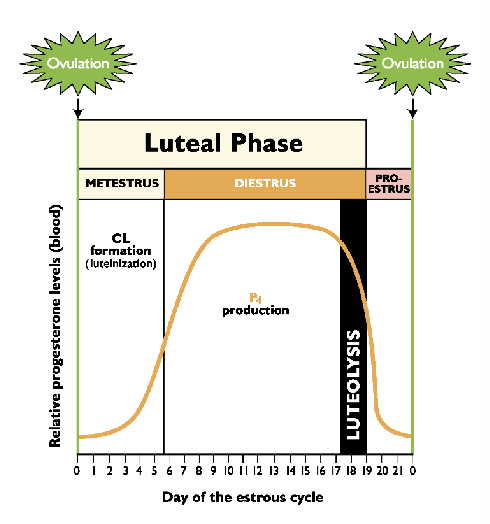
Luteal Phase
1/28
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
What are the two stages of the luteal phase? What is the major
The luteal phase extends from ovulation until CL regression
Two stages:
Metestrus - Luteinization
Diestrus
Characterized by fully functional CL
Luteolysis (CL regression)
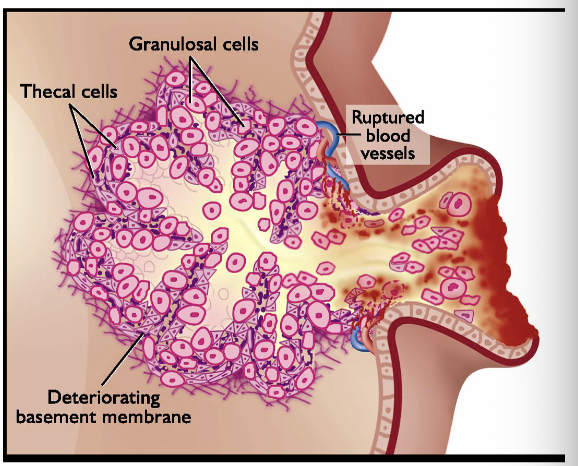
What is luteinization?
A process whereby cells of ovulatory follicle differentiate into luteal tissue
Theca interna and granulosa cells of follicle undergo dramatic
This transformation is largely governed by LH
PGE2 plays a role in remodeling too
Describe the corpus luteum. Mention the two cell types
Large luteal cells (LLC) originate from granulosa cells
20-70 microns
3x increase in size and volume (hypertrophy)
Small luteal cells (SLC) originate from theca interna
< 20 microns
5x increase in cell number (hyperplasia)
Both large and small luteal cells are steroidgenic (able to produce steroids)
Synthesize and secrete P4
SLC are LH-dependent, LLC produce P4 constitutively
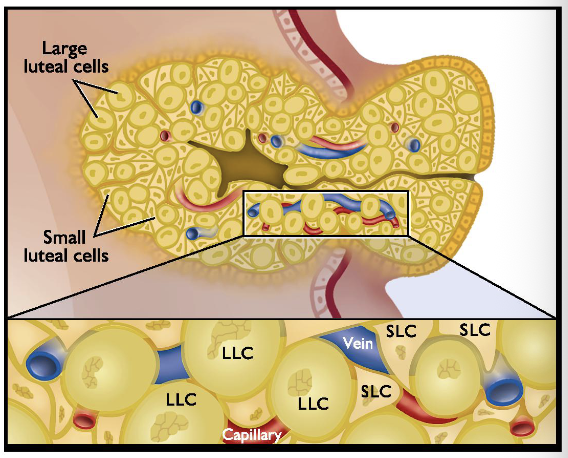
Describe the functional capactiy of the corpus luteum
Blood flow to CL= 6-10mL/min/g tissue
Most luteal cells are near capilaries
High metabolic demand; CL consumes 2-6 times more oxygen per unit weight than the liver, kidney, or heart
Non-steroidogenic cells proliferate too:
Endothelial cells, fibrobasts, white blood cells
Adds CL enlargement
Proliferation of cells in developing CL has a growth rate that rivals rapidly growing tumors
Insufficient CL function = Decrease P4
What is required for progesterone synthesis?
