ANHB2212 - Weeks 1-3 of Development
1/76
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
77 Terms
Ovum
A mature haploid egg cell
Zygote
A fertilized, diploid single-celled egg
Embryo
The egg from the first mitotic division/cleavage.
Fetus
The developing human organism from 8 weeks once all main body parts are recognisable.
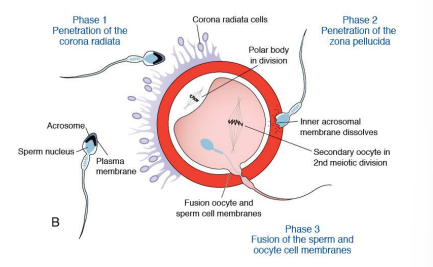
Describe the process of fertilization.
1 - Sperm penetrates the corona radiata
2 - Release of acrosomal enzymes allows sperm to penetrate the zona pellucida
3 - Sperm penetration causes cortical granules to release their contents, rendering the zona pellucida impenetrable to others.
4 - DNA replication of male and female pronucleus that fuse to form a diploid zygote that initiates mitosis to form a 2-celled embryo
Proliferation
Increase in cell number
Cavitation
Formation of internal space
Differentiation
Alteration of developmental trajectory
Migration
Cell movement from one place to another
Induction
Cell triggers neighboring cells to differentiate
Combination
Combination of multiple germ layers to form whole organs
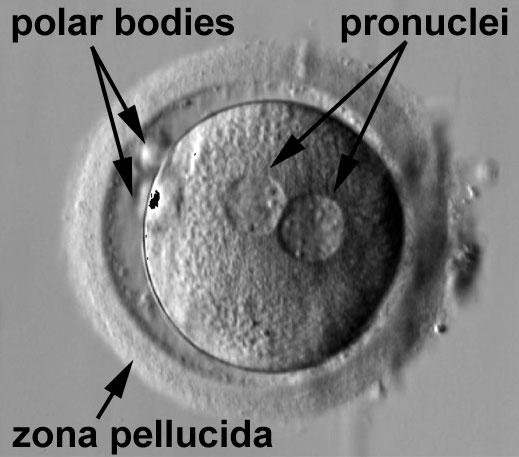
Pronuclear Stage
Zygote approximately 12 to 15 hours after fertilization (human).
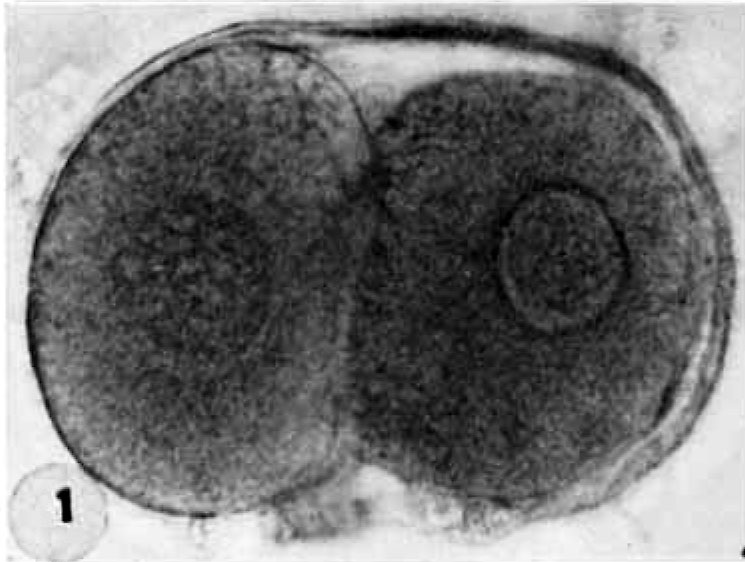
Cleavage
Repeated mitotic divisions during week one of embryonic development (days 0-4) that occurs as the conceptus migrates down the uterine tube.
