Immunology
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
21 Terms
What happens to the balance between anti- and pro-inflammatory cytokines with increasing weight
Shift to more pro-inflammatory cytokines
What type of adipose tissue (location) is more inflammatory?
Visceral adipose tissue is more inflammatory compared to subcutaneous adipose tissue.
What can happen to the size of adipocytes in individuals with obesity?
An enlargement of adipocytes can happen in obesity.
In general what happens to the secretion level of leptin and adiponectin from adipocytes in individuals with obesity?
Increased secretion on leptin
Decreased secretion of adiponectin
With increasing body weight adipocytes can become insulin resistant - what effect would this have on FFA stored in adipocytes?
Release of FFA from insulin resistant adipocytes
With increasing body weight what can happen in the muscles? (regarding lipids and insulin)
Lipid accumulation and insulin resistance
Obesity typically lead to chronic low-grade inflammation in adipose tissue - mention three common pro-inflammatory cytokines which are released from adipose tissue.
TNF-α, IL-6, and MCP-1
Which chemokines/cytokines are central for the development of atherosclerosis?
Leptin
TNFalfa
MCP-1
IL-6
Adiponectin (protect agenst atherosclerosis)
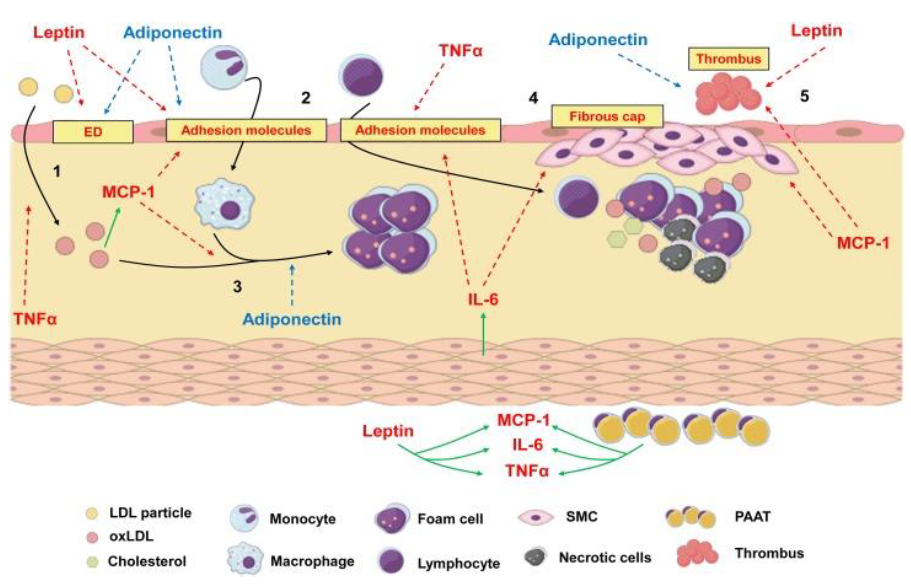
Explain how the central chemokines/cytokines are involved in the development of atherosclerosis.
TNFalfa is releast from adipose tissue (AT) and immune cells and it acts on endothelial cell → dysfunction cells → easier for LDL to pass the endotheial cell layer. TNF alfa stimulat at the same time adhesion molecules that stimulat lymphocyte and monocyte and that end with inflammation
MCP-1 is releast from AT. MCP-1 stimulat monocyte to come and convert them to macrophages there will eat the oxidised LDL and thereby they will be form cell. The form cell will increase the inflammation and promote the plaque formation. MCP-1 promoter also the thrombus formation.
IL-6 is also releast from AT. IL-6 stimulates immune cell activation and the formation of plaque in that way they stimulat the smooth mucsle cell.
Leptin is releast from AT. Leptin stimulat monocytes and macrophages activiti. That increase the inflammation and promote plaque and thrombus formation.
Adiponectin inhibit the macrophages and therefor minimis form cells and inflamation. Adiponectin promote endothelial cell function and “inhibit” recrutation of monocytes.
Simpel answer: (from Chat)
LDL infiltration into the vessel wall initiates inflammation.
TNF-α and MCP-1 recruit monocytes, which differentiate into macrophages.
Macrophages engulf oxLDL, forming foam cells, leading to plaque growth.
IL-6 and TNF-α further promote inflammation, leading to plaque instability.
Leptin exacerbates inflammation, while adiponectin counteracts it.
Thrombosis occurs upon plaque rupture, increasing the risk of heart attacks
What are cytokines?
Small proteins which send signals to the immune system and are responsible for communication between cells
They can be both pro- and antiinflammatory
They regulate immunity and inflammation
What are chemokines?
Small signaling proteins - a subgroup of cytokines
Primarily regulate immune cell migration and traficking
What are adipokines?
Inflammatory molecules released by adipocytes/Cytokines released by adipose tissue
They recruit immune cells, primarily macrophages, which contribute to inflammation
Examples: Leptin, resistin, TNF-alpha
Mention some adipokines that promote insulin resistance
Pro-inflammatory cytokines such as
TNF-alpha
IL-6
Resistin
Leptin (at high levels)
How does TNF-alpha and IL-6 contribute to insulin resistance?
