Chapter 20 Blood Vessels and Circulation
1/104
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
105 Terms
arteries
carry blood away from the heart to capillaries; have thicker tunica media and narrower lumen than veins
Have more elastic and collagen fibers (spring back to shape)
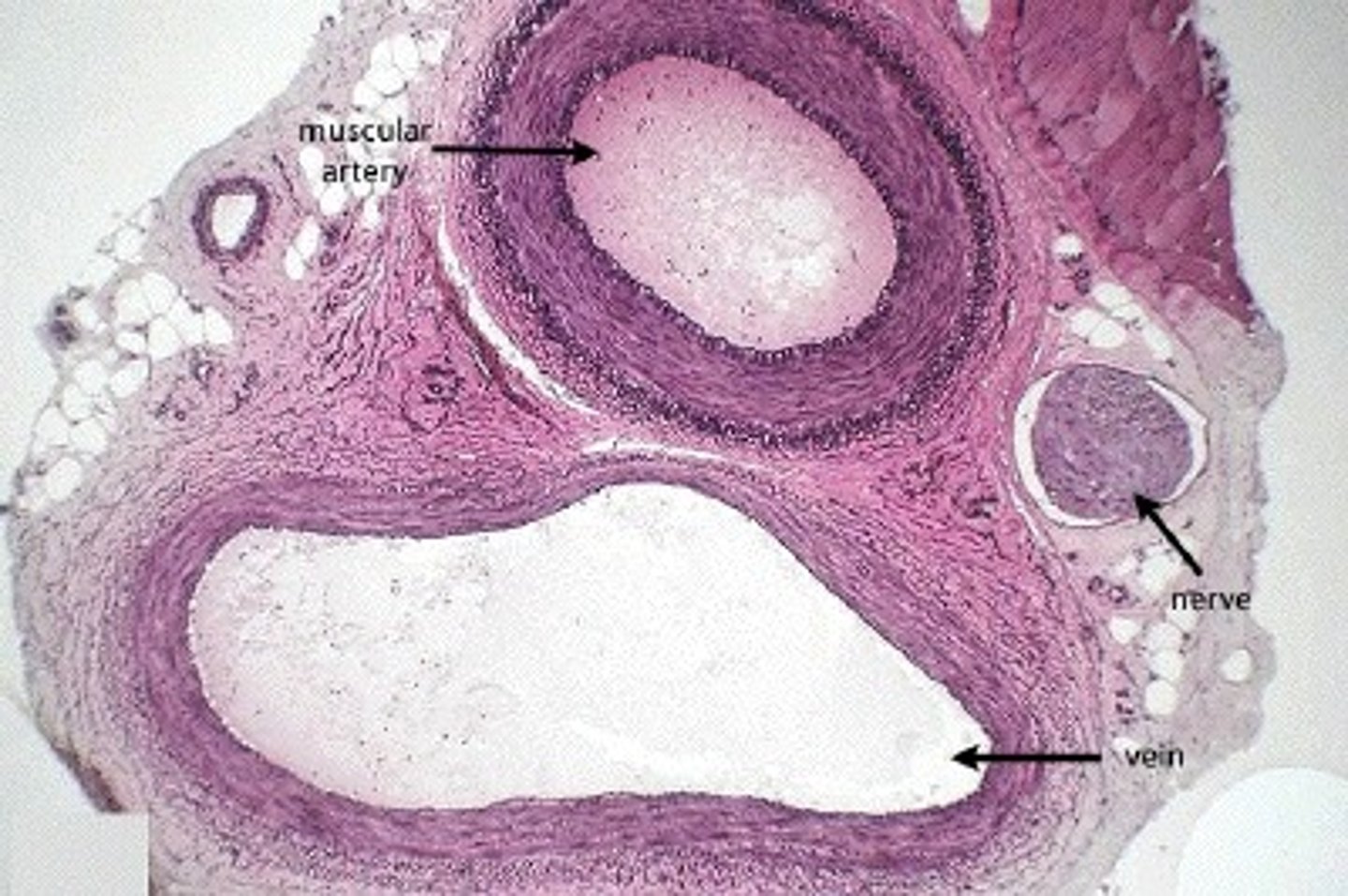
capillaries
microscopic vessel through which exchanges take place between the blood and cells of the body; found between arteries and veins; contain only tunica intima - allows for rapid gas and nutrient exchange
veins
carry blood back to the heart; have thicker tunica externa and larger lumen than arteries
Have less elastic and collagen fibers
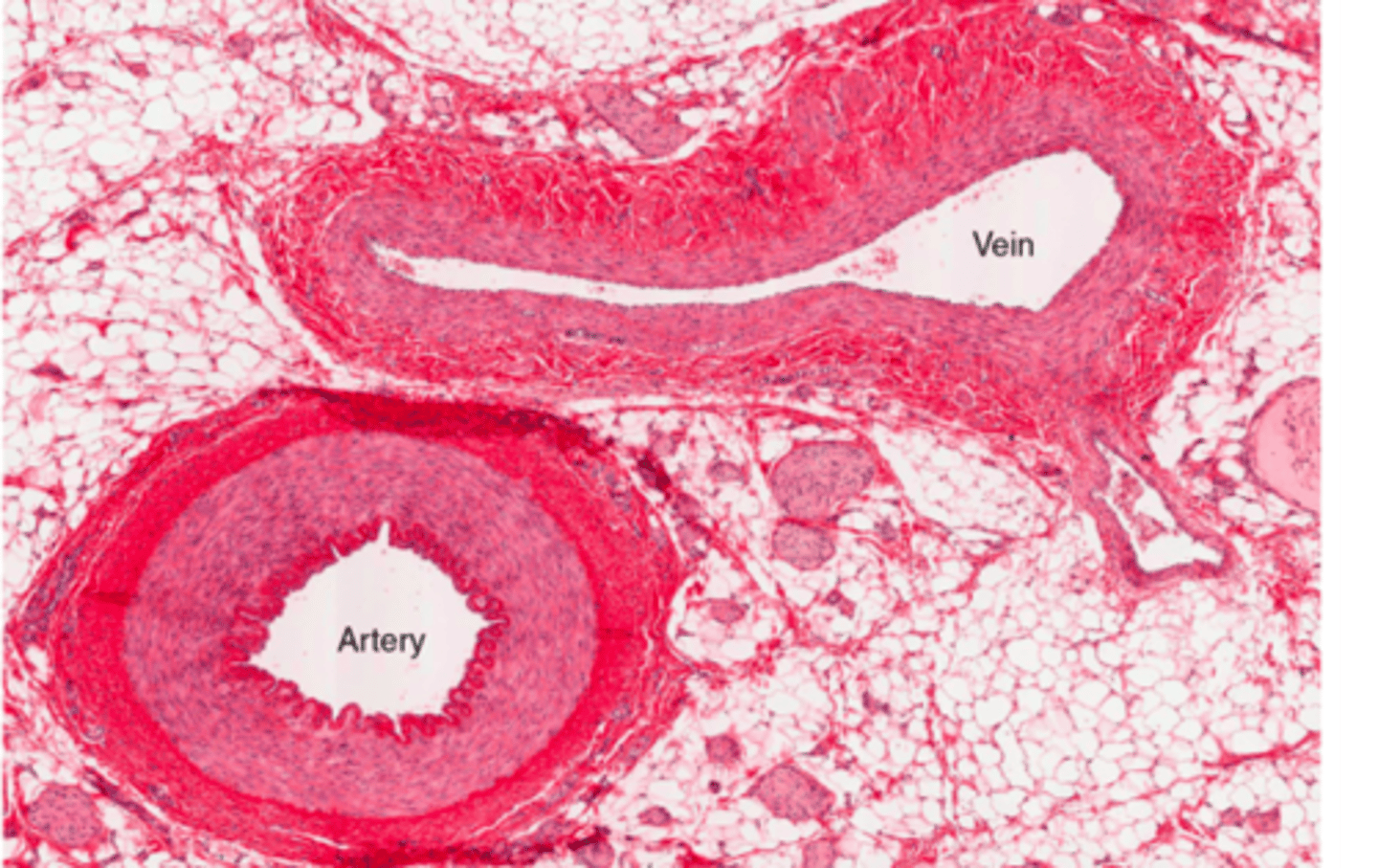
companion vessels
arteries and veins that lie next to each other serving the same body region
lumen
space within a tubular part or organ, such as the space within a blood vessel
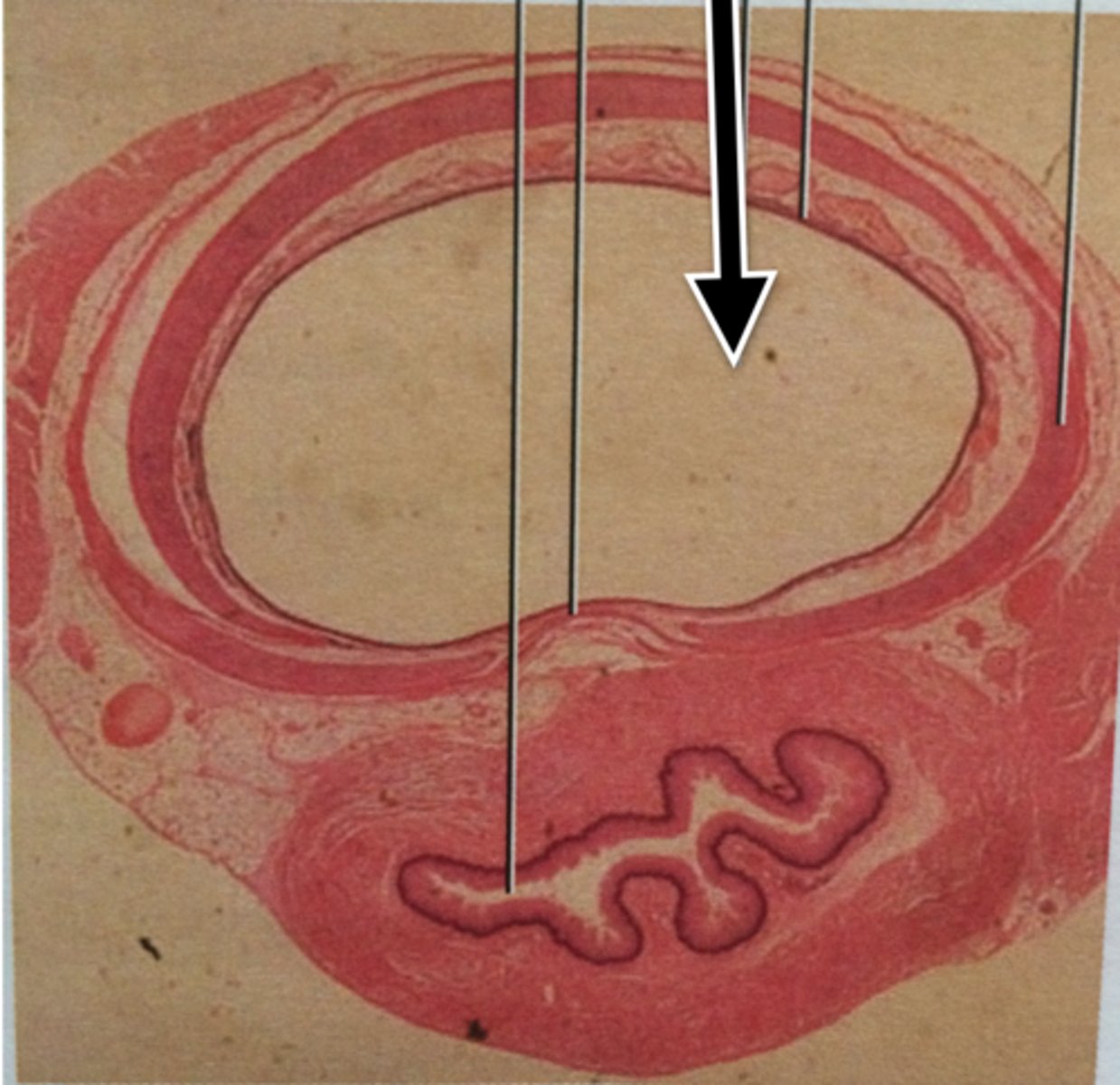
tunica intima
the innermost layer of a blood vessel; made primarily of simple squamous epithelium

tunica media
The middle and thickest layer of tissue of a blood vessel wall, composed of elastic tissue and smooth muscle cells that allow the vessel to expand or contract in response to changes in blood pressure and tissue demand
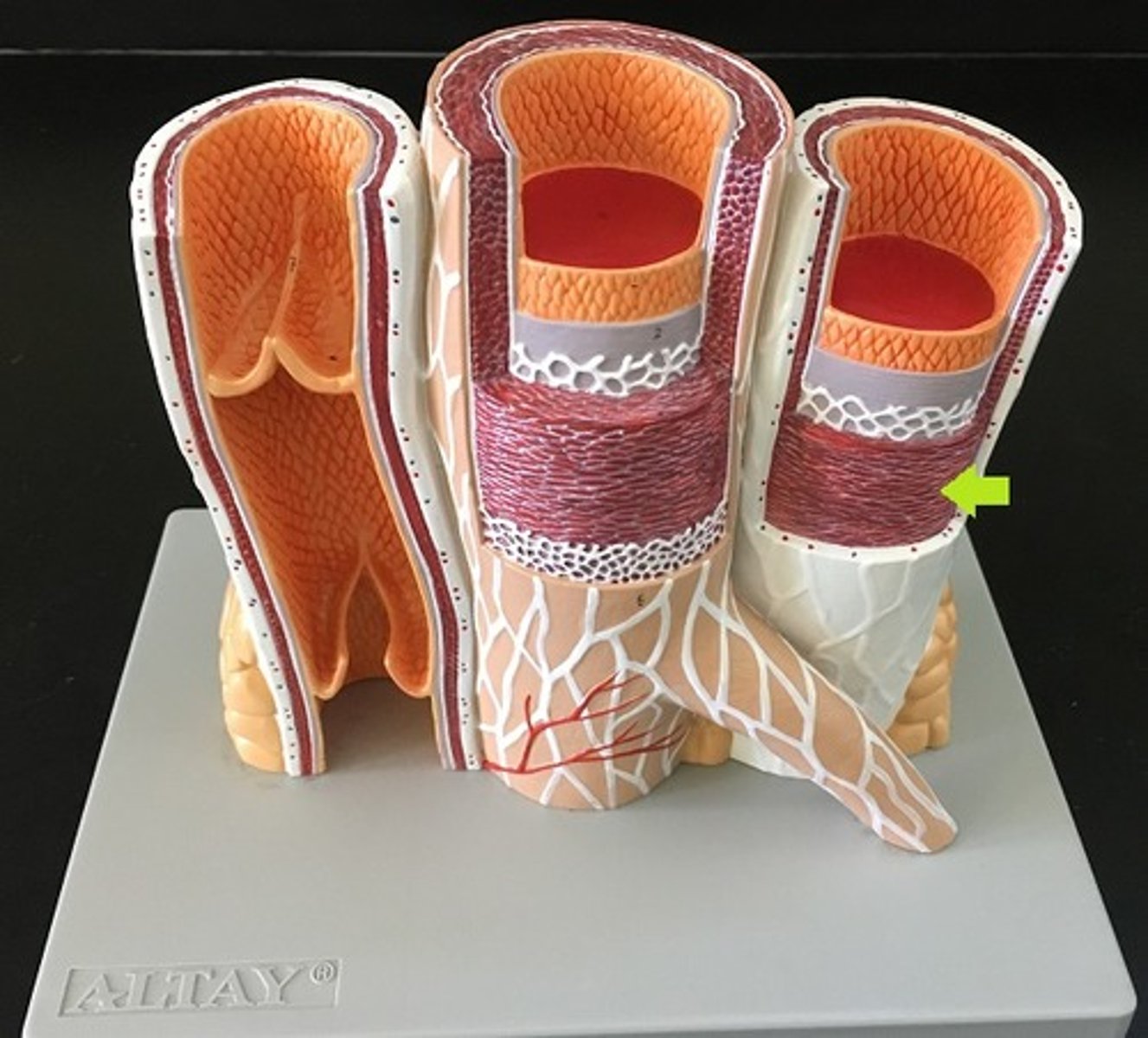
vasodilation
widening of blood vessel lumen diameter
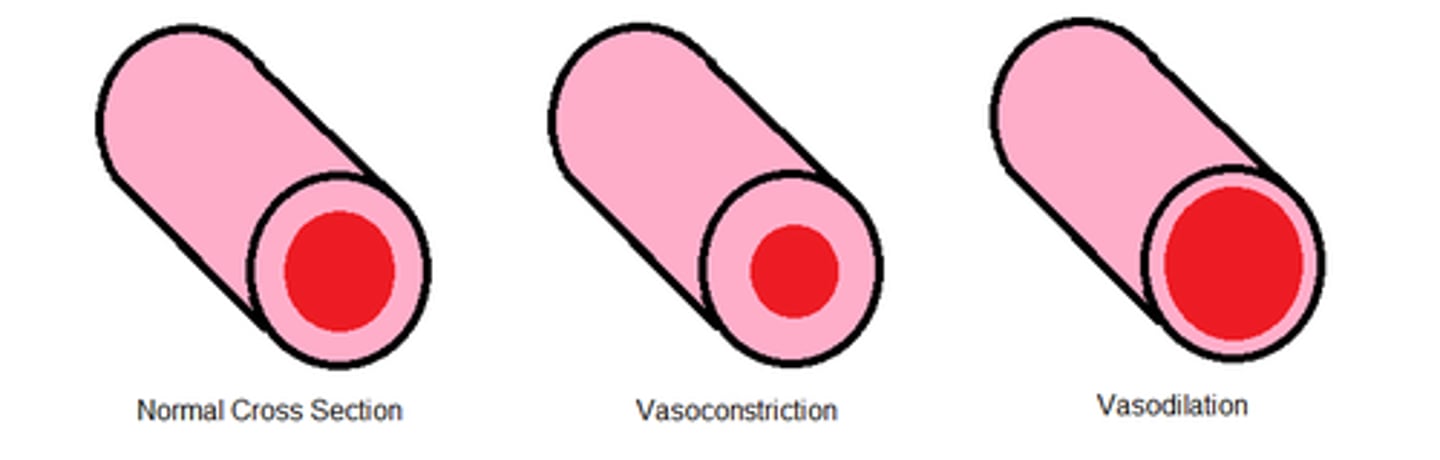
vasoconstriction
narrowing of blood vessel lumen diameter
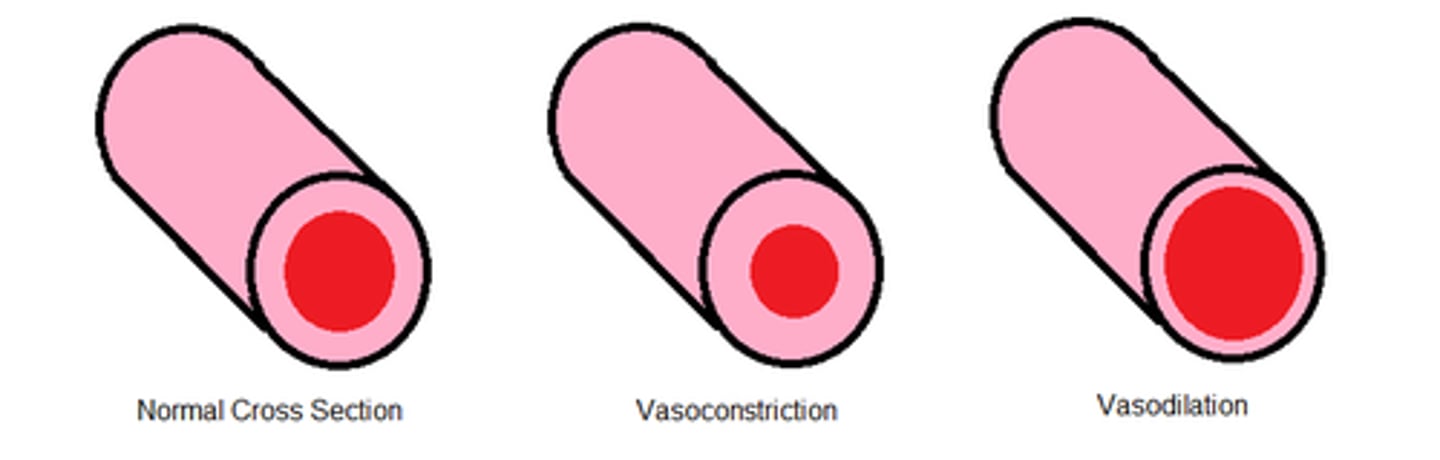
tunica externa
outer layer of a blood vessel which connects/anchors it to surrounding tissues
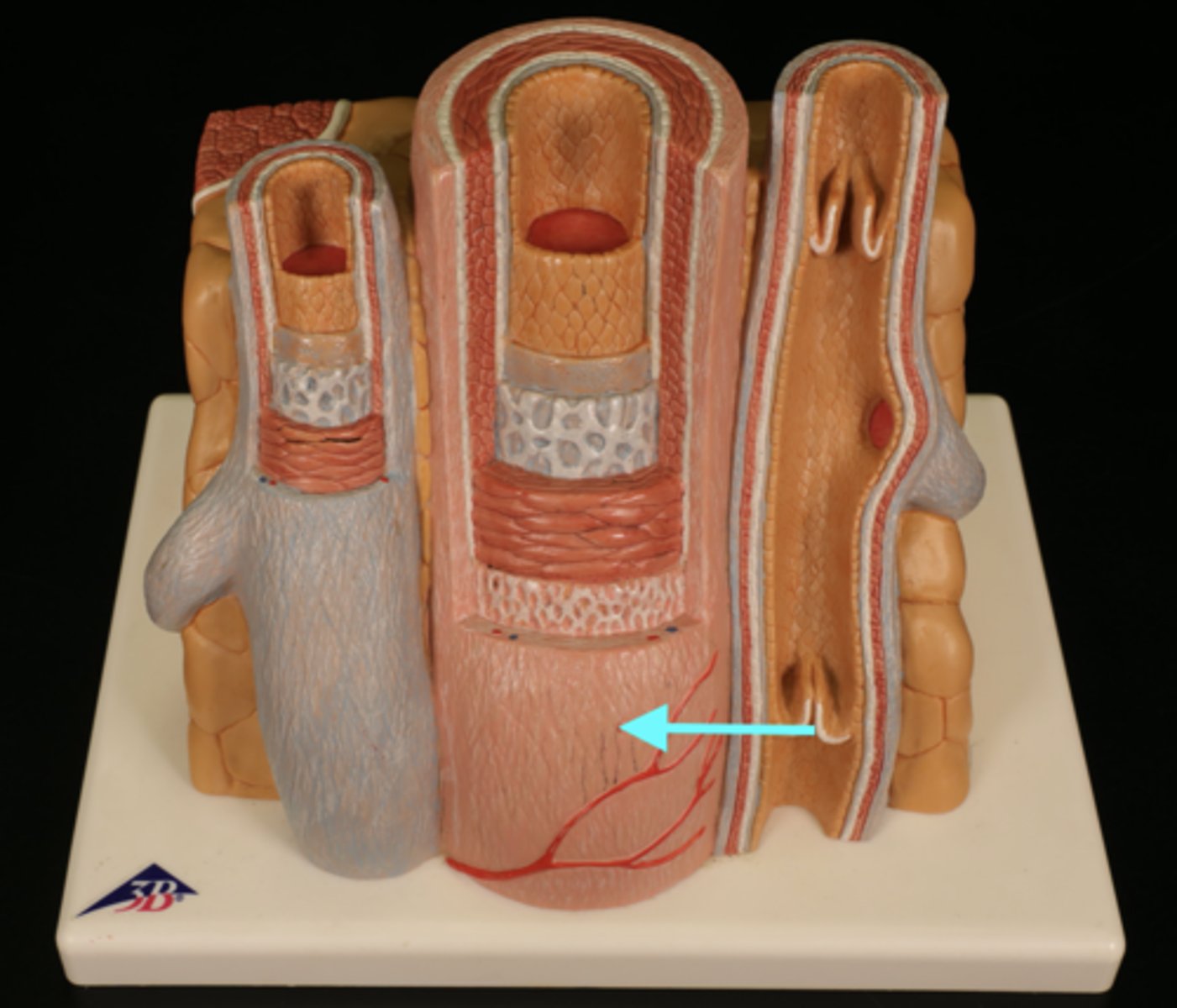
types of arteries
elastic (conducting), muscular (distributing), arterioles
elastic (conducting) arteries
largest arteries; conduct blood from heart to muscular arteries; large proportion of elastic fibers
muscular (distributing) arteries
medium sized arteries; distribute blood to specific body regions; most name arteries are this type
arterioles
smallest arteries; smooth muscle usually somewhat constricted (vasomotor tone)
vasomotor tone
produced by constant action of sympathetic vasoconstrictor nerves; blood vessels typically slightly constricted
types of capillaries
continuous, fenestrated, sinusoid
continuous capillaries
