring
1-5 lessions
7-14 days
few
short
non-keratinized
self limited
KANKER SORES
major apathae
larger
scarring
2-6 weeks
1-10 lessions per episode
any surface
frequent reoccurence
if in young pt. check for IBD
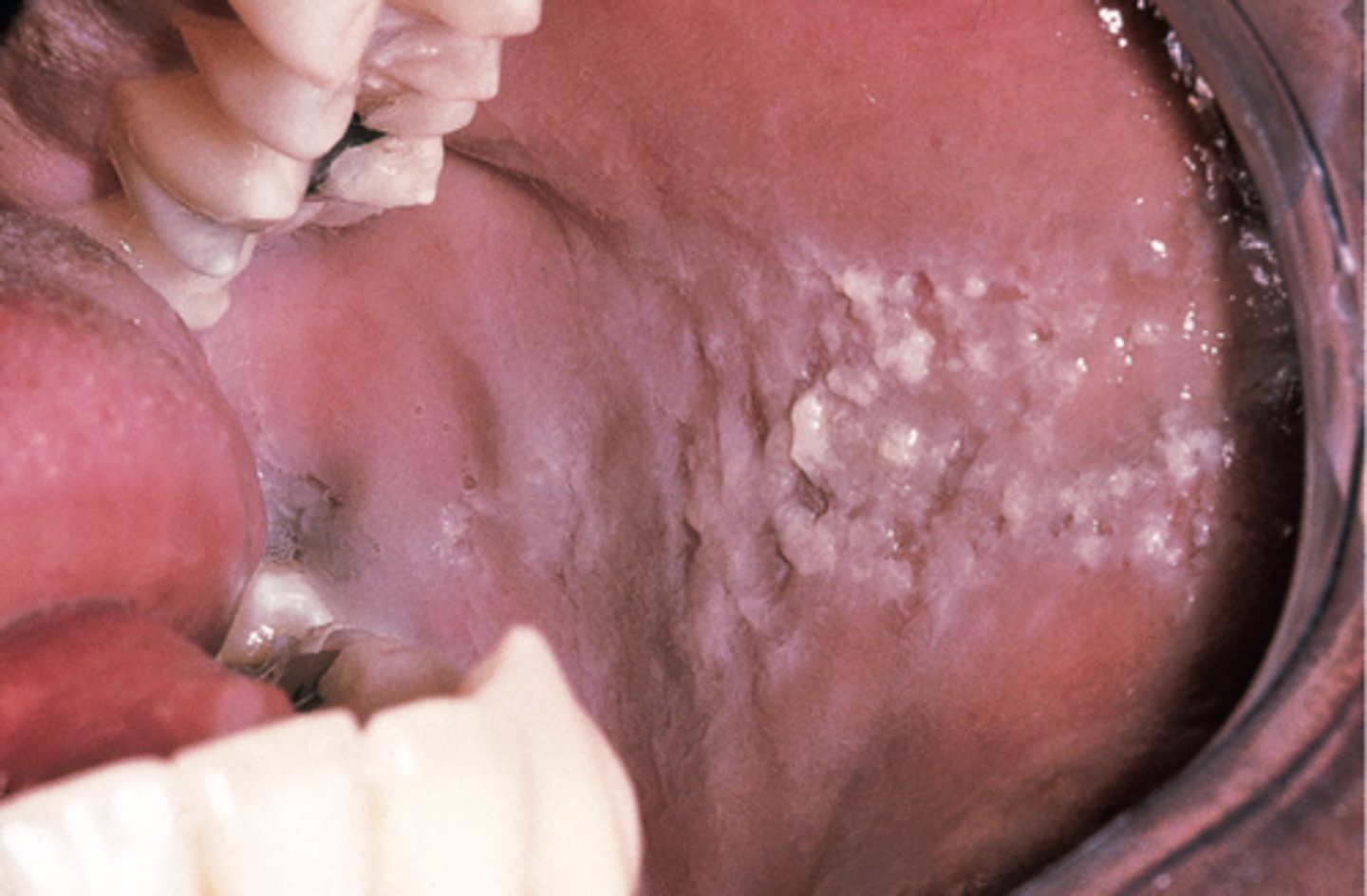