Normally, when insulin binds to its receptor, IRS-1 is phosphorylated on tyrosine residues, which activates insulin signaling and promotes glucose uptake.
TNF-α and IL-6 activate inflammatory pathways (e.g., JNK, NF-κB), leading to serine phosphorylation of IRS-1 (instead of tyrosine phosphorylation), which impairs insulin receptor activation.
In addition, TNF-alpha and IL-6 increase free fatty acid (FFA) release, which disrupts glucose metabolism.
How does high leptin levels contribute to insulin resistance?
Normally leptin levels:
Induce satiety
Regulate fat metabolism together with insulin
High leptin levels (as can be seen in obesity) can induce leptin resistance thereby not regulating appetite by inducing satiety.
High leptin levels are pro-inflammatory and also impair insulin signalling - making cells insulin resistant.
What role does resistin play in the development of insulin resistance?
Resistin promotes insulin resistance by increasing inflammation and hepatic glucose production.
Which adipokines can improve insulin sensitivity?
Anti-inflammatory cytokines such as
Adiponectin
Omentin
SFRP5
How does adiponectin improve insulin sensitivity?
Enhances AMPK activation, promoting glucose uptake and fatty acid oxidation.
Suppresses TNF-α and IL-6 production, reducing inflammation.
How does omentin and SFRP5 improve insulin sensitvity?
They improve insulin sensitivity by suppressing inflammation and oxidative stress.
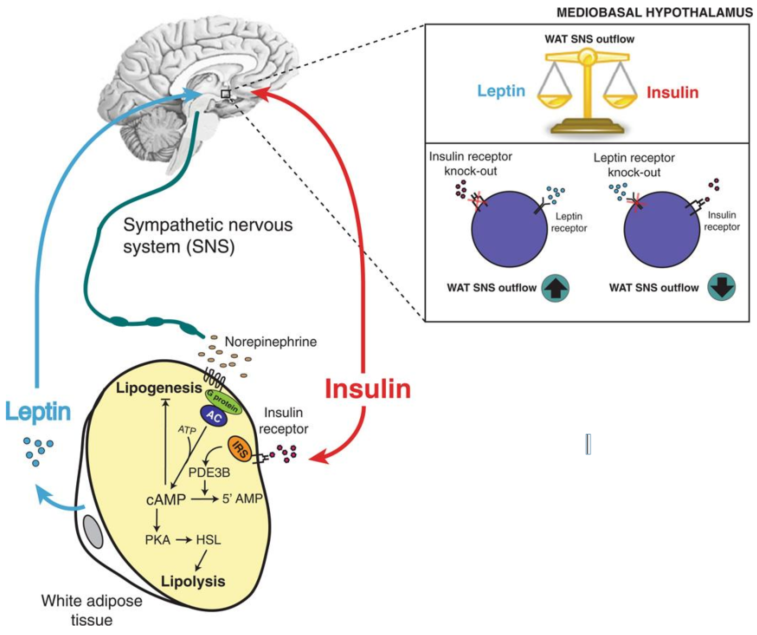
Explain this figure
The figure illustrates the interaction between leptin and insulin in regulating white adipose tissue metabolism via the sympathetic nervous system.
Leptin and insulin coordinate fat metabolism through neural and hormonal pathways ensuring energy homeostasis in white adipose tissue:
Leptin signals to hypothalamus that release norepinephrine to the white adipose tissue promoting lipolysis (fat breakdown)
Insulin promotes lipogenesis (fat storage).
Thereby the two; leptin and insulin balance each other.
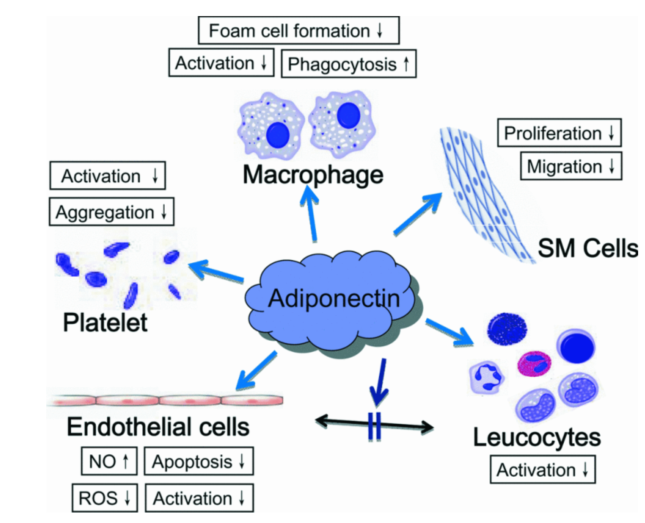
How does adiponectin play a role in atherosclerosis?
Adiponectin
increase NO production in the endothelial cells - good for the endothelial function.
decrease formation of foam cells
Increase macrophage phagocytosis - the engulfment, digestion and destruction of pathogens, dead cells and debris by macrophages
Decrease smooth muscle cell proliferation and migration - good: if too much migrates to the intima the vessel will narrow a lot!
Protects against thrombus formation by decreasing platelet activation and aggregation