GW BGZ 2024 Case 9 - Take care of your bacteria and they will take care of you
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
What is the gut microbiome?
The gut microbiome is the community of microorganisms (bacteria, archaea, viruses, fungi) living in the gastrointestinal tract, mostly in the colon. Dominant bacterial groups:
Firmicutes: ferment carbohydrates
Bacteroidetes: digest fiber and polysaccharides
Actinobacteria: support gut barrier and carbohydrate metabolism
Proteobacteria: increase during dysbiosis
It is dynamic, highly diverse, and influenced by diet and lifestyle.
What are the main functions of the gut microbiome?
Metabolic: Ferments fiber → produces SCFAs (acetate, propionate, butyrate), supports energy, lipid, and glucose metabolism.
Barrier/structural: Maintains intestinal lining, strengthens tight junctions, prevents leaky gut.
Immune regulation: Modulates T-cells, promotes immune tolerance, controls inflammation.
Protective: Competes with pathogens and produces antimicrobial compounds.
What is dysbiosis?
Dysbiosis is an imbalance in the gut microbiome, marked by:
Reduced microbial diversity
Loss of beneficial bacteria
Overgrowth of harmful species
Associated with metabolic diseases, inflammatory disorders, and mood problems.
What is the gut–brain axis?
A bidirectional communication system linking the gut and brain through:
Neural pathways: vagus nerve
Endocrine pathways: gut hormones (GLP-1, PYY, ghrelin), cortisol
Immune pathways: cytokines and inflammatory mediators
Metabolic pathways: microbial metabolites like SCFAs and neuroactive compounds
It influences mood, cognition, and stress response.
How does the gut microbiome influence mood?
Neurotransmitters: Produces/regulates serotonin, GABA, dopamine precursors
Inflammation control: SCFAs reduce chronic low-grade inflammation
Gut barrier: Prevents LPS leakage into bloodstream, which otherwise triggers inflammation
Vagus nerve signaling: Direct calming communication to brain
Stress regulation: Modulates HPA axis and cortisol levels
How does the gut microbiome regulate body weight?
Appetite/satiety: SCFAs stimulate GLP-1 and PYY → feel full sooner
Energy extraction: Microbes break down indigestible carbs → extra calories
Inflammation: Dysbiosis → leaky gut → metabolic endotoxemia → fat storage
Metabolism: SCFAs improve insulin sensitivity and lipid metabolism
Gut–brain axis: Signals influence hunger, cravings, and eating behavior
Why is microbial diversity important?
High diversity → better immune and metabolic health, more resilience
Low diversity → higher risk of chronic disease, inflammation, and dysbiosis
How does diet affect the gut microbiome?
Rapid changes: Microbiome can shift within 24–48 hours of diet changes
Western diet (high fat, low fiber): ↓ diversity, ↑ harmful bacteria, ↑ inflammation
Plant-based/high-fiber diet: ↑ beneficial bacteria, ↑ SCFAs, improved metabolism
Long-term diet: Shapes microbial composition, functional capacity, and disease risk
Metabolites: Diet determines whether microbes produce beneficial (SCFAs) or harmful metabolites
What are the effects of protein on the microbiome?
Undigested protein (~10–12%) reaches the colon → fermented by microbes.
Beneficial effects: increased satiety, SCFA production in moderation.
Harmful effects (excess/low fiber): ammonia, hydrogen sulfide, phenols, indoles → damage gut barrier, inflammation, potential insulin resistance.
Source matters:
Animal protein (especially red/processed): more harmful metabolites
Plant protein: often comes with fiber → supports SCFA production, diversity
What are the effects of dietary fats on the microbiome?
Saturated/trans fats: promote dysbiosis, leaky gut, inflammation, metabolic endotoxemia
Unsaturated fats: support microbial diversity, beneficial bacteria, gut barrier
Mechanism: fats → bile acid secretion → microbiome converts to secondary bile acids → activate TGR5 receptor → regulates GLP-1, satiety, energy expenditure
High-fat diets: can reduce diversity, increase pro-inflammatory bacteria
What is the effect of fiber on the microbiome?