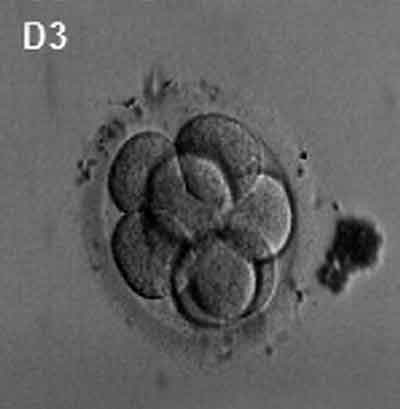
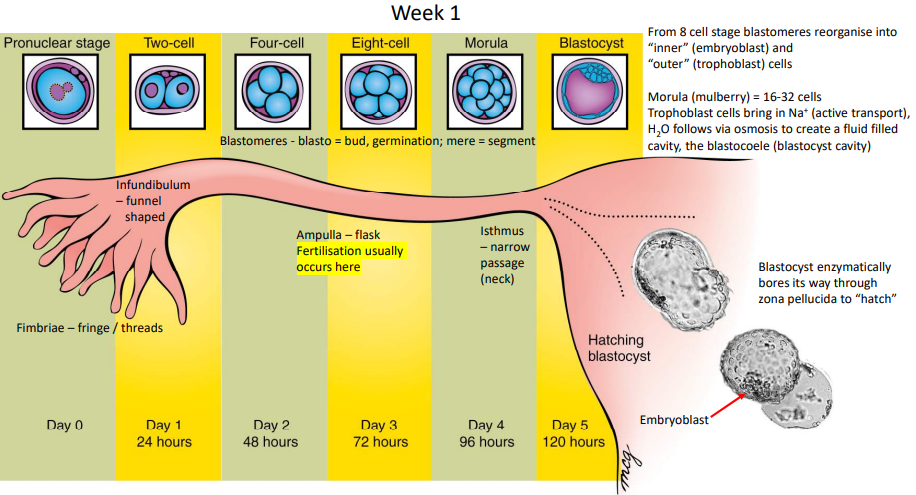
What occurs at the 8-cell stage of cleavage?
Blastomeres reorganise into inner embryoblast cells and outer trophoblast cells (now termed a blastocyst)
Where does fertilisation usually occur?
Ampulla of the uterine tube
What occurs at the 16-32 cell stage of cleavage?
The conceptus reaches the uterus and is now termed a Morula. At this stage, trophoblasts bring Na+ into the conceptus via active transport where H2O follows via osmosis to form the blastocoele (blastocyst cavity)
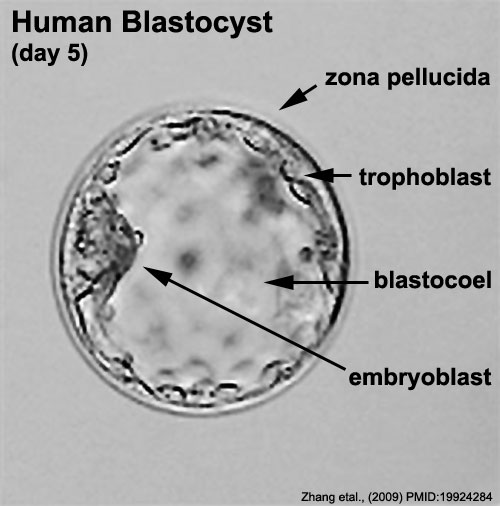
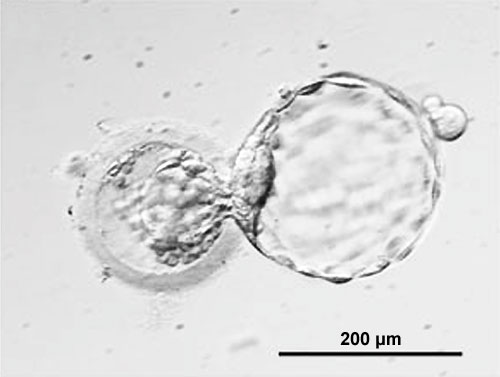
Describe hatching
At day 5, the blastocyst enzymatically bores its way through the zona pellucida.
