Metabolism & Nutrition Basics of Nutrition & Obesity
1/57
Earn XP
Description and Tags
Test 3
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
58 Terms
Why do nutritional requirements change?
Nutrient requirements change throughout the lifespan in relation to growth/development, activity, and changes in metabolism and body composition
Nurses’ role when it comes to nutritional requirements
Assessment of patients’ usual patterns
Health promotion
Patient/family education
Pregnancy & Lactation
Weight gain occurs during pregnancy
Adequate nutrition during pregnancy is essential
Pregnant women should avoid caffeine, alcohol, unpasteurized dairy (bacteria), raw eggs (bacteria), or undercook fish/processed meats (bacteria)
When who are pregnant/lactating should ask their healthcare provider which medicines are safe to take during pregnancy
The need for most vitamins and mineral (folic acid and iron) increases during pregnancy and lactation
Prenantal vitamins
Infants
Most rapid period of growth
Breastfeeding is recommended as the major source of nutrition for the first 6 months
Has all the essential the baby needs and antibodies
Cow’s milk is not recommended for infants under the age of one year
Could cause GI bleeding
Solid food introduced at about 6 months
New food should be introduced one a t a time over a 5-7 day period to obese for indications of allergy to intolerance
Reduced allergies, asthma, or eczema as well as other things throughout life
Toddlers & Pre-Schoolers
Growth rate slows
Mobility, coordination, muscle mass, and bone density increase
Can usually feed themselves and verbalize food like/dislikes (develop attitudes toward food)
Learn from parents
Children this age often have inadequate intake of fruits and vegetables, and/or excessive intake of sweetened fruit drinks
Know normal schedule
Know normal intake
Encourage excesses throughout the day
School-aged Children
Children have erratic growth patterns
By about age 12 or 13, most kids have lost all their baby teeth and have a full set of permanent teeth
Digestive system matures
Pre-adolescent growth-spurt
Socialization and independence increase
Advertising had an impact on children’s food choices
Adolescents
Period of rapid maturation (puberty/growth spurt)
Girls: menstruation, fat deposition
Boys: increase the muscle mass, lean tissue, bone growth
Nutritional requirements increase during puberty
Adolescents are likely to consume inadequate amounts of fruits, vegetables, and dairy products
Exercise: sports, play outside, life weights (after hitting puberty)
Adults
Growth ceases
Decline in basal metabolic rate each decade
Nutritional needs level off → few calories needed
Weigh gain results if adjustments in caloric intake are not made
*Even if you are healthy, depending on your diet you can become obsess
Older adults
Decrease in physical activity
Loss of lean body mass
Loss of teeth can make chewing more difficult
Decrease in peristalsis can result in constipation
Increase fiber and water to avoid this
Caloric needs decrease
Need for nutrients increase
Risk for malnutrition (chronic illness, limited income, islcaotion, age related physiologic changes)
Cultural & Religious Consideration when it comes to Nutritional Requirements
Special food preparations (Kosher → Separate their dairy from their meat)
Restrictions on meat intake (Islam, Orthodox Judaism)
Fasting on religious holidays (Ramadan for Muslims, Ash Wednesdays/Lent for Catholics)
Cultural & Religious Consideration - Nursing Implications
Assess patient’s dietary restrictions/food preferences
Picky eaters
Ask patient about folk/home remedies
Onions = cold/respiratory
Garlic
Teas
Honey = vocal are, allergies, antibacterial properties
Integrate cultural food preferences into the patient’s diet
Encourage family involvement (may bring in food from home if prescribed diet and hospital policy permits)
Metabolism
Process of changing foods into energy to fuel body functions
Nutrients
Substances used by the body for growth, development, activity, reproduction, lactation, health maintenance, and recovery from illness or injury
Calories
Calories are the energy that is stored in food and used for body processes
A general guideline for the average adult is approximately 2000 calories per day to maintain their weight
Basal Metabolic Rate (BMR)
The number of calories necessary to maintain the body at rest