capillaries with cells joined together by tight junctions forming continuous lining; small intercellular clefts allow passage of smaller molecule through vessel wall; most common type of capillary
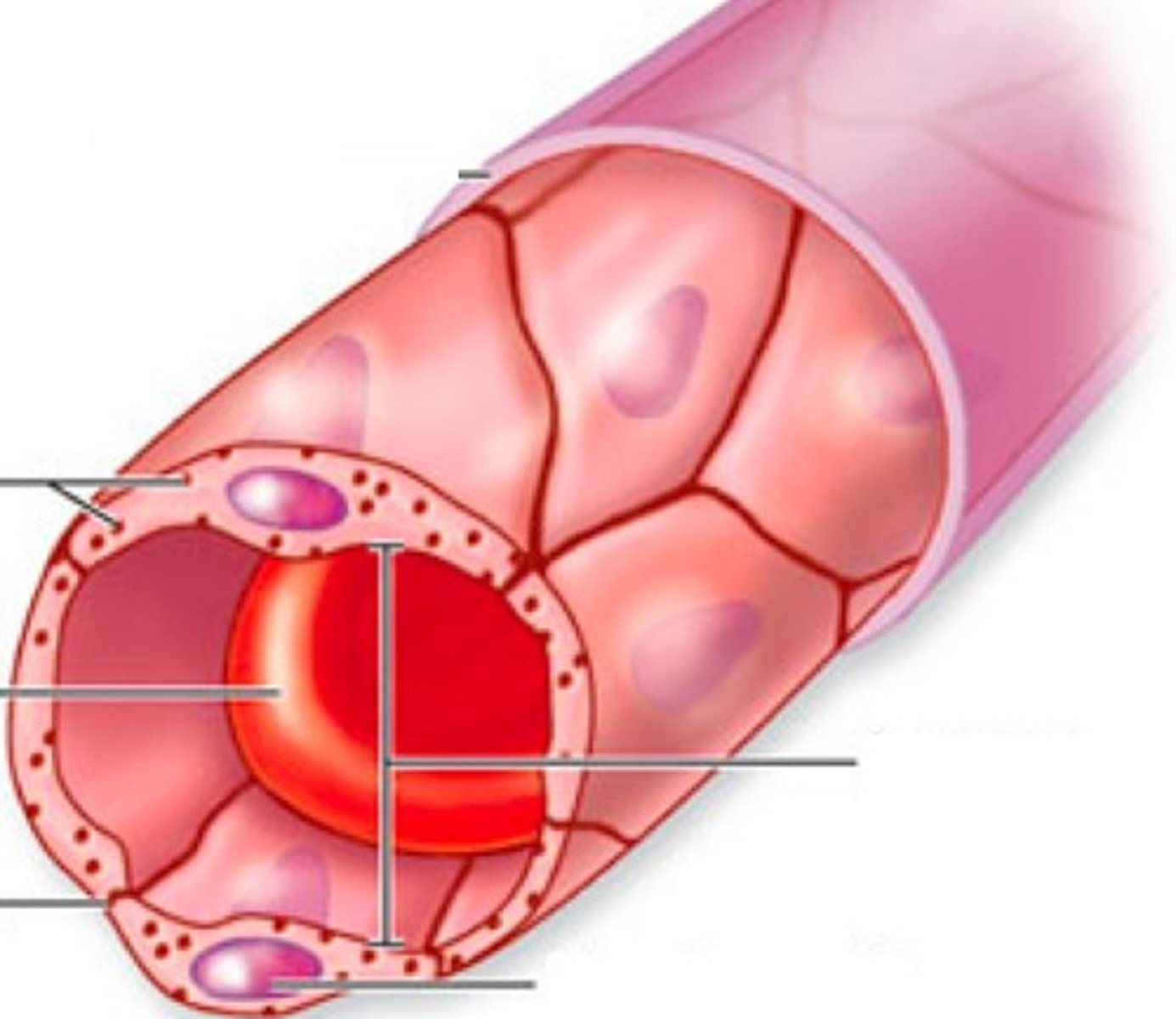
fenestrated capillaries
capillaries with cells joined together by tight junctions forming continuous lining, but cells have fenestrations (pores); small plasma proteins able to pass though pores; found where much fluid transport happens (intestines and kidneys)
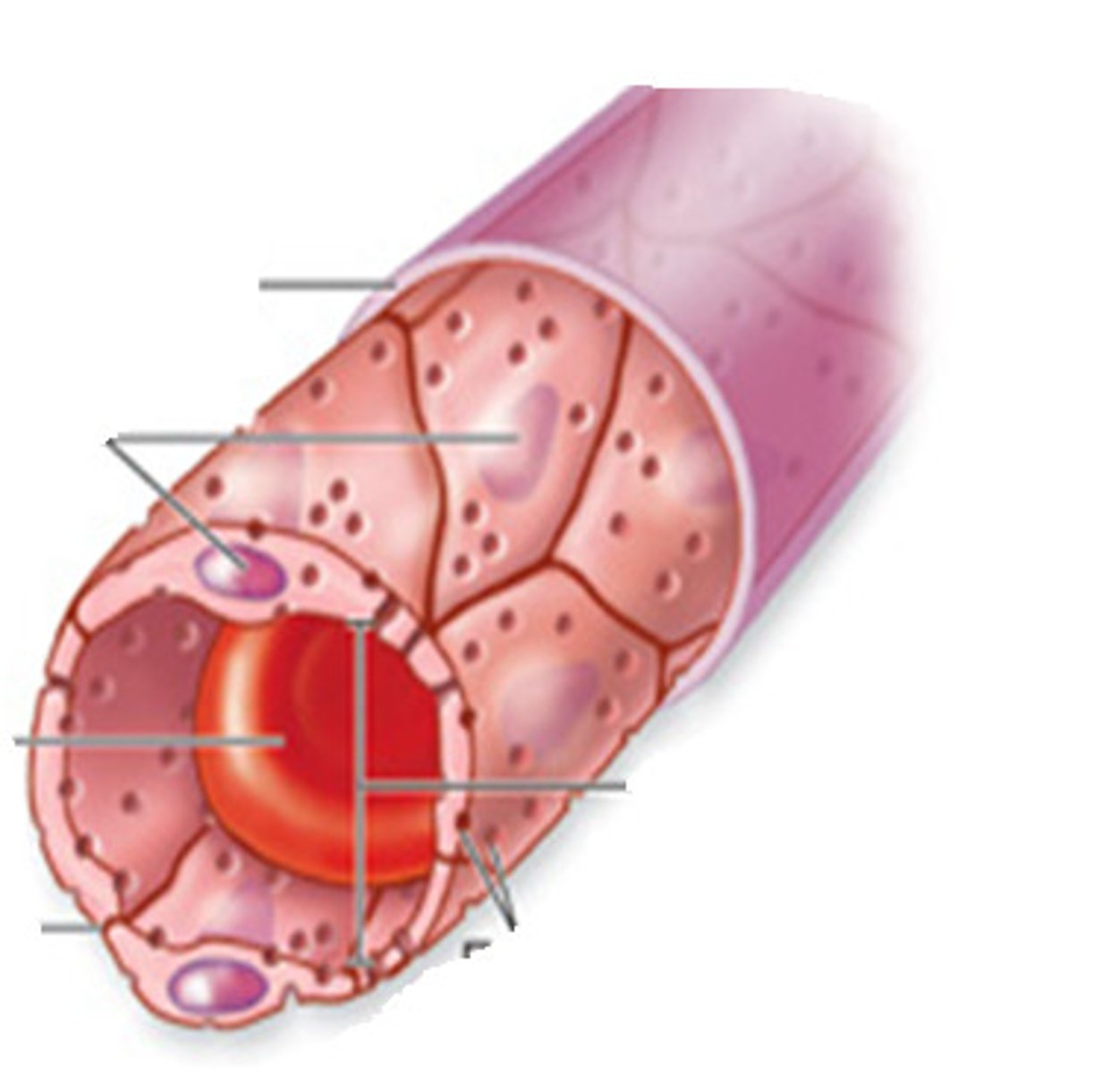
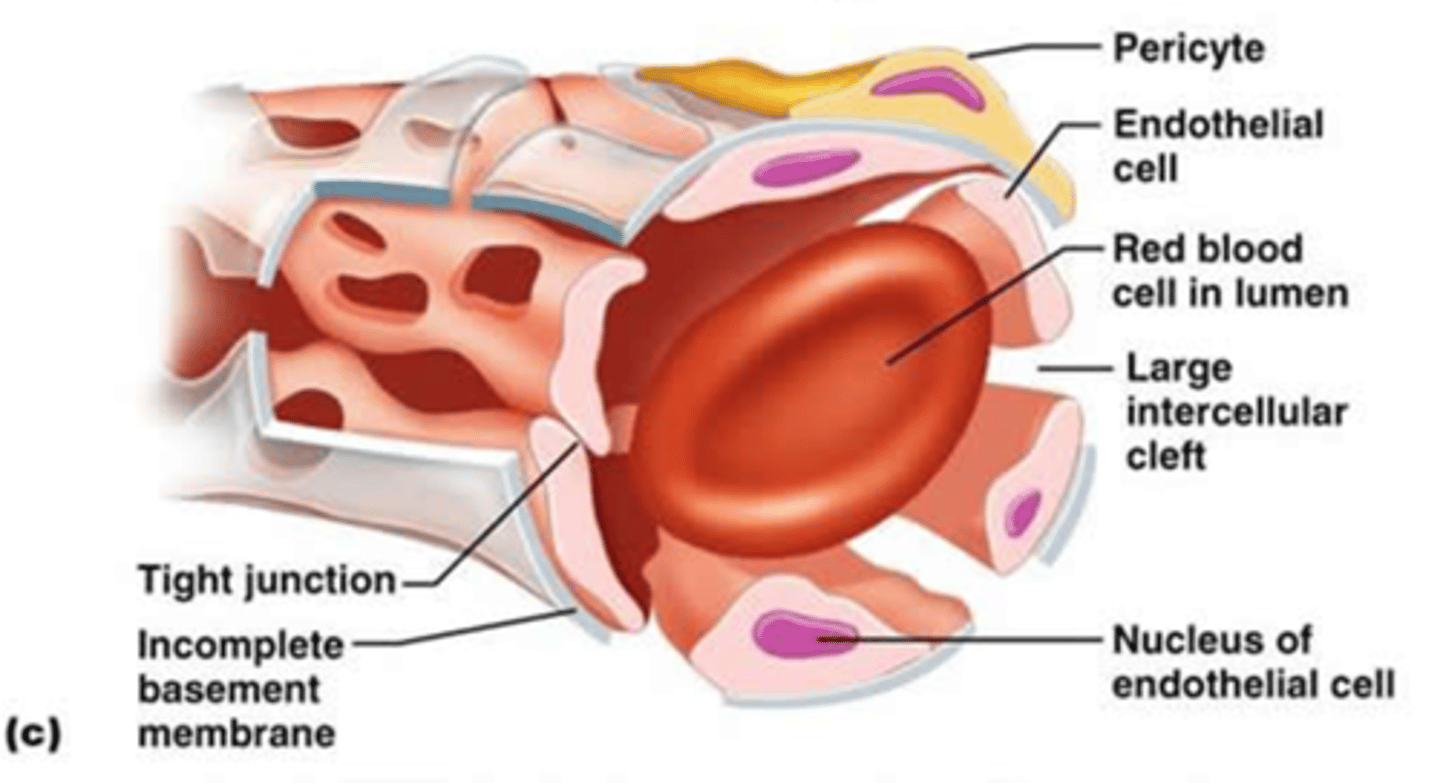
sinusoids
capillaries where the endothelial cells form an incomplete lining with large gaps; allow transport of large substances (formed elements and large proteins); found in bone marrow, spleen, and some endocrine glands
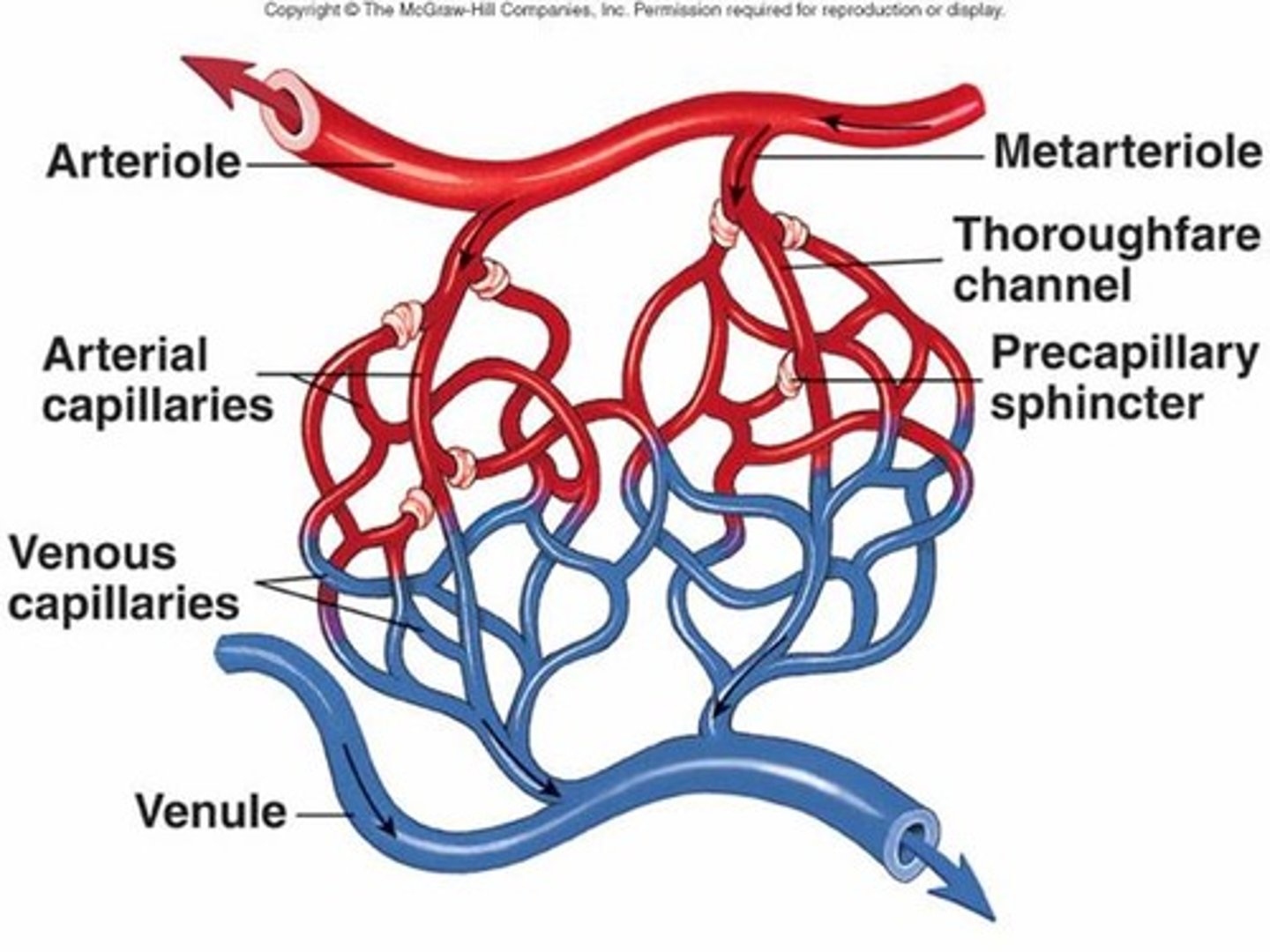
capillary beds
network of capillaries that function together; fed by metarteriole
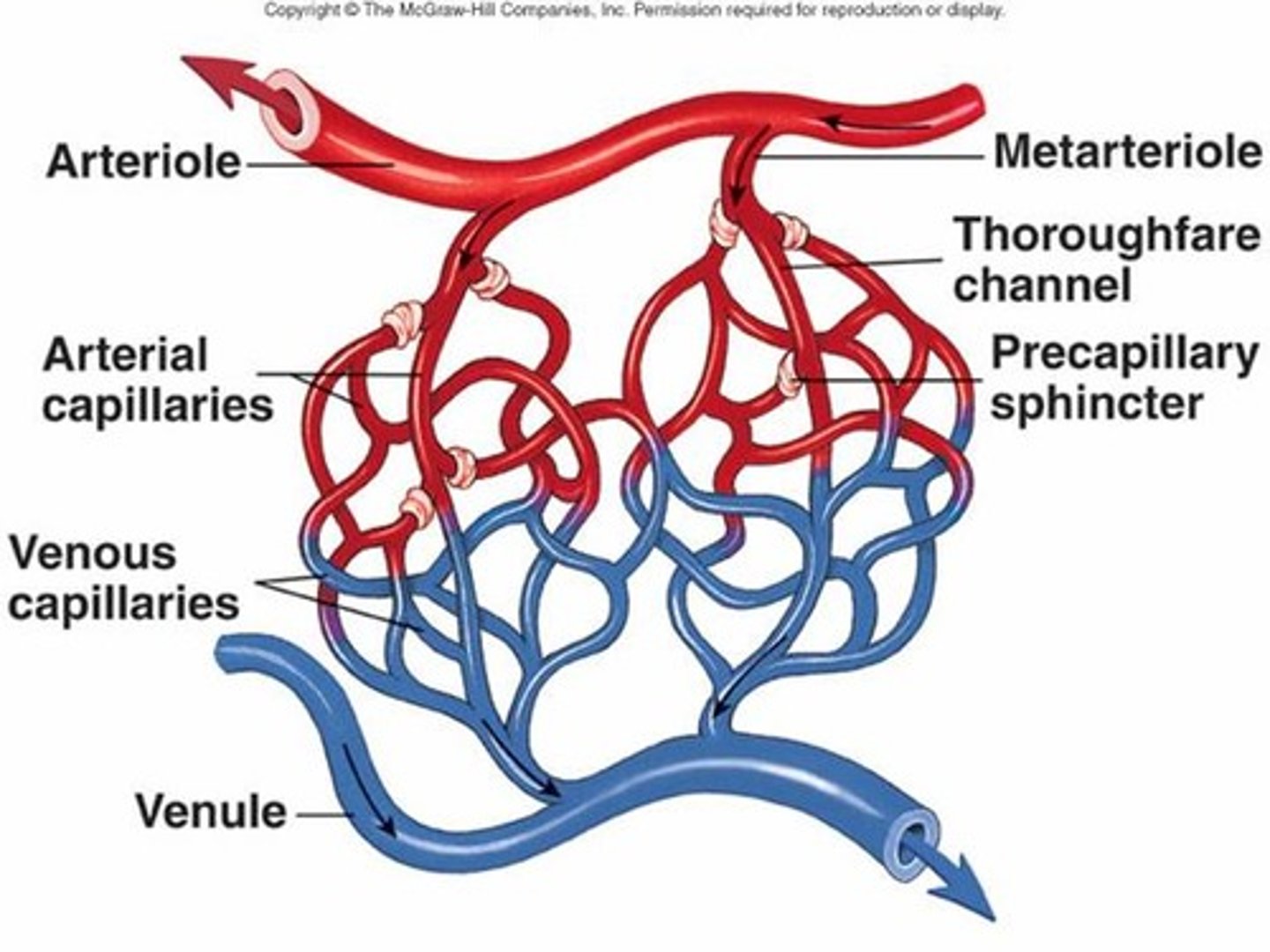
metarteriole
Short vessels that link arterioles and capillaries
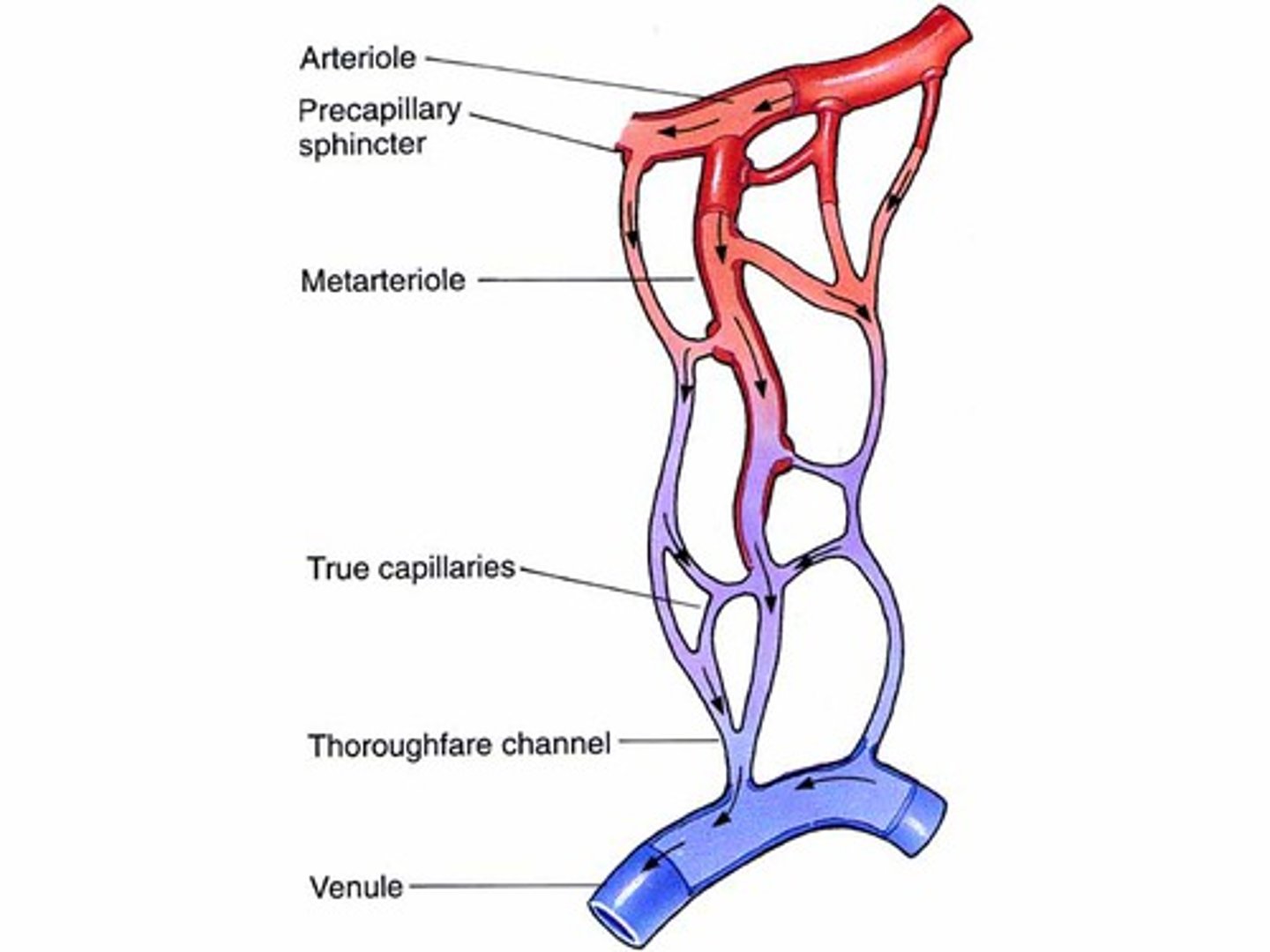
precapillary sphincter
band of smooth muscle that adjusts the blood flow into each capillary
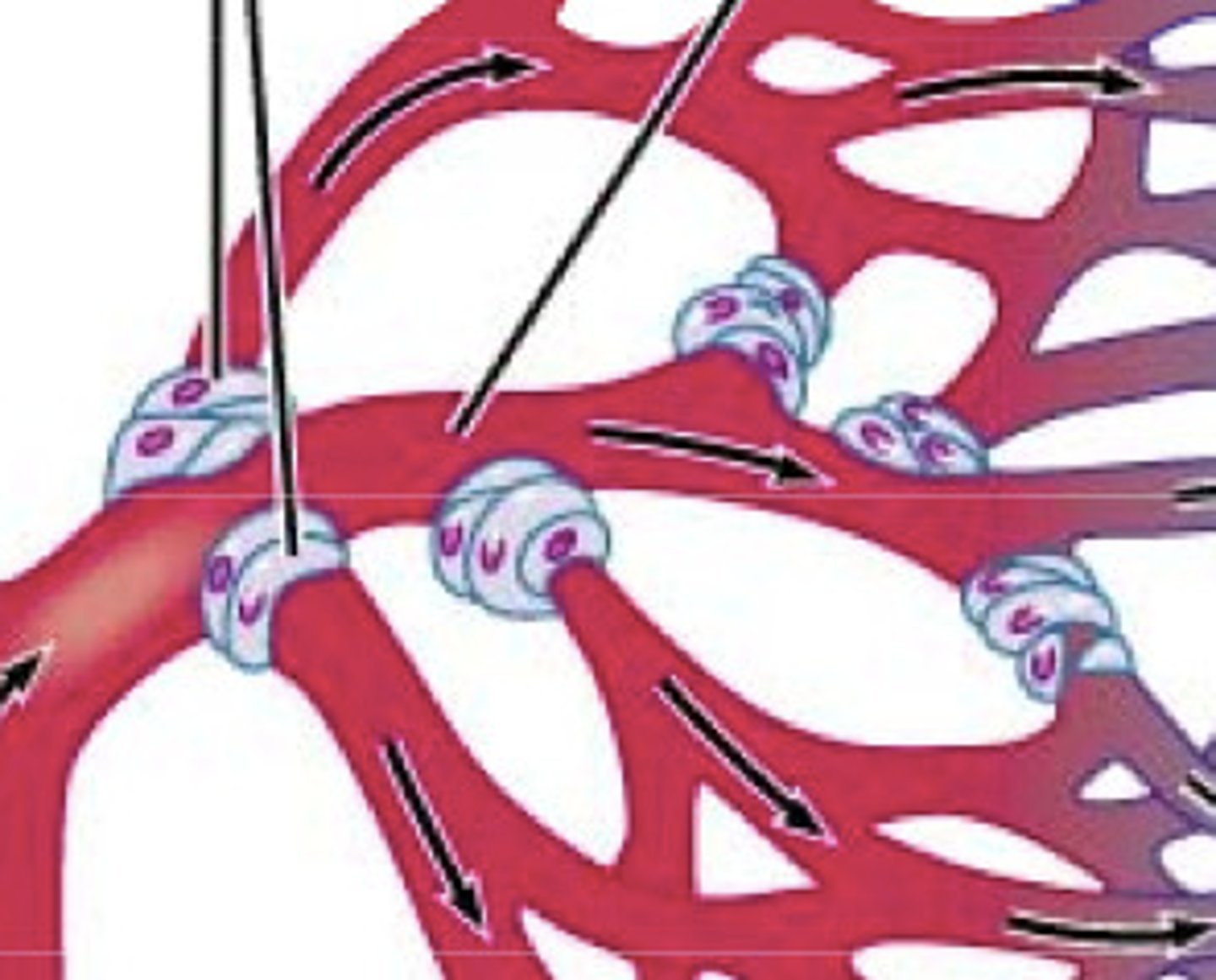
vasomotion
Contraction and relaxation cycle of capillary sphincters; causes blood flow in capillary beds to constantly change routes
perfusion
Circulation of blood within an organ or tissue in adequate amounts to meet current needs of the cells; amount of blood entering capillaries per unit time per gram of tissue (mL/min/g)
venules
small vessels that transfer blood from the capillaries; merge to form veins
small and medium-sized veins
companion vessels with muscular arteries; contain valves
large veins
companion vessels with elastic arteries; contain valves
blood reservoir
at rest systemic veins contain 55% of blood in circulation; blood moved into circulation via vasoconstriction and shifted back through vasodilation
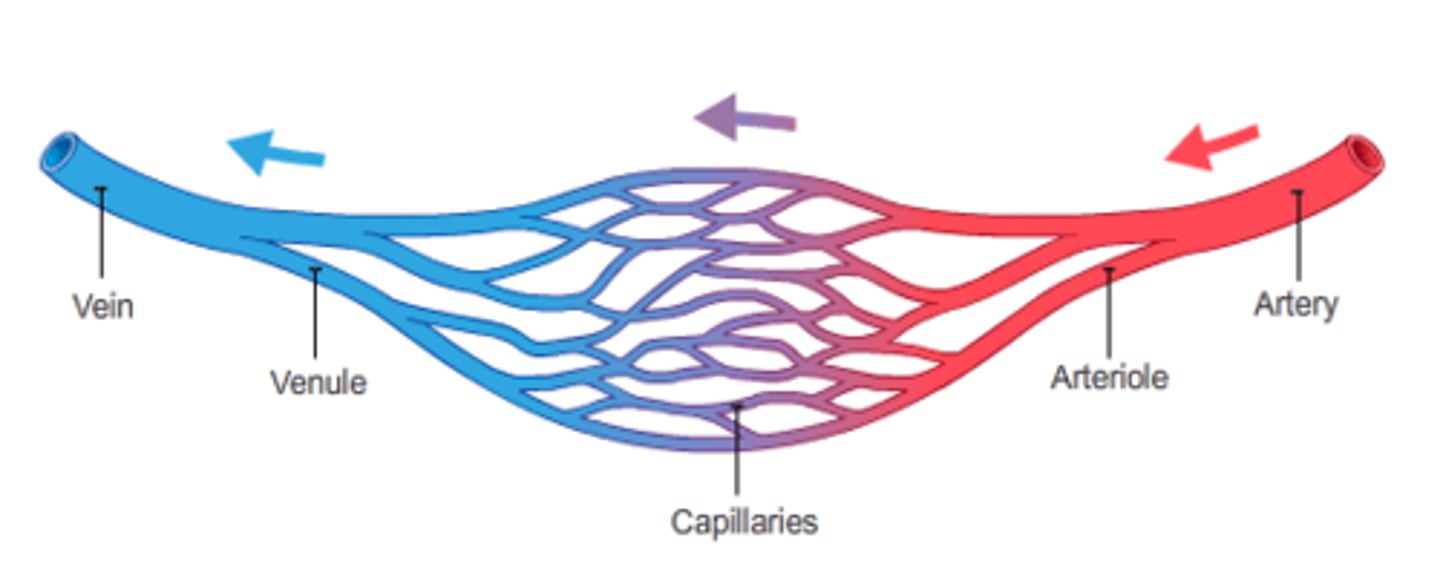
simple vessel pathway
one major end artery delivers blood to an organ or region; one end artery branches into arteries that branch into arterioles, each arteriole feeding into a capillary bed; the capillary bed is drained by a venule; venule merge into one major vein; ex. splenic artery to spleen to splenic vein