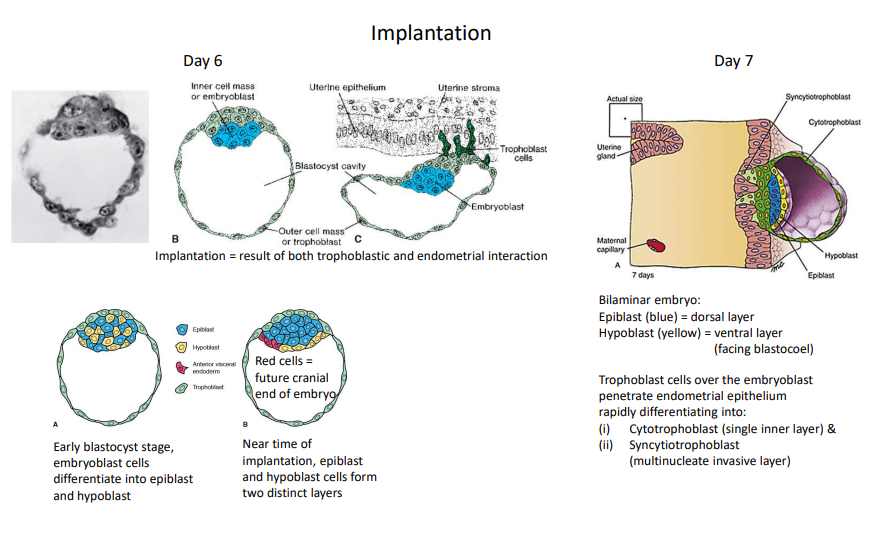
Describe implantation.
On day 6, trophoblasts attach to the endometrium. In the early blastocyst stage, embryoblasts differentiate into epiblasts and hypoblasts. Near implantation, these form two distinct layers. At day 7, trophoblasts penetrate the endometrial epithelium, rapidly differentiating into inner cytotrophoblasts and outer syncytiotrophoblasts.
Cytotrophoblast
Single inner cellular layer of the trophoblast. It is mitotically active and builds and nourishes the syncytiotrophoblast.
Syncytiotrophoblast
Multinucleate invasive outer layer of trophoblast. It lacks cell membranes and obtains nutrients for the developing embryo.
Summarise what occurs during week 1 of embryonic development.
Day 0 - Pronuclear stage
Day 1 - Cleavage begins, 2-cell stage
Day 2 - 4-cell stage
Day 3 - 8-cell stage, embryoblasts and trophoblasts form
Day 4 - Morula, blastocoele forms
Day 5 - Hatching
Day 6 - Implantation, epiblast and hypoblast formed from embryoblasts (bilaminar embryo)
Day 7 - Implantation, cytotrophoblast and syncytiotrophoblast formed from trophoblast
What does the anterior visceral endoderm eventually form?
Cranial end of embryo
Etymology: Zygote
Yoked or joined
Etymology: Zona
Zone, band or layer
Etymology: Pellucid
Clear, translucent, allows for passage
Etymology: Morula
Mulberry
Etymology: Blast
Germ, bud or sprout
Etymology: Tropho
Nourishment, food or feeding
Etymology: Cyst
Bladder, pouch or bag
Etymology: Coele
Hollow, cavity or chamber
How is the amniotic cavity formed?
At day 8, epiblast separates from trophoblast to form amnioblasts that create the amniotic cavity.
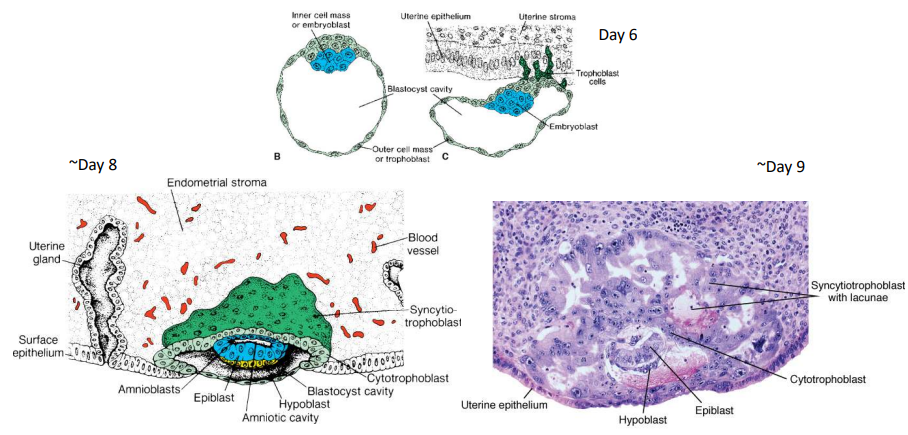
How are lacunae formed?
