Anaesthesia - safety, preparation and species specific
1/41
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
42 Terms
What are factors increase the risk of death in dogs/cats?
Dog | Cat |
|
|
|
|
How can you improve anesthetia prognosis and safety?
19 checks to be repeated
before induction
before first incision
before recovery
decrease post op morbidity/mortality by 36-48%
pre-op patient examination
good history
physical status - American Society of Anaesthesiologist (ASA)
post op tests to check progress of known disease/ unsuspected abnormalities
anaesthetic machine check
before each anaesthetic
x1 breathing system = breathing OR non-rebreathing
x1 vaporizer
monitoring equipment
how the info is obtained
how reliable is it
clinical significance of values
Define psychological safety and why it is important
Psychological Safety = a work environment where an individual feels safe to express ideas, ask questions and admit mistakes without fear of embarrassment or punishment
Importance
enhance communication
reduce error + systematic errors (report these!)
increase collaboration
reduce hierarchy in team
EVERYONE has the right to say something
improve patient safety
continuous learning and growth
What is in the anaesthetic plan?
pre-anaesthetic patient assessment
anticipated problems
related - species, patient specific
procedural
contingency planning
anaesthesia drug and support therapy
types of IV fluids system
IV rates/dose
peri-operative = premed, local, post op
physiological monitoring
hypoxaemia
hypercapnia
hypotension
hypothermia
bradycardia
post anaesthesia recovery
collaboration with hospital team
Define hypoxaemia, what causes it and how to monitor / fix it
Hypoxaemia
decrease in O2 in arterial blood
normal = PaO2<60mmHg or SpO2<90%
most likely to occur during induction
causes
low inspired O2
hypoventilation (room air → 100% O2)
shunt or venous administration
ventilation-perfusion mismatch
diffusion impairment
monitor with pulse Ox machine
minimise risk and treatment
issue with O2 supply, ET tube, equipment
optimise ventilation
low cardiac output or low peripheral perfusion, check pulse
Define hypercapnia, what causes it and how to monitor / fix it
Hypercapnia
increase in PaCO2 in arterial blood or ET CO2
normal ETCO2 = 35-45 mmHg
causes
most anaesthetics cause resp depression
decreased elimination of CO2
intervention
ET tube already in = each to fix
ventilation - manometer or capnograph
assess depth of anaesthesia
Define hypotension, what causes it and how to monitor / fix it
Hypotension
mean arterial blood pressure (MAP) is <60 mmHg
common anaesthesia complication
monitor
non-invasive blood pressure monitor = doppler
invasive blood pressure monitor = arterial catheter
causes
identify cause of reduced blood flow to heart
identify cause of reduced pump function
identify cause of reduced vascular resistance
intervention
turn vaporiser down if possible (reduce depth of isoflurane)
consider bradycardia meds, circulating volume deficit and vasopressor meds
if already bradycardic and hypotensive → give anticholinergic
Remember:
Cardiac Output = Heart Rate x Stroke Volume
MAP = Cardiac Output x Systemic Vascular Resistance
Define hypothermia, what causes it and how to monitor / fix it
Hypothermia
core temperature ideally <36 degrees
consider surface area to volume ratio of patient
radiation (core → enviro = 40%)
convection (air and alcohol swab = 30%)
evaporation (cleaning fluids for open wound = 15%)
respiration (breathing = 10%)
conduction (heat of table = 5%)
prevent
forced air warmers - minimise radiation and convection loss
prewarming
fluid warmers
be cautious of burns
List the key safety considerations during recovery
when to deflate cuff + extubate
secure air way to prevent aspiration of drugs or abdomen contents
Is the patient moving air = ventilating?
feel for air flow
listen
watch chest wall and abdominal movements
maintain SpO2 >95%
Continue monitoring the patient
oxygenation
warming
IV fluids
analgesia - grimace pain scale
bladder care - express before start to recover
Dog | Cat |
|
|
What are the major components (10) of an aesthetic machine and their function
Gas Cylinder = coloured (O2 is white, nitrous oxide is blue, CO is light brown). Pressure of the gas in the cylinder is proportional to the contents EXCEPT nitrous oxide as it is stored as both a liquid and gas. Cylinders differ size (C, D, E)
Oxygen Pressure Gauge = measures the level in the cylinder and in the flowmeter (useable = 400 kPa)
Flow Meter = controls gas flow to patient, measure to the TOP of the bobbin, or the MIDDLE of the ball
Vaporiser = changes inhalant from a liquid to a vapour + adds a controlled amount of vapour to fresh gas flow (e.g. isoflurane)
Common Gas Outlet = where breathing system attaches to anaesthetic machine. Delivers mix of vaporiser and O2. If you press the red button, you can flush O2 though to drain out remaining isoflurane.