end artery
a single artery that is the only source of blood for an organ
alternative vessel pathways
arterial anastomosis, venous anastomosis, arteriovenous anastomosis; and portal system
arterial anastomosis
two or more arteries converge to supply the same region; ex. superior and inferior epigastric arteries suppling abdominal wall

venous anastomosis
two or more veins drain same body region; ex. basilic, brachial, and cephalic veins drain upper limb
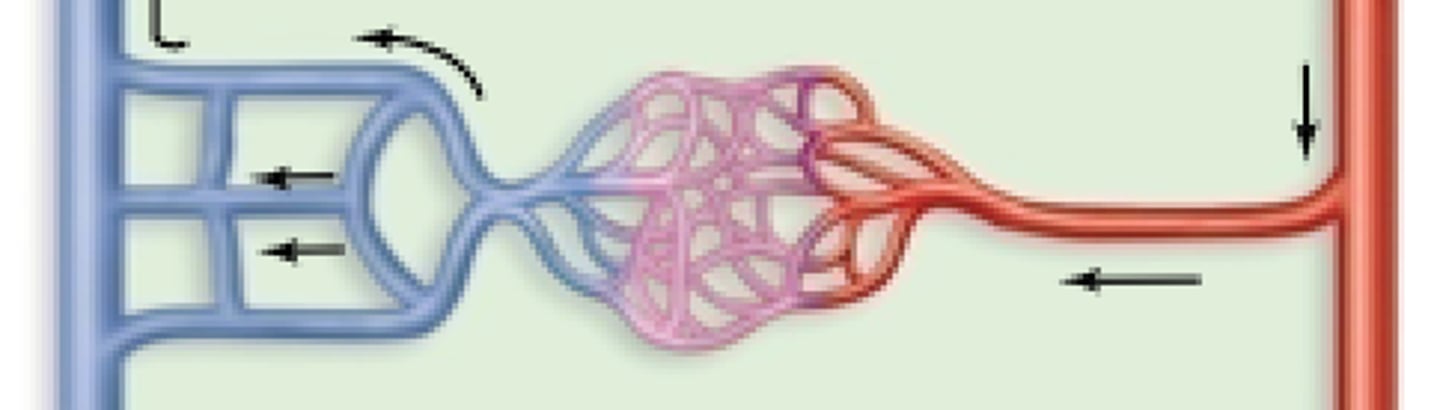
arteriovenous anastomosis
artery flows directly into vein bypassing capillaries; allows areas to be bypassed if body hypothermic; ex. fingers, toes, ears
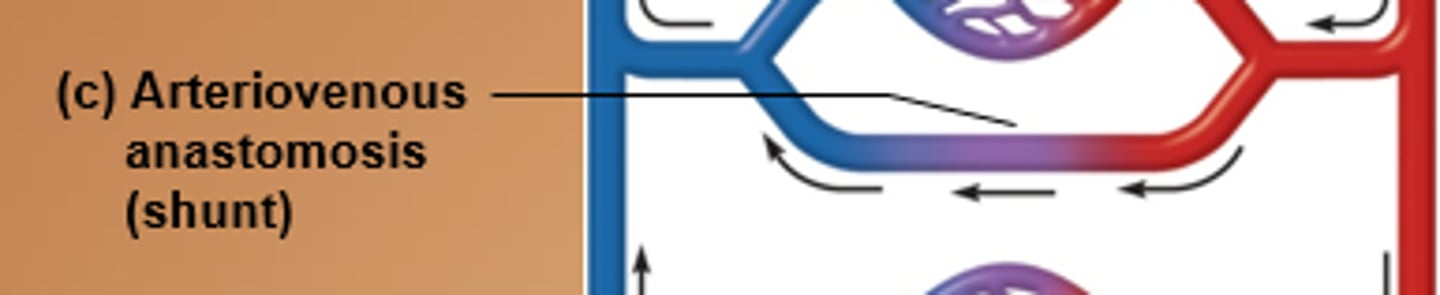
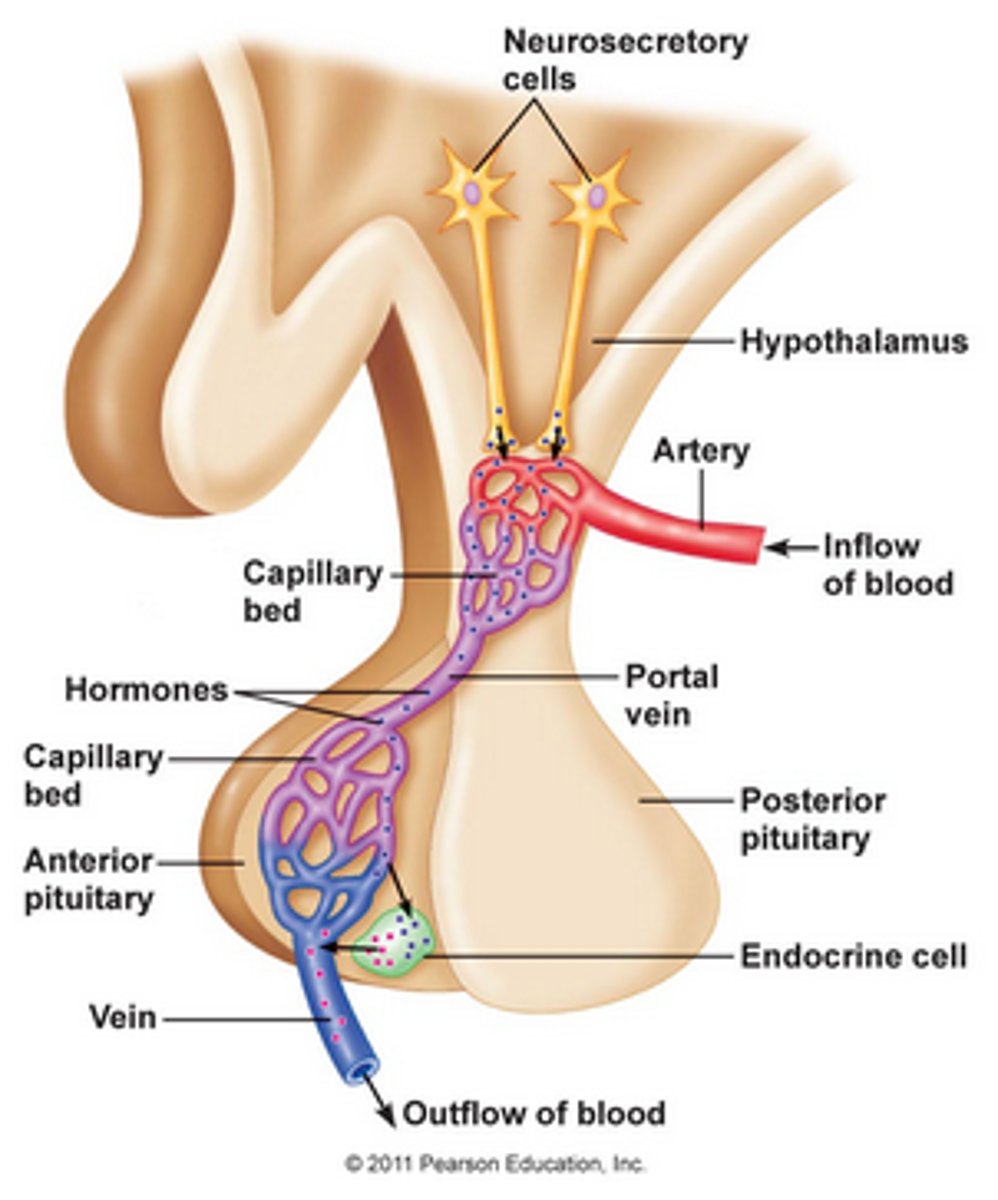
portal system
two capillary beds in sequence; path artery → capillary bed → portal vein → capillary bed → vein; ex. hepatic portal system and hypothalamo-hypophyseal portal system
total cross-sectional area
sum of diameters of all vessels of a certain type; as area of the vessels increases, the velocity of flow decreases.; are greatest in capillaries so blood flow is slowest, which allows time for exchange of gases and nutrients
blood flow velocity
speed of blood movement through vessels
capillary exchange
the movement of substances into and out of capillaries (between blood and interstitial fluid; processes include diffusion, vesicular transport, and bulk flow
diffusion
movement of molecules from an area of higher concentration to an area of lower concentration; small solute diffuse through cells or intercellular clefts and large molecules diffuse through fenestrations or gaps in sinusoids
vesicular transport
transport of substances through cell in membrane bound sac (vesicle); occurs both side of capillary (into/out of blood vs into/out of interstitial fluid)
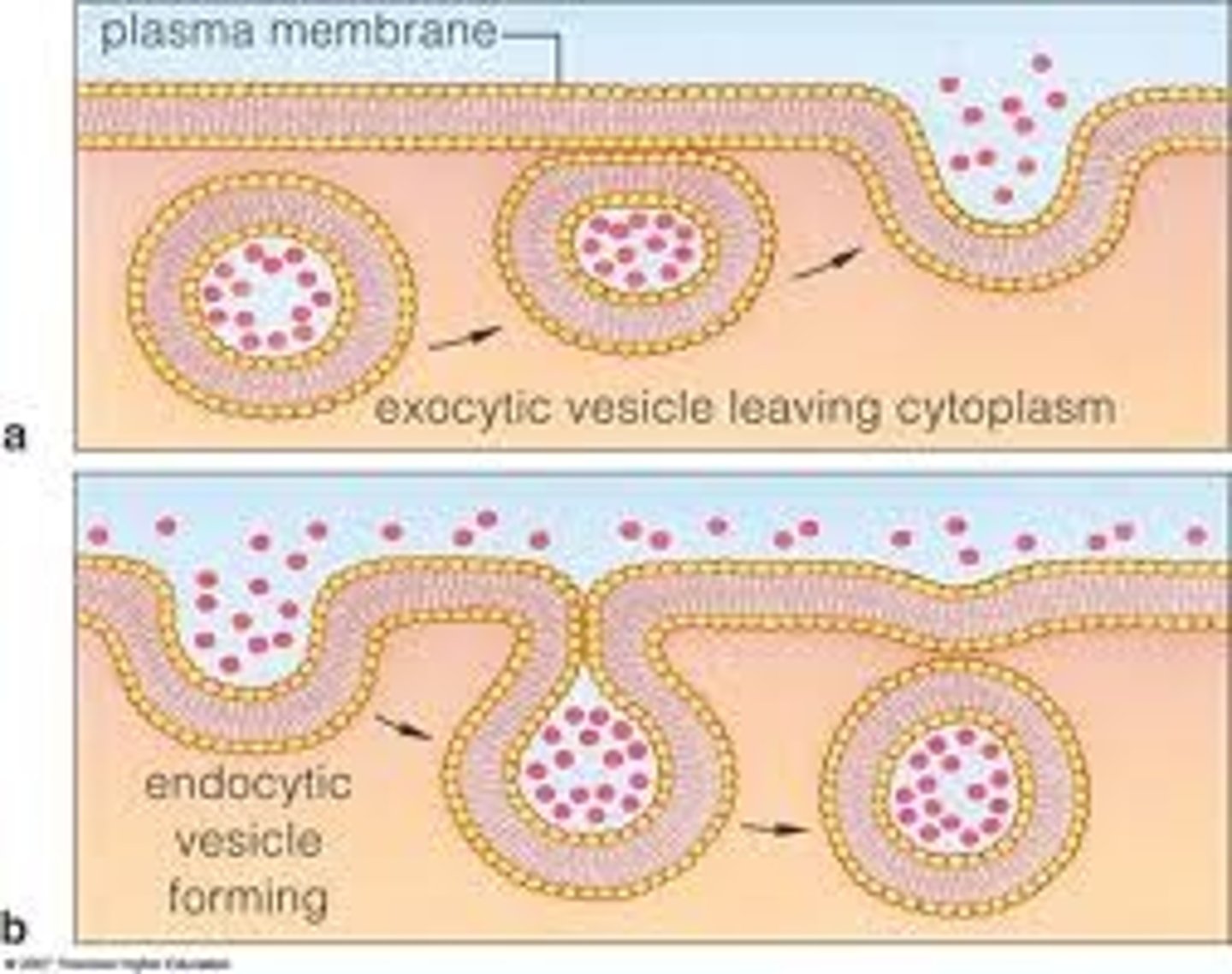
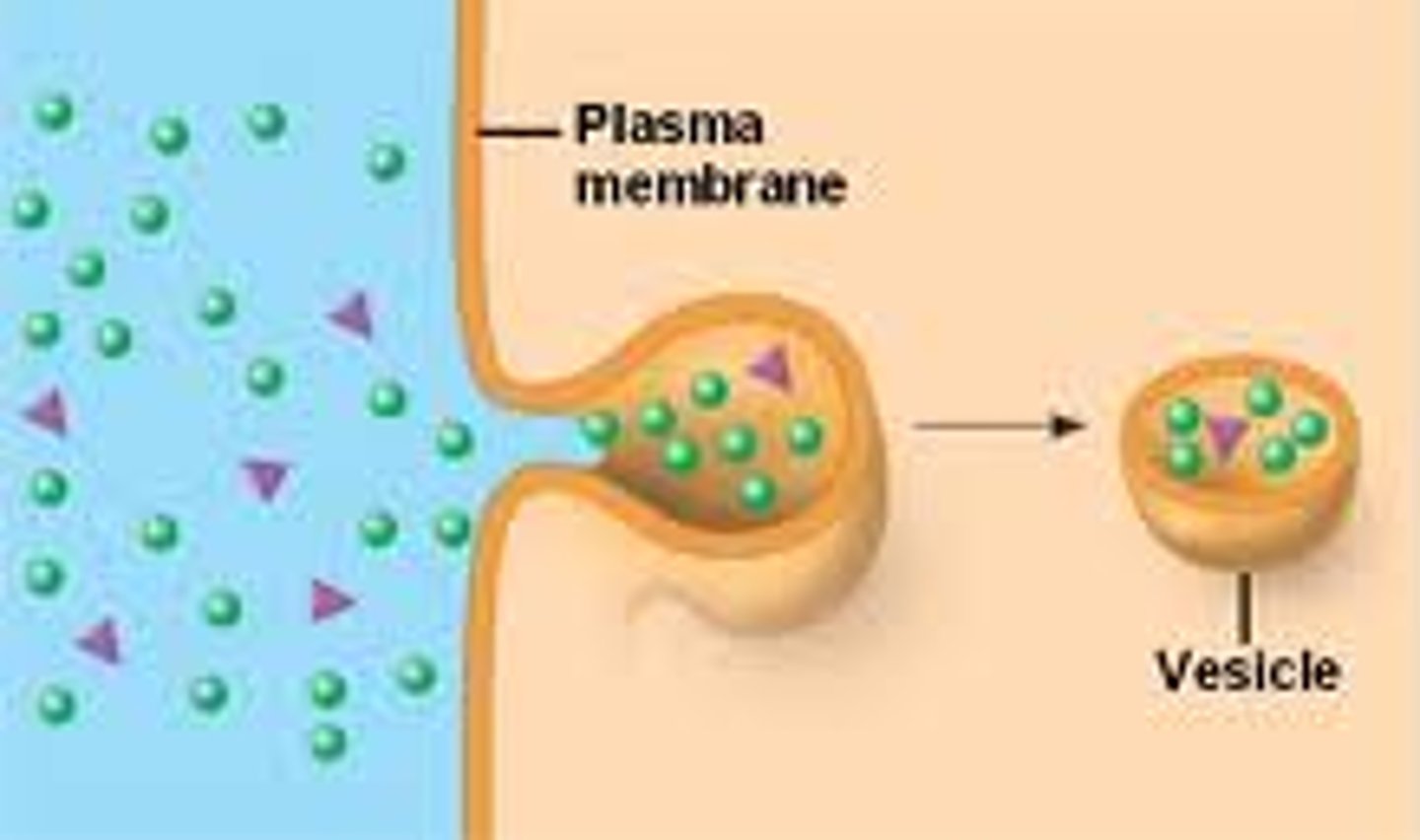
pinocytosis
A type of endocytosis in which the cell ingests extracellular fluid and its dissolved solutes
exocytosis
a process by which the contents of a cell vesicle are released to the exterior through fusion of the vesicle membrane with the cell membrane
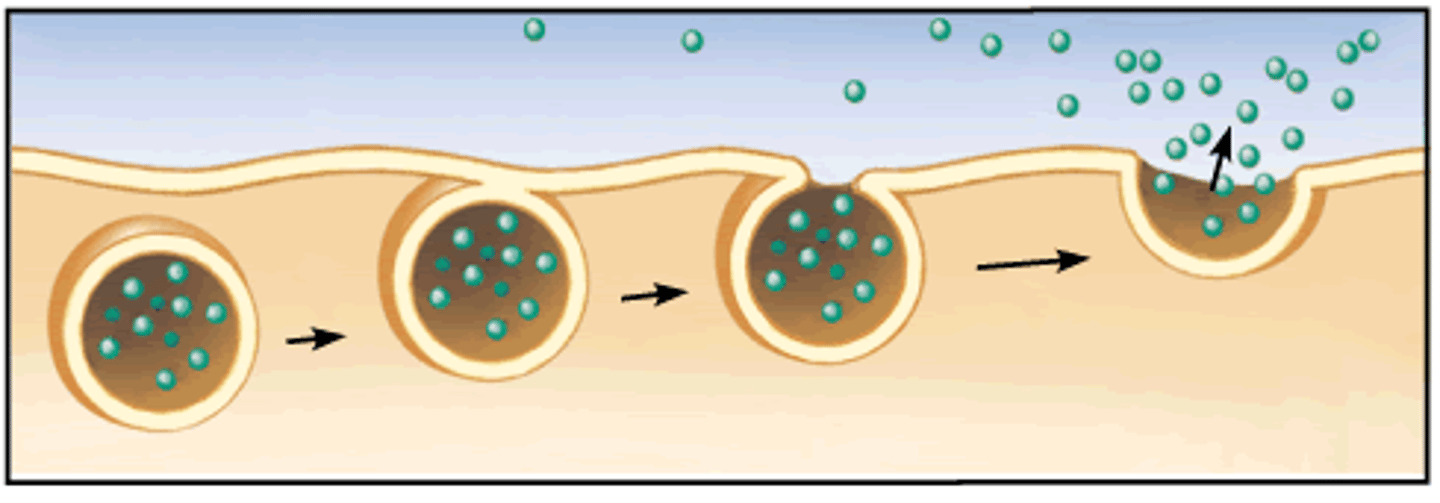
bulk flow