Soluble fiber (oats, legumes, fruits): fermented → SCFAs → regulate metabolism, strengthen gut barrier, reduce inflammation
Insoluble fiber (whole grains, vegetables): adds bulk, supports gut motility and structure
Microbiota-accessible carbohydrates (MACs): promote diversity and beneficial bacteria
Low fiber intake: microbes may degrade mucus → gut barrier damage, inflammation
SCFAs roles: appetite regulation (GLP-1, PYY), energy metabolism, anti-inflammatory effects, gut-brain signaling
What are probiotics and prebiotics?
Probiotics: live microorganisms that confer health benefits
Compete with harmful bacteria, support gut barrier, modulate immunity, produce SCFAs
Sources: yogurt, kefir, fermented vegetables
Prebiotics: non-digestible fibers that feed beneficial microbes, increase SCFA production
Sources: inulin, FOS, garlic, onions, bananas
Synbiotics: combination of probiotics + prebiotics → enhance survival and activity of probiotics
What role does the gut microbiome play in metabolic diseases (T2DM, obesity)?
Carbohydrate fermentation → beneficial:
Produces SCFAs → improve insulin sensitivity, reduce inflammation, strengthen gut barrier, regulate appetite and energy balance
Protein fermentation → potentially harmful:
Produces ammonia, phenols, indoles, hydrogen sulfide, BCFAs → damage gut lining, increase inflammation, promote insulin resistance
Dysbiosis: reduced diversity, altered microbial composition → chronic low-grade inflammation, impaired metabolic regulation
Mechanisms:
Increased gut permeability → endotoxemia (LPS)
Altered SCFA/harmful metabolite balance → disrupted insulin signaling and energy metabolism
Key concept: metabolic health depends on balance between carbohydrate vs protein fermentation
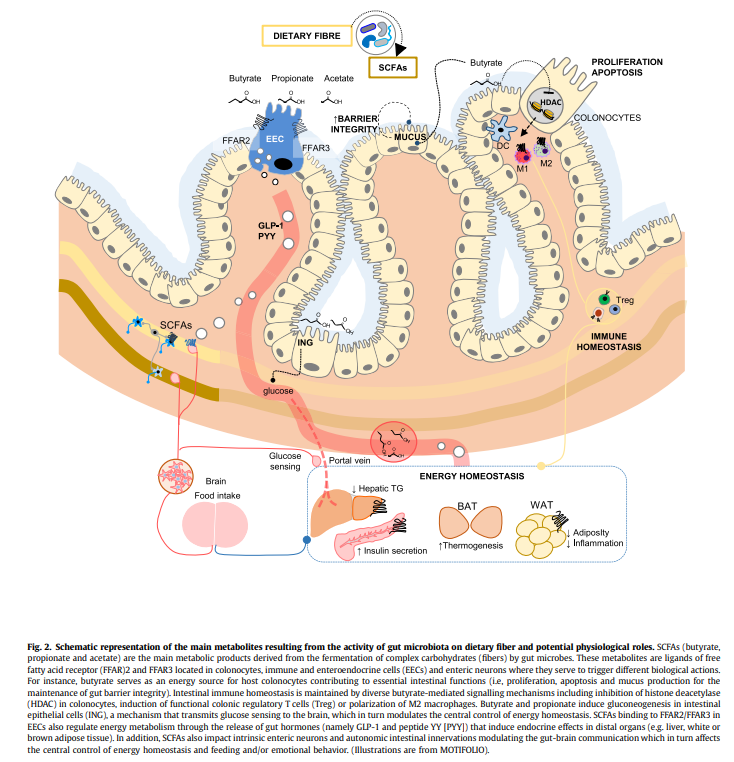
What are short-chain fatty acids (SCFAs) and their effects? (CHO metabolites)
SCFAs are metabolites produced by gut microbes fermenting dietary carbohydrates, mainly acetate, propionate, and butyrate.
