Hearing Science Exam 2
1/79
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
80 Terms
Outer ear Helps
Funnel sound & localization
Parts of the Outer Ear
lobule
tragus
cavum concha
crus of helix
triangular fossa
helix
scaphoid fossa
superior crus of antihelix
inferior crus of antihelix
cymba concha
antihelix
EAM
antitragus
Ear canal
1/3 cartilage; makes ear wax
2/3 osseous: isthmus
Outer ear function
sound transmission
Middle ear protection
major resonator
sound localization
resonance & diffraction
Azimuth Estimation
determination of the direction of the horizontal plane
binaural
Elevation estimation
determination of the direction of the vertical plane
monaural
distance estimation
determination of how far we are away from a sound source
atresia
no ear canal
anotia
no pinna & ear canalM
Microtia
malformed pinna
cauliflower ear
swelling of pinna due to trauma
external otis
swimmers ear
infection
exostoses
bony growth on ear canal
Middle ear function
convert air based sound into mechanical energy into the inner ear
parts of inner ear
tympanic membrane
ossicles
eustachian tube
Tympanic membrane
lateral process manubrium (of mallues)
umbo
cone of light
pars tensa
pars flaccida
tympanosclerosis
scarring on the TM due to ear infection, tubes, ruptures
anatomy of ear canal
cartilaginous portion
bone portion
isthmus: narrow area where it moves from cartilage to bone
ear wax
open-closed tube amplifying sound: 2000-5000hz
Amplification of sound
8 dB
Sound movement
pinna (acoustical)
EAC
tympanic membrane (mechanical)
ossicles; malleus, incus, stapes
oval window (hydraulic)
scala vestibuli
basilar membrane
cochlear hair cells
IHC (electrical)
afferent neuron
auditory nerve
Azimuth Estimation
along horizontal plane
binaural
Elevation Estimation
Vertical plane
monaural
Distance estimation
how far we are from the sound source
includes sound intensity & amount of sound refelcted
2 localization cues
interaural time difference
interaural level difference
Interaural time difference
sound gets to one ear faster than the other, helps you know where the sound is coming from based on this timing
Interaural level difference
based on the shadow your head makes which affects the sound waves, some sounds will be louder to one ear than another
Monaural Cues
help us estimate the elevation (vertical plane) of incoming sound
reflected path vs direct path used to tell you how high a sound is coming from
Degree for best noise
45 degrees
2 main functions of outer ear
funnel sound/ sound transmission
localization
protection of the inner ear
Middle ear disorders
mastoiditis
cholesteatoma
mastoidectomy
otitis media
Mastoiditis
infection of mastoid hair cells
Cholesteatoma
tympanic membrane majorly contracted, problem w/ eustachian tube
cyst with skin cells
non-cancerous growth of skin-like cells in the middle ear
Mastoidectomy
removal of mastoid air cells
Otitis Media
infection of middle ear
4 steps of middle ear infection
inflammation leading to the narrowing of eustachian tube
increase in neg pressure
mucus excretions lead to bacterial colonization
bacteria buildup & pus
inner ear hearing loss
Sensorineural
conductive
Sensorineural
through air and the outer/ middle earCo
Conductive hearing loss
bone conduction
presbycusis
acoustic trauma, drugs, age, infection, congenital
impedance
moving from air-filled space to fluid causes an impedance mismatch of 4000
fixes of impedance
difference in surface area
ossicular lever
buckling effect
Differences in surface area
TM is larger than oval window, so force becomes more focused and thus more powerful
Ossicular lever
rotational motion at the incudomallear joint due to the ligaments attaching to malleus and the incus
increase force by 1.2dB or 1.5 times
Buckling effect
aka catenary lever
conical shape of the tympanic membrane means less movement with vibration and thus more force at the oval window
increase by 6 dB
Area Ratio : pressure transformer
increase energy by 17 fold
ratio of tympanic membrane area compared to the footplate of the stapes area
acoustic reflex
tensor tympani and stapedius will contract and stiffen the ossicular chain
basilar membrane
wider at apex
high frequencies resonate at base
sound enters scala vestibuli
sound waves within the cochlea are transverse
Modiolus
part of cochlea
bony axis of cochlea
osseous cavity where all spiral ganglion and nerve endings from the organ of corti join together to create the auditory nerve
provides structure for cochlea
Frequency
The basilar membrane is tonotopically organized, meaning there are areas that resonate with specific frequencies. The base of the membrane is more geared towards higher frequencies because it is stiffer and the apex is more geared to higher frequencies because it is less stiff.
