1- Oral Manifestations of Dermatologic Disease (Dr. Lerman)
1/126
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
127 Terms
desquamative gingivitis
What is a clinical term to describe a manifestation of what is usually lichen planus, a hypersensitivity reaction, or mucous membrane pemphigoid?
NO (not a plaque induced gingivitis)
Is desquamative gingivitis a diagnosis?
desquamative gingivitis
What is gingiva that demonstrates superficial peeling of epithelium characterized by the formation + rupture of mucosal vesicles?
desquamative gingivitis
This is the clinical manifestation of which condition?
- Female predilection
- Diffuse, markedly erythematous gingiva
- Generally involves attached tissues
- Sensitivity to spicy foods
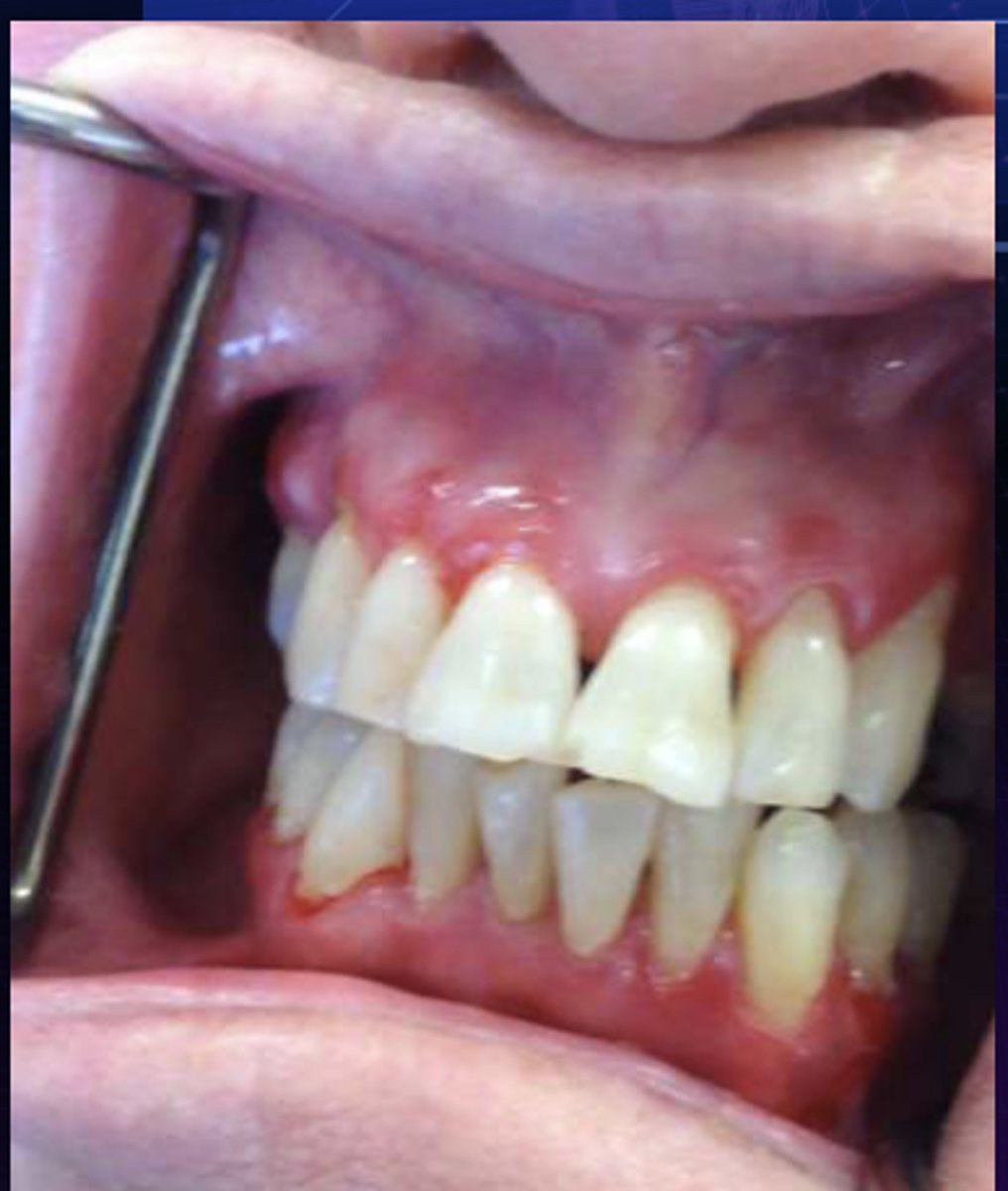
nikolsky sign: pressure to affected area with an object/compressed air → new vesicle formation or sloughing
What is a way to clinically diagnose desquamative gingivitis?
desquamative gingivitis
What condition?
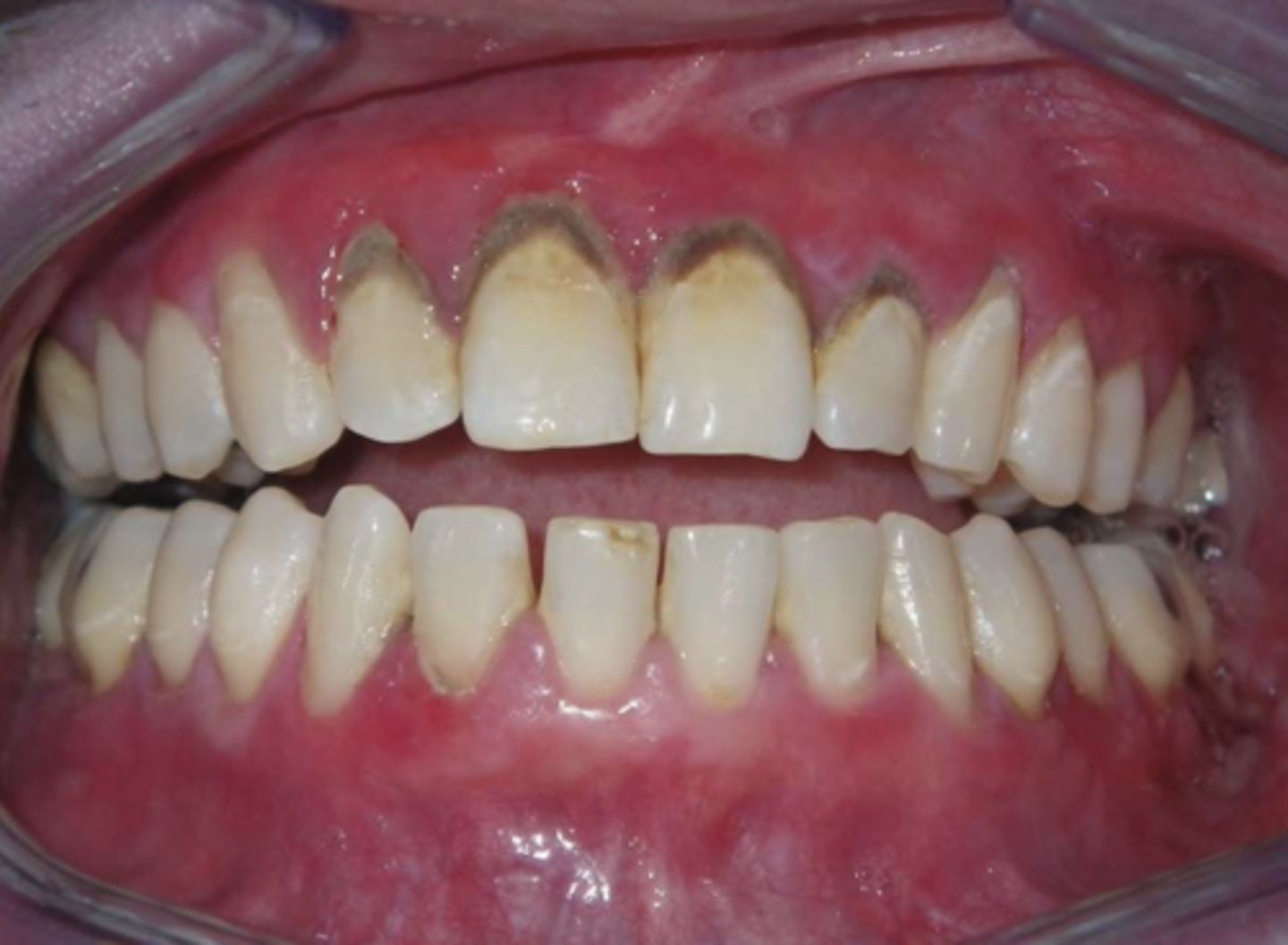
desquamative gingivitis
What condition?
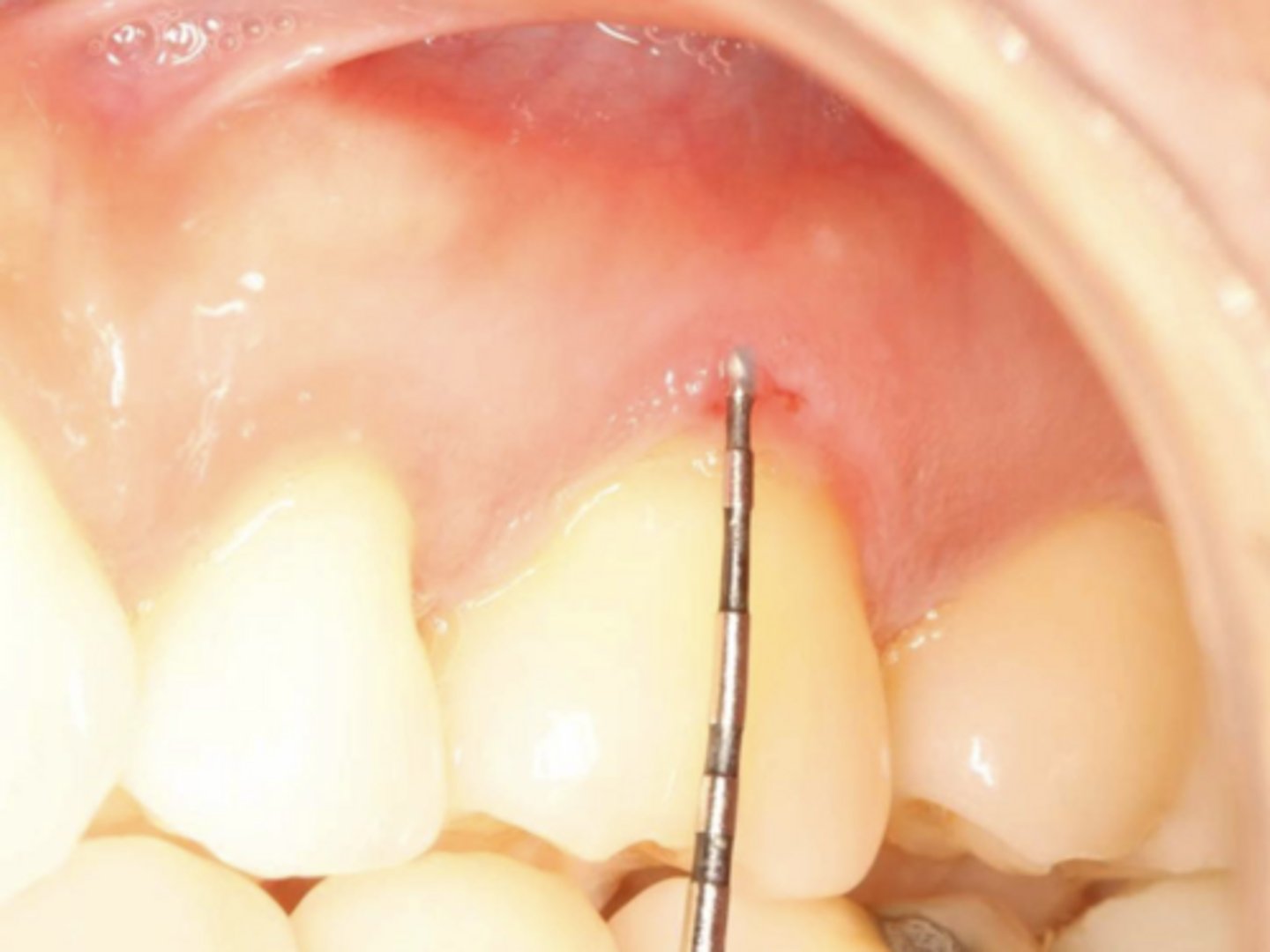
- Idiopathic lichen planus
- Lichenoid drug eruptions
- Lupus erythematosus
- Graft versus host disease
4 types of Lichenoid Diseases
- Idiopathic lichen planus
- Lichenoid drug eruptions
- Lupus erythematosus
- Graft versus host disease
- Oral manifestations of hepatitis C
- Lichen planus pemphigoides
- Chronic ulcerative stomatitis
what are the 7 lichenoid processes
lichen planus
These are clinical features of what condition?
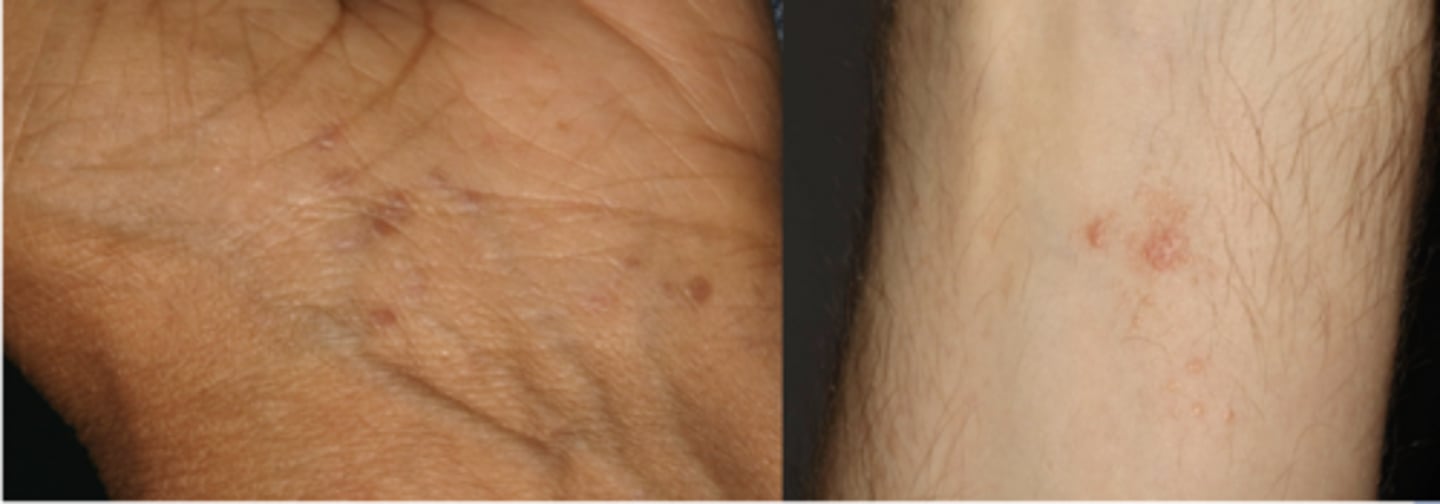
Skin lesions
- 1% of population
- Purple, polygonal, pruritic papules
- Flexor surfaces of extremities
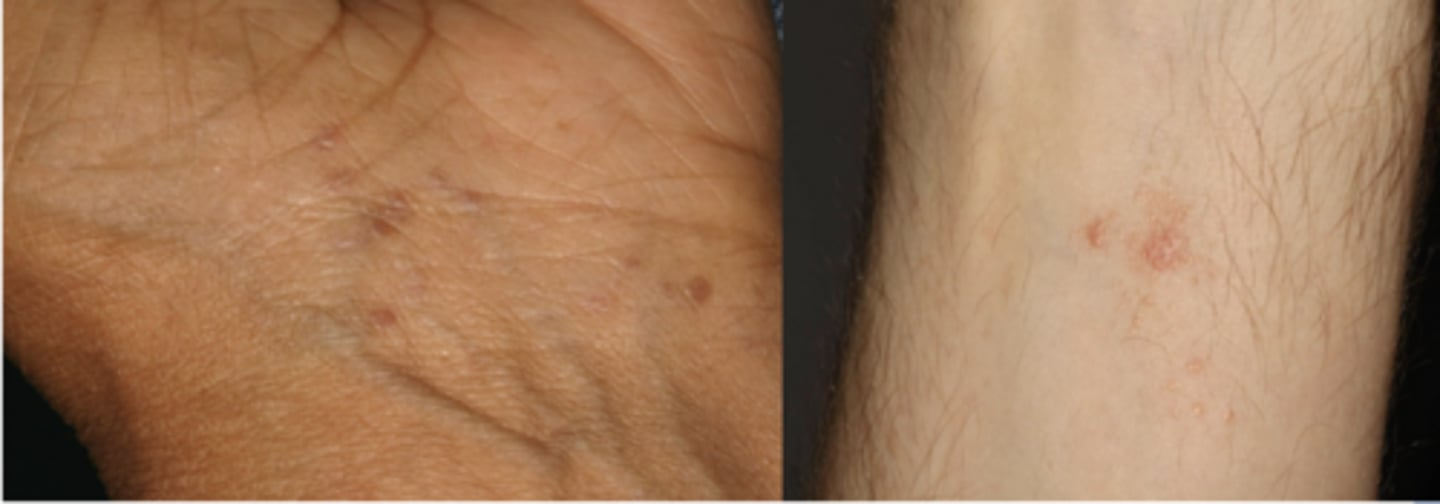
lichen planus
What condition?
Reticular
Erosive/erythematous
Ulcerative
R E U
What are the 3 oral variants of lichen planus?
reticular
What oral variant of lichen planus is most common?
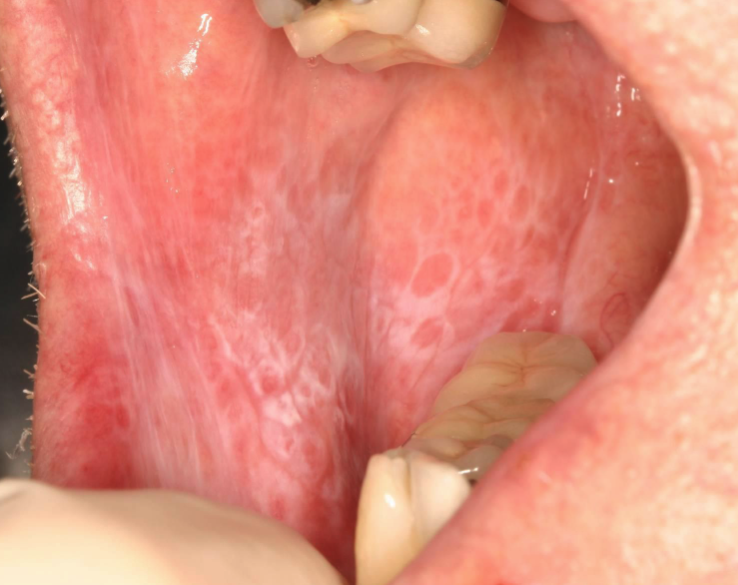
lichen planus (reticular)
What condition?
