BGSU BIOL 3320 Lecture Exam 4- Urinary
1/122
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
123 Terms
filter, excrete, regulate, detoxify
functions of the kidneys
yes
do kidneys stimulate the production of red blood cells?
respiratory, integumentary, digestive, urinary
the four body systems that carry out excretion
metabolic waste
wastesubstance produced by the body
Blood urea nitrogen (BUN)
level of nitrogenous waste in blood
azotemia
-presence of urea or other nitrogenous elements in the blood
-elevated BUN
-May indicate renal insufficiency
uremia
excessive BUN
-presence of urinary waste in the blood
-syndrome of diarrhea ,vomiting, dyspnea, and cardiac arrhythmia stemming from the toxicity of nitrogenous waste
-Treatment is hemodialysis or organ transplant
retroperitoneal
pertaining to behind the peritoneum (membrane that lines the abdominal cavity)
retroperitoneal
pertaining to the kidneys position in the body: the kidneys are _______________
right kidney; right
the ______ is slightly lower due to the large ____ lobe of the liver
fibrous capsule
a transparent capsule that prevents infections in surrounding regions from spreading to the kidney
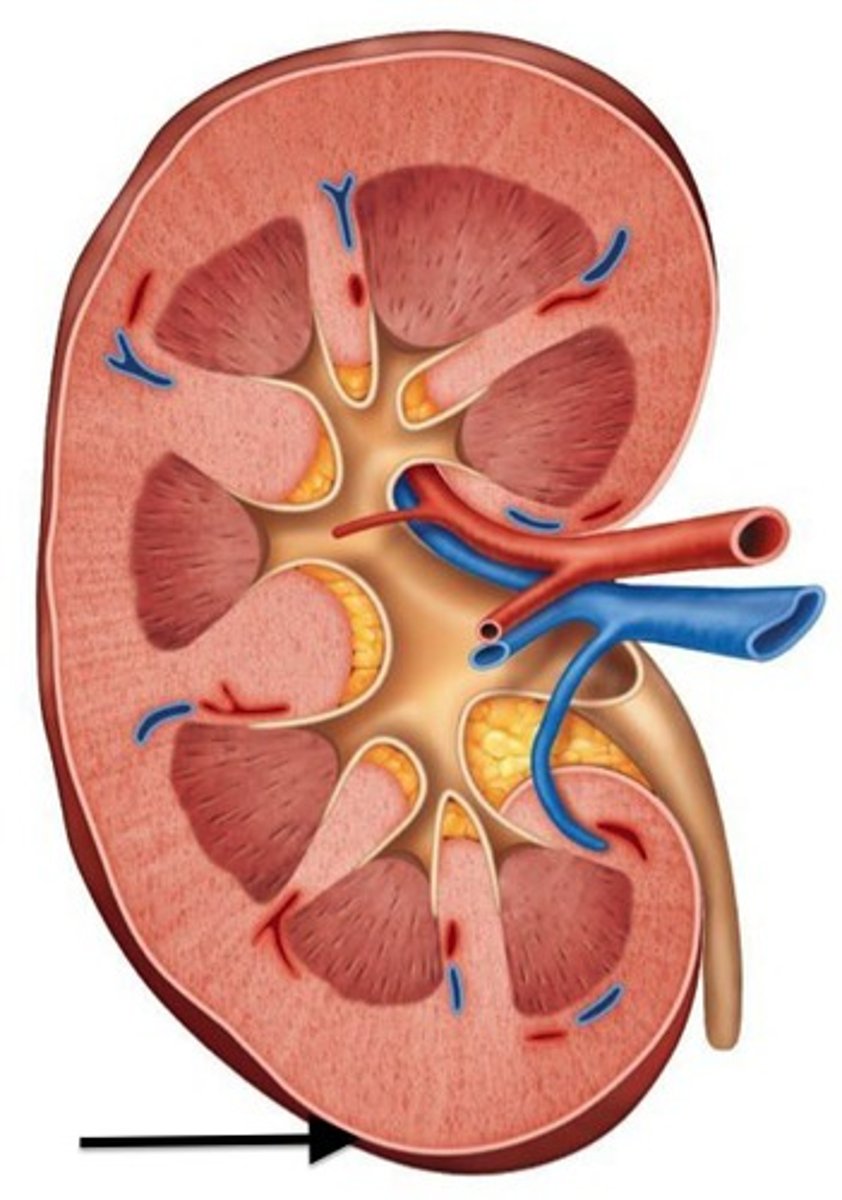
renal cortex
outer region of the kidney
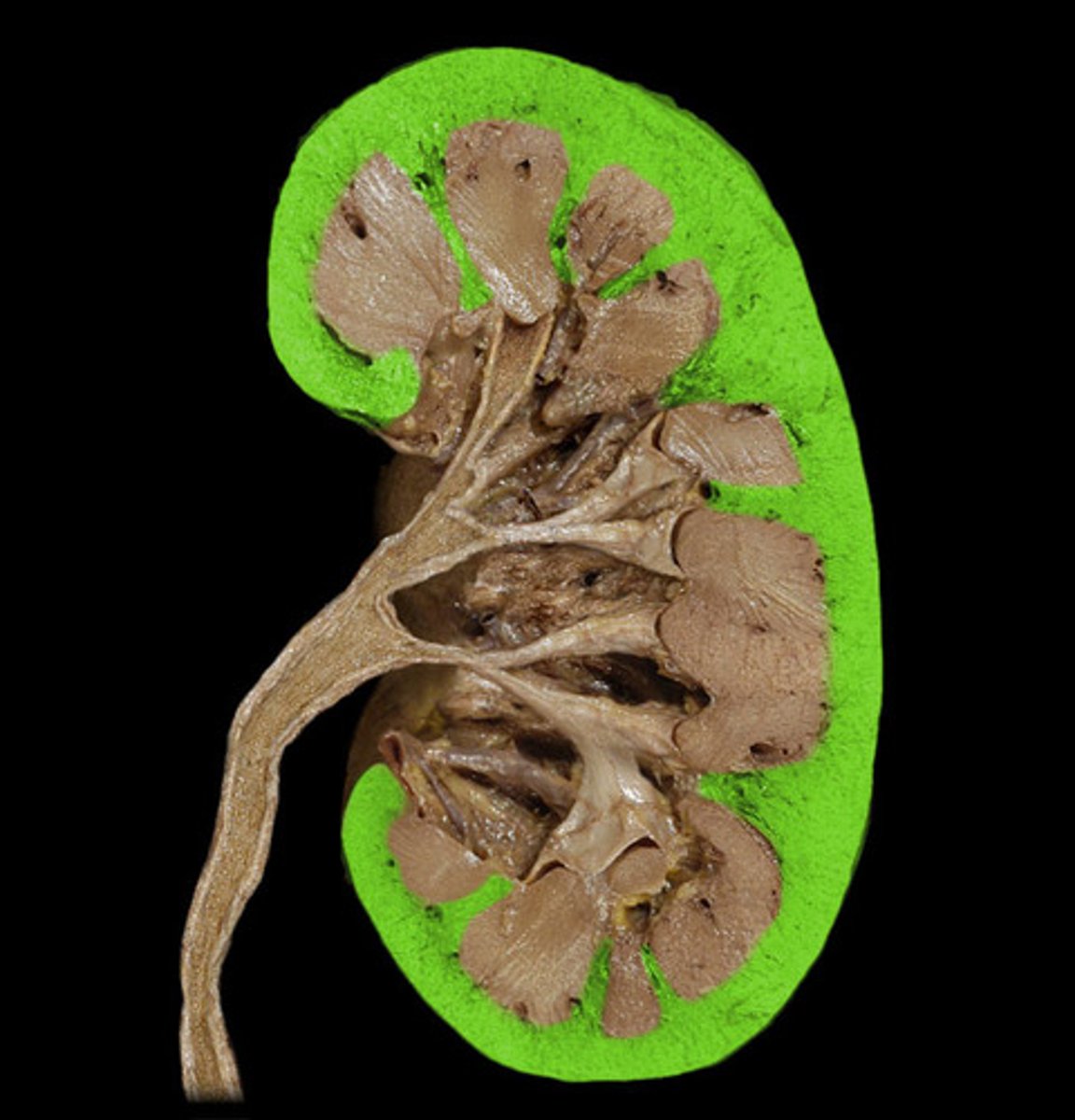
renal medulla
inner portion of the kidney
