A&P Ch. 5 The Integumentary System
1/116
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
117 Terms
Integument
skin
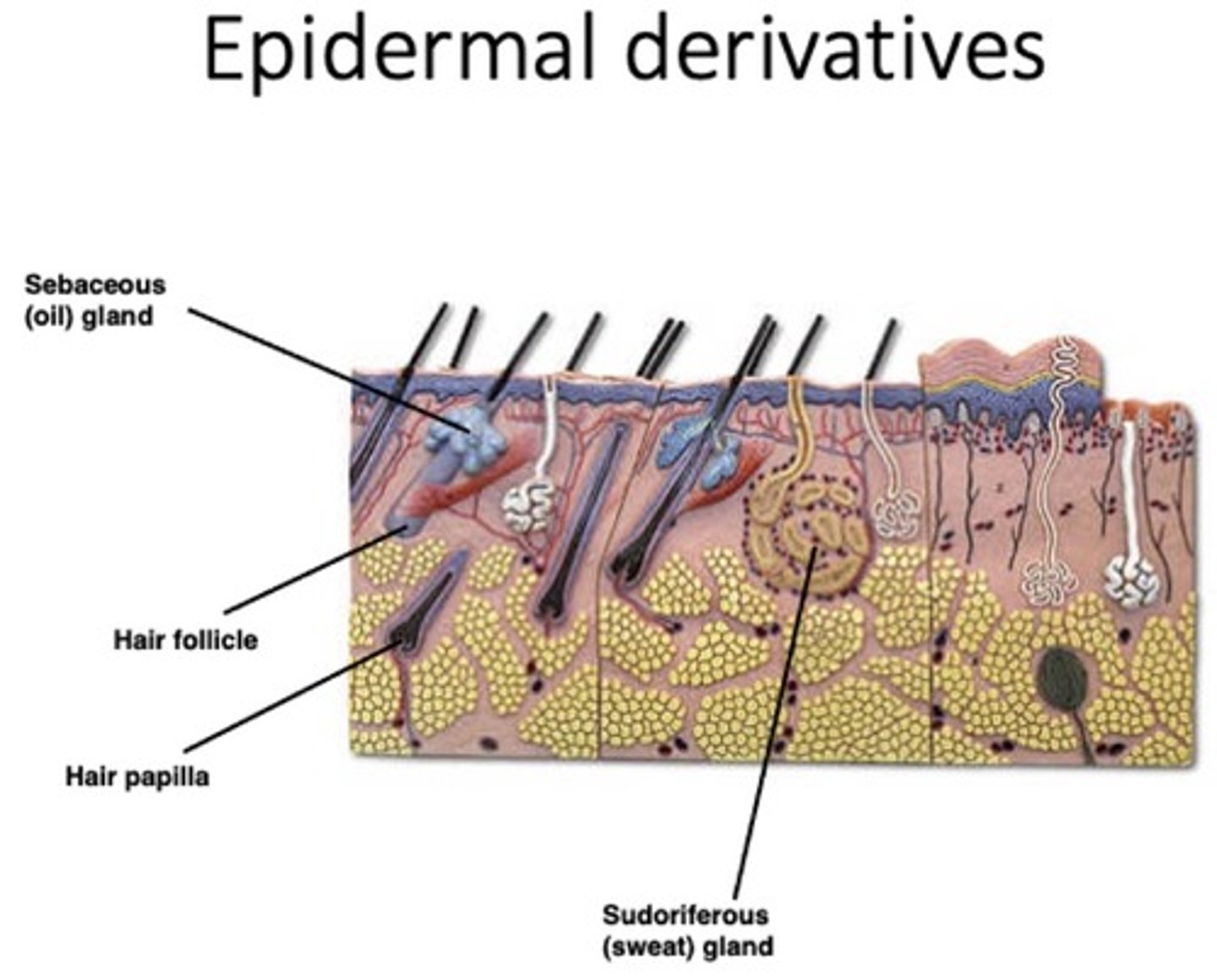
Skin derivatives (Appendages) (4)
Sweat (sudoriferous) glands,
Sebaceous (oil) glands,
Hair and hair follicles,
Nails
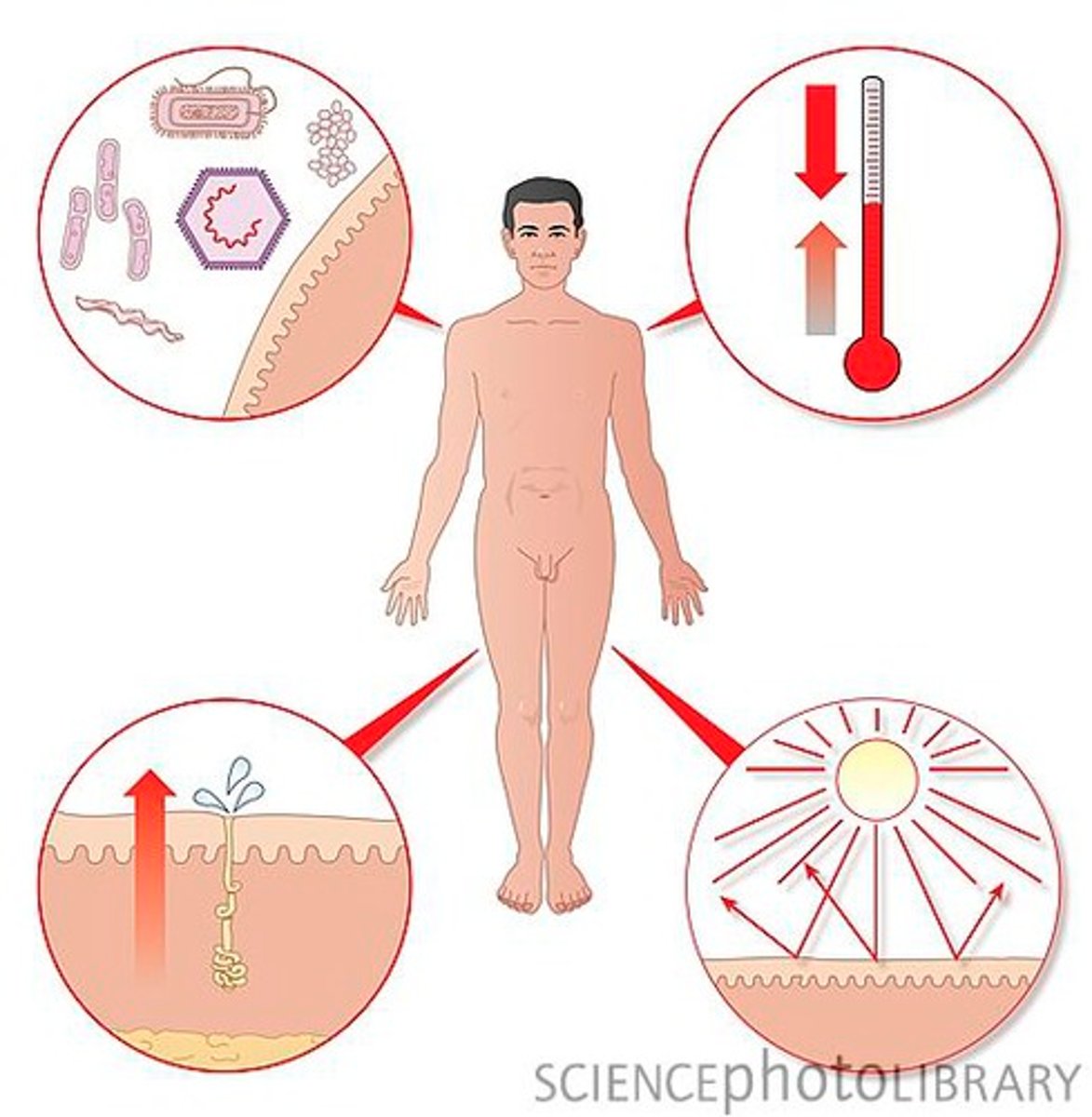
Skin functions (6)
Protection,
Body temperature regulation,
Cutaneous Sensation,
Metabolic functions,
Blood Reservoir,
Excretion
3 types of protection barriers
chemical, physical, biological
What does skin protect deeper tissue from?
Mechanical damage,
Chemical damage,
Bacterial damage,
Thermal damage,
Ultraviolet radiation,
Desiccation
Example of Mechanical damage:
When you fall and scrape your skin

Example of Chemical damage:
Handling household chemicals,
protects against acids & bases
Example of Bacterial damage:
skin infections;
No pathogen or bacteria can penetrate intact skin.
Example of Thermal damage:
Burn your skin,
Protects against hot & cold

Example of Ultraviolet radiation:
Sun burn,
(melanocytes) Protects against sun

Example of Desiccation:
Dehydration;
Water loss

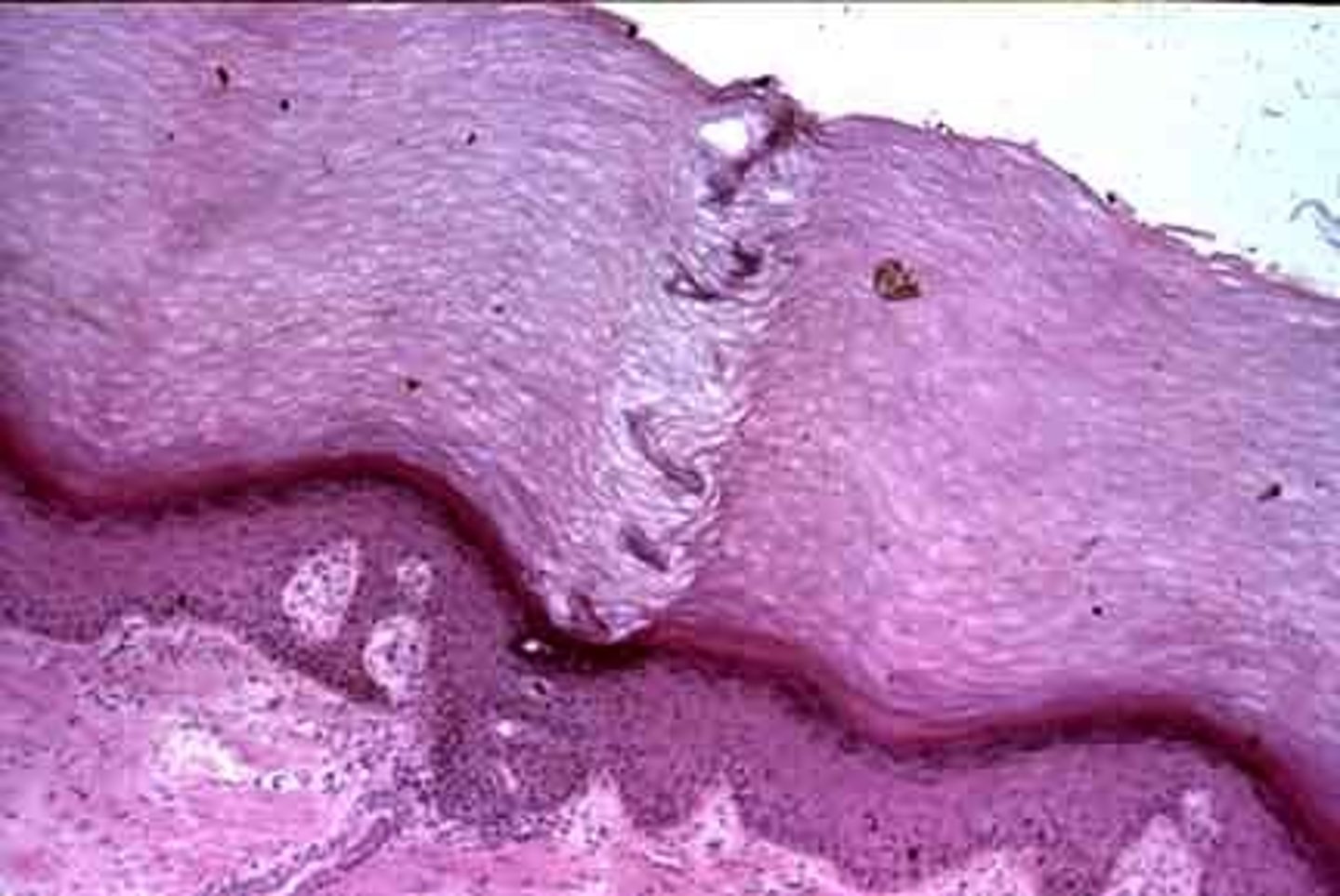
What tissue type protects deeper tissue?
Stratified Squamous epithelium with keratin
How does skin regulate body temperature?
With sweat glands through evaporative cooling

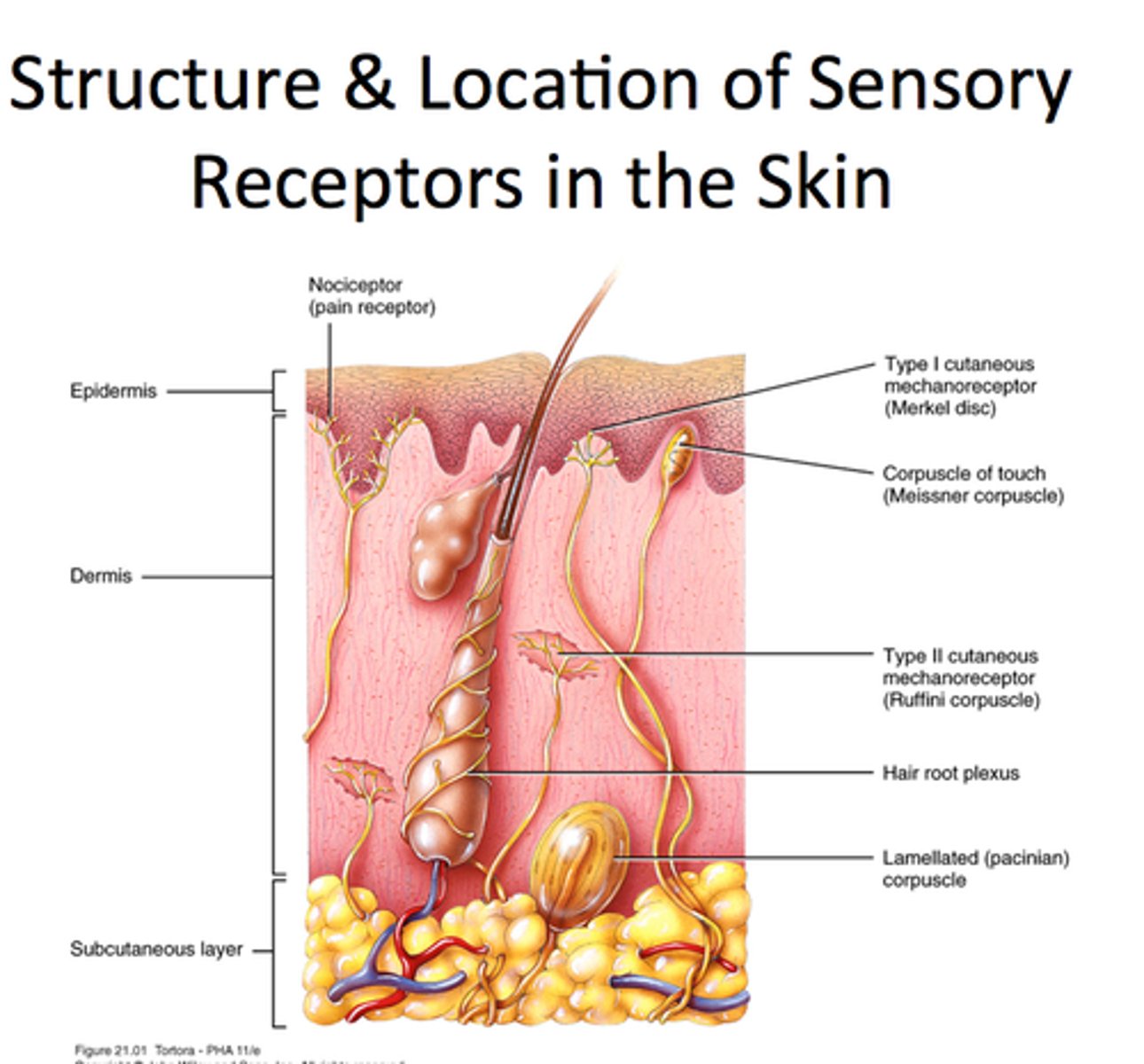
Cutaneous sensations of skin
Temperature, touch, and pain
(nerve endings)
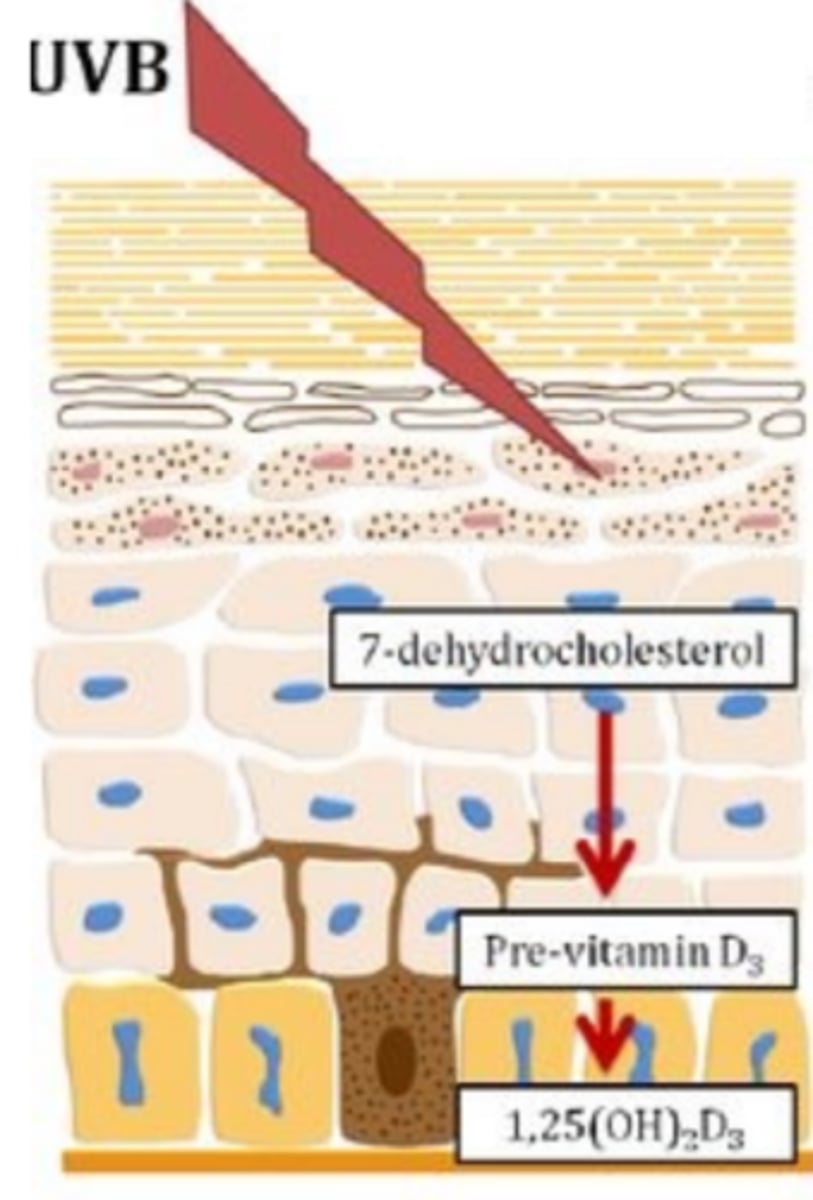
Metabolic functions of skin
synthesis of vitamin D in dermal blood vessels,
vitamin D precursor for calcium (need Vitamin D to absorb Calcium)
Blood Reservoir (Skin)
The skin can hold 5% of body's total blood volume.
What can the skin's blood reservoir be used for?
Can be shunted (pulled from) into general circulation for use by vigorously working muscle and/ or other body organs

Excretion (skin)
Elimination of nitrogen-containing wastes
Example of nitrogen-containing waste
Ammonia, Urea, Uric acid