- Often asymptomatic
- Posterior buccal mucosa (bilaterally)
- Lacy white striations (Wickham striae)
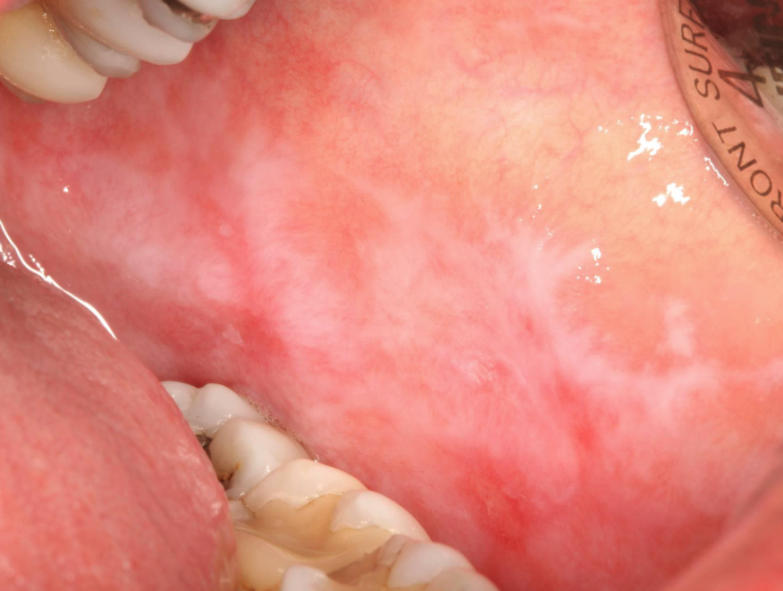
lichen planus (reticular)
Wickham striae (lacy white striations) is a classic feature of what condition?
lichen planus (reticular)
What condition?
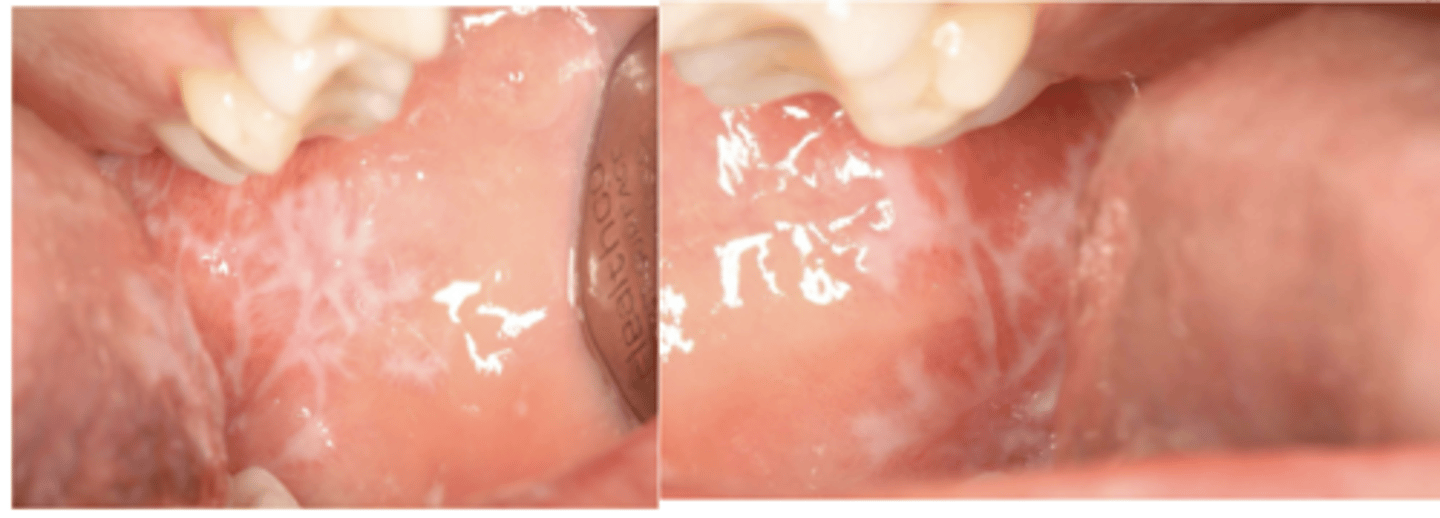
lichen planus (reticular)
What condition?
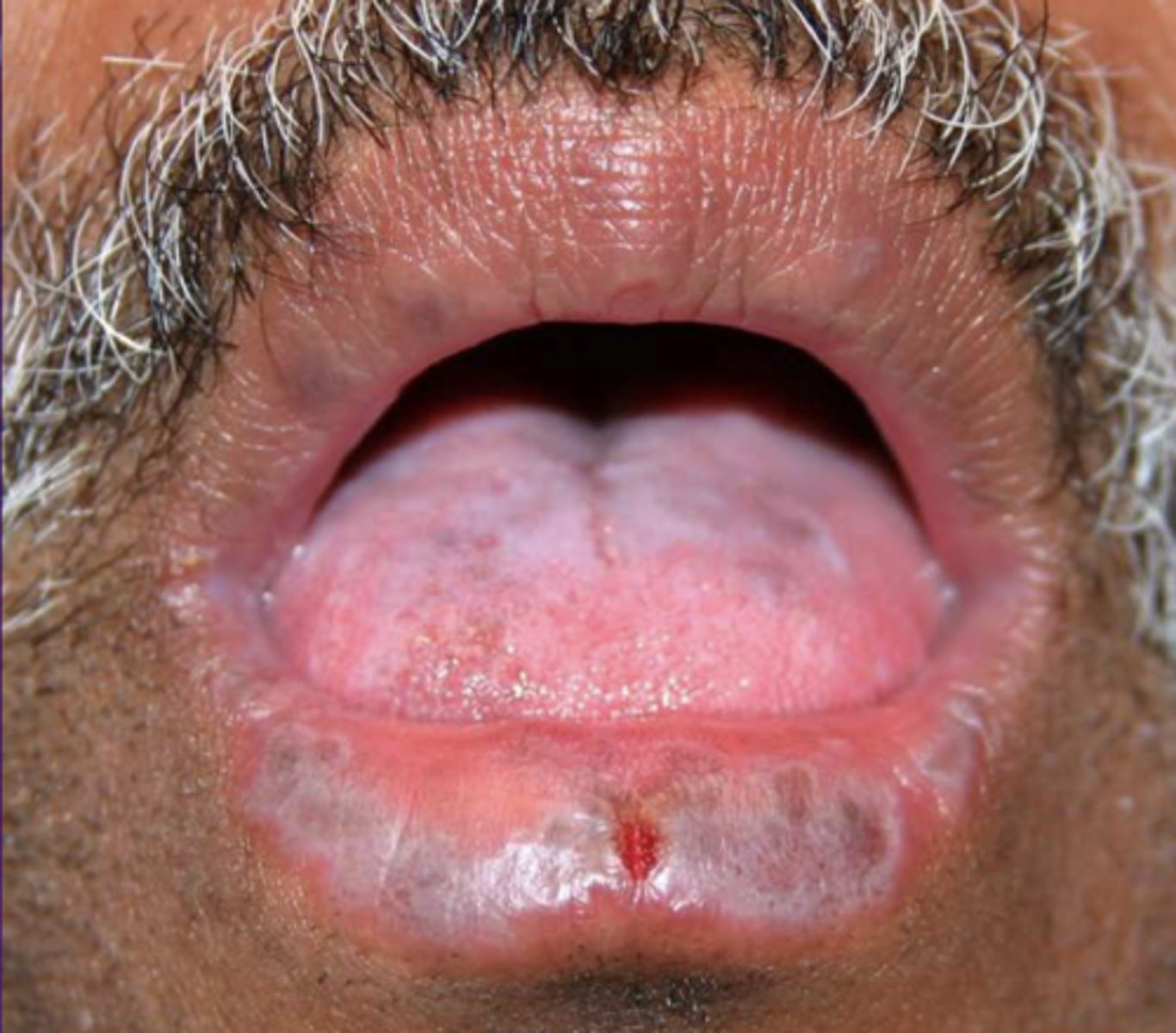
lichen planus (reticular)
What condition?
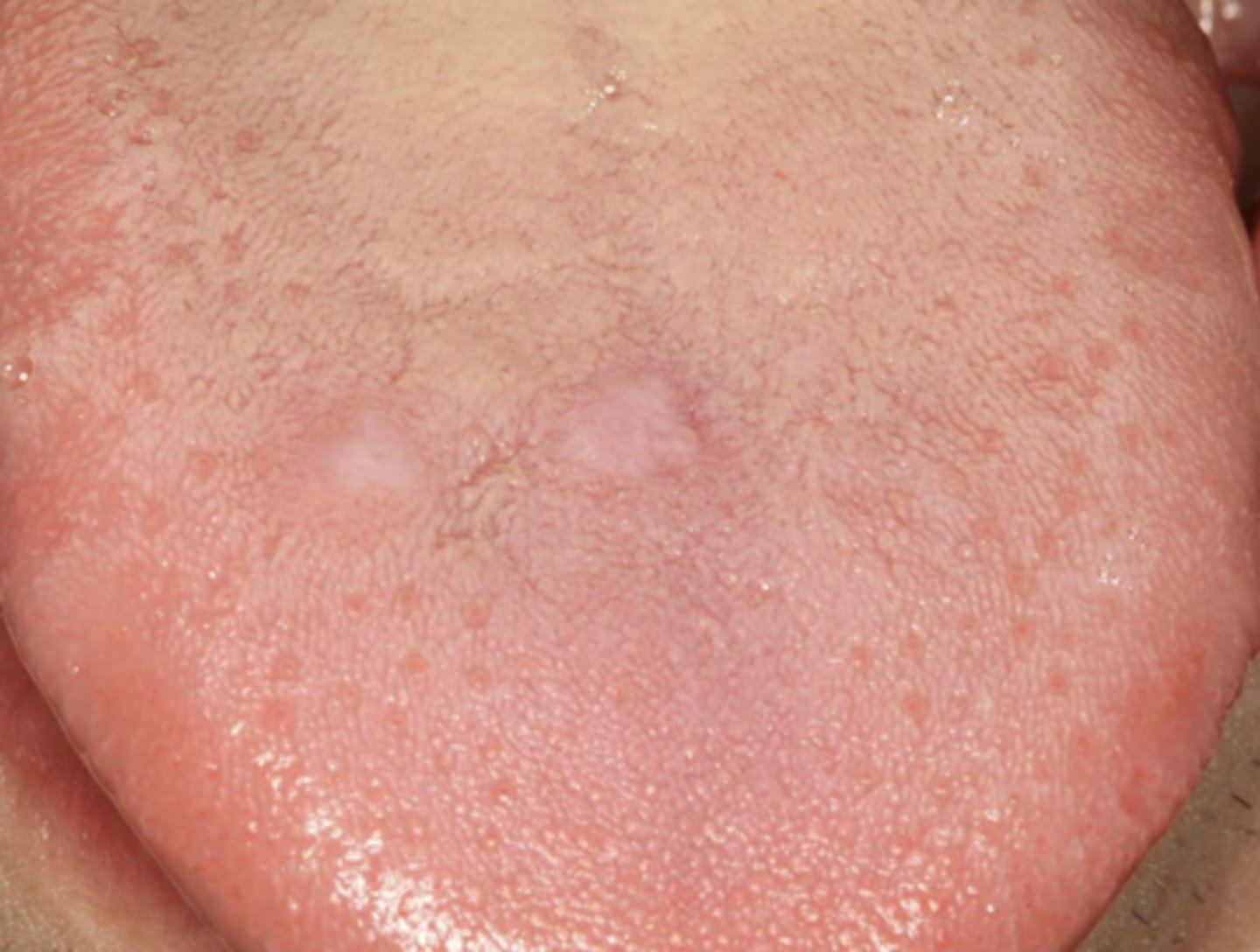
lichen planus (erosive/erythematous)
What type of lichen planus?
- Often symptomatic
- Striae at periphery of erythema
- May cause desquamative gingivitis
- Must be distinguished from mucous membrane pemphigoid or pemphigus
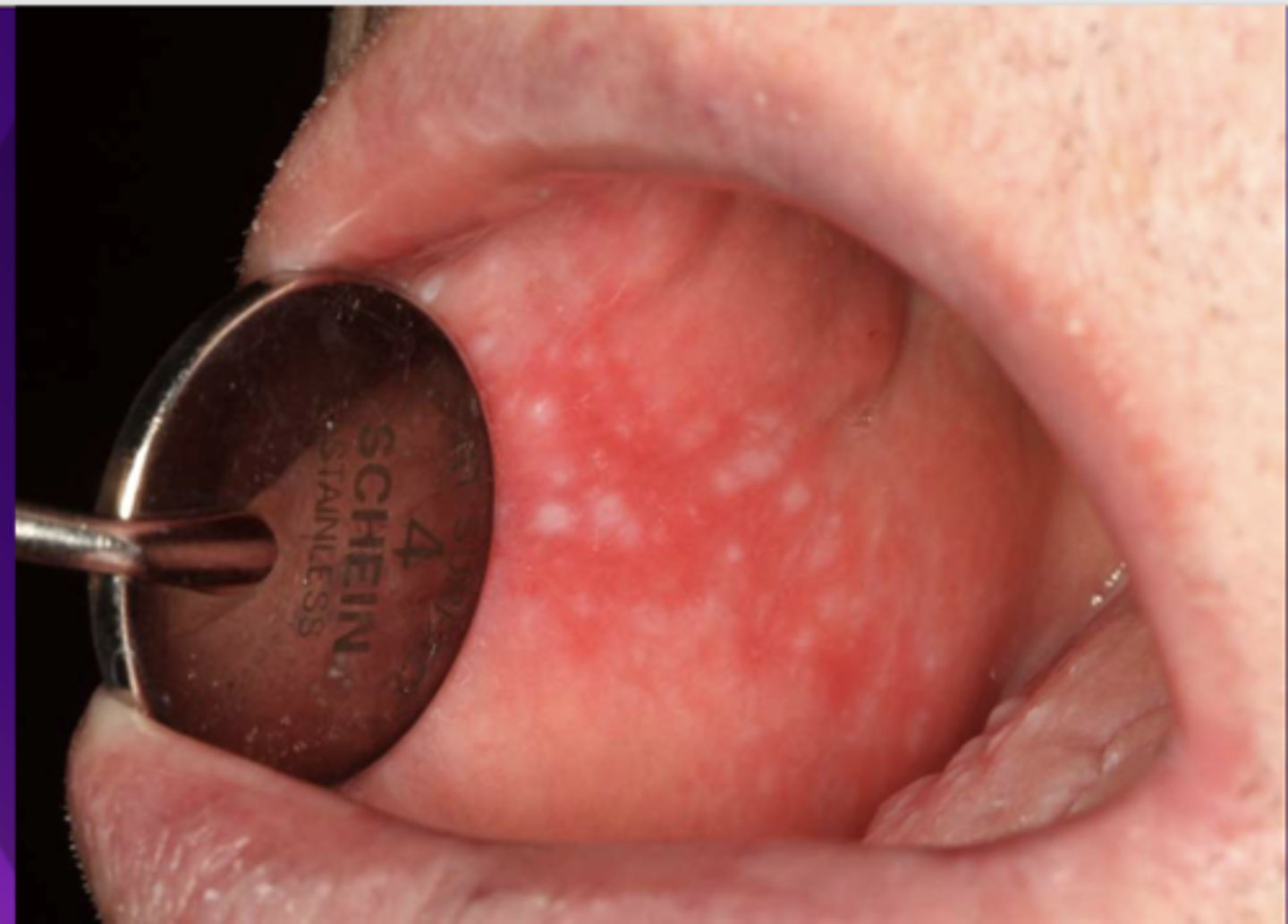
lichen planus (erosive/erythematous)
What condition?
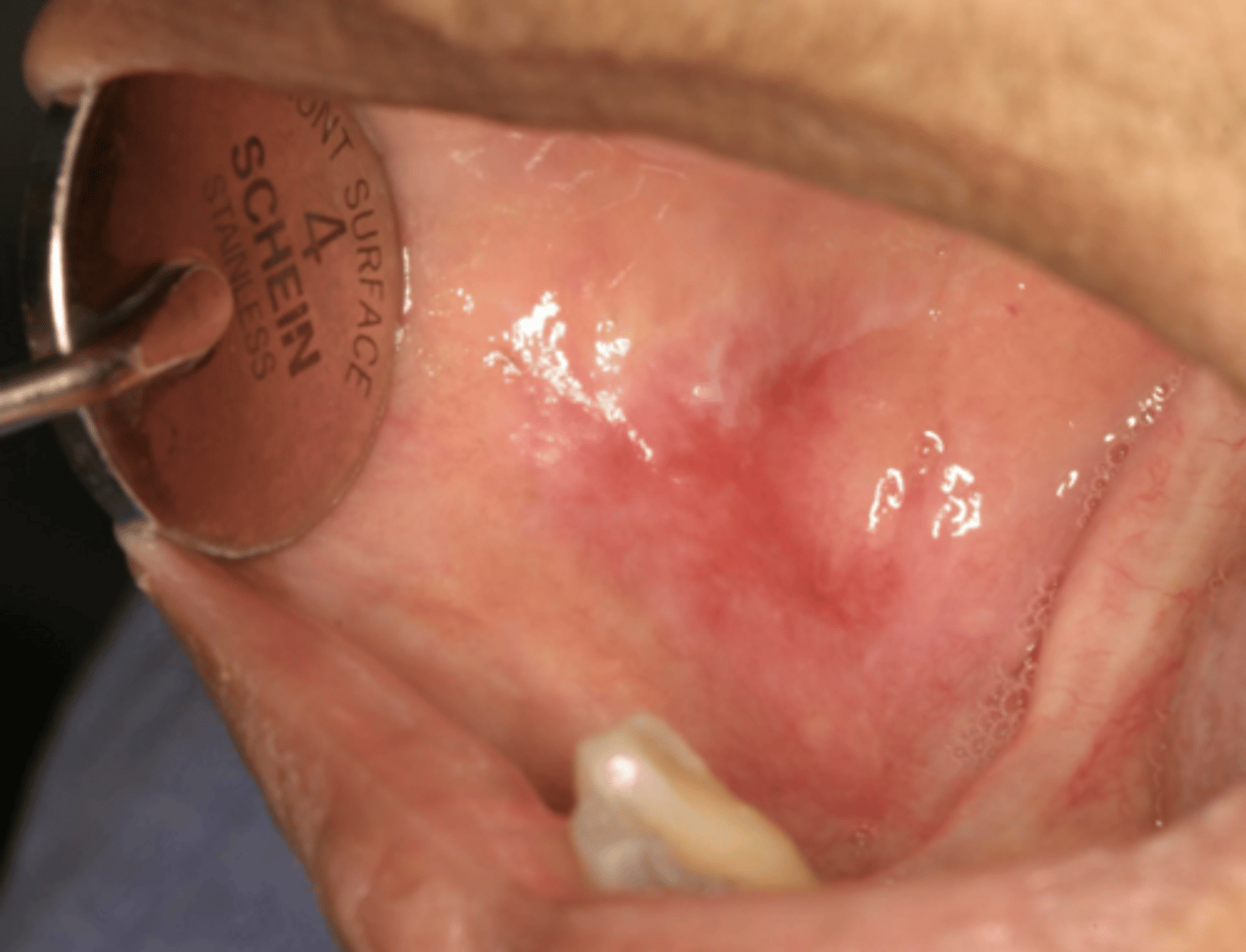
lichen planus (erosive/erythematous)
What condition?
