Chapter 23 - Respiratory system Pt.2 A&P ii
1/66
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
Barometric (atmospheric) air pressure
air pressure outside of the body
Intra-alveolar pressure
air pressure in the alveoli
Alveolar Pulmonary Ventilation
occurs during quiet resting
alveolar pressure equals atmospheric pressure, not bc of air movement
What occurs in the alveolar pulmonary ventilation for air to move into the lungs
alveolar pressure is less than atmospheric when the thoracic volume increases (inspiration starts, pressure below atmospheric pressure, approx. -1mm Hg)
What occurs in the alveolar pulmonary ventilation for air to move out of the lungs
alveolar pressure greater than atmospheric, due to a decrease in thoracic volume (during expiration)
What occurs in the alveolar pulmonary ventilation for air to have no movement
Alveolar pressure equates to atmospheric pressure (at end of expiration and inspiration)
Factors that affect alveolar ventilation
lung recoil
elastic recoil (elastic fibers in alveolar walls to return back to their regular shape)
surface tension: film of fluid lines in the alveoli
surfactant: prevents lungs from collapsing by reducing surface tension (produced by type ii pneumocytes)
Disorder in Ventilation: Infant respiratory distress syndrome
common in premature babies because of inadequate surfactant. Usually on oxygen and surfactant (injected or in an endotracheal tube)
What action does negative pleural pressure cause the lungs to do during inspiration?
causes the lungs to expand, pulling them outward like a suction
Ventilation Disorder: Pneumothorax
a positive pleural pressure (air can’t leave), the opening between the pleural cavity and air that causes a loss of pleural pressure, causing the lungs to collapse
Ventilation disorder: Pleural effusion
Abnormal accumulation of fluid in the pleural area, caused by heart failure, infection, or cancer
What is pulmonary edema and what causes it?
excess fluid in the lungs
caused by pneumonia, contact with toxins, medication and cancer
Factors Affecting Diffusion Through the Respiratory Membrane: Partial pressure gradients
gas moves from higher partial pressure to lower partial pressure
normally partial pressure of oxygen is higher in alveoli than blood
Factors Affecting Diffusion Through the Respiratory Membrane: Membrane thickness
The thicker the respiratory membrane, the lower the diffusion rate.
diseases like tuberculosis/pneumonia can increase thickness
Factors Affecting Diffusion Through the Respiratory Membrane: Surface area
decreased surface area decreases diffusion rate
diseases like emphysema/lung cancer can reduce available surface area
Disorder: Black lung
coaler miner’s lung; build up of inhaled coal dust that causes inflammation, fibrosis, and necrosis
Emphysema
A form of COPD caused by smoking, damaging alveolar sacs with CO2 deposits
Adult hemoglobin
one hemoglobin can carry up to four oxygen molecules, boundeed the the heme portion
The 3 ways to transport carbon dioxide
As a bicarbonate (70%) , by transport of hemoglobin (in the amino portion of the globin chains), or transportation in the plasma
Haldane effect
helps uptake/absorption carbon dioxide in the tissues
hemoglobin that has just released oxygen bind more faster to carbon dioxide rather than hemoglobin that has oxygen still attached
How can CO2 negatively impact the blood?
makes it more acidic
Function of the carbonic acid-bicarbonate buffer system
helps blood resist change in ph
how does the carbonic acid-bicarbonate buffer system work if hydrogen (H+) levels in the blood are too high?
Blood pH is too acidic
excess H+ is removed by combining w/ HCO3 to form H2CO3, which separates into CO2 & H2O, which increases CO2 lvls (since H+ makes blood lvls more base, more CO2 increases acidity, returning it to homeostasis)
how does the carbonic acid-bicarbonate buffer system work if hydrogen (H+) levels in the blood are too low?
Blood pH is too basic
Carbonic acid (H2CO3) breaks down into H+ & HCO3-
What is the alkaline reserve of the carbonic acid-bicarbonate buffer system?
HCO3 (Bicarbonate molecule)
How does inspiration rate affect blood ph?
increased inspiration rate lowers CO2 & increases ph, & vice versa
How does the enzyme carbonic anhydrase help in the transportation of CO2 as a bicarbonate ions
reverse catalyzes the production of carbonic acid from carbon dioxide and water
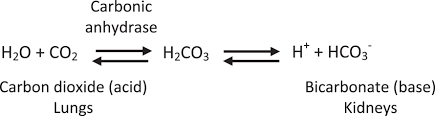
Alveolar Gas Exchange (slide 24)** REVIEW IN SLIDES
Alveolar gas exchange is the passive diffusion of oxygen
from the alveoli into pulmonary capillaries and carbon dioxide from the blood into the alveoli. Driven by partial pressure gradients across the thin respiratory membrane, binds to hemoglobin while it is exhaled, ensuring blood oxygenation and waste removal.
Systemic Gas Exchange (slide 25)** REVIEW IN SLIDES
The diffusion of oxygen from systemic capillaries into tissues and carbon dioxide from tissues into blood. Driven by pressure gradients, it fuels cellular metabolism. This process occurs throughout the body's tissues, distinct from pulmonary gas exchange in the lungs.
Why does the destruction of alveoli in emphysema cause difficulty in breathing?
Lack of surface area
What causes pneumothorax?
hole in pleura due to trauma
Why does a higher percentage of carbon dioxide get carried in plasma vs oxygen?