Basal LH secretion
Cholesterol
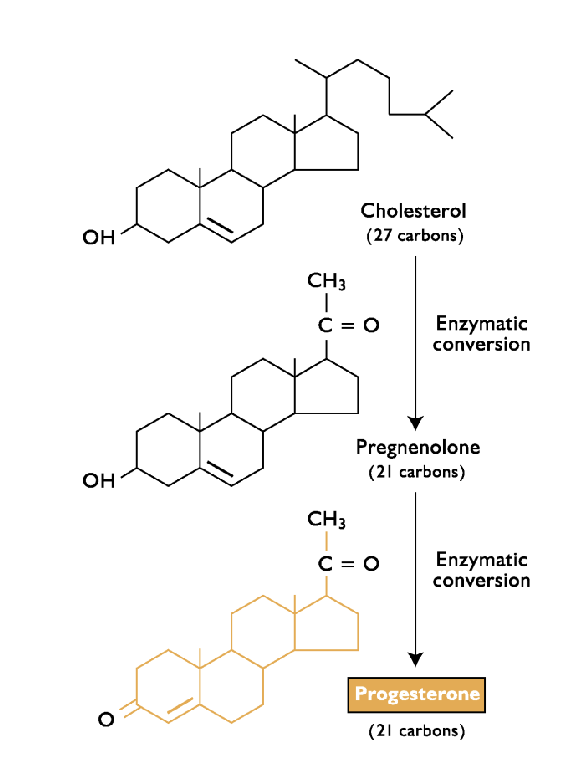
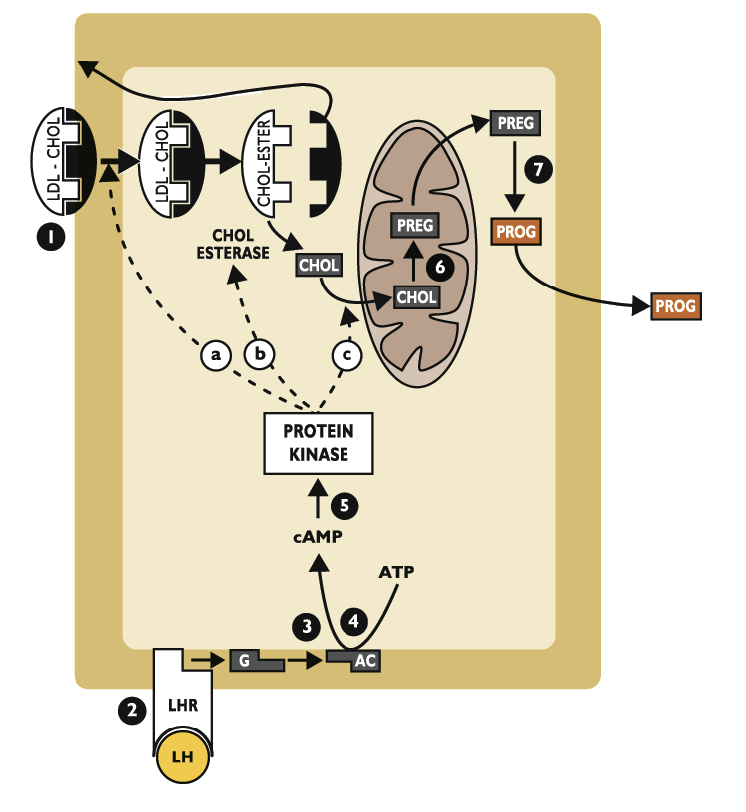
What are the steps of progesterone biosynthesis?