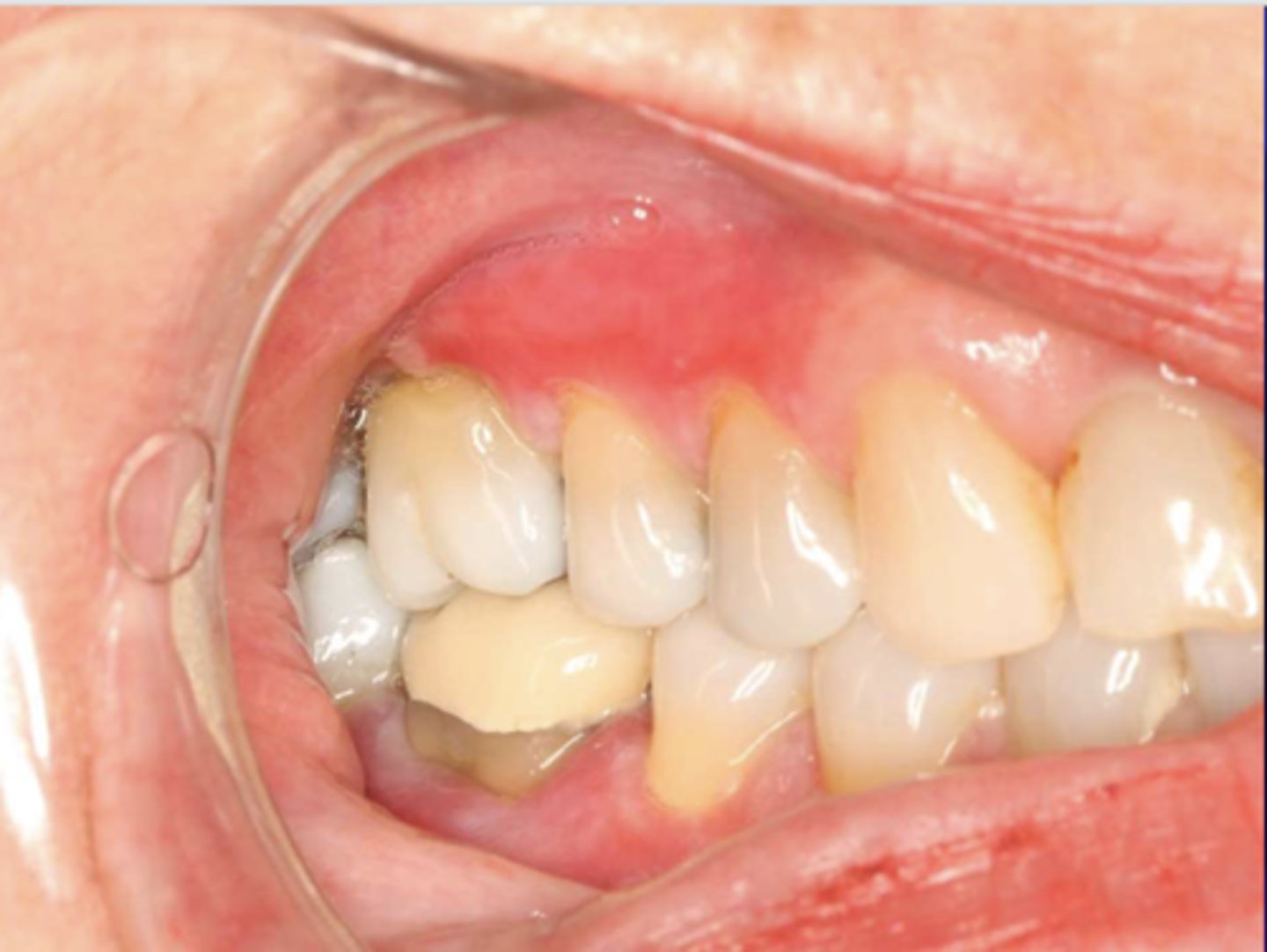
lichen planus (erosive/erythematous)
What condition?
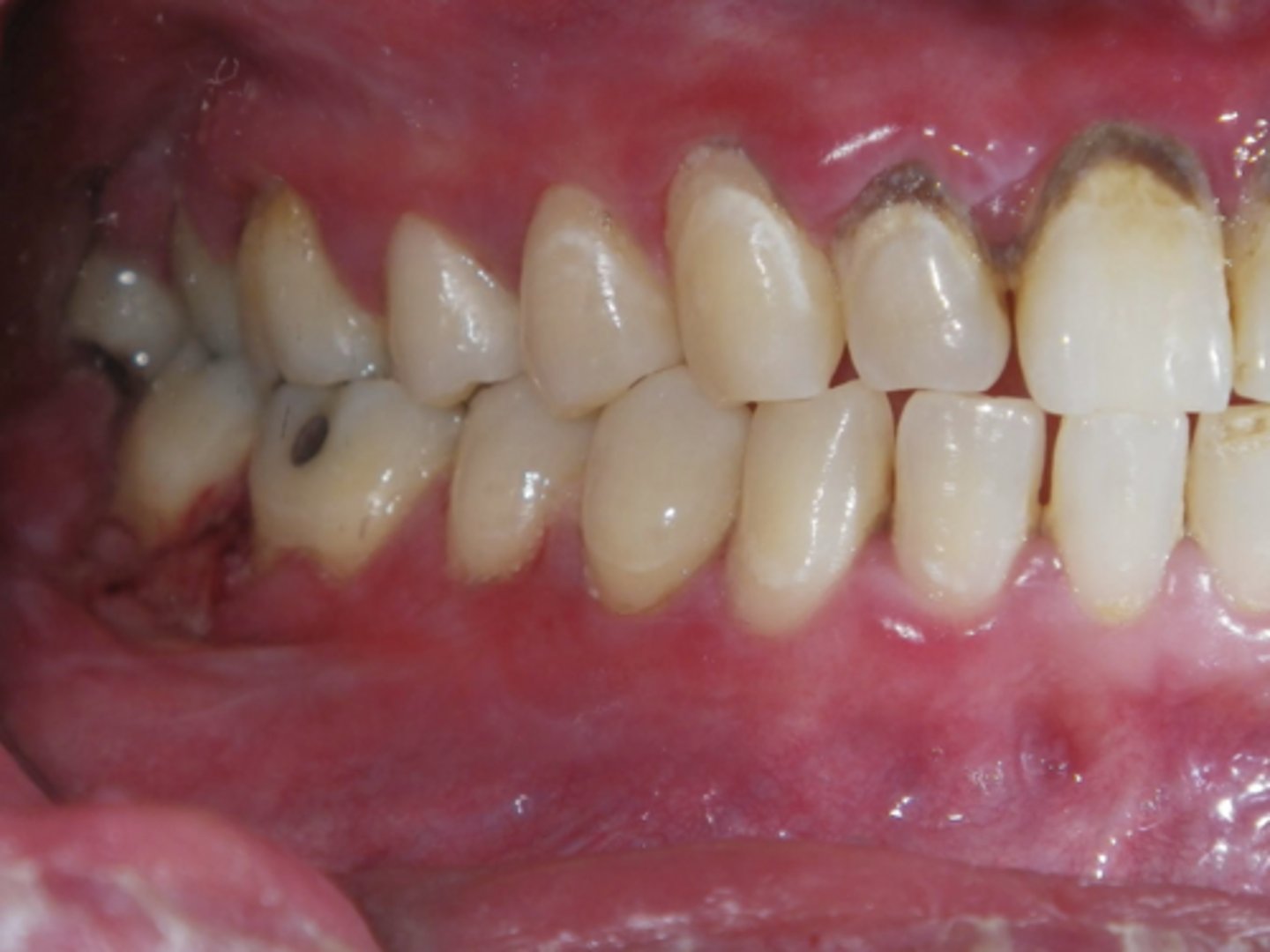
lichen planus (ulcerative)
What type of lichen planus?
- Least common form
- Usually symptomatic
- Ulcers w/ striae + erythema
- May cause desquamative gingivitis
- Must be distinguished from mucous membrane pemphigoid or pemphigus
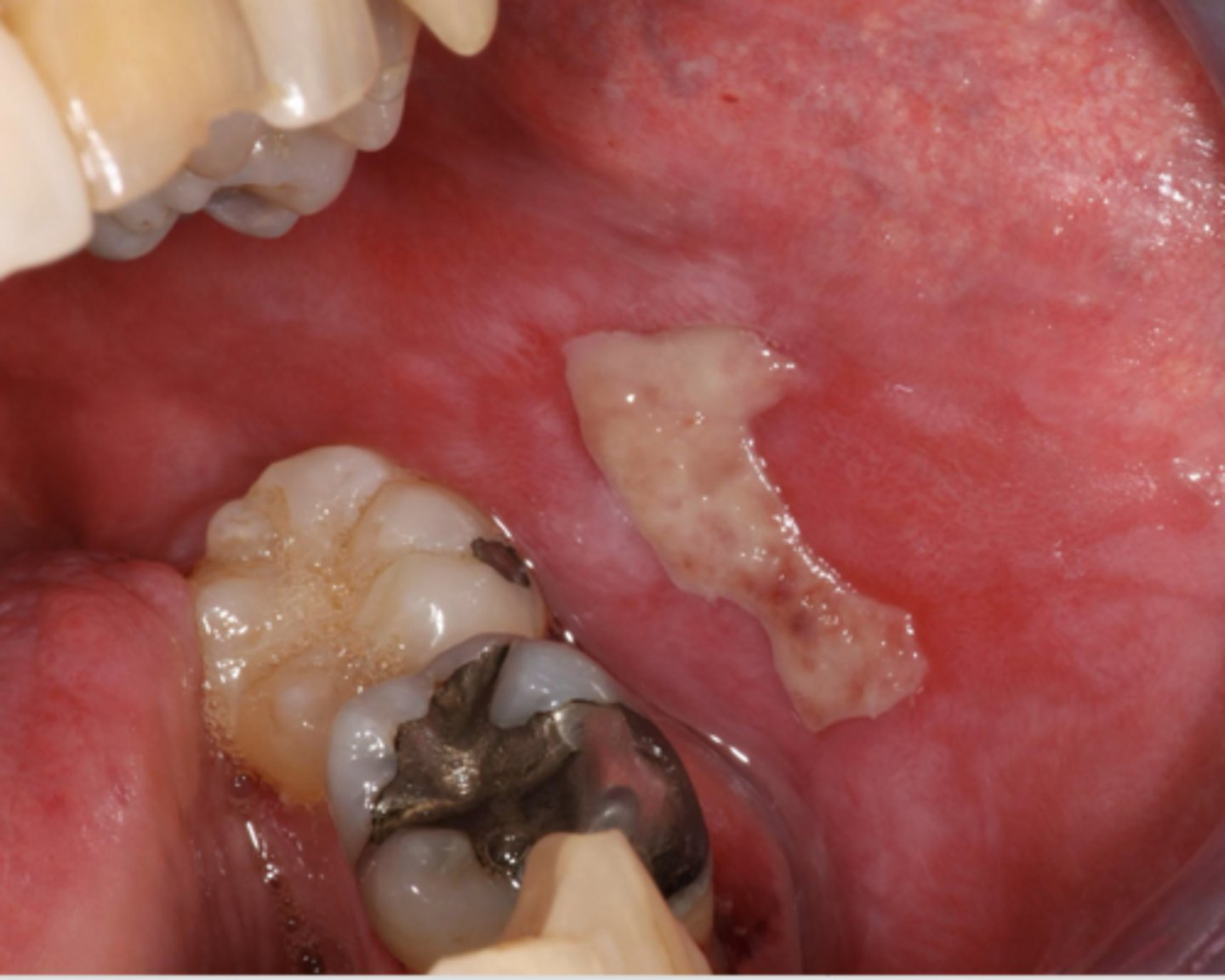
lichen planus (ulcerative and some reticular and erythematous seen)
What condition?
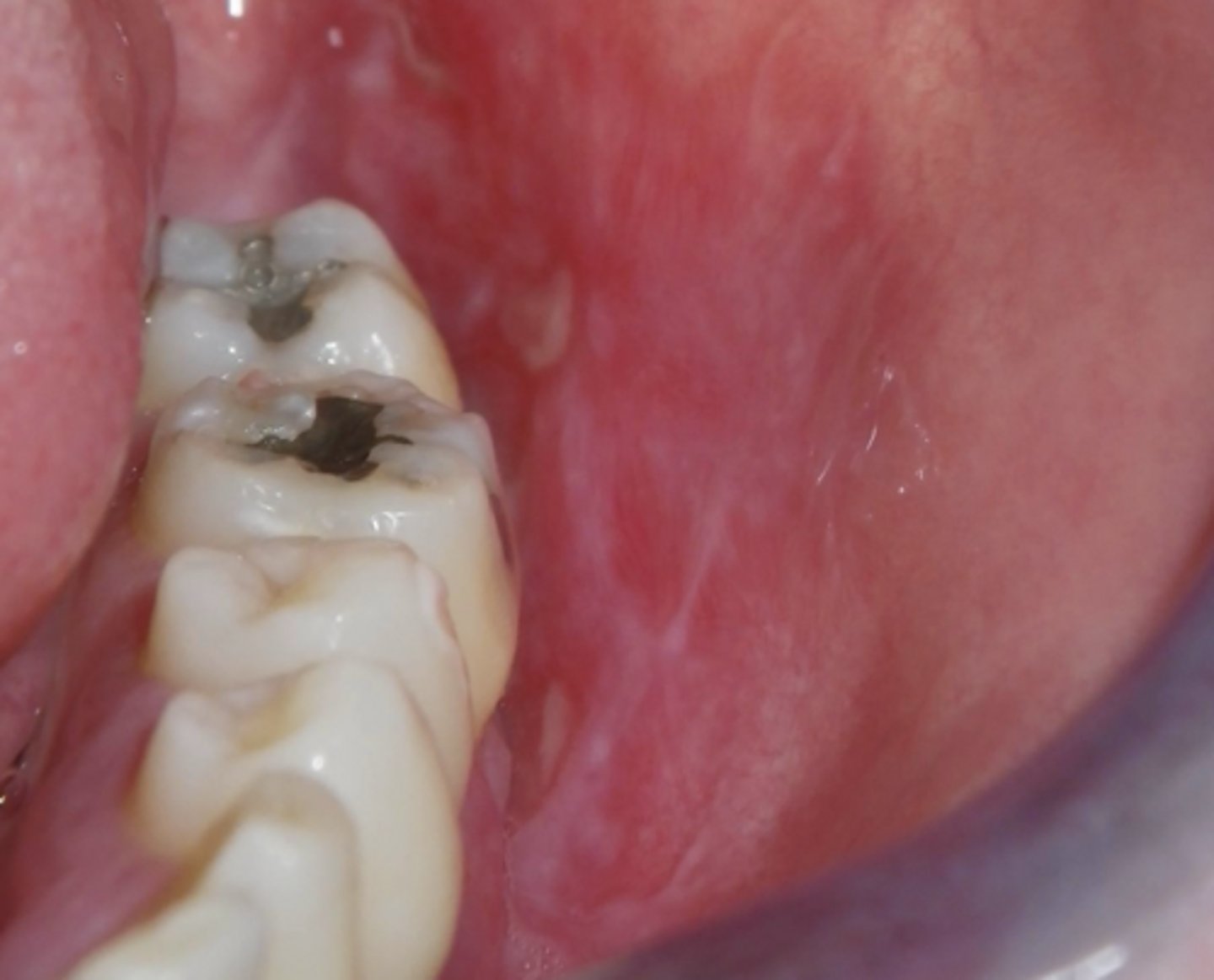
- NSAIDs
- Anti-hypertensive agents
- Anti-hyperglycemic agents
- Cholesterol lowering agents
- Anti-hypothyroidism agents
- Anti-gout medications
- Amalgam restorations
- Cinnamon flavoring agents
- Herbal remedies
Lichen planus is associated with which 9 medications
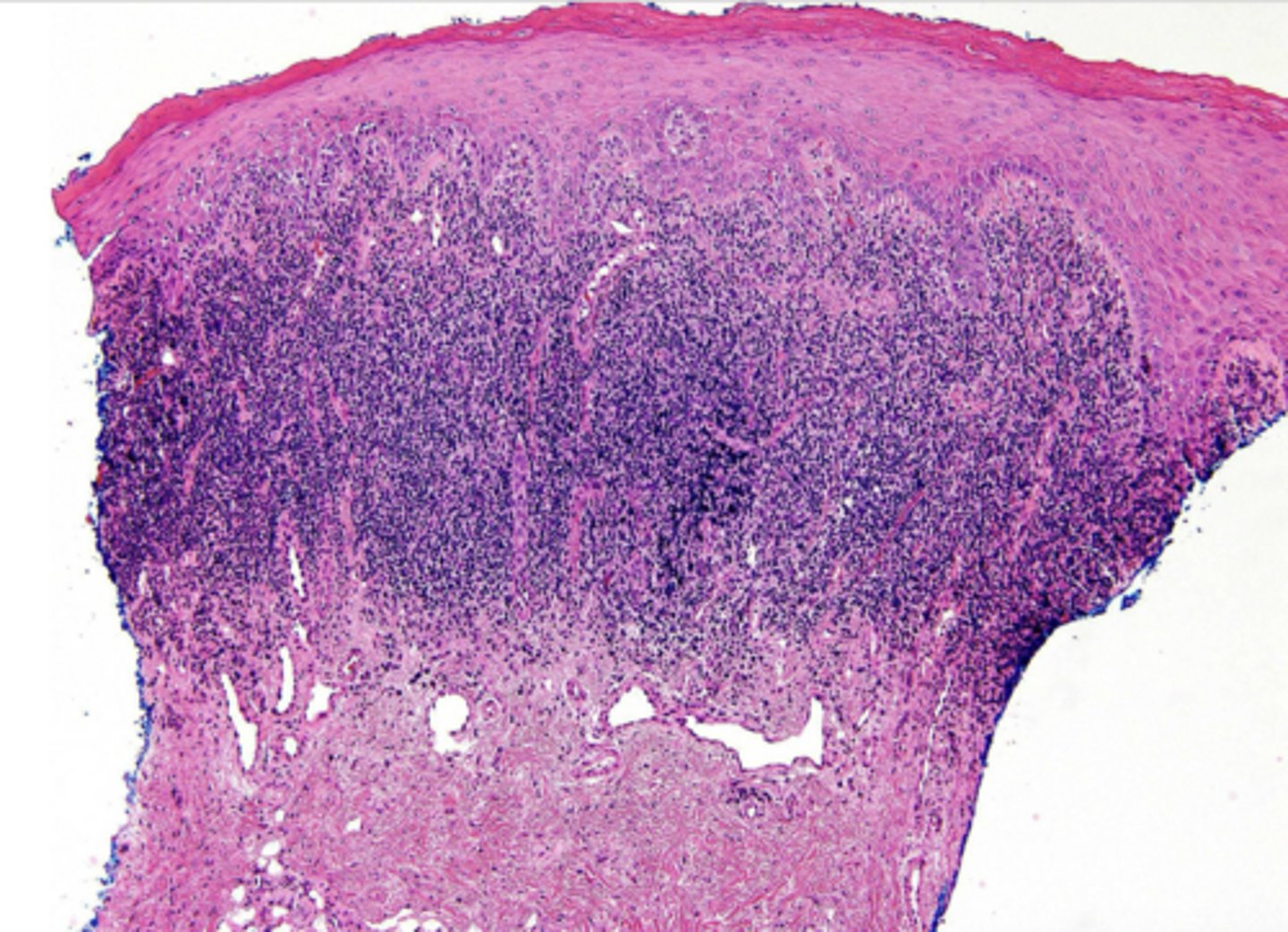
- Orthokeratosis or parakeratosis
- Colloid bodies
- Saw tooth rete ridges
- Band-like infiltrate of lymphocytes
5 histopath features of lichen planus
basal
What cell layer of the epithelium undergoes degeneration with lichen planus?
