Clover Learning Fluoroscopy
1/168
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
169 Terms
Which of the following terms is often used to describe fluoroscopy imaging?
a. Static
b. Reverse
c. Dynamic
d. Viscous
c. Dynamic
Which of the following are types of cases that would utilize fluoroscopy? (Select three)
a. Upper gastrointestinal (GI) study
b. Urinary studies
c. Cervical spine x-ray
d. Orthopedic surgeries
a. Upper gastrointestinal (GI) study
b. Urinary studies
d. Orthopedic surgeries
What is the primary function of fluoroscopy in medical imaging?
a. Creating real-time, moving images of internal body structures
b. Producing high-resolution, static images of bones
c. Enhancing the visibility of soft tissues in static images
d. Creating 3-dimensional (3D) reconstruction of internal body structures
a. Creating real-time, moving images of internal body structures
How does fluoroscopy differ from traditional radiography in regard to image type?
a. Fluoroscopy produces only static images
b. Fluoroscopy produces images of moving structures
c. Fluoroscopy cannot be used for diagnostic purposes
d. Fluoroscopy is only used in vascular units
b. Fluoroscopy produces images of moving structures
Compared to traditional radiography, a lower milliamperage (mA) is needed during fluoroscopy to:
a. Reduce exposure time
b. Increase image brightness
c. Reduce patient dose
d. Improve image resolution
c. Reduce patient dose
Where is the x-ray tube typically located in a fluoroscopic system with an image intensifier?
a. In front of or above the patient
b. Within the upright bucky
c. Adjacent to the display monitor
d. Behind or beneath the patient
d. Behind or beneath the patient
Which of the following procedures commonly uses fluoroscopy?
a. GI studies
b. MRI of the brain
c. Chest x-ray
d. Mammography
a. GI studies
Healthcare workers can reduce their occupational dose during fluoroscopy procedures by wearing which of the following? (Select three)
a. Lead apron
b. Thyroid shield
c. Sterile gloves
d. Lead gloves
e. Lead curtain
a. Lead apron
b. Thyroid shield
d. Lead gloves
Which of the following components increases the brightness of the fluoroscopic image to ensure it is of diagnostic quality?
a. Collimator
b. Filtration
c. Anti-scatter grid
d. Image intensifier
d. Image intensifier
The exposure time is typically longer in fluoroscopy compared to traditional radiography in order to:
a. Produce higher contrast in the images
b. Reduce the need for patient repositioning
c. Allow for the capture of dynamic, moving images
d. Minimize the use of contrast agents
c. Allow for the capture of dynamic, moving images
The primary function of an R/F room is to perform which of the following?
a. Only radiographic procedures
b. Only fluoroscopic procedures
c. Radiographic and fluoroscopic procedures
d. MRI scans
c. Radiographic and fluoroscopic procedures
In a conventional R/F room, the table is composed of what material?
a. Reinforced plastic
b. Steel
c. Radiolucent material
d. Lead
c. Radiolucent material
In a conventional R/F room, the purpose of the lead curtain is to:
a. Serve as a privacy curtain for the patient
b. Block scatter radiation coming from the patient during fluoroscopy
c. Help enhance the image quality
d. Assist in controlling the temperature of the room
b. Block scatter radiation coming from the patient during fluoroscopy

In a conventional R/F room, the purpose of the Bucky tray is to:
a. House the image intensifier
b. Block primary radiation from reaching the operator
c. Block scatter radiation from reaching the operator
d. Hold an image receptor plate in position for static radiographic images
d. Hold an image receptor plate in position for static radiographic images
What is the purpose of the ceiling-mounted x-ray tube in an R/F room?
a. Capture static radiographic images of patients only at the wall bucky
b. View internal structures in motion
c. Capture static radiographic images of patients using either the table bucky or the wall bucky
d. Capture static radiographic images of patients only at the table bucky
c. Capture static radiographic images of patients using either the table bucky or the wall bucky
How is the x-ray beam activated during a fluoroscopic procedure?
a. Through a dead man switch (e.g. foot pedal or hand exposure switch
b. By adjusting the settings on the viewing monitor
c. By adjusting the height and angle of the ceiling-mounted x-ray tube
d. Because the x-ray beam is continuous in fluoroscopic rooms, there is no need for activation
a. Through a dead man switch (e.g. foot pedal or hand exposure switch
How does the dead man switch differ from the emergency shut-off switch in an R/F room?
a. Dead man switch shuts off the machine in an emergency, while the emergency shut-off activates the x-ray beam
b. Dead man switch is used for radiographic procedures, while emergency shut-off switch is used for fluoroscopic procedures.
c. Dead man switch activates the x-ray beam, while the ER shut-off switch shuts down the entire room
d. Dead man switch is always located on the wall, while the ER shut-off is always located inside the foot pedal exposure control
c. Dead man switch activates the x-ray beam, while the ER shut-off switch shuts down the entire room
Interventional fluoroscopy provides physicians with which of the following?
a. Imaging without the use of radiation
b. Real-time visualization for precise procedures
c. Retrospective images for post-analysis
d. Macroscopic overview of a specific body part
b. Real-time visualization for precise procedures
Which of the following fluoroscopy types is primarily used for diagnostic purposes?
a. Conventional fluoroscopy
b. Interventional fluoroscopy
c. Digital subtraction angiography (DSA)
d. Vascular fluoroscopy
a. Conventional fluoroscopy
What is the purpose of the "smiley face" sticker feature on mobile fluoroscopy systems?
