Perceptual Disorders Post Stroke: Pusher Syndrome and Spatial Neglect
1/86
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
87 Terms
what is Pusher Syndrome?
leaning and active pushing toward the hemiplegic side with no compensation for the instability, and resistance to passive correction toward midline
what are 4 other names for pusher syndrome?
“ipsilateral pushing”, “contraversive pushing”, “pushing behavior” and “lateropulsion”
pushing occurs in the _______ plane
frontal
- tilt to side
we must consider the direction - low brainstem stroke push ______ due to vestibulospinal disorders
ipsilesionally
is lateropulsion more prevalent in supratentorial or infratentorial?
infratentorial
lateropulsion prevalence decreases from ____ to late _____ phase
acute ; subacute
clinical demographics: Typically ______ hemispheric lesions
R > L
clinical demographics: what part of the brain is effected during pusher syndrome?
posterolateral thalamus
clinical demographics: individuals with ______ impairments and severe _____
hemisensory; neglect
Presence of "lateropulsion" after stroke is associated with what 3 things?
- Need for longer rehabilitative stay*
- Reduced functional outcomes
- Decreased likelihood of Discharge home
time to recovery from pusher syndrome differed based on number of ____
deficits
- vision, neglect, sensation, motor
prognosis: few still "push" ____ months post stroke although with newer activities, you may see mild return of this behavior
6
- transition to outside walking from only inside
prognosis: given an additional ____-____ weeks in rehab, people with post-stroke lateropulsion can achieve functional improvements similar to those without lateropulsion
3-4
people with pusher syndrome believe there is a ______ of body orientation to gravity
misperception
Subjective perception of body as oriented upright when tilted _____ degrees tot he _____ side
18; ipsilesional
"impaired ________ __________" or "graviceptive neglect"
truncal graviception
in pusher syndrome, the body does not align with ____ ____
visual vertical
in pusher syndrome, they have a feeling of ________ _______ when transitioning - if they feel "secure" pushing will decrease
