BIOL 2510 Wonil Choi - Exam 3
1/428
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
429 Terms
(Lecture 1 Fun fact) The bladder can stretch to hold up to
2 cups of urine
The urinary system is composed of
kidneys
ureters
urinary bladder
urethra
The kidneys
filter blood and convert filtrate into urine
Ureters
the liquid waste is transported by the ureters (Kidneys → Urinary bladder)
Urinary bladder
Stores urine until it is eliminated from the body
Urethra
Urine is eliminated through the urethra
Kidneys (Diagram)
What is A on the diagram?
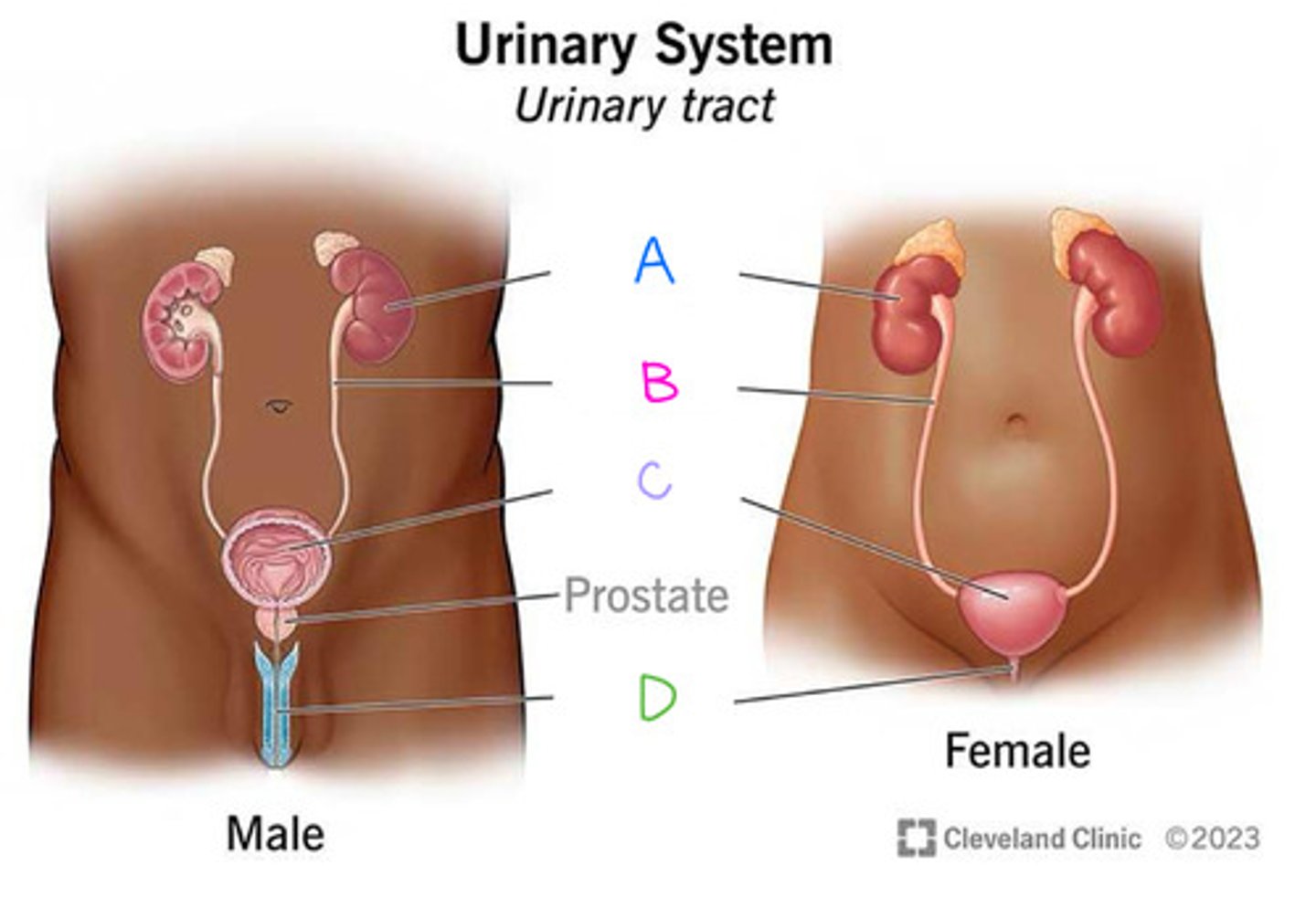
Ureters (Diagram)
What is B on the diagram?
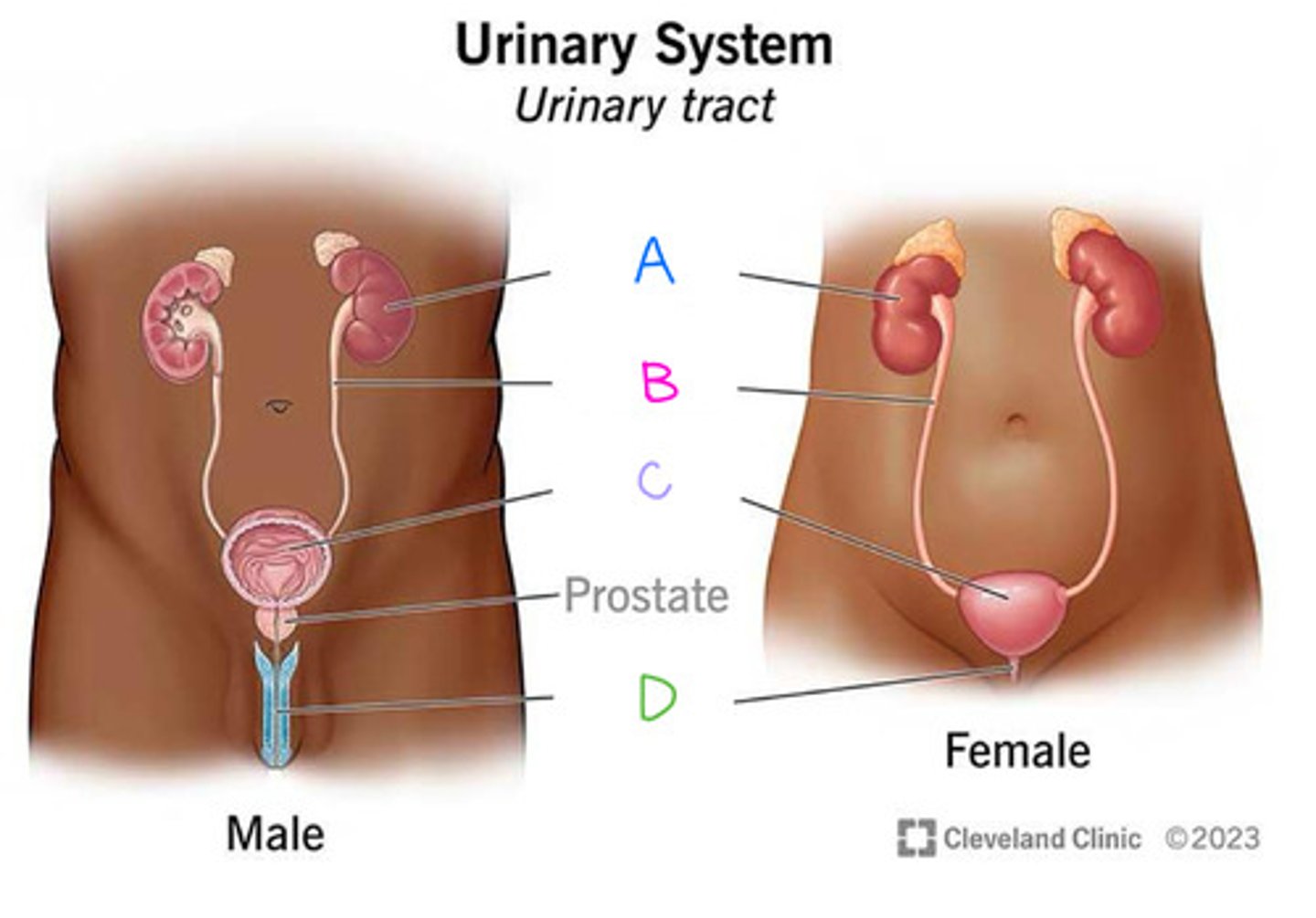
Urinary Bladder (Diagram)
What is C on the diagram?
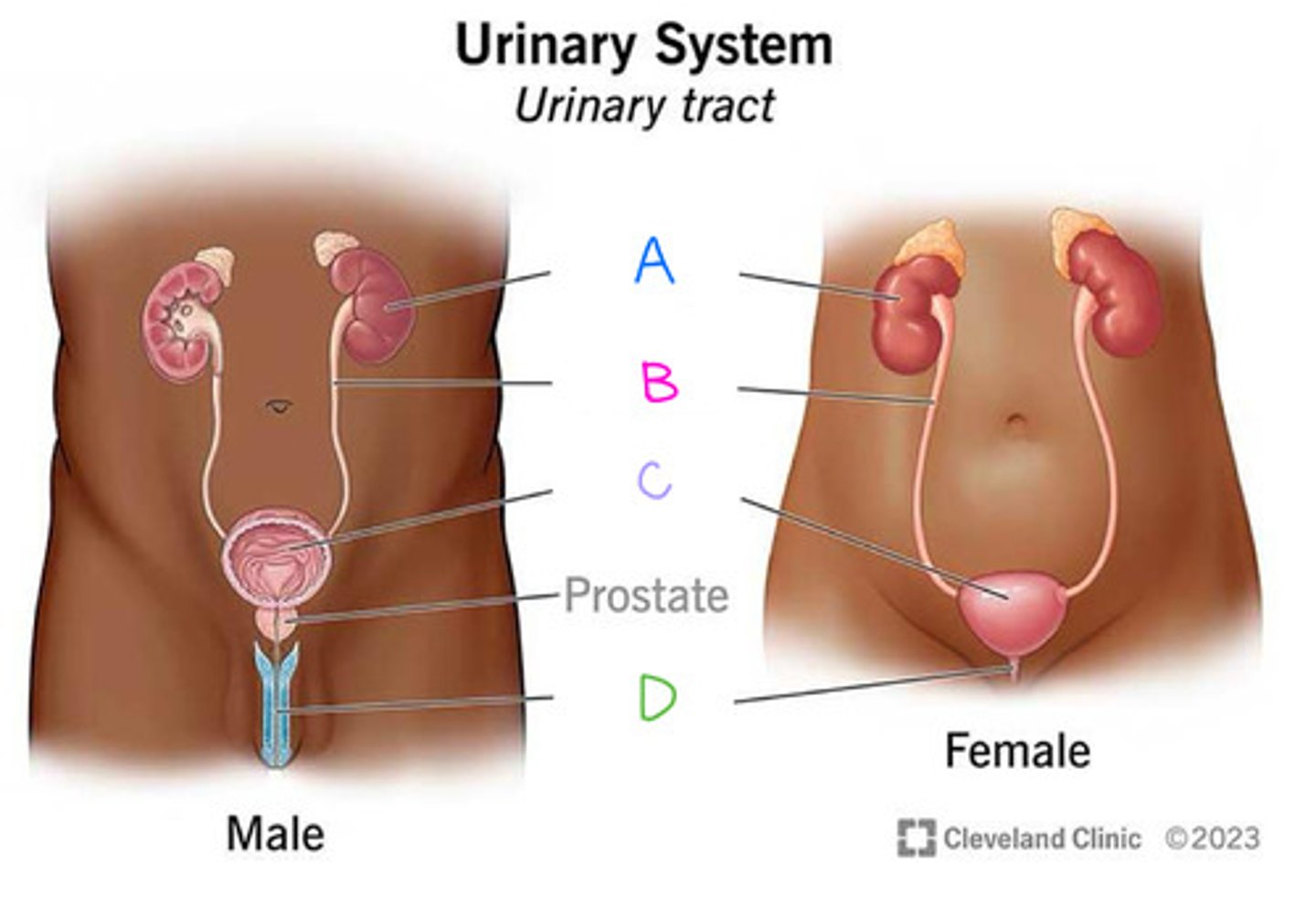
Urethra (Diagram)
What is D on the diagram?