- Observation if asymptomatic
- Topical corticosteroids
What is the typical treatment for lichen planus?
Lichen planus
What condition?
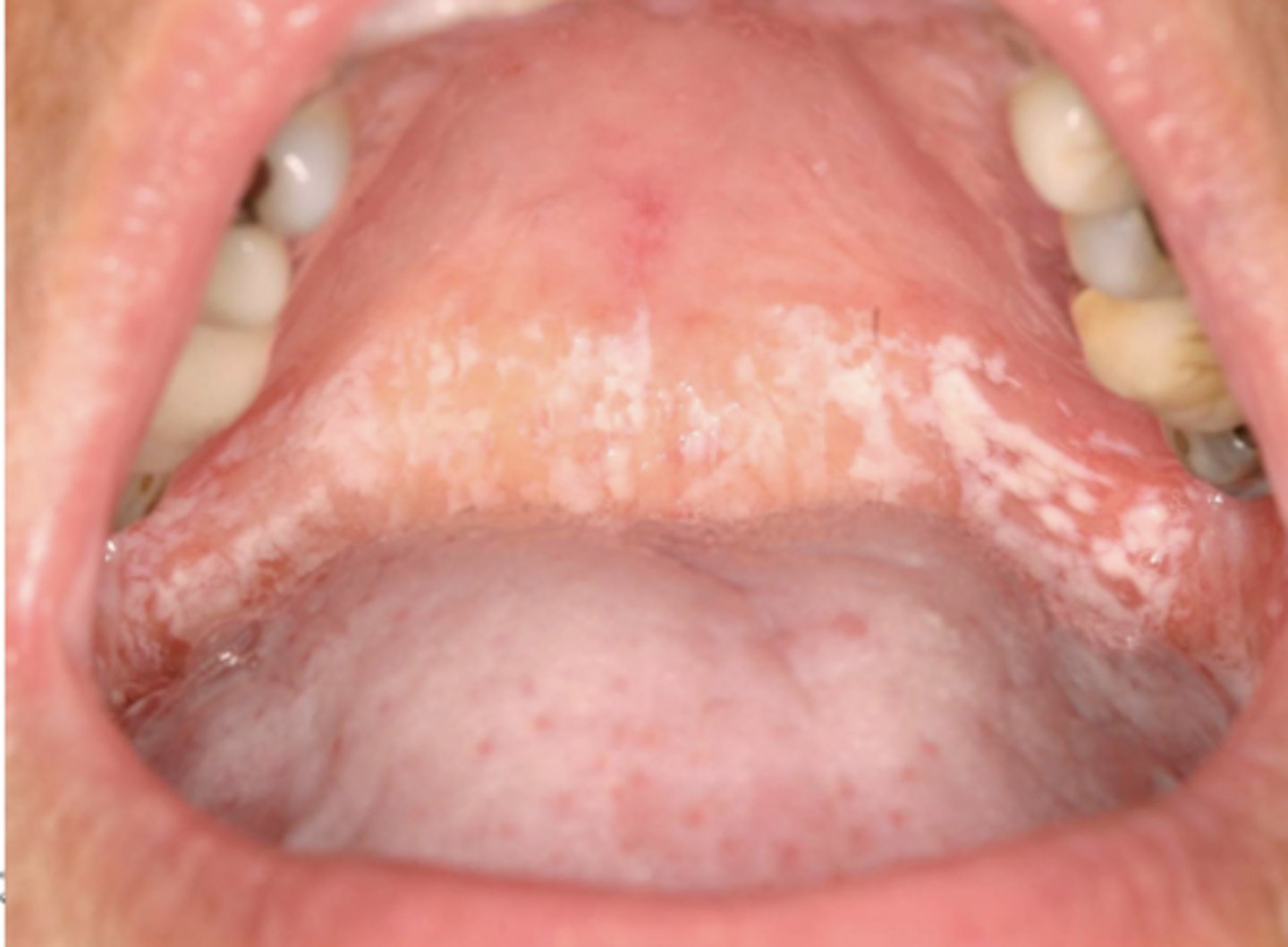
- Fluocinonide or clobetasol gel 0.05% (warn pt regarding label)
- Dexamethasone mouthrinse 0.5mg/5ml
which 2 topical corticosteroids are prescribed for lichen planus
squamous cell carcinoma (life-long follow-up recommended)
Lichen planus has a 0.9% increased risk of developing what
systemic lupus erythematosus (SLE)
What condition?
- Multi-system disease with skin + oral lesions
- 8-10:1 female predilection
- Average age at diagnosis = 31 years
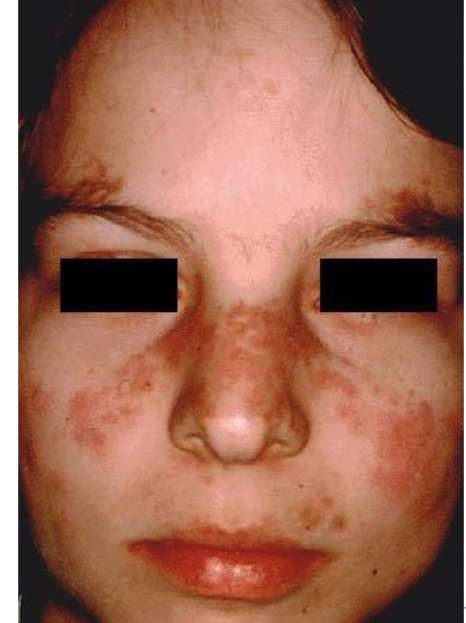
- Early stages non-specific
- Fever, weight loss, arthritis, fatigue, malaise
- 40-50% butterfly rash over malar area and nose
- Kidney involvement in 40-50%
- Cardiac involvement
5 clinical features of systemic lupus erythematosus (SLE)
systemic lupus erythematosus (SLE)
These are clinical features of what condition?
- Oral lesions in 5-40% pts
- - Lichenoid lesions of palate, buccal mucosa, or gingiva
- - May involve vermilion (lupus cheilitis)
- - Ulceration, pain, erythema, hyperkeratosis seen in varying degrees
SLE
Patient presents with an ulcer on the buccal mucosa and along with fever, butterfly malar rash and reports weight loss and fatigue. What condition?
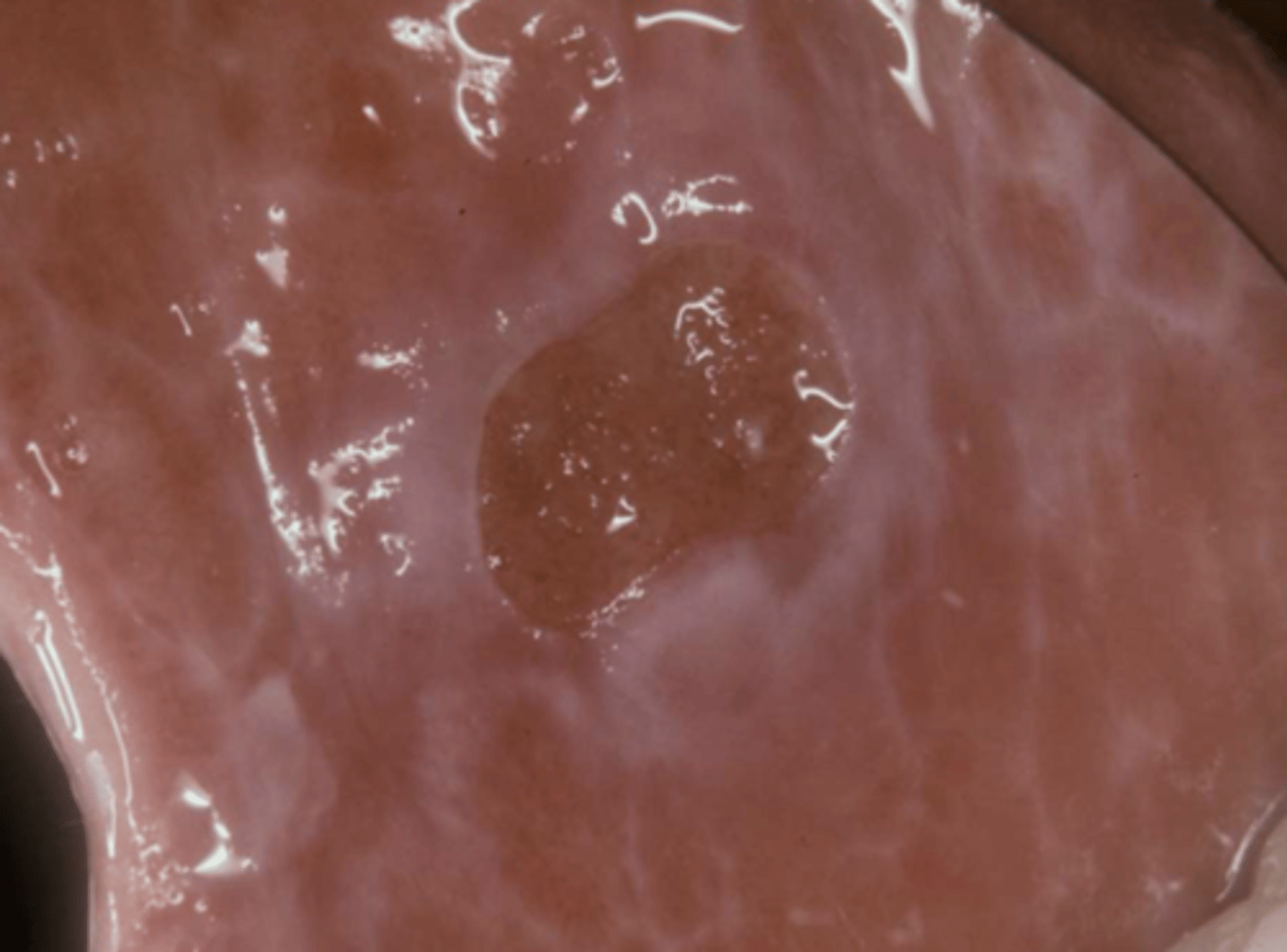
systemic lupus erythematosus (SLE)
Patient also presents with kidney disease. What condition do you suspect?
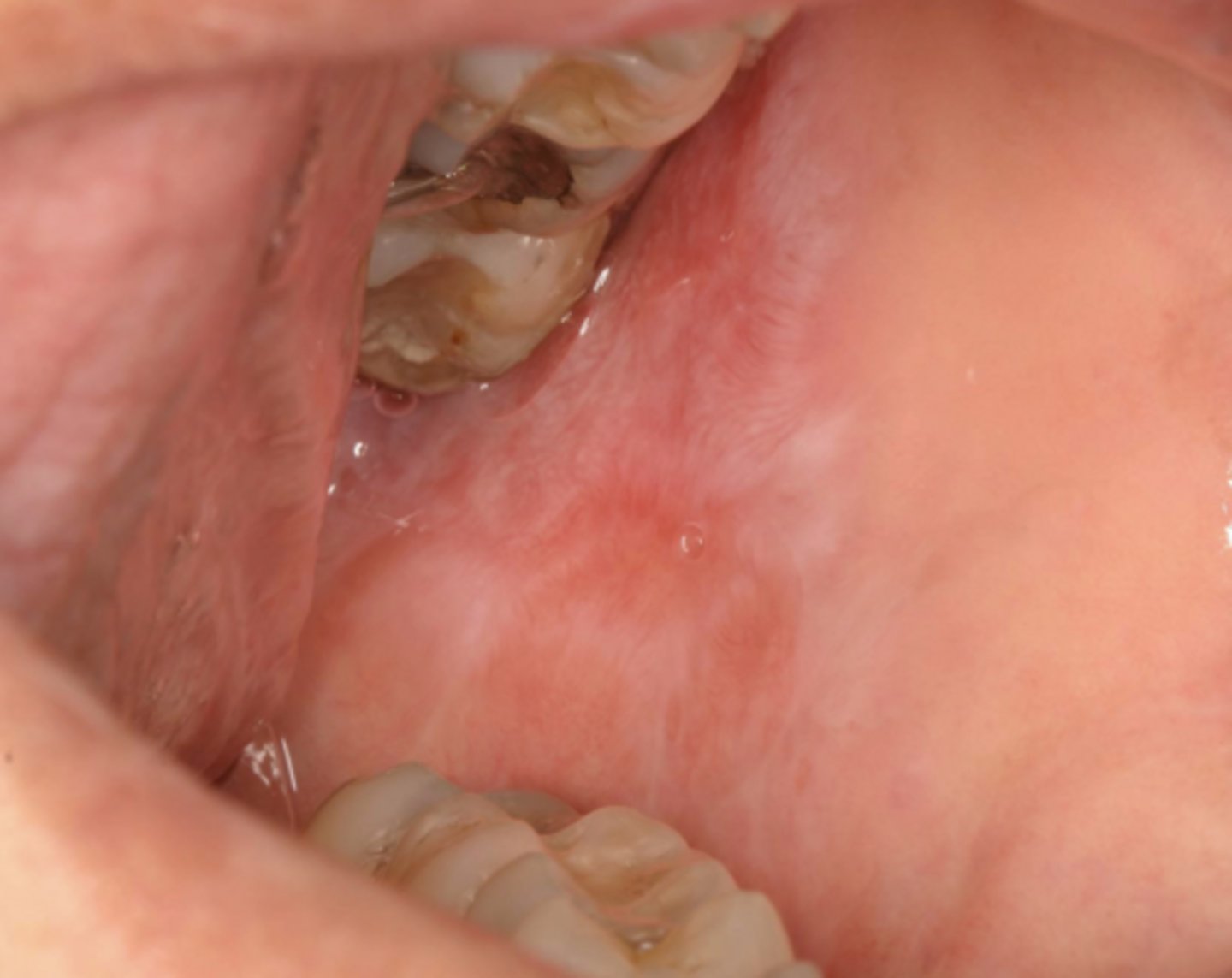
systemic lupus erythematosus (SLE)
Patient also presents with a butterfly malar rash. What condition do you suspect?
