nurs 210: chapter 18 - cardiovascular system, heart
1/86
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
87 Terms
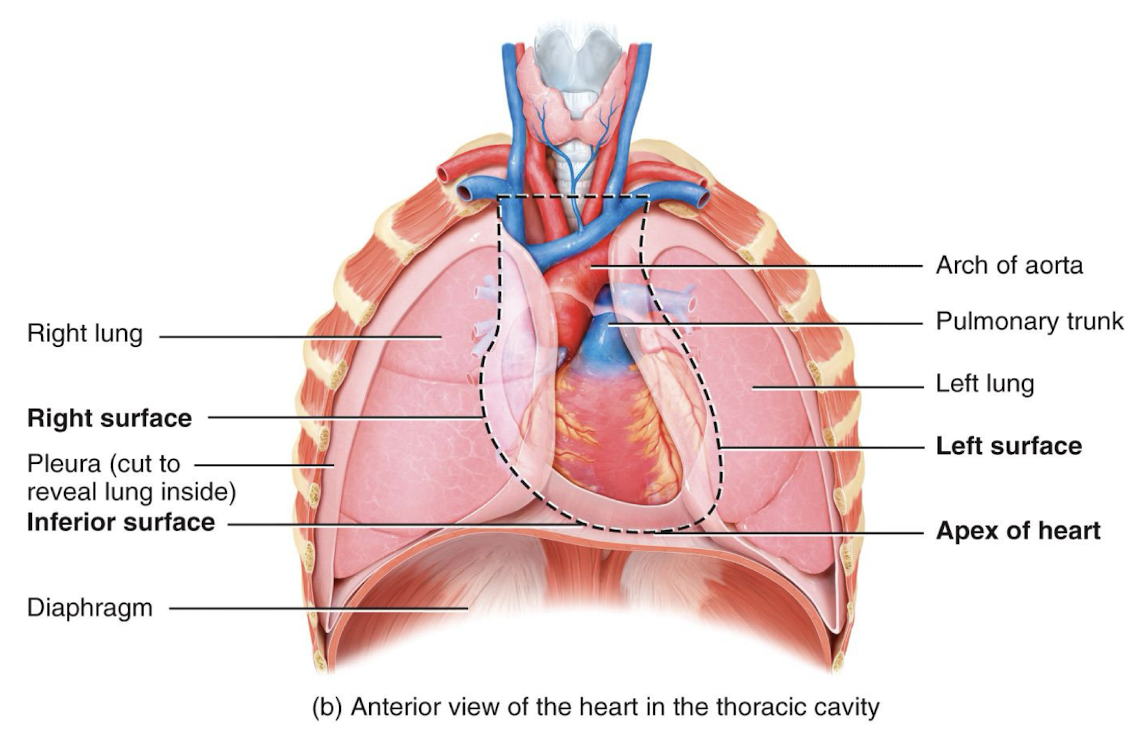
the heart is located in:
the mediastinum
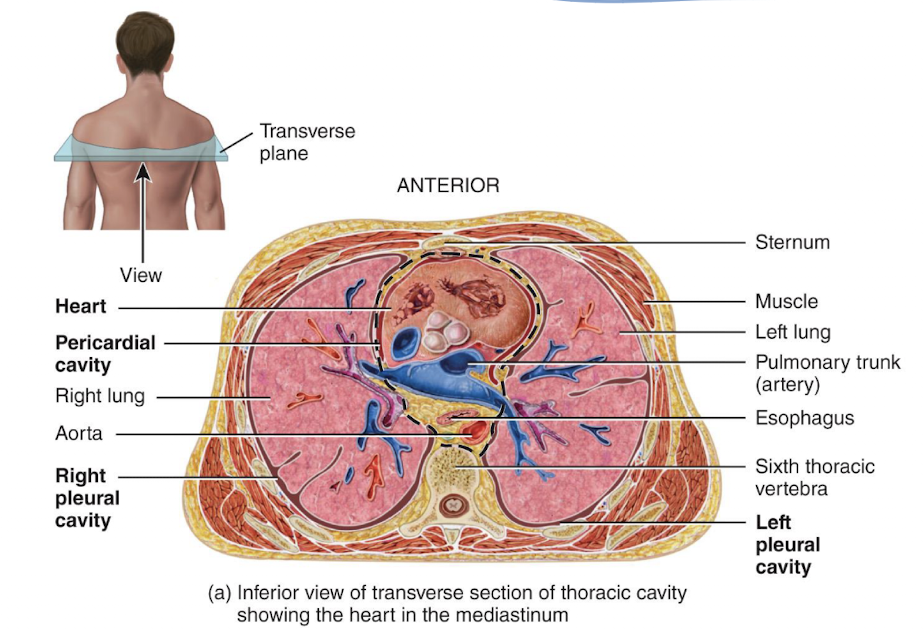
picture of location of heart
the heart is enclosed and held in place by:
the pericardium
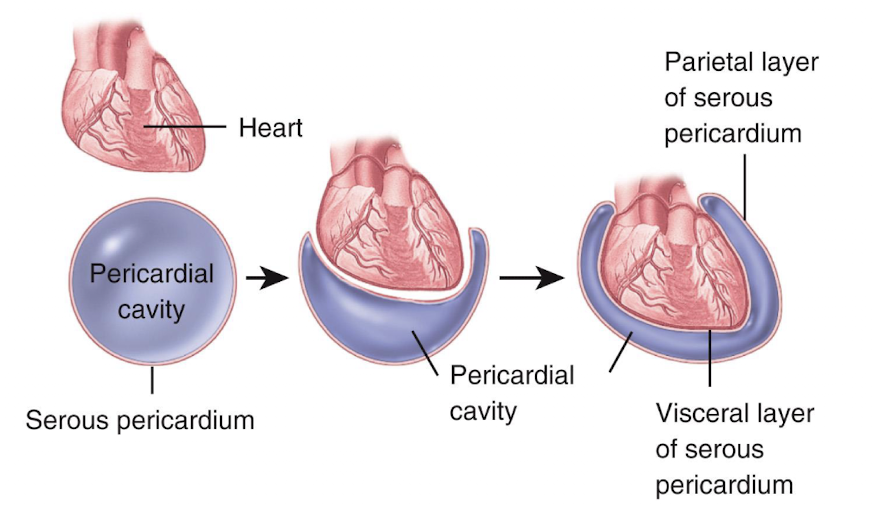
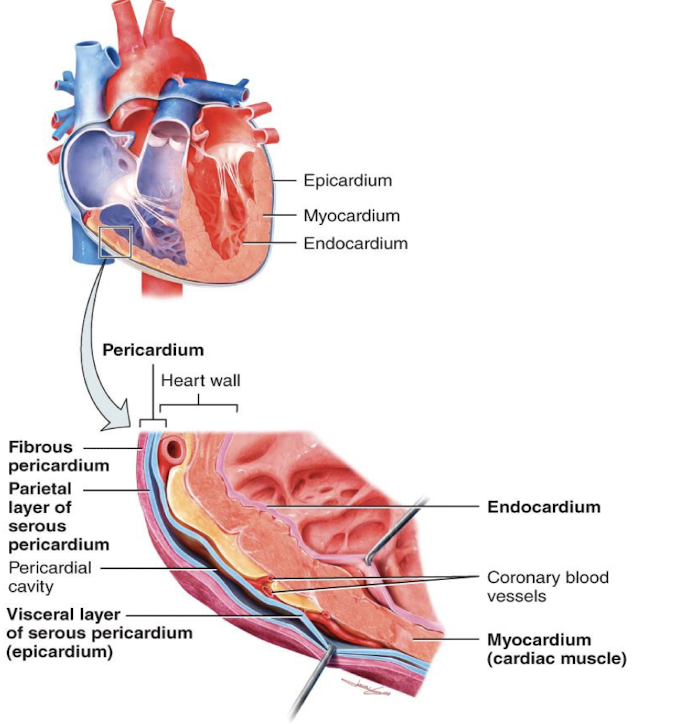
pericardium consist of:
an outer fibrous pericardium and an inner serous pericardium
serous pericardium has 2 layers:
visceral, parietal
visceral and parietal layers are separated by:
the serous cavity, which is a fluid-filled space
the walls of the heart has 3 layers:
epicardium
myocardium
endocardium
1 being the outermost, 3 being the innermost
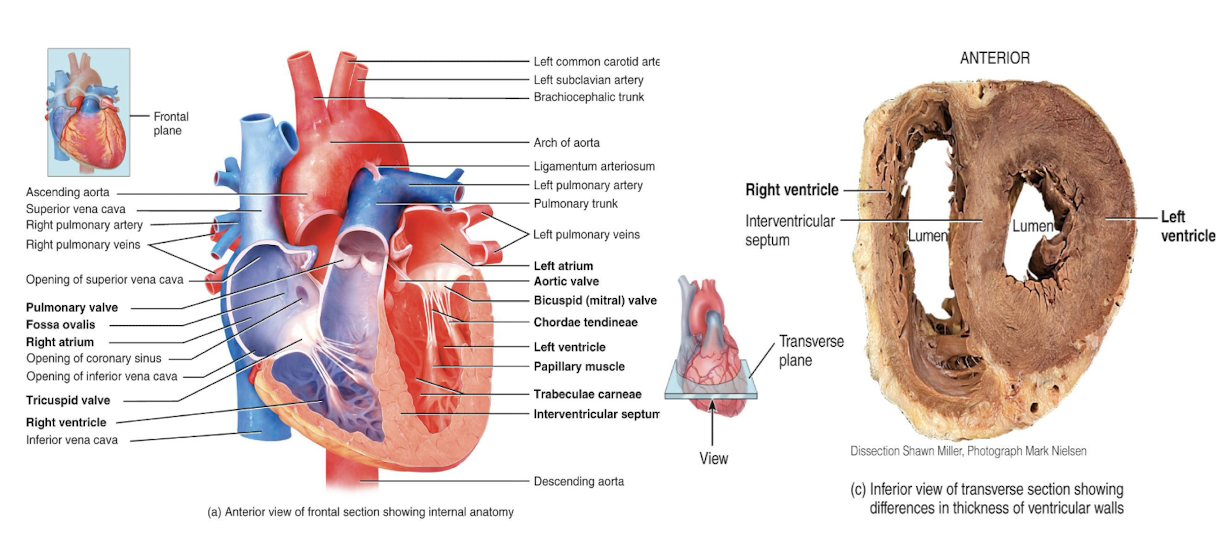
chambers of the heart include:
two upper atria, and two lower ventricles
right atrium receives blood from:
superior and inferior vena cava, along with the coronary sinus
right ventricle receives blood from:
the right atrium and sends blood to the lungs
left atrium receives blood from:
the pulmonary veins
left ventricle receives blood from:
the left atrium and sends blood all over the body
the wall of the left ventricle is more:
thicker than that of the right ventricle since it pumps blood throughout entire body, while right only does for lungs
heart valves ensure:
unidirectional blood flow through heart, along with opening and closing in response to pressure changes
two major types of valves:
atrioventricular valves, semilunar valves
atrioventricular valves (right and left)
located between atria and ventricles, which prevent back flow from ventricles into atria
semilunar valves (right and left)
located between ventricles and major arteries, prevent back flow from arteries into ventricles
two atrioventricular (AV) valves are:
tricuspid and mitral (bicuspid)
tricuspid valve (right AV valve)
made up of three cusps and lies between the atria and ventricle
mitral valve (left AV valve, bicuspid valve)
made up of two cusps and lies between left atria and ventricle
chordae tendineae
anchor cusps of AV valves to papillary muscles that function to: hold valve flaps in closed position, prevent flaps from everting back into atria
picture of function of atrioventricular (AV) valves when opened
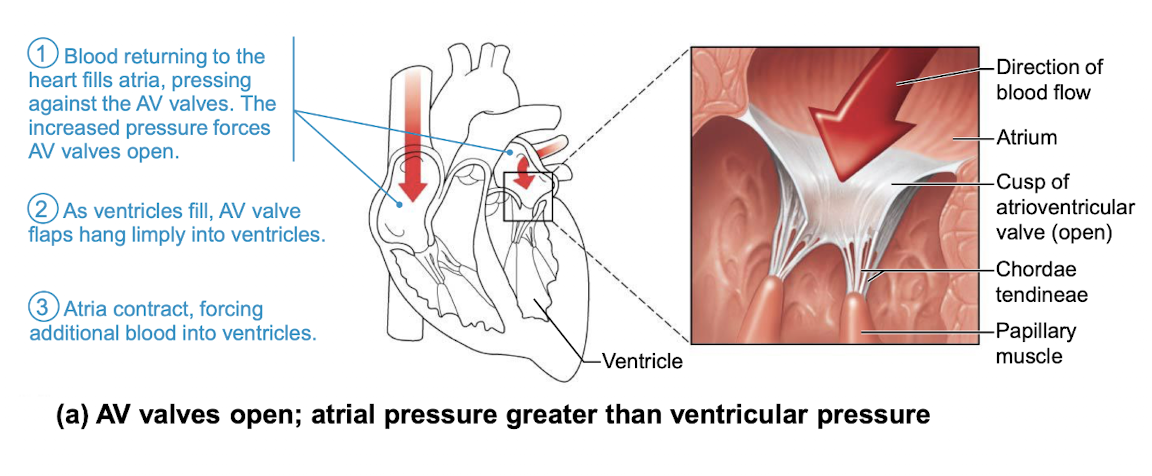
picture of function of atrioventricular (AV) valves when closed
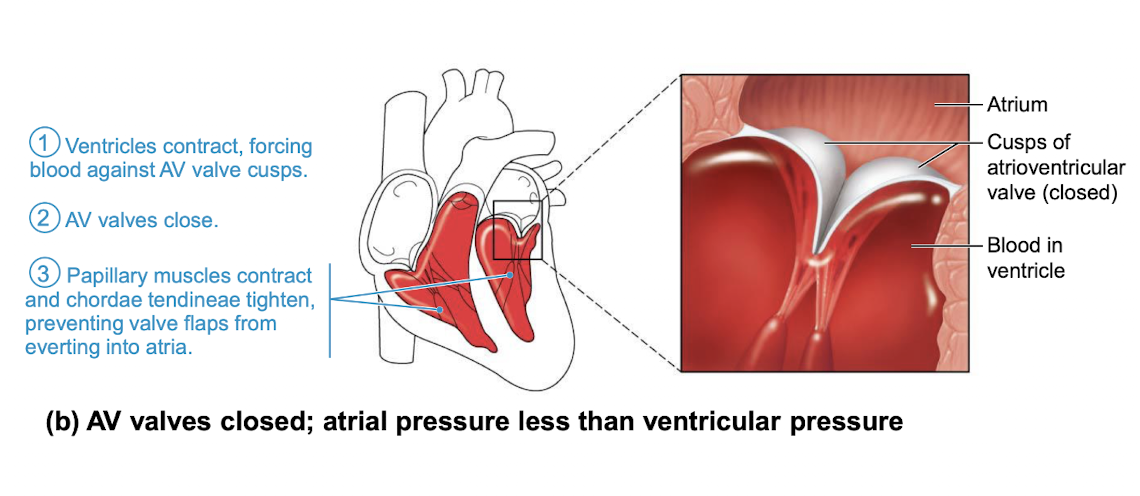
two semilunar (SL) valves prevent:
backflow from major arteries back into ventricles
the semilunar (SL) valves also:
open and close in response to pressure changes, with each valve consisting of three cusps that roughly resemble a half moon
pulmonary semilunar valve
located between right ventricle and pulmonary trunk
aorta semilunar valve
located between left ventricle and aorta
picture of function of semilunar valves opening:
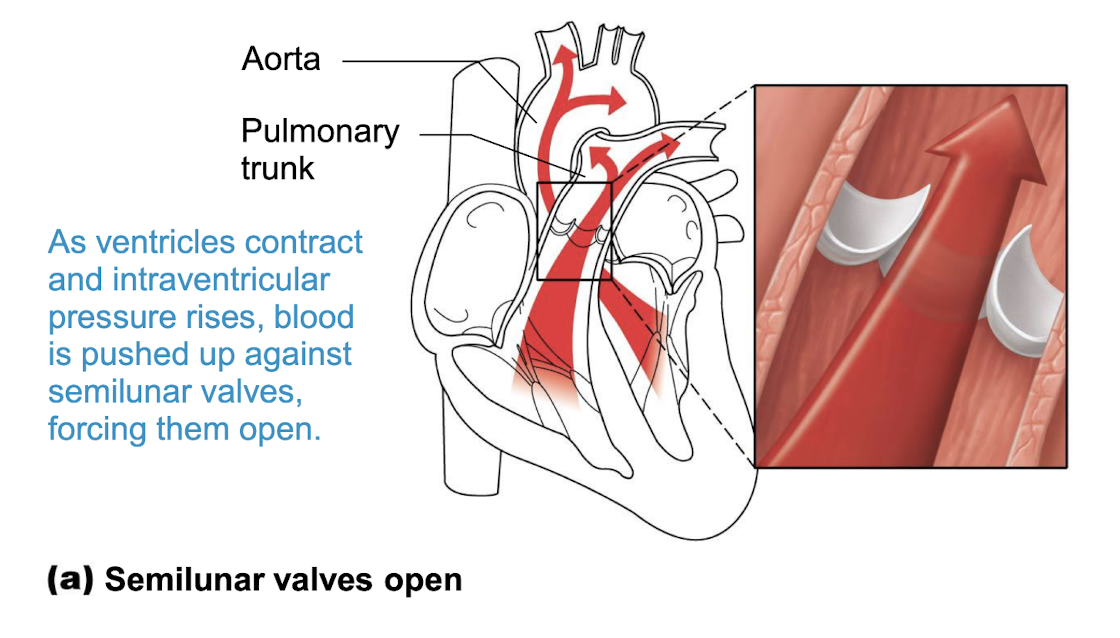
picture of semilunar valves closing:
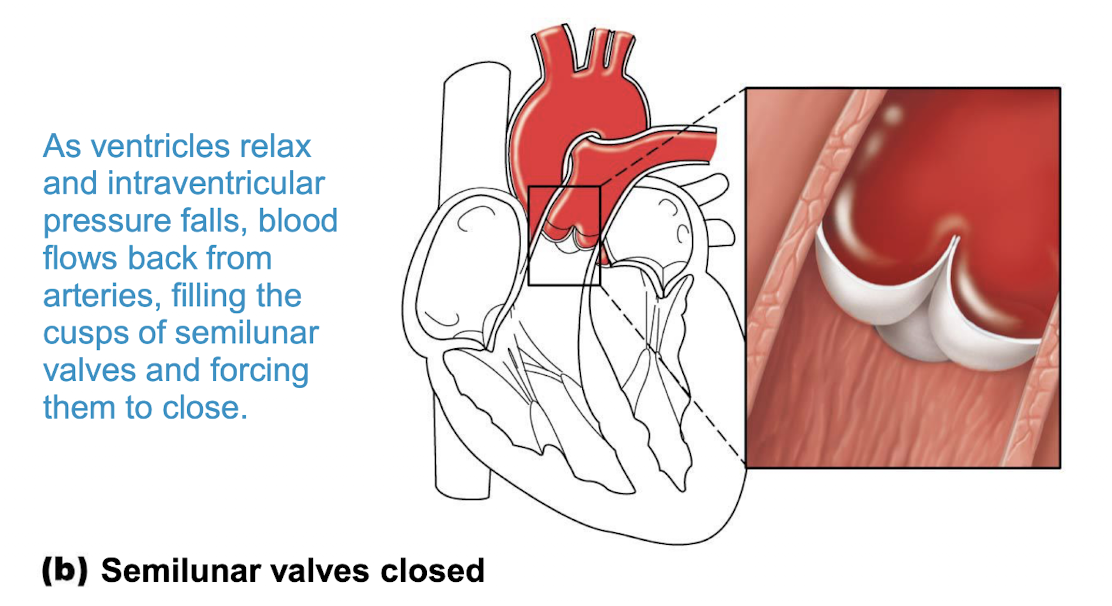
picture of heart valves and chordae tendineae:
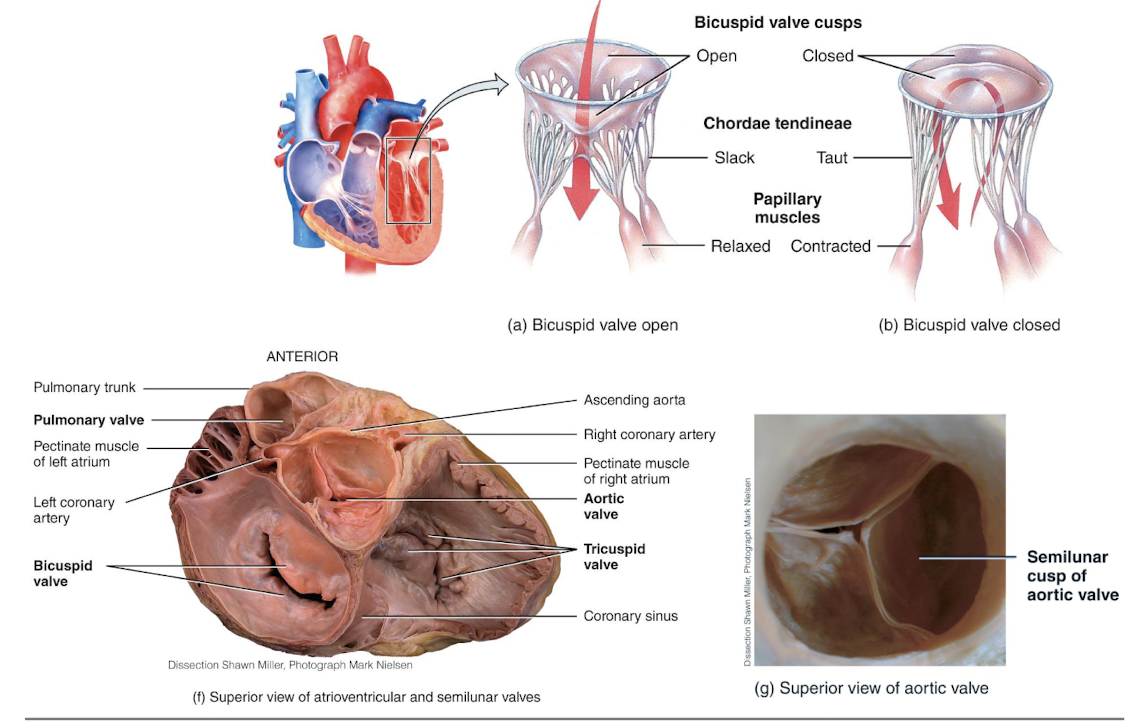
picture of blood flow through heart:
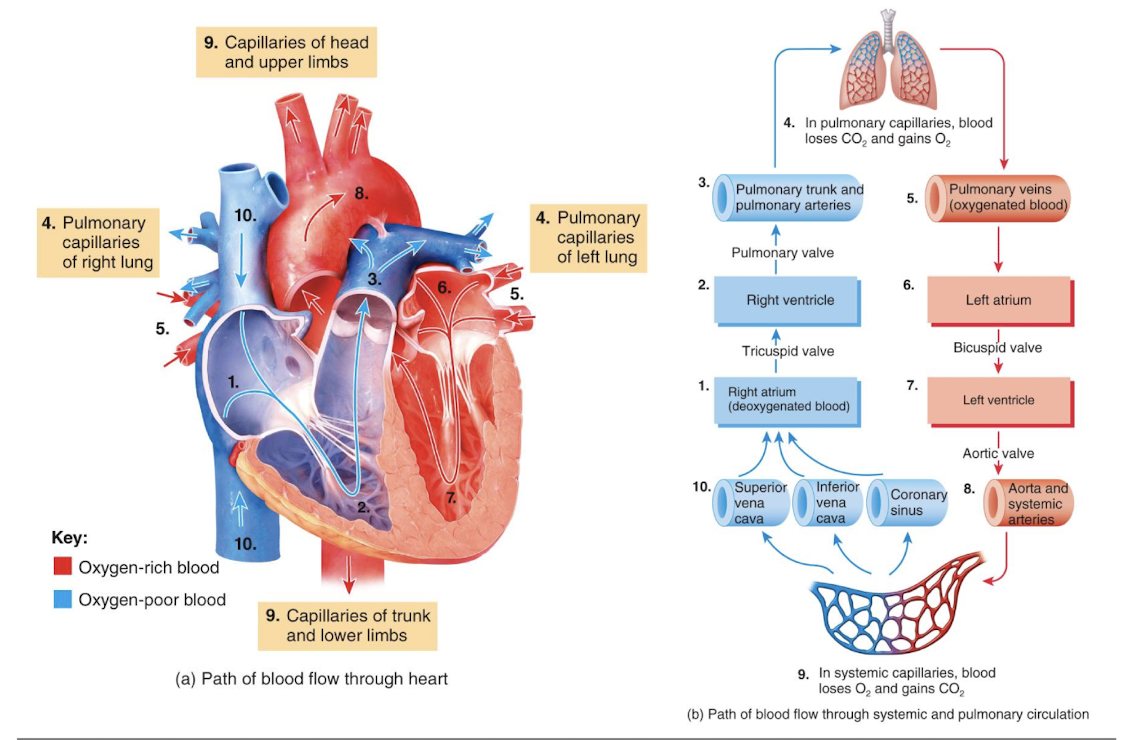
blood flow through coronary arteries delivers:
oxygenated blood and nutrients to the myocardium, with branches arising from ascending aorta
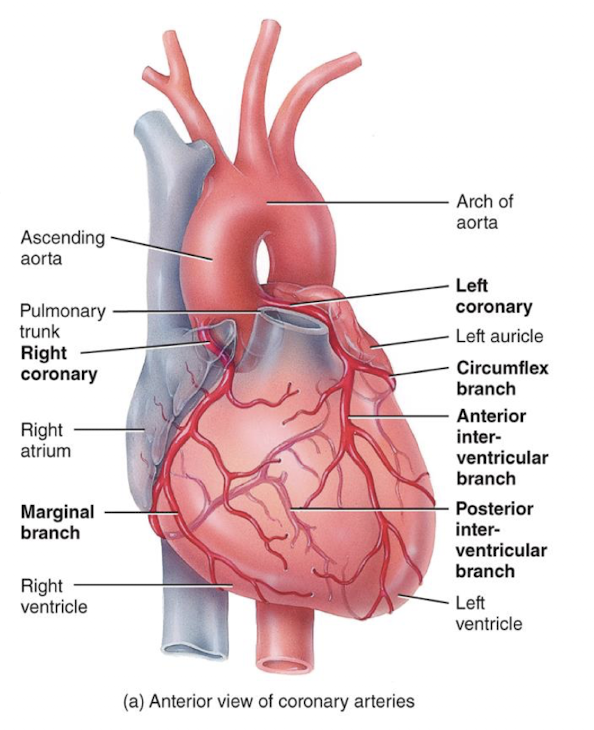
coronary veins remove:
cardbon dioxide and wastes from myocardium, with branches convering at the coronary sinus
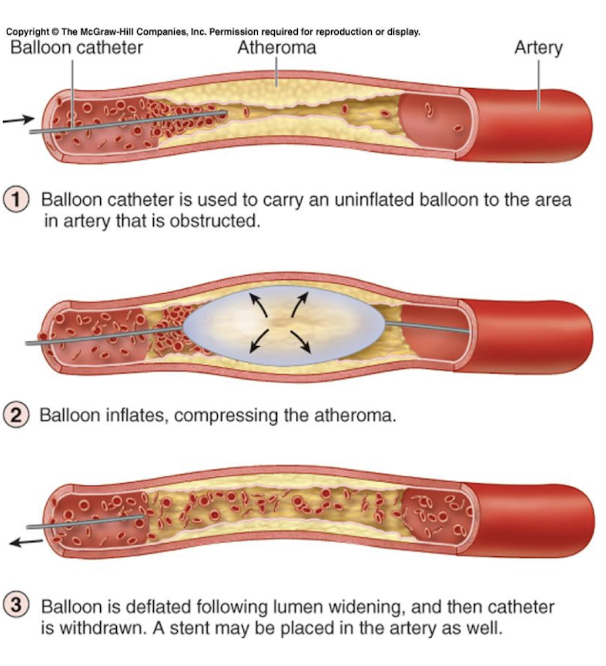
coronary arteries are a frequent site of:
occlusion that can lead to a myocardial infarction (heart attack); leads to prolonged coronary blockage, areas of cell death are repaired with noncontractile scar tissue