Receptor-mediated endocytosis - cholesterol enters cell
Cholesterol transported from cytoplasm into mitochondria by StAR (rate limiting step)
Cytochrome P450 SCC converts cholesterol to pregnenolone
Pregnenolone converted to P4 in smooth endoplasmic reticulum via 3-beta hydroxysteroid dehydrogenase (3B-HSD)
Describe specifically the first step of progesterone synthesis
Cholesterol is dlivered to the luteal cell primarily via lipoprotein (LDL or HDL)
LDL-CHOL binds to membrane-bound receptor (R)
LDL-CHOL-R complex is internalized
Cholesterol is released from the receptor complex as cholesterol esters
Receptor is “recycles” back to plasma membrane
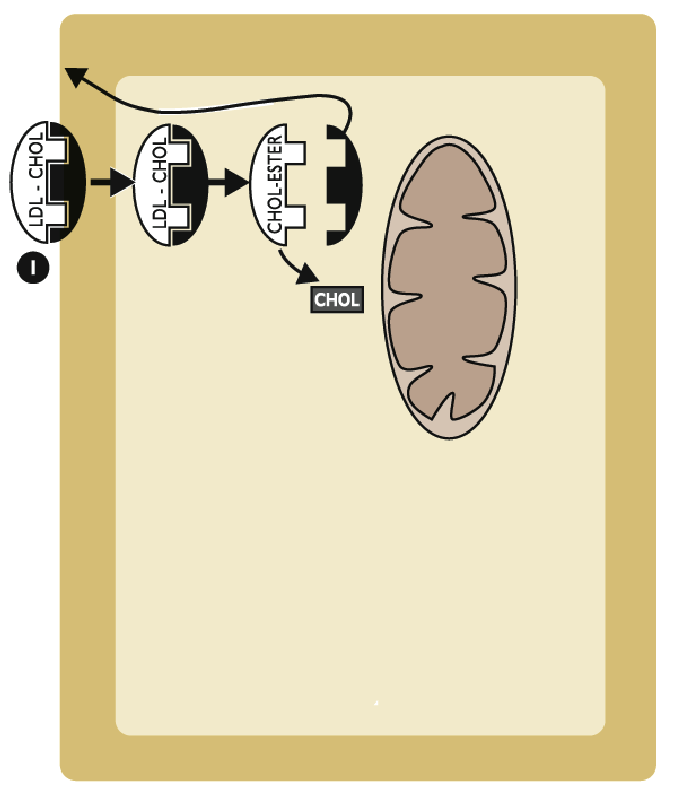
Describe steps 2-4 for progesteron synthesis
LH binds to LH receptor (LHR) on plasma membrane
