
Looks like no one added any tags here yet for you.
Lice/Cheyletiellosis
Sarcoptic mange
Harvest mites (chiggers)
Otoacariasis (tick or mite)
Demodicosis (demodex)
Malassezia
Flea Allergy Dermatitis (FAD)
Atopic Dermatitis (atopy) & Food allergy
Glucocorticoids: topical
betamethasone
Glucocorticoids: systemic: short acting
prednisone, prednisolone
ATB: G-
enrofloxacin, Marbofloxacin (fluoroquinolone), Gentamicin
ATB: G+
clavamox/synulox (Amoxicillin-Clavulanic Acid), Penicillin G, Clindamycin
Antifungal/antibact topical: (shampoo)
w/ chlorhexidine
Antifungal: topical
Ketoconazole
Antifungal: systemic
Itraconazole, fluconazole, ketaconazole
Cytokine disruptor
Apoquel
Cytokine neutraliser
Lokivetmab (cytopoint)
Decrease cytokine production: systemic
Atopica (cyclosporine)
Decrease cytokine production: topical
Tacrolimus
Antihistamine
benedryl, hypoxyzine, cyproheptadine
Antipruritic shampoo
colloidal oatmeal
Skin supplement
Omega 3 & 6 FA
Flea control: spot on
fipronil, selamectin
Flea control: shampoo
permethrin (toxic to cats), pyrethrin
Flea control: systemic
afoxolaner, fluralaner
Antiviral: herpes
Acyclovir, cidovir
drug contraindicated for ulcers
corticosteroids → speeds protease activity → worsens condition & slows healing
Glucocorticoids: systemic: long acting
dexamethasone
when is CCS contraindicated?
when their immunosuppressive affect is undesirable or causes risk → NSAIDs can usually be used instead because they do not have an immunosuppressive affect
Feline miliary dermatitis
Feline eosinophilic complex
Broad spectrum ATB (well used ones)
Doxycycline, Tetracycline, Sulfonamides
Eardrum rupture: what to know/do
DO NOT APPLY DRUGS IN CASE OF A RUPTURED EARDRUM!! Give oral ATB or oral antifungals.
Clean ear w/ warm saline only. Continue till drains clear or if drains w/ blood. Eardrum should heal on its own in 4 weeks.
If unsure because too much debris & c/n visualise tympanic membrane → rinse w/ warm saline till you can visualise structure & proceed w/ appropriate method.
Drying agents: ears
acid w/ or w/o alcohol → yeast & bacteria
salicylic acid → keratolytic agent, antimicrobial
EDTA → antimicrobial, antibiofilm
Topical antiseptic: ears
acetic acid, chlorhexidine (pseudomonas resistant)
ATB: Pseudomonas
Tobramycin
What is used to clean ears?
Carbamine peroxide (tympanic membrane intact) or warm saline (ruptured tympanic membrane/unsure of its state)
Skin adnexa
Sweat glands, sebaceous glands, hair follicles, nails.
Diseases of skin adnexa (3x)
Sebaceous adenitis – Inflammation of sebaceous glands, w/ overproduction of sebum. Genetic. Tx: anti-seborrheic shampoo, cyclosporine, ATB.
Supracaudal gland hyperplasia – overproduction of sebum & androgen, causes a bald spot on the tail of male dogs.
Claw infections:
Infectious: secondary bacteria, fungi. Others: endocrine disorders, allergy, auto-immune disorders, neoplasia
Tx: Treat underlying cause, remove all loose claws. long-term systemic ATB. Anti-fungal (itraconazole), chlorhexidine soak
Common Skin Tumours in Dogs
Lipoma: Benign fatty tumour; soft, movable lumps.
Sebaceous Gland Tumour: Benign tumour from sebaceous glands; firm nodules.
Mast Cell Tumour (MCT): Malignant; raised, firm masses that may itch.
Fibrosarcoma: Malignant tumour of fibrous tissue; irregular, infiltrative masses.
Histiocytoma: Benign, round tumour; often red and can regress.
Transmissible Venereal Tumour (TVT): Contagious malignant tumour; ulcerated masses on genitals.
Adenoma/Adenocarcinoma: Benign/malignant glandular tumours; varies in appearance.
Common Skin Tumours in Cats
Squamous Cell Carcinoma (SCC): Malignant; non-healing ulcers, often on head/ears.