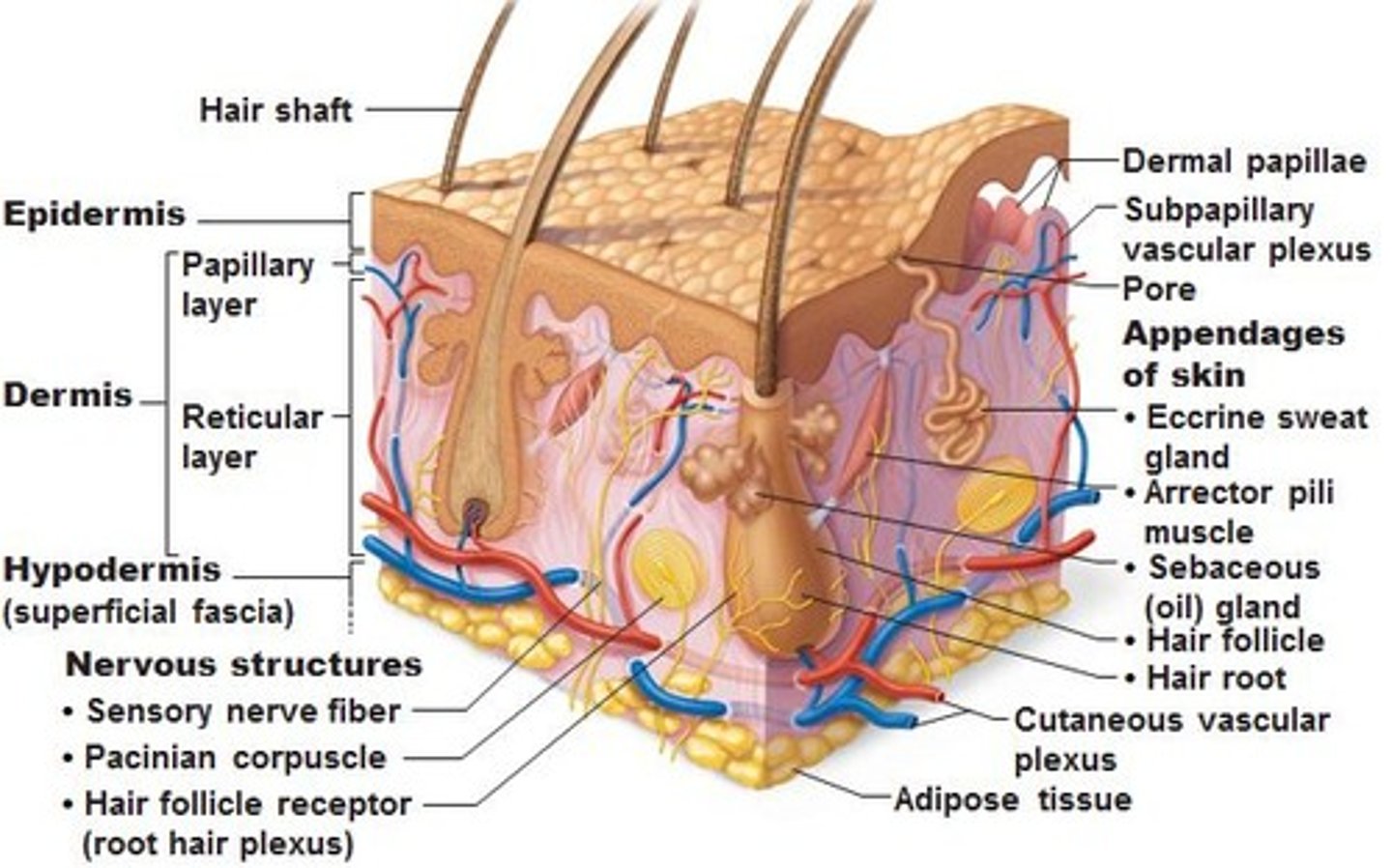
Skin structure (3 layers of skin)
Epidermis,
Dermis,
Hypodermis
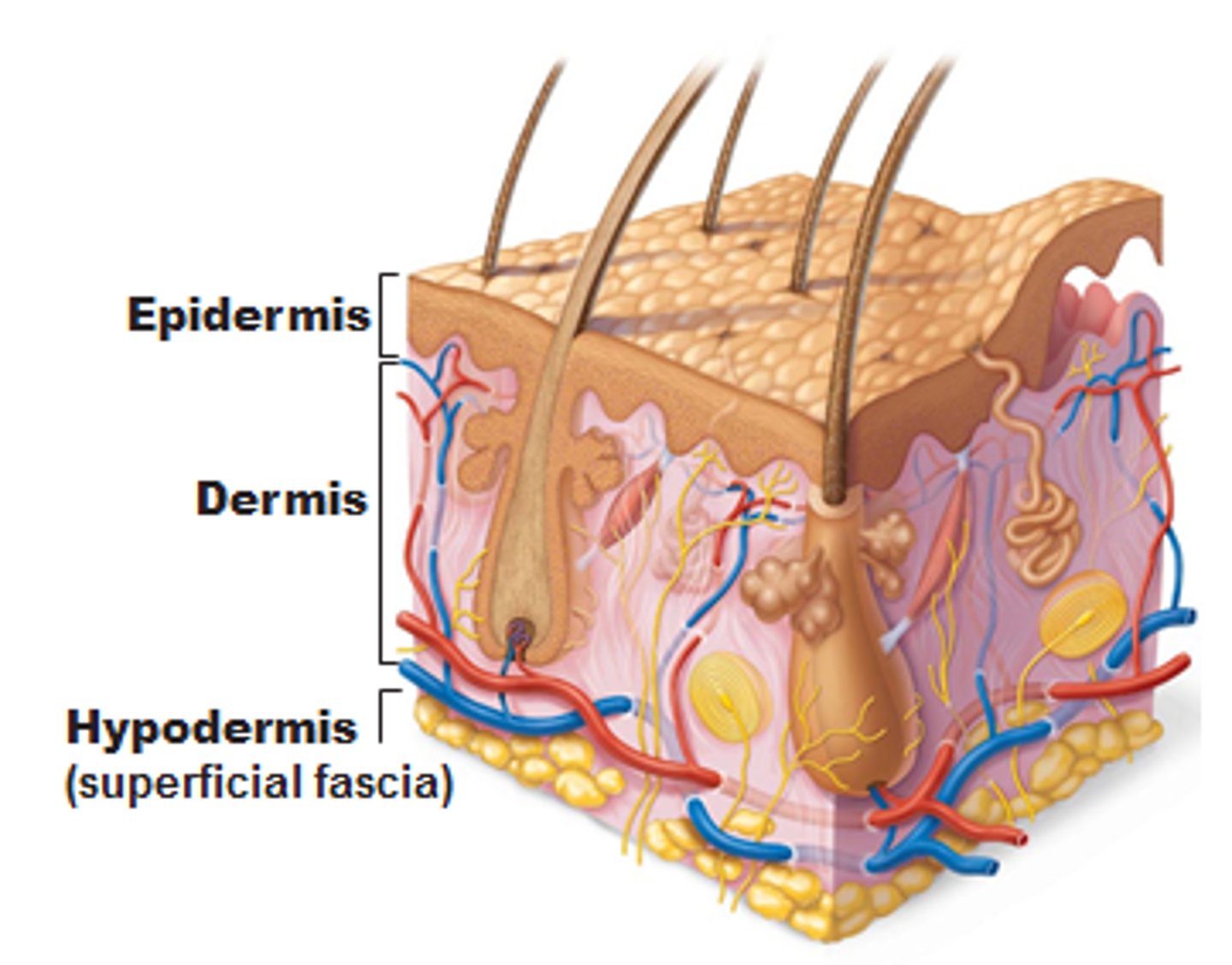
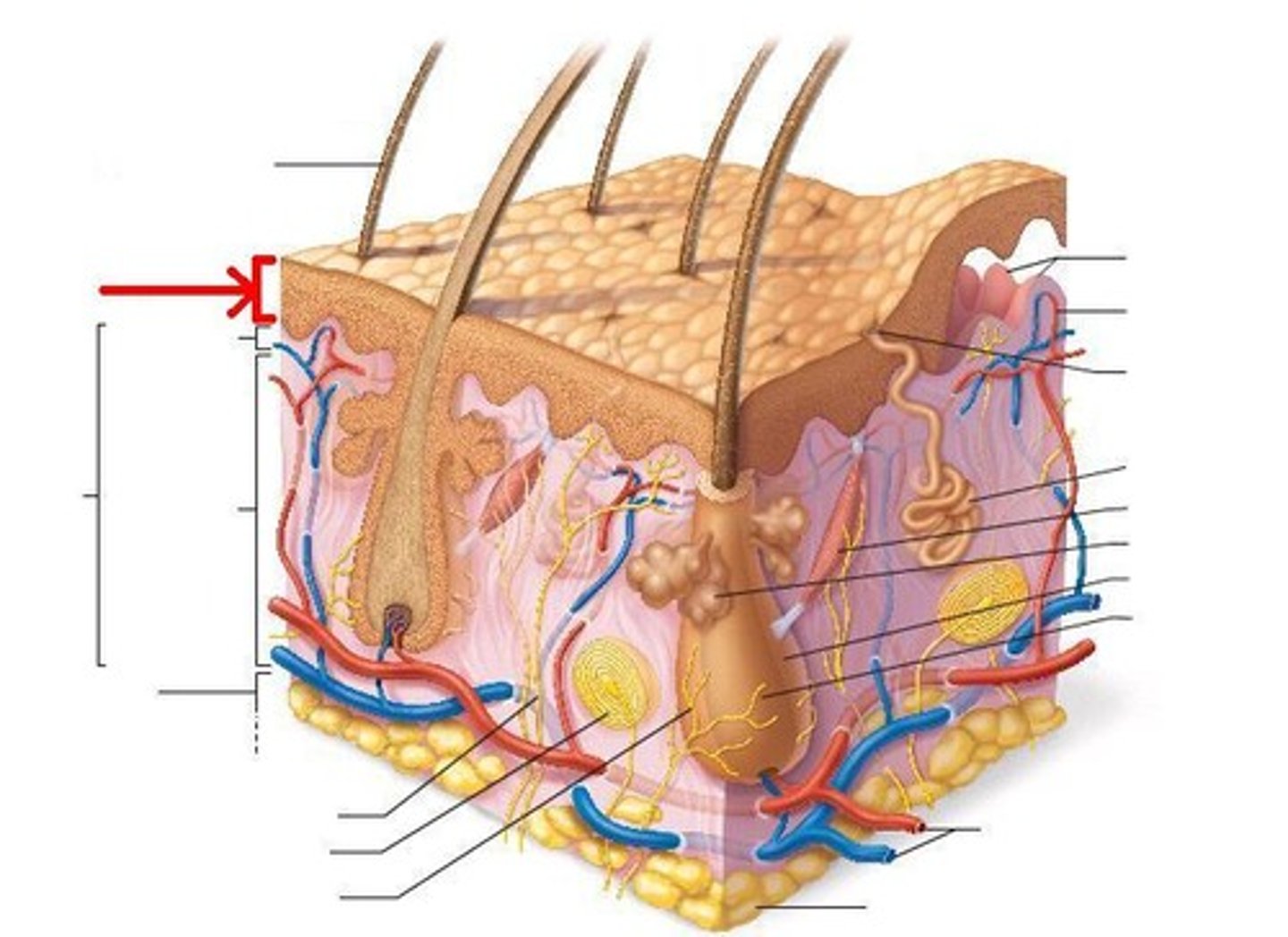
Epidermis structure
Stratified squamous epithelium with keratin,
Cells tightly connected together by desmosomes,
Keratinocytes form several layers,
5 strata layer
Keratinocyte
epidermal cell that produces keratin
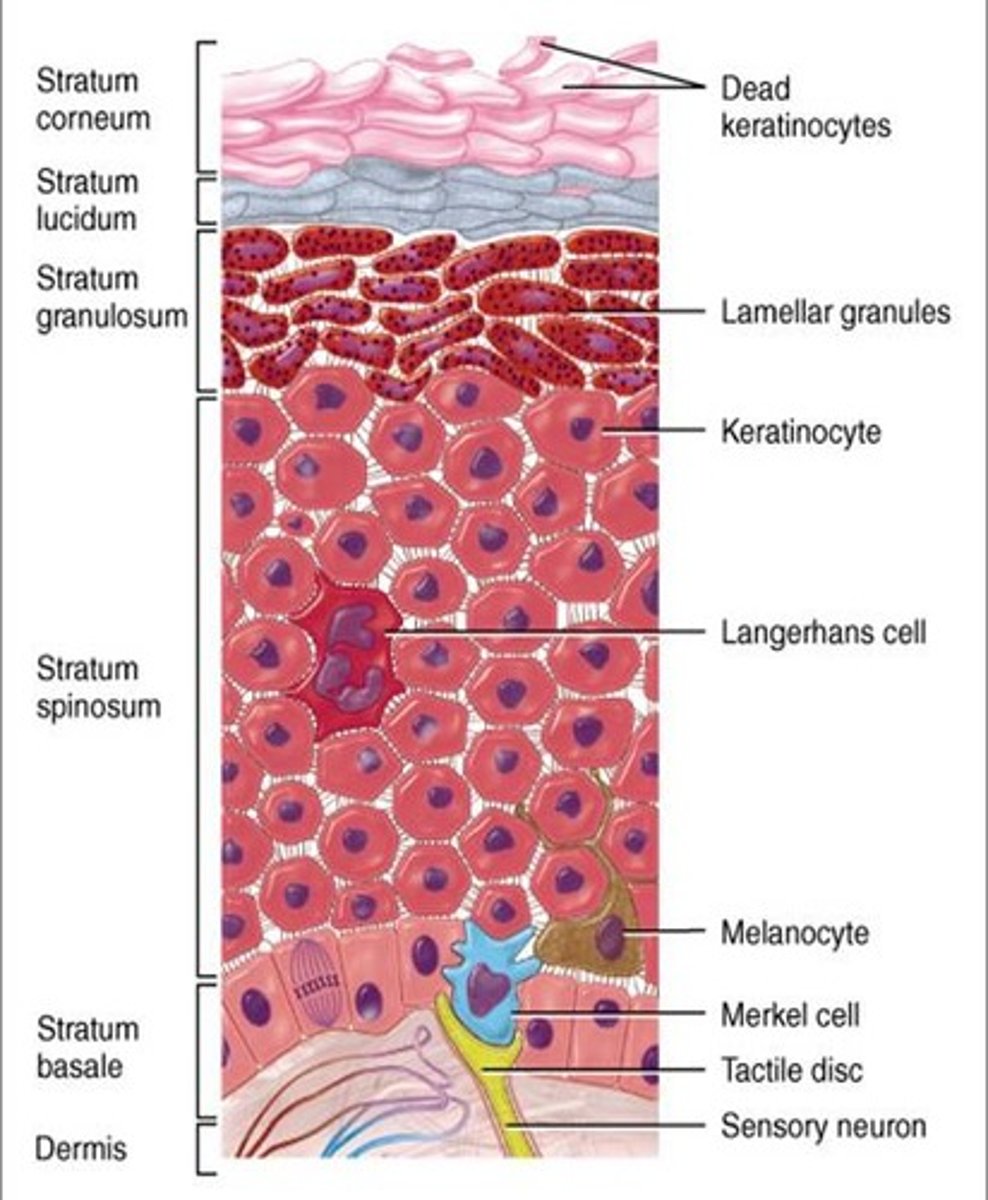
Strata (stratum)
layers
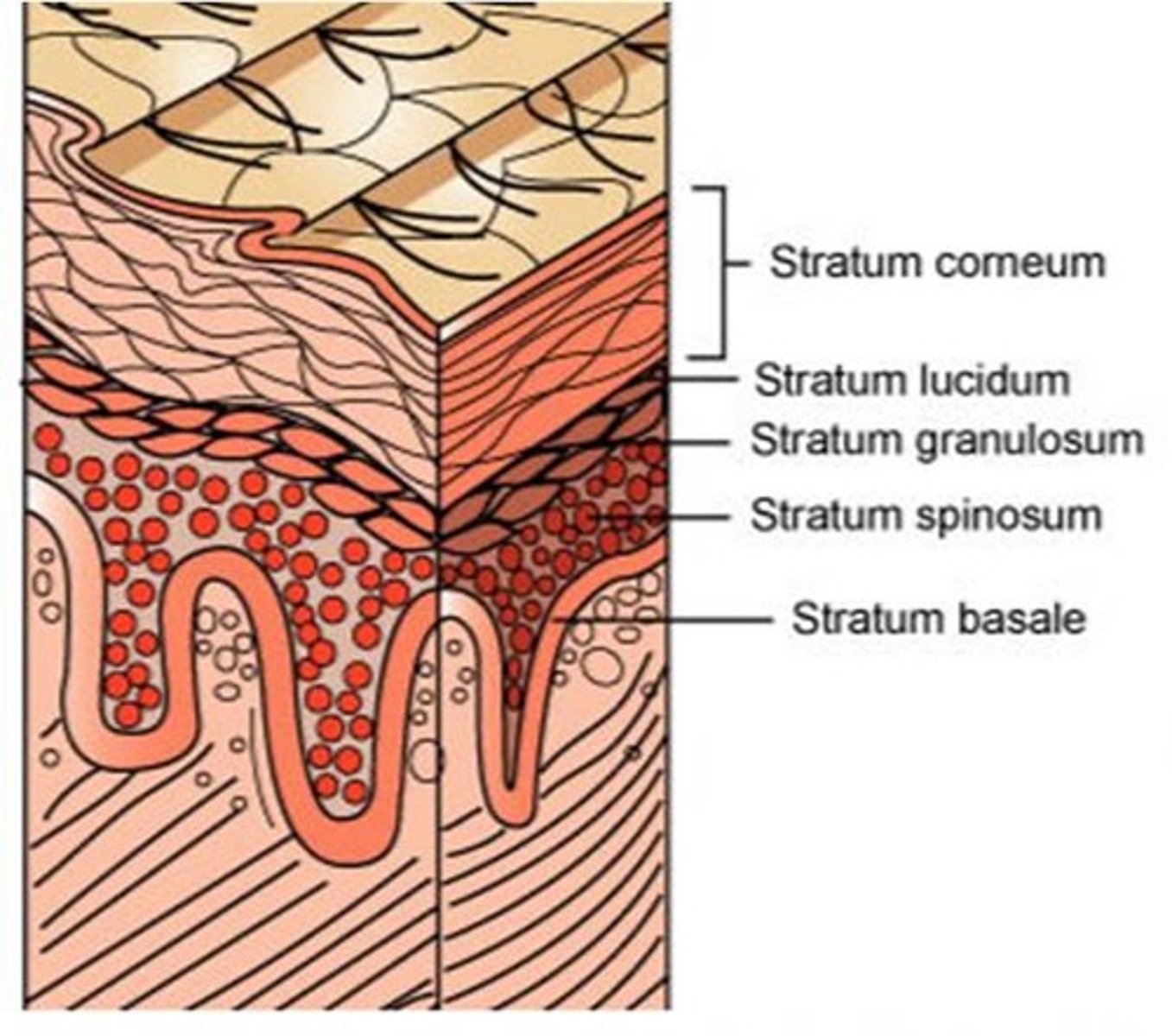
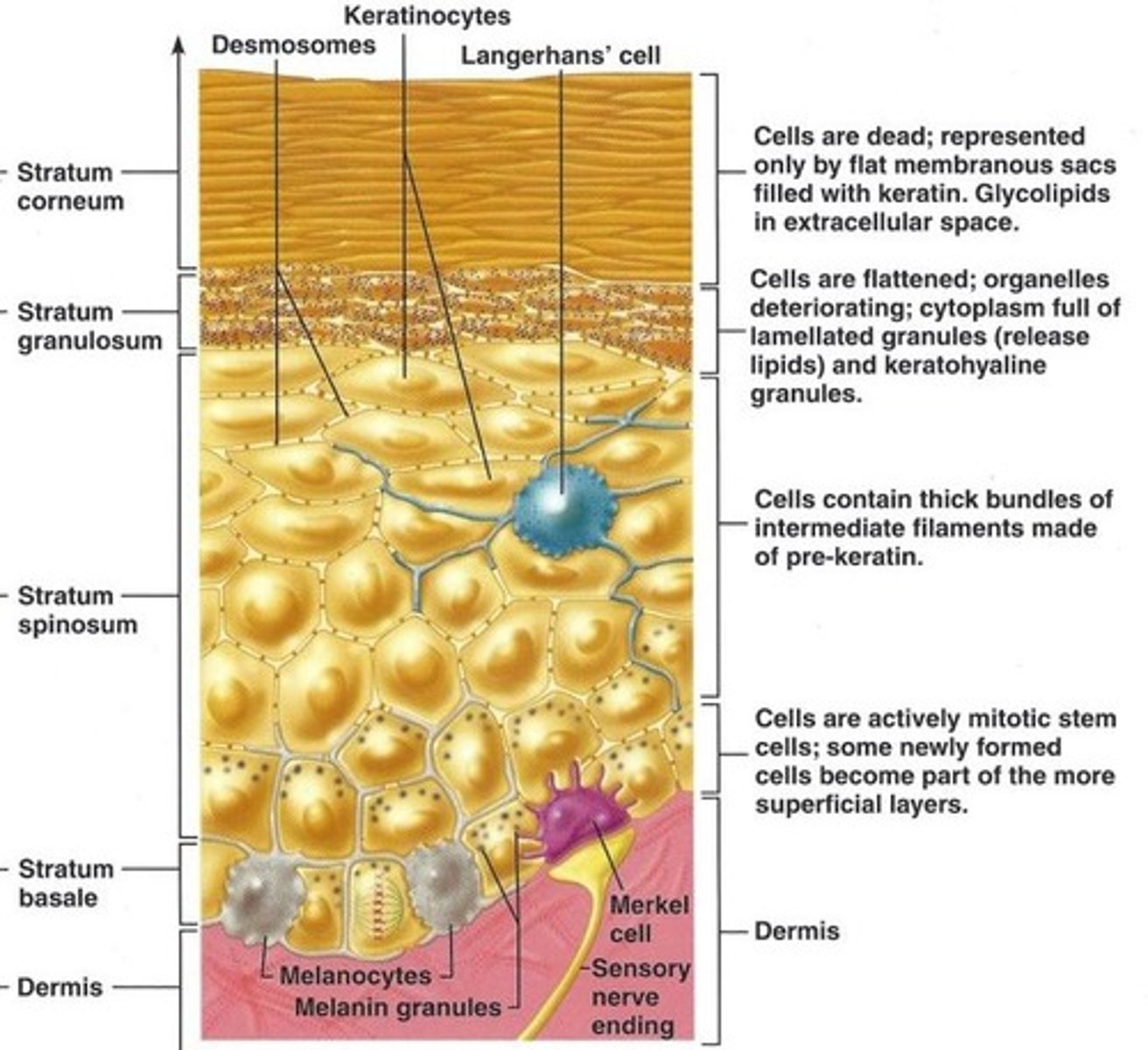
5 strata of epidermis
stratum basale,
stratum spinosum,
stratum granulosum,
stratum lucidum,
stratum corneum
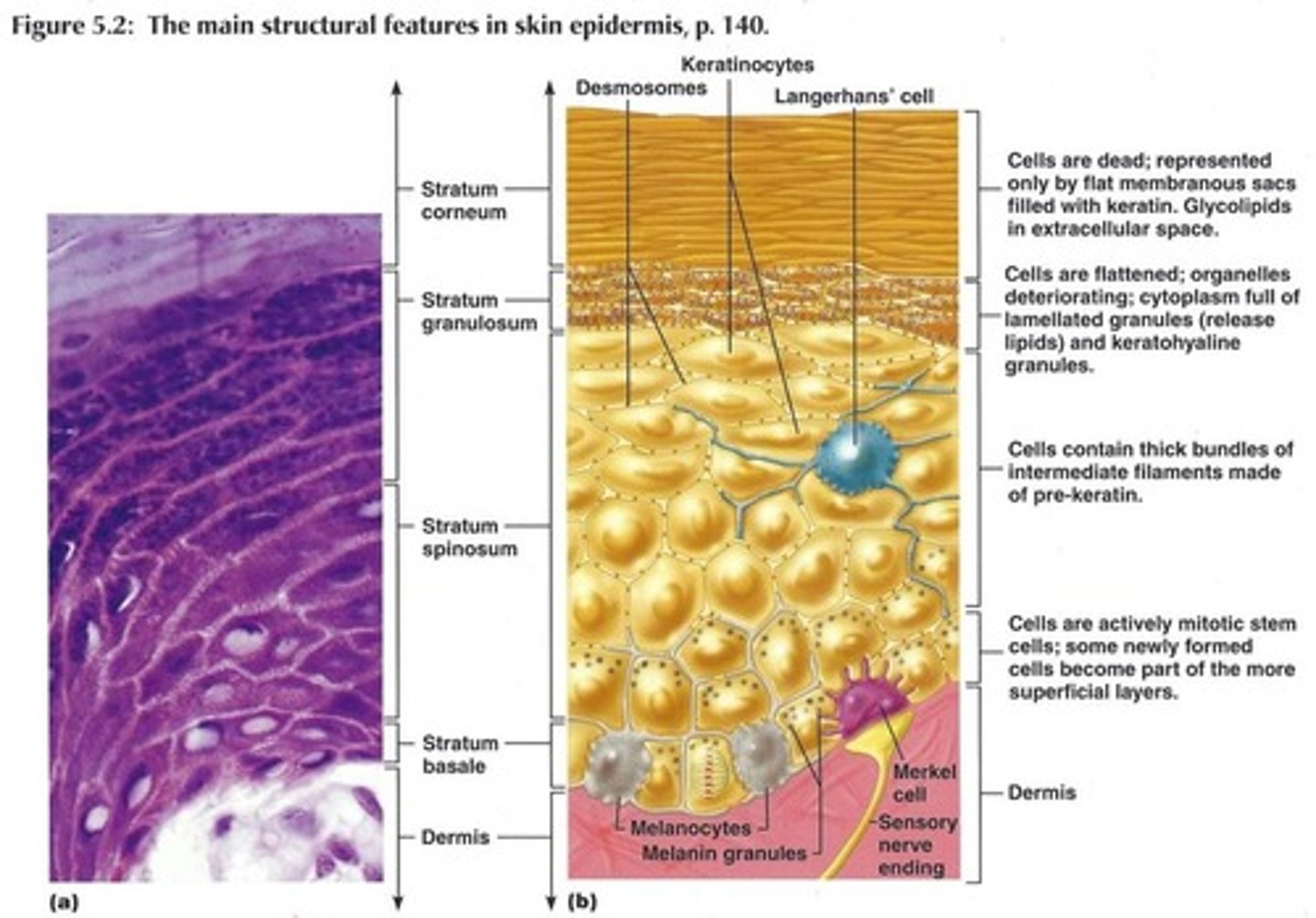
Stratum Basale
Single row of cells that serve as origin of keratinocytes for all superficial strata,
High mitotic activity,
Contains melanocytes,
Bottom of Epidermis
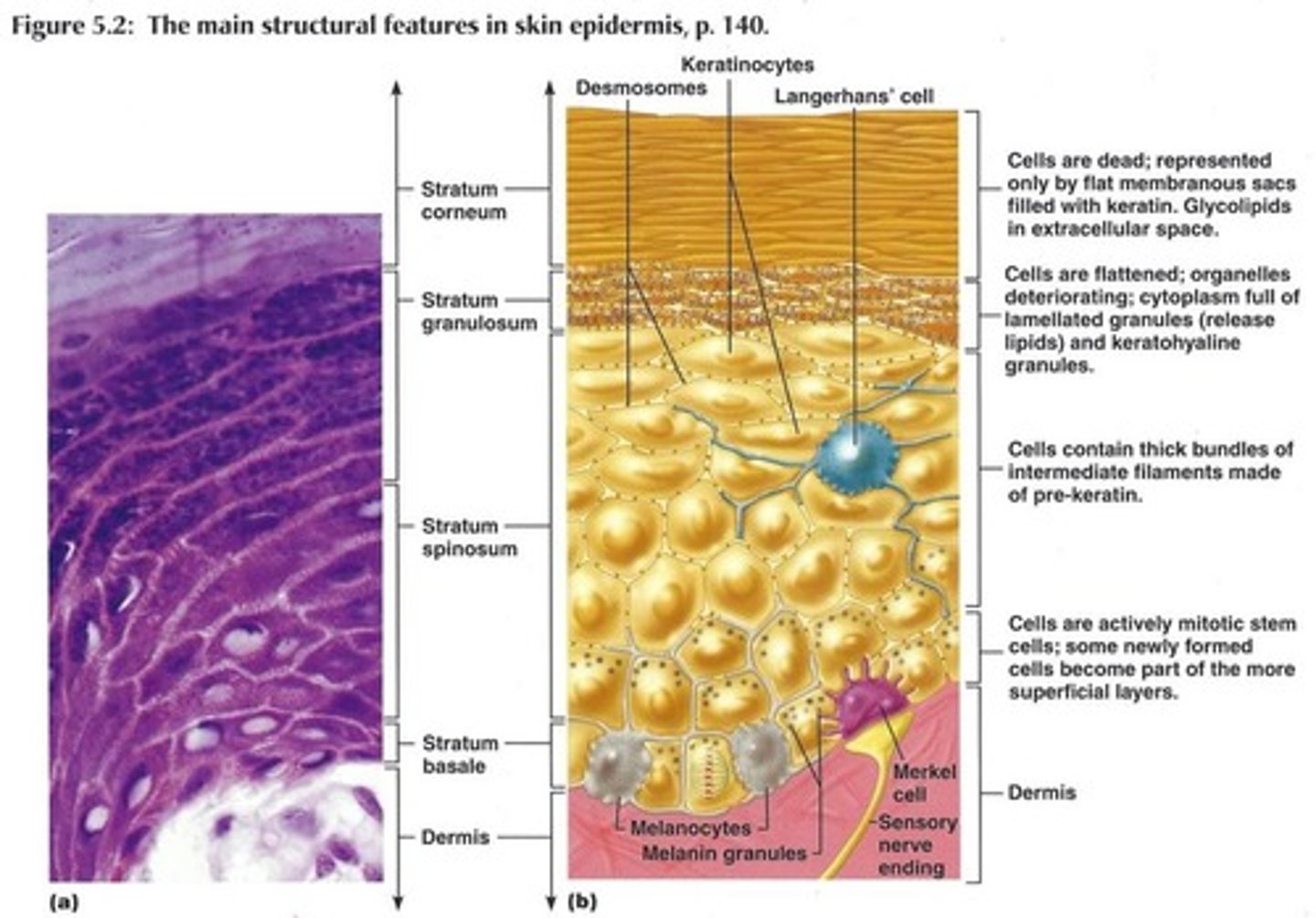
Melanocytes
cells that produce melanin
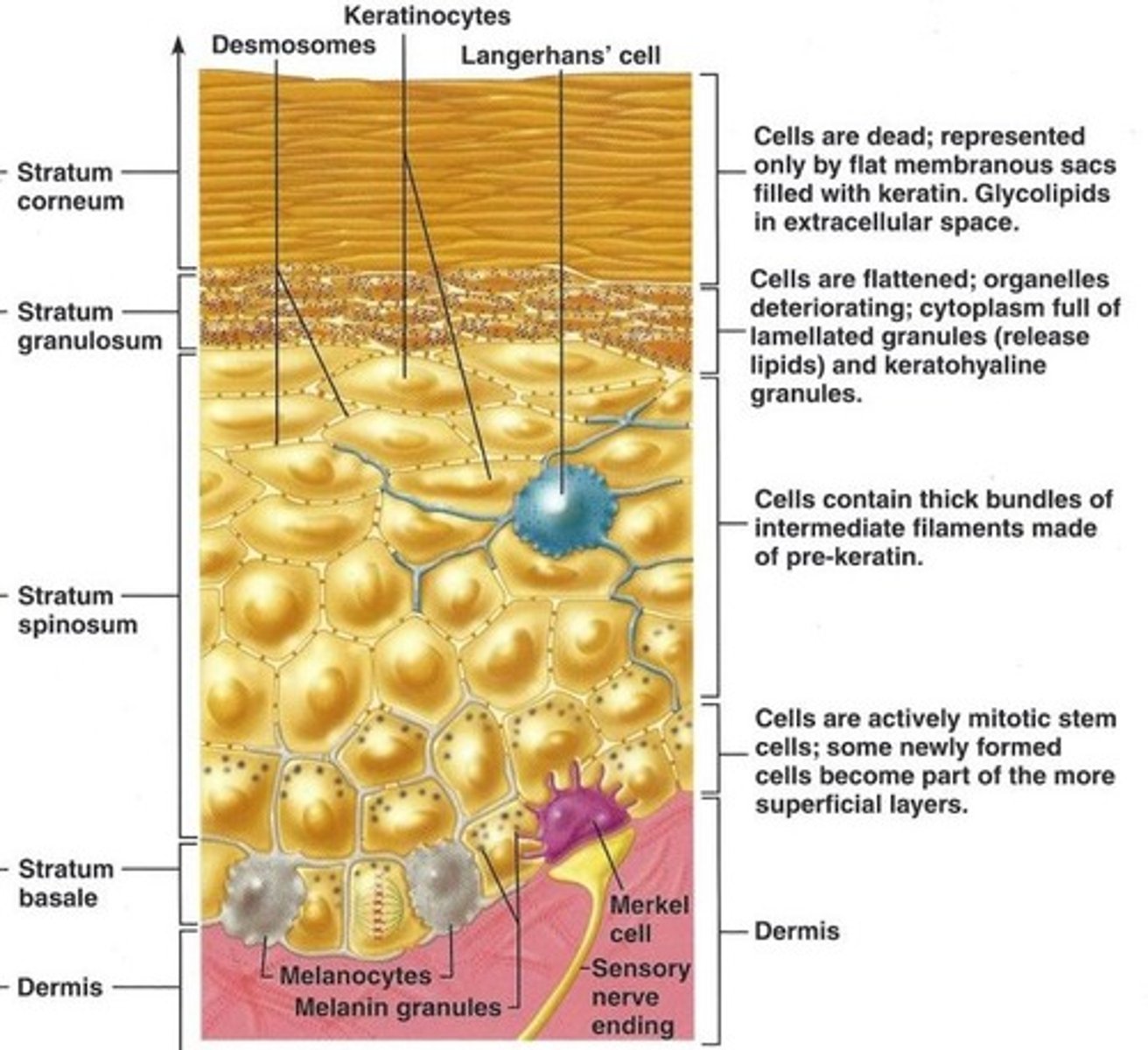
What cell type accounts for 10-20% of stratum basale
melanocytes
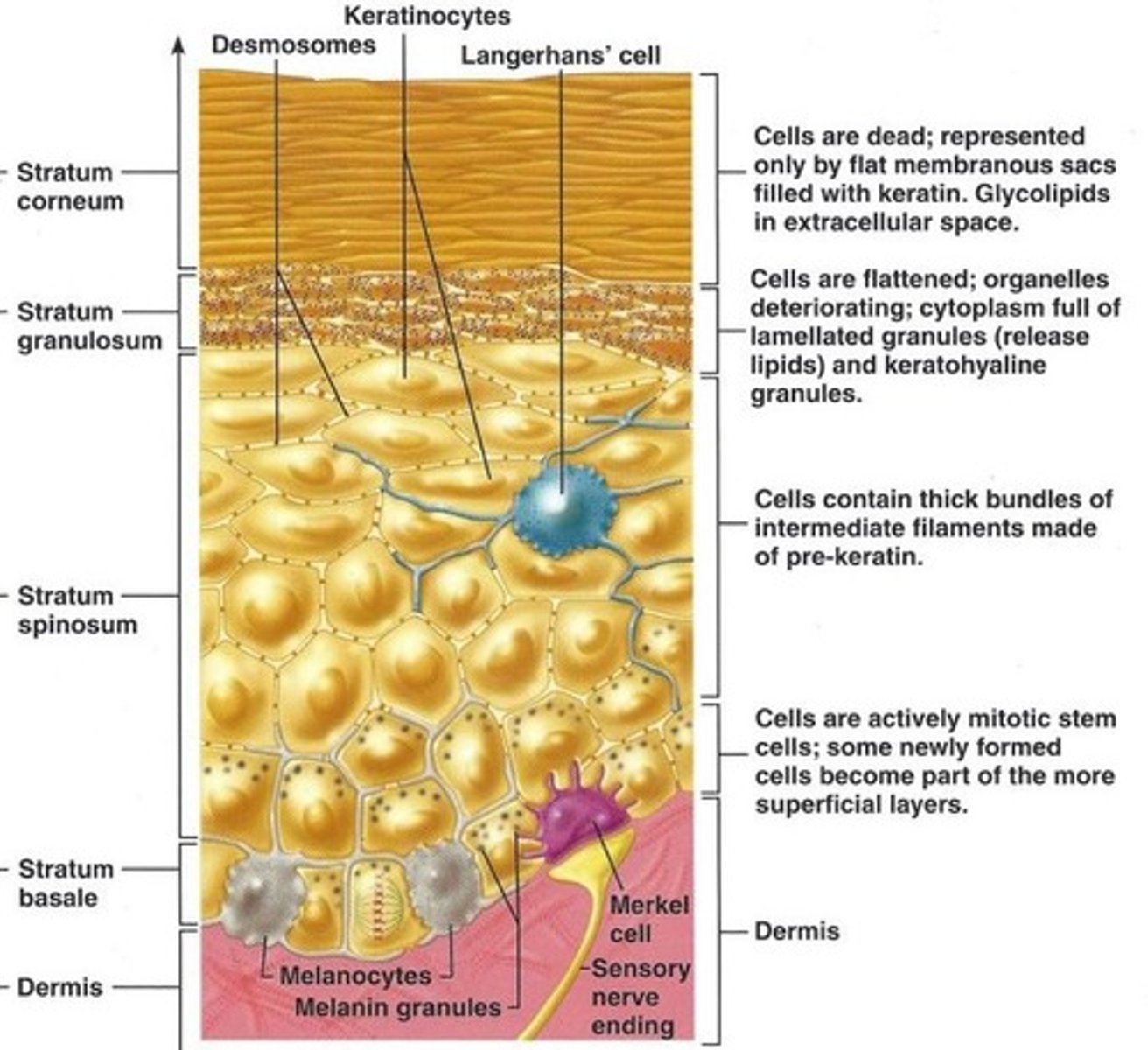
Stratum Corneum
Located at exposed surface skin (most superficial),
20-30 cell layers thick & accounts for three- quarters of epidermal thickness,
Protective barrier of dead, durable, and expendable cells
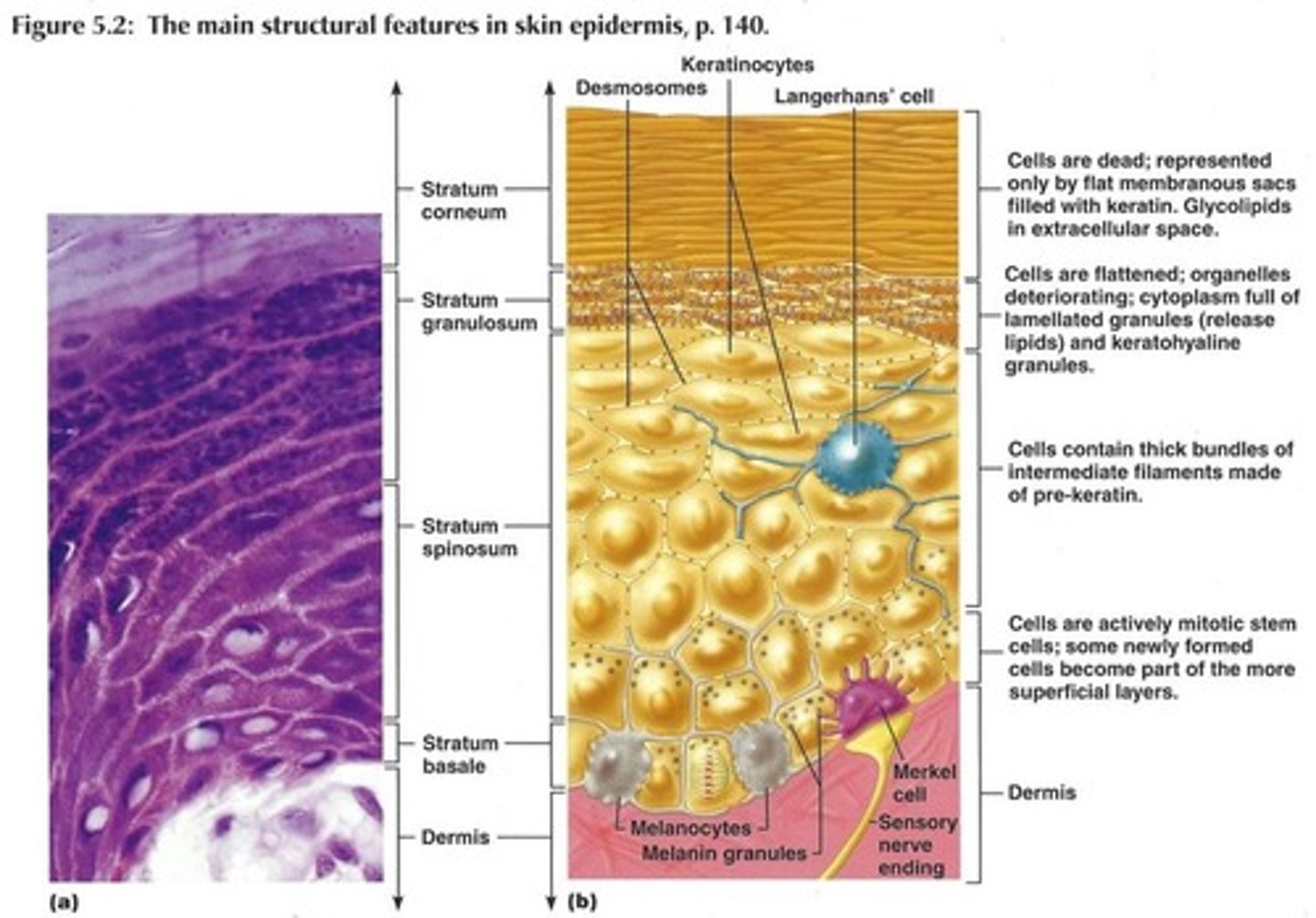
Stratum corneum protective barrier:
Cells are filled with keratin (literally keratin filled plasma membranes),
Helps give epidermis its protective properties,
Thickness varies depending on use (Calluses)
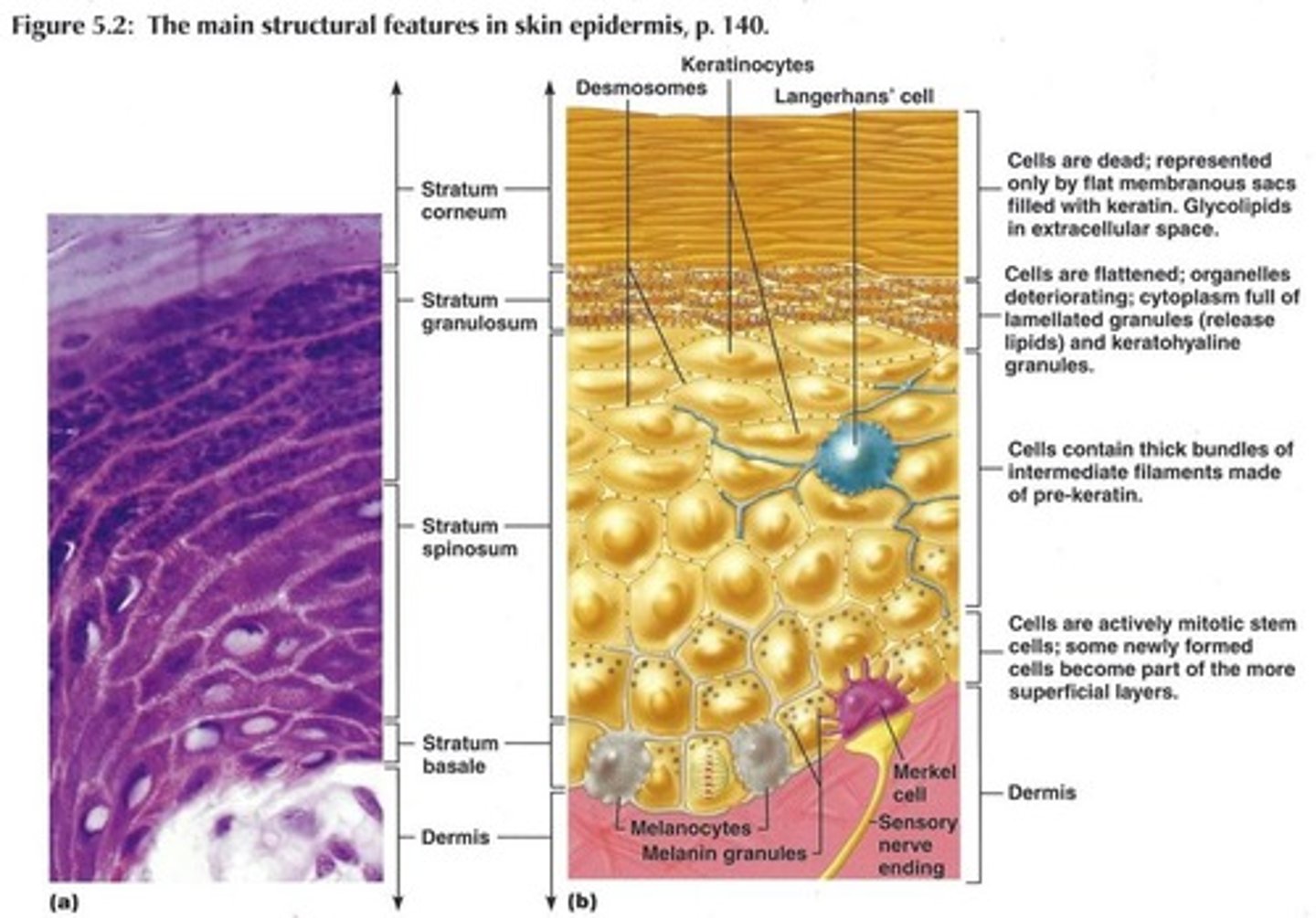
why is the top layer of skin dead
Because its far from a nutrient source
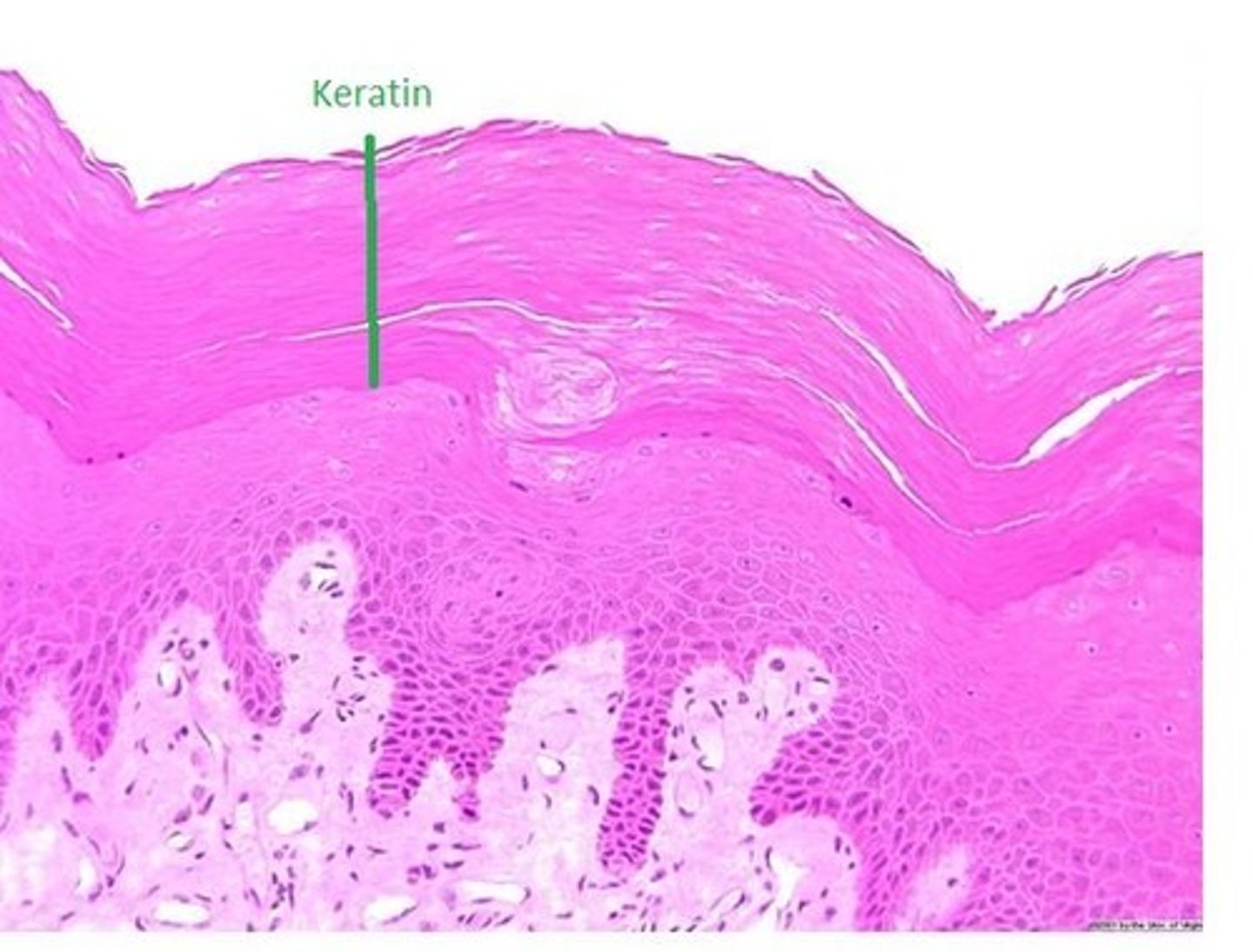
When do the dead skin cells (keratinocytes) fall off?
every time you towel dry, change clothes, etc... (basically anything) the dead skin cells fall off