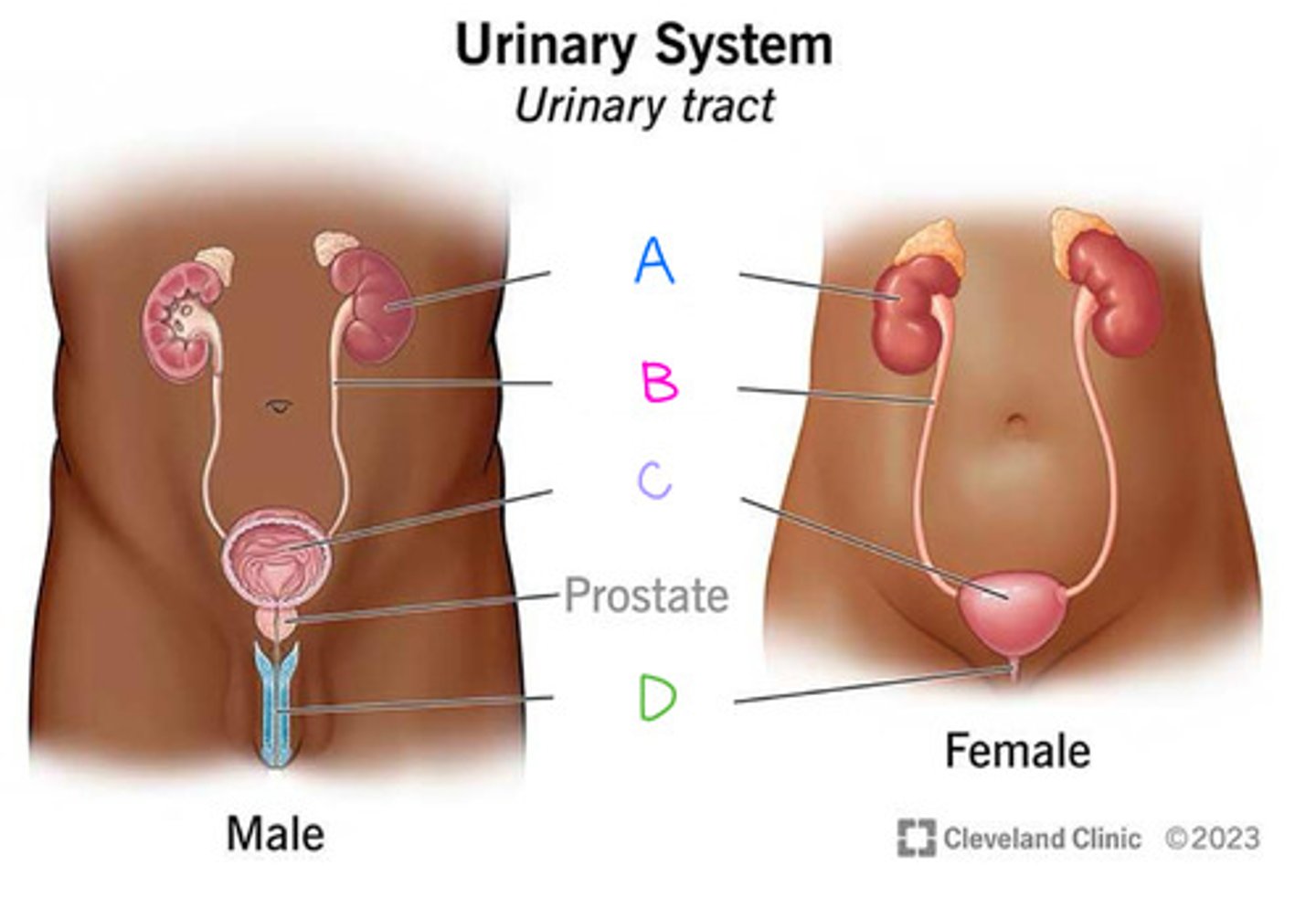
When filtrate is converted to urine, 3 different physiological processes occur:
1 - elimination of metabolic wastes
2 - Regulation of ion wastes
3 - regulation of acid-base balance
(Kidneys) Elimination of metabolic wastes
the kidneys remove waste within the filtrate (e.g. urea, uric acid) so these substances do not reach toxic levels within the blood
(Kidneys) Regulation of ion levels
the kidneys help control the blood's ion balance, such as sodium, potassium, calcium, and phosphate ions by eliminating them in the urine
(Kidneys) Regulation of acid-base balance
the kidneys maintain acid-base balance by altering blood levels of both hydrogen and bicarbonate ions
(Kidneys) Regulation of blood pressure
the kidneys help regulate blood pressure by excreting fluid in the urine
regulating fluid lost in the urine helps regulate blood volume
the kidneys can also release enzyme "renin", which is required for production of angiotensin II (a hormone that increases blood pressure)
Renin
hormone secreted by the kidney that leads to the production of angiotensin II which increases blood pressure (influences vasoconstriction)
(Kidneys) Elimination of biologically active molecules
small molecules (e.g. hormones, drugs) are filtered, but are not reclaimed, and then become part of urine
In addition to filtering blood and processing filtrate to form urine, your _______ perform/participate in other functions
kidneys
(Kidneys) Formation of Calcitrol
this hormone increases the absorption of calcium from the small intestine (increased blood calcium concentration)
(Kidneys) Production and release of erythropoietin
Kidney's response to low blood oxygen levels by secreting this hormone (EPO)
erythropoietin
hormone that leads to increased erythrocyte formation
(Kidneys) Potential to engage in gluconeogenesis
during fasting or starvation
to product glucose from noncarbohydrate sources to maintain normal blood glucose levels
Your kidneys take care of your blood by: removing ________ materials from the blood
Unwanted
Your kidneys take care of your blood by: maintaining blood plasma ____
Ions
Your kidneys take care of your blood by: regulating blood __
pH
Your kidneys take care of your blood by: altering blood ______
volume
Your kidneys take care of your blood by: regulating the number of ____________
Erythrocytes
Your kidneys take care of your blood by: Maintaining _____ _______ ______ during fasting or starvation
blood glucose levels
Healthy kidney means
Healthy blood
Shape of Kidneys
symmetrical bean shaped
Each kidney has a concave medial border called
Hilum
The Hilum is where
the vessels, nerves, and ureter connect to the kidney
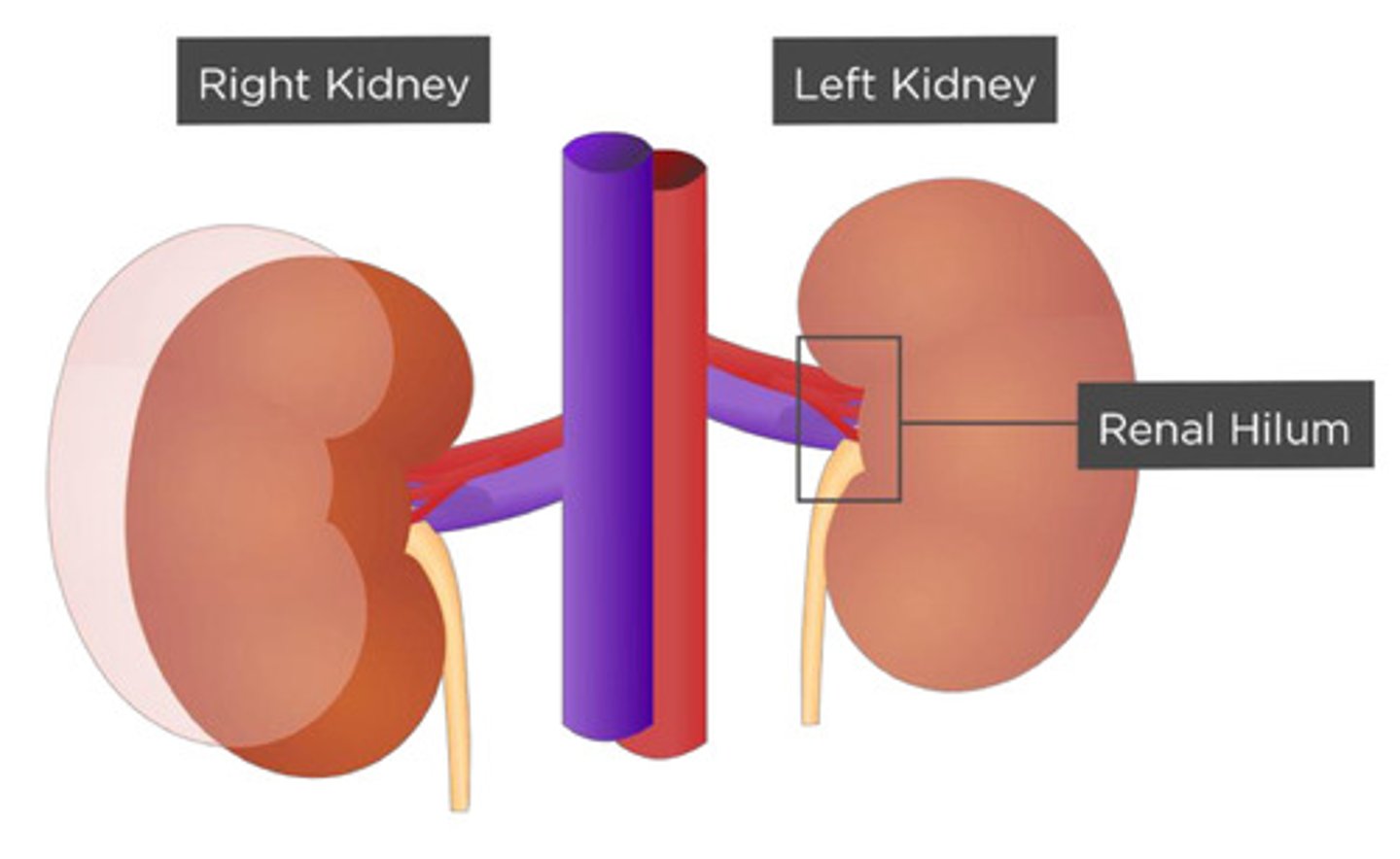
An _______ gland sits on the superior aspect of each kidney
Adrenal
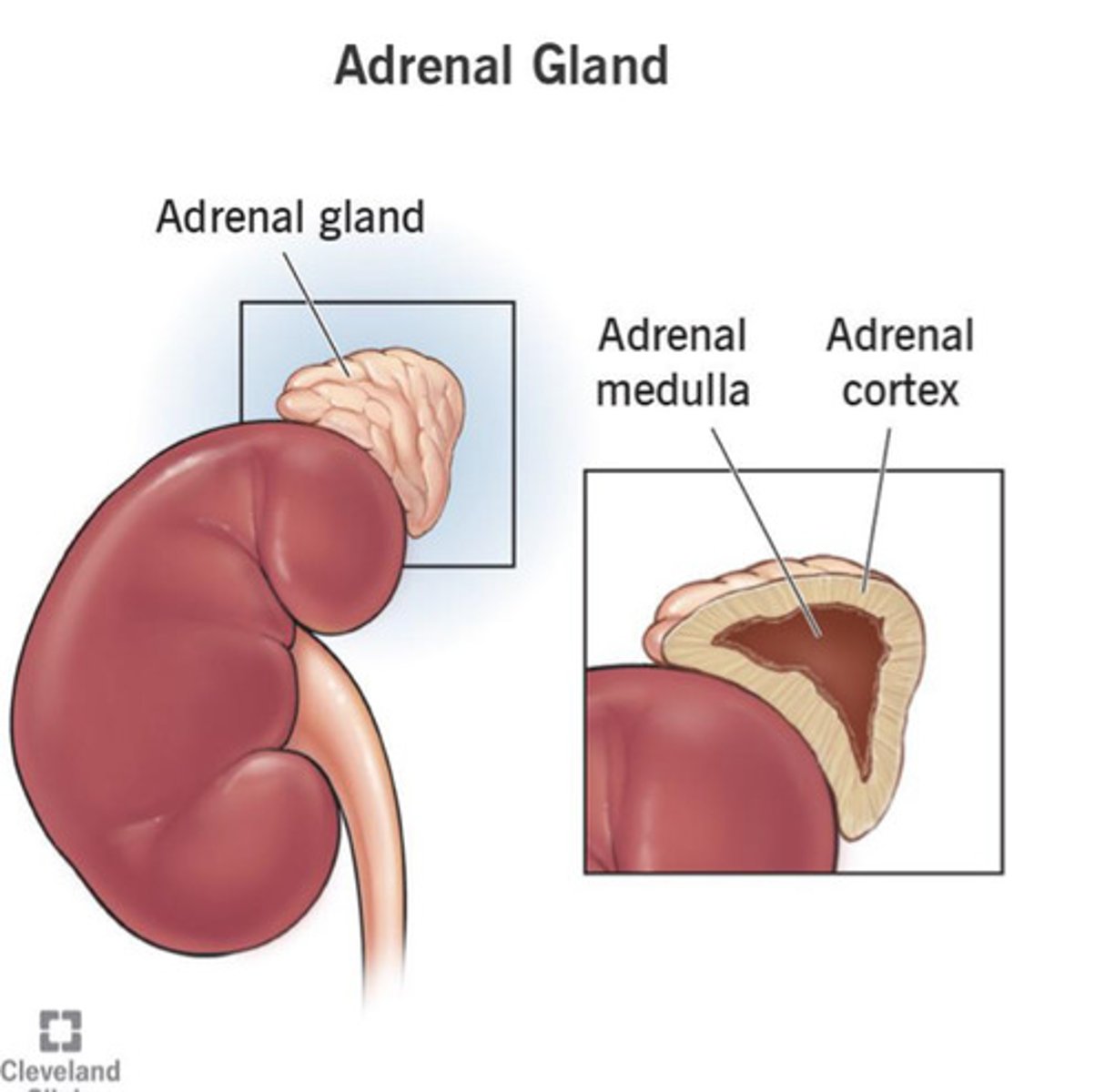
Kidneys are located along the
posterior abdominal wall, lateral to the vertebral column (Retroperitoneal)
The left kidney is found between the level of the
T12 and L3
The right kidney is located ________ to the left kidney; why?
Inferior
due to the position of the liver
Each kidney is surrounded and supported by several tissue layers
fibrous capsule (renal capsule)
perinephric fat (adipose capsule)
renal fascia
paranephric fat
(INNERMOST TO OUTERMOST!)
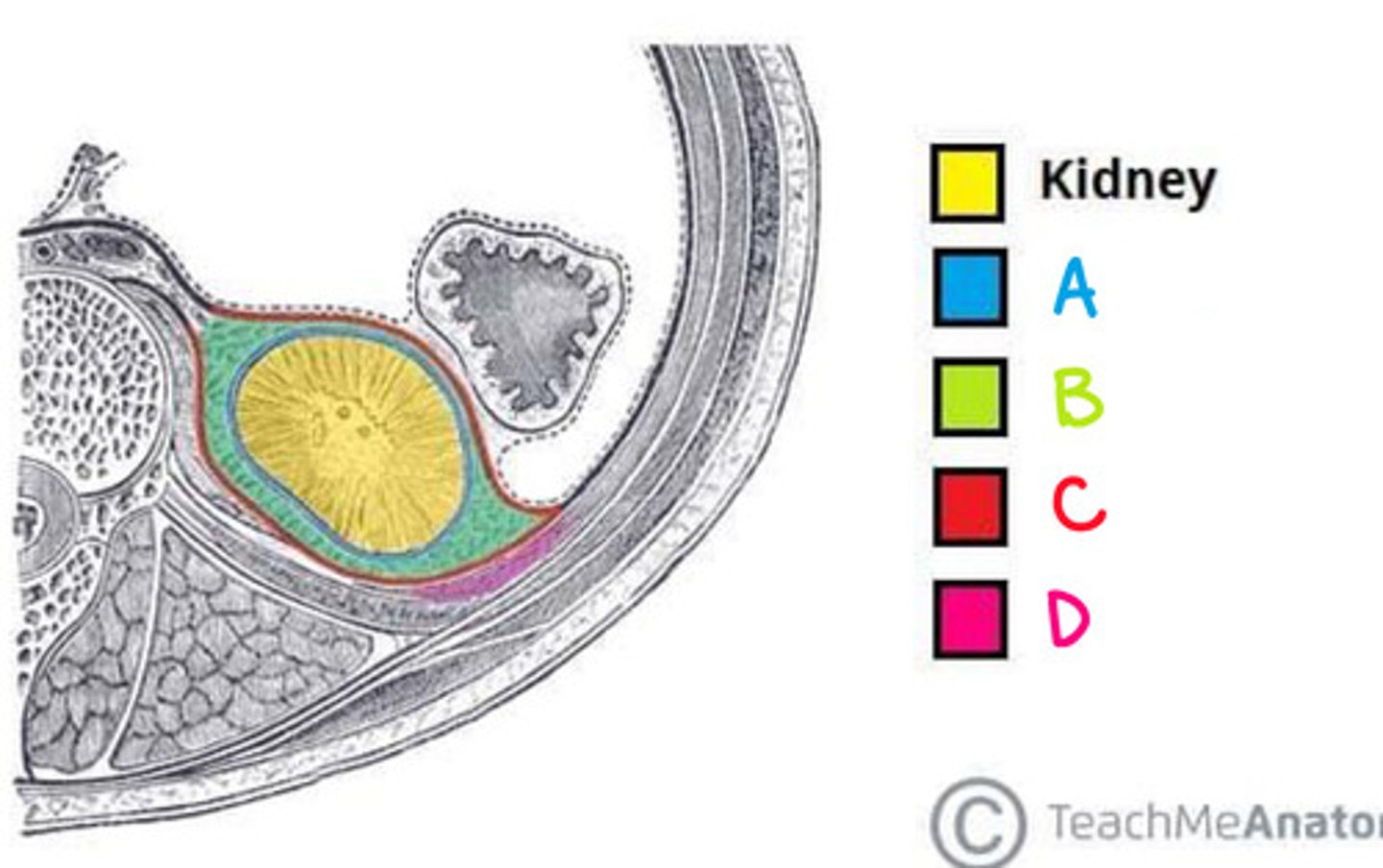
Fibrous Capsule (Renal capsule) (Diagram)
What is A on the diagram?