Basal Cell Tumour: Typically benign; firm, round nodules.
Mast Cell Tumour: Can be benign or malignant; firm, raised lumps.
Fibrosarcoma: Malignant; infiltrative masses, often post-vaccination.
Lymphoma: Malignant; plaques or nodules on skin.
Feline Eosinophilic Granuloma Complex: Red, itchy lesions; related to allergies.
Tumour staging
TNM
which is CCS is preferred for cats?
Prednisolone
Immunosuppressants
Azathioprine (Imuran), Cyclosporine (Atopica, Neoral), Chlorambucil (Leukeran), Cyclophosphamide
Adverse effect of prolonged steroid use:
Gastric ulcers
H2 blockers: eg + what it does
Cimetidine - blocking H2 receptors on the stomach lining, reducing the secretion of gastric acid.
Synthetic thyroid drug:
levothyroxine (L-Thyroxine)
Anti-thyroid drugs:
Methimazole/thiamazole (Felimazole) or carbimazole (Vidalta)
Drug for: Bradycardia
atropine, glycopyrrolate
Drug for: Tachycardia
Propanolol, or. increase analgesia/anaesthesia
Drug for: Ventricular Arrhythmia
lidocaine, procainamide
Drug for: Hyperkalemia
0.9% saline, calcium gluconate
Drug for: Hypocalcemia
Calcium gluconate
Drug for: Hypoglycemia
Dextrose
Drug for: Bronchoconstriction
Terbutaline
Sedatives
Midozolam, acerpromizine, diazepam
Drug for: Cardiac Arrest
Adrenaline, atropine
Drug for: Pulmonary Arrest
Adrenaline, lignocaine (or can acupuncture GV-26 point aka nose septum)
Premedication/sedation:
medetomidine + acerpromizine + midozolam; medetomidine + butorphenol; medetomidine + butorphenol + diazepam
Induction agent: IV
Propofol (0.6 w/o premed, 0.3 w/ premed), Alfaxolone
Induction agent: gas
Isoflurane, sevoflurane
Injection anaesthesia: Barbiturates
Thiopental, pentobarbitol
Injection anaesthesia: Non-barbiturates
Propofol
Injection anaesthesia: Dissociative
Ketamine - provides analgesia & amnesia w/ retention of reflexes (laryngeal, ocular, pedal, pinnal)
Inhalation anaesthesia
Isoflurane, sevoflurane
Crystalloid fluids:
Ringer’s lactate (0.9% NaCl), KCl, Hypertonic Saline (7.2% NaCl)
Post-op Pain Meds:
Morphine, buprenorphine, fentanyl
Where is the physis? What is specific for it?
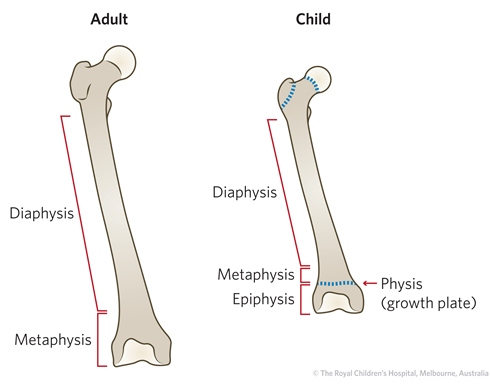
Between meta & epiphysis (growth plate). Present in young animals, not adults.