a. Identify the correct C-arm
b. Provide patients with entertainment
c. Assist in correctly orienting the image
d. Indicate the front of the machine
c. Assist in correctly orienting the image
In Fluoroscopy, the function of the image intensifier is to:
a. Enhance the color of the image
b. Reduce patient does
c. Magnify the image size
d. Brighten the fluoroscopic image
d. Brighten the fluoroscopic image
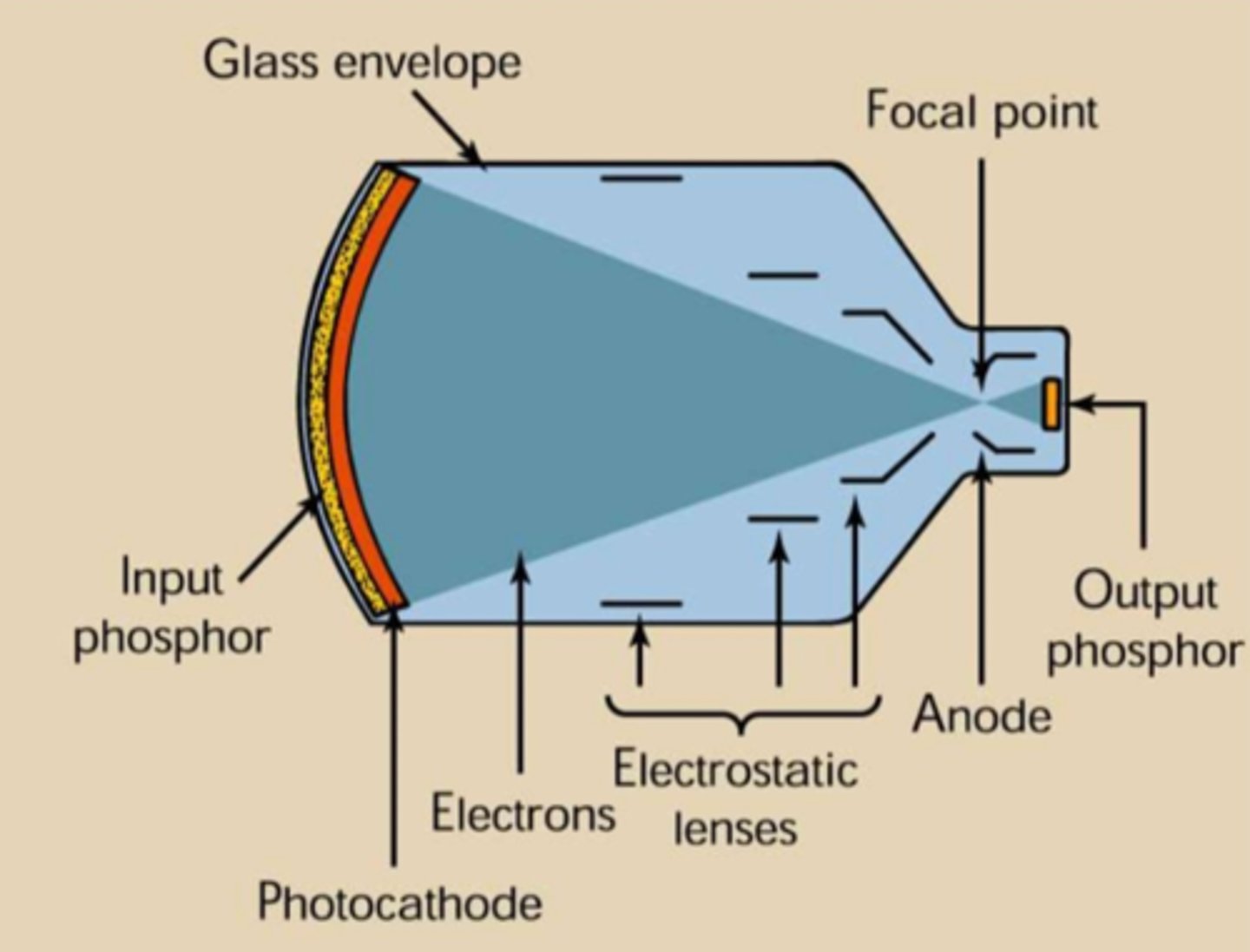
Which two of the following are components of the image intensifier? (Select two)
a. Input phosphor
b. Photodiode
c. Thin film transistor (TFT)
d. Photocathode
a. Input phosphor
d. Photocathode
What is the role of the anti-scatter grid in the image intensifier?
a. Increase image contrast
b. Increase spatial resolution
c. Decrease image contrast
d. Convert x-ray into light photons
a. Increase image contrast
( by absorbing scatter radiation, it reduces the amount of scatter radiation that passes through the input phosphor. )
What is the purpose of electrostatic focusing lenses within an image intensifier?
a. Reduce scatter radiation?
b. Funnel the photoelectrons into a concentrated stream
c. Convert photoelectrons back to light photons
d. Emit photoelectrons through photoemission
b. Funnel the photoelectrons into a concentrated stream
What is the final image intensifier energy conversion that occurs before the visualization of the image on monitor?
a. X-rays to light photons
b. Photoelectrons to light photons
c. Light photons to an analog signal
d. Analog signal to Digital signal
d. Analog signal to Digital signal
Which of the following components collects light photons from the output phosphor and converts them to electrons?
a. Vidicon television pick-up tube
b. Charge-coupled-device (CCD)
c. Analog - to - digital converter ADC)
d. Input phosphor
b. Charge-coupled-device (CCD)
Which of the following is the first order of events when operating an image intensifier?