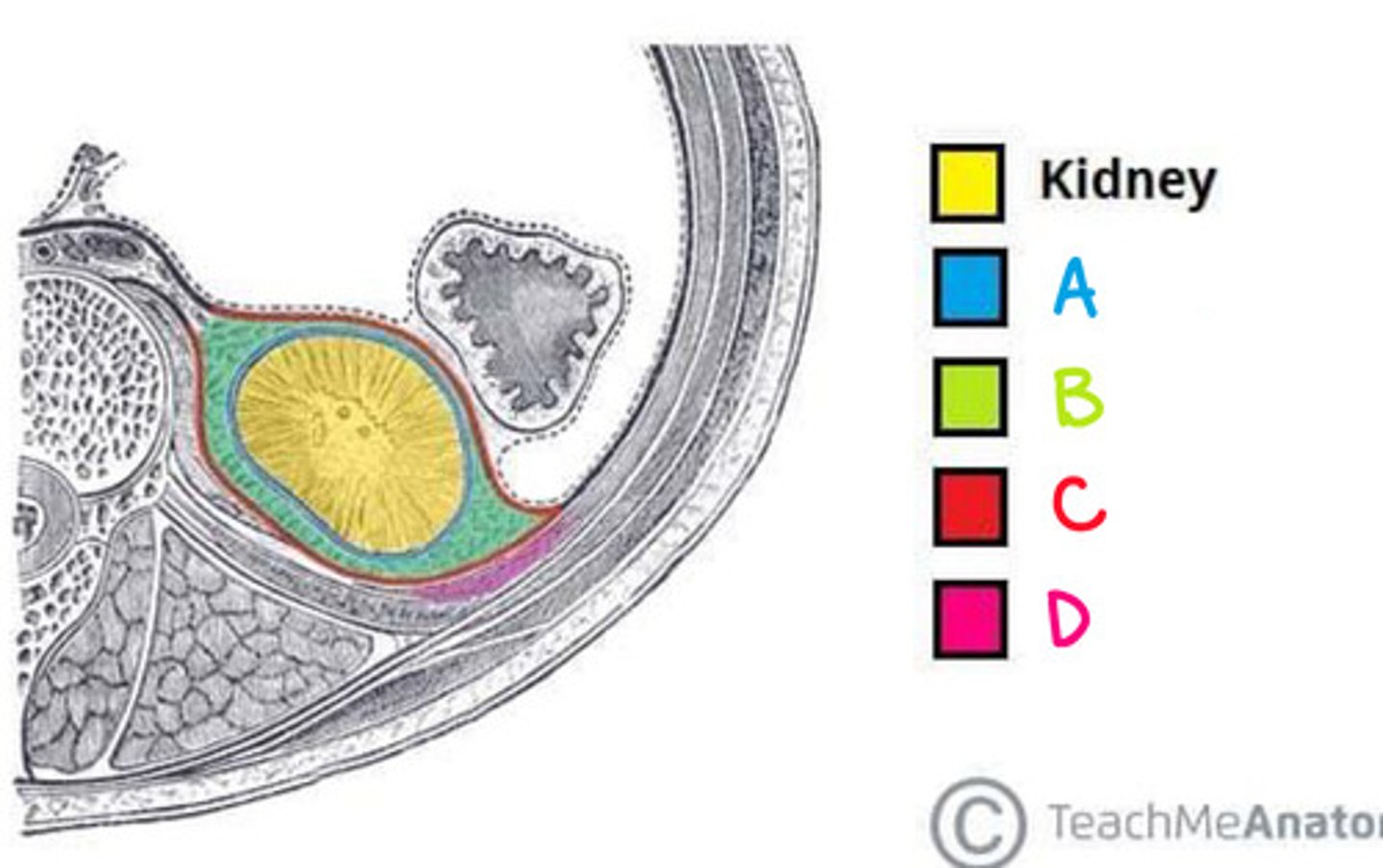
Perinephric Fat (Adipose capsule) (Diagram)
What is B on the diagram?
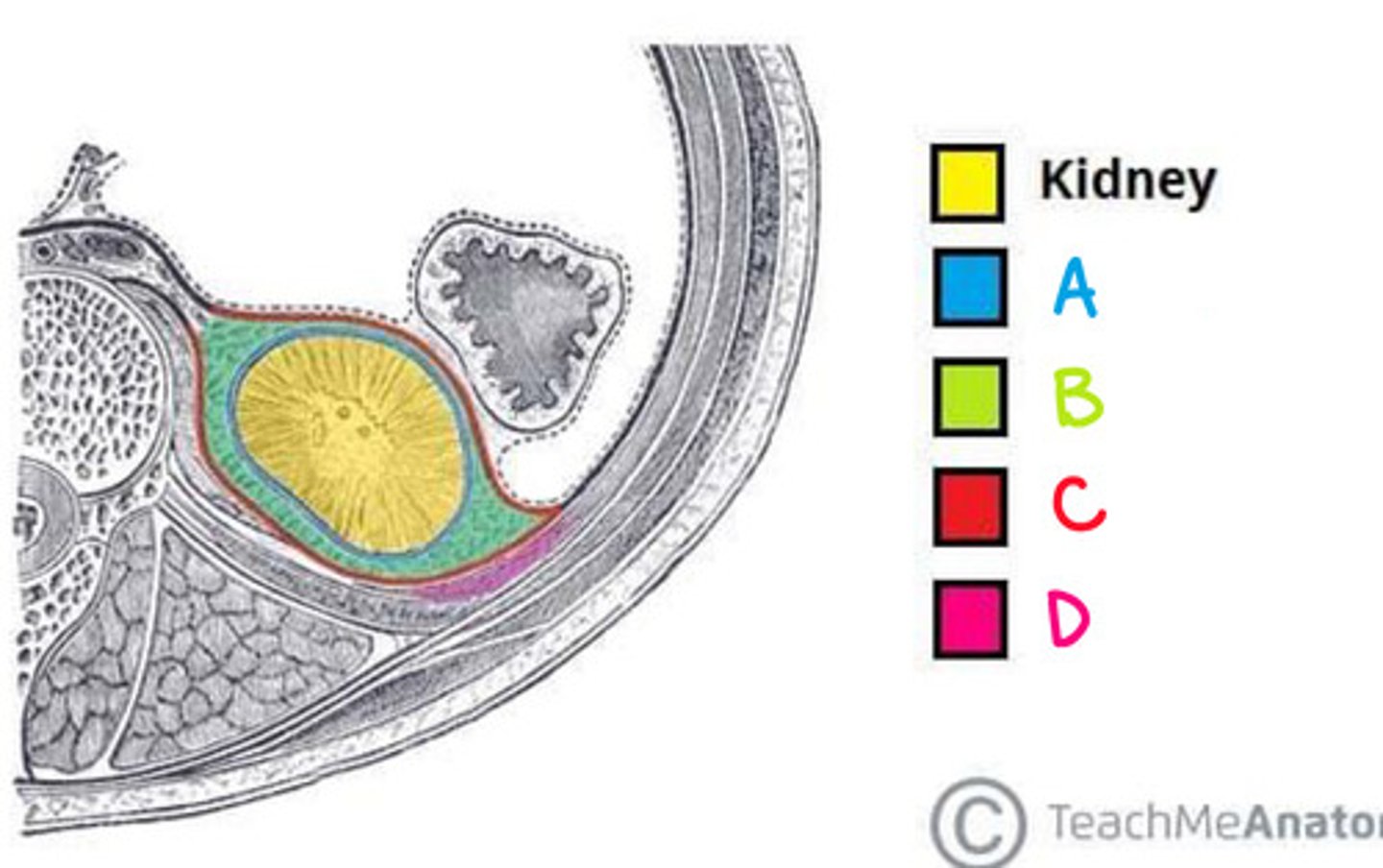
Renal Fascia (Diagram)
What is C on the diagram?
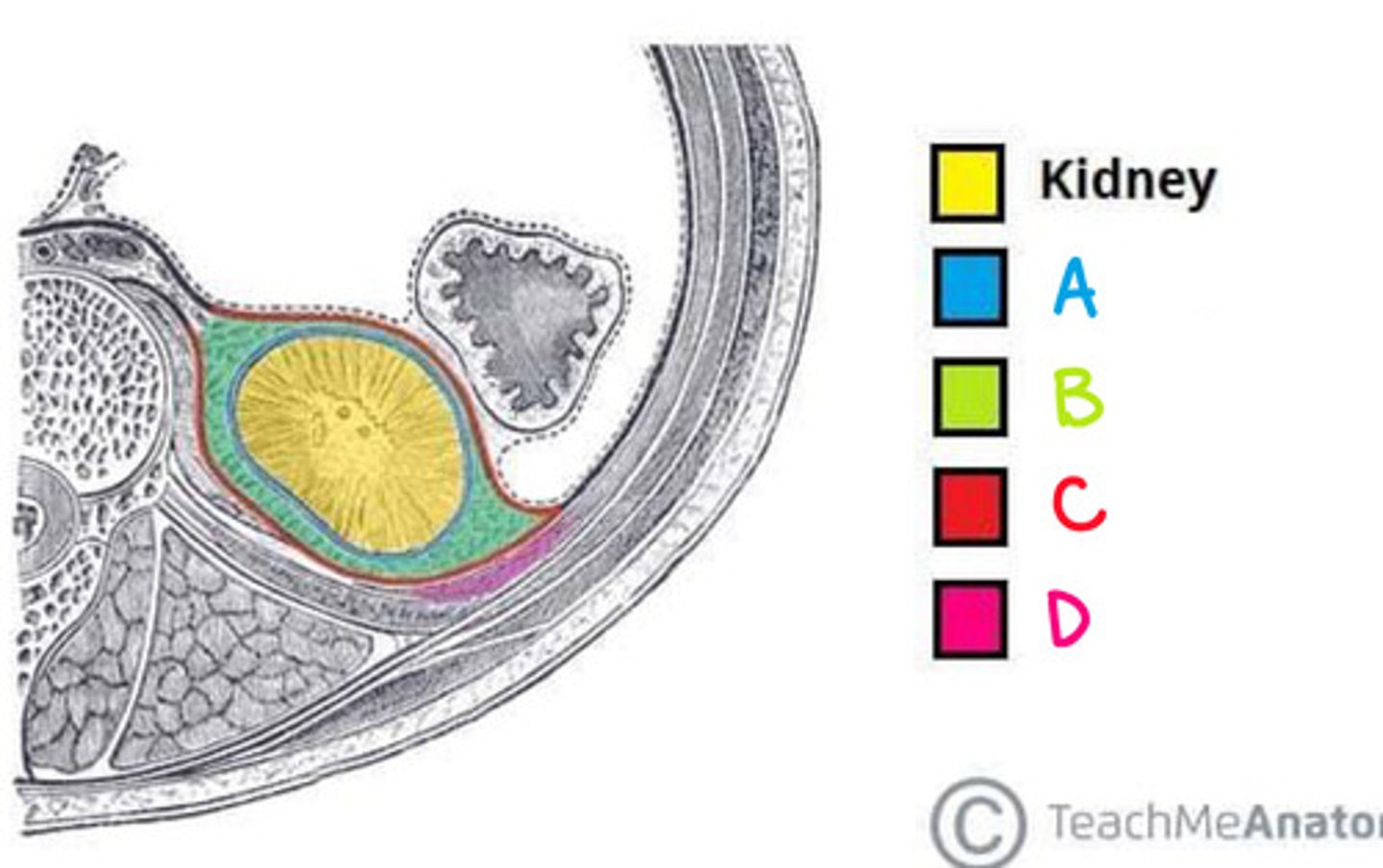
Paranephric fat (Diagram)
What is D on the diagram?