movement of a fluid due to a difference in pressure between two locations - from high pressure to low pressure
filtration
a process that separates materials based on the size of their particles; fluid moving out of blood - small molecules pushed out with fluid, but large stuck inside vessel; occurs on arterial end of capillary
reabsorption
process by which water and dissolved substances are taken back into the blood; occurs on venous end of capillary
hydrostatic pressure (HP)
the force exerted by a fluid against the walls of its container
blood hydrostatic pressure (HPb)
Force exerted per unit area by blood on vessel wall; promotes filtration from capillary
interstitial fluid hydrostatic pressure (HPif)
force of interstitial fluid on outside of blood vessel; close to zero in most tissues
net hydrostatic pressure
difference between blood and interstitial fluid hydrostatic pressures; equals HPb - HPif
colloid osmotic pressure (COP)
the pull on water due to the presence of proteins (colloid)
blood colloid osmotic pressure (COPb)
draws fluid into blood due to blood proteins (e.g., albumins); promotes reabsorption (opposes the dominant hydrostatic pressure)' clinically called oncotic pressure
Interstitial fluid colloid osmotic pressure (COPif)
draws fluid into interstitial fluid; relatively low due to few proteins
net colloid osmotic pressure
difference between blood and interstitial fluid osmotic pressures; equals COPb - COPif
Net Filtration Pressure (NFP)
the difference between net hydrostatic pressure and net osmotic pressure; equals (HPb - HPif) - (COPb - COPif)
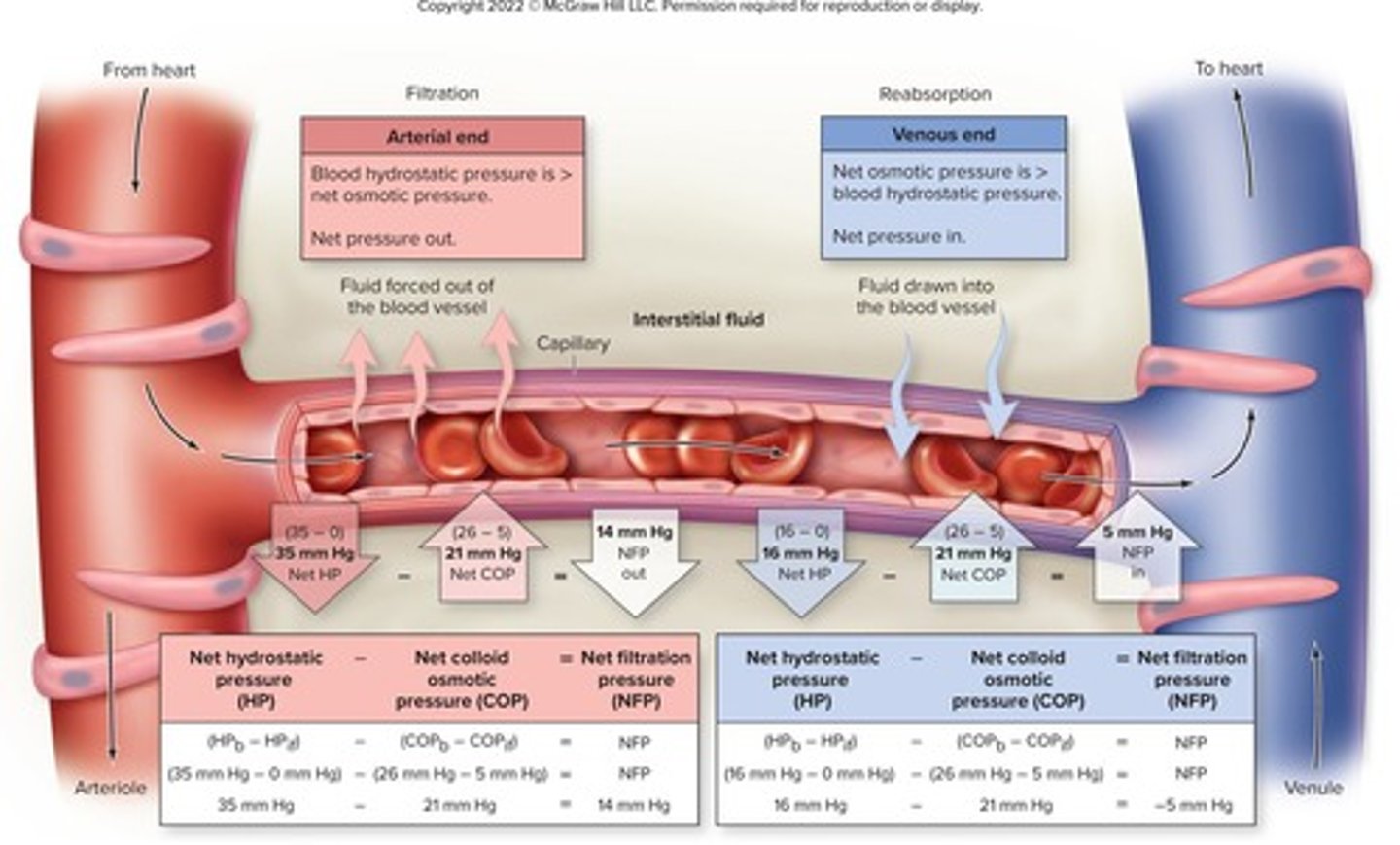
NFP at arterial end of capillary
high; favors filtration
NFP at venous end of capillary
low; favors reabsorption
lymphatic system
the network of vessels that picks up excess fluid from interstitial fluid (that isn't reabsorbed), filters it, and returns it to venous circulation
local blood flow
the blood delivered locally to the capillaries of a specific tissue; dependent on: degree of vascularity, myogenic response, local regulatory factors, and total blood flow
degree of vascularization
the extent of blood vessel distribution within a tissue, determines the potential ability of blood delivery; metabolically active tissues have more vessels
angiogenesis