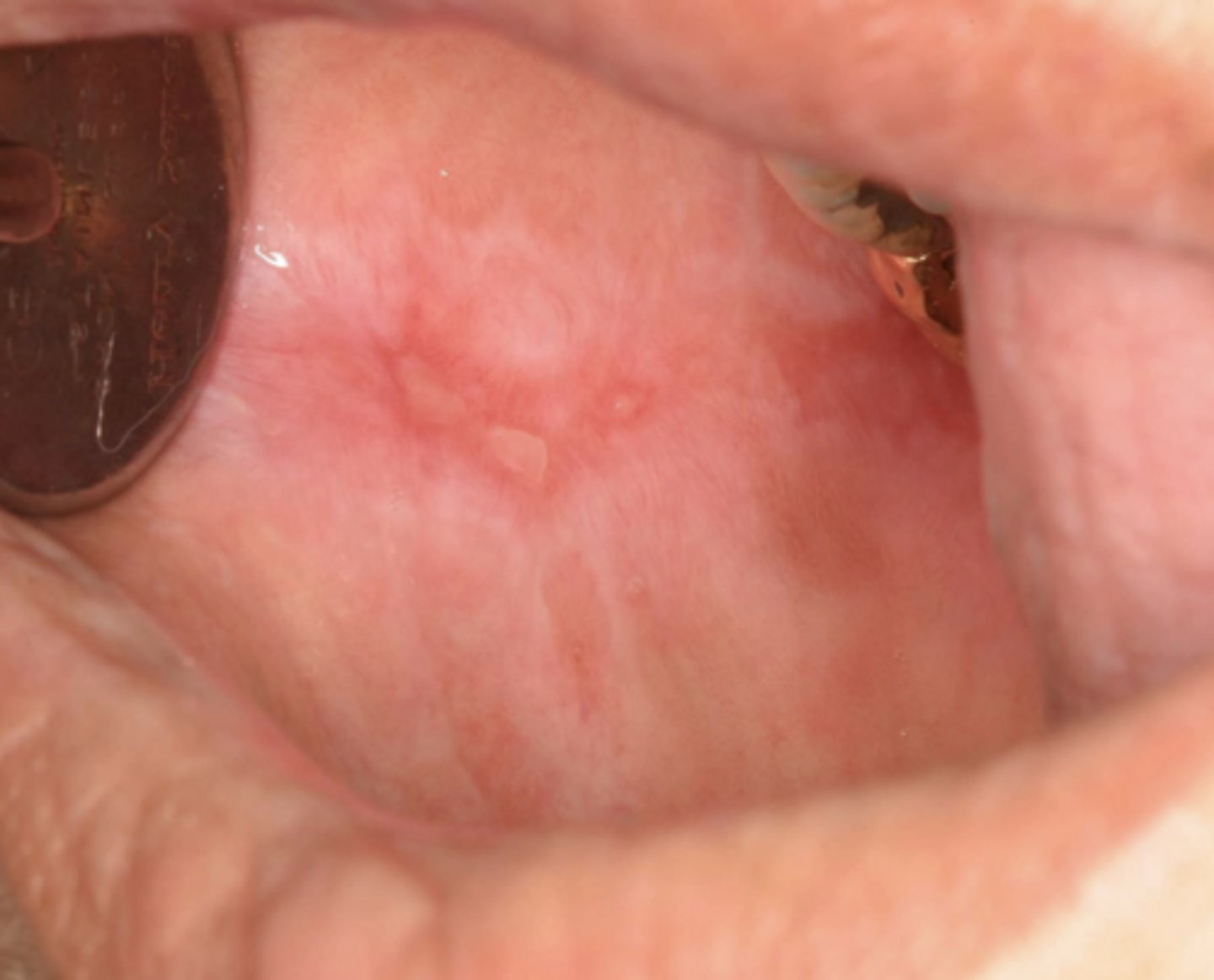
discoid lupus
Chronic Cutaneous Lupus Erythematosus (CCLE) is also known as what?
sun exposure
CCLE presents with skin and oral lesions but has no systemic signs/symptoms. What is it exacerbated by?
Atrophy with scarring
Healing of Chronic Cutaneous Lupus Erythematosus (CCLE) results in what?
Chronic Cutaneous Lupus Erythematosus (CCLE)
These are clinical features of what condition?
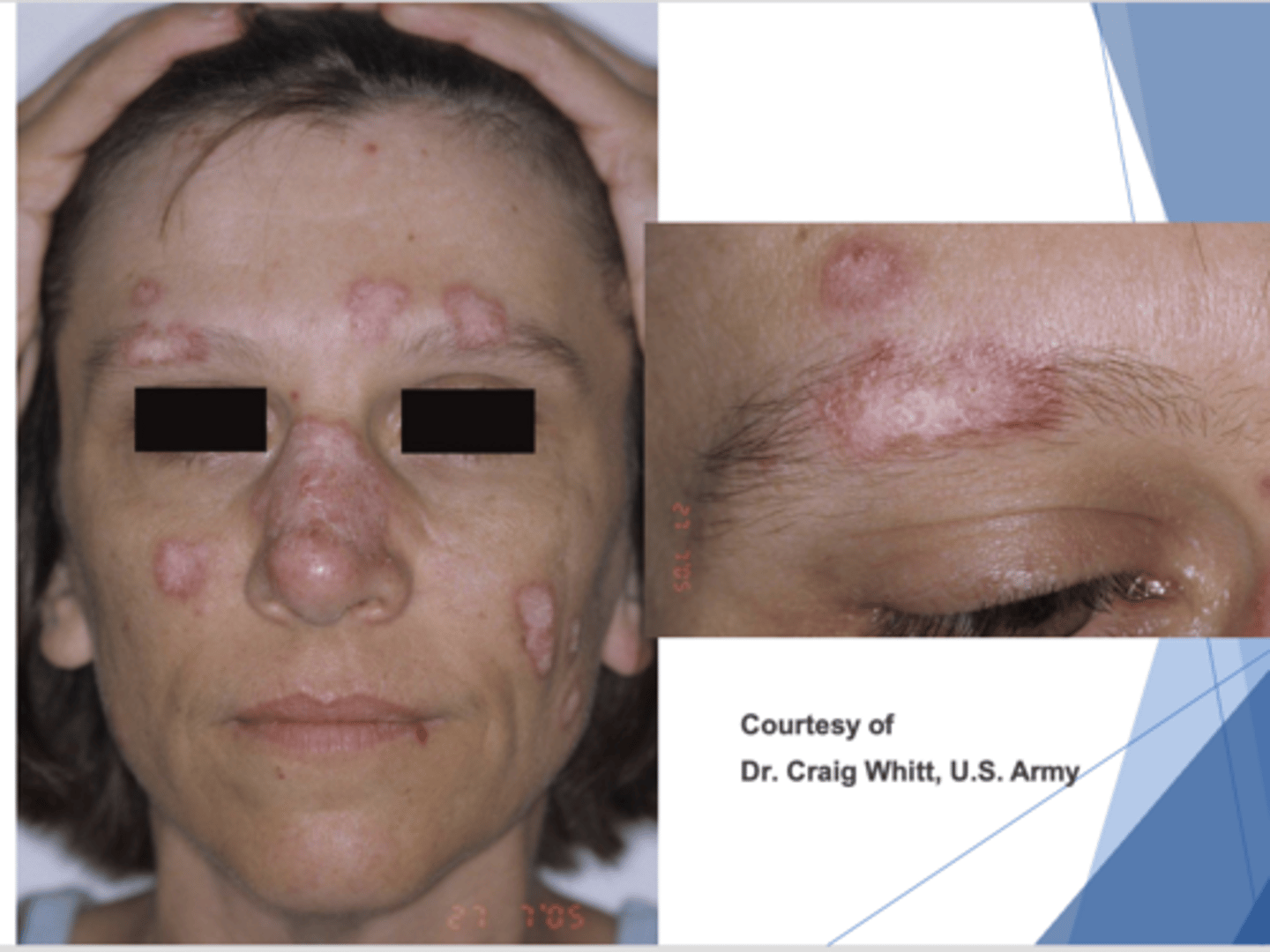
- Scaly red patches on sun-exposed skin
- Oral lesions identical to lichen planus
- Rarely without skin lesions
Chronic Cutaneous Lupus Erythematosus (CCLE)
Patient presents with these oral lesions but reports no other symptoms. Patient also has some hyperpigmented lesions on skin. What is the most likely differential?
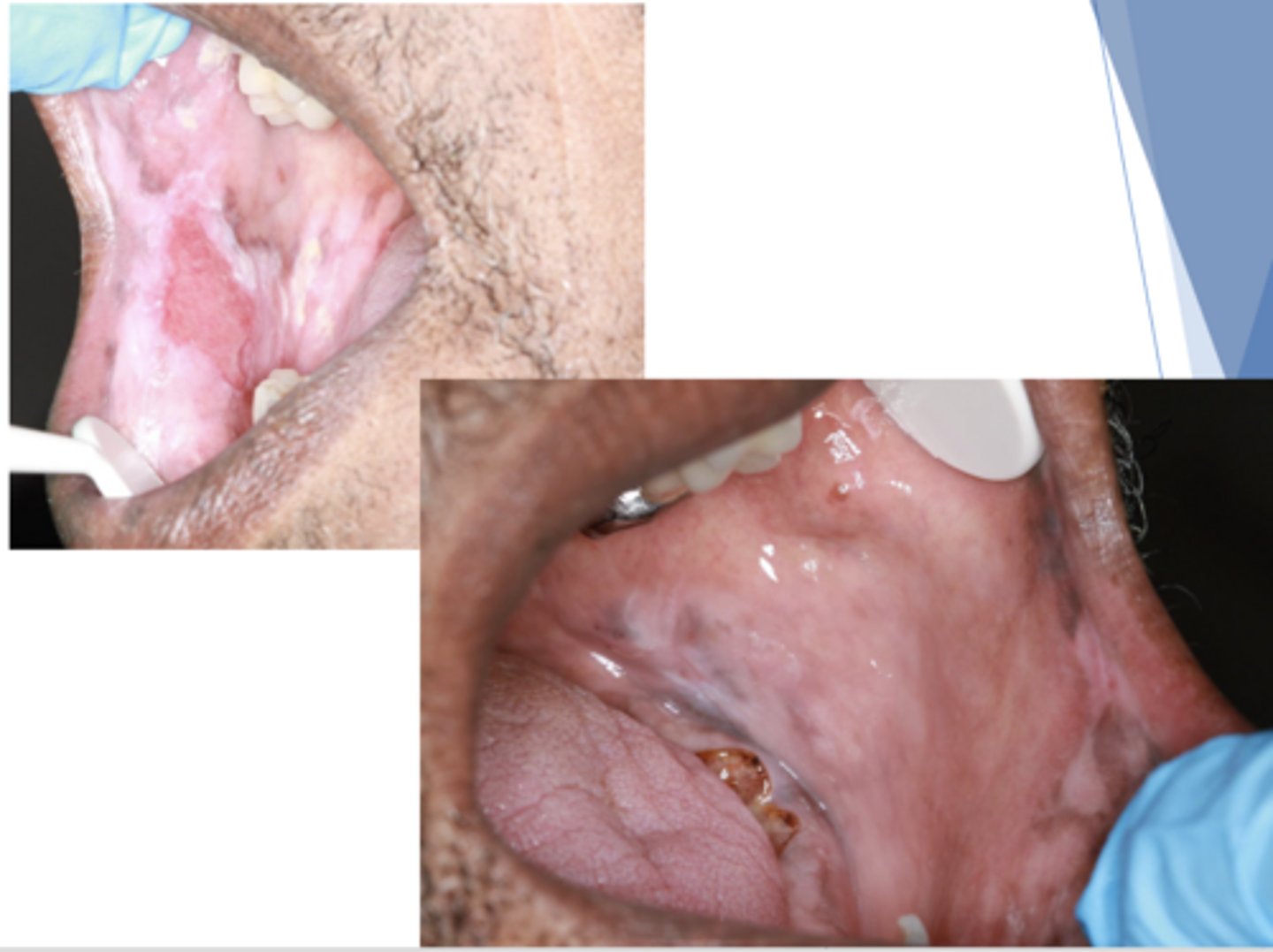
Chronic Cutaneous Lupus Erythematosus (CCLE)
Patient presents with these oral lesions but reports no other symptoms. Patient also has some hyperpigmented lesions on skin. What is the most likely differential?
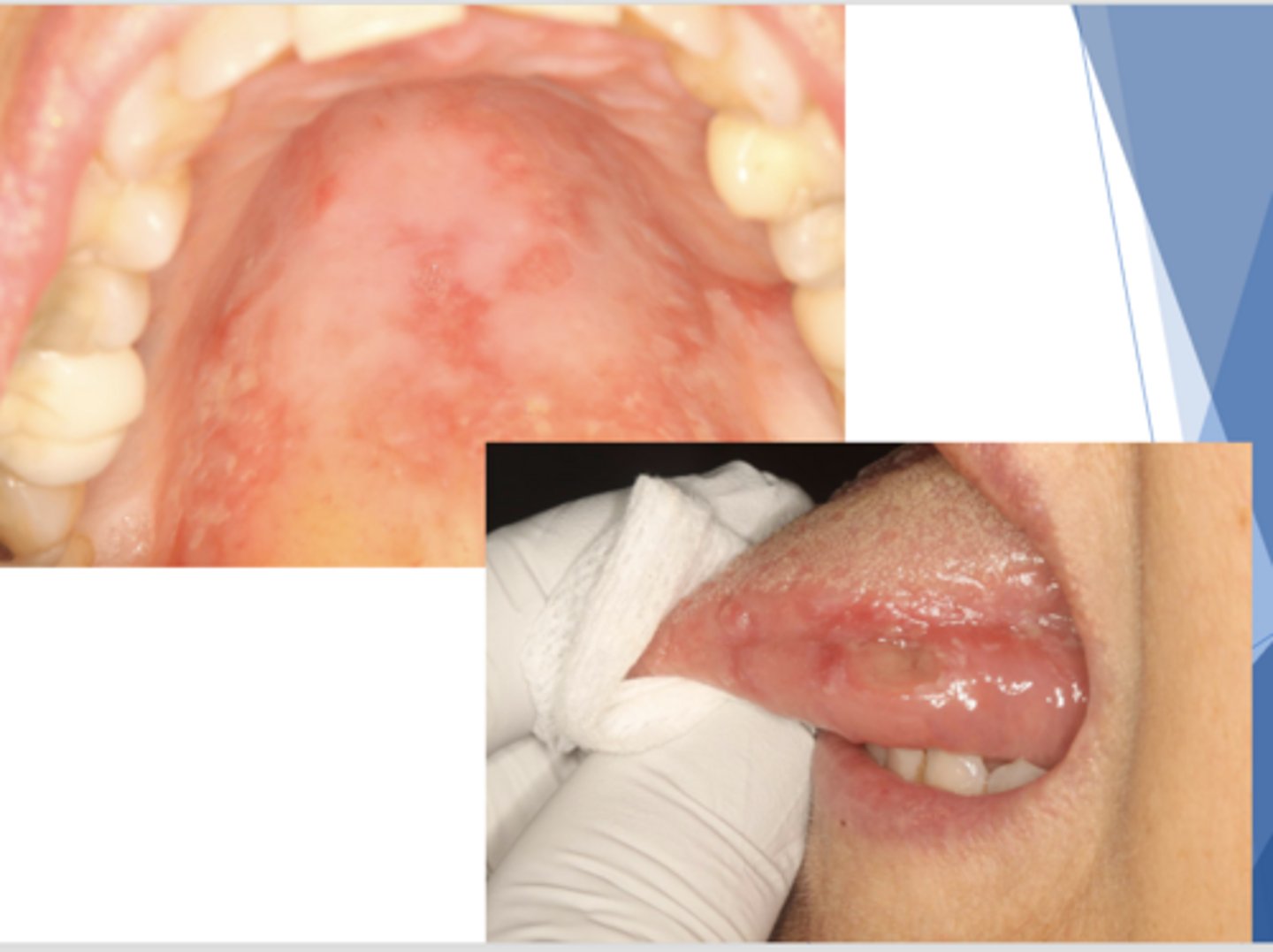
Chronic Cutaneous Lupus Erythematosus (CCLE)
These lesions are most likely caused by what condition?
- Oral lesions resemble lichen planus
- DIF shows IgM, IgG, and C3 in granular band at basement membrane
2 histopath features of Lupus Erythematosus
- Avoid sun exposure
- Mild disease managed with NSAIDs + anti-malarial medications
What is the treatment for Lupus Erythematosus?
95%
Systemic lupus erythematosus (SLE) has a ____% 5 year survival
75%
Systemic lupus erythematosus (SLE) has a ____% 15 year survival
Renal failure
What is the #1 cause of death in patients with SLE?
Men (Prognosis depends on which organs involved and frequency of reactivation)
SLE has a worse prognosis in what gender?
- Avoid sun exposure
- Topical corticosteroids
- Thalidomide or anti-malarial medications for resistant cases
tx for Chronic Cutaneous Lupus Erythematosus (CCLE)
5%
__% of CCLE pts will transform to systemic lupus erythematosus
50%
__% of CCLE pts resolve after several years
skin
most CCLE pts’ symptoms remain confined to ____
Graft vs. Host Disease (GVHD)
What condition is seen in allogeneic hematopoietic stem cell transplant recipients in which engrafted cells recognize they are not in their own environment and attack host as perceived foreign body?
- Better histocompatibility match
- Younger age
- Cord blood received
- Female gender
Patients with GVHD have a milder form of the disease if they have which 4 factors
acute GVHD
Acute or chronic GVHD?
- Seen within 100 days of transplant
- 50% of patients affected
- Presentation ranges from mild rash to diffuse sloughing (resembles TEN)
- Diarrhea, nausea, vomiting, liver dysfunction, abdominal pain
- 33-75% of patients
acute GVHD
Acute or chronic GVHD?
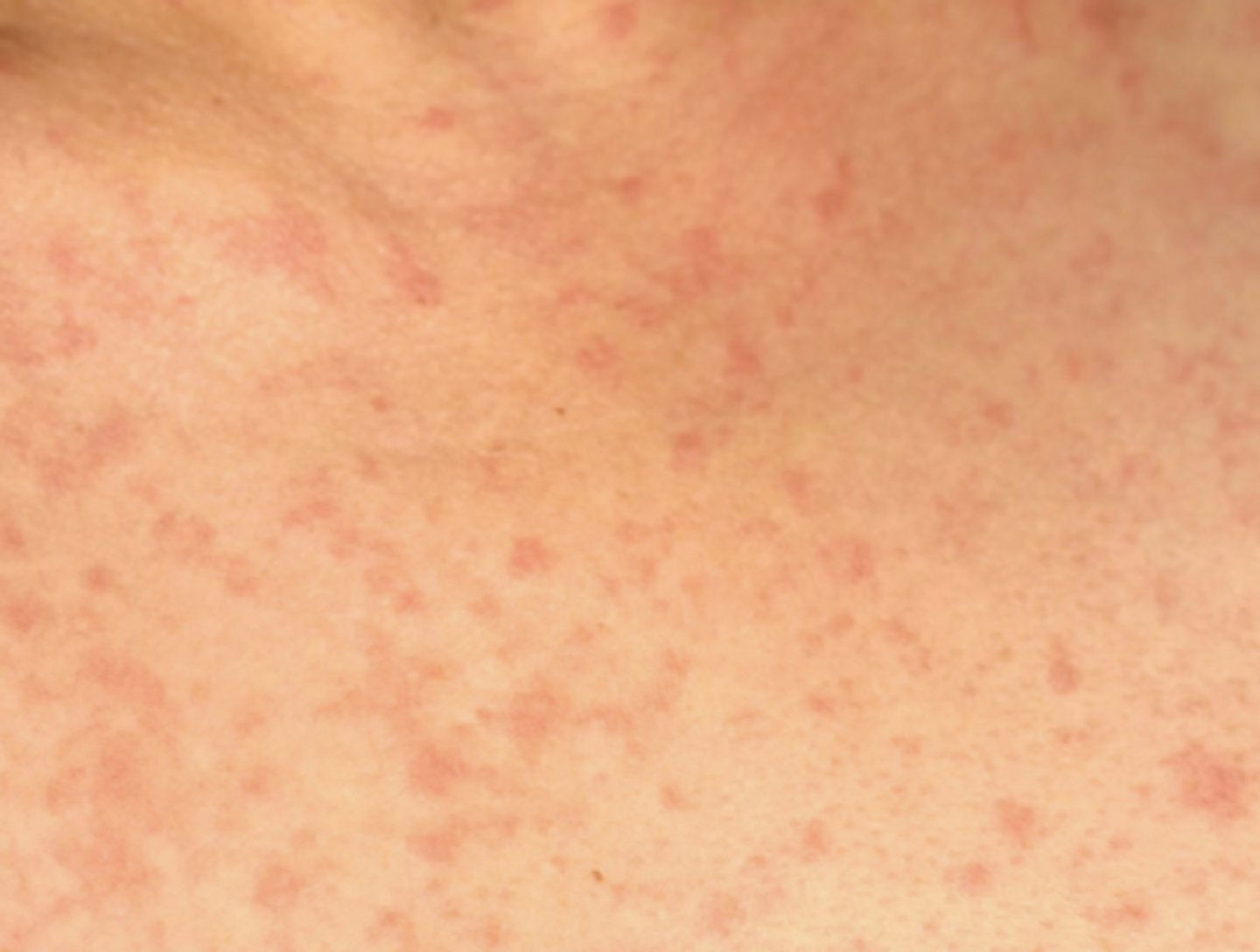
chronic GVHD
Acute or chronic GVHD?