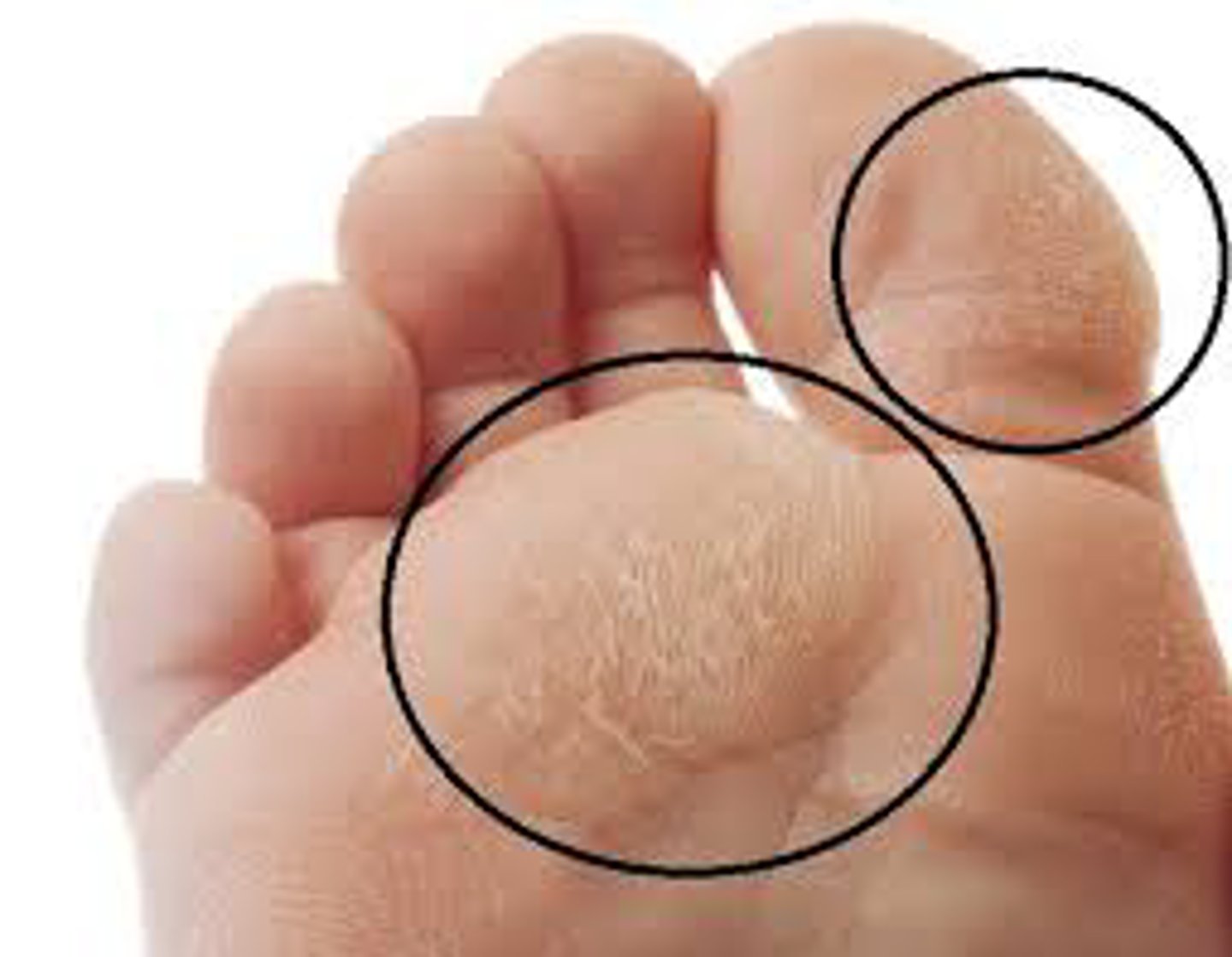
Calluses
a hardened thickened place on the skin,
caused by friction and pressure from repeated actions,
can develop on palms of hands and soles of feet
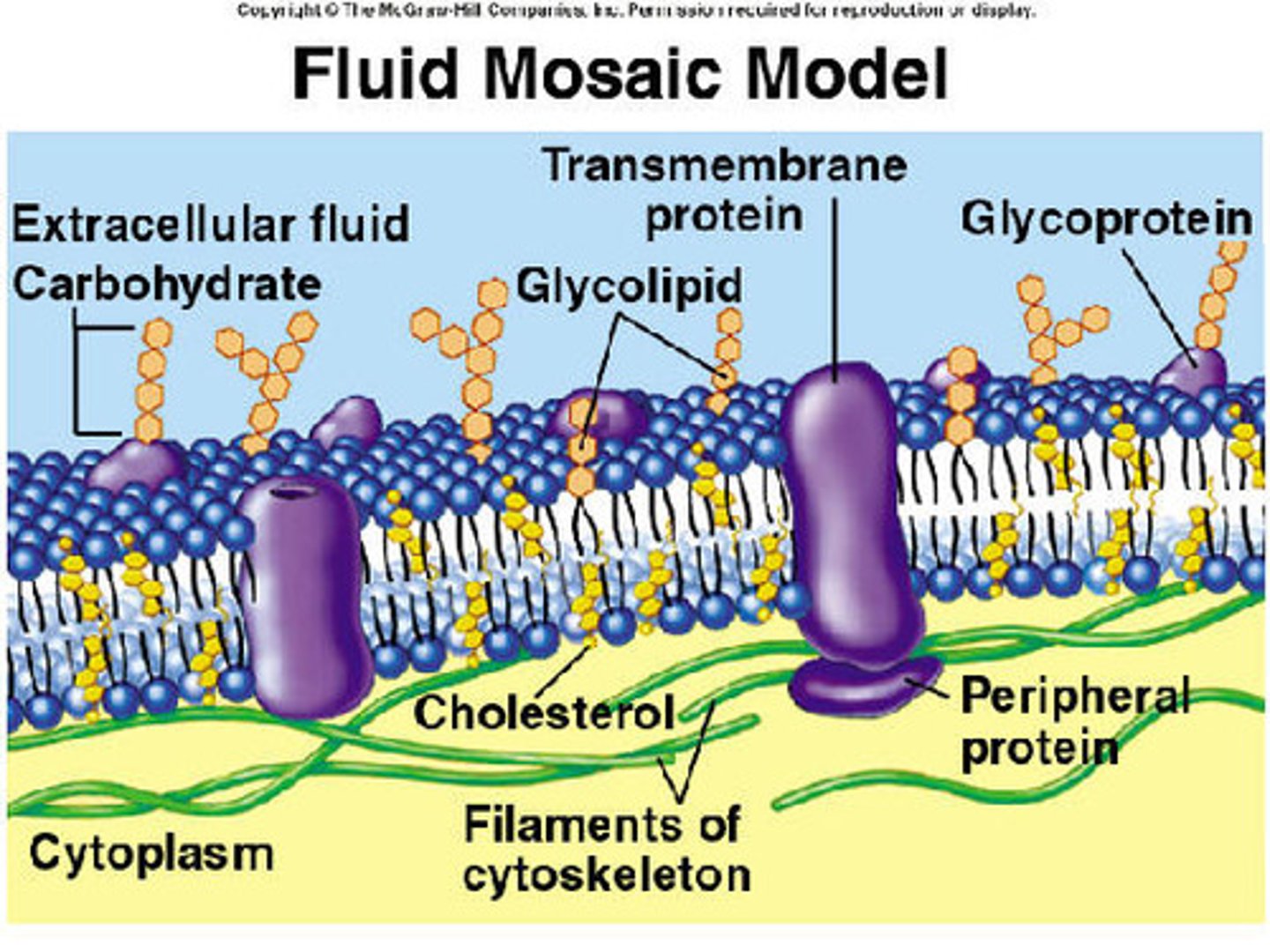
Glycolipids
Secreted between cells,
provides waterproofing and preserves some permeability characteristics on the skin,
Allows for transdermal medications (nicotine patches, etc.)
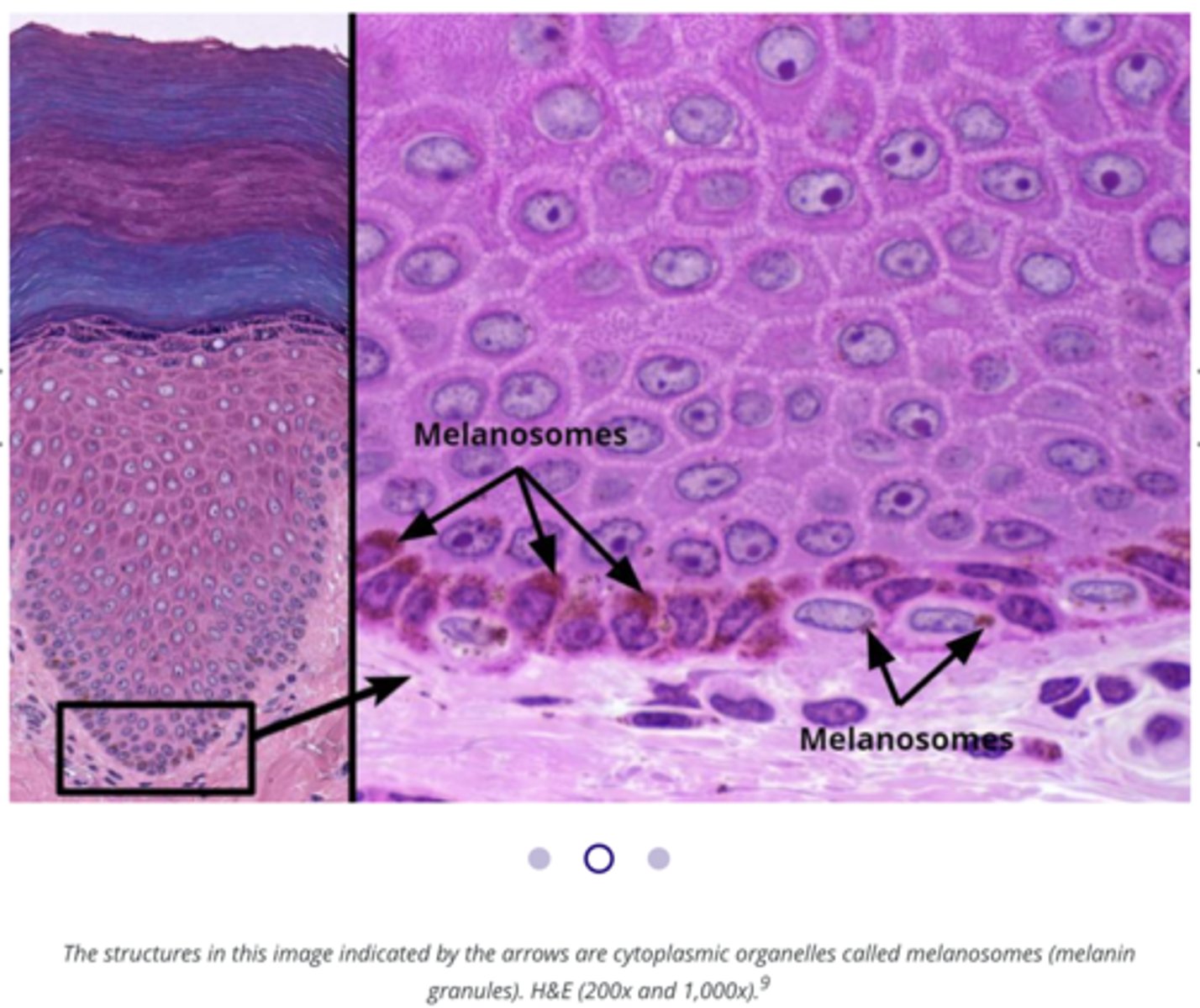
Melanin
A protein,
Pigment produced by melanocytes,
Gets packaged in melanosomes and then deposited into keratinocytes in more superficial layers,
Melanin granules then position themselves on superficial (or sunny) side of keratinocyte nucleus to protect against UV radiation,
Amount of melanosomes produced depends on:
Amount produced depends on genetics and exposure to sunlight

Melanin packaged into vesicles called:
Melanosomes
Why doesn't a skin tan last long?
Lysosomes see melanosomes as an invaders & attack them.
What is critical for melanin production?
Tyrosinase (acts on the amino acid tyrosine)
Albinism
Most common form of albinism is the:
Failure to produce tyrosinase

