Aquifer 17: 4-year-old female refusing to walk
1/48
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
49 Terms
Differential Diagnosis of Limp or Refusal to Walk
Leukemia
Osteomyelitis
Reactive arthritis
Septic arthritis
Trauma
Transient synovitis
JIA
Slipped capital femoral epiphysis
Legg Calve Perthes disease
How can leukemia cause limping
- BM replacement by leukemic cells > bone pain > limp, refusal to walk, localized discomfort of jaw, long bones, vertebral column, hip, scapula or ribs.
- Bone pain may precede systemic signs such as fever and weight loss.
- Always considered in a child refusing to walk.
How can OM present
- Presents with bony tenderness and refusal to bear weight (when affecting a leg bone).
- Fever is present in 50%
- Ilium or proximal femur may present with hip pain.
What is reactive arthritis
- Inflammatory arthritis
- 2-4 weeks after an infection elsewhere in the body (GIT/GUT)
- Mono or oligoarticular
Reactive arthritis joint aspiration
- Aspiration of synovial fluid may show inflammatory cells but the gram stain and culture are negative.
Reactive arthritis presentation
- Classic association with urethritis and conjunctivitis is uncommon in children.
- Children are frequently afebrile at presentation.
What age does septic arthritis occur
0 to 6 years.
How does septic arthritis present
- Single joint, usually LL
- High fever is common, decreased appetite, irritability, malaise
What is transient synovitis
- Inflammation and swelling of the tissues around the hip joint during or following a viral URI.
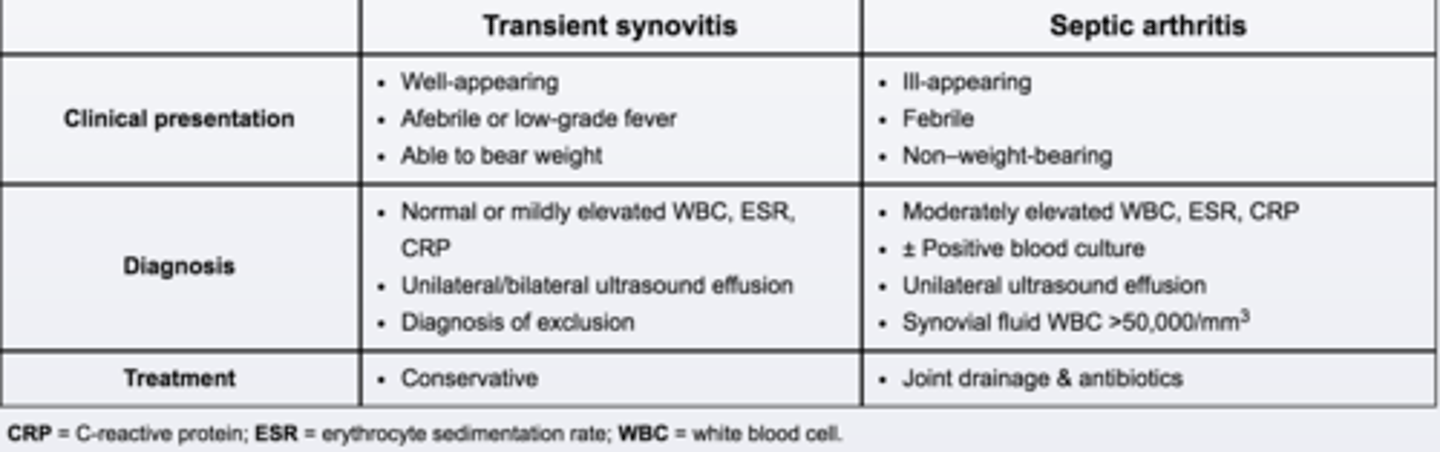
How does transient synovitis present
- Acute onset of joint pain w/o significant constitutional symptoms other than low-grade fever.
What age does transient synovitis occur
Peak age is 3 to 8 years.
Transient synovitis tx
Rest and ibuprofen.
How long does TS last
The pain resolves within 3 to 10 days.
