Microbio Quiz #4 - Chapters 15, 16, and 17.1
1/106
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
107 Terms
Immunity
What is the ability to resist infection (Team effort, in a two-tiered approach)
Innate immunity (nonspecific immunity)
This form of immunity is the non-inducible (hard-wired or inborn) ability to recognize and destroy an individual pathogen or its products. DOES NOT require previous exposure
Lysozyme
An example of innate immunity can be found with this enzyme that is found in various body fluids, including tears, salvia and egg white. This enzyme weakens the cell wall (peptidoglycan) and causes the bacteria to burst and die)
Adaptive immunity (specific immunity)
This form of immunity is the acquired ability to recognize and destroy a particular pathogen or its products. It depends on previous exposure (specificity) and is directed toward an individual molecule component of the pathogen (antigen)
Barriers to infection in the human body (examples that inhibit microbial growth and prevent pathogen infection and invasion)
Removal of particles, skin, stomach acidity (pH 2), normal microbiota, flushing of urinary tract, lysozyme, mucus and cilia lining trachea, mucus antibacterial peptides and phagocytes, blood and lymph, rapid pH change, epithelial cells are all examples of?
Innate and Adaptive
What are the two branches of immunity?
Innate
Which branch of immunity is classified as the first line of defense, immediate response, not specific, present before birth and always on from the time of infection, through the incubation period and until the infection ends?
Adaptive
Which branch of immunity is classified as specific to its target, slower to activate, must “see” the antigen, and generates memory cells?
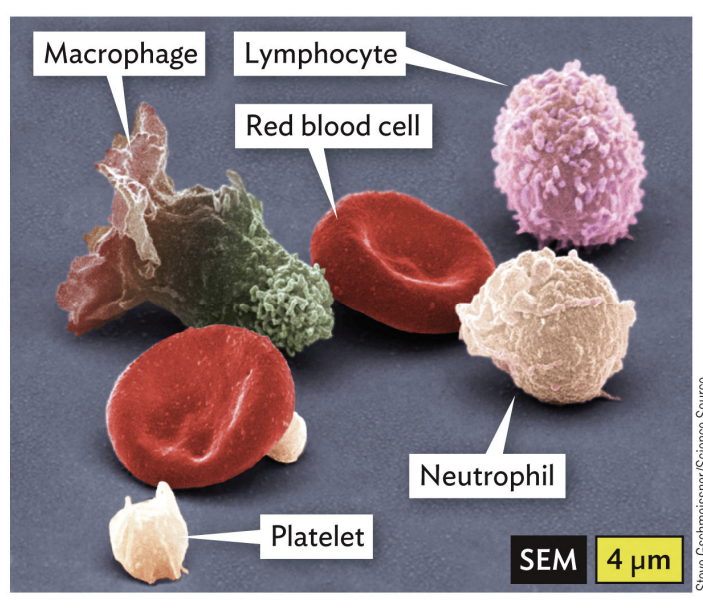
White blood cells (WBCs) of innate immunity
Polymorphonuclear leukocytes (PMNs), monocytes, macrophages, dendritic cells and mast cells are all examples of?
Hematopoietic stem cells (HSCs) in the bone marrow
Cells of the innate and adaptive immune system stem from what?
Eosinophils, basophils, and neutrophils (found in BLOOD)
What are the 3 types of Polymorphonuclear leukocytes (PMNs) (granulopoiesis)?
Macrophages and dendritic cells (found in TISSUE)
What are the 2 types of monocytes (circulating WBCs/monocytopoeisis)?