Oxygen Flush = delivers high flow O2 from common gas outlet. This bypasses the flow meter and vaporiser to deliver pure O2 (do not press whilst patient attached)
APL (Adjustable Pressure Limiting) Valve OR Pop Off Valve OR Spill Valve = if open, allows the excess gas to escape into the scavenging system, release waste gas. Allows the breathing system to connect to scavenging system. If closed, allows intermittent positive pressure ventilation.
Reservoir or Rebreathing Bag = holds gas for patient, can be used to produce manual breaths/ventilate, used to monitor resp rate
Scavenge System = consists of APL Valve, interface and waste gas elimination system (passive or active)
Passive = dose not use negative pressure
Active = slight vacuum
Breathing Systems =
Full rebreathing system: flow rate = metabolic O2 need
Adults = 10+ kg (and also paediatric = 2-9 kg)
Partial rebreathing system: flow rate between metabolic O2 need and RMV
Non-rebreathing system: flow rate is greater than RMV
Patients less than 7-10 kg
List some key safety considerations of anaesthetic machines that can be fatal
if a gas cylinder is knocked over and reducing valve is broken off the cylinder, may act as a missile and be secured/fixed
always ensure adequate O2 in the cylinder and that is is on, BEFORE starting anaesthesia
never press an O2 flush button whilst the breathing circuit is still attached to the patient = death as patient lungs will explode with extreme pressure
if the APL valve is left closed with the patient attached to to the breathing circuit = death as increased pressure in thorax reduces venous return + cardiac output
active scavenge systems that does not contain an interface that prevents the build up of positive or negative pressure = death of patient due to the remove of gas from the patient
when 50% of soda lime cannister has changed colour, is MUST be replaced unless not effective
What is mechanical dead space?
The dead space of a breathing system = volume from where fresh gas enters the system to the beginning of the patients airway (incisor teeth)
one-way valves that stop closing will cause increase in dead space = allows rebreathing of CO2

Explain the components of rebreathing systems and their purpose
One Way Valves
ensures one-way movement of gas around circuit
attached to CO2 absorbent canister (yellow circles)
checked and cleaned regularly for maximum efficiency
increased moisture may cause them to get stuck in open position
if stop closed will cause dead space
malfunctioning = detected as inspired CO2 on capnograph
Rebreathing Tube
connects circuit breathing system to patient
Y-piece = heated and non-heated
Co-axial or F-cuit (inside each other)
Advantages = reduce bulk + warming inspired gas
Disadvantages = if inner tube breaks, patients will inspire CO2
Soda Lime Cannister
chemical absorbent that removes CO2 from exhaled gas
white granules → purple when exhausted
pink granules → white when exhausted
fresh granules will crumble and you can feel them produce chemical reactions due to heat of cannister
exhausted granules are hard and will show as inspired CO2 on capnograph
change this as soon as 50% of cannister has changed colour
Explain the components of non-rebreathing systems and their purpose
Under 10kg
Ayre’s T Piece
FG (central outlet) = delivers fresh gas from anaesthesia machine
P (right side) = connects to patient
EG (left side) = directs exhaled gas away from patient
Mapleson D
rebreathing bag attached
pop-off valve open
scavenge system is attached at the level of the pop-off valve
List the gas flow rates: rebreathing, partial rebreathing and non-rebreathing systems
Flow rate for rebreathing system = 4-10 ml/kg/min
O2 flow rate = metabolic O2 requirement
Flow rate for partial rebreathing system = 20-50 ml/kg/min
flow rate is between metabolic requirement for O2 and resp minute volume
Flow rate for minimal-rebreathing system = 100-200 ml/kg/min
flow rate is greater than resp minute volume
pre-oxygenation and beginning an anaesthetic or priming circuit
Flow rate for non-rebreathing system = 300-500 ml/kg/min
no soda lime to remove CO2 so higher gas flow rate is needed to remove CO2
Advantages and disadvantages of rebreathing systems
Advantages | Disadvantages |
|
|
Advantages and disadvantages of non-rebreathing systems
Advantages | Disadvantages |
|
|
How do plan before anaesthesia ? (SHEAP)
SHEAP
Signalment
age = speed of drug metabolism
dog breed = greyhound, boxer, brachycephalic, collies, shepherds have varied recovery
cat = specifies differences
size = metabolic rate + hypertension
History
current medications
wellness - current disease or clinical signs
has it been fasted?