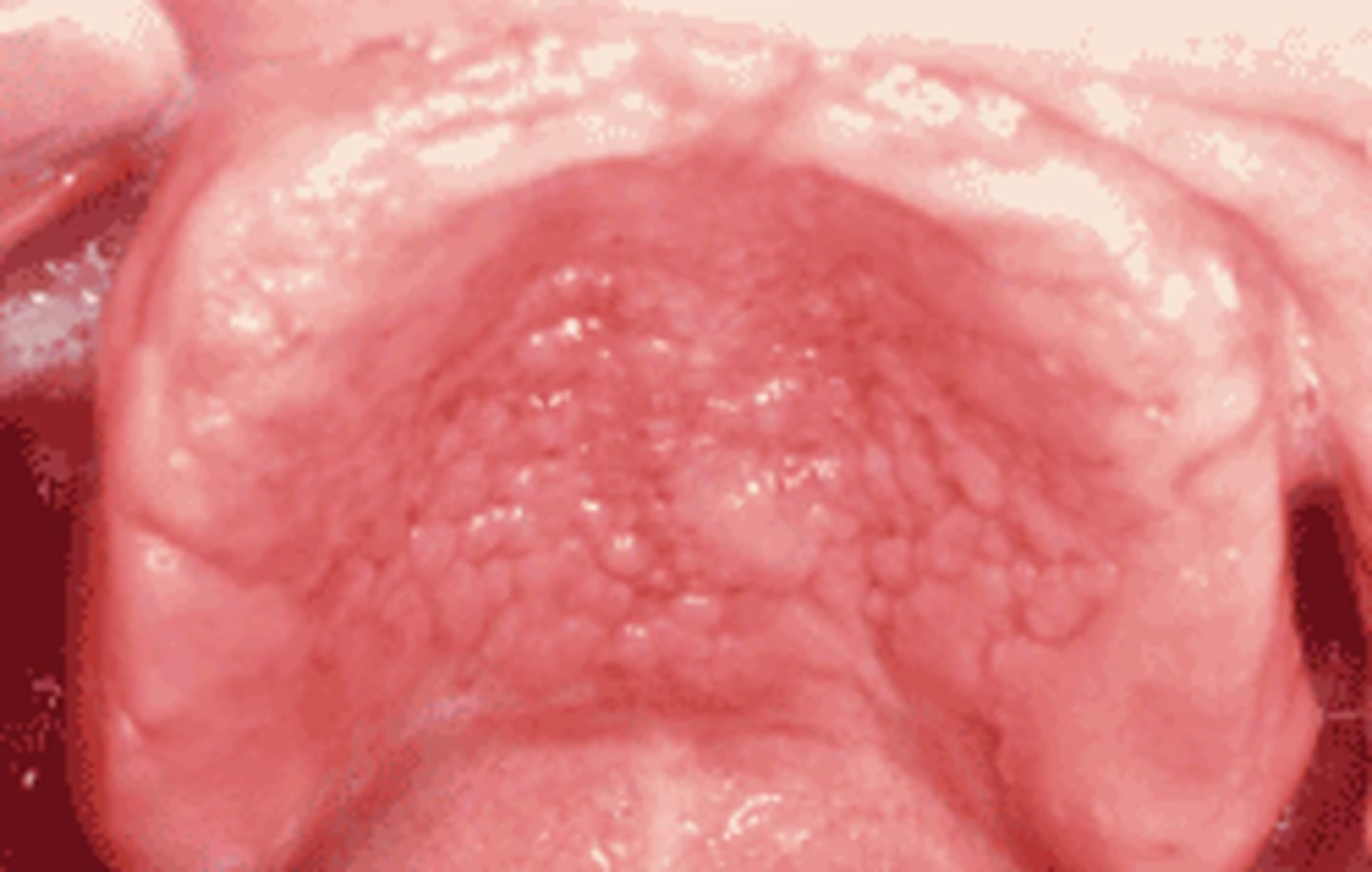
denture stomatis (erthmatous candida)
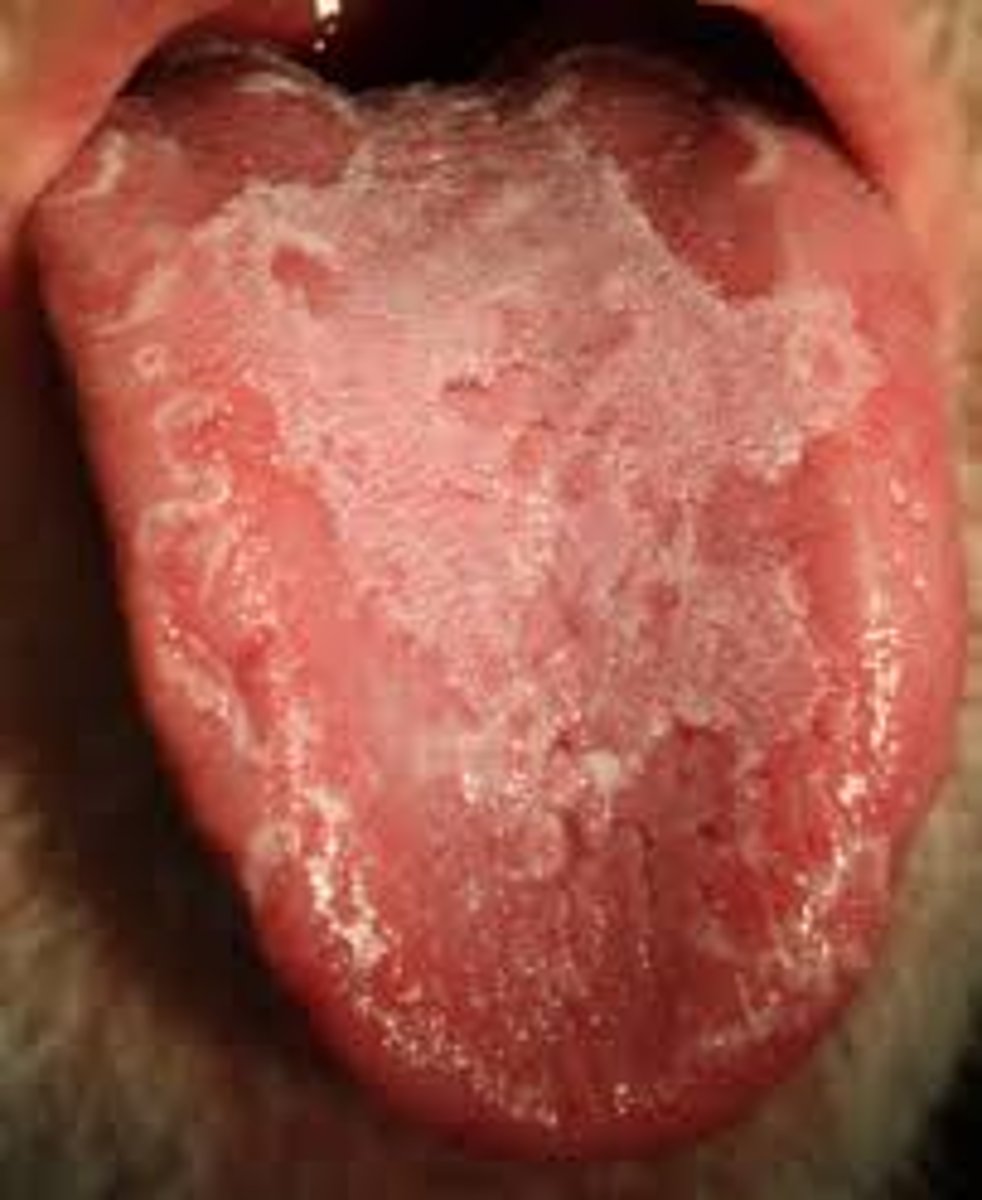
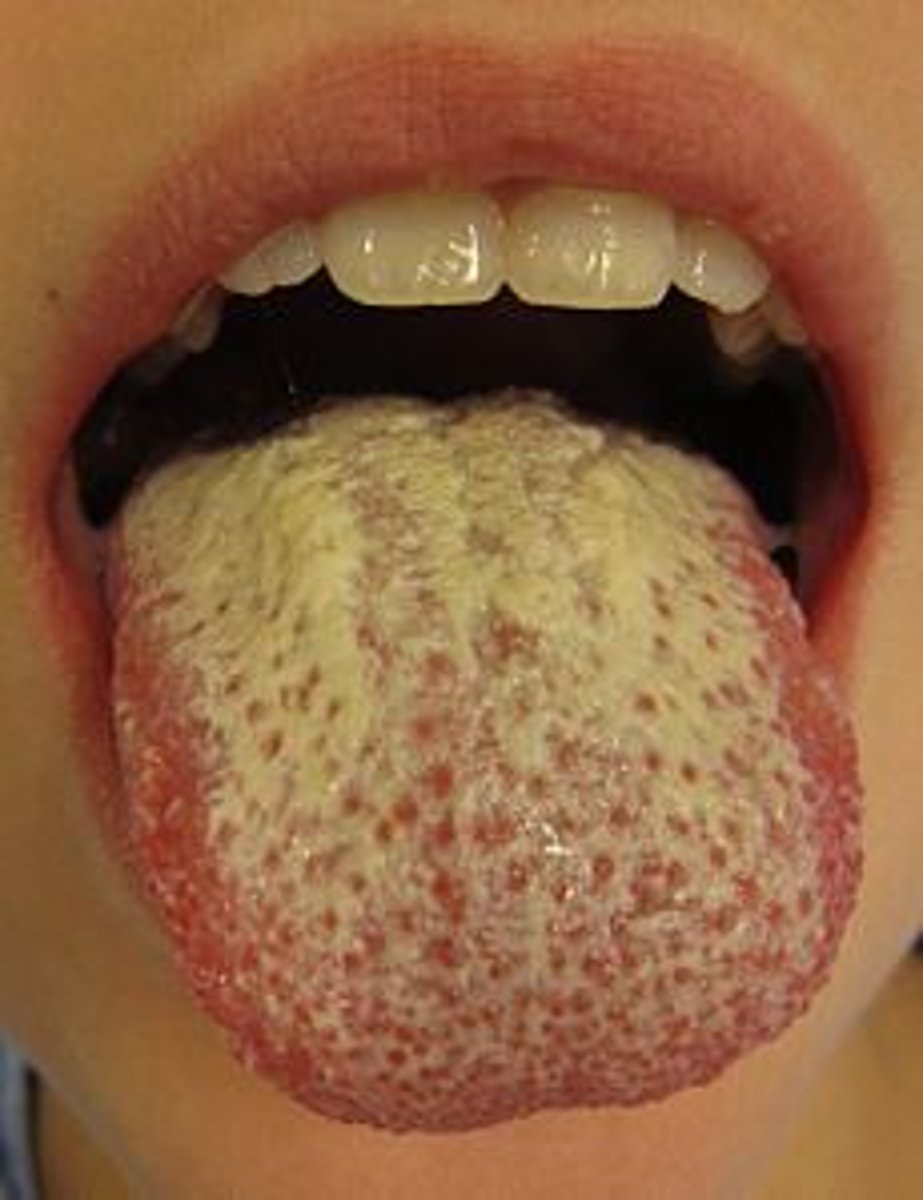
pseudomembranous candiasis
thrush
adherent white plaques resembling cottage cheese
remove with scrapping
txt. with atx.