- Continuation of acute form or develops >100 days after transplant
- 33-64% of patients affected
- 80% of patients
lichen planus
GVHD resembles what condition clinically + microscopically?
Graft vs. Host Disease (GVHD)
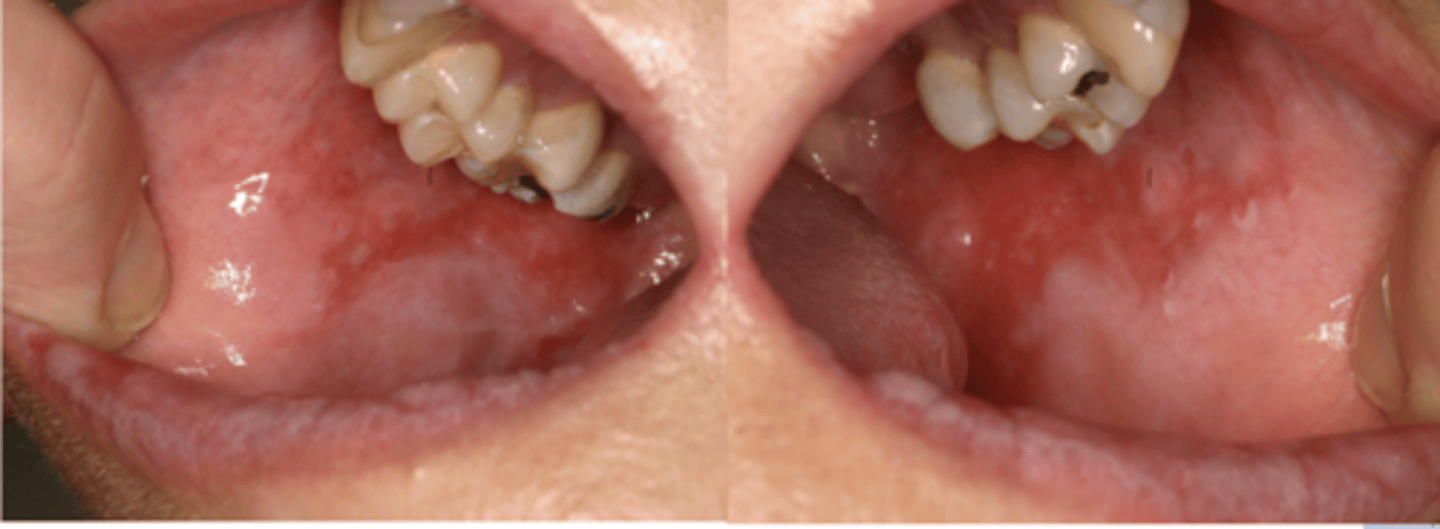
Patient presents with these oral lesions and recently received an allogeneic hematopoietic stem cell transplant. What is the most likely differential?
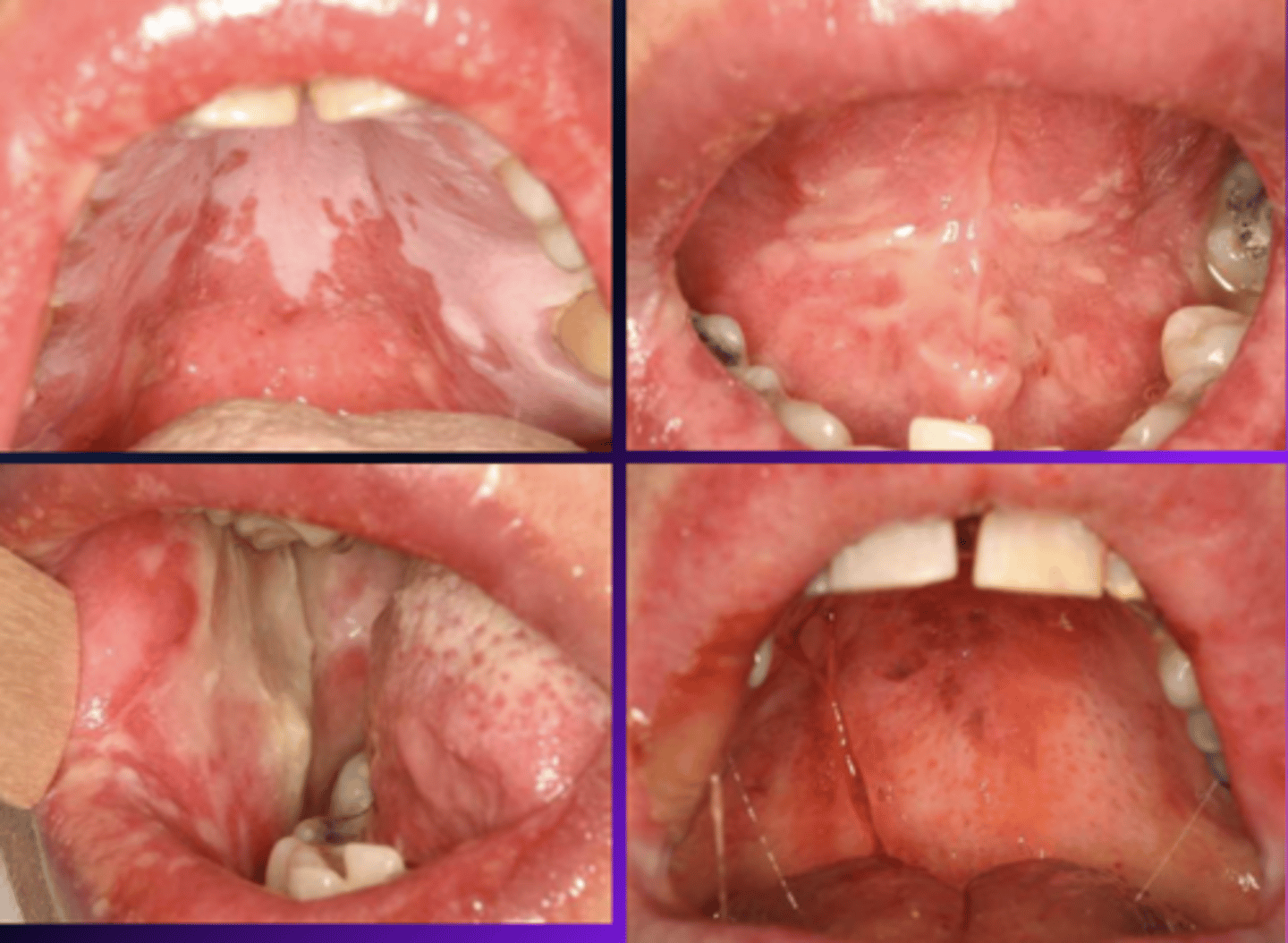
Graft vs. Host Disease (GVHD)
Patient presents with these oral lesions and recently received an allogeneic hematopoietic stem cell transplant. What is the most likely differential?
- Prevention
- Topical or intra-lesional steroids for oral ulcers
- Topical fluoride and/or sialogogues for patients with hyposalivation
tx options for Graft vs. Host Disease (GVHD)
Oral squamous cell carcinoma
GVHD patients are at an increased risk of what disease due to a prolonged inflammatory state and immunosuppression?
- Pemphigus vulgaris
- Mucous membrane pemphigoid
2 types of autoimmune diseases w/ oral manifestations
- Direct immunofluorescence
- Indirect immunofluorescence
What are the 2 widely used techniques to identify autoantibodies?
Direct immunofluorescence (DIF)
What type of immunofluorescence?
- Identifies auto-antibodies bound to pt’s tissue
- Antibodies directed against human immunoglobulins tagged w/ fluorescein
- Pt’s tissue incubated w/ anti-human antibodies
- Section viewed w/ UV light source to determine area of antibody deposition
Direct immunofluorescence (DIF)
What type of immunofluorescence?
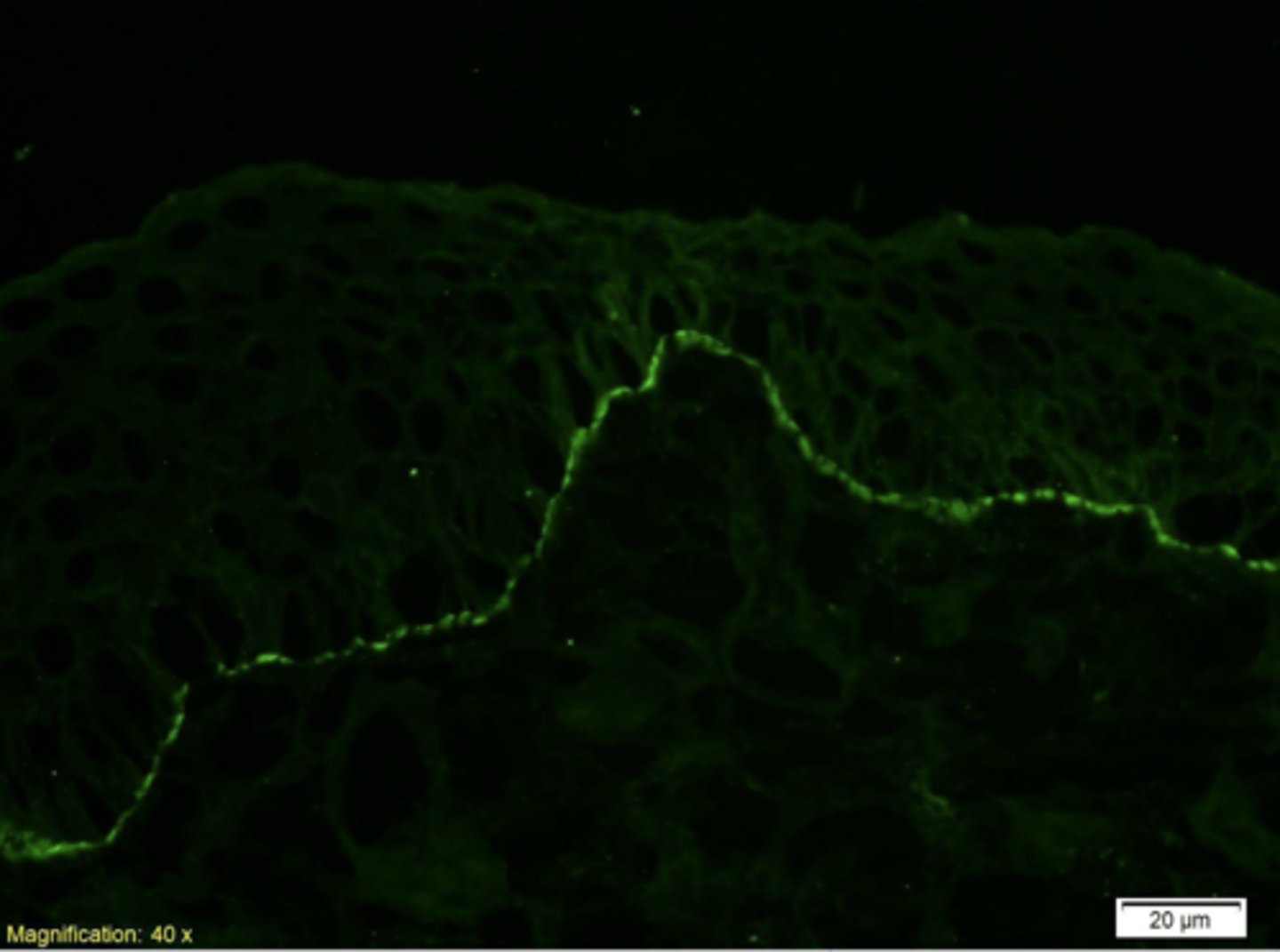
indirect immunofluorescence (IF)
What type of immunofluorescence?
- Identifies auto-antibodies circulating in patient’s blood
- Frozen section of tissue similar to human oral mucosa incubated with patient’s serum
- Autoantibodies in serum bind to homologous structure in tissue
Vesiculobullous
When considering ________ disease…
- Always include intact epithelium
- Submit separate biopsies in:
- - 10% formalin for H&E
- - Michel medium for DIF
- Defer empiric treatment, if possible, until after biopsy is complete
10% formalin
A patient with suspected pemphigus vulgaris undergoes an incisional biopsy for routine histopathologic evaluation (H&E staining). Which transport medium should the specimen be placed in?
Michel medium
A second biopsy is taken from perilesional tissue in a patient with suspected mucous membrane pemphigoid for direct immunofluorescence (DIF). Which transport medium is most appropriate?
Pemphigus vulgaris (PV)
What is the most common type of pemphigus?
Pemphigus vegetans
What pemphigus' is rare but sometimes has oral lesions: vulgaris, vegetans, erythematosus, foliaceus?
- Pemphigus erythematosus
- Pemphigus foliaceus
E F
Which 2 pemphigus' are skin lesions only: vulgaris, vegetans, erythematosus, foliaceus?
Pemphigus vulgaris (PV)
What condition?
- Potentially life-threatening skin + mucous membrane disease
- Incidence = 1-5 cases per million
- Antibodies to desmosomes
- Usually seen over 50 years of age
- No gender predilection
Ashkenazi Jewish
Pemphigus vulgaris (PV) is more common in people of what descent?
Desmosomes
Pemphigus vulgaris is an autoimmune disease in which autoantibodies attach components of what?
- Painful chronic oral sores, dysphagia, weight loss
- Oral lesions
- - 50% show oral lesions first
- - Almost all show oral lesions eventually
- Positive Nikolsky sign
3 clinical signs of Pemphigus vulgaris (PV)
Pemphigus vulgaris (PV)
What condition?
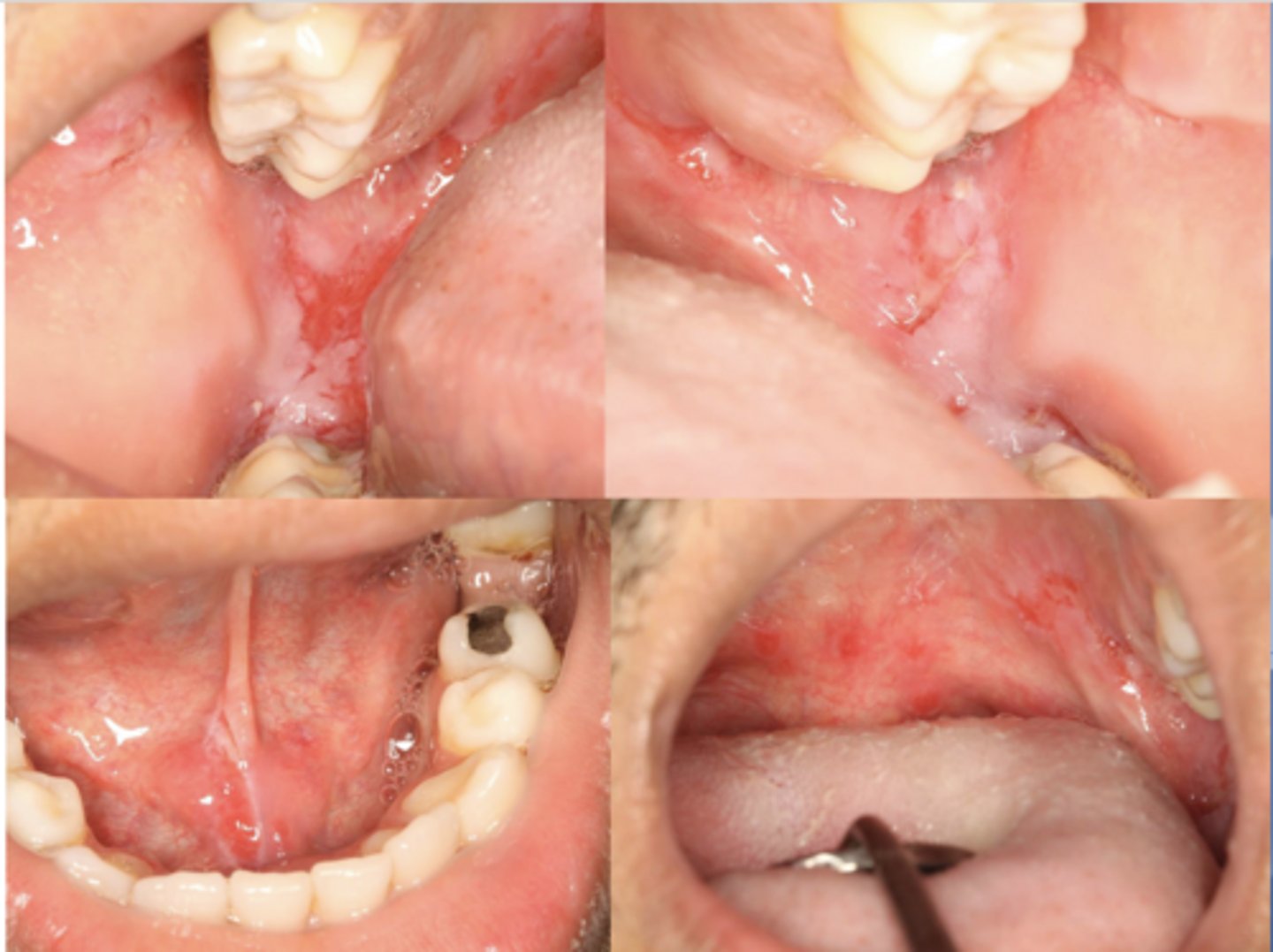
Pemphigus vulgaris (PV)
What condition?