Fibrous capsule (renal capsule)
directly adhere to the external surface of the kidney
mainly composed of dense irregular connective tissue
maintains kidney's shape, protects it from trauma, and prevents pathogens from penetrating the kidney
Perinephric fat (adipose capsule)
composed of Adipose connective tissue
provides cushion and stabilization for the kidney
Renal Fascia
composed of dense irregular connective tissue
anchors the kidney to surrounding structures
Paranephric fat
the outermost layer surrounding the kidney
composed of adipose connective tissue (cushioning and stabilization)
Renal ptosis and hydronephrosis
the loss of adipose connective tissue in very thin elderly or individuals with anorexia may result in renal ptosis
the dropping of the kidney
Dropping of the kidney from renal ptosis can ultimately cause
a "kink" in the Ureter, which leads to
decreased urine flow,
urine backs up into the proximal part of the ureter,
and enlargement of the renal pelvis
When the kidney is sectioned coronally, the
parenchyma ("functioning tissue") is visible
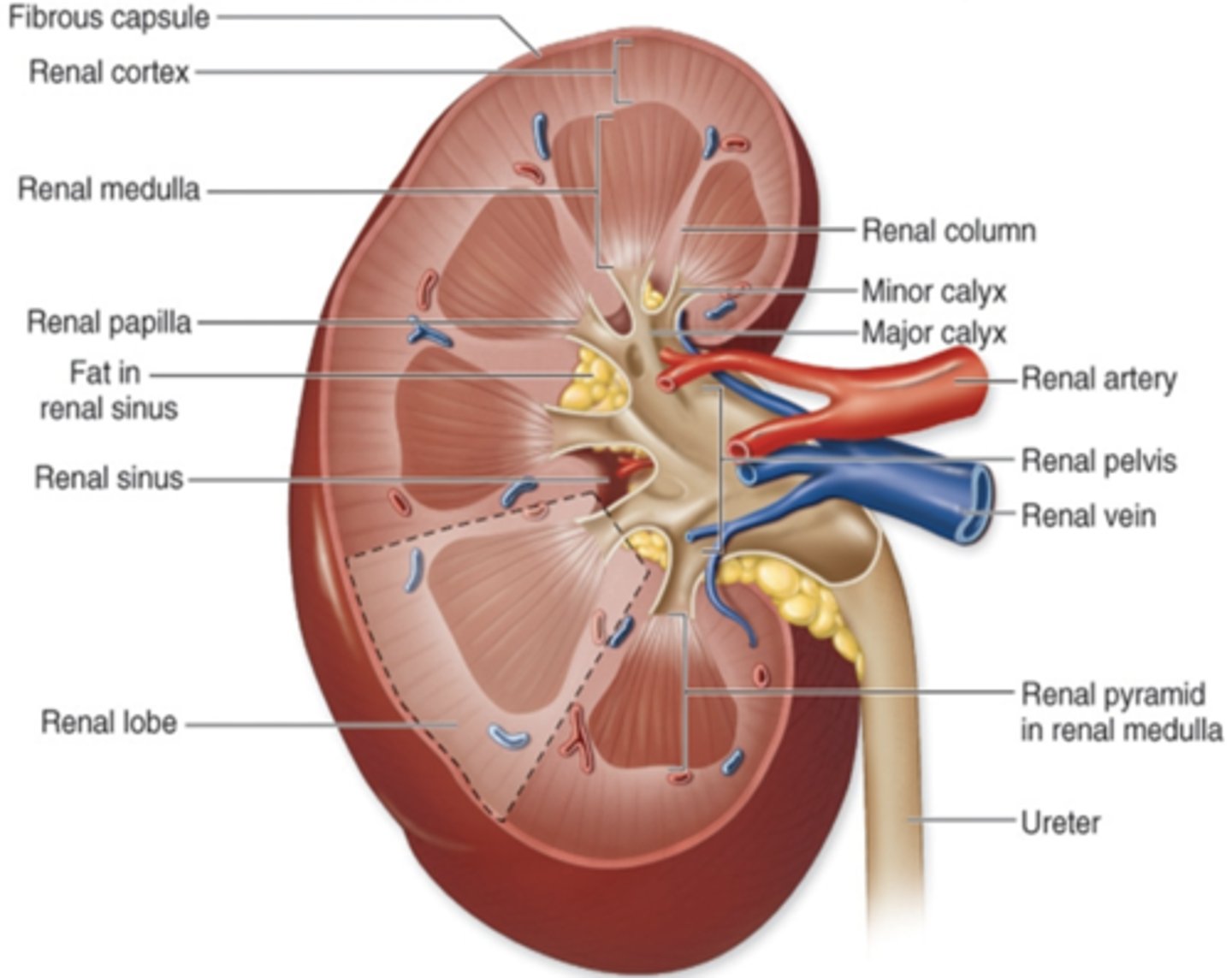
2 distinct regions of the parenchyma
outer renal cortex
inner renal medulla
Renal Columns
extensions of the cortex
project into the medulla and subdivide it into renal pyramids (medullary pyramids)
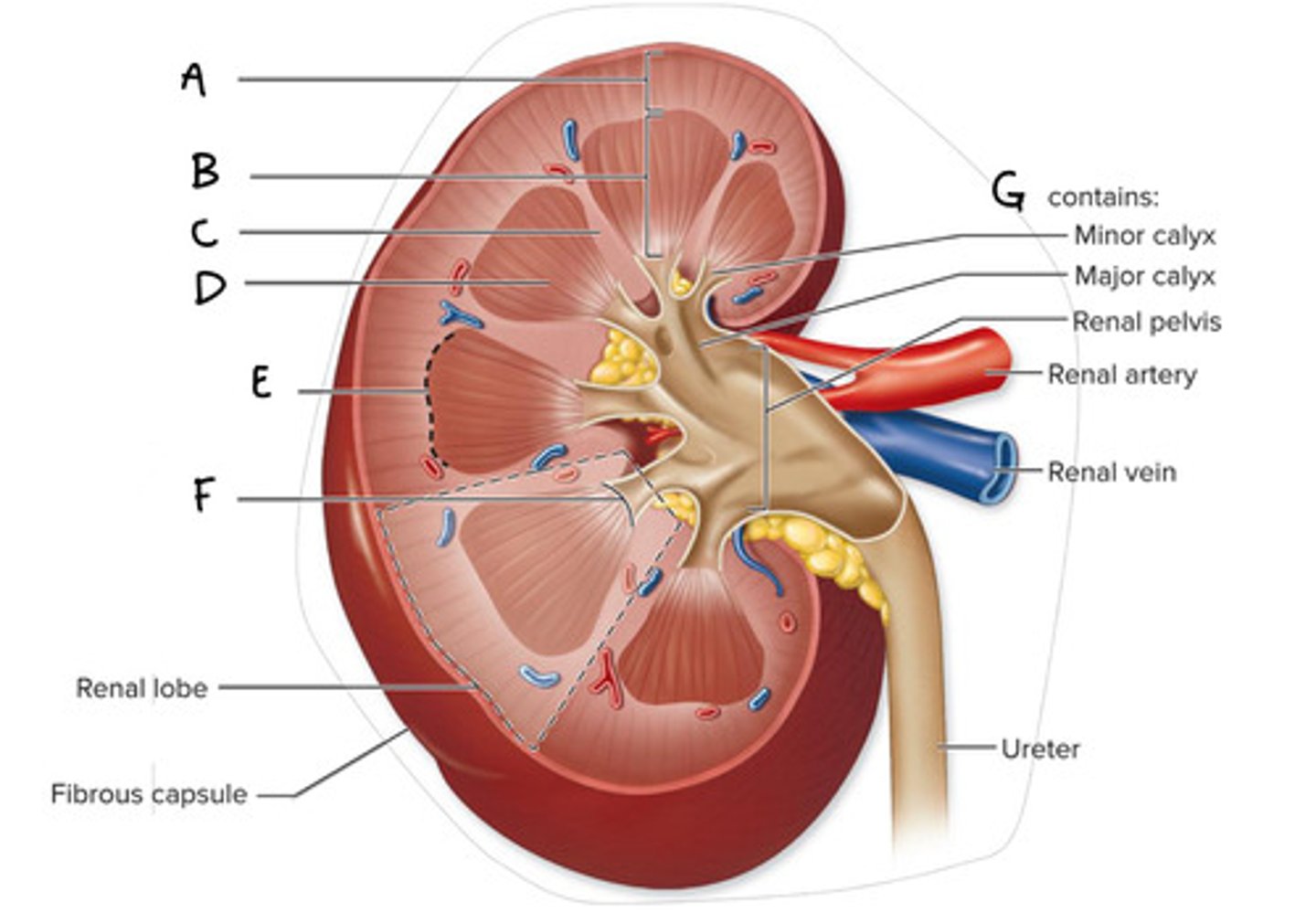
Renal cortex (Diagram)
What is A on the diagram?
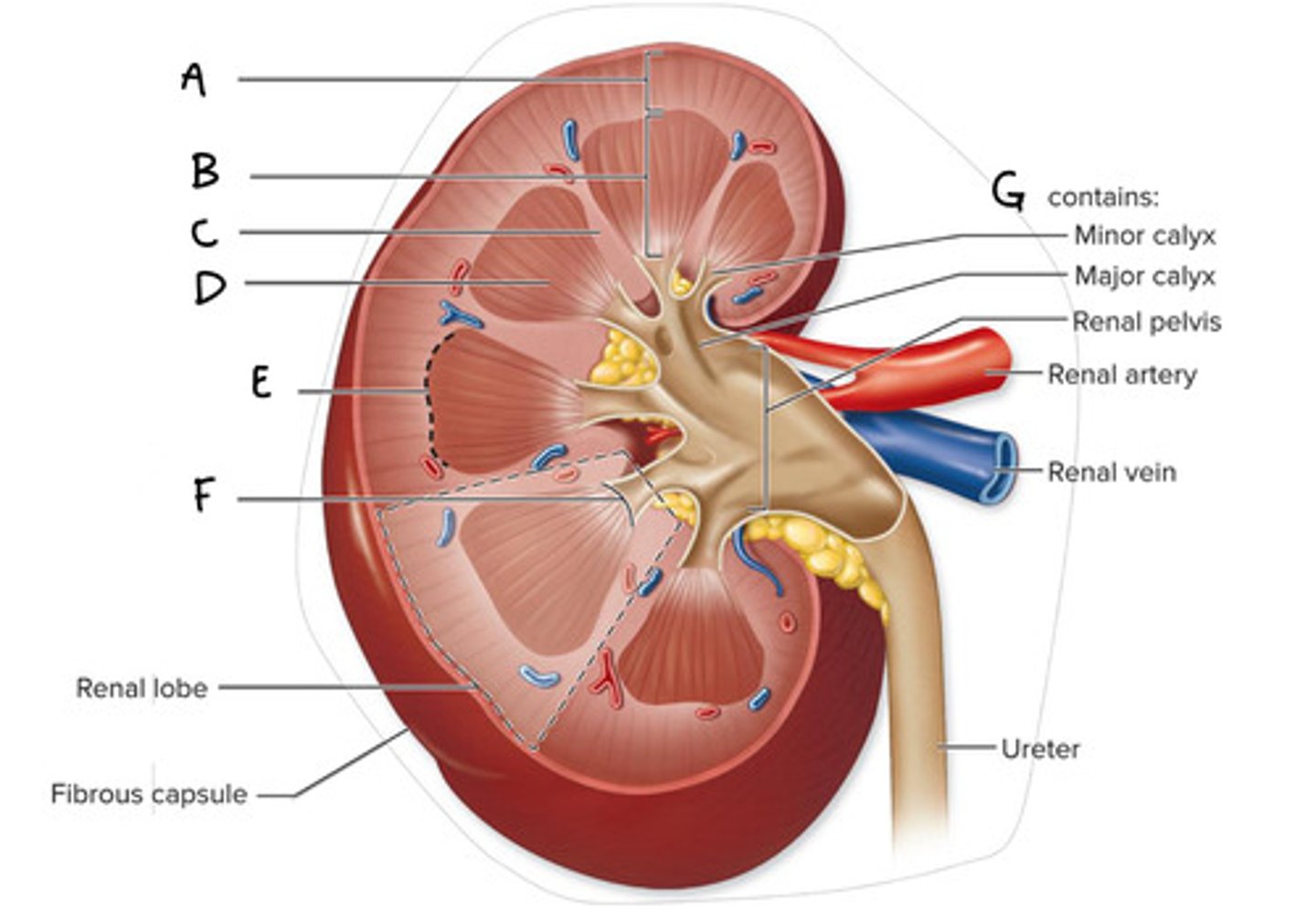
Renal Medulla (Diagram)
What is B on the diagram?
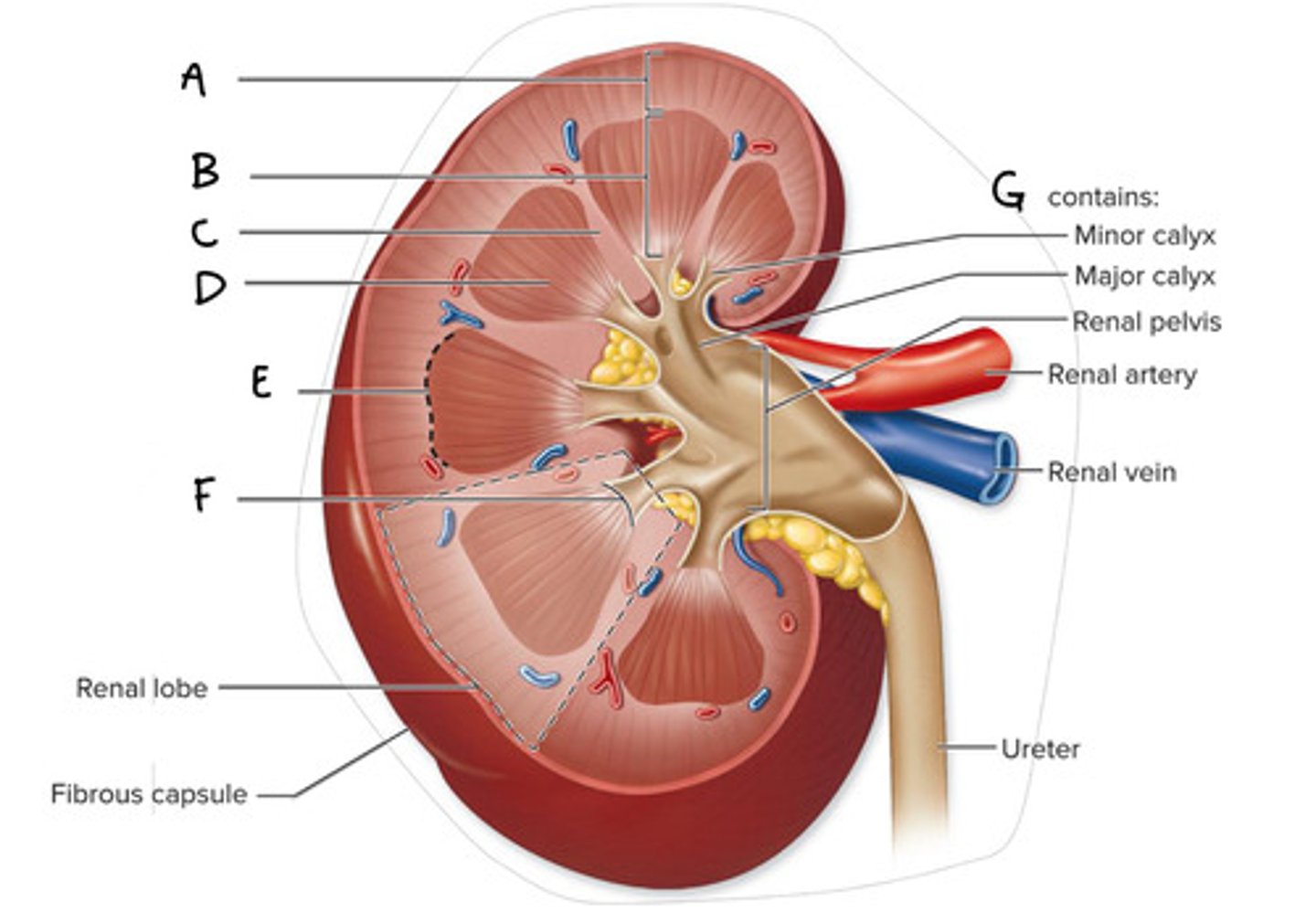
Renal Column (Diagram)
What is C on the diagram?