LHR activates G protein (G) that activates membrane-bound adenylate cyclase (AC)
ATP is converted to cyclic AMP (cAMP), the second messenger
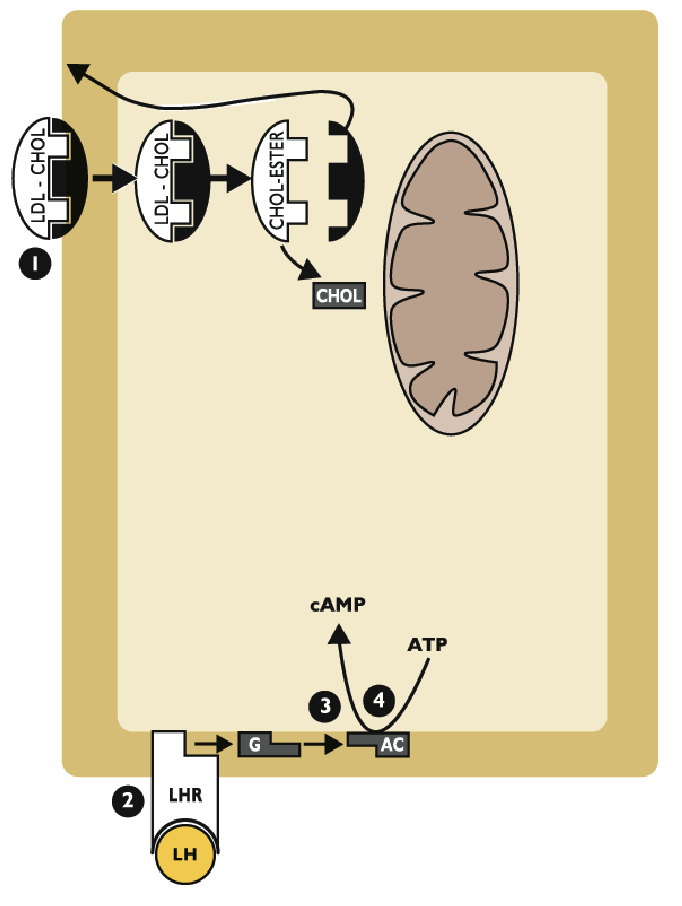
What is the 5th step in progesterone synthesis
cAMP activates protein kinases, which:
Increase rate of LDL-CHOL receptor internalization
activates cholesterol esterase (cleaves cholesterol from its ester)
Promote entry of cholesterol into mitochondria
Example: catalyzing synthesis of StAR
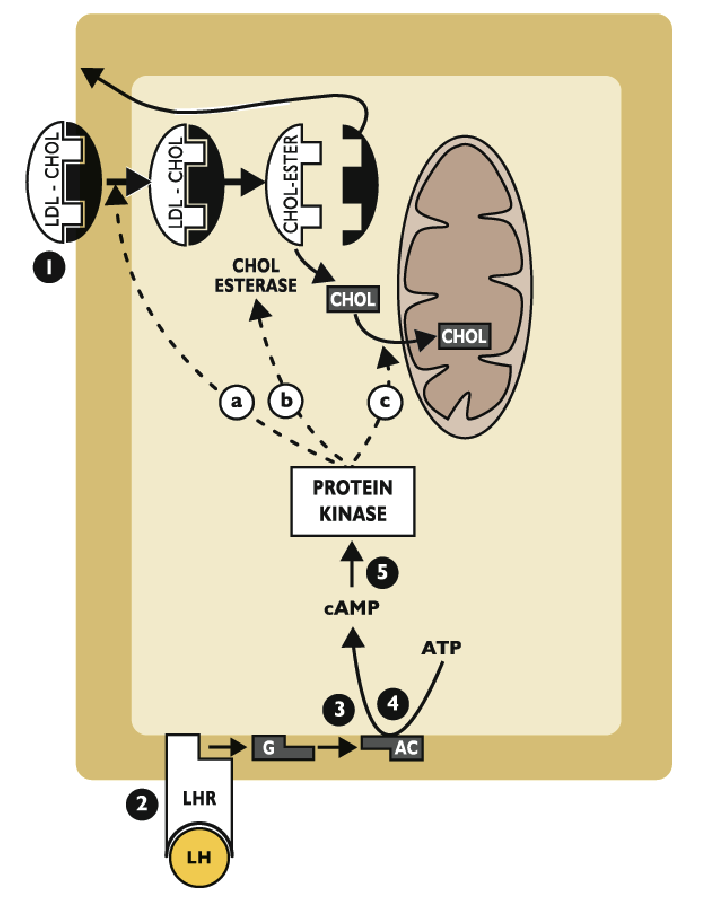
What is the 6th step of progesterone synthesis
In mitochondria, cholesterol makes pregnenolone
Enzyme: cytochrome P450 side-chain cleaveage (CYP450scc)
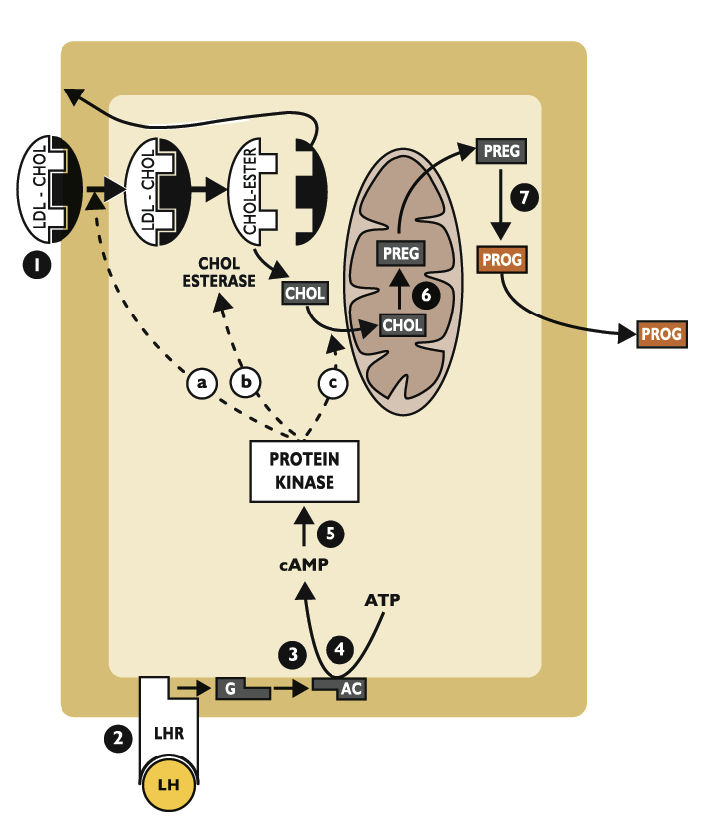
What is the 7th of progesterone synthesis?