Mast cells
These cells contain many granules rich in histamine and heparin, help with inflammation and wound healing. Unlike PMNs, they reside in connective tissues and mucosa and DO NOT circulate in the bloodstream
Neutrophils
These PMNs make up nearly all WBCs in the blood and can engulf microbes by phagocytosis (destroying large particles)
Basophils and eosinophils
These PMNs phagocytose (engulf) less efficiently than neutrophils and release products that are often toxic to the microbe
Monocytes
These WBCs circulate in the blood, engulf foreign materials and differentiate into macrophages and dendritic cells
Macrophages
A type of monocyte that is widely distributed throughout the body, phagocytose and are present on antigens on cell surface to T cells
Dendritic cells
These cells are another type of monocyte located in the spleen, lymph nodes and langerhans in skin. They phagocytose and present SMALL antigens on their cell surface to T cells and are different from macrophages in structure
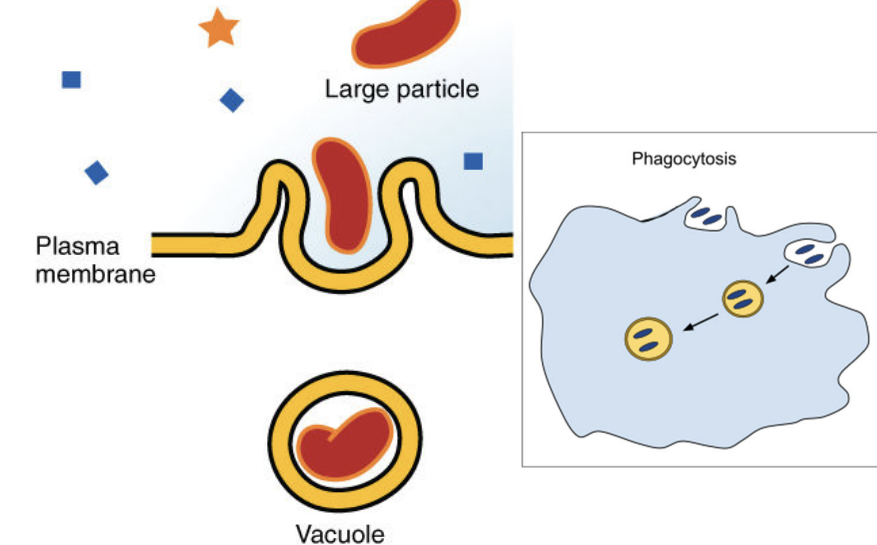
Phagocytose (phagocytosis) (“see” particle as foreign or self)
The process by which a phagocyte (a type of white blood cell) surrounds and destroys foreign substances (such as bacteria) and removes dead cells
Steps of phagocytosis (an immune cell is eating the germ it grabs it, swallows it, digests it, and spits out the trash)
1. A bacterium (germ) sticks to the outside of the immune cell (phagocyte)
2. Immune cell sees its "arms" (pseudopods) to reach out and grab the germ
3. The immune cell wraps around the germ as it gets pulled inside forming a bubble called a phagosome
4. Destruction begins with a lysosome (digestive chemicals inside the cell) that fuses with the bubble and forms a phagolysosome.
5. Germ is broken down as the lysosome releases enzymes and chemicals into the bubble which break down the germ, cutting it into harmless pieces.
6. Lastly, waste is released as the broken pieces of the germ (called debris) are released out of the immune cell.
Phagocytosis and opsonization
What are the two main ways to recognize alien cells and particles?
Opsonization
When recognizing alien particles, this process occurs when antibodies coat pathogens and help with phagocytosis (encapsulated organisms are HARDER to phagocytose). Extracellular bacteria approach macrophage, the antibodies bind to bacteria and the Fc portion of the antibodies binds to receptors on the macrophage surface as the antibodies then link the bacteria and macrophage aiding phagocytosis
4,500 - 11,000 /ul
What is the normal Total WBC count in a sample?
12,000 - 30,000
What is the elevated total WBC count for acute bacterial infection?
54%-62% (During acute bacterial infections, increased # and more immature forms (band cells) and can be reduced during viral infection)
Neutrophils: Normal total WBC count
1-3% (parasitic infections and allergy increased)
Eosinophils: Normal total WBC count
0-0.75% (allergy increased)
Basophils: Normal total WBC count
25-33% (viral infections incrased)
Lymphocytes: Normal total WBC count
3-7% (typically increase with chronic infections)
Monocytes: Normal total WBC count
Extracellular pathogens (live OUTSIDE host cells)
In bacterial infections, most bacteria are ______
Innate immunity (phagocytosis)
In bacterial infections, the immune system relies mainly on ______
Neutrophils
In bacterial infections, ______ are the primary responders that engulf and destroy bacteria
Macrophages
In bacterial infections, these form of monocytes also participate in phagocytosis and inflammation
Neutrophilia (increase in neutrophils in blood)
What is the result of bacterial infections?
Viral
What infection relies more on adaptive immunity?
Intracellular pathogens (they replicate INSIDE host cells)
In viral infections, most viruses are ______
Cell-mediated immunity (T and B lymphocytes)
In viral infections, the immune system must use _________
Cytotoxic T cells (CD8+)
In viral infections, _______ destroy virus infected cells
Helper T cells (CD4+)
In viral infections, ______ activate cytotoxic T cells and B cells
B cells
_____ produce antibodies that neutralize free viral particles
Lymphocytosis (increase in lymphocytes in blood)
What is the result of viral infections?