The ________ directs blood from the ________ of the heart to the lungs. Backflow of blood to the heart is prevented by ________. Blood from the lungs returns to the heart via ________.
pulmonary tract, right ventricle, pulmonary valve, pulmonary veins
The ________ directs blood from the ________ of the heart to the systemic sirculation. Backflow of blood to the heart is prevented by ________. Blood from the organs returns to the heart via ________.
aorta, left ventricle, aorta semilunar valve, veins?
cardiac muscle cells are:
self-excitable, and therefore, autorhythmic; they repeatedly generate spontaneous action potentials that trigger heart contractions, with these cells forming the conduction system: the route for propagating action potentials through heart muscles
picture of the conduction system:
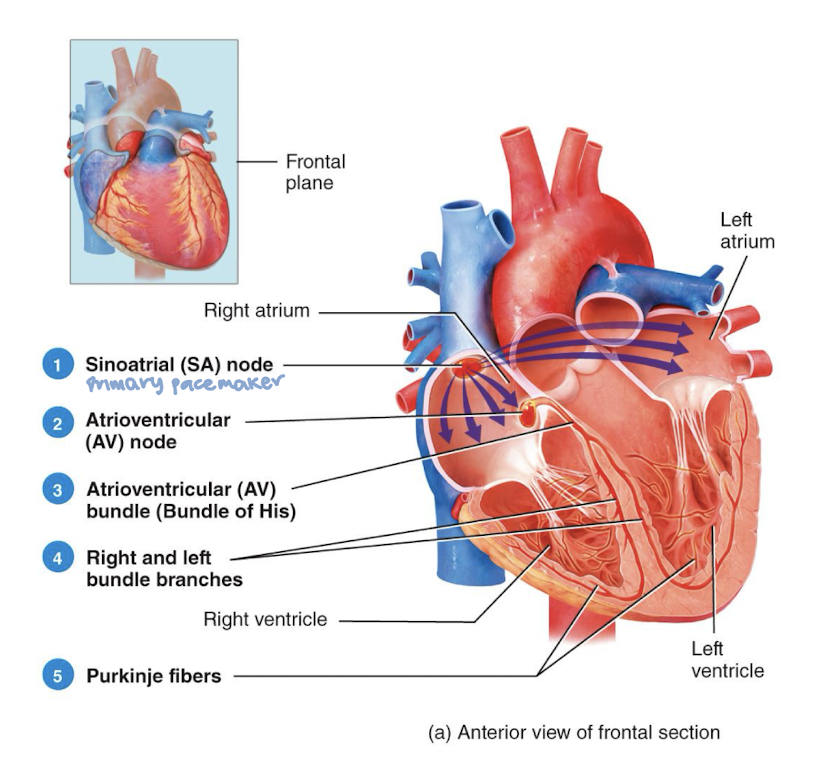
autorhhythmic cells in SA node are:
the natural pacemaker of heart since they initiate action potentials
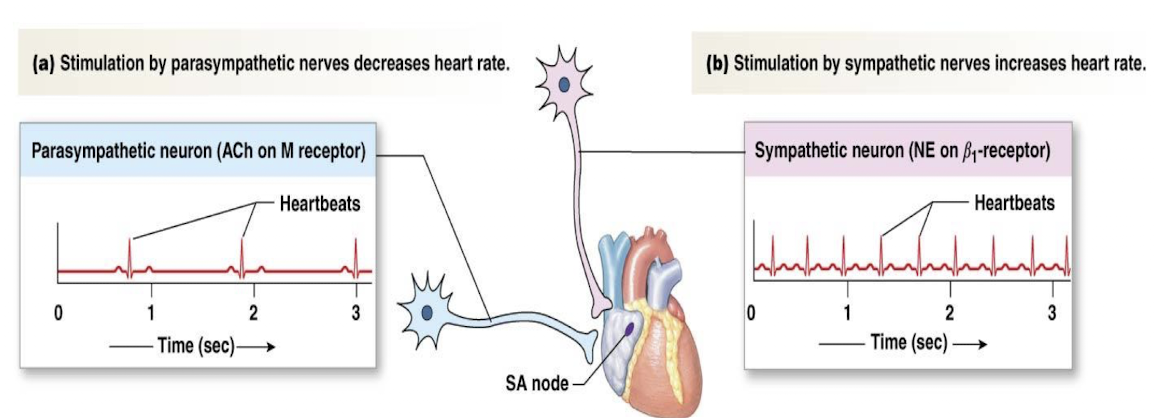
signals from the nervous system and hormones (like epinephrine) can:
modify heart rate and force of contraction, but not responsible for initiating the excitation of cardiac muscle
electrocardiogram (EKG or ECG)
a recording of the electrical changes that accompany each heart cycle