Get more coilers if you are active because you are burning more
Nutrition Facts
Servings : how many servings per that container
Calories : how much energy you get from a serving of that food
Nutrients : how much of every nutrient is in the package
Percent daily value (%DV) : 5% is low, 20% is high
Macro-Nutrients
Essential nutrients that supply energy/build tissue
Carbohydrates
Proteins
Fats
Micro-Nutrients
Needed in smaller amounts to regulate and control body processes
Vitamins
Minerals
Carbohydrates
What are they:
Composed of carbon, hydrogen, and oxygen
Make up approximately 45-65% of total daily calories
Sources:
Sugars
table sugars
fruits (sucrose)
Starches
grains (bread, pasta)
beans
fiber (vegetables, oatmeal)
Lactose
dairy products
Functions:
Converted to glucose (stored in liver) in bloodstream for used as energy
Hyperglycemia = too much glucose in blood → give insulin
Excess glucose = sotred as fat
Protein
What is it:
Composed of chains of amino acids (wound healing, muscle building)
Vital component of every cell in the body
Most adults require around 0.75g/kg/day of dietary protein
Sources:
Animal sources: dairy products, meat, poultry, fish, eggs
Plant-based: Peas/beans, nuts, soy products
Supplemtens: shakes, pills
Functions:
Provide energy
Tissue growth/repair
Regulate fluid balance
Form antibodies
Transport fats and other substances through the bloodstream
Regulate acid/base balance
Increase protein intake when they came out of surgery or have pressure injury → wound healing
Fats (Lipids)
What are they:
Lipids
Make up approx. 20-35% of total daily calories
Sources:
Triglycerides: Predominant form of fat in food. Major storage form of fat in the body
Snack and produced food
Saturated fats: Found mainly in animal sources (i.e., meat, dairy products-butter)
Bad fats (LDL)
Unsaturated fats: Usually found in plant sources (i.e., olive oil, avocado, nuts)
Good fats (HDL)
Trans-fats: Man-made fats. Found in processed foods. Commercial food processors add hydrogen to unsaturated fats (hydrogenation); this changes the fats into a more solid and stable form (purpose is to extend shelf-life for processed foods)
Changes how the body breaks it down
High in cholesterol
Functions:
Most concentrated source of energy in the diet
Hormone production
Form adipose tissue and protect internal nonagons
Provide insulation to main body temperature
Adi the body in absorption of fat-soluble vitamins
Cholesterol
What is it:
Fat-like substance found only in animal products
Component of cell membranes (brain & nerve cells)
It is not recommended to exceed more than 300 mg/day of dietary cholesterol
Functions:
Used to synthesize bile acids
Precursor of steroid hormones/Vitamin D
Types:
High-density lipoprotein (HDL): carries cholesterol from tissues to the liver, which removes it from the body
Removed from out body
Low-density lipoprotein (LDL): carries cholesterol to arteries and tissues
Build up causing atherosclerosis
Vitamins
What are they
Organic compounds “Coenzymes” which facilitate chemical reactions in the body
Functions:
Essential for the metabolism of carbohydrates, protein, and fat
Types:
Water soluble: B-Complex, C
Fat soluble: A, D, E, K
Vitamin A
Sources:
liver
carrots/egg yolks
fortified milk
milk with vitamins added in
Functions:
Important for vision, immune function, healthy skin
Elder adults need it most
Vitamin D
Sources:
Dietary sources
fish oils
fortified milk
fortified cereals
Non-food source
sunlight
Functions:
Important for calcium and phosphorus metabolism, bone strength
Bone fractures, osteoporosis, osteoarthritis
Vitamin E
Sources:
vegetable oils
wheat germ
whole grains
Functions:
Antioxidant- which prevents or delays some types of cell damage from exposure to “free-radicals
“Free-radicals” →increase chances of getting cancer
Red blood cell synthesis
Caution: if taking anticoagulants, don’t take vitamin E due to increase chances of bleeding
Vitamin K
Sources:
green leafy vegetables (i.e., spinach, lettuce)
synthesized in the intestines from gut bacteria
newborns are given a Vitamin K injection to prevent hemorrhagic disease
Functions:
Important for blood clotting
Caution: if you have a DVT, TE, bypass, or stents don’t take Vitamin K because we don’t want them clotting → taking Warfarin (Coumadin)
Vitamin B Complex
B1 Thiamine-Energy/Metabolism (glucose) → given for alcohol withdraw
