Grade 12 Kinesiology - Unit 1 Test Review
1/120
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
121 Terms
5 Types of Bones + example of each
Long bones (e.g. femur)
Short bones (e.g. carpals)
Flat bones (e.g. skull)
Irregular bones (e.g. vertebrae)
Sesamoid bones (e.g. patella)
Appendicular vs Axial Skeleton
appendicular: bones of the limbs
axial: skull, vertebrae, ribs, sternum
Does the appendicular or axial skeleton allow for more movement?
appendicular
Compact Bone vs Cancellous Bone
compact: thick part of the bone, responsible for structural integrity
cancellous: filled with marrow in its cavities, responsible for shock absorption
Epiphyseal Plate vs Epiphyseal Line
epiphyseal plate: “growth plates,” occur at various locations in the epiphysis
epiphyseal line: occurs when epiphyseal plates have fused together after growth has stopped
Epiphysis
ends of long bones
Diaphysis
shaft of long bones
Articulating Cartilage
located on both ends of bone
allows for smooth movement while protecting the ends of the bones
Cartilage does not have any _____ supply or _____ endings. _____ supply is crucial to heal properly.
blood, nerve, blood
How can you know if a bone has stopped growing?
if you take an x-ray and you can see their epiphyseal line (means epiphyseal plates have fused and growth has stopped)
How does compact bone form?
begins as cartilage
osteoblasts deposit osteoid into the cartilage
inorganic salts are deposited into the osteoid
osteoid hardens creating the bone
How does cancellous bone form?
begins as fibrous membranes
osteoblasts release osteoid into the membranes which forms a sponge-like bundle of fibres
cancellous bone formation develops outwards from these centres in the membrane
Osteocytes
bone cells
Osteoblasts
bone forming cells
Osteoclasts
bone-destroying cells
Ossification
production of new bone
Ossification Centers/Epiphyseal Plates
places where growth of bone occurs
Bone Remodelling
further development of the bone in which it is continuously created and destroyed
process is most active during the early years of human growth
Remodeling of bone begins to decline at around age __.
35
After 40, there is about a _-__% loss of bone mass per decade of life.
5-10%
How do Bones Heal?
same way when bone is growing
callus is formed at the site of the break, which forms a new true bone as strong (or even stronger) than the one before it
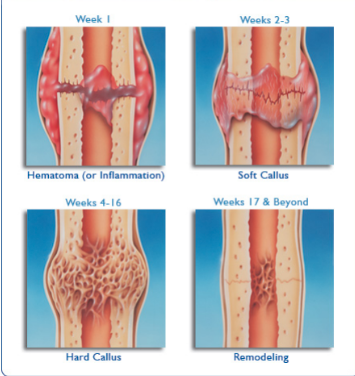
Stages of Bone Healing
Hematoma (swelling with blood)
Soft callus formed
Hard callus formed
Remodelling (old bone tissue is absorbed and replaced with new bone tissue)
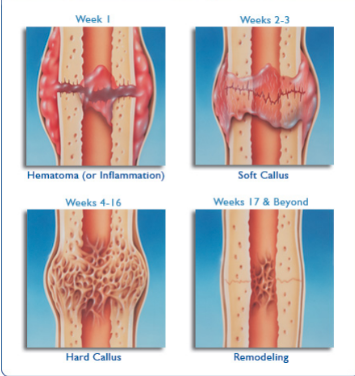
Callus
temporary structure that forms when a bone is healing from a break
3 Types of Muscle Tissue
Smooth muscle
Cardiac muscle
Skeletal muscle
Smooth Muscle
surround internal organs
contract slowly
involuntary
fatigue resistant
have spindle shaped fibres
are arranged in dense sheets
Cardiac Muscle
only found in the heart
involuntary
very fatigue resistant
striated (striped) fibers
arranged in layers
Skeletal Muscle
striated (striped) in form
not fatigue resistant
voluntary
Skeletal muscle is also known as ________ muscle.
striated
Antagonistic Muscles
pairs of opposing muscles that perform the exact opposite movement of each other, composed of:
Agonist - prime mover (for that specific movement)
Antagonist - opposing mover
e.g. biceps brachii and triceps brachii are an antagonistic muscle pair
Stabilizers
muscles that provide support to hold a joint in place so antagonistic muscle pairs can perform movements
Tendon
connect muscle to bone
Ligament
connect bone to bone
Sensory vs Motor Pathways
sensory: collect info from sensors throughout the body + transmits that info to the brain
motor: conduct signals to activate muscle contractions for movement
All-or-None Principle
all the muscle fibres in a motor unit need to pass the threshold (of enough acetylcholine/electrical charge) for the contraction to happen
when a motor unit is stimulated to contract, it will do so to its fullest potential every single time.
there is either a full contraction or NO CONTRACTION AT ALL
Central Nervous System (CNS)
brain + spinal cord
Peripheral Nervous System (PNS)
sensory + motor pathways
Muscle Twitch
single nerve impulse + the resulting contraction
True or False: one motor neuron may be responsible for stimulating several muscle fibres.
True
Motor Unit
a group of muscle fibres that are contracted via the same motor neuron
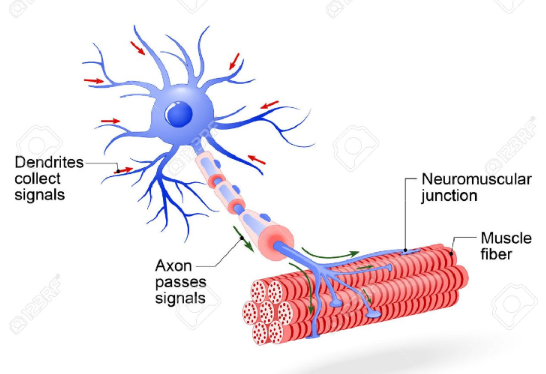
All muscle fibres of one motor unit are always the ____ muscle type.
same
Muscles needed to perform precise movements generally consist of ____ motor units and a ___ muscle fibres.
many, few
Muscles needed to perform less precise movements are carried out by muscles of _____ motor units with ____ fibres per unit.
fewer, many
The Neuromuscular Junction
has the:
axon
axon terminal
synaptic cleft
receptor
neurotransmitter (acetylcholine)
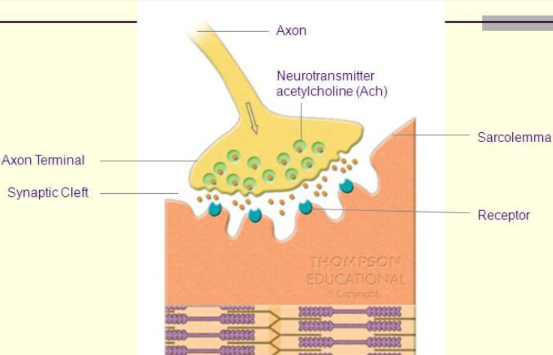
Axon
carries nerve signal
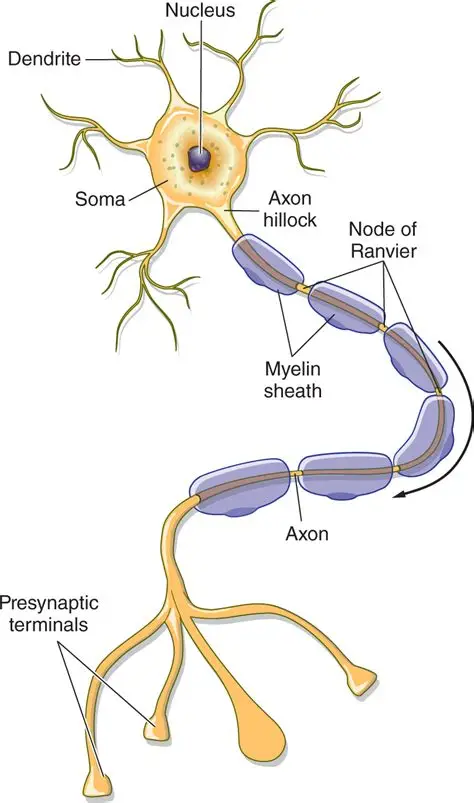
Axon Terminal
where the nerve and muscle meet
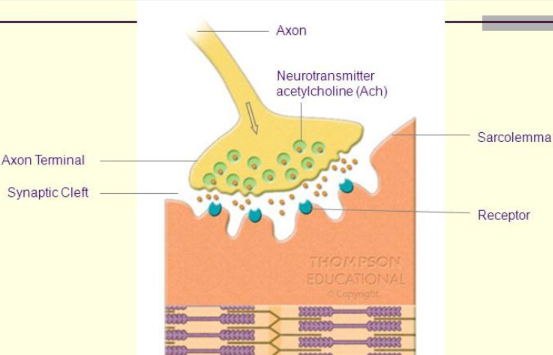
What is the neurotransmitter used for muscle contractions?