losing balance
the posterior thalamus and extra-thalamic structures are needed for intact processing of ______ and control of ______ body posture
gravity ; upright
what are the 6 extra-thalamic structures?
- inferior frontal gyrus
- middle temporal gyrus
- precentral gyrus
- inferior parietal lobe
- parietal white matter
- superior longitudinal fasciculus
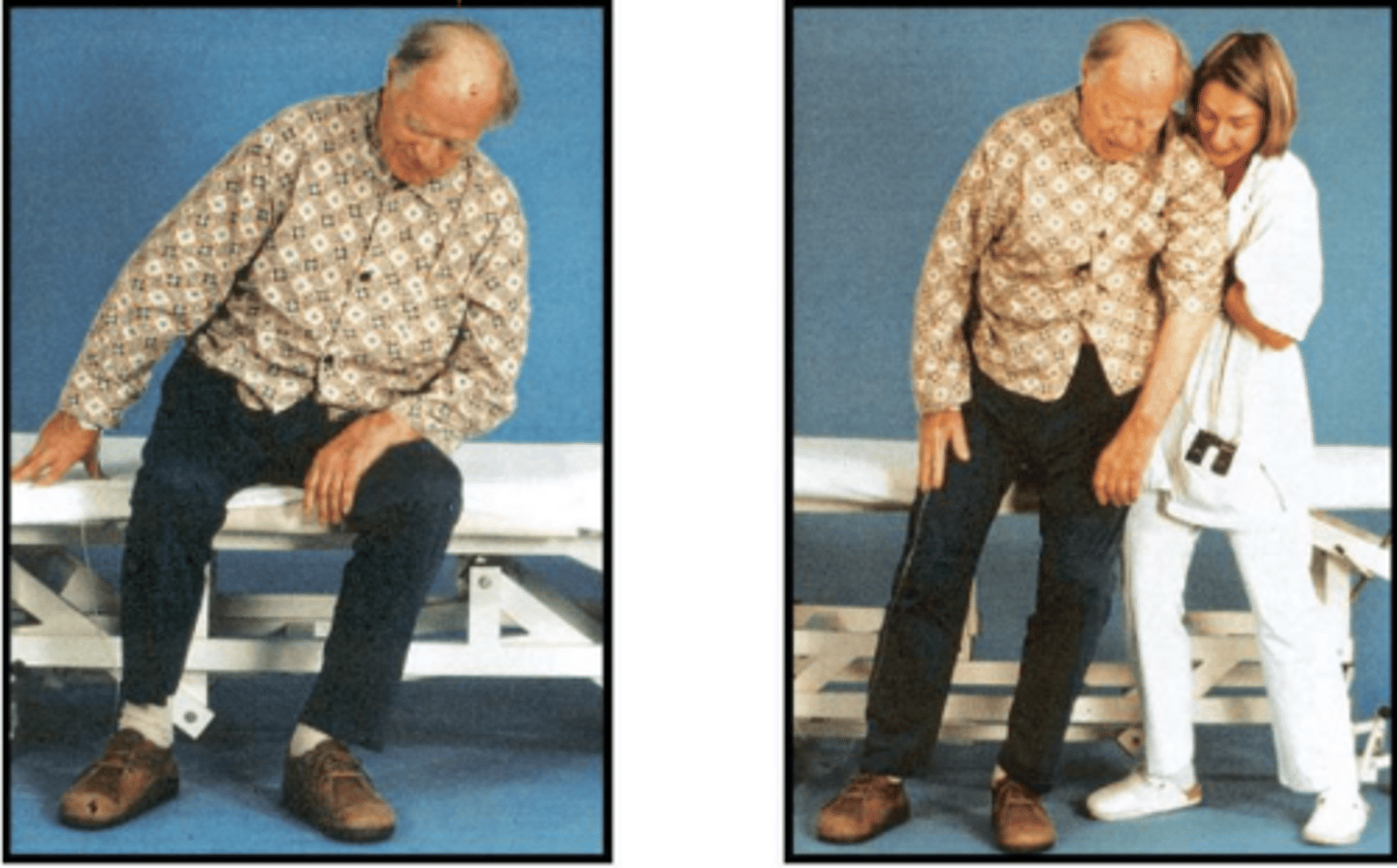
what are 5 big points when it comes to the presentation of pusher syndrome?
- Lateral tilt towards contra-lesional side in sitting and standing
- Abduction and extension of non-paretic extremities when in physical contact with a surface
- Resistance to any attempt at passive correction
- Are unaware they are not upright (18 degree tilt)
- Ability to maintain head in vertical with severe lateral lean

4 possible DDx for pusher syndrome =
- Typical Hemiplegia
- Listing phenomenon
- Ipsilesional Lateropulsion
- Thalamic astasia
what does someone with Typical Hemiplegia do?
- Will recognize that they are falling but can't stop falling because of their weakness
- Will try and use their "less affected" hand to pull themselves to prevent the balance loss
- Healthy respect/fear of falling to the hemiplegic side
what is Listing Phenomenon?
Loss of balance toward hemiparetic side
- Patient's trunk "lists" toward affected side
- Patient will attempt to hold onto something or utilize non-paretic hand to prevent loss of balance
what is "Lateropulsion" (ipsilateral)?
Tendency to fall sideways frequently seen in Wallenberg's syndrome
- Falls to the side of lesion
- No active pushing or Resistance to passive correction
what is Thalamic Astasia?
Unable to stand unsupported
- Fall backward or to affected side when left unsupported
- During Supine/Sit will utilize UE's to pull up
- No pushing or active resistance to correction
when during the assessment of pusher syndrome will you see their presentation increase?
transitions
2 outcome measures for pusher syndrome =
- Standardized Scale for Contraversive Pushing
- Burke Lateropulsion
who is the scale for contraversive pushing designed for?