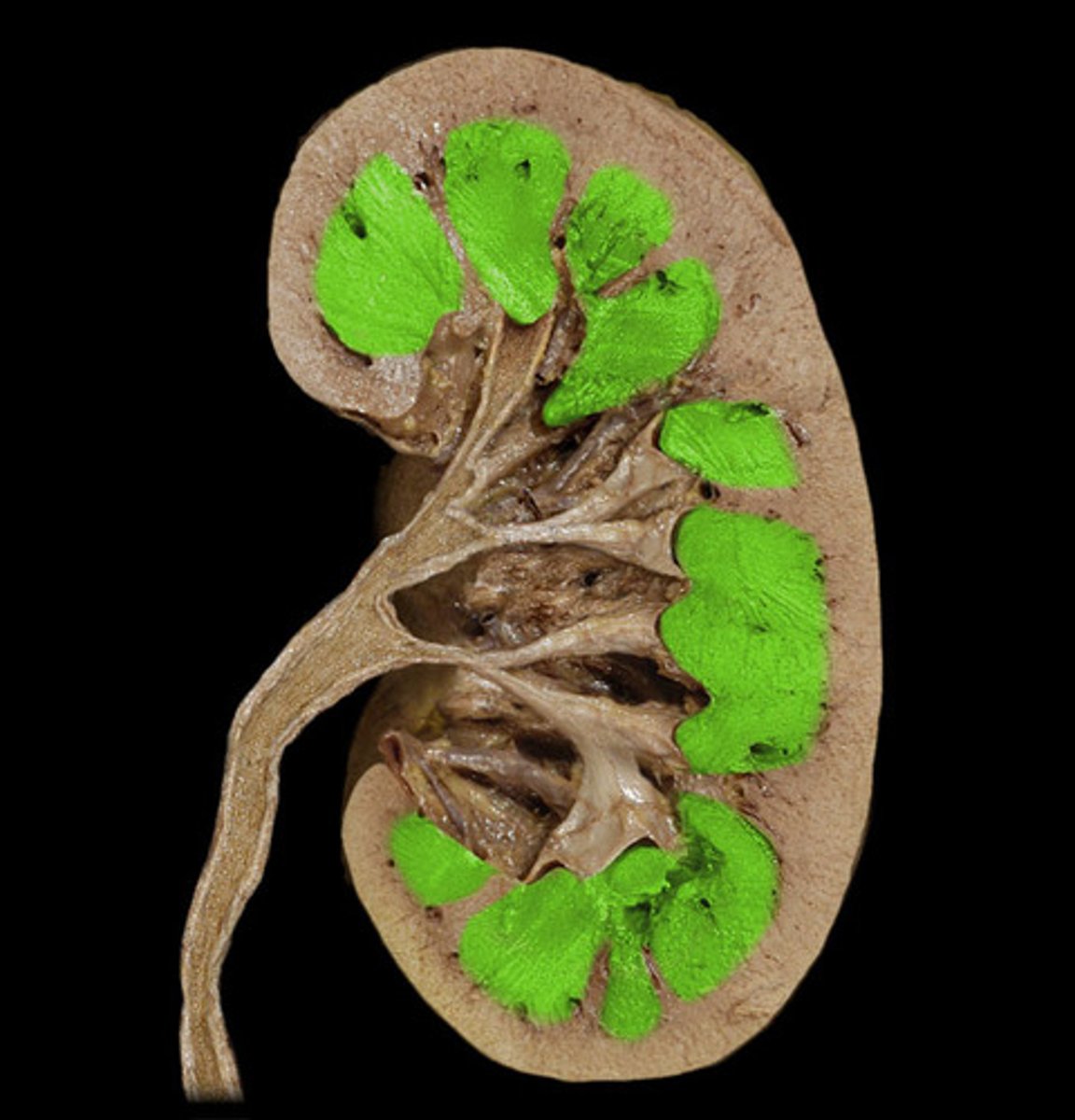
renal papilla
apex of renal pyramid
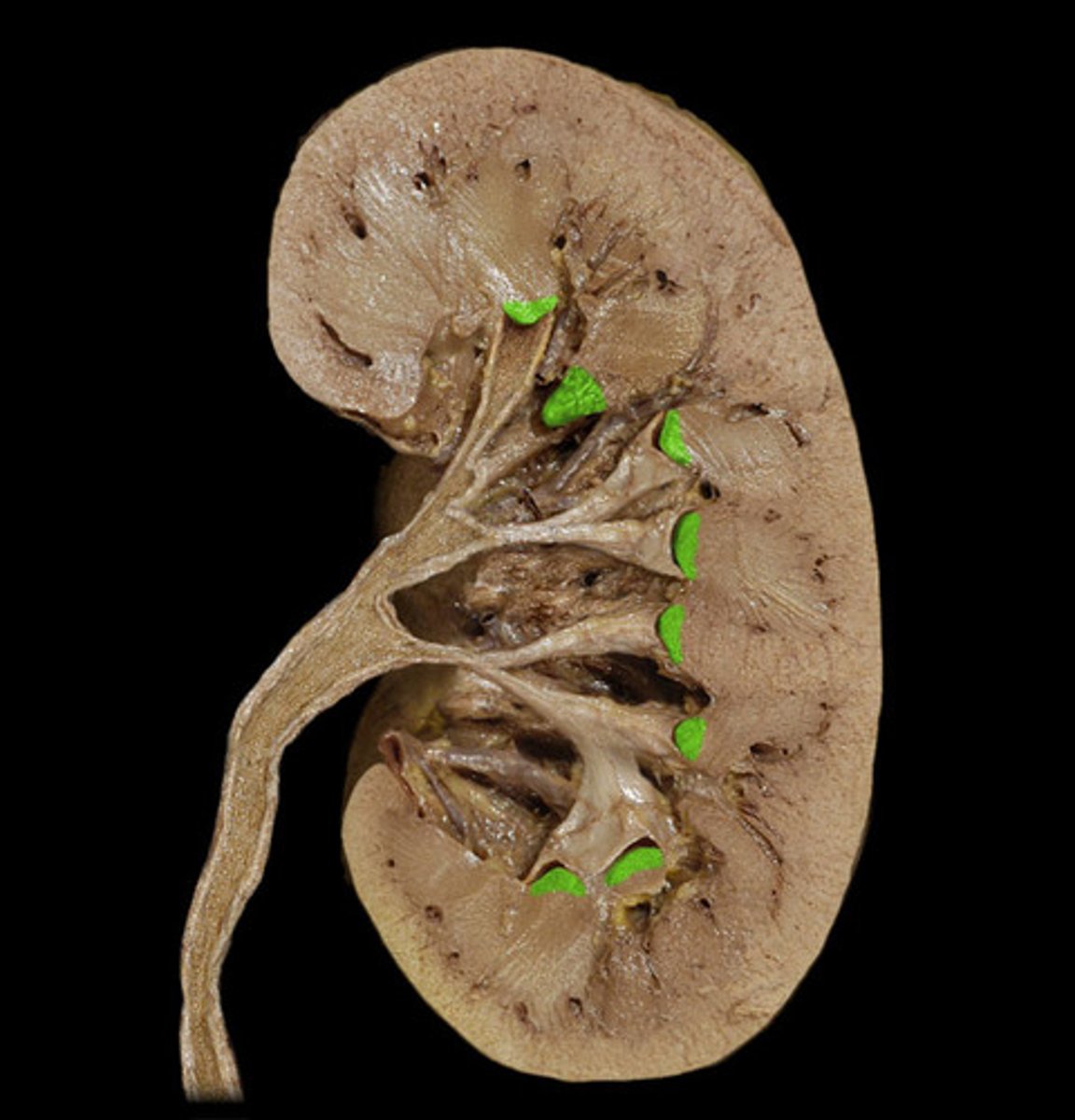
renal sinus
cavity that contains blood and lymphatic vessels, nerves, and urine-collecting structures
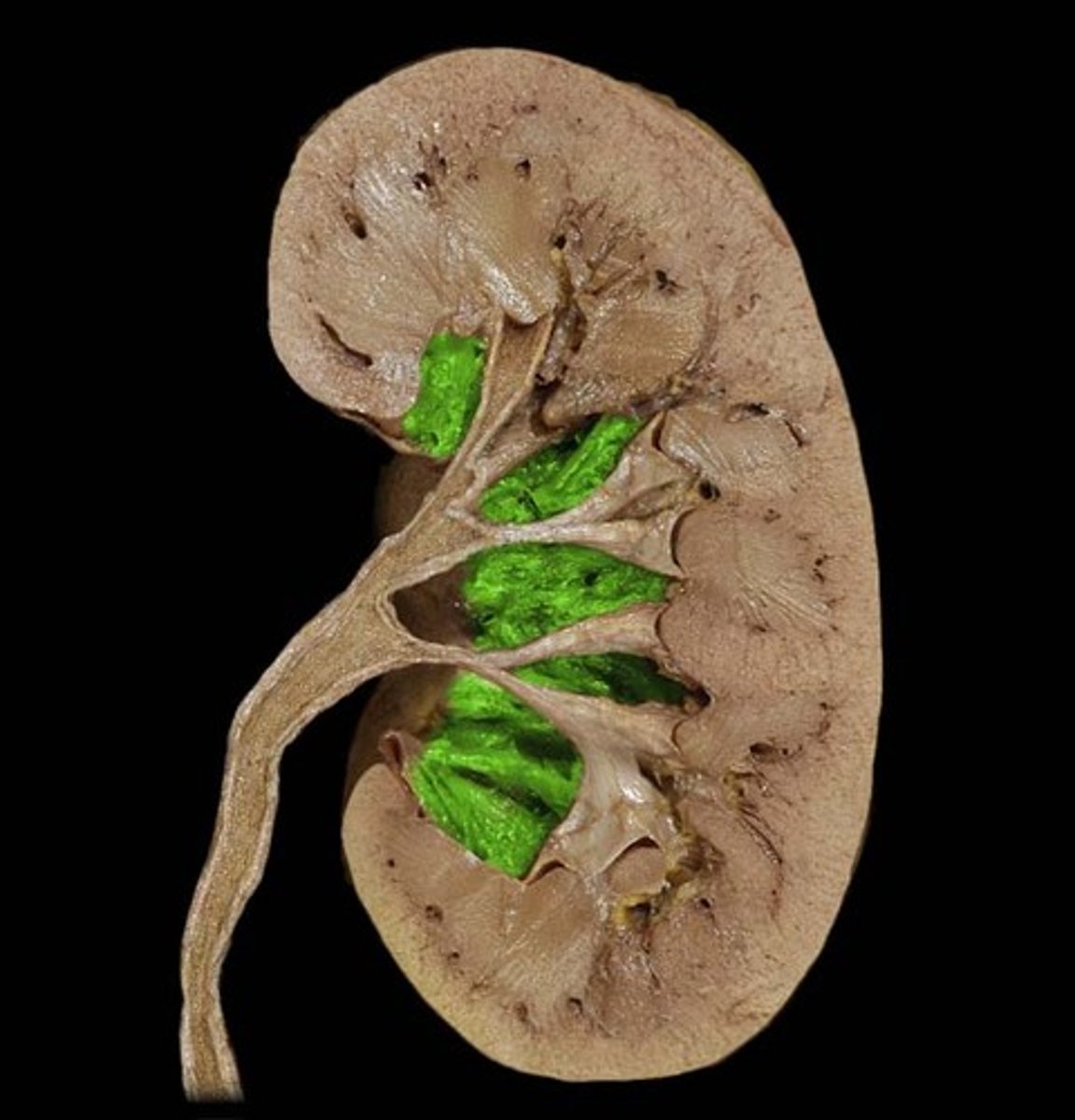
renal pelvis
funnel-shaped reservoir that collects the urine and passes it to the ureter
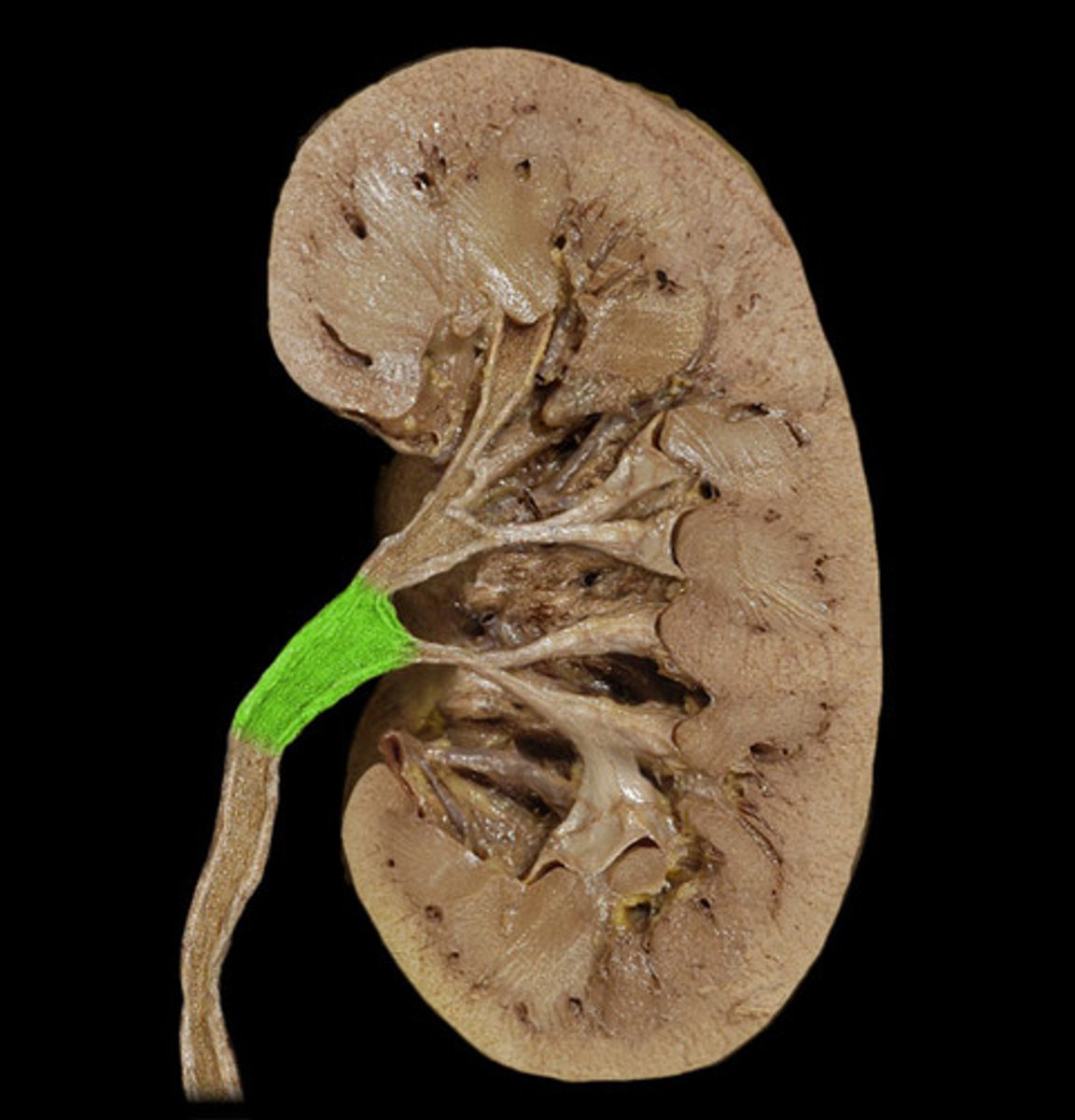
major calyx
The cavity formed by the convergence of several minor calyces, which drain urine from the minor calyxes into the renal pelvis
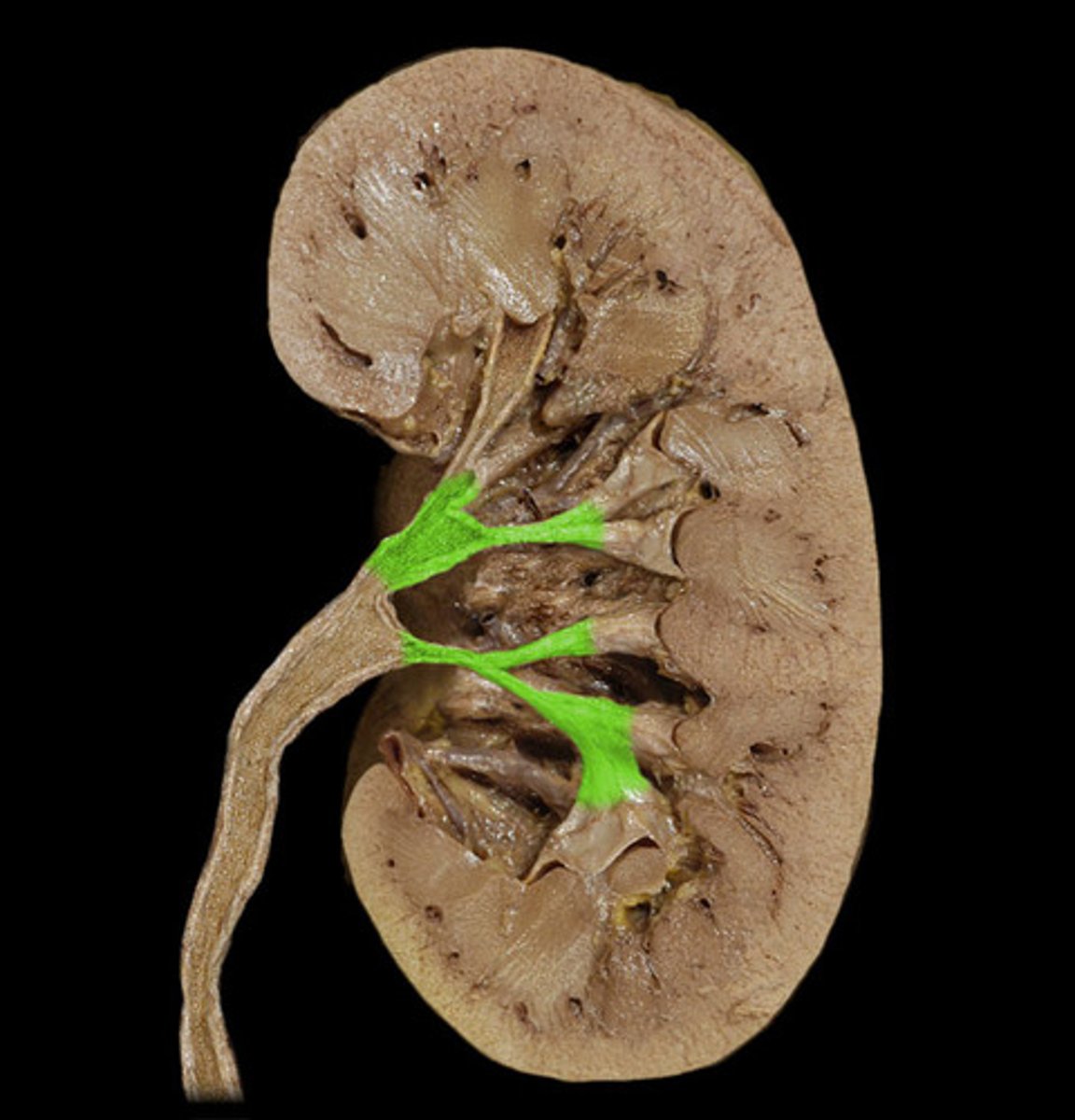
minor calyx
a cup-shaped extension of the pelvis that encircles the apex of a pyramid