acetylcholine
Dendrite
receives signals
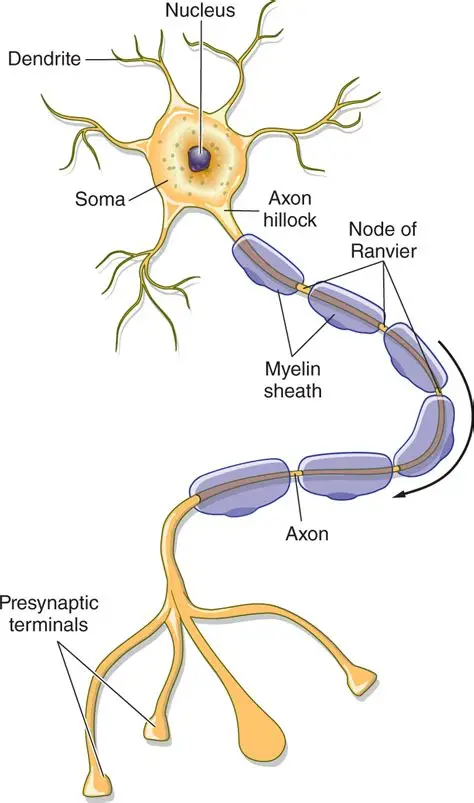
Summary of Muscle Contraction (sliding filament theory)
signal from brain/spinal cord
electrical impulse sent along neurons down the axon
signal reaches motor unit
signal moves through dendrite + axon towards axon terminal
signal triggers vesicles containing NT acetylcholine to release NT across synaptic cleft
acetylcholine binds with receptors on muscle
binding with receptors triggers calcium to be released by sarcoplasmic reticulum
calcium binds to troponin found on actin
causes tropomyosin to move, exposing myosin binding sites
myosin heads have ATP bonded, which break down to ADP + Pi, causing myosin heads to move and bind with binding sites on actin
cross bridges have formed
myosin moves the actin, "shortening the muscle”
another ATP is used to break the cross bridge between actin + myosin
(so long as calcium is bonded) contraction continues
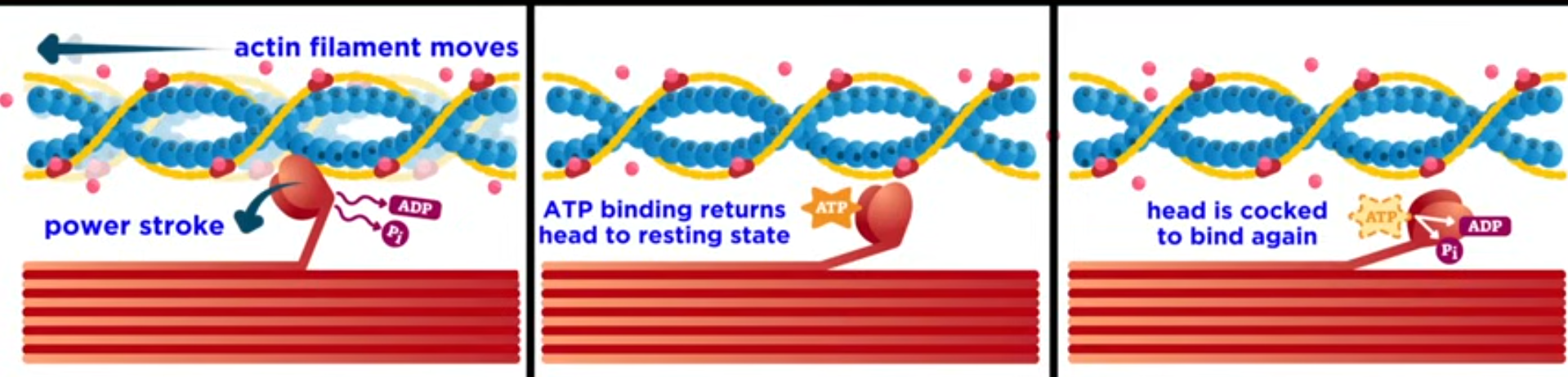
Concentric Contractions
muscle fibres shorten
Eccentric Contractions
muscle fibres lengthen
Isometric Contraction
muscle fibres do not change in length
Isotonic Exercise