formation of new blood vessels to increase potential perfusion; seen in muscle in response to increase aerobic training (over weeks/months)
regression
return to previous state of blood vessels; for example when someone that has been doing aerobic training stops training for an extended period (weeks/months)
myogenic response
intrinsic ability of vascular smooth muscle to respond to pressure changes; stretch in arteriole wall due to increased blood pressure causes smooth muscle to contract - returns local flow to original levels; less stretch in wall due to decreased pressure causes smooth muscle to relax - returns flow to original levels
local regulatory factors
alter blood flow based on tissue needs such as when more metabolically active or when tissue is damaged; primarily accomplished with vasoactive chemicals (vasodilators and vasoconstrictors)
vasodilators
in local flow, substances that dilate arterioles and relax pre-capillary sphincters; increases flow to capillary beds
vasoconstrictors
in local flow, substances that constrict arterioles and contract pre-capillary sphincters; decreases flow to capillary beds
autoregulation
the ability of tissues to regulate their own blood supply; when tissue activity perfusion can be inadequate and activity increases substances produced (CO₂, lactic acid H⁺, K⁺) - these substances act as vasodilators; vessels constrict when perfusion has increased due to negative feedback
reactive hyperemia
transient increase in organ blood flow that follows a brief period of disruption
blood flow changes due to tissue damage
inflammation causes release of histamine and bradykinin to cause vasodilation; damage to tissues can cause release of leukotrienes and thromboxanes to cause vasoconstriction - to reduce blood loss
total blood flow
amount of blood transported through the cardiovascular system per unit time; equal to cardiac output; can increase with exercise; proportional to pressure gradient divided by resistance (Pressure/Resistance); increases as pressure increases; decreases as resistance increases
blood pressure
the pressure that is exerted by the blood against the walls of blood vessels; highest in the arteries where it fluctuates between two pressures; typically recorded as systolic/diastolic pressures; lowest in veins