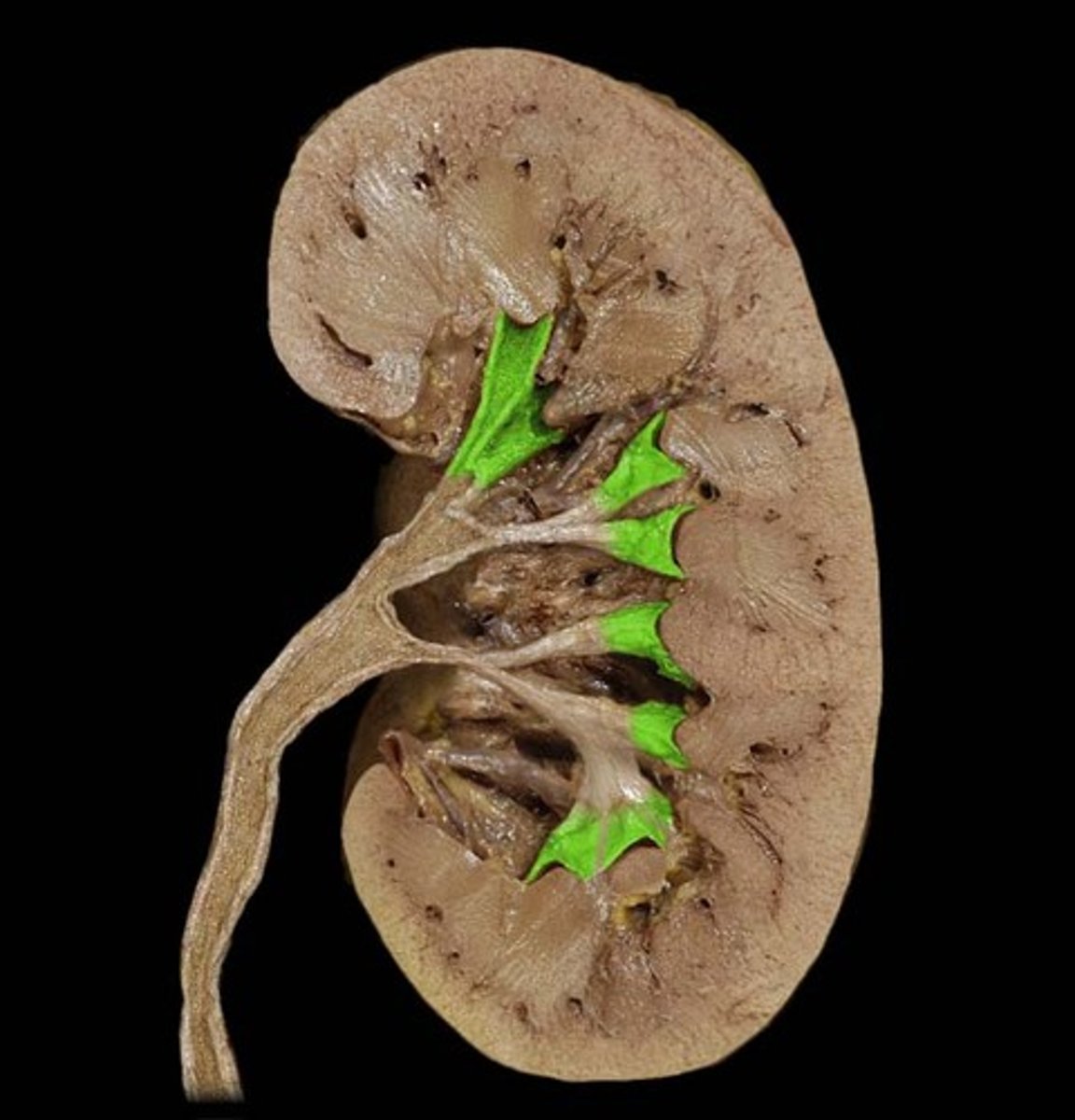
renal column
Inward extensions of the cortex tissue separating the renal pyramids.
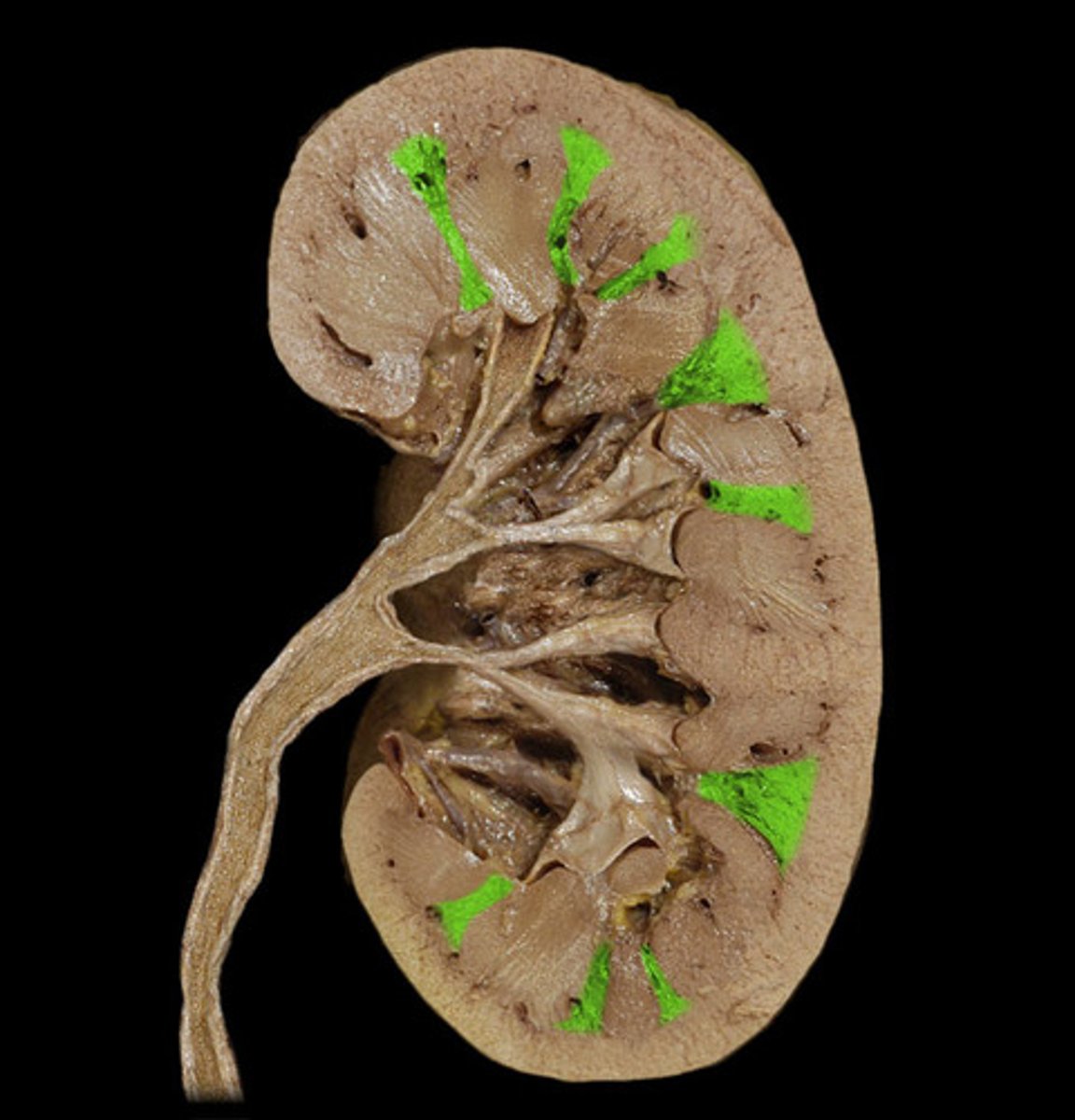
renal pyramid
triangular-shaped division of the medulla of the kidney
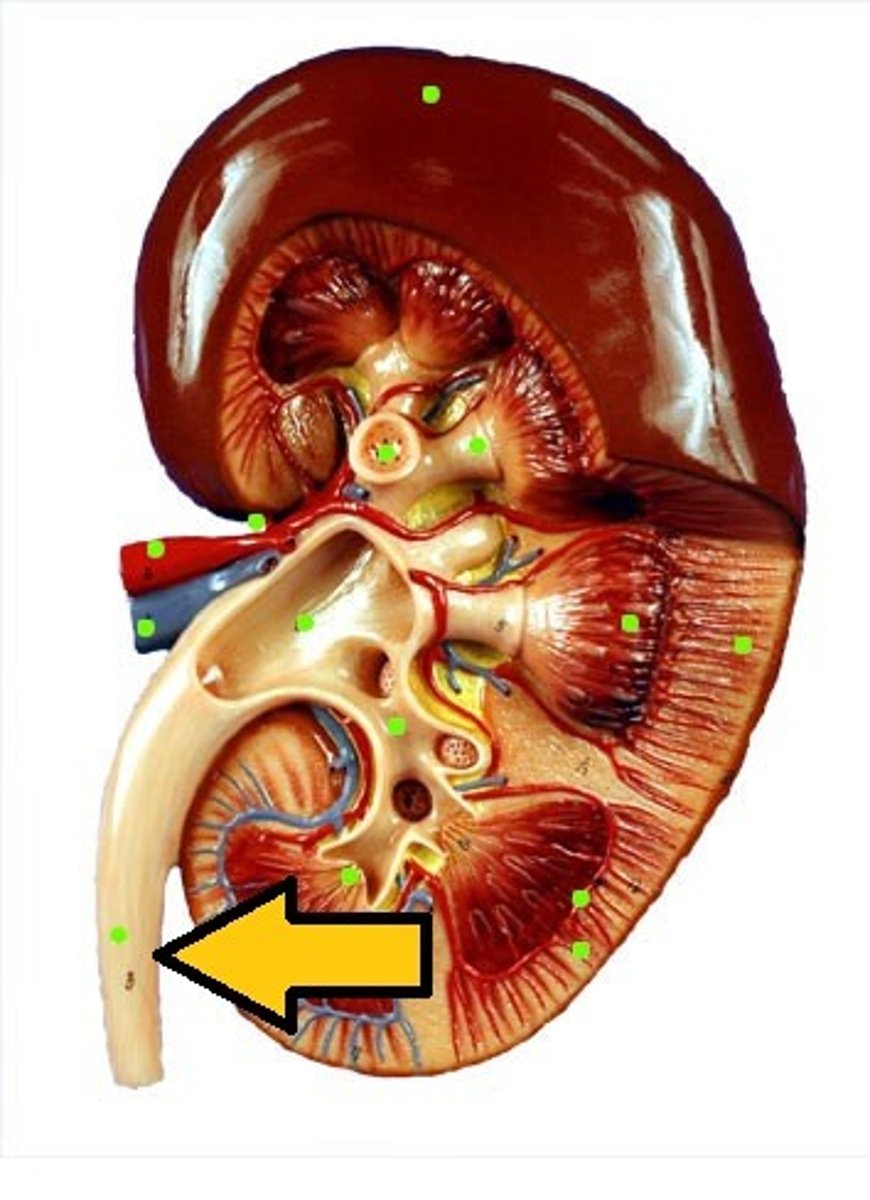
ureter
A duct leading from the kidney to the urinary bladder.
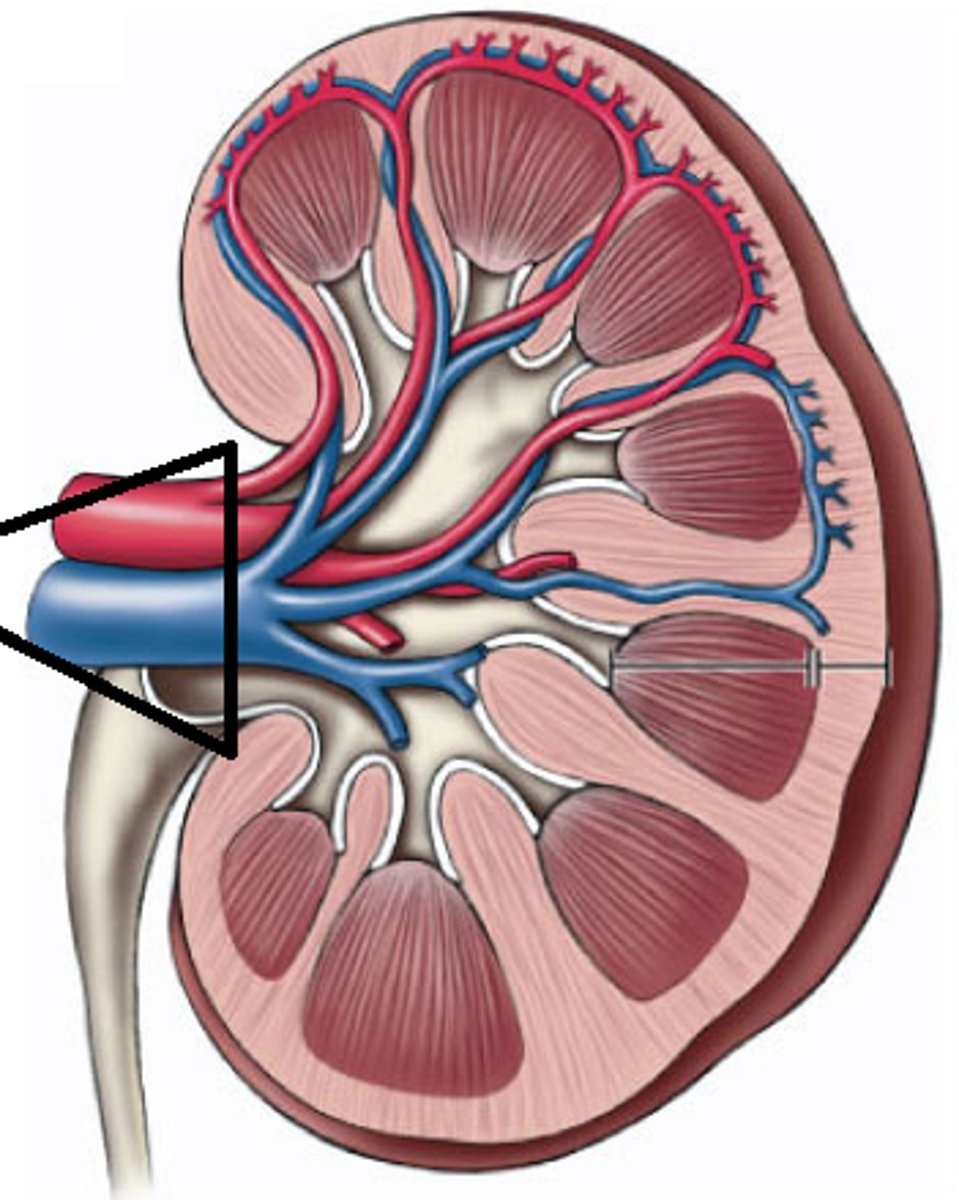
renal blood vessels
renal parenchyma
glandular tissue that forms urine, encircles renal sinus, two zones include the outer renal cortex and the inner renal medulla
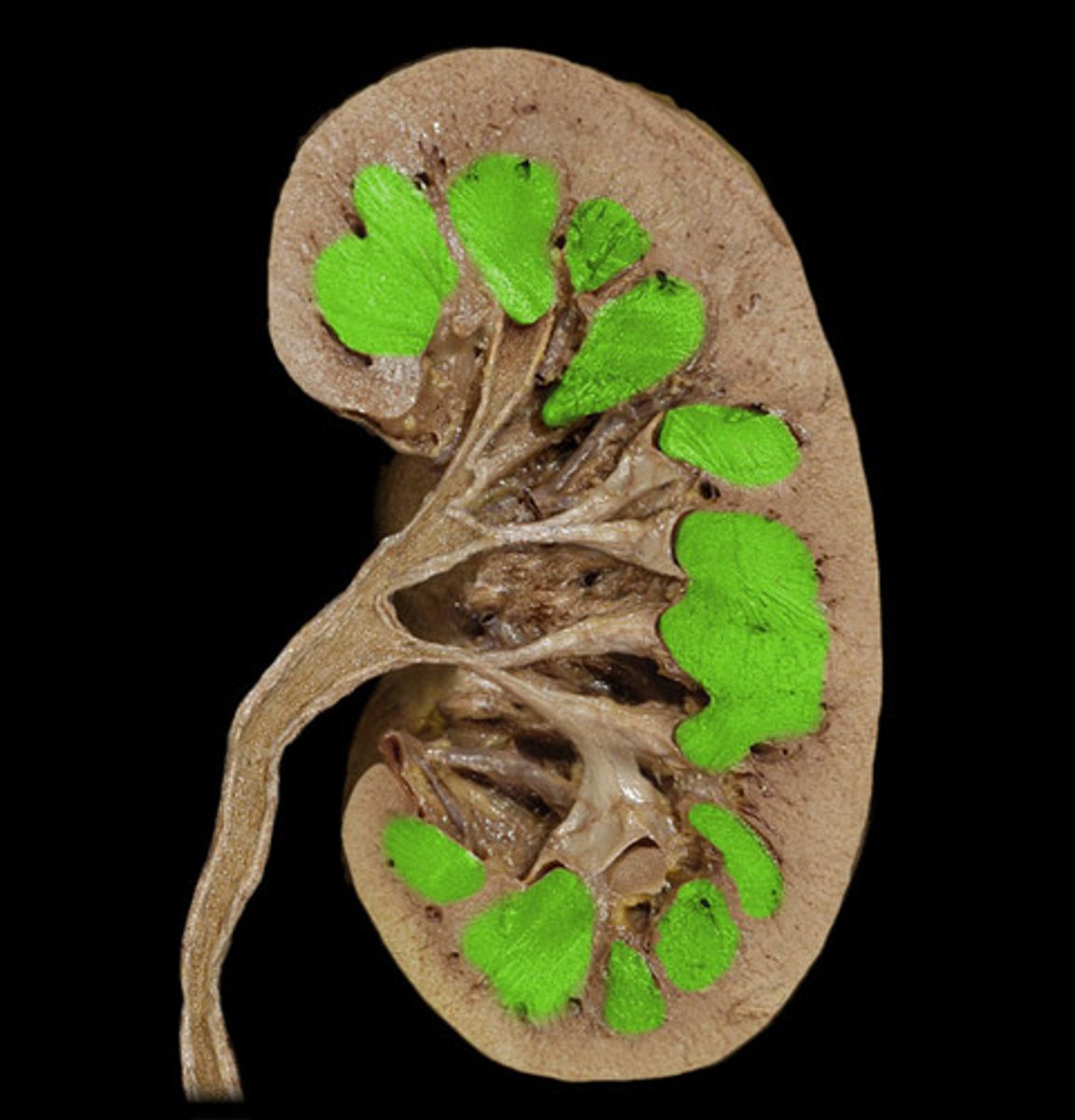
lobe of kidney
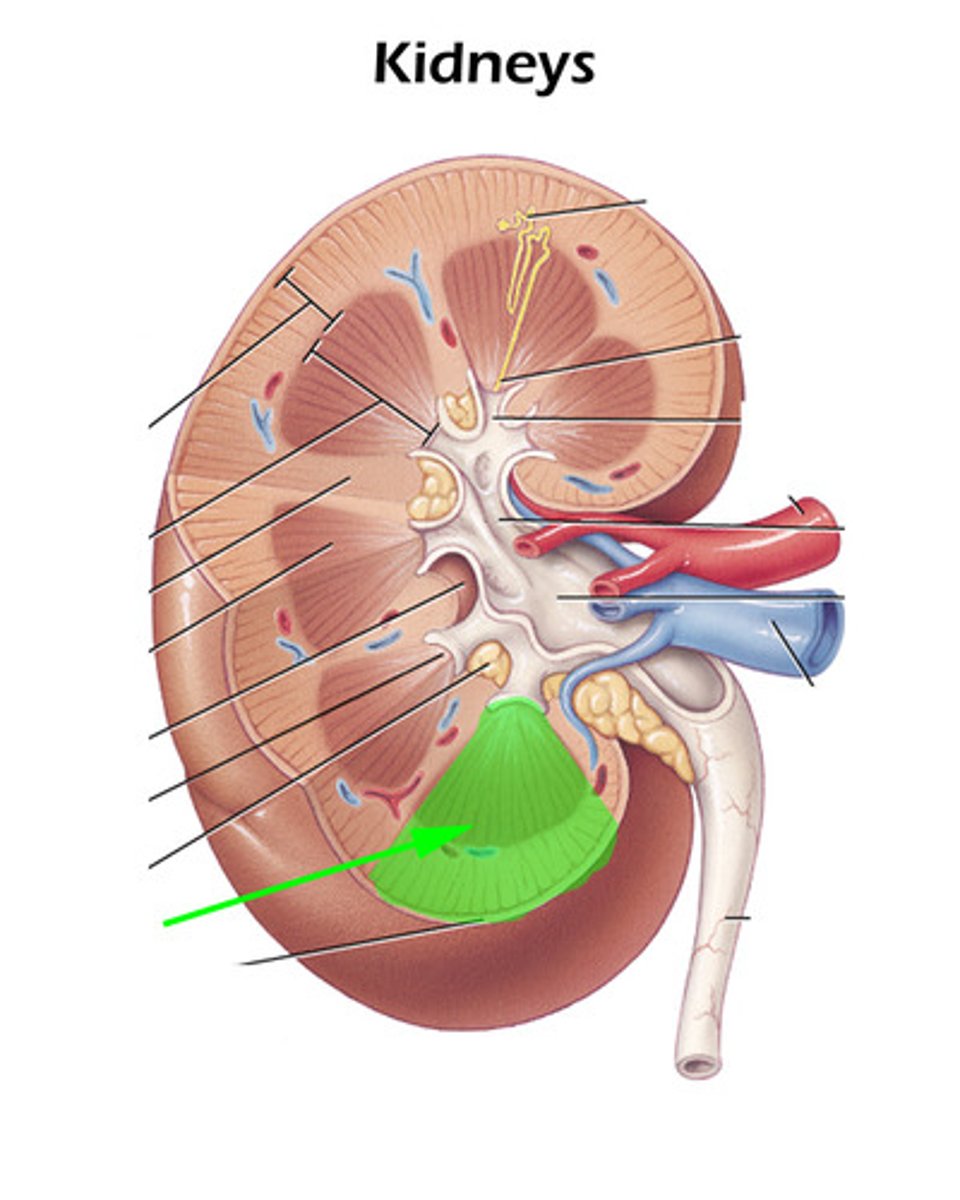