Pregnenolone leaves the mitochondria and is converted to progesterone in the smooth endoplasmic reticulum
Enzyme: 3-beta hydroxysteroid dehydrogenase (3B-HSD)
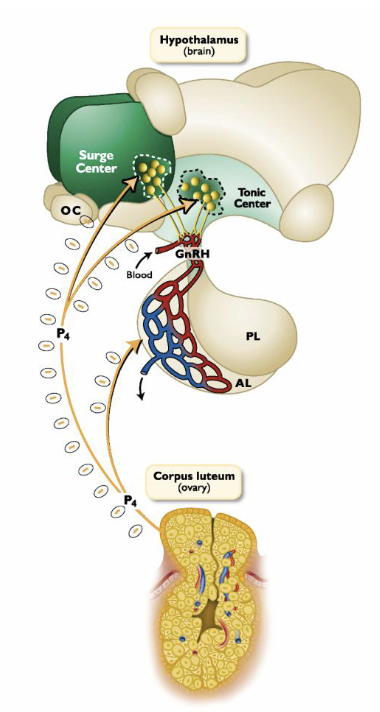
What are the primary target organs of progesterone? What effect does it have on the brain?
Hypothalamus (brain)
Female Tract
Mammary gland
Inhibitory effects on the hypothalamus:
Decreases GnRH pulse fequency
Prevents preovulatory LH surge
Prevents behavioral estrus
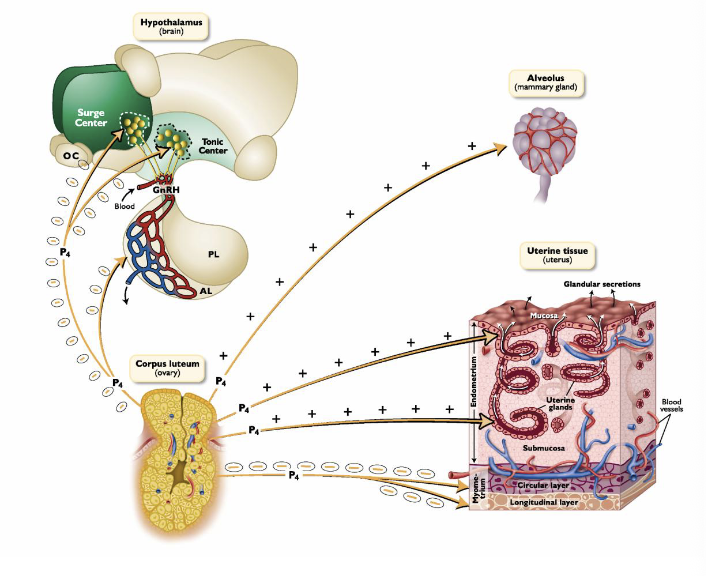
What are the major effects of progesterone on the female tract and mammary glands
Stimulates endometrial gland growth
Stimulates nutrient secretions by the oviducts and endometrium
Blocks myometrial contractions
Quiteting effect on myometrium in cow, ewe, sow
Allows for proper attachment of conceptus
Stimulates production of thick cervical mucus
Mammary glands:
Causes final alveolar development of mammary glands prior to parturition
What is Luteolysis? What are the two types?
Luteolysis - destruction of the corpus luteum
1st Functional luteolysis:
Decreased progesterone (P4) production
2nd Structural luteolysis
Physical degradation, shrinkage, and apoptosis of luteal cells
Programmed cell death - ordered biochemical and morphological changes in the cell (not necrosis)
What are the hormones that control luteolysis?