controlled shortening + lengthening of the muscle
Isometric Exercise
muscle fibres maintain a constant length and there is no motion
Isokinetic Exercise
using machines to control the speed of contractions
Epimysium
sheath enveloping entire muscle
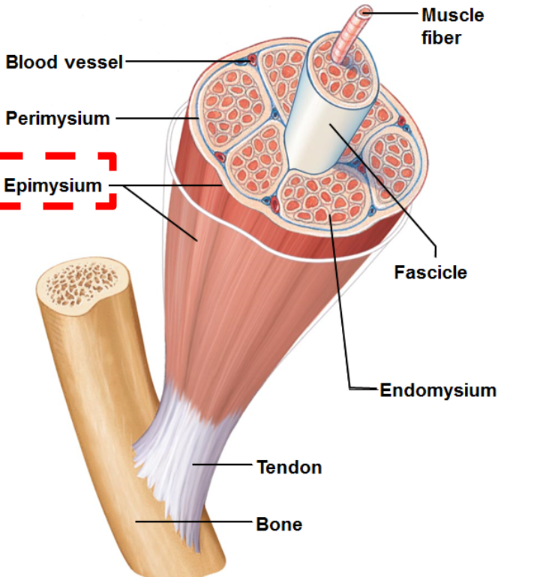
Perimysium
sheath of connective tissue that covers fascicle
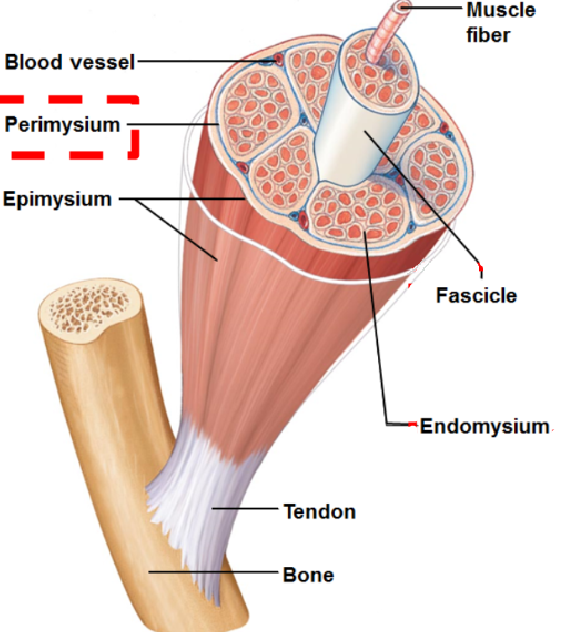
Fasicle
bundle of muscle fibres
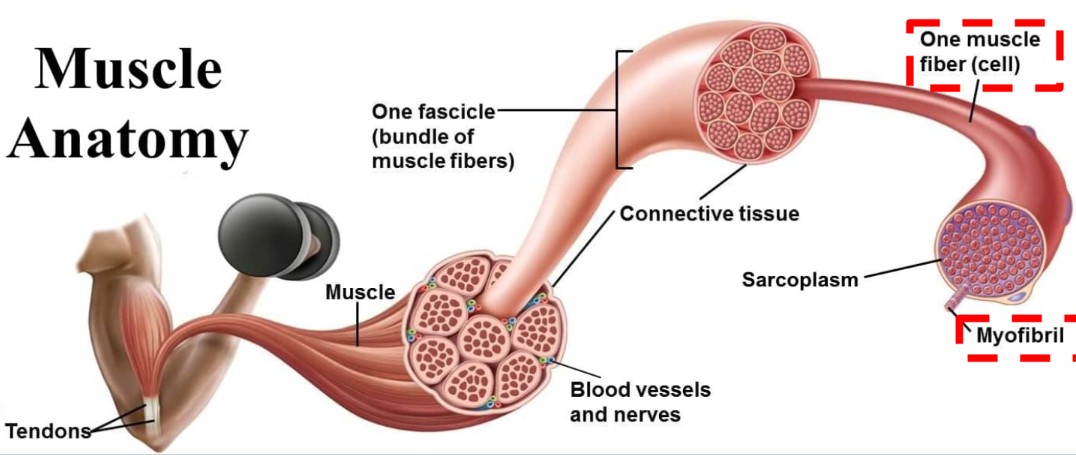
Endomysium
sheath of connective tissue surrounding each individual muscle fibre
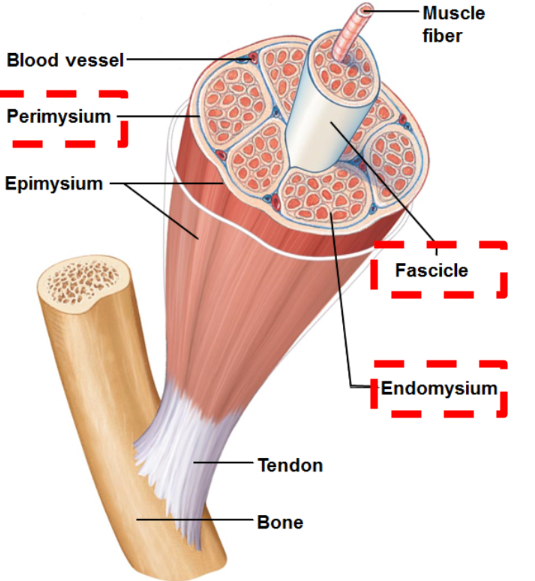
Myofibrils
make up the muscle fibres
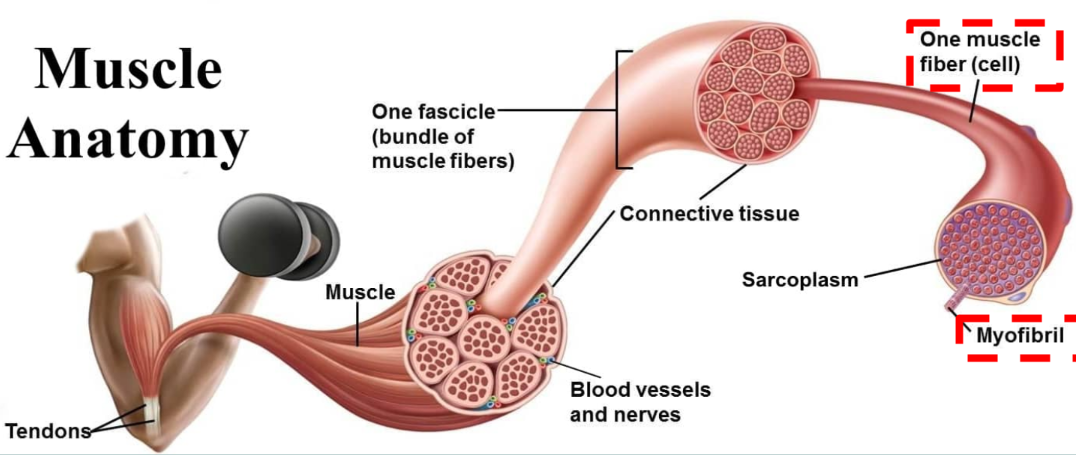
Sarcolemma
muscle membrane
beneath the endomysium
contains the muscle fibre’s cytoplasm (sarcoplasm)
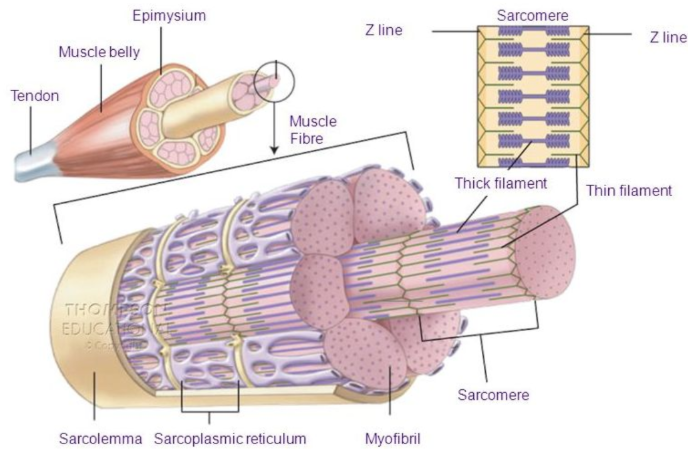
Sarcoplasm
muscle fibre’s cytoplasm
in the sarcolemma
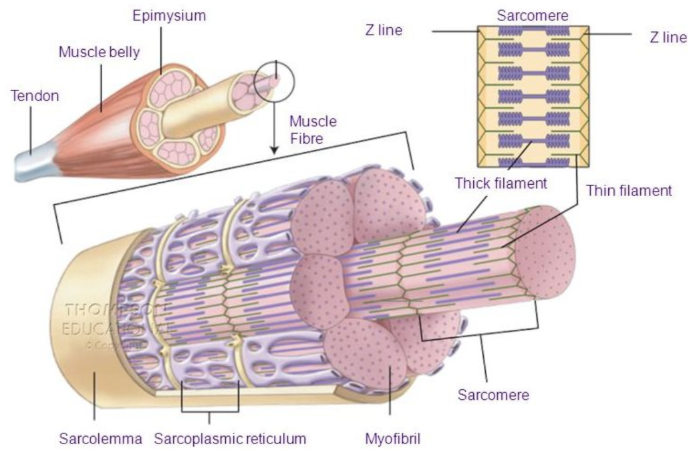
Sarcomeres
repeating units of skeletal muscle that contain actin and myosin
makes up a myofibril
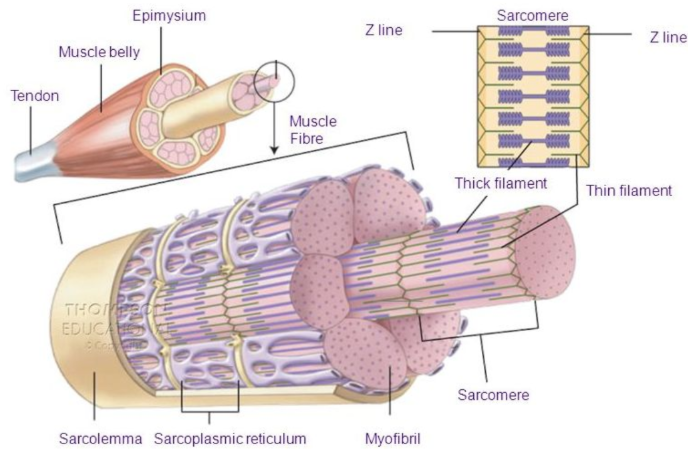
Sarcoplasmic Reticulum
network of web-like structures that run up and down the sarcomeres providing calcium for muscle contraction