a. Light photons strike the input phosphor
b. X-rays strike the output phosphor
c. X-rays strike the input phosphor
d. Electrons strike the input phosphor
c. X-rays strike the input phosphor
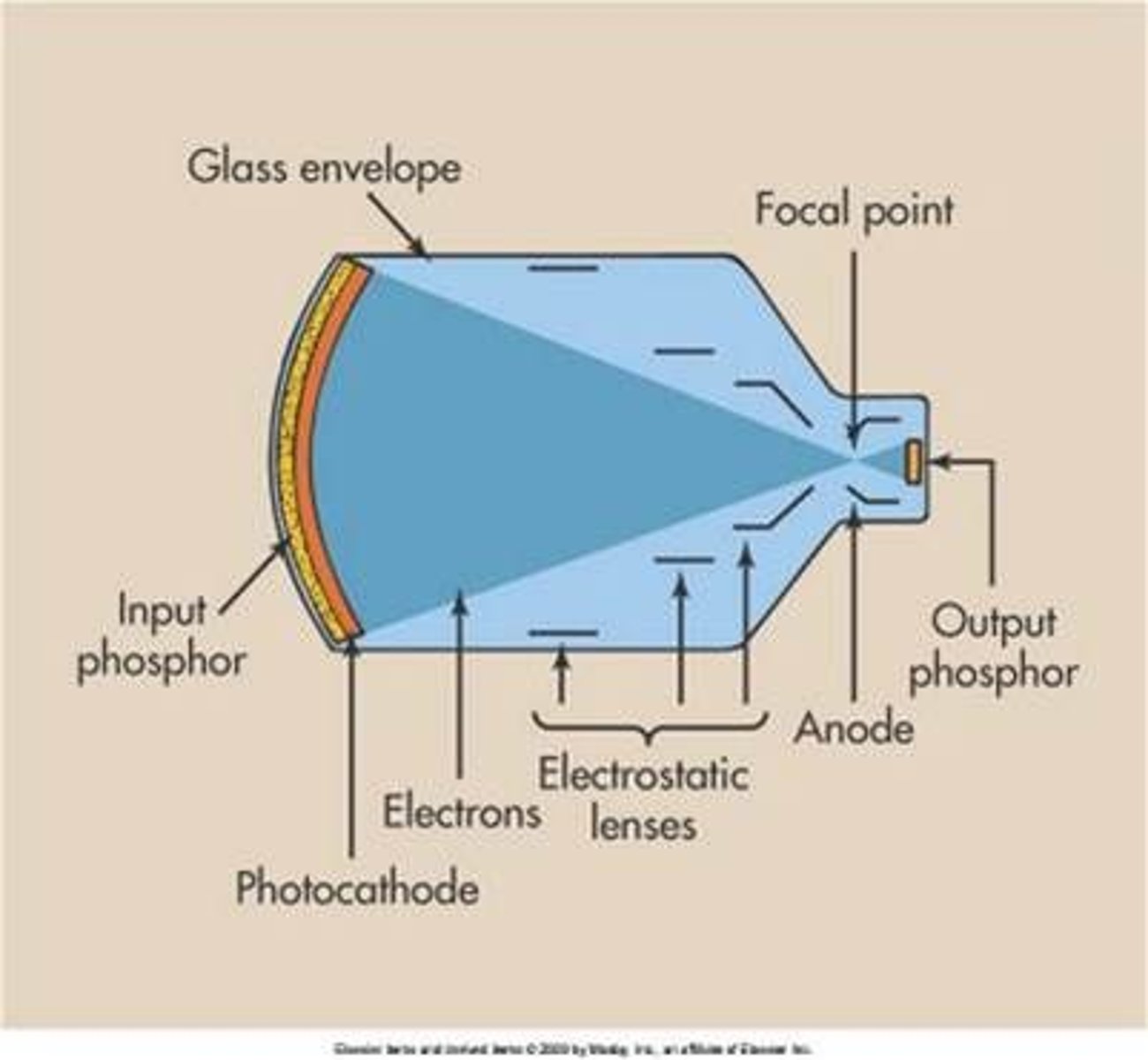
What is the voltage difference between the photocathode and anode assembly in an image intensifier?
a. 50-220 volts
b. 15,000-18,000 volts
c. 25,000-30,000 volts
d. 35,000-45,000 volts
c. 25,000-30,000 volts
The output phosphor of the image intensifier
Composed of zinc cadmium sulfide.
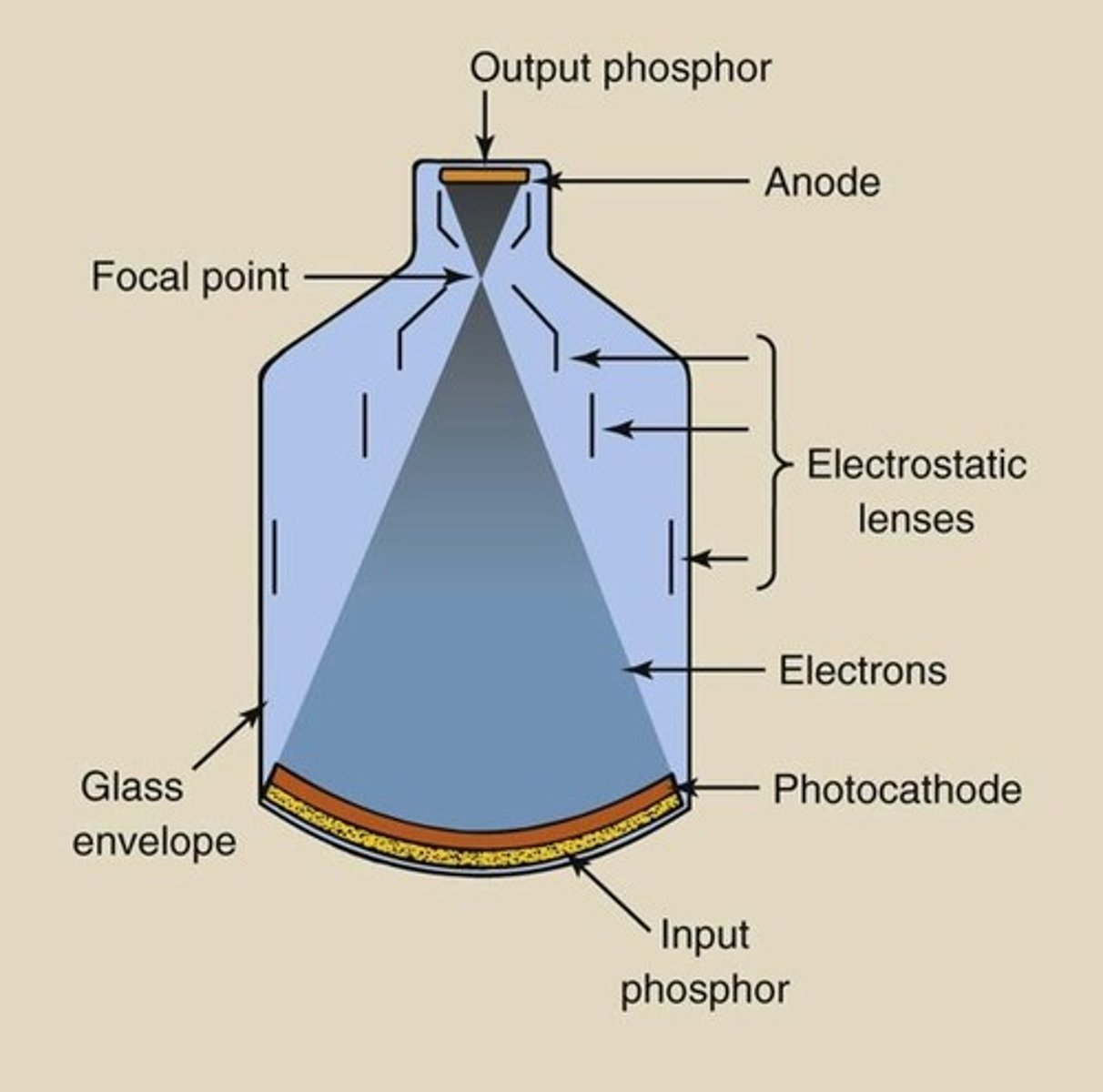
The input phosphor of the image intensifier