Butyrate: primary fuel for colonocytes; strengthens gut barrier, supports epithelial growth and repair.
Acetate & Propionate: regulate lipid and glucose metabolism; acetate serves peripheral tissues as energy, propionate regulates gluconeogenesis in the liver.
General effects of SCFAs:
Reduce inflammation
Stimulate satiety hormones GLP-1 and PYY → reduce food intake
Improve insulin sensitivity
Contribute to gut-brain communication and energy homeostasis
Overall: SCFAs are highly beneficial, supporting gut integrity, metabolism, and immune regulation.
What is lactate and its role in the microbiome?
Lactate is an intermediate metabolite, not a final product.
It is converted by other microbes into butyrate or propionate, supporting cross-feeding.
This process enhances SCFA production indirectly and contributes to maintaining a healthy gut microbial ecosystem.
What is succinate and its significance?
Succinate is an intermediate from carbohydrate fermentation.
It can be converted into propionate, contributing to SCFA pools.
Context-dependent effects:
In balance: beneficial for metabolism
In excess: can accumulate → promote inflammation and dysbiosis
What harmful metabolites are produced from protein fermentation?
Protein fermentation produces several metabolites that are often toxic or pro-inflammatory:
Ammonia: from amino acid deamination; toxic to colonocytes, impairs energy metabolism, disrupts tight junctions, increases gut permeability, promotes inflammation
Phenols (including p-cresol): from aromatic amino acids; cytotoxic, increase oxidative stress, impair gut barrier, systemic effects include insulin resistance and kidney impact
Indoles: from tryptophan; low levels beneficial for gut barrier and anti-inflammatory signaling, high levels toxic and pro-inflammatory
Hydrogen sulfide (H₂S): from sulfur-reducing bacteria; inhibits butyrate oxidation, damages mucus layer, increases gut permeability, toxic at high levels
Branched-chain fatty acids (BCFAs): from valine, leucine, isoleucine; markers of protein fermentation, may alter cell membranes, associated with impaired gut barrier, less beneficial than SCFAs
What is p-cresol and its systemic effects?
p-Cresol is a phenol produced from tyrosine metabolism.
Local effects: toxic to intestinal cells, impairs gut barrier integrity
Systemic effects: absorbed and processed in the liver, affects kidneys, accumulates in kidney dysfunction, may contribute to insulin resistance and ectopic fat accumulation
Overall: potentially harmful; human evidence still limited, but it is a significant protein fermentation metabolite linked to metabolic disturbances
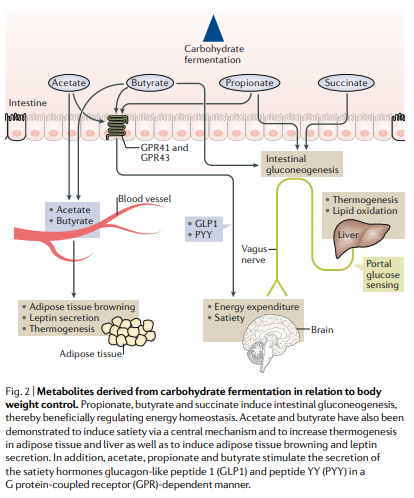
What are the general roles of carbohydrate fermentation metabolites?
Carbohydrate fermentation primarily produces SCFAs, lactate, succinate, and small amounts of ethanol.
Regulate metabolism: SCFAs modulate glucose and lipid metabolism, support liver gluconeogenesis, and provide peripheral energy.