blood pressure gradient
the change in blood pressure from one end of a blood vessel to its other end; driving force to move blood through vasculature; increased by increased cardiac output
arterial blood pressure
measure of the pressure exerted by the blood as it flows through the arteries; pulses with cardiac cycle
systolic pressure (SP)
blood pressure in the arteries during contraction of the ventricles (during systole); highest pressure generated; recorded as upper number in blood pressure ratio
diastolic pressure (DP)
blood pressure in the arteries during relaxation of the ventricles (during diastole); lowest pressure generated; recorded as lower number in blood pressure ratio
pulse pressure (PP)
pressure added to the arteries due to contraction of the heart; equals difference between systolic and diastolic pressures (SP- DP)
pulse
beat of the heart as felt through the walls of the arteries
mean arterial pressure (MAP)
average arterial blood pressure across entire cardiac cycle; provides index of perfusion (<60 may indicate insufficient blood flow); equal to diastolic pressure + 1/3 of pulse pressure (DP + (1/3*PP))
capillary blood pressure
high enough for exchange of substances, low enough to not damage tissues; higher on arterial end (favors filtration) and lower on venous end (favors reabsorption)
venous return
The amount of blood returned to the heart by the veins; depends on pressure gradient, skeletal muscle pump, respiratory pump, and valves
skeletal muscle pump
pumping effect of contracting skeletal muscles on blood flow through underlying vessels
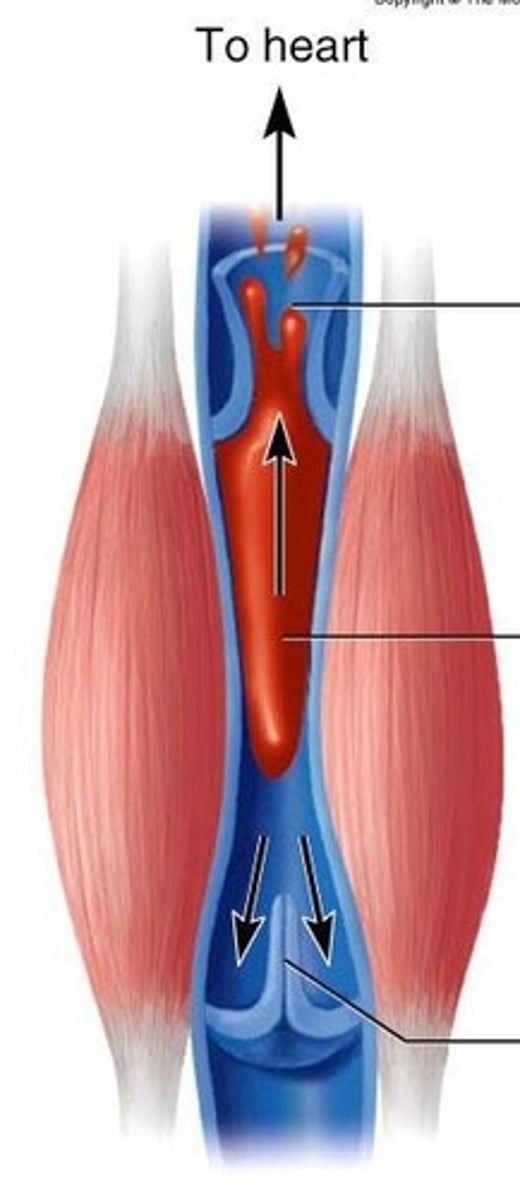
vein valves
prevent backflow of blood in veins

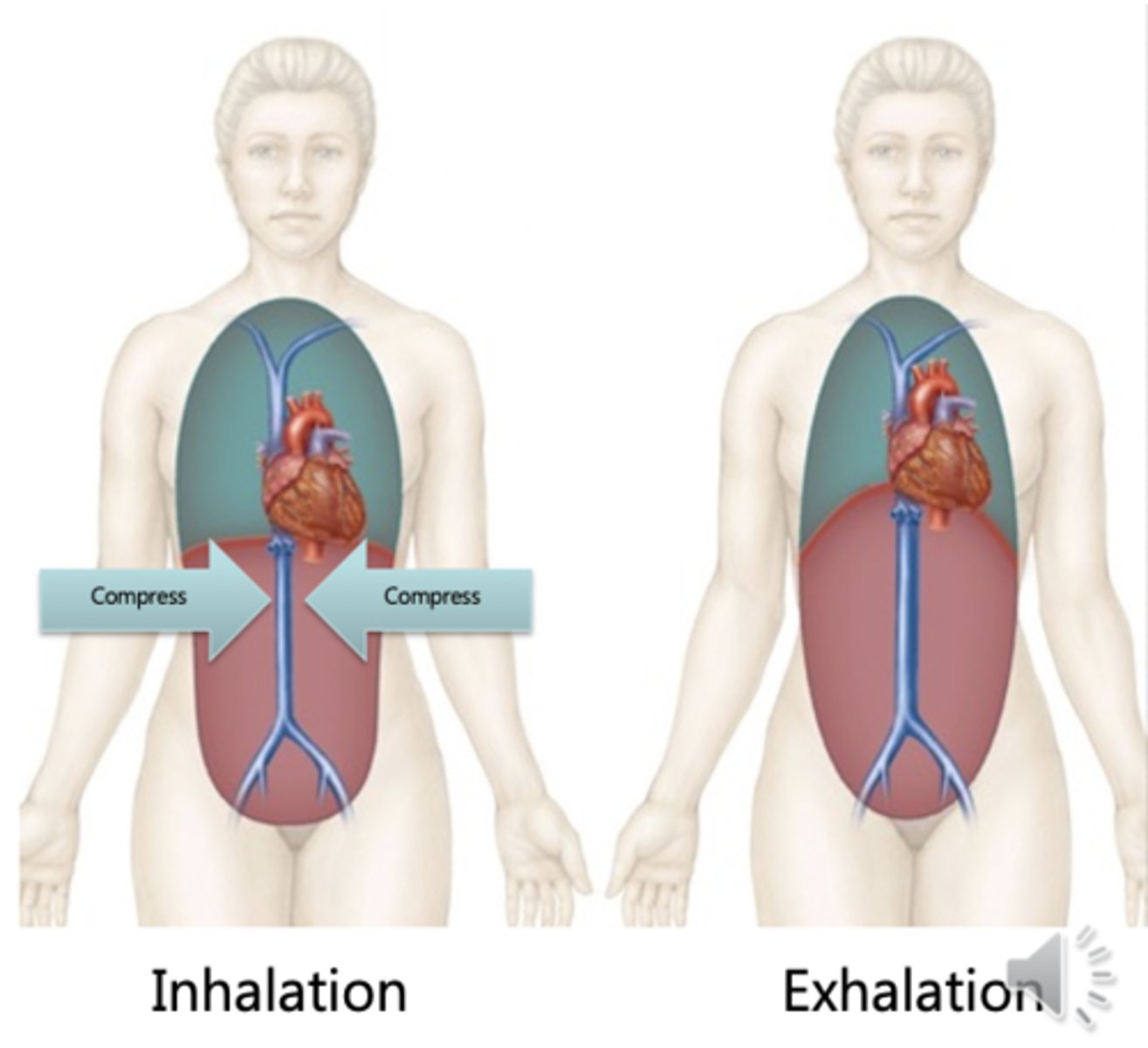
respiratory pump
cycling pressure changes during breathing move blood toward heart by squeezing abdominal veins as thoracic veins expand; in inspiration, abdominal pressure increases and blood forced up from abdominal area into thoracic area; in expiration, abdominal pressure decreases and blood from lower limbs allowed into abdominal veins (like when taking kink out of hose) - thoracic pressure also increases causing blood to be pushed into heart from this area
resistance