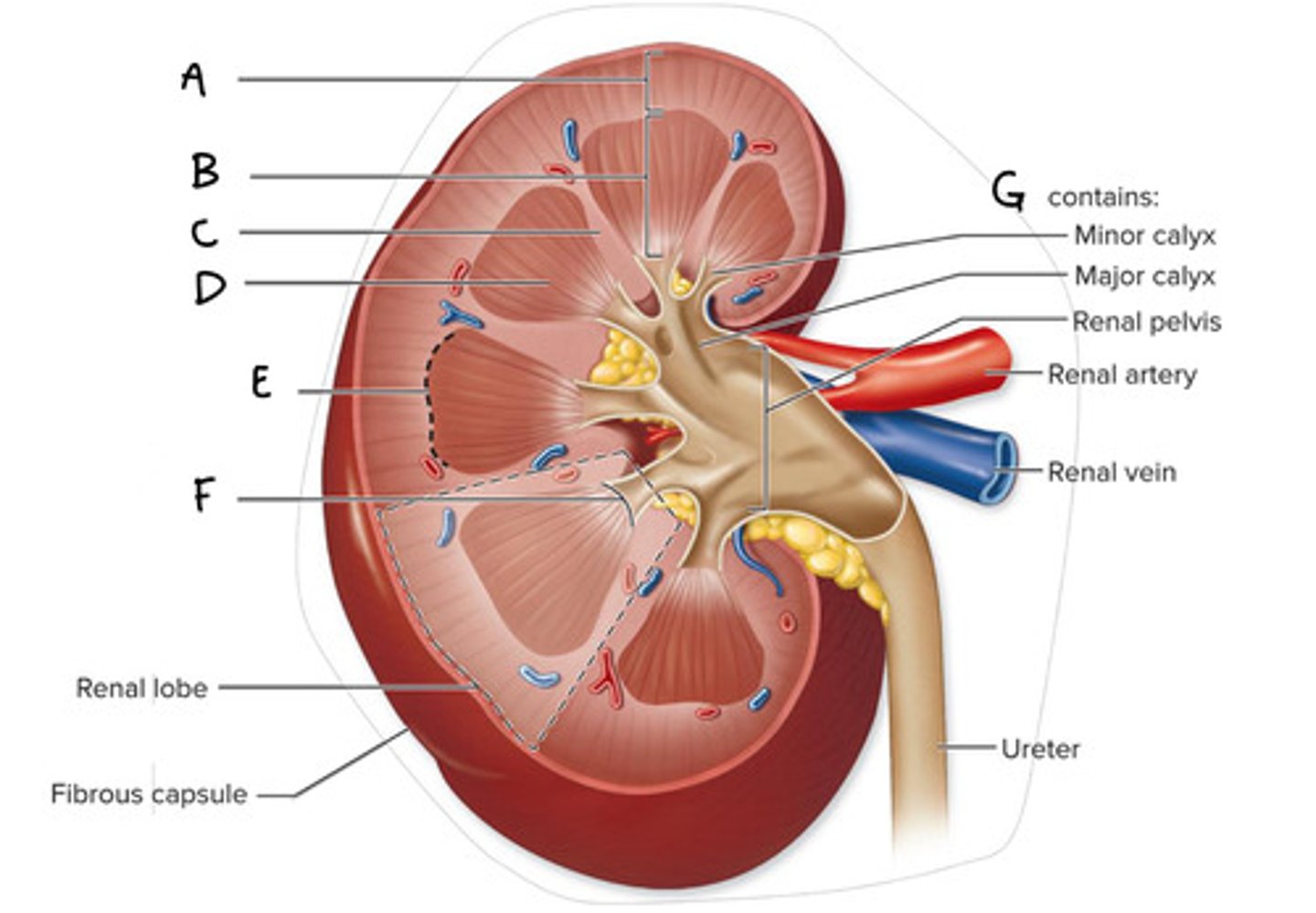
Renal Pyramid (Medullary Pyramid) (Diagram)
What is D on the diagram?
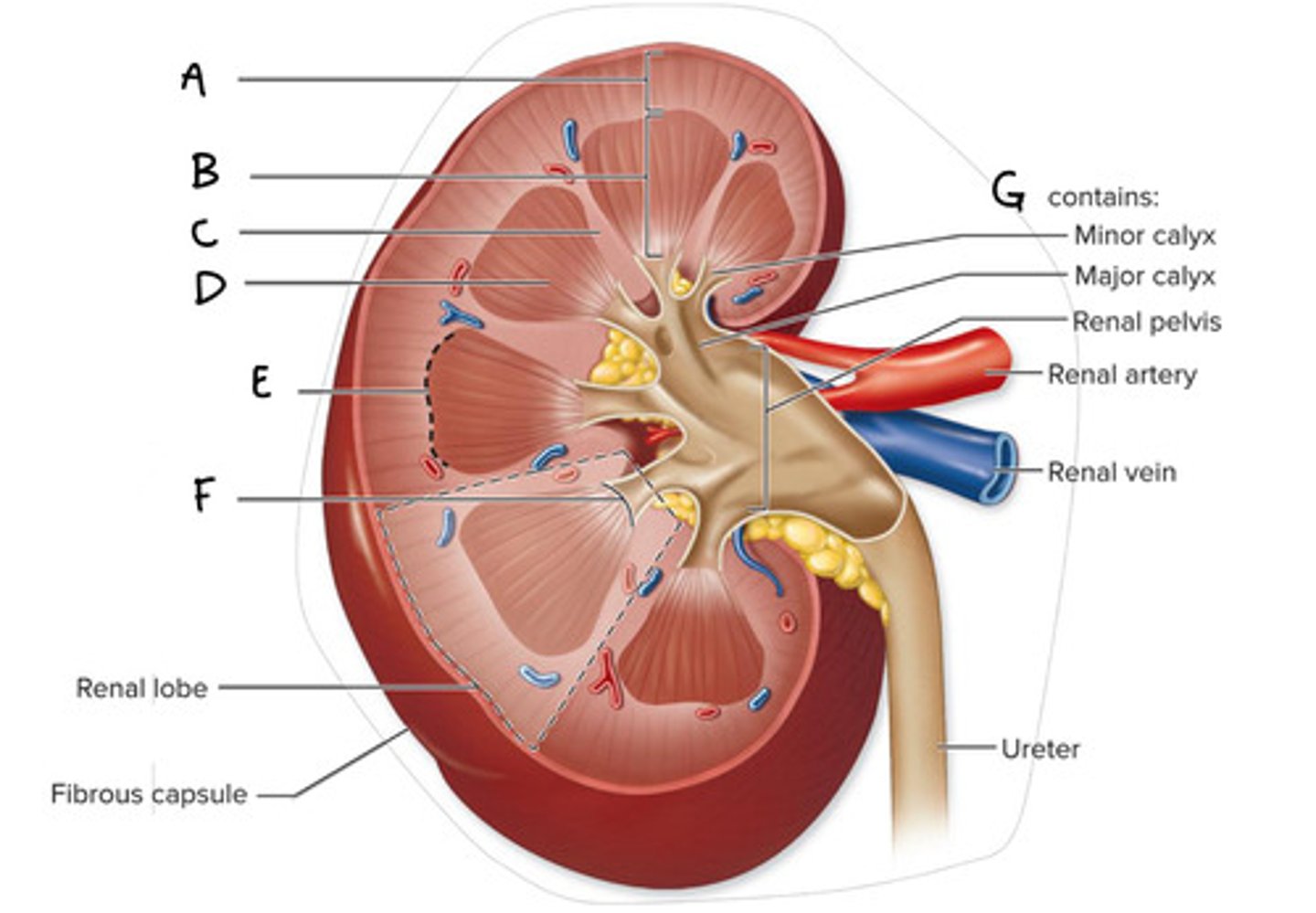
Corticomedullary Junction (Diagram)
What is E on the Diagram?
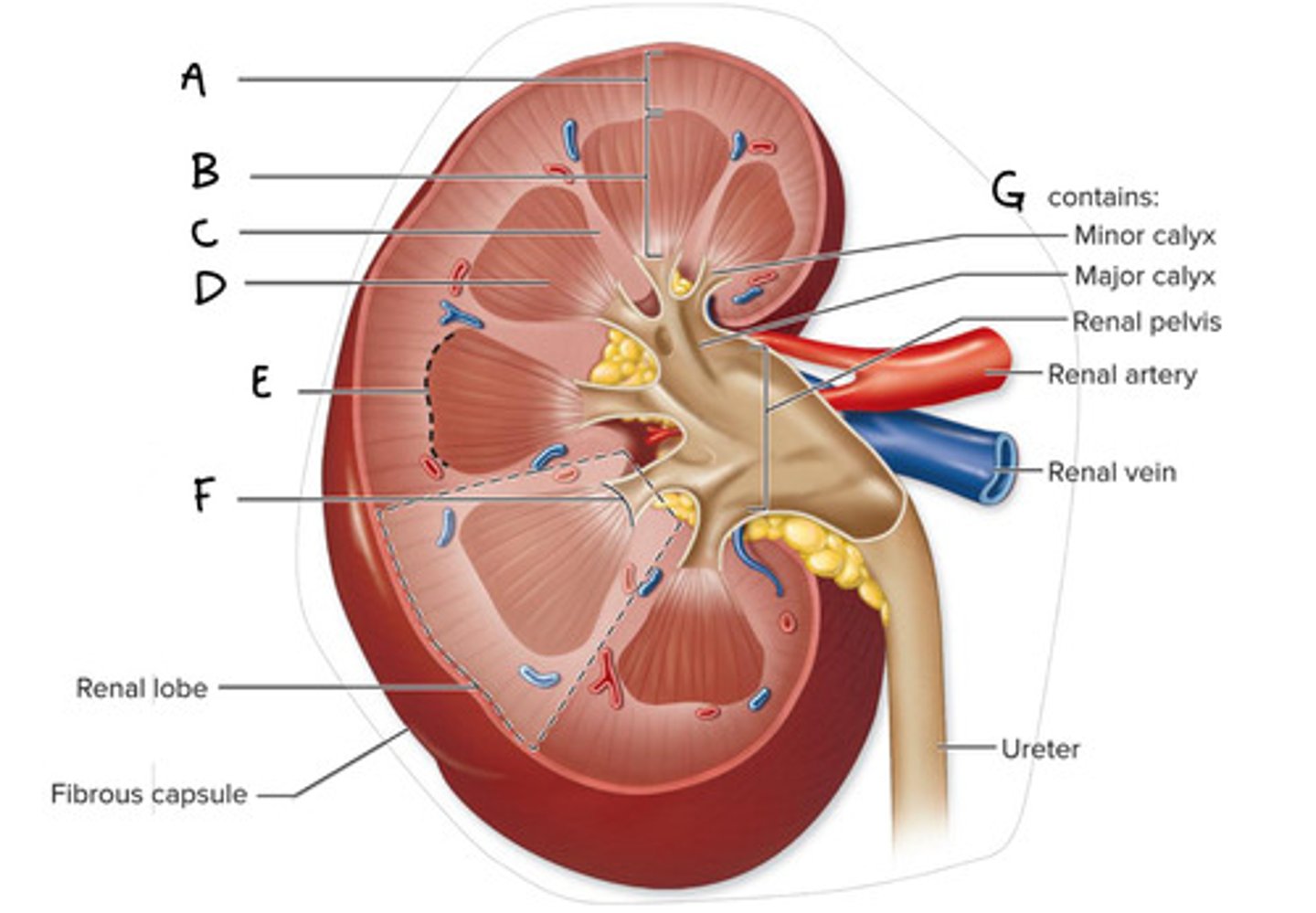
Renal Papilla (Diagram)
What is F on the diagram?
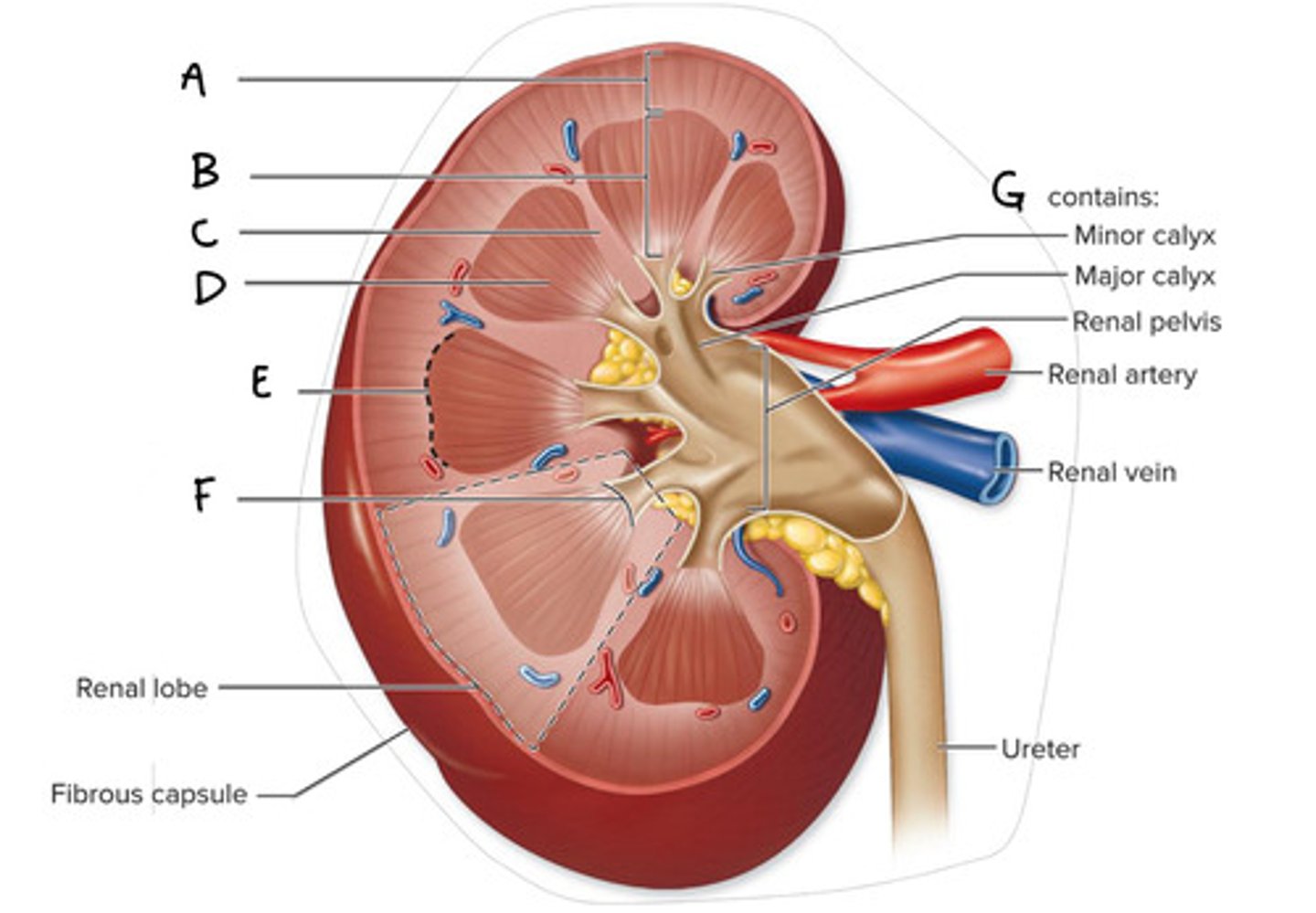
Renal Sinus (Diagram)
What is G on the diagram?
