Cardiac muscle mechanics
1/49
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
50 Terms
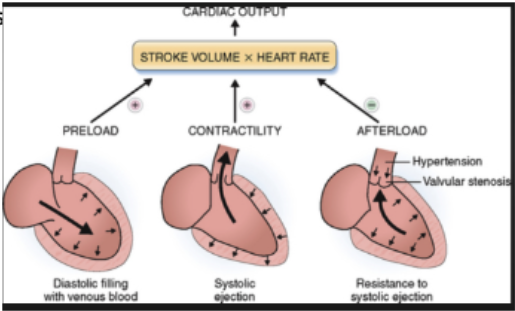
what 3 factors regulate stroke volume?
preload
afterload
contractility (inotropy)
what is preload?
initial stretching of the cardiac myocytes prior to contraction
average ventricular sarcomere length at end of diastole
in the intact heart, sarcomere length is related to …?
the stretch of the ventricular wall
when is ventricular wall stretch at max?
at the end diastolic volume (EDV) or end diastolic pressure (EDP)
what does an increase in either EDV or EDP do?
stretches sarcomeres
increases force of next contraction
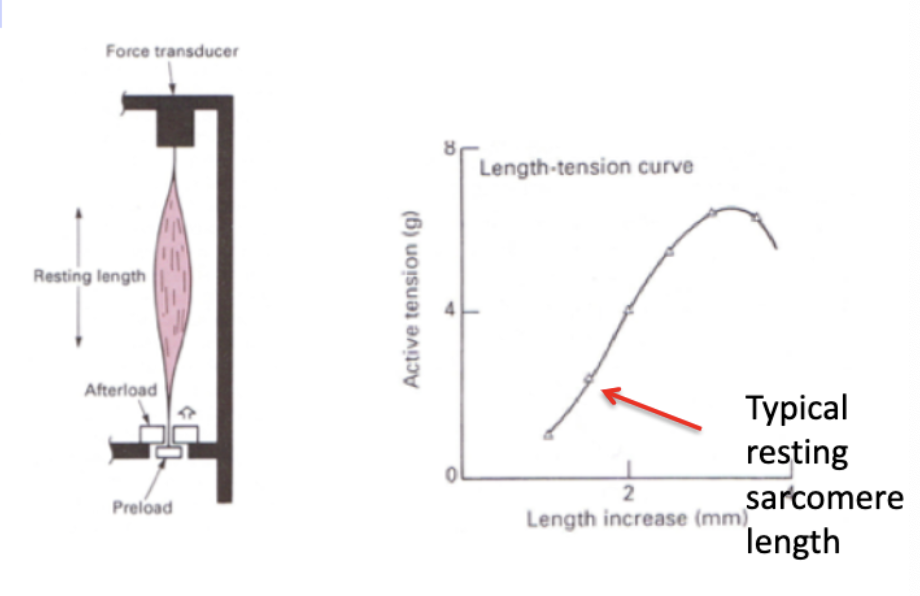
explain the experiment done to demonstrate length-tension relationship in isolated papillary muscle and the effect of changing preload on force development?
initial length of muscle is controlled by adjusting the lower support
length is held constant (isometric) and the active tension is recorded after stimulation
graph shows that increasing length (sarcomere stretch) results in increasing contractile force
up to a point
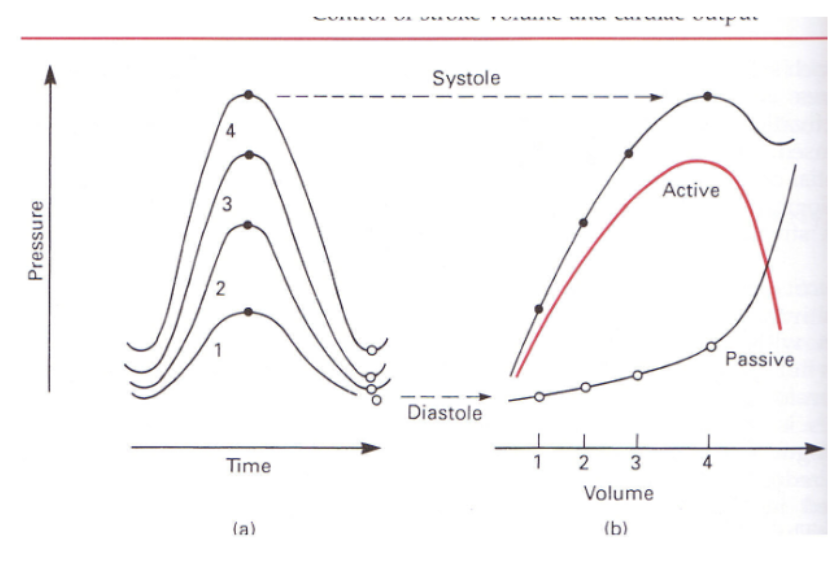
what was Otto Frank’s experiment on intact hearts? what did it demonstrate?
