NEW CONTENT FOR FINAL!!!
1/78
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
79 Terms
skeletal muscles
muscles attached to bone + voluntary movement
cardiac muscles
muscles attached to heart + involuntary movement
smooth muscles
muscles on the walls of hollow visceral organs + involuntary movement
sarcomeres
filaments that are arranged into orderly parallel stacks + generates more force
how are sarcomeres visible
as bands in skeletal and cardiac muscles only
muscle fiber
each really big muscle cell
made up of myofibrils that are divided into sarcomere
how do muscles create movement
by contraction or shortening muscles
how is muscle contraction done?
by having filaments with the molecules actin and myosin slide on each other, shortening the
length of the muscle cells (sarcomeres).
Parts of the sarcomere
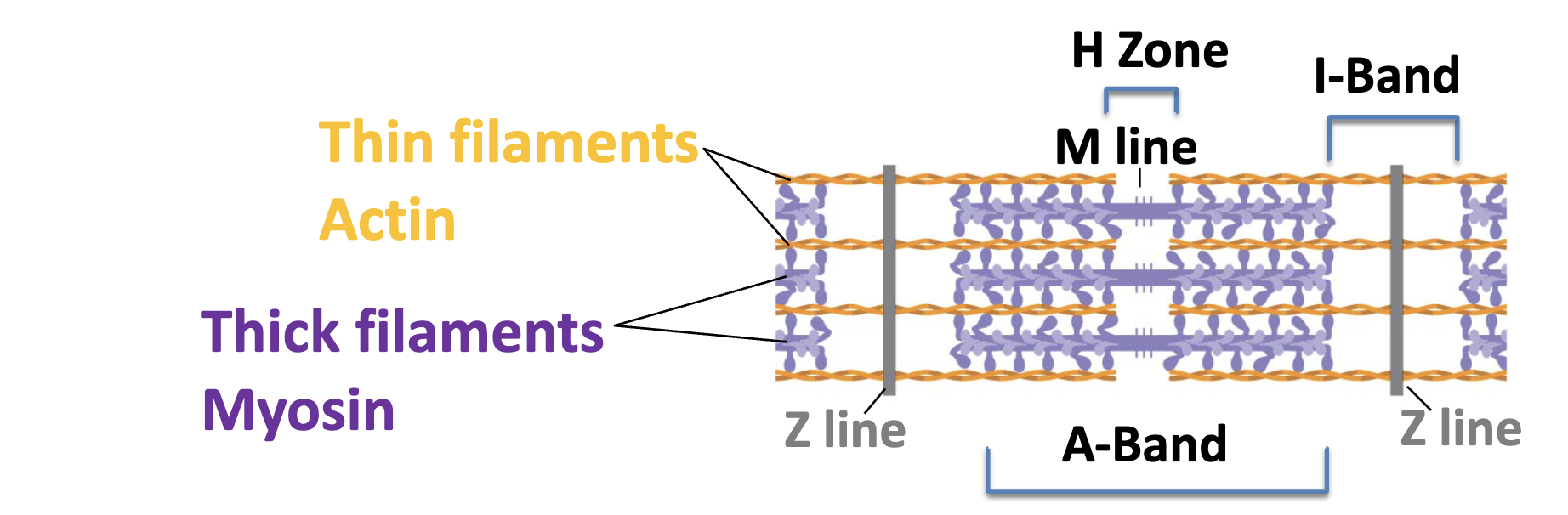
Sliding filament model
During contraction, the thick and thin filaments slide together lengthwise
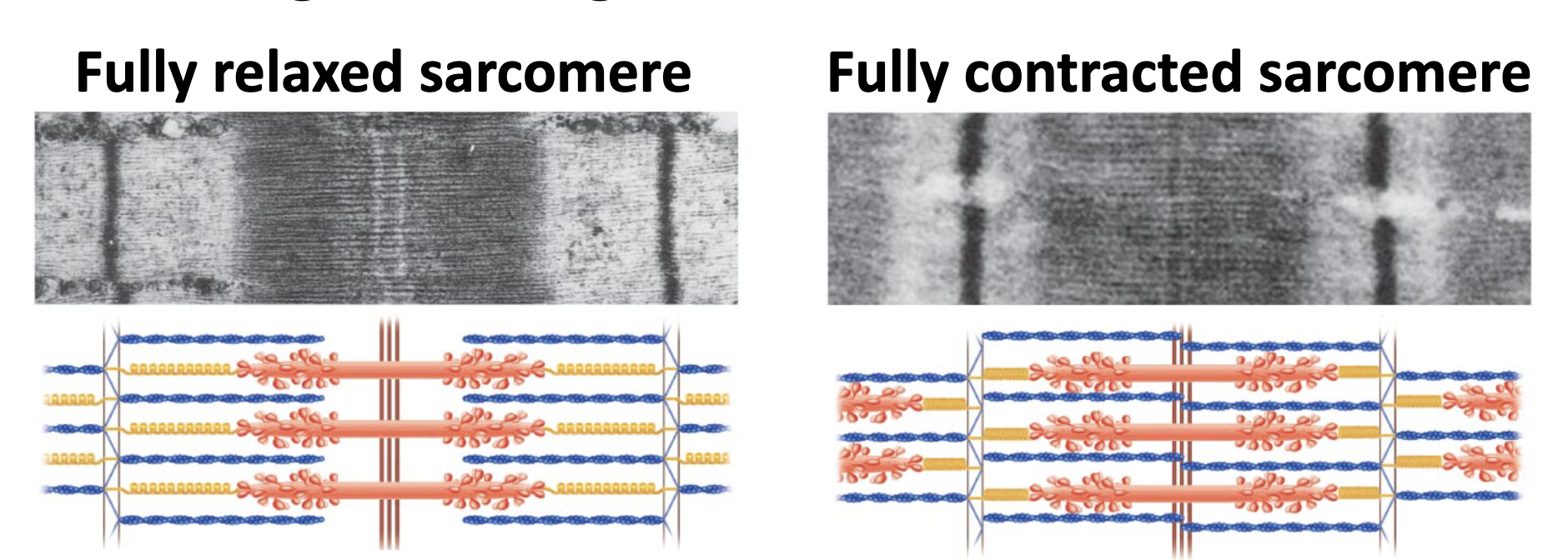
what are the steps of Skeletal Muscle Fiber Contraction
1) Neuron has AP, activates neuromuscular junction
2) Muscle has AP, signal propagates to rest of muscle
3) Muscle contracts using cross bridge cycling
neuromuscular junction
the neuron/muscle synapse that functions very similarly to a neuron/neuron synapse
acetylcholine
the nuerotransmitter in skeletal muscles
Acetylcholine release at the nueromuscular junction
1) An action potential in the neuron opens voltage-gated calcium channels.
2) Calcium influx into the neuron causes the release of acetylcholine.
3) Acetylcholine binds to its receptor on the muscle fiber, opening a channel that lets in
sodium.
4) Acetylcholine is broken down in the cleft
When the sodium channels open in the muscle, what happens?
Sodium enters the muscle, effect is depolarizing
what type of receptor is acetylcholine
an acetylcholine-gated cation channel receptor
Signal propagation: From nueromuscular junction to the sarcomere
1) If enough acetylcholine receptors are activated, there will be a muscle action potential.
2) AP travels down the membrane and throughout the fiber in structures called T-tubules.
sarcoplasmic reticulum (SR)
A membrane-bound organelle that uses Ca2+ pumps to accumulate Ca2+ inside itself
how does the sliding filament model work on a molecular level?
the sliding occurs because myosin heads in thick filaments repeatedly grab onto actin in thin filaments and pull
Filaments without calcium
Myosin heads cannot bind to actin because tropomyosin is in the way.
how do changes in actin, troponin, tropomyosin, myosin, or calcium would influence
muscle contraction.