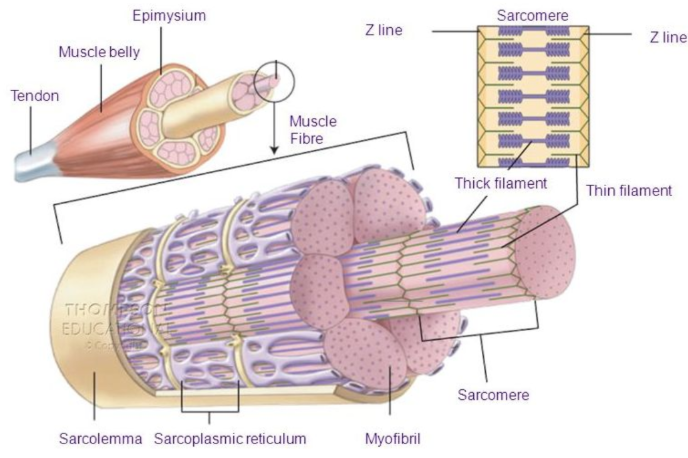
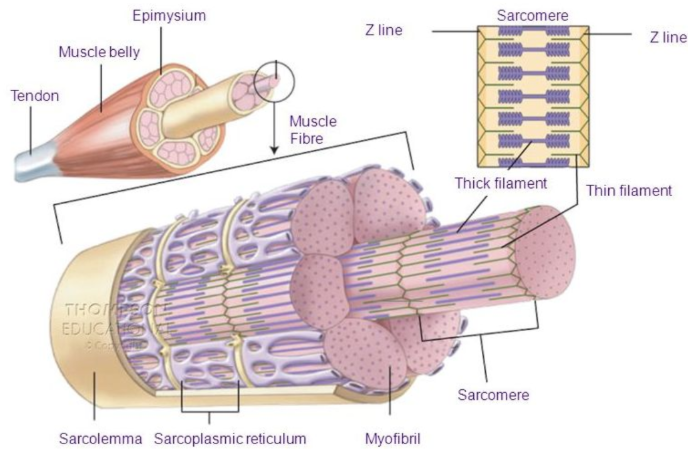
Summary of Anatomy of Skeletal Muscle
(superficial → deep)
epimysium
perimysium
endomysium
muscle fibre
sarcolemma
sarcoplasmic reticulum
myofibrils → sarcomeres
actin/myosin
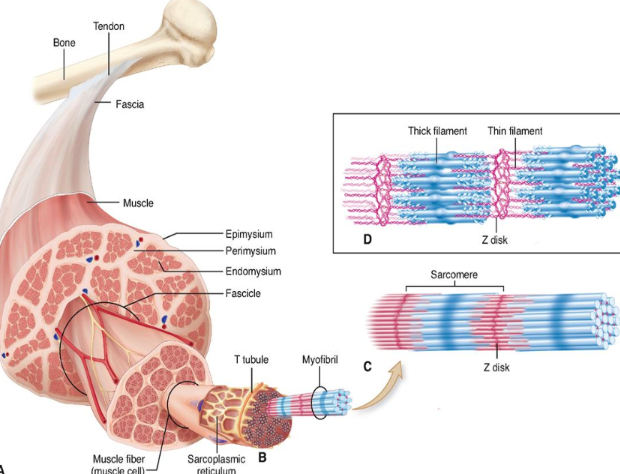
Myosin and Actin
thick and thin protein filaments (respectively) within the myofibrils
make up the muscle fibres at a cellular level
Myosin
made up of a “head” and a “tail” and looks like a golf club
head is attachment site for actin
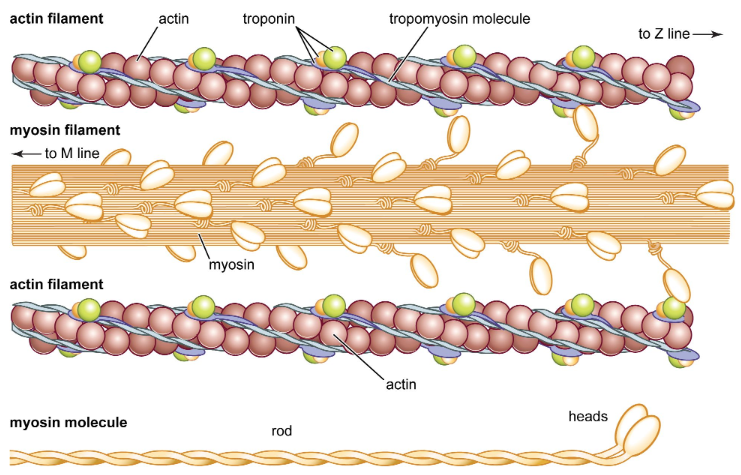
Actin
has 2 proteins: troponin + tropomyosin
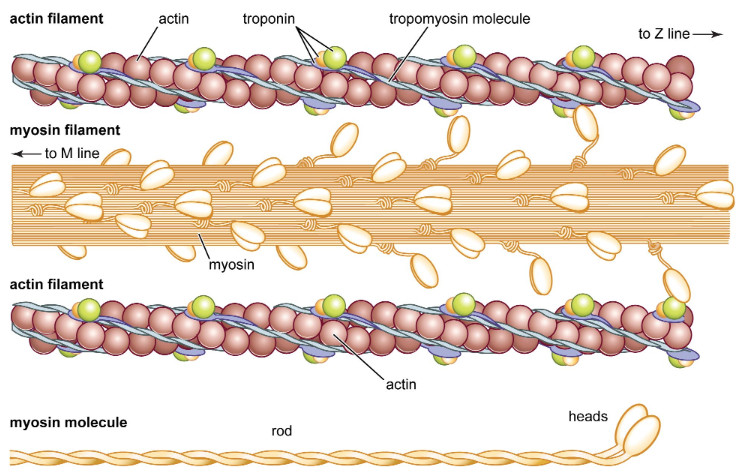
Troponin vs Tropomyosin
troponin: has binding site for calcium
tropomyosin: “stringy-looking” cord-like structure that covers the binding site for actin
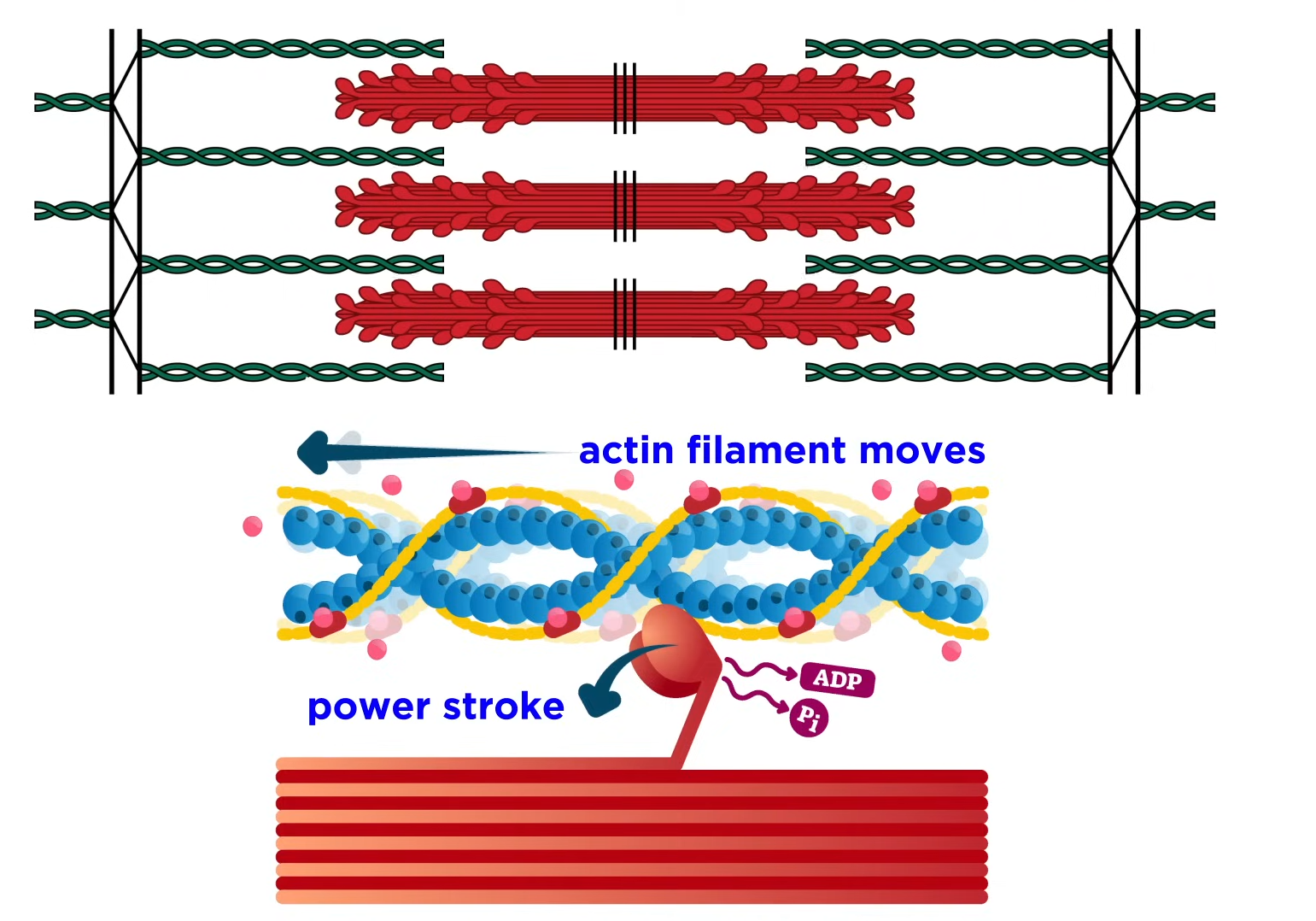
When a muscle is relaxed, ___________ in actin covers the binding site (preventing myosin from latching on). To contract the muscle, _______ needs to be released to bind to ________, which removes ___________ from the binding sites, allowing myosin to latch on and pull the actin.