Corticomedullary Junction
the wide base of the renal pyramids
external edge of the medulla, where it meets the cortex
Renal papilla
medially directed tip of the renal pyramid
Each kidney also contains a medially located space called
renal sinus
the Renal sinus of the kidney
urine drainage area
minor and major calyces and renal pelvis
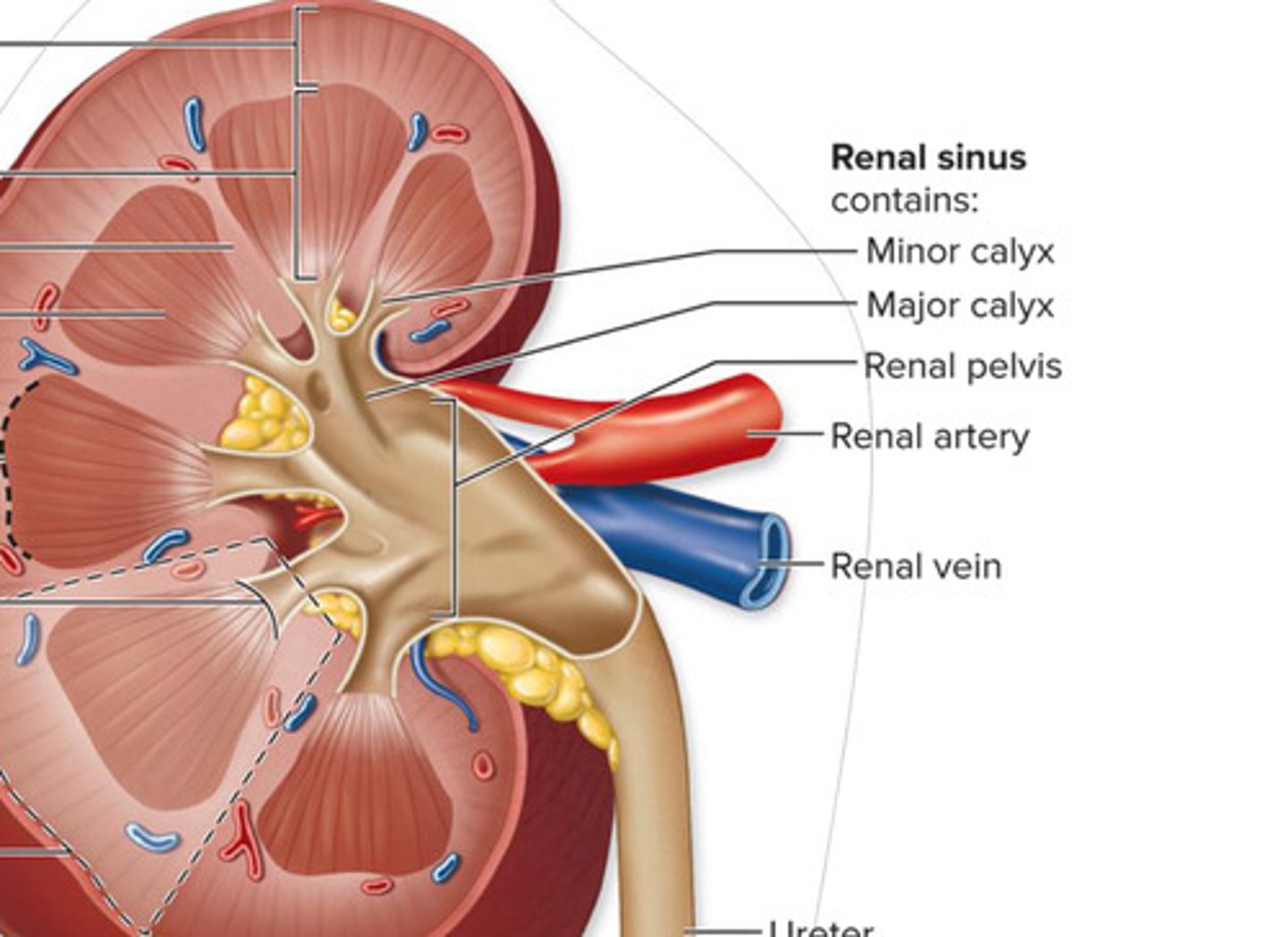
The Functional anatomy of the kidney includes
nephrons
collecting tubules
collecting ducts
and other associated structures
Nephron
microscopic, functional filtration unit of the kidney
Each nephron consists of 2 major structures
a renal corpuscle and a renal tubule
Almost all renal corpuscles and renal tubules
reside in the cortex (outer region)
Renal corpuscle
an enlarged, round portion of a nephron housed within the renal cortex
composed of 2 structures: glomerulus and glomerular capsule
2 structures that make up the renal corpuscle
glomerulus
glomerular (Bowman's) capsule
the glomerulus and bowman's capsule are only found in the
cortex
Nephron diagram
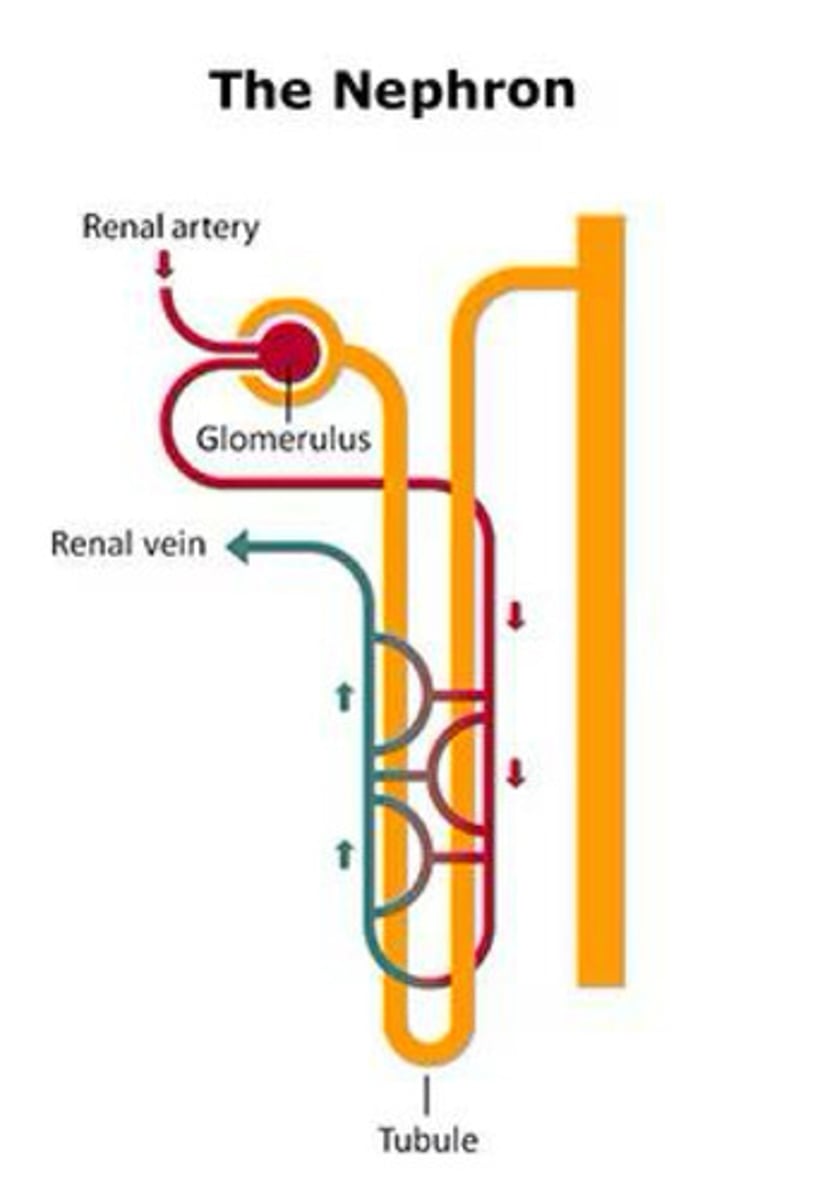
Nephron diagram 2 (Note the Bowman's capsule and Glomerulus!)
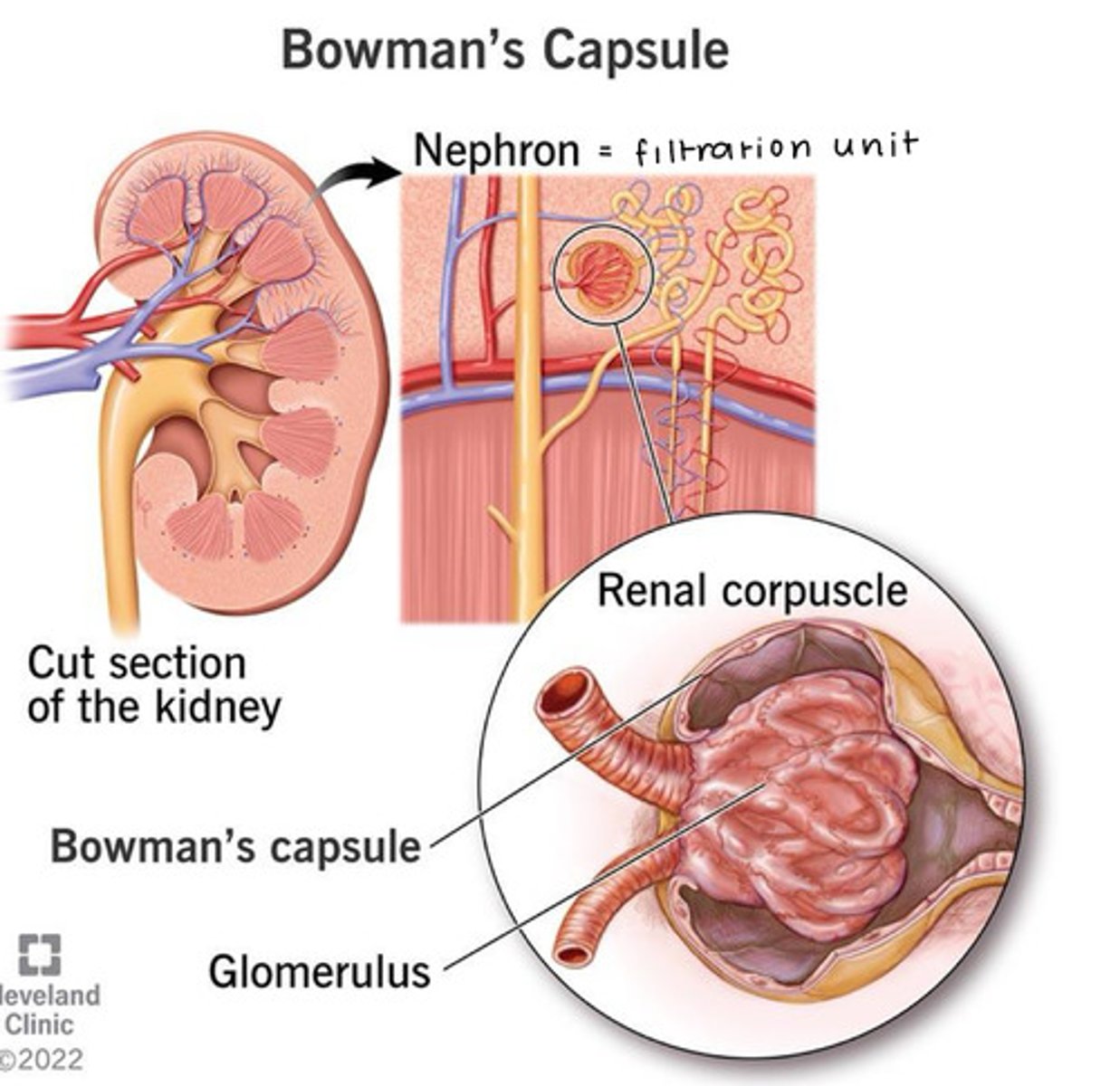
Glomerulus
a thick tangle of capillary loops (glomerular capillaries)
blood enters the glomerulus by an ________ arteriole and exits by an ________ arteriole
afferent; efferent
Glomerular (Bowman's) Capsule is formed by 2 layers:
visceral and parietal
Between the visceral layer and parietal layer of the glomerular capsule is a
capsular space that receives filtrate, which is then modified to form urine
Your renal corpuscle has 2 opposing poles, what are they?