friction the blood encounters as it moves through the vessels; due to contact between blood and vessel wall; opposes blood flow; affected by viscosity, vessel length, and lumen size
blood viscosity
resistance of fluid to its flow; greater thickness is greater viscosity, which raises resistance; depends on percentage of particles in fluid - increases with increases in plasma proteins or formed particles; decreases with anemia; increases with dehydration
vessel length
the farther liquid travels through a tube, the more cumulative friction/resistance it encounters; typically remains constant but can changes with weight changes; pressure and flow also decline with distance
vessel radius
half the diameter of the lumen of a vessel; smaller lumen has more resistance, less flow
relationship between flow, pressure, and resistance
flow = pressure/resistance; as pressure increases, flow increases (as pressure decreases flow decreases); as resistance increases, flow decreases (as resistance decreases, flow increases)
autonomic reflexes of blood pressure
regulate blood pressure short-term; components: change in blood pressure/stretch of vessel (stimulus) → baroreceptors (sensory receptors) → sensory neurons → cardiovascular center (control center) → motor neurons of ANS → heart and blood vessels (effectors)
blood pressure primarily involves baroreceptor reflex, but can be influenced by chemoreceptor reflex
baroreceptor reflex
the primary reflex pathway for homeostatic control of blood pressure
decreased blood pressure (reduced stretch of vessel wall) → reduced baroreceptors activation → increase in sensory nerve signals → activation of cardioacceleratory center and vasomotor center in brain; inhibition of cardioinhibitory center → increase in sympathetic nerve signals and decrease in parasympathetic nerve signals → increased heart rate, increased stroke volume, and increased vasoconstriction
increased blood pressure (increased stretch of vessel wall) → increased baroreceptors activation → decreased sensory nerve signals → activation of cardioinhibitory center and decreased activation of cardioacceleratory center and vasomotor center→ increase in parasympathetic nerve signals and decrease in sympathetic nerve signals → decreased heart rate, decreased stroke volume, and decreased vasoconstriction
vasomotor center