he wanted to study effects of diastolic stretch on contraction
ligated aorta so contractions would be isovolumic
fluid injected into ventricle to stretch walls to varying degrees to stimulate increasing EDV
RESULTS: increases in EDV produced increases in contractile force (similar to results of experiments on papillary muscle
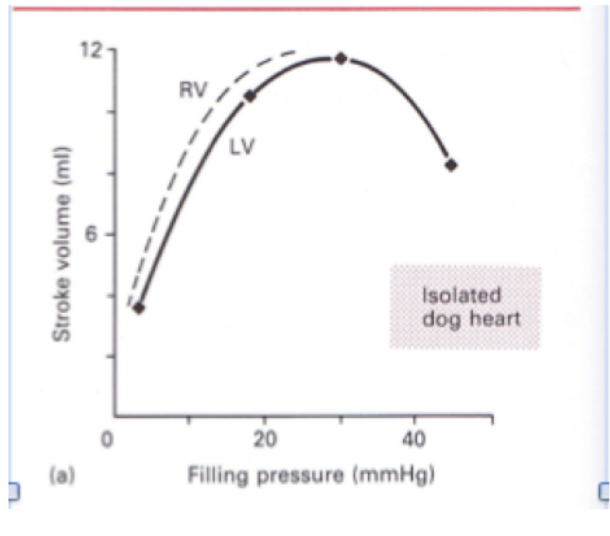
describe Ernest Starling’s experiment on ejecting mammalian hearts. what did it demonstrate?
controlled filling pressure by adjusting the height of a reservoir of blood
RESULT:
increased filling pressure ➙increased EDV or EDP
increased SV at a constant aortic pressure
what is the Frank-Starling Law of the Heart/Frank-Starling Mechanism?
The greater the volume of blood entering the heart during diastole (end-diastolic volume or pressure), the greater the volume of blood ejected during systolic contraction (stroke volume) and vice-versa
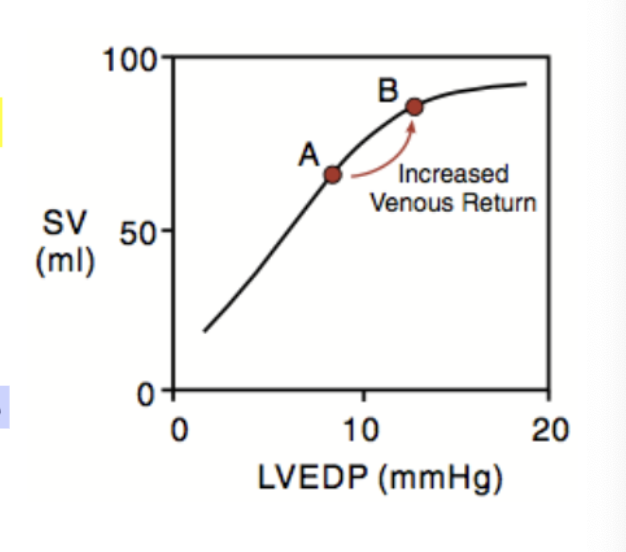
how do you increase EDP/ED?
increasing venous return to the heart (exercise, gravity, etc.)
t/f: stretching a resting cardiac fiber causes an immediate rise in contractile force in the very next contraction
true
what are possible values that can be plotted on the X axis of the Starling curve?