the vascular and tubular poles
the vascular pole of the renal corpuscle is where the
afferent and efferent arterioles are attached to the glomerulus
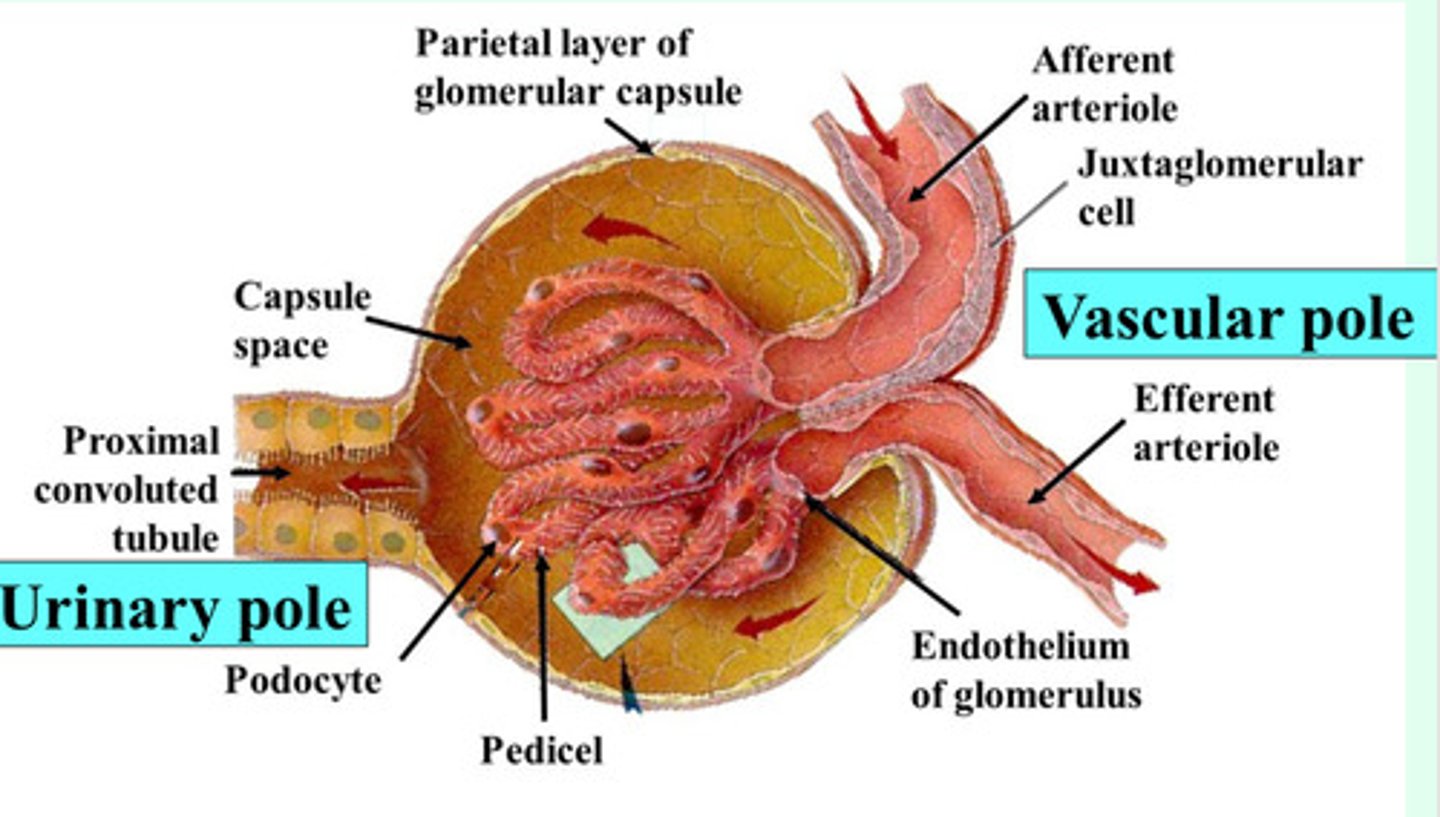
the tubular pole of the renal corpuscle is where the
renal tubule originates
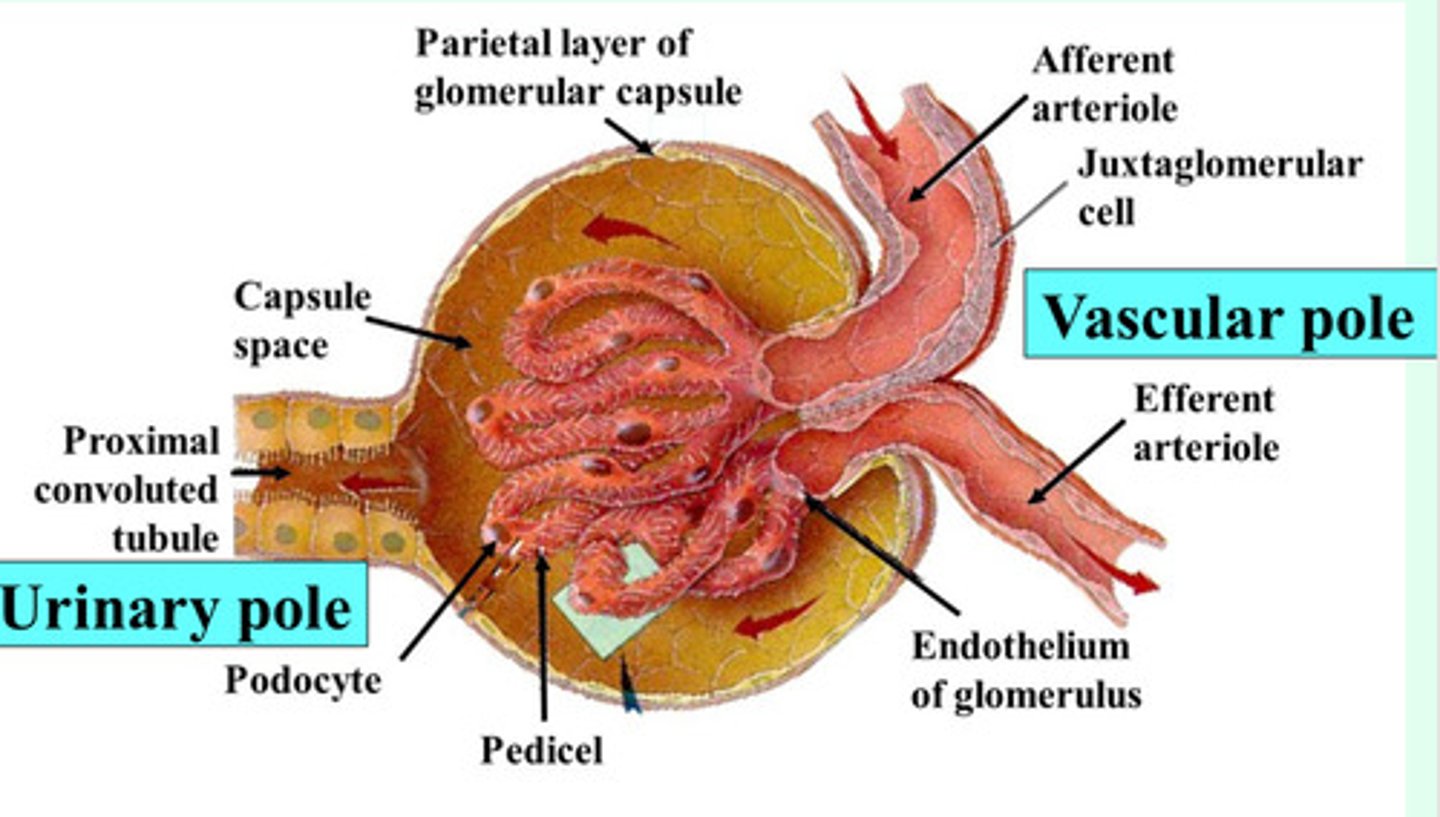
The renal tubule makes up the remaining part of the nephron and consists of 3 continuous sections
the proximal convoluted tubule (PCT)
the nephron loop (loop of Henle)
the distal convoluted tubule (DCT)
the convoluted tubules usually reside in the
cortex
the loop of Henle typically extends
from the cortex to the medulla
(Lecture 2 Fun fact) UTIs are more common in
women than in men
One of the reasons for this is because they have shorter urethra (easier for bacteria to reach your bladder)
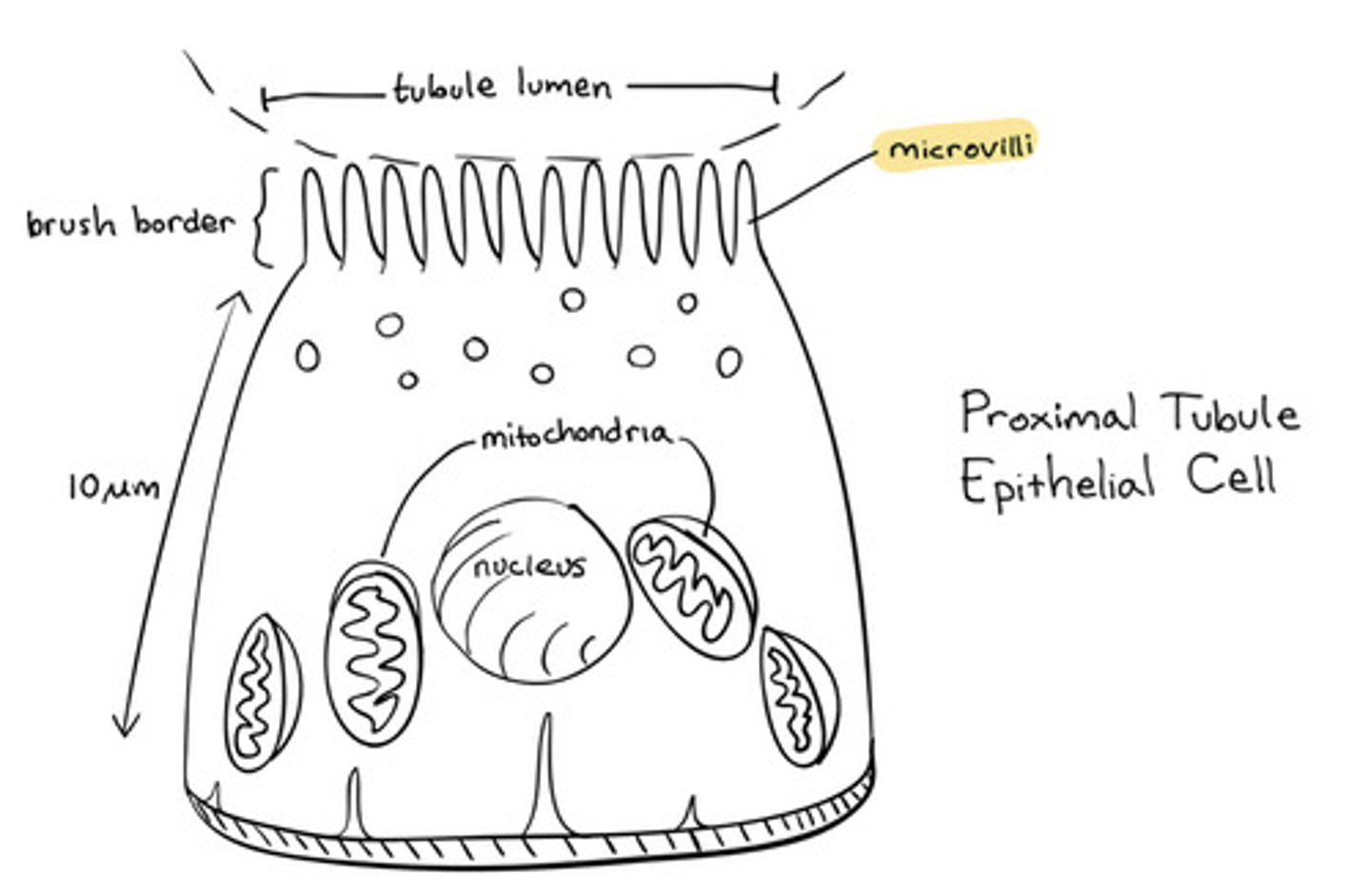
The proximal convoluted tubule (PCT)
the first region of the renal tube
originates from the tubular pole (simple cuboidal epithelium with apical microvilli)
brush border
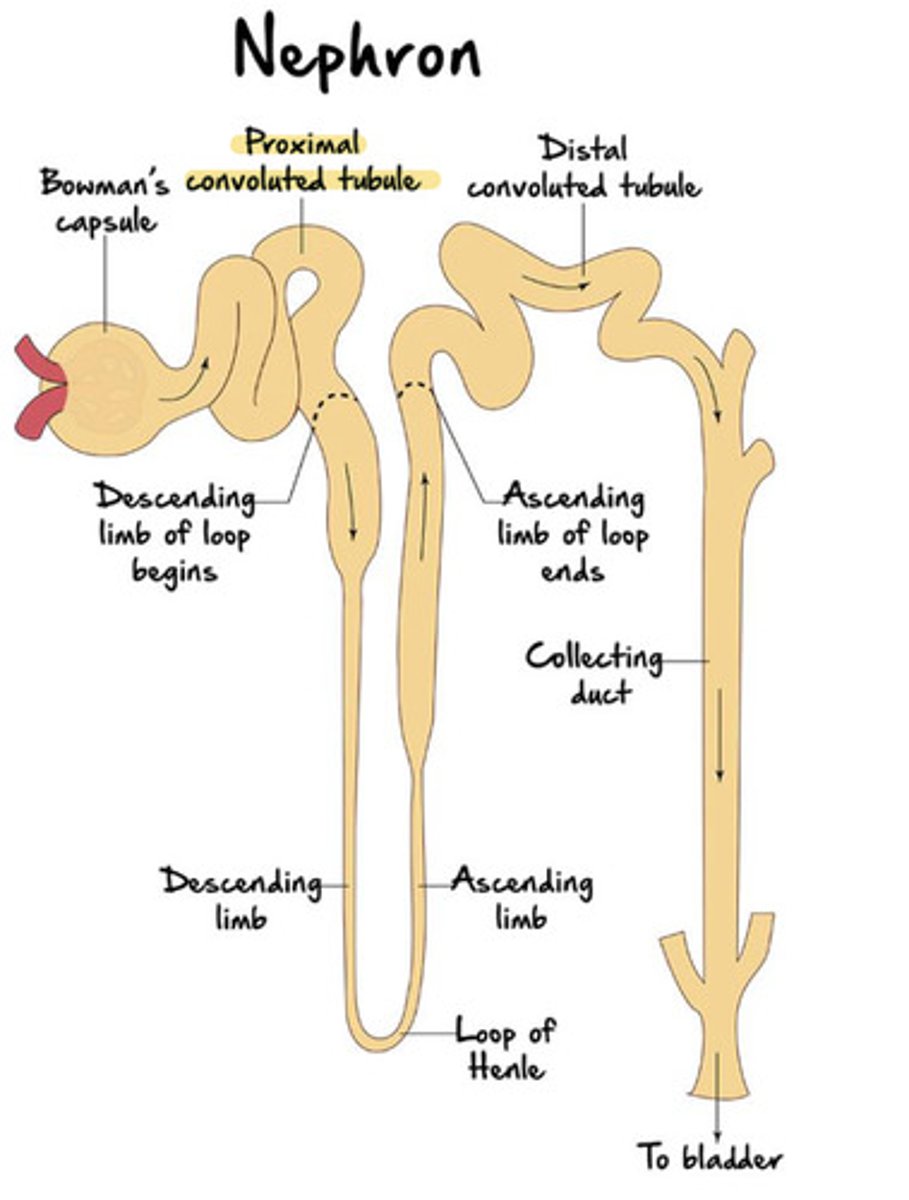
The microvilli of the proximal convoluted tubule are for
Reabsorption
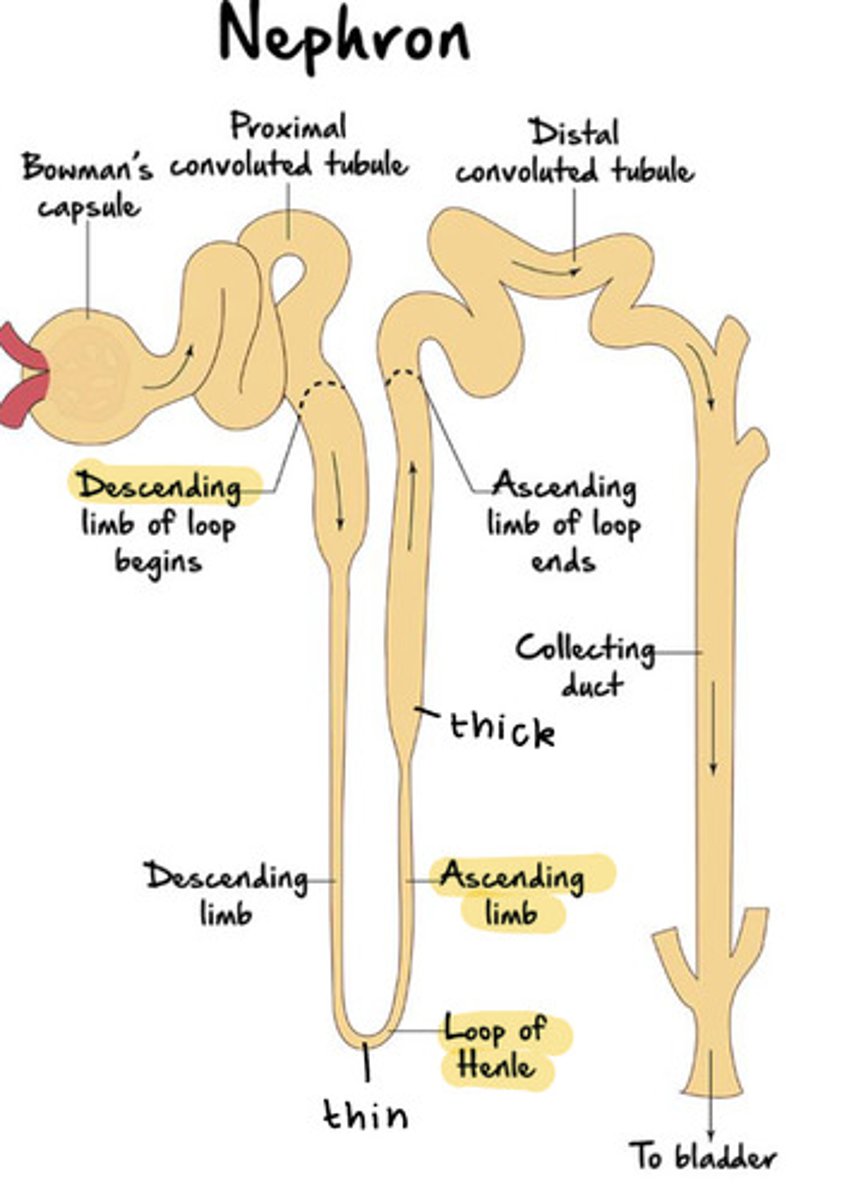
Loop of Henle (Nephron loop) consists of two regions
ascending and descending limbs that are continuous at a hairpin turn within the medulla
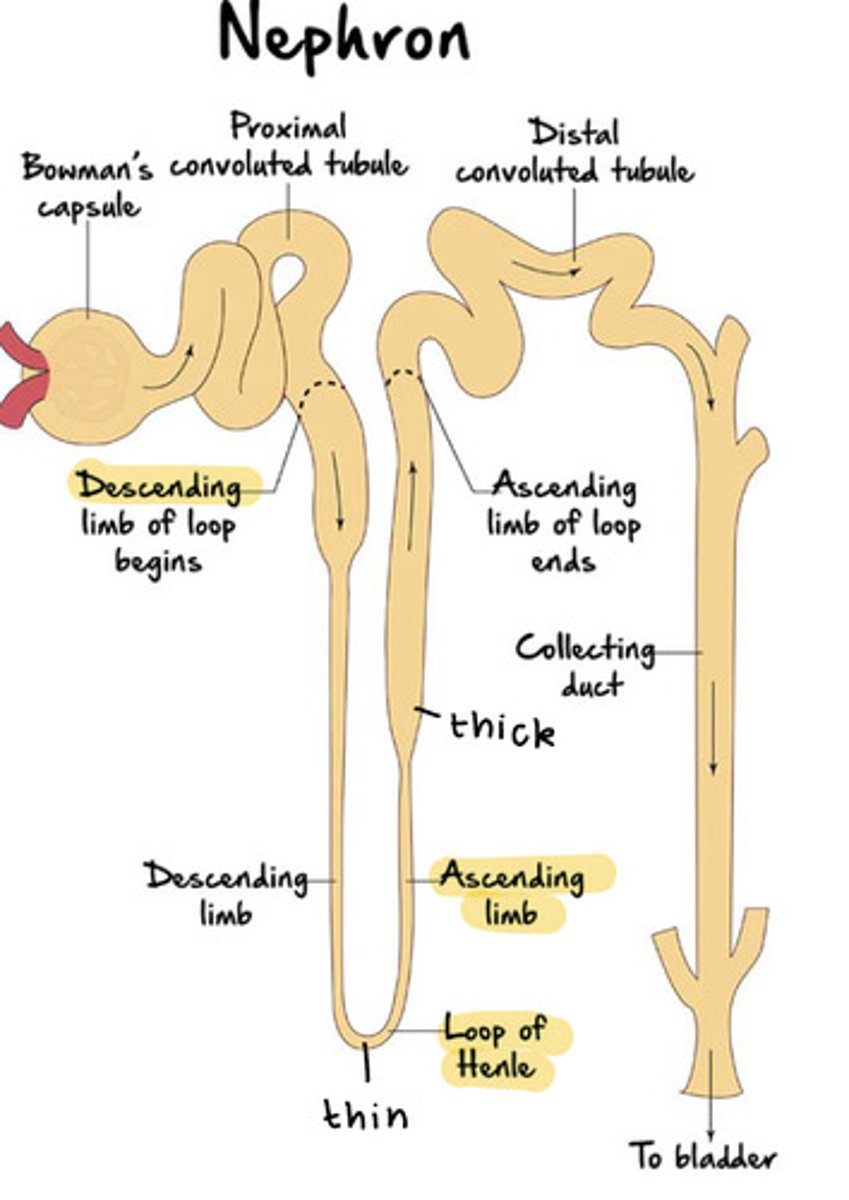
The loop of henle consists of
thick and thin regions as well
Distal Convoluted Tubule (DCT)
