Lecture 16: Rheumatology
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
Non-Inflammatory Arthritis
AM stiffness < 1 hour
Pain
Worst at end of day
Worsens with activity
Improves with rest
Normal ESR/CRP
WBC less than 2000
Inflammatory Arthritis
AM stiffness > 1 hour
Pain
Worst at start of day
Improves with activity
Worsens with rest
Elevated ESR/CRP
Osteoarthritis
Can involve any articular joint (from c-spine down to toes)
Mono especially in cases of post-traumatic OA
Polyarthritis more common in hands
Heberden (DIP) vs Bouchard Nodes (PIP) (bony enlargement)
Associated w/ obesity
Osteoarthritis Treatment
Lifestyle Modification: Weight Loss, Diet, Exercise
Tylenol
NSAIDs (PO and topical)
Intraarticular Steroids
Duloxetine
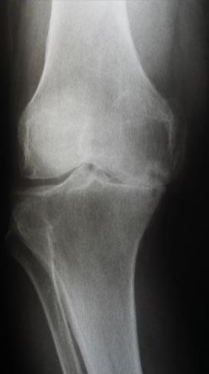
Osteoarthritis
Rheumatoid Arthritis
Polyarticular Symmetric Inflammatory arthritis
Small joints of hands (spares DIPs)
Affects most joints (not DIPs or Lumbar/Thoracic Spine)
Leads to joint destruction if untreated
Chronic, systemic inflammatory disorder
Extraarticular manifestations
Swan neck deformity, Boutonniere deformity, Ulnar Deviation
Autoantibodies: Rheumatoid Factor (RF) and Cyclic citrullinated Peptide (CCP): more specific
Genetic Association: HLA-DR4, Female, Smoking
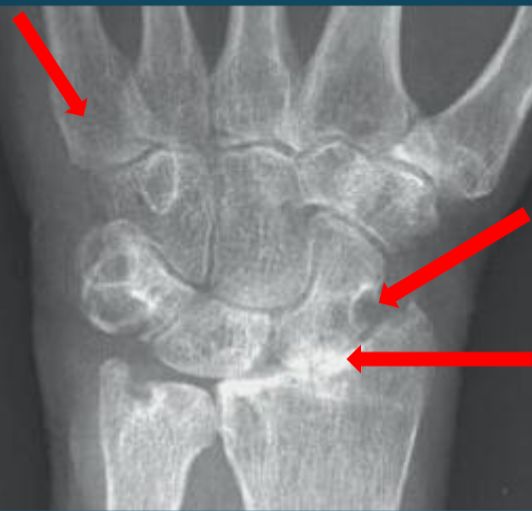
Rheumatoid Arthritis
periarticular osteopenia
erosions
joint space narrowing
Rheumatoid Arthritis Extraarticular Manifestations
SubQ Nodules
Pericarditis
Interstitial Lung Disease
Scleritis
Felty’s Syndrome
Rheumatoid Arthritis + Neutropenia + Splenomegaly
Caplan’s Syndrome
Rheumatoid Arthritis + pneumoconiosis
Coal-miners
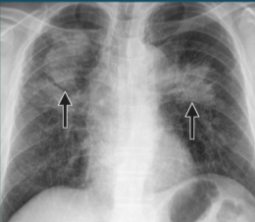
pneumoconiosis
Rheumatoid Arthritis Treatment
NSAIDs: Renal (CKD, AIN), GI (PUD, gastritis), CV (MI)
Glucocorticoids: Weight gain, insulin resistance, “buffalo hump”, cushingoid features, osteoporosis, psychosis, acne, adrenal insufficiency if ill or med abruptly withdrawn
Methotrexate (1st line DMARD): teratogenic, hepatotoxic, ILD
Anti-TNF (1st line biologic): Etanercept, Infliximab, Adalimumab
Biologic DMARDs
Adverse Effects:
Increases susceptibility to Infection
TB
Endemic Fungi
Drug-induced lupus (dsDNA)
Contraindications:
Active infection
Malignancy
CHF
Demyelinating disorders (MS)
Seronegative Spondyloarthropathies
Back pain (inflammatory axial arthritis): chronic, insidious, AM stiffness, better with exercise
Inflammatory arthritis
Imaging: Sacroiliitis on XR or MRI
Labs: HLA B27
Uveitis
Enthesitis
Dactylitis (sausage digits)
Psoriatic Arthritis
Psoriasis + Psoriatic Arthritis
Inflammatory axial arthritis (back pain)
Inflammatory polyarthritis
Can affect DIPs (unlike RA)
Arthritis mutilans subtype (very rare)
Nail Pitting
Sausage Digits
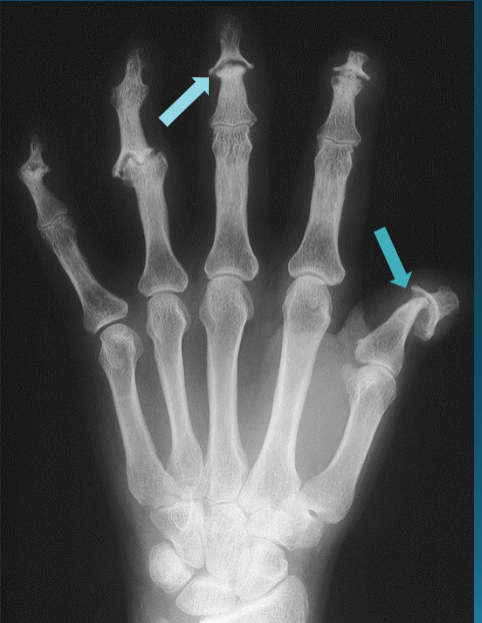
Psoriatic Arthritis
DIP Involvement → Pencil in Cup Deformity
Psoriatic Arthritis Treatment
Methotrexate
TNF inhibitors (1st line): Adalimumab, Etanercept, Infliximab
Ankylosing Spondylitis
diagnosis is confirmed by spine radiographs (especially of SI joints)
Bamboo Spine
Minor trauma → vertebral fractures
Aortic Regurgitation
Apical pulmonary fibrosis
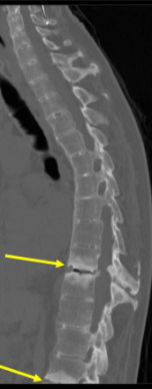
Ankylosing Spondylitis
Ankylosing Spondylitis Treatment
First line Therapy: NSAIDs, Physical Therapy