preload
EDV
EDP
sarcomere length
venous return
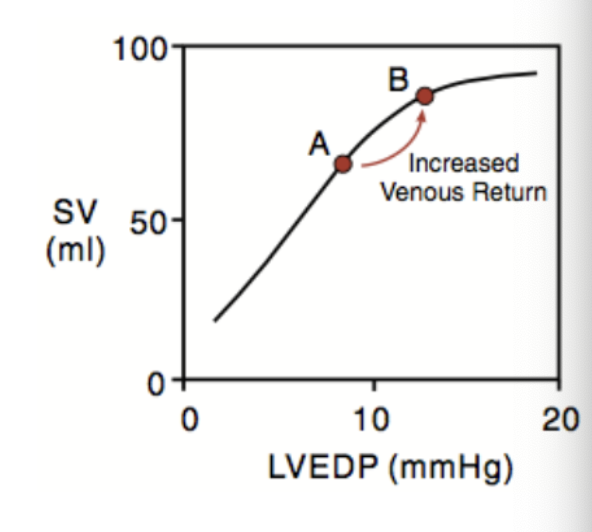
what are possible values that can be plotted on the Y axis of the Starling curve?
contractile force
SV
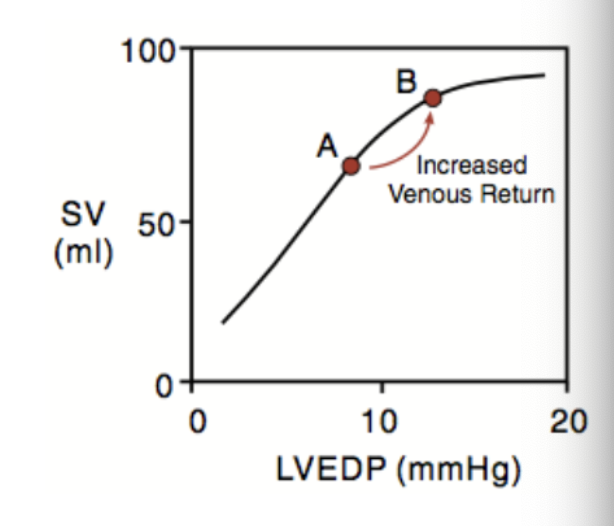
what are the mechanisms underlying Frank-Starling law?
myofilament overlap
length-dependent activation
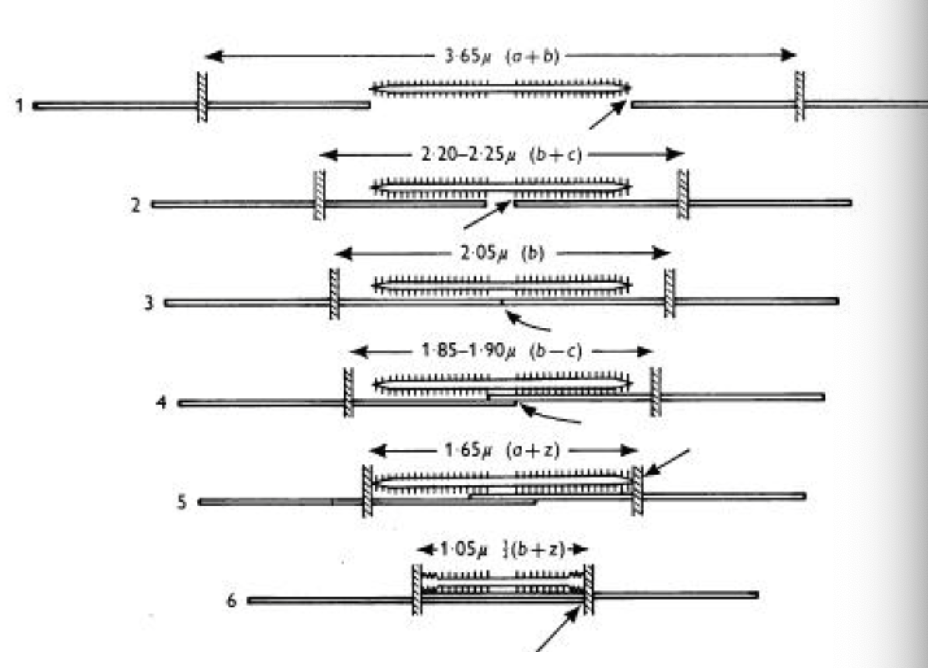
explain the mechanism of myofilament overlap with varying degrees of stretch? (mechanism of Frank-Starling)
• at sarcomere lengths < ~ 2 microm, opposing actin filaments can overlap in the center interfering with crossbridge formation.