Maintain gut health: butyrate fuels colonocytes, supports epithelial repair, and maintains healthy gut environment
Appetite and energy balance: stimulate GLP-1 and PYY, increasing satiety and modulating food intake
Insulin sensitivity: SCFAs enhance insulin signaling, reduce inflammation, and lower metabolic disease risk
Gut barrier function: strengthen tight junctions, reduce “leaky gut,” and lower endotoxemia (LPS translocation)
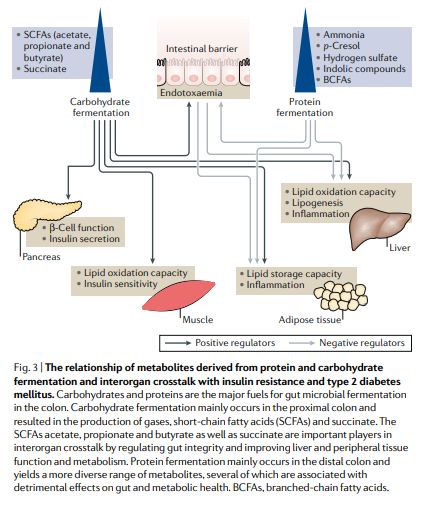
How do protein fermentation metabolites affect gut and metabolic health?
Protein fermentation produces mostly harmful metabolites: ammonia, phenols, indoles, hydrogen sulfide, BCFAs, and p-cresol.
Effects on gut: toxic to colonocytes, disrupts epithelial energy metabolism, damages tight junctions, increases permeability, promotes inflammation
Systemic effects: may impair glucose metabolism, contribute to insulin resistance, ectopic fat deposition, and kidney burden (p-cresol)
Nuance: some indole derivatives may be beneficial at low levels for anti-inflammatory signaling and gut barrier support
Overall: excess protein fermentation shifts microbiome toward a pro-inflammatory, less beneficial state, contrasting carbohydrate fermentation. This can lead to metabolic diseases such as T2DM and NAFLD
What is the difference between microbiota and microbiome?
Microbiota: the community of microorganisms (bacteria, fungi, viruses, archaea) living in a specific environment
Microbiome: includes the microbiota plus their genetic material and metabolic products
The microbiome therefore reflects not only which microbes are present, but also their functional capacity
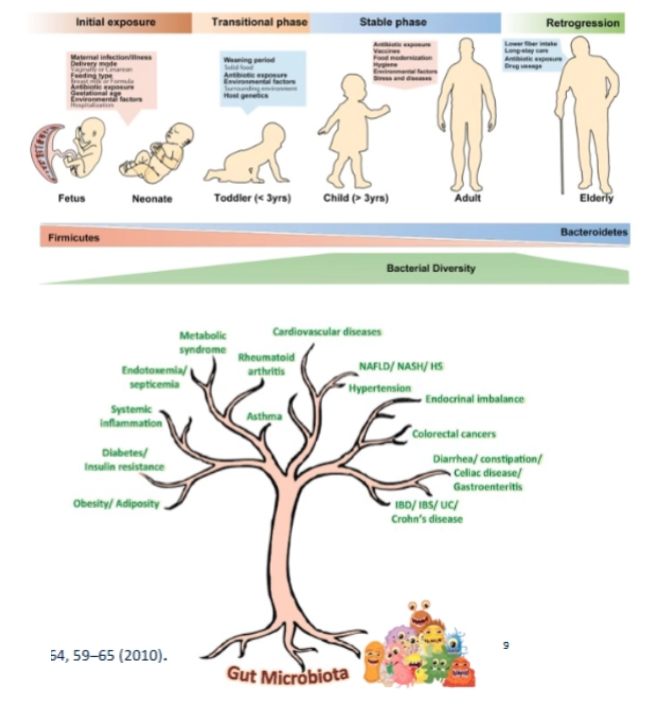
What are the main characteristics of the human gut microbiota?
Composed of bacteria, archaea, fungi, and viruses
Bacteria are the most dominant and diverse group (~2000 species identified)
Fully matures around age 2–3 years
Strongly influenced by early-life factors (birth mode, diet, antibiotics)
Each individual has a unique microbial composition (“microbial fingerprint”)
Contains ~100 trillion microorganisms
Weighs up to 1.5 kg
Encodes ~150 times more genes than the human genome
Functions as a “superorganism” that plays a crucial role in host metabolism
Highest density of microbes in colon
Why is the gut microbiota considered a “superorganism”?