B2 Riboflavin- Energy/Metabolism
B3 Niacin- Energy/Metabolism (treats high cholesterol and triglyceride levels)
B5 Pantothenic Acid- Metabolism
B6 Pyridoxine- Metabolism, hormone regulation, brain development/function
B7 Biotin- Metabolism
B9 Folate- Synthesis/repair of DNA and RNA, RBC production → pregnant women need to take to help with fetal development
B12 Cyanocobalamin-Metabolism/RBC synthesis (hemoglobin) → anemia
Vitamin C
Sources:
citrus fruits
berries
broccoli
peppers
Functions:
antioxidant
enhances iron absorption
Minerals
What are they:
Inorganic elements found in body fluids/tissues
Functions:
provide structure within the body
regulate body processes
Calcium
Sources:
dairy products
green (broccoli, spinach)
soy products
Functions:
important for bone formation, and muscle function (cardiac muscle contraction)
Phosphorus
Sources:
dairy products
meat
poultry
eggs
breads/cereals
soft drinks
Functions:
important for acid-base balance, and bone/tooth formation
Works with calcium
Magnesium
Sources:
green leafy vegetables
grains
beans/nuts
Functions:
bone/tooth formation, protein synthesis, carbohydrate metabolism, regularity in cardiac muscle contraction
Helps with patients who have arrhythmia
Sodium
Sources:
salt
processed foods (snack items, fast food)
Functions:
major role in acid-base balance, and fluid balance. when sodium levels are too high, it causes elevation in BP and fluid retention
Where sodium goes, water goes
Limit intake to less than 2,300 mg/day
Potassium
Sources:
fruits (banana, tomatoes, avocado)
leafy vegetables (spinach)
Functions:
important role in fluid balance/acid-base balance, cardiac muscle contraction
Too high or too low = increase risk of arrhythmia
Kidney failure = restrict intake
Chloride
Source:
Salt
Functions:
acid-base and fluid balance (linked with sodium levels), important for respiratory function and cardiac function (BP regulation)
Saline solution = potassium chloride
Iron
Source:
meats
whole grains (commercially prepared breads and cereals are often fortified with iron)
beans
nuts
seeds
green leafy vegetables (spinach, broccoli)
Functions:
binds with hemoglobin in the blood stream (oxygen transport)
Take with vitamin C
Iodine
Sources:
iodized salt
seafood
food additives
Functions
important for thyroid function
Zinc
Sources:
oysters
meats
peas
beans
nuts
Functions:
important for immunity
reduce length of cold when taking zinc
Water
Facts:
accounts for 50% of an adult’s total weight
2/3 of body’s water is contained in the cells
Sources:
beverages (80%)
solid foods (20%)
water intake should be 2-3 liters/day for adults
Functions:
aids in digestion, absorption, circulation, excretion, and metabolism
intake should equal output (fluid balance altered in server dehydration, GI illness, hemorrhage, sever burns, hypovolemia → when plasma is too low)
Promoting optimal intake
Achieve adequate nutrients within energy needs
Maintain calorie balance over time to achieve and sustain a healthy weight
Focus on chiming nutrient dense foods and beverages (whole foods = fruits/vegetables)
Balancing Calories to Manage Weight
control total calorie intake to manage body weight
increase exercise = increase calorie intake
Increase physical activity
go for a walk
track in a watch
increase due to physicians recommendation
Foods & Nutrients to Increase
Increase fruit and vegetable intake
Increase whole-grain intake (replace refined grains)
White bread = bleach added to flour
Wheat bread = more grains and fibers
Increase intake of fat-free/low-fat milk products
Choose a variety of proteins
Increase fiber intake
Choose foods that provide more essential nutrients (potassium, calcium, vitamin D)
Food & Nutrients to Decrease
Decrease daily sodium intake (read food labels, avoid adding salt to meals)
Don’t add extra salt
Less than 2g (200mg) per day
Consume less that 10% of calories from saturated fats
Junk/fast food
Consume less that 300 mg/day of dietary cholesterol
Meat, eggs, dairies
Decrease intake of calories from solid fats and added sugars (fast food, snack foods)
Limit alcohol consumption
Building Healthy Patterns
Select eating pattern that meets nutrient needs
Account for food/beverages: food dairy, health apps
Regular physical activity: at least 150 min/week (or 30 minutes, 5 days a week)
Track activity
Use of appropriate diets
ASSESS!!!