Inadequate Response to NSAIDs → TNF inhibitors: Adalimumab, Etanercept, Infliximab
IBD-Related Arthritis
IBD + Ankylosing Spondylitis
Reactive Arthritis
Conjunctivitis, Uveitis, Urethritis
Circinate Balanitis
Oligoarticular Arthritis (knee>ankle)
Back pain
Most patients spontaneously remit
>2-3 weeks following GI or GU infection
Patient with joint pain + h/o infectious diarrhea or an STI
Screen all patients for STI’s!
Responds well to NSAIDs and time
Resistant cases (<25%) may require DMARDs/Biologics
Gout Overview
Abrupt onset of inflammatory joint pain, warmth, and swelling over the course of several hours to a day
Exquisite pain
Asymmetric joint involvement
MTP (podagra), ankles, knees, elbows, hands
Tophi (nodules filled with chalky-white uric acid crystal deposits) near affected joints (olecranon bursa, hands, etc) or on pinna of ear
Gout pathogenesis, epidemiology, and cause of flare ups
Under-excretion of uric acid
Males, CKD
Gout Flare Causes:
Intake of purine-rich foods (red meat, shellfish)
Alcohol (binge drinking)
Use of diuretics (furosemide or thiazides)
Pseudogout
acute calcium pyrophosphate (CPP) crystal arthritis
Knees >>> wrists > ankles > elbows > shoulders
Presents very similar to gout
Weakly positively birefringent rhomboid CPP crystals
Blue
Gout
Needle-shaped
Birefringence: Strongly Negative
Color when parallel to polarized light: Yellow
Septic Arthritis
Severely painful red, swollen joint held in slight flexion
Staph aureus (IV drug users), Streptococcus
R/o concomitant endocarditis
Neisseria gonorrhoeae (multiple partners)
Septic arthritis is an emergency!
Next step after arthrocentesis → Consult Ortho ASAP for surgical debridement
Systemic Lupus Erythematosus
Systemic autoimmune disorder characterized by immune-mediated damage (to kidneys, brain, blood cells, skin)
Young African American, Hispanic, or Asian Females
Rash (Discoid or Malar)
Arthritis
Serositis (pleuritis/pericarditis)
Hematologic Changes (low wbc/plt/hgb)
Oral Ulcers
Renal Disease (Lupus Nephritis) → UA: RBC’s or proteinuria
Photosensitivity
ANA Positive
Immune-mediated disorder (+dsDNA, +Sm, low c3/c4)
Neurological Changes (Seizures, psychosis)
Lupus presents with a facial droop, left-sided weakness, and a new murmur
Libman Sacks Endocarditis → Embolic CVA
Neonatal lupus
Heart Block + Rash
Dermatomyositis
Proximal muscle weakness + Rashs
Elevated CK, Aldolase, AST/ALT
anti-Jo-1
Imaging: Muscle inflammation on MRI
On boards, will be the quadriceps
Strongly associated with malignancy → Paraneoplastic syndrome
Order age-appropriate cancer screening
Heliotrope Rash
Gottron’s Papules
Sjogren’s Syndrome
Dry Eyes/Mouth + Inflammatory Arthritis
Decreased saliva → increased caries
Can co-exist with other rheumatic diseases
Labs: anti-SSA/SSB
10-20x increased risk of Non-Hodgkins Lymphoma (MALToma)
Associated with Type 1 RTA
Parotid Swelling
Lymphocytic Glandular Infiltration
Systemic Sclerosis (Scleroderma)
Limited: Associated with CREST syndrome
Calcinosis, Raynauds, Esophageal dysmotility, Sclerodactyly, Telangiectasias
+ Anti-Centromere
Pulmonary (MCC Death): ILD, pHTN
Sarcoidosis
Most common in African Americans
Dyspnea
Lymphadenopathy
RA-like arthritis
Hypercalcemia
Elevated ACE level
Non-caseating granulomas
Lofgren’s Syndrome
Type of Sarcoidosis
Hilar Adenopathy
Erythema Nodosum
Peri-ankle arthritis