tropomyosin, calcium, troponin, tropomyosin
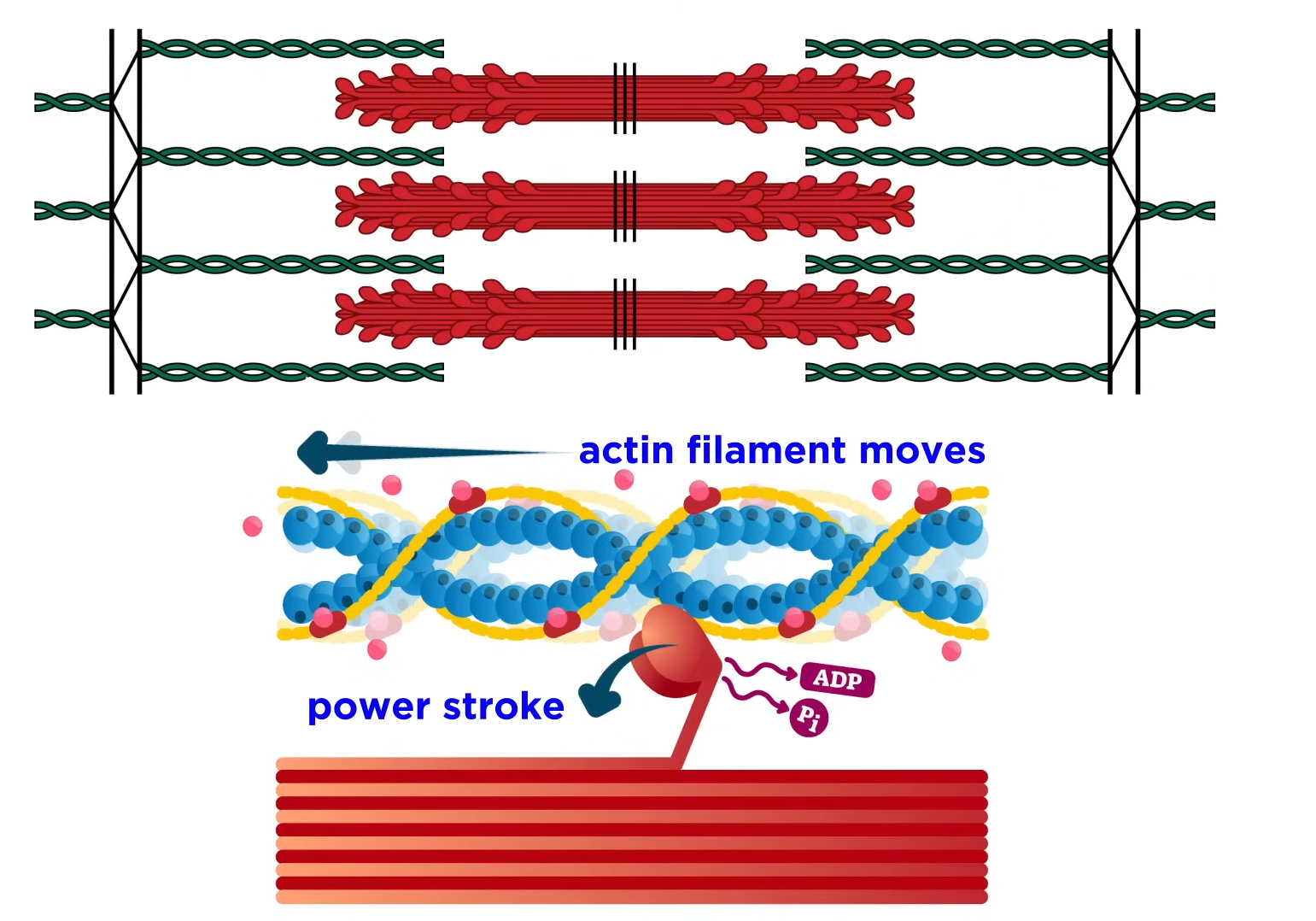
Musculoskeletal System
system that allows for movement
Sarcomeres are made up of 2 types of protein myofilaments:
Actin (thin filament)
Myosin (thick filament)
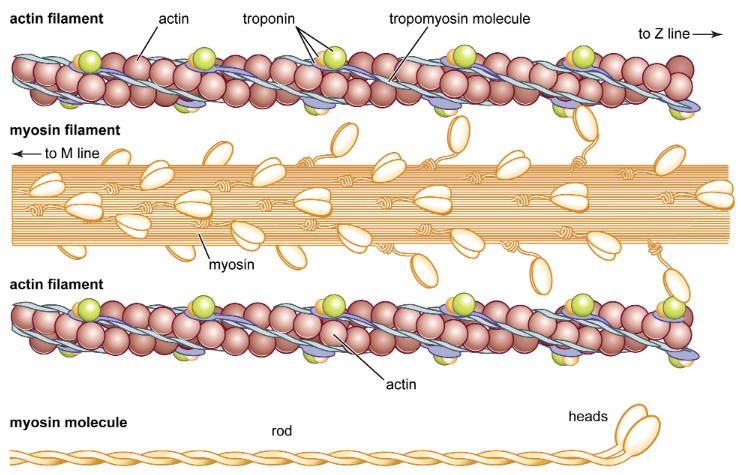
Each myosin is surrounded by _ actin filaments.
6
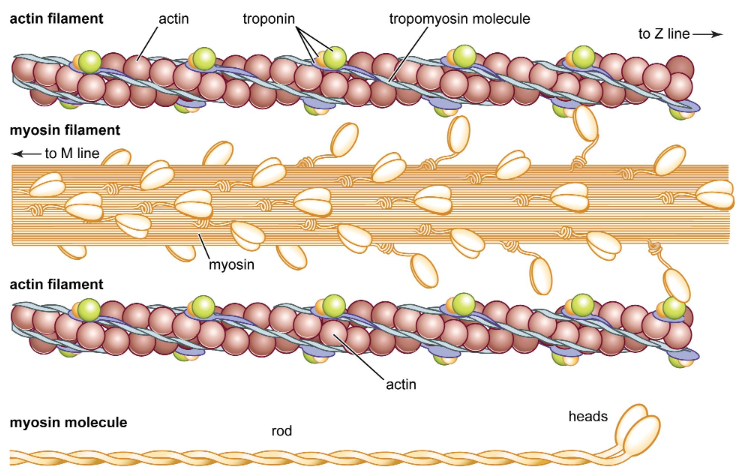
What is the '“trigger mechanism” for muscle contraction? Why?