segmental arteries, interlobular arteries, arcuate arteries, cortical radiate arteries, afferent arterioles
oxygenated blood enters the kidney through the renal artery, list the path of oxygenated blood from there to the glomerulus
the glomerulus
the filtration of blood, plasma, and small solutes happens here
efferent arterioles, peritubular capillaries (most) OR vasa recta
after filtration in the glomerulus, the blood continues and leaves the glomerulus via these arterioles in order
cortical radiate vein, arcuate vein, interlobar vein
after exiting the glomerulus via the efferent arterioles and peritubular capillaries OR vasa recta, the deoxygenated blood eventually ends up in the renal vein, but first passes through these in order
Renal artery, Segmental artery , Interlobar artery, Arcuate artery, Cortical radiate artery, Afferent arteriole, Glomerulus, Efferent arteriole, Peritubular capillaries/vasa recta, Cortical radiate vein, Arcuate vein, Interlobar vein, Renal vein
Renal artery → Segmental artery → Interlobar artery → Arcuate artery → Cortical radiate artery → Afferent arteriole → Glomerulus → Efferent arteriole → Peritubular capillaries/vasa recta → Cortical radiate vein → Arcuate vein → Interlobar vein → Renal vein
try and retype this without looking! This is the path of blood circulation from the renal artery to the renal vein through the kidney.