Dermis
Strong, flexible connective tissue
(leather is made from the Dermis)
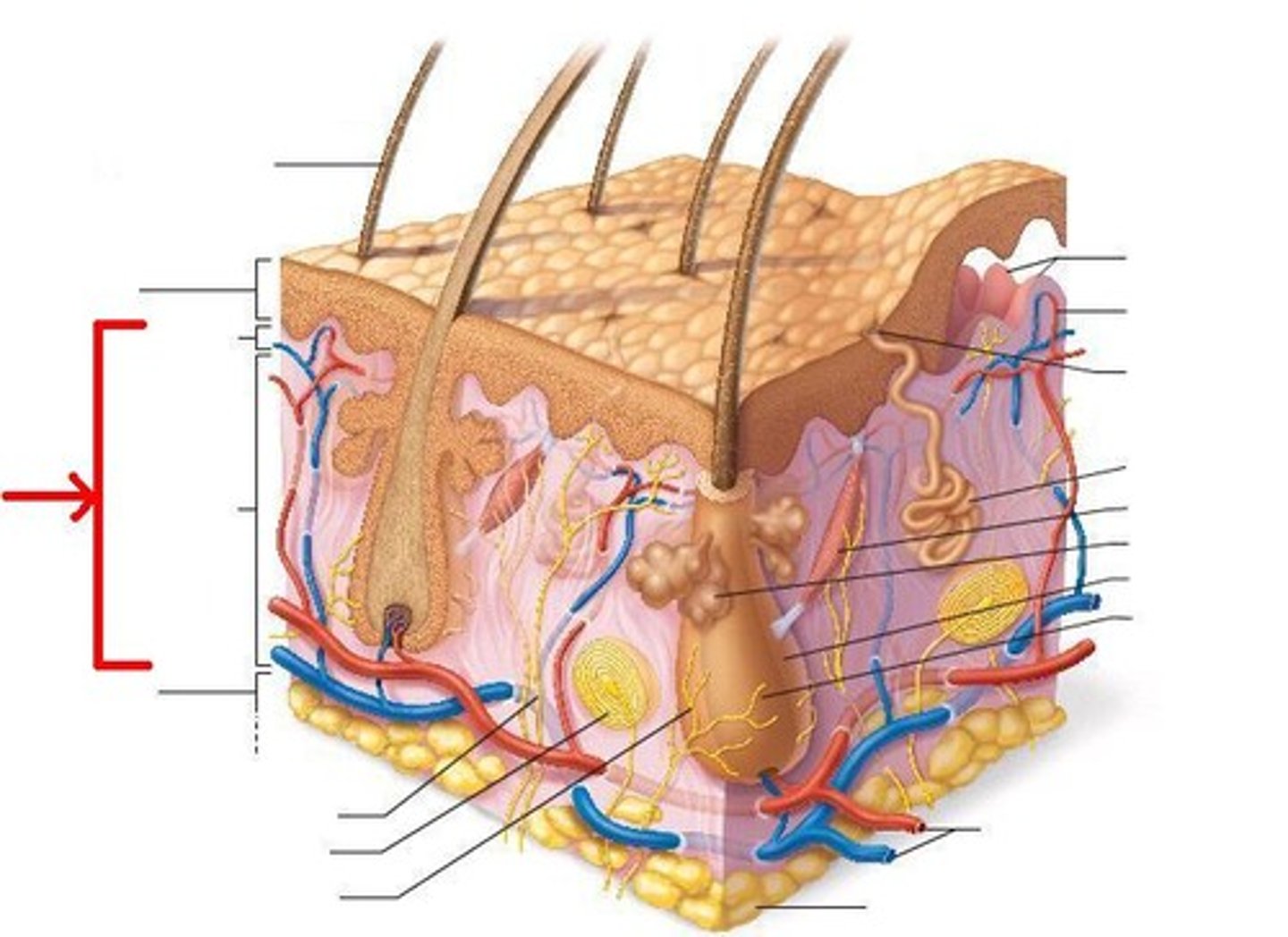
The two layers of the Dermis
Papillary Layer
Reticular Layer
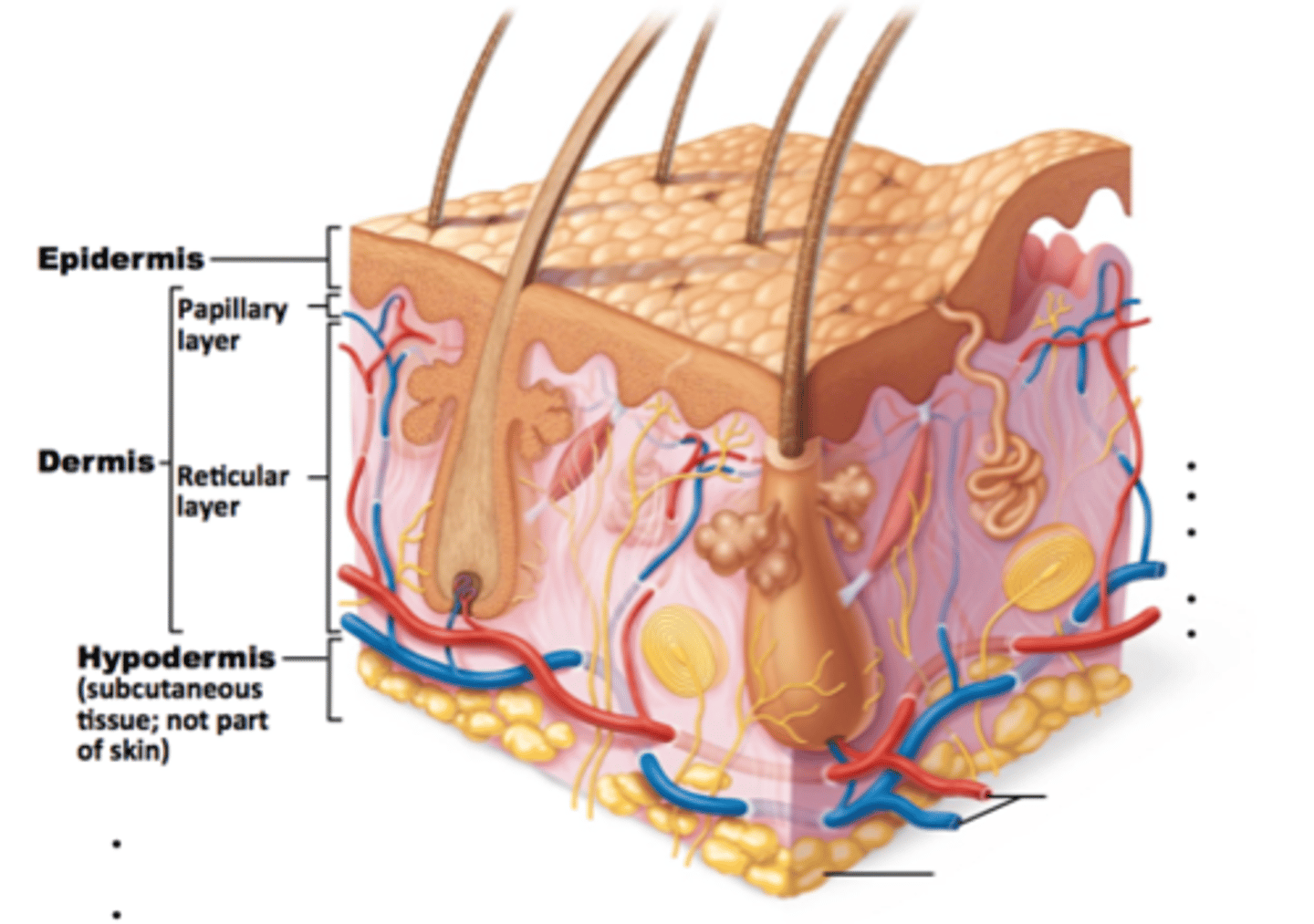
Papillary Layer
20% of the Dermis,
Thin, superficial layer of areolar connective tissue,
Supports and nourishes overlaying epidermis,
Projections called Dermal Papillae,
Pain receptors,
Capillary loops
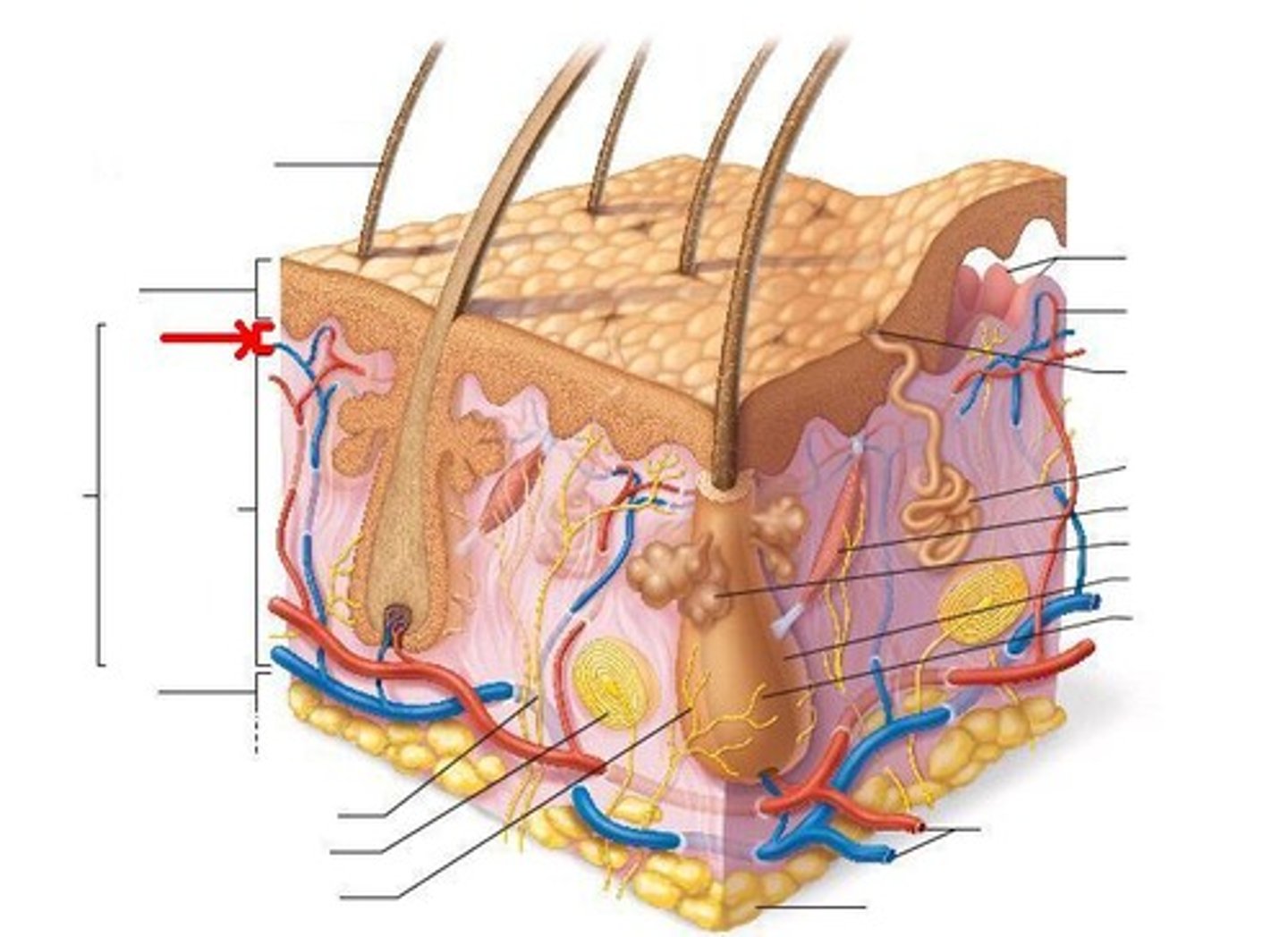
Dermal Papillae
Increases surface area and serves as basis for friction ridges and fingerprints (nipple like projections)
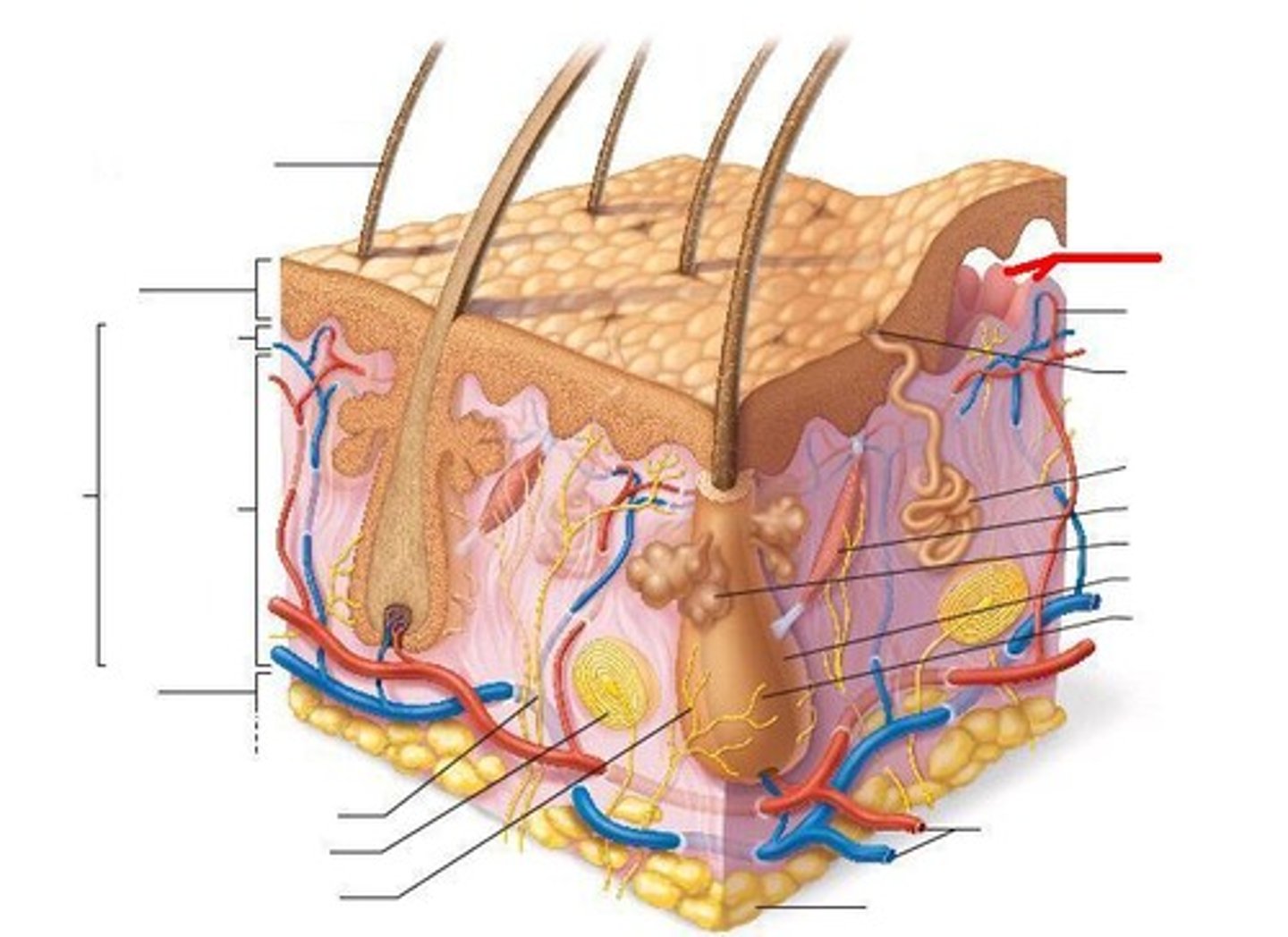
Capillary Loops
Smaller blood vessels that give blood and nutrients to stratum basale
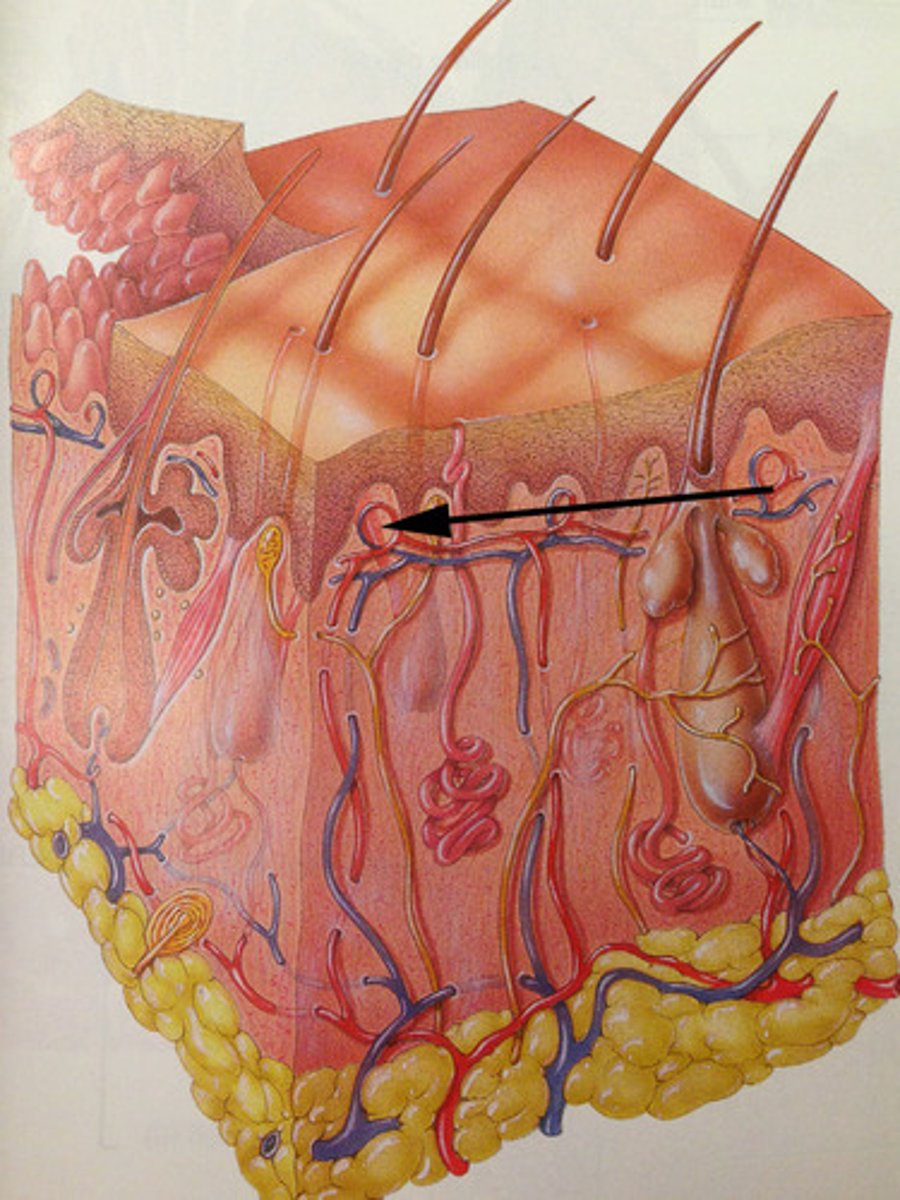
Nerves with free nerve endings
Detect pain, hot & cold, light touch
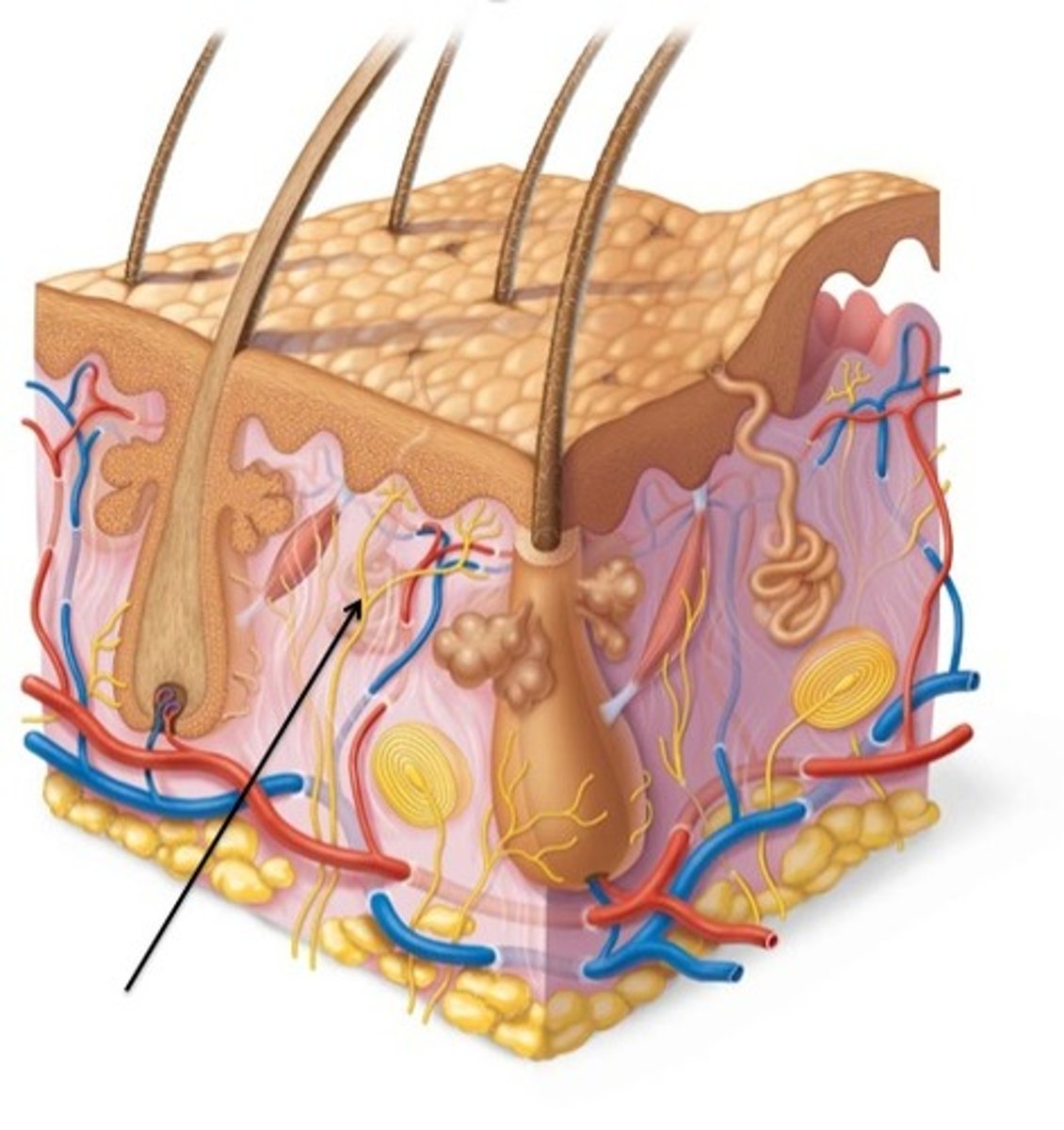
Reticular Layer
Accounts for 80% of dermis thickness,
Dense irregular connective tissue with meshwork of collagen and elastic fibers,
Has blood vessels,
Glands,
Nerve receptors
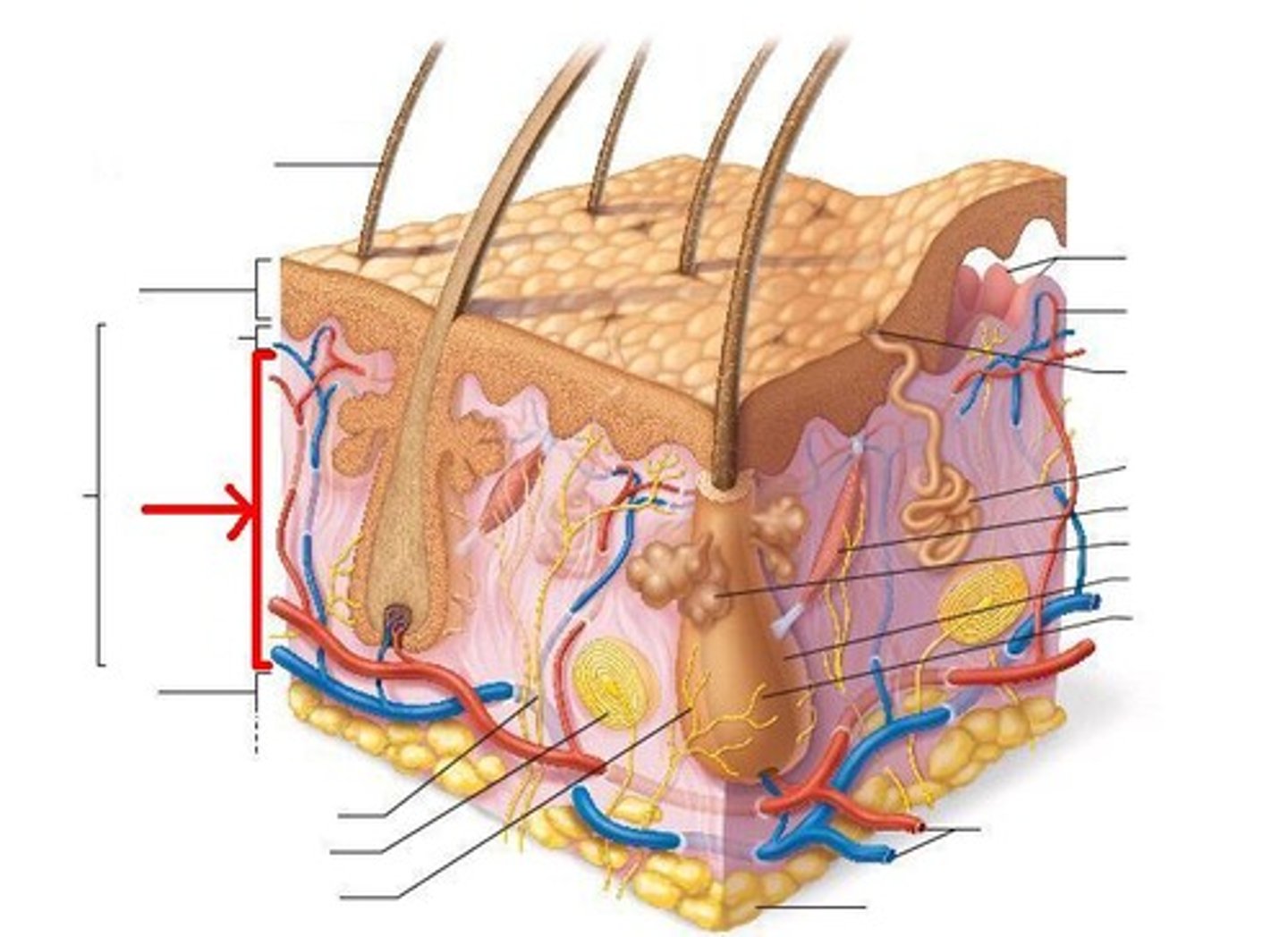
Hypodermis (subcutaneous)
Technically not part of the skin,
Anchors skin to underlying organs,
Composed mainly of adipose tissue (accounts for half of the body's stored fat)
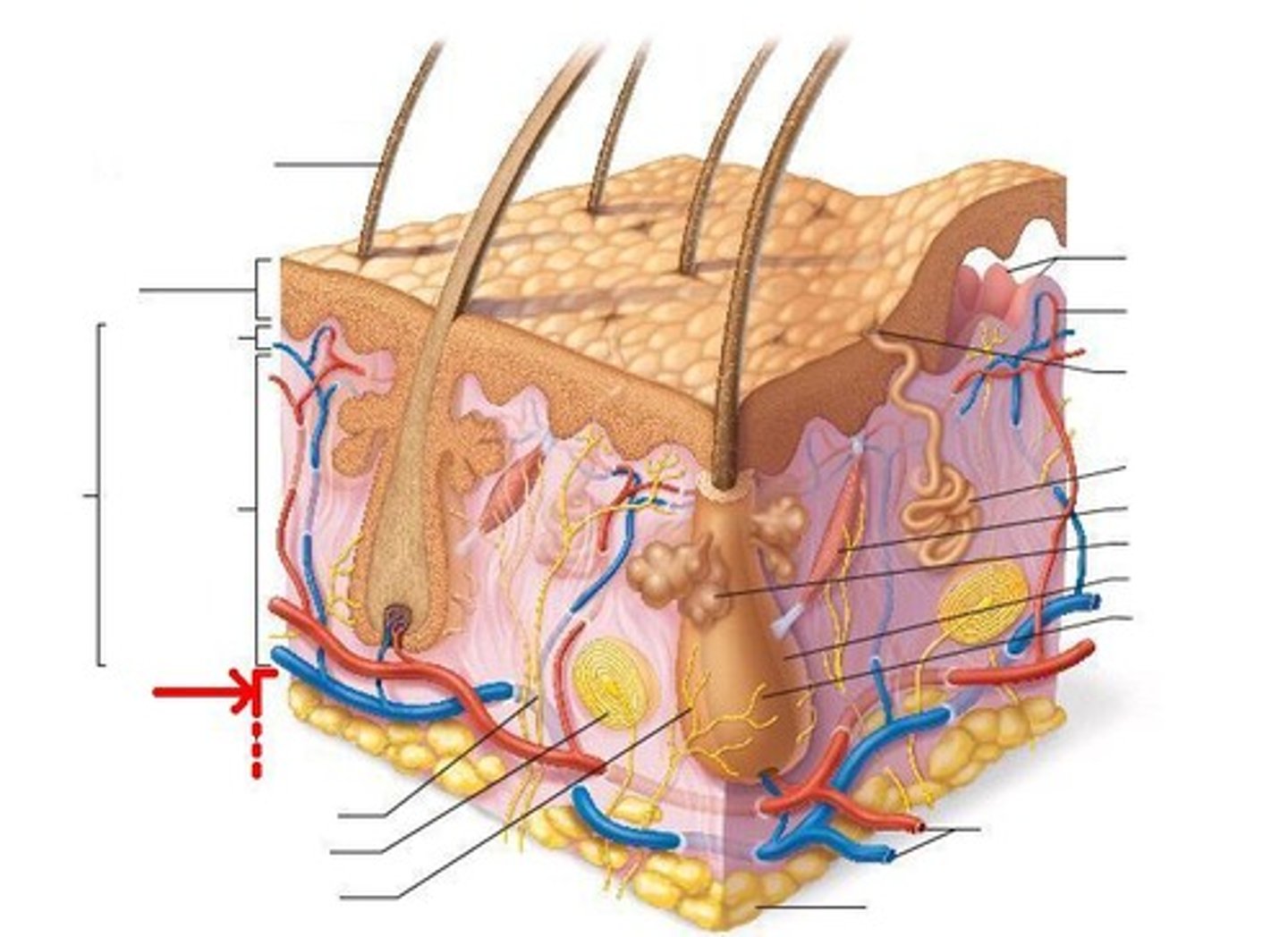
Lamellar Corpuscle
Deep pressure receptors
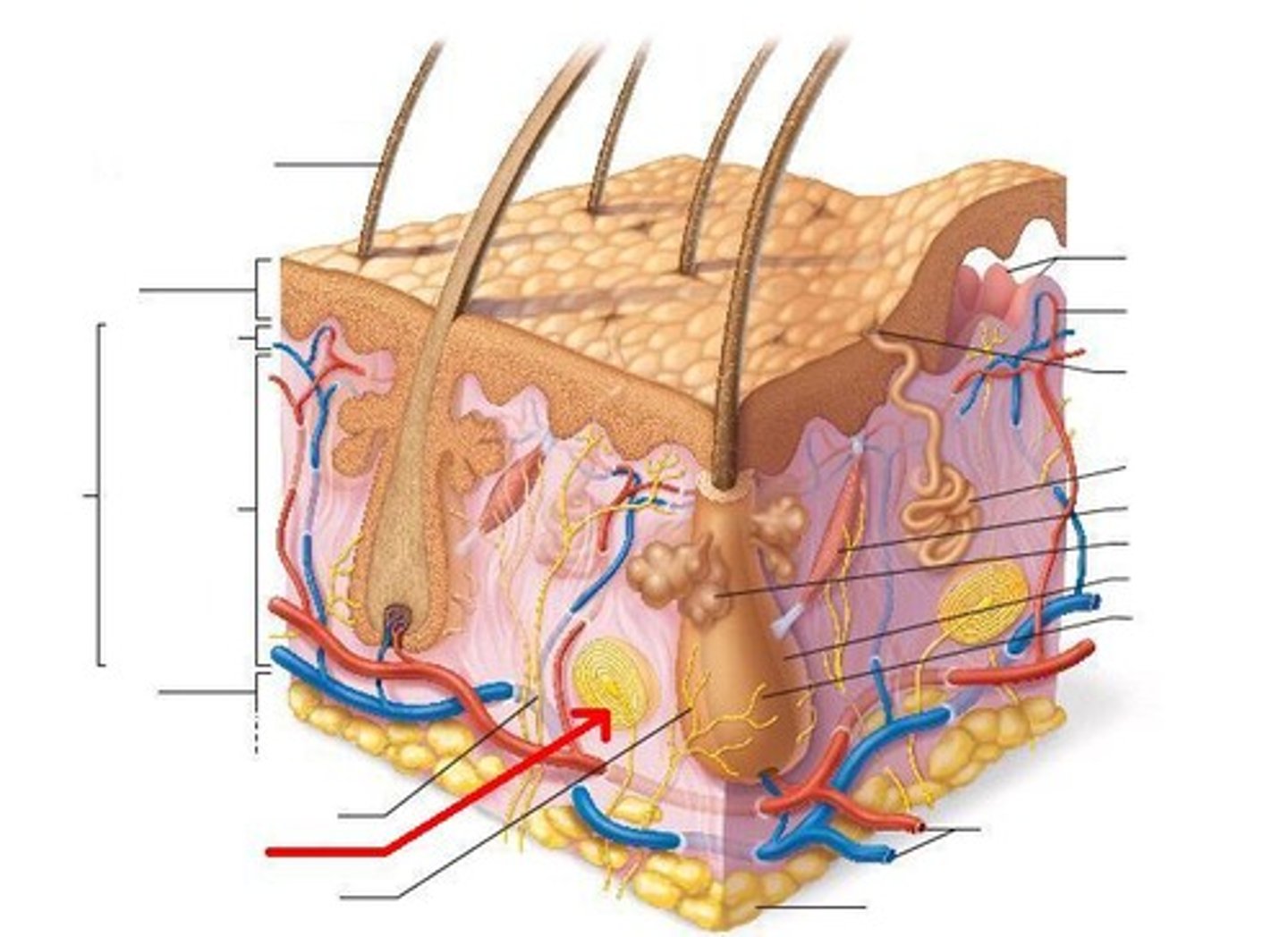
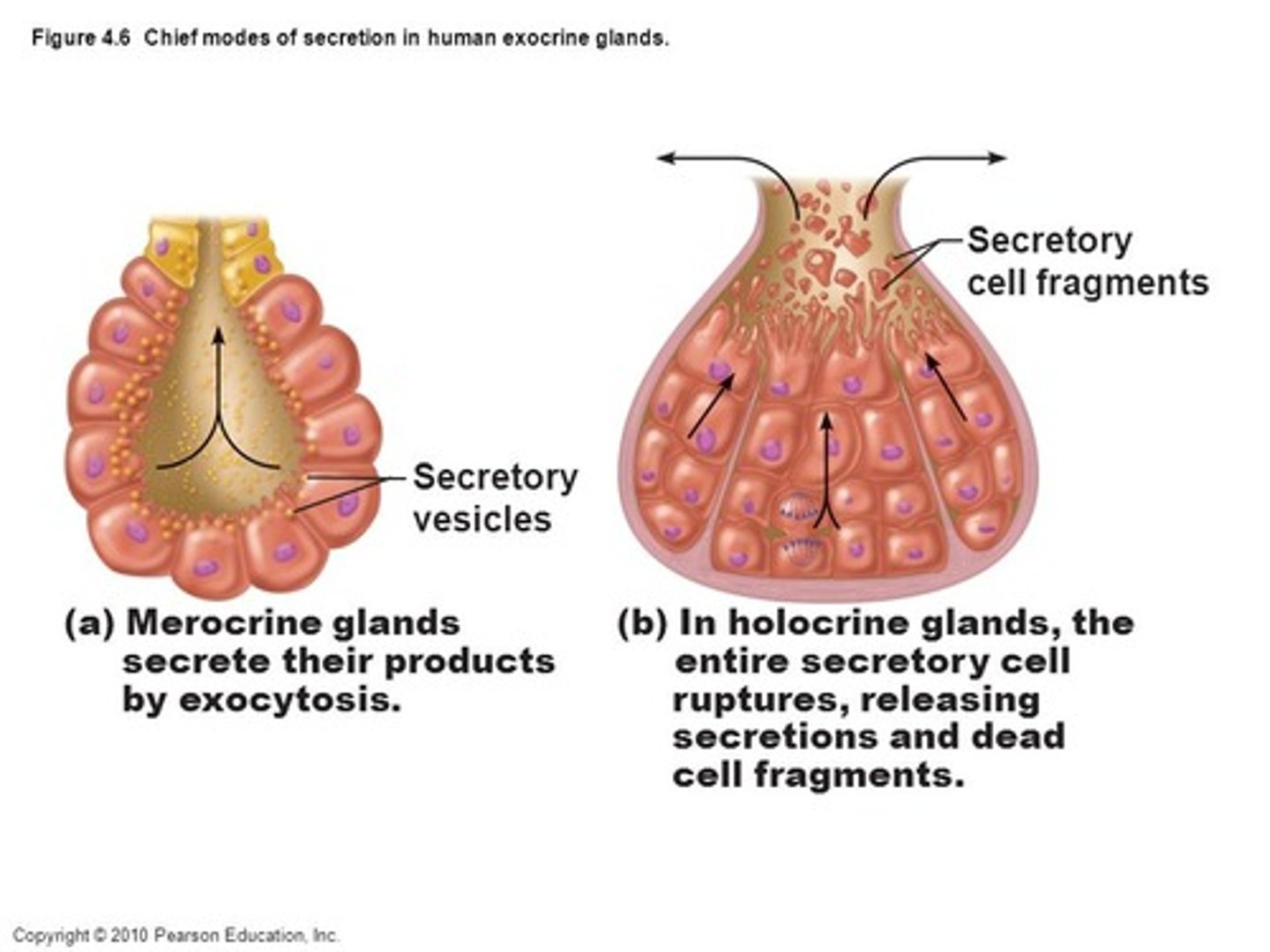
Sebaceous glands
Produces oil (sebum) (softens & lubricates hair & skin),
Most with ducts that empty into hair follicles,
Distributed body wide except for palms of hands and soles of feet,
Activated at puberty (under hormonal control)
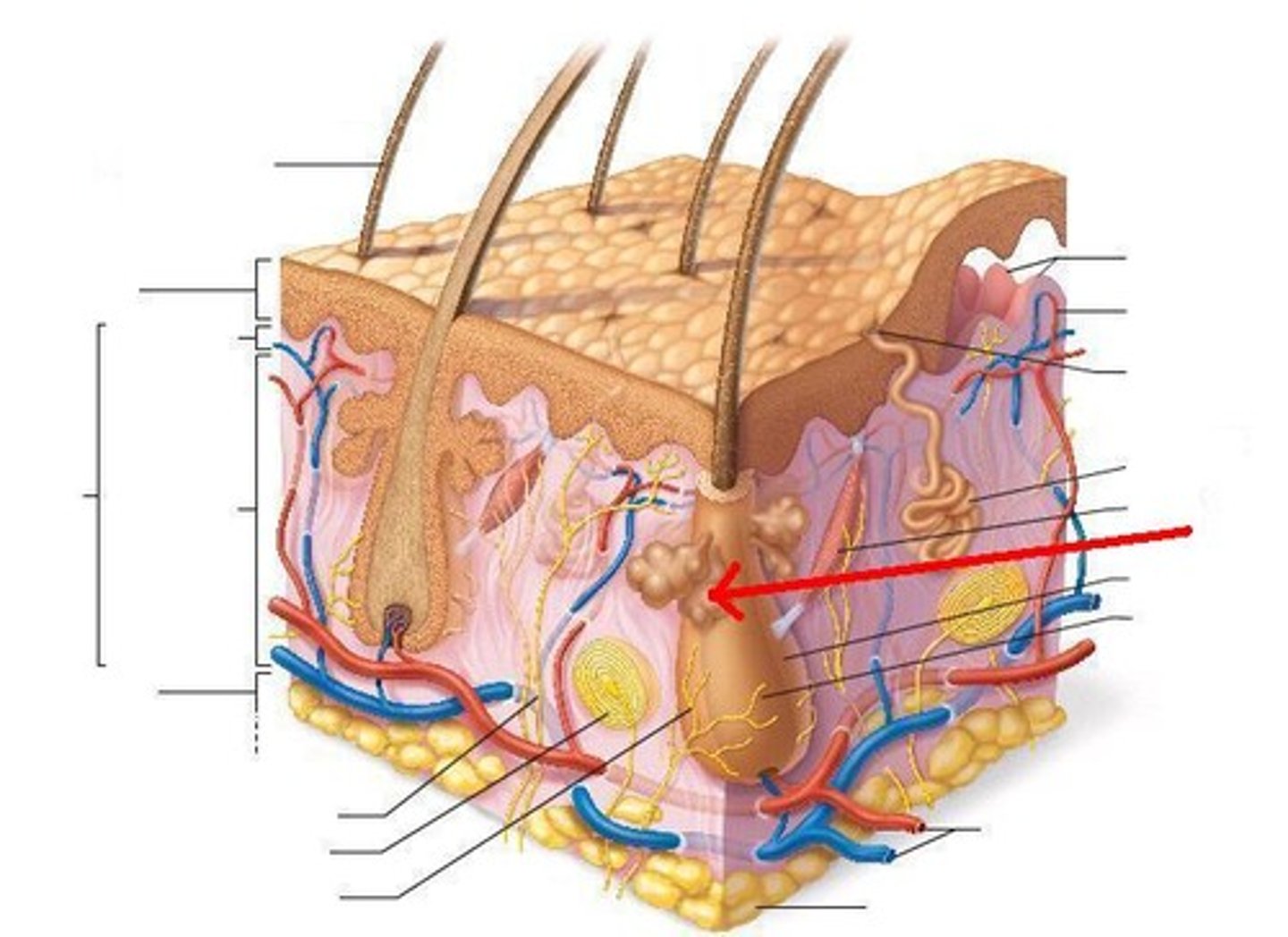
Sebaceous glands are clinically known to cause:
Acne
How does accutane work?
It shuts down the sebaceous glands,
It stops mitosis*
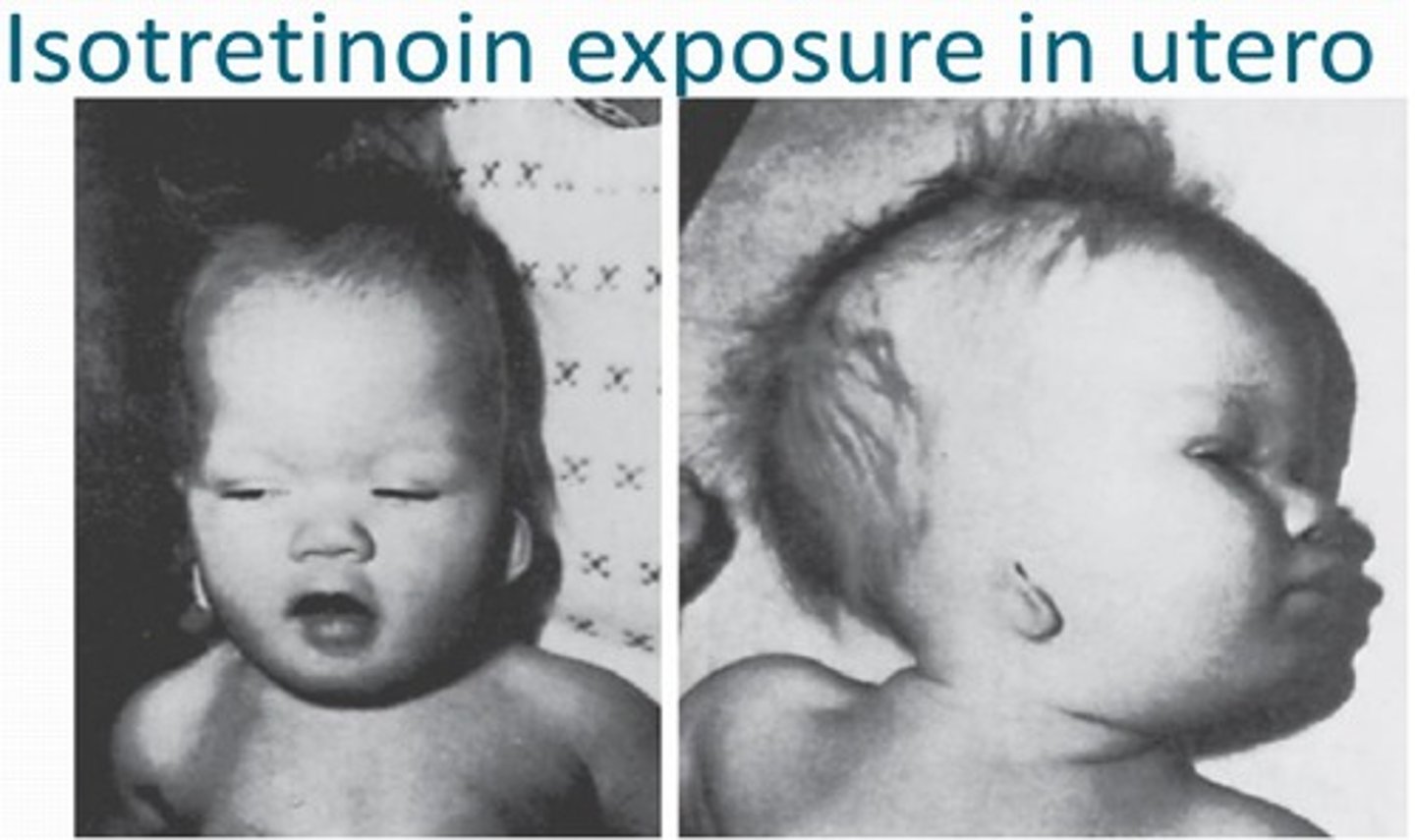
Accutane is a teratogenic
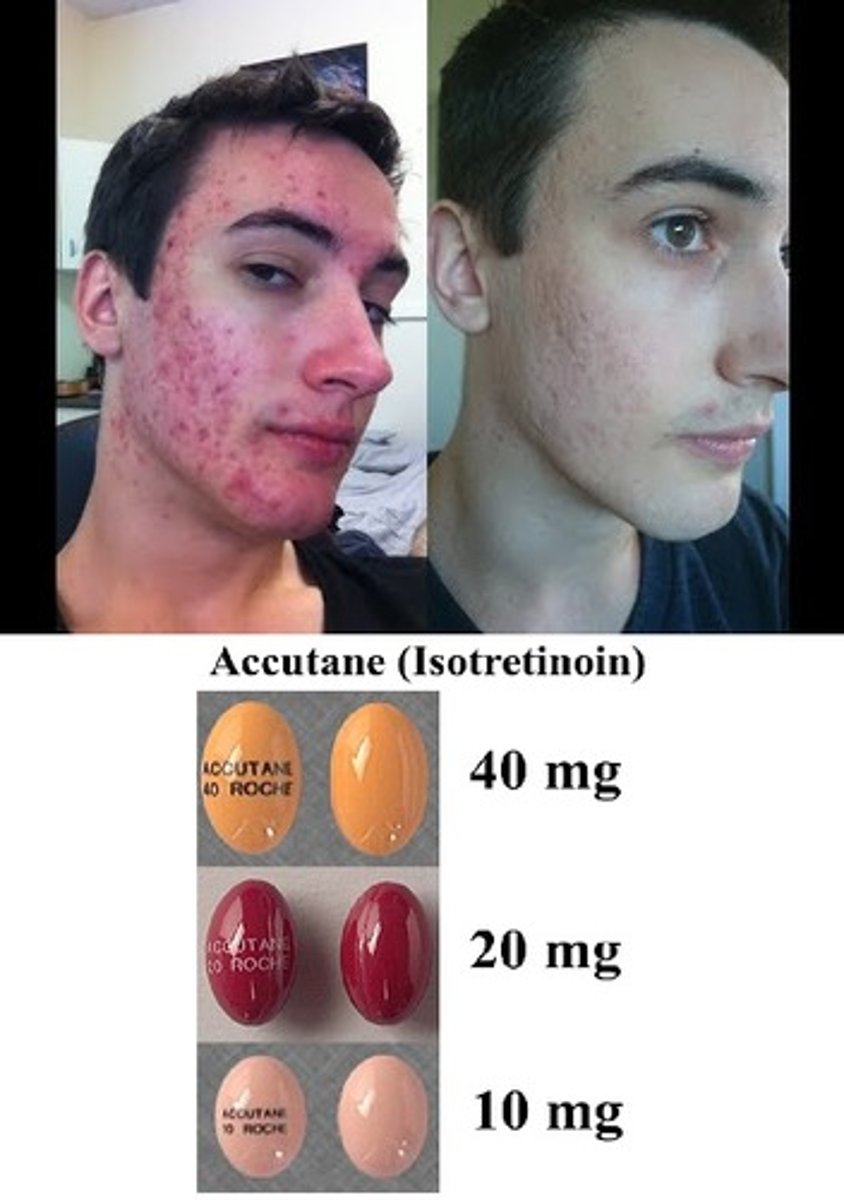
Teratogenic
Causes birth defects,
Accutane causes birth defects by shutting down mitosis, which is how babies form
Sebum
oily substance secreted by sebaceous glands
Sweat (sudoriferous) glands
Widely distributed in skin (up to 3 million body wide)
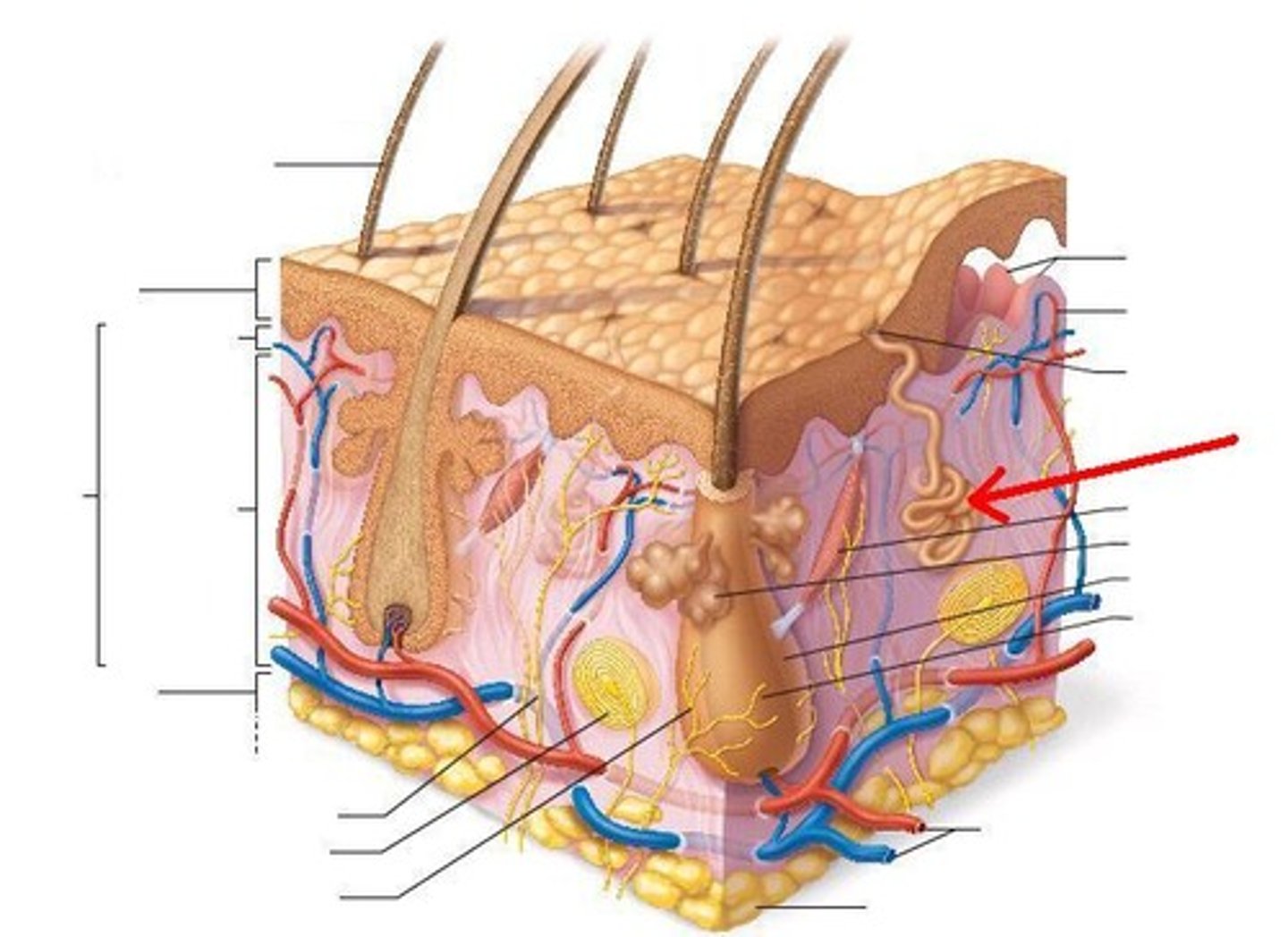
2 types of Sweat (sudoriferous) glands
Eccrine,
Apocrine
(exocytosis)
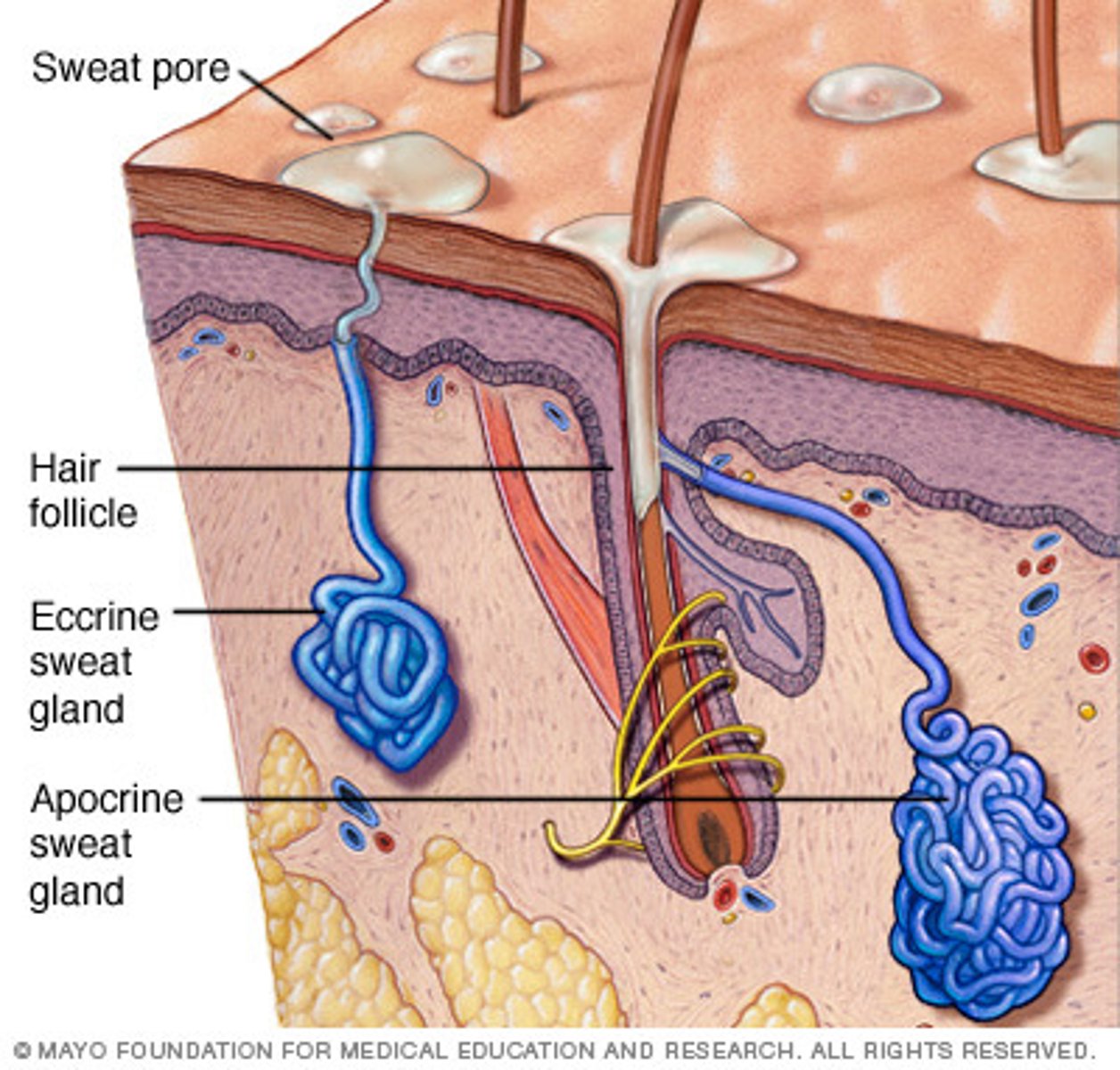
Eccrine gland
Coiled, tubular portion in dermis with opening via duct to pore on the skin surface,
Distributed body wide (most numerous),
Helps dissipate excess heat through evaporative cooling
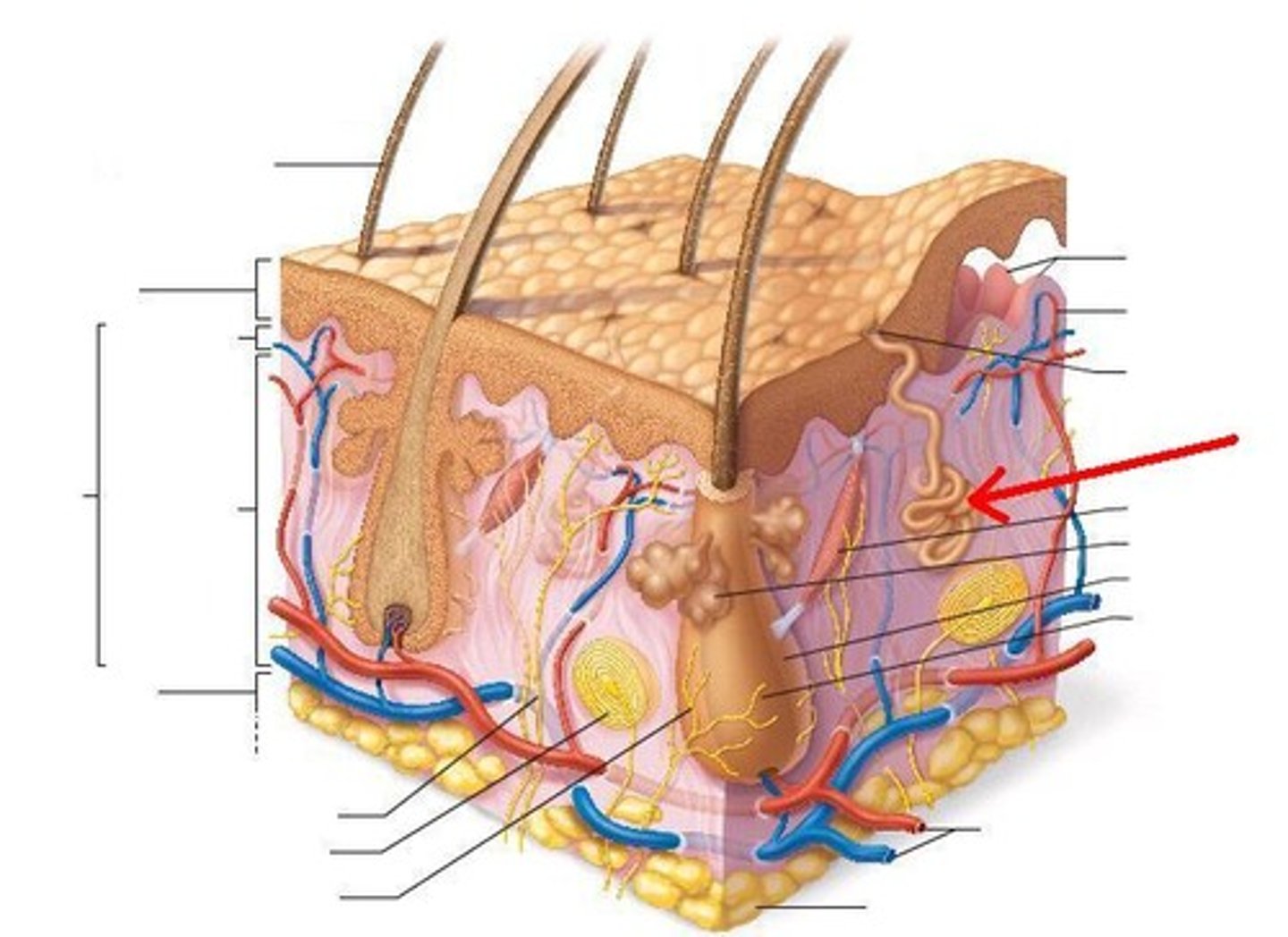
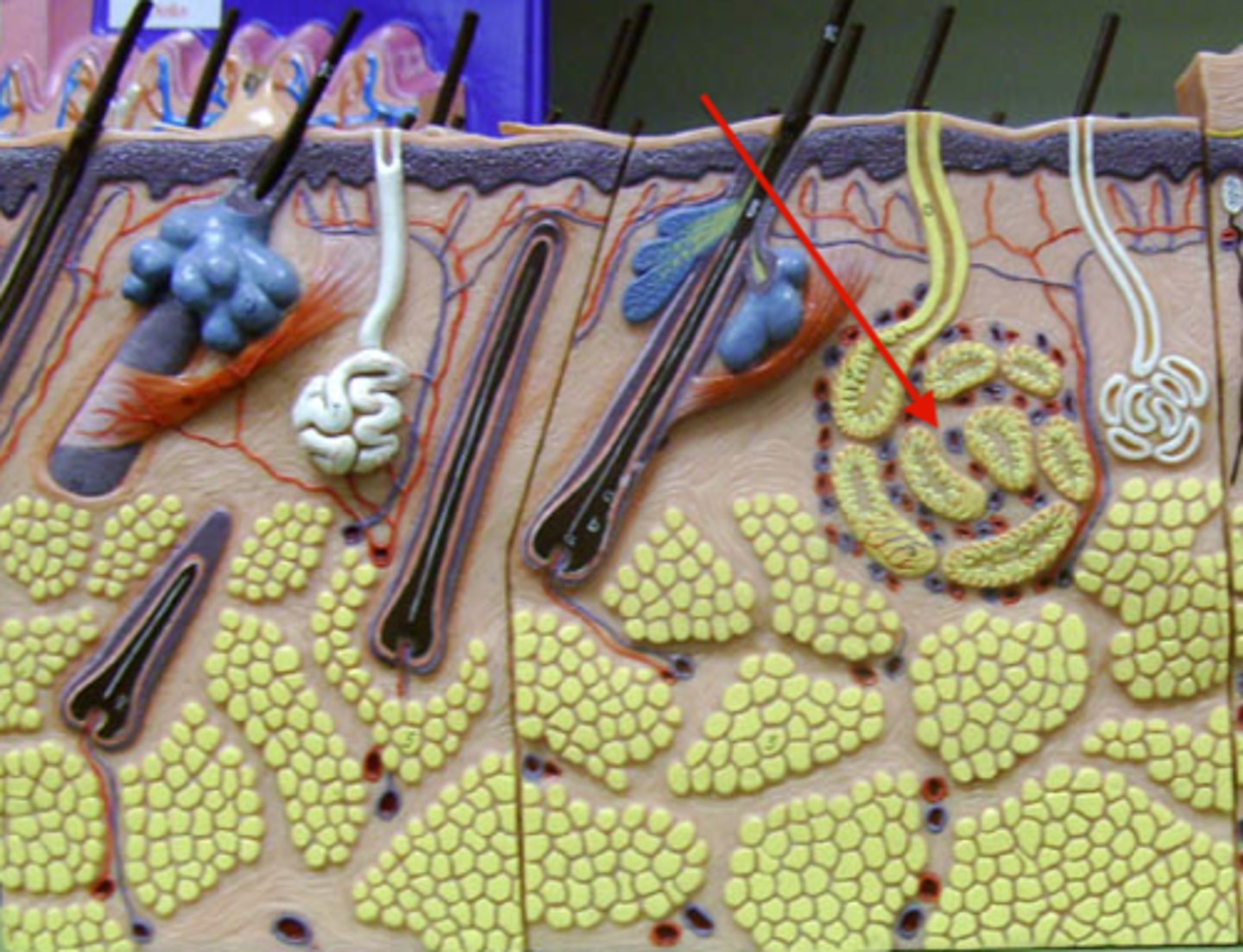
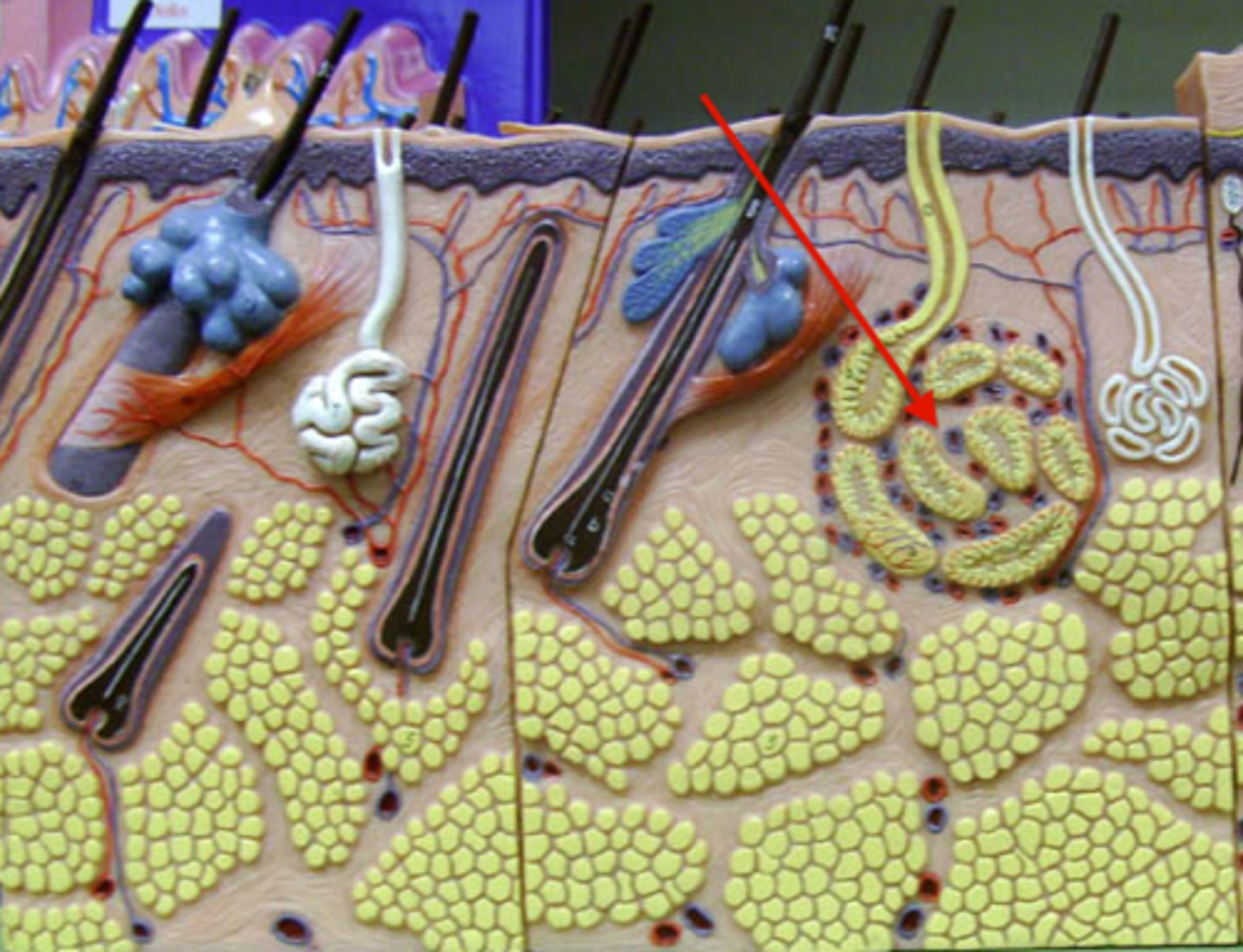
Apocrine gland
Ducts empty into hair follicles,
Localized to axillary and pubic (anogenital) areas,
Activated by stress, pain, and sexual excitement; not temp,
Fatty acid and protein secretion
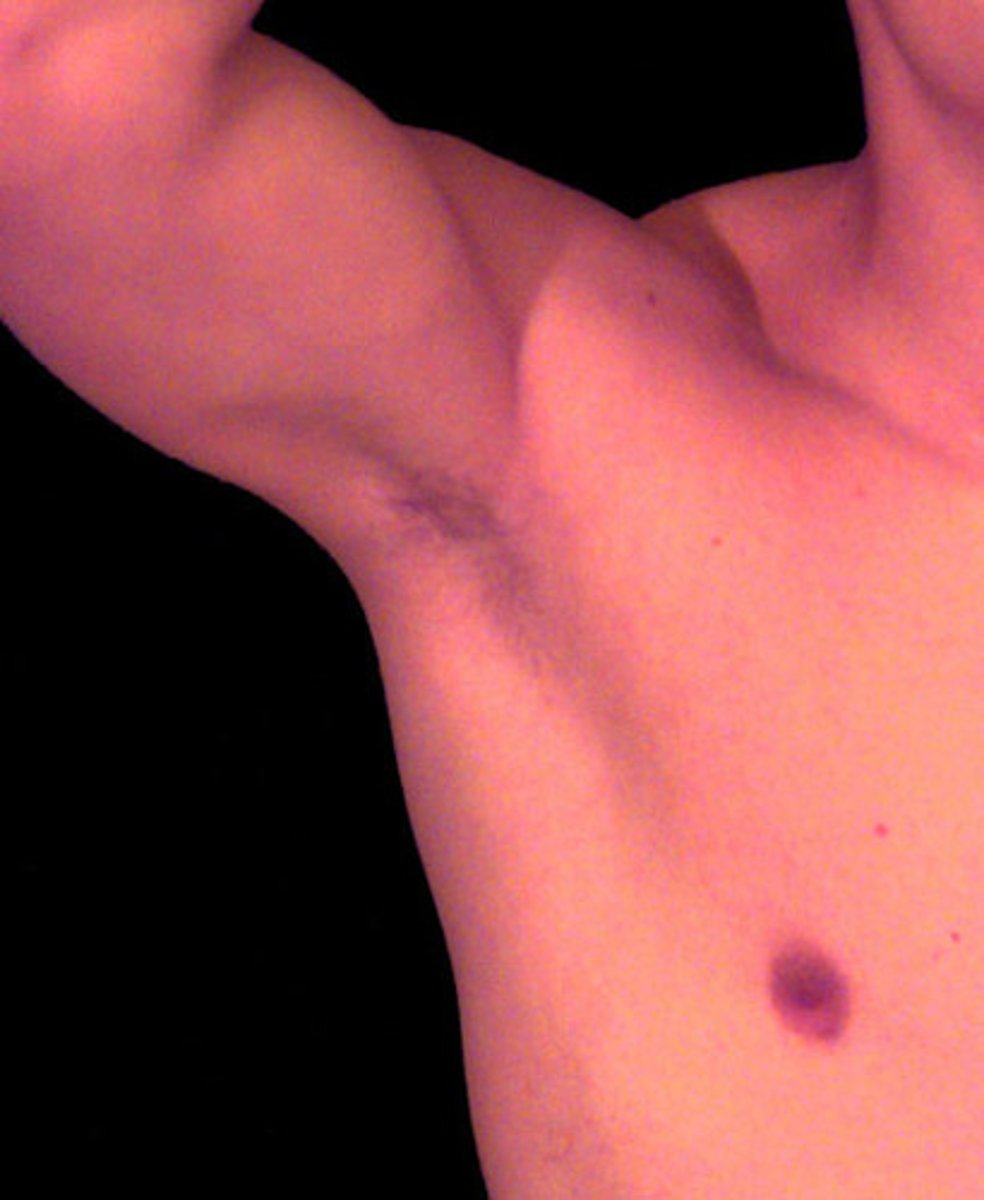
Axillary area
armpit
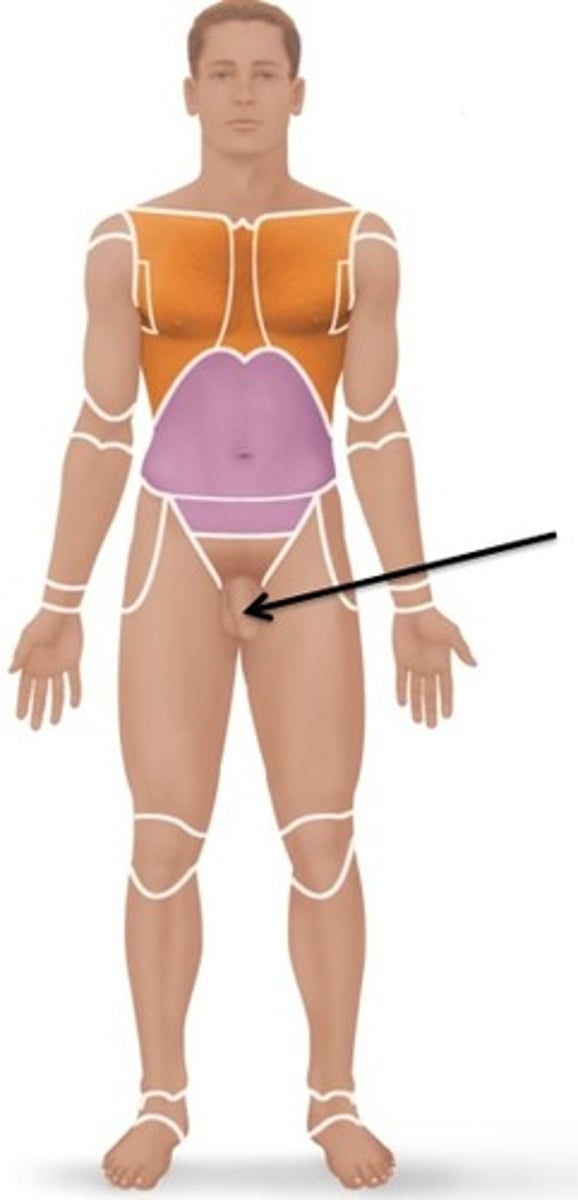
Pubic (anogenital) area
Anus and genitals
How many apocrine glands are there?
only 2,000
What causes body odor?
bacterial breakdown of apocrine sweat
(fatty acid and protein secretion)