release of calcium ions
they bind to troponin which causes tropomyosin to stop blocking the binding sites on actin, so myosin can bind to actin and cause muscle contraction
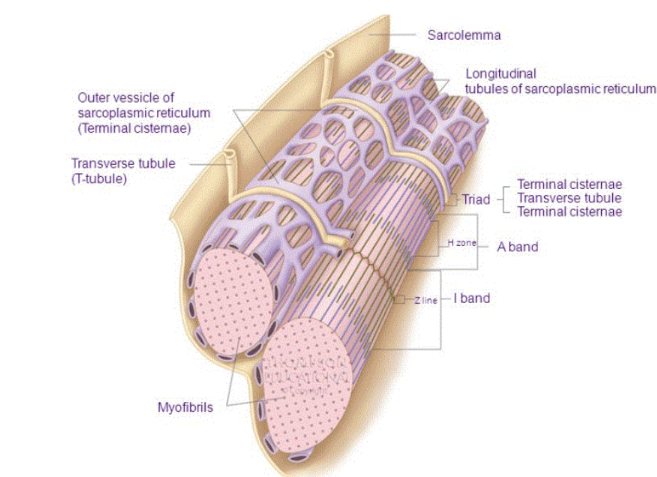
Terminal Cisternae
releases calcium ions into the sarcoplasm
sacs that form part of the sarcoplasmic reticulum
Myosin Cross Bridge
temporary attachment of myosin heads to actin
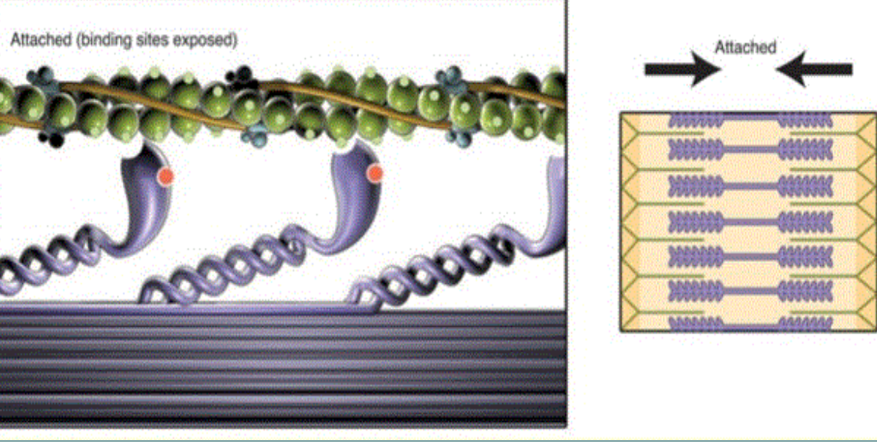
After the myosin heads pull the actin, another ___ is attached to the myosin heads to replace the previously used one. This secondary ___ triggers the release of the myosin head from the attachment sites. The ATP is then immediately broken down into ___ & a __ molecule again, to repeat the whole process over again if calcium is still attached to the actin
ATP, ADP, Pi
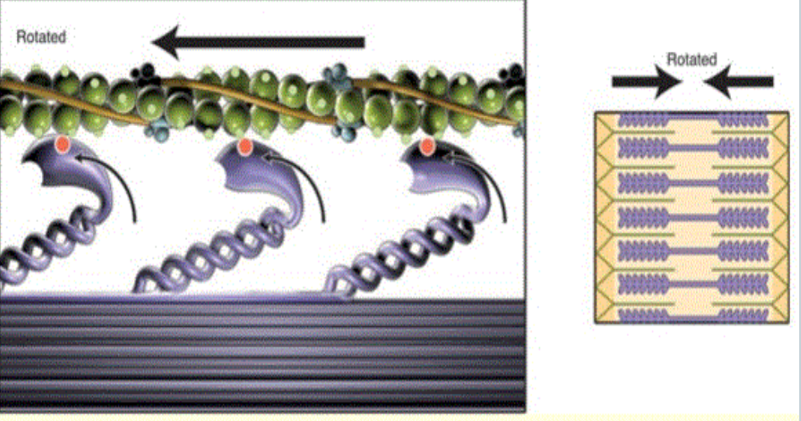
Muscle contraction will continue until the calcium is released from actin and the re-uptake of the calcium ions into the ____________ _________ takes place.
sarcoplasmic reticulum
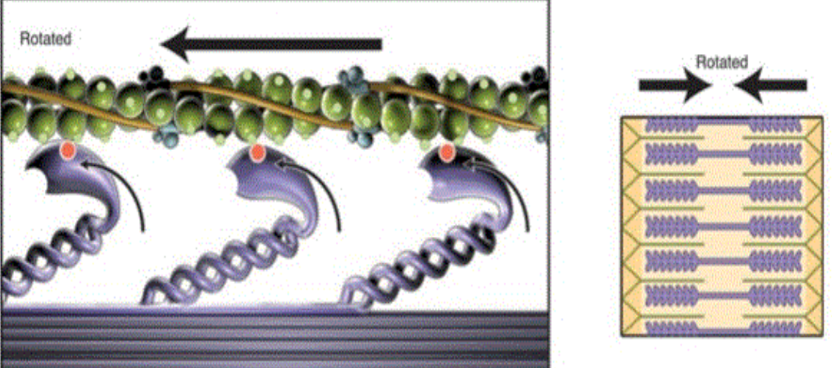
Repeatedly, myosin cross bridges attach, ______, detach and reattach in rapid succession. This process results in the sliding or overlap of the filaments, a shortening of the sarcomere, and what we see and know as muscle ___________.
rotate, contraction
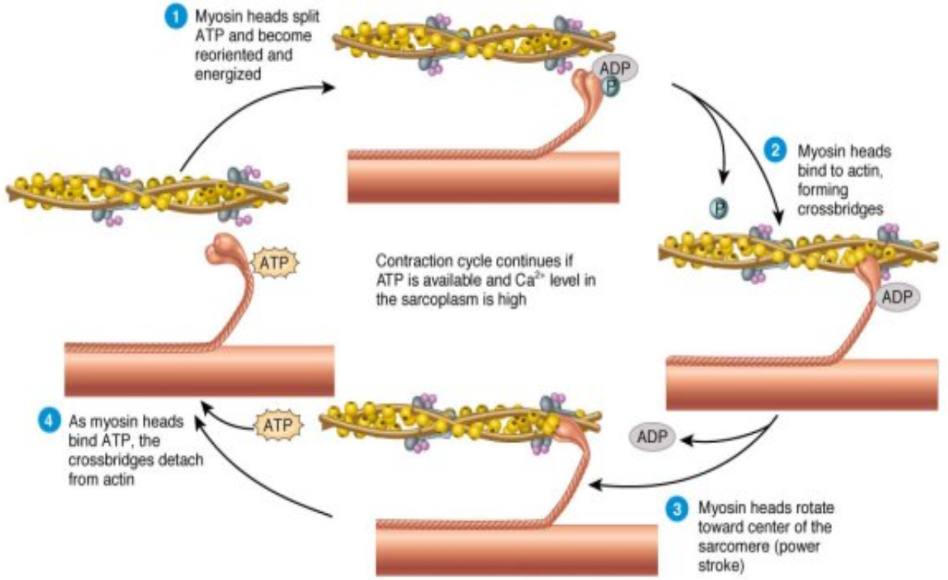
sliding filament theory
sliding filament theory
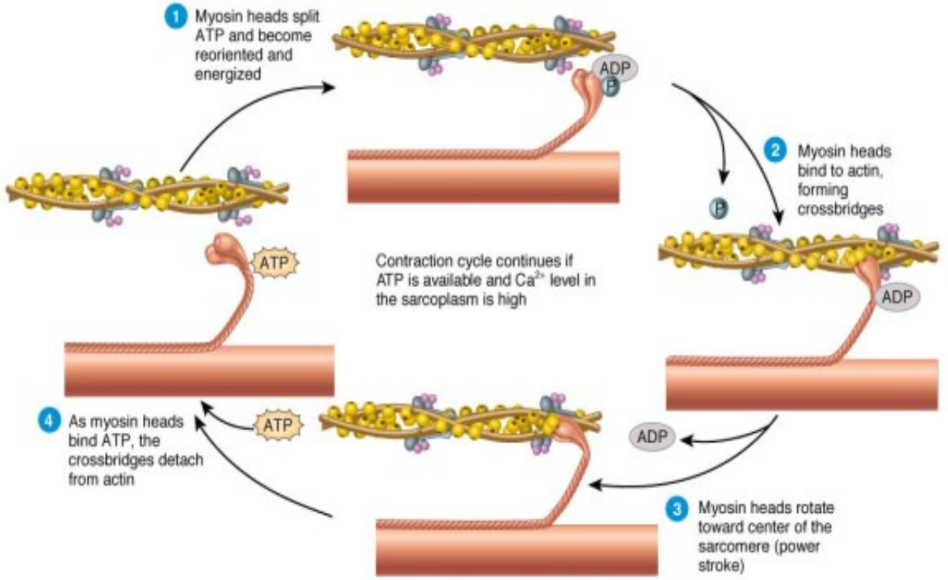
Cross Bridge Formation
head of the myosin filaments temporarily attaches themselves to the actin filaments
Cross Bridge Movement
myosin pulls and rotates actin
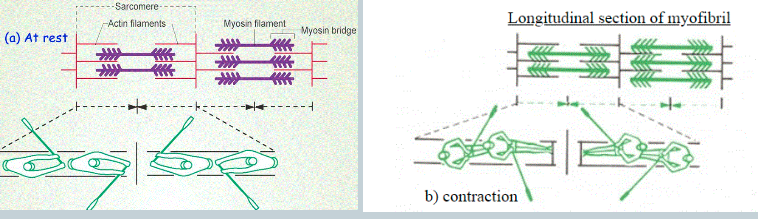
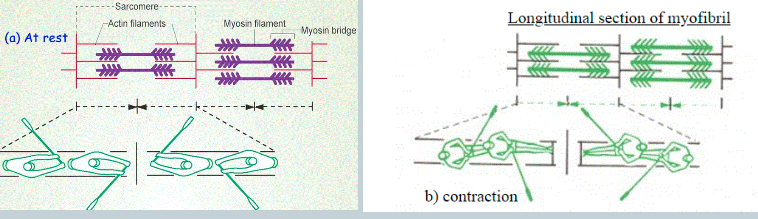
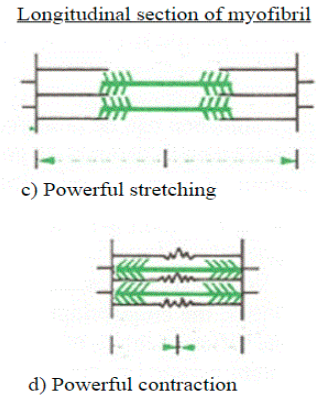
Sarcomeres should be at an optimal distance apart for muscle contraction. This optimal distance is 0.00__-0.00__ micrometres.