• with stretch, the sarcomere lengths allow for more optimal cross-bridge formation.
• with further stretch, the filaments are pulled apart, decreasing overlap and crossbridge formation
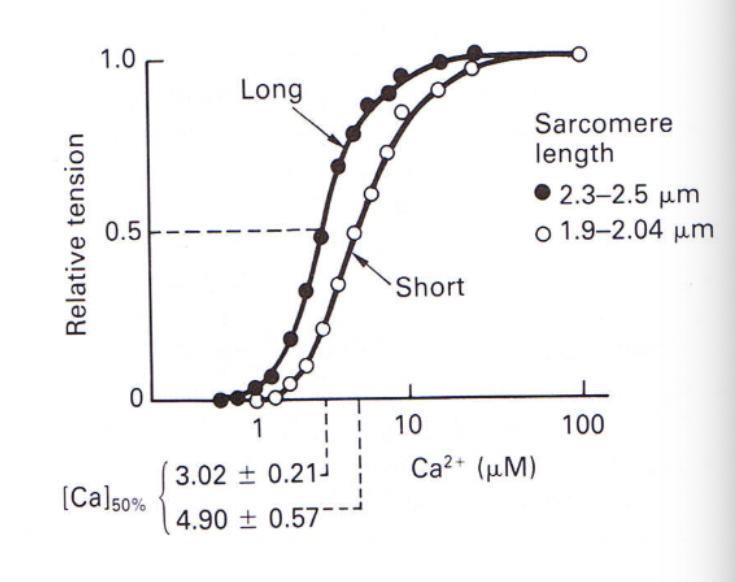
what is length-dependent activation? (mechanism of Frank-Starling)
Stretching the myofibers increases the affinity of troponin C for Ca++ as shown in the binding curves
∴ At longer sarcomere lengths, Ca++ activates more thin filaments at physiological concentrations
preload is affected by compliance changes. what is compliance?
ratio of volume change to pressure change
All ventricles exhibit increasing ________- at higher volumes
“stiffness” (decreasing compliance)
what is the effect of ventricular hypertrophy on cpliance, volume in the ventricle at a given EDP, and sarcomere stretch?
Ventricular hypertrophy decreases compliance and decreases the volume in the ventricle at a given EDP - this decreases sarcomere stretch
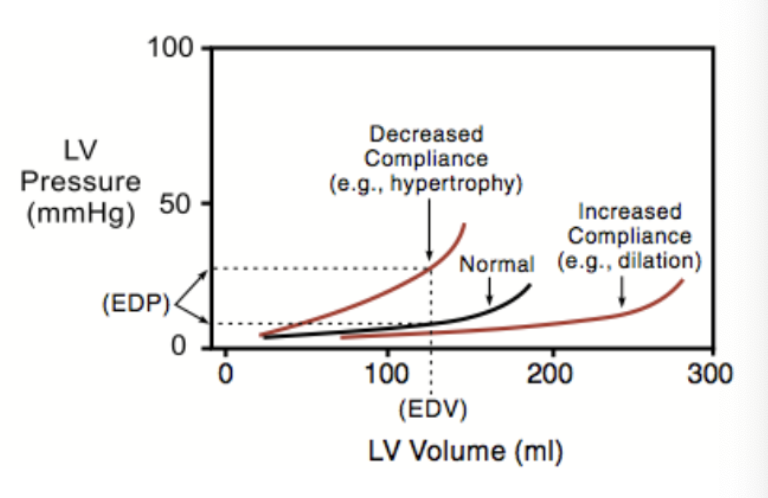
what is the effect of dilation of ventricles due to chronic volume overload on compliance and EDV?