2 Modified sweat glands
Ceruminous glands,
Mammary glands
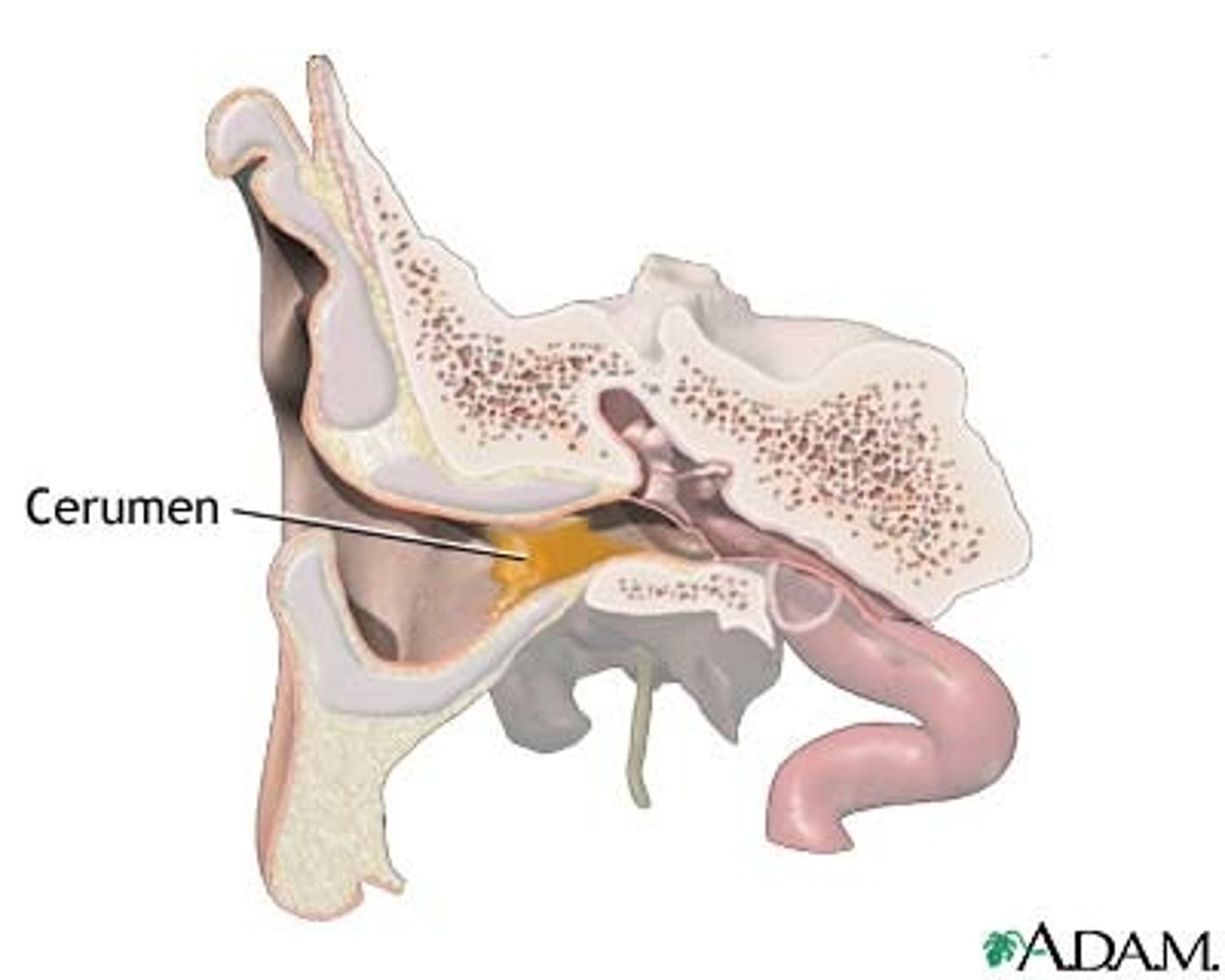
Ceruminous glands
Found in lining of external ear canal,
Secretion mixes with sebum(oil) to produce cerumen (earwax)
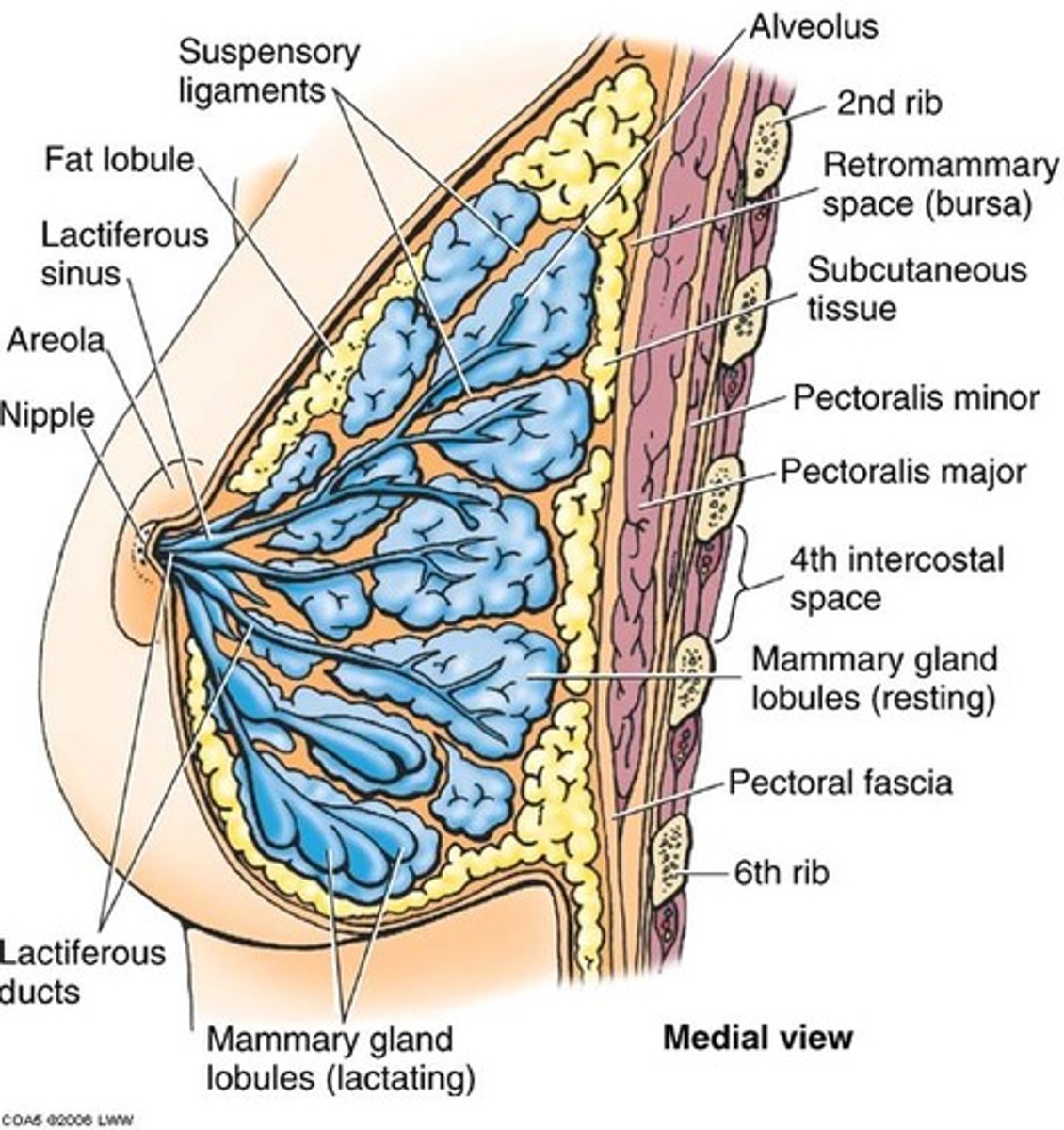
Mammory glands
produce milk
Hair
Distributed body wide except for palms, soles, lips, nipples. & part of external genitalia,
Strand of dead, hard keratinized epithelial cells projecting from an invaginated tunnel in the epidermal and dermal layers called the hair follicle
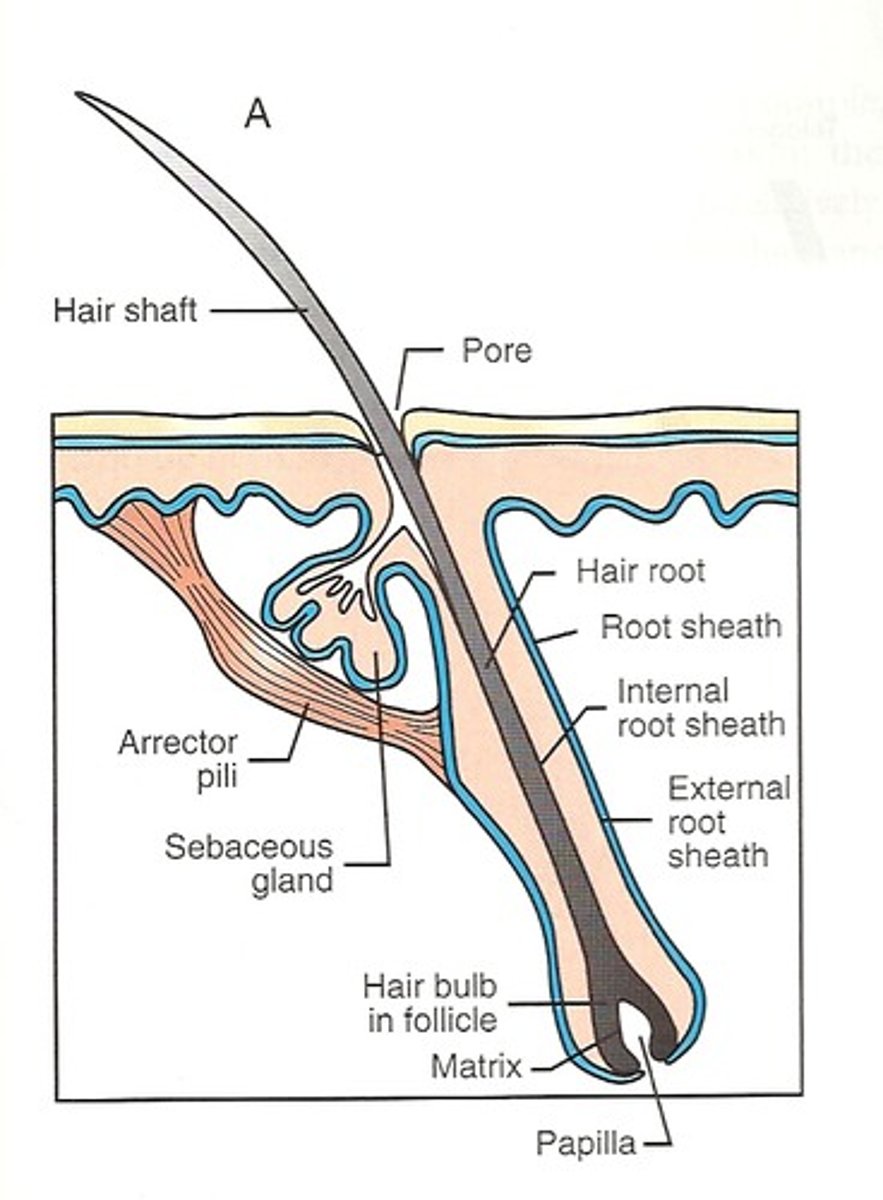
Hair follicle
Tubular invaginations of the epidermis,
Formed by mitotically active stratum basale cells,
Melanocytes provide pigment for hair color,
Dermal capillaries provide blood supply
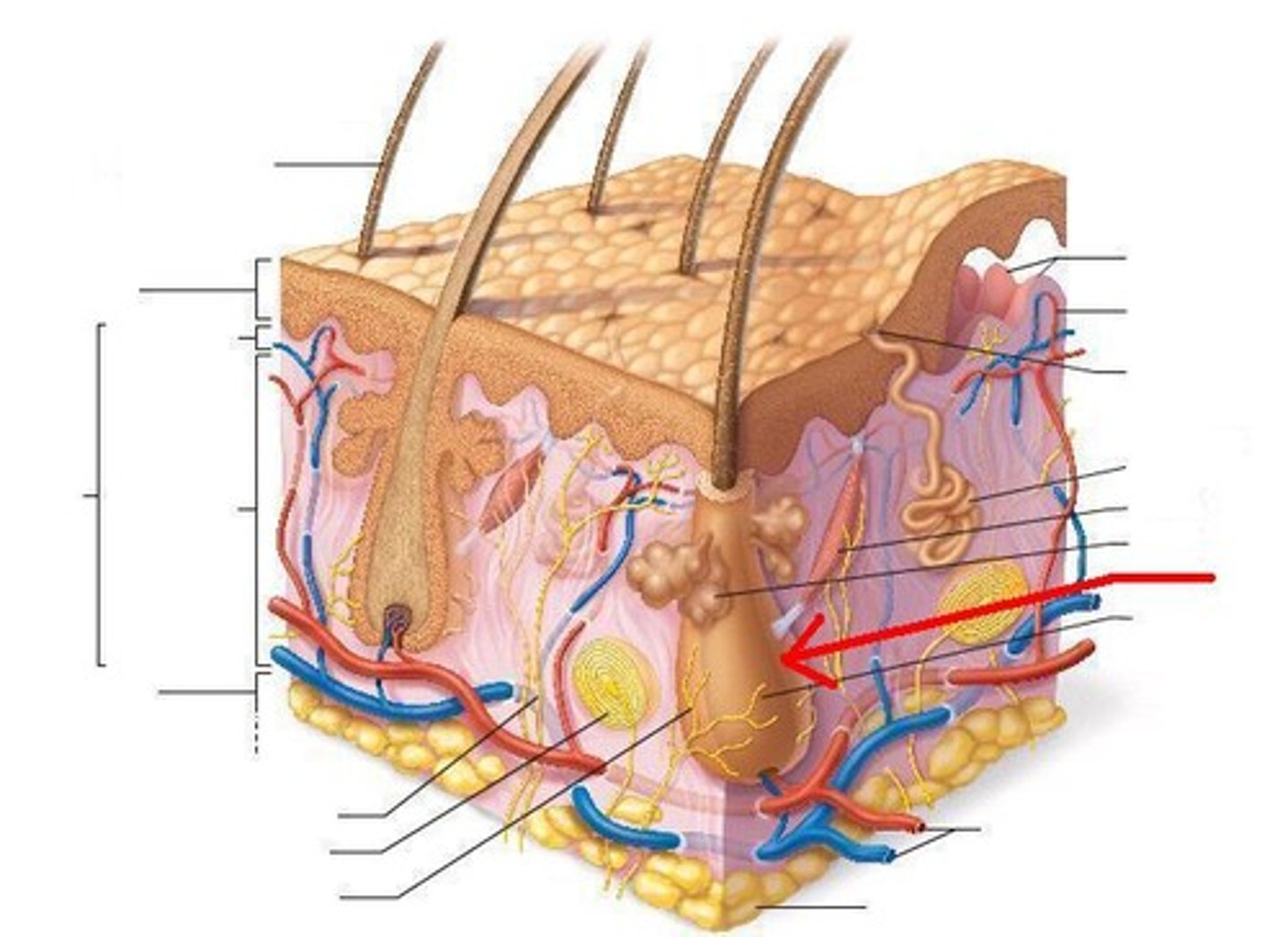
Parts of hair
Bulb,
Root,
Shaft
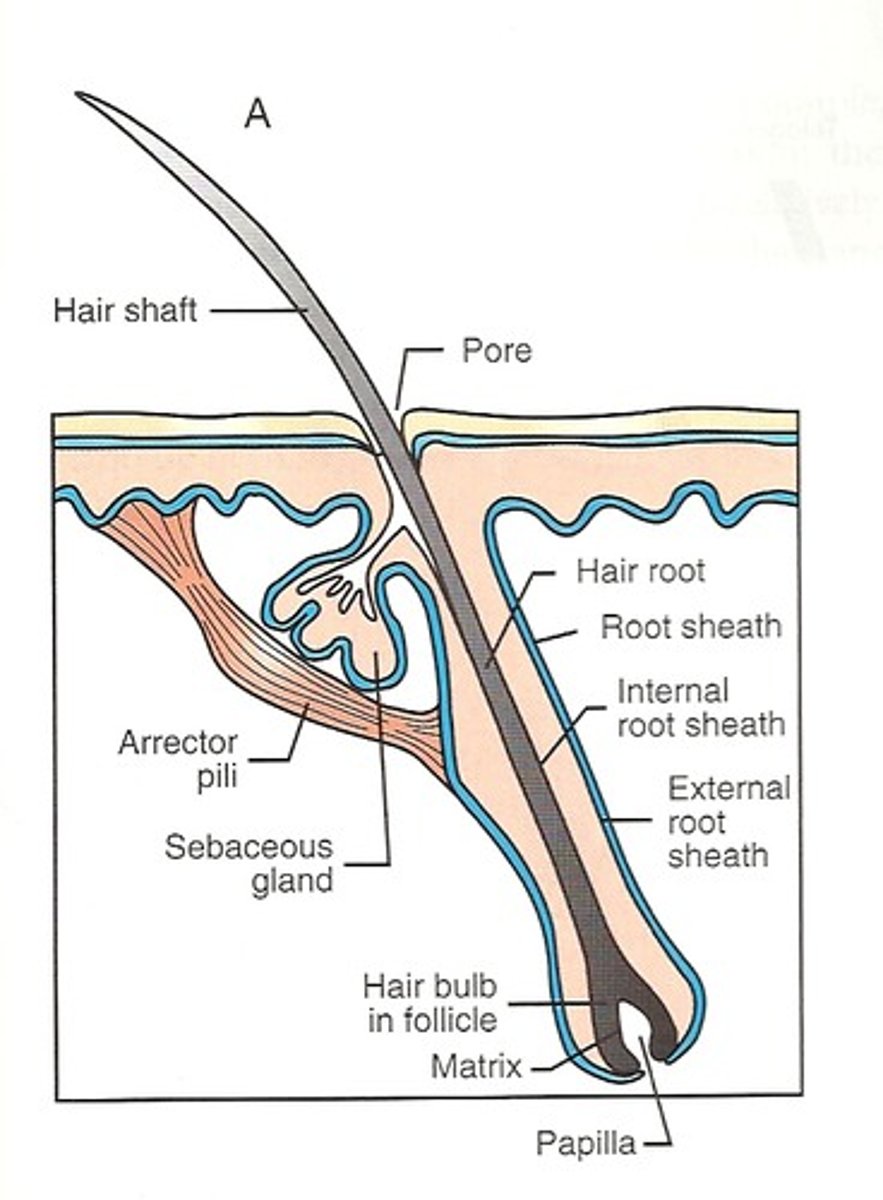
Bulb
Growth zone at inferior end of hair follicle
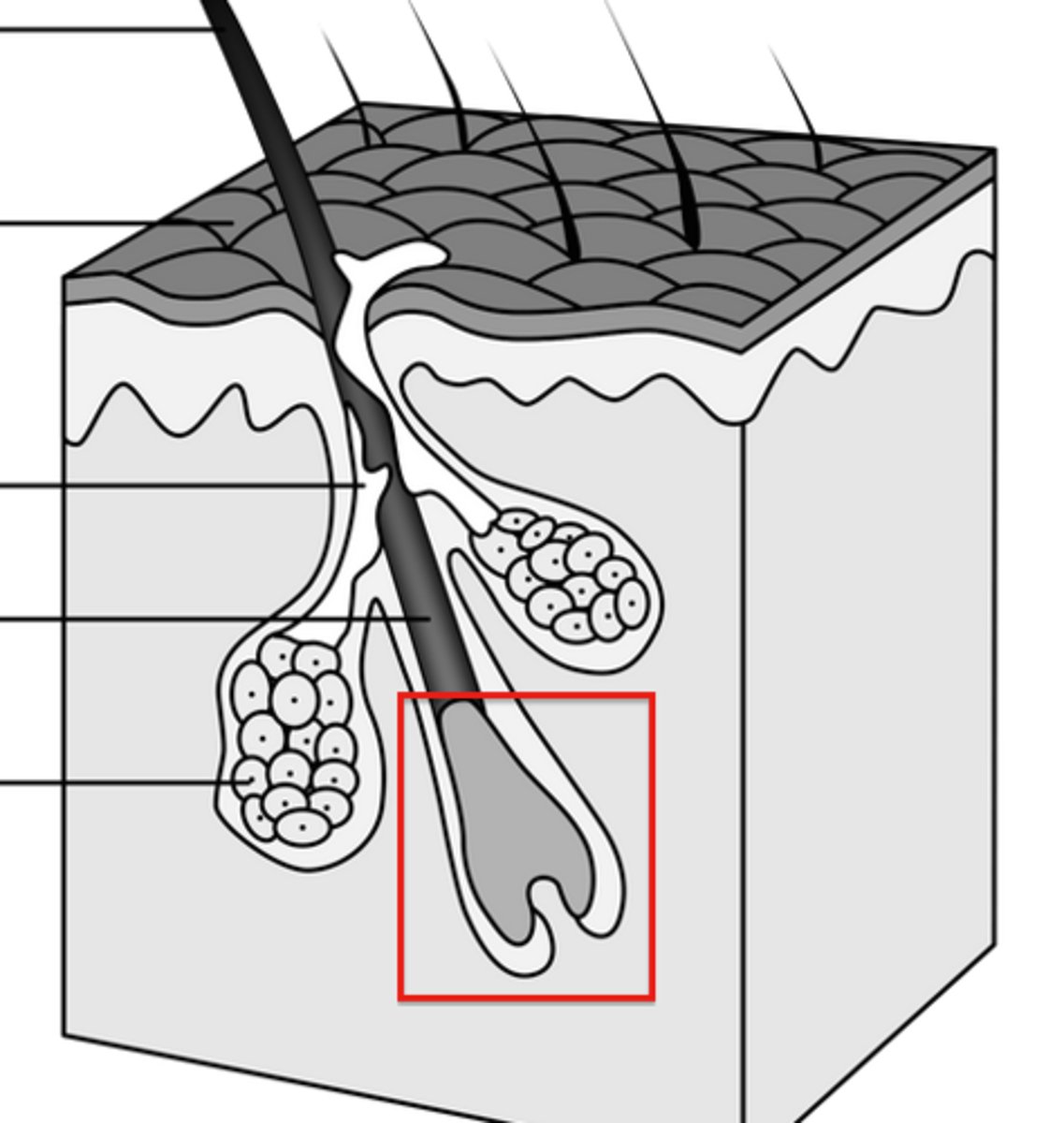
Root
Part of the hair enclosed in hair follicle
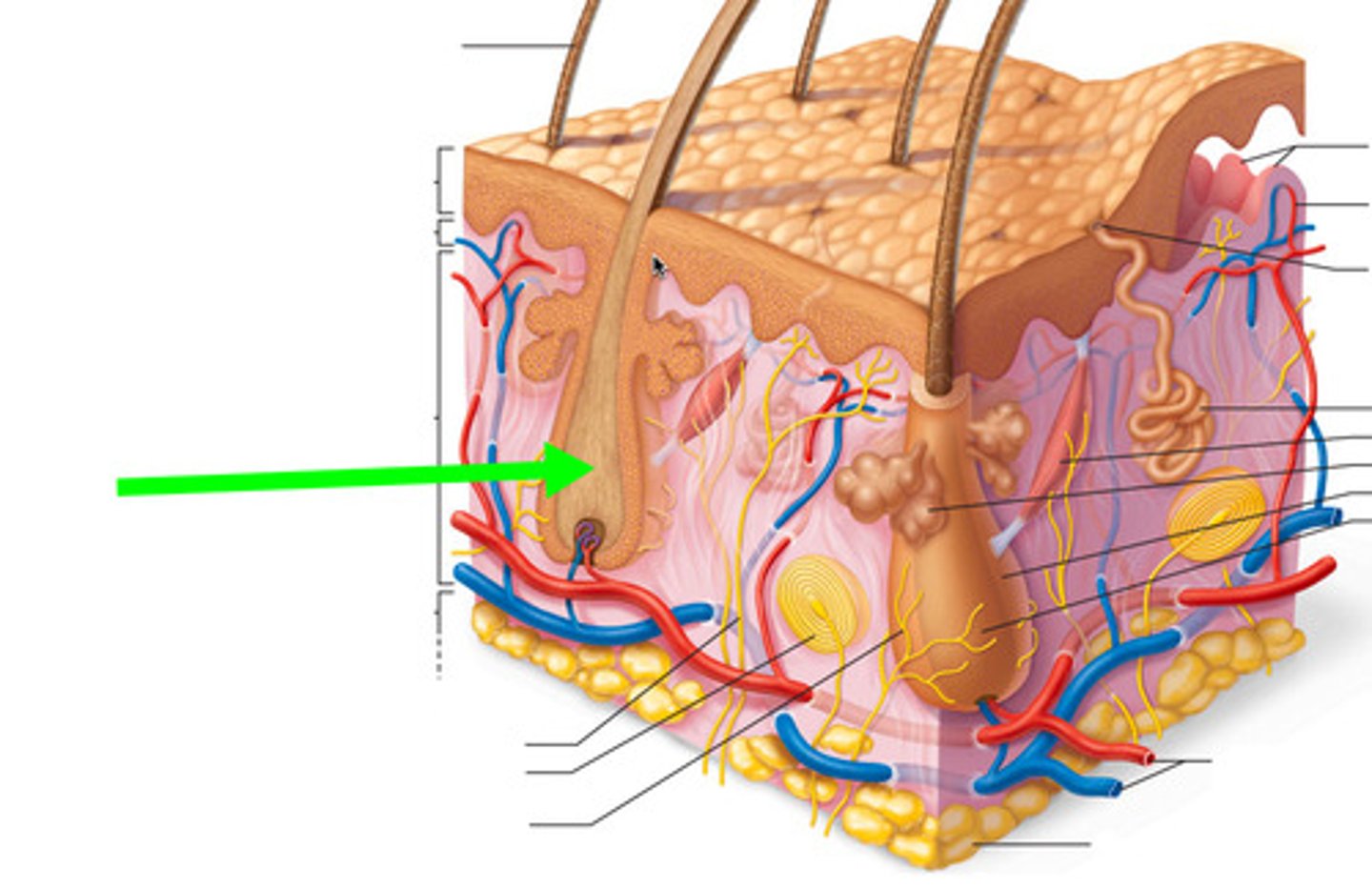
Shaft
Visible part of hair; projects from surface of skin
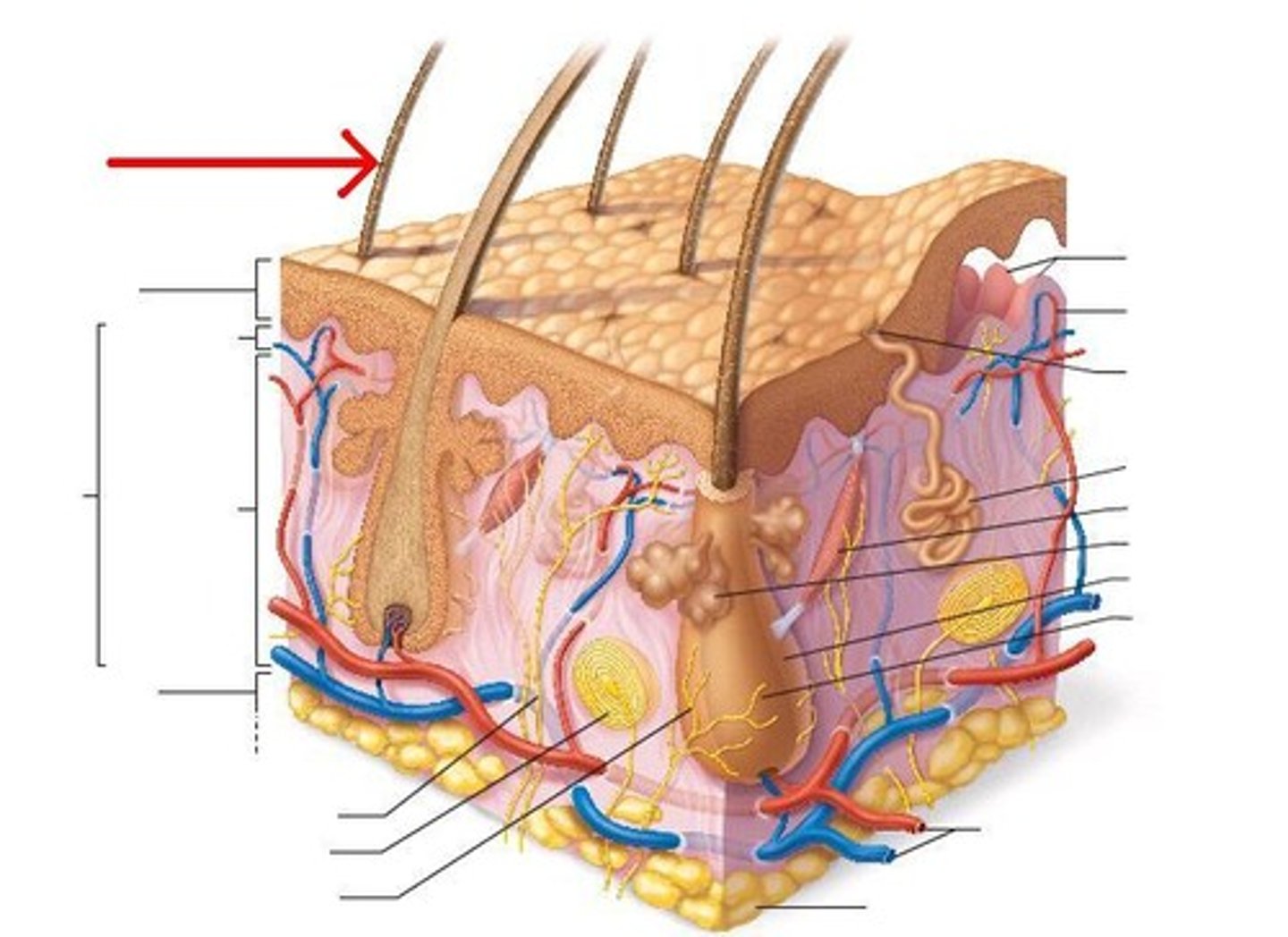
Arrector Pili muscle (smooth muscle)
Can move hair like in goosebumps
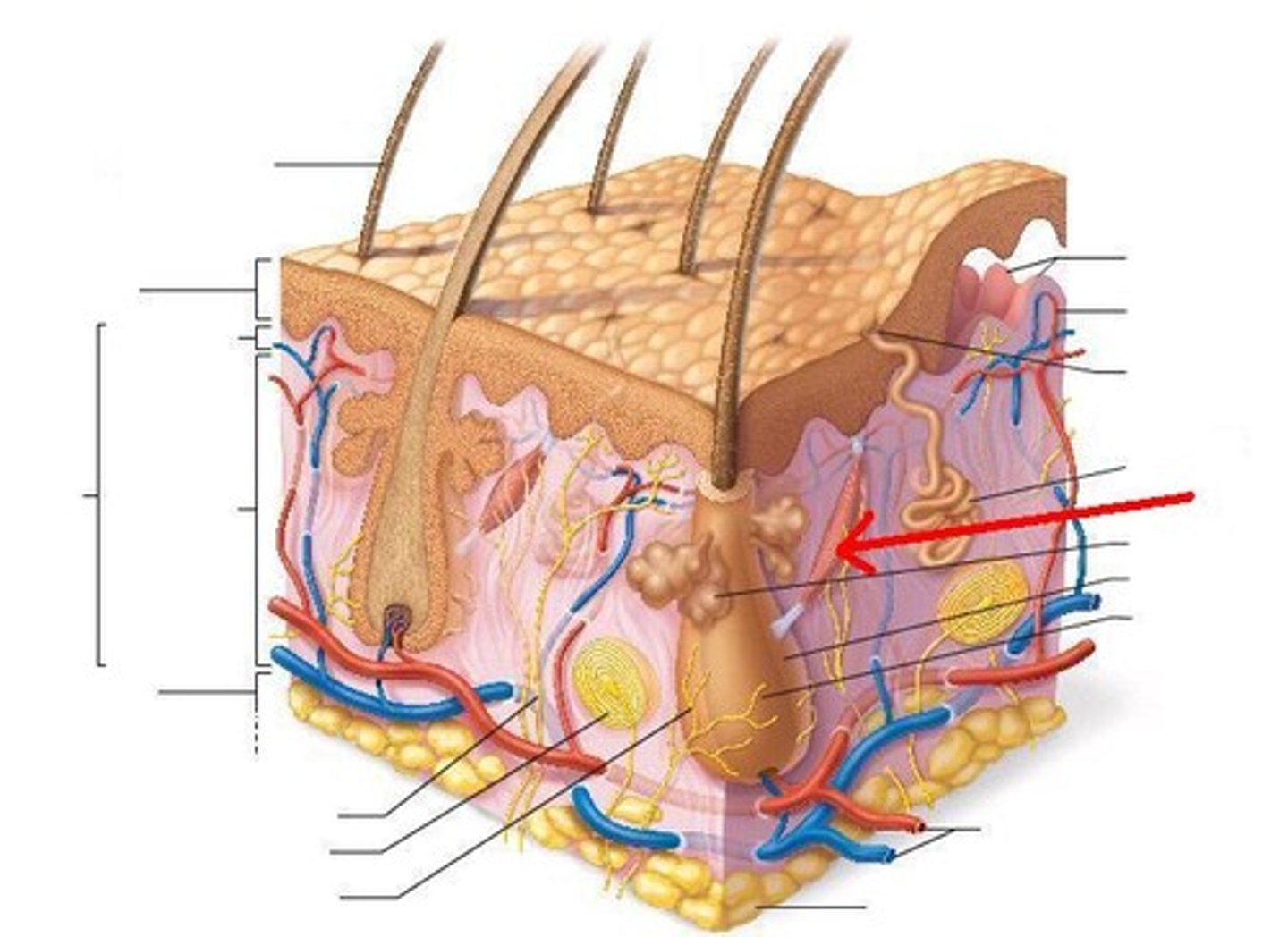
What is clinically used for hair growth?
Minoxidil
ex) in drug known as Rogaine