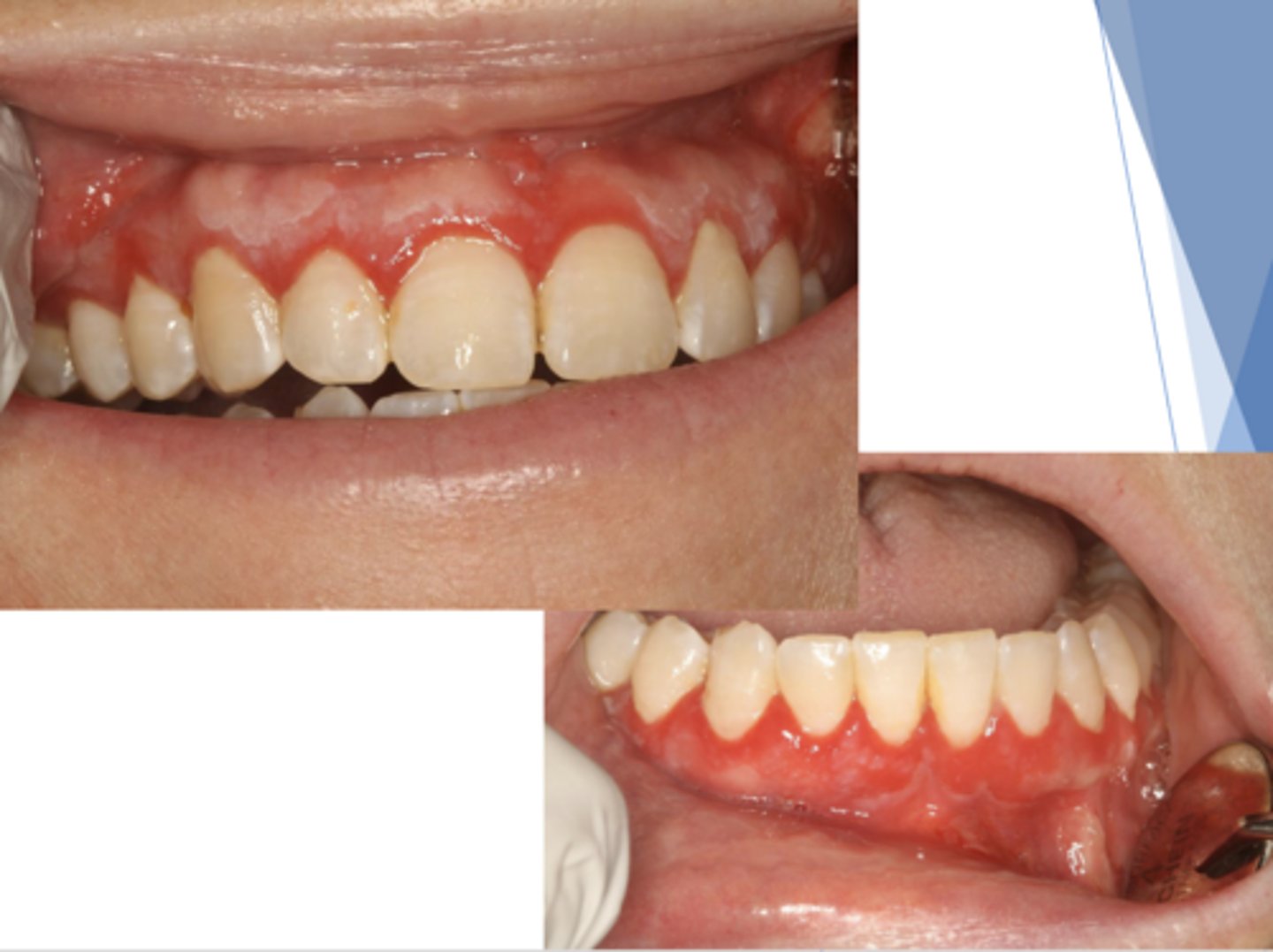
Pemphigus vulgaris (PV)
What condition?
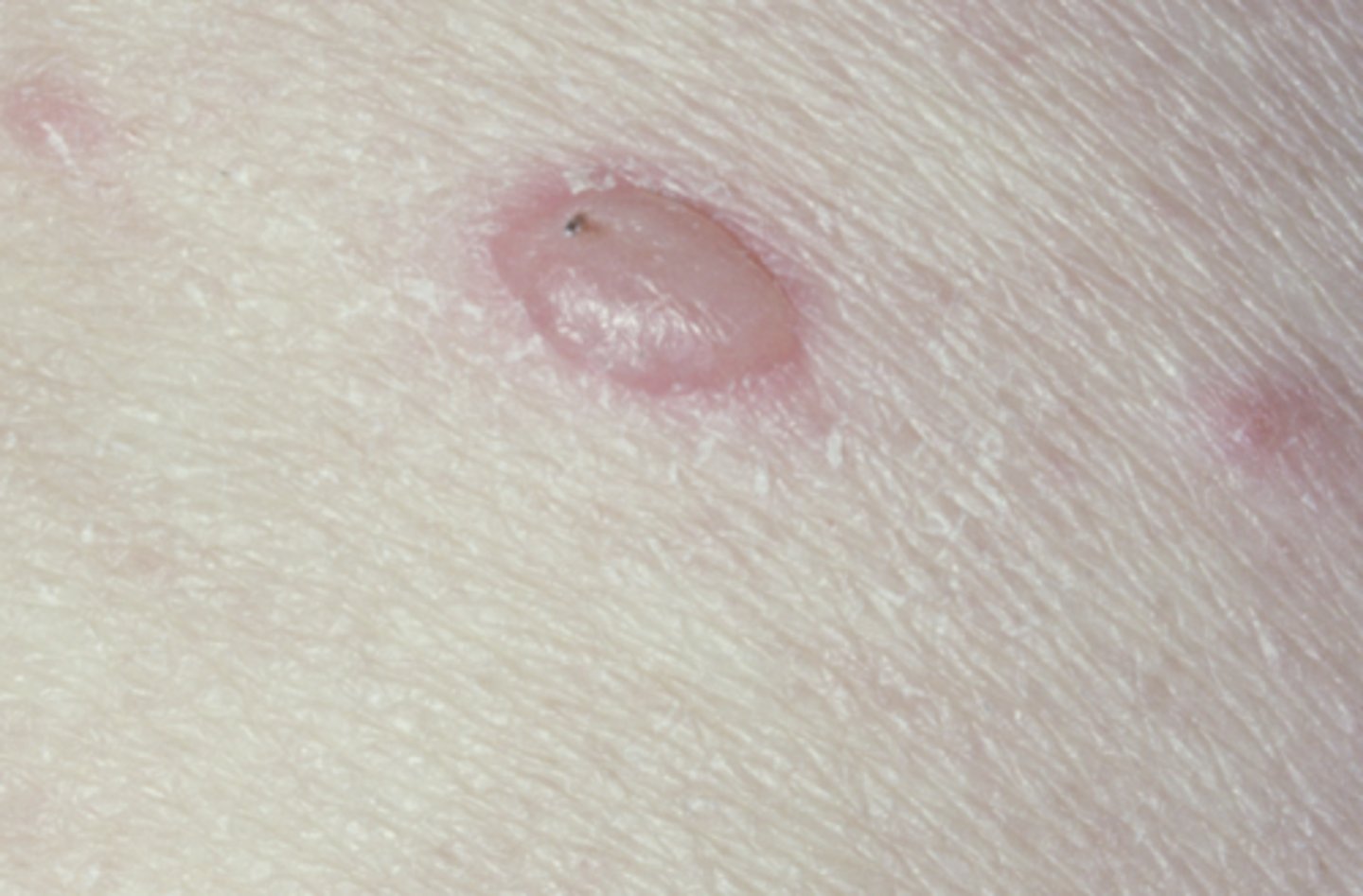
Pemphigus vulgaris (PV)
What condition?
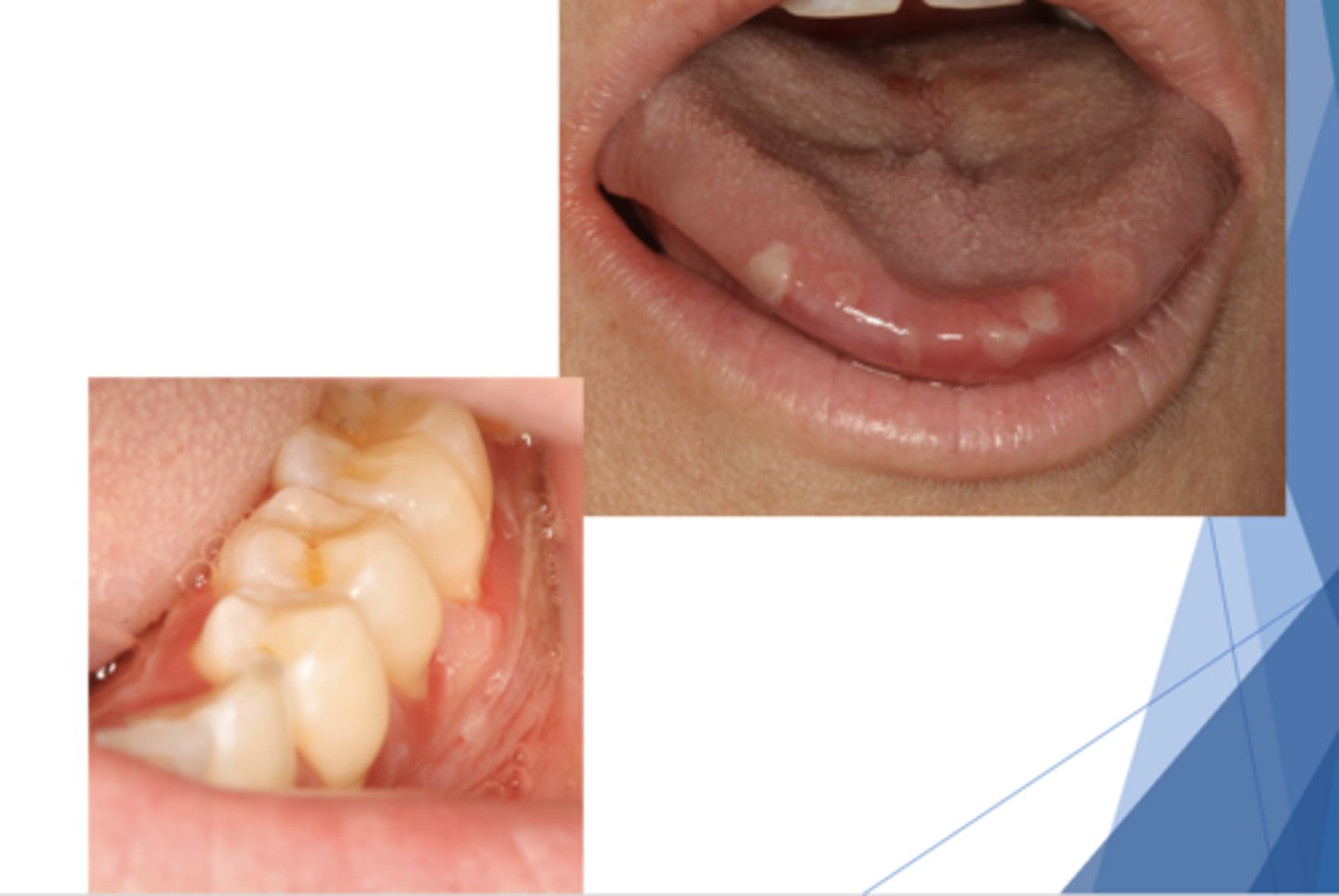
Pemphigus vulgaris (PV)
What condition has this histology?
- Perilesional tissue required for diagnosis
- Intraepithelial separation above basal layer (SUPRA-basilar cleavage)
- Acantholysis of spinous layer
- Rounded Tzanck cells
- Generally positive w/ direct/indirect immunofluorescence
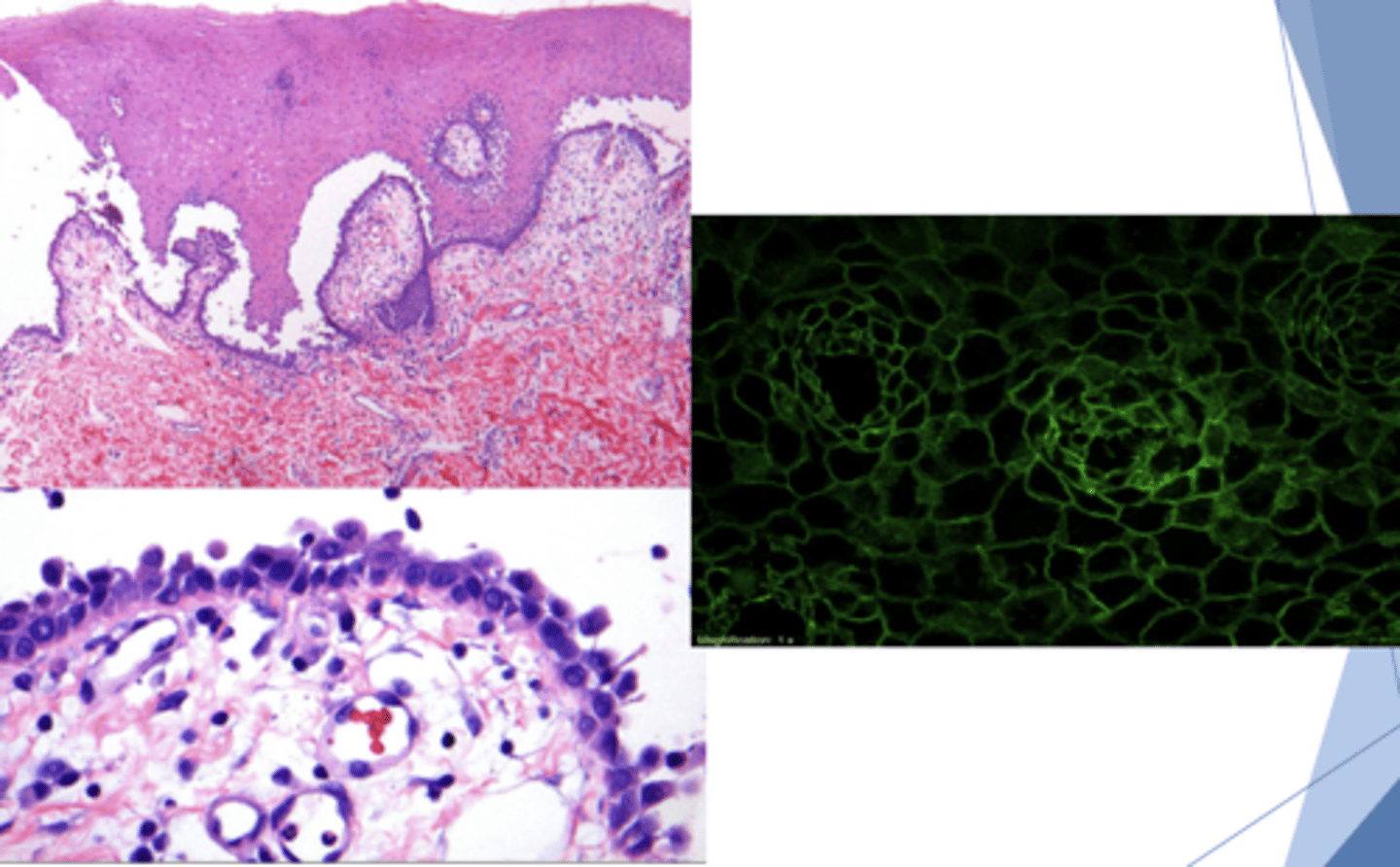
- Corticosteroids
- Azathioprine (immunosuppressant)
- Immunoglobulin therapy
3 tx options for Pemphigus vulgaris (PV)
80%
if Pemphigus vulgaris (PV) goes untreated, mortality approaches __%
Mucous Membrane Pemphigoid
What condition was formerly known as "benign mucous membrane pemphoid" or "cicatricial pemphigoid"?
Hemidesmosomes
Mucous membrane pemphigoid is an autoimmune disorder with autoantibodies to what?
Mucous Membrane Pemphigoid
What is twice as common: Mucous Membrane Pemphigoid or Pemphigus Vulgaris?
50-60, female (2:1)
Mucous membrane pemphigoid has an average age of ____-______ and a (male/female) predilection
Only ocular involvement
Only oral cavity involvement
Mucosal & cutaneous lesions
Multiple mucosal surfaces, no significant skin disease
4 subtypes of Mucous Membrane Pemphigoid
Mucous Membrane Pemphigoid
These are clinical features of what condition?