Designed to classify patients based on severity of behavioral and clinical impairments
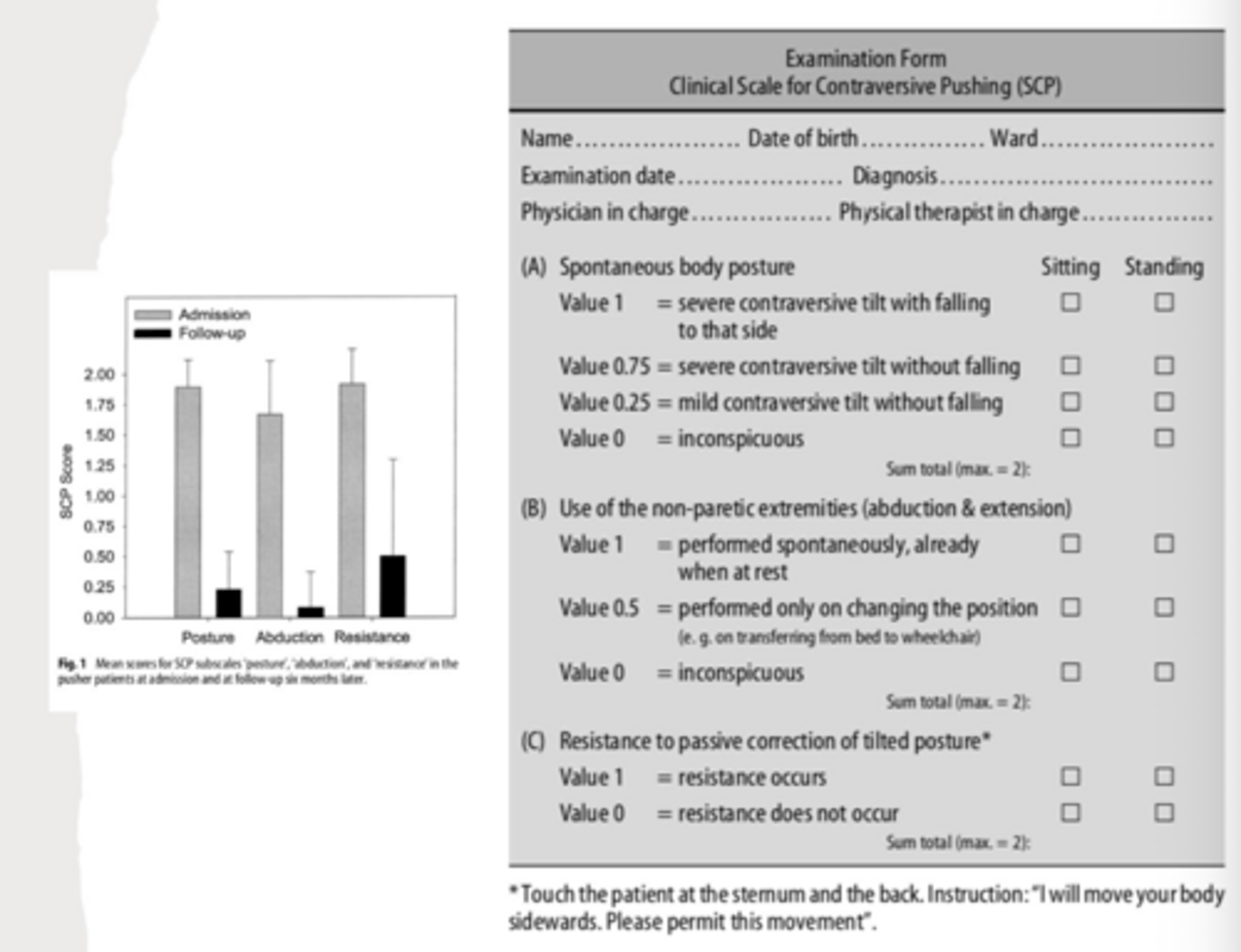
Scale for Contraversive Pushing assesses what 3 things?
- posture: symmetry of spontaneous posture while sitting and standing,
- extension: the use of the ipsilesional arm or leg to extend the area of physical contact to the ground while sitting and standing
- resistance: resistance to passive correction of posture while sitting and standing.
scoring of the scale for contraversive pushing =
- 2 points maximum per section and total of 6 points
- Higher score is more impaired
- clients are scored as possessing contraversive pushing if all 3 criteria are present, reaching a total score of at least 1 for each criterion
what does the burke lateropulsion scale assess?
"contraversive lateropulsion" across several functional tasks
who is the burke lateropulsion scale more sensitive for?
mild pusher behavior in standing and walking
scoring of the burke lateropulsion scale =
- Scoring based on the degree and point of onset of resistance to passive correction (sit, stand) or degree of pushing evident (supine, transfer, walking): The greater the resistance noted by the therapist, the higher the score.
- HIGHER IS MORE IMPAIRED
- Cutoff score of of ≥3 correlates with severe balance impairments and impaired perception of vertical in frontal plane
what are 3 different treatment approaches for pusher syndrome?