Carbon dioxide has a higher solubility coefficient, allowing easier dissolvement into the plasma
How is the majority of carbon dioxide carried in the blood?
As a bicarbonate ion
Name the enzyme that RBCs make to convert carbon dioxide and water to carbonic acid
Carbonic anhydrase
Which way does the carbonic acid-bicarbonate buffer shift when there is too many hydrogen ions present? How does the respiratory respond?
Toward more carbon dioxide and respiration increases
What muscles are involved with quiet inspiration and are they relaxed/contracted?
External intercostals and diaphragm/ contracted
Which structure would not be a dead air space in the respiratory system?
Alveoli
Restrictive disease: Pulmonary Fibrosis
loss of elasticity, with scar tissue that covers the lungs, that makes it difficult for inhalation/exhalation
all volumes are reduced- total lung capacity is reduced
Replacement of lung tissue with fibrous connective tissue, making the lungs less elastic; exposure to asbestos or coal dust is a common cause
Obstructive Disease: COPD, Asthma, Pnuemonia
still has elasticity, but the lining of the airway is obstructed
Inhale normally, exhale reduced
-IRV/TV normal
-ERV reduced
-RV increaased
can lead to barrel chest
Disease: COPD
Destruction of alveolar walls; increased coughing increases pressure on the alveoli, causing rupture and destruction; loss of alveoli decreases surface area for gas exchange and decreases the lungs’ ability to expel air; progression can be slowed, but there is no cure; in combination with bronchitis
Caused by long term exposure to irritants. The most common cause is cigarette smoke.
Regulation of Blood CO2: Hypercapnia
medullary chemoreceptors detect CO2 in the blood lvls are too high, making the ph decreased (meaning h+/hydrogen is decreased)
How does the body regulate itself from hypercapnia
the phrenic nerve sends a message to the diaphragm/ other respiratory muscles, causing increased contraction rate, which increases the rate of breathing.
as a result, CO2 is expelled in the lungs, which causes the blood ph to increase
Regulation of blood CO2: Hypocapnia
medullary chemoreceptors detect decrease in CO2, & increase in blood ph (higher hydrogen lvls) in the blood
How does the body regulate itself from hypocapnia
the phrenic nerve sends a msg to the diaphragm and other respiratory muscles and slows the breathing rate, which increases CO2 lvls and decreases ph.
Disease: Bronchitis
Inflammation of the bronchi caused by irritants, such as cigarette smoke or infection; swelling impairs breathing; bronchitis can progress to emphysema
Disease: Dust Pneumonia
occurs when dust particles are inhales in excessive amounts where they cause inflammation and fluid development in
the alveoli. Most notable during the Dust Bowl in the 1930s.
Disease: Tuberculosis
caused by the bacterium Mycobacterium tuberculosis, which forms small, lump-like lesions called tubercles; the immune system targets tubercles and causes larger lesions; certain strains of tuberculosis are resistant to antibiotics
Which gas can be carried dissolved in the blood plasma at a higher concentration because it has a higher solubility coefficient
Carbon dioxide
What area of the brainstem regulates the normal involuntary rhythm of breathing?
ventral respiratory group in the medulla
When pH of a solution is low, what ion is in high concentration?
Hydrogen (H+)
Regulation of pulmonary ventilation: Local Control
management of gas levels by region and not by CNS (ex. piece of lung has cancer & would not get good alveolar ventilation, and would thereby experience vasoconstriction of the alveolar capillaries to reduce blood flow
Regulation of pulmonary ventilation: Neural control
voluntary, regulation occurs during eating/speaking
involuntary, regulation occurs during sleep or performing tasks
What part of the medulla oblongata produces eupnea (normal, involuntary rhythm of breathe)
ventral respiratory group
What part of the medulla oblongata is responsible for recieving input from chemoreceptors/mechanoreceptors/other sources to modify the respiratory rhythm?
Dorsal respiratory group
What part of the brainstem is connected to the medulla respiratory center and plays a role is switching between inspiration and expiration
The pontine respiratory group (pons)
Regulator of pulmonary ventilation: Chemoreceptor function
function: maintains O2, CO2, & pH of the blood
note that carbon monoxide is more important than oxygen as a regulator of the respiration rate
pCO₂
partial pressure of carbon monoxide
Which nerve does the medulla use to regulate breathing
Phrenic nerve
Hypoxia
decrease in oxygen levels below normal values
once pCO₂ lvls drop at least 50% of normal rate, carotid & aortic body chemoreceptors sends msgs to the respiratory to increase inspiration rate
Hering-Bruer Reflex
regulates & monitors the volume of the lungs to prevent over-inflation of the lungs
What is the function of proprioceptors?
movement of the limbs
True or false: When hemoglobin releases a hydrogen ion this increases the affinity of carbon dioxide to the hemoglobin to bind
False - it increases the affinity of oxygen to the hemoglobin to bind
Each hemoglobin molecule can carry how many oxygen molecules?
4
When pH of a solution of a solution is low,
what ion is in high concentration?
H+
What area of the brainstem regulates the normal involuntary rhythm of breathing?
ventral respiratory group
Which gas can be carried dissolved in the blood plasma at a higher concentration because it has a higher solubility coefficient?
Co2
When chemoreceptors in the body detect hypocapnia, what will happen to correct the condition?
decreased respiration rate (hypoventilation)