infants affected
mild burning and unpleasent taste
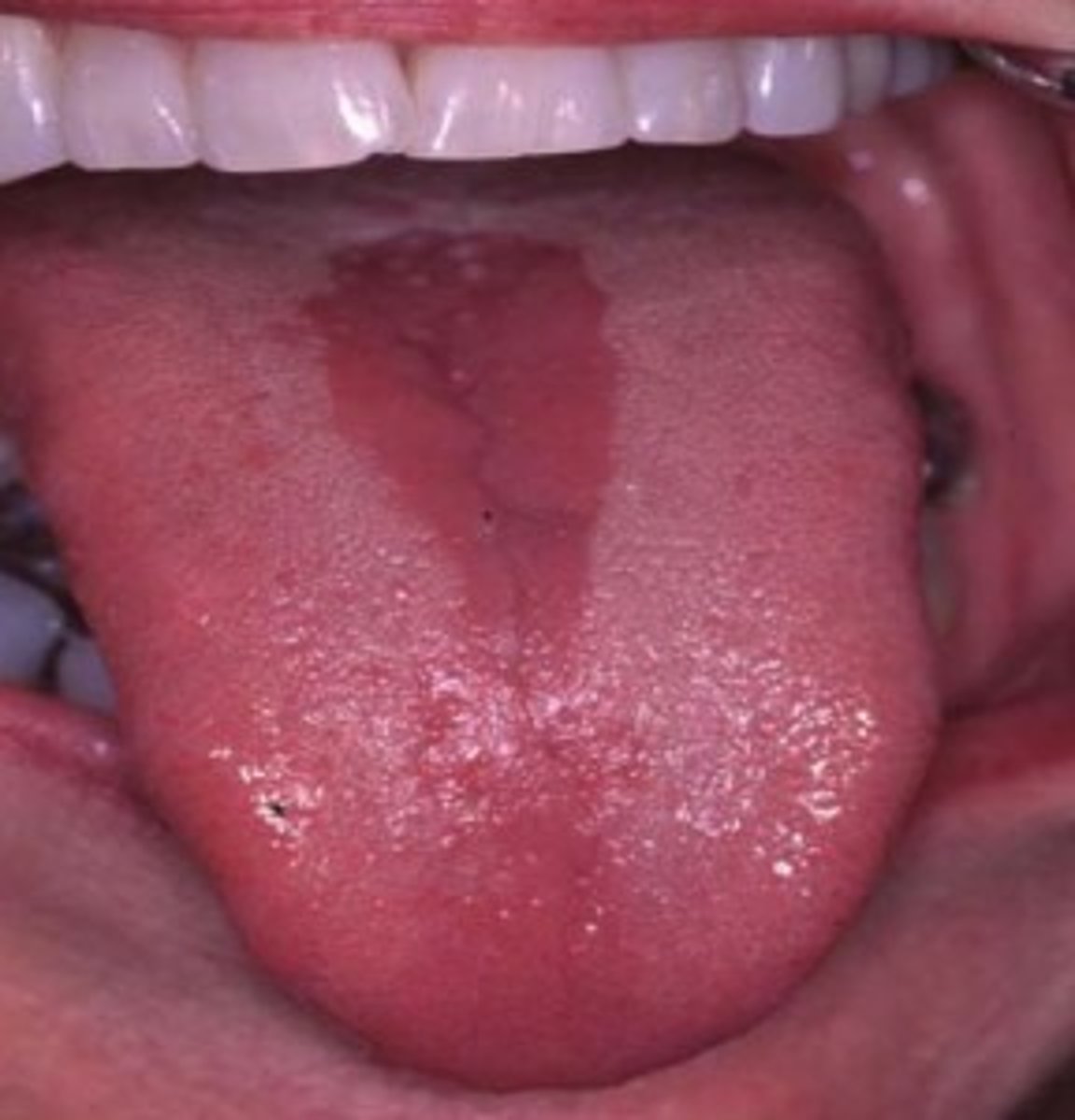
median rhomboid glossitis
burn
midline
angular chelitis
anti-fungal cream
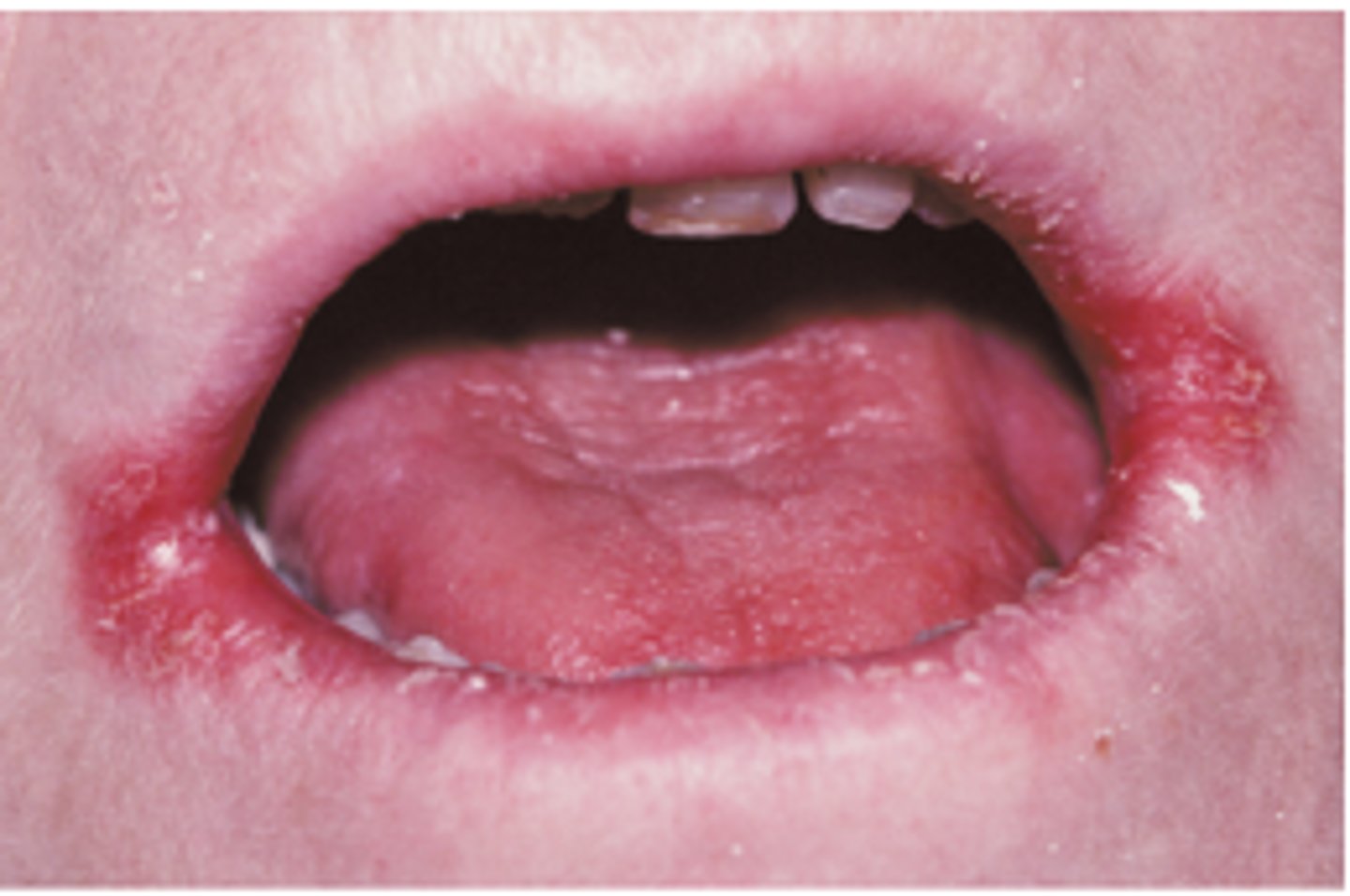
primary HSV