Nail structures
Nail fold (lateral & proximal skin coverings),
Eponychium (cuticle),
Nail body
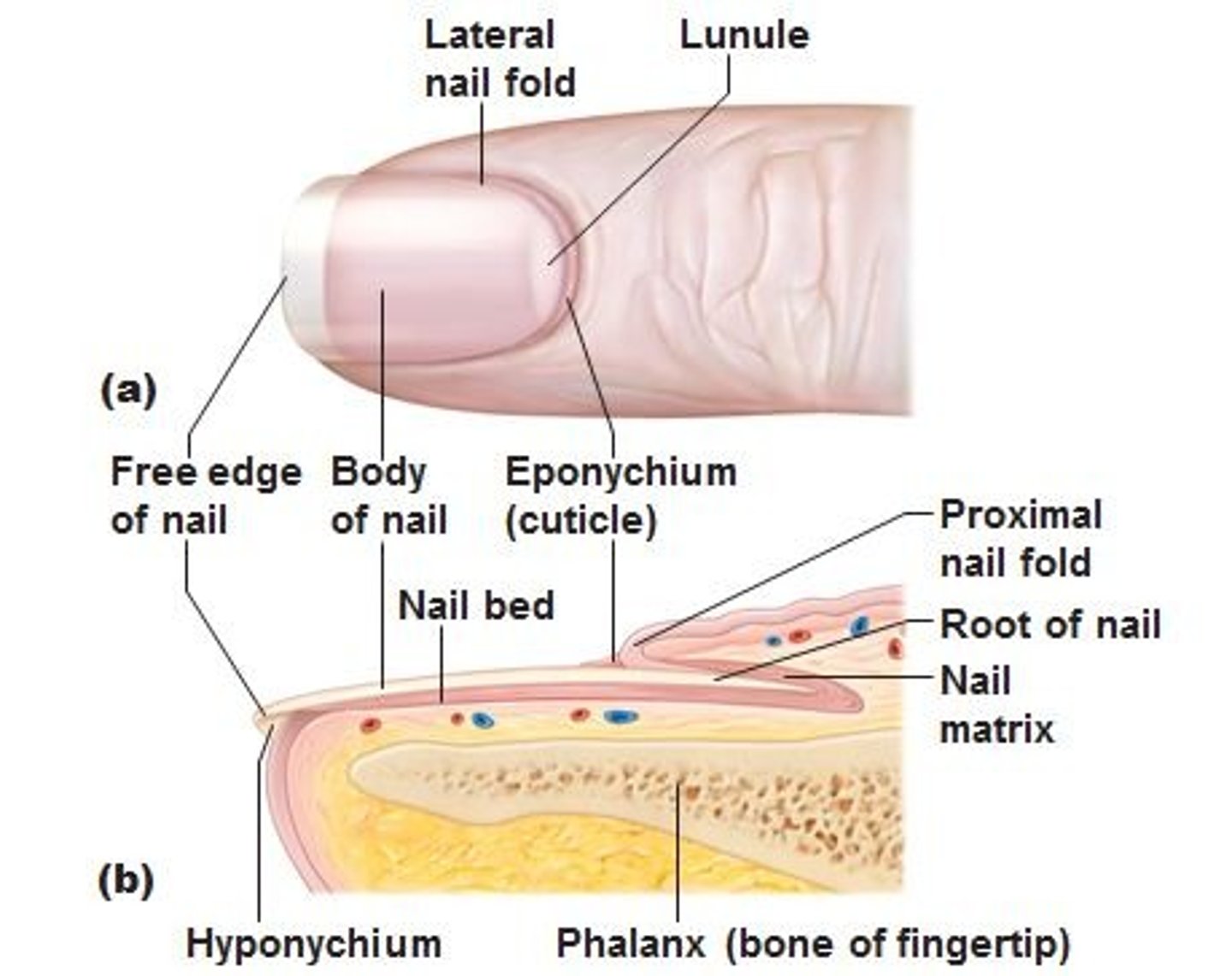
Nail Fold
Lateral and proximal skin coverage for nails
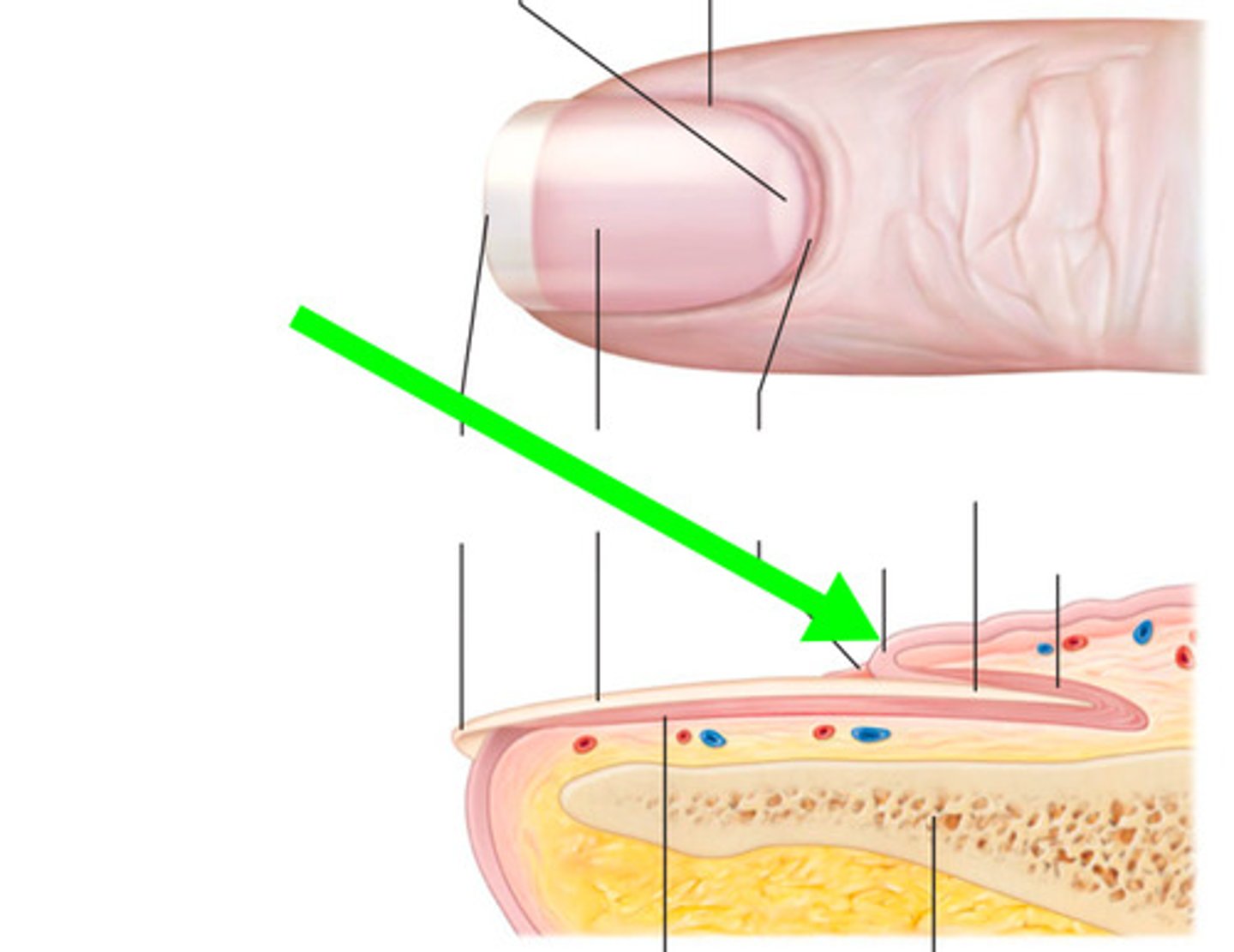
Eponychium
Cuticle
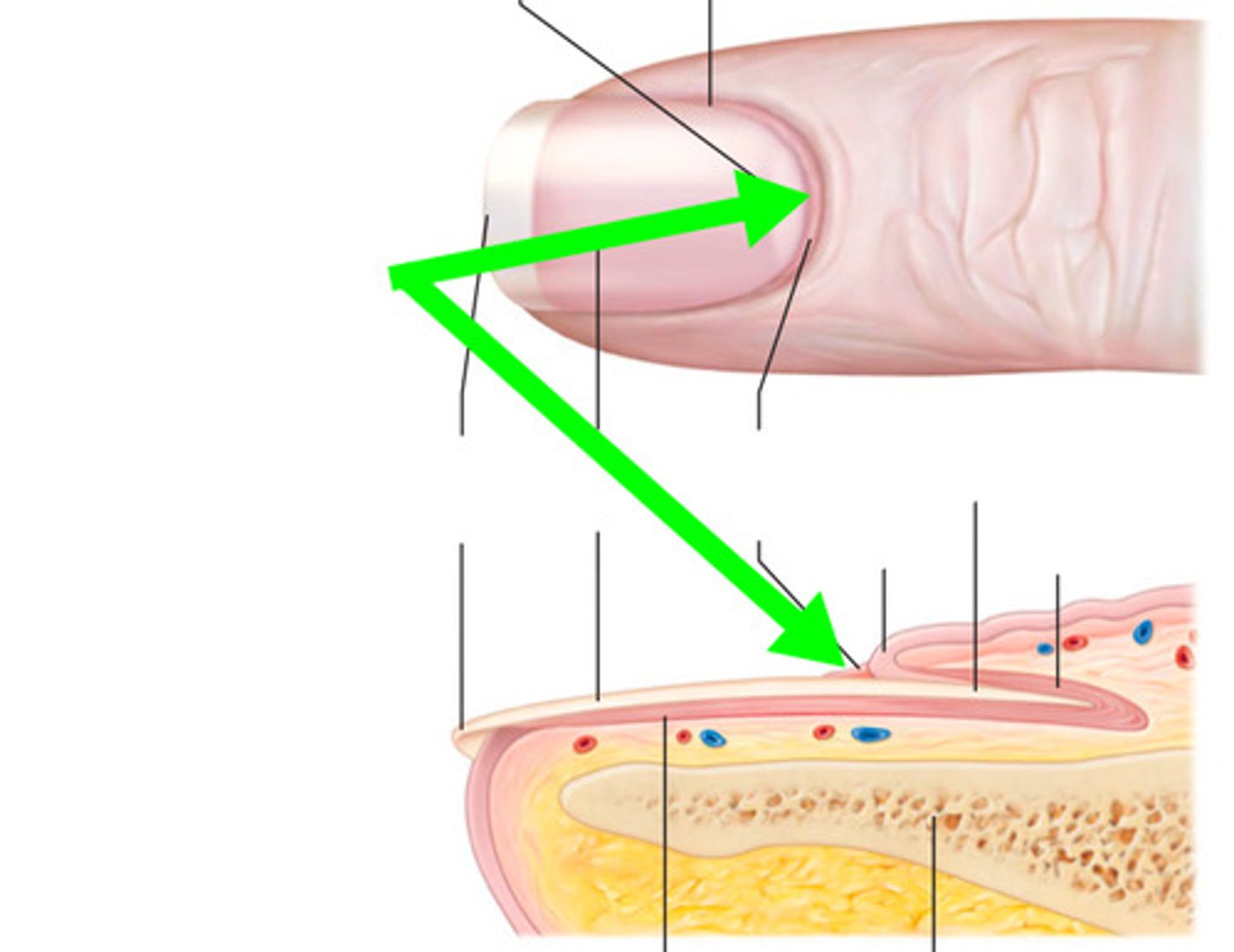
Nail Body
Sheet of hard keratin attached to nail bed,
Lunula
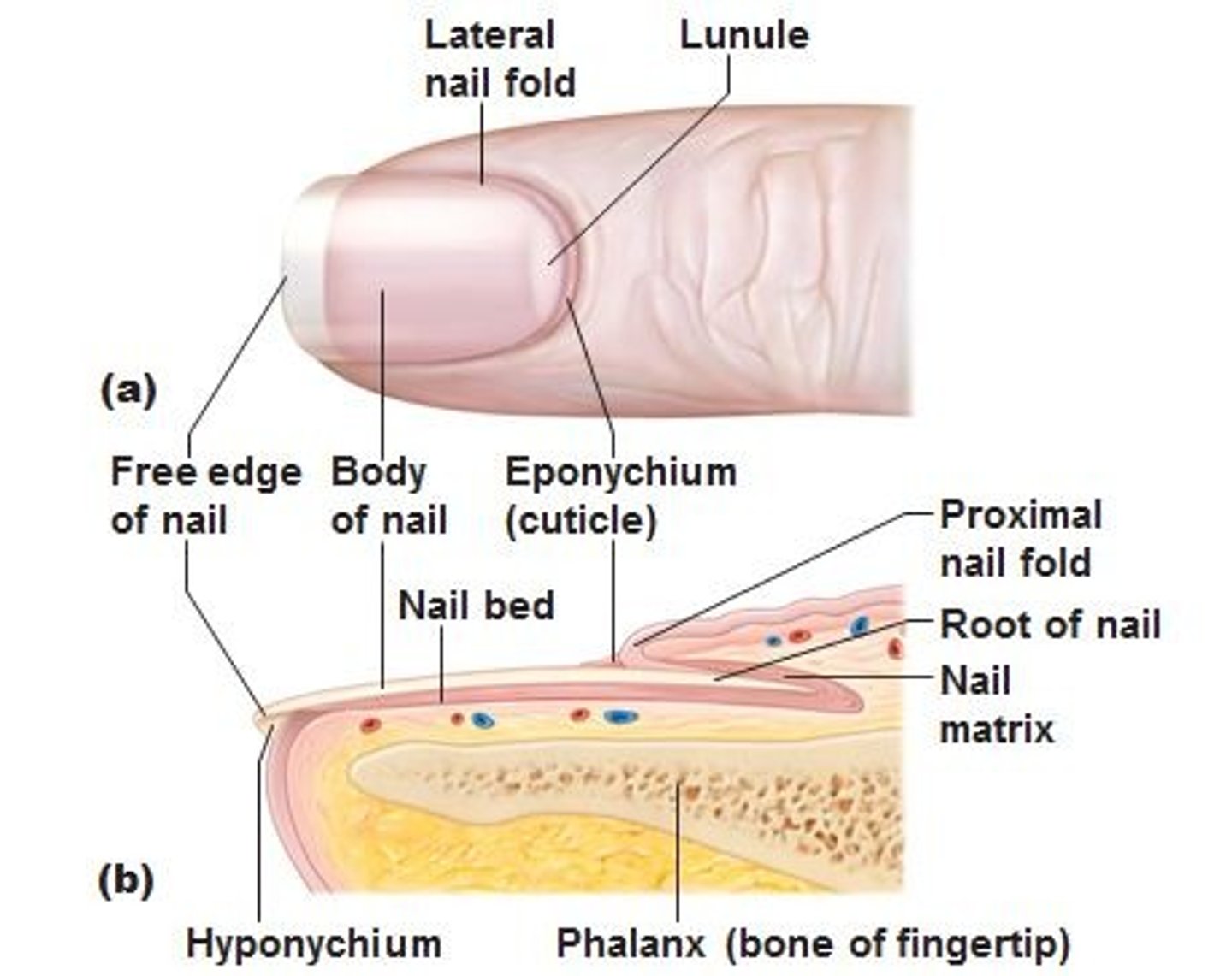
Lunule/Lunula
Crescent shaped vascular area at proximal end of the nail bed and visible through the nail. (white area at base of nail),
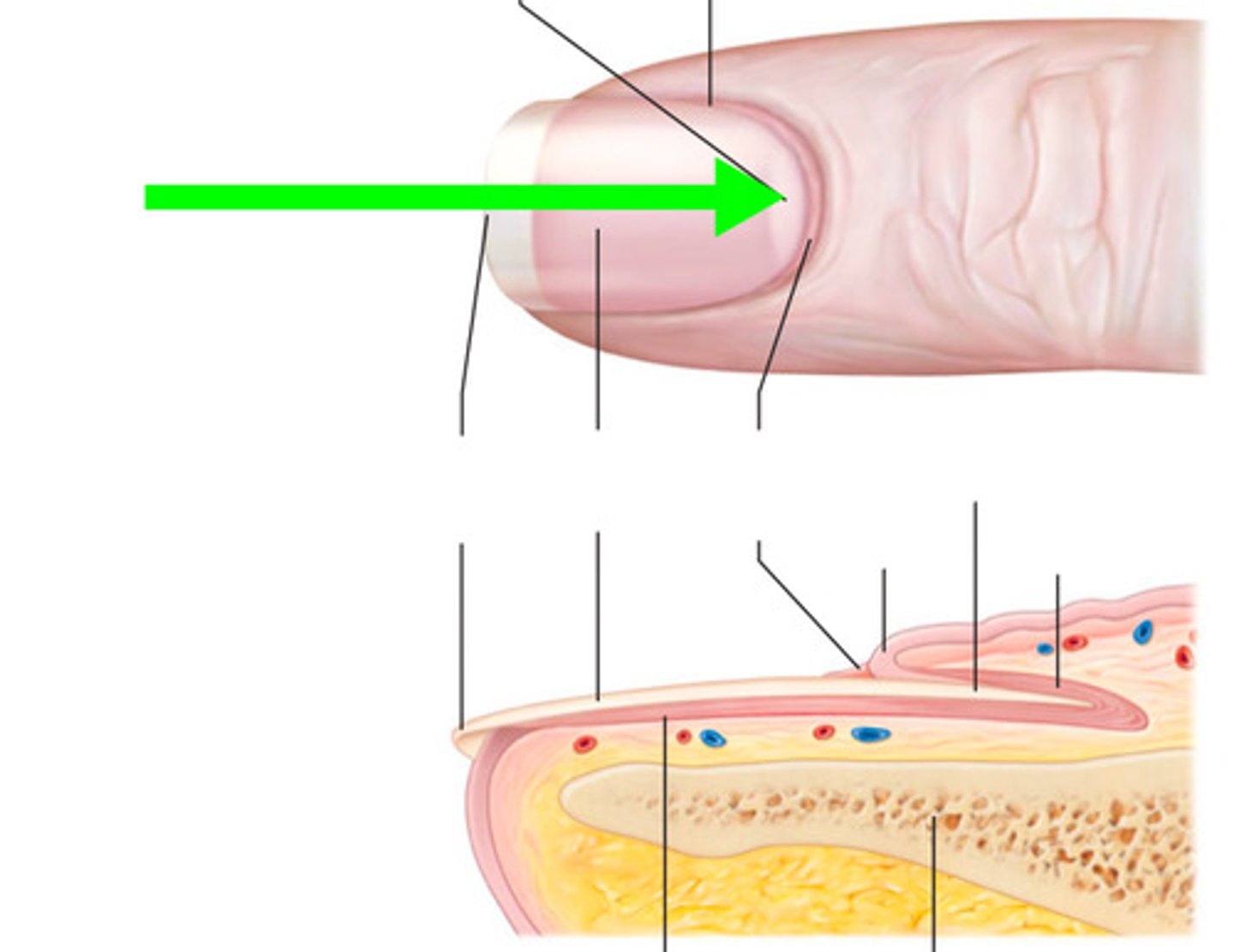
What is the Lunule used to check?
Used for visual check of oxygen status in patients