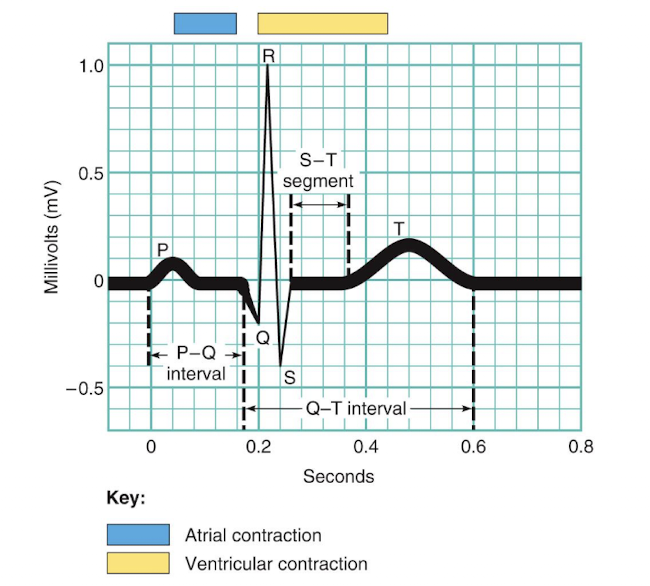
electrocardiogram main features
p wave, qrs complex, t wave, p-r interval, s-t segment, q-t interval
p wave
depolarization of SA node and atria
QRS complex
ventricular depolarization and atrial repolarization
t wave
ventricular repolarization
p-r interval
beginning of atrial excitation to beginning of ventricular excitation
s-t segment
entire ventricular myocardium depolarized
q-t interval
beginning of ventricular depolarization through ventricular repolarization
in an electrocardiogram, mechanical events occur after electrical events, with:
contraction following action potential
mechanical events of electrocardiogram:
heart rate: time between two p waves or two q waves
rhythm: regular pattern
waves analysis: presence and shape
segment length: constant
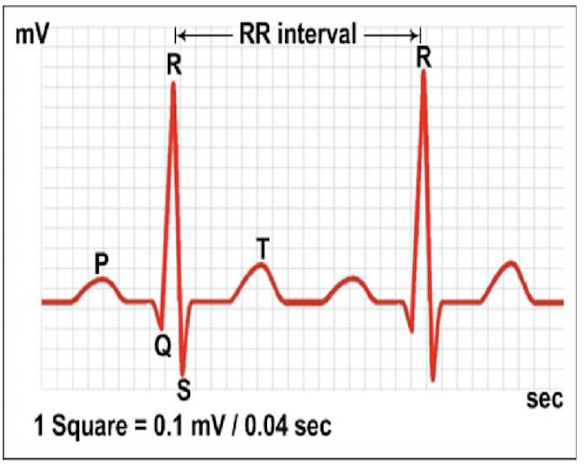
defects in intrinsic conducting system may cause:
arrhythmias, tachycardia, bradycardia, fibrillation
arrhythmias
irregular heart rhythms
tachycardia
abnormally fast heart rate (>100 heart/min)
bradycardia
heart rate slower than 60 beats/min
fibrillation
rapid, irregular contractions, heart becomes useless for pumping blood
one cardiac cycle consists of:
the contraction (systole) and relaxation (diastole) of both atria, rapidly followed by the systole and diastole of both ventricles
cardiac cycle elements:
electrical events, pressure changes, heart sounds, volume changes, mechanical events
picture of electrical events (ECG)
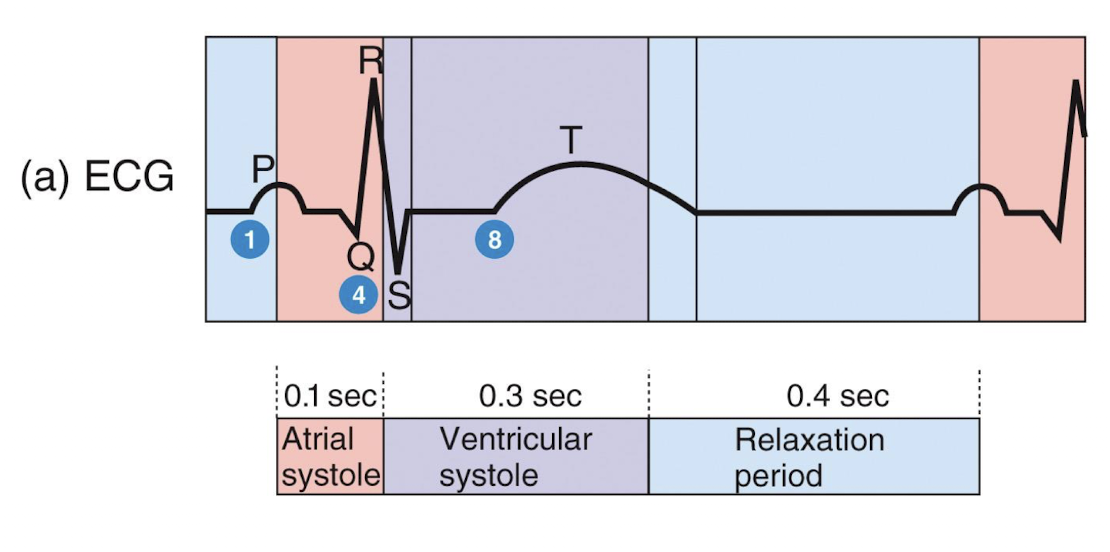
picture of cardiac cycle mechanical events
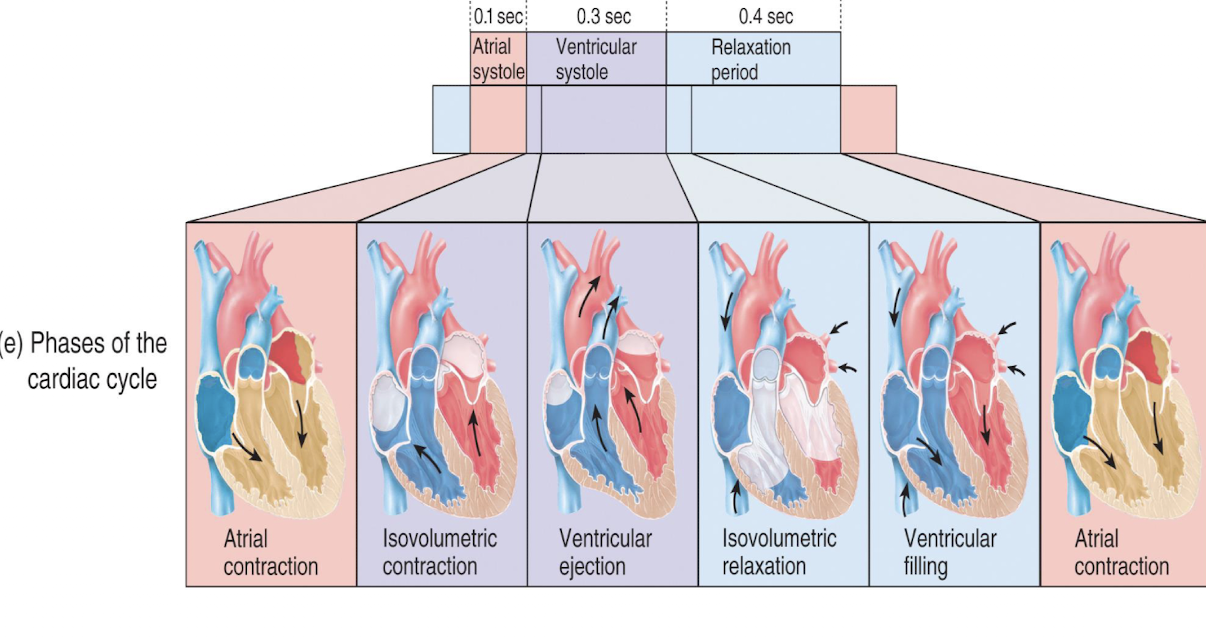
atrial systole
atrial depolarization triggers atrial systole (p wave), atrial contract, pushing remaining 20% of blood into ventricle
isovolumetric contraction
atria relax and ventricles begin to contract, with the rising ventricular pressure causing the AV valves to close; isovolumentric contract phase is split-second period when ventricles close completely, volume remains constant, and ventricles continue to contract; ventricular pressure exceeds pressure in larg arteries, SL valves forced open
ventricular ejection
SL valves open and blood is ejected in arteries
isovolumetric relaxation
early diastole; following ventricular repolarization (t wave), ventricles relax; ventricular pressure drops, causing SL valves to close; ventricles are completely closed chambers (all valves closed); referred to as isovolumetric relaxation phase
atria continue to fill during ventricular systole and when atrial pressure exceeds ventricular pressure:
AV valves will open
ventricular filling
mid-to-late diastole; pressure is low, 80% of blood passively flows from atria through open AV valves into ventricles
picture of heart sounds
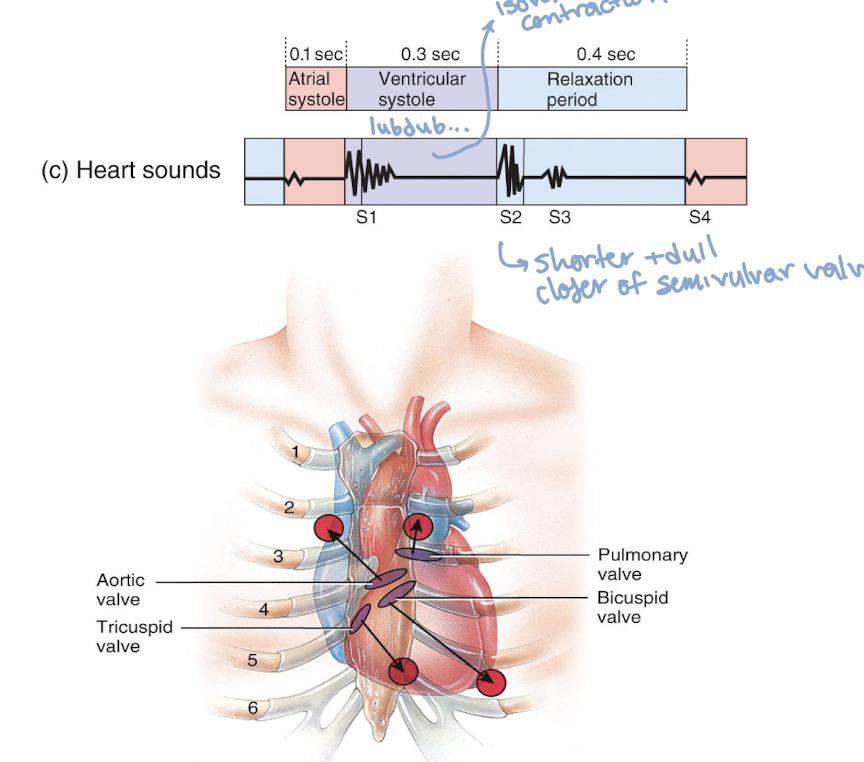
two sounds (lub-dup)
associated with closing of heart valves; first sound is closing of AV valves at start of ventricular sound, with the second sound being the closing of SL valves at beginning of ventricular diastole
heart murmurs
abnormal heart sounds heard when blood hits obstructions
picture of volume changes
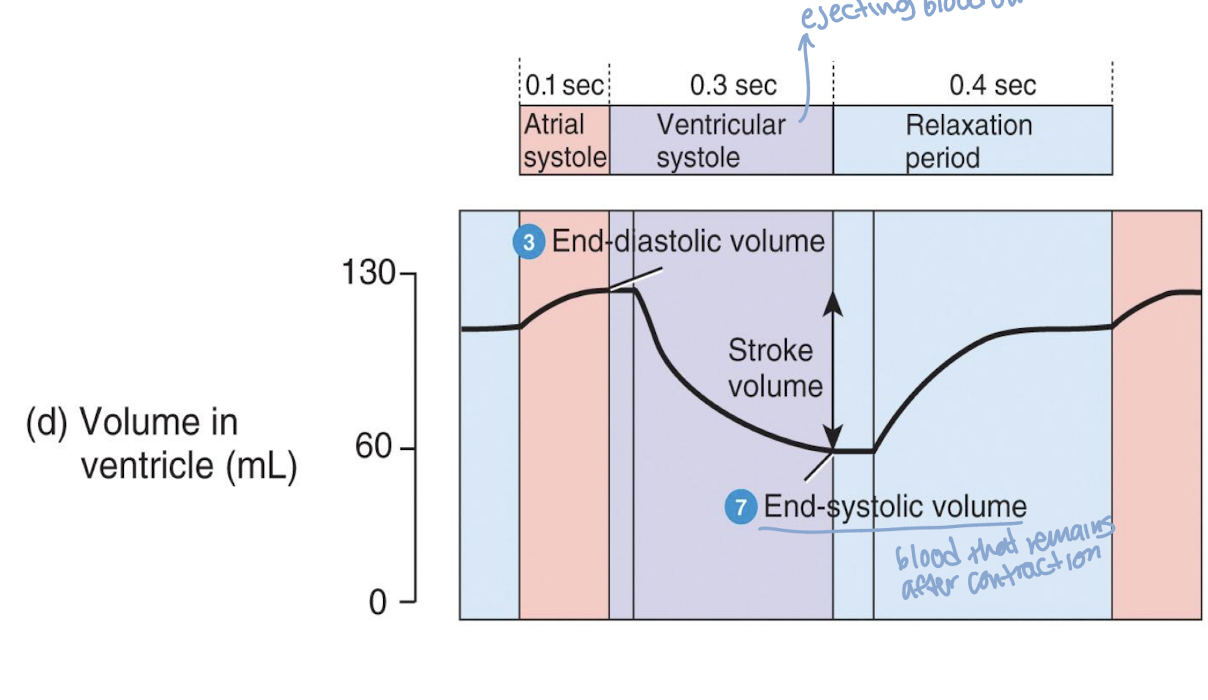
end diastolic volume (EDV)
volume of blood in each ventricle at end of ventricular diastole
end systolic volume (ESV)
volume of blood remaining in each ventricle after systole
stroke volume (SV)
amount of blood pumped out of ventricle in one beat/contraction
mathematical way to interpret volume changes:
SV = EDV - ESV
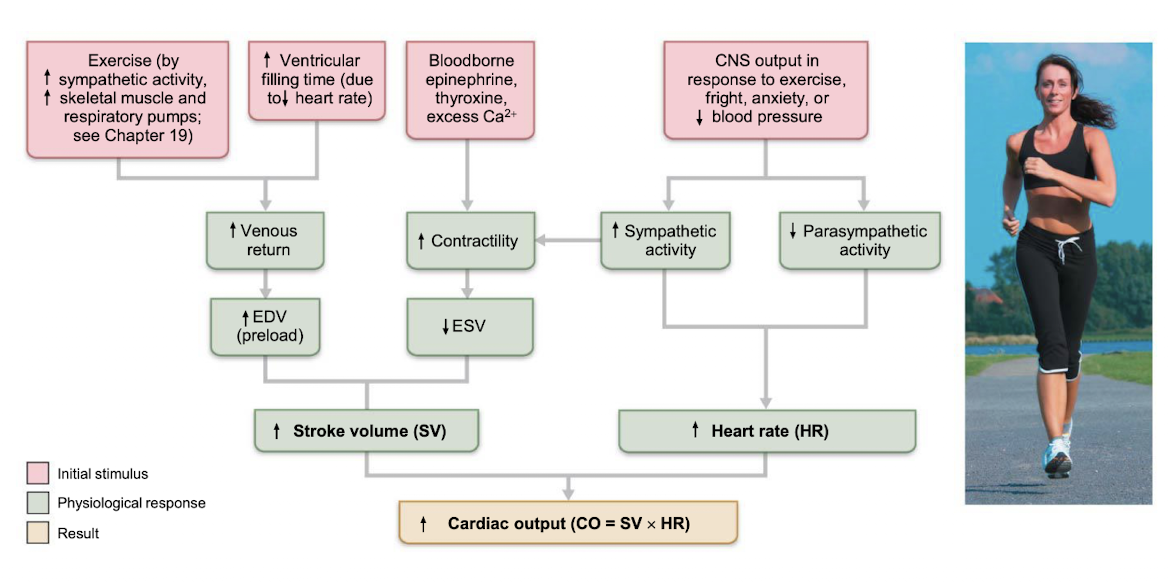
cardiac output
volume of blood ejected from left or right ventricle into the aorta or pulmonary trunk each minute
CO output calculation
CO (mL/min) = SV (mL/beat) x (beat/min)
ejection fraction
a measurement (%) of the percentage of blood leaving your heart each time it contracts