Inflammation
What is defined as a localized response to tissue injury or infection that helps contain and eliminate pathogens?
Bring immune cells and molecules to the infection site and promote healing to prevent spread of infection
What is the purpose of inflammation?
Pathogen-associated molecular patterns (PAMPs) recognized by immune cells (via TLRs) and cytokine release (IL-1, TNF-α, IL-6).
What is inflammation triggered by?
Redness (increased blood flow), Heat (increased metabolism and blood flow), Swelling (fluid and immune cell accumulation), Pain (chemical mediators stimulating nerves), and Loss of function (result of pain and tissue damage, limiting normal movement or activity)
What are the 5 cardinal/key signs of inflammation? HERPA
Mast cells (release histamine to increase vascular permeability) and Neutrophils and macrophages (migrate to the site (chemotaxis) and phagocytose pathogens)
What are the 2 main immune cells involved in inflammation?
Infection (microorganisms grow and produce cell damaging compounds) and macrophages (phagocytosis and release inflammatory mediators and cytokines to communicate with other cells)
What are examples of signals leading to inflammation?
Vasoactive factors
These increase vascular permeability by loosening tight junctions between epithelial cells leading to the initiation of dilation
The host becomes infected via a splinter and resident macrophages engulf pathogens and release cytokines
What is the first step of extravasation (acute inflammation)?
Extravasation
The movement of neutrophils through capillary vascular walls
Vasodilation
This slows blood flow and as a result increases blood volume in the affected area. The more permeable vessel allows the escape of plasma into the tissues
Localized swelling, redness, and heat
Both vasodilation and extravasation cause what 3 symptoms?
Vasoactive factors
What stimulate local nerve endings causing pain
Chronic inflammation
What results from the persistent presence of a foreign body causing permanent tissue damage?
Causes of chronic inflammation
Infection (mycobacterium TB, actionmyces bovis survive in macrophages) that continually stimulate the basic inflammatory response, nonliving irritant material, wood splinters, asbetos particles, and surgical implants are all?
Granuloma
These are a structured collection of immune cells that walls off a persistent pathogen the body cannot eliminate the body’s attempt to wall off infection/irritant
Innate mechanisms are present at birth, but adaptive mechanisms develops after exposure to a antigen
What is the main difference between innate immunity mechanisms and adaptive immunity mechanisms?
Complex and slow development, cross-regulated defense network, memory response
What are the 3 keys properties of adaptive immunity?
Does not recognize the whole microbe
The immune system _________, it recognizes innumerable pieces of it
Antigen
These are anything that can elicit an immune response (If the antigen itself can elicit an immune response it is termed an immunogen)
Immunogen
If the antigen itself can elicit an immune response it is a ____
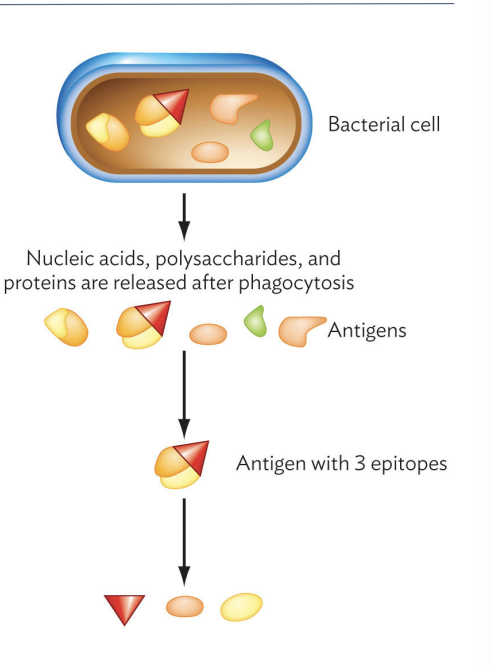
Epitope
These have specific binding sites on an antigen (can have more than one)
Engulf a microbe and break it down into component antigens
The adaptive immune response begins when cells of the innate immune response _____
Antigen presenting cells (APCs)
These phagocytic cells are called ______ (dendritic cells and macrophage)
Major histocompatibility complex MHC proteins
APCs place antigen and epitopes on their cell surface called _____ in order to present to the T lymphocytes
True
T/F: The display of antigens on MHC happens all the time in the background even in uninfected cells
B and T cells (antigen reactive leukocytes, white blood cells, cells that circulates in the blood and body fluids and is involved in counteracting foreign substances and disease)
What are the two types of lymphocytes (adaptive immunity cells)
B cells (antibody-mediated or humoral immunity)
These types of cells produce antibodies and work against EXTRAcellular antigens during both cell-mediated and humoral immunity
T cells (cell-mediated immunity)
During cell-mediated immunity, these produce antigen specific receptor proteins on their surfaces and are against INTRAcellular antigens
Humoral and Cell-mediated
What are the two forms of adaptive immunity?