originates in the renal cortex at the end of the loop of Henle's ascending limb and extends into a collecting tubule
also composed of simple cuboidal epithelium (like the PCT), but have sparse, short, apical microvilli
for this reason, they do not have the "fuzzy edge" when looked under the microscope
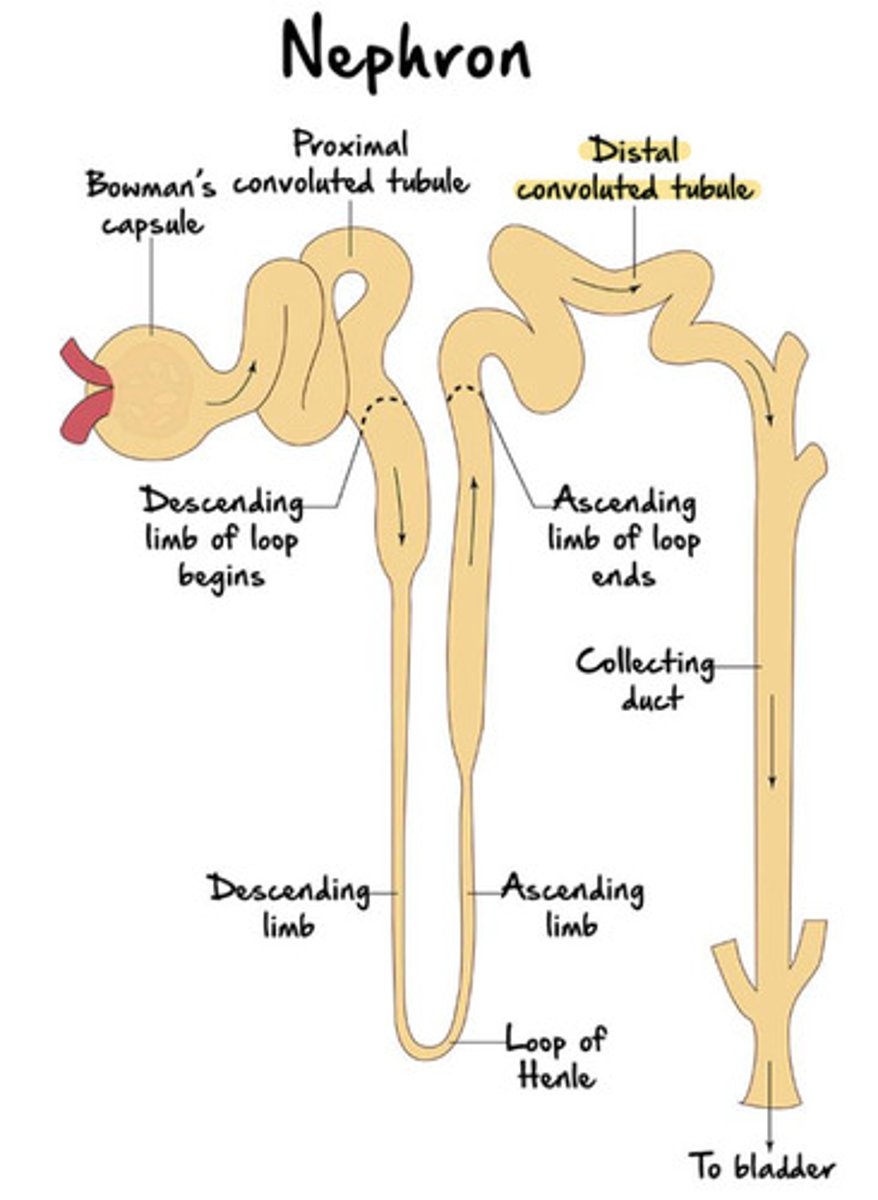
Why does the DCT not have the "fuzzy edge" seen under a microscope?
Because reabsorption primarily happens in the PCT
Cortical nephron: where is its renal corpuscle located?
renal corpuscle located near the edge of the cortex
Cortical nephron: Loop of Henle
short loop of Henle that barely penetrates the medulla
Cortical nephrons make up __% of nephrons
85
Juxtamedullary nephrons make up __% of nephrons
15
Juxtamedullary nephrons: where is its renal corpuscle?
renal corpuscle is adjacent to the corticomedullary junction
Juxtamedullary nephrons: loop of Henle
long Loop of Henle deep into the medulla
Cortical nephron vs Juxtamedullary nephron (Diagram)
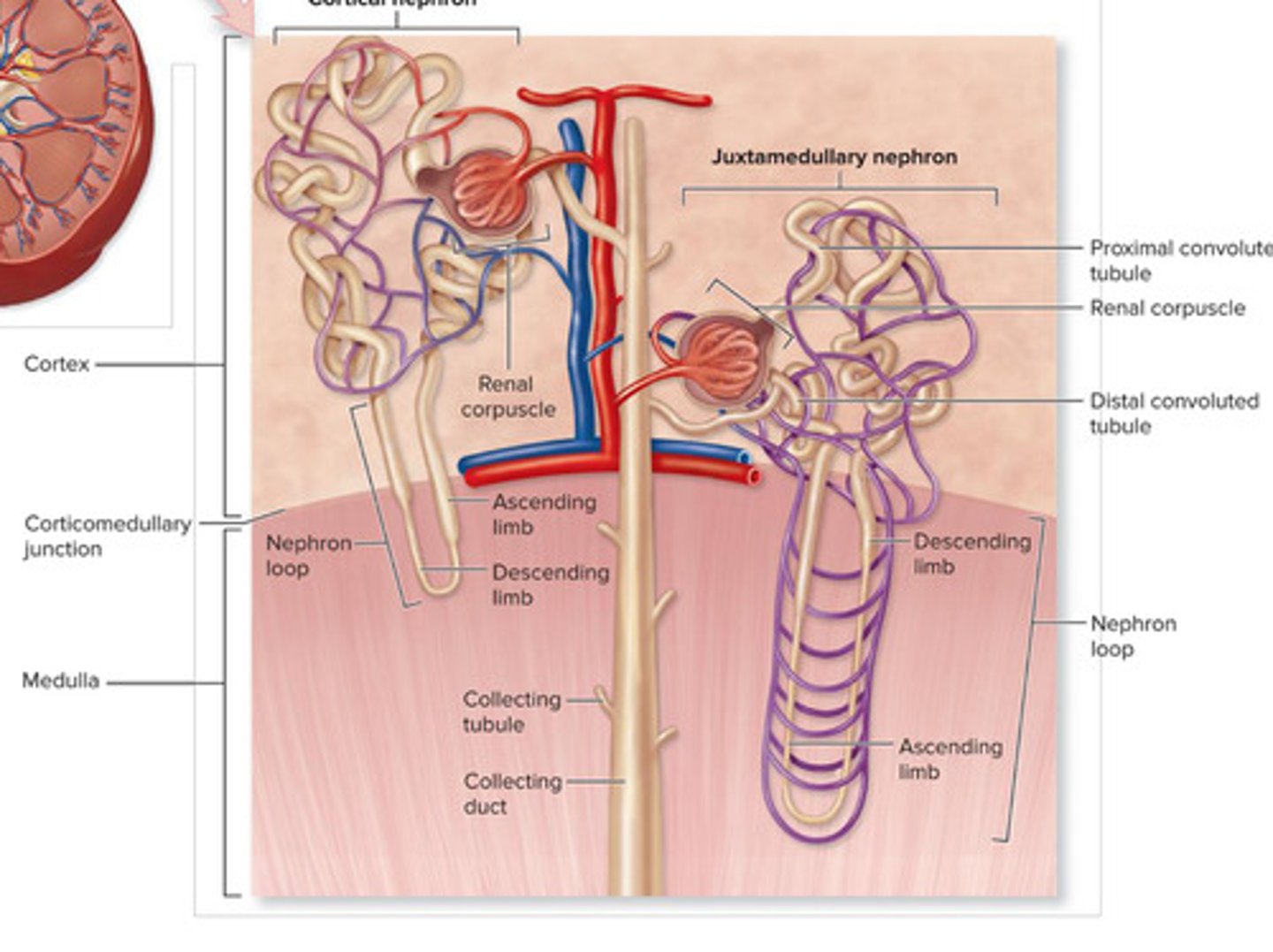
Several nephrons drain into each
collecting tubule
Each kidney has thousands of collecting _______, and they eventually empty into larger collecting _____
tubules; ducts
the collecting ducts and tubules both project through the renal medulla toward the
renal papilla
The collecting ducts then drain into a
papillary duct
Where are papillary ducts found?
within the Renal Papilla
Then, from the papillary ducts, it is drained to the
minor calyx