- restore head control, stimulate activity in lateral trunk flexors on affected side, regain midline in standing and walking, regain stair climbing
-treatment in "earth-vertical" - leverage visual feedback
-some individuals are unable to appropriately utilize visual input- impaired visual vertical and neglect
pusher syndrome treatment: due to limited research evidence, the panel does not recommend routine use of what 8 things?
- Video games referring to horizontal/vertical.
- Virtual reality training.
- Transcranial direct current stimulation.
- Functional neuromuscular electrical stimulation.
- Transcutaneous electrical nerve stimulation applied to the contralesional side of the neck.
- Whole-body tilt apparatus.
- Force platform bio-feedback.
- Recumbent stepper.
what are 5 specific rehab strategies for pusher syndrome?
- Task specific training
- Early orientation to upright
- Address additional perceptual impairments
- Modify positions throughout day
- Somatosensory cuing
Pusher Syndrome Static Seated Treatment includes =
- visual cues to midline
- sensory feedback
- Eliminate ipsilesional extremity
Pusher Syndrome Static Standing Treatment includes =
- Visual cues to midline
- sensory feedback and elevated heights for external cue.
- block pushing with bolster/wall etc. - Eliminate ipsilesional
extremity
Pusher Syndrome Dynamic Seated Treatment includes =
- Move in/out of midline
- Trial varied positions
- Eliminate/Use ipsilesional
Pusher Syndrome Dynamic Standing Treatment includes =
- Reaching, stepping
- step-ups
- Functional transfers- Face the surface
- Eliminate/Use ipsilesional
- BWSTT*
what is the goal of pusher syndrome treatment?
to self-identify body position in relation to midline
what are 4 things we must think about when it comes to pusher syndrome and wheelchair positioning/mobility?
- Need appropriate seating system
- Supportive cushion and backrest for midline
- Pelvic positioning
- Scanning and visual tape to improve awareness with neglect
what is Spatial Neglect?
inattention to stimuli in the contralesional space
- Not intentional or conscious
- Not attributed to primary sensory or motor deficits
spatial neglect is a heterogenous disorder with various subtypes, what are the 2?
- distinct spatial regions
- spatial attention deficits
what are examples of distinct spatial regions when it comes to spatial neglect?
personal, peripersonal or extrapersonal
what are examples of spatial attention deficits when it comes to spatial neglect?
person-centered (egocentric) vs stimulus centered (allocentric)
spatial neglect is usually an injury to which hemisphere?
right hemisphere > left hemisphere
patients with stroke present with neglect in the _____ phase
acute
Spatial Neglect is a stronger predictor of what post stroke?
dependence than paralysis or communication disability
what are some persistent symptoms for those who experience spatial neglect?
- reduced independence in IADL
- fall risk (6.5x more)
what is someone with spatial neglects average LOS in rehab?
10 days more
those with spatial neglect are 45% less likely to go _____ post IRF
home
many people experiencing spatial neglect are unaware of what 2 things?
- their symptoms
- consequences of deficits (anosognosia)
the damaged neural networks with spatial neglect are critical for spatial _____ and _____ orientation
processing ; attention
in spatial neglect, damage to the neural networks typically involve ____ hemispheres
both
- each hemisphere pays more attention toward contralateral side of space and deploys more processing resources to contralateral space
with injury - _____ hemisphere is more activated than _____ hemisphere, resulting in excessive bias - "neglecting" the _____ side
intact ; injured ; contralateral
what does it mean if someone has personal space symptoms with spatial neglect?
body parts or body surface
- ex. Shave only R side of face
what does it mean if someone has peri-personal space symptoms with spatial neglect?
within arms reach
- Ex. Difficulty finding utensils on the L side of the food tray
what does it mean if someone has extra-personal space symptoms with spatial neglect?
beyond arms reach
- ex. Overlooking furniture or people across the room on L side
what does it mean is someones symptoms are ego-centric with spatial neglect?