Oxytocin (from LLC, hypothalamus)
Progesterone (from CL)
Prostaglandin F2-alpha (from endometrium)
Exceptions: primates, dog, cat
What is required in many species for luteolysis?
The uterus is required (in many species)
CL and endometrium must communicate for successful luteolysis
If luteolysis does not occur, animal remains in a sustained luteal phase
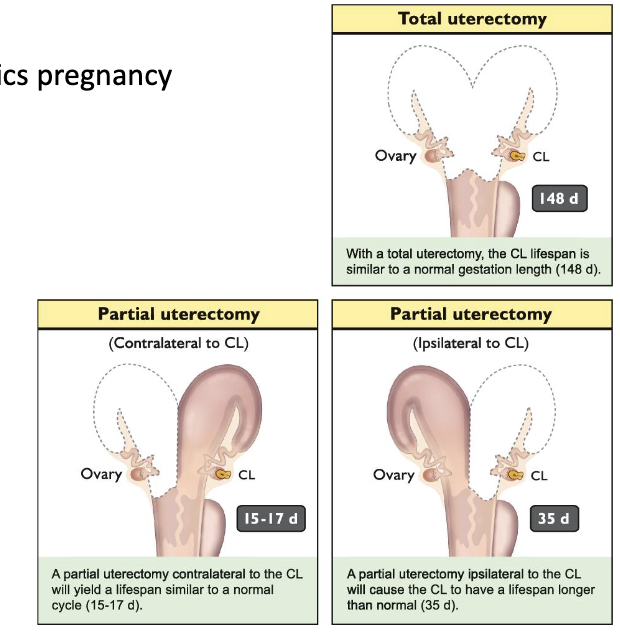
Describes what happens if we remove different parts of the uterus
Remove uterus after ovulation prolongs CL lifespan; mimics pregnancy
Removal of contralateral horn: CL lifespan unaffected
Remove ipsilateral horn: Increased CL lifespan
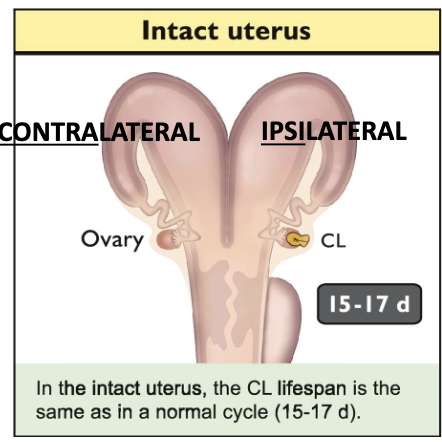
What is the luteolytic hormone in sheep
PGF2a
What is the vascular countercurrent exchange?
Where PGF2a is transported to the ipsilateral ovary via the uter-ovarian vascular countercurrent transport system
Present in cow, ewe, and sow
Relatively high concentrations; no dilution in circulation
PGF2a leaves endometrium via UOV → Passively diffuses from UOV into closely apposed OA → Transported directly to ovary → Luteolysis
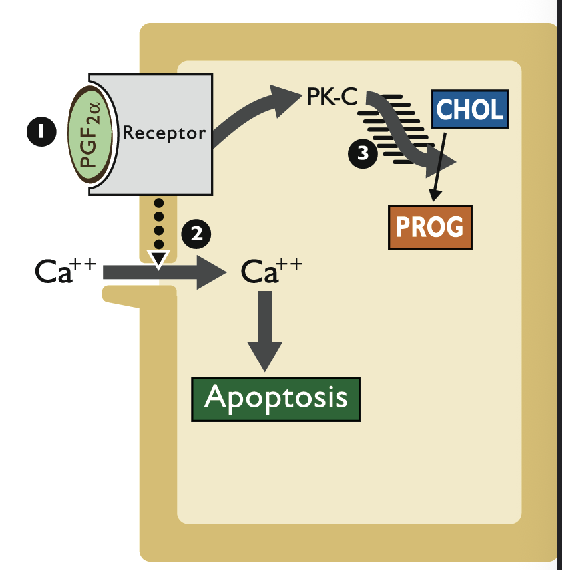
What are the steps resulting in loss of luteal progesterone secretion
PGF2a binds to receptor on plasma membrane
PGF2a-R complex opens Ca++ channels
PGF2a-R complex activates protein kinase C (PK-C) - Inhibits P4 synthesis
What does luteolysis result in
Cessation of P4 secretion
CL structural regression to form corpus albicans
Removal of negative feedback by P4 on GnRH