Dilation of ventricles due to chronic volume overload increases compliance and allows a greater EDV at a lower EDP with stretched sarcomeres
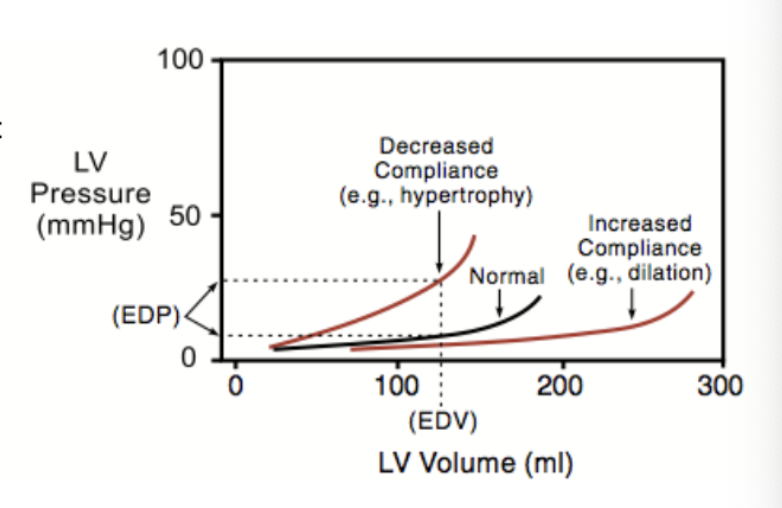
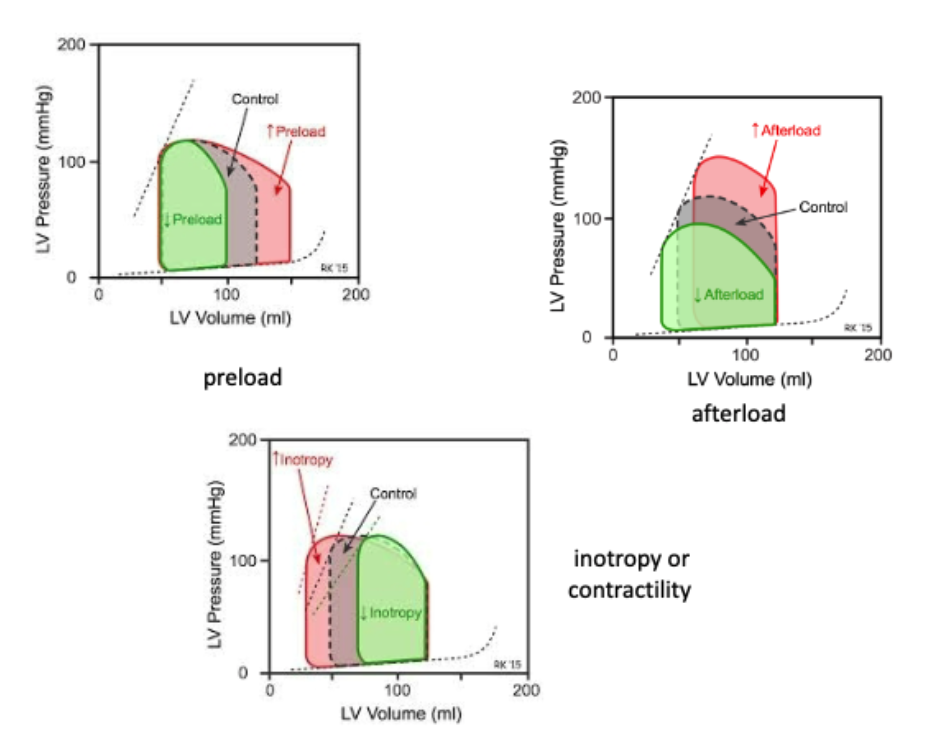
what values are being plotted on a flow volume loop illustrating Frank-Starling regulation of SV? what does it demonstrate?
left ventricular pressure vs volume
increased venous return → increased EDV (preload) → increased SV → invreased ventricular stroke
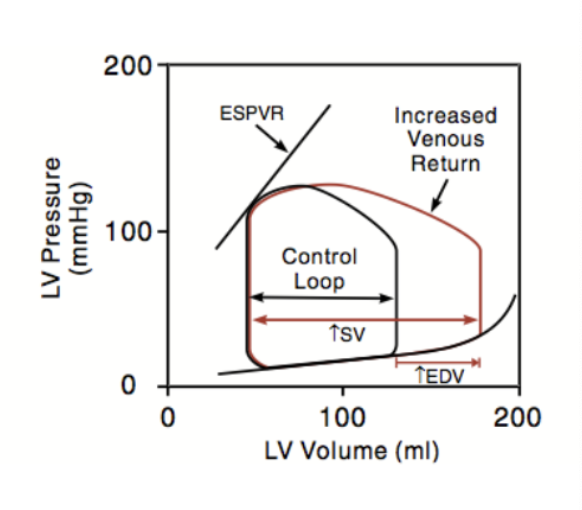
Because preload affects cardiac function by changing the sarcomere length, this type of regulation is called …?