At day 9, they are developed within syncytiotrophoblast to enable the transfer of nutrients, gases, and wastes.
How is Heuser's Membrane / Exocoelomic Membrane formed?
At day 9, some hypoblasts migrate along the inner cytotrophoblast lining of the blastocoel and secrete extracellular matrix that forms the membrane that surrounds the blastocoel, now called the primary yolk sac.
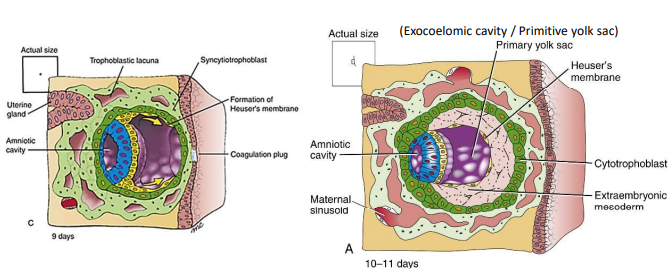
How is the extraembryonic mesoderm formed?
At day 10-13, a new layer forms between inner surface of cytotrophoblast & outer surface of amnion and Heuser's membrane.
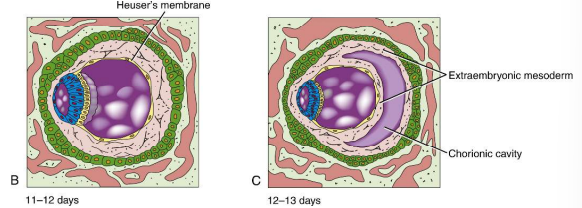
How is the chorionic cavity formed?
Small pockets within the extraembryonic mesoderm coalesce on day 13.
Entymology: Exo
Outside
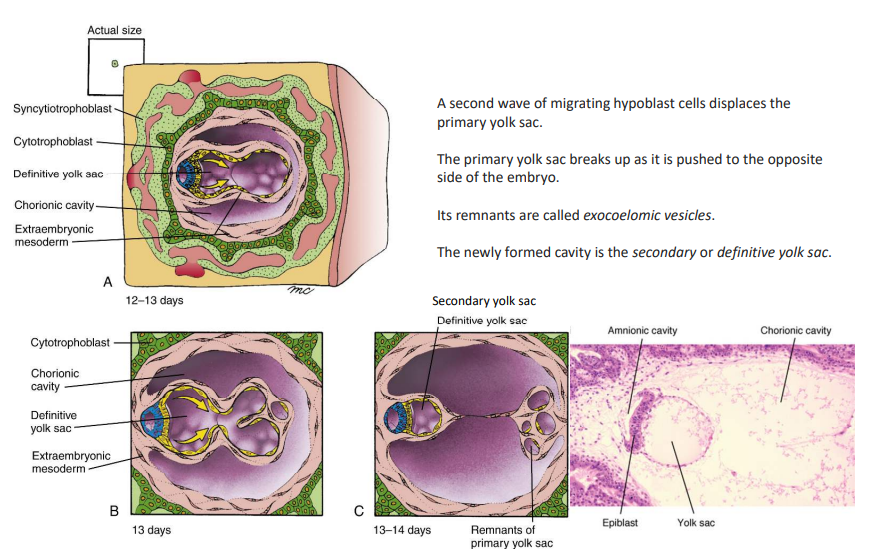
How is the definitive yolk sac formed?
At days 12-13, a second wave of migrating hypoblasts displaces the primary yolk sac, where it is broken and pushed to the opposite side of the embryo. On day 14, the new cavity is called the definitive yolk sac, and its remnants are exocoelomic vesicles.
How is the connecting stalk formed?
On days 14-15, it develops from extraembryonic mesoderm.