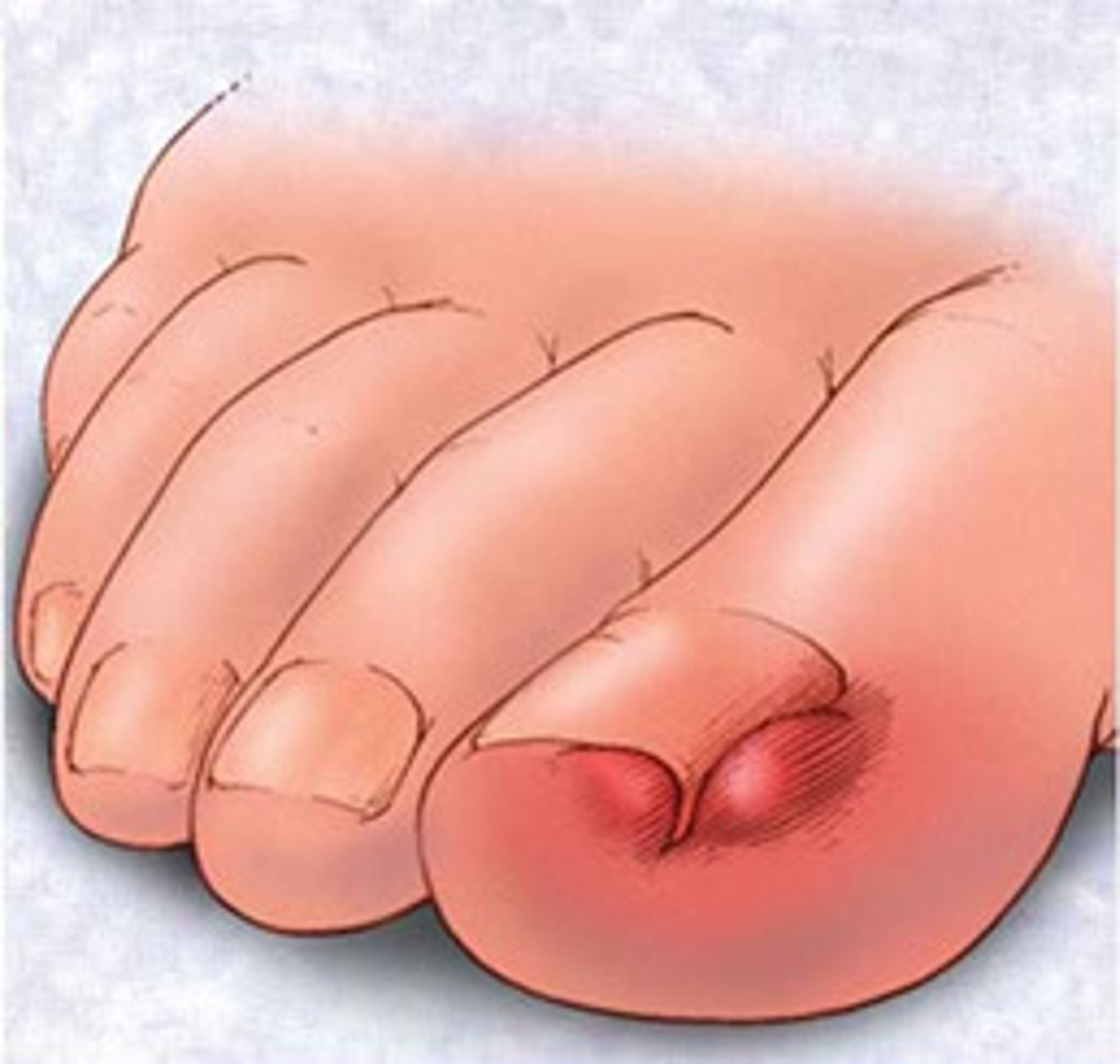
Eponychiitis
Ingrown toenail
6 Clinical applications of the integumentary system:
Injection sites,
Blisters,
Lines of cleavage,
Decubitus ulcers (bed sores),
Burns,
Skin Cancer

Injection sites
Intradermal (ID)
Subcutaneous (SQ)
Intramuscular (IM)
Intravenous (IV)
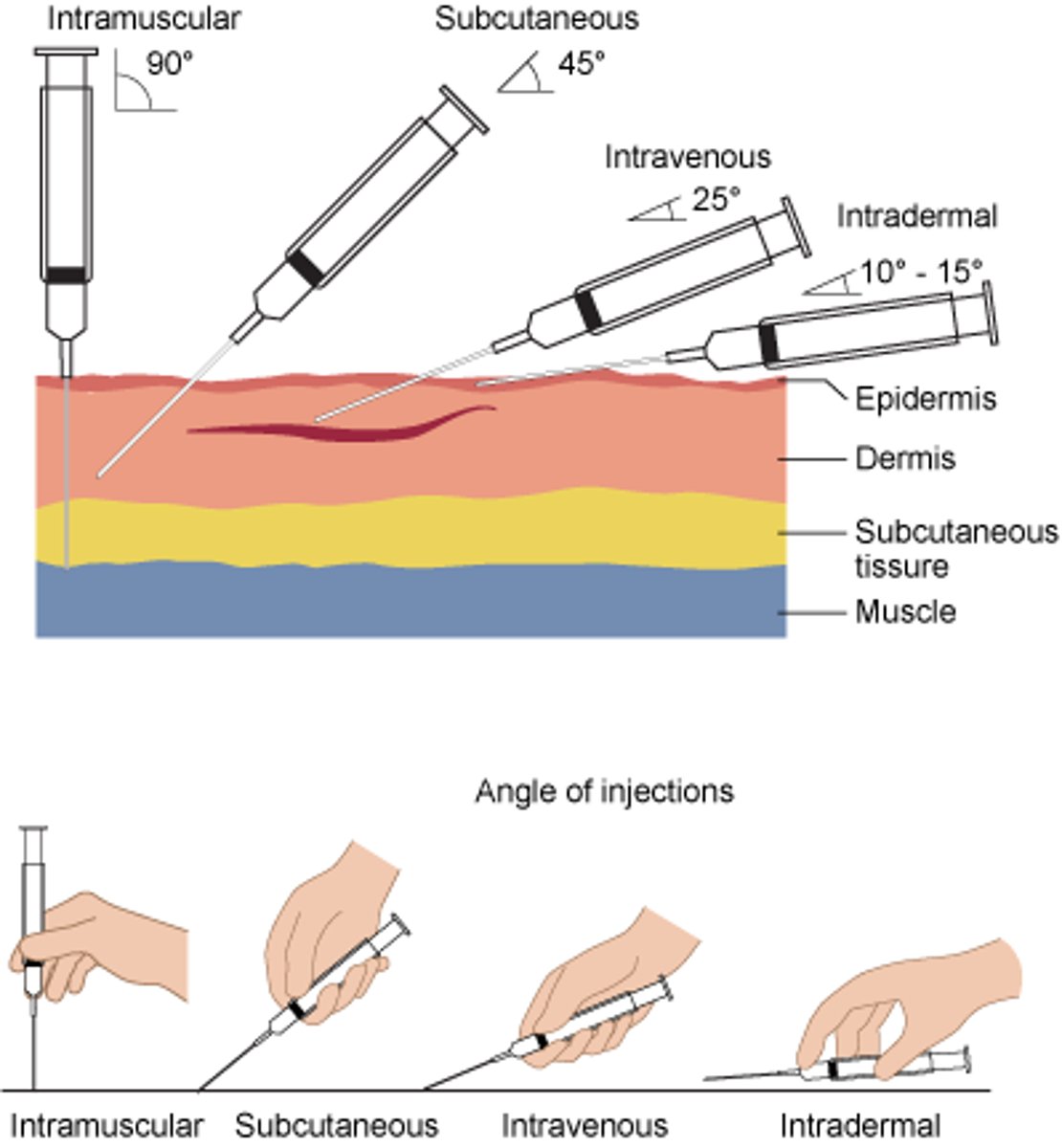
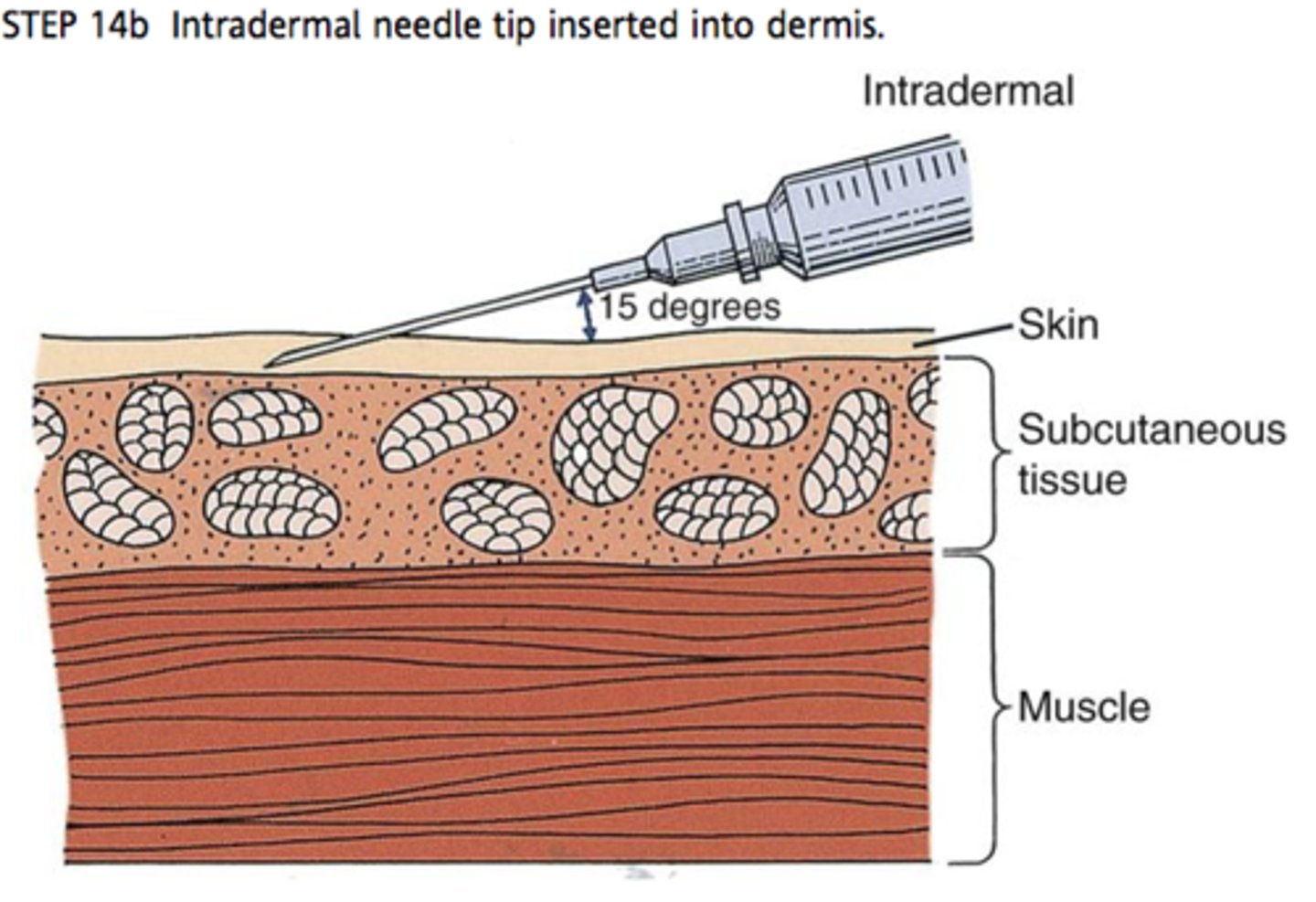
Intradermal (ID)
Injection between epidermis and nervous
ex) TB test
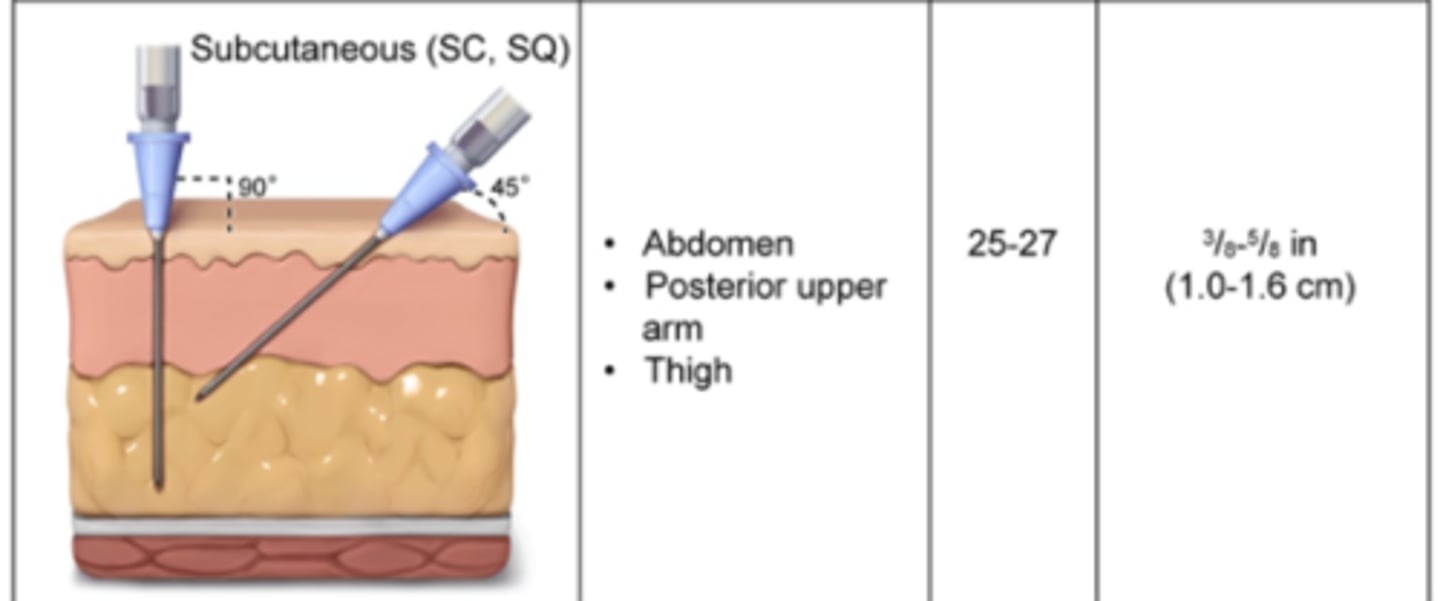
Subcutaneous (SQ)
Injection in the hypodermis
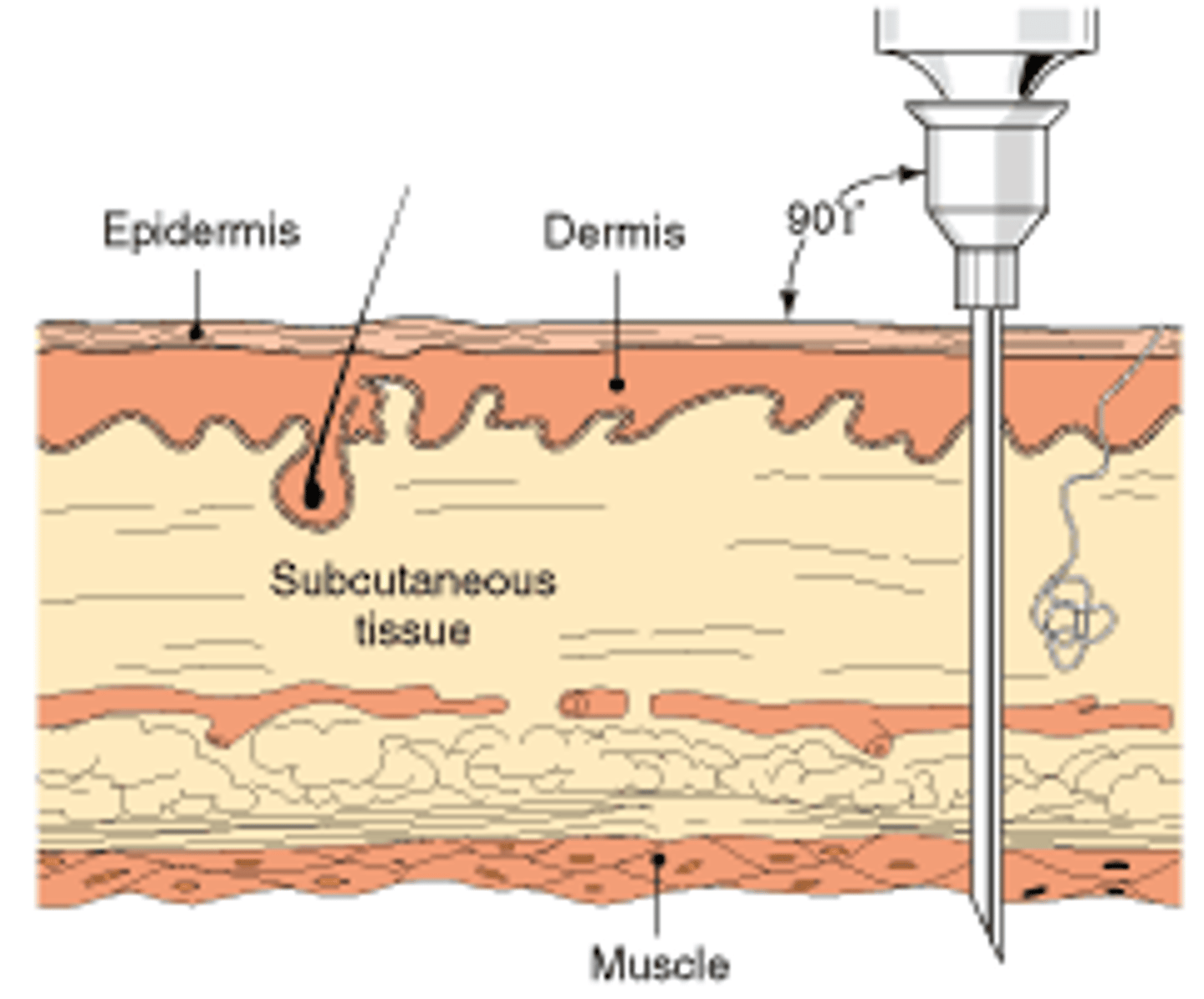
Intramuscular (IM)
Injection into the muscle
Intravenous (IV)
Injection into vein
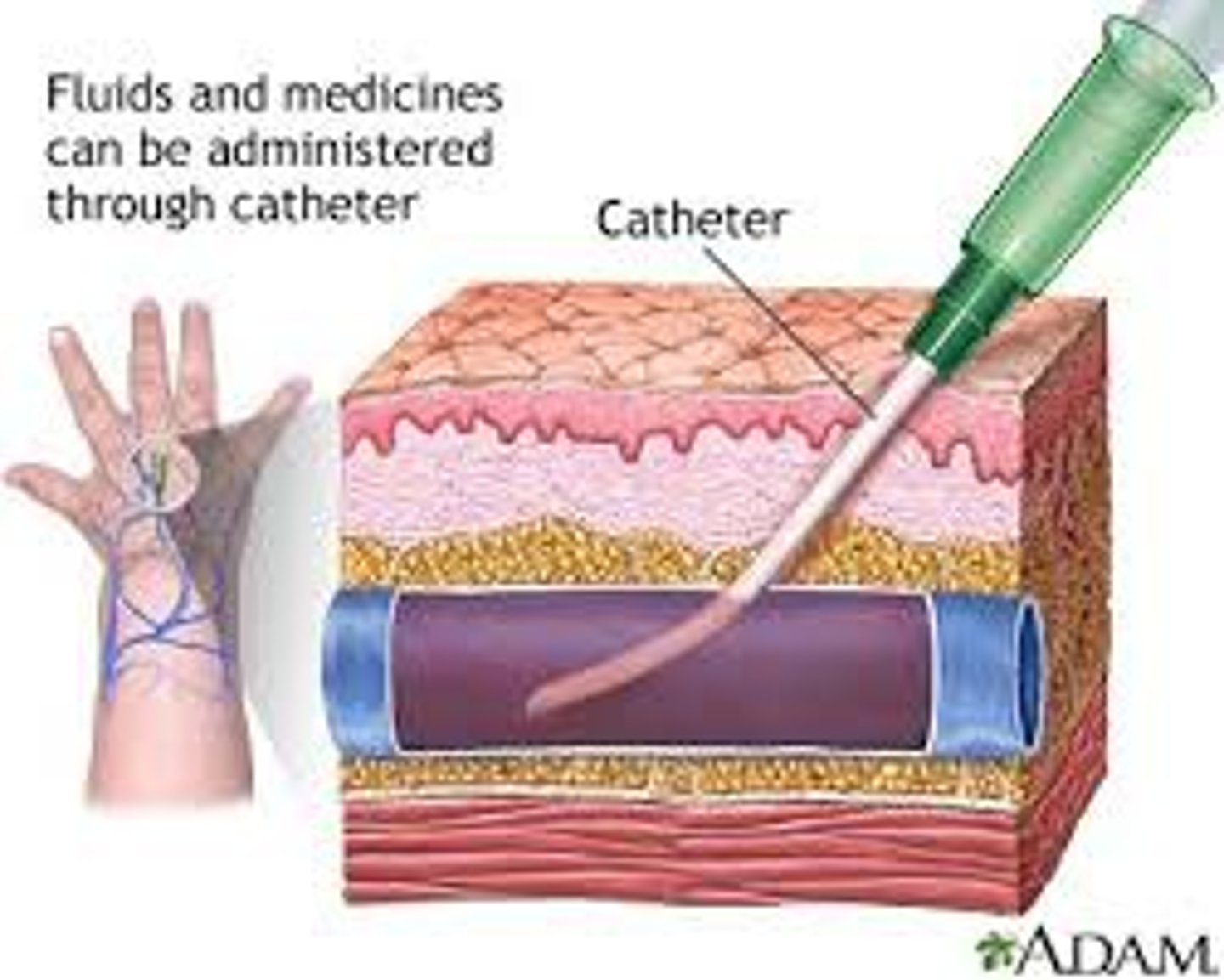
Blisters
Fluid-filled pocket between epidermis and dermis
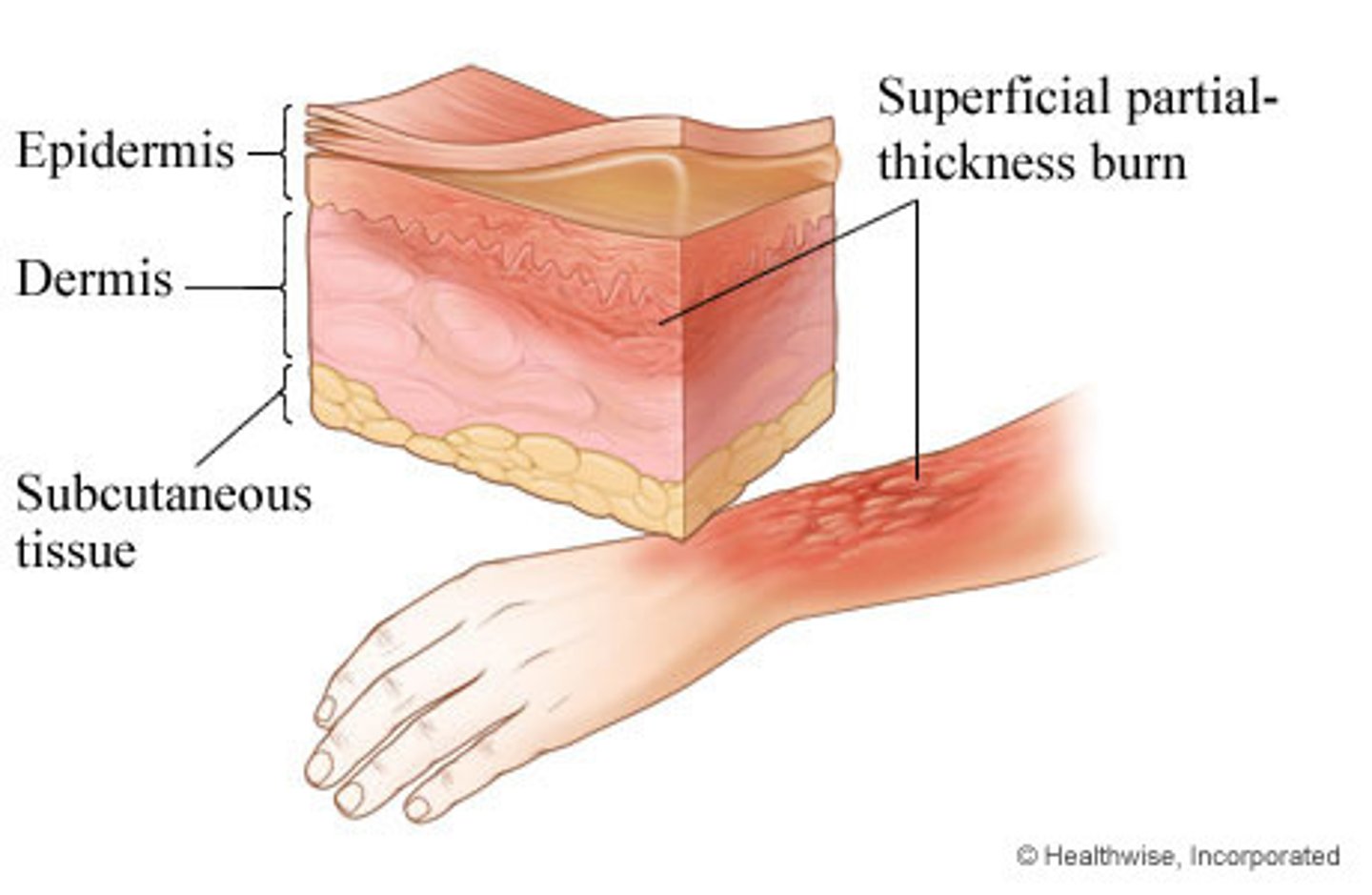
Lines of Cleavage
Formed by uniform alignment of collagen and elastic fibers