Humoral (form of adaptive immunity)
This form of adaptive immunity contains antibodies (proteins that circulate in the bloodstream and recognize foreign structures called antigens) and plasma cells (B cells that have been stimulated by antigen to produce antibodies)
Cell-mediated (form of adaptive immunity)
During this form of adaptive immunity, T cells recognize the antigen and can stimulate B cells + destroy infected host cells
Cytotoxic T cells and Helper T cells
What are the two types of cells in cell-mediated immunity?
Cytotoxic T cells (TC cells) KILL the infected host cell
These cells bind antigen presented on antigen-presenting cells. Upon activation, these cells leave the lymph node and find host cells presenting the same antigen
Helper T cells (TH cells)
These cells link the two forms of adaptive immunity and DETERMINE whether antibody or cell-mediated mechanisms will predominate in response to an antigen
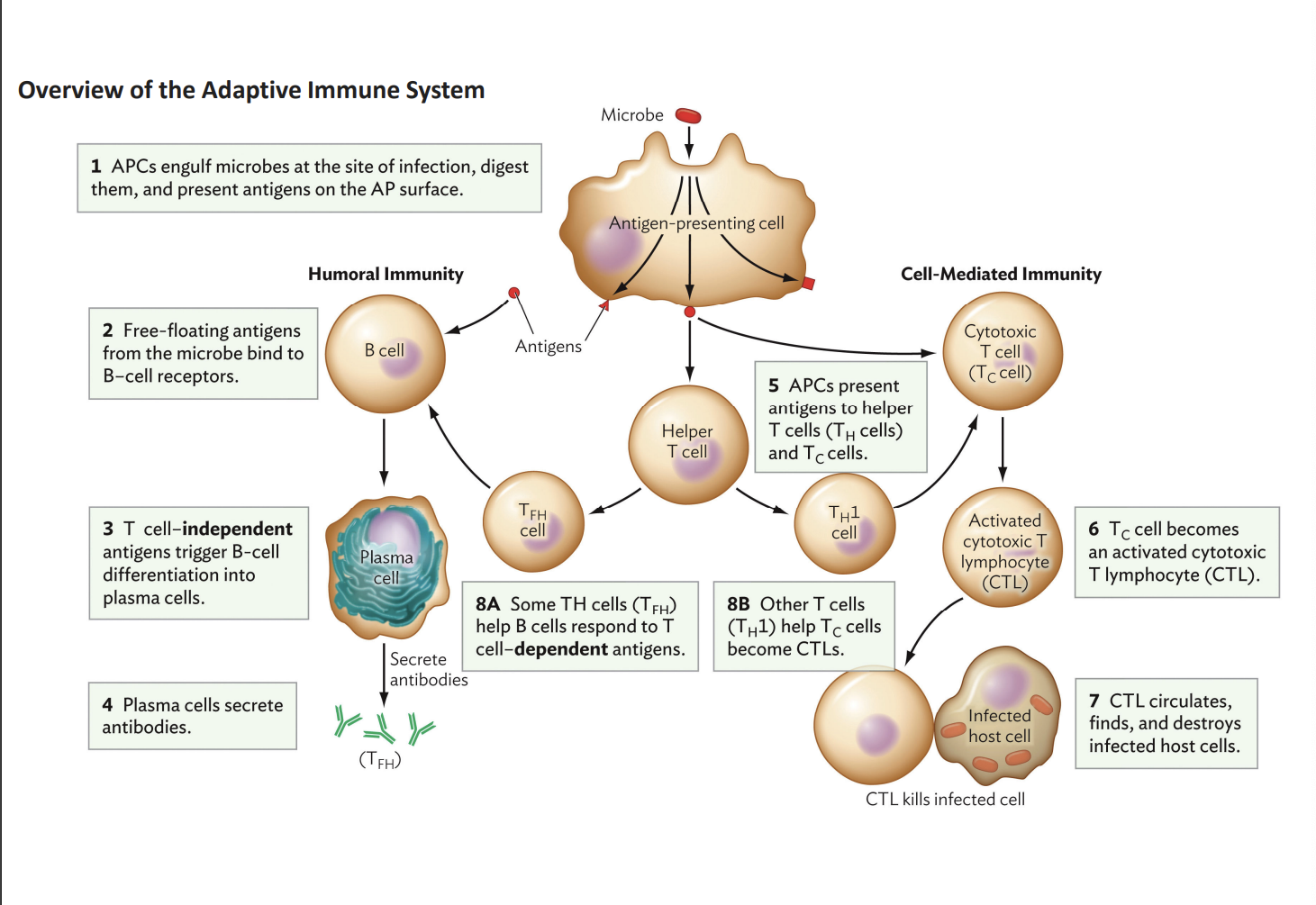
B cells (to make antibodies) and T cells (to kill infected cells)
The adaptive immune system defends your body by recognizing and attacking specific germs (microbes) by using what two types of cells?