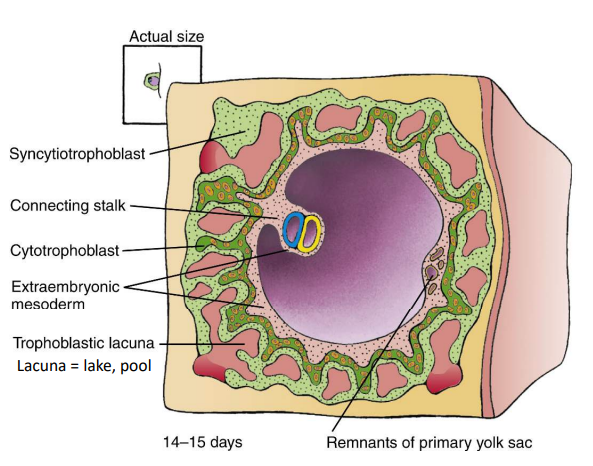
What does the connecting stalk suspend?
Bilaminar embryo, amniotic cavity and yolk sac in the expanded chorionic cavity.
When is the bilaminar embryo formed?
When embryoblasts differentiate into epiblast and hypoblast.
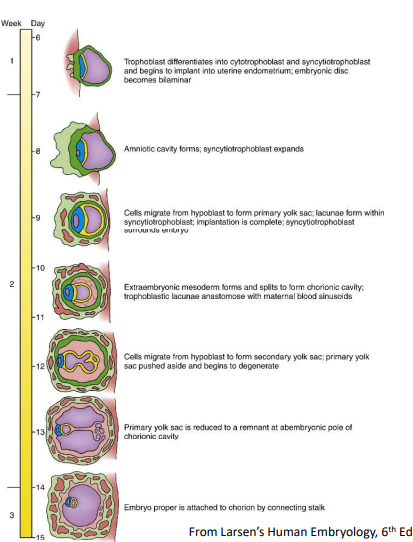
Summarise what occurs during week 2 of embryonic development.
Day 8 - Amniotic cavity formed
Day 9 - Lacunae and Heuser's membrane formed
Day 10-13 - Extraembryonic mesoderm and chorionic cavity formed
Day 14 - Definitive yolk sac formed
Day 14-15 - Connecting stalk formed
How is the primitive streak formed?
On day 15, the embryonic disc elongates to form the primitive streak along the midline of the epiblast.
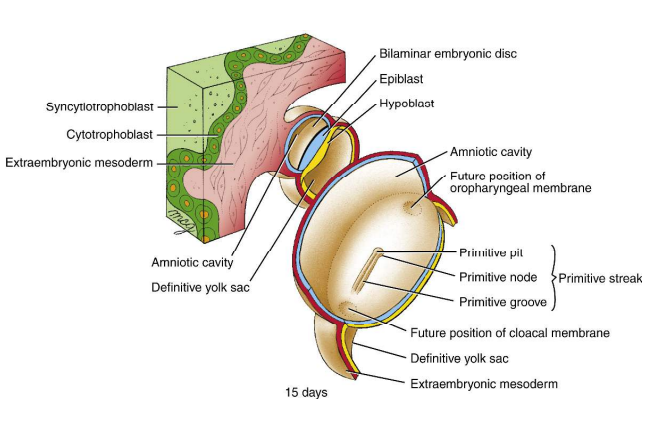
When is the embryo defined directionally?
At day 15 when the primitive streak is formed.
What is the dorsal surface of an embryo?
Epiblast
What is the ventral surface of an embryo?
Hypoblast
What is the caudal end of an embryo?
Towards primitive streak
What is the cranial end of an embryo?
Away from primitive streak
How is medial and lateral defined for an embryo?
By its primitive streak as the midline
Gastrulation
At days 14-15, multiplying epiblasts migrate down into the primitive groove to replace the hypoblast layer with endoderm. At day 16, a second wave of epiblast migration forms intraembryonic mesoderm, with the remaining epiblast being labelled ectoderm.