Recurrence and Prognosis of TS
- Small chance of recurrence
- No serious or long-lasting consequences
- Does not predispose to arthritis in the future.Ibuprofen Dosing and Concentration
JIA diagnostic criteria
- <16 years
- Arthritis in at least 1 joint for more than 6 weeks
JIA subtypes, oligoarticular JIA presentation
- Oligoarticular > F, onset before 5y, knees and ankles are the most common joints involved

What is the most common hip disorder in adolescents
Slipped capital femoral epiphysis
What is SCFE
- Posterior displacement of the capital femoral epiphysis from the femoral neck through the cartilage growth plate
- Causes limp and impaired internal rotation
- Occurs more in adolescents with obesity, suggesting that mechanical strain on the growth plate could be at least partially responsible for the slip. Endocrine factors also may be important.
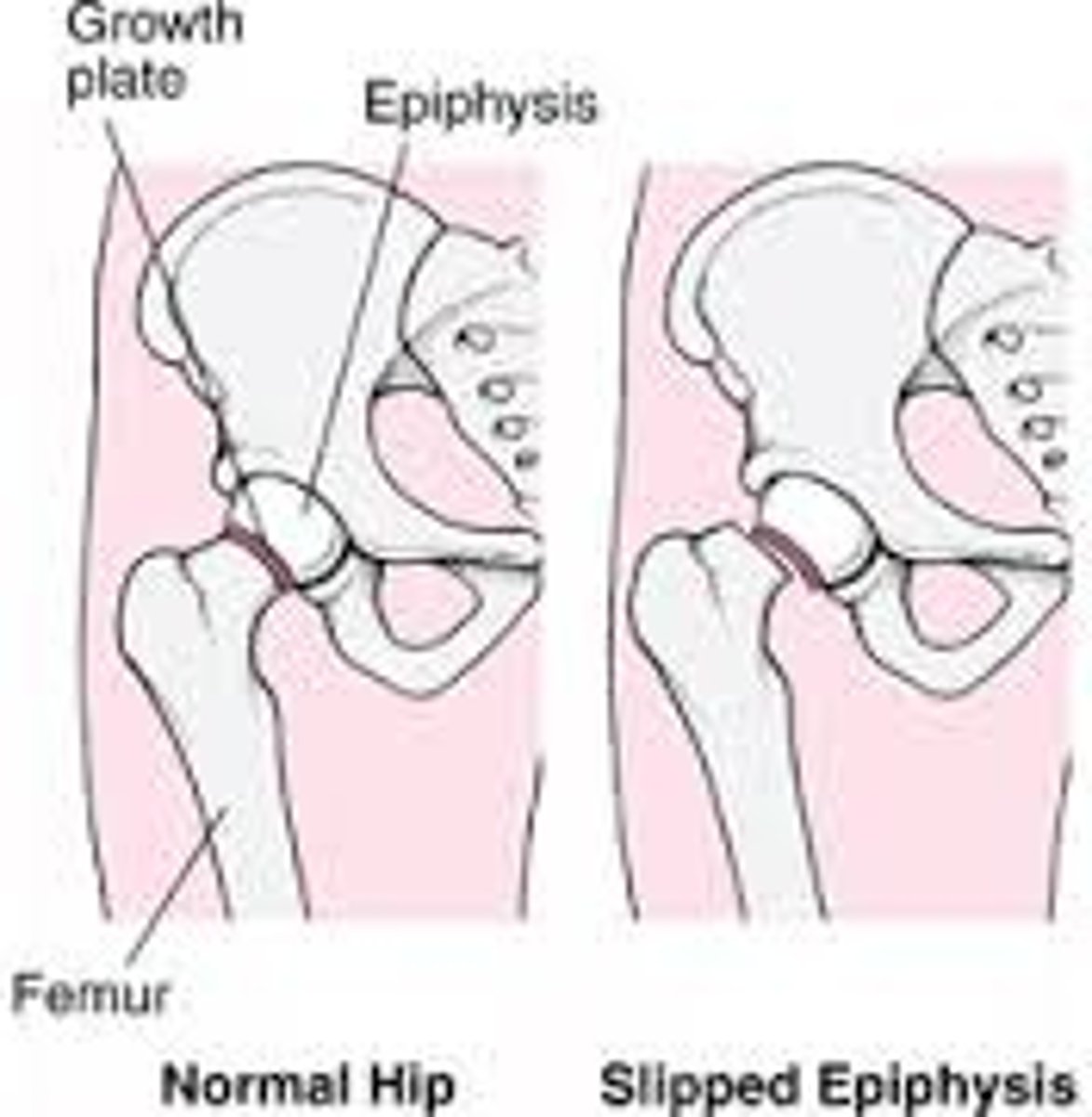
How does SCFE present
months of vague hip or knee symptoms and limp with or without an acute exacerbation
How to diagnose SCFE
- Plain film showing posterior displacement of the femoral head, like an ice-cream scoop slipping off a cone.