Phagocytosis (phagocytes release the antigen and the phagocyte displays the antigen on special molecules called MHC)
The immune system recognizes a microbe by the release of antigen by phagocytes or antigen presentation during ____?
Flags them
During humoral immunity, the antibody coats pathogens and ______ for destruction by other cells in the immune system
Clonal selection
What occurs when an activated B cell proliferates into many clones or copies of itself and thus can turn to plasma cell faster?
Naive B cells
What type of cells never encountered an antigen?
F(ab) 2 region (antigen binding sites differ some bind peptidoglycan only vs another antigen)
This region contains antigen binding sites and highly variable amino acid sequences
Variable regions (VL and VH)
In the chains of antibodies, these regions are where binding is REVERSIBLE and contains non-covalent bonds (ionic or hydrophobic bonds)
FC region
This region is known as the tail in every antibody important for anchoring antibodies to the surface of certain host cells. Ultimately, the region binds receptors on host cells
Primary antibody response
During this response, an antigen binds to B-cell receptor (SPECIFIC to that particular antigen) and the B cell is activated and begins to proliferate and differentiate into a plasma cell (antibody secreting and memory cells)
Endoplasmic reticulum
The plasma cell cytoplasm is stuffed with _____ needed to support the incredible increase in protein synthesis associated with antibody production
Secondary antibody response
This response is the basis of immunization and takes place after B-cell activation (memory cells are generated). When memory B cells encounter an antigen again they quickly trigger a robust _______?
Antigen presentation with antigen-presenting cells (APCs)
For T Cells to recognize antigens, T-cell activation requires ______?
Class I and II MHC molecules
What are the two types of molecules for major histocompatibility complex (MHC) proteins present antigens
Class I MHC molecules
These are found on all nucleated cells (NOT red blood cells)
Class II MHC molecules
These are found only on dendritic cells, macrophages, and B cells
MHC class I and II presentation
What are examples of two presentation that allow T Cells to recognize antigens by processing and presentation?
MHC class II presentation
During antigen presentation, extracellular pathogens (pathogens that are phagocytosed) take part in digestion and are presented on MHC class II molecules
MHC class I presentation
During antigen processing, intracellular pathogens grow in the cytoplasm of the cell, degrade, and are presented on MHC class I molecules
In the thymus
Where are T cells developed?
CD8 cytotoxic T cells and CD4 T helper cells
What are the two types of T-cell receptors in the adaptive immune system?
CD8 cytotoxic T cells
These receptors are also known as killer T cells and are a type of white blood cell that kill infected or cancerous cells by releasing toxic molecules
CD4 T helper cells
These cells modulate humoral and cell-mediated immunity, stimulates B-cell to differentiate into plasma cells or facilitates Tc to CTL conversion
T cell receptor (TCR)
This binds antigen on the surface of T cells, it binds peptides (antigen) within MHC molecules and is associated with the CD3 complex (cell signaling)
Clonally selected cells to multiply
When TCR binds to MHC antigen complex, CD3 signals proliferation of T cells causing what?
Active cytotoxic T cells (TC) kill infected cells
During cell-mediated immunity, these cells _______. Every cell has MHC I molecules except red blood cells. The MHC I displays bits of the cell’s own proteins and infected cells present on viral proteins (antigen) as a result of viral infection and replication