Salter Harris classification
Fracture classification
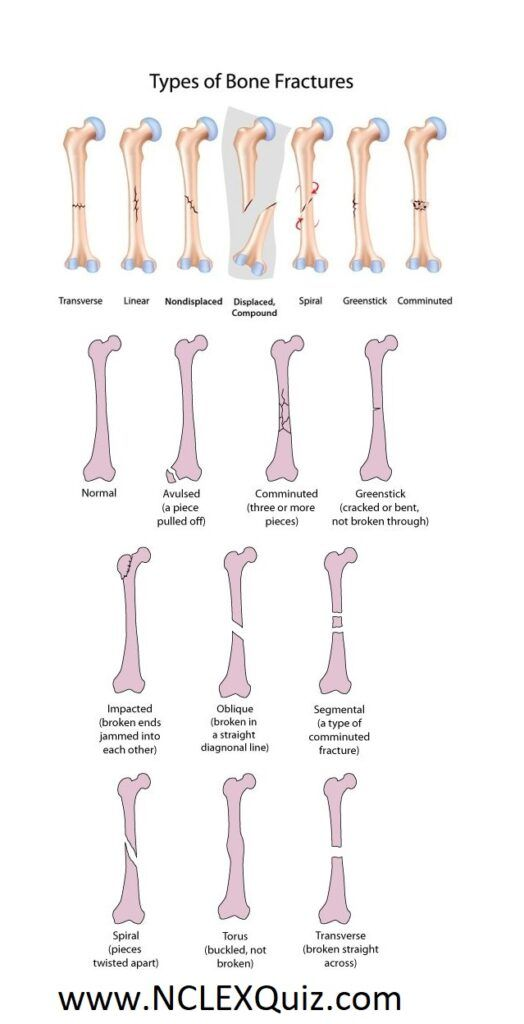
Types of Drawer tests:
Cranial & caudal
Caudal drawer test:
Proximal tibia moves caudally if rupture of CaCL
Cranial drawer test:
Proximal tibia moves cranially if rupture of CrCL
Patella Luxation Grading:
0-4
0: 0 degree;
1: 15 degrees;
2: 25 degrees;
3: till 60 degrees;
4: over 60 degrees
Hip Dysplasia Grading:
A-E;
A: normal (NA over 105), no OA (FHC: medial)
B: near normal (NA over 105), no OA, mild joint incongruency (FHC: medial or on)
C: Mild HD (NA btw 100-105), Mild OA, mild joint incongruency (FHC: on border or immediately lateral)
D: Moderate HD (NA btw 90-100), OA, joint incongruency (FHC: lateral)
E: Severe HD (NA less than 90), severe OA w/ joint deformation, severe joint incongruency (FHC: very lateral)
Chondroprotectives:
Glucosamines, hyaluronic acids,
Screening of elbow dysplasia is done according to?
International Elbow Working Group (IEWG)
Elbow dysplasia grades:
0-3
Grade 0: Normal elbows. No OA or primary lesions.
Grade 1: Mild ED w/ osteophytes < 2mm. Sclerosis present.
Grade 2: Moderate OA w/ osteophytes 2-5mm
Grade 3: Severe OA w/ osteophytes > 5mm or obvious UAP, FCP, OCD
Diuretic:
increase fluid excretion (urinate): Furosemide
Anti-diuretic:
decrease fluid excretion: Desmopressin, ADH
Antiemetics:
Cerenia, Maropitant
Treat metabolic acidosis:
Sodium Bi-carbonate
Hypertension drug:
Ace-inhibitors
Hypotension drug:
fluids, dopamine
Gastric acid reducing drug:
Famotidine, cimetidine
Drug against uric acid in blood:
Allopurinol - for ammonium urate & gout
Anti Seizures drugs!
Diazepam (can give IV or per rectum in emergency / rarely occurring seizures.
Phenobarbital (for recurring seizures). Bromide (only dog).
Propofol – Will not stop seizure activity, but external manifestations.
Long term Tx: Keppra (Levetiracetam)
Sedative
Diazepam
Ototoxic drug:
Aminoglycoside ATB: streptomycin/neomycin & Macrolide ATB (Erthromycin)
Anti-tussive:
Hydrocodone, Codeine, Dextromethorphan,
Bronchodilators
Theophylline, Aminophylline
Core Dog Vacc:
CDV, CPV, CAV
Lepto & Rabies core if in endemic region
Core Cat Vacc:
FPV, FHV, FCV
FeLV & Rabies core if in endemic region
Eosinophilia
Parasites, allergies
Neutrophilia + Monocytosis
Start of infection + inflammation
Lymphocytosis
Long infection
Mydriatic
tropicamide (short acting), atropine (very long acting)
Drugs: ↓ production of aqueous humour
Non-specific Beta blockers (timolol), Carbonic anhydrase inhibitors (Acetazolamide)
Drugs: ↑ outflow of aqueous humour:
Prostaglandin analogues, Parasympathomimetics (cholinergics)
Drugs: ↓ production & ↑ outflow:
Hyperosmotics: Mannitol, Epinephrine/Dipivefrin, Brimonidine (alpha-2 agonist)