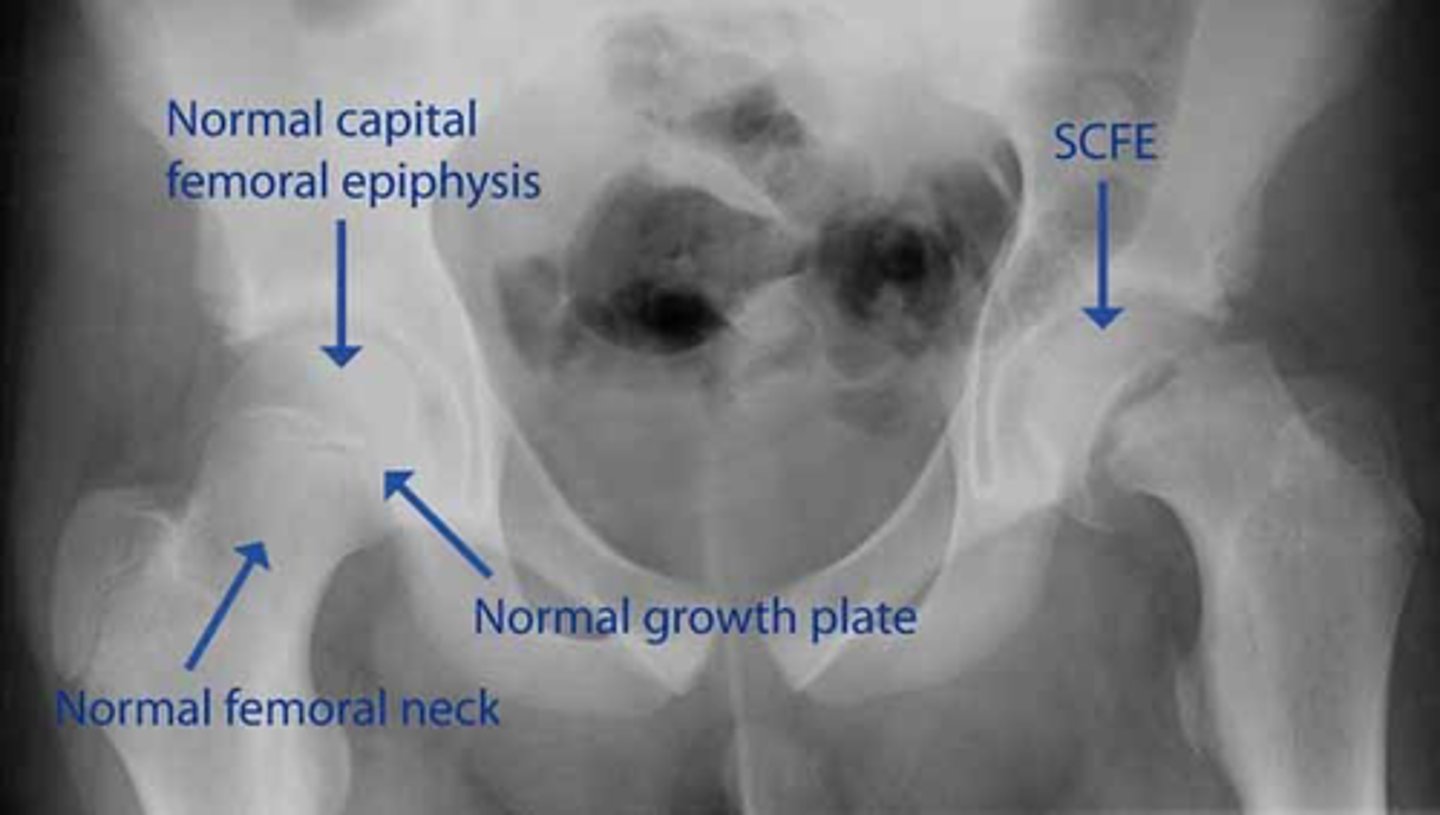
SCFE prognosis
- Depends on degree of slip and accompanying complications like avascular necrosis of the femoral head and destruction of the articular cartilage
SCFE tx
Pinning to stabilize the epiphysis but no manipulation.