It has a massive genetic capacity exceeding that of the human genome
Performs essential metabolic functions that humans cannot perform alone (e.g. fiber fermentation)
Produces metabolites that regulate host physiology
Interacts with immune, metabolic, and endocrine systems
Acts almost like an additional metabolic organ
How quickly can diet influence the gut microbiome?
Changes can occur within 24–48 hours
Short-term dietary changes rapidly alter microbial composition
However, long-term dietary patterns are required for sustained effects
Example: animal-based diets can temporarily increase diversity but may not be beneficial long-term
Why are dietary fibers important for the microbiome?
Fibers are the preferred energy source for gut microbes
Promote growth of beneficial bacteria
Increase production of SCFAs
Improve metabolic health (body weight, cholesterol, blood pressure, glucose regulation)
Higher fiber intake is consistently associated with better health outcomes
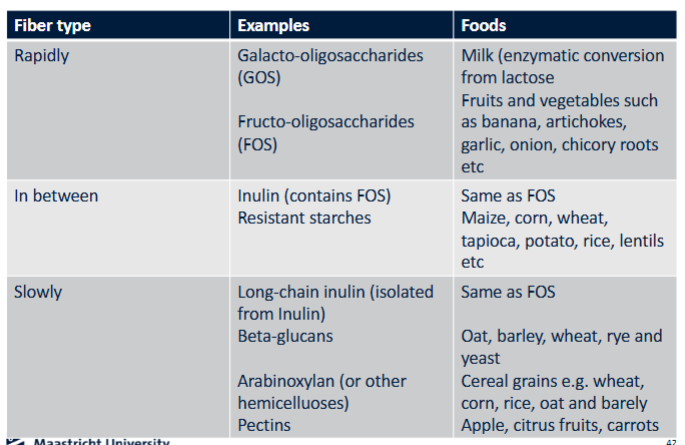
What is the difference between fermentable and non-fermentable fibers?
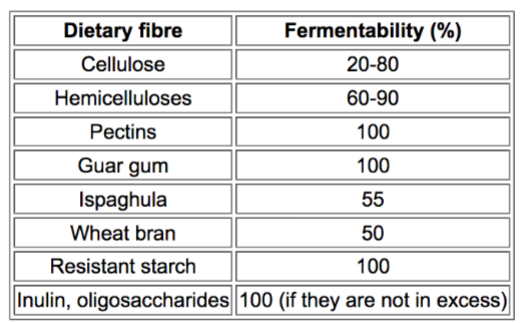
Not all fibers are fully fermentable
Fermentable fibers (prebiotics): used by microbes to produce beneficial metabolites (e.g. inulin, resistant starch)
Non-fermentable fibers: mainly contribute to stool bulk and gut motility
Both types are important for gut health
What are prebiotics and probiotics?
Prebiotics: non-digestible food components (fibers, polyphenols) that stimulate growth of beneficial bacteria
Probiotics: live microorganisms that provide health benefits when consumed
Prebiotics act as “food” for probiotics
Together, they support microbial balance and function
What are the main products of fiber fermentation?
Short-chain fatty acids (SCFAs): acetate, propionate, butyrate
Intermediate metabolites: lactate, succinate
Gases: carbon dioxide, hydrogen, methane
SCFAs are the most important metabolites for metabolic health
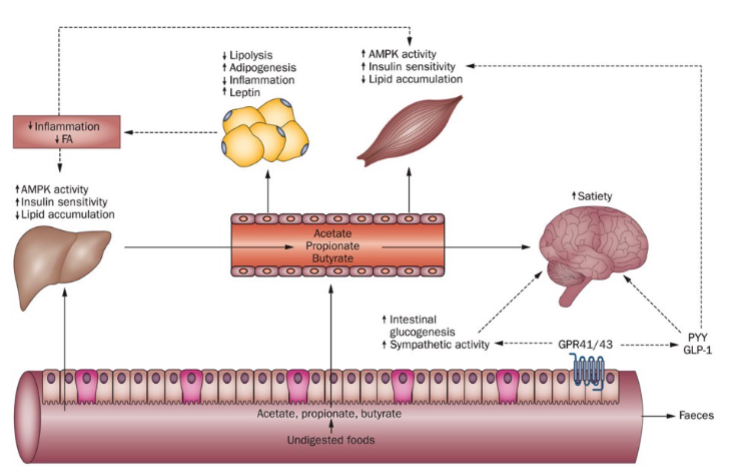
What are the functions of SCFAs in the body?