- Often restricted to gingiva
- 25% with oral lesions develop eye lesions
- Positive Nikolsky sign
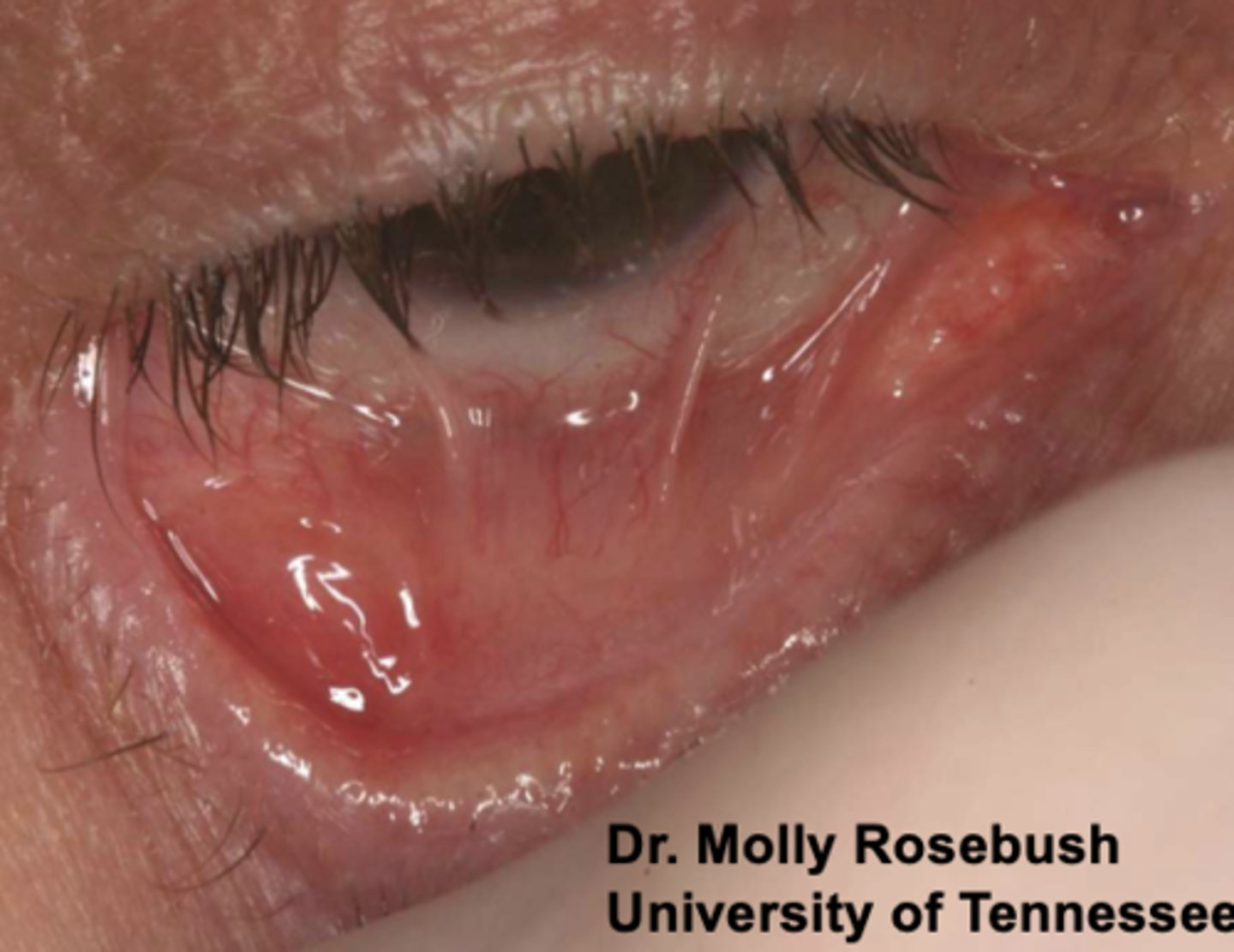
Symblepherons (adhesions)
Entropions (inward turning eyelids)
Trichiasis (irritation secondary to eyelids rubbing against globe)
3 ocular features of mucous membrane pemphigoid
25%
____% of those with mucuous membrane pemphigoid who have oral lesions develop eye lesions
ocular lesions
What is the most significant complication of mucous membrane pemphigoid?
Mucous Membrane Pemphigoid
Patient presents with these lesions along with ocular lesions including symblepherons, entropions, trichiasis. What is the most likley differential?
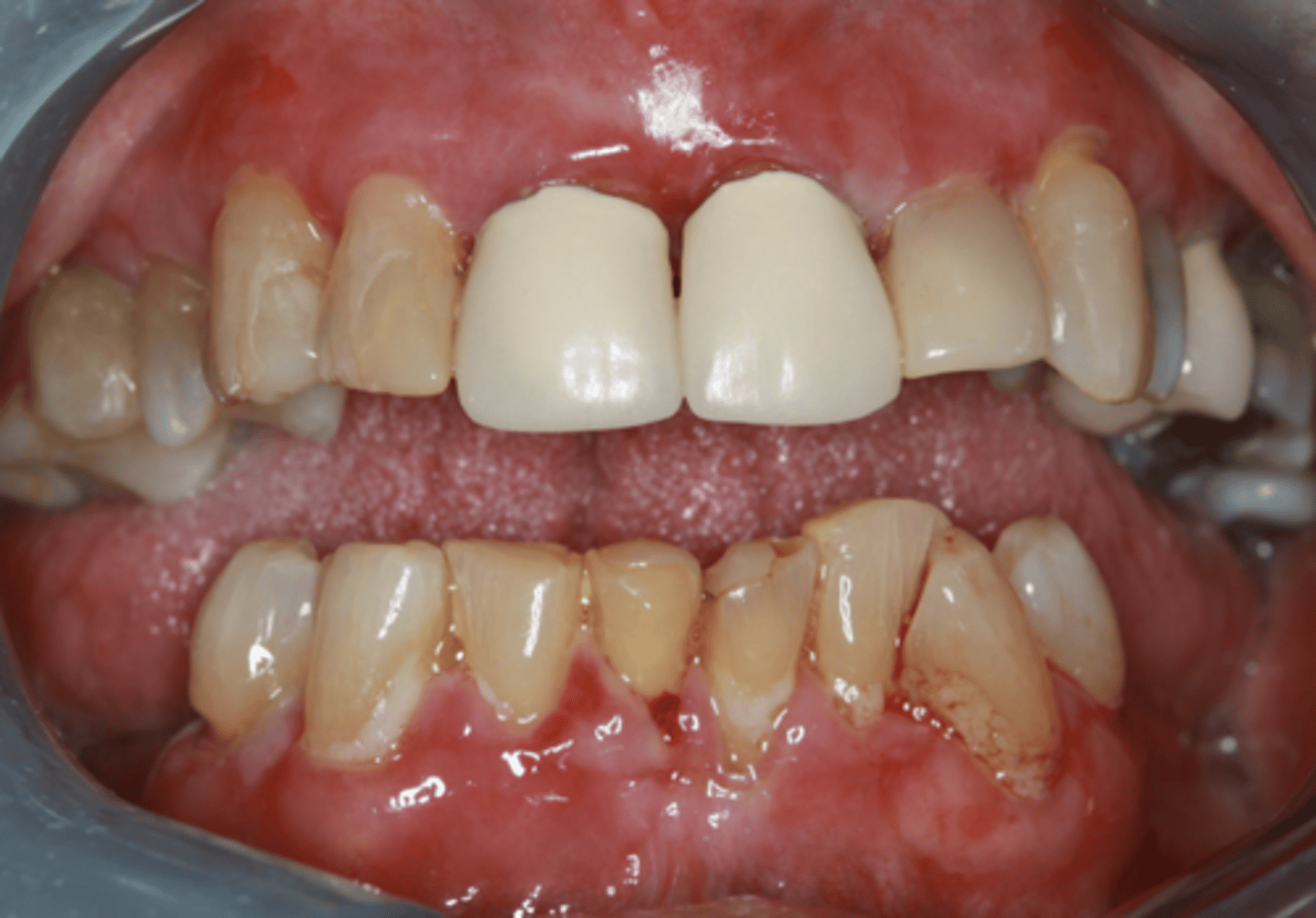
Mucous Membrane Pemphigoid
Patient presents with an autoimmune disorder with autoantibodies to hemidesmosomes. What condition do you suspect?
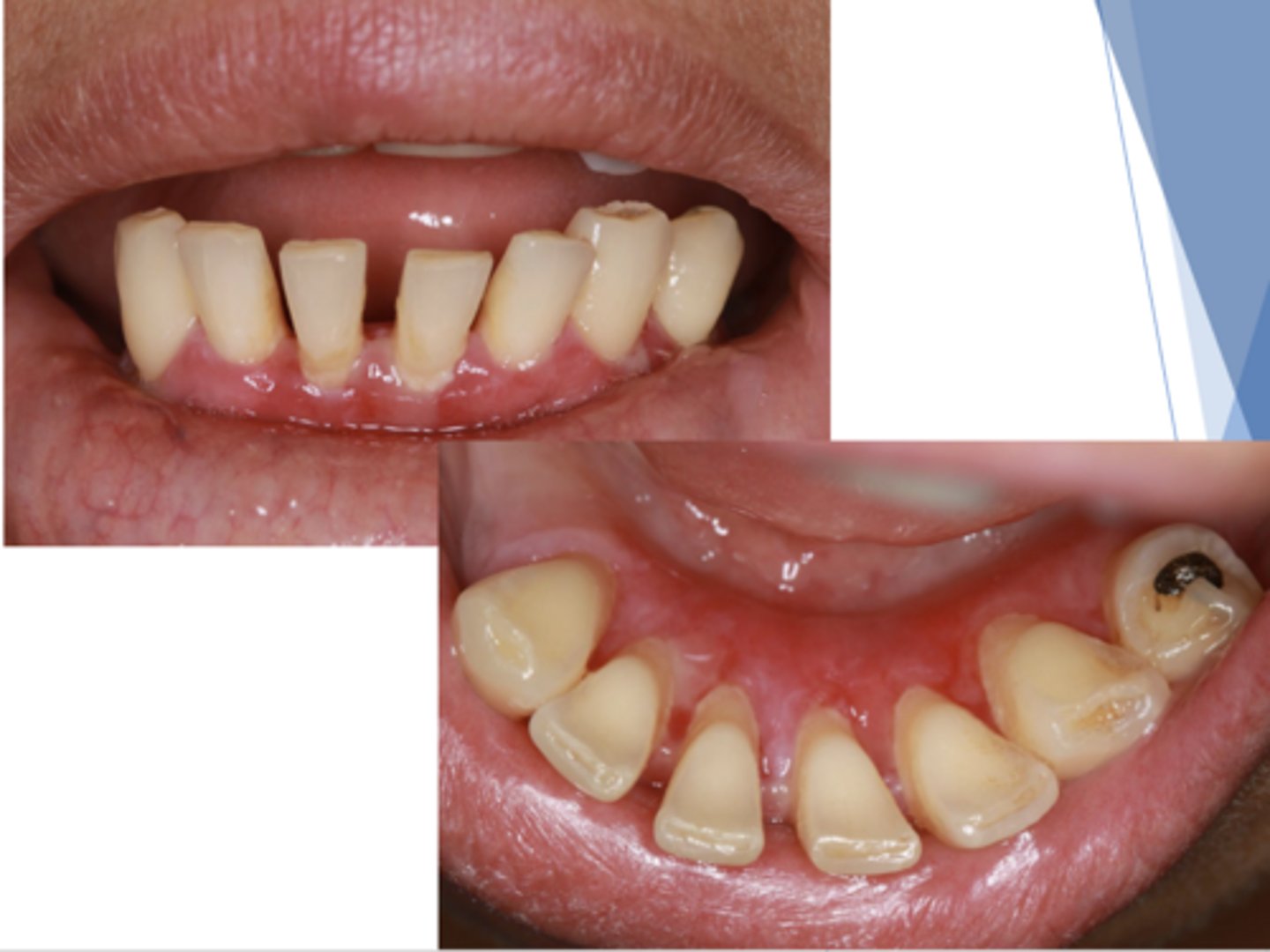
Mucous Membrane Pemphigoid
Patient presents with an autoimmune disorder with autoantibodies to hemidesmosomes. What condition do you suspect?
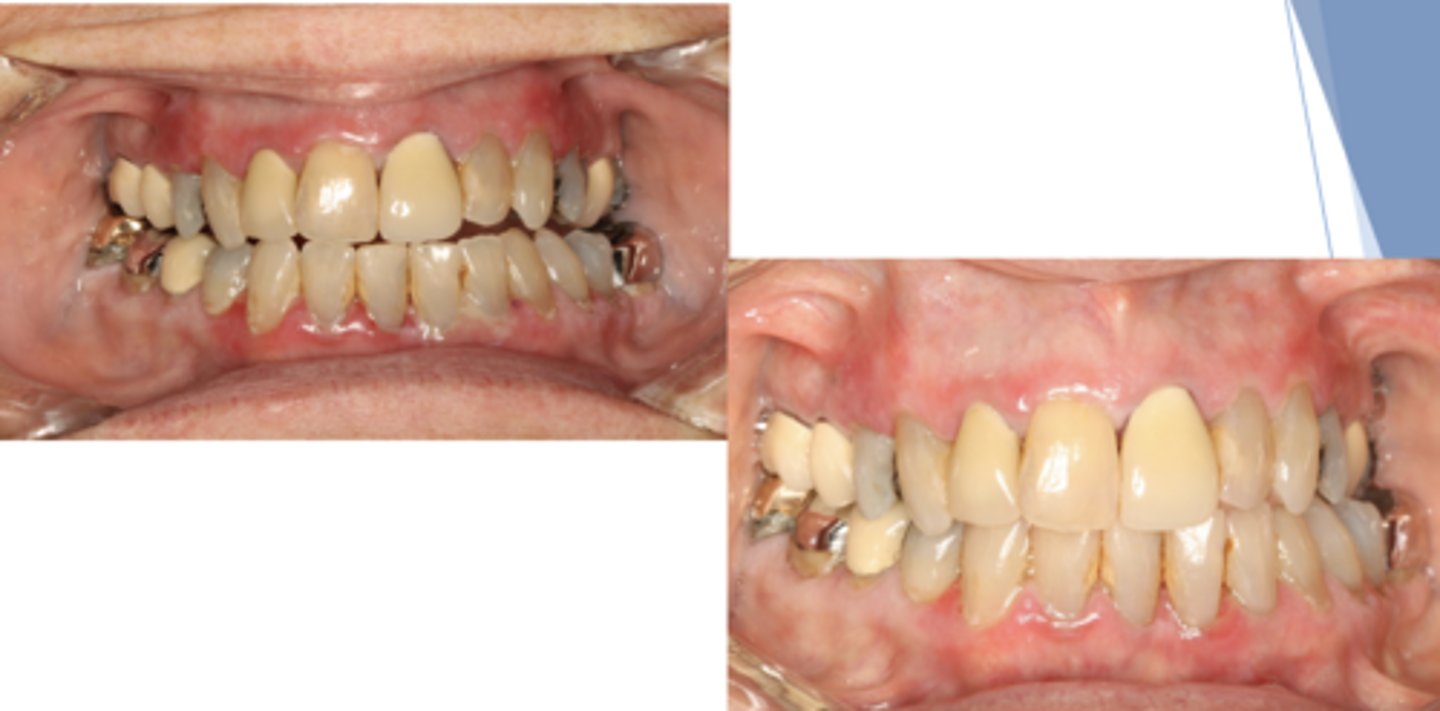
Mucous Membrane Pemphigoid
Patient presents with these lesions along with ocular lesions and an autoimmune disorder with autoantibodies to hemidesmosomes. What condition do you suspect?
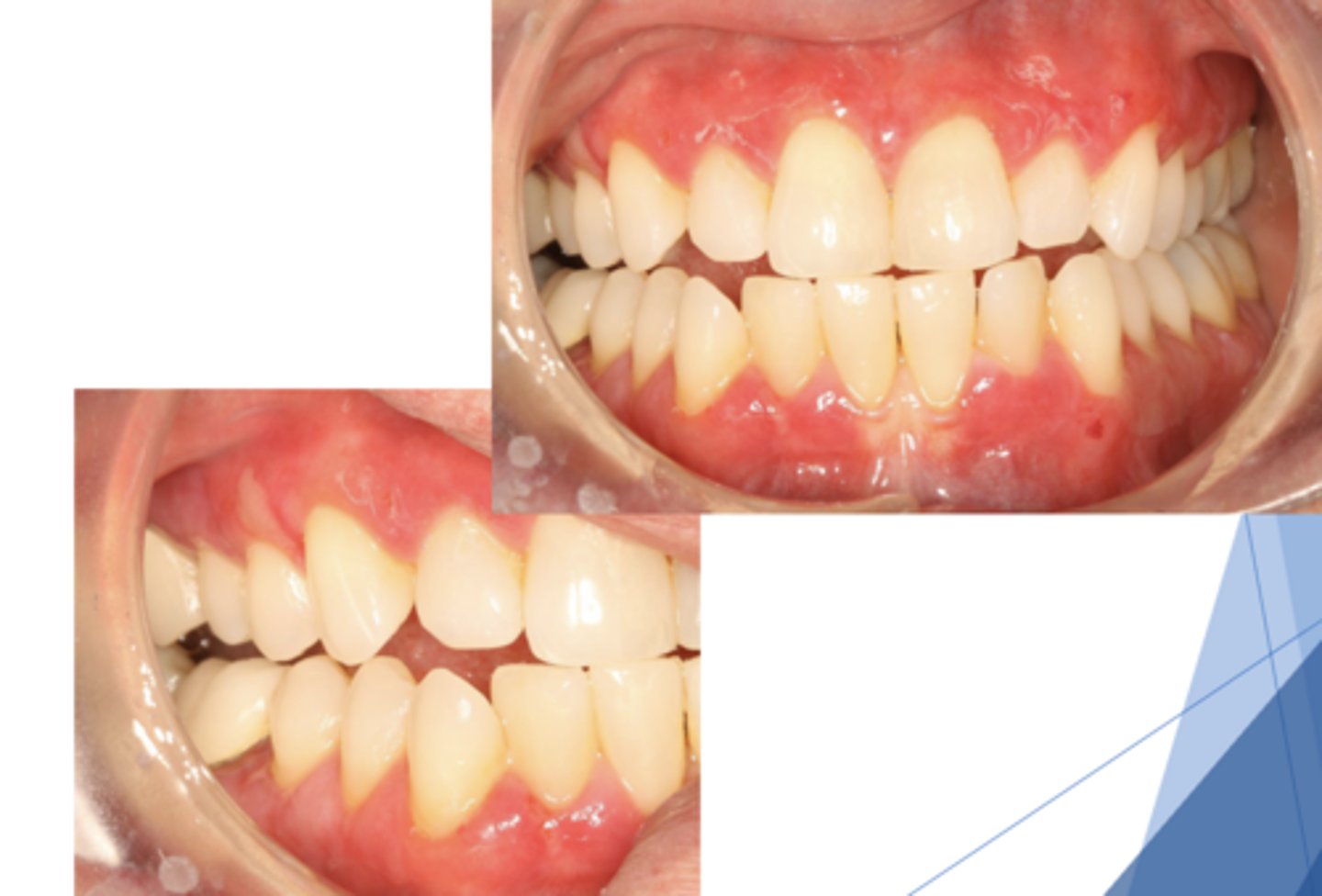
Mucous Membrane Pemphigoid
Patient presents with these lesions along with ocular lesions and an autoimmune disorder with autoantibodies to hemidesmosomes. What condition do you suspect?