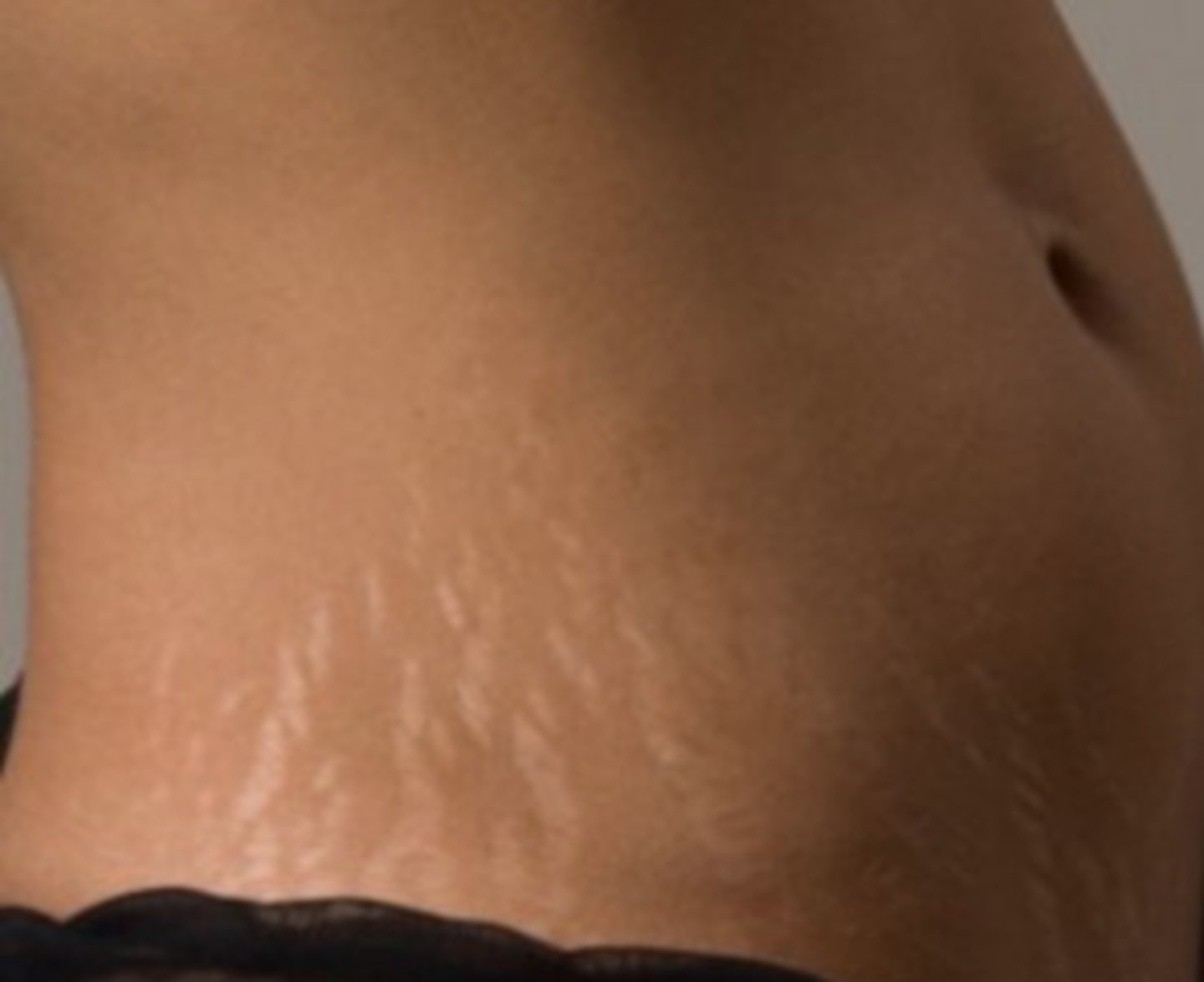
Stretch Marks
Formed by stretching collagen fibers beyond the point of repair
Decubitus ulcers (bed sores)
1)Blood Supply Restricted -> Ischemia (oxygen reduced) -> necrosis (tissue death),
2)Bacterial infections result, difficult to heal, secondary intention
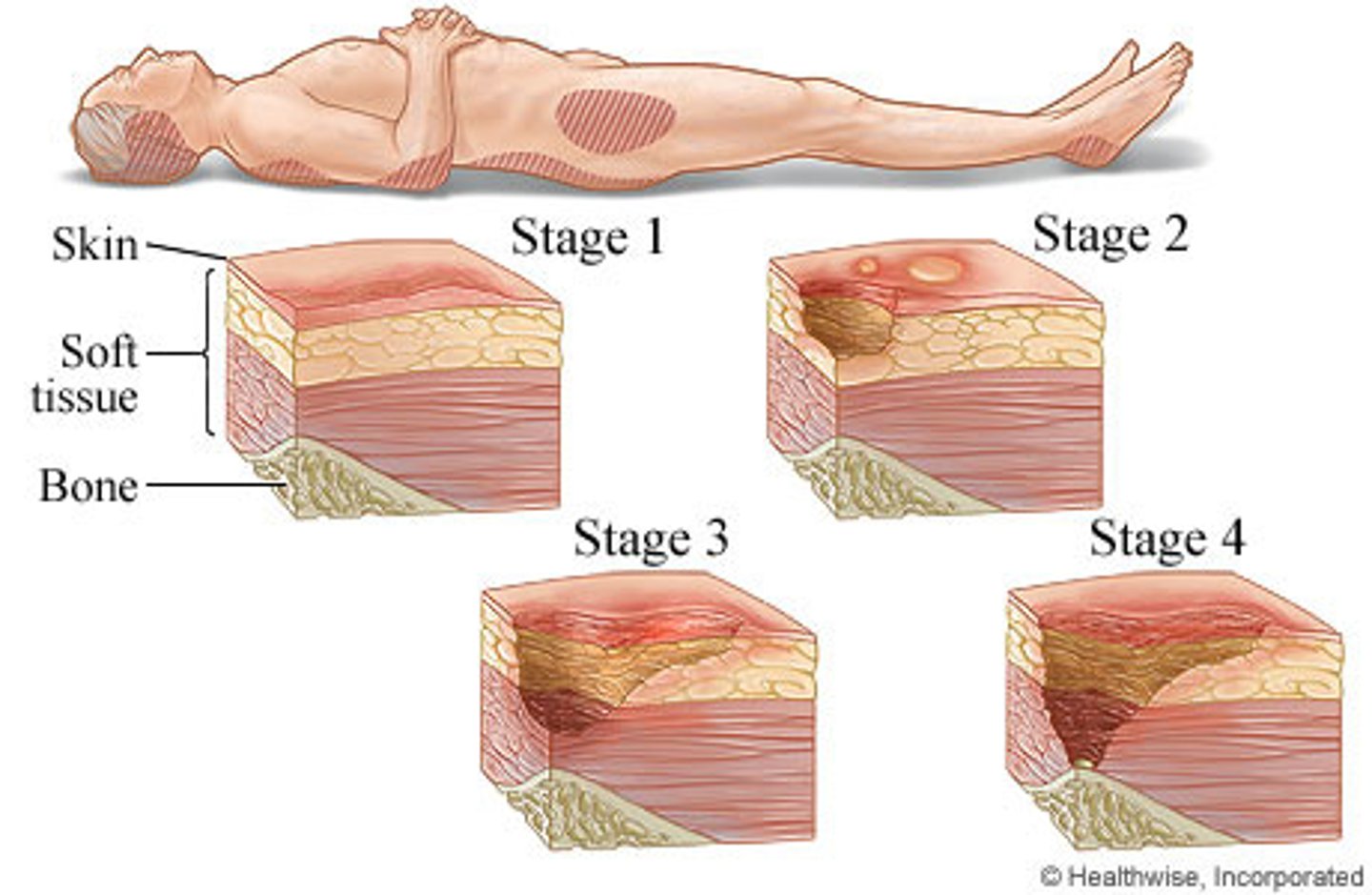
How decubitus ulcers form:
Blood Supply Restricted -> Ischemia (oxygen reduced) -> necrosis (tissue death)
** Like pinching a garden hose, the nutrients cannot get to the skin from having weight constantly on a bony part of body without padding. The open wound causes bacteria to get in.

What areas are at higher risk for Decubitus ulcers?
The least padded areas (elbow, heels, backbone)
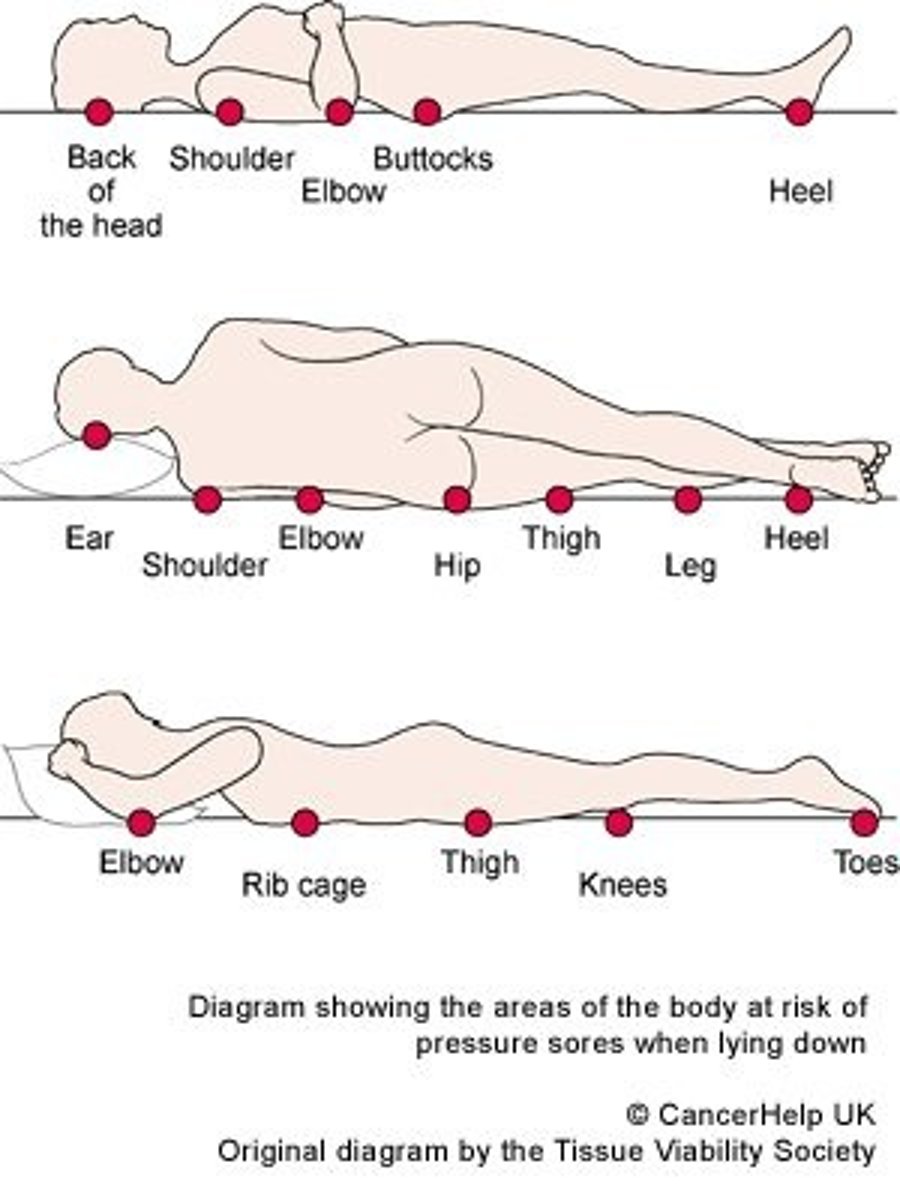
What patients are high risk for Decubitus ulcers?
Elderly in care homes (less body fat for padding)

How can decubitus ulcers be prevented?
Rotating patient positions,
Artificial padding,
Clean bedding
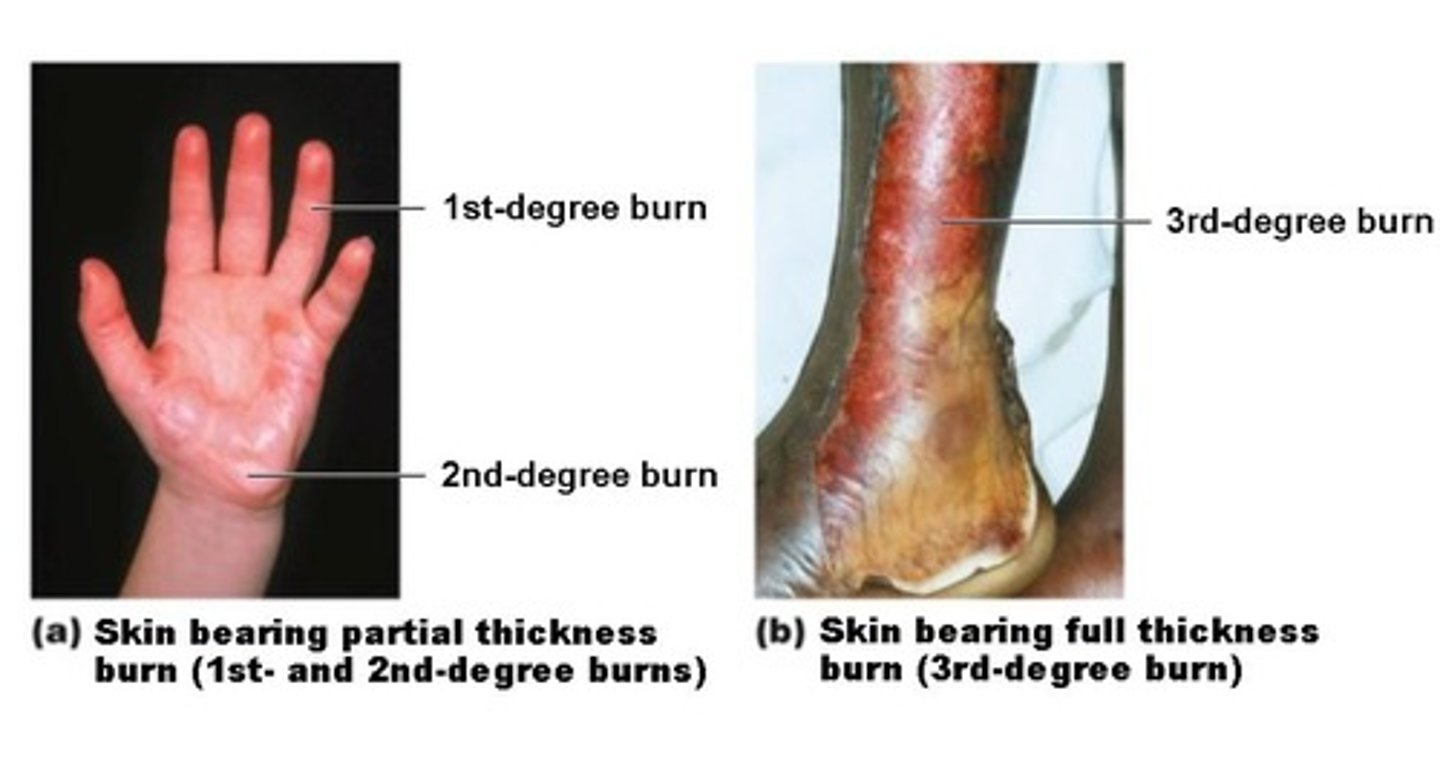
Burns
Tissue damage inflicted by heat, electricity, UV radiation, or chemicals that denature proteins and cause cell death in affected areas
Associated dangers of burns (RICED)
Renal failure,
Infection (sepsis),
Circulatory shock,
Electrolyte imbalance,
Dehydration

Burn dangers: Catastrophic loss of body fluids can lead to:
Dehydration,
Electrolyte imbalance,
Renal Failure,
Circulatory shock
(DERC)
Sepsis
Widespread bacterial infection
Leading cause of death in burn victims:
Sepsis
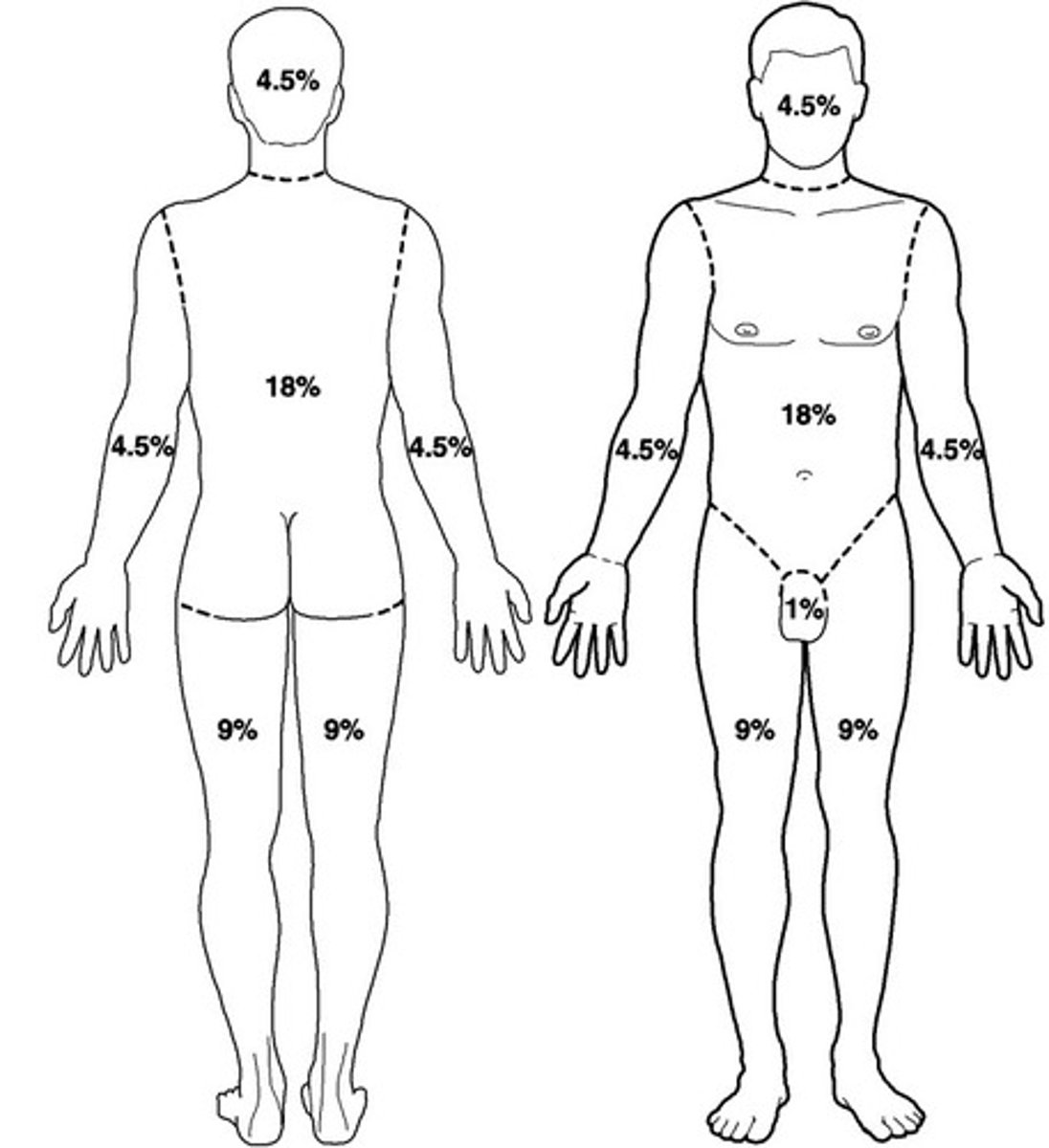
Rules of Nine
Way to approximate the extent of burns,
Special tables are used when greater accuracy is desired
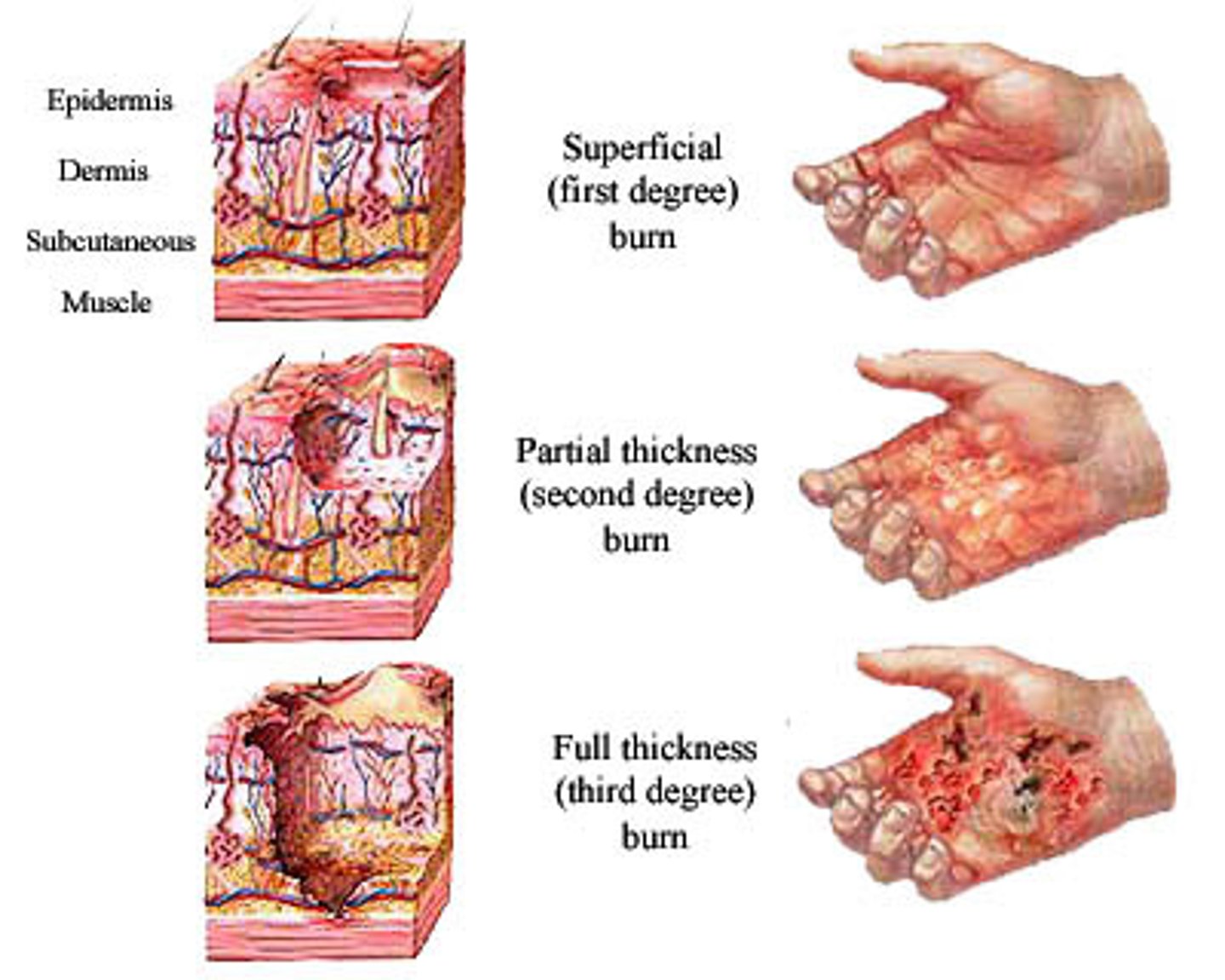
Severity of burns
1st degree
2nd degree
3rd degree