heterometric regulation
in preload, from beat to beat, the heart can adjust its force of contraction to pump the volume of blood that fills it in the previous diastole. the ejected volume will change to give the same ESV by either:
If there is increased venous return, the extra blood over and above the “normal” EDV will be ejected
If there is decreased venous return, the volume ejected will be decreased
what is afterload?
the load against which the heart must contract to eject the blood
what are the major components of afterload?
for the left ventricle, a major component is the aortic pressure
for the right, the pulmonary arterial pressure
ventricular wall stress
o = Pr/h
what is the formula for ventricular wall stress (o)?
o = Pr/h
P: intraventricular pressure
r: radius
h: wall thickness
afterload increases with ________ and decrases with ______
afterload increases with increasing pressure during systole and decreases with ventricular hypertrophy
describe the experiment on papillary muscle done to demonstrate the force-velocity relationship and effects of increasing afterload.
• The papillary muscle is allowed to shorten against varying afterloads
• Y intercept = maximum shortening velocity at 0 (extrapolated) afterload
• With increasing afterload, velocity decreases
• X intercept = the load at which the force cannot lift the loa
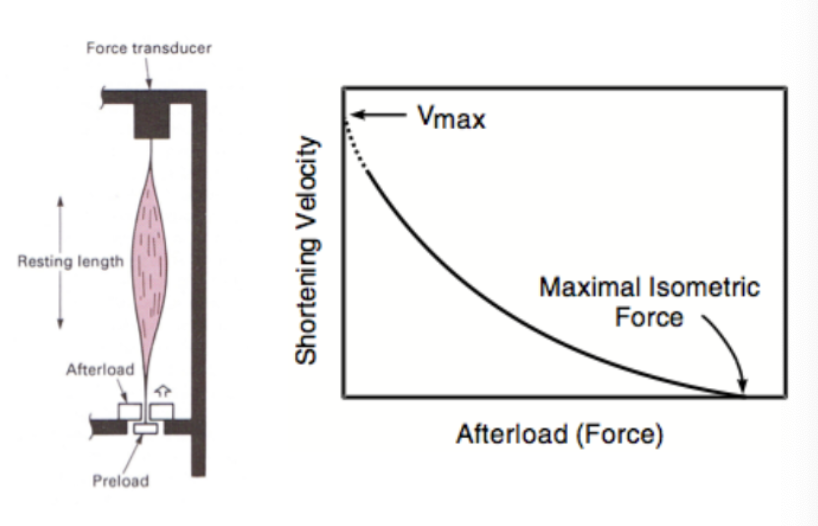
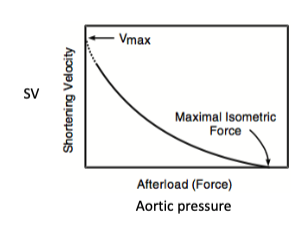
what is the relationship between afterload force (aortic pressure) and shortening velocity (stroke volume)?
greater force (aortic pressure) = slower shortening velocity / less blood being pumped in (stroke volume)
in the intact heart, increasing aortic pressure represents increasing ______
afterload
increased aortic pressure (afterload) increases/decreases the SV
decreases
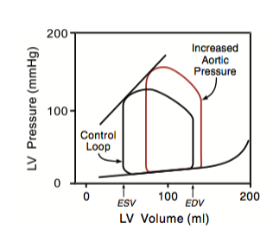
Afterload effects on cardiac perfomance are not a function of sarcomere length and are termed _______
homeometric regulation
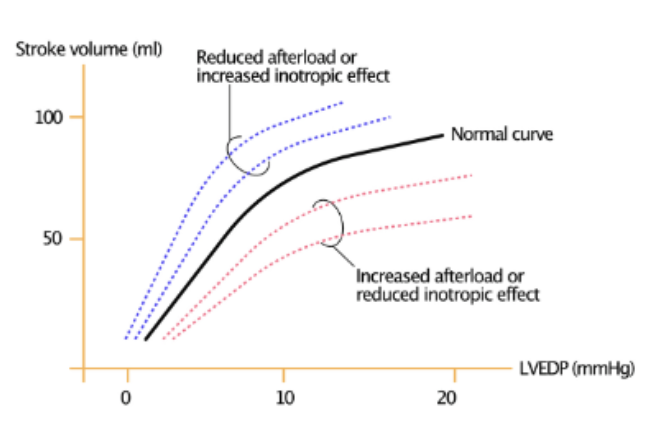
An increase in afterload shifts the Frank-Starling curve in what direction?