Legg Calve Perthes disease age group
- M
- 4-10 years.
What is Legg-Calve-Perthes disease?
- Idiopathic avascular necrosis of the femoral head
- Various etiologies: infectious, trauma, developmental, and prothrombotic conditions.
How does LCP present, course/prognosis
- Indolent/chronic course
- Typically self-resolving, but may lead to complications including femoral head deformity and degenerative arthritis.
LCP tx
- Referral to an orthopedic surgeon > preventing damage to the hip by containing the femoral head within the acetabulum, ideally through conservative methods.
Signs of accidental trauma
- Bruises over bony prominences (e.g., shins and forearms)
Signs of non accidental trauma
Bruises seen over well-cushioned areas (e.g., buttocks, back, and genitalia)
Taking a History in a Child With a Limp
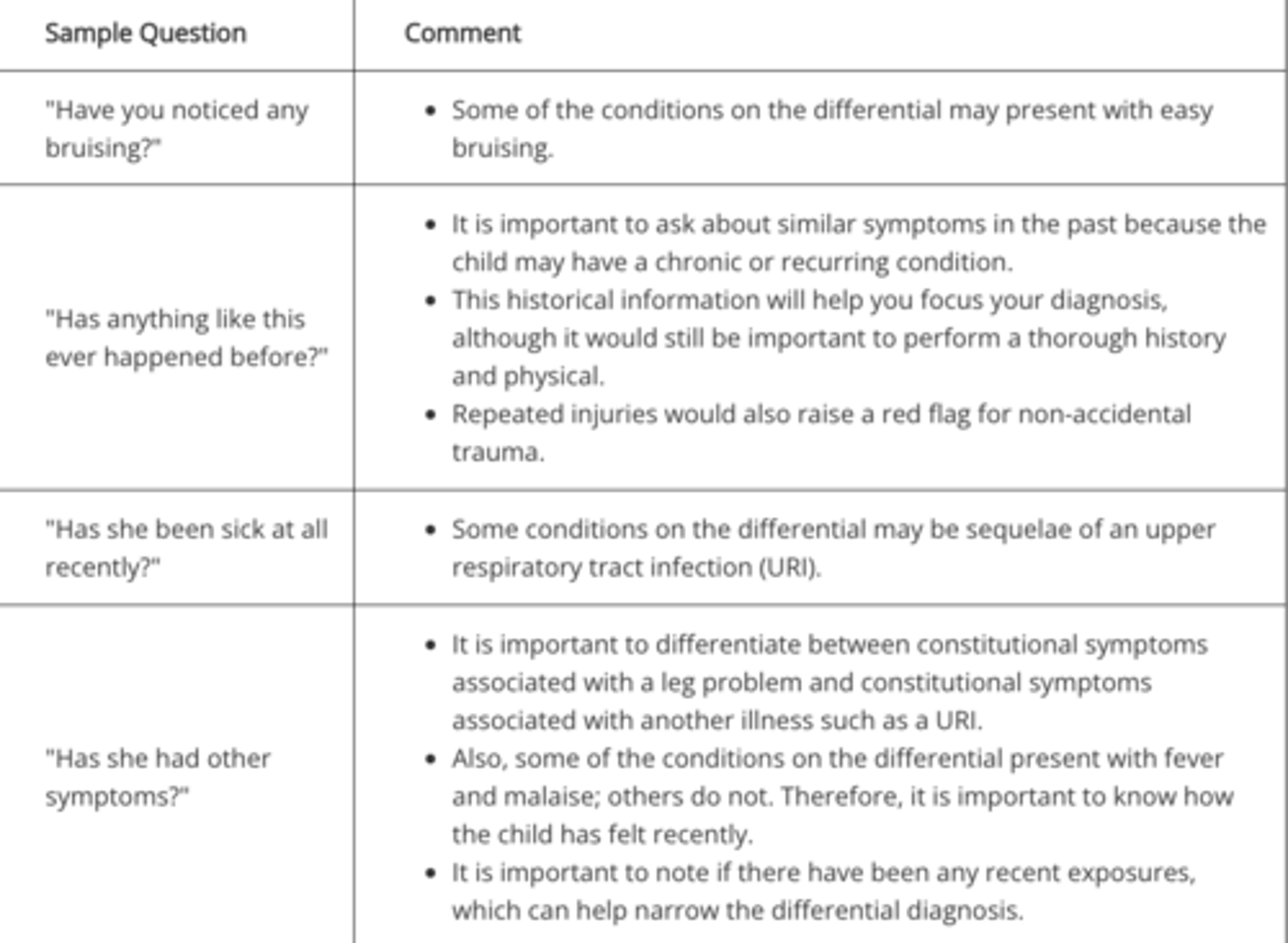
What is lyme disease
tick-borne illness caused by Borrelia burgdorferi.
How does lyme disease present
- Erythema migrans (macular, annular, red rash expanding slowly from site of tick bite)
- Arthritis (mono/oligoarticular, large joints like knee)
- Fever, malaise, fatigue, and headache.
Is arthritis common in Lyme disease
- Arthritis is the 2nd most common manifestation of Lyme disease
- Most common manifestation of late Lyme disease.
When does arthritis present in LD
- Weeks to months after the skin lesion (absence of erythema migrans does not exclude)
- May relapse or occur only once.
Leukemia presents with
- Pallor, bruising, lymphadenopathy or hepatosplenomegaly
- Pain is bony tenderness, unaffected by position or movement of the joint.
Strongest risk factors for septic arthritis
CRP > 2 .0 mg/dL (20 mg/L) and non-weight bearing) i