-at early age
-systemic symptoms
-vessicles followed by ulcers which may involved both keratnized and non-keratinized tissue
-punched out erosions in gingiva
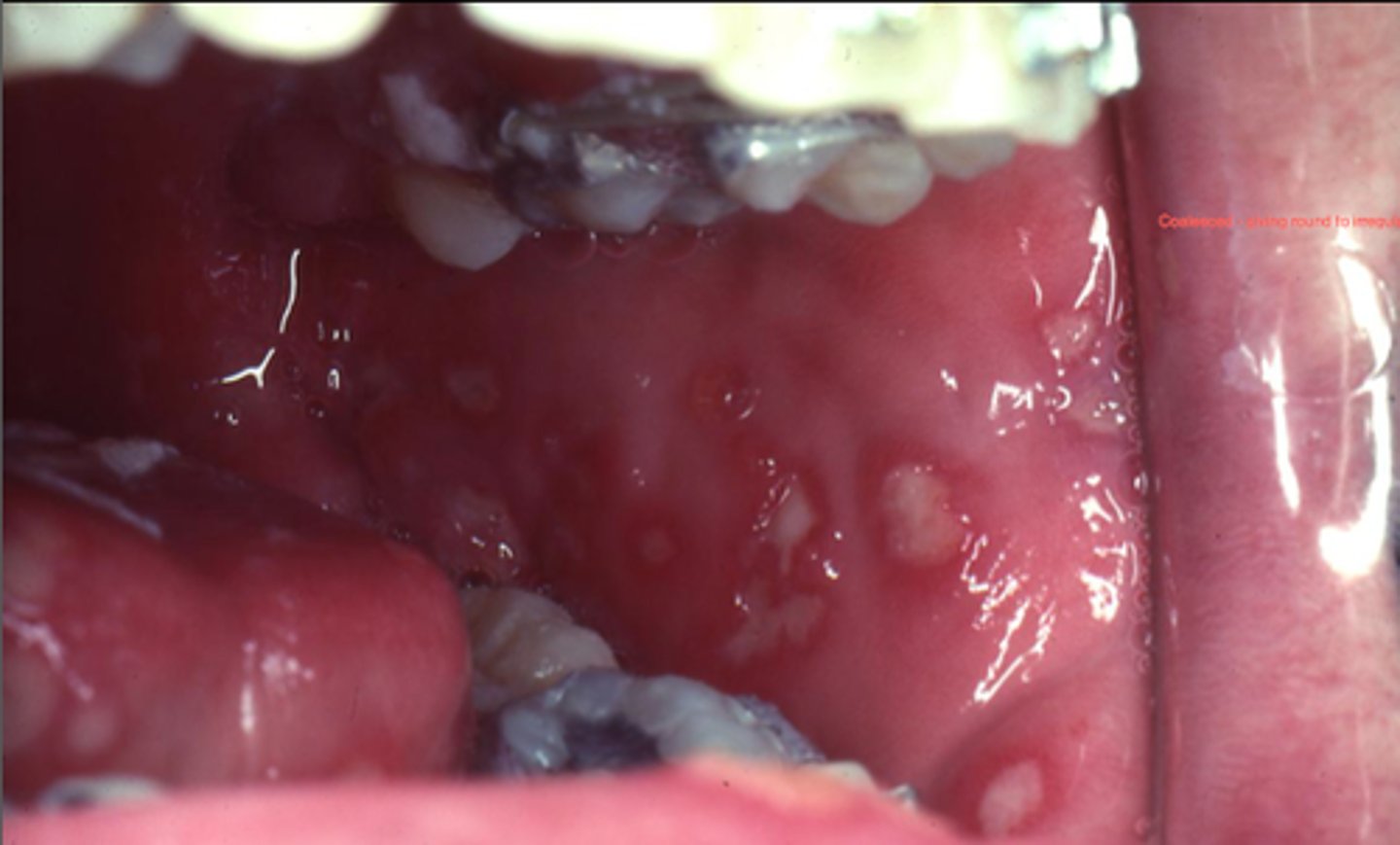
secondary /recurrent HSV
-triggered by trauma
-keratinized mucosa
-extraoral reoccurences = herpes labialis
-intraoral reoccurences limited to keratinized mucosa
-antivirals kay shorten duration
-can give anti-viral (valtrex) before appt.