body-centered/viewer-centered
- Individuals make errors/omissions on L side
- Typically focused on more in research- Greater disability risk
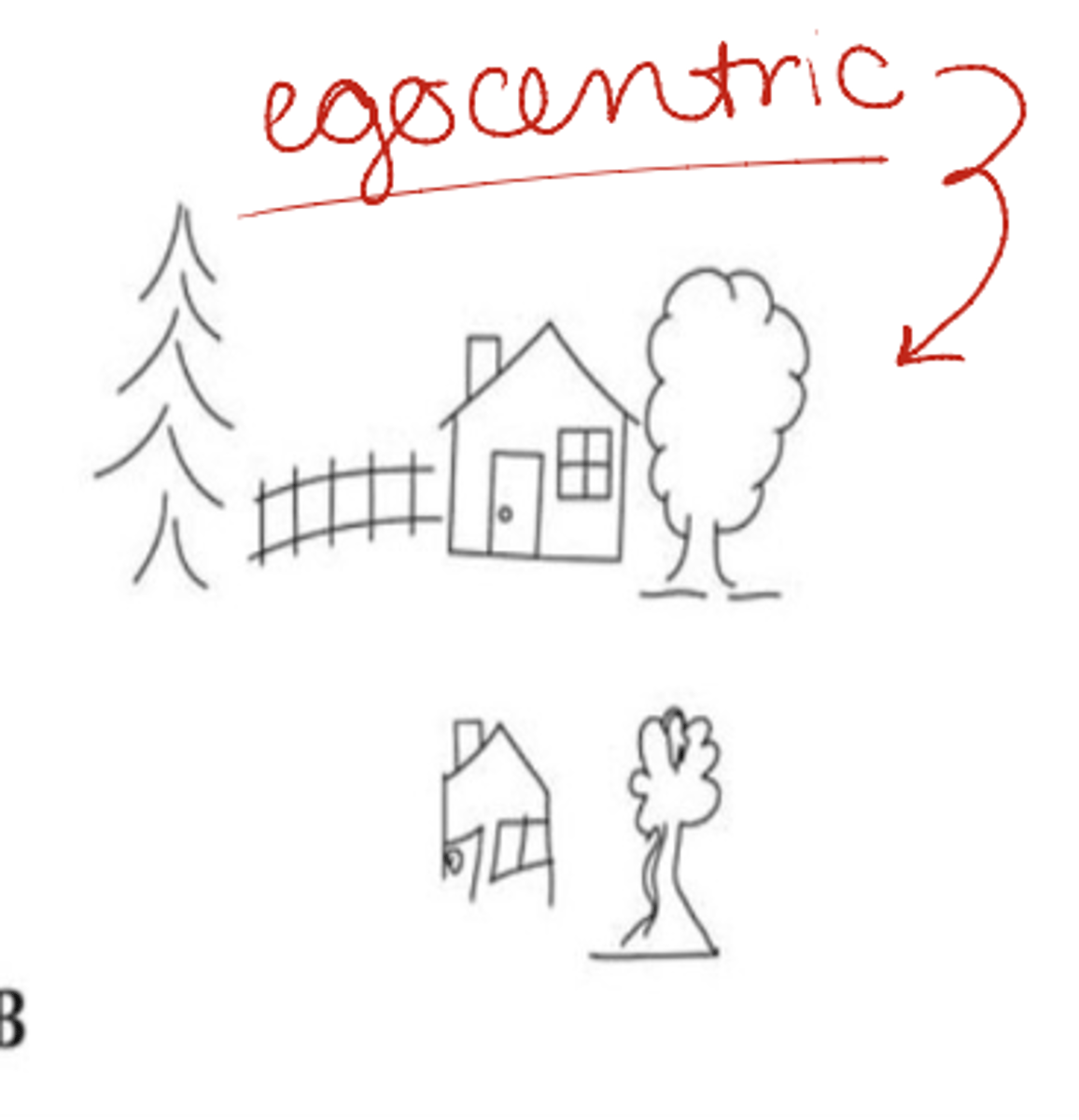
what does it mean if someones symptoms are allocentric with spatial neglect?
stimulus-centered/object centered
- Errors on the L side of an object, regardless of position relative to the individual

what are visual field cuts in someone with spatial neglect?
loss of vision (hemianopia) or 1 quarter (quadrantanopia) of the visual field
- SENSORY deficit caused by damage to the retina, primary visual cortex and corresponding pathways
- Remains consistent across tasks
spatial neglect is a ______ syndrome, caused by damage to the attention neural networks
neuropsychological
oculomotor symptoms of spatial neglect are not related to ____ processing, but instead are related to ability to control _____ or _____ movement
visual ; gaze ; eye
oculomotor symptoms of spatial neglect may vary depending on what 3 things?