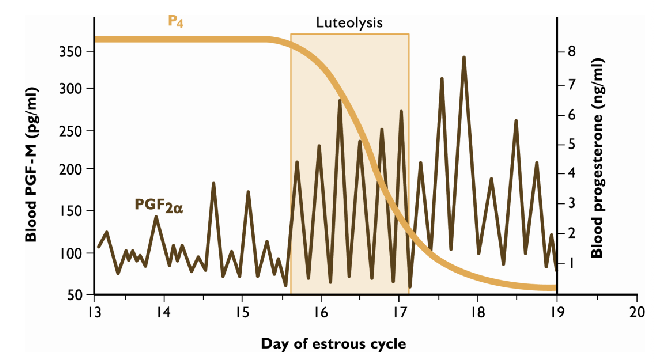
Describe the first half of the estrous cycle and Late luteal phase
First half of the estrous cycle: P4 prevents PGF2a secretion by blocking oxytocin receptors in uterus
After 10-12 days, P4 loses its blocking ability; precise mechanism is unknown
Late luteal phase: oxytocin and PGF2a stimulate each other in a positive feedback manner
Injection of oxytocin → PGF2a secretion from uterus
Injection of PGF2a → rapid release of ovarian oxytocin
A critical number of PGF2a pulses within a given timespan is required to induce complete luteolysis
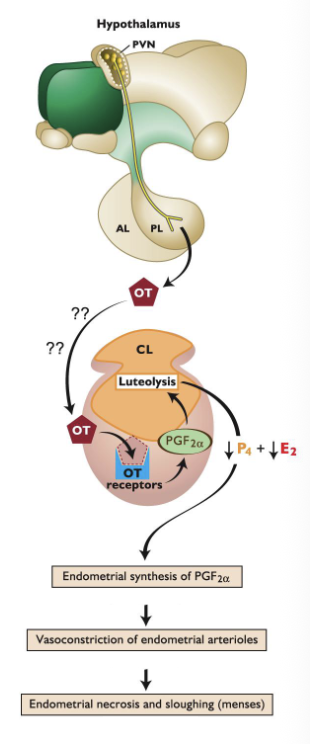
What is the proposed mechanism of luteolysis in primates
The uterus is not required for luteolysis in humans/primates:
Uterectomy does not affect cyclicity
Rhythmic pattern of folliculogenesis, luteal develpment, and luteolysis will occur even if uterus is removed
Proposed mechanism:
oxytocin from posterior pituitary acts on ovary, binds receptor
Small amounts of PGF2a are released, act directly on CL
Endometrial PGF2a causes localized vasocontriction of endometrial arterioles, which initiates menstruation
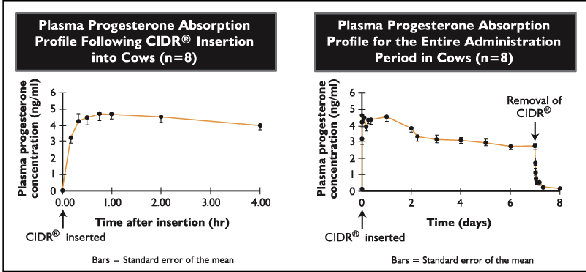
What can be used to synchronize estrus in cattle (introvaginal)
EAZI-BREED CIDR
Controlled internal drug release
Progesterone intravaginal insert
CIDR is inserted for 7 days
Administer Lutalyse on 6th day
Cows and heifers will enter estrus within 2-3 days of CIDR removal
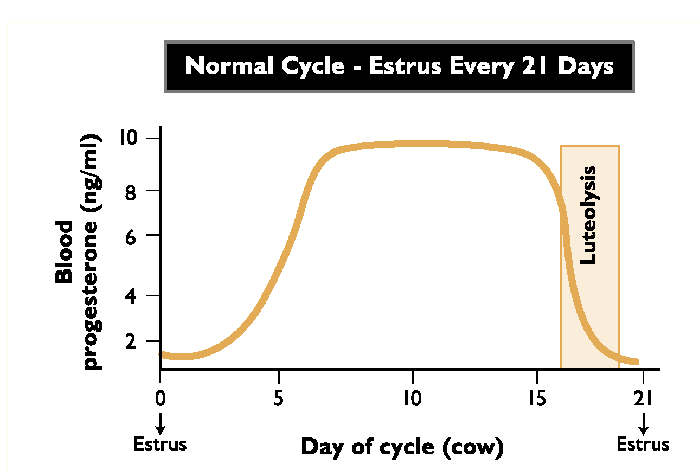
What does a normal estrus cycle look like? When is estrus?