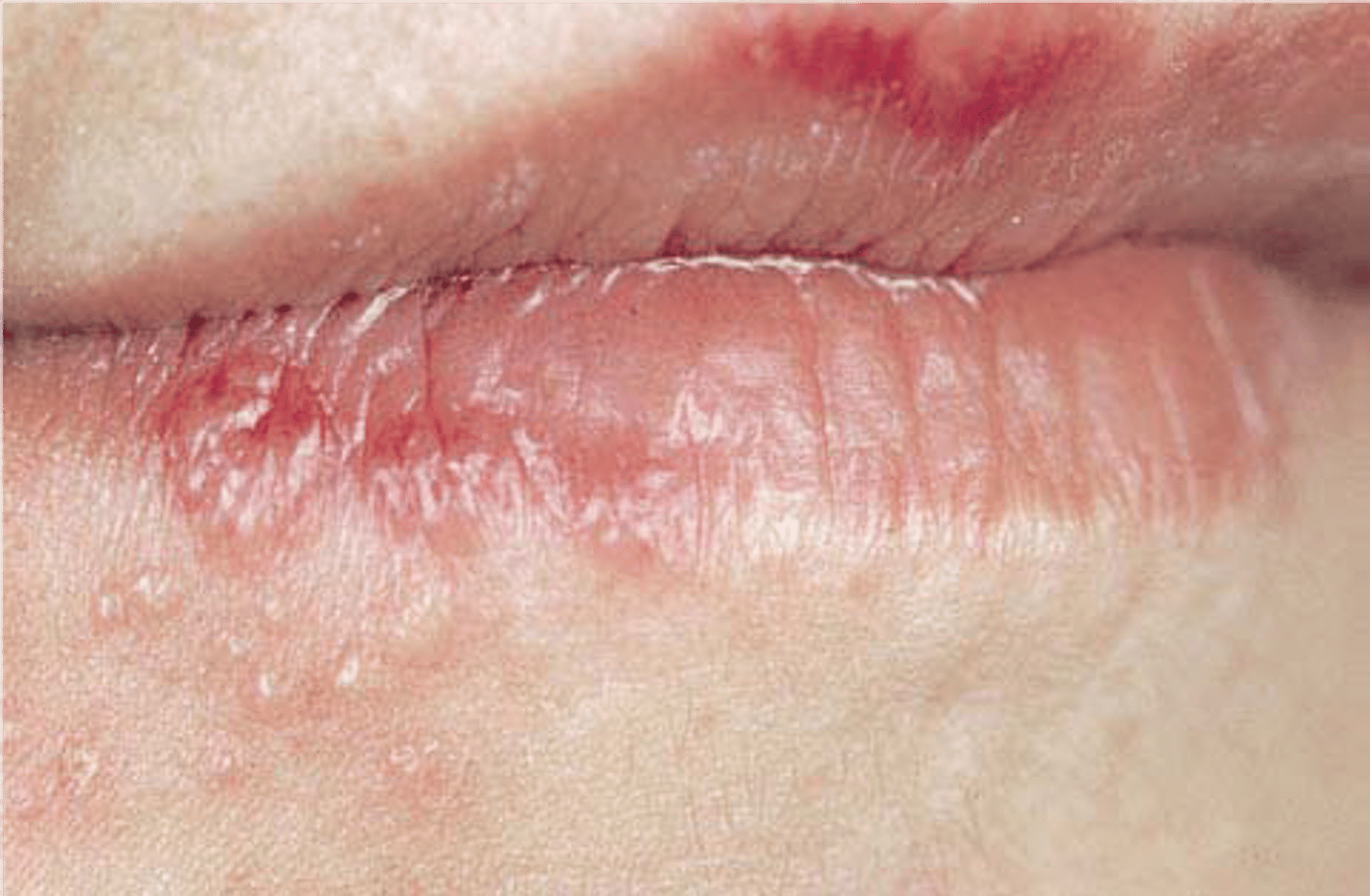
what are the differential diagnosis for white lessions ?
traumatic hyperkeratosis
oral lichen planus
hyperplastic candidasis
dysplasia (leukoplakia)