Predictors of septic arthritis of the hip

Evaluation of Painful Hip Lab tests
- CBC
- CRP
- ESR
- Blood culture (+ve in SA, OM)
Where can ESR + CRP be elevated
Infections
Malignancies
Inflammatory conditions
JIA
Leukemia
ESR is a
- Indirect measurement of fibrinogen elevation (fibrinogen is an acute phase reactant which increases with inflammation)
- Higher levels of fibrinogen lead to increased cohesion of erythrocytes and therefore a faster rate of erythrocyte sedimentation
ESR Elevation time course
- Slow rise in response to an inflammatory stimulus
- May not return to normal for weeks after clinical improvement occurs.
ESR specificity
- Not specific for inflammation > also abnormal in pregnancy and anemia
- Low to moderate reproducibility
What is CRP
- Direct quantification of an acute phase response
CRP Elevation time course
- Quick elevation, starts at 4-6h after initial insult, peaking at 36 to 50 hours, and returning to normal within 3 to 7 days after the stimulus is withdrawn.
CRP specificity
- More specific than ESR
- High reproducibility
How is septic arthritis diagnosed
Arthrocentesis
US hip joint
- Confirms effusion and guides aspiration
Characteristics of Synovial Fluid in Septic Arthritis

Most Common Causative Organisms in SA

SA TX
Empiric IV antibiotics
- Immediately after joint fluid is obtained and sent for culture.
- Coverage narrowed once a specific organism and its antibiotic sensitivities are identified.
Surgical incision and drainage
- Remove debris and reduce the pressure in the hip joint.
Prolonged course of antibiotics and repeated aspiration or incision and drainage to remove reaccumulated purulent effusion.
Ibuprofen Dosing and Concentration