- task
- alertness
- cognitive capacity, etc!
what is the clinical presentation of someone with a R sided lesion, L sided neglect?
- Propensity to gaze toward R at rest or shift gaze R
- Responds to R when approached from L
- Tilt in W/C or sit with head and eyes turned R
- Difficulty caring for L arm and Leg
- Unable to use or lift arm spontaneously
- Miss words on L side of sentence
- Struggle to locate items on L or place items to L
- Difficulty avoiding objects on L
- Lack awareness or concern about weakness on L
- Appear unfazed when encountering obstacles during a task, unable to explain the issue
_____ detection of spatial neglect is necessary to improve outcomes
early
currently there is no ____ ____ for how to screen, assess, or diagnose spatial neglect
gold standard
what are 3 outcome measures for spatial neglect?
Behavioral Inattention Test:
- (BIT-C)Conventional subtest: 6 paper-based tests
- Measures impairment level in peri-personal space
Catherine Bergego Scale:
- Measures impact at functional level in a range of daily
Kessler Foundation Neglect Assessment Process
- a component of the CBS
what are other, not as fancy, outcomes measures you can use with spatial neglect?
- Object drawing
- Figure copying
- Target cancellation
- Line Bisection Test
- Text Reading
- Extinction in visual, tactile, auditory and motor
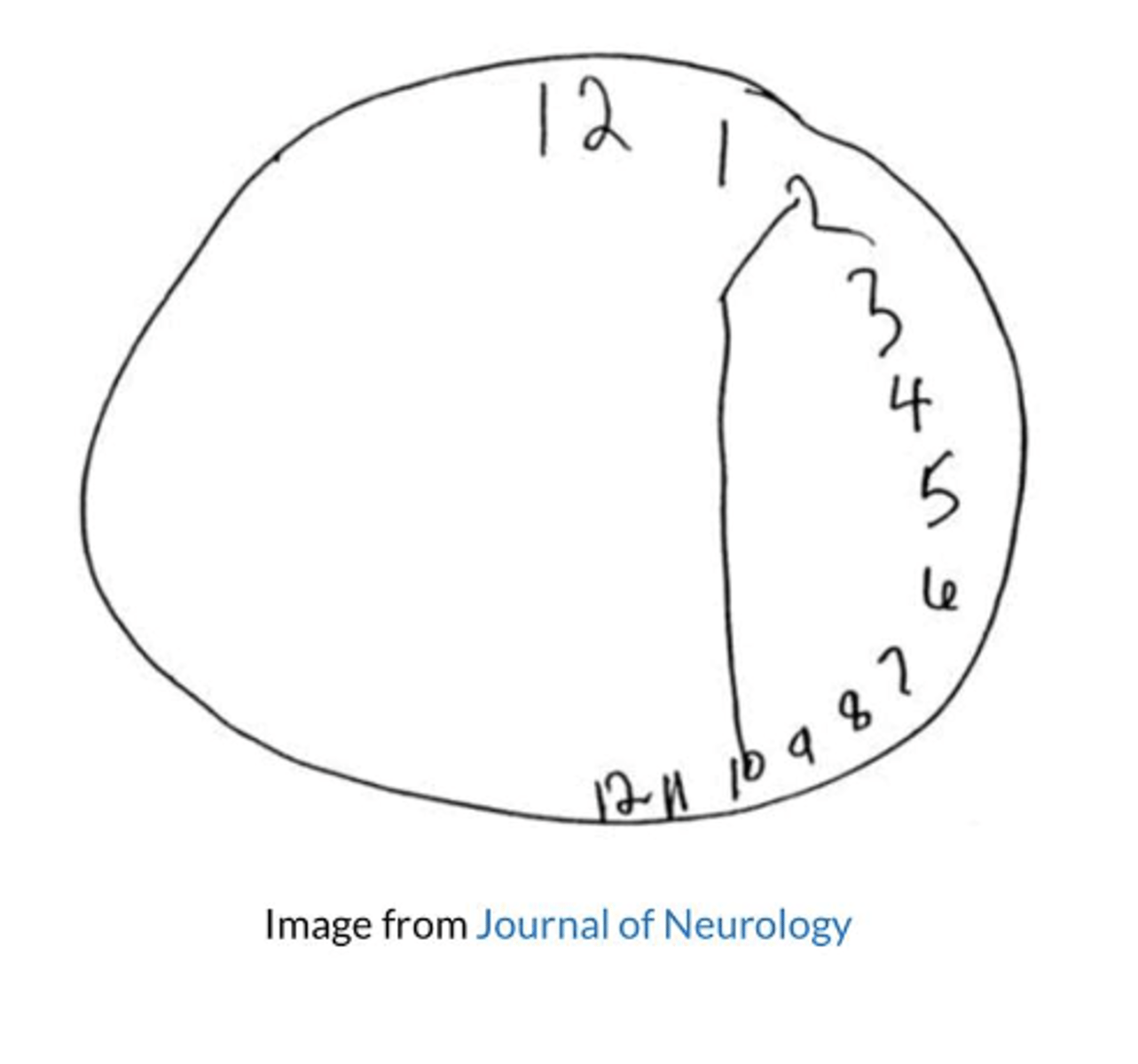
what is the clock drawing test outcome measure for spatial neglect?
