AC GI intubation & nutrition
1/16
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
17 Terms
*Religious restrictions
muslims
christians
hinduism
judaism
church of christ of latter-day saints
muslims: no pork, alcohol, caffeine
ramadan: fasting from sunrise to sunset
christianity:
baptists: minimal or no alcohol assumption
catholics: lent and meatless days
hinduism: no meats, alcohol
judaism: no pork, mixing with milk or dairy products with meat dishes
church of christ of latter day saints: no alcohol, tobacco, no caffeine
*Alternative food diets
vegans?
ovo-lacto?
lacto?
pescatarian?
medical diets are.. (2)
vegans: no meats (incl. dairy & eggs)
ovo-lacto: no meats, dairy, and eggs are okay
lacto: no meats, eggs, milk is okay
pescatarian: no meat, fish, and shellfish is okay
medical diets: casein & gluten free +++ ketogenic diets (for epilepsy)
Nutritional screening
purpose?
risk factors?
lab tests!
to identify malnutrition or at risk patients
risk factors: unintentional weight loss, modified diets, altered nutritional symptoms (diarrhea + constipation) (iV fluids for more than 4-7 days)
lab tests: the most readily plasma protein is albumin
*Types of therapeutic diets? (liquids)
name as many as discussed!
if they are NPO for an extensive amount of time/ any GI surgery, they are at risk for… ? and they should be put on what diet?
clear liquids (tea)
full liquid (ice cream, custards)
pureed/thickened liquids
mechanical soft (flaked fish, cottage cheese, rice)
soft/low residue (pasta, casseroles)
high fiber (fresh uncooked fruits, steamed veggies)
low sodium (restrictions: 4g, 2g, 1g, 500mg
risk for aspiration, put them on clear liquids
Promoting appetite
number one way to promote appetite is to?
brush your teeth
Oral feedings:
maintain independence & dignity by..
assess for?
high risk patients have:
verbal coaching while feeding provides positive reinforcements
allow patients to select their own foods
aspiration risk
decreased alertness, poor gag reflex, difficulty managing saliva, oral suction at bedside
Decrease risk for aspiration
provide __ minute rest periods before eating
feed on the stronger side of their mouth (unilateral weakness (1/2- 1tsp)
remain upright for at least 30-60 min after meal
patient should swallow twice to clear pharynx
inspect mouth for pocket of food
30 min
Dysphagia
defined as?
warning signs?
leads to?
be aware of ?
put them on a ___ diet
feed slowly, smaller size bites
match speeding of feeding to patients readiness
difficulty swallowing
due to neurological, muscular, obstruction type of disorders
cough during eating, change in voice after swallowing food, abnormal movements of mouth, tongue, lips, abnormal gag reflex
malnutrition and aspiration pneumonia
be aware of silent aspiration
put them on a liquid, thin/ low viscosity diet, honey-like
Oral feedings: visual deficits
identify food location on meal plate (meat at 9 o clock)
GI Intubation - types
temporary tubes
small bore: Dobhoff (weighted)
DONT NEED TO KNOW NAMES OF TUBES
You need something large to decompress the stomach. if you’re feeding alone, use a small one because its more comfortable
Nasogastric (ng)
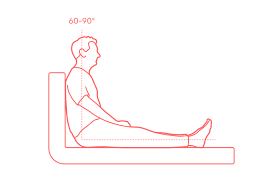
*Inserting an NG tube
place patient in..
determine the length and mark with tape (NEMU. no longer NEX).
nemu: nose, ears, mid umbilicus
if patient is awake, have them ___ ___ while placing GI tube (it simulates actually swallowing and can ease the tube down quicker + more comfortably)
remove tube if they go through respiratory distress
high Fowlers position (90 degree
*NEX vs NEMU
always use NEMU for ___
NEX(xyphoid) in general underestimates the length and ends up more in lungs than it actually sits int he stomach
kids
*Contraindications for NGT?
suspected or confirmed basilar skull fractures
trauma to the face or facial fractures
esophageal obstruction or perforation
combative patients
*GI intubation
how do you check that its properly in there?
still perform oral care
if you see red color on strip, do not need xray
use Xray (KUB), or pH strips
*Oral Medication via enteral tube
flush tube with at least _ sterile water in between meds
15-30mL but depends on patient
*Enteral feeding
when you’re feeding them, they should be in ___ position
if not?
start them off full strength, but if its uncomfortable then do half strength
high Fowlers
they aspirate if not