Ca2+ binds to troponin. Troponin moves tropomyosin off the binding sites so the actin and myosin can form cross bridges
Steps of cross bridge cycling
1) Cross bridges form.
2) Working (power) stroke: myosin head turns and pulls thin filament to contract.
3) ATP binding to the myosin detaches the cross bridges.
4) Energy from ATP hydrolysis moves myosin back into the initial state.
What will happen to muscle contraction when the nerve stops firing?
Contraction ends gradually as Ca2+ is pumped back
In rigor mortis, why is the muscle stiff?
There is a lot of calcium but no ATP, so the cross-bridges cannot be released
Contrasting muscle contraction in death and life
LIVING - you always have some ATP around, but the calcium is sequestered in SR
DEATH - membranes break down and calcium is around, but there is no more ATP being made.
how do you get to the sympathetic and parasympathetic nervous systems
through the peripheral nervous system → autonomic nervous syste,
parasympathetic division
“Rest and digest”
Promotes maintenance functions and conserves body energy
Promotes low blood pressure, low heartrate, and digestion
sympathetic division
“fight or flight
Mobilizes the body during activity
Promotes high blood pressure, high heartrate, and faster and deeper breathing, but inhibits digestion
adrenal gland and stress
When stressed, the adrenal gland both…
Releases cortisol + is stimulated by the sympathetic division to release epinephrine and norepinephrine.
what are the Two parallel stress pathways
nueral and endocrine
Effects of epinephrine and norepinephrine on the body
they are nuerotransmitters + hormones
Increased heart rate and vasoconstriction → increased blood pressure
Stimulate liver to break down glycogen → Increase blood sugar
cortisol effects on body
acne + getting sick easily
Epinephrine/ norepinephrine effects on body
increased heart rate, stomachaches, headaches
both cortisol and Epinephrine/ norepinephrine effects on body
inability to sleep + fatigue + tiredness
innate behaviors
Instinctive, based on genetics, evolved through natural selection, inborn, unaffected by environment, low variation in population
ex) newborn instincts
learned behaviors
based on experience, trial and error, high variation in population
ex) social skills, tricks in pets
optogenetics
Making neurons express channels that are light-sensitive
How to force a neuron to fire with light
through optogenetics
“fire together, wire together”
mental experiences or actions that occur simultaneously and repeatedly strengthen the connections between neurons, making those pathways stronger and more automatic
how do you test the idea of ‘fire together, wire together’
1) Force neurons to “fire together” that normally wouldn’t.