nephron
functional unit of the kidney
collecting duct
a nephron does not include the __________
renal corpuscle and renal tubule
two major parts of a nephron
corpuscle; tubule
the renal ___________ filters the blood plasma and the renal ____________ tubule is a long coiled tube that converts filtrate to urine
glomerulus, glomerular capsule, proximal convoluted tubule, nephron loop, distal convoluted tubule
what is the path of filtrate, the fluid that derives from plasma that eventually becomes urine, through a nephron, then exits out the collecting duct
proximal convoluted tubule, nephron loop, distal convoluted tubule, collecting duct
what makes up the renal tubule
papillary ducts, minor calyx, major calyx, renal pelvis, ureter, bladder, urethra
after exiting a nephron through the collecting duct, filtrate or urine follows what path to exit the body
glomerulus
what are the capillaries inside the glomerular capsule
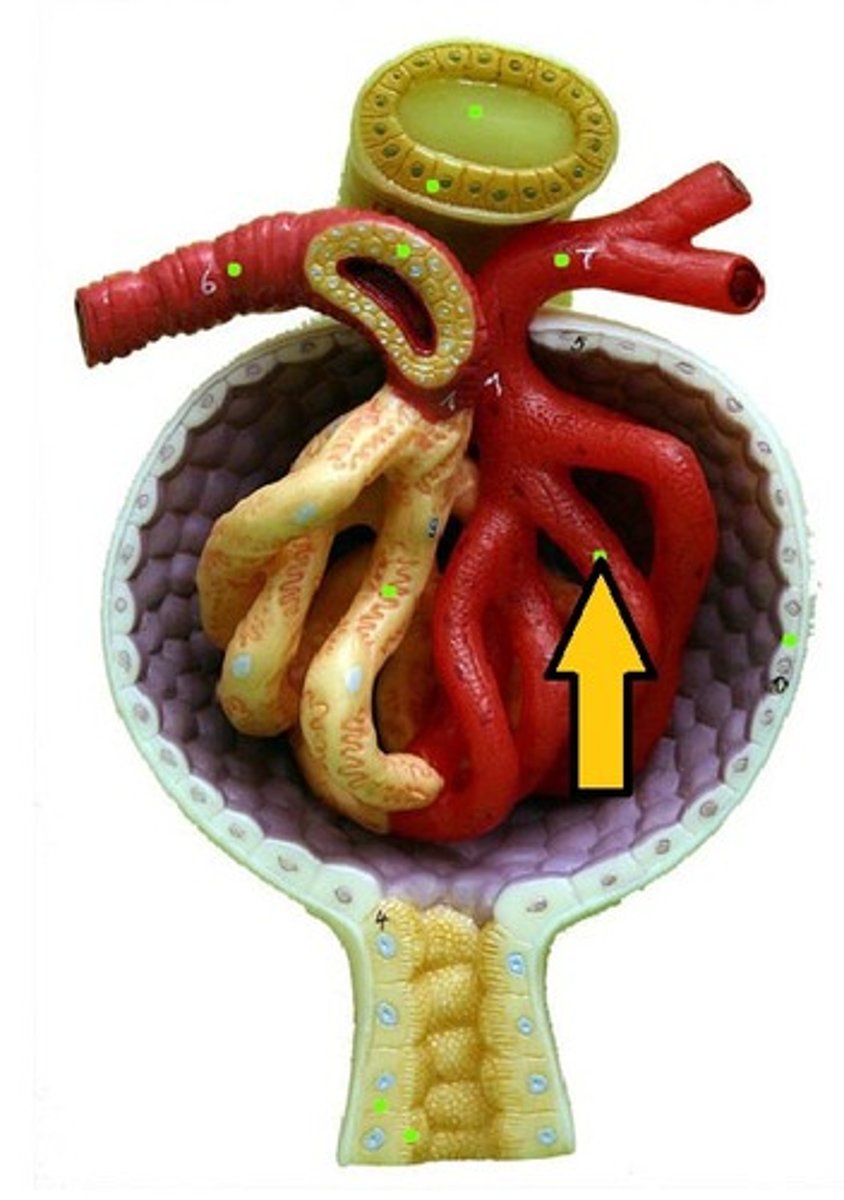
peritubular capillaries
what are the capillaries that surround the proximal and distal convoluted tubules
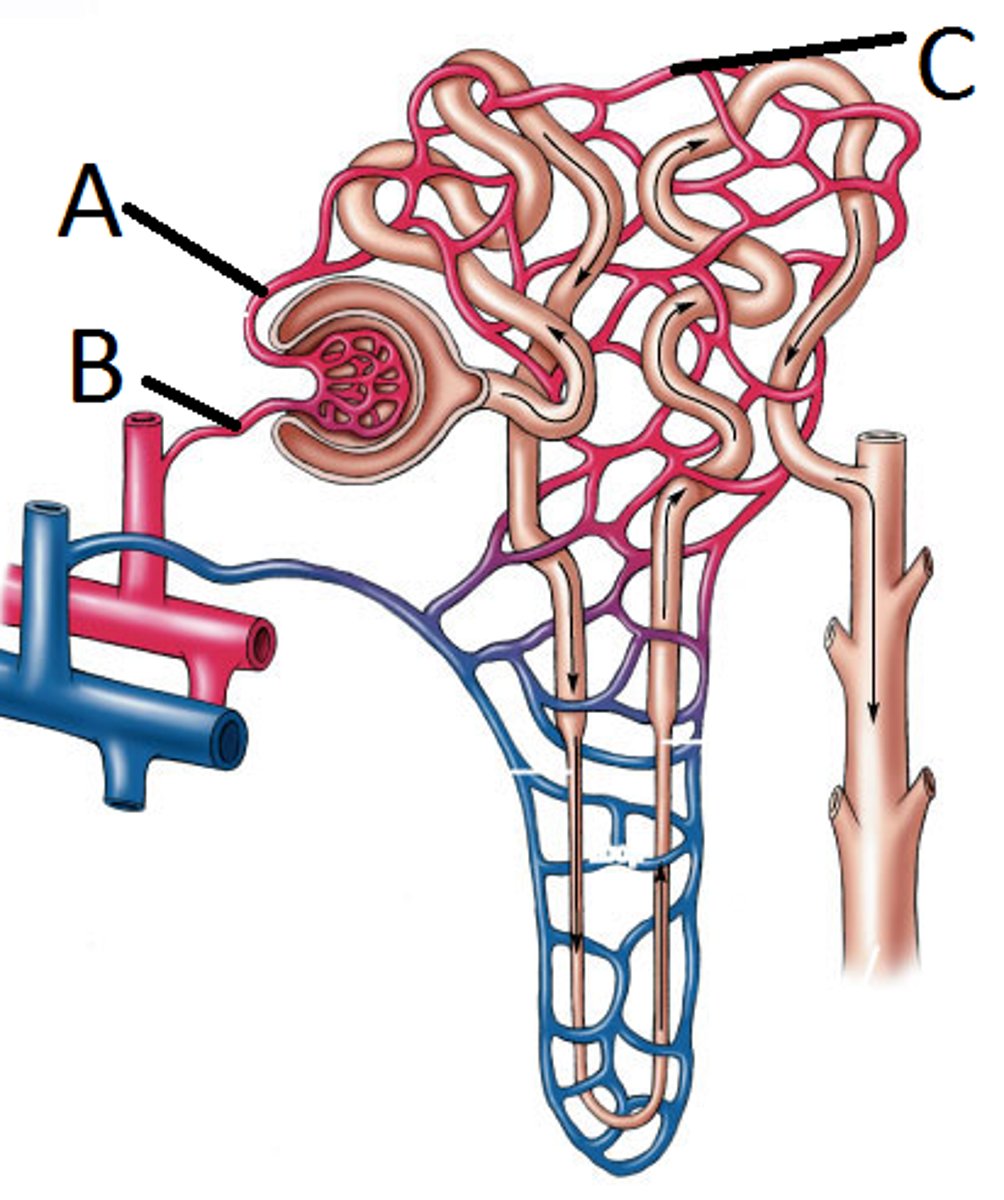
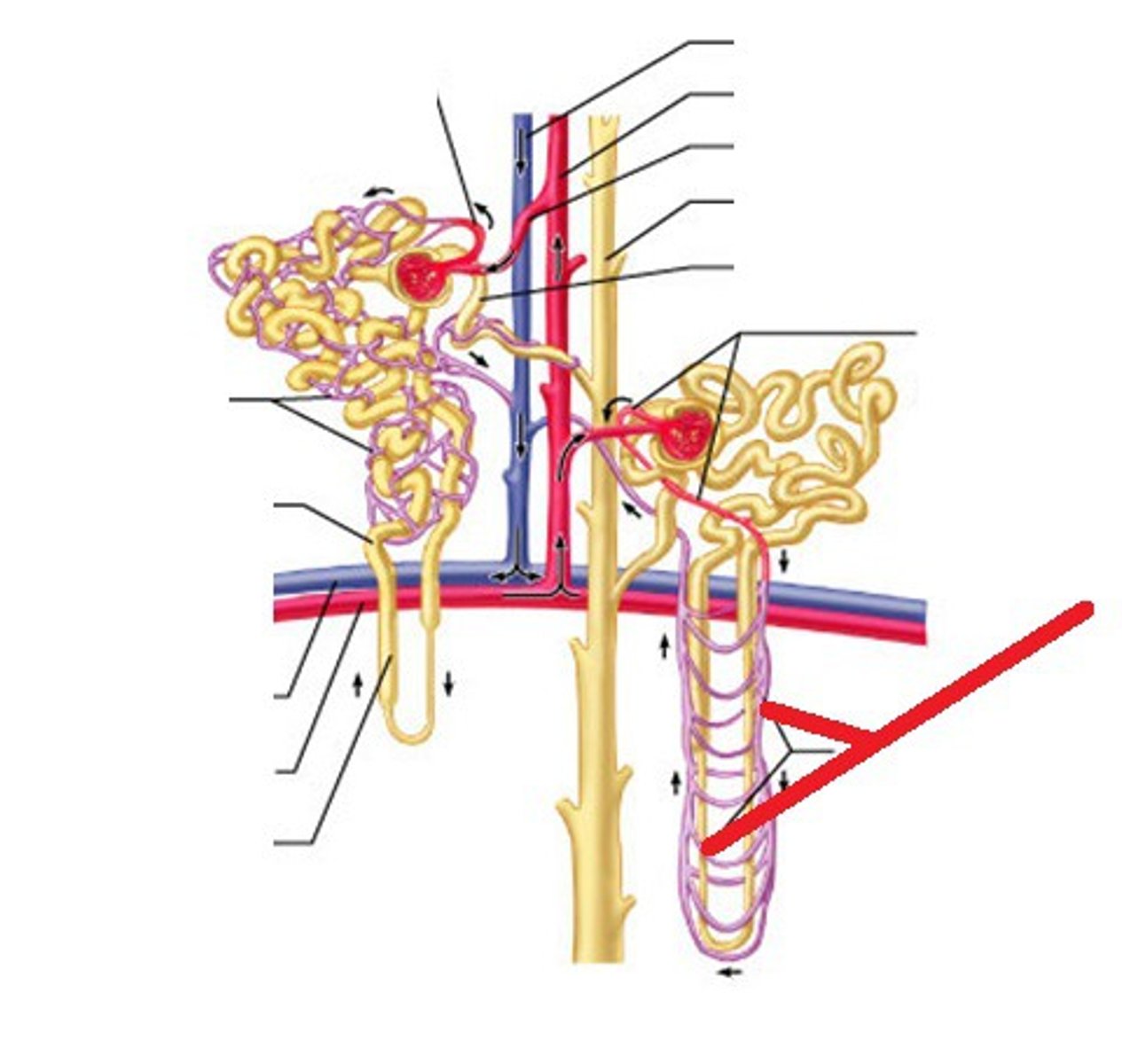
vasa recta
what are the capillaries that surround the nephron loop
vascular pole
the side of the corpuscle where the afferent arterial enters the corpuscle and the efferent arteriole leaves
urinary pole
the opposite side of the corpuscle where the renal tubule begins
visceral layer, parietal layer (this layer sits on top of capillaries)
the glomerular capsule has two layers:
glomerulus (capillaries) , glomerular capsule
the renal corpuscle consists of the ________ and the two layered_________________________
cortical
a _____________ nephron is found in the outer cortex, has a short loop of henle and is 85% of all nephrons
Capillaries: peritubular
juxtamedullary
a ____________________ nephron is near the cortex medulla junction, has a long loop of henle and is about 15% of all neurons
Capillaries: vasa recta
SALT GRADIANT IN MEDULLA
glomerular filtration, tubular reabsorbtion (removes everything useful), tubular secretion (removes addition waste from the blood and adds them to filtrate) , water conservation
how is urine made from blood plasma ?
glomerular filtrate
this is the fluid in the capsular space during urine formation
Similar to blood plasma except that it has almost no protein
fenestrated endothelium of glomerular capillaries, basement membrane, filtration slits
what are the 3 parts of the filtration membrane
podocyte
These cells form a porous membrane surrounding the endothelial cells of the glomerulus.
proteinuria
protein in the urine
hematuria
blood in the urine
blood hydrostatic pressure
What pressure pushes water and solutes out of the glomerulus and drives filtration
colloid osmotic pressure
What pressure pulls water back into capillaries due to plasma proteins
they increase
What happens to BHP and filtration if the afferent arteriole dilates
they decrease
What happens to BHP and filtration if the afferent arteriole constricts
they increase
What happens to BHP and filtration if the efferent arteriole constricts
they decrease
What happens to BHP and filtration if the efferent arteriole dilates
increase both
How does high systemic blood pressure affect glomerular BHP and filtration
decrease both
How does low systemic blood pressure affect glomerular BHP and filtration
GFR inreases
What happens to GFR when blood hydrostatic pressure increases
Filtrate moves too fast; reabsorption decreases, may cause dehydration
What happens if GFR is too high
Filtrate moves too slowly; too much reabsorption, including wastes
What happens if GFR is too low?
filtration decreases
What happens to filtration when both BHP and NFP decrease
affernet and efferent arterioles
Which arterioles control pressure in the glomerulus and influence GFR
afferent arteriole
Which arteriole brings blood into the glomerulus and controls how much blood enters for filtration
efferent arteriole
Which arteriole carries blood out of the glomerulus and helps control how much pressure builds up inside the capillaries