Clusters of neuron cells bodies located in medulla oblongata that control blood vessel diameter; acts together with cardiac centers to integrate blood pressure control; sends only sympathetic signals
chemoreceptor reflexes
respond to changes in chemical composition of blood, particularly pH and dissolved gases; high carbon dioxide and low pH stimulate chemoreceptors and vasomotor center - increases BP and shift blood to lungs to expire carbon dioxide which helps raise blood pH
blood volume
the total amount of blood circulating within the body; influenced by fluid intake, output, and retention; can be influenced by hormones
hormonal regulation of blood pressure
used to help maintain blood pressure long-term
-Renin-angiotensin system
-Aldosterone
-Antidiuretic hormone (ADH)
-Atrial natriuretic peptide (ANP)
renin-angiotensin system
low blood pressure or sympathetic activated → renin (kidneys) released → inactive angiotensinogen (release from liver into blood) activated into angiotensin I → angiotensin-converting enzyme (ACE) converts angiotensin I to the activated angiotensin II → angiotensin II causes vasoconstriction, stimulates thirst and reduced urine output to increase volume, and stimulates release of ADH and aldosterone → raises blood pressure
antidiuretic hormone (ADH)
hormone produced by hypothalamus and stored/released from the posterior pituitary gland; release stimulated by increased blood concentration or angiotensin II; increases water reabsorption in kidneys (decreases urine output), stimulates thirst, and causes vasoconstriction to raise blood pressure
aldosterone
released from adrenal cortex in response to decreases in sodium levels or angiotensin II; increases absorption of sodium ion and water (decreases urine output)
atrial natriuretic peptide (ANP)
hormone secreted from atrial cells of the heart in response to stretch of atrial walls due to an increase in blood volume; stimulates vasodilation and increases urine output
sphygmomanometer
blood pressure cuff; typically used to measure blood pressure at the brachial artery
hypertension
chronically elevated blood pressure; may lead to damage in blood vessel walls
atherosclerosis
condition in which fatty deposits called plaque build up on the inner walls of the arteries