heart
1/216
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
217 Terms
heart anatomy q
what is the main function of the cardiovascular system
to deliver and remove molecules to meet the bodys demands
what system regulat the CV system
nervous and endocrine
what are the three main components of the cardiovascular system
heart, blood vessels. blood
what is the primary function of the heart
pumpms blood through the body
what regulator role does the heart have
sensory and endocrine functions for blood pressure and blood volume
what is the main function of blood vessels
act as tubular conduit system for blood
how do blood vessles help regulat the body
they act as sensory and effector organs for blood pressure regulation and blood distribution
what is teh primary function of blood
carriers materials to and from cells
what important communication role does blood have
transports hrmones between organs and systems
if the endorcine system releases hormones that increase blood volume, which component of the CV system directly carries out this change
blood and blood vessels (adjust distributiona nd pressure)
why are blood vessles considered both sensory and effector organs
they can detect changes like pressure and respond by constricging or dilating
if the heart has endocrine functions why is it important beyond just pumping
it helps reuglar blood pressure and volume by releasing hormones
what do the atria do
recieve blood
what do the ventricles do
pump blood out of the heart
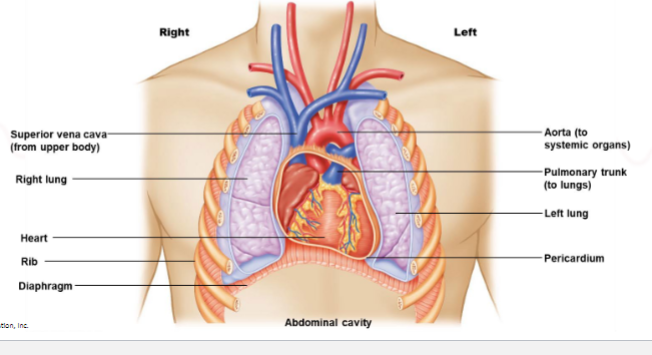
what is the pericardium
a protective sac that surrounds the heart
what are the two man parts of the pericardium
fibrous and serous
what is the function of the fibrous pericardium
provides protecion and prevents overexpansions of the heart
what is the function of serous pericardium
reduces friction as the heart beats
what is the heart wall made of
cardium (layer of cardiac tissue, mainly myocardium)
what is the function of myocardium
contracts to pump blood
which has tichker myocardium atria or ventricels
ventricles
why are the ventricles thicker
they pump blood out of the heart at higher pressure
which ventricle has the thickers left or right
leftw
why is the left ventricle thicker
it pumps blood to the entier body (systemic circulation) requiring higher pressure
what is the function of atrioventricular valves
allows blood flow from atria to ventricles and prevent backflow
when do AV valves open
when ventricles are relaxedw
what causes AV valves to open
blood entering the atria pushes valve cusps into the ventriceslw
when do AV valves close
when ventircles contract
what causes AV valvves to close
blood pressure pushes agains the cusps
what is the function of papillary muscles
contract to tighten chordae tendineae
what do chordae tendineae do
prevent AV valve cusps from flipping into the atria
what is the function of smielunar valves
allow blood to leave the ventricles and prevent backflow
when do semi vales open
when ventircels contract
what causes semi valves to open
blood pressure from ventircles pushing against the cuspswh
when do semi valves close
when ventricles relaxe
what causes them to clsoe
blood in the arteries pushes back against the cusps
Front: If the chordae tendineae were damaged, what would happen?
Back: AV valves could prolapse (flip into atria), causing backflow of blood
Front: Why don’t semilunar valves need chordae tendineae?
Back: Their structure and arterial pressure prevent backflow without needing support
Front: If the left ventricle became weaker, which circulation would be most affected?
Front: If the left ventricle became weaker, which circulation would be most affected?
Front: During ventricular contraction, which valves are open and which are closed?
Back: Semilunar valves open; AV valves closed
in what direction does blood flow in arteries vs veines
arteries carry blod away from the heart, veins carry blood toward the hear
what connect artiers and veins
capilliaries
what are arterioles
small branches of arteries leading to capillaries
what are venules
small vessels that collect blood from capilaires into veins
are artiers typically oxygenated or deoxygenated
oxygenated except pulmonary arters
how do artery walls compare to viens
arteries are thicker
what are capilaires made of
basement membrnaes (very thin for exchange)
what are artiers and veins made of
connective tissues, smooth muscle , and endothelium
what percentage of blood is plasma
55
what % is rbc
45
what % is wbc and platlets