Examination
cardiovascular system
respiratory system
body condition score
demeanour
Assessment
body systems
problem list = why did it present today? previous?
differential diagnoses
ASA status (American Society Anaesthesiologist Pain Scale)
Plan
Diagnostics
Blood work
Reassess
ASA status again
Plan drugs
list of potential complications
patient specific = history, signalment
body systems = exam, assessment
procedure considerations
5 H’s + B: (Hypotension, Hypoventilation, Hypothermia, Hypoxaemia, Bradycardia)
Anaesthesia Drug Plan (PIMS)
Preanesthetic stabilisation
dehydration, hypovolaemia or electrolyte abnormalities
pre-oxygenate 3-5 mins prior to induction w will fitting mask
Rebreathing = 100-200 ml/kg/min
Non-rebreathing = 300-500 ml/kg/min
Premedication and Analgesia Plan
contraindications?
route? - usually before catheterisation
monitor respiratory and cardiovascular response
usually opioid ± sedative
Opioids = gabapentin or trazadone, methadone, morphine, butorphanol, buprenorphine
Sedative = acepromazine, midazolam, diazepam,
Both = medetomidine, dexmedetomidine,
Induction agent
Injectable = most common, titrate to effect
Eg: alfaxalone, propofol, ketamine, midazolam, diazepam, thiopental
Inhalant = mask or a box if can’t place catheter
O2 + drug (usually isoflurane)
monitor depth when in box, increased stress
pollutes environment
Maintenance drugs
Inhalant and/or CRI
Monitoring equipment = SPO2, ETCO2, doppler, ECG, BP
Supportive therapy
fluids
cardiovascular support = minimum 30% O2 for 5 mins post inhalant, check O2 levels with SPO2
post op analgesia
Key notes for Intubation and Extubating in Dogs vs Cats
Intubation
occurs after induction drug
Cats = susceptible to laryngospasm → must spray/drop lignocaine first and wait 20-30 seconds after
0.1-0.2 ml of 2% is normal
5mg/kg or more = overdose
Cats = susceptible to tracheal necrosis and rupture
use an uncuffed ET tube (must check for leakage)
use a cuffed ET tube must inflate carefully
Post Intubation
connect breathing system and ETCO2
tie ET tube in place, below the connector and inflate if required
check for depth or life
turn on maintenance
always disconnect patient when changing position to ensure trachea does not get damaged by ET tube
never leave a patient with ET tube in unattended
Extubating - Dog | Extubating - Cat |
If oral procedure or risk of regurg:
Brachycephalic = always leave intubated until vigorously attempting to expel ET tube, then extubate |
|
C-Section Considerations (elective or emergency)
All C-Sections
General anaesthetic considerations
Hypoventilation, Hypothermia, Hypoxaemia, Hypotension
Physiological alterations induced by pregnancy
early =physiological - progesterone and oestrogen
later = mechanical - enlarged uterus
Maternal pathology (obstetrical complications like blood loss)
Pharmacology of drugs effected mother and neonates
Analgesia
Neonatal revival
Emergency:
often electrolyte and haematological imbalances (Ca)
higher mortality rate in puppies delivered by c-section due to maternal physiological state due to prolonged labour and foetal stress in utero
Neonates
good preparation
O2, masks and ET tubes x many of each
suction
warm and dry towels
vigorous rubbing to stimulate
may be hypoxic → bradycardia = potentially give adrenaline?