2) Check to see if they “wired together” to produce a false, composite (mixed) memory that is
associated with the neurons you forced to fire together
hippocampus
nuerons in the hippocampus, the stimulus they respond to best is a particular location,
thing, or event
Different Sets of Neurons Fire in Different Locations or Situations!
what is learning?
a change in synapse
involves both strengthening and weakening synapses
what can a change in synapse be?
Change in number of neurons
Change in number of synapses
Change at the synapses location themselves
strengthening a synapse
when an AP in the presynaptic neuron will cause a bigger response in the postsynaptic neuron
weakening a synapse
when an AP in the presynaptic neuron will cause a smaller response in the postsynaptic neuron
synaptic plasticity
he ability of neural connections (synapses) to strengthen or weaken over time in response to increased or decreased activity
what are the two main ways the immune system protects yourself
Innate Immune System + Adaptive Immune System
main process for immune system
Recognize a pathogen → Activate and mobilize forces to defend against it → Attack it → Control and end the attack
innate Immune System
rapid response, found in all plants/animals, general, only a few signals
adaptive immune system
acquired, slow response, very specific signals, only in vertebraes
what does Innate Immune Protection look like
inflammation, sweat, mucus, tears
cytokines
molecules that signal to other cells to do something
what are the cells of the innate immune system
macrophages, nuetrophils, dendritic cells, eosinophils
macrophages
Engulfs and destroys (phagocytoses) pathogens, dead cells, debris. Secretes cytokines.
talks to the adaptive immune system
dendritic cells
Talks to adaptive immune system
nuetrophils
Phagocytoses pathogens, first responder. Secretes cytokines
eosinophils
Attacks larger pathogens like parasites and cancer cells
which of these consequences will occur if an animal doesn’t make macrophages?
Bacteria will grow more + the adaptive immune system won’t be activated as quickly
pathogens
can be distinguished from the body’s own cells because they: cause damage + have certain characteristics
PAMPs (pathogen-associated molecular patterns)
types of signals that are shared by classes of pathogens
detected by TLR (toll like receptor)
Toll-like receptor (TLR)
a receptor found in all cells of the innate immune system so they can recognize any PAMP
antigen
a substance that triggers the body's immune system to produce antibodies because it can be detected by antibodies in B cells and T-cell receptors in T cells
antibody
made by cells of the adaptive immune system
detect and bind to specific antigens
adaptive immune system steps
A pathogen enters the body
the immune system recognizes a specific antigen (unique marker)
B and T cells that match that antigen are activated
B cells make antibodies, T cells attack infected cells
Some cells become memory cells to remember and fight it in the future
Two arms of the adaptive immune system
Cell-mediated arm + Humoral arm
humoral arm
B-cells divide to make plasma cells, which secrete antibodies
cell mediated arm
Cytotoxic T-cells kill infected body cells (& cancer cells)
why do you need two arms in the adaptive immune system
Sometimes, pathogens are in blood/body fluids, and antibodies can reach them.
– Humoral arm
Sometimes, pathogens are inside body cells (viruses and some bacteria), and you just need to kill those infected body cells
– cell mediated arm
memory B cells and memory T cells
react to the antigens of the pathogen directly and quickly
– So quickly you usually don’t feel sick.
– Memory can last for decades
Traditional Vaccines
Receive an antigen from a source that won’t make you sick
antigen sources: Dead microbe, Weakened microbe, Part of a microbe
mRNA vaccines
inside the dendritic cell, mRNA codes for pathogen protein
antigen source: mRNA from pathogen
If someone has an autoimmune disorder, would you treat it by strengthening or weakening their immune system?
Weakening their immune system!!
People with autoimmune disorders have an immune system attacking their own bodies. If
the immune system is strengthened, it will attack the body better, which is bad
autoimmunity
when the immune system mistakenly attacks the body's own healthy cells, tissues, or organs
self tolerance + how to develop it
Self-tolerance is the ability of the adaptive immune system to recognize the body’s own cells as “self” and avoid attacking them.
develops through central tolerance (self-reactive T and B cells are eliminated during development) and peripheral tolerance (remaining self-reactive cells are inactivated or suppressed, e.g., by regulatory T cells).
muscle weakness
muscle weakness is often caused by issues in nerves.
does acetlycholine enter muscle ?
NO! Acetylcholine is secreted into the synaptic cleft and binds to a receptor on the muscle. It never actually enters the muscle.
Troponin = tropomyosin ?? True or false
FALSE
Troponin and tropomyosin are both in the thin
filaments. Tropomyosin binds to actin, preventing it
from binding to myosin. Troponin detects calcium;
when calcium is present, it moves tropomyosin off
the myosin binding sites
what is ATP required for?
ATP is required for the cross bridge to break.
antibiotics
Antibiotics are drugs given to kill or stop the growth of bacteria.