-converts incoming xray photons into light photons (25, 17, 12 in)
- usually made of cesium iodide
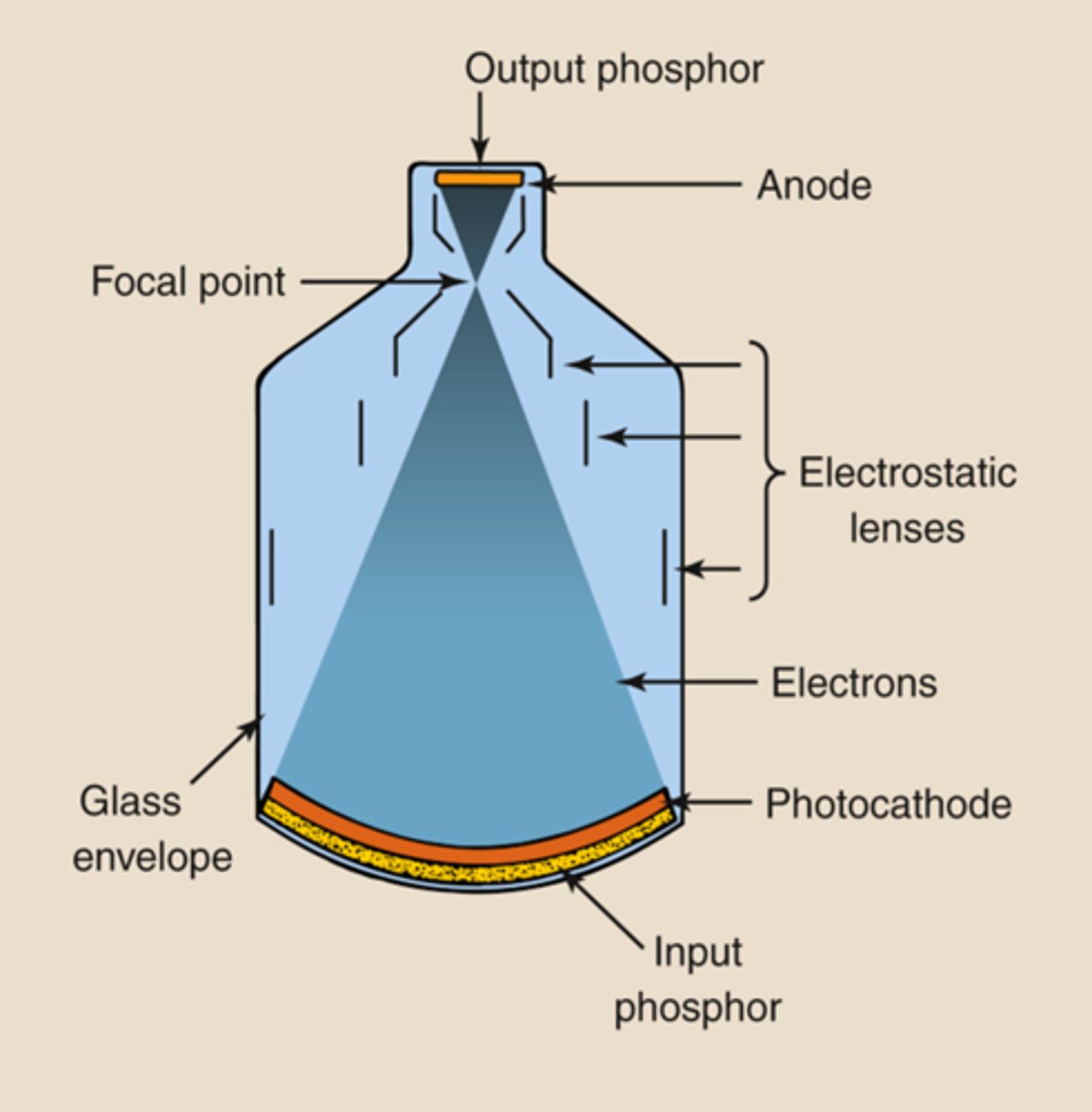
Using a grid in fluoroscopy will increase which of the following? (Select two)
a. OID
b. Image quality
c. SID
d. Patient dose
b. Image quality
d. Patient dose
When using an image intensifier in fluoroscopic imaging, where is the grid located?
a. On the output phosphor
b. On the x-ray tube
c. Behind the input phosphor
d. In front of the input phosphor
d. In front of the input phosphor
Which of the following is accurate regarding grids used in fluoroscopic imaging ?
a. Fluoroscopic imaging grids have a lower grid ration than radiographic imaging grids
b. Fluoroscopic imaging grids have a higher grid ration than radiographic imaging grids
c. Fluoroscopic grids contain a crossed pattern
d. Fluoroscopic grids grids tend to have a Moiré effect
a. Fluoroscopic imaging grids have a lower grid ration than radiographic imaging grids
What type of grid orientation is often found in conventional fluoroscopic grids?
a. Crossed
b. Linear
c. S-shaped pattern
d. Moire pattern
b. Linear
In order to decrease patient dose while performing a fluoroscopic procedure on a pediatric patient, the operator should:
a. Increase the grid ratio
b. Use a crossed grid instead of a linear grid
c. Increase the mA station
d. Remove the grid
d. Remove the grid
When performing a fluoroscopic procedure on an adult patient, the operator notes decreased image contrast due to high scatter production. Which of the following steps would improve the image contrast?
a. Add on a grid
b. Remove the grid
c. Increase the mA
d. Increase the kVp
a. Add on a grid
Crossed grids in fluoroscopic imaging are: (Select two)
a. Often used in conventional fluoroscopy
b. Often used in interventional fluoroscopy
c. Two sets of lead strips orientated 90 degrees from one another
d. One sets of lead strips in a linear orientation
b. Often used in interventional fluoroscopy
c. Two sets of lead strips orientated 90 degrees from one another
Lower ratio grids can be utilized in conventional fluoroscopy because of the:
a. Decreased SID
b. Lower mA values
c. Higher mA values
d. Decreased density of contrast media
b. Lower mA values
Which two of the following are characteristics of fluoroscopic grids? (Select two)
a. Lead strips that can change their orientation with the angle of the central ray
b. Fluoroscopy grid ratios offer grid ratios similar to radiographic grids
c. Fluoroscopy grids absorb scatter radiation to improve image contrast
d. Fluoroscopy grids absorb primary radiation to improve spatial resolution
b. Fluoroscopy grid ratios offer grid ratios similar to radiographic grids
c. Fluoroscopy grids absorb scatter radiation to improve image contrast
In fluoroscopic imaging, grids improve image quality by:
a. Reducing patient dose
b. Absorbing scatter radiation
c. Increasing detector element size
d. Absorbing primary radiation
b. Absorbing scatter radiation
The measure of the ability of an image intensifier to increase the brightness level of the image is referred to as which of the following?
a. Minification gain
b. Brightness gain
c. Amplification
d. Automatic gain
b. Brightness gain
Which of the following occurs when three incident photons strike the input phosphor and produce 4,500 light photons from the output phosphor?
a. Minification gain decreases
b. Flux gain is 1,500
c. Brightness gain is 1,500
d. Flux gain is 13,500
b. Flux gain is 1,500
( 4500 light photons/3 incident photons)
An image intensifier has an input phosphor diameter of 14 inches (35cm) and an output phosphor diameter of 1 inch (2.5 cm). What is the minification gain?
a. 0.072
b. 88
c. 196
d. 1,225
c. 196
( 1,225/6.25=196 )
Which of the following accurately describes flux gain in fluoroscopy?
a. Concentration of photoelectrons from the input phosphor to the output phosphor
b. Kinetic energy gained by accelerating photoelectrons from the photocathode to the output phosphor
c. Ratio of the square of the diameter of the input phosphor to the square of the diameter of the output phosphor
d. Product of brightness gain multiplied by the minification gain.
b. Kinetic energy gained by accelerating photoelectrons from the photocathode to the output phosphor
What is the flux gain formula?
flux gain = number of output light photons/ number of input xray photons
How is image intensifier efficiency related to patient dose?
a. Directly related: higher efficiency requires a higher radiation dose
b. Proportional but not directly related: lower efficiency requires a lower radiation dose
c. Image intensifier efficiency and patient dose are not related
d. Inversely related: higher efficiency requires a lower radiation dose
d. Inversely related: higher efficiency requires a lower radiation dose
minification formula
input diameter^2/output diameter^2
( dI^2/dO^2 )
Brightness gain formula
minification gain x flux gain
what formula is used to calculate the conversion factor in fluoroscopy?
Intensity of light at the o/p phosphor / Intensity of radiation at the input phosphor (approximately 1 percent of brightness gain )
If 100 x-ray photons reach a 30 cm input phosphor and 5000 light photons are produced at a 2.5 cm output phosphor, What is the brightness gain of the image intensifier?
a. 34
b. 144
c. 5,000
d. 7,200
d. 7,200
( 5000/100=50 flux gain
30 cm^2/2.5cm^2=144 minification
50 x 144 = 7,200 brightness gain )
Which three of the following are functions of ABC in fluoroscopy? (Select three)
a. Adjusting exposure factors
b. Controlling x-ray
c. Controlling the size of the field of view
d. Compensating for variations in patient anatomy and density
a. Adjusting exposure factors
b. Controlling x-ray
d. Compensating for variations in patient anatomy and density
During fluoroscopy procedures, ABC is typically preferred over manually setting exposure factors because:
a. Operators are unable to set manual exposure factors during fluoroscopy procedures
b. ABC provides a constant signal intensity that compensates for changes in thickness and density
c. Manual settings commonly produce more radiation exposure resulting in overexposure to the patient
d. Federal regulations require ABC to always be used during fluoroscopy procedures
b. ABC provides a constant signal intensity that compensates for changes in thickness and density
When radiation levels are high, Automatic Gain Control (AGC) functions by:
a. Increasing the amplification
b. Decreasing the amplification
c. Increasing the kVp
d. Increasing the mA
b. Decreasing the amplification
How can operators improve image quality when performing a fluoroscopy procedure using Automatic Exposure Control (AEC)? (Select two)
a. Decrease the kVp peak setting
b. Center the anatomical part of interest to the center of the image receptor
c. Increase the mA setting
d. Collimate to the size of the anatomical area
b. Center the anatomical part of interest to the center of the image receptor
d. Collimate to the size of the anatomical area
The Automatic Brightness Control (ABC) system adjusts for variations in patient positioning, part thickness, tissue density, and contrast media density during a fluoroscopic procedure by:
a. Using the signal from the image receptor to adjust the kVp and mA
b. Adjusting the SID
c. Adjusting the OID
d. Using the signal from x-ray tube to adjust the kVp and mA
a. Using the signal from the image receptor to adjust the kVp and mA
What is the role of Automatic Gain Control (AGC) when ABC has reached the maximum kVp peak and mA threshold, but the image is still not of optimal quality?
a. AGC adjusts the exposure factors
b. AGC adjusts the amplification of the incoming signal depending on detected radiation levels
c. AGC increases the x-ray beam quality
d. AGC overrides the ABC to manually set the kVp and mA
b. AGC adjusts the amplification of the incoming signal depending on detected radiation levels
Which of the following is another name for ABC?
a. ACC
b. ARC
c. AERC
d. ASI
c. AERC
( Automatic Exposure Rate Control, Automatic Brightness Stabilization, Automatic Dose Control, and
Automatic Dose Rate Control are other names. )
Low dose and high dose settings on the ABC system are important during fluoroscopy procedures because the dose settings:
a. Allow the operator to switch off the machine quickly
b. Provide additional options to adjust the x-ray tube's heat capacity
c. Offer additional flexibility so the operator can modify the field of view
d. Allow the system to adapt to different patient sizes and anatomy while controlling radiation exposure.
d. Allow the system to adapt to different patient sizes and anatomy while controlling radiation exposure.
Which of the following patient position adjustments would require the ABC to increase the exposure factors for a barium swallow fluoroscopy procedure? (Select two)
a. Moving from the proximal (upper) esophagus to the distal (lower) esophagus
b. Moving from the distal (lower) esophagus to the esophagus proximal (upper)
c. Changing from an AP esophagus position to a lateral esophagus position
d. Changing from an to a lateral esophagus position AP esophagus position
a. Moving from the proximal (upper) esophagus to the distal (lower) esophagus
c. Changing from an AP esophagus position to a lateral esophagus position
Vignetting:
- causes-
- Effect -
Correction -
Decrease in image brightness around the edges of the image.
- causes by -Curved input phosphor OID
-Effect- Reduces contrast and detail on the edges of the image
(correction- image processing, Adjusting image intensifier, and Reducing OID. )
Pincushioning:
caused by-
Effect of-
Parts of the image appear curved or bent inward toward the center of the image.
caused by-Curved input phosphor
Effect of-Inaccuracy of measurements
(can be corrected by image processing)
S-Shape images in Fluoroscopy:
Caused by-
Effect -
Parts of the image appear curved or bent inward toward the center of the image.
Caused by-External magnetic fields, Misangulation of the x-ray beam
Effect -Inaccuracy of measurements
(can be corrected by image processing)
Blooming:
Caused by-
Effect -
Parts of the image white out, Loses visual sharpness.
Caused by-High energy x-ray photons hitting the input phosphor
Effect -Loss of acuity
(Can be corrected by Proper patient positioning, Centering anatomy of interest, and Appropriate collimation)
Veiling Glare:
Caused by-
Effect -
-Type of blooming
-Contrast reducing haze on the fluoroscopic image
Caused by-Scattering of x-ray, light, and electron energies inside the image intensifier
Effect - Contrast reducing haze , Impacts image clarity
(can be corrected by grids and appropriate collimation.)
Lag:
Correction by
Delay in the response time of the image intensifier to changes in beam intensity
(can be corrected by Frame averaging and High-speed image intensifier.)
Noise
Caused by-
Effect -
Grainy or mottle image
Caused by- Detector does not receive enough radiation
Effect - Impacts the image clarity
(can be corrected by Increasing mA and/or kVp and Decrease SID)
Peripheral fall-off of image brightness with image intensifier is primarily due to the:
a. Flat surface of the output phosphor
b. Divergence of the incident x-ray beam
c. Concave, curved shape of the input phosphor
d. Position and convergence of the internal electrostatic focusing plates
c. Concave, curved shape of the input phosphor
Which of the following minimizes fluoroscopic image blooming with image intensifier?
a. Increased fluoroscopic mA
b. Increased kVp
c. Increased fluoroscopic SID
d. More precise positioning of the patient anatomy
d. More precise positioning of the patient anatomy
Which image intensifier error is potentially caused by external magnetic fields, and will result in parts of the image appearing curved or bent in a "S" shaped pattern?
a. Image lag
b. S-shaped distortion
c. Vignetting
d. Blooming
b. S-shaped distortion
Fluoroscopic image noise is directly related to the:
a. Incident radiation dose to the receptor
b. Fluoroscopic beam collimation
c. Use of a change-coupled device (CCD)
d. X-ray tube anode angle
a. Incident radiation dose to the receptor
During a fluoroscopy procedure in an R/F room, the operator notices a decrease in image clarity due to the presence of noise. What adjustment should be made to reduce the image noise in the following image?
a. Decrease mAs
b. Increase SID
c. Decrease kVp
d. Decrease SID
d. Decrease SID
( image noise occurs when the detector does not receive enough radiation. )
Which two of the following would impact a provider's ability to make an accurate diagnosis or to perform a procedure accurately when using image intensifiers? (Select two)
a. Detector element size (DEL)
b. Distortion within the image
c. Artifacts present within the image
d. Size of the image receptor matrix
b. Distortion within the image
c. Artifacts present within the image
When using an image intensifier, the operator notices a loss of brightness at the periphery of the image, as seen in the following image. Which of the quality issues has occurred?
a. Vignetting
b. Pincushioning
c. S-shaped distortion
d. Blooming
a. Vignetting
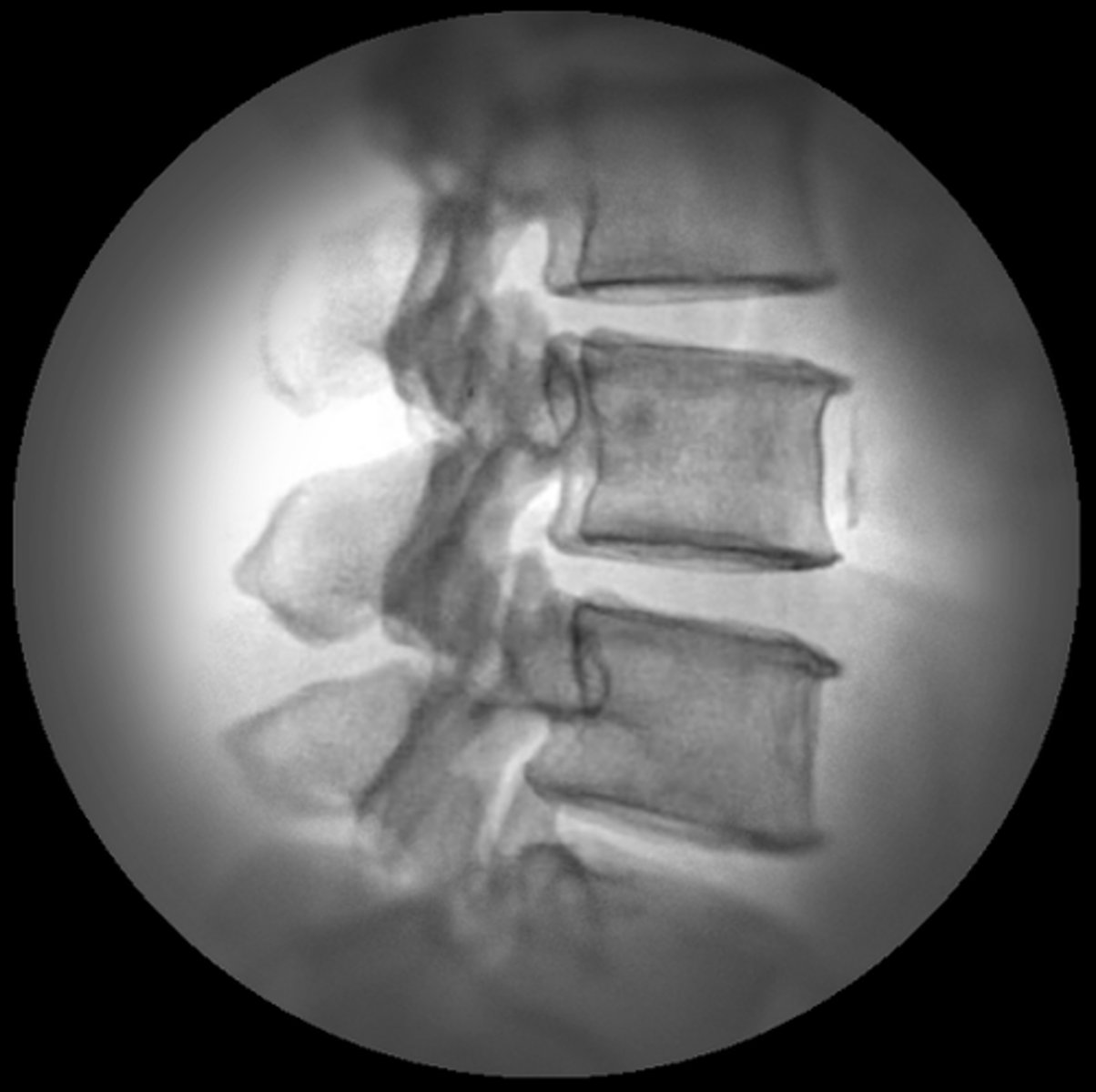
Which two of the following fluoroscopic quality issues are not caused by the design of the image intensifier?
a. Lag
b. Vignetting
c. Noise
d. Blooming
a. Lag
c. Noise
The use of frame averaging would correct which of the following fluoroscopic image quality issues?
a. Noise
b. Blooming
c. Vignetting
d. Lag
d. Lag
When x-ray, light, and electron energies scatter within the image intensifier and result in a contrast-reducing haze, which quality issue will occur?
a. Lag
b. Noise
c. Veiling glare
d. Pincushioning
c. Veiling glare
Which three of the following are accurate regarding current fluoroscopy monitors?
a. Fluoroscopic viewing monitors display
b. Fluoroscopic viewing monitors can be suspended from the ceiling
c. Fluoroscopic viewing monitors brightness is controlled manually by the operator
d. Fluoroscopic viewing monitors can be found on wheeled carts or attached to a c-arm
a. Fluoroscopic viewing monitors display
b. Fluoroscopic viewing monitors can be suspended from the ceiling
d. Fluoroscopic viewing monitors can be found on wheeled carts or attached to a c-arm
It is important to record fluoroscopic images because of the need to: (Select three)
a. Review and analyze fluoroscopic images
b. Communicate findings in the fluoroscopic images
c. Legally document fluoroscopic images that are taken during procedures
d. Record fluoroscopic images to aid in improving image quality
a. Review and analyze fluoroscopic images
b. Communicate findings in the fluoroscopic images
c. Legally document fluoroscopic images that are taken during procedures
In fluoroscopy, what is the primary difference between the image recording process of an image intensifier and the recording process of a flat panel detector?
a. Flat panel detector utilize a vidicon tube
b. Image intensifiers use a thin-film transistor (TFT)
c. Flat panel detectors use a thin-film transistor (TFT)
d. Image intensifier directly convert x-ray photons into an electrical signal
c. Flat panel detectors use a thin-film transistor (TFT)
How does image quality differ between image intensifiers that use charge-coupled devices (CCD) and image intensifiers that use vidicons?
a. CCD results in lower spatial resolution and more image blooming or lag
b. CCD results in higher spatial resolution and more image blooming or lag
c. CCD results in lower spatial resolution and less image blooming or lag
d. CCD results in higher spatial resolution and less image blooming or lag
d. CCD results in higher spatial resolution and less image blooming or lag
After the electrical signal has been created in a fluoroscopic system, it is:
a. Directly displayed on the monitor
b. Sent to an ADC, then sent to a monitor for viewing
c. Stored on a thin-film TFT, then sent to a monitor for viewing
d. Sent to a vidicon to convert into light
b. Sent to an ADC, then sent to a monitor for viewing
What component of the fluoroscopic system is responsible for converting the electrical signal into a digital signal?
a. Vidicon
b. CCD
c. ADC
d. TFT
c. ADC
In modern fluoroscopic systems with an II, hos is the CCD connected to the output phosphor?
a. Fiber-optically
b. Electronically
c. Via the vidicon
d. Via the TFT
a. Fiber-optically
What is the purpose of the TFT in a flat panel detector fluoroscopy system?
a. Convert the electrical signal into a digital signal
b. Store and release the electrical signal before it is converted into a digital signal
c. Convert light photons into an electrical signal
d. Connect the flat panel detector to the monitor
b. Store and release the electrical signal before it is converted into a digital signal
Which of the following demonstrates the correct order of image recording components in a fluoroscopy system that uses a flat panel detector?
a. Charged-coupled device (CCD), ADC, computer, viewing monitor
b. TFT, ADC, computer, viewing monitor
c. ADC, CCD, computer, viewing monitor
d. ADC, TFT, computer, viewing monitor
b. TFT, ADC, computer, viewing monitor
Which of the following statements regarding digital flat panel detectors is accurate?
a. Digital flat panel detectors are typically larger than image intensifiers?
b. Digital flat panel detectors use direct conversion and a scintillating phosphor
c. Digital flat panel detectors use indirect conversion and a scintillating phosphor
c. Digital flat panel detectors use indirect conversion and a scintillating phosphor
Which three of the following are advantages of flat panel detectors compared to image intensifiers? (Select three)
a. Improved spatial resolution
b. Wider dynamic range
c. Higher patient dose
d. Lower patient dose
a. Improved spatial resolution
b. Wider dynamic range
d. Lower patient dose
Which of the following lists the components of a flat panel detector in order?
a. TFT array, photodiode layer, and scintillating layer
b. Photodiode layer, TFT array, and scintillating layer
c. scintillating layer, TFT array, and ADC
d. scintillating layer, Photodiode layer, and TFT array
d. scintillating layer, photodiode layer, and TFT array
Which two of the following reasons explain why flat panel detectors produce higher quality images when compared to a image intensifiers? (Select two)
a. Flat panel detectors have a smaller field of view
b. Flat panel detectors require more energy conversions
c. Flat panel detectors have a larger field of view
d. Flat panel detectors have a wider dynamic range
c. Flat panel detectors have a larger field of view
d. Flat panel detectors have a wider dynamic range
What is the function of the photodiode layer in a flat panel detector?
a. Convert x-rays to visible light
b. Collects the electrical signal
c. Converts light photons to an electrical signal
d. Acts as an ADC
c. Converts light photons to an electrical signal
Why do flat panel detectors have fewer image artifacts than image intensifiers?
a. Flat panel detectors have a smaller fov and shorter dynamic range
b. The surface on flat panel detectors allows a more uniform path from the x-ray source
c. Image intensifiers have a more efficient energy conversion process
d. Image intensifiers have a wider dynamic range
b. The surface on flat panel detectors allows a more uniform path from the x-ray source
Flat panel detectors are more efficient than image intensifiers because they require:
a. More energy conversions
b. Fewer energy conversions
c. An ADC
d. A circular shape versus a rectangular shape
b. Fewer energy conversions
When compared to image intensifiers, flat panel detectors result in which of the following?
a. Increased patient dose because of the wider dynamic range
b. Decreased patient dose because of the high efficiency of the flat panel detectors
c. Increased patient dose because of energy conversions that a flat panel detector uses
d. Equal amount of patient dose for both II and flat panel detectors.
b. Decreased patient dose because of the high efficiency of the flat panel detectors
X-ray photons converted into light photons
scintillation
(cesium or gadolinium)
light photons converted into electrical signal
photodiode
(amorphous silicon)
electrical signal sent to ADC
TFT
Which of the following statements are accurate regarding fluoroscopic systems that use flat panel digital detectors for fluoroscopy?
a. Flat panel detectors replace the image intensifier tube
b. Flat panel detectors do not need a fluoroscopic grid
c. Flat panel detectors do not require a fluoroscopic lead drape to protect the operator
d. Flat panel detectors still present image quality issues such as vignetting and image fall-off
a. Flat panel detectors replace the image intensifier tube
What is the sequence of energy conversions that occur in a flat panel detector during a fluoroscopic procedure?
a. Electrical signal, to light photons, to x-ray photons
b. x-ray to light photons, to electrical signals, to digital signals
c. x-ray to electrical signals, to light photons, to digital signals
d. light photons to x-ray, to electrical signals, to digital signals
b. x-ray to light photons, to electrical signals, to digital signals
How does the fill factor of a Detector Element (DEL) affect the contrast and spatial resolution of a fluoroscopic image?
a. Fill factor and contrast and spatial resolution are inversely proportional
b. Fill factor and contrast and spatial resolution are directly proportional
c. Fill factor does not affect the contrast and spatial
d. The contrast is directly proportional to the fill factor, while spatial resolution is inversely proportional
b. Fill factor and contrast and spatial resolution are directly proportional
A flat panel detector consists of which of the following layers?
a. Scintillation layer, photodiode layer, and CCD
b. Photodiode layer, TFT, and ADC
c. Scintillation layer, ADC, TFT array
d. Scintillation layer, photodiode layer, and TFT
d. Scintillation layer, photodiode layer, and TFT