pharmacological = naloxone or last resort doxapram
Cardiovascular, Respirator, GI and CNS changes with pregnancy and effects on anaesthetic
Cardiovascular
increased blood volume → increase cardiac output + high HR
BP unchanged
Anaesthesia = risk of hypotension if low BV, CO, HR, uterine blood
Prevention = monitor BP + IV fluids (avoid overload + vasopressors)
Respiratory
increased respiratory minute volume and oxygen consumption
decreased functional residual capacity
Anaesthesia =
more rapid uptake of anaesthesia agents
increased risk of hypoxaemia
increased atelectasis (lung collapse) especially if in dorsal
Prevention = pre-oxygenate, ventilate and sustain inhalation
Gastrointestinal
emptying of contents is slowed
decreased oesophageal sphincter tone
increased gastrin and intragastric pressure
Anaesthesia =
risk of aspiration pneumonia
acidic stomach contents
unknown fasting status if emergency
Prevention = rapid induction, intubation and cuff inflation but extra care with extubating
Central Nervous System
decreased anaesthetic requirements
venous engorgement epidural space
Anaesthetic = risk of overdose, lower epidural volume needed
Prevention = monitor depth, use short acting and reversible drugs
Pharmacology of Drugs when Pregnant
Pathology
dehydrated / hypovolaemic / electrolytes → risk of toxaemia
stress and exhausted → limited self regulation
pre-existing disease
medications = Oxytocin
potential risk of haemorrhage
Pharmacology
decreased MAC (minimal alveolar concentration) = decreased dose
use weights prior to pregnancy
placental transfer = assume all drugs willl cross into placenta
effected by blood flow, thickness, SA, diffusion of drugs
analgesia is needed for C-section
opioids - short acting and reversible
local anaesthetic - epidural or midline local pre/post incision
NSAID - in recovery
Premed = none or a short acting opioid
Induction = propofol or alfaxalone (titrate to effect)
AVOID = ketamine, thiopentone, benzodiazepines and alpha 2 agonists
Maintenance = low dose Isoflurane + O2 also oxytocin intraoperatively
Post birth = methadone IV, NSAIDS
Anaesthetic plan for horse in field or hospital
Equine anaesthetic mortality = 1:100
cardiovascular arrest, fractures, respiratory obstruction, myopathy, neuropathy or myelomacia
increased risk if = foals, geriatric, high ASA status, if in dorsal recumbency, emergency, fracture repair surgery
decreased risk if = short procedure, total IV anaesthetic, using acepromazine
Pre-anaesthetic
informed risk and consent in writing
exam + accurate weight for drug dosing
bloods and lab tests ideal but often not possible
preparation if in field
IV catheter (aseptic) = 14 G with 3.25 or 5 inch catheter
fasting = no evidence/should not be fasted. Just wash out mouth prior
cannot vomit, so little risk of regurgitation
may remove shoes or bandage hooves to prevent injury in recovery
use NSAIDS and antimicrobials prior to anaesthetic
Potential problems or complications with GA in horses
Hypoventilation (high PaCO2)
drugs used, effected by anatomy, size and weight
dorsal recumbency = pressure on lungs → low tidal volume
Hypoxaemia (low PaCO2)
can occur even if on 100% O2
ventilation perfusion mismatch → shunting (due to anatomy)
Hypotension (myopathy)
ideally, mean arterial blood pressure is above 60 mmHg (below leads to myopathy)
monitor BP closely due to large body weight compression
Neuropathy
peripheral nerve injury
Fractures or major injury
increase muscle relation pre induction and good analgesia
lubricate and protect eye
Field location vs hospital
consider weather and temperature
grass is ideal
Other = breed, procedure, pathology, analgesia
Prevention
reduce procedure time
always 100% O2 and controlled ventilation when possible
naso-trachael tubes for recovery (obligate nasal breathers)