1
what is the shape of erthyocytes RBC
biocanve disc
why are RBc bioncanve
increases surface area and flexibilty
what is the main function of RBC
transport oxygen and some carbond dioxide
what is the path of blood flow through the heart and body
Left atrium → left ventricle → body → capillaries (O₂ out, CO₂ in) → right atrium → right ventricle → lungs → back to left atrium
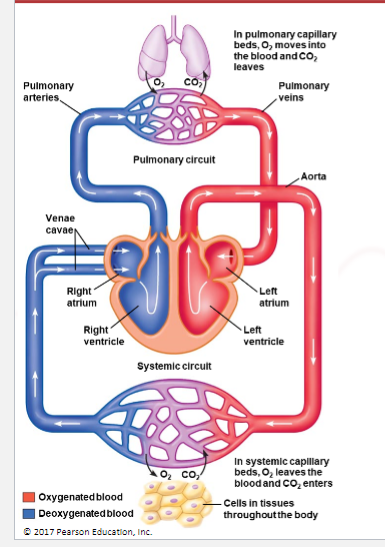
what happens at the capillaries in the systemic ciruclation
oxygen leaves and carbon enters
what do the lungs do in ciruclation
add oxygen to blood and remove carbon
what are the venae cavae
two large veins that return blood the to right atrium
what is series blood flow
blood flow through organs one after another
what is parallel blood flow
blood is distributed to multiple organs at the same time
why is parallel blood flow important
ensures all organs recive equal oxygen and nutrients
what advantage does parallel flow give the body
allows independent regulation of blood flow to different organs
what is regional control of blood flow
adjusting blood flow to specific organs based on need
why must cardiac muscle contract in a synchronized manner
to effectively pump blood throguh the body
what coordinates heart contractions
the conduction system in the myocardium
what is autorthmiticty
the hears ability to generate its own electrical activty
is the carida muscle myogenic or neurogenic
myogenic (self initiated)
is skeletal muscle myogenic or neurogenic
neurogenic (requires nerve input0
what are pacemaker cells
specialized cells that spontaneously generate action potentiasl
where are pacemaker cells primairly located
SA and AV node
which node sets the pace of the heart
SA node
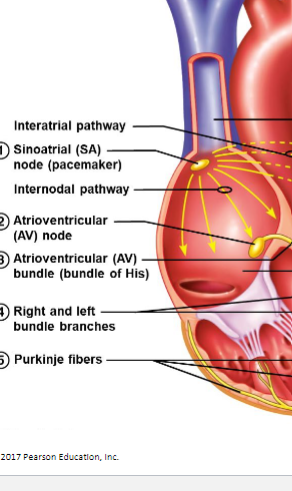
what is the function fo conduction fibers
transmit action potentials through the ehart
what is unique about conduction fibers
they are large damtere cardiac cells that conduct signals quickly
if capilaries were thicker how would gas exchange be affected
it would decrease because diffusion distance increases
why can the body send more blood to muscles during exericse
paralles flow allows redistribution of blood
if the sa node stops working what happens
another pacemaker like AV node takes over but at a slower rate
why is the heart bale to beat without the nervous sytem input
becuase it is myogenic and has autorhythmic pacemaker cells
if arteirs lose elasticity how would blood presusre be affected
blood presure would increase
what is the normal conduction pathway of the heart
Back: SA node → atrial muscle → AV node → AV bundle → right and left bundle branches → Purkinje fibers → ventricular muscle
what happens to the AP at the AV node
conduction slows to allow the atria to contract before the ventricels
where does the AP start
SA NODE
how does the AP potential travel to the apex of the heart (THE BODY)
rapidly through the conduction system ( AV bundle → bundle branches → Purkinje fibers
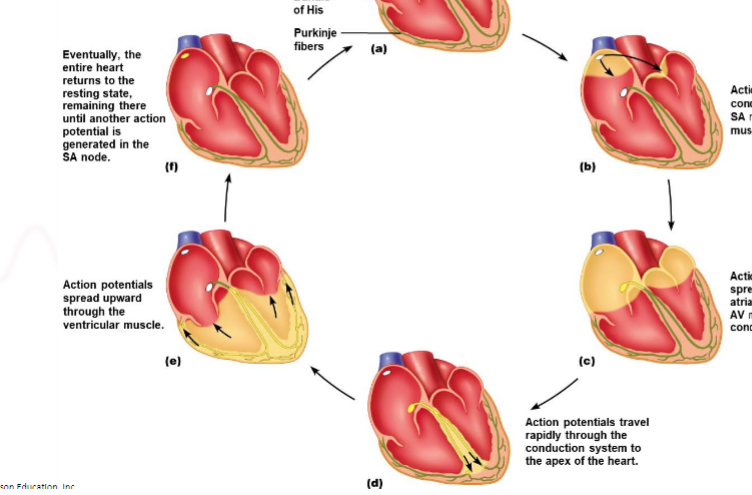
how does ventricular contraction occur after the AP reaches the apex
AP spreads upwards throughly ventricular muscle, causing coordinated contraction
what happens after the action passes through the heart
the heart reutrns to resting state untile the next AP
what is an ecg
non invasice recoridng of the hearts electrical activty
why can electrical acitvty be recorded on the body surface
body fluids conduct the electircal current generated by nervous nad muscle tissue
what does each ECG lead represent
a differntly electrical view of the heart showign direction and magnitude of current
which direction does current flow in a standard ECG lead
Back: Positive electrode → left atrium/ventricle; negative electrode → right atrium/ventricle (direction depends on lead)
what does the p wave reprensent
atrial depolarization
what does p wave represent
atrial depolarization
what does QRS complex represent
ventricular depolarization
what does the t wave represent
ventricular repolarization
what does an ecg loook like
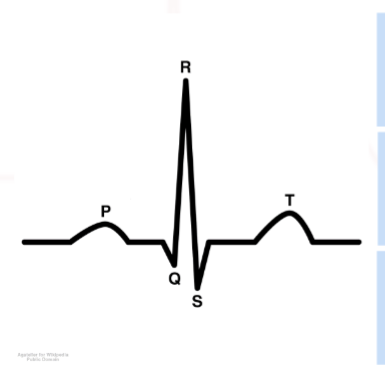
what is lead 1 positve nad negative
+ left arm
- right arm
what is lead 2 pos and neg
pos left leg
neg right arm
what is led 3 pos and neg
pos left leg
neg left arm
how do the p wave, qrs, t wave direction relate to lead polarity
waves point toward the positive electrod, away from positive= downward deflection
what ECG wave corresponds to ventricular depolarization
QRS
what wave relates to ventricular repolariation
T wave