- Quickly assesses visuospatial and praxis abilities, and may determine the presence of both attention and executive dysfunctions
- Versions: verbal command; copy command; time setting instructions
- Scoring: no standardized system available but looking for errors
- Need paper and pencil
what is the single letter cancellation test (SLCT) outcome measure for spatial neglect?
- Evaluate the presence and severity of visual scanning deficits, and is used to evaluate unilateral spatial neglect
- Paper and Pencil Test; one 8.5″x11″ sheet of paper containing 6 lines with 52 letters per line
- Cancelling the letter "H"; misses from total available

what are 5 possible interventions for spatial neglect?
- Behavioral
- rTMS
- Virtual reality
- Robot assistance
- Prism adaptation
what is the visual perception and self-monitoring intervention for spatial neglect?
- Most often verbally mediated
- May use visual perception and monitoring intended for self-implementation
- Training of visual awareness
- Mental imagery- Ex. "lighthouse" strategy
- Videotaped feedback
what are ways you can integrate mobility training in interventions with spatial neglect?
- Early standing with trunk rotation to the left
- Use of a standing frame with left-sided environmental interactions
- Combine with reading activities for scanning
- Use of weight bearing with scanning and rotation
- Can use locomotion device for safety purpose
what are ways you can integrate functional training in interventions with spatial neglect?
- Incorporate self cueing/attention training
- Can force activity to the left side of space -remapping effects
- Use of scanning in ADL training - eating, reading, grooming
when documenting spatial neglect, you want to support the ______ movement system, with what the client is able to accomplish
whole
- "Unable to move head or eyes past midline without verbal cues."
- "Gait training for 120 feet with min assist due to difficulty with obstacle negotiation on the L side of space resulting in Loss of Balance"
no _____ specific to spatial neglect to improve symptoms
medications
what 6 medications do we for sure NOT want to use with spatial neglect?
- Anticholinergics
- Antidopaminergics
- Sedatives
- Hypnotics
- Phenytoin (Anti-convulsant)
- Benzodiazepines
what are the 3 problems in assessment and treatment of spatial neglect?
1. Many have intact ability to perceive, attend to and represent the external spatial environment (WHERE functions) but may have spatially biased motor output errors (AIMING functions)
2. Training conscious strategies may be ineffective for spatial motor-intentional "AIMING"
3. Studies which lump together spatial neglect symptoms may impact results and treatment recommendations
what is "where" (visual perceptual) spatial neglect?
Perceptual -attentional and representational network mediates directional spatial awareness, vigilance, estimation and imagery
what is the "aiming" (motor-intentional) spatial neglect?
a dysfunction in initiation/execution of motor-intentional behavior
resulting in hypokinetic and hypometric leftward movement.
- Motor-intentional network mediates directional action, response inhibition, motor regulation.
how do we detect "where" (visual perceptual) spatial neglect?
- Visual-perceptual: visual extinction to stimuli, visual search tasks
- Mental imagery/internal representation deficits -Ex. Mental number line, or a map
how do we detect "aiming" (motor-intentional) spatial neglect?