monitor = capnograph, pulse Ox, arterial blood gas
use adequate padding underneath and between limbs
if in lateral recumbency, pull down leg forward
if in dorsal recumbency, support front legs, avoid overextension in hind
avoid overextension of neck and remove halters
Premeds, Induction and Maintenance drugs during equine anaesthetic
Premedication = sedate, muscle relaxant and analgesia
local blocks as much as possible = standing surgery is best
5 point stance = x4 legs and head down
Acepromazine
mild tranquilisation but no analgesia
reduced risk of death peri-operatively
smooth induction
vasodilation
Alpha 2 Agonists
sedates, relaxes and analgesia
may cause bradycardia, hypertension, increased urine, increase blood glucose, and motion
Opioids
well when with alpha 2 agonist (sedate + analgesia)
minimal cardiovascular effects
may cause excitement but slow GIT → colic
methadone is better then butorphanol
Induction = predictable, controlled and uneventful
standing → lateral recumbency requires adequate sedation and muscle relaxation (may use mechanical tools)
always bolus drugs to ensure they don’t panic
Co-induction:
Diazepam or midazolam = central muscle relaxant
Guiafensin = central muscle relaxant (causes haemolysis)
Induction agents
Ketamine = increase HR/BP, minimal RR and GIT SE, only provides analgesia not muscle relaxant
Alfaxalone and Propofol = mainly for foals
Maintenance
TIVA = total intravenous anaesthesia, intermittent bolus or CRI
45-60 mins max
gravity infusion set or infusion pump/syringe pump
be careful with intermittent bolusing and maintaining steady GA
Inhalation = isoflurane, sevoflurane or desflurne
dose dependant cardiovascular depression
no analgesia
Monitoring and Recovery from GA in equine
Monitoring during Anaesthesia
Depth = movement, muscle twitching, RR, CO
light = eye movement is normal, minimal change in HR + BP
Cardiovascular = MM colour, CRT, HR, pulse, direct/indirect BP
Respiratory = RR, capnograph, pulse oximetry, arterial blood gas
Recovery
critical period
improve with analgesia, positioning, oxygen, using halters
Potential problems with anaesthetic in cattle
dorsal recumbency
oesophageal opening is submerged by rumen content → regurgitation/reflux → aspiration pneumonia (foreign body or bacteria) → disease progression = dead in 24-48 hrs
fermentation gas accumulate + cannot eructate → bloat
increased pressure on diaphragm = decreased tidal volume + increase risk of regurgitation and aspiration
decreased lung space + inspiration = hypoventilation due to increased CO2 + hypoxaemia
ischaemic myopthy and nerve injury
increased body weight in recumbency, non-expandable muscle facia can lead to ischemia + muscle swelling → myopathy and nerve injury
not as prone to hypertension as horses
salivation
huge volumes of fluid can pool in pharynx and mouth → risk of aspiration and depletes circulating plasma volume
cattle = 50L / 24hours
sheep = 8-16L / 24hours
Ways to prevent common GA problems in cattle
good clinical exam
fasting
will reduce volume of rumen and slow fermentation
list risk if they do regurgitate
Cattle: withhold food for 24-48 hrs and water for 12-24 hrs
Sheep/Goat: withhold food 12-18 hrs and water for 8-12 hrs
Neonates: do NOT withhold food or water (risk of hypoglycaemic and hypovolaemic)
intubation
use palpation of endotracheal tube into trachea
inflate cuff rapidly to avoid aspiration
hard to intubate = use Drinkwater gag, thread stomach tube through tracheal tube, intubate, slide out then inflate cuff
Cattle: don’t laryngospasm
Sheep, goats, alpacas: prone to laryngospasms
occiput elevation (poll)
elevate occiput/poll to discourage passive reflux and encourage any regurgitated material to drain
padding and positions
soft surface and padding between limbs