If the sarcomeres are stretched further apart than optimal distance → _____ cross bridges can form → ____ force produced.
If the sarcomeres are too close together → cross bridges interfere with one another as they form → ____ force produced.
19, 22
fewer, less
less
Excitation-Contraction Coupling
converting chemical E (ATP) into mechanical E
Joints
points at which bones connect
What system are joints part of?
articular system
Articular System
joints + their surrounding tissues that make connections between bones and muscle to make movement possible
Why are joints highly susceptible to injury?
because they are points of great stress (since they are involved in all our movements)
3 Types of Joints
Fibrous Joints
Cartilaginous Joints
Synovial Joints
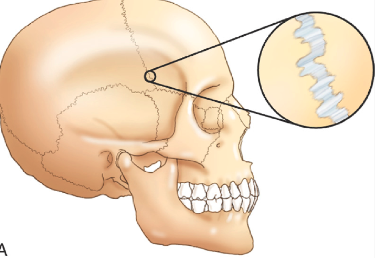
Fibrous Joint (+ example)
bones connected by fibrous tissues
allow NO MOVEMENT
ex. sutures between the bones of the skull
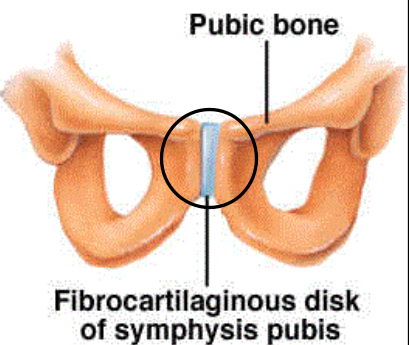
Cartilaginous Joint (+ example)
bones connected by cartilage
SLIGHT MOVEMENT possible
ex. symphysis pubis
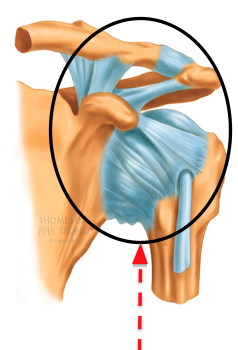
Synovial Joint (+ example)
bones ‘connected’ by synovial fluid, cartilage, and ligaments
MUCH MOVEMENT possible
ex. knee joint
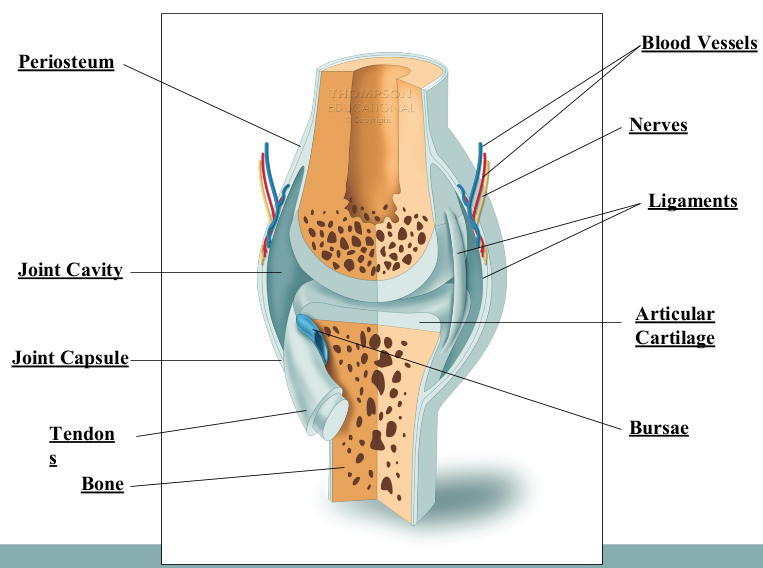
Characteristics of Synovial Joints
articulating cartilage
joint capsule
synovial membrane
fibrous capsule
joint cavity
bursae
intrinsic ligaments
extrinsic ligaments
Articulating Cartilage (Synovial Joints)