What does the giving a PGF2a incjection in day 0-6 have?
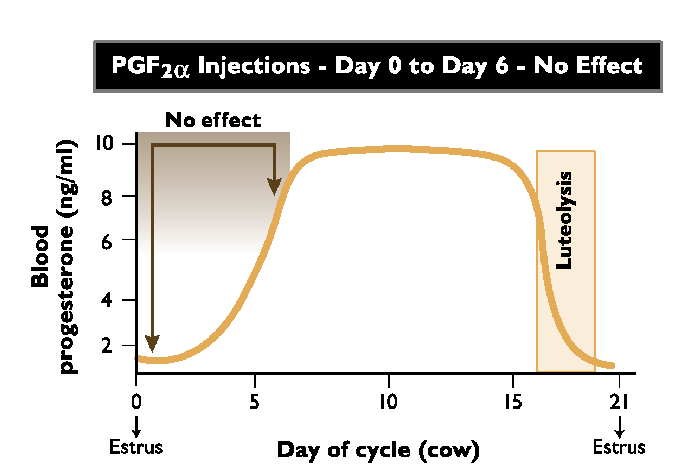
No effect
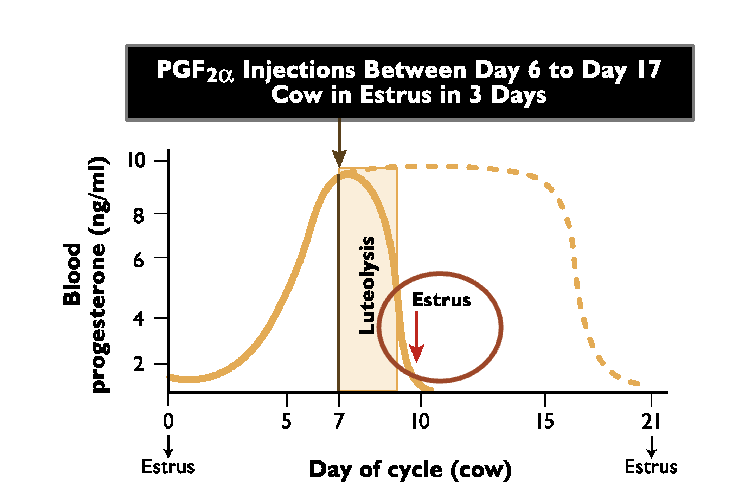
What does giving a PGF2a injection between day 6 and 17 effect?
Cow enters estrus within 3 days after injection
What are the different ways to detect estrus?
Mount detection aids:
Kamar pressure-sensitive mount detector
Heat detector animals
Vasectomized bull
Activity monitors/pedometers
Increased activity during estrus
“AM-PM rule” → breed 12 hours after observing cow in standing heat
Describe the steps of Ovsynch
GnRH is administered into cows that are eligable to be inseminated (must be cycling)
If there is a dominant follicle on the ovary, the cow will ovulate in response
If the cow doesn’t have a dominant follicle, GnRH will promote follicular growth
7 days later - Administer PGF2a to induce luteolysis; cow will enter follicular phase
48 hours later - Administer second injection of GnRH to induce ovulation
16 hours later - Perform timed artificial insemination (without estrus detection)