Renal autoregulation, sympathetic control, hormonal control
What are the three homeostatic mechanisms that regulate GFR
renal autoregulation
Which GFR control mechanism allows the kidneys to adjust their own blood flow without outside help
myogenic mechanism
This is a part of the renal autoregulation of GFR: When BP rises, afferent arteriole constricts to prevent too much filtration. When BP falls, it dilates to maintain GFR
tubuloglomerular feedback
this is part of the renal autoregulation of GFR: The macula densa in the distal tubule detects NaCl levels and tells the afferent arteriole to constrict or dilate accordingly
Macula densa cells sense NaCl levels and signal afferent arteriole to adjust GFR
What is tubuloglomerular feedback
It decreases due to afferent arteriole constriction
What happens to GFR during sympathetic nervous system activation
Renin-Angiotensin-Aldosterone System (RAAS)
What hormone system helps maintain GFR during low blood pressure
NaCl concentration in the distal tubule filtrate
What do macula densa cells sense and respond to
Trigger afferent arteriole constriction to lower GFR
What does high NaCl in the distal tubule signal the macula densa to do?
Signal granular cells to release renin and increase GFR
What does low NaCl in the distal tubule signal the macula densa to do?
Relay signals and adjust glomerular capillary surface area to regulate filtration
What is the role of mesangial cells in the juxtaglomerular apparatus?
Granular (juxtaglomerular) cells
What cells release renin in response to low BP or low NaCl
afferent arteriole, down
when exercising, the sympathetic nervous system contricts the ____________________, so BHP goes _________ and the entire urinary system slows
It constricts the afferent arteriole to reduce GFR and conserve fluid
What role does the sympathetic nervous system play during low blood pressure?
Release renin to activate RAAS and raise BP
What does the sympathetic nervous system stimulate granular cells to do?
granular cells
specialized cells in the walls of renal arterioles that synthesize and release renin
renin
hormone secreted by the kidney; it raises blood pressure by influencing vasoconstriction (narrowing of blood vessels)
sympathetic nervous system
What nervous system detects low blood pressure and tells granular cells to release renin?
renin
What do granular (juxtaglomerular) cells in the kidneys release when BP drops?
angiotensinogen
What protein in the blood does renin convert into angiotensin I?
ACE (angiotensin-converting enzyme)
What enzyme in the lungs converts angiotensin I to angiotensin II?
Stimulates aldosterone release, ADH release, thirst, and vasoconstriction
What are the major effects of angiotensin II?
Aldosterone
What hormone does angiotensin II stimulate the adrenal glands to release?
ADH (antidiuretic hormone)
What hormone does angiotensin II stimulate the pituitary gland to release?
Increases water reabsorption at the collecting duct
What effect does ADH have on the kidneys?
Increases sodium (and water) reabsorption in the distal tubule and collecting duct
What does aldosterone do in the nephron?
Causes widespread vasoconstriction
How does angiotensin II affect blood vessels?
Increases blood pressure
How does vasoconstriction affect blood pressure?
Increases blood pressure
How does retaining more water in the blood affect blood pressure?
To restore blood pressure and blood volume
What is the overall goal of the RAAS system?
aldosterone
What hormone is released when BP is low and acts on the DCT and collecting duct to increase Na⁺ reabsorption
ADH
What hormone is released when blood osmolarity is high (low BP) and acts on the collecting duct to increase water reabsorption
ANP
What hormone is released when atrial stretch is high (high BP) and increases Na⁺ and water excretion to lower BP
proximal convoluted tubule, salt
the _________________ absorbs about 65% of glomerular filtrate and absorbs most anything OTHER THAN _________