an LV ejection fraction of 55% or higher is considered ______. 55% or lower is considered ______.
higher, reduced
three factors regulate stroke volume:
preload, contractility, afterload
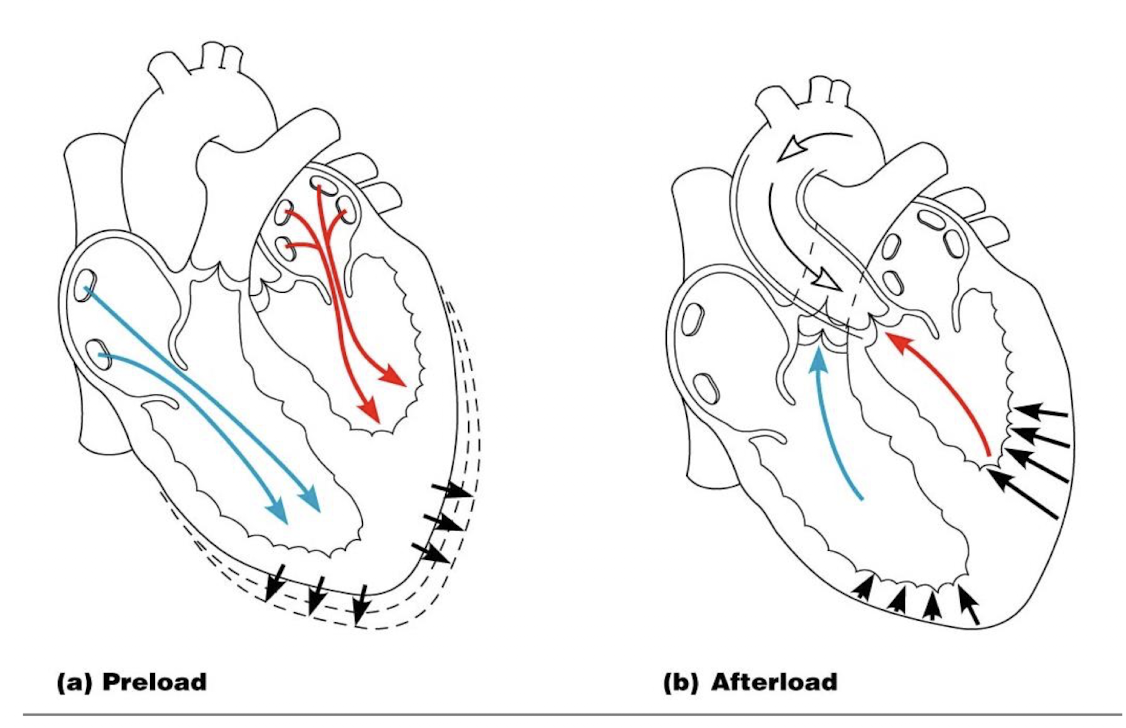
preload
degree to which cardiac muscle cells are stretched just before they contract; as stretch of ventricular wall (preload) increase, so does stroke volume; most important factor in preload stretching of cardiac muscle is venous return, amount of blood returning to heart
contractility
contractile strength at given muscle length
afterload
pressure that ventricles must overcome to eject blood; back pressure from arterial blood pushing on SL valves is major pressure, determined. by peripheral vascular resistance, increased afterload decreases SV
picture of preload and afterload
The ________ is the amount of blood in a ventricle at the beginning of systole.
end diastolic volume
The ________ is the amount of blood in a ventricle after it has contracted and before it begins to refill
end systolic volume
The amount of blood returning to the heart is the ________.
venous return
The amount of blood pumped out of the heart during one contraction is the ___________.
stroke volume
picture of regulation of cardiac output