Body Mass Index (BMI)
Weight in kg divided by sure of heath in meter
Provides an estimation of body fat and can be used as an assessment of an individual’s nutritional status
What can produce incorrect BMI’s
athletes
anemia (retaining fluid)
dehydration
high muscle mass
older people
people who have lost muscle mass (ex. cachexia)
Underweight BMI
<18.5
Normal weight BMI
18.5-24.9
Overweight BMI
25-29.9
Obesity BMI
30 or greater
diabetes, hypertension, and types of cancers
Morbid Obesity BMI
>40
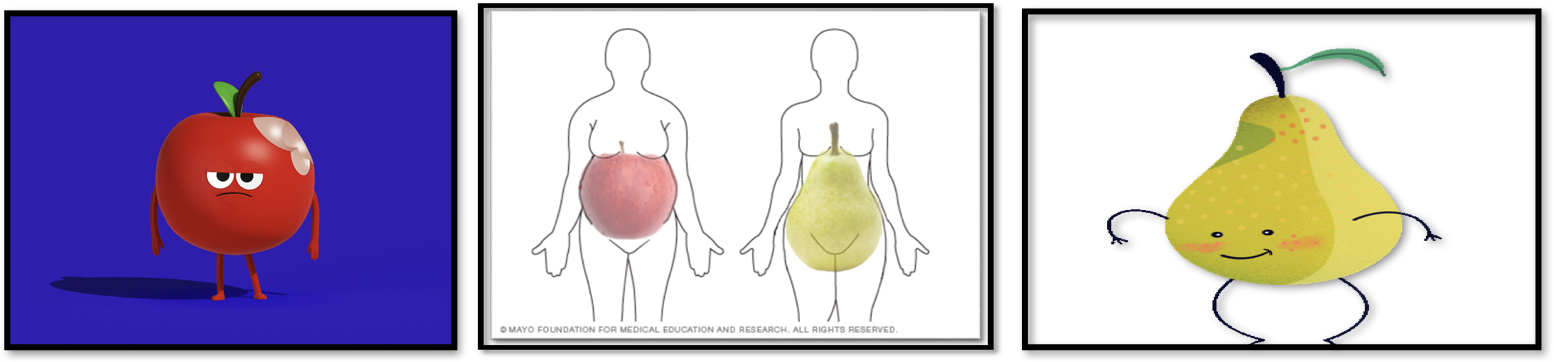
Body Fat Distribution
Apple vs. Pear shape
Apples are at a higher risk then pear
Central obesity (apple): waist circumference of ≥ 40 in men and ≥35 in for women is indicative of increase cardio-metabolic risk (heart disease, diabetes)
Fat covering most abdominal muscles
Obesity
BMI over 30, body weight is over 20% then what it should be
Epidemiology:
More than 20% of adults in the United States are obese
Over 30% of young people (between 2-19) are overweight/obese
Etiology (related factors):
Genetic → parents that are obsess = children are more likely to be obese (how you are grown up)
Environmental → lack of available location to be active
Biochemical → chronic system inflammation and stress
Behavioral → high fat diet, number of calories consumed, lack of exercise
Obesity and Biopychosocial Health Problems
About half of all American adults—117 million individuals—have one or more preventable chronic conditions, many of which are related to poor quality eating patterns and physical inactivity (Examples: Cardiovascular disease, high BP, type 2 diabetes, some cancers, and poor bone health)
Nurses’ role: health promotion and patient/family education
Food/Drug Interactions: Absorption
drugs taken by mouth are absorbed through the lining of the stomach or small intestine
some drugs gave decreased effects when taken with food
review dosage instructions:
“Must be taken on an empty stomach”
administer 30 minutes to 1 hour before or 2 hours after eating
example: thyroid replacement
Food/Drug Interactions: Gastric Irritation
some drugs need to be taken with food to avoid gastric irritation, indigestion, or gastric ulcers
review dosage instruction
“Must be taken with food”
administer during mealtime
examples: aspirin, non-steroidal anti-inflammatory drugs (ibuprofen)
Food/Drug Interactions: Food that Alter Metabolism/Action of Medications
Grapefruit juice:
interferes with the metabolism of certain medications resulting in an increased serum level of the medication
example: cholesterol lowering medication → Atorvastatin (Lipitor)
Foods with Vitamin K (green leafy vegetables):
decrease the anticoagulant effects of blood thinner medication warfarin (Coumadin)
Herbal supplements:
Cause potential interactions with prescribed medication (important to ask patients what over the counter meds/supplements that are taking)