Serve as energy sources (especially butyrate for colonocytes)
Regulate glucose and lipid metabolism
Stimulate satiety hormones (GLP-1 and PYY)
Improve insulin sensitivity
Reduce inflammation
Strengthen gut barrier by enhancing tight junctions
Reduce endotoxemia (LPS translocation)
Influence gut-brain axis and energy balance
How do SCFAs improve body weight control and insulin sensitivity?
Increase secretion of GLP-1 and PYY → reduce appetite and food intake
Improve insulin signaling pathways
Reduce systemic inflammation
Enhance fat oxidation and energy expenditure
Strengthen gut barrier → reduce metabolic endotoxemia
Regulate hepatic glucose production (especially propionate)
What happens when dietary protein reaches the colon?
Approximately 10–12 g of protein reaches the colon daily (Western diet)
Microbes ferment these proteins (proteolytic fermentation)
Produces metabolites that are often harmful or less beneficial than SCFAs
Amount depends on protein type (animal vs plant) and digestibility
What metabolites are produced from protein fermentation?
Ammonia
Phenols (including p-cresol)
Indoles
Hydrogen sulfide (H₂S)
Branched-chain fatty acids (BCFAs)
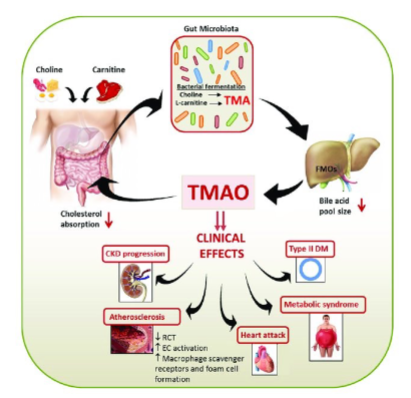
Trimethylamine N-oxide (TMAO, especially from red meat)
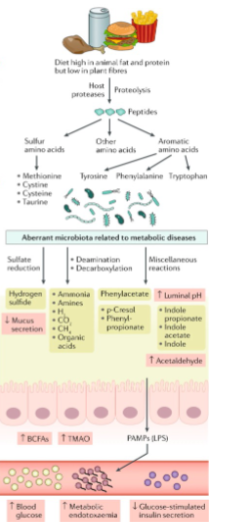
What are the effects of protein fermentation metabolites?
Often toxic to gut epithelial cells
Damage gut barrier integrity
Increase gut permeability (“leaky gut”)
Promote inflammation
Contribute to metabolic dysfunction (insulin resistance, liver fat accumulation)
Associated with kidney dysfunction (e.g. p-cresol)
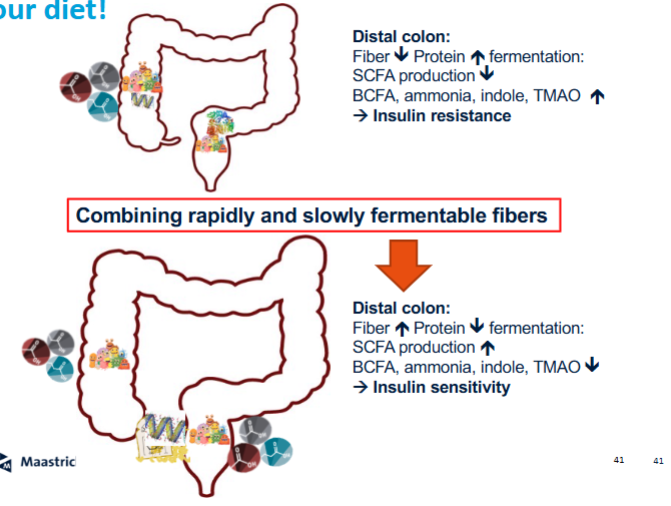
Why is fiber intake important in preventing harmful protein fermentation?