Intensity
is processed by the outer hair cells, more energy and “loudness” is going to mean it is more intense.
Duration and timing:
how long the sound is and when the sound happens, the length of the vibration indicates how long the duration of the sound is.
IHC Shearing
shear away from modiolus towards longer stereocilia
open ion gates where potassium comes in = depolarization
calcium opens side gates
OHC Shearing
shear against tectorial membrane
depolarization
when positive potassium ions enter the cell
stereocilia are sheared away from the modiolus
Hyperpolarization
membrane potential of the cell becomes/ stays more negative
stereocilia are sheared towards the modiolus
Type 1 Afferent Neurons
95%
covered in myelin and connected to IHC’s
20 type 1 afferent for each IHC
Type II
5%
thinner
not covered in myelin connected to OHC’s
attached to multiple outer hair cells
Spiral Ganglion
group of afferent neurons within modiolus
Endolymph
high in potassium
positive charge
scala media
Perilymph
high in sodium
positive charge
scala tympani / vestibuli
Fluid & depolarization
As the stereocilia shear, the potassium from the endolymph flows into the cell, causing a chain reaction that leads to action potentials – the electrochemical responses to sound
OHC depolarization
basilar membrane move up
tectorial membrane moves up
sterocilia get moved and ion gates open
potassium enters and depolarizes the cell
sharpens frequency codes
results in electromotility
Cochlear amplifier
depolarization of OHC (electromolity)
It matters because less IHC will be stimulated (sharp), but the IHCs that are stimulated and stimulated more (tallness). Sounds are clear like we want them.
When the OHC’s are damaged, sounds are muffled.
Place Theory
frequency is coded by place stimulation along cochlea/ basilar membrane
physiologcial principle: based on stiffness and width of the basilar membrane
Each IHC & OHC tuned to a specific frequnecy
Characteristic frequnecy
each IHC & OHC is tuned to a specific frequency
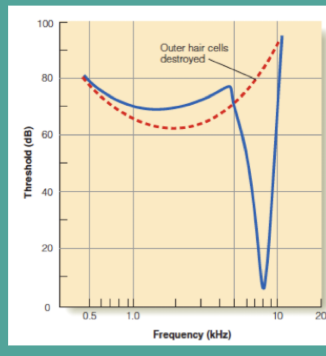
blue line: normal functioning , 8,000hz
red: no response to frequency, impaired hearing. Takes a lot more dB to stimulate and loss of characteristic frequency, muffled speech
Temporal Theory
basic premise: frequency is coded by the frequency of nerve impulses generated by the incoming sound
Psychological Premise: all auditory neurons have a resting firing rate. the firing rate increases when IHC’s are excited and decreased when IHC’s are inhibited
can’t account for higher frequencies
Volley Principle
group of neurons that work together help hearing up to 5k Hz
frequency is coded by the frequency of nerve impulses generated by the incoming sound
individual auditory neurons can only fire up to 1000 Hz
neuron groups work as teams to code higher frequency
Frequency Coding
Place theory + Temporal Theory
Intensity Cody
coded by number and type of activated neurons
Dynamic range
the intensity range between a neuron's threshold and saturation point. Most often between 24 and 40 dB.
Physiological principle
greater intensity = larger amplitude & broader traveling
this stimulates larger population of IHC and auditory neurons
3 types with different firing rates
(high spontaneous, mid spontaneous, low spontaneous)
Low Intensity = high spontaneous
High Intensity = Low spontaneous
Cochlear Implant
cochlear implant applies direct stimulation to the auditory nerve with electrical signals In
Intensity Coding
rate of electrode firing
Air
travels through outer/ middle/ inner ear to get to cochlea
50-60 dB better than bone conduction
Bone
vibrations of skull stimulate cochlea
bypass outer/ middle ear ; hearing
Bone conduction: own voice
vibrations of skull from high pressure sounds produced when speaking that lead to hearing via bone conduction
Direct Vibrations: bone conduction
vibrations to skull that go straight to cochlea, mechanical energy directly to the cochlea
bone conduction: high intensity
difference with bone and air conduction, bone conduction is less efficient by 50-60 dB
conductive hearing loss: measure
seeing if the bone conduction ratings are better than the air conduction hearing test