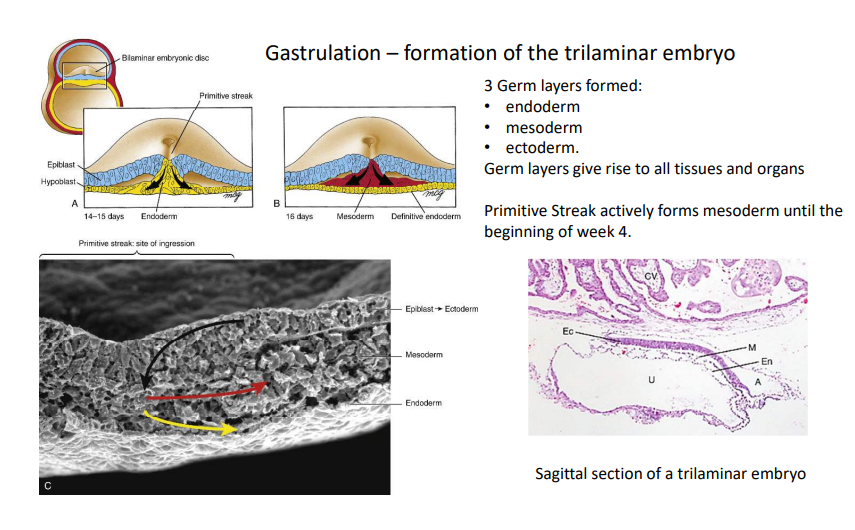
Oropharyngeal Membrane
Membrane with an absence of mesoderm at the cephalic end of the embryo that is the location of the future primitive mouth.
Cloacal Membrane
Membrane with an absence of mesoderm at caudal end of embryo that is the location of future anus
How is the notochord formed?
At day 17, the notochordal plate separates from the endoderm and fuses to form the solid notochord.
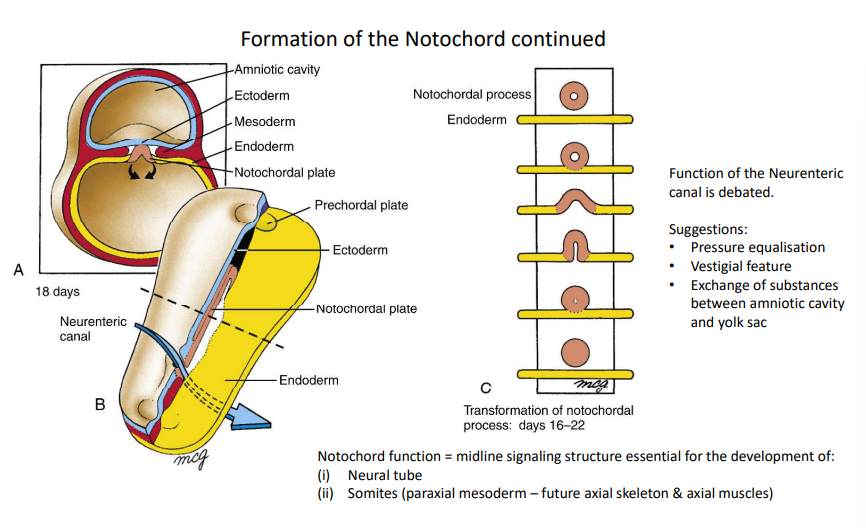
What is the purpose of an open notochordal process?
It forms the neuroenteric canal for communication between the yolk sac and amniotic cavity.
How is the allantois formed?
On day 16, the allantois appears as a small outpouching from the caudal wall of the yolk sac that projects into the connecting stalk.
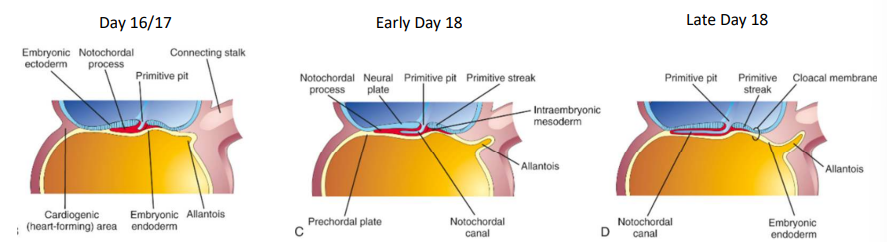
Etymology: Allantois
Sausage-shaped
What is the purpose of the allantois?
Early blood formation (vasulogenesis) and is associated with the urinary bladder. Allantois blood vessels give rise to umbilical arteries and veins.