Fiber promotes saccharolytic fermentation over proteolytic fermentation
Ensures microbes use carbohydrates instead of proteins as energy source
Reduces production of toxic metabolites
Maintains healthier gut environment
Particularly important in the distal colon where fiber availability is lower
How is obesity linked to the gut microbiome?
Obesity is associated with altered microbiota composition (dysbiosis)
Reduced microbial diversity
Increased energy extraction from diet
Increased inflammation due to endotoxemia
Altered SCFA production and signaling
Changes in gut permeability
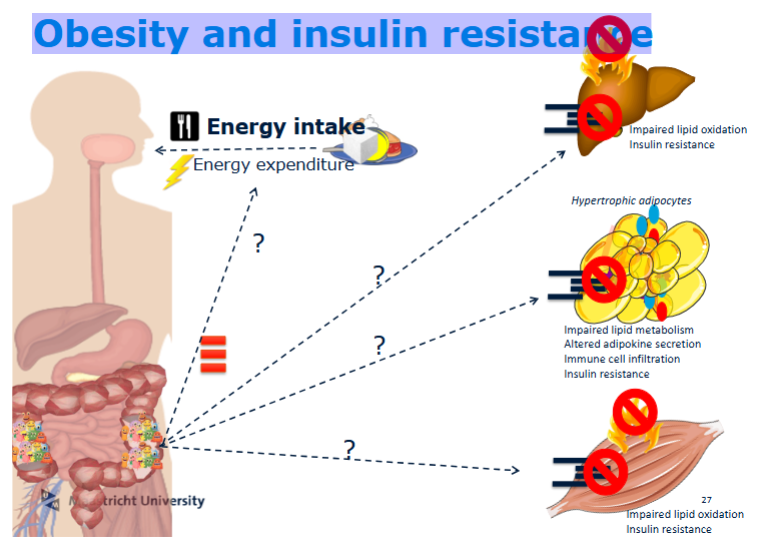
What is insulin resistance and how is it related to the microbiome?
Insulin resistance occurs when cells do not respond properly to insulin
Insulin can bind receptor, but signaling cascade is impaired
Leads to reduced glucose uptake and increased fat storage
Microbiome contributes via:
Inflammation
Altered metabolite production
Increased gut permeability (LPS leakage)
What role does butyrate play in metabolic health?
Primary energy source for colon cells
Maintains gut barrier integrity
Reduces inflammation
Improves insulin sensitivity
Supports overall gut health
Only produced by specific gut bacteria
What is the importance of combining different types of fiber?
Different fibers ferment at different rates (rapid vs slow)
Combining them ensures continuous SCFA production in the colon
Supports microbial diversity
Maximizes metabolic benefits
What are the key differences between carbohydrate and protein fermentation?
Carbohydrate fermentation:
Produces SCFAs
Anti-inflammatory
Improves metabolism
Supports gut barrier
Protein fermentation:
Produces toxic metabolites
Pro-inflammatory
Damages gut barrier
Associated with metabolic diseases
What are the key take-home messages about diet and the microbiome?
Gut microbiota strongly influences metabolism
Diet can rapidly alter microbiota composition
Fiber intake promotes beneficial microbial activity and SCFA production
Protein fermentation produces harmful metabolites
Increasing fiber intake can suppress harmful fermentation processes
Microbiome modulation is a key factor in preventing and managing metabolic diseases
What are the most important things to know for the exam?
Definitions of microbiota vs microbiome
Types of fermentable carbohydrates (e.g. inulin, resistant starch)
Products of fiber fermentation (SCFAs, gases, intermediates)
Products of protein fermentation (ammonia, phenols, indoles, H₂S, BCFAs, p-cresol, TMAO)
Effects of SCFAs on body weight and insulin sensitivity
Harmful effects of protein-derived metabolites on gut and metabolic health