- Asymmetry of body posture and movement and Motor extinction
- Hemispatial hypometria
- Directional hypokinesia- can be eyes, hands or whole body
about prism adaptations and spatial neglect chart
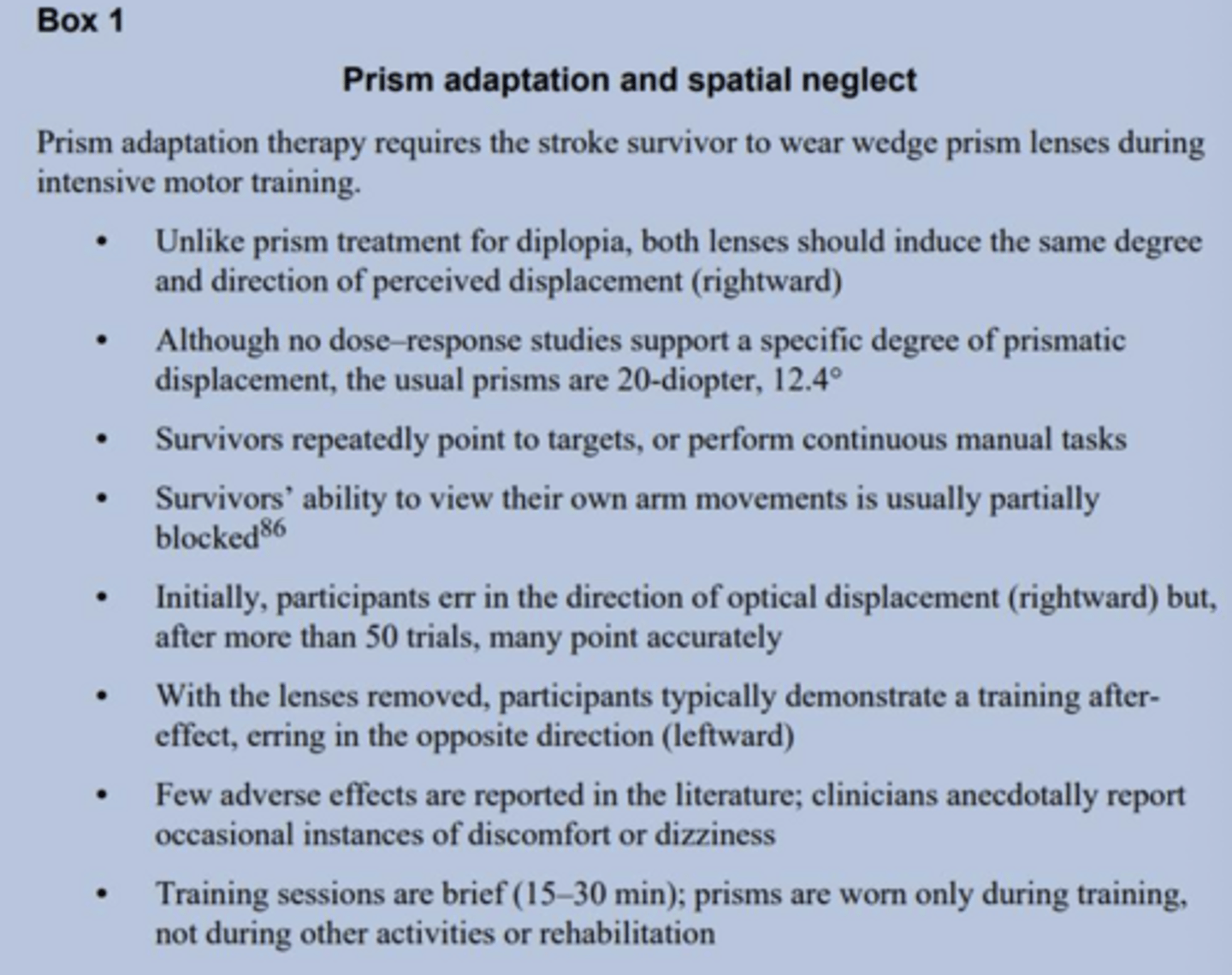
what is prism adaptations in interventions of spatial neglect?
- Experience /Activity dependent task that requires errors in movement.
- Thought to induce a change in perceptual processing from retina object location—>body movement
- Visual information displaced to R results in reaching movements to L
- Results in after effects that generalizes to daily life tasks.