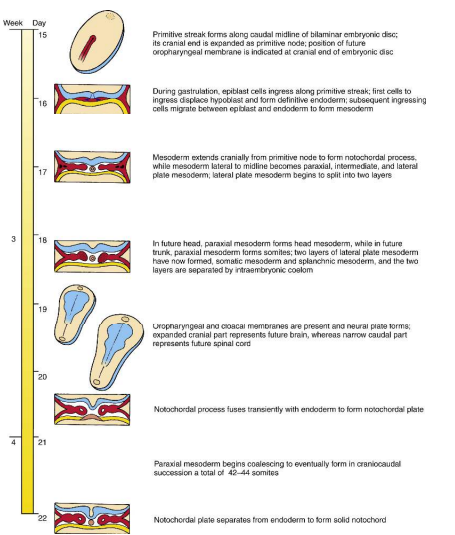
Summarise what occurs during week 3 of embryonic development.
Day 15 - primitive streak formed
Day 14-16 - Gastrulation
Day 16 - Allantois appears
Day 17 - Notochord formed
How is the primary stem villus of the placenta formed?
At days 11-13, it forms as cytotrophoblast and syncytiotrophoblast push intro the endometrium.
How is the secondary stem villus of the placenta formed?
At day 16, it forms as extraembryonic mesoderm, cytotrophoblast and syncytiotrophoblast push intro the endometrium.
How is the tertiary stem villus of the placenta formed?
At day 21, it forms as blood vessels appear from extraembryonic mesoderm.
What 4 layers do gases, nutrients and wastes move through during maternal and embryonic circulation?
1. endothelium of villus capillaries
2. loose connective tissue in villus core
3. cytotrophoblast
4. syncytiotrophoblast
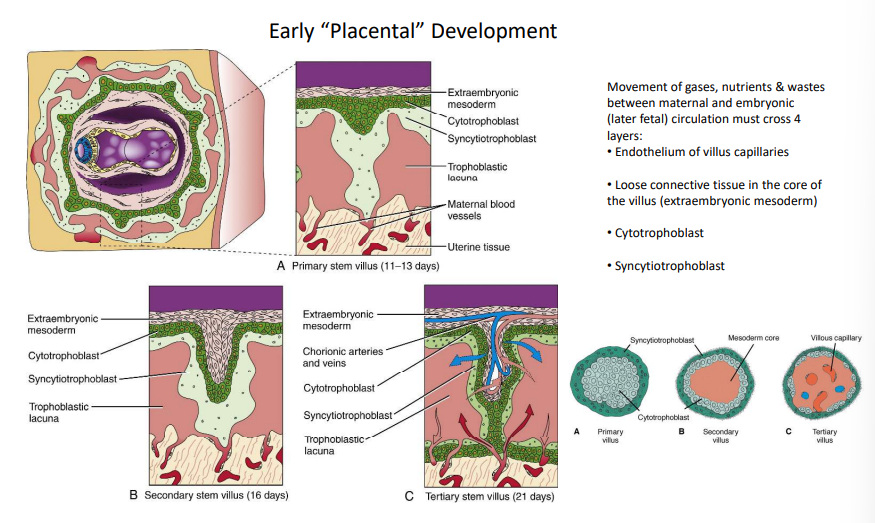
What happens at the end of week 3 regarding early placental development?
Tertiary villi capillaries make contact with the capillaries of mesoderm of chorionic plate & connecting stalk, which make contact with developing intraembryonic circulatory system
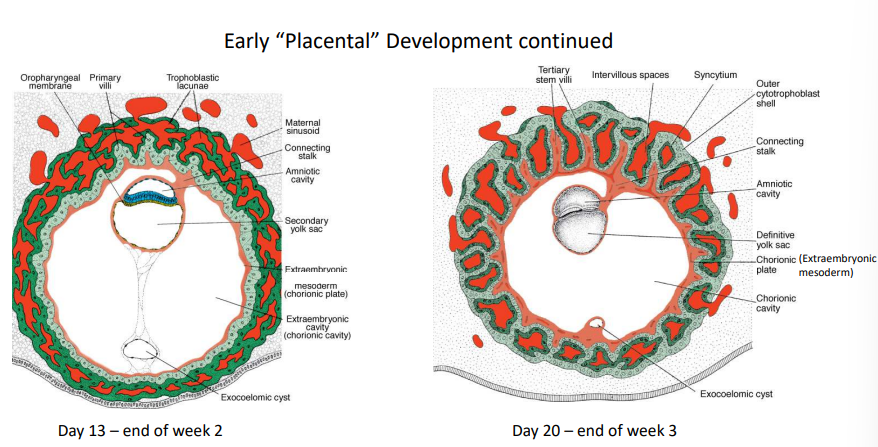
When does the primary heart tube start beating? What does this mean?