downward and to the right– this decreases SV at any preload
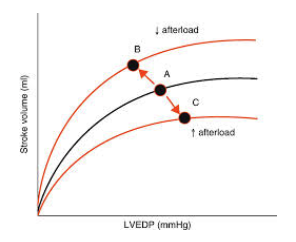
A decreased afterload shifts the F-S curve in what direction?
upward and to the left– this increases SV at any preload
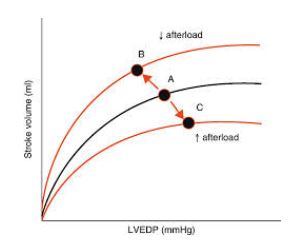
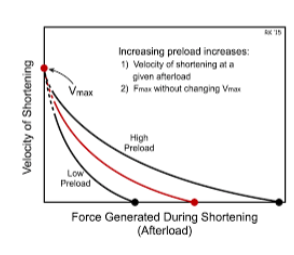
An increase in preload shifts the shortening velocity upward/downward and the X intercept to higher isometric force generatio
upward
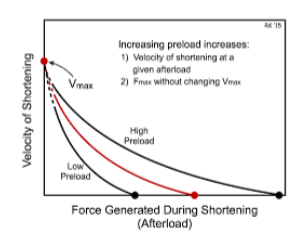
A decrease in preload shifts the velocity upward/downward and the X intercept to lower isometric force
downward
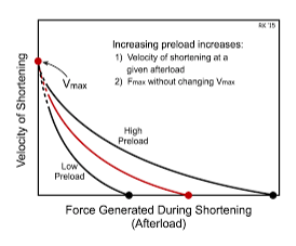
do changes in preload alter Vmax?
no. Changes in preload do not alter Vmax
what is the intrinsic measure of cardiac function independent of extrinsic factors like preload and afterload?
inotropy
what is inotropy related to?
rate of force development during ejection
ESPVR (end-systolic pressure-volume relationship)
how can the inotropic state be increased?
inotropic state is increased by sympathetic stimulation to the heart and by epinephrine released by the adrenal medulla
how can the inotropic state be decreased?
parasympathetic stimulation
how does increased inotropy or decreased afterload affect contractile force?
increased contractile force (stroke volume) at any preload
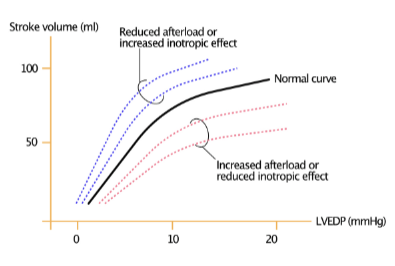
how does decreased inotropy or increased afterload affect contractile force?
decreased contractile force (SV) at any preload
how does increase in intoropy affect velocity of shortening (SV?) how does decrease in intoropy affect velocity of shortening (SV?)
an increase in inotropy increases velocity of shortening (SV) at any afterload
decreased inotropy decreases velocity of shortening at any afterload
how does increase in intoropy affect Vmax? how does decrease in intoropy affect Vmax?
increase in inotropy → increases Vmax
decrease in inotropy → decreases Vmax
Positive inotropic effects result from:
i) Increased rate of delivery of Ca++ to the myofibrils
ii) Increased binding of Ca++ to troponin C
iii) Increased rate of cross-bridge cycling
Inotropic state can be influenced by other factors such as
increased heart rate which can increase intracellular Ca++
loss of inotropy can lead to?
heart failure, cardiomyopathy, ischemia, etc
what drugs can be used clinically to increase inotropy?
digoxin, beta-adrenergic receptor agonists