pull lower leg forward
minimise duration
ensure good blood pressure throughout
left lateral recumbency is better (more pressure onto rumen to prevent distending)
Premeds, Induction and Maintenance drugs during cattle anaesthetic
intramuscular = dart gun
intravenous = jugular catheter, tail vein or auricular vein
cattle = jugular, 10-14 G, be aware of carotid artery
small ruminants = jugular or cephalic, 20-18 G
remember cattle are food animals so need to have short half lives and not damage muscles too much
Premedicant and Sedation
Xylazine
most common, cattle are extremely sensitive (1/10th horse)
IV or IM = onset is 5-20 mins, lasts 35-40 mins
reversible with alpha 2 agonist (atipamezole)
SE = bradycardia, no swallow reflex, uterine contraction, reduced uterine blood flow (bad if calf), inhibit thermoreg
Alpha 2 Agonists
can cause hypnosis and recumbency
Acepromazine
Benzodiazepines = Diazepam, midazolam, zolasepam
not for standing sedation in adult ruminants → ataxia
Opioids
Induction
restrain in crush with rope if needed
10-14 G catheter in jugular vein
IV xylazine bolus → sternal recumbency (release from crush)
follow up with ketamine ± midazolam or diazepam
or follow up with thiopentone
intubate trachea, inflate cuff
intubate oesophagus + pass bore stomach tube
Maintenance
inhalation + O2 is ideal
IV if procedure is less than 45 mins but must give O2 as well
Monitory and recovery after GA in cattle
Monitoring
physical movement, jaw chewing, ear movement, response to stimuli
deep = eye will be ventral or even central if very deep
use HR, pulse pressure, MM colour, CRT
direct blood pressure by catheterising auricular artery or doppler
ECG for cardiac dysrhythmias
Recovery
sternal recumbency as soon as possible to allow rumen gas to escape
may regurgitate so always leave ET tube in with cuff inflated
only extubate (with cuff inflated still) when strong swallows
can reverse xylazine to help
Analgesia
NSAIDS = meloxicam, ketoprofen
Opioids = butorphanol, morphine, methadone
Alpha 2 agonists = short term only
Local = lidocaine and bupivacaine (take care if food producing)
Types of local anaesthesia and procedures used for cattle
Local options = lidocaine, bupivcaine
Benefits = surgery is whilst standing so safer but needs restraint
Complications = toxicity, infection or neuronal injury
Uses =
blocks for dehorning
blocks for teats or udder
inverted L block
Low or caudal epidural
paravertebral block, petersen block, retrobulbar block
auriculopalpebral
Key general considerations for paediatric vs geriatric under GA
Paediatric | Geriatric |
|
|
Both Predisposed to Hypoxaemia:
respiratory fatigue - may need intermittent ventilation
atelectasis (lung collapse)
Hypoxaemia
Assisting Paediatric and Geriatrics under GA
lots of preoxygenation to increase O2 reserve
prepare a ventilator + good size breathing bag
use a monometer to measure this
close monitoring with pulse oximetry (SPO2) and capnography
Paediatric | Geriatric |
|
|
Key paediatric considerations under GA and how to manage
Consideration | Management / Prevention | |
CVS (Heart) |
|
|
Liver (Hepatic) |
|
|
Renal (Kidney) |
|
|
CNS |
|
|
Thermoreg |
|
|
Key geriatric considerations under GA and how to manage
Consideration | Management / Prevention | |
CVS (Heart) |
|
|
Liver (Hepatic) |
|
|
Renal (Kidney) |
|
|
CNS |
|
|
Thermoreg |
|
|
Induction, Maintenance and analgesia drugs used in paediatric / geriatric
Premeds
IV = low stress and low anxiety
Paediatric = not required or low dose opioid
Geriatric = short acting + reversible = opioid ± benzodiazepine or ACP
Acepromazine = sedate (no analgesia), not reversible, may cause vasodilation, hypotension, hypothermia, liver metabolism
Midazolam or Diazepam (co-induction) = centrally acting muscle relaxant, no cardiovascular SE, can be unpredictable