on the ends of bones
protects the ends of the bones, acts as shock absorber
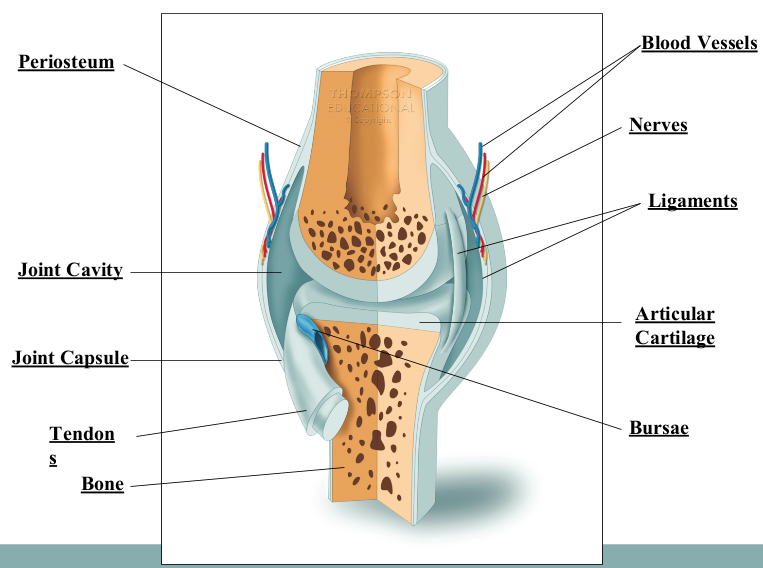
Joint Capsule (Synovial Joints)
fibrous structure that consists of the synovial membrane and fibrous capsule
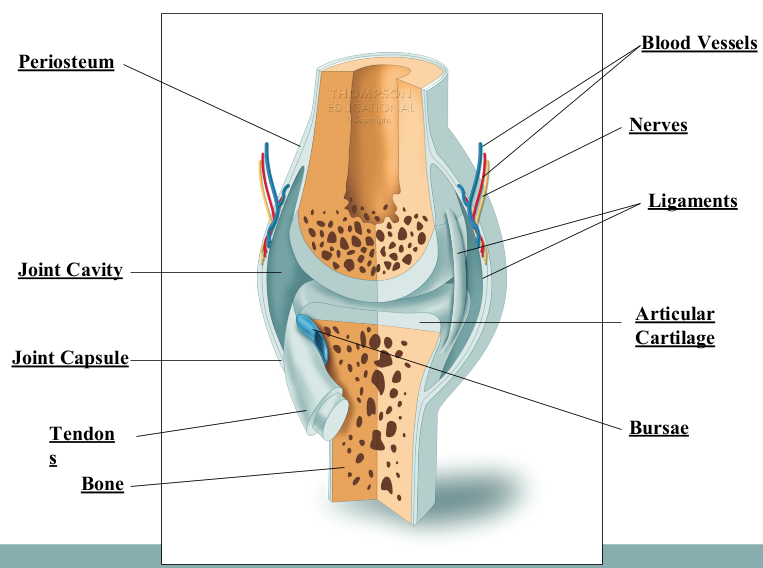
Synovial Membrane vs Fibrous Capsule (Synovial Joints)
synovial membrane - membrane that allows certain nutrients to pass through (more permeable, functional)
fibrous capsule - keeps synovial fluid from leaking (less permeable, structural)
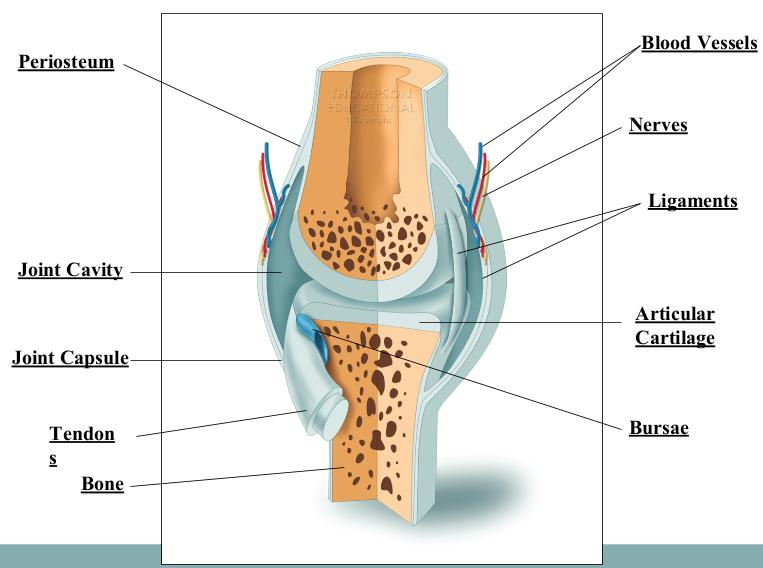
Joint Cavity (Synovial Joints)
located between the articulating surfaces
houses the synovial fluid
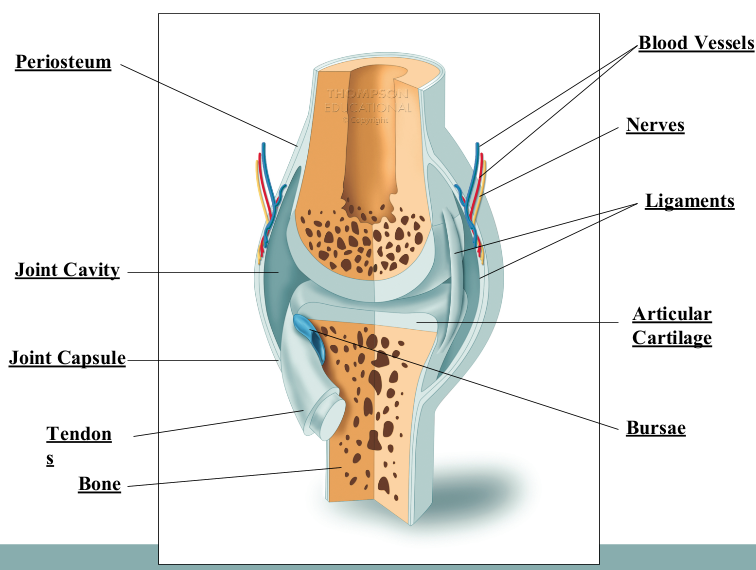
Synovial Fluid Purpose
to lubricate the synovial joint (reduce friction) and provide nutrients for the articulating cartilage
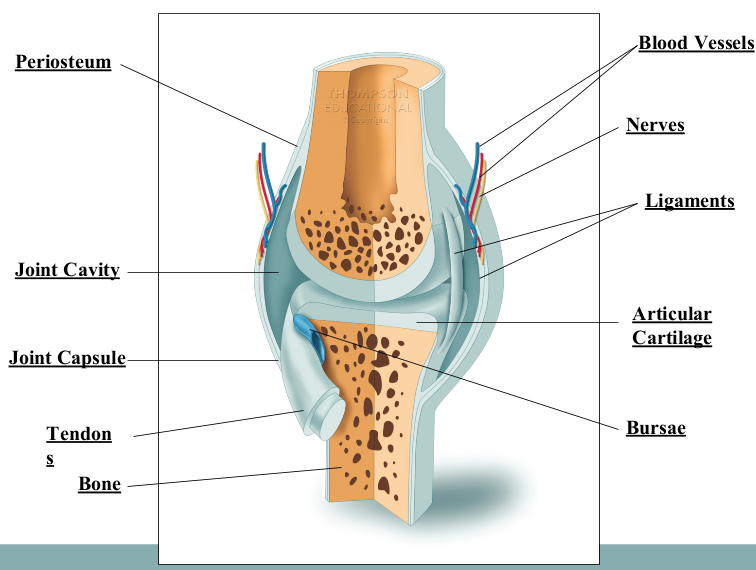
Bursae (Synovial Joints)
small, flattened fluid sacs found at the friction points between tendons, ligaments and bones
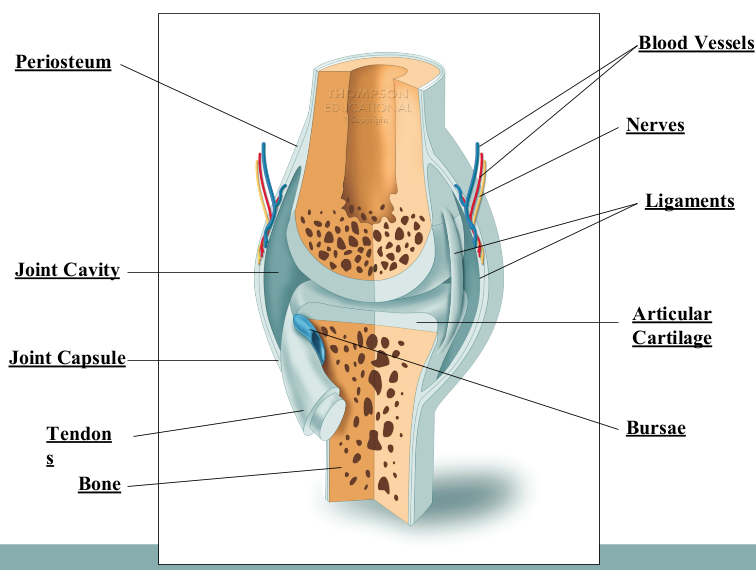
Intrinsic Ligaments vs Extrinsic Ligaments (Synovial Joints)
intrinsic - thick bands of fibrous connective tissue that help thicken and reinforce the joint capsule
extrinsic - separate from the joint capsule, helps to reinforce joint by holding bones together
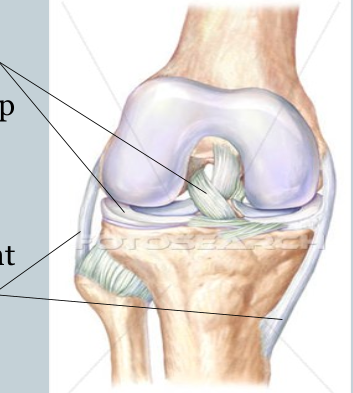
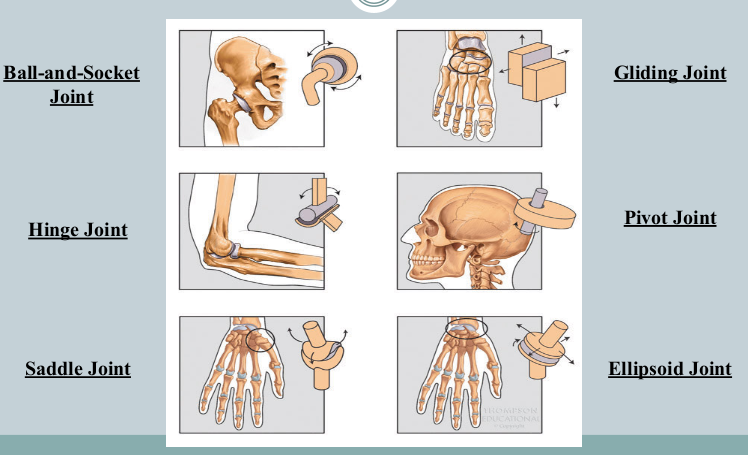
Types of Synovial Joints
gliding joint
hinge joint
pivot joint
ellipsoid joint
saddle joint
ball-and-socket joint