Week 4
The villous system is sufficiently developed to support the rapidly growing embryo
Regionalisation of the Mesoderm
Primitive Pit:
• Notochord
Primitive Streak:
• Paraxial mesoderm
• Intermediate mesoderm
• Lateral plate mesoderm
Paraxial Mesoderm
Develops somites at the beginning of day 21.
Somites
Paired cuboidal bodies on either side of developing neural tube
Intermediate Mesoderm
Sits between somites and lateral plate mesoderm.
Lateral Plate Mesoderm
A single layer that splits into the somatopleure and splanchnopleure.
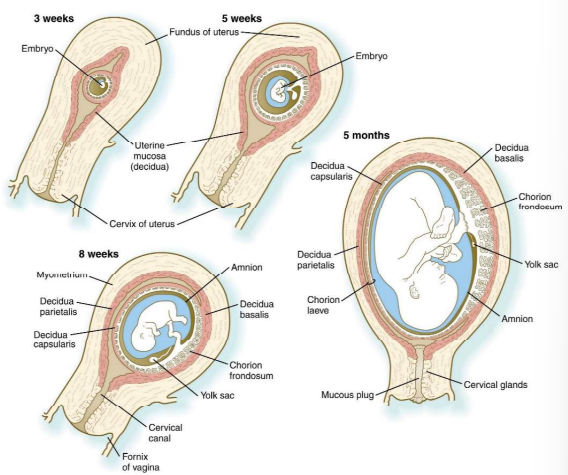
Summarise placental development
• Early = trophoblast derivatives + extraembryonic mesoderm (Chorion)
• Chorion + cavity surrounds the embryo, amnion, yolk sac & body stalk
• After implantation villi develop uniformly around the entire chorion
• Over time, tertiary villi preferentially colonise the region closest to the umbilical cord (embryonic pole)
• Villi on the opposite side (aembryonic pole) fail to thrive and atrophy
• At about 14 weeks the amnion and chorion fuse and become indistinguishable • Failure of complete chorioamniotic fusion can lead to premature birth or birth defects
Substances transferred from mother to fetus
oxygen, water, electrolytes, nutrients (glucose, amino acids, lipids), hormones, antibodies (passive immunity), vitamins, iron, trace elements, drugs, alcohol & other toxins, some viruses (e.g., chicken pox & rubella
Substances transferred from fetus to mother
Carbon dioxide, water, electrolytes, urea, uric acid, creatinine, bilirubin, hormones (e.g., human chorionic gonadotrophin (HCG), progesterone, estrogen)
What are the 3 main fetal hormones?
GnRH
HCG
Human placental growth hormone
GnRH
Cytotrophoblast produces a homologue of GnRH that is released by the hypothalamus.
HCG
GnRH stimulates syncytiotrophoblast to secrete HCG (that is released by the anterior pituitary) to rescue the corpus luteum that produces progesterone.
Human placental growth hormone
Functions to regulate maternal glucose levels so fetus is ensured adequate nourishment Causes maternal liver and other organs to increase glucose supply for fetal use
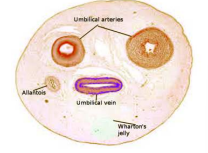
Describe the umbilical cord
Connecting stalk elongates and becomes narrower as pregnancy progresses
Umbilical cords are generally 55-61cms long Can range from 40 to +90cms (neither extreme is good, beyond 70cms is concerning)
Umbilical cord is a conduit for the umbilical vessels
2 arteries (arise from internal iliac arteries and carry blood from fetus to placenta)
1 vein (arises from venules in the placenta and carries blood from placenta to fetus)
Vein carries oxygenated blood and nutrients from mother to fetus
No muscle except smooth muscle of the blood vessels
No nerves – vasodilation or vasoconstriction occur via locally produced vasoactive substances (e.g. nitrous oxide – vasodilation & catecholamines – vasoconstriction)
Umbilical structures are supported by Wharton’s jelly = mesenchymal substance (connective tissue) in which the umbilical blood vessels are supported function: to resist compressive and bending forces on the umbilical vessels