Opioids = pure mu agonist (methadone) = may cause bradycardia, hypoventilation
Induction
pre-oxygenate
titrate slowly
ideally alfaxalone or propofol (short half life + non cumulative)
avoid ketamine and thiopentone
Maintenance
Inhalation may cause vasodilation but minimal metabolism
Ideal = IV isoflurane
ensure balanced / multimodal
Analgesia
CRI or incremental dose intra /post operatively
ideally opioids (morphine and fentanyl) or ketamine
regional anaesthesia, local and nerve blocks
be careful with toxicity
Anatomy primary + secondary changes in brachycephalic patient
Aim = leave hospital alive (morality rate is 2.5% vs normal is 0.5%)
Primary Changes = Brachycephalic Airway Obstructive Syndrome (BOAS)
stenotic nares
elongated soft palate
large tongue
abnormal nasopharyngeal tubinates
hypoplastic trachea → diagnose on radiograph (ideal larger than 0.16)
= increased airway resistance and negative pressure
Secondary Changes
excessive pharyngeal tissue
mucosal inflammation and oedema
laryngeal saccule eversion
tonsil eversion
arytenoid cartilage collapse
bronchial collapse
pulmonary oedema
gastro-oesophageal reflux
Comorbidities
oesophageal, gastric and duodenal inflam → regurg + vomit
aspiration pneumonia
congenital cardiac conditions
Other
increased vagal tone → bradycardia
excessive skin → hard to intubate
prominent eyes → hard to restrain + ulcerations
Premed, Induction and Maintenance drugs for the brachycephalic patient under GA
Premedication / Sedation
if very stressed give IM or IV
if low HR, premed with atropine or glycopyrrolate
contraindicated with alpha 2 adrenergic agonist
give anticholinergic if increased vagal tone
low dose opioid (methadone) ± very low dose acepromazine
boxes do not give ace
dexmedetomidine ± opioid (minimal relaxation of pharyngeal muscles)
corticosteroid (dexmethasone) for airway surgery to decrease inflam/irritation
esomeprazole to decrease regurg and gastric upset
Induction
minimise change of obstruction and maintain blood oxygen
good airway assessment or rapid intubation + airway protection
preoxygenate then rapid induction IV
Use alfaxalone or propofol
Maintenance
TIVA and/or inhalant anaesthesia
Injectable = alfaxalone or propofol
Inhalants = isoflurane or sevoflurane
Local blocks (opioid bolus or infusion) = methadone, fentanyl, morphine
Supportive Care, Recovery for the brachycephalic patient
Parameters
decreased PaO2
increased PaCO2 and PCV
often increased ASA status and BCS
Supportive Care
Pre-oxygenate to avoid obstructions = decreased stress + pain
catheter before premed to decrease stress
anticholinergic (atropine or glycopyrrolate) if already low HR
fluids = Hartmans 6ml/kg/hr
mannitol pharyngeal swabs = decrease swelling via osmosis
be ready to reintubate
Recovery
respiratory distress and obstruction common
pharyngeal oedema
regurgitation → aspiration pneumonia
always be ready to reintubate ± tracheostomy
leave ET tube in as long as possible until they reject OR use intranasal O2
death
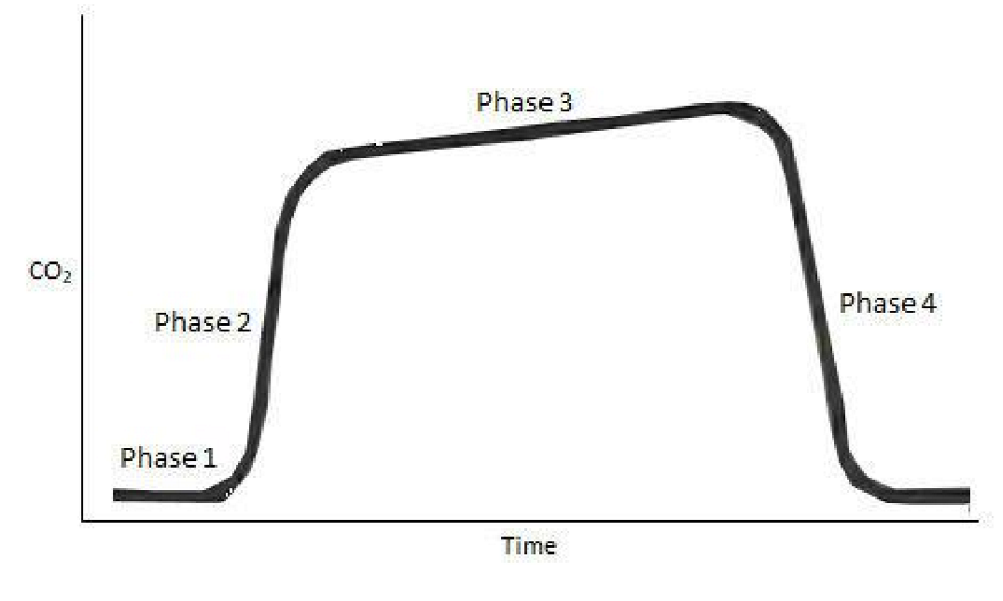
Capnography
measures ventilation by the the expired CO2 / end titdal CO2
either side-stream or main stream
confirms airway confirmation and indicates hypercapnia or respiratory acidosis
Each wave:
Inspiratory baseline - assess inspired Co2 and indicate breathing
Start of expiration (anatomical dead space)
Plateau (alveola gas)
Inspiration
Electrocardiogram (ECG)
Wave measures the electrical function of the heart to identify cardiac arrhythmias
can have electrical activity without mechanical activity
each heart beat should have P, QRS and T wave
leads 1 and 2 cranial to heart, then one caudal to heart “smoke over fire” (white is right, black is left, red is other)
read on lead 2 (closest to heart, left = black)