W9, RAAS Drugs, Vasodilators, & Anti-hypertensives
1/137
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
138 Terms
What are long term effects of hypertension?
Heart failure, weakening vessels, risk of cardiovascular disease (CVD) and stroke
What are lifestyle modifications to help manage hypertension?
Switch to low-sodium diet or DASH diet, increase exercise, quit smoking
True/False: There is a cure, atropine, to hypertension
False; there is no cure to hypertension, just lifelong treatment
What are 5 ways to promote patient adherence to treatment of hypertension?
Education, self-monitoring, minimizing side effects, have collaborative relationship, simplify regimen
What is education about hypertension nurse could provide to patient to promote adherence to treatment?
Hypertension could lead to stroke, heart disease or kidney disease, and by treating it patient could live a longer healthier life
What is self-monitoring nurse could teach patient to promote adherence to treatment of hypertension?
Track BP daily to help with monitoring
What are ways nurse could help patient minimize side effects of hypertension to promote adherence to treatment?
Encourage patient to report side effects, start patient on lower doses and increase dosage as needed
In addition to collaborating with patient, who else should nurse collaborate with to promote adherence to treatment of hypertension?
Collaborate with patient’s family too
How could nurse simply regimen for patient to promote adherence to treatment of hypertension?
Give patient pill to take once or twice a day (instead of 3 or 4 times a day or multiple pills for example)
Why might it be difficult for patients to adhere to treatment of hypertension?
Treatment is life-long and there are no manifestations (signs or symptoms) of hypertension
Why might patient not believe they need to treat their hypertension?
There are no manifestations (signs or symptoms) of hypertension
What is hypertension also known as?
The silent killer
Why is hypertension also known as the silent killer?
There are no manifestations (signs or symptoms) of hypertension, so people might not even know they have hypertension or they might not believe they need treatment
What are manifestations (signs and symptoms) of hypertension?
Typically none until it has caused significant damage to the body or becomes severely elevated (usually in severe or crisis cases)
What are 5 drugs classified as ACE inhibitors?
Lisinopril, captopril, enalapril, benazepril, ramipril
What does “ACE” in ACE inhibitors stand for?
Angiotensin-Converting Enzyme (inhibitors)
What is classification of lisinopril, captopril, enalapril, benazepril, and ramipril?
ACE inhibitors
What is suffix in name of all ACE inhibitors?
-pril
True/False: Lisinopril, captopril, enalapril, benazepril, and ramipril are Angiotensin-Converting Enzyme inhibitors
True (Angiotensin-Converting Enzyme is full name of ACE inhibitors)
What are therapeutic uses of ACE inhibitors (lisinopril, captopril, enalapril, benazepril, ramipril)?
Hypertension, MI, HF, LV dysfunction, diabetic and non-diabetic nephropathy, prevention of MI, stroke, and death
What is mechanism of action of ACE inhibitors?
To suppress formation of Angiotensin II which will cause dilation of blood vessels, reduction in blood volume, and prevention of pathologic changes in heart and blood vessels, and to increase bradykinin to cause vasodilation
What are 2 mechanisms of action of ACE inhibitors?
To suppress formation of Angiotensin II (from Angiotensin I), to increase bradykinin
When ACE inhibitors suppress formation of Angiotensin II (mechanism of action), what does that cause?
Causes dilation of blood vessels, reduction in blood volume, and prevention of pathologic changes in heart and blood vessels
When ACE inhibitors increase bradykinin (mechanism of action), what does that cause?
Causes vasodilation
What is bradykinin?
Peptide that causes vasodilation
What is typical function of Angiotensin II?
Potent vasoconstrictor that stimulates release of aldosterone (which typically reabsorbs water and sodium)
True/False: The mechanism of action of ACE inhibitors is (1) to suppress formation of Angiotensin II which will cause dilation of blood vessels, reduction in blood volume, and prevention of pathologic changes in heart and blood vessels, and (2) to increase bradykinin to cause vasodilation
True
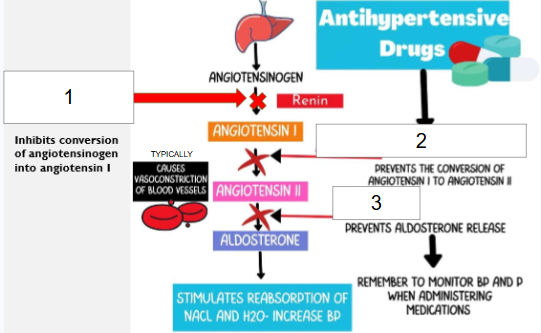
Which number (#1, #2, or #3) represents the mechanism of action of ACE inhibitors?
#2 because ACE inhibitors prevent conversion of angiotensin I to angiotensin II, which also prevents aldosterone release (causing vasodilation and reduction in blood volume overall)
Which part of mechanism of action of ACE inhibitors (suppression of formation of Angiotensin II or increase of bradykinin) causes adverse effect of cough?
Increase of bradykinin because ACE inhibitors cause vasodilation in lungs too
When taking ACE inhibitors, how does increase of bradykinin (mechanism of action of ACE inhibitors) cause adverse effect of cough?
Bradykinin accumulates in lungs, causes vasodilation, and irritates airway receptors, which can lead to dry, persistent cough
True/False: Due to mechanism of action of ACE inhibitors that increases bradykinin, this increase causes bradykinin to accumulate in lungs and cause vasodilation, which irritates airway receptors and can lead to dry, persistent cough (adverse effect)
True
What are adverse effects of ACE inhibitors?
Cough, angioedema, first-dose hypotension, hyperkalemia, renal failure, fetal injury
Why might hyperkalemia occur as adverse effect when taking ACE inhibitors?
Might occur due to inhibition of aldosterone release (which typically makes kidneys excrete potassium and retain sodium and water)
What is angioedema?
Allergic reaction where face, lips, and airway swells up
True/False: If patient experiences angioedema while taking ACE inhibitors, patient will not continue to take this drug (drug will be stopped immediately)
True
True/False: ACE inhibitors should be used with caution in patients with kidney failure
True, ACE inhibitors can be beneficial to these patients but require close monitoring
What are drug interactions to watch out for when taking ACE inhibitors?
Diuretics, antihypertensive agents, drugs that raise potassium, lithium, NSAIDs
Why should diuretics and ACE inhibitors not be taken together?
Diuretics will intensify first-dose hypotension
Why should antihypertensive agents and ACE inhibitors not be taken together?
Together will cause increased hypotension (most likely too much)
Why should drugs that raise potassium and ACE inhibitors not be taken together?
Together can cause increased hyperkalemia
Why should lithium and ACE inhibitors not be taken together?
Will lead to lithium toxicity
Why should NSAIDs and ACE inhibitors not be taken together?
NSAIDs will reduce antihypertensive effect of ACE inhibitors
What should nurse educate patient taking ACE inhibitors to check everyday?
To check BP everyday
What is mnemonic of side effects of ACE inhibitors?
CAPTOPRIL
What does mnemonic CAPTOPRIL stand for (tells side effects of ACE inhibitors)?
Cough, Angioneurotic edema, Proteinuria, Taste disturbance and Teratogenic, Other (Fatigue), Potassium increased, Renal impairment, Itch, Low BP
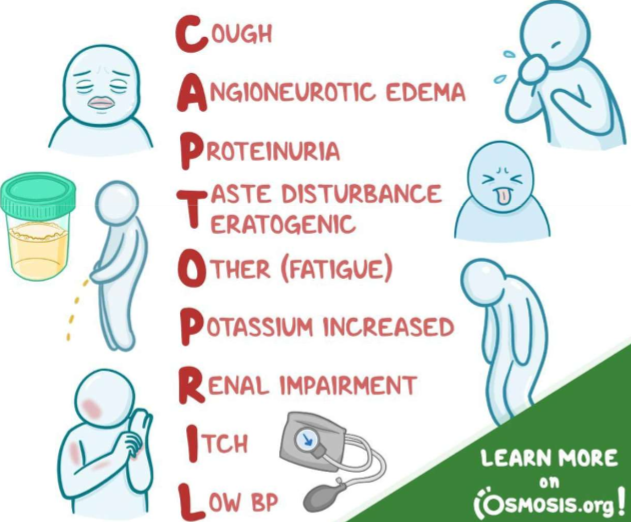
Which drug’s side effects are displayed here?
ACE inhibitors
True/False: ACE inhibitors decrease peripheral vascular resistance without affecting cardiac output, cardiac rate, and cardiac contractility
True
What is fun way to remember ACE inhibitors drug names all end with -pril?
Think ACE inhibitors as April (A for ACE inhibitors and -pril for the ending!)
True/False: Some side effects of ACE inhibitors include dizziness, orthostatic hypotension, nonproductive cough, GI distress, and headache
True
What do ARBs stand for?
Angiotensin II receptor blockers
What are 2 drugs classified as ARBs?
Losartan, Valsartan
What is suffix of all drugs classified as ARBs?
-sartan
What is classification of losartan and valsartan?
ARBs
What are therapeutic uses of ARBs (losartan and valsartan)?
Hypertension, HF, diabetic nephropathy, MI, prevention of MI, stroke, and death in high risk patients, patients who cannot tolerate ACEs
True/False: ARBs are typically started if patient cannot tolerate ACE inhibitors due to cough or angioedema for example
True
Why do ARBs not present with adverse effect of cough like ACE inhibitors?
Mechanism of action of ARBs doesn’t increase bradykinin like ACE inhibitors do, and increased bradykinin is what causes adverse effect of cough
True/False: Both ARBs and ACE inhibitors cause adverse effect of cough
False; only ACE inhibitors cause adverse effect of cough because mechanism of action of ARBs doesn’t increase bradykinin like ACE inhibitors do, and increased bradykinin is what causes adverse effect of cough
What is mechanism of action of ARBs?
To block actions of angiotensin II by blocking access of angiotensin II to its receptors in blood vessels, adrenal glands, and all other tissues, which causes dilation of arterioles and veins, prevention of angiotensin II from inducing pathologic changes in cardiac structure, and increase in renal excretion of sodium and water (because aldosterone is blocked too)
True/False: Mechanism of action of ARBs is to block actions of angiotensin II by blocking access of angiotensin II to its receptors in blood vessels, adrenal glands, and all other tissues, which causes dilation of arterioles and veins, prevention of angiotensin II from inducing pathologic changes in cardiac structure, and increase in renal excretion of sodium and water (because aldosterone is blocked too)
True
Why is effect of mechanism of action of ARBs increase in renal excretion of sodium and water?
By blocking actions of angiotensin II, aldosterone is prevented from being released, and aldosterone typically reabsorbs sodium and water, so without aldosterone being released, sodium and water will be excreted instead of reabsorbed
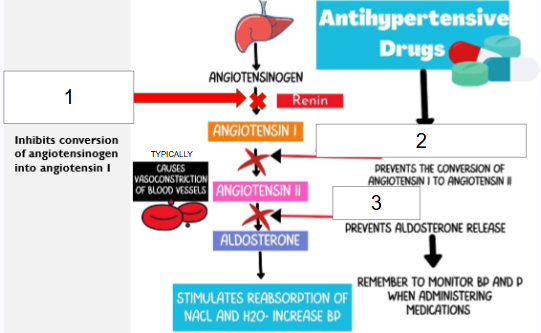
Which number (#1, #2, or #3) represents the mechanism of action of ARBs?
#3 because ARBs block actions of angiotensin II by blocking access of angiotensin II to its receptors in blood vessels, adrenal glands, and all other tissues (which causes dilation of arterioles and veins, prevention of angiotensin II from inducing pathologic changes in cardiac structure, and increase in renal excretion of sodium and water because aldosterone is blocked too)
What are adverse effects of ARBs?
Angioedema, fetal harm, renal failure
What is a drug interaction to watch out for when taking ARBs?
Other antihypertensives
Why should other antihypertensives and ARBs not be taken together?
Together will cause increased hypotension
True/False: ARBs have decreased risk of hyperkalemia as adverse effect
True

Which drug’s mechanism of action and adverse effects are being described here?
Angiotensin II receptor blockers (ARBs)
True/False: Losartan and valsartan are classified as angiotensin II receptor blockers
True (angiotensin II receptor blockers is full name of ARBs)
What is prototype of direct renin inhibitors?
Aliskiren
What is classification of aliskiren?
Direct renin inhibitor
What decreases absorption of direct renin inhibitors (aliskiren)?
High fat meals
Since high fat meals decrease absorption of direct renin inhibitors (aliskiren), when should aliskiren be taken if patient wants to consume high fat meal?
Aliskiren should be taken at same time, so about an hour before meals
True/False: High carb meals decrease absorption of aliskiren
False; high fat meals decrease absorption of aliskiren
What is mechanism of action of direct renin inhibitors (aliskiren)?
Acts on renin to inhibit conversion of angiotensinogen into angiotensin I which then suppresses entire RAAS, and thus will cause vasodilation, decreased blood volume, and no aldosterone release
What is therapeutic use of direct renin inhibitors (aliskiren)?
Hypertension
Which drug’s mechanism of action is being described: Acts on renin to inhibit conversion of angiotensinogen into angiotensin I which then suppresses entire RAAS, and thus will cause vasodilation, decreased blood volume, and no aldosterone release?
Direct renin inhibitors (aliskiren)
True/False: Direct renin inhibitors (aliskiren) mechanism of action is to act on renin to inhibit conversion of angiotensinogen into angiotensin I which then suppresses entire RAAS, and thus will cause vasodilation, decreased blood volume, and no aldosterone release
True
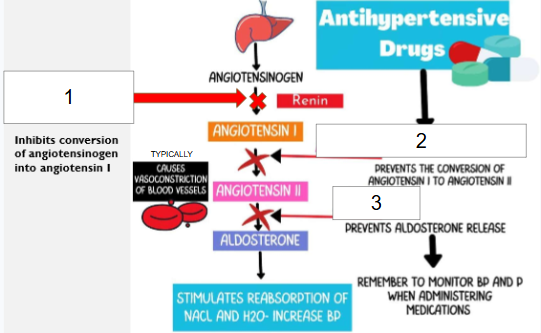
Which number (#1, #2, or #3) represents the mechanism of action of direct renin inhibitors (renin)?
#1 because direct renin inhibitors (aliskiren) act on renin to inhibit conversion of angiotensinogen into angiotensin I which then suppresses entire RAAS, and thus will cause vasodilation, decreased blood volume, and no aldosterone release
True/False: ACE inhibitors stop entire RAAS
False; direct renin inhibitors stop entire RAAS
What are adverse effects of direct renin inhibitors (aliskiren)?
GI effects, diarrhea, abdominal pain, indigestion, fetal harm
True/False: Direct renin inhibitors (aliskiren) have lower incidence of angioedema and hyperkalemia
True
What are drug interactions to watch out for when taking direct renin inhibitors?
Atorvastatin and Ketoconazole, Irbesartan, Furosemide
Why should Atorvastatin and Ketoconazole not be taken with direct renin inhibitors?
Atorvastatin and Ketoconazole can significantly increase levels of direct renin inhibitors, which can cause toxicity
Why should Irbesartan not be taken with direct renin inhibitors?
Irbesartan can significantly decrease direct renin inhibitors, so effect won’t be as helpful
Why should Furosemide not be taken with direct renin inhibitors?
Direct renin inhibitors will decrease effect of furosemide
What is drug classified aldosterone antagonist (potassium-sparing diuretic)?
Spironolactone
What is classification of spironolactone?
Aldosterone antagonist (potassium-sparing diuretic)
When is spironolactone (aldosterone antagonist potassium-sparing diuretic) used?
If patient does not respond well to ACE inhibitors or ARBs, or could be used in conjunction with either ACE inhibitors or ARBs
True/False: Spironolactone, an aldosterone antagonist potassium-sparing diuretic, is used if patient does not respond well to ACE inhibitors or ARBs, or could be used in conjunction with either ACE inhibitors or ARBs
True
If patient doesn’t respond well to treatment from ACE inhibitors or ARBs, what drug is taken then (either taken alone, or in conjunction with ACE inhibitors or ARBs)?
Spironolactone (aldosterone antagonist potassium-sparing diuretic)
What is mechanism of action of spironolactone?
Blocks aldosterone which will cause retention of potassium as well as increased excretion of sodium and water, to ultimately reduce blood volume and reduce blood pressure
True/False: Mechanism of action of spironolactone is to increase reabsorption of sodium and water, to ultimately increase blood volume and blood pressure
False; mechanism of action of spironolactone is to block aldosterone which will cause retention of potassium as well as increased excretion of sodium and water, to ultimately reduce blood volume and reduce blood pressure
What are therapeutic uses of spironolactone?
Hypertension, heart failure
What are adverse effects of spironolactone?
Hyperkalemia, endocrine effects, fetal harm
What should nurse educate patient about when taking spironolactone?
Educate patient to use salt substitutes and to watch diet so potassium levels don’t go up too high and cause adverse effect of hyperkalemia
What are endocrine effects that could appear as adverse effect to spironolactone?
Deepening of voice, hirsutism (excessive facial hair growth in women), menstrual irregularities
What is biggest adverse effect of spironolactone?
Hyperkalemia
What are drug interactions to watch out for when taking spironolactone?
Drugs that raise K+ levels, ACE inhibitors, ARBs, direct renin inhibitors
Why should spironolactone be used with caution when taken with ACE inhibitors, ARBs, or direct renin inhibitors?
ACE inhibitors, ARBs, and direct renin inhibitors are other antihypertensive drugs, so watch out for too much hypotension
Why should spironolactone and drugs that raise K+ levels not be taken together?
Could cause too much potassium in bloodstream (hyperkalemia) together
What are 2 drugs